Abstract
Summary
This cross-sectional study investigated the association between the modified 2006 American Heart Association Diet and Lifestyle Recommendations (AHA-DLR) and bone mineral density in Chinese adults. We found that better adherence to the AHA-DLR associated with higher bone mineral density (BMD) at multiple sites.
Introduction
Accumulating evidence shows that cardiovascular disease (CVD) and osteoporosis are associated with each other, yet little research has focused on whether strategies to reduce CVD risk could also benefit bone health. We aimed to assess the association between adherence to the modified 2006 American Heart Association Diet and Lifestyle Recommendations (AHA-DLR) and BMD in Chinese adults.
Methods
We included 2092 women and 1051 men aged 40–75 years in this community-based cross-sectional study. Dietary information was assessed using a 79-item food frequency survey through face-to-face interviews at baseline (2008–2010) and 3 years later (2011–2013). Adherence to the AHA-DLR was assessed using modified diet and lifestyle scores (American Heart Association Diet and Lifestyle Score (AHA-DLS)) adjusted for bone health. BMD for the whole body, lumbar spine, total hip, femur neck, and trochanter sites was measured using dual-energy X-ray absorptiometry in 2011–2013.
Results
After adjusting for potential covariates, greater adherence to the modified AHA-DLS was positively and dose-dependently associated with BMD. The mean BMD was 1.93–3.11% higher in quartile 4 (vs. 1) (all p values <0.01) at multiple sites. Five-unit increases in the modified AHA-DLS score were associated with 4.20–6.07, 4.44–8.51, and 3.36–4.67 mg/cm2 increases in BMD at multiple sites for the total subjects, males, and females, respectively (all p values <0.01).
Conclusions
Better adherence to the AHA-DLR shows protective associations with BMD at multiple sites in the middle-aged and elderly Chinese population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis and cardiovascular disease (CVD) are two important causes of morbidity and mortality in the elderly. They present great public health challenges worldwide. Rather than being two unrelated diseases exclusively related to age, increasing evidence suggests that these two chronic conditions are associated with each other [1–3], sharing risk factors (e.g., smoking, physical activity, and vitamin D deficiency) [1] and several common pathophysiological mechanisms (e.g., oxidative stress, inflammation, and dyslipidemia) [2, 4]. Epidemiological studies have shown that subjects exposed to either of these two diseases are more likely to suffer a higher risk of the other disorder [5–9]. Evidence has also shown that several approaches, such as the Mediterranean diet, could help prevent both chronic diseases [10–12], and strategies to reduce CVD risk may also benefit bone health.
The 2006, the American Heart Association Diet and Lifestyle Recommendations (AHA-DLR) was released by the AHA to reduce CVD risk in the general population [13]. A total of nine main components make up the AHA-DLR, including balancing caloric intake and physical activity for a healthy body weight; consuming a high-fiber diet rich in vegetables, fruit, whole grain, and fish (especially oily fish); limiting the intake of saturated fat, trans fat, cholesterol, salt, and added sugar; consuming alcohol moderately; and following these principles when eating outside the home [13]. Bhupathiraju et al. developed an original AHA Diet and Lifestyle Score (AHA-DLS) based on the principles of the AHA-DLR [14], with higher scores representing better adherence to the AHA-DLR. They found that higher scores were associated with a better dyslipidemia condition [14], a higher bone mineral density (BMD), and a lower osteoporosis risk (all p values <0.05) in older Puerto Ricans [15]. However, these results were based on a relatively small sample (fewer than 1000) of a particular Hispanic population with health disparities and high-risk factors for both CVD and osteoporosis [16, 17]. More studies of other populations are needed to better understand the problem, but no other studies on this field have been found.
The purpose of this cross-sectional study is to investigate the association between the AHA-DLR and BMD at the whole body, lumbar spine, and hip sites in middle-aged and elderly Chinese.
