Abstract
Purpose
The objective was to analyze the treatment and complications of the patients after a major amputation of the upper and lower extremities. Risk factors and predictors of a prolonged hospital stay should be outlined.
Methods
This is a retrospective study of a national Level-1 Trauma center in Germany. In a 10-year period, patients were identified by major amputations in the upper and lower extremities. The medical reports were considered and the results were split into four main groups with analysis on basic-, clinical data, the course on intensive care unit and the outcome. A recovery index was established. The patients’ degree of recovery was summed up. Statistical analysis was performed.
Results
81 patients were included. A total of 39 (48.1%) major amputations were carried out on the lower leg and 34 (42.0%) involved the thigh. There were two instances (2.5%) of hip joint disarticulation. 6 major amputations were done on the upper extremities (n = 3 on the upper arm, n = 3 on the forearm). 13.83 ± 17.10 days elapsed between hospital admission and major amputation. The average length of hospital stay was 38.49 ± 26,75 days with 5.06 ± 11.27 days on intensive care unit. Most of the patients were discharged home followed by rehabilitation. A significant correlation was found between the hospital length of stay and the increasing number of operations performed (p = 0.001). The correlation between the hospital length of stay and the CRP level after amputation was significant (p = 0.003).
Conclusions
Major amputations in trauma patients lead to a prolonged stay in hospital due to severe diseases and complications. Especially infections and surgical revisions cause such lengthenings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Major amputations of the upper and lower extremities have a significant impact on the quality of life of the affected patients. From the indication of amputation to the reintegration into private and professional life, patients usually go through a longer stay in the hospital, followed by inpatient and outpatient rehabilitation measures [1].
Amputation of the extremities is one of the most ancient surgical procedures [2]. In the beginning, the surgical amputation was crude and had to be carried out extremely rapidly because it was performed without anesthesia after removing the amputated extremity, the stump was crushed in hot oil to generate hemostasis. Amputation is the oldest major operation and has been practiced for punitive, ritualistic, and therapeutic reasons for thousands of years [3].
The reasons that lead to an amputation can be manifold, including infectious diseases, peripheral and central vascular diseases, diabetes mellitus (DM), diseases of the musculoskeletal system and the connective tissues, cancer, external causes like trauma, skin diseases, and congenital malformations [4].
Amputation procedures may therefore be urgent operations or may be scheduled electively. Currently, major amputations are performed obviously under anesthesia and monitoring, it is performed as an ultima ratio measure, after all procedures and treatments to save a extremity have been exhausted, since major amputations have a high rate of complications such as bleeding and hematoma, postoperative infection, surgical wound necrosis, contractures, pain, dermatological problems and lastly in a not so small percentage is a cause of death; in a systematic review van Netten et al. [5] reported that the 30 days mortality in patients that underwent a major amputation ranged from 7 to 22%.
The care and complications of major amputations in the public health system in Germany have not been well described so far. The objective of this article was to analyze, in a retrospective cohort of a national Level-1 Trauma center in Germany, the treatment and complications of the patients that underwent a major amputation of the upper or lower extremity in a ten-year follow-up.
Methods
Patient cohort
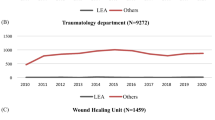
This retrospective study was performed at the Department for Orthopedics and Trauma Surgery at the University Hospital Schleswig-Holstein, Campus Kiel. The study period was from January 2009 to December 2020. The study was approved by the local ethics committee (number D 434/19). Major amputations were defined as amputations above the wrist and ankle. The patients were identified according to the International Statistical Classification of Diseases and Related Health Problems (ICD-10) as well as the Operation and Procedure Code (OPS). They were assigned either by ICD-10 code identifying traumatic major amputations in the upper and lower extremities (ICD S38.3, ICD S48.1, ICD S78.1, ICD S88.0, ICD S88.1) or by the OPS code identifying amputations and disarticulations of extremities (OPS 5-862, OPS 5-864). The resulting sample contains both male and female patients with a minimum age of 16 years Graph. 1.
