Abstract
Purpose
Unlike postoperative changes in posterior tibial slope after medial open-wedge high tibial osteotomy, sagittal osteotomy inclination has not been examined. It has been recommended that the osteotomy line in the sagittal plane be parallel to the medial posterior tibial slope. The purpose of this study was to determine the frequency of parallel osteotomy in medial open-wedge high tibial osteotomy.
Methods
To determine the sagittal osteotomy inclination, the angle between the medial joint line and the osteotomy line was measured in the lateral radiograph. A positive angle value indicates that the osteotomy is anteriorly inclined relative to the medial posterior tibial slope. Correlation between the sagittal osteotomy inclination and posterior tibial slope was also evaluated.
Results
The mean sagittal osteotomy inclination was 15.1 ± 7.5°. The majority 87.1 % of knees showed an anterior-inclined osteotomy. There was a significantly positive correlation between the postoperative posterior tibial slope and the sagittal osteotomy inclination (r, 0.33; 95 % confidence interval (CI) 0.19–0.46; P < 0.001). The postoperative change in posterior tibial slope also showed a significantly positive correlation with the sagittal osteotomy inclination (r, 0.35; 95 % CI 0.21–0.47; P < 0.001).
Conclusion
Although parallel osteotomy in the sagittal plane relative to the medial joint line was planned, only 12.9 % of cases achieved osteotomy parallel to the medial posterior tibial slope in the sagittal plane. Because of high rate of the anterior-inclined osteotomy and their correlations with posterior tibial slope, surgeons should make all efforts to perform parallel osteotomy relative to medial posterior tibial slope.
Level of evidence
IV
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Many favourable results for medial open-wedge high tibial osteotomy (OWHTO) have recently been reported [1, 21, 32, 33]. The most important aim of medial OWHTO is to achieve balanced load sharing between the medial and lateral compartments by correcting the varus deformity of the knee [24, 32, 38]. However, in addition to an alignment change in the coronal plane to achieve load distribution, one of the possible adverse results of medial OWHTO is a change in sagittal alignment; previous studies have reported that the posterior tibial slope (PTS) can be increased after medial OWHTO [10, 11, 24, 30, 32]. To prevent an increase in the postoperative PTS (Post-PTS) compared with the preoperative PTS (Pre-PTS), it is recommended that the anterior distraction of the medial opening gap be smaller than the posterior distraction; in fact, the anterior distraction should ideally be 50–66 % of the posterior distraction [5, 22, 36].
Unlike postoperative changes in PTS after medial OWHTO, osteotomy inclination in the sagittal plane has not been examined. It is recommended that the osteotomy line in the sagittal plane be parallel to the medial PTS [2, 4, 6, 27, 32, 38]. Miller et al. [27] stated that parallel osteotomy in the sagittal plane is required to avoid inadvertent alteration of the native tibial posterior slope. A concise review by Amendola asserted that the osteotomy inclination in the sagittal plane is critical and should mimic the proximal tibial joint slope to avoid a very thin proximal posterior bony fragment [2, 32]. With the true anteroposterior (AP) view of the medial tibial plateau under an image intensifier, the two overlapping Kirschner wires, which represent the starting line of the osteotomy, can be used to obtain a parallel osteotomy relative to the medial PTS [23, 24, 38]. However, lateral radiographs of medial OWHTO in previous studies showed a sagittal osteotomy inclination that was not parallel to the medial PTS [8–11, 19, 20, 26, 31, 34, 35, 39, 40]. The anterior-inclined osteotomy (AIO) was defined as an osteotomy slope that was anteriorly inclined relative to the medial tibial slope (Fig. 1). As was the case with the lateral radiographs in previous studies, AIO was frequently found than parallel osteotomy on postoperative lateral radiographs of the knees. Concerning the discriminative points of our report, this report is the first to describe the sagittal osteotomy inclination during medial OWHTO. It seems to be imperative to inform other orthopaedic surgeons of this phenomenon because inappropriately inclined osteotomy in the sagittal plane may have an influence on PTS and its changes.
