Abstract
Purpose
Suicide is a leading cause of death in patients with schizophrenia. This nationwide cohort study investigated the incidence of each suicide method in patients with schizophrenia compared with the general population.
Methods
In total, records of 174,039 patients with schizophrenia were obtained from the National Health Insurance Research Database in Taiwan from 2001 to 2016. This schizophrenia cohort was linked with the national mortality database, and 26,926 patients died during this follow-up period. Of the deceased, 3033 had died by suicide. Univariate Cox regression was used to estimate the demographic variables associated with suicide. We estimated the difference in the proportion of each suicide method used in patients with schizophrenia compared with the general population. The incidence and standardized mortality ratio (SMR) of each suicide method were calculated and stratified based on sex.
Results
Patients aged 25–34 years exhibited the highest suicide risk. Compared with the general population, patients with schizophrenia were more likely to commit suicide by jumping and drowning and less likely to use charcoal-burning and hanging. Women showed a higher incidence of suicide by drowning and jumping than did men. Comorbidity with substance use disorders (SUDs) was associated with a high suicide SMR (26.9, 95% confidence interval [CI] = 23.4–28.9), particularly for suicide by jumping (61.2, 95% CI = 48.3–76.3).
Conclusions
Patients with schizophrenia had higher suicide rates for all methods than did the general population. Suicide method differed based on sex. Patients with SUDs exhibit a high SMR for each suicide method and warrant intensive clinical attention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Schizophrenia is a debilitating mental illness [1], and studies have indicated that compared with healthy people, patients with mental illness have their lifespans decreased by 11–20 years and mortality rate increased by two to four times [2,3,4]. Although most patients with schizophrenia died of natural causes, a substantial portion of patients also died by suicide [2,3,4,5]. Studies have estimated the lifetime risk of suicide mortality for schizophrenia to be 4.90–6.55% [5, 6]. Subsequently, the estimated lifetime risk of suicide in schizophrenia decreased, but the standardized mortality ratio (SMR) of suicide for schizophrenia remained higher than that for the general population [2, 7]. A recent population-based cohort study in Denmark [8] reported that the age-specific mortality rate ratio for suicide in patients with schizophrenia was 10.76. Furthermore, the ratios for men and women stratified by sex were 9.12 and 14.85, respectively. The risk of suicide was reported to be high in patients with schizophrenia during inpatient stay and during the first month after discharge; moreover, the risk was lower when the follow-up time was longer [9]. Death by suicide is a critical topic related to schizophrenia, and studies have revealed that risk factors for suicide in patients with schizophrenia are the period after the first episode of psychosis [7, 10], the male sex [5, 7], history of suicide attempts [11], and presence of psychiatric comorbidities [12].
Currently, international studies that have explored suicide methods adopted by people with schizophrenia are few with inconsistent findings. For instance, one US study investigated 115 suicide cases collected from the Maryland Chief Medical Examiner’s Office from September 1989 to August 1998; of these, 15 cases involved people with schizophrenia. The study found that people with schizophrenia were most likely to jump from heights to commit suicide and adopted suicide methods with high fatality rates [13]. Another study [14] involving 16 rural county offices in China compared suicide in schizophrenia (n = 38) with that in other psychiatric disorders (n = 150) and in the absence of psychiatric disorders (n = 204). The findings revealed that people with schizophrenia were more likely to ingest pesticides, followed by hanging and drowning themselves. A Taiwan study collected information of the patients with schizophrenia who were ever admitted to a psychiatric hospital in Taipei between January 1, 1985, and December 31, 2000 (n = 4327), and subsequently, 78 patients committed suicide. The study reported that the methods of suicide were mostly jumping, drug overdose, and hanging, in that order [15]. However, the aforementioned studies had a limitation of a small sample size (< 100), and studies with larger sample sizes are needed to estimate the distribution of suicide methods adopted by patients with schizophrenia.
