Abstract
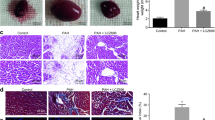
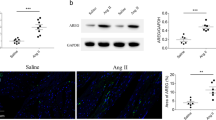
Previous studies show a woman’s pregnancy is correlated with post-reproductive longevity, and nulliparity is associated with higher risk of incident heart failure, suggesting pregnancy likely exerts a cardioprotection. We previously reported a cardioprotective phenomenon termed myocardial hypertrophic preconditioning, but it is unknown whether pregnancy-induced physiological hypertrophic preconditioning (PHP) can also protect the heart against subsequent pathological hypertrophic stress. We aimed to clarify the phenomenon of PHP and its mechanisms. The pluripara mice whose pregnancy-induced physiological hypertrophy regressed and the nulliparous mice underwent angiotensin II (Ang II) infusion or transverse aortic constriction (TAC). Echocardiography, invasive left ventricular hemodynamic measurement and histological analysis were used to evaluate cardiac remodeling and function. Silencing or overexpression of Foxo3 by adeno-associated virus was used to investigate the role of FoxO3a involved in the antihypertrophic effect. Compared with nulliparous mice, pathological cardiac hypertrophy induced by Ang II infusion, or TAC was significantly attenuated and heart failure induced by TAC was markedly improved in mice with PHP. Activation of FoxO3a was significantly enhanced in the hearts of postpartum mice. FoxO3a inhibited myocardial hypertrophy by suppressing signaling pathway of phosphorylated glycogen synthase kinase-3β (p-GSK3β)/β-catenin/Cyclin D1. Silencing or overexpression of Foxo3 attenuated or enhanced the anti-hypertrophic effect of PHP in mice with pathological stimulation. Our findings demonstrate that PHP confers resistance to subsequent hypertrophic stress and slows progression to heart failure through activation of FoxO3a/GSK3β pathway.






Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, Falk V, Gonzalez-Juanatey JR, Harjola VP, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GMC, Ruilope LM, Ruschitzka F, Rutten FH (2016) ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the European society of cardiology (ESC) developed with the special contribution of the heart failure association (HFA) of the ESC. Eur Heart J 37(27):2129–2200. https://doi.org/10.1093/eurheartj/ehw128
Wei X, Wu B, Zhao J, Zeng Z, Xuan W, Cao S, Huang X, Asakura M, Xu D, Bin J, Kitakaze M, Liao Y (2015) Myocardial hypertrophic preconditioning attenuates cardiomyocyte hypertrophy and slows progression to heart failure through upregulation of S100A8/A9. Circulation 131(17):1506–1517. https://doi.org/10.1161/CIRCULATIONAHA.114.013789
Ma LL, Ding ZW, Yin PP, Wu J, Hu K, Sun AJ, Zou YZ, Ge JB (2021) Hypertrophic preconditioning cardioprotection after myocardial ischaemia/reperfusion injury involves ALDH2-dependent metabolism modulation. Redox Biol 43:101960. https://doi.org/10.1016/j.redox.2021.101960
Ma LL, Kong FJ, Dong Z, Xin KY, Wang XX, Sun AJ, Zou YZ, Ge JB (2021) Hypertrophic preconditioning attenuates myocardial Ischaemia-reperfusion Injury by modulating SIRT3-SOD2-mROS-dependent autophagy. Cell Prolif 54(7):e13051. https://doi.org/10.1111/cpr.13051
Ma LL, Kong FJ, Ma YJ, Guo JJ, Wang SJ, Dong Z, Sun AJ, Zou YZ, Ge JB (2021) Hypertrophic preconditioning attenuates post-myocardial infarction injury through deacetylation of isocitrate dehydrogenase 2. Acta Pharmacol Sin 42(12):2004–2015. https://doi.org/10.1038/s41401-021-00699-0
Wu J, Lu J, Huang J, You J, Ding Z, Ma L, Dai F, Xu R, Li X, Yin P, Zhao G, Wang S, Yuan J, Yang X, Ge J, Zou Y (2020) Variations in energy metabolism precede alterations in cardiac structure and function in hypertrophic preconditioning. Front Cardiovasc Med. https://doi.org/10.3389/fcvm.2020.602100