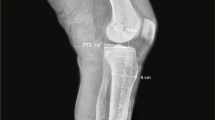
a Using the posterior cortical line as the anatomical reference line, the posterior tibial slope (PTS) was measured on lateral radiographs of the knees. For the measurement of osteotomy inclination, the angle between the medial joint line and the osteotomy line, the lowest line of the proximal segment, was measured from the lateral radiograph of the knee; this measure is the sagittal obliquity of osteotomy relative to medial joint line (SOOJ). b The anterior-inclined osteotomy, parallel osteotomy and posterior-inclined osteotomy were defined as an SOOJ more than 5°, between 5° and −5°, and less than −5°, respectively
The main purpose of the present study was to reveal the frequency of parallel osteotomy in medial OWHTO using postoperative lateral radiographs. Although Miller et al. [27] noted that parallel osteotomy in medial OWHTO is mandatory to prevent inadvertent PTS alteration, hypothesis of the current report is that sagittal osteotomy inclination has no significant correlation with radiological parameters, such as PTS.
Materials and methods
The current study was performed in a single institution (Veterans Health Service Medical Center, Seoul, South Korea). Medical records and radiographs of the patients who underwent medial OWHTO performed by the senior author (JRY) between 2008 and 2014 were reviewed, retrospectively. Indications for medial OWHTO were as follows: symptomatic medial joint osteoarthritis, varus aligned knee with more than 5° of mechanical tibio-femoral angle, near-normal range of motion (<10° of flexion contracture), medium-to-high level of activity, and healthy lateral and patellofemoral compartments. Patients who underwent medial OWHTO and those with apparent and visible osteotomy lines on the postoperative lateral radiographs of their knees were included in the study. In 21 knees, the osteotomy line was too obscure to measure or too curved, usually convexly downward, to be defined as a line. Therefore, these knees were not included in the study. Exclusion criteria were as follows: (1) previous knee surgery before medial OWHTO and (2) concomitant surgery for the ligamentous structures. After the application of these criteria, 136 patients (66 men, 70 women; 170 knees) were included. The mean patient age was 57.7 years [standard deviation (SD) 9.8; range 20–74]. The mean body mass index was 26.3 kg/m2 (SD 3.4). Among the 170 knees, 82 (48.2 %) right knees and 88 (51.8 %) left knees were subjected to surgery.
Surgical procedure
Preoperative planning (aimed angle of correction and amount of distraction) of medial OWHTO was as same as previous recommendations using the Fujisawa point (a lateral point 62 % from the most medial point of the tibial plateau) and Miniaci method [15, 17, 18, 24, 25, 28].
An oblique skin incision was made from the posteromedial corner of the proximal tibia to the insertion site of the pes anserine tendon. The superior third of the pes anserine tendon was detached from the tibial cortex using an electrocautery device. Next, subperiosteal elevation of the superficial medial collateral ligament was performed. Through this subperiosteal space, a Hohmann retractor was inserted along the posterior cortex of the proximal tibia to protect the neurovascular structure within the popliteal fossa. With the knee fully extended, a true AP view of the tibial plateau was taken using the image intensifier. A Kirschner wire was placed from the medial tibial cortex to the lateral cortical hinge point. The starting point of the first wire was approximately 2 cm medial to the medial border of the tibial tuberosity and just above the insertion of the pes anserine tendon. This wire was approximately 3–4 cm below the medial joint line. Under fluoroscopy, a second Kirschner wire was inserted parallel to the first wire. The second wire was located 2 cm posteromedial to the first wire. These wires determined the line of the horizontal osteotomy, which should be parallel to the inclination of the tibial slope in the sagittal plane [2, 4, 27, 38]. The intraosseous lengths of the two wires were measured, and the same length was marked on the oscillating saw.
