Abstract
Purpose
To compare the prevalence and pattern of comorbid substance use disorders (SUD) between patients with schizophrenia, bipolar disorder, and depressive illness.
Methods
Data on presence of alcohol use disorder (AUD) and non-alcohol drug use disorder (DUD) were retrieved from the Norwegian Patient Register for individuals born between 1950 and 1989 who in the period 2009–2013 were diagnosed with schizophrenia, bipolar disorder or depressive illness according to the 10th version of the WHO International Classification of Diseases. The prevalence of AUD only, DUD only, or both was compared between men and women across age and diagnostic groups.
Results
The prevalence of SUD was 25.1 % in schizophrenia (AUD: 4.6 %, DUD: 15.6 %, AUD and DUD: 4.9 %), 20.1 % in bipolar disorder (AUD: 8.1 %, DUD: 7.6 %, AUD and DUD: 4.4 %), and 10.9 % in depressive illness (AUD: 4.4 %, DUD: 4.3 %, AUD and DUD: 2.2 %). Middle-aged men with bipolar disorder had the highest prevalence of AUD (19.1 %) and young men with schizophrenia had the highest prevalence of DUD (29.6 %). Of the specific DUDs, all but sedative use disorder were more prevalent in schizophrenia than the other groups. Cannabis and stimulant use disorder was found among 8.8 and 8.9 %, respectively, of the men with schizophrenia.
Conclusions
The alarmingly high prevalence of DUD among young patients with severe mental disorders should encourage preventive efforts to reduce illicit drug use in the adolescent population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The presence of comorbid substance use disorders (SUD) poses a substantial challenge in the treatment of patients with severe mental disorders [1]. Comorbid SUDs are associated with more severe psychotic and depressive symptoms [2, 3], more frequent hospitalizations [4], more involuntary hospitalization [5], and poorer treatment response and outcome [6, 7]. Most studies of comorbidity between severe mental disorders and SUD are based on data from surveys or clinical samples. Results from representative US population surveys have indicated that 30–50 % of individuals with psychotic illness [8, 9] or affective mood disorder [10, 11] have a comorbid alcohol use disorder (AUD) or non-alcohol drug use disorder (DUD). More recently, two smaller clinical studies from Scandinavian populations have reported similar results with prevalences of 20–30 % for SUD in schizophrenia [12, 13] and bipolar disorder [7, 14].
Although these figures are disturbingly high, the mechanisms underlying the comorbidity between severe mental disorders and SUD are poorly understood. Comorbidities can reflect a number of relationships, including self-medication, common etiology or direct causation [15], and can vary between types of substances and mental disorders as well as sex and age. It is therefore necessary to estimate comorbidity in samples that are large enough to allow all these latter factors to be taken into consideration.
Surveys and clinical studies rely on informed consent from study participants, thus excluding individuals not able or willing to participate in clinical and diagnostic assessments. The samples may therefore be biased towards patients with higher level of functioning, while severely ill patients with poor outcome may be underrepresented. National mandatory health registers, on the other hand, are not based on active consent, and will capture all individuals with the diagnosis in question who have been in contact with the health care system. The large number of patients listed in nationwide registries will also allow for analyses stratified by sex and age. We are not aware of any prior study using population-based health registries to estimate the comorbidity between severe mental disorders and SUD.
Aims of the study
By utilizing data from the Norwegian Patients Register (NPR), which is a mandatory national registry covering all patients receiving public specialist health care in Norway, we aimed to estimate and compare the prevalence of comorbid SUD among individuals with and without severe mental disorders in Norway. More specifically, we estimated the prevalence of AUD and DUD separately for the three disorders schizophrenia, bipolar disorder, and depressive illness, and investigated differences in proportion and type of SUD across diagnosis, sex and age.
Methods
Subjects
The NPR is an administrative database of records reported by all government-owned hospitals and outpatient clinics, and by all private health clinics that receive governmental reimbursement. In Norway, governmentally funded mental health clinics offering in- and outpatient treatment are available across the country to serve the entire population of need. The NPR has included the unique personal identification number since 2008. Consequently, person-specific data are available from 2008 onwards. Substance use treatment facilities have reported data to the NPR from 2009 onwards. Diagnostic codes in the NPR follow the World Health Organization’s International Classification of Diseases, version 10 (ICD-10).