Furthermore, few studies in the early 2000s on schizophrenia suicide involved large sample sizes. For instance, a UK study obtained statistics on 960 cases of suicide by people with schizophrenia from April 1, 1996, to March 31, 2000, from the UK Office for National Statistics and found that these suicides involved violent death, with 27% jumping from a height or in front of a moving vehicle, compared with 10% of the remaining sample [16]. A Swedish study [17] investigated suicide attempters and found that psychotic disorders were independent risk factors for successful suicide. Further stratification of the methods of suicide attempt by co-occurring psychiatric disorder, hanging and comorbid psychotic disorder suggested high rates of suicide during the entire follow-up. Moreover, a Taiwan study involving people with various psychiatric illnesses from 2000 to 2004 found that people with schizophrenia (n = 703) were more likely to commit suicide by jumping than were people diagnosed as having other psychiatric illnesses [18]. In the past 2 decades, charcoal-burning has been a novel suicide method common in Asian countries [19]. Studies have argued that the demonstration of the charcoal-burning suicide methodology in media reports and painlessness of this methodology have contributed to a rapid increase in charcoal-burning suicide in many countries; furthermore, easy access to charcoal has been a contributing factor [19,20,21,22,23,24]. However, whether patients with schizophrenia are more or less likely to use this method than is the general population is unknown.
This study recruited 174,039 patients with schizophrenia in Taiwan from 2001 to 2016, of whom 3033 died by suicide during a 16-year follow-up period. Several essential factors were investigated. We compared suicide methods used by people with schizophrenia with those used by the general population. Furthermore, we investigated differences in suicide methods used by people with schizophrenia based on sex. Finally, this study explored the SMR of each suicide method used by patients with schizophrenia stratified on the basis of the comorbidity of substance use disorders (SUDs) or other psychiatric disorders.
Materials and methods
This study used Taiwan National Health Insurance (NHI) Research Database (NHIRD; N = 23,000,000), maintained by the Health and Welfare Data Science Center and contains the registration files and medical claims data of beneficiaries covered by the NHI program. The program was implemented in 1995 and provides easy access to medical services for the 23,000,000 citizens of Taiwan. NHI-insured residents can visit any NHI-affiliated hospitals or clinics in Taiwan to use their medical services. The NHI Administration randomly audits medical records, and the Joint Commission of Taiwan is responsible for monitoring the accreditation of NHI hospitals to ensure system and information accuracy. Currently, the NHIRD is frequently used for research and is a data source for many epidemiological studies published in review journals [25,26,27].
Definition of Schizophrenia Cohort
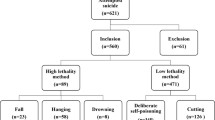
From the NHIRD, we selected both inpatients and outpatients diagnosed as having psychiatric disorders (International Classification of Diseases, Ninth Revision, Clinical Modification [ICD-9-CM] codes 290.x–319.x; International Classification of Diseases, Tenth Revision, Clinical Modification [ICD-10-CM] codes F01–F99) between 2001 and 2016 (n = 10,422,350). Next, we eliminated patients diagnosed as having affective psychosis (ICD-9-CM codes: 296.0–296.16, 296.4–296.81, 296.89, and 296.9; ICD-10-CM codes F30.x and F31.x; n = 188,902) between January 1, 2000, and December 31, 2016. Then, we selected patients diagnosed as having psychiatric illness codes ICD-9-CM 295.xx and ICD-10-CM F20.X and F25.x (n = 174,039). Patients with missing information regarding sex were then eliminated, leaving 170,322 patients diagnosed as having schizophrenia with available data records. The date first diagnosed as schizophrenia during the study period was defined as the baseline. This sample was defined as the schizophrenia cohort (Fig. 1).
Identification of suicide mortality events
We linked the aforementioned schizophrenia cohort with the national mortality database (January 1, 2001 to December 31, 2016) to obtain the mortality status for each study participant. In total, 26,926 participants died during the study period. The national cause-of-death statistics were classified according to the ICD-9-CM codes before December 31, 2014, and ICD-10-CM codes after January 1, 2015. Therefore, we defined suicide codes as E950–E959 according to the ICD-9-CM classification and X60–X84 and Y87.0 according to the ICD-10-CM classification. Of the deceased, 3033 patients died by suicide.