The horizontal osteotomy was performed just below the two Kirschner wires with the knee flexed to 90°. Using the previously marked depth on the saw and fluoroscopic images, horizontal osteotomy was performed up to 1 cm medial to the lateral tibial cortex. Ascending osteotomy was followed. With the three-chisel technique, the horizontal osteotomy was gradually opened [38]. The desired correction angle was achieved, and the osteotomy gap was maintained with two laminar spreaders. Using the image intensifier, the appropriate mechanical axis of the lower extremity was checked with a long alignment rod or the cable of the electrocautery device.
The medial tibia was fixed using four different fixation plates. In 60 knees (35.3 %), the Decisive Wedge Locking Plate® (Tradimedics Co., Gwangju, Korea) was utilized, and in 51 knees (30.0 %) the TomoFix™ Medial High Tibial Plate (Synthes, Solothurn, Switzerland) was used. The Aescula Open Wedge Plate® (B. Braun-Aesculap, Melsungen, Germany) and OhtoFix Plate® (Ohtomedical Co., Goyang, Korea) were used for 34 knees (20.0 %) and 25 knees (14.7 %), respectively [16]. To maintain the Pre-PTS, the height of the anterior gap of the osteotomy was 60–70 % that of the posterior gap [5, 36]. The remaining steps of medial OWHTO and postoperative management were as described in the previous technical notes [23, 24, 38].
Radiological evaluation
Standing AP and lateral radiographs were taken of the entire lower extremities and knees. As we described earlier, a standing AP radiograph of the entire lower extremity was used to estimate the correction angle. In the same radiograph, pre- and postoperative hip–knee–ankle (HKA) angles were measured (Pre- and Post-HKA, respectively). Using the posterior cortical line as the anatomical reference line, Pre- and Post-PTS were measured on lateral radiographs of the knees [41]. The difference between Post- and Pre-PTS (PrePost-PTS) was also calculated. A positive value indicates an increase in PTS after medial OWHTO. All postoperative measurements were taken 2 weeks after surgery. To measure osteotomy inclination in the sagittal plane, the angle between the medial joint line and the osteotomy line, which was the lowest line of the proximal bony segment, was measured from the lateral radiograph of the knee; this measure was the sagittal obliquity of the osteotomy relative to the medial joint line (SOOJ) (Fig. 1).
A positive SOOJ value indicated that the anterior portion of the osteotomy was distally inclined relative to the medial joint line. As shown in Fig. 1, the AIO, parallel osteotomy and posterior-inclined osteotomy (PIO) were defined as an SOOJ more than 5°, between 5° and −5°, and less than −5°, respectively. Because no knees had PIO, the cases were divided into Group P (parallel osteotomy) and Group A (AIO). All measurements were performed twice in a 2-week period by two independent orthopaedic surgeons (SYL and SHY). Because there could have been an error in measuring of the SOOJ on a plain radiograph, the SOOJ on an X-ray (SOOJ-X ray) was compared with that on computed tomography (SOOJ-CT). A total of 106 knees were included in the postoperative CT study.
The current study was approved by the Ethics Committee of the Veterans Health Service Medical Center (institutional review board approval number: 2014-07-005).
Statistical analysis
The SOOJ reliability was evaluated using intraclass correlation coefficients (ICCs). Inter- and intraobserver reliabilities were calculated using the ICCs and defined as follows: <0.40, poor agreement; 0.40–0.75, fair to good; and >0.75, excellent [13]. The SOOJ-X ray and SOOJ-CT measurements were compared using a paired t test and Bland–Altman analysis [3]. On Bland–Altman analysis, the 95 % limits of agreement were defined as a mean difference of ±1.96 SD. Using the independent t test and Fisher’s exact test, the parameters of the Groups A and P including age, sex, side, body mass index, fixatives, Pre-HKA, Post-HKA, Pre-PTS, Post-PTS and PrePost-PTS were compared. Finally, a correlation analysis of the SOOJ and Post-PTS was performed. The correlation between the SOOJ and the PrePost-PTS was also analysed. P values under 0.05 were considered significant. The statistical analyses were performed using SPSS v20.0 (SPSS Inc., Chicago, IL, USA) and a trial version of MedCalc for Windows v13.0 (MedCalc Software, Ostend, Belgium). To determine sample size, a power analysis for detection of differences among the groups was performed sing a significance level of 0.05, a power level of 0.80 and effect size of 0.91 from the preliminary study. Minimum 20 knees were required for each group.