For the present study, we confined the study population to individuals born between 1950 and 1989 (24–63 years of age by the end of the study period) who in the period 2009–2013 were registered at least twice in the NPR with an ICD-10 diagnosis of schizophrenia (F20), bipolar disorder (F30–31), or depressive illness (F32–34). To assure diagnostic specificity, patients in the bipolar disorder group were excluded if they had also been diagnosed with a schizophrenia spectrum disorder [schizophrenia, schizotypal disorder (F21), delusional disorder (F22), or schizoaffective disorder (F25)], and patients in the depressive illness group were excluded if they had been diagnosed with a schizophrenia spectrum or bipolar disorder (F20–31). Since this is the first nationwide registry-based study of psychotic disorders in Norway, we aimed to compare prevalence and pattern of comorbid SUD across broader groups of psychotic disorders. Hence, we included three additional comparison groups consisting of patients registered twice or more with; (1) delusional disorder, (2) schizoaffective disorder, or (3) depressive disorder with psychotic symptoms (F32.3, F33.3). To assure diagnostic specificity in these groups as well, patients in the delusional and schizoaffective disorder groups were excluded if they also had a diagnosis of schizophrenia, and patients in the depressive disorder with psychotic symptoms group were never diagnosed with a schizophrenia spectrum or bipolar disorder.
For analyses of comorbid SUD, the following ICD-10 categories were included: AUD, registered with the ICD-10 code F10 at least once, but never registered with F11–F19; DUD, registered with F11–F19 at least once, but never registered with F10; AUD and DUD, registered at least once with F10 and at least once with F11–F19 during the period 2009–2013. The reason for not requiring at least two registrations for SUD diagnoses was to maximize the detection rate. The true prevalence of SUD in the Norwegian population is unknown. As a proxy for a general population comparison group, we retrieved the following information from NPR:
-
1.
Number of individuals who were registered with an AUD, but never with a DUD.
-
2.
Number of individuals who were registered with a DUD, but never with an AUD.
-
3.
Number of individuals who were registered with both AUD and DUD.
To explore the distribution of specific substances of abuse, we calculated the number of individuals registered at least once with each of the diagnoses F11—opiate use disorder, F12—cannabis use disorder, F13—sedative use disorder, F15—stimulant use disorder, and F19—polysubstance use disorder. The groups are not mutually exclusive since we did not exclude patients registered with multiple SUDs.
The use of anonymous research files does not require regulatory ethics approval in Norway. To preserve patient anonymity, the NPR grouped year of birth into 5-year cohorts (1950–1954, 1955–1959, 1960–1964, 1965–1969, 1970–1974, 1975–1979, 1980–1984, 1985–1989), and included only information on sex and the number of registrations with the relevant diagnoses in the research file.
Statistical analysis
Five-year prevalence estimates of severe mental disorders and SUD were obtained by dividing the number of patients within each diagnostic category, by the mean number of Norwegian residents with corresponding age and sex in the period between 2009 and 2013. Population figures were obtained from the website of Statistics Norway (http://www.ssb.no). Prevalence of comorbid SUD for each diagnostic category was estimated by dividing number of patients with both the specific severe mental disorder and SUD by the total number of patients with the disorder.
Results
Five-year prevalence of psychotic and affective disorders
Among 2,659,966 adult individuals (1,360,153 men and 1,299,813 women) born between 1950 and 1989, we identified 9,002 persons (5,842 men and 3,160 women) constituting 0.34 % of the population (0.43 % of the men and 0.24 % of the women) who were registered twice or more in the NPR with a schizophrenia diagnosis in the period 2009–2013. A total of 15,540 individuals (6,306 men and 9,234 women), constituting 0.58 % of the population (0.46 % of the men and 0.71 % of the women), were diagnosed with bipolar disorder, and 87,540 individuals (32,104 men and 55,436 women), constituting 3.3 % of the population (2.4 % of the men and 4.3 % of the women), were registered with depressive illness. For further details regarding prevalence of other diagnostic categories, see Table 1.
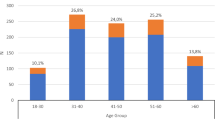
More men than women were diagnosed with schizophrenia and delusional disorder, while more women than men were diagnosed with schizoaffective disorder, bipolar disorder, depressive disorder with psychotic symptoms, and depressive illness. The difference in prevalence between men and women was highest in the youngest age groups for schizophrenia, bipolar disorder and depressive illness, while the sex difference was modest in the oldest age groups (Fig. 1).