Lin H, Zhu Y, Zheng C, Hu D, Ma S, Chen L, Wang Q, Chen Z, Xie J, Yan Y, Huang X, Liao W, Kitakaze M, Bin J, Liao Y (2021) Antihypertrophic memory after regression of exercise-induced physiological myocardial hypertrophy is mediated by the long noncoding RNA Mhrt779. Circulation 143(23):2277–2292. https://doi.org/10.1161/CIRCULATIONAHA.120.047000
Zhu Y, Zheng C, Zhang R, Yan J, Li M, Ma S, Chen K, Chen L, Liu J, Xiu J, Liao W, Bin J, Huang J, Lin H, Liao Y (2022) Circ-Ddx60 contributes to the antihypertrophic memory of exercise hypertrophic preconditioning. J Adv Res. https://doi.org/10.1016/j.jare.2022.06.005
Sanghavi M, Rutherford JD (2014) Cardiovascular physiology of pregnancy. Circulation 130(12):1003–1008. https://doi.org/10.1161/CIRCULATIONAHA.114.009029
Kara RJ, Bolli P, Karakikes I, Matsunaga I, Tripodi J, Tanweer O, Altman P, Shachter NS, Nakano A, Najfeld V, Chaudhry HW (2012) Fetal cells traffic to injured maternal myocardium and undergo cardiac differentiation. Circ Res 110(1):82–93. https://doi.org/10.1161/CIRCRESAHA.111.249037
Felker GM, Thompson RE, Hare JM, Hruban RH, Clemetson DE, Howard DL, Baughman KL, Kasper EK (2000) Underlying causes and long-term survival in patients with initially unexplained cardiomyopathy. N Engl J Med 342(15):1077–1084. https://doi.org/10.1056/NEJM200004133421502
Haghikia A, Podewski E, Libhaber E, Labidi S, Fischer D, Roentgen P, Tsikas D, Jordan J, Lichtinghagen R, von Kaisenberg CS, Struman I, Bovy N, Sliwa K, Bauersachs J, Hilfiker-Kleiner D (2013) Phenotyping and outcome on contemporary management in a German cohort of patients with peripartum cardiomyopathy. Basic Res Cardiol 108(4):366. https://doi.org/10.1007/s00395-013-0366-9
Gagnon A (2015) Natural fertility and longevity. Fertil Steril 103(5):1109–1116. https://doi.org/10.1016/j.fertnstert.2015.03.030
Hall PS, Nah G, Howard BV, Lewis CE, Allison MA, Sarto GE, Waring ME, Jacobson LT, Manson JE, Klein L, Parikh NI (2017) Reproductive factors and incidence of heart failure hospitalization in the women’s health initiative. J Am Coll Cardiol 69(20):2517–2526. https://doi.org/10.1016/j.jacc.2017.03.557
Ni YG, Berenji K, Wang N, Oh M, Sachan N, Dey A, Cheng J, Lu G, Morris DJ, Castrillon DH, Gerard RD, Rothermel BA, Hill JA (2006) Foxo transcription factors blunt cardiac hypertrophy by inhibiting calcineurin signaling. Circulation 114(11):1159–1168. https://doi.org/10.1161/CIRCULATIONAHA.106.637124
Sundaresan NR, Gupta M, Kim G, Rajamohan SB, Isbatan A, Gupta MP (2009) Sirt3 blocks the cardiac hypertrophic response by augmenting Foxo3a-dependent antioxidant defense mechanisms in mice. J Clin Invest 119(9):2758–2771. https://doi.org/10.1172/JCI39162
Ricke-Hoch M, Bultmann I, Stapel B, Condorelli G, Rinas U, Sliwa K, Scherr M, Hilfiker-Kleiner D (2014) Opposing roles of Akt and STAT3 in the protection of the maternal heart from peripartum stress. Cardiovasc Res 101(4):587–596. https://doi.org/10.1093/cvr/cvu010
Papait R, Cattaneo P, Kunderfranco P, Greco C, Carullo P, Guffanti A, Vigano V, Stirparo GG, Latronico MV, Hasenfuss G, Chen J, Condorelli G (2013) Genome-wide analysis of histone marks identifying an epigenetic signature of promoters and enhancers underlying cardiac hypertrophy. Proc Natl Acad Sci U S A 110(50):20164–20169. https://doi.org/10.1073/pnas.1315155110
Li J, Umar S, Iorga A, Youn JY, Wang Y, Regitz-Zagrosek V, Cai H, Eghbali M (2012) Cardiac vulnerability to ischemia/reperfusion injury drastically increases in late pregnancy. Basic Res Cardiol 107(4):271. https://doi.org/10.1007/s00395-012-0271-7
