Abstract
Purpose
The purpose of the present study was to investigate the effect of the unloader brace on medial compartment dynamic joint space (DJS) during gait, while simultaneously recording ground reaction force (GRF) in varus knee osteoarthritis (OA) patients using a highly accurate biplane radiography system which allowed continuous measurement of DJS from heel strike through the midstance phase of gait. The hypothesis was that DJS in the medial compartment would be greater with the unloader brace than without the brace during gait.
Methods
After 2 weeks of daily use of the unloader brace, ten varus knee OA patients (age 52 ± 8 years) walked with and without the brace on an instrumented treadmill, while biplane radiographs of the OA knees were acquired at 100 Hz. Medial compartment DJS was determined from heel strike to terminal stance (0–40% of the gait cycle) using a validated volumetric model-based tracking process that matches subject-specific 3D bone models to the biplane radiographs. The GRF during gait was collected at 1000 Hz. Repeated-measures ANOVA was used to explore differences in medial compartment DJS and GRF between the unbraced and braced conditions. A patient-reported subjective questionnaire related to the brace use was collected at the time of the test.
Results
Medial compartment DJS was significantly greater with the unloader brace than without the brace during gait (P = 0.005). The average difference was 0.3 mm (95% confidence interval 0.1–0.4 mm). No significant difference was observed in terms of vertical GRF between the two conditions. The questionnaire showed participants felt reduced pain when wearing the brace.
Conclusion
The unloader brace has the significant effect of increasing medial compartment DJS during gait, which supports the underlying premise that the unloader brace reduces pain by increasing medial joint space during dynamic loading activities.
Level of evidence
III.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Knee osteoarthritis (OA) most frequently involves the medial compartment of the tibiofemoral (TF) joint. Unloader braces are intended to reduce pain and improve function by unloading the medial compartment of the TF joint in varus knee OA patients [14]. A recent meta-analysis of randomized trials suggests that unloader bracing can provide small-to-moderate improvements in pain and function [16].
Multiple mechanisms by which the unloader braces alter knee joint biomechanics have been proposed [15]. These mechanisms include altering the distribution of the load and decreasing knee adduction moment, increasing joint stability and TF joint space of the medial compartment, lessening muscle co-contraction, and improving proprioception [4, 6, 15, 19,20,21,22,23, 25]. Although a systematic review and meta-analysis has suggested that the unloader braces can alter knee joint loads through a combination of mechanisms [15], controversy still exists as to whether the brace has the real effect of increasing TF joint space in the medial compartment during functional activity [6, 9, 11, 13, 18]. Some studies have shown that the brace increased joint space [6, 13, 18], but others have shown no significant effect of the brace on the joint space [9, 11]. Furthermore, these previous studies which investigated TF joint space width [6, 9, 11, 13, 18] have not reported ground reaction forces (GRF) with and without the brace, which could be a confounding factor affecting knee joint loading and hence medial compartment joint space. TF joint space narrowing has been shown to be associated with greater knee pain [17, 24]: thus, it is of importance to assess the change of joint space with and without the unloader brace.
Therefore, the purpose of the present study was to investigate the effect of an unloader brace on dynamic joint space during gait in medial compartment in OA patients while simultaneously recording GRF. While most of these previous studies [6, 11, 13, 18] measured medial condyle separation at only specific points in the gait cycle (i.e., heel strike, midstance, toe-off) using a two-dimensional fluoroscopic analysis, the novelty of the present study was to measure the dynamic joint space in the medial compartment continuously over the stance phase of gait using a highly accurate biplane radiography system with three-dimensional sub-millimeter accuracy [1]. The hypothesis was that dynamic joint space in the medial compartment would be greater with the unloader brace than without the brace during gait.
Materials and methods
Ten subjects (8 male/2 female, age 52 ± 8 years; range 39–63) with symptomatic knee OA primarily in one limb were enrolled in this study. They had a mean body mass index of 27.1 ± 4.2 kg/m2 and a mean weight-bearing femorotibial angle of 180.1° ± 2.5°. According to the Kellgren/Lawrence grading scale [12], two subjects had grade I, five subjects had grade II, and three subjects had grade III knee OA of the medial TF compartment. Inclusion criteria were: age of 35–65 years, OA affected primarily one knee, and 10° or less varus knee alignment. Exclusion criteria were ligament instability, a history of tibial or femoral fracture, previous knee surgery, cardiovascular disease, diabetes, neurological impairment or impaired balance, rheumatoid arthritis, previous large radiation exposure, current pregnancy, or knee injection within the previous 6 months. Each subject was provided with a custom-made unloader brace (Defiance, DJO Inc.) and received instruction on brace fitting by a trained orthotist. After a minimum 2 weeks of documented daily brace use of at least 2 h per day, a single test session was performed. The accommodation period was set before the test for the subjects to become accustomed to the brace.