Five-year prevalence of SUD
Among patients with schizophrenia, 25.1 % were also registered with a SUD diagnosis (AUD: 4.6 %, DUD: 15.6 %, AUD and DUD: 4.9 %). Corresponding figures for bipolar disorder were 20.1 % (AUD: 8.1 %, DUD: 7.6 %, AUD and DUD: 4.4 %), and for depressive illness 10.9 % (AUD: 4.4 %, DUD: 4.3 %, AUD and DUD: 2.2 %). The prevalence of SUD regardless of comorbid disorders was 2.4 % (AUD: 1.0 %, DUD: 1.0 %, AUD and DUD: 0.4 %). See Table 2 for details regarding prevalence of SUD for other diagnostic categories.
The 5-year prevalence of SUD was higher for men than women for both AUD and DUD in all diagnostic groups.
In schizophrenia, cannabis and stimulant use disorders were the most prevalent specific SUDs among men and stimulant use disorder was the most prevalent specific SUD among women (Table 3). For bipolar disorder, depressive illness and in the population, cannabis use disorder was the most prevalent specific SUD among men and sedative use disorder was the most prevalent specific SUD among women.
When the sample was stratified by age intervals, the prevalence of any SUD was gradually declining with age both for men and women with schizophrenia, while the prevalence of any SUD was more stable across age in bipolar disorder, depressive illness, and in the population (Fig. 2). The total prevalence of SUD was 43.5 % among men and 30.3 % among women in their mid-20s with schizophrenia, while in bipolar disorder, the total prevalence of SUD was 29.5 % among men and 19.3 % among women in their mid-20s. The relative distribution of types of SUD changed from predominantly DUD in younger age to predominantly AUD in older age for all diagnostic groups. The highest prevalence of AUD (19.1 %) was found among men with bipolar disorder in their mid-50s, and the highest prevalence of DUD (29.6 %) was found among men with schizophrenia in their mid-20s.
Five-year prevalence of alcohol use disorders (AUD), non-alcohol drug use disorders (DUD) or both AUD and DUD among men and women with schizophrenia (SCZ, upper row), bipolar disorder (BIP, upper middle row), depressive illness (DEP, lower middle row), and among population individuals who were registered with AUD and/or DUD regardless of other diagnoses (POP, bottom row) born between 1950 and 1989. Data obtained from the Norwegian Patient Register for the period 2009–2013. Note differences in range of y-axis across panels
Discussion
We will highlight three major findings of the present study on prevalence and pattern of comorbid SUD among patients diagnosed with severe mental disorders in specialist health service in Norway between 2009 and 2013. (1) Patients with schizophrenia, bipolar disorder and depressive illness had up to a tenfold higher prevalence of SUD compared to the population estimate. (2) Patients with schizophrenia had three times higher prevalence of DUD than AUD, while patients with bipolar disorder, depressive illness and the population had equal prevalence of AUD and DUD. (3) The prevalence of SUD was particularly high among young patients with schizophrenia.
Registry-based versus population-based samples
This is to our knowledge the first registry-based study of comorbid SUD in severe mental disorders. A direct comparison with findings from population surveys is not straightforward due to differences in sampling characteristics. While registry-based samples are not dependent on patients’ informed consent, they will only include people who have been in contact with the health care system, which implies a bias towards more severely affected patients. On the other hand, population surveys may detect individuals with a diagnosis who are not in treatment but will exclude patients not able or willing to participate, which implies a bias towards higher functioning and less disabled patients. These differences may induce diagnosis-dependent bias in estimates of prevalence. Severe mental disorders, such as schizophrenia and bipolar disorder, will to a larger extent be found in registry-based samples, while disorders such as mild to moderate depression and anxiety disorders will to a larger extent be reached by population surveys.