Results
Regarding SOOJ reliability, all inter- and intraobserver ICCs showed excellent agreement: the interobserver ICC was 0.88 [95 % confidence interval (CI) 0.80–0.94]. The ICC was 0.94 for observer 1 (95 % CI 0.89–0.97) and 0.88 for observer 2 (95 % CI 0.79–0.93). Regarding SOOJ validity, the SOOJ-X ray and the SOOJ-CT were compared, and there was no significant difference between the two measurements. The mean difference (SOOJ-X ray–SOOJ-CT) was 0.14° (+1.96 SD, 1.81°; −1.96 SD, 0.85°) (Fig. 2).
Bland–Altman plot of the differences between two measurements of the sagittal obliquity of osteotomy relative to the medial joint line (SOOJ). Analysis using the Bland–Altman plot showed that the mean difference in the SOOJ measured by plain radiograph (SOOJ-X ray) and that measured by computed tomography (SOOJ-CT) was 0.14° (+1.96 SD, 1.81°; −1.96 SD, 0.85°)
Table 1 shows the perioperative radiographic measurements. The mean SOOJ was 15.1°, and 87.1 % of the knees showed AIO. Figure 3 shows the distribution of SOOJ in all cases. A comparison between parallel osteotomy group (Group P) and anterior-inclined osteotomy group (Group A) revealed no significant differences except for mean SOOJ (Table 2). Although there were no significant differences in Post-PTS and PrePost-PTS among the two groups, Group A showed an increased tendency in Post-PTS and PrePost-PTS compared with Group P. There was a significant positive correlation between Post-PTS and the SOOJ (r, 0.33; 95 % CI 0.19–0.46; P < 0.001) (Fig. 4). PrePost-PTS also showed a significant positive correlation with SOOJ (r, 0.35; 95 % CI 0.21–0.47; P < 0.001) (Fig. 4). The Pre-HKA, Post-HKA and Pre-PTS were not significantly correlated with SOOJ (P = 0.57, 0.18 and 0.27, respectively).
a Scatter plot of sagittal obliquity of osteotomy relative to medial joint line (SOOJ) and the postoperative posterior tibial slope (Post-PTS). There was a significant positive correlation between the Post-PTS and SOOJ [r, 0.33; 95 % confidence interval (CI) 0.19–0.46; P < 0.001]. b Scatter plot of the SOOJ and postoperative change of posterior tibial slope (PrePost-PTS). The PrePost-PTS also showed a significant positive correlation with the SOOJ [r, 0.35; 95 % CI 0.21–0.47; P < 0.001]
Discussion
The most important finding of the present study was a surprisingly high incidence of AIO (87.1 %) despite of an effort to perform osteotomy parallel to the posterior slope of medial joint line. There was a significant positive correlation between the PTS in the postoperative period (Post-PTS and PrePost-PTS) and SOOJ. The current study was motivated by the lateral radiographs of previous studies in very prestigious orthopaedic surgery journals [8–11, 19, 20, 34, 35, 39, 40]. Although a number of experts have recommended using parallel osteotomy in the sagittal plane, there has been little rationale to support this. These rationales include the inadvertent increase in PTS and preventing very thin proximal posterior bony fragments [2, 27]. Furthermore, we could not find any scientific evidence to support parallel osteotomy in medial OWHTO. To our knowledge, this is the first report of the osteotomy line inclination in the sagittal plane and to describe the AIO phenomenon. The high incidence of AIO and its relationship with PTS highlight the causes of AIO and its influence on PTS.