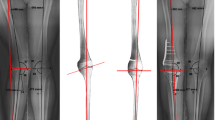
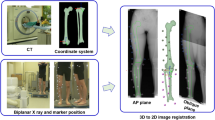
Dynamic in vivo kinematic data collection and processing was performed after allowing participants to become comfortable in the laboratory setting and practice waking on the treadmill. Subjects walked (1.0 m/s) on an instrumented treadmill (Bertec corp., Columbus, OH, USA) with and without the brace. The subjects wore the brace with the setting they had become accustomed to over the 2-week accommodation period. Three trials were collected for each condition (unbraced and braced), and average data of the three trials were used for the analysis. The order of with and without the brace was randomized among the subjects. During the walking trials, biplane radiographs of OA knees were acquired at 100 frames/s with radiographic settings of 80 kVp, 125 mA, and 1 ms duration pulsed exposures. The custom biplane radiography system was vertically configured to eliminate obstruction by the metal brace (Fig. 1a). Radiographs were collected shortly before the heel strike through the push-off phase. Heel strike was detected using the vertical GRF signal from the dual-belt instrumented treadmill, collected at 1000 Hz. Bone geometry was determined from a high-resolution computed tomography (CT) scan (approximately, 0.52 × 0.52 × 0.52 mm voxels). Tibiofemoral motion was determined from the biplane radiographs from initial contact to terminal stance phase (gait cycle 0–40%) using a previously validated model-based tracking process (Fig. 1b) [1]. The accuracy of this bone tracking system has been validated during in vivo running to be 0.3 ± 0.1 mm, 0.4 ± 0.2 mm, and 0.7 ± 0.2 mm in the medial–lateral, proximal–distal, and anterior–posterior directions, respectively, and to be 0.9° ± 0.3°, 0.6° ± 0.3°, and 0.3° ± 0.1° for flexion–extension, external–internal rotation, and abduction–adduction, respectively [1]. Variability in bone motion tracking by different operators is very small (0.02 mm in translation and 0.06° in rotation) [2] because the final matching process is performed by a computer algorithm. Six degree-of-freedom rotations of the tibia relative to the femur were calculated for each trial using the conventions proposed by Grood and Suntay [8]. Raw data were filtered at 10 Hz using a fourth-order Butterworth filter to calculate joint kinematics in an anatomical coordinate system.
Configuration of the dynamic stereo X-ray (DSX) system. a The biplane radiography system was vertically configured to eliminate obstruction by the metal brace, and subjects walked with one foot on each tread of an instrumented treadmill. b Calculation of tibiofemoral motion using a validated model-based tracking process
Calculation of dynamic medial joint space
Dynamic joint space in the medial compartment was measured based on a previously reported method [3]. Briefly, the medial tibial plateau was divided into nine sub-regions and the average minimum distance between femur and tibia subchondral bone was calculated in each region (Fig. 2). The region with the smallest joint space over the three walking trials was selected for the analysis (the region 5 in 9 out of 10 subjects). The data from one subject were excluded from the 20–40% of the gait cycle joint space analysis because the knee was out of the field of the biplane radiographs.
Medial compartment regions used to calculate the dynamic joint space. a The medial tibial plateau was divided into nine sub-regions, and the average joint space in each region was obtained over every 10% of the gait cycle. b The average joint space measurement from 0 to 10% of the gait cycle from one subject. The region with the smallest joint space (region 5 in 9/10 subjects) was selected for the analysis
Calculation of GRF during gait
Ground reaction forces during gait were collected by the instrumented treadmill at 1000 Hz and normalized by each subject’s body weight. Output parameters were averaged over 10% intervals of the gait cycle. Data from 0 to 40% of the gait cycle (heel strike to terminal stance) were included in the analysis (Fig. 3). The GRF data from two subjects (different from the subjects who was excluded from dynamic joint space measurement) were excluded from the GRF analysis, because the GRF data were not recorded in one subject and in another subject because the feet did not land entirely on separate force plates.
