Abstract
Severe burn injuries are defined by a prolonged hypermetabolic response characterized by increases in resting energy expenditure, systemic catabolism, and multi-organ dysfunction. The sustained elevation of catecholamines following a burn injury is thought to significantly contribute to this hypermetabolic response, leading to changes in adipose tissue such as increased lipolysis and the browning of subcutaneous white adipose tissue (WAT). Failure to mitigate these adverse changes within the adipose tissue has been shown to exacerbate the post-burn hypermetabolic response and lead to negative outcomes. Propranolol, a non-selective β-blocker, has been clinically administered to improve outcomes of pediatric and adult burn patients, but there is inadequate knowledge of its effects on the distinct adipose tissue depots. In this study, we investigated the adipose depot-specific alterations that occur in response to burn injury. Moreover, we explored the therapeutic effects of β-adrenoceptor blockade via the drug propranolol in attenuating these burn-induced pathophysiological changes within the different fat depots. Using a murine model of thermal injury, we show that burn injury induces endoplasmic reticulum (ER) stress in the epididymal (eWAT) but not in the inguinal (iWAT) WAT depot. Conversely, burn injury induces the activation of key lipolytic pathways in both eWAT and iWAT depots. Treatment of burn mice with propranolol effectively mitigated adverse burn-induced alterations in the adipose by alleviating ER stress in the eWAT and reducing lipolysis in both depots. Furthermore, propranolol treatment in post-burn mice attenuated UCP1-mediated subcutaneous WAT browning following injury. Overall, our findings suggest that propranolol serves as an effective therapeutic intervention to mitigate the adverse changes induced by burn injury, including ER stress, lipotoxicity, and WAT browning, in both adipose tissue depots.
Key messages
-
Burn injury adversely affects adipose tissue metabolism via distinct changes in both visceral and subcutaneous adipose depots.
-
Propranolol, a non-selective β-adrenergic blocker, attenuates many of the adverse adipose tissue changes mediated by burn injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
According to the WHO, every year, approximately 11 million individuals sustain burn injuries, resulting in an estimated 180,000 deaths globally [1]. The high morbidity and mortality in these patients are largely driven by a persistent hypermetabolic stress response that is characterized by insulin resistance, increased lipid catabolism, and multi-organ dysfunction [2]. Following a burn injury, the hypermetabolic response is triggered to restore homeostasis and “survive the initial insult” by mobilizing energy reserves to meet increased energy demands necessary for maintaining organ function and supporting skin regeneration [2]. Unfortunately, this survival response becomes dysregulated in both duration and magnitude, going well beyond the needs of the patient, often persisting for years after the initial trauma [3].
In fact, immunological and metabolic profiling of blood from burn patients has revealed a 40-fold increase in catecholamines (CAs) following a burn injury [2]. Moreover, urinary epinephrine and norepinephrine are also elevated for months following a severe burn (> 30% total body surface area (TBSA) in adults) [2]. This heightened and persistent increase in CAs has been implicated as a major driver of several facets of the post-burn hypermetabolic response, especially within the adipose tissue [4]. Indeed, the release of CAs has been demonstrated to promote the browning of white adipose tissue (WAT) and the expression of uncoupling protein 1 (UCP1), which aids in dissipating excess energy as heat [4, 5]. WAT browning activation in burn patients has been implicated as a potential driver of post-burn hypermetabolism and has been associated with insulin resistance (IR), muscle catabolism, and hepatic steatosis [6,7,8]. CAs have also been found to activate β-adrenergic receptors expressed in adipocytes, leading to the stimulation of downstream targets that promote increased lipolysis, mitochondrial biogenesis, endoplasmic reticulum (ER) stress, and resting energy expenditure (REE) [9]. To that end, it has been suggested that inhibiting β-adrenergic signaling in burn patients could significantly reduce post-burn metabolic changes in adipose tissue and the associated adverse hypermetabolic response, thereby improving outcomes.
