Abstract
Purpose
This study aims to examine and compare the effects of direct and indirect exposure to armed conflicts on the mental health of primary school students in the three southernmost provinces of Thailand.
Methods
A school-based survey was conducted. Detailed exposure of traumatic events both directly and indirectly were measured by a self-completed questionnaire. Behavioral–emotional problems were measured by the Strength and Difficulty Questionnaire and screening for post-traumatic stress disorder (PTSD) was done using the Children’s Revised Impact of Events Scale (CRIES). Multivariate analysis adjusted for gender and other covariates was used to determine the effect of direct and indirect exposure of armed conflict on mental health problems.
Results
Out of 941 students included in the study, almost half had direct exposure to an armed conflict event. Overall, 42.1% of students had at least one behavioral–emotional problem (47.6% and 38.5% in the direct- and indirect-exposed groups, respectively) and 30.5% was found to have PTSD (37.3% and 25.9% in the direct- and indirect-exposed groups, respectively). Students who had direct exposure to an armed conflict event had a two times higher odds of mental health problems than their peers. Other modifiable factors of mental health problems were receiving news from two sources including other adults and media, and exposure to other non-conflict-related traumatic life events.
Conclusions
Children living in armed conflict areas of southern Thailand, although without any direct exposure to traumatic events, also suffered from mental health problems. Research on appropriate interventions for these children should be further conducted.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Southern Thailand has generally been a peaceful region until 2004 when armed conflicts began to arise causing widespread disruption to the region. The cause of the conflict is multifactorial; political issues and economic hardship as well as differences in ethnicity and religion being the major contributing factors. Unlike other war zones, the situation is intermittent and unpredictable and has a wide range of intensity. Many weapons of war have been used. Local residents still live with the situation as part of their daily lives.
Children born in 2004 and residing in the three southernmost provinces have experienced a prolonged and stressful situation. According to a report by the Deep South Watch, an organization aiming to raise awareness of the conflict, a total of 238 children have died from violent events, 1151 have been injured, 36 handicapped and 6998 have become orphans [1]. Moreover, schools have been destroyed through arson or bombings with many teachers killed.
Direct exposure to traumatic events, including seeing a family member injured or killed and having a home shelled or demolished, can affect a child’s mental health and cause behavioral and emotional problems such as post-traumatic stress disorder (PTSD) [2,3,4,5,6]. Current intervention programs are currently targeting this group of children. However, the majority of children in the conflict areas have also had indirect exposure such as hearing the bombs exploding and gun shots being fired as well as listening to or watching the events from radio or television news reports. The effect of indirect exposure on the children’s mental health and whether they need support or intervention has not yet been established. The study, therefore, aims to examine the effects of the conflict on children born and raised in the conflict areas with a special emphasis on those who have had direct and indirect exposure to violent events.
Methods
Study subjects and study sampling
A school-based survey was conducted in 2015 among primary school students in Yala, Narathiwat and Pattani provinces. All schools were listed from the Primary Educational Service Area Office. The schools were first categorized into three intensity levels (low, moderate and high) based on the number of violent events, deaths and injuries reported in 2015 and then by school type (public, private and Islamic). From the resulting 9 school groups, 18 schools were randomly selected, 2 from each group. All sixth graders in the selected schools who were able to communicate in the Thai language were invited to participate in the study. Six graders were selected because they represented a cohort born when the conflict is believed to have commenced.
Study measurement
A teacher distributed a set of questionnaires to each student to complete in their classroom. The questionnaire included questions asking about their demographic characteristics, school absence, exposure to the armed conflict situation including intensity of event, history of conflict situation, injuries and deaths seen or heard, type of violence witnessed, duration and source of information about the violent events.