Statistical analysis
Differences in the incidence of suicide mortality between the sexes were investigated using Gehan’s generalized Wilcoxon test [28] and life-table survival analysis. We conducted a univariate Cox proportional hazards regression to estimate social demographic variables and their correlations with future suicide mortalities (Table 1). Furthermore, this study obtained the suicide methods of all suicides in the general population of Taiwan from January 1, 2001 to December 31, 2016 (n = 59,103). We then compared differences in suicide mortality between people diagnosed as having schizophrenia and the general population, analyzing and estimating the differences for each suicide method between these two groups (Table 2). This analysis was conducted using logistic regression through adjustment of sex and age.
We calculated the survival (contribution) time of each schizophrenia cohort member from their first schizophrenia diagnosis until their suicide or the end of this study (December 31, 2016) using which we calculated the suicide incidence rate. The incidence rate is the number of suicides divided by contributor years. We used Wilcox (Gehan) to analyze and compare differences in incidence rates (Table 3). The SMR was used as an index to calculate risk factors for suicide methods according to various comorbidity combinations within 1 year before the baseline. The results are presented as three groups: without psychiatric comorbidity, comorbid with SUDs, and comorbid with non-SUD psychiatric comorbidity (Table 4). All statistical analyses were conducted using the SAS System for Windows, (version 9.4; SAS Institute, Cary, NC, USA). A p value of < 0.05 was considered statistically significant.
Results
Demographics and cumulative incidence of suicide
Table 1 presents the demographic information of patients with schizophrenia (n = 170,322), including those who died by suicide (n = 3033). Univariate Cox proportional hazards regression analysis demonstrated that women exhibited lower risks of schizophrenia (hazard ratio [HR] = 0.74, 95% confidence interval [CI] = 0.69–0.80, p < 0.001) than did men. Relative to the youngest age group (< 20 years), the 30–39-year age group exhibited the highest suicide risk (HR = 2.20, 95% CI = 1.89–2.56, p < 0.001), followed by the 20–29-year (HR = 1.95, 95% CI = 1.67–2.27, p < 0.001) and 40–49-year (HR = 1.91, 95% CI = 1.63–2.23, p < 0.001) age groups; patients aged ≥ 60 years had the lowest suicide risk. Urbanization level and unemployment did not evidently affect suicide risk. Comorbidities of SUD (HR = 3.26, 95% CI = 2.89–3.68, p < 0.001) and a non-SUD psychiatric comorbidity (HR = 1.54, 95% CI = 1.42–1.67, p < 0.001) were associated with high suicide risks (Table 1).
Figure 1 presents the cumulative incidence of suicide mortality stratified by sex. According to our life-table analysis, the cumulative incidence was significantly higher in men than in women (p < 0.001). The results revealed the suicide rate to be relatively high in the early phase of illness. The 1-year cumulative incidence rates for men and women were 0.00565 and 0.00429, respectively; the 2-year cumulative incidence rates were 0.00862 and 0.00644, respectively; and the 3-year cumulative incidence rates were 0.0114 and 0.00873, respectively.
Suicide methods before schizophrenia development and in general population
Table 2 compares differences in suicide mortality between patients diagnosed as having schizophrenia (n = 3033) and the general population of Taiwan (n = 59013). Logistic regression analysis revealed that compared with the general population, patients diagnosed as having schizophrenia were more likely to commit suicide through drowning (odds ratio [OR] = 1.48, 95% CI = 1.27–1.73, p < 0.001) and jumping (OR = 1.71, 95% CI = 1.52–1.93, p < 0.001) and less likely through charcoal-burning (OR = 0.45, 95% CI = 0.40–0.51, p < 0.001) and hanging (OR = 0.71, 95% CI = 0.63–0.80, p < 0.001). No statistical difference was observed in the suicide methods used by men and women.
Suicide method incidence based on sex in patients with schizophrenia
Among the 170,332 patients diagnosed as having schizophrenia, men had higher incidence rates of suicide mortality than women did. Among men, the suicide mortality rate was 252.4 cases in every 100,000 people (p < 0.001), which was higher than that for women. Compared with men, women were more likely to commit suicide through drowning (23.8 cases in every 100,000 people; p < 0.001) and jumping (61.2 cases in every 100,000 people; p = 0.045).
