Abstract
A breach of T cell tolerance is considered as a major step in the pathogenesis of rheumatoid arthritis. In collagen-induced arthritis (CIA) model, immunization with type II collagen (COL2) leads to arthritis in mice through T cells responding to the immunodominant COL2259–273 peptide. T cells could escape from thymus negative selection because endogenous COL2259–273 peptide only weakly binds to the major histocompatibility complex class II (MHCII) molecule Aq. To investigate the regulation of T cell tolerance, we used a new mouse strain BQ.Col2266E with homozygous D266E mutations in the Col2 gene leading to a replacement of the endogenous aspartic acid (D) to glutamic acid (E) at position 266 of the COL2259–273 peptide, resulting in stronger binding to Aq. We also established BQ.Col2264R mice carrying an additional K264R mutation changed the lysine (K) at position 264 to eliminate the major TCR recognition site. The BQ.Col2266E mice were fully resistant to CIA, while the BQ.Col2264R mice developed severe arthritis. Furthermore, we studied two of the most important non-MHCII genes associated with CIA, i.e., Ncf1 and Fcgr2b. Deficiency of either gene induced arthritis in BQ.Col2266E mice, and the downstream effects differ as Ncf1 deficiency reduced Tregs and was likely to decrease expression of autoimmune regulator (AIRE) while Fcgr2b did not. In conclusion, the new human-mimicking mouse model has strong T cell tolerance to COL2, which can be broken by deficiency of Fcgr2b or Ncf1, allowing activation of autoreactive T cells and development of arthritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is a chronic autoimmune disease which is believed to be initiated and driven by a breach of T cell tolerance to unknown self-antigens [1]. RA is classified by a set of clinical criteria [2], the major group, classified as seropositive RA, is characterized by increased levels of certain autoantibodies like rheumatoid factors (RF) and antibodies to citrullinated proteins (ACPA) which could appear several years ago before the clinical onset [3]. Seropositive RA is strongly associated with a related set of major histocompatibility complex class II (MHCII) alleles [4, 5], but the association is not linked to the appearance of autoantibodies but rather to the onset of an inflammatory attack on the joints [6]. MHCII molecules are receptors on antigen-presenting cells (APCs), which bind and present antigenic peptides to T cells. The peptides presented to T cells prior to the onset of RA are believed to be derived from self-proteins, but the regulative factors operating in this process remain to be explored. Clues are sought in attempts to identify variant genes outside the MHCII region, but those have been difficult to identify and to study functionally due to linkage disequilibrium. However, qualified guesses indicate several genes that may control T cell tolerance, including Fc gamma receptor (FCGR) locus containing FCGR2B polymorphism and Neutrophil cytosolic factor 1 (NCF1) polymorphism which was identified in rats [7] and later been positioned both as a copy number variation (CNV) and disease causative SNP in human [8,9,10].
To be able to understand how disruption of T cell tolerance could lead to the development of arthritis, we need to study suitable animal models. Since RA is a highly heterogeneous disease related to largely unknown genetic and environmental factors, there are variant animal models developed and used. The most thoroughly characterized mouse model is collagen-induced arthritis (CIA) which is commonly induced by immunization with non-self (bovine/rat/chicken/human) COL2 [11]. It is also inducible with mouse COL2 but then results in a less susceptible but more chronic disease [12]. However, in all cases, the immune response is entirely dependent on T cell recognition of a single peptide located at position 259–273 number from the start of the COL2 triple helical structure which binds to the MHC II molecule Aq[13]. In this immunodominant peptide, the main TCR interaction site is a lysine at position 264 (K264), which can be hydroxylated and glycosylated [14]. Also, mouse COL2 differs from the non-self COL2 at position 266 by only one aspartic acid (D266). The non-self COL2 instead has glutamic acid (E266) leading to 12 times tighter binding to Aq, which explains why it is more efficiently presented and elicits a stronger response after immunization [15, 16].
To investigate the mechanism of T cell tolerance operating in CIA model, we have previously developed a mutated COL2 (D266E) transgenic mouse strain, i.e., the mutated mouse collagen (MMC) strain to allow the non-self COL2 to be expressed in the joint cartilage [17]. MMC mice were less susceptible but not completely resistant to CIA, depending on the interaction of non-MHC genes. Using MMC mice, we showed that autoreactive T cells specific for the non-glycosylated COL2259–273 peptide undergo efficient central tolerance in an autoimmune regulator (AIRE) dependent manner [18]. However, the MMC transgenic strain still expresses the endogenous mouse COL2 which likely leads to the formation of heterotrimers in the cartilage and confounding immune responses. To establish a more physiologic context for the regulation of T cell tolerance, we generated a new strain BQ.Col2266E, with homozygous D266E mutations, leading to a complete replacement of aspartic acid (D) with glutamic acid (E) at position 266 in the immunodominant COL2259–273 peptide. In addition, we also made the BQ.Col2264R strain which carries K264R mutations besides existing D266E mutations, leading to a change in TCR recognition site by replacing lysine (K) with arginine (R) at position 264, which has proved to prevent T cell recognition of the COL2 peptide [19]. After immunization with non-self COL2, no arthritis was observed in BQ.Col2266E mice, while BQ.Col2264R mice developed severe arthritis. Also, we have previously been able to position several genetic polymorphisms controlling autoimmune arthritis in mice and rats outside the MHC region—Ncf1 controlling oxidative burst as one of the subunits of NOX2 complex [20, 21] and the inhibitory Fc receptor Fcgr2b[22]. To study whether they could break T cell tolerance and allow the development of CIA driven by autoreactive T cells, we intercrossed Fcgr2b and Ncf1 deficient mice with the BQ.Col2266E strain and found that both genes could additively break the T cell tolerance and allow the development of arthritis.
Materials and methods
Mice
Mice were bred and kept at Comparative Medicine’s Annex (KM-A) which is an animal facility of barrier C in Karolinska Institute in Stockholm, Sweden. Mice were housed under specific pathogenic-free conditions (FELASA II) in intra-ventilated cages with sterilized wood shavings and paper nesting material, fed with standard chow and water ad libitum. The animal genotyping and experimental protocols were approved by Stockholm regional animal ethics committee, Sweden (12923–2018, N35/16). Experiments using arthritis models were performed in male mice that were between 10 and 12 weeks old. For experiments with naïve mice, mice between 8 and 10 weeks old of the same sex were used. All the mice with BQ.Col2266E background are littermates.
B10.Q (C57BL/10.Q) founders have been fully backcrossed and maintained in our laboratory for a long time. Fcgr2b knockout (Fcgr2b−/−) mice and Ncf1 mutated (Ncf1m1j/m1j) mice were obtained from Jackson Laboratory and were fully backcrossed into B10.Q background for more than 10 generations in our laboratory to introduce H2-q haplotype in the MHC locus. The knock-in C57BL/6 J.Col2D266E (BQ.Col2266E) and C57BL/6 J.Col2K264R (BQ.Col2264R) mouse lines were generated by introducing point mutations at exon22 (p.D466E, c.1398 T > A) or (p.K464R, c.1391A > G; p.D466E, c.1398 T > A) of Collagen Type II Alpha 1 Chain (Col2a1) gene via CRISPR/Cas9 technology, respectively (Shanghai Biomodel Organism Science and Technology Development Co., Ltd, China). In our animal facility, these lines were backcrossed at least 5 generations into B10.Q background to introduce the H-2q haplotype in the MHC locus. B10Q.Ncf1m1j/m1j and B10Q.Fcgr2b−/− were crossed with BQ.Col2266E homozygous mice to produce BQ.Col2266E.Ncf1m1j/m1j and BQ.Col2266E.Fcgr2b−/− mice with their littermates.