Possible causes of AIO
The pes anserine tendon, which runs anteroinferior to the medial joint line, could be a cause of AIO (Fig. 5) [29]. Because the anterior guiding wire was placed just above the pes anserine tendon prior to fixing the posterior wire, the partially detached pes anserine tendon could have interfered with the second wire during placement of the two wires parallel to the medial joint line (Fig. 5). Complete detachment of the pes anserine from its insertion would prevent such interference (Fig. 5) [23, 38]. Although experts and the technical guide of the TomoFix™ Medial High Tibial Plate, one of the most commonly used plates in medial OWHTO, recommend fixing the posterior guiding wire before the anterior wire, the anterior wire was placed before the posterior wire because we assumed that placing the anterior wire first would make it easier to determine the plate position [24, 25]. We occasionally experienced difficulty fixing the most distal (“D”) screw of the proximal part of the TomoFix™ Medial High Tibial Plate, so we attempted to obtain sufficient space for this screw by fixing the anterior wire first. We applied this technique to all other cases with other types of plates as well. However, this difficulty in plate placement using the posterior wire first manoeuver seems to be derived from inadequate exposure of the proximal tibia and insufficient detachment of the pes anserine tendon. Although the aforementioned cause is speculative, we recently achieved parallel osteotomy using the posterior wire first manoeuver with sufficient pes anserine tendon detachment. Further investigation is required. Another possible cause of AIO is the tibial anterior cortex, which is naturally anteriorly inclined relative to the sagittal tibial axis. In the operative field, the anterior tibial crest is more apparent than the medial joint line. When osteotomy is performed carelessly in the sagittal plane perpendicular to the anterior tibial crest, AIO is inevitable. Finally, superficial medial collateral ligament seems to make some contribution to AIO. Because the superficial medial collateral ligament is located at the posteromedial part of the tibia, the posterior portion of surgical field is usually tight, and a tight posteromedial field causes less freedom in the osteotomy saw position compared with an anteromedial surgical field. Usually, the posterior part of the saw tends to be more superior to its anterior part, in an anterior-inclined manner in sagittal plane.
a Intraoperative photograph taken during medial open-wedge high tibial osteotomy (OWHTO). Medial joint line was indicated using two syringe needles. Relative to the medial joint line, the pes anserine tendon (*) is running anteroinferiorly. b A schematic illustration of the medial OWHTO showing the partially detached pes anserine tendon. Since we placed the anterior guiding wire (solid circle) just above the pes anserine tendon prior to the posterior wire fixation (empty circle), the partially detached tendon interfered with the second wire, making it difficult to place the two wires parallel to the medial joint line (line 1). The osteotomy connecting the anterior and posterior wires just above the tendon (solid triangle) results in the anterior-inclined osteotomy (line 2). c If the pes anserine tendon is completely detached from its insertion, this interference during placement of the second wire does not occur
Possible mechanisms by which AIO influences PTS
Contrary to our hypothesis, there was an increasing tendency of PTS in the knees with AIO. Although there were relatively weak correlation coefficients between the SOOJ and the Post- and PrePost-PTS (r = 0.33 and 0.35, respectively), these findings showed that the SOOJ influences changes in the PTS after medial OWHTO. From the present findings, we cannot conclude the mechanism by which AIO influences PTS. However, we suppose that AIO increases PTS because of the geometrically different features of the tibial cut plane according to the osteotomy inclination in the sagittal plane. Similar to our hypothesis, some might insist that the osteotomy inclination is not correlated with postoperative PTS change. Unless the anterior gap distraction is modified under the image intensifier, this hypothesis appears to be wrong. As was mentioned earlier, we applied anterior and posterior distraction gaps in a 2–3 ratio with the preoperatively calculated amount. During the distraction, PTS change was not checked under an image intensifier. If the AIO is correlated with PTS change, even to a small degree, the amount of distraction from that of the preoperative calculation should be modified in a situation of AIO. However, additional studies will be able to provide mathematical evidence of the correlation between the osteotomy inclination and PTS.