Questionnaires
Participants kept daily logs of brace use, documenting activities and duration of use each day. A patient-reported subjective questionnaire related to the brace use was collected at the time of the test.
The study was approved by the University of Pittsburgh institutional review board (ID: PRO08060104), and all subjects provided informed consent before enrollment.
Statistical analysis
Statistical analyses were performed using SPSS software v25.0 (IBM Software Group, Chicago, IL, USA). Two-way repeated measures ANOVA (gait cycle × brace condition) was used to explore differences in medial compartment dynamic joint space and vertical GRF between the two conditions (unbraced and braced). When significant main effects were found, post hoc paired t tests with Holm–Bonferroni correction [10] identified the differences between the two conditions during corresponding gait cycle periods. The significance level was set as P < 0.05. Using a sample size of ten participants, 80% power, and a correlation between repeated measurements of 0.7, the study was powered to detect an effect size of Cohen f = 0.31, which is a medium to large effect (0.25–0.40) [5].
Results
The dynamic joint space in the medial compartment was significantly greater with the unloader brace than without the brace during gait (P = 0.005; Figs. 4a, 5). During the first 10% of the gait cycle, the difference in dynamic joint space between braced and unbraced was the greatest. The average difference between the two conditions was 0.3 mm (95% confidence interval 0.1–0.4 mm). No significant difference was observed in terms of vertical GRF between the unbraced and braced conditions (n.s; Fig. 4b).
a Medial compartment dynamic joint space and b vertical ground reaction forces during gait in the unbraced and braced conditions. Data are shown as mean ± 1 standard error. a Medial dynamic joint space with and without the brace. Asterisk indicates significant differences between conditions when accounting for multiple comparisons. b No significant difference was observed in ground reaction forces between the two conditions. Note the error bars indicate among-subject variability; however, statistical analysis was performed using within-subject comparisons. n.s. not significant
The questionnaire showed participants felt reduced pain and were comfortable when wearing the brace, which allowed them to perform activities that were painful without the brace (Table 1).
Discussion
The main finding of this study was that the unloader knee brace induced a small (0.3 mm on average), but significant increase in medial compartment dynamic joint space during gait, supporting the hypothesis. The increase of medial compartment joint space when wearing the brace was consistent from heel strike to terminal stance. Considering that the minimum joint space is between 2 and 3 mm during the impact phase of gait for these OA patients (Fig. 4a), the 0.25 mm increase corresponds to roughly a 10% increase in medial compartment joint space when wearing the brace during gait. No significant differences in vertical GRF during gait were found between the unbraced and braced conditions. It is important to note that the testing conditions replicated real-life use of the brace. The subjects wore the brace with the setting they had become accustomed to over the 2-week accommodation period, not an extreme setting that could have induced additional medial compartment joint space, but would have been intolerable over an extended period of use. Moreover, the subjective questionnaire indicated that participants felt reduced pain and were comfortable when wearing the brace. Although a multitude of factors affect patients’ subjective feelings, the current study supports the underlying premise that unloader braces decrease pain by increasing the joint space in the medial compartment in varus knee OA patients. This is an important observation because identifying the mechanism(s) by which OA unloader braces affect patient pain and function provides a basis for improving brace design and patient care. By identifying and quantifying this mechanism by which the OA brace improves pain and function, this study provides confidence to surgeons that prescribing the brace to OA patients can lead to real changes in joint mechanics that improve pain and function.
The present finding supports previous results that demonstrated the unloader brace significantly increased the joint space in the medial compartment [6, 13, 18]. As a limitation, these previous studies measured medial condyle separation at only specific points in the gait cycle (i.e., heel strike, midstance, toe-off) using a two-dimensional fluoroscopic analysis. In contrast, the present study measured the dynamic joint space in the medial compartment continuously over the stance phase of the gait using highly accurate biplane radiography system with three-dimensional sub-millimeter accuracy [1].
Some previous studies have reported no significant difference in medial compartment joint space between unbraced and braced conditions [9, 11]. One possible explanation for the discrepancy between the current results and previous findings, such as by Horlick et al. [11], is that they utilized a two-dimensional measurement using anterior–posterior plain radiograph during standing. This type of measurement is less precise than the current measurement technique and does not account for dynamic changes in joint space during gait. On the other hand, Haladick et al. [9] used a similar biplane radiography system and found bracing had no effect on medial compartment joint space. A possible explanation for the discrepancy is that Haladick et al. evaluated the minimum distance at one geometric point between the femur and tibia, while the averaged dynamic joint space was evaluated within a sub-region of area in the current study.