Animal models
Three kinds of RA mouse models were used in this study. Collagen-induced arthritis (CIA): mice were immunized intradermally at the base of the tail with 100 ul emulsion made from 100 µg rat or bovine type II collagen (COL2) produced in our laboratory dissolved in acetic acid solution and complete Freund’s adjuvant (BD, Difco) in one-to-one configuration mixed by an emulsifier machine [23] (BTB, POWER-Kit). Mice were boosted at day 35 with 50 ul emulsion made of 50 µg COL2 in incomplete Freund’s adjuvant (BD, Difco) mixed by machine. The scoring usually started at around day 15, with an interval of 2–3 days. Glucose-6-phosphate isomerase-induced arthritis (GIA): mice were immunized intradermally at the base of the tail with 100 ul emulsion made from 10 ug human GPI325–339 (Biomatik) in Dulbecco’s phosphate-buffered saline (DPBS) (Thermo Fisher Scientific, Gibco) and CFA (BD, Difco) in one-to-one configuration. The scoring started from day 8 and was recorded every day. Collagen antibody-induced arthritis (CAIA): pathogenic anti-COL2 antibodies (M2139, ACC1, 15A, L10D9) were produced by corresponding hybridomas and then purified based on affinity chromatography [24]. After purification, antibodies were dialyzed in PBS and then concentrated to 10 mg/ml. These 4 antibodies were mixed at same amount and stored at 4 ℃ or on ice prior to injection. All mice were injected with 2 mg (200 ul) of cocktail on day 0, intravenously. The scoring started right after the antibody cocktail injection and was recorded for 3 weeks with an interval of 1–2 days. The scoring method was same for all these models. Each visibly inflamed (erythema and swelling) ankle or wrist was given up to 5 points, each inflamed knuckle and toe was given 1 point, together the maximum score per mouse was 60. Mice were killed when reach the experiment endpoint or ethics endpoint according to the ethical permit.
ELISA
For measurement of anti-COL2 antibody, blood was collected from mice on day 21, 35 and 49. Serum was obtained from blood after 10,000 rpm centrifugation for 10 min and kept in − 20 freezers until used. The 96-well ELISA plates (Thermo Fisher Scientific, Nunc MaxiSorp) were coated with COL2 diluted in DPBS to a final concentration of 10 µg/ml, 50 ul per well, overnight at 4 °C. After coating, plates were washed 5 times with ELISA buffer (0.1% Tween 20 in PBS). Plates were then blocked with 1% BSA in DPBS for 1 h at RT. Serum was diluted with DPBS into different concentrations: 1:1600 for IgG1 detection, 1:400 for IgG2b detection, 1:6400 for total IgG detection. The plates were washed 5 times and 50 ul of the diluted serum was added per well in triplicates, then incubated for 2 h at RT. The plates were washed 5 times and the detective antibody was added (1:4000 in DPBS): goat anti-mouse IgG(H + L)-HRP (Southern Biotech), goat anti-mouse IgG1-HRP (Southern Biotech) and goat anti-mouse IgG2b-HRP (Southern Biotech), 50 ul per well, incubated for 1 h at RT. The plates were washed 5 times, 50 ul of 1:5000 ExtrAvidin® -Peroxidase (Sigma) DPBS dilution was added per well and incubated for 45 min at RT. The ABTS solution was prepared by adding 1 ABTS tablets (Boehringer Mannheim) into 5 ml of 1X ABTS buffer diluted from 10X ABTS buffer (Boehringer Mannheim) for 1 plate. The plates were incubated in the dark for around 20 min until the color appears then read at 405 nm (OD405). For quantification of total IgG, a standard serum sample was used allowing comparison with a standard curve. For IL-2 detection, the experimental procedure was essentially the same. Plates were coated with homemade IL-2 monoclonal antibodies (Clone: JES6-IA12) diluted with DPBS to a final concentration of 2 ug/ml. After 5 times washing, 50 ul of medium containing IL-2 was added per well and the plates were incubated for 2 h at RT or overnight at 4 °C. The secondary biotinylated antibody (Clone: JES6-5H4) was diluted to 0.5 ug/ml. After washing, 50 ul of Eu-labeled streptavidin diluted with DPBS (PerkinElmer, 1:1000) were added per well and the plates were incubated for 30 min. After washing, the enhancement solution (PerkinElmer) was added, and the plates were read at 620 nm (OD620).
Histology
Mice were killed on day 90 of the CIA experiment. The left hind paw was collected and the skin around the joint was removed. Paws were fixed in 4% formaldehyde solution (Histolab), then decalcified with 10% EDTA for over 3 weeks. Dehydration was done by a machine in Histological Core Facility of KI. Tissue was embedded in paraffin and cut into 5 μm slides (Microtomes HM360). All the slides were stained with hematoxylin–eosin (H&E).
Flow cytometry
Inguinal lymph nodes were collected 10 days post immunization; thymi were collected from naïve mice. To make single-cell suspensions, lymph nodes were directly ground up and passed through 40 µm filters, while thymi were cut into pieces and digested with enzyme solutions as previously described [25]. Between every step below the samples were washed with DPBS 150–180 ul and were centrifuged at 350g for 5 min at RT to remove supernatant. Cells were added into 96-well U bottom plates at 1–10 × 106 cells per well (adjusted for certain experiments), then stained with LIVE/DEAD™ Fixable Dead Cell Stain (Thermo Fisher Scientific, Invitrogen) for 5 min on ice. Samples were blocked with homemade FcR block (Anti-mouse CD16/CD32, Clone: 2.4G2) for 10 min on ice, then stained with the antibodies (listed below) in 50 µl of PBS dilution on ice for 20 min in the dark. Cells were then washed with PBS and FACS buffer and ran on the Attune NxT flow cytometer (Thermo Fisher Scientific, Invitrogen). For intracellular staining, cells were washed, fixed, and permeabilized using BD Cytofix/Cytoperm (BD) set and then stained intracellularly with antibodies diluted with permeabilization buffer (BD) all according to manufacturer’s instructions. For FOXP3 staining, samples were fixed and permeabilized by eBioscience Foxp3/Transcription Factor Staining Buffer (Thermo Fisher Scientific, Invitrogen) set according to the protocols. For intracellular cytokine staining, cells were stimulated in vitro with the mixture of phorbol 12-myristate 13-acetate (PMA) 100 ng/ml, ionomycin 1 µg/m1, and BFA 10 µg/ml in 100 ul medium per well for 4 h at 37 °C prior to fixation, permeabilization, and staining.
Antibodies and others
Antibodies: antibodies were purchased from BD, Biolegend, Thermo Fisher Scientific unless stated otherwise. CD16/CD32 (2.4G2, in house); CD3 (145-2C11); TCRb (H57-597); TCRgd (GL3); Gr-1 (RB6-8C5); Ter-119 (TER-119); CD4 (RM4-5); CD8 (53–6.7); H-2, I-Aq (M5/114.15.2); F4/80 (BM8); CD19 (1D3, 6D5); CD11b (M1/70); Ly6G (1A8); Ly6C (HK1.4); CD11c (HL3, N418); FOXP3 (FJK-16s); CD25 (7D4); CD44 (IM7); CD69 (H1.2F3); CD45 (30-F11); EpCAM (G8.8); IL-33R (U29-93); IFN-γ (XMG1.2); IL-17A (TC11-18H10.1); NK1.1 (PK136); AIRE (5H12); NCF1(D-10); Ly51 (6C3); CD32b (AT130-2). Others: UEA-1, FITC conjugated (Thermo Fisher Scientific, Invitrogen).
Oxidative burst detection
For Fc receptor-induced ROS detection, spleens were isolated and ground through 40 ul filters to make single-cell suspensions. Red cells were lysed with ammonium-chloride-potassium (ACK) buffer. Cells were stained for cell markers and then stimulated by Fc OxyBURST™ Green Assay Reagent (Thermo Fisher Scientific) which are IgG-bound immunocomplex conjugated with H2DCF according to the protocols from the manufacturer. Samples were then washed with cold DPBS and put on the ice for 10 min to stop the ROS production then ran on a flow cytometer at relatively high speed.