Behavioral–emotional problems were measured by the Strength and Difficulty Questionnaire (SDQ) Thai version, which was validated by the Department of Mental Health [7]. The questionnaire is a standardized test recommended for children aged between 4 and 16 years. A total of 25 items are categorized into 5 domains: emotional problems, conduct disorders, hyperactivity disorders, peer problems, and pro-social behaviors. Each domain is measured using 5 questions measured on a 3-point rating scale: not true (0), somewhat true (1), certainly true (2), thus the scores for each domain range from 0 to 10. A total difficulty score below 17 is considered as normal, 17–18 as borderline and 19–40 as abnormal. A pro-social behavior score of 4 or more is considered as having some strength and less than 4 is considered as having no strength.
The Children’s Revised Impact of Events Scale (CRIES) was used to screen for post-traumatic stress disorder. It was translated and validated in the Thai context [8]. The scale includes 13 items measured on a four-point scale: not at all (0), rarely (1), sometimes (3) and often (5). Those with a total score below 25 are considered as normal and those with scores between 25 and 65 are considered to be at risk of PTSD.
When needed, the teacher and the researcher clarified any questions inquired by students. Each student took about 30 min to complete the questionnaire.
Data management and analysis
Checking for completeness of data was done immediately after collecting the data. Data were entered and validated by EpiData software version 3.1 [9] and analyzed using R version 3.3.3 [10]. Descriptive statistics including mean and standard deviation (SD) for continuous variables and frequency and percentage for categorical variables were used to present students’ characteristics and detailed experiences of conflict situations. Any of the following events arising from the armed conflict was considered to be a violent or traumatic event: burning of a school or government building; bomb blast; fighting involving weapons, gunshots. Direct exposure to a violent event was defined as being a witness to any event while indirect exposure was defined as having only heard about an event via the media or word of mouth. The scores of SDQ and CRIES were interpreted based on the standard cutoff levels and compared between students who had direct and indirect exposure of a violent event by the Chi square test. Ordinal and logistic regression analyses were used to examine factors associated with the three levels of behavioral–emotional problems and binary outcome of PTSD, respectively. For each factor, the strength of association was presented using an adjusted odds ratio (OR) and 95% confidence interval (CI). The analyses were adjusted for sampling weights.
Ethical consideration
This study was approved by the Institutional Ethics Committee of the Faculty of Medicine, Prince of Songkla University, Thailand. All students were informed that they had the right to refuse to participate in the study or withdraw from it at any time without any negative consequences. Written informed assent was obtained from the parents of all students. Confidentiality of data was assured to all participants. A research psychologist was on-call to provide mental support to a student at the school and provide referral for further management in case it was needed.
Results
A total of 941 6th-year students participated in the study. Table 1 presents the demographic characteristics and school absenteeism for all students. Girls slightly outnumbered boys and the mean (SD) age was 12.3 (0.6) years. Most (85.5%) were Muslim and the majority lived with both parents. The rate of school absenteeism in the past month was about 75% and was mostly due to sickness. Approximately 15% of the students were absent from school due to armed conflict events.
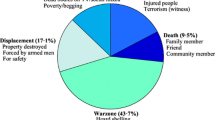
Table 2 shows characteristics of exposure to violent events due to armed conflicts. Almost half (44.6%) of the students had ever witnessed or had direct exposure to a violent event of whom most (66.4%) were exposed more than once in their lifetime. One-third of the students witnessed or heard a violent event while traveling from home to school or vice versa. The average age of witnessing their first event was 10 years and more than half occurred within the past 12 months of the interview. The most common types of violent event were bombing (51.7%), and fighting or shooting (49.0%). Fifty-two students said that they witnessed or heard that a school or government building had burned down. Most (83.8%) witnessed first-hand a person being injured or killed, but the majority of victims were not known to the student. The main sources of armed conflicts information the students heard were mainly from television and other people, particularly their own family members and teachers.
Overall, 42.1% (SE = 2.0) of students had at least one behavioral–emotional problem and 30.5% (SE = 1.8) had a high risk of PTSD. The most common problems were peer-related (16.3%, SE = 1.9) and emotional (13.3%, SE = 1.4). The percentage of students found to have inadequate pro-social behaviors was 17.9% (SE = 1.6). Table 3 compares the mental health outcomes between students who had direct exposure to violent events and those who had indirect exposure. The percentage of students who had at least one behavioral–emotional problem was 47.6% for those who had direct exposure and 38.5% for those who had indirect exposure. The direct exposure group had a significantly higher prevalence of emotional problems (17.7% vs 10.3%) than the indirect-exposure group. The prevalence of PTSD was 37.3% among those who had direct exposure to a violent event and 25.9% among those who had indirect exposure (p < 0.001).