Data collection
The patients´ medical documentation, surgical reports and discharge letters were considered from the digital hospital information system Agfa ORBIS (Version 08043701.04000.DACHL). The results were split into four main data groups: (1) Basic data, (2) Clinical data, (3) Intensive Care Unit and (4) Outcome. A recovery index was established in the context of major amputations. Furthermore, the patients’ degree of recovery was summed up according to three distinct parameters: degree of mobility, level of care and type of physiotherapy. Each parameter is comprised of three levels to which we assigned 0, 1 and 2 points, respectively. A higher level and thus a higher number of points is associated with a higher degree of recovery (see Tables 1 and 2). Finally, we assigned patients to three distinct groups based on the sum of their three individual scores. Group 1 consists of patients with 0–1 points implying that these patients achieved level 1 at most in one category. Group 2 consists of patients with 2–4 points. Finally, group 3 consists of patients with 5–6 points representing patients that achieved level 3 at least in 2 categories.
Statistical analysis
Retrospective analysis of data collected from patient records. Results are provided as mean ± standard deviation (SD). Statistical analysis was performed using IBM®, SPSS Statistics version 24. The T-test, Mann-Whitney-U-test, Kruskal-Wallis-test and Pearson-analysis were applied. A p-value ≤ 0.05 was considered statistically significant.
Results
Epidemiological data
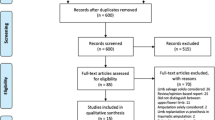
In the 10-year period 81 patients out of 471 patients were included due to the criteria.
The average age of the patients was 60.79 ± 16.07 years. The patient group consisted of 65 (80.2%) male patients and 16 (19.8%) female patients. The distribution of the different ages is shown in Fig. 1.
The medical conditions appeared mainly as arterial hypertension (59,3%), diabetes (34,6%), and coronary artery disease (28,4%). 57 patients (70,4%) had at least one newly diagnosed postoperative comorbidity Figs. 2 and 3.
A total of 39 (48.1%) major amputations were carried out on the lower leg and 34 (42.0%) involved the thigh. There were two instances (2.5%) of hip joint disarticulation. In the upper extremity, three (3.7%) major amputations were performed each on the forearm and on the upper arm. In total, 41 (50,6%) patients were amputated at their left extremity and 35 (43,2%) patients at their right extremity. In 5 (6,2%) patients the amputation was performed on both sides. The average number of operations conducted per major amputation was 4.7 ± 3.7. Various reasons and symptoms were detected that occurred in the cohort of 81 patients. Infections of the extremities were present in 46 cases. Amputation due to traumatic injury was carried out in 29 patients. A peripheral arterial disease was present in 17 patients. 11 patients had a diabetes, 8 patients had a cancerous disease and drug abuse was observed in 1 patient Tables 3 and 4.
Clinical course
On average, 13.83 ± 17.10 days elapsed between hospital admission and major amputation. In 45 (55.6%) cases, one hospital stay was required for treatment, with a maximum of 9 stays (1.85 ± 1.48). In 16 (19,8%) cases, the major amputation took place on the day of admission Figs. 4 and 5.
The shortest period of hospitalization was 8 days. The longest one was 174 days (38,49 ± 26,75 days). The average length of hospital stay was 38.49 ± 26,75 days. 35 (43.2%) patients spent at least one night in the intensive care unit. The mean number of days in the intensive care unit was 5.06 ± 11.27 days. 22 patients had mechanical ventilation (Max 44 days, mean 2,18 ± 7,10 days) Tables 5, 6 and 7.
The most common postoperative complications included re-operations and necrosis. Microbiological swabs were taken in 68 (84%) patients. In 16 (19.8%) patients, both microbiological and pathological tissue examinations were performed. A positive detection of bacteria was found in 57 (70.4%) patients. 23 (28,4%) patients had a negative result, and in 1 (1,2%) case there was no finding being documented. 35 (61,4%) patients were multi-drug resistant.