Our study has a number of limitations. Although the same ratio of anterior and posterior distraction was principally applied according to the preoperative planning of each case, an unintended ratio and the amount of osteotomy distraction may have been a confounding variable in the correlation analysis between the SOOJ and PTS. Because the amount of distraction was not recorded intraoperatively, further adjustment with this factor in the correlation analysis was not possible. Using a navigation system, solutions for the aforementioned limitations and confirmation of parallel osteotomy in the sagittal plane would be achieved. In addition, our speculation on the cause of AIO was inconclusive, so additional investigations with cadavers will be required. Because of the lack of clinical outcomes related to SOOJ in the current study, future well-designed studies that compare AIO and parallel osteotomy groups are also needed. Finally, because the sample size of the current study was relatively small, the current findings should be confirmed in a larger cohort.
Despite these limitations, the current study is the first, to our knowledge, to evaluate the frequency of AIO and its correlation with PTS. Although parallel osteotomy in the sagittal plane has been recommended in a number of references, no study could prove its rationale. We believe the current study provides evidence of the efficacy of parallel osteotomy in medial OWHTO. In four points, the clinical relevance of parallel osteotomy can be suggested. First, it should be confirmed whether parallel osteotomy relative to medial PTS is achieved using an image intensifier in the lateral view. From our results and many lateral radiographs from previous studies, there is high possibility of AIO after the medial OWHTO [8–11, 20, 26, 34, 35, 39, 40]. Second, if the pes anserine tendon interferes with parallel osteotomy performance, full rather than partial detachment of the tendon is recommended [32, 37]. Because many results of anterior cruciate ligament reconstruction using a hamstring autograft, in which the semitendinosus and gracilis tendons are completely harvested, have shown no apparent functional disability after tendon removal, complete detachment of the tendon in medial OWHTO should be permitted without concerns [7, 12, 14]. Third, as recommended by numerous authors and surgical technique guides, fixation of the posterior Kirschner wire prior to the anterior wire is helpful for achieving parallel osteotomy (Fig. 5) [24, 25, 38]. Finally, if the AIO has already occurred, the distracted angle of the osteotomy gap could differ from the intended angle calculated by the preoperative planning to maintain the native PTS.
Conclusion
Although parallel osteotomy in the sagittal plane relative to the medial joint line was planned, only 12.9 % of cases achieved osteotomy parallel to the medial PTS in the sagittal plane. Because of high rate of the AIO and their correlations with posterior tibial slope, surgeons should make all efforts to perform parallel osteotomy relative to medial posterior tibial slope.