ELISpot
The 96-well ELISpot plates (Millipore) were prewetted in an ultra clean bench with 15 ul freshly prepared 35% EtOH for less than 1 min, washed with sterilized DPBS and coated with anti-mouse IFN-γ capture antibody (Clone: R46A2, Mabtech) diluted to 10 ug/ml, 50 ul per well, then incubated overnight at 4 °C. Single cell suspensions from lymph nodes were prepared as described in the Flow cytometry part. The plates were washed 2 times, then non-modified or galactosylated COL2 peptide was added, cells were diluted with complete DMEM (DMEM + Glutamax (Gibco), 5% FBS (Gibco), 60 µg/ml penicillin C (Sigma)) 200 ul in total per well to eventually have 0.5 M or 1 M cells and peptides at a final concentration of 10 µg/ml. Concanavalin A (diluted with complete DMEM,1:1000) was used as positive control, medium without any stimulator was used as negative control. The plates were incubated for 24 h in a cell incubator, the liquid was flicked out, whereafter the plates were washed twice with DPBS and 3 times with ELISpot buffer (0.01% Tween 20 in PBS). Biotinylated anti-IFN-γ antibodies (clone: An18, Mabtech) were added at 50 ul per well, 4 ug/ml diluted with 0.5% BSA/DPBS, then incubated for 2 h at RT. The plates were washed 5 times with ELISpot buffer, then 50 ul of streptavidin–alkaline phosphatase (1:2500 in DPBS) were added and incubated for 30–45 min at RT. The plates were washed with buffer and DPBS 3 times, respectively, and 100 ul pre-filtered (0.45 µm) BCIP (Sigma) solution (1 tablet in 10 ml ddH2O) was added, and plates were incubated in the dark until the spots appeared. The plates were thoroughly rinsed with water, dried, and counted using ImmunoScan ELISpot Analyzer (CTL Europe).
Tetramer staining
The biotinylated Gal-COL2259–273-specific tetramers were previously produced and stocked at − 20 °C. The single cell suspensions from lymph nodes were prepared in cDMEM. Then 5 M cells were added per well in 96-well U bottom plates, the plates were then centrifuged, and supernatant was discarded. The cells were resuspended with 200 ul cDMEM containing 50 nM Dasatinib (SantaCruz) and homemade FcR block (Anti-mouse CD16/CD32, Clone: 2.4G2) and incubated at RT for 30 min. The plates were centrifuged, and supernatant was discarded, then resuspended with 50 ul biotinylated Gal-COL2259–273-specific tetramers and streptavidin PE conjugate (Thermo Fisher Scientific, Invitrogen) mixed in ddH2O (final concentration of tetramers around 0.4 mg/ml), the plates were incubated in the dark at RT for 30 min. 10 ul antibody mixture were added per well and plates were incubated for another 30 min. The cells were washed with FACS buffer twice and then analyzed by flow cytometry.
Antigen-presenting assay
HCQ3 and HCQ4 T cell hybridomas have previously been described [26]. These cells were thawed and cultured in cDMEM overnight. Thymi were isolated and ground into single-cell suspensions as described above. Thymic DCs were sorted using CD11c MicroBeads UltraPure (Miltenyi biotec) and MS column (Miltenyi biotec) according to the manufacturer’s protocol. Subsequently, 0.05 M of DCs and 0.15 M HCQ3 or HCQ4 cells with antigens (COL2 molecule, final concentration 100 ug/ml) in cDMEM or pure medium were added per well in 96-well U bottom plates and incubated for 15 h at 37 °C. 5 mM N-acetyl-L-cysteine (Nac) were added in some groups to remove ROS. Plates were centrifuged at 350g for 10 min, 50 ul of supernatant were taken for IL-2 detection (described in ELISA part), the rest were resuspended, stained, and analyzed by flow cytometry.
Statistics
Statistical analyses were performed with GraphPad Prism software, version 8.0.1 (GraphPad Software, San Diego, CA). Unless otherwise stated, the Mann–Whitney U test was used to compare the means of two groups. Data were shown as mean ± standard error or mean ± standard deviation. P value < 0.05 was considered as significant: *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001.
Results
BQ.Col2 266E mice have strong T cell tolerance reducing arthritis susceptibility, whereas BQ.Col2 264R mice develop severe arthritis
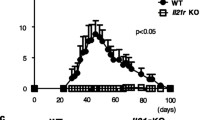
To determine the tolerance state of BQ.Col2266E and BQ.Col2264R mice, the susceptibility to develop arthritis and ex vivo T cell phenotype were checked. We induced CIA in BQ.Col2266E and BQ.Col2264R mice by immunization with COL2 at day 0 and boosted at day 35, B10Q mice were used as wild-type control. The results showed that BQ.Col2266E mice were almost completely resistant to CIA (Fig. 1a) but could still mount some immune response as seen by COL2-specific IgG response at day 35 (Fig. 1b). We further analyzed the T cell-specific response to galactosylated COL2 peptide (Gal-COL2259–273) 10 days post immunization through IFN-γ ELISpot. Porcine pepsin was used as positive control since COL2 was prepared with pepsin digestion. Notably, in Aq-expressing mice, contrary to mice with Ab allele, pepsin contamination does not influence arthritis development [27]. The data showed that BQ.Col2266E mice with either homozygous or heterozygous D266E mutations had much less activated COL2-specific T cells compared with B10Q mice, and pepsin did not affect the results (Fig. 1c). All the evidence suggested that BQ.Col2266E mice were resistant to the CIA induced by non-self COL2 and did not have detectable autoreactive T cells. Thus, the tighter binding of COL2259–273 to Aq led to a more efficient presentation of the peptide and induced stronger T cell tolerance.
BQ.Col2266E mice are resistant to CIA whereas the BQ.Col2264R mice develop severe arthritis. BQ.Col2266E mice carried homozygous D266E mutations in Col2 gene thus expressing non-self COL2. BQ.Col2264R mice had an additional K264R mutation to eliminate the TCR recognition site of the immunodominant peptide of COL2. a CIA was induced at day 0 by i.d. injection of rat COL2 emulsified in CFA (Male mice, BQ.Col2266E: n = 8, BQ.Col2264R: n = 13, B10Q: n = 6) and mice were boosted at day 35 with rat COL2 emulsified in IFA. Arthritis score and incidence were followed for 68 days (all the mice were included in statistics despite onset or not), mice with severe arthritis were killed during the experiment according to ethical permit. The statistical significance given on the top of the symbol of BQ.Col2266E group represents difference compared with B10Q group at indicating days. Score data were shown as mean ± standard error (same for all the score data in this study) and collected from one experiment. b Serum titration of anti-COL2 IgG antibodies was determined at day 35. Data were collected from one experiment. c Mice were immunized with rat COL2 emulsified in CFA (Male mice, B10Q: n = 6, BQ.Col2266E homo: n = 5, BQ.Col2266E het: n = 3, BQ.Col2264R homo: n = 6, BQ.Col2264R het: n = 3) and killed at day 10 to obtain primed lymph node cells, which were then stimulated with Gal-COL2 peptide to detect the Ag-specific T cells response by ELISpot. Data were collected from one experiment. d GIA was induced at day 0 by i.d. injection of GPI peptide emulsified in CFA (Male mice, B10Q: n = 10, BQ.Col2266E: n = 12). Arthritis severity was followed for 26 days (all the mice were included in statistics despite onset or not). Data were collected from one experiment. Each symbol represents one animal in (b) and (c). Statistics were done by the Mann–Whitney U test, *p < 0.05, **p < 0.01
In contrast, the BQ.Col2264R mice, in which the COL2 peptide did not share the key endogenous COL2-specific TCR recognition site at position 264, developed arthritis (Fig. 1a). BQ.Col2264R mice also had comparable anti-COL2 IgG titer and strong ex vivo T cell response to the Gal-COL2259–273 peptide which in this case had no indication of tolerance (Fig. 1b, c), suggesting that eliminating the recognition site of TCR could reverse resistance to CIA induced by the D266E mutation. Taken together, both D266E and K264R mutations were as expected functionally dominant, and heterozygous as well as homozygous mice showed identical results.
