Abstract
μ-opioid receptor (MOR) is a class of opioid receptors that is critical for analgesia, reward, and euphoria. MOR is distributed in various brain regions, including the hippocampus, where traditionally, it is believed to be localized mainly at the presynaptic terminals of the GABAergic inhibitory interneurons to exert a strong disinhibitory effect on excitatory pyramidal neurons. However, recent intensive research has uncovered the existence of MOR in hippocampal astrocytes, shedding light on how astrocytic MOR participates in opioid signaling via glia-neuron interaction in the hippocampus. Activation of astrocytic MOR has shown to cause glutamate release from hippocampal astrocytes and increase the excitability of presynaptic axon fibers to enhance the release of glutamate at the Schaffer Collateral-CA1 synapses, thereby, intensifying the