References
Akizuki S, Shibakawa A, Takizawa T, Yamazaki I, Horiuchi H (2008) The long-term outcome of high tibial osteotomy: a ten- to 20-year follow-up. J Bone Joint Surg Br 90:592–596
Amendola A (2003) Unicompartmental osteoarthritis in the active patient: the role of high tibial osteotomy. Arthroscopy 19(Suppl 1):109–116
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Bonasia DE, Dettoni F, Sito G, Blonna D, Marmotti A, Bruzzone M, Castoldi F, Rossi R (2014) Medial opening wedge high tibial osteotomy for medial compartment overload/arthritis in the varus knee: prognostic factors. Am J Sports Med 42:690–698
Chae DJ, Shetty GM, Lee DB, Choi HW, Han SB, Nha KW (2008) Tibial slope and patellar height after opening wedge high tibia osteotomy using autologous tricortical iliac bone graft. Knee 15:128–133
Cho SW, Kim DH, Lee GC, Lee SH, Park SH (2013) Comparison between autogenous bone graft and allogenous cancellous bone graft in medial open wedge high tibial osteotomy with 2-Year follow-up. Knee Surg Relat Res 25:117–125
Cooley VJ, Deffner KT, Rosenberg TD (2001) Quadrupled semitendinosus anterior cruciate ligament reconstruction: 5-year results in patients without meniscus loss. Arthroscopy 17:795–800
Cotic M, Vogt S, Feucht MJ, Saier T, Minzlaff P, Hinterwimmer S, Imhoff AB (2014) Prospective evaluation of a new plate fixator for valgus-producing medial open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-014-3287-8
Cotic M, Vogt S, Hinterwimmer S, Feucht MJ, Slotta-Huspenina J, Schuster T, Imhoff AB (2014) A matched-pair comparison of two different locking plates for valgus-producing medial open-wedge high tibial osteotomy: peek-carbon composite plate versus titanium plate. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-014-2914-8
El-Azab H, Glabgly P, Paul J, Imhoff AB, Hinterwimmer S (2010) Patellar height and posterior tibial slope after open- and closed-wedge high tibial osteotomy: a radiological study on 100 patients. Am J Sports Med 38:323–329
El-Azab H, Halawa A, Anetzberger H, Imhoff AB, Hinterwimmer S (2008) The effect of closed- and open-wedge high tibial osteotomy on tibial slope: a retrospective radiological review of 120 cases. J Bone Joint Surg Br 90:1193–1197
Eriksson K, Hamberg P, Jansson E, Larsson H, Shalabi A, Wredmark T (2001) Semitendinosus muscle in anterior cruciate ligament surgery: morphology and function. Arthroscopy 17:808–817
Fleiss JL, Levin BA, Paik MC (2003) Statistical methods for rates and proportions, 3rd edn./Joseph L. Fleiss, Bruce Levin, Myunghee Cho Paik, edn. Wiley-Interscience, Hoboken, NJ
Fu F, Christel P, Miller MD, Johnson DL (2009) Graft selection for anterior cruciate ligament reconstruction. Instr Course Lect 58:337–354
Fujisawa Y, Masuhara K, Shiomi S (1979) The effect of high tibial osteotomy on osteoarthritis of the knee. An arthroscopic study of 54 knee joints. Orthop Clin North Am 10:585–608
Han SB, Bae JH, Lee SJ, Jung TG, Kim KH, Kwon JH, Nha KW (2014) Biomechanical properties of a new anatomical locking metal block plate for opening wedge high tibial osteotomy: uniplane osteotomy. Knee Surg Relat Res 26:155–161
Han SB, Lee DH, Shetty GM, Chae DJ, Song JG, Nha KW (2013) A “safe zone” in medial open-wedge high tibia osteotomy to prevent lateral cortex fracture. Knee Surg Sports Traumatol Arthrosc 21:90–95
Hernigou P (2002) Open wedge tibial osteotomy: combined coronal and sagittal correction. Knee 9:15–20
Jung KA, Kim SJ, Lee SC, Song MB, Yoon KH (2008) ‘Fine-tuned’ correction of tibial slope with a temporary external fixator in opening wedge high-tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 16:305–310
Jung KA, Lee SC, Hwang SH, Song MB (2009) ACL injury while jumping rope in a patient with an unintended increase in the tibial slope after an opening wedge high tibial osteotomy. Arch Orthop Trauma Surg 129:1077–1080
Lee DC, Byun SJ (2012) High tibial osteotomy. Knee Surg Relat Res 24:61–69