According to clinical guidelines in Norway, all patients with psychotic illness should be referred to specialist health care for diagnostic evaluation and initiation of treatment. In Norway, there are governmentally funded mental health hospitals with in- and outpatient clinics serving the entire population. There is a maximum annual fee for outpatient treatment, while inpatient treatment is free of charge. A number of psychologists and psychiatrists have their own private practice but receive reimbursement from the Government, and their patients do not have to pay more than the abovementioned maximum annual fee. Some private therapists do not receive reimbursement and consequently charge more from their patients. For patients with severe mental illness, who often have restricted economic capacity, private treatment is less of an option. All public and private specialist health services financed by the Government are obliged to report data to the NPR. We assume therefore that most patients diagnosed with schizophrenia in Norway in the period 2009–2013 are included in the present study. The prevalence estimates of depressive illness and substance use disorders, however, are presumably too low, since these patients are often treated by GPs or do not seek treatment at all.
Prevalence of SUD in schizophrenia
Among 9,002 patients registered at least twice with schizophrenia, 2,261 (25.1 %) were also diagnosed with a SUD in the 5-year period. In large US population surveys such as the Epidemiological Catchment’s Area (ECA) study [8] and the National Comorbidity Survey (NCS) [9], about half of patients with schizophrenia had a lifetime history of comorbid SUD. However, in the National Comorbidity Survey Replication (NCS-R), which is the most recent survey, lifetime prevalence of any SUD was 26.5 % [16]. Some of the discrepancy across studies may be due to a more restrictive definition of AUD in DSM-IV, which was applied in NCS-R, compared to DSM-III and DSM-III-R which was applied in the earlier surveys. In two recent clinical studies of first-episode non-affective psychosis patients in Norway and Denmark, in which patients were recruited from the clinic and assessed for DSM-IV diagnoses using structured interviews, 20–30 % of the patients also met diagnostic criteria for a current SUD [12, 13]. A putative explanation for lower prevalence estimates of comorbid SUD in registry-based samples may be that clinicians tend to focus on the main diagnosis and may fail to report relevant secondary diagnoses. However, our finding of a 25.1 % 5-year prevalence of SUD among patients with schizophrenia is in line with prevalence estimates from the most recent population survey from the US (NCS-R) and clinical studies from Scandinavia.
We report a three times higher proportion of DUD than AUD among patients with schizophrenia. In contrast, AUD were more common than DUD among patients with schizophrenia in both the ECA study [8] and NCS [9], while prevalence of AUD and DUD was similar among patient with schizophrenia in the NCS-R [16]. Recent clinical studies have demonstrated higher prevalence of DUD than AUD in first-episode psychosis patients [12, 13], while AUD and DUD were equally prevalent in a mixed sample of patients with schizophrenia [14]. In two meta-analyses of clinical studies of patients with schizophrenia, lifetime prevalence was 20.6 % for AUD [17] and 26.1 % for cannabis use disorders [18]. The results from the meta-analyses are in line with our finding of higher risk of DUD than AUD in schizophrenia. The trend for higher risk of DUD than AUD among patients with schizophrenia found in recent studies may represent a cohort effect reflecting availability of substances of abuse. In Norway, the availability of illicit drugs has increased steadily during the last 20–30 years (data available at the Norwegian Institute for Alcohol and Drug Research website http://www.sirus.no).
Prevalence of SUD in bipolar disorder
Among 15,540 patients registered at least twice with bipolar disorder but never with schizophrenia, 3,120 (20.1 %) were also diagnosed with a SUD in the 5-year period. In contrast, 61 % of patients with bipolar disorder had a lifetime SUD in the ECA [8], while the prevalence was 42.3 % in the NCS-R [19] and 36.6 % in the World Mental Health Survey [20]. In the National Epidemiological Survey on Alcohol and Related Conditions (NESARC), which is the hitherto largest study from one country, including more than 40,000 adult US citizens, lifetime prevalence was 58.0 % for AUD and 37.5 % for DUD among patients with bipolar disorder type I [10]. A clinical study of 125 bipolar disorder patients in Oslo demonstrated that 30 % also had a lifetime SUD [7], while a review of epidemiological and clinical studies concluded that about 40 % of patients with bipolar disorder type I and 20 % of patients with bipolar disorder type II had a lifetime SUD [21]. Our finding of a 5-year prevalence of 20.1 % for SUD in bipolar disorder is lower than expected from survey and clinical studies and may reflect that only a subset of patients with bipolar disorder and SUD are enrolled in specialist health service during a given 5-year period.