Outcome
A total of 37 (45,7%) patients were discharged home, 27 (33,3%) patients were transferred to a rehabilitation facility, 8 (9,9%) patients to another hospital, and 9 (11,1%) patients passed away during their hospital stay. 18 with a lower leg amputation and 13 patients with a thigh amputation were directly discharged home. Additionally, 14 patients with a lower leg amputation and 11 patients with a thigh amputation were subsequently transferred from the acute care hospital to an inpatient rehabilitation facility. Before their demise, 6 (66,7%) patients underwent a major amputation on the thigh, while 3 (33,3%) patients experienced such a procedure on the lower leg. 77,8% (n = 7) of the deceased patients were male.
The results regarding the hospital length of stay and patient age showed no significant correlation (p = 0.738). Similarly, there was no significant correlation found between the hospital length of stay and gender (p = 0.962). In the analysis of different topographic amputations in relation to hospital length of stay, no significant differences were observed, whether considering equal variance (p = 0.752) or unequal variance (p = 0.756). Regarding the number of surgeries, a significant correlation was found between the hospital length of stay and the increasing number of operations performed (p = 0.001). The analysis of red blood cell transfusions revealed no significant impact on the hospital length of stay (p = 0.341). The C-reactive protein (CRP) level upon admission showed no significant indications of influencing the hospital length of stay (p = 0.883). However, a significant positive correlation was identified between the hospital length of stay and the CRP level after amputation, characterized by a moderate strength (p = 0.003). The different types of infections leading to major amputation showed no significant differences and correlations concerning the hospital length of stay (p = 0.678). A significant difference was observed between the detection of a multidrug-resistant pathogen and a non-multidrug-resistant pathogen concerning the hospital length of stay (p = 0.043). Intensive care support demonstrated a positively significant correlation with the number of days in the intensive care unit of moderate strength (p = 0.002). If the patient was additionally intubated, the analysis revealed a significantly positive correlation with the hospital length of stay of moderate strength (p = 0.000). Concerning the hospital length of stay and postoperative complications, there were no significant correlations found between the duration of stay and cardiac complications (p = 0.325), postoperative sepsis (p = 0.720), or postoperative pneumonia (p = 0.572). However, a significant association was identified between postoperative acute kidney injury (p = 0.016) and postoperative wound healing disturbances (p = 0.000), leading to subsequently prolonged hospital length of stay.
Discussion
The reasons for a major amputation can be manifold. Diseases such as diabetes or vascular disorders show a global variation [6] and are the two major diseases leading to amputation of the lower extremity in industrial nations [7]. Amputations can be caused by severe trauma [8]. Extended soft tissue injuries and complex injuries can cause major amputation during hospital stay. Trauma represents the most common reason for major amputation of the upper extremity [9].
Compared to other countries, amputation rates are relatively high in Germany [7]. Over 70% of lower extremity amputations are necessary due to diabetes or vascular diseases [10].
In our evaluation, infections due to systemic disease were the primary cause for major amputations (56.8%), followed by amputation due to traumatic injuries (35.8%). We wanted to evaluate the risk factors that led to a deterioration in outcome after major amputation. Especially microvascular diseases cause increased infection susceptibility and impairs wound healing [11]. Peripheral neuropathy affects nearly 50% of adults with diabetes diseases during lifetime and is associated with ulcera, infection and lower extremity amputation [12]. In addition to the depth of the ulceration, the age of the patient also plays a decisive role in the infection [13].
We detected 39 (48.1%) major amputations of the lower leg and 34 (42%) of the thigh.
Even though amputations can occur at any age, most amputations take place between the ages of 51 and 80 [13]. In our evaluation, the average age of the included patients was 60.79 ± 16.07 years. Higher age and comorbidities are risk factors for worse outcome after major amputation [14]. Comorbidities and premedication can affect wound healing after primary surgery [15]. We evaluated an average number of surgeries conducted per major amputation was 4.7 ± 3.7. Primary wound closure was performed in all cases. Postoperative wound healing disturbance was documented for 47 patients (56.8%). Compared to other evaluations, the complication rate is high. Low et al. evaluated 2879 patients and 41.8% required at least one revision and 27.5% of amputees showed at least one major post-surgical complication [16]. Besides comorbidities and higher body mass index, the level of amputation appears to play a significant role for wound complications [17].