The suicide mortality incidence rates for drug overdose, charcoal-burning or gas asphyxiation, hanging, firearms, and cutting were higher among men than among women, with 69.3, 51.4, and 44.0 cases of hanging, charcoal-burning or gas asphyxiation, and drug overdose per 100,000 people, respectively (p < 0.001; Table 3).
Standardized mortality ratio (SMR)
Of the three groups of the cohort based on comorbidity—namely, without psychiatric comorbidities, comorbidities with SUDs, and comorbidities with non-SUD psychiatric comorbidity—patients with the comorbidities with SUDs group had the highest mortality rate (SMR = 13.1). The distribution of the causes of death is presented in Table 4.
The comorbidities with SUDs group also had the highest SMR among cases with suicide mortality (26.9, 95% CI = 23.4–28.9) and the highest SMR for each method of suicide, particularly jumping from heights (61.2, 95% CI = 48.3–76.3; Table 4).
We investigated differences between men and women for various indicators, including the crude incidence of cause of death (Table 1), SMRs of cause of death (Table 2), and SMR of each suicide method (Table 3). Regarding mortality through specific causes, the mortality rate through unnatural causes were significantly higher in men than in women (p < 0.001); furthermore, men exhibited a higher incidence of suicide mortality than women did (p < 0.001). SMRs of deaths among women through unnatural causes (15.72, 95% CI = 15.03–16.43) and suicide (17.34, 95% CI = 16.39–18.34) were higher than those among men.
Discussion
Strengths of this study
The strengths of this study included a large sample size of patients diagnosed as having schizophrenia representing the entire Taiwan population. This study revealed that patients with schizophrenia were more likely to commit suicide by jumping from heights or drowning than were the general population. Male and female patients with schizophrenia were likely to commit suicide by hanging and jumping, respectively. Thus, sex differences existed in their suicide methods. Furthermore, this study found that patients with schizophrenia comorbid with SUD were most likely to commit suicide (SMR = 26.0), particularly by jumping (SMR = 61.2).
Risk factors for suicide in patients with schizophrenia
This study substantiated that patients with schizophrenia were at the highest suicide risk at ages 22–44 years, whereas the risk significantly decreased after 55 years. This finding was consistent with previous studies, which verified that patients with schizophrenia exhibited a high suicide rate immediately after the first schizophrenia diagnosis [7, 10]. This phenomenon suggests that young and newly diagnosed patients with schizophrenia may be unable to adapt to their illness and therefore commit suicide. This information is helpful for clinical staff members to provide early intervention to prevent suicide among patients newly diagnosed as having schizophrenia. This study found the high suicide rate among patients with schizophrenia to be unacceptable, especially in the early phases of illness. A recent study [29] reported that early intervention was associated with reductions in long-term suicide rates. Therefore, patients in the early phase of schizophrenia warrant early intervention due to the high suicide rates.
This study found that although female patients with schizophrenia had fewer incidences of suicide than male patients did, they exhibited a higher suicide SMR than did men (17.3 vs. 11.9). This finding appears to be paradoxical and could be explained by women in the general population having a much lower suicide rate than did men and by the difference in suicide rates between men and women with schizophrenia being relatively small. Therefore, men with schizophrenia had a higher suicide rate than did women, and women with schizophrenia had higher SMRs. The findings of this study are similar to those of a study in Stockholm County, Sweden, from 1973 to 1995, which indicated that among all patients with schizophrenia, the suicide SMR was 15.7 and 19.7 for male and female patients, respectively [30]. Another study in Taiwan demonstrated that the SMRs for suicides in patients with schizophrenia were 23.9 and 46.1 for male and female patients, respectively [31]. The aforementioned study yielded higher SMRs than did this study, possibly because the participants were selected from hospitals and therefore involved cases with more severe illnesses, leading to higher suicide SMRs. Thus, suicide mortality in both male and female patients with schizophrenia requires attention and increased prevention measure.
Suicide methods used by patients with schizophrenia
This study verified that for committing suicide, compared with the general population, patients with schizophrenia were more likely to adopt jumping from heights or drowning and less likely to adopt charcoal-burning or hanging.