Methods
Study populations
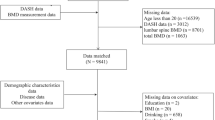
This study is based on the Guangzhou Nutrition and Health Study (GNHS), a community-based prospective cohort study designed to investigate the nutritional determinants of cardiometabolic outcomes and osteoporosis. The study was first conducted between July 2008 and July 2010 (baseline) in urban Guangzhou. Detailed information can be found in previous articles [18]. Briefly, a total of 3169 subjects aged 40–75 years completed the baseline survey, and 2520 of them were retained and completed the same survey and BMD measurements during a 3-year follow-up. At follow-up, 832 subjects were newly recruited and completed the corresponding survey and measurements. After eliminating 209 subjects for the following reasons: (i) a history of serious chronic disease, such as hyperthyroidism or malignancy; (ii) use of related medication for osteoporosis; (iii) core related data missing; and (iv) extreme energy intake (<600 or >3500 kcal/day for women and <800 or >4200 kcal/day for men), a total of 3143 subjects (including 2371 follow-up subjects and 772 newly recruited subjects) provided complete BMD data and surveys and were included in this cross-sectional analysis. Informed consent was obtained from all of the subjects. The Ethics Committee of the School of Public Health at Sun Yat-sen University approved the study.
Measurements and data collection
During both the baseline and the follow-up, we invited subjects to the School of Public Health at Sun Yat-sen University for the relevant measurements and face-to-face interviews. A structured questionnaire survey was conducted to collect information related to demographics (e.g., age, gender, marital status, household income, education status), lifestyle factors (e.g., smoking, drinking, physical activity), history of disease and medications, and habitual dietary intake and use of calcium supplements. Physical activity was measured and translated into MET h/day as described previously [19]. Height and weight were measured with the subjects in light clothes and no shoes, and body mass index (BMI, using kg/m2) was then calculated.
Assessment of dietary intake
Dietary information was collected using a prevalidated 79-item food frequency questionnaire (FFQ) [20]. The subjects were asked to report the approximate frequencies and portion sizes of the foods they consumed during the preceding year based on provided pictures. The average daily intake of total energy and specific nutrients was then calculated according to the China Food Composition Table 2002 [21]. Trans fatty acids were calculated based on the research data available for the Chinese diet in China [22], and added sugars were calculated from major sources of sugars in the food categories of sugars, cakes, and sugar-sweetened beverages. The average values were calculated for the 2342 subjects who provided both baseline and follow-up dietary data, and only one kind of dietary data was provided and used in the analysis of the 801 new subjects.
American Heart Association Diet and Lifestyle Scores
The 2006 AHA-DLR were released by the AHA to reduce the CVD risk in Americans over 2 years of age. The AHA-DLS was calculated as in a previous article [14] except for the following. We assigned sodium intake a score of 0–10 according to the participants’ urinary sodium/creatinine (Na/Cr, mmol/mmol) levels because of a lack of dietary sodium data. Scores ranging from a minimum of 0 to maximums of 4, 6, and 10 were assigned to subjects according to their adherence to each of the subcomponents. Because BMD is strongly affected by weight, the modified AHA-DLS excluded the BMI components from the original scales, and we further adjusted it in the statistical analyses. The highest possible score for the modified AHA-DLS was 100, where a higher score represented better adherence to the AHA-DLR.
Assessment of bone mineral density
During the follow-up (2011–2013), the subjects’ BMD (g/cm2) at the whole body (WB), lumbar spine (LS), total hip (TH), femur neck (FN), and trochanter (TR) was measured using dual-energy X-ray absorptiometry (DXA) (Discovery W, Hologic Inc., Waltham, MA, USA) and analyzed with Hologic Discovery software version 3.2. The in vivo coefficients of variation of the duplicated BMD measurements in 30 subjects after repositioning were 1.18% (WB), 0.87% (LS), 1.02% (TH), 1.92% (FN), and 1.82% (TR). The long-term CV of the measurements was 0.26%, a value found by testing the phantom daily between March 2011 and May 2015.
Statistical analysis
Common characteristics were presented as means and standard deviations (SDs) for the continuous variables and as frequencies and percentages for the categorical variables. All of the analyses were performed with SPSS 17.0 for Windows (SPSS, Inc., Chicago, USA).
Subjects with a higher total energy intake tended to have a higher intake of nutrients, so we adjusted the modified AHA-DLS for total energy intake using the residual method [23]. We assessed the associations between the modified AHA-DLS—both as a continuous (five-unit increases) measure and as a categorical (sex-specific energy-adjusted quartiles) measure—and BMD by using general linear regression and analysis of covariance (ANCOVA). Two covariance models were used in all analyses with model I adjusted for age and sex and model II further adjusted for BMI, marital status, education, household income, smoking status, calcium supplement use, and daily total energy intake and dietary calcium intake (calcium from AHA-DLR components was excluded). Stratified analyses were performed according to gender, and years since menopause and use of estrogen were added as factors for females only. Bonferroni tests were conducted to make multiple comparisons between quartiles.