Indeed, propranolol, a non-selective β-adrenergic receptor (β-AR) antagonist, has been widely used clinically in burn patients and trauma patients to reduce cardiac work and stress. In fact, propranolol has been shown to be safe and effective in reducing REE, accelerating wound closure, and improving cardiac function in burn patients [10]. Despite its well-documented clinical effects, however, there are few studies that provide mechanistic insights into the effect of propranolol on adipose tissue metabolism, particularly in the context of burn and trauma patients. An additional challenge is that the limited studies exploring the effects of propranolol on adipose tissue have solely examined its impact on subcutaneous WAT, generalizing the findings to all adipose tissue in the body. This is problematic as the adipose tissue is not a homogenous organ but contains distinct depots. Indeed, adipose tissue can be classified as subcutaneous, found just below the dermal layer, such as inguinal WAT (iWAT), or visceral, located deep within the body and surrounding the organs, like epididymal WAT (eWAT) [11]. Regrettably, studies examining the specific responses of distinct adipose depots (subcutaneous vs. visceral) to burn trauma are largely lacking, and whether a similar pathological significance exists for visceral and/or subcutaneous adipose tissue in burn patients is yet to be determined.
The current study addressed the question of whether the distinct adipose tissue depots respond differently to thermal trauma. Based on recent studies in the field of obesity demonstrating a greater impact of visceral fat compared to subcutaneous fat on adverse patient outcomes [12], we hypothesized that different fat depots would exhibit significant differences in their response to burn trauma. Moreover, we explored the therapeutic effects of β-adrenoceptor blockade via the clinically approved drug propranolol in attenuating the burn-induced pathological changes within the different adipose tissue depots. Namely, we assessed the effects of propranolol on three hallmarks of the post-burn hypermetabolic response: (1) ER stress, (2) lipolysis, and (3) WAT browning. These effects were tested in both iWAT and eWAT of mice subjected to a full-thickness burn injury.
Materials and methods
Animals
Male wild-type C57BL/6 J (WT) mice (6 weeks old, weighting an average of 24.0 g ± 1.0) were purchased from Jackson Laboratories (stock no. 000664, Bar Harbor, Maine) and housed at ambient temperatures of approximately 23–24 °C. Mice were cared for in accordance with the Guide for the Care and Use of Laboratory Animals (National Academies Press, 2011). After arrival, mice were acclimated to our facility for 2 weeks before the commencement of the experiments. By the date of the experiments, the mice were 8 weeks old and weighted the following (sham group, 25.08 g; burn group, 25.31; and burn + prop group, 25.48). Mice were then randomly assigned to the three main groups (sham, burn, burn + propranolol).
Mouse thermal injury model
We used a previously well-characterized rodent burn injury model [13]. Mice received a 30% TBSA full-thickness burn. We inflicted the burn using a 3 cm × 4 cm (12 cm2) mold, covering approximately 15% of the surface area of a 24-g mouse (75.8 cm2). A full-thickness third-degree dorsal scald burn encompassing 15% TBSA and a 15% wound on the ventral surface was induced by immersing the dorsum of the mice in 98 °C water for 10 s and the ventral region for 2 s. All mice were anesthetized with 2.5% isoflurane and shaved along the dorsal spine region prior to the injury. Ringer’s lactate (2–3 mL) was injected subcutaneously in all treatment mice to protect the spine, and buprenorphine (0.05–0.1 mg/kg body weight) was injected before and after the burn injury, when necessary, as required for pain management. Mice were subsequently housed individually in sterile cages and fed ad libitum until sacrifice. Sham (control) mice underwent identical experimental procedures, with the exception of the burn injury group. Adipose tissue (inguinal, epididymal) and plasma were collected upon sacrifice and stored at − 80 °C until analysis.
Drug treatment
Propranolol hydrochloride was acquired from Cayman Chemicals and dissolved in sterile ddH2O. After 24 h following the thermal injury, propranolol was intraperitoneally administered at a daily dose of 10 mg/kg for a total of 5 days. Sham (control) mice underwent identical experimental procedures, with the exclusion of the thermal injury, and were given the same treatment. Tissue and blood were collected 6 days post-burn injury (24 h after the last treatment).
Western blot
Adipose tissues (eWAT and iWAT) were lysed in RIPA buffer (50 mM Tris–HCl pH 7.5, 150 mM NaCl, 1% Igepal, 0.5% sodium deoxycholate, 0.1% SDS, 1 mM NaF and protease inhibitors) using tissue beater. Total protein was separated on SDS-PAGE gels, transferred to nitrocellulose membrane, and incubated with primary antibodies directed against the following proteins acquired from Cell Signaling: p-eIF2α (Cat. 9721S), JNK (Cat. 3708S), p-HSL ser660 (Cat. 45804S), and HSL (Cat. 8457S). Additionally, c-ATF6 (Cat. PA520215) was procured from Thermo Fisher. The nitrocellulose membranes were then imaged with the use of an enhanced chemiluminescence (ECL) substrate (Bio-Rad) and the ChemiDoc™ MP System (Bio-Rad). Finally, the membranes were analyzed using the ImageJ software to quantify band intensity and calculate the absorbance ratio relative to a housekeeping internal control protein.