Table 4 presents the results of the multivariate analysis to determine factors associated with behavioral–emotional problems and PTSD adjusting for gender. Students who had direct exposure to conflict events had a higher odds of behavioral–emotional problems (OR 2.22, 95% CI 1.17–4.21) compared to students who had indirect exposure. Students who were exposed to the conflict via the media were more likely to have behavioral–emotional problems than students who had exposure only via others (OR 1.81, 95% CI 1.16–2.84). Students were more likely to have PTSD if they had past exposure to other traumatic life events such as house fire, house robbery or natural disaster such as flooding (OR 1.18, 95% CI 1.02–1.38).
Discussion
This survey was conducted to assess the mental health problems of a cohort of children born when the armed conflict was deemed to have begun in 2004. All students were either directly or indirectly exposed to at least one violent event. The students were found to have a high prevalence of behavioral–emotional problems as well as an increased odds of PTSD. These mental health problems were found in both direct- and indirect-exposure groups but the prevalence was significantly higher in the direct exposure group. The students’ mental health was worsened if they were exposed to violent events from both media and other adults and also to other traumatic life events unrelated to the conflict.
This study reports a five-times higher prevalence of behavioral–emotional problems among children aged around 12 years (42.1%) than that reported among adolescents aged 15–18 years (8.7%) in 2008, 4 years after violence in the area was deemed to have begun [11]. The prevalence of post-traumatic stress disorder among the students found in this study (30.5%) was higher than that reported from previous studies in Thailand 10 years ago in the same area (14–21.9%) [4, 12] and in conflict-affected areas from Kuwait (2%) [13], Lebanon (26%) [14], Sri-Lanka (8.5%) [15], Iraq (10–30%) and Israel (5–8%) [5]. This strongly suggests an increasing trend of mental health problems among children and adolescents exposed to the prolonged conflict over time as also found in studies from Israel [16,17,18]. This study finding urgently calls for appropriate mental health interventions for our young generations.
Our study found that children who directly experienced traumatic events were more likely to develop psychiatric and behavioral or emotional problems than children who had indirect experience, a result consistent with previous studies from Palestine [19, 20] and Afghanistan [21]. However, based on the high magnitude of mental health problems found in the indirect-exposure group in this study, interventions should not only target those with direct experience but also include those indirectly exposed to violence from the mass media or through other adults. Moreover, children exposed to content about violent events either reported by the mass media or from others in this study as well as from the study in Palestine [19] had more anticipatory anxiety and cognitive expressions of distress. Thus, the content from mass media and other adults should be carefully adjusted to be age appropriate.
The prevalence of mental health problems varies widely among countries affected by armed conflict situations [13,14,15,16,17,18]. The magnitude and severity of the problems can be modified by various factors [22]. Our study found that children exposed to other traumatic life events, such as natural disasters, had increased odds of having mental health problems. A previous study among Muslim adults in southern Thailand reported that migration from the community and economic effects of the unrest were associated with an increase in psychiatric symptoms [23]. Others reported daily stressors [24, 25], food shortage during a period of conflict [21], being female [26], exposure to five or more traumatic events and being separated from parents [27], and caregivers mental health status and area of residence [28, 29] were all associated with increased mental health problems. Social support may be a potential mediator, alleviating the effect of war trauma on psychological distress [13] while some local residents showed some habituation to the violence [30]. In addition to giving psychotherapy to children with mental health problems, family and social support should also be given to ameliorate mental health problems among children in areas affected by the conflict.