Meanwhile, to confirm the observed tolerance in the BQ.Col2266E mice was antigen-specific, we immunized the mice with another self-antigen glucose 6-phosphate isomerase (GPI) peptides, and they were fully susceptible to GPI-induced arthritis (Fig. 1d).
Additive effect of Fcgr2b and Ncf1 protect against CIA in BQ.Col2 266E mice
After validation of the BQ.Col2266E strain, we investigated the role of two non-MHC genes that could be of importance for regulating T cell tolerance, i.e., Fcgr2b and Ncf1. To directly address whether deficiency of Fcgr2b or Ncf1 could break the T cell tolerance to COL2, we crossed B10Q.Fcgr2b−/− knockout mice and B10Q.Ncf1m1j/m1j mutated mice with BQ.Col2266E strain to produce BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j littermates, respectively. These mice were immunized at day 0 with COL2 and boosted at day 35 to induce CIA. B10Q, B10Q.Fcgr2b−/− and B10Q.Ncf1 m1j/m1j mice were used as control.
As expected, insertion of Ncf1m1j/m1j especially Fcgr2b−/− enhanced the susceptibility to arthritis (Fig. 2a). Importantly, we found that BQ.Col2266E.Fcgr2b−/− mice developed severe arthritis with high incidence while Ncf1m1j/m1j mutation allowed the development of arthritis in mice with the D266E mutation but with much milder disease (Fig. 2a) (Table 1). Histology of paw joints taken on day 90 confirmed the scoring data showing severe bone and cartilage destruction and active synovial inflammation in arthritic BQ.Col2266E.Fcgr2b−/− mice, only synovitis in BQ.Col2266E.Ncf1m1j/m1j mice and healthy joints in BQ.Col2266E mice (Fig. 2b). Furthermore, BQ.Col2266E.Fcgr2b−/− mice showed higher anti-COL2 IgG titers compared with BQ.Col2266E.Fcgr2b+/+ littermates on both day 21 and day 49 (Fig. 2d). We have previously shown that the pathogenic effect of anti-COL2 antibodies is downregulated by FCGR2B, and we confirmed this also in BQ.Col2266E mice, which is much more susceptible to collagen antibody-induced arthritis (CAIA) if deficient in Fcgr2b (Fig. 2c). As activation of B cells leading to the production of COL2-specific IgG is T cell-dependent, it argues that T cell tolerance is also affected.
Fcgr2b knockout and Ncf1 mutation reverse resistance to CIA in BQ.Col2266E mice. Fcgr2b knockout mice and Ncf1m1j/m1j mutated mice were crossed with BQ.Col2266E strain to produce BQ.Col2266E. Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j littermates, respectively. a CIA was induced at day 0 by i.d. injection of bovine COL2 emulsified in CFA (Male mice, B10Q.Fcgr2b−/−: n = 16, B10Q.Ncf1m1j/m1j: n = 12, B10Q: n = 17, BQ.Col2266E. Fcgr2b−/−: n = 16, BQ.Col2266E.Ncf1m1j/m1j: n = 17, BQ.Col2266E: n = 14, including BQ.Col2266E. Fcgr2b+/+ and BQ.Col2266E.Ncf1+/+ mice) and mice were boosted at day 35 with bovine COL2 emulsified in IFA. Arthritis score and incidence were followed for 80 days (all the mice were included in statistics despite onset or not), mice with severe arthritis were killed during the experiment according to ethical permit. The upper statistical significance represents difference between BQ.Col2266E. Fcgr2b−/− group and BQ.Col2266E group at indicating days, the lower one is between BQ.Col2266E.Ncf1m1j/m1j and BQ.Col2266E groups. Data were pooled from two independent experiments with similar results (see details in Table 1). b Representative histology images of ankle joints from left hind paws taken at day 90 stained with H&E were showed (scale bar: 100 μm).The arrows from top to bottom in BQ.Col2266E. Fcgr2b−/− group indicated damaged cartilage, bone erosion and synovial inflammation. The arrow in BQ.Col2266E.Ncf1m1j/m1j group indicated mild synovitis. c CAIA was induced by i.v. injection of pathogenic anti-COL2 antibodies mixture (Male mice, BQ.Col2266E.Fcgr2b−/−: n = 5, BQ.Col2266E.Fcgr2b+/+: n = 5). Arthritis scores were followed for 23 days. Data were collected from one experiment. d Serum levels of anti-COL2 IgG, IgG1, IgG2b antibodies at day 21 and day 49 were shown as OD values (Serum dilution: IgG: 1:6400; IgG1:1:1600; IgG2b:1:400). Data from different date were separately collected from one experiment. Each symbol represents one animal in (d). Statistics were done by the Mann–Whitney U test, *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001
These data together showed that lack of capacity to produce oxidative burst due to the Ncf1m1j/m1j mutation, or inhibitory signal due to the Fcgr2b deficiency could both revert the resistance to CIA in BQ.Col2266E mice, but to different extents.
Fcgr2b −/− and Ncf1 m1j/m1j break T cell tolerance to COL2
To investigate whether Fcgr2b−/− deletion and Ncf1m1j/m1j mutation affect T cell tolerance in the BQ.Col2266E mice, we firstly addressed a possible shift in the phenotype of CD4+ T cells. We collected lymphocytes from draining inguinal lymph nodes 10 days after COL2 immunization in BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j mice with their wild-type littermates, then stained the cells with or without PMA stimulation in vitro to perform flow cytometry. The results showed no difference in the frequency of CD3+CD4+CD25+FOXP3+ T cells between groups (Fig. 3a, b), which was also previously found in naïve B6 and B6.Ncf1m1j/m1j mice [28]. Moreover, we observed a trend of increases in Th1 and Th17 frequencies of CD4+ T cells which are strongly related to the development of CIA (Fig. 3a, b), and a clear elevation of IL-33R expressing T cells in BQ.Col2266E.Fcgr2b−/− mice compared with BQ.Col2266E.Fcgr2b+/+ littermates (Fig. 3a, b). IL-33 has previously been reported its pathological roles in RA [29] and activation of IL33R+ T cells has been shown to increase the incidence of adjuvant-free CIA driven by Gal-COL2-specific T cells [30].