We also assessed the associations between each of the modified AHA-DLS subcomponents (one-unit increases) in the linear regression. Analyses were adjusted for the covariates in model II.
Results
Our study included 2092 women and 1051 men (Table 1). The mean (SD) age was 59.7 (5.5) years for women (95.4% of whom were postmenopausal) and 62.4 (6.5) years for men. Subjects with higher modified energy-adjusted AHA-DLS scores tended to be younger, to have a lower BMI and higher dietary calcium intake, were more likely to use calcium supplements, and smoked less (all p trends <0.01).
Higher modified AHA-DLS scores were positively and dose-dependently associated with 1.84–2.61% higher BMD (quartile 4 vs. 1, all p values <0.01) at all of the bone sites after adjusting for age and gender in the total subjects (Table 2). The associations were strengthened when other variables (e.g., BMI, education, smoking) were further adjusted for in model II (all p trends <0.001). The BMD values were 1.93–3.11% higher in the top (vs. bottom) quartiles of the modified AHA-DLS (all p values <0.001). Similar associations were found in both women and men (p interactions 0.118–0.395) (Table 3).
In the linear regression models, after adjusting for potential covariates, every five-unit increase in the AHA-DLS score was associated with 4.20–6.07, 4.44–8.51, and 3.36–4.67 mg/cm2 higher BMD at different bone sites for the total subjects, men, and women, respectively (all p values <0.05) (Table 4). For the subcomponent analyses, higher scores for physical activity, fruit and vegetables, whole grains, fish, and urinary Na/Cr levels and lower scores for dietary saturated fat and cholesterol were associated with a higher BMD at several bone sites after adjusting for the potential covariates (all p values <0.05) (Table 5).
Discussion
In this community-based cross-sectional study, we observed a favorable association between higher modified AHA-DLS scores and BMD at multiple sites in middle-aged and elderly Chinese adults. Previous studies suggested that one SD decrease in the total hip BMD was associated with an 85% (95% CI, 70–101%) increase in the risk of total osteoporotic fractures [24]. Therefore, a 0.021 g/cm2 (or 0.18 and 0.19 SDs for men and women) higher BMD at the total hip in quartile 4 (vs. 1) of AHA-DLS score in our study would be associated with a 15.4–15.9% decrease in osteoporotic fractures in future. Our findings suggest that the AHA-DLR, which was first introduced to reduce CVD risk, could also benefit bone health in this population.
An increasing number of epidemiological studies support a close biological relationship between osteoporosis and CVD [5–7], although whether the strategies conducted specifically for CVD prevention could also benefit bone health has received less attention. To our knowledge, there is only one direct study in this field whose results are consistent with ours. A five-unit increase in the modified AHA-DLS score was associated with a 0.005–0.008 g/cm2 higher BMD and lower risk (OR, 0.83–0.96, all p values <0.05) for osteoporosis/osteopenia at both the femur and lumbar spine sites in 933 Puerto Ricans aged 47–79 years [15]. Nevertheless, our results are consistent with those of several other studies that focused on healthy dietary patterns with similar principles. For instance, the Mediterranean diet (which is characterized by a higher intake of fiber, fruits and vegetables, and fish; moderate drinking; and limited saturated fat intake), which first received attention for CVD protection, was also associated with lower hip fracture incidence in 48,814 men and 139,981 women at a follow-up in the EPIC study 9 years later [11] and was also associated with a higher calcareous bone BMD (p trend = 0.001) in a cross-sectional study of 200 Spanish women [25]. In addition, increasing evidence suggests that the Dietary Approaches to Stop Hypertension (DASH) diet (which is characterized by a higher intake of high-fiber grains, vegetables, and fruits and restrained intake of fat and cholesterol) might also benefit bone health by blocking the bone resorption process [26, 27]. These results highlight the possibility of addressing two major public health problems with a single set of guidelines.
In the subcomponent analysis, after adjusting for potential covariates, a higher level of physical activity was associated with a higher BMD at all bone sites (all p values <0.001). This favorable association is consistent with the results of previous studies. More vigorous physical activity was associated with a higher femur neck BMD (β = 0.09, p < 0.001) in a cross-sectional study of 1228 70-year-old Swedish subjects [28] and a 39% lower risk of hip fractures (95% CI, 0.54–0.69) in a meta-analysis of 1,235,768 subjects [29]. The positive association between a higher intake of fruits and vegetables, whole grains, fish, and sodium restriction and BMD found in our study is consistent with previous studies [30–33], which reinforces the role of nutrition in protecting bone health. However, higher scores (a lower intake) for saturated fat and cholesterol were associated with a lower BMD at several hip sites. These results are in conflict with several former studies that found detrimental associations with bone health [34, 35]. More studies are needed to clarify the issue. Nevertheless, a positive association with BMD was found at all bone sites when dietary subcomponents were combined. Our results reinforce the importance of combining positive exercise and diet to better protect bone health.