Strengths and limitations
This study gained some insight into the conflict situation and mental health problems among primary school students and received trust and good cooperation from teachers and schools. This was because the field researchers were from the study areas—they understood the context and the culture well, and could communicate in the local dialect. The outcome measurements were validated and standardized in the Thai context. We have two main limitations. The first one is the limited ability of children to recall violent events when they were less than 3 years of age. However, it is likely that the ability to recall past events would be similar among children in the two groups and this limitation would have a minimal effect on the findings. Second, as this was a school-based study we did not include children who were not enrolled in school. However, the number of children out of school should be minimal since primary school education is compulsory for all children in Thailand.
Conclusions and recommendations
In the prolonged conflict situation that has disrupted the three southernmost provinces of Thailand, a high prevalence of mental health problems was found. It is evident throughout the community in students who have had direct and indirect exposure to traumatic events. Psychoeducation on how content from the mass media and other adults affect the mental health of primary school-aged students should be given. Culturally, appropriate interventions should be further developed and implemented not only to those directly exposed but also to those who have had indirect exposure.
References
Deepsouthwatch Report (2017) Children situation report in Deepsouth Thailand. Deepsouthwatch.org, https://deepsouthwatch.org/sites/default/files/archives/docs/dj_children_in_southern_conflict_2017_edited_clean.pdf. Accessed 11 Jul 2018
Javidi H, Yadollahie M (2012) Post-traumatic stress disorder. Int J Occup Environ Med 3:2–9
Phothisat C (2012) Post-traumatic stress disorder (PTSD) symptoms in children of police officers working in the unrest areas of the Southern Provinces of Thailand. J Psychiatr Assoc Thail 1(57):323–334
Panyayong B, Juntalasena S (2009) Mental health problems among students in the area with continuous insurgency in the deep South of Thailand. J Mental Health Thail 1(17):1–11
Dimitry L (2012) A systematic review on the mental health of children and adolescents in areas of armed conflict in the Middle East. Child Care Health Dev 38:153–161
Prasad A, Prasad P (2009) Children in Conflict Zones. Med J Armed Forces India 65:166–169. https://doi.org/10.1016/S0377-1237(09)80134-2
Wongpiromsarn Y, Wipulakorn P, Nuanmanee S et al (2011) Strengths and Difficulties Questionnaire (SDQ) Thai improved version: change and administration. J Ment Health Thail 19:128–134
Ketumarn P, Piyasilpa V (2009) Posttraumatic stress disorder in children and adolescents: lesson learned from 5-year psychosocial intervention program for schools in Takuapa after tsunami. J Psychiatr Assoc Thai 54:81S–106S
Lauritsen JM, Bruus ME (2005) A comprehensive tool for validated entry and documentation of data. EpiData Assoc, Odense
Core Team R (2017) A language and environment for statistical computing. R Found Stat Comput, Vienna
Tohkani M (2011) Emotional problems and prosocial behavior of adolescents who encounter with unrest situation in three southern border provinces of Thailand. J Psychiatric Assoc Thail 56:363–375
Yongpitayapong C, Wangthong A (2014) Post-traumatic stress disorder symptoms in students at Ban Takumchum school, Amphur Nongjik, Pattani. J Psychiatr Assoc Thail 59:325–333
Llabre MM, Hadi F, La Greca AM, Lai BS (2015) Psychological distress in young adults exposed to war-related trauma in childhood. J Clin Child Adolesc Psychol 44:169–180. https://doi.org/10.1080/15374416.2013.828295
Karam EG, Fayyad J, Karam AN et al (2018) Outcome of depression and anxiety after war: a prospective epidemiologic study of children and adolescents. J Trauma Stress 27:192–199. https://doi.org/10.1002/jts.21895