This study found that people with schizophrenia were likely to commit suicide by jumping, which is consistent with other studies [13, 16]. A study [32] provided a possible explanation by analyzing those who attempted suicide by jumping based on hospital records of a general hospital and reported that the psychotic symptoms of patients—such as disorganization or cognitive impairment—may interfere with the preparations for suicide; therefore, such patients tend to commit suicide by jumping. As patients with schizophrenia are indeed likely to develop psychotic symptoms, they may be less likely to choose suicide methods that require planning, such as jumping.
Our study also found that people with schizophrenia were more likely than the general population to commit suicide by drowning. A study [33] argued that most cases of suicide by drowning involved adult men with depression; because of their mental incapacity, they chose places with easy access to water. Studies comparing suicide methods among people with schizophrenia mostly focused on suicide methods more prevalent among people with schizophrenia, such as jumping from heights; few studies have investigated suicide by drowning, and further study is required for the possible mechanisms.
Charcoal-burning is a novel suicide method that has become common in Asian countries over the past 20 years [19]. However, the present study revealed that patients with schizophrenia were less likely to commit suicide using charcoal-burning than was the general population, which is consistent with previous studies. A Taiwan study showed that 73 cases of suicide attempts through charcoal-burning from 2000 to 2010, patients with moderate to severe depression represented the majority (49.3%), and patients with schizophrenia were rare [34]. Another study indicated that from 2000 to 2004 in Taiwan, the highest and lowest rates of suicide by charcoal-burning were among nonpsychotic people and patients with schizophrenia, respectively [18]. Thus, charcoal-burning is less common in patients with schizophrenia than in other functional groups because schizophrenia symptoms affect their functional ability. Suicide by charcoal-burning requires multiple steps, which may present a barrier to people with schizophrenia who prefer simpler suicide methods [4, 13, 14].
In terms of sex differences, our study revealed that male patients with schizophrenia are more likely to commit suicide by hanging, charcoal-burning, and drug overdose, whereas female patients with schizophrenia mostly commit suicide by jumping from heights and drowning. Although the possible explanations remain speculative, these findings could provide clinical caregivers as a reference for suicide prevention.
Increased risk while comorbid with SUDs
Studies [35, 36] have shown that patients with schizophrenia were prone to using violent suicide methods with high fatality rates. However, the SMR of each suicide method in this study, either violent or nonviolent, was significantly higher than that of the general population, particularly jumping from a high place (SMR: 31.3) and drowning (SMR: 23.5). This information is a crucial reference for prevention and intervention.
This study substantiated that patients with schizophrenia comorbid with SUDs within 1 year before the baseline had high suicide SMRs. However, this finding should be interpreted with caution, because it is unclear whether the individuals had active SUDs at the time of death according to the register data. This study preliminarily indicated a potential association between comorbidity with SUDs and a relatively high risk of suicide. Studies have reported that SUDs are a risk factor for suicide [16, 37, 38]. A study [39] showed that using illegal drugs triples mortality by unnatural causes.
In this study, of 3033 mortality cases, 356 involved SUD within 1 year before the baseline. Regarding the major diagnosis of psychiatric comorbidity related to SUD, 165 cases involved alcohol use disorder and 191 involved drug use disorder. A total of 45 cases were comorbid with both alcohol and drug use disorders. Patients with schizophrenia who drink alcohol might exhibit poor general executive functioning and decision-making skills, increasing their likelihood of attempting suicide [38]. Thus, patients with schizophrenia comorbid with drug or alcohol addiction would be prone to suicidal behaviors as a result of decreased general executive functioning and decision-making capacity after drug or alcohol use. Comorbidity with drug and alcohol addiction could have a synergistic effect on suicide risk.
Furthermore, this study verified that among the three comorbidity groups, the group comorbid with SUDs exhibited the highest SMRs in suicide methods. In this group, the SMR for suicide by jumping from heights was as high as 61.2; this exceedingly large number indicates that the impulse control of patients with schizophrenia is impaired because of psychoactive substance use. Furthermore, subject to psychoactive substance use, SMRs for other suicide methods were exceedingly high. Thus, future medical care should particularly focus on suicide prevention for patients with schizophrenia using psychoactive substances.