We report similar rates of AUD and DUD in bipolar disorder. This finding is in line with results from the ECA study [8], while prevalence of AUD was higher than DUD for patients with bipolar disorder in the other large population surveys [4, 19, 20], as well as in recent clinical studies from Norway [7, 14]. The discrepancy in distribution of AUD and DUD between the present study and previous survey and clinical studies may be due to the fact that presence of DUD is related to a poorer treatment response [7]. Hence, bipolar disorder patients with comorbid DUD may be overrepresented in specialist health registry samples.
Prevalence of SUD in depressive illness
Among 87,540 patients registered at least twice with depressive illness but never with schizophrenia or bipolar disorder, 9,522 (10.9 %) were also registered with a comorbid SUD in the 5-year period. This figure is lower than the 20–40 % reported from US population surveys [8, 11]. We found that prevalence of AUD and DUD was of similar magnitude among patients with depressive illness. This was also the case among patients with unipolar depression in the ECA study [8], while AUD was more than twice as prevalent as DUD among patients with major depressive disorder in the NESARC [11]. Our finding of similar proportions of AUD and DUD in depressive illness may reflect the fact that DUD is overrepresented in specialist health registry samples due to a more severe disease course.
Prevalence of SUD in the population
Among all registered individuals born between 1950 and 1989, 2.4 % were registered in the NPR with a SUD (AUD only 1.0 %, DUD only 1.0 %, AUD and DUD 0.4 %) between 2009 and 2013. The prevalence estimate of AUD was considerably lower than expected based on data from previous population surveys in Norway [22, 23], which indicates that only a small fraction of patients with AUD are found and registered in specialist health care. The true prevalence of DUD in Norway is unknown. Kringlen and co-workers found that 3.4 % of the population in Oslo met DSM-III-R criteria for a lifetime drug abuse or dependence [22], while drug use disorders were present in only 0.4 % of the population in a rural county of Western Norway [23]. Our results demonstrate that among patients in specialist health care in Norway, the prevalence of SUD is up to ten times higher in patients with schizophrenia, bipolar disorder, or depressive illness compared to the proportion of the general population who are registered with a SUD in the NPR.
Pattern of SUD comorbidity across diagnoses
When comparing prevalence and pattern of SUD across diagnostic groups, we found that DUD was three times more common than AUD among patients with schizophrenia, while AUD and DUD were equally common among patients with bipolar disorder or depressive illness, and among patients with SUD regardless of other disorders. The findings are in line with results of a clinical study specifically comparing substance use in patients with schizophrenia and bipolar disorder, where stimulant use was more prevalent in schizophrenia, while patients with bipolar disorder had a higher rate of alcohol consumption [24]. When we included a broader spectrum of psychotic disorders, the pattern of higher risk of DUD than AUD in schizophrenia spectrum disorders and equal risk of AUD and DUD in affective disorders was compelling (Table 2). If differences in types of comorbid SUD in severe mental illness were mainly determined by availability of drugs, one would expect similar distributions of AUD and DUD across diagnostic boundaries and time.
One possible explanation for the strong link between schizophrenia and DUD is that certain illicit drugs are involved in the causal pathways for schizophrenia. Use of cannabis and amphetamine, which was particularly prevalent among men with schizophrenia in the present study (Table 3), may induce or exacerbate psychotic symptoms both in healthy and mentally ill persons [25]. There is also a strong association between cannabis use and earlier onset of schizophrenia [26], which indicates that use of cannabis is a risk factor for schizophrenia [27]. It remains puzzling that patients with schizophrenia tend to use substances which are known to exacerbate psychotic symptoms and impede on cognitive functioning. There is some preclinical evidence for shared neurobiological vulnerability between schizophrenia and illicit drug use [28], but the specific mechanisms are not fully known.
Both psychotic illness and SUD have a peak onset in late adolescence and early adulthood. The onset of both disorders may be abrupt or insidious, which makes it difficult to ascertain the direction of causation for the comorbidity. The pattern of comorbid SUD reported in the present study may reflect specific pathophysiological mechanisms underlying schizophrenia and affective disorders. Future longitudinal studies in genetically informative samples are needed to disentangle the etiological mechanisms for the co-occurrence of severe mental disorders and SUD.