Siriwardhana C, Pannala G, Siribaddana S et al (2013) Impact of exposure to conflict, tsunami and mental disorders on school absenteeism: findings from a national sample of Sri Lankan children aged 12–17 years. BMC Public Health 13:560. https://doi.org/10.1186/1471-2458-13-560
Dubow EF, Boxer P, Huesmann LR et al (2012) Cumulative effects of exposure to violence on posttraumatic stress in Palestinian and Israeli youth. J Clin Child Adolesc Psychol 41:837–844. https://doi.org/10.1080/15374416.2012.675571
Slone M, Mann S (2016) Effects of war, terrorism and armed conflict on young children: a systematic review. Child Psychiatry Hum Dev 47:950–965. https://doi.org/10.1007/s10578-016-0626-7
Thabet AA, Tawahina AA, Sarraj EE, Vostanis P (2008) Exposure to war trauma and PTSD among parents and children in the Gaza strip. Eur Child Adolesc Psychiatry 17:191. https://doi.org/10.1007/s00787-007-0653-9
Thabet AAM, Abed Y, Vostanis P (2002) Emotional problems in Palestinian children living in a war zone: a cross-sectional study. Lancet 359:1801–1804
Massad SG, Nieto FJ, Palta M et al (2011) Health-related quality of life of Palestinian preschoolers in the Gaza Strip: a cross-sectional study. BMC Public Health 11:253. https://doi.org/10.1186/1471-2458-11-253
Seino K, Takano T, Mashal T et al (2008) Prevalence of and factors influencing posttraumatic stress disorder among mothers of children under five in Kabul, Afghanistan, after decades of armed conflicts. Health Qual Outcomes 6:29
Foster H, Brooks-Gunn J (2015) Children’s exposure to community and war violence and mental health in four African countries. Soc Sci Med 146:292–299. https://doi.org/10.1016/j.socscimed.2015.10.020
Ford K, Jampaklay A, Chamratrithirong A (2017) Mental health in a conflict area: migration, economic stress and religiosity in the three southernmost provinces of Thailand. Int J Soc Psychiatry 63:91–98. https://doi.org/10.1177/0020764016685119
Miller KE, Omidian P, Rasmussen A et al (2008) Daily stressors, war experiences, and mental health in Afghanistan, daily stressors, war experiences, and mental health in Afghanistan. Transcult Psychiatry 45:611–638. https://doi.org/10.1177/1363461508100785
Miller KE, Rasmussen A (2010) War exposure, daily stressors, and mental health in conflict and post-conflict settings: bridging the divide between trauma-focused and psychosocial frameworks. Soc Sci Med 70:7–16
Perkins JD, Ajeeb M, Fadel L, Saleh G (2018) Mental health in Syrian children with a focus on post-traumatic stress: a cross-sectional study from Syrian schools. Soc Psychiatry Psychiatr Epidemiol 53:1231–1239. https://doi.org/10.1007/s00127-018-1573-3
Macksoud MS, Aber JL (1996) The war experiences and psychosocial development of children in Lebanon. Child Dev 67:70–88. https://doi.org/10.1111/j.1467-8624.1996.tb01720.x
Panter-Brick C, Eggerman M, Gonzalez V, Safdar S (2009) Violence, suffering, and mental health in Afghanistan: a school-based survey. Lancet 374:807–816. https://doi.org/10.1016/S0140-6736(09)61080-1
Tol WA, Song S, Jordans MJD (2013) Annual Research Review: resilience and mental health in children and adolescents living in areas of armed conflict—a systematic review of findings in low- and middle-income countries. J Child Psychol Psychiatry 54:445–460. https://doi.org/10.1111/jcpp.12053
Ford K, Jampaklay A, Chamratrithirong A (2018) Coming of age in a conflict area: mental health, education, employment, migration and family formation in the southernmost provinces of Thailand. Int J Soc Psychiatry 64:225–234
Acknowledgements
This study was financially supported by the Discipline of Excellence Program, Epidemiology Unit, Faculty of Medicine, Prince of Songkla University, Thailand. We are grateful to all teachers and students who participated in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Jayuphan, J., Sangthong, R., Hayeevani, N. et al. Mental health problems from direct vs indirect exposure to violent events among children born and growing up in a conflict zone of southern Thailand. Soc Psychiatry Psychiatr Epidemiol 55, 57–62 (2020). https://doi.org/10.1007/s00127-019-01732-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-019-01732-8