Study limitations
This study has several limitations. First, the analysis was conducted using database records. We could not track the mortality status for individuals with schizophrenia who migrated out of the country during the study period. However, such individuals constituted a small fraction of all patients, and the findings should not have been affected. Second, those who died by suicide could be misclassified as other causes, e.g., accidental death, typically owing to insurance benefits or social stigma reasons [40]. Third, our data did not include information on lifestyle, and therefore, the correlation between lifestyle and suicide method chosen cannot be investigated. Fourth, this study excluded patients with contact to services during 2000 to exclude potential prevalent patients with schizophrenia. To enroll a larger sample size with a long-term follow-up period, we used a shorter wash-out period (i.e., 1 year) instead of a longer wash-out period. However, selection bias could exist, because this study may include prevalent patients who lived and received continuous treatment after 2001. Future studies should include incident subjects with schizophrenia only.
Implications
This study found that compared with the general population, people with schizophrenia are prone to attempting suicide through methods that do not require tools, such as jumping from heights or drowning. Suicide methods that require tools—such as charcoal-burning and hanging—are less common, indicating a difference in functional ability among individuals with schizophrenia compared with the general population. In future, prevention efforts should focus on these suicide methods to reduce the suicide risk among patients with schizophrenia. In addition, patients with SUDs exhibit high SMRs for all suicide methods. Thus, patients with schizophrenia comorbid with SUDs possess poor decision-making skills and are prone to impulsive suicidal behaviors, which increased their suicide risk. This is the high-risk group for suicide that must be focused on to control their suicidal behaviors in the early stages.
References
McGrath J, Saha S, Chant D, Welham J (2008) Schizophrenia: a concise overview of incidence, prevalence, and mortality. Epidemiol Rev 30:67–76
Ajdacic-Gross V, Weiss MG, Ring M, Hepp U, Bopp M, Gutzwiller F, Rossler W (2008) Methods of suicide: international suicide patterns derived from the WHO mortality database. Bull World Health Organ 86(9):726–732
Nordentoft M, Wahlbeck K, Hallgren J, Westman J, Osby U, Alinaghizadeh H, Gissler M, Laursen TM (2013) Excess mortality, causes of death and life expectancy in 270,770 patients with recent onset of mental disorders in Denmark, Finland and Sweden. PLoS ONE 8(1):e55176
Abdeen MS, Shaker NM, Elrassas HH, Hashim MA, Abo Zeid MY (2019) Characteristics of the schizophrenia suicide attempts in comparison with the suicide attempts with other diagnosed psychiatric disorders: an Egyptian study. Int J Soc Psychiatry 65(5):368–377
Nordentoft M, Mortensen PB, Pedersen CB (2011) Absolute risk of suicide after first hospital contact in mental disorder. Arch Gen Psychiatry 68(10):1058–1064
Palmer BA, Pankratz VS, Bostwick JM (2005) The lifetime risk of suicide in schizophrenia: a reexamination. Arch Gen Psychiatry 62(3):247–253
Dutta R, Murray RM, Hotopf M, Allardyce J, Jones PB, Boydell J (2010) Reassessing the long-term risk of suicide after a first episode of psychosis. Arch Gen Psychiatry 67(12):1230–1237
Plana-Ripoll O, Pedersen CB, Agerbo E, Holtz Y, Erlangsen A, Canudas-Romo V, Andersen PK, Charlson FJ, Christensen MK, Erskine HE, Ferrari AJ, Iburg KM, Momen N, Mortensen PB, Nordentoft M, Santomauro DF, Scott JG, Whiteford HA, Weye N, McGrath JJ, Laursen TM (2019) A comprehensive analysis of mortality-related health metrics associated with mental disorders: a nationwide, register-based cohort study. Lancet 394(10211):1827–1835