Mice defective in Fcgr2b or Ncf1 allows activation of COL2-specific T cells. Inguinal lymph node cells were obtained at 10 days post immunization with bovine COL2 emulsified in CFA. a and b Lymph node cells were stained with T cell markers with (for IFN-γ, IL-17 detection) or without PMA stimulation and intracellularly stained for cytokines and FOXP3 to show the T cell sub-populations (Female mice, BQ.Col2266E. Fcgr2b−/−: n = 7, BQ.Col2266E. Fcgr2b+/+: n = 5, BQ.Col2266E.Ncf1m1j/m1j: n = 6, BQ.Col2266E.Ncf1+/+: n = 5). Representative FACS gating of Treg cells (CD3+CD4+CD25+FOXP3+), CD3+CD4+IFN-γ+ T cells, CD3+CD4+IL-17+ T cells and CD3+CD4+IL-33R+ T cells were showed. The frequencies of each sub-populations among CD3+CD4+ T cells were showed. For results from BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Fcgr2b+/+ mice, data were collected from one experiment. For results from BQ.Col2266E.Ncf1m1j/m1j and BQ.Col2266E.Ncf1+/+ mice, data from two experiments with similar results were pooled together. c Lymph node cells were stimulated with galactosylated COL2 peptide (Gal-COL2259–273) or non-modified COL2 peptide (COL2259–273) to detect the Ag-specific T cells by ELISpot (Female mice, BQ.Col2266E. Fcgr2b−/−: n = 11, BQ.Col2266E. Fcgr2b+/+: n = 8, BQ.Col2266E.Ncf1m1j/m1j: n = 6, BQ.Col2266E.Ncf1+/+: n = 6). Data from two experiments with similar results were pooled together. d Lymph node cells were stained with Gal-COL2259–273-specific tetramers (Male mice, BQ.Col2266E. Fcgr2b−/−: n = 6, BQ.Col2266E. Fcgr2b+/+: n = 5). The FACS gating strategy were showed, Link = CD19, CD11b, MHCII. e The frequency of Gal-COL2259–273 tetramer+ T cells among CD3+CD4+ T cells were showed, the total Gal-COL2259–273 tetramer+ T cell number were calculated through the frequency of total lymphocyte times the number of cells read from cell counter. Data were collected from one experiment. Each symbol represents one animal in (b), (c) and (e). Statistics were done by the Mann–Whitney U test, *p < 0.05, **p < 0.01
We also analyzed the antigen-specific T cells response in the primed lymph node cells from BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j mice 10 days after immunization with COL2. These cells were stimulated with non-modified COL2 peptide (COL2259–273) or Gal-COL2259–273 peptide and analyzed with IFN-γ ELISpot assays. The results showed that BQ.Col2266E.Fcgr2b−/− mice had greatly increased autoreactive T cell responses to both non-modified and Gal-COL2 peptides (Fig. 3c), suggesting Fcgr2b could be important for T cell tolerance considering that tolerance to non-modified COL2 peptide is established in the thymus [18]. The BQ.Col2266E.Ncf1m1j/m1j also showed an increased T cell response towards non-modified COL2 peptide compared with littermates, which is consistent with previous findings with MMC mice [31] (Fig. 3c). To further confirm the finding of increased autoreactive T cells, we performed Gal-COL2259–273-specific tetramers staining in lymph node cells from BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Fcgr2b+/+ littermates 10 days after COL2 immunization. The results showed that both the frequency and total number of Gal-COL2-specific T cells were all elevated in BQ.Col2266E.Fcgr2b−/− mice (Fig. 3d, e). Thus, both Fcgr2b−/− and Ncf1m1j/m1j could break T cell tolerance to COL2 and increase the autoreactive T cells.
Fcgr2b and Ncf1 regulate tolerance through different mechanisms
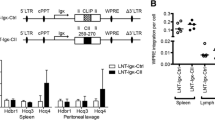
As both Fcgr2b and Ncf1 protected against the breach of T cell tolerance and development of arthritis, we next addressed the possibility that they operate in the same pathway, i.e., that they epistatically interact. Therefore, we made new cross-breeding on the BQ.Col2266E or B10Q background inducing deficiency of both Fcgr2b and Ncf1 and immunized them with COL2 together with control groups, then recorded the development of arthritis. The results showed B10Q. Fcgr2b−/−.Ncf1m1j/m1j developed the most severe arthritis with early onset and 100% incidence, compared with other strains (Fig. 4a). Thus, both Ncf1 and Fcgr2b deficiency contributed to the arthritis susceptibility. Similarly, BQ.Col2266E. Fcgr2b−/−.Ncf1m1j/m1j mice, with the D266E mutation, had more severe disease than BQ.Col2266E. Fcgr2b−/−.Ncf1+/+ littermates (Fig. 4a). The interaction between Fcgr2b and Ncf1 was additive, indicating that the pathways whereby they influence arthritis are mainly independent on each other. It does not exclude an epistatic interaction involving some part of the effect that could be hidden by other effects, for example, FcR stimulated by immune complexes (IC) could activate the NOX2 complexes inducing a substantial release of ROS. And we showed that Fcgr2b deficiency could lead to elevated ROS production induced by IC in DCs in vitro (suppl Fig. 1).
Both Fcgr2b and Ncf1 deficiency contributed to the enhanced arthritis susceptibility. B10Q.Fcgr2b−/−.Ncf1m1j/m1j and BQ.Col2266E.Fcgr2b−/−.Ncf1m1j/m1j were developed to address the interaction between Fcgr2b and Ncf1. a Mice from indicated groups were i.d. injected with bovine COL2 emulsified in CFA and were boosted at day 35 with bovine COL2 emulsified in IFA (except for B10Q.Fcgr2b−/−.Ncf1m1j/m1j group). Arthritis score and incidence were followed for 60 days (all the mice were included in statistics despite onset or not), mice with severe arthritis were killed during the experiment according to ethical permit. (Male mice, B10Q.Fcgr2b−/−.Ncf1m1j/m1j: n = 8, B10Q.Fcgr2b−/−.Ncf1+/+: n = 12, BQ.Col2266E.Fcgr2b−/−. Ncf1m1j/m1j: n = 10, BQ.Col2266E.Fcgr2b−/−. Ncf1+/+: n = 13).Data were collected from one experiment. b and d Draining lymph node cells were obtained at 10 days post bovine COL2 immunization (Female mice, BQ.Col2266E.Fcgr2b−/−. Ncf1m1j/m1j: n = 4, BQ.Col2266E.Fcgr2b−/−. Ncf1+/+: n = 8),CD3+CD4+ CD69+ T cells and CD3+CD4+CD25+FOXP3+ Treg cells were detected by FACS. The represent FACS gating and the frequency of each population were showed. Data were collected from one experiment. c Draining lymph node cells were obtained at 10 days post bovine COL2 immunization and stimulated with galactosylated COL2 peptide (Gal-COL2259–273) or non-modified COL2 peptide (COL2259–273) (Female mice, BQ.Col2266E.Fcgr2b−/−. Ncf1m1j/m1j: n = 4, BQ.Col2266E.Fcgr2b−/−. Ncf1+/+: n = 8). The COL2-specific T cells were detected by IFN-γ ELISpot. Data were collected from one experiment. Each symbol represents one animal in (c) and (d). Statistics were done by the Mann–Whitney U test, *p < 0.05
We proceeded to perform a T cell recall assay and checked the phenotype of T cells from draining lymph nodes of BQ.Col2266E.Fcgr2b−/− mice, with different Ncf1 alleles, 10 days post immunization and found interesting differences. Although the numbers of IFNγ-expressing COL2-specific T cells did not differ significantly (Fig. 4c), there was a relative expansion of activated CD4+CD69+ T cells and a reduction of FOXP3+ Tregs in mice with deficient Ncf1 (Fig. 4b, d), indicating that Ncf1 might influence T cell tolerance through Tregs generation.
Different roles of FCGR2B and NCF1 on antigen-presenting cells in thymus
Previous studies have shown that medullary thymic epithelial cells (mTECs), as well as recirculating DCs express and present a variety of tissue-restricted antigens (TRAs) including COL2 peptide in a transcription factor AIRE-dependent way [18, 32], which is the key step for negative selection of COL2-specific T cells in the thymus. To investigate whether FCGR2B or NCF1 could influence central T cell tolerance by affecting AIRE, we first checked the expression of AIRE on mTECs and other FCGR2B-expressing APCs in the thymus. We isolated thymi from naïve BQ.Col2266E.Fcgr2b−/− mice and BQ.Col2266E.Fcgr2b+/+ littermates, then differentiated mTECs (CD45−EpCAM+UEA-1high) as previously described [25] (Fig. 5a) as well as B cells (CD45+CD19+), macrophages (CD45+CD11b+F4/80+), neutrophils (CD45+CD11b+Ly6G+), DCs (CD45+Link−CD11c+) by flow cytometry (fig. S2a). The results showed that FCGR2B was not expressed on mTECs (Fig. S2b). The expression of AIRE in mTECs, B cells and other FCGR2B-expressing cells in the thymus were not affected by FCGR2B deficiency (Figs. 5b, S2a).