Histology and immunohistochemistry
Excised adipose tissue was immediately placed in formalin and kept for 24 h prior to transfer to a 70% ethanol solution. Tissues were then paraffinized and sectioned in 5 µm lengths. These sections were stained with either hematoxylin and eosin (H&E) or incubated with UCP1 antibody (Sigma) prior to DAB staining.
Quantitative PCR
Total RNA isolated from adipose tissues was analyzed by quantitative RT-PCR. Briefly, RNA was isolated from tissues using TRIzol-chloroform (Life Technologies) with subsequent purification using the RNeasy Kit (Qiagen) according to the manufacturer’s instructions. RNA (2 µg) was transcribed to cDNA using the high-capacity cDNA reverse transcription kit (Applied Biosystems). Real-time quantitative PCR was performed using the Applied Biosystems Step One Plus Real-Time PCR System. The primer sequences used are available upon request.
Respiration assays
Oxygen consumption rates were measured in freshly excised adipose tissues (inguinal adipose depots). Tissues were minced in mitochondrial isolation buffer (MHSE + BSA; 210 mM mannitol, 70 mM sucrose, 5 mM HEPES, 1 mM EGTA, 0.5% (w/v) fatty acid–free BSA, pH 7.2). The tissue was then homogenized using a Teflon glass homogenizer. Mitochondria were isolated via differential centrifugation. Briefly, the homogenate was centrifuged at 600 g for 10 min, and the supernatant was decanted into a new tube. This fraction was centrifuged at 9000 g for 10 min to obtain a mitochondrial pellet, which was subsequently resuspended in 50 µL MHSE + BSA. BCA assays (Thermo Scientific) were performed to gauge protein concentrations. Mitochondrial bioenergetics were assessed using a Seahorse XF96 analyzer (Agilent Technologies). Mitochondrial respiration in a coupled state (10 µg/well) was measured in mitochondrial assay solution (220 mM mannitol, 70 mM sucrose, 10 mM KH2PO4, 5 mM MgCl2, 2 mM HEPES, 1 mM EGTA, and 0.2% (w/v) fatty acid–free BSA, pH 7.2, at 37 °C) containing succinate as a substrate (10 mM) and rotenone (2 µM) (complex II-driven respiration). State 3 respiration (phosphorylating respiration) was triggered via the injection of a cocktail containing 4 mM ADP along with 10 mM pyruvate, 2.5 mM glutamate, and 2.5 mM malate. State 4 respiration was assessed by the addition of 2.5 µg/mL oligomycin, while maximal uncoupler-stimulated respiration was observed following the injection of 4 µM carbonyl cyanide 4-(trifluoromethoxy)phenylhydrazone (FCCP). Antimycin A (4 µM), a complex III inhibitor, was added at the end of the experiment to inhibit mitochondrial respiration. Mitochondria from at least four mice were included in each Seahorse analysis, and every sample was analyzed in triplicate. The Seahorse XF Wave software was used to group the respiration data from separate mice into a single representative curve, and data was normalized to mitochondrial protein content.
Lipid quantification
Plasma free fatty acid (FFA) levels were measured with the FFA Quantification kit from Abcam (#65341). Blood was extracted from mice during sacrifice and centrifuged with EDTA at 3000 rpm for 10 min. Plasma was separated, and levels of FFA were measured according to the manufacturer’s instructions.
Statistical analyses
All data are presented as the mean ± SEM. All graphs were created and analyzed statistically using GraphPad Prism 6.0 (San Diego, CA) or Microsoft Excel. Statistical differences between groups were evaluated using a Student’s t-test or one-way analysis of variance (ANOVA) followed by Sidak’s post-hoc tests for multiple comparisons, where appropriate, with significance accepted at p < 0.05 (*). Individuals performing the statistical analysis as well as the main investigator were both blinded as to the intervention and treatment groups.