In our evaluation, 48.1% of major amputations were hold on the lower leg and 42.0% were performed at the thigh.
Low et al. demonstrated higher complication and revision rates after trauma-related lower leg amputation compared to thigh amputation [16]. Due to swelling, reperfusion injury or extended infection, a primary wound closure is not indicated in all cases. Primary care with negative pressure wound therapy can decrease the risk of wound complications [18]. Further debridements and secondary soft tissue coverage are necessary in progress [19].
Hospital stay after major amputations show great variation and depends on patient age, preexisting diseases and complication rate [7, 20].
The average length of hospital stay was 38.49 ± 26,75 days in our evaluation. The hospital stay increased in line with the number of operations and showed a correlation with wound healing disturbance, acute kidney injury and CRP level after amputation. Patients with diabetes diseases are prone to develop renal complications [21]. Patients with diabetes generate infections more often than patients without diabetes [22].
The expression of CRP is regulated by infection or tissue inflammation. The acute-phase protein is stimulated by Cytokines [23]. A correlation of high CRP level and prolonged hospital stay has been demonstrated for other diseases before [24]. Hospital stay in case of multiresistant pathogen was longer compared to non-multiresistant pathogens. Previous evaluations showed, that infection due to multiresistant bacteria are associated with higher mortality and longer hospital stay [25]. We found no significant correlation between hospital stay and patients age and gender. These results differ from some other evaluations, although there were differences in the study design, average age and number of secondary diseases. Higher amputation and complication rates in males might be attributed to larger proportion in smoking and alcohol consumption and poor foot care [26]. Peek et al. found male patients more willing to undertake major amputation of lower extremity, but female patients showed higher mortality related to these procedures [27]. In our evaluation a mortality rate of 9 (11.1%) during hospital stay was evaluated. Postoperative mortality rates during 30 days after operation can range from 4 to 22% [5]. Risk factors for increased mortality rates are age, renal disease, and vascular disease [14]. Considering various revision procedures and complications, the outcome after 30 days evaluation appears good in international comparison. 37 patients were discharged home after hospital stay and 27 patients were transferred to a rehabilitation clinic. Early surgical treatment, prior identification of bacteria and adequate antibiotic therapy appear to be decisive for improving the outcome.
Conclusion
In our evaluation, the most common postoperative complications included re-operations, necrosis, and wound infections. The length of hospital stay was especially influenced by number of operations and CRP level after operation. Significant difference was observed between the detection of a multidrug-resistant pathogen and a non-multidrug-resistant pathogen concerning the hospital length of stay. The results underline the importance of a careful surgical approach to amputation, germ determination and antibiotic therapy. The bacterial spectrum and the primary surgical treatment appear to have a decisive influence on the duration of inpatient treatment.
Data availability
No datasets were generated or analysed during the current study.
References
Solarz MK, Thoder JJ, Rehman S. Management of Major Traumatic Upper Extremity amputations. Orthop Clin North Am. 2016;47(1):127–36.
Markatos K, et al. Hallmarks of amputation surgery. Int Orthop. 2019;43(2):493–9.
Mavroforou A, et al. Punitive limb amputation. Clin Orthop Relat Res. 2014;472(10):3102–6.
Beckman JA, et al. Microvascular Disease, Peripheral Artery Disease, and amputation. Circulation. 2019;140(6):449–58.
van Netten JJ, et al. Early post-operative Mortality after Major Lower Limb Amputation: a systematic review of Population and Regional Based studies. Eur J Vasc Endovasc Surg. 2016;51(2):248–57.
Moxey PW, et al. Lower extremity amputations–a review of global variability in incidence. Diabet Med. 2011;28(10):1144–53.
Spoden M, Nimptsch U, Mansky T. Amputation rates of the lower limb by amputation level - observational study using German national hospital discharge data from 2005 to 2015. BMC Health Serv Res. 2019;19(1):8.
Clasper J, Ramasamy A. Traumatic amputations. Br J Pain. 2013;7(2):67–73.