Mikhail MA, M’Hamdi H, Welsh J, Levicar N, Marley SB, Nicholls JP, Habib NA, Louis LS, Fisk NM, Gordon MY (2008) High frequency of fetal cells within a primitive stem cell population in maternal blood. Hum Reprod 23(4):928–933. https://doi.org/10.1093/humrep/dem417
Morris EA, Hale SA, Badger GJ, Magness RR, Bernstein IM (2015) Pregnancy induces persistent changes in vascular compliance in primiparous women. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2015.01.005
Laufer N (2015) Introduction: fertility and longevity. Fertil Steril 103(5):1107–1108. https://doi.org/10.1016/j.fertnstert.2015.03.012
Greer EL, Maures TJ, Hauswirth AG, Green EM, Leeman DS, Maro GS, Han S, Banko MR, Gozani O, Brunet A (2010) Members of the H3K4 trimethylation complex regulate lifespan in a germline-dependent manner in C. elegans. Nature. https://doi.org/10.1038/nature09195
Jaspers L, Kavousi M, Erler NS, Hofman A, Laven JS, Franco OH (2017) Fertile lifespan characteristics and all-cause and cause-specific mortality among postmenopausal women: the Rotterdam Study. Fertil Steril. https://doi.org/10.1016/j.fertnstert.2016.11.006
Petrov G, Regitz-Zagrosek V, Lehmkuhl E, Krabatsch T, Dunkel A, Dandel M, Dworatzek E, Mahmoodzadeh S, Schubert C, Becher E, Hampl H, Hetzer R (2010) Regression of myocardial hypertrophy after aortic valve replacement: faster in women? Circulation 122(11 Suppl):S23–S28. https://doi.org/10.1161/CIRCULATIONAHA.109.927764
Cao DJ, Jiang N, Blagg A, Johnstone JL, Gondalia R, Oh M, Luo X, Yang KC, Shelton JM, Rothermel BA, Gillette TG, Dorn GW, Hill JA (2013) Mechanical unloading activates FoxO3 to trigger Bnip3-dependent cardiomyocyte atrophy. J Am Heart Assoc 2(2):e000016. https://doi.org/10.1161/JAHA.113.000016
Choi S, Jeong HJ, Kim H, Choi D, Cho SC, Seong JK, Koo SH, Kang JS (2019) Skeletal muscle-specific Prmt1 deletion causes muscle atrophy via deregulation of the PRMT6-FOXO3 axis. Autophagy 15(6):1069–1081. https://doi.org/10.1080/15548627.2019.1569931
Trivedi CM, Luo Y, Yin Z, Zhang M, Zhu W, Wang T, Floss T, Goettlicher M, Noppinger PR, Wurst W, Ferrari VA, Abrams CS, Gruber PJ, Epstein JA (2007) Hdac2 regulates the cardiac hypertrophic response by modulating Gsk3 beta activity. Nat Med 13(3):324–331. https://doi.org/10.1038/nm1552
Ahmad F, Lal H, Zhou J, Vagnozzi RJ, Yu JE, Shang X, Woodgett JR, Gao E, Force T (2014) Cardiomyocyte-specific deletion of Gsk3alpha mitigates post-myocardial infarction remodeling, contractile dysfunction, and heart failure. J Am Coll Cardiol 64(7):696–706. https://doi.org/10.1016/j.jacc.2014.04.068
Cho J, Zhai P, Maejima Y, Sadoshima J (2011) Myocardial injection with GSK-3beta-overexpressing bone marrow-derived mesenchymal stem cells attenuates cardiac dysfunction after myocardial infarction. Circ Res 108(4):478–489. https://doi.org/10.1161/CIRCRESAHA.110.229658
van de Schans VA, van den Borne SW, Strzelecka AE, Janssen BJ, van der Velden JL, Langen RC, Wynshaw-Boris A, Smits JF, Blankesteijn WM (2007) Interruption of Wnt signaling attenuates the onset of pressure overload-induced cardiac hypertrophy. Hypertension 49(3):473–480. https://doi.org/10.1161/01.HYP.0000255946.55091.24
Lin H, Li Y, Zhu H, Wang Q, Chen Z, Chen L, Zhu Y, Zheng C, Wang Y, Liao W, Bin J, Kitakaze M, Liao Y (2019) Lansoprazole alleviates pressure overload-induced cardiac hypertrophy and heart failure in mice by blocking the activation of beta-catenin. Cardiovasc Res. https://doi.org/10.1093/cvr/cvz016
Hao H, Li X, Li Q, Lin H, Chen Z, Xie J, Xuan W, Liao W, Bin J, Huang X, Kitakaze M, Liao Y (2016) FGF23 promotes myocardial fibrosis in mice through activation of beta-catenin. Oncotarget 7(40):64649–64664. https://doi.org/10.18632/oncotarget.11623