The role of Fcgr2b or Ncf1 on antigen-presenting cells in thymus. a Thymi were obtained from naïve BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j mice together with their littermates then digested and stained for AIRE. Representative FACS images of mTECs gating (CD45−EpCAM+UEA-1high) and histogram of AIRE expression were shown (red: BQ.Col2266E.Fcgr2b−/−, blue: BQ.Col2266E.Fcgr2b+/+). b The frequency of AIRE+ mTECs among total mTECs and AIRE expression in AIRE+ mTECs (shown as mean fluorescence intensity (MFI)) from BQ.Col2266E.Fcgr2b−/− and BQ.Col2266E.Ncf1m1j/m1j mice and their littermates were showed. (Male mice: BQ.Col2266E. Fcgr2b−/−: n = 4, BQ.Col2266E. Fcgr2b+/+: n = 5, Female mice: BQ.Col2266E.Ncf1m1j/m1j: n = 4, BQ.Col2266E.Ncf1+/+: n = 4). Data were collected separately for BQ.Col2266E.Fcgr2b littermates and BQ.Col2266E.Ncf1 littermates, both from one experiment. c and d Thymi were obtained from naïve B10Q and B10Q.Ncf1 m1j/m1j mice and stained for AIRE (Male mice: B10Q.Ncf1 m1j/m1j:n = 6, B10Q:n = 5). Representative FACS images of thymic B cells (CD45+CD19+) gating and AIRE+ B cells (CD45+CD19+AIRE+) gating were shown. Thymic B cells frequency of single live cells and AIRE+ B cells frequency of thymic B cells were shown. AIRE expressions of these populations were also shown as MFI, respectively. Data were collected from one experiment. e Representative FACS images of CD4+TCRb+ T hybridoma cells gating and CD69 or CD25 expression on hybridoma T cells with or without incubation with thymic DCs were shown, no extra antigen was added. f HCQ3 and HCQ4 hybridoma T cells were incubated with or without thymic DCs in the presence of COL2 molecules (Antigen) or no antigen for 15 h, 5 mM N-acetyl-L-cysteine (Nac) were added in some groups to remove ROS. After incubation, the supernatant medium was measured for IL-2 by ELISA, the results were shown as OD values (OD620). The rest part was stained for CD69/CD25/CD44, then detected by FACS, the results were shown as MFI, respectively (Female mice: BQ.Col2266E. Fcgr2b−/−: n = 6, BQ.Col2266E. Fcgr2b+/+: n = 5). Data were collected from one experiment. Each symbol represents one animal in (b), (d) and (f). Statistics were done by the Mann–Whitney U test, *p < 0.05, **p < 0.01
NCF1 on the other hand was expressed on mTECs and other thymus APCs (Fig.S2c), suggesting that NCF1 deficiency might affect the function of mTECs. Therefore, we went on to check the AIRE expression in BQ.Col2266E.Ncf1m1j/m1j mice and compared with BQ.Col2266E.Ncf1+/+ littermates. The results showed that the Ncf1m1j/m1j mutation could to some extent decrease the expression of AIRE in mTECs (Fig. 5b) indicating the possibility of an impaired TRAs expression and presentation. Interestingly, besides BQ.Col2266E background mice, we also found that the Ncf1 mutation could decrease the AIRE expression in thymus B cells in B10Q.Ncf1m1j/m1j mice compared with wild-type mice (Fig. 5c, d), suggesting the possible range of Ncf1 effects.
Because FCGR2B was found not to be expressed on mTECs, we hypothesized that it might affect central tolerance through other FCGR2B-expressing APCs in the thymus. DCs express FCGR2B and have been shown to be an important APC type in central T cell tolerance induction [33, 34]. To determine whether thymus DCs could pick up the COL2 peptide in vivo and present it to autoreactive thymocytes, we used two kinds of T cell hybridomas producing IL-2 after stimulation—HCQ3 cells which are specific for the Gal-COL2 peptide and HCQ4 cells which are specific for non-modified COL2 peptide [26]. We isolated single cells from thymi obtained from naïve BQ.Col2266E.Fcgr2b−/− mice and BQ.Col2266E.Fcgr2b+/+ littermates and sorted DCs by magnetic separation using ultra-pure CD11c microbeads. We incubated the thymic DCs with either HCQ3 or HCQ4 cells with or without corresponding antigens in the medium, then detected the T cells activation markers CD25 and CD69 on T cell hybridomas by flow cytometry, and IL-2 in the supernatants was measured by ELISA. The results showed that both T cells responded even without extra added antigens, indicating that the thymus DCs were loaded with both non-modified and Gal-COL2 peptides, which could activate COL2-specific T cell hybridomas (Fig. 5e), confirming previous data on recirculating thymic DC[18]. However, thymic DCs from BQ.Col2266E. Fcgr2b−/− mice had an unaltered ability to activate HCQ3 and HCQ4 T cells compared with BQ.Col2266E.Fcgr2b+/+ mice (Fig. 5f). Still, the activation function of the DCs is redox-regulated as we noticed that removing ROS by adding 5 mM N-acetyl-L-cysteine (Nac) decreased the expression of activation marker CD44 and IL-2 secretion of the hybridoma T cells (Fig. 5f).
Taken together, both Fcgr2b and Ncf1 regulate immune tolerance but through different mechanisms. Deficiency of Ncf1 decreased the numbers of Tregs, an effect that may depend on antigen-presenting cells (mTECs, B cells and DCs) in the thymus, which was likely to be associated with decreased AIRE expression.
Discussion
In both mice and humans, the T cell response to COL2 is directed to the same immunodominant target—the COL2259–273 peptide binding Aq in mice and DR*0401 in humans [13], which is also the key immune target in CIA. In this study, we showed that a mutation of COL2 in mice changing the aspartic acid (D) to a glutamic acid (E) at position 266 (as in humans), allowing a stronger binding to the MHCII molecules, leads to profound T cell tolerance and decreased susceptibility to arthritis. FCGR2B, as well as NCF1, could break the T cell tolerance although through different mechanisms. NCF1 is likely to be associated with the control of thymus-derived Treg development.
This study provides a mouse model for the human autoreactive T cell response to COL2 and allows studies of T cell tolerance regulation. Such studies are not possible in the classical CIA model, which activates heterogenous COL2-reactive T cells that do not recognize the endogenous COL2 peptide in vivo. Also, we clearly demonstrated that by using the BQ.Col2264R mice in which the major T cell recognition site is eliminated through mutation of the lysine at position 264, allowing a pure non-self T cell response, resulted in severe arthritis. We have earlier used a transgenic model which express mutated mouse COL2 [17] but with unphysiological expression, since the endogenous mouse COL2 is also expressed, and heterotrimeric molecules will be formed. In comparison, the transgenic model showed less pronounced protection against arthritis together with the Ncf1 mutation [31].
Ncf1 was first positionally cloned from rats with autoimmune arthritis [7] and later positioned both as a copy number variation (CNV) and disease causative SNP (rs201802880, or NCF1–339) in humans [8,9,10]. The Ncf1m1j/m1j mutations decreasing NCF1 function, leading to a diminished induction of ROS, are causative alleles for both arthritis and lupus [7,8,9,10, 20, 21, 35]. The downstream mechanisms explaining the exaggerated activation of T cells are however likely to be complex, involving not only oxidation of antigenic peptides during processing and changing the activity of the APCs but also directly affecting the interacting T cells by changing T cell surface redox level or possibly triggering differentiation to Tregs [36,37,38]. We have previously proposed the possibility that ROS from APCs may operate as an immunologic transmitter to regulate T cells auto-reactivity [39], which could affect TCR signaling through lipid rafts in the plasma membrane that are believed to be regulated by redox signaling [40]. Whether T cell selection in the thymus is oxidatively regulated is still not known, but it has been reported that single positive CD4+ thymocytes developed an increased level of ROS during maturation [41]. In our study, we reported that the Ncf1m1j mutation could to some extent lower the AIRE expression in mTECs, thus affecting the expression and presentation of TRAs which could reduce the efficiency of T cell-negative selection and promote the release of potential autoreactive T cells to the periphery [42]. Interestingly, Aire knockout can also reduce the ROS level in CD4+ SP thymocytes in B6 mice [41]. Using the new BQ.Col2266E mice, we showed that Ncf1 mutation leads to decreased Tregs. COL2 peptide is presented during T cell selection in the thymus and the observed downregulation of AIRE in mTECs and B cells might explain the observed reduction of Tregs. These results add other possibilities on how NCF1 regulates the immune system.