Ziegler-Graham K, et al. Estimating the prevalence of limb loss in the United States: 2005 to 2050. Arch Phys Med Rehabil. 2008;89(3):422–9.
Narres M, et al. Incidence of lower extremity amputations in the diabetic compared with the non-diabetic population: a systematic review. PLoS ONE. 2017;12(8):e0182081.
Behroozian A, Beckman JA. Microvascular Disease increases amputation in patients with peripheral artery disease. Arterioscler Thromb Vasc Biol. 2020;40(3):534–40.
Hicks CW, Selvin E. Epidemiology of Peripheral Neuropathy and Lower Extremity Disease in Diabetes. Curr Diab Rep. 2019;19(10):86.
Pran L, et al. Major Lower Limb amputations: recognizing pitfalls. Cureus. 2021;13(8):e16972.
Thorud JC, et al. Mortality after nontraumatic major amputation among patients with diabetes and peripheral vascular disease: a systematic review. J Foot Ankle Surg. 2016;55(3):591–9.
Beyene RT, Derryberry SL Jr., Barbul A. The Effect of comorbidities on Wound Healing. Surg Clin North Am. 2020;100(4):695–705.
Low EE, Inkellis E, Morshed S. Complications and revision amputation following trauma-related lower limb loss. Injury. 2017;48(2):364–70.
Brien O P.J., et al. Risk factors for early failure of surgical amputations: an analysis of 8,878 isolated lower extremity amputation procedures. J Am Coll Surg. 2013;216(4):836–42. discussion 842-4.
Zayan NE, et al. Incisional negative pressure wound therapy: an effective Tool for Major Limb Amputation and Amputation Revision Site Closure. Adv Wound Care (New Rochelle). 2019;8(8):368–73.
Stanger K, Horch RE, Dragu A. Severe mutilating injuries with complex macroamputations of the upper extremity - is it worth the effort? World J Emerg Surg. 2015;10:30.
Essien SK, Zucker-Levin A. Factors associated with prolonged post-operative acute care length of stay in limb amputation patients in Saskatchewan, Canada. BMC Health Serv Res. 2021;21(1):1128.
Monseu M, et al. Acute kidney Injury predicts major adverse outcomes in diabetes: synergic impact with low glomerular filtration rate and Albuminuria. Diabetes Care. 2015;38(12):2333–40.
Muller LM, et al. Increased risk of common infections in patients with type 1 and type 2 diabetes mellitus. Clin Infect Dis. 2005;41(3):281–8.
Pepys MB, Hirschfield GM. C-reactive protein: a critical update. J Clin Invest. 2003;111(12):1805–12.
Travlos A et al. C-Reactive protein as a predictor of survival and length of Hospital stay in Community-Acquired Pneumonia. J Pers Med, 2022. 12(10).
Giraldi G, et al. Healthcare-Associated infections due to Multidrug-resistant organisms: a Surveillance Study on Extra Hospital stay and direct costs. Curr Pharm Biotechnol. 2019;20(8):643–52.
Amin L, et al. Gender differences in the impact of poverty on health: disparities in risk of diabetes-related amputation. Diabet Med. 2014;31(11):1410–7.
Peek ME. Gender differences in diabetes-related lower extremity amputations. Clin Orthop Relat Res. 2011;469(7):1951–5.
Acknowledgements
We would like to thank Mrs. Deike Misfeldt for statistical support.
Author information
Authors and Affiliations
Contributions
M.W. conducted the study and wrote the manuscript. T.-M. W. undertook the study and gathered the data. T.K. and P.B. supported the process to issue the data. A.S. enabled us to conduct the study. S.F.-O. wrote the manuscript and enforced the correction.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Weuster, M., Klüter, T., Wick, T.M. et al. Risk factors and predictors of prolonged hospital stay in the clinical course of major amputations of the upper and lower extremity a retrospective analysis of a level 1-trauma center. Eur J Trauma Emerg Surg (2024). https://doi.org/10.1007/s00068-024-02587-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00068-024-02587-8