Age-stratified analyses
One striking finding in the present study was that schizophrenia differs from affective disorders with respect to the age trend of SUD comorbidity. In schizophrenia patients, the prevalence of SUD was about 30–40 % in the youngest cohorts, predominantly due to illicit drug use disorders, while the proportion of AUD and DUD decreased sharply with increasing age. In contrast, patients with bipolar disorder and depressive illness had a quite similar prevalence of SUD across age, but the type of SUD changed from predominantly DUD in younger age to predominantly AUD in older age. These findings may indicate that there are specific mechanisms that render patients with schizophrenia more vulnerable to illicit drug use disorders, particularly in early phase of their illness, while patients with affective disorders are at increasing risk for developing an AUD along the disease course.
Implications of the study
Given that comorbid SUD complicates treatment and is associated with worse outcome of severe mental disorders [1–7], the high prevalence of DUD among young patients with schizophrenia must be taken into account by clinicians and health authorities. Of particular importance is the widespread use of cannabis and stimulants, which may be expected to increase, given the political movement in US and elsewhere aiming to legalize use of cannabis. The results of the present study should encourage preventive efforts to reduce illicit drug use in the adolescent population, and clinical facilities serving young patients with psychotic disorders should offer special treatment options focusing on harmful use of substances.
Strengths and limitations
The major strength of the present study was the use of a mandatory health registry which covers the entire population treated in specialist health care facilities, leading to minimal dropout. The large sample size enabled an in-depth analysis of comorbid SUD across diagnosis, age and sex. By including all patients registered with a psychotic or affective disorder in the NPR in the period 2009–2013, we assured that the sample represents the range of patients found in the clinic.
However, the results must be interpreted with the following limitations in mind. First, the study only included people who had been in contact with specialist health care services during 5 years. Findings from population-based surveys have demonstrated that less than half of subjects fulfilling criteria for one or more mental disorders have received professional treatment [20, 29]. In consequence, the 5-year prevalence estimates reported in the present study are lower than the true prevalence of severe mental disorders and comorbid SUD in the population. Second, the ratio of comorbid to single disorder patients will always be higher in hospital than population settings as first demonstrated by Berkson in 1946 [30]. Comorbid cases usually have a more severe form of disease compared to single disorder cases [31], which increases the probability of being found in treatment samples. To amend for Berkson’s bias, we included a comparison group consisting of patients registered in NPR with a SUD notwithstanding other diagnoses. Third, diagnoses of psychotic disorders and SUD in the NPR have not yet been subjected to formal validity testing. Two recent reports comparing clinical and research-based diagnostic evaluations among first-time admitted patients in Northern Norway demonstrated good agreement for schizophrenia, but inconsistent report of comorbid diagnoses [32], and moderate agreement for affective disorders [33]. In parallel, systematic assessments of diagnostic accuracy in similar registries in other Nordic countries have shown acceptable agreement between register diagnoses of psychotic disorders and research diagnoses based on scrutiny of case notes or structured diagnostic interviews [34–37]. To maximize the detection of comorbid cases, we evaluated all diagnoses set by any specialist health care facility across 5 years and did not require that comorbid diagnoses were set on the same occasion as the primary diagnosis, and we did not require two or more registrations for each type of SUD for the patient to be characterized as a comorbid case. Fourth, even though we applied the mean population figure across 2009–2013 as denominator for prevalence estimates, there might be bias due to unknown rate of emigration and deaths in the background population.