Results
Propranolol administration improves burn-induced ER stress in the eWAT adipose depot
Within the hierarchy of pathways altered during the hypermetabolic response to burn injury is the ER, a key site for maintaining the function and integrity of cellular homeostasis in response to stress [14]. Indeed, the ER stress response was recently proposed to be one of the critical signaling pathways mediating the catastrophic consequences of altered adipose tissue metabolism, such as inflammation, lipolysis, and IR following a burn injury [4]. We have also previously shown that CAs induce ER stress within the adipose tissue via stimulation of β-adrenergic receptors [9]. Thus, we first investigated the effect of both a burn injury and treatment with propranolol, a non-specific β-AR antagonist, on ER stress in different adipose tissue depots using a well-established murine model of thermal injury. As illustrated in Fig. 1A–C, we found that key ER stress markers such as cleaved-ATF6 (p < 0.01), p-eIF2α (p < 0.01), and p-JNK (p < 0.05) were activated in the eWAT depot of burn mice. Interestingly, the eWAT of mice treated with propranolol showed reduced levels of cleaved-ATF6 (p < 0.01), p-eIF2α (p < 0.05), and p-JNK (p < 0.01) compared to non-treated burned mice. Notably, analysis of the iWAT depot revealed that the levels of ER stress markers such as cleaved-ATF6, p-eIF2 α, and p-JNK were unaffected by burn injury or administration of propranolol (Fig. 2A–C). These results suggest that the ER stress response mediated by a burn injury is likely adipose tissue depot-specific and that propranolol treatment restores ER integrity only in the eWAT adipose depot following a burn injury.
Propranolol decreases burn-induced endoplasmic reticulum stress in epididymal white adipose tissue. A Representative Western blot for cleaved-ATF6 and corresponding densitometry quantification. B Representative Western blot for phospho-eIF2α and corresponding densitometry quantification. C Representative Western blot for phospho-JNK and corresponding densitometry quantification. Control (n = 4); burn (n = 6); burn + propranolol treatment (n = 6). Values are represented as mean ± standard error. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Burn injury does not induce endoplasmic reticulum stress in inguinal white adipose tissue. A Representative Western blot for cleaved-ATF6 and corresponding densitometry quantification. B Representative Western blot for phospho-eIF2α and corresponding densitometry quantification. C Representative Western blot for phospho-JNK and corresponding densitometry quantification. Control (n = 4); burn (n = 5); burn + propranolol treatment (n = 6). Values are represented as mean ± standard error. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Propranolol administration reduces lipolysis in both eWAT and iWAT adipose depots
Our work and other previous studies have shown that ER stress can trigger lipolysis within adipocytes, and if left unmitigated, this significant efflux of lipids can facilitate adverse complications like metabolic syndrome and hepatic steatosis [8, 9]. Therefore, we hypothesized that the inhibition of burn-induced catecholamine release via propranolol could also alleviate lipolysis within both adipose tissue depots. To confirm that lipolysis was increased in the burn group and attenuated in the propranolol group, we examined the activation of hormone-sensitive lipase (HSL Ser660) and adipose triglyceride lipase (ATGL), two canonical regulators of lipolysis at the cellular level [15]. In eWAT, we found that both ATGL (p < 0.05) and HSL (p < 0.05) were activated after burn injury and that propranolol treatment inhibited their activity post-burn (ATGL p < 0.001; HSL p < 0.05) (Fig. 3A, B). This cellular effect on the lipolysis pathway by propranolol was further confirmed via histological examination of eWAT adipose tissue sections. At the macroscopic level, examination of lipid droplet size via H&E staining showed that the burn group had smaller lipid droplets (p < 0.001) compared to the controls, indicating increased lipolysis, whereas the propranolol treatment mice showed larger lipid droplets (p < 0.001) indicating reduced lipolysis in eWAT adipose tissue depots of post-burn mice (Fig. 3C).