Previous evidence suggests that several important biological mechanisms of CVD [36], including oxidative stress, inflammation (e.g., C-reaction protein (CRP) and interleukin-6 (IL-6)), and dyslipidemia, also play important roles in the development of osteoporosis by inhibiting the osteoblastic bone formation process and promoting osteoclast bone resorption [37–40]. Although few direct data were found, the favorable association of AHA-DLR with BMD might stem from several components that mitigate these detrimental factors. Increased physical activity was inversely associated with a lower risk of elevated CRP in 14,461 American adults [41] and positively associated with an increase in total antioxidant capacity (TAC) in 3042 Greek adults [42]. The greater Mediterranean diet score, which shares several components with AHA-DLR, was associated with lower levels of blood CRP and IL-6 in a meta-analysis of randomized clinical trials (RCT) [43] and with greater TAC in Greek adults [42]. Better adherence to the DASH diet and sodium reduction improved the serum profile of CRP and glutathione in an RCT [44] and decreased bone turnover markers, such as serum osteocalcin and the C-terminal telopeptide of type I collagen, in another RCT of 186 adults [26]. These results suggest an association between the AHA-DLR and these mechanisms, although further interventional studies are needed to identify the causal relationship.
The strength of this study is that we examined the association between the AHA-DLR and BMD at multiple sites using a large sample size. In addition, the dietary data averages for the majority of our population were used for analysis, providing a better estimation of habitual dietary intake. However, our study has several limitations. First, the cross-sectional design cannot identify a causal relationship, although we used the average values of dietary intake to better estimate habitual consumption over the period before the BMD assessment, attenuating the possibility of causal inversion in the majority of the subjects. Second, dietary calcium was adjusted for in the analysis for a more prudent consideration, which might have resulted in an excessive correction and underestimation of the association, although we excluded calcium from the AHA-DLR components in the analysis. Nevertheless, positive results were still observed at most bone sites. Third, blood vitamin D status of the participants was not available for the adjustments in the analyses of this study, which might increase the possibility of residual confounding. Finally, the subjects, who were recruited as volunteers, might have led healthier lifestyles or engaged in more healthy activities, which might attenuate the positive association. However, health-related factors, such as education and economic status, smoking, and the use of calcium supplements, did not significantly modify the AHA-DLR–BMD association (p interaction range 0.069–0.993).
In conclusion, we observed that better adherence to the AHA-DLR (as indicated by a higher modified AHA-DLS score) was favorably associated with BMD at multiple sites in middle-aged and elderly Chinese. Our results support the hypothesis that strategies to reduce the CVD risk might also benefit bone health and that a single set of guidelines might thus contribute to the prevention of these two major public problems.
References
Lello S, Capozzi A, Scambia G (2015) Osteoporosis and cardiovascular disease: an update. Gynecol Endocrinol 31:590–594
Lampropoulos CE, Papaioannou I, D’Cruz DP (2012) Osteoporosis—a risk factor for cardiovascular disease. Nat Rev Rheumatol 8:587–598
Makovey J, Macara M, Chen JS, Hayward CS, March L, Sambrook PN (2013) High osteoporotic fracture risk and CVD risk co-exist in postmenopausal women. Bone 52:120–125
Crepaldi G, Maggi S (2009) Epidemiologic link between osteoporosis and cardiovascular disease. J Endocrinol Investig 32:2–5
Tanko LB, Christiansen C, Cox DA, Geiger MJ, McNabb MA, Cummings SR (2005) Relationship between osteoporosis and cardiovascular disease in postmenopausal women. J Bone Miner Res 20:1912–1920