References
Negrete JC (2003) Clinical aspects of substance abuse in persons with schizophrenia. Can J Psychiatry 48:14–21
Margolese HC, Malchy L, Negrete JC, Tempier R, Gill K (2004) Drug and alcohol use among patients with schizophrenia and related psychoses: levels and consequences. Schizophr Res 67:157–166
Turkington A, Mulholland CC, Rushe TM, Anderson R, McCaul R, Barrett SL, Barr RS, Cooper SJ (2009) Impact of persistent substance misuse on 1-year outcome in first-episode psychosis. Br J Psychiatry 195:242–248
Cantor-Graae E, Nordström LG, Mcneil TF (2001) Substance abuse in schizophrenia: a review of the literature and a study of correlates in Sweden. Schizophr Res 48:69–82
Opsal A, Clausen T, Kristensen O, Elvik I, Joa I, Larsen TK (2011) Involuntary hospitalization of first-episode psychosis with substance abuse during a 2-year follow-up. Acta Psychiatr Scand 124:198–204
Kavanagh DJ, McGrath J, Saunders JB, Dore G, Clark D (2002) Substance misuse in patients with schizophrenia: epidemiology and management. Drugs 62:743–755
Lagerberg TV, Andreassen OA, Ringen PA, Berg AO, Larsson S, Agartz I, Sundet K, Melle I (2010) Excessive substance use in bipolar disorder is associated with impaired functioning rather than clinical characteristics, a descriptive study. BMC Psychiatry 10:9. doi:10.1186/1471-244X-10-9
Regier DA, Farmer ME, Rae DS, Locke BZ, Keith SJ, Judd LL, Goodwin FK (1990) Comorbidity of mental disorders with alcohol and other drug abuse. Results from the Epidemiological Catchment Area (ECA) Study. JAMA 264:2511–2518
Kendler KS, Gallagher TJ, Abelson JM, Kessler RC (1996) Lifetime prevalence, demographic risk factors, and diagnostic validity of nonaffective psychosis as assessed in a US community sample. The National Comorbidity Survey. Arch Gen Psychiatry 53:1022–1031
Grant BF, Stinson FS, Hasin DS, Dawson DA, Chou SP, Ruan WJ, Huang B (2005) Prevalence, correlates, and comorbidity of bipolar I disorder and axis I and II disorders: results from the National Epidemiologic Survey on alcohol and related conditions. J Clin Psychiatry 66:1205–1215
Hasin DS, Goodwin RD, Stinson FS, Grant BF (2005) Epidemiology of major depressive disorder: results from the National Epidemiologic Survey on alcoholism and related conditions. Arch Gen Psychiatry 62:1097–1106
Larsen TK, Melle I, Auestad B, Friis S, Haahr U, Johannessen JO, Opjordsmoen S, Rund BR, Simonsen E, Vaglum P, McGlashan TH (2006) Substance abuse in first-episode non-affective psychosis. Schizophr Res 88:55–62
Nesvåg R, Lange EH, Faerden A, Barrett EA, Emilsson B, Ringen PA, Andreassen OA, Melle I, Agartz I (2010) The use of screening instruments for detecting alcohol and other drug use disorders in first-episode psychosis. Psychiatry Res 177:228–234
Ringen PA, Melle I, Birkenaes AB, Engh JA, Faerden A, Jónsdóttir H, Nesvåg R, Vaskinn A, Friis S, Larsen F, Opjordsmoen S, Sundet K, Andreassen OA (2008) Illicit drug use in patients with psychotic disorders compared with that in the general population: a cross-sectional study. Acta Psychiatr Scand 117:133–138
Neale MC, Kendler KS (1995) Models of comorbidity for multifactorial disorders. Am J Hum Genet 57:935–953
Kessler RC, Birnbaum H, Demler O, Falloon IR, Gagnon E, Guyer M, Howes MJ, Kendler KS, Shi L, Walters E, Wu EQ (2005) The prevalence and correlates of nonaffective psychosis in the National Comorbidity Survey Replication (NCS-R). Biol Psychiatry 58:668–676
Koskinen J, Löhönen J, Koponen H, Isohanni M, Miettunen J (2009) Prevalence of alcohol use disorders in schizophrenia—a systematic review and meta-analysis. Acta Psychiatr Scand 120:85–96
Koskinen J, Löhönen J, Koponen H, Isohanni M, Miettunen J (2010) Rate of cannabis use disorders in clinical samples of patients with schizophrenia: a meta-analysis. Schizophr Bull 36:1115–1130
Merikangas KR, Akiskal HS, Angst J, Greenberg PE, Hirschfeld RM, Petukhova M, Kessler RC (2007) Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry 64:543–552