Propranolol treatment attenuates burn-induced lipolysis in epididymal white adipose tissue. A, B Representative Western blot for ATGL and phospho-HSL (Ser 660) and their corresponding densitometry quantification. C H&E staining of eWAT collected from control, burn, and burn mice treated with propranolol and corresponding quantification. Control (n = 5); burn (n = 6); burn + propranolol treatment (n = 6). Values are represented as mean ± standard error. *p ≤ 0.05, **p ≤ 0.01
We next looked at the iWAT depot to see if there were any inter-organ differences in the effect of propranolol treatment on lipolysis. We found a comparable pattern of increased phosphorylation of HSL (p < 0.05) and activation of ATGL (p < 0.05) in the iWAT depot of post-burn mice that was attenuated upon propranolol administration (p < 0.05) (Fig. 4A, B). Histological examination of the iWAT depot also showed reduced lipid droplet sizes in the burn group, indicative of an increased lipolytic response (p < 0.001). In contrast, burn mice treated with propranolol showed larger lipid droplets, suggesting post-burn treatment effectively reduced lipolysis in this depot (p < 0.05) (Fig. 4C). Together, these findings suggest that, at both the cellular and organ level, propranolol attenuates lipolysis and potentially the circulation of detrimental FFAs that emanate from both adipose tissue depots following a burn injury.
Propranolol treatment attenuates burn-induced lipolysis in inguinal white adipose tissue. A, B Representative Western blot for ATGL and phospho-HSL (Ser 660) and corresponding densitometry quantification. C H&E staining of iWAT collected from control, burn, and burn mice treated with propranolol and corresponding quantification. Control (n = 5); burn (n = 6); burn + propranolol treatment (n = 6). Values are represented as mean ± standard error. *p ≤ 0.05, **p ≤ 0.01
Propranolol administration reduces β-adrenergic-stimulated browning and mitochondrial activity of iWAT
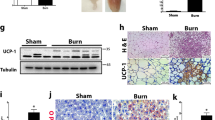
It was recently discovered that burn injury also induces WAT browning, a process in which white adipocytes become beige adipocytes and adopt brown-like features (i.e., increased mitochondrial content and UCP1 expression) [7, 16]. This phenotypic switch, driven mainly by catecholamines, has been implicated in causing IR, muscle catabolism, hepatic steatosis, and, most importantly, increased mortality in burn patients [6, 8]. Therefore, we next sought to see whether the pharmacological blockade of catecholamine signaling via propranolol would also inhibit burn-induced WAT browning. Having previously shown that only the iWAT adipose depot undergoes browning post-burn injury, we investigated the therapeutic effects of propranolol, focusing on the iWAT depot. Consistent with previous reports, our analysis showed that mRNA expression of the key WAT browning marker, UCP1, was significantly increased in the iWAT of post-burn mice (p < 0.05). Interestingly, propranolol-treated post-burn mice showed significantly decreased UCP1 mRNA expression compared to non-treated counterparts (p < 0.05) (Fig. 5A). In corroboration of our gene expression findings, UCP1 protein expression was also markedly decreased in propranolol-treated mice relative to the non-treated burn group (Fig. 5B).
Propranolol decreases UCP1-mediated uncoupling in inguinal white adipose tissue post-burn injury. A mRNA expression and B immunohistochemistry protein staining of key browning gene in iWAT collected from control, burn, and burn mice treated with propranolol. C Mitochondrial oxygen consumption rate in iWAT collected from control, burn, and burn mice treated with propranolol. D, E Basal mitochondrial respiration rate and mitochondrial coupling efficiency in iWAT collected from control, burn, and burn mice treated with propranolol. F, G State 3 and state 3u mitochondrial respiration rates in iWAT collected from control, burn, and burn mice treated with propranolol. Control (n = 4); burn (n = 4); burn + propranolol treatment (n = 4). Values are represented as mean ± standard error. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Having established that propranolol effectively attenuated the adverse WAT browning response in burn mice, we next wanted to determine whether this drug’s protective effects extended to the mitochondria, a key organelle implicated in mediating the post-burn hypermetabolic response. To that effect, iWAT was collected following euthanasia and immediately homogenized for assays of mitochondrial activity via Seahorse XF96 flux assays. Consistent with previous reports, post-burn mice showed an increased mitochondrial oxygen consumption rate (OCR) at all states (Fig. 5C, D). Remarkably, propranolol reduced the hypermetabolic phenotype of mitochondria after injury, reflected by the reduction in respiration profiles relative to untreated mice at 7 days post-burn (p < 0.05). Additionally, propranolol treatment significantly improved the coupling efficiency of mitochondria to ATP production relative to the burn group alone (p < 0.05) (Fig. 5E). Moreover, propranolol treatment significantly attenuated burn-induced state 3 mitochondrial respiration relative to the burn group (p < 0.05) (Fig. 5F, G). Together, these findings confirm that propranolol both decreases burn-induced WAT remodeling and restores mitochondrial respiration.