As the only inhibitory IgG Fc receptor, FCGR2B could counterbalance the activation signals by co-ligation with activating FcRs or BCR through immune complexes to exert its diverse regulatory functions in innate and adaptive immunity. Deficiency of Fcgr2b is associated with several autoimmune diseases including SLE, RA, anti-glomerular basement membrane (GBM) disease, and multiple sclerosis (MS) [43]. Mouse strains with targeted Fcgr2b deletions have been extensively studied on different models resulting in diverse reports regarding its role in autoimmunity [44, 45]. Briefly, in autoimmune arthritis models, deficiency of Fcgr2b could increase the susceptibility mainly through autoantibody production, and the regulation of the DCs function as well as peripheral B cell tolerance [46, 47]. Although studies have reported various pathways for Fcgr2b regulating the T cell function [48, 49], not much were specifically focused on its role in T cell tolerance. The difficulties to sort out its role could partly be due to linked effects with neighboring genes, including other Fc-receptors. Notably, in this study, we used a congenic fragment originally from the 129 strain containing a targeted Fcgr2b deletion, which means other genes besides Fcgr2b could contribute to the results. In a forward genetic cloning study, we identified that both FcgR3 and Fcgr2b alleles within the same haplotype, both contribute and operate in an additive way [22].
We now showed that in a controlled autoimmune setting, deficiency of Fcgr2b is associated with activation of autoreactive T cells and enhancement of CIA. It is known that activation of FcR induce a ROS response through activation of the NOX2 complex and we initially hypothesized that Ncf1 and Fcgr2b genes could interact. However, we have no evidence for this, instead the major mechanism by which these two genes control the induction of T cell tolerance and enhance arthritis seem to be different.
We conclude that for the first time a new human-mimicking model for RA is described, in which an adequate autoreactive MHCII-restricted T cell response to COL2 can be followed. Both Ncf1 and Fcgr2b locus are important to maintain T cell tolerance, providing insights for more possibilities of their regulatory functions.
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The animal genotyping and experimental protocols used in this study were approved by Stockholm regional animal ethics committee, Sweden (12923-2018, N35/16).
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Weyand CM, Goronzy JJ (2021) The immunology of rheumatoid arthritis. Nat Immunol 22:10–18. https://doi.org/10.1038/s41590-020-00816-x
Aletaha D, Neogi T, Silman AJ et al (2010) 2010 rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Ann Rheum Dis 69:1580–1588. https://doi.org/10.1136/ard.2010.138461
Rantapää-Dahlqvist S, de Jong BAW, Berglin E et al (2003) Antibodies against cyclic citrullinated peptide and IgA rheumatoid factor predict the development of rheumatoid arthritis. Arthritis Rheum 48:2741–2749. https://doi.org/10.1002/art.11223
Stastny P (1978) Association of the B-cell alloantigen DRw4 with rheumatoid arthritis. N Engl J Med 298:869–871. https://doi.org/10.1056/NEJM197804202981602
Raychaudhuri S, Sandor C, Stahl EA et al (2012) Five amino acids in three HLA proteins explain most of the association between MHC and seropositive rheumatoid arthritis. Nat Genet 44:291–296. https://doi.org/10.1038/ng.1076
Wouters F, Maurits MP, van Boheemen L et al (2022) Determining in which pre-arthritis stage HLA-shared epitope alleles and smoking exert their effect on the development of rheumatoid arthritis. Ann Rheum Dis 81:48–55. https://doi.org/10.1136/annrheumdis-2021-220546
Olofsson P, Holmberg J, Tordsson J et al (2003) Positional identification of Ncf1 as a gene that regulates arthritis severity in rats. Nat Genet 33:25–32. https://doi.org/10.1038/ng1058
Olsson LM, Nerstedt A, Lindqvist A-K et al (2012) Copy number variation of the gene NCF1 is associated with rheumatoid arthritis. Antioxid Redox Signal 16:71–78. https://doi.org/10.1089/ars.2011.4013
Olsson LM, Johansson ÅC, Gullstrand B et al (2017) A single nucleotide polymorphism in the NCF1 gene leading to reduced oxidative burst is associated with systemic lupus erythematosus. Ann Rheum Dis 76:1607–1613. https://doi.org/10.1136/annrheumdis-2017-211287
Zhao J, Ma J, Deng Y et al (2017) A missense variant in NCF1 is associated with susceptibility to multiple autoimmune diseases. Nat Genet 49:433–437. https://doi.org/10.1038/ng.3782
Holmdahl R, Bockermann R, Backlund J, Yamada H (2002) The molecular pathogenesis of collagen-induced arthritis in mice—a model for rheumatoid arthritis. Ageing Res Rev 1:135–147. https://doi.org/10.1016/S0047-6374(01)00371-2
Holmdahl R, Jansson L, Larsson E et al (1986) Homologous type II collagen induces chronic and progressive arthritis in mice. Arthritis Rheum 29:106–113. https://doi.org/10.1002/art.1780290114
Michaëlsson E, Andersson M, Engström A, Holmdahl R (1992) Identification of an immunodominant type-II collagen peptide recognized by T cells in H-2q mice: self tolerance at the level of determinant selection. Eur J Immunol 22:1819–1825. https://doi.org/10.1002/eji.1830220722
Corthay A, Bäcklund J, Holmdahl R (2001) Role of glycopeptide-specific T cells in collagen-induced arthritis: an example how post-translational modification of proteins may be involved in autoimmune disease. Ann Med 33:456–465. https://doi.org/10.3109/07853890109002094
Holmdahl R, Jansson L, Gullberg D et al (1985) Incidence of arthritis and autoreactivity of anti-collagen antibodies after immunization of DBA/1 mice with heterologous and autologous collagen II. Clin Exp Immunol 62:639–646
Kjellén P, Brunsberg U, Broddefalk J et al (1998) The structural basis of MHC control of collagen-induced arthritis; binding of the immunodominant type II collagen 256–270 glycopeptide to H-2Aq and H-2Ap molecules. Eur J Immunol 28:755–767. https://doi.org/10.1002/(SICI)1521-4141(199802)28:02%3c755::AID-IMMU755%3e3.0.CO;2-2
Malmström V, Michaëlsson E, Burkhardt H et al (1996) Systemic versus cartilage-specific expression of a type II collagen-specific T-cell epitope determines the level of tolerance and susceptibility to arthritis. Proc Natl Acad Sci 93:4480–4485. https://doi.org/10.1073/pnas.93.9.4480
Raposo B, Merky P, Lundqvist C et al (2018) T cells specific for post-translational modifications escape intrathymic tolerance induction. Nat Commun 9:353. https://doi.org/10.1038/s41467-017-02763-y
Batsalova T, Dzhambazov B, Merky P et al (2010) Breaking T cell tolerance against self type II collagen in HLA–DR4–transgenic mice and development of autoimmune arthritis. Arthritis Rheum 62:1911–1920. https://doi.org/10.1002/art.27460
Zhong J, Olsson LM, Urbonaviciute V et al (2018) Association of NOX2 subunits genetic variants with autoimmune diseases. Free Radic Biol Med 125:72–80. https://doi.org/10.1016/j.freeradbiomed.2018.03.005
Hultqvist M, Olofsson P, Holmberg J et al (2004) Enhanced autoimmunity, arthritis, and encephalomyelitis in mice with a reduced oxidative burst due to a mutation in the Ncf1 gene. Proc Natl Acad Sci USA 101:12646–12651. https://doi.org/10.1073/pnas.0403831101