Merikangas KR, Jin R, He JP, Kessler RC, Lee S, Sampson NA, Viana MC, Andrade LH, Hu C, Karam EG, Ladea M, Medina-Mora ME, Ono Y, Posada-Villa J, Sagar R, Wells JE, Zarkov Z (2011) Prevalence and correlates of bipolar spectrum disorder in the World Mental Health Survey Initiative. Arch Gen Psychiatry 68:241–251
Cerullo MA, Strakowski SM (2007) The prevalence and significance of substance use disorders in bipolar type I and II disorder. Subst Abuse Treat Prev Policy 2:29. doi:10.1186/1747-597X-2-29
Kringlen E, Torgersen S, Cramer V (2001) A Norwegian psychiatric epidemiological study. Am J Psychiatry 158:1091–1098
Kringlen E, Torgersen S, Cramer V (2006) Mental illness in a rural area: a Norwegian psychiatric epidemiological study. Soc Psychiatry Psychiatr Epidemiol 41:713–719
Ringen PA, Lagerberg TV, Birkenaes AB, Engn J, Faerden A, Jónsdottir H, Nesvåg R, Friis S, Opjordsmoen S, Larsen F, Melle I, Andreassen OA (2008) Differences in prevalence and patterns of substance use in schizophrenia and bipolar disorder. Psychol Med 38:1241–1249
Di Forti M, Morrison PD, Butt A, Murray RM (2007) Cannabis use and psychiatric and cognitive disorders: the chicken or the egg? Curr Opin Psychiatry 20:228–234
Di Forti M, Sallis H, Allegri F, Trotta A, Ferraro L, Stilo SA, Marconi A, La Cascia C, Reis Marques T, Pariante C, Dazzan P, Mondelli V, Paparelli A, Kolliakou A, Prata D, Gaughran F, David AS, Morgan C, Stahl D, Khondoker M, Maccabe JH, Murray RM (2014) Daily use, especially of high-potency cannabis, drives the earlier onset of psychosis in cannabis users. Schizophr Bull 40:1509–1517. doi:10.1093/schbul/sbt181
Arseneault L, Cannon M, Witton J, Murray RM (2004) Causal association between cannabis and psychosis: examination of the evidence. Br J Psychiatry 184:110–117
Chambers RA, Krystal JH, Self DW (2001) A neurobiological basis for substance abuse comorbidity in schizophrenia. Biol Psychiatry 50:71–83
Kessler RC, McGonagle KA, Zhao S, Nelson CB, Hughes M, Eshleman S, Wittchen HU, Kendler KS (1994) Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey. Arch Gen Psychiatry 51:8–19
Berkson J (1946) Limitations of the application of fourfold table analysis to hospital data. Biom Bull 2:47–53
Newman DL, Moffitt TE, Caspi A, Silva PA (1998) Comorbid mental disorders: implications for treatment and sample selection. J Abnorm Psychol 107:305–311
Oiesvold T, Nivison M, Hansen V, Skre I, Ostensen L, Sørgaard KW (2013) Diagnosing comorbidity in psychiatric hospital: challenging the validity of administrative registers. BMC Psychiatry 13:13. doi:10.1186/1471-244X-13-13
Øiesvold T, Nivison M, Hansen V, Sørgaard KW, Østensen L, Skre I (2012) Classification of bipolar disorder in psychiatric hospital. a prospective cohort study. BMC Psychiatry 12:13–14. doi:10.1186/1471-244X-12-13
Jakobsen KD, Frederiksen JN, Hansen T, Jansson LB, Parnas J, Werge T (2005) Reliability of clinical ICD-10 schizophrenia diagnoses. Nord J Psychiatry 59:209–212
Dalman C, Broms J, Cullberg J, Allebeck P (2002) Young cases of schizophrenia identified in a national inpatient register—are the diagnoses valid? Soc Psychiatry Psychiatr Epidemiol 37:527–531
Ekholm B, Ekholm A, Adolfsson R, Vares M, Osby U, Sedvall GC, Jönsson EG (2005) Evaluation of diagnostic procedures in Swedish patients with schizophrenia and related psychoses. Nord J Psychiatry 59:457–464
Pihlajamaa J, Suvisaari J, Henriksson M, Heilä H, Karjalainen E, Koskela J, Cannon M, Lönnqvist J (2008) The validity of schizophrenia diagnosis in the Finnish Hospital Discharge Register: findings from a 10-year birth cohort sample. Nord J Psychiatry 62:198–203
Acknowledgments
This project was funded by the Norwegian Institute of Public Health. We thank Martin Mydske Nilsen for practical support.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nesvåg, R., Knudsen, G.P., Bakken, I.J. et al. Substance use disorders in schizophrenia, bipolar disorder, and depressive illness: a registry-based study. Soc Psychiatry Psychiatr Epidemiol 50, 1267–1276 (2015). https://doi.org/10.1007/s00127-015-1025-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-015-1025-2