Discussion
Recent evidence suggests that the adipose tissue is much more than a passive storage organ. Indeed, adipose tissue is a highly metabolically active organ that controls systemic metabolism by secreting various adipokines, releasing FFAs, and undergoing processes such as browning [17]. What is even more intriguing are recent discoveries suggesting potentially distinct functions for various WAT depots throughout the body [18]. These functional differences are present post-differentiation but likely stem prior to the maturation of these adipocytes, as microarrays have shown different expression values for development-related genes in addition to functional ones [19]. These inherited functional differences between adipose depots are also evident in their responses to stress, suggesting that each fat depot may react uniquely to trauma insults. We investigated whether this could be the scenario following burn injuries, as the role of the adipose tissue in the context of burn trauma has been largely neglected until the recent discovery of WAT browning [7, 16]. Furthermore, studies examining fat in the context of burn-induced hypermetabolism have only concentrated on subcutaneous fat, largely overlooking other fat depots, including visceral fat. Therefore, in this paper, we sought to characterize some of the hallmark responses to burn trauma of both subcutaneous (iWAT) and visceral (eWAT) adipose depots using a murine model of burn injury. We thus delved into the characterization of the two largest depots in our mouse model by measuring some of the hallmarks of burn injury, including ER stress, browning, and lipolysis. Furthermore, we also assessed the therapeutic potential of propranolol in mitigating many of the adverse adipose changes that occur after burn.
We first examined ER stress, which, to our knowledge, has not previously been examined, within the different adipose depots following a burn injury. ER stress is the accumulation of mis- and unfolded proteins within the cell, which occur in response to stressors. Interestingly, we found distinct ER stress responses in the two adipose depots, with only the eWAT adipose depot experiencing burn-induced ER stress activation. Mechanistically, these differences in ER stress responses between the iWAT (subcutaneous) and eWAT (visceral) depots may be attributed to various factors. These include the eWAT depot’s higher expression of β-adrenergic receptors, greater innervation by the sympathetic nervous system, and increased susceptibility to immune cell infiltration and inflammatory cytokines. These factors collectively create an environment more favorable for heightened ER stress responses [20, 21].
Unmitigated ER stress within adipocytes has been shown to stimulate the induction of lipolysis and disrupt glucose homeostasis [22, 23]. We found increased activation of ATGL and HSL, two mammalian lipases responsible for up to 80% of lipolysis, in both adipose depots [15]. This activation of the signaling pathways involved in lipolysis was confirmed systemically by increased serum FFA levels in post-burn mice. Although we believe that ER stress was the main mediator in the activation of lipolysis in the eWAT adipose depot, this was likely not the case for iWAT. It is likely that the lipolysis pathways activated in the iWAT were a result of WAT browning rather than ER stress.
Outside of ER stress, another key response of the adipose tissue to burn trauma is the phenomenon known as WAT browning. WAT browning entails the remodeling of adipocytes within WAT depots to acquire properties of brown adipocytes, i.e., an increase in mitochondrial content and oxidative capacity to facilitate energy expenditure [24]. Indeed, browning has been observed in subcutaneous WAT of burn patients and cancer patients, two conditions that are characterized by hypermetabolism, large increases in resting energy expenditure and whole-body catabolism [7, 16, 25]. Consistent with previously published data by us and others, key WAT browning markers were expressed in iWAT (subcutaneous) of post-burn mice.
The last aspects of our studies were focused on identifying if propranolol, a non-selective β-adrenergic antagonist, has been widely used clinically in burn patients to diminish many of the adverse adipose responses to burn injury [26]. Interestingly, we found that propranolol administration in post-burn mice significantly reduced ER stress in eWAT (visceral) and lipolysis in both adipose depots (eWAT and iWAT). Additionally, propranolol treatment attenuated iWAT (subcutaneous) browning in post-burn mice. Our propranolol findings are in line with studies that have shown that WAT browning is largely driven by β-adrenergic receptor activation and likely explains how this drug attenuated burn-induced WAT browning [27]. Thus, identifying the therapeutic effects of propranolol treatment on both adipose depots is important, as it supports the use of this drug as an effective addition to our drug therapy toolset used in treating burn-induced hypermetabolism.