Nordentoft M, Laursen TM, Agerbo E, Qin P, Hoyer EH, Mortensen PB (2004) Change in suicide rates for patients with schizophrenia in Denmark, 1981–97: nested case–control study. BMJ 329(7460):261
Ventriglio A, Gentile A, Bonfitto I, Stella E, Mari M, Steardo L, Bellomo A (2016) Suicide in the early stage of schizophrenia. Front Psychiatry 7:116
Mork E, Walby FA, Harkavy-Friedman JM, Barrett EA, Steen NE, Lorentzen S, Andreassen OA, Melle I, Mehlum L (2013) Clinical characteristics in schizophrenia patients with or without suicide attempts and non-suicidal self-harm—a cross-sectional study. BMC Psychiatry 13:255
Popovic D, Benabarre A, Crespo JM, Goikolea JM, Gonzalez-Pinto A, Gutierrez-Rojas L, Montes JM, Vieta E (2014) Risk factors for suicide in schizophrenia: systematic review and clinical recommendations. Acta Psychiatr Scand 130(6):418–426
Kreyenbuhl JA, Kelly DL, Conley RR (2002) Circumstances of suicide among individuals with schizophrenia. Schizophr Res 58(2–3):253–261
Lyu J, Zhang J (2014) Characteristics of schizophrenia suicides compared with suicides by other diagnosed psychiatric disorders and those without a psychiatric disorder. Schizophr Res 155(1–3):59–65
Kuo CJ, Tsai SY, Lo CH, Wang YP, Chen CC (2005) Risk factors for completed suicide in schizophrenia. J Clin Psychiatry 66(5):579–585
Hunt IM, Kapur N, Windfuhr K, Robinson J, Bickley H, Flynn S, Parsons R, Burns J, Shaw J, Appleby L (2006) Suicide in schizophrenia: findings from a national clinical survey. J Psychiatr Pract 12(3):139–147
Runeson B, Tidemalm D, Dahlin M, Lichtenstein P, Langstrom N (2010) Method of attempted suicide as predictor of subsequent successful suicide: national long term cohort study. BMJ 341:c3222
Chen YY, Lee MB, Chang CM, Liao SC (2009) Methods of suicide in different psychiatric diagnostic groups. J Affect Disord 118(1–3):196–200
Chang SS, Chen YY, Yip PS, Lee WJ, Hagihara A, Gunnell D (2014) Regional changes in charcoal-burning suicide rates in East/Southeast Asia from 1995 to 2011: a time trend analysis. PLoS Med 11(4):e1001622
Chen YY, Tsai CW, Biddle L, Niederkrotenthaler T, Wu KC, Gunnell D (2016) Newspaper reporting and the emergence of charcoal burning suicide in Taiwan: a mixed methods approach. J Affect Disord 193:355–361
Liu KY, Beautrais A, Caine E, Chan K, Chao A, Conwell Y, Law C, Lee D, Li P, Yip P (2007) Charcoal burning suicides in Hong Kong and urban Taiwan: an illustration of the impact of a novel suicide method on overall regional rates. J Epidemiol Community Health 61(3):248–253
Chang YH, Hsu CY, Cheng Q, Chang SS, Yip P (2019) The evolution of the characteristics of charcoal-burning suicide in Hong Kong, 2002–2013. J Affect Disord 257:390–395
Yoshioka E, Saijo Y, Kawachi I (2016) Spatial and temporal evolution of the epidemic of charcoal-burning suicide in Japan. Soc Psychiatry Psychiatr Epidemiol 51(6):857–868
Choi YR, Cha ES, Chang SS, Khang YH, Lee WJ (2014) Suicide from carbon monoxide poisoning in South Korea: 2006–2012. J Affect Disord 167:322–325
Chen YL, Pan CH, Chang CK, Chen PH, Chang HM, Tai MH, Su SS, Tsai SY, Chen CC, Kuo CJ (2020) Physical illnesses before diagnosed as schizophrenia: a nationwide case–control study. Schizophr Bull 46:785–794
Chen PH, Tsai SY, Pan CH, Chang HM, Chen YL, Su SS, Chen CC, Kuo CJ (2020) Incidence and risk factors of sudden cardiac death in bipolar disorder across the lifespan. J Affect Disord 274:210–217
Chen PH, Tsai SY, Pan CH, Chang CK, Su SS, Chen CC, Kuo CJ (2019) Mood stabilisers and risk of stroke in bipolar disorder. Br J Psychiatry 215(1):409–414
Lee ET (1992) Statistical methods for survival data analysis. Wiley, New York