Lee YS, Park SJ, Shin VI, Lee JH, Kim YH, Song EK (2010) Achievement of targeted posterior slope in the medial opening wedge high tibial osteotomy: a mathematical approach. Ann Biomed Eng 38:583–593
Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11:132–138
Lobenhoffer P, Galla M, Agneskirchner JD (2008) Osteotomies around the knee: indications, planning, surgical techniques using plate fixators. Thieme, Stuttgart
Lobenhoffer P, Heerwaarden Rv, Agneskirchner J (2014) Kniegelenknahe osteotomien indikation; planung; operationstechniken mit plattenfixateuren. Thieme publisher, Teningen
Longino PD, Birmingham TB, Schultz WJ, Moyer RF, Giffin JR (2013) Combined tibial tubercle osteotomy with medial opening wedge high tibial osteotomy minimizes changes in patellar height: a prospective cohort study with historical controls. Am J Sports Med 41:2849–2857
Miller BS, Downie B, McDonough EB, Wojtys EM (2009) Complications after medial opening wedge high tibial osteotomy. Arthroscopy 25:639–646
Miniaci A, Ballmer FT, Ballmer PM, Jakob RP (1989) Proximal tibial osteotomy. A new fixation device. Clin Orthop Relat Res 246:250–259
Mochizuki T, Akita K, Muneta T, Sato T (2004) Pes anserinus: layered supportive structure on the medial side of the knee. Clin Anat 17:50–54
Noyes FR, Goebel SX, West J (2005) Opening wedge tibial osteotomy: the 3-triangle method to correct axial alignment and tibial slope. Am J Sports Med 33:378–387
Rodner CM, Adams DJ, Diaz-Doran V, Tate JP, Santangelo SA, Mazzocca AD, Arciero RA (2006) Medial opening wedge tibial osteotomy and the sagittal plane: the effect of increasing tibial slope on tibiofemoral contact pressure. Am J Sports Med 34:1431–1441
Rossi R, Bonasia DE, Amendola A (2011) The role of high tibial osteotomy in the varus knee. J Am Acad Orthop Surg 19:590–599
Saito T, Kumagai K, Akamatsu Y, Kobayashi H, Kusayama Y (2014) Five- to ten-year outcome following medial opening-wedge high tibial osteotomy with rigid plate fixation in combination with an artificial bone substitute. Bone Joint J 96:339–344
Sariali E, Catonne Y (2009) Modification of tibial slope after medial opening wedge high tibial osteotomy: clinical study and mathematical modelling. Knee Surg Sports Traumatol Arthrosc 17:1172–1177
Schaefer TK, Majewski M, Hirschmann MT, Friederich NF (2008) Comparison of sagittal and frontal plane alignment after open- and closed-wedge osteotomy: a matched-pair analysis. J Int Med Res 36:1085–1093
Song EK, Seon JK, Park SJ (2007) How to avoid unintended increase of posterior slope in navigation-assisted open-wedge high tibial osteotomy. Orthopedics 30:S127–S131
Song EK, Seon JK, Park SJ, Jeong MS (2010) The complications of high tibial osteotomy: closing- versus opening-wedge methods. J Bone Joint Surg Br 92:1245–1252
Staubli AE, De Simoni C, Babst R, Lobenhoffer P (2003) TomoFix: a new LCP-concept for open wedge osteotomy of the medial proximal tibia–early results in 92 cases. Injury 34(Suppl 2):B55–B62
Wang JH, Bae JH, Lim HC, Shon WY, Kim CW, Cho JW (2009) Medial open wedge high tibial osteotomy: the effect of the cortical hinge on posterior tibial slope. Am J Sports Med 37:2411–2418
Yang JH, Lee SH, Nathawat KS, Jeon SH, Oh KJ (2013) The effect of biplane medial opening wedge high tibial osteotomy on patellofemoral joint indices. Knee 20:128–132
Yoo JH, Chang CB, Shin KS, Seong SC, Kim TK (2008) Anatomical references to assess the posterior tibial slope in total knee arthroplasty: a comparison of 5 anatomical axes. J Arthroplasty 23:586–592
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this manuscript have no financial conflicts of interest to report regarding this work.
Rights and permissions
About this article
Cite this article
Lee, SY., Lim, HC., Bae, J.H. et al. Sagittal osteotomy inclination in medial open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 25, 823–831 (2017). https://doi.org/10.1007/s00167-016-4115-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4115-0