In this study, we report for the first time that propranolol impacts key pathways involved in mediating the post-burn hypermetabolic stress response, including adipose browning, lipolysis, and ER stress, thus elucidating its clinical efficacy in improving outcomes after injury. A significant limitation of our work is the exclusive use of male mice. While the impact of sex differences on outcomes after burn injury remains largely unexplored, conducting future studies with female mice will help determine whether the influence of propranolol on post-burn adipose dysfunction displays sexual dimorphism. Additionally, while our study provides valuable insights into the effects of burn injury and propranolol treatment on adipose tissue, it may benefit from a larger sample size to further validate these findings. However, the robustness of our results and the consistency of the observed effects across adipose tissue depots suggest that our study provides a solid foundation for future research in this area.
Conclusion
In summary, our findings demonstrate that burn results in many changes to adipose tissue as a whole, including ER stress, lipolysis, and remodeling to adipose browning. We also provided evidence that propranolol, a clinically approved drug for use in burn patients, can attenuate several of the pathological adipose alterations in both depots induced by burn.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Smolle C, Cambiaso-Daniel J, Forbes AA et al (2017) Recent trends in burn epidemiology worldwide: A systematic review. Burns 43:249–257. https://doi.org/10.1016/j.burns.2016.08.013
Williams FN, Herndon DN, Jeschke MG (2009) The hypermetabolic response to burn injury and interventions to modify this response. Clin Plast Surg [Internet]. [cited 2022 Apr 4];36(4):583. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3776603/
Jeschke MG, van Baar ME, Choudhry MA, Chung KK, Gibran NS, Logsetty S (2020) Burn injury. Nat Rev Dis Prim 61 [Internet]. 2020 Feb 13 [cited 2022 Jun 1];6(1):1–25. Available from: https://www.nature.com/articles/s41572-020-0145-5
Song J, Finnerty CC, Herndon DN, Boehning D, Jeschke MG (2009) Severe burn-induced endoplasmic reticulum stress and hepatic damage in mice. Mol Med [Internet] 15(9–10):316–320
Abdullahi A, Auger C, Stanojcic M, Patsouris D, Parousis A, Epelman S, Jeschke MG (2019) Alternatively activated macrophages drive browning of white adipose tissue in burns. Ann Surg 269(3):554–563
Abdullahi A, Samadi O, Auger C, Kanagalingam T, Boehning D, Bi S et al (2019) Browning of white adipose tissue after a burn injury promotes hepatic steatosis and dysfunction. Cell Death Dis 1012 [Internet]. 2019 Nov 18 [cited 2022 Apr 4];10(12):1–14. Available from: https://www.nature.com/articles/s41419-019-2103-2
Patsouris D, Qi P, Abdullahi A, Stanojcic M, Chen P, Parousis A et al (2015) Burn induces browning of the subcutaneous white adipose tissue in mice and humans. Cell Rep [Internet]. [cited 2022 Jun 1];13(8):1538–44. Available from: https://pubmed.ncbi.nlm.nih.gov/26586436/
Abdullahi A, Jeschke MG (2016) White adipose tissue browning: a double-edged sword. Trends Endocrinol Metab 27(8):542–552
Abdullahi A, Wang V, Auger C, Patsouris D, Amini-Nik S, Jeschke MG (2020) Catecholamines induce endoplasmic reticulum stress via both alpha and beta receptors. Shock 53(4):476–484
Herndon DN, Rodriguez NA, Diaz EC, Hegde S, Jennings K, Mlcak RP, Suri JS, Lee JO, Williams FN, Meyer W, Suman OE, Barrow RE, Jeschke MG, Finnerty CC (2012) Long-term propranolol use in severely burned pediatric patients: a randomized controlled study. Ann Surg 256(3):402–411
Lee MJ, Wu Y, Fried SK (2013) Adipose tissue heterogeneity: implication of depot differences in adipose tissue for obesity complications. Mol Aspects Med [Internet]. [cited 2022 Jun 1];34(1):1. Available from: /pmc/articles/PMC3549425/