Chan SKW, Chan SWY, Pang HH, Yan KK, Hui CLM, Chang WC, Lee EHM, Chen EYH (2018) Association of an early intervention service for psychosis with suicide rate among patients with first-episode schizophrenia-spectrum disorders. JAMA Psychiatry 75(5):458–464
Osby U, Correia N, Brandt L, Ekbom A, Sparen P (2000) Mortality and causes of death in schizophrenia in Stockholm county. Sweden Schizophr Res 45(1–2):21–28
Ko YS, Tsai HC, Chi MH, Su CC, Lee IH, Chen PS, Chen KC, Yang YK (2018) Higher mortality and years of potential life lost of suicide in patients with schizophrenia. Psychiatry Res 270:531–537
Todorov L, Vulser H, Pirracchio R, Thauvin I, Radtchenko A, Vidal J, Guigui P, Limosin F, Lemogne C (2019) Suicide attempts by jumping and length of stay in general hospital: a retrospective study of 225 patients. J Psychosom Res 119:34–41
Muccino E, Crudele GD, Gentile G, Marchesi M, Rancati A, Zoja R (2015) Suicide drowning in the non-coastal territory of Milan. Int J Legal Med 129(4):777–784
Lin C, Yen TH, Juang YY, Leong WC, Hung HM, Ku CH, Lin JL, Lee SH (2012) Comorbid psychiatric diagnoses in suicide attempt by charcoal burning: a 10-year study in a general hospital in Taiwan. Gen Hosp Psychiatry 34(5):552–556
Park CHK, Yoo SH, Lee J, Cho SJ, Shin MS, Kim EY, Kim SH, Ham K, Ahn YM (2017) Impact of acute alcohol consumption on lethality of suicide methods. Compr Psychiatry 75:27–34
Huang YC, Wu YW, Chen CK, Wang LJ (2014) Methods of suicide predict the risks and method-switching of subsequent suicide attempts: a community cohort study in Taiwan. Neuropsychiatr Dis Treat 10:711–718
Gonzalez-Pinto A, Aldama A, Gonzalez C, Mosquera F, Arrasate M, Vieta E (2007) Predictors of suicide in first-episode affective and nonaffective psychotic inpatients: five-year follow-up of patients from a catchment area in Vitoria. Spain J Clin Psychiatry 68(2):242–247
Adan A, Capella MD, Prat G, Forero DA, Lopez-Vera S, Navarro JF (2017) Executive functioning in men with schizophrenia and substance use disorders. Influence of lifetime suicide attempts. PLoS ONE 12(1):e0169943
Revier CJ, Reininghaus U, Dutta R, Fearon P, Murray RM, Doody GA, Croudace T, Dazzan P, Heslin M, Onyejiaka A, Kravariti E, Lappin J, Lomas B, Kirkbride JB, Donoghue K, Morgan C, Jones PB (2015) Ten-year outcomes of first-episode psychoses in the MRC AESOP-10 study. J Nerv Ment Dis 203(5):379–386
Cheng AT (1995) Mental illness and suicide. A case–control study in east Taiwan. Arch Gen Psychiatry 52(7):594–603
Acknowledgements
This manuscript was edited by Wallace Academic Editing.
Funding
This research was supported by grants from the Ministry of Science and Technology, Taiwan (MOST 105-2314-B-532-006-MY3 and MOST 108-2314-B-532-005) and Taipei City Hospital (10501-62-015 and 10601-62-002). The funding sources had no involvement in the study design, data collection, analysis, or interpretation, report writing, or decision to submit the paper for publication.
Author information
Authors and Affiliations
Contributions
Drs. Pan and Kuo conceived and designed the study. Dr. Kuo acquired the data. Mr. Su performed the statistical analysis. Drs. Tsai and CC Chen provided administrative and material support. Drs. Pan and Kuo and Ms Wang drafted the manuscript. Drs. PH Chen, Chang and YL Chen made critical revisions to the manuscript for important intellectual content, and Drs. Tsai and CC Chen supervised the study.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pan, CH., Chen, PH., Chang, HM. et al. Incidence and method of suicide mortality in patients with schizophrenia: a Nationwide Cohort Study. Soc Psychiatry Psychiatr Epidemiol 56, 1437–1446 (2021). https://doi.org/10.1007/s00127-020-01985-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-020-01985-8