Another limitation of all of these previous studies which measured medial joint space [6, 9, 11, 13, 18] was that they did not report the GRF with and without the brace, which could be a cofounding factor affecting joint space. Duivenvoorden et al. [7] demonstrated no significant difference in vertical GRF and knee adduction moment between the braced and unbraced conditions; however, they did not assess the joint space in the medial compartment which is a more direct measurement than knee adduction moment. The novelty of the present study is that it is the first study to investigate both joint space measurement and vertical GRF with and without bracing during gait. No significant differences in vertical GRF during gait were found between unbraced and braced conditions, suggesting that in the present study the increase of medial compartment joint space was not due to decreased external limb loading during gait while wearing a brace. Additionally, as demonstrated by the present data, the joint space in the medial compartment decreased as the vertical GRF increased (Fig. 4). This demonstrates the importance of recording external loads when assessing the joint space during dynamic functional activities.
Some limitations in the present study should be noted. First, the small sample size may have precluded identifying some true differences (type II error), especially in relation to the GRF analysis which excluded two subjects. However, in spite of the small sample size, a significant difference was identified in the present study, suggesting the measurement technique and tested activity were sufficient to identify the dynamic joint space changes in the medial compartment that occurred in knee OA patients. Second, only one type of unloader brace was used in the present study; thus, results may differ with a different design and fit of the unloader brace. Third, the mechanical axis of the lower limb was not evaluated using long-film radiographs. Fourth, the valgus angle of the brace was not uniform and depended upon each subject. However, the subjects wore the brace with the setting they had become accustomed to, thus this brace setting replicated real-life use of the brace. Finally, the conclusions are only applicable to the level walking activity tested. Although walking is the most common functional activity for the knee, the effects of OA unloader braces during other common activities of daily living remain to be determined.
The clinical relevance of the current findings is clear. The unloader knee brace induced a small, but significant increase in medial compartment dynamic joint space during gait, and the subjects felt reduced pain when wearing the brace. By identifying and quantifying this mechanism by which the OA brace improves pain and function, this study provides confidence to surgeons that prescribing the brace to OA patients can lead to real changes in joint mechanics that improve pain and function.
Conclusion
The unloader knee brace induced a small but significant increase in medial compartment dynamic joint space during gait, while no significant differences were found in vertical GRF during gait, suggesting that the increase of medial joint space with bracing was not due to decreased external limb loading during gait. The subjects felt reduced pain when wearing the brace. By identifying and quantifying this mechanism by which the OA brace improves pain and function, this study provides confidence to surgeons that prescribing the brace to OA patients can lead to real changes in joint mechanics that improve pain and function.
References
Anderst W, Zauel R, Bishop J, Demps E, Tashman S (2009) Validation of three-dimensional model-based tibio-femoral tracking during running. Med Eng Phys 31(1):10–16
Anderst WJ, Baillargeon E, Donaldson WF III, Lee JY, Kang JD (2011) Validation of a noninvasive technique to precisely measure in vivo three-dimensional cervical spine movement. Spine (Phila Pa 1976) 36(6):E393–E400
Anderst WJ, Tashman S (2003) A method to estimate in vivo dynamic articular surface interaction. J Biomech 36(9):1291–1299
Briem K, Ramsey DK (2013) The role of bracing. Sports Med Arthrosc 21(1):11–17
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Erlbaum, Hillsdale
Dennis DA, Komistek RD, Nadaud MC, Mahfouz M (2006) Evaluation of off-loading braces for treatment of unicompartmental knee arthrosis. J Arthroplast 21(4 Suppl 1):2–8