Farhat GN, Newman AB, Sutton-Tyrrell K, Matthews KA, Boudreau R, Schwartz AV, Harris T, Tylavsky F, Visser M, Cauley JA (2007) The association of bone mineral density measures with incident cardiovascular disease in older adults. Osteoporos Int 18:999–1008
Lai SW, Liao KF, Lai HC, Tsai PY, Lin CL, Chen PC, Sung FC (2013) Risk of major osteoporotic fracture after cardiovascular disease: a population-based cohort study in Taiwan. J Epidemiol 23:109–114
Shen C, Deng J, Zhou R, Chen J, Fan S, Li Z, Hu Y, Zhong Q (2012) Relation between bone mineral density, bone loss and the risk of cardiovascular disease in a Chinese cohort. Am J Cardiol 110:1138–1142
Sennerby U, Melhus H, Gedeborg R, Byberg L, Garmo H, Ahlbom A, Pedersen NL, Michaelsson K (2009) Cardiovascular diseases and risk of hip fracture. JAMA 302:1666–1673
Fung TT, Rexrode KM, Mantzoros CS, Manson JE, Willett WC, Hu FB (2009) Mediterranean diet and incidence of and mortality from coronary heart disease and stroke in women. Circulation 119:1093–1100
Benetou V, Orfanos P, Pettersson-Kymmer U et al (2013) Mediterranean diet and incidence of hip fractures in a European cohort. Osteoporos Int 24:1587–1598
Bamia C, Lagiou P, Buckland G et al (2013) Mediterranean diet and colorectal cancer risk: results from a European cohort. Eur J Epidemiol 28:317–328
Lichtenstein AH, Appel LJ, Brands M et al (2006) Diet and lifestyle recommendations revision 2006: a scientific statement from the American Heart Association nutrition committee. Circulation 114:82–96
Bhupathiraju SN, Lichtenstein AH, Dawson-Hughes B, Tucker KL (2011) Adherence index based on the AHA 2006 diet and lifestyle recommendations is associated with select cardiovascular disease risk factors in older Puerto Ricans. J Nutr 141:460–469
Bhupathiraju SN, Lichtenstein AH, Dawson-Hughes B, Hannan MT, Tucker KL (2013) Adherence to the 2006 American Heart Association diet and lifestyle recommendations for cardiovascular disease risk reduction is associated with bone health in older Puerto Ricans. Am J Clin Nutr 98:1309–1316
Lloyd-Jones D, Adams RJ, Brown TM et al (2010) Heart disease and stroke statistics—2010 update: a report from the American Heart Association. Circulation 121:e46–e215
Tucker KL, Falcon LM, Bianchi LA, Cacho E, Bermudez OI (2000) Self-reported prevalence and health correlates of functional limitation among Massachusetts elderly Puerto Ricans, Dominicans, and non-Hispanic white neighborhood comparison group. J Gerontol A Biol Sci Med Sci 55:M90–M97
Chen GD, Zhu YY, Cao Y, Liu J, Shi WQ, Liu ZM, Chen YM (2015) Association of dietary consumption and serum levels of vitamin a and beta-carotene with bone mineral density in Chinese adults. Bone 79:110–115
Zhang ZQ, Deng J, He LP, Ling WH, Su YX, Chen YM (2013) Comparison of various anthropometric and body fat indices in identifying cardiometabolic disturbances in Chinese men and women. PLoS One 8:e70893
Zhang CX, Ho SC (2009) Validity and reproducibility of a food frequency questionnaire among Chinese women in Guangdong province. Asia Pac J Clin Nutr 18:240–250
Yang YX, Wang G, Pan X (2002) China food composition table. Peking University Medical Press, Beijing
Liu DM (2008) Analysis of isomers of trans fatty acids in food and investigation of the consumption of trans fatty acids in Chinese. Dissertation, Nanchang University
Brown CC, Kipnis V, Freedman LS, Hartman AM, Schatzkin A, Wacholder S (1994) Energy adjustment methods for nutritional epidemiology: the effect of categorization. Am J Epidemiol 139:323–338
Leslie WD, Lix LM, Tsang JF, Caetano PA (2007) Single-site vs multisite bone density measurement for fracture prediction. Arch Intern Med 167:1641–1647
Rivas A, Romero A, Mariscal-Arcas M, Monteagudo C, Feriche B, Lorenzo ML, Olea F (2013) Mediterranean diet and bone mineral density in two age groups of women. Int J Food Sci Nutr 64:155–161
Lin PH, Ginty F, Appel LJ, Aickin M, Bohannon A, Garnero P, Barclay D, Svetkey LP (2003) The DASH diet and sodium reduction improve markers of bone turnover and calcium metabolism in adults. J Nutr 133:3130–3136