Doyle SL, Donohoe CL, Lysaght J, Reynolds JV (2012) Visceral obesity, metabolic syndrome, insulin resistance and cancer. Proc Nutr Soc 71(1):181–189
Abdullahi A, Amini-Nik S, Jeschke MG (2014) Animal models in burn research. Cell Mol Life Sci 71(17):3241–3255
Abdullahi A, Barayan D, Vinaik R, Diao L, Yu N, Jeschke MG (2020) Activation of ER stress signalling increases mortality after a major trauma. J Cell Mol Med 24(17):9764–9773
Schweiger M, Schreiber R, Haemmerle G, Lass A, Fledelius C, Jacobsen P, Tornqvist H, Zechner R, Zimmermann R (2006) Adipose triglyceride lipase and hormone-sensitive lipase are the major enzymes in adipose tissue triacylglycerol catabolism. J Biol Chem 281(52):40236–40241
Sidossis LS, Porter C, Saraf MK, Børsheim E, Radhakrishnan RS, Chao T et al (2015) Browning of subcutaneous white adipose tissue in humans after severe adrenergic stress. Cell Metab [Internet] 22(2):219–227
Sakers A, De Siqueira MK, Seale P, Villanueva CJ (2022) Adipose-tissue plasticity in health and disease. Cell 185(3):419–446
Kwok KHM, Lam KSL, Xu A (2016) Heterogeneity of white adipose tissue: molecular basis and clinical implications. Exp Mol Med [Internet] 48(3):e215
Tchkonia T, Lenburg M, Thomou T, Giorgadze N, Frampton G, Pirtskhalava T et al (2007) Identification of depot-specific human fat cell progenitors through distinct expression profiles and developmental gene patterns. Am J Physiol Endocrinol Metab [Internet]. [cited 2022 Jun 1];292(1)
Fontana L, Eagon JC, Trujillo ME, Scherer PE, Klein S (2007) Visceral fat adipokine secretion is associated with systemic inflammation in obese humans. Diabetes 56(4):1010
Item F, Konrad D (2012) Visceral fat and metabolic inflammation: the portal theory revisited. Obes Rev [Internet] 13(SUPPL.2):30–39
Rutkowski DT, Wu J, Back SH, Callaghan MU, Ferris SP, Iqbal J et al (2008) UPR pathways combine to prevent hepatic steatosis caused by ER stress-mediated suppression of transcriptional master regulators. Dev Cell [Internet] 15(6):829–840
Özcan U, Yilmaz E, Özcan L, Furuhashi M, Vaillancourt E, Smith RO et al (2006) Chemical chaperones reduce ER stress and restore glucose homeostasis in a mouse model of type 2 diabetes. Science [Internet] 313(5790):1137–1140
Arner P (1998) Not all fat is alike. Lancet 351(9112):1301–1302
Petruzzelli M, Schweiger M, Schreiber R, Campos-Olivas R, Tsoli M, Allen J, Swarbrick M, Rose-John S, Rincon M, Robertson G et al (2014) A switch from white to brown fat increases energy expenditure in cancer-associated cachexia. Cell Metab 20(3):433–447
Finnerty CC, Herndon DN (2013) Is propranolol of benefit in pediatric burn patients? Adv Surg. [cited 2022 Jun 1];47(1):177
Blondin DP, Nielsen S, Kuipers EN, Severinsen MC, Jensen VH, Miard S, Jespersen NZ, Kooijman S, Boon MR, Fortin M et al (2020) Human brown adipocyte thermogenesis is driven by β2-AR stimulation. Cell Metab 32(2):287-300.e7
Funding
This work was supported by grants from the Canadian Institutes of Health Research (#123336), the Canada Foundation for Innovation Leader’s Opportunity Fund (#25407), and the National Institutes of Health (2R01GM087285-05A1; R01AG080040-01A1; 1R01GM133961-01A1). Abdikarim Abdullahi was supported by the Canadian Institutes of Health Research (CIHR) Postdoctoral Fellowship.
Author information
Authors and Affiliations
Contributions
AA, LBM, SB, and OS designed and performed experiments as well as wrote the manuscript; FK and DB helped with writing and editing the manuscript; GR performed experiments and analyzed data; MGJ designed studies, directed the studies, and wrote portions of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bieerkehazhi, S., Abdullahi, A., Khalaf, F. et al. β-Adrenergic blockade attenuates adverse adipose tissue responses after burn. J Mol Med 102, 1245–1254 (2024). https://doi.org/10.1007/s00109-024-02478-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-024-02478-w