Chen Z, Xie J, Hao H, Lin H, Wang L, Zhang Y, Chen L, Cao S, Huang X, Liao W, Bin J, Liao Y (2017) Ablation of periostin inhibits post-infarction myocardial regeneration in neonatal mice mediated by the phosphatidylinositol 3 kinase/glycogen synthase kinase 3beta/cyclin D1 signalling pathway. Cardiovasc Res 113(6):620–632. https://doi.org/10.1093/cvr/cvx001
Li Y, Wang Z, Kong D, Li R, Sarkar SH, Sarkar FH (2008) Regulation of Akt/FOXO3a/GSK-3beta/AR signaling network by isoflavone in prostate cancer cells. J Biol Chem 283(41):27707–27716. https://doi.org/10.1074/jbc.M802759200
Luo M, Wu C, Guo E, Peng S, Zhang L, Sun W, Liu D, Hu G, Hu G (2019) FOXO3a knockdown promotes radioresistance in nasopharyngeal carcinoma by inducing epithelial-mesenchymal transition and the Wnt/beta-catenin signaling pathway. Cancer Lett 455:26–35. https://doi.org/10.1016/j.canlet.2019.04.019
Zhao Y, Wang C, Hong X, Miao J, Liao Y, Hou FF, Zhou L, Liu Y (2019) Wnt/beta-catenin signaling mediates both heart and kidney injury in type 2 cardiorenal syndrome. Kidney Int 95(4):815–829. https://doi.org/10.1016/j.kint.2018.11.021
Hao H, Ma S, Zheng C, Wang Q, Lin H, Chen Z, Xie J, Chen L, Chen K, Wang Y, Huang X, Cao S, Liao W, Bin J, Liao Y (2021) Excessive fibroblast growth factor 23 promotes renal fibrosis in mice with type 2 cardiorenal syndrome. Aging (Albany NY) 13(2):2982–3009. https://doi.org/10.18632/aging.202448
Shingo T, Gregg C, Enwere E, Fujikawa H, Hassam R, Geary C, Cross JC, Weiss S (2003) Pregnancy-stimulated neurogenesis in the adult female forebrain mediated by prolactin. Science 299(5603):117–120. https://doi.org/10.1126/science.1076647
Acknowledgements
YL acknowledges grants from the National Natural Science Foundation of China (81770271 to YL), the Joint Funds of the National Natural Science Foundation of China (U1908205 to YL), the National Natural Science Foundation of China (82170278 to YL), and the Municipal Project of Research and Utilization of Healthcare Key Technology in Guangzhou (202206010199 to YL). JX was supported by the Scientific Research Project of Gannan Medical University (ZD201825 to JX).
Funding
This work was supported by grants from the National Natural Science Foundation of China (81770271 to YL), the Joint Funds of the National Natural Science Foundation of China (U1908205 to YL), the National Natural Science Foundation of China (82170278 to YL), and the Municipal Project of Research and Utilization of Healthcare Key Technology in Guangzhou (202206010199 to YL), the Scientific Research Project of Gannan Medical University (ZD201825 to JX).
Author information
Authors and Affiliations
Contributions
JX and CZ performed experimental design and executed most of the experiments, data analyses, and wrote the manuscript. MS, WL, and HL contributed to the technical, and material support. ML, MH, LC, SM, YZ, HL, JX, WL, and JB contributed to the data interpretation and discussion. LY contributed to the concept design, data interpretation, writing and revising the manuscript. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures were performed in accordance with our Institutional Guidelines for Animal Research, and this investigation conformed to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (National Institutes of Health Publication, 8th Edition, 2011). This study was approved by ethics review board of Southern Medical University.
Consent for publication
This study does not contain any individual person’s data. All authors agree for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xie, J., Zheng, C., Shen, M. et al. Pregnancy-induced physiological hypertrophic preconditioning attenuates pathological myocardial hypertrophy by activation of FoxO3a. Cell. Mol. Life Sci. 80, 267 (2023). https://doi.org/10.1007/s00018-023-04909-2
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-023-04909-2