Vaartjes D, Klaczkowska D, Cragg MS et al (2021) Genetic dissection of a major haplotype associated with arthritis reveal FcγR2b and FcγR3 to act additively. Eur J Immunol 51:682–693. https://doi.org/10.1002/eji.202048605
Topping LM, Romero-Castillo L, Urbonaviciute V et al (2022) Standardization of antigen-emulsion preparations for the induction of autoimmune disease models. Front Immunol 13:892251. https://doi.org/10.3389/fimmu.2022.892251
Li Y, Tong D, Liang P et al (2020) Cartilage-binding antibodies initiate joint inflammation and promote chronic erosive arthritis. Arthritis Res Ther 22:120. https://doi.org/10.1186/s13075-020-02169-0
Xing Y, Hogquist KA (2014) Isolation, identification, and purification of murine thymic epithelial cells. J Vis Exp JoVE. https://doi.org/10.3791/51780
Corthay A, Bäcklund J, Broddefalk J et al (1998) Epitope glycosylation plays a critical role for T cell recognition of type II collagen in collagen-induced arthritis. Eur J Immunol 28:2580–2590. https://doi.org/10.1002/(SICI)1521-4141(199808)28:08%3c2580::AID-IMMU2580%3e3.0.CO;2-X
Bäcklund J, Li C, Jansson E et al (2013) C57BL/6 mice need MHC class II Aq to develop collagen-induced arthritis dependent on autoreactive T cells. Ann Rheum Dis 72:1225–1232. https://doi.org/10.1136/annrheumdis-2012-202055
Efimova O, Szankasi P, Kelley TW (2011) Ncf1 (p47phox) is essential for direct regulatory T cell mediated suppression of CD4+ effector T cells. PLoS One 6:e16013. https://doi.org/10.1371/journal.pone.0016013
Xu D, Jiang H-R, Li Y et al (2010) IL-33 exacerbates autoantibody-induced arthritis. J Immunol Baltim Md 1950 184:2620–2626. https://doi.org/10.4049/jimmunol.0902685
Hagenow K, Gelderman KA, Hultqvist M et al (2009) Ncf1-associated reduced oxidative burst promotes IL-33R+ T cell-mediated adjuvant-free arthritis in mice. J Immunol Baltim Md 1950 183:874–881. https://doi.org/10.4049/jimmunol.0900966
Hultqvist M, Bäcklund J, Bauer K et al (2007) Lack of reactive oxygen species breaks T cell tolerance to collagen Type II and allows development of arthritis in mice. J Immunol 179:1431–1437. https://doi.org/10.4049/jimmunol.179.3.1431
Sansom SN, Shikama-Dorn N, Zhanybekova S et al (2014) Population and single-cell genomics reveal the Aire dependency, relief from Polycomb silencing, and distribution of self-antigen expression in thymic epithelia. Genome Res 24:1918–1931. https://doi.org/10.1101/gr.171645.113
Ardouin L, Luche H, Chelbi R et al (2016) Broad and largely concordant molecular changes characterize tolerogenic and immunogenic dendritic cell maturation in thymus and periphery. Immunity 45:305–318. https://doi.org/10.1016/j.immuni.2016.07.019
Perry JSA, Russler-Germain EV, Zhou YW et al (2018) Transfer of cell-surface antigens by scavenger receptor CD36 promotes thymic regulatory T cell receptor repertoire development and allo-tolerance. Immunity 48:923-936.e4. https://doi.org/10.1016/j.immuni.2018.04.007
Kelkka T, Kienhöfer D, Hoffmann M et al (2014) Reactive oxygen species deficiency induces autoimmunity with type 1 interferon signature. Antioxid Redox Signal 21:2231–2245. https://doi.org/10.1089/ars.2013.5828
Gelderman KA, Hultqvist M, Holmberg J et al (2006) T cell surface redox levels determine T cell reactivity and arthritis susceptibility. Proc Natl Acad Sci USA 103:12831–12836. https://doi.org/10.1073/pnas.0604571103
Gelderman KA, Hultqvist M, Pizzolla A et al (2007) Macrophages suppress T cell responses and arthritis development in mice by producing reactive oxygen species. J Clin Invest 117:3020–3028. https://doi.org/10.1172/JCI31935
Kraaij MD, Savage NDL, van der Kooij SW et al (2010) Induction of regulatory T cells by macrophages is dependent on production of reactive oxygen species. Proc Natl Acad Sci USA 107:17686–17691. https://doi.org/10.1073/pnas.1012016107
Holmdahl R, Sareila O, Olsson LM et al (2016) Ncf1 polymorphism reveals oxidative regulation of autoimmune chronic inflammation. Immunol Rev 269:228–247. https://doi.org/10.1111/imr.12378
Nordzieke DE, Medraño-Fernandez I (2018) The plasma membrane: a platform for intra- and intercellular Redox signaling. Antioxid Basel Switz 7:E168. https://doi.org/10.3390/antiox7110168
Jin R, Teng F, Xu X et al (2013) Redox balance of mouse medullary CD4 single-positive thymocytes. Immunol Cell Biol 91:634–641. https://doi.org/10.1038/icb.2013.57
Griffith AV, Fallahi M, Venables T, Petrie HT (2012) Persistent degenerative changes in thymic organ function revealed by an inducible model of organ regrowth. Aging Cell 11:169–177. https://doi.org/10.1111/j.1474-9726.2011.00773.x
Smith KGC, Clatworthy MR (2010) FcgammaRIIB in autoimmunity and infection: evolutionary and therapeutic implications. Nat Rev Immunol 10:328–343. https://doi.org/10.1038/nri2762
Verbeek JS, Hirose S, Nishimura H (2019) The complex association of FcγRIIb with autoimmune susceptibility. Front Immunol. https://doi.org/10.3389/fimmu.2019.02061
Espéli M, Smith KGC, Clatworthy MR (2016) FcγRIIB and autoimmunity. Immunol Rev 269:194–211. https://doi.org/10.1111/imr.12368
Li F, Smith P, Ravetch JV (2014) Inhibitory Fcγ receptor is required for the maintenance of tolerance through distinct mechanisms. J Immunol Baltim Md 1950 192:3021–3028. https://doi.org/10.4049/jimmunol.1302934
Espéli M, Clatworthy MR, Bökers S et al (2012) Analysis of a wild mouse promoter variant reveals a novel role for FcγRIIb in the control of the germinal center and autoimmunity. J Exp Med 209:2307–2319. https://doi.org/10.1084/jem.20121752
Morris AB, Farley CR, Pinelli DF et al (2020) Signaling through the inhibitory Fc receptor FcγRIIB induces CD8 T cell apoptosis to limit T cell immunity. Immunity 52:136-150.e6. https://doi.org/10.1016/j.immuni.2019.12.006
van Montfoort N, ’t Hoen PAC, Mangsbo SM et al (2012) Fcγ receptor IIb strongly regulates Fcγ receptor-facilitated T cell activation by dendritic cells. J Immunol Baltim Md 1950(189):92–101. https://doi.org/10.4049/jimmunol.1103703
Acknowledgements
The authors thank Carlos Palestro and Louisa Palestro for taking good care of the animals and Bingze Xu for her contribution in production of peptides and collagen.
Funding
Open access funding provided by Karolinska Institute. This work was supported by grants from the Knut and Alice Wallenberg Foundation (KAW 2015.0063), the Swedish Cancer Foundation (190341Pj01H), the National Natural Science Foundation of China (32070913), the Innovation Capacity Support Plan of Shaanxi Province (2020GHJD-06, S2020-ZC-GHJD-0012), Beihang University (KG16080401).
Author information
Authors and Affiliations
Contributions
QL, JZ, and RH contributed to conception and design of the study. QL, HL, VU, ZX and CH collected and analyzed data. RH acquired funding of the study. RH and JZ supervised the study. QL wrote the first draft of the manuscript. QL and RH reviewed and edited the manuscript. All authors read and approved the submitted version.
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, Q., Zhong, J., Luo, H. et al. Two major genes associated with autoimmune arthritis, Ncf1 and Fcgr2b, additively protect mice by strengthening T cell tolerance. Cell. Mol. Life Sci. 79, 482 (2022). https://doi.org/10.1007/s00018-022-04501-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-022-04501-0