Doyle L, Cashman KD (2003) The effect of nutrient profiles of the dietary approaches to stop hypertension (DASH) diets on blood pressure and bone metabolism and composition in normotensive and hypertensive rats. Br J Nutr 89:713–724
Johansson J, Nordstrom A, Nordstrom P (2015) Objectively measured physical activity is associated with parameters of bone in 70-year-old men and women. Bone 81:72–79
Qu X, Zhang X, Zhai Z, Li H, Liu X, Liu G, Zhu Z, Hao Y, Dai K (2014) Association between physical activity and risk of fracture. J Bone Miner Res 29:202–211
Park SM, Joung JY, Cho YY, Sohn SY, Hur KY, Kim JH, Kim SW, Chung JH, Lee MK, Min YK (2015) Effect of high dietary sodium on bone turnover markers and urinary calcium excretion in Korean postmenopausal women with low bone mass. Eur J Clin Nutr 69:361–366
Shin S, Sung J, Joung H (2015) A fruit, milk and whole grain dietary pattern is positively associated with bone mineral density in Korean healthy adults. Eur J Clin Nutr 69(4):442–448
Chen YM, Ho SC, Woo JL (2006) Greater fruit and vegetable intake is associated with increased bone mass among postmenopausal Chinese women. Br J Nutr 96:745–751
Farina EK, Kiel DP, Roubenoff R, Schaefer EJ, Cupples LA, Tucker KL (2011) Protective effects of fish intake and interactive effects of long-chain polyunsaturated fatty acid intakes on hip bone mineral density in older adults: the Framingham osteoporosis study. Am J Clin Nutr 93:1142–1151
Corwin RL, Hartman TJ, Maczuga SA, Graubard BI (2006) Dietary saturated fat intake is inversely associated with bone density in humans: analysis of NHANES III. J Nutr 136:159–165
Jeong TD, Lee W, Choi SE, Kim JS, Kim HK, Bae SJ, Chun S, Min WK (2014) Relationship between serum total cholesterol level and serum biochemical bone turnover markers in healthy pre- and postmenopausal women. Biomed Res Int 2014:398397
Mangge H, Becker K, Fuchs D, Gostner JM (2014) Antioxidants, inflammation and cardiovascular disease. World J Cardiol 6:462–477
Mundy GR (2007) Osteoporosis and inflammation. Nutr Rev 65:S147–S151
Wilson C (2014) Bone: oxidative stress and osteoporosis. Nat Rev Endocrinol 10:3
Tarakida A, Iino K, Abe K, Taniguchi R, Higuchi T, Mizunuma H, Nakaji S (2011) Hypercholesterolemia accelerates bone loss in postmenopausal women. Climacteric 14:105–111
Yamaguchi T, Sugimoto T, Yano S, Yamauchi M, Sowa H, Chen Q, Chihara K (2002) Plasma lipids and osteoporosis in postmenopausal women. Endocr J 49:211–217
Richardson MR, Boyer WR, Johnson TM, Churilla JR (2015) Vigorous intensity physical activity and C-reactive protein in U.S. adults. Metab Syndr Relat Disord 13:453–457
Kavouras SA, Panagiotakos DB, Pitsavos C, Chrysohoou C, Arnaoutis G, Skoumas Y, Stefanadis C (2010) Physical activity and adherence to Mediterranean diet increase Total antioxidant capacity: the ATTICA study. Cardiol Res Pract 2011:248626
Schwingshackl L, Hoffmann G (2014) Mediterranean dietary pattern, inflammation and endothelial function: a systematic review and meta-analysis of intervention trials. Nutr Metab Cardiovasc Dis 24:929–939
Razavi Zade M, Telkabadi MH, Bahmani F, Salehi B, Farshbaf S, Asemi Z (2016) The effects of DASH diet on weight loss and metabolic status in adults with non-alcoholic fatty liver disease: a randomized clinical trial. Liver Int 36(4):563–571
Acknowledgements
This study was jointly supported by the National Natural Science Foundation of China (81472965, 81130052), the 5010 Program for Clinical Researches (No. 2007032) of the Sun Yat-sen University (Guangzhou, China), and Danone Institute China Diet Nutrition Research & Communication Grant in 2012.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
None.
Additional information
Geng-dong Chen and Ding Ding contributed equally to this article
Rights and permissions
About this article
Cite this article
Chen, G.D., Ding, D., Tian, H.Y. et al. Adherence to the 2006 American Heart Association’s Diet and Lifestyle Recommendations for cardiovascular disease risk reduction is associated with bone mineral density in older Chinese. Osteoporos Int 28, 1295–1303 (2017). https://doi.org/10.1007/s00198-016-3857-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3857-3