Duivenvoorden T, van Raaij TM, Horemans HL, Brouwer RW, Bos PK, Bierma-Zeinstra SM, Verhaar JA, Reijman M (2015) Do laterally wedged insoles or valgus braces unload the medial compartment of the knee in patients with osteoarthritis? Clin Orthop Relat Res 473(1):265–274
Grood ES, Suntay WJ (1983) A joint coordinate system for the clinical description of three-dimensional motions: application to the knee. J Biomech Eng 105(2):136–144
Haladik JA, Vasileff WK, Peltz CD, Lock TR, Bey MJ (2014) Bracing improves clinical outcomes but does not affect the medial knee joint space in osteoarthritic patients during gait. Knee Surg Sports Traumatol Arthrosc 22(11):2715–2720
Holm S (1979) A simple sequentially rejective multiple test procedure. Scand J Stat 6(2):65–70
Horlick SG, Loomer RL (1993) Valgus knee bracing for medical gonarthrosis. Clin J Sport Med 3(4):251–255
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16(4):494–502
Komistek RD, Dennis DA, Northcut EJ, Wood A, Parker AW, Traina SM (1999) An in vivo analysis of the effectiveness of the osteoarthritic knee brace during heel-strike of gait. J Arthroplast 14(6):738–742
Minzlaff P, Saier T, Brucker PU, Haller B, Imhoff AB, Hinterwimmer S (2015) Valgus bracing in symptomatic varus malalignment for testing the expectable “unloading effect” following valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 23(7):1964–1970
Moyer RF, Birmingham TB, Bryant DM, Giffin JR, Marriott KA, Leitch KM (2015) Biomechanical effects of valgus knee bracing: a systematic review and meta-analysis. Osteoarthr Cartil 23(2):178–188
Moyer RF, Birmingham TB, Bryant DM, Giffin JR, Marriott KA, Leitch KM (2015) Valgus bracing for knee osteoarthritis: a meta-analysis of randomized trials. Arthritis Care Res (Hoboken) 67(4):493–501
Muraki S, Oka H, Akune T, Mabuchi A, En-yo Y, Yoshida M, Saika A, Suzuki T, Yoshida H, Ishibashi H, Yamamoto S, Nakamura K, Kawaguchi H, Yoshimura N (2009) Prevalence of radiographic knee osteoarthritis and its association with knee pain in the elderly of Japanese population-based cohorts: the ROAD study. Osteoarthr Cartil 17(9):1137–1143
Nadaud MC, Komistek RD, Mahfouz MR, Dennis DA, Anderle MR (2005) In vivo three-dimensional determination of the effectiveness of the osteoarthritic knee brace: a multiple brace analysis. J Bone Jt Surg Am 87(Suppl 2):114–119
Pollo FE, Otis JC, Backus SI, Warren RF, Wickiewicz TL (2002) Reduction of medial compartment loads with valgus bracing of the osteoarthritic knee. Am J Sports Med 30(3):414–421
Ramsey DK, Briem K, Axe MJ, Snyder-Mackler L (2007) A mechanical theory for the effectiveness of bracing for medial compartment osteoarthritis of the knee. J Bone Joint Surg Am 89(11):2398–2407
Ramsey DK, Russell ME (2009) Unloader braces for medial compartment knee osteoarthritis: implications on mediating progression. Sports Health 1(5):416–426
Reeves ND, Bowling FL (2011) Conservative biomechanical strategies for knee osteoarthritis. Nat Rev Rheumatol 7(2):113–122
Richards JD, Sanchez-Ballester J, Jones RK, Darke N, Livingstone BN (2005) A comparison of knee braces during walking for the treatment of osteoarthritis of the medial compartment of the knee. J Bone Jt Surg Br 87(7):937–939
Sasaki E, Tsuda E, Yamamoto Y, Maeda S, Inoue R, Chiba D, Okubo N, Takahashi I, Nakaji S, Ishibashi Y (2014) Nocturnal knee pain increases with the severity of knee osteoarthritis, disturbing patient sleep quality. Arthritis Care Res (Hoboken) 66(7):1027–1032
Segal NA (2012) Bracing and orthoses: a review of efficacy and mechanical effects for tibiofemoral osteoarthritis. PM R 4(5 Suppl):S89–S96
Funding
University of Pittsburgh received a research grant from DJO, Inc. DJO also provided the Defiance braces used for the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest in association with the present study.
Ethical approval
The institutional review board (IRB) for human subject research in University of Pittsburgh approved all aspects of this study (ID: PRO08060104).
Informed consent
Informed consent was obtained from all patients before the enrollment.
Rights and permissions
About this article
Cite this article
Nagai, K., Yang, S., Fu, F.H. et al. Unloader knee brace increases medial compartment joint space during gait in knee osteoarthritis patients. Knee Surg Sports Traumatol Arthrosc 27, 2354–2360 (2019). https://doi.org/10.1007/s00167-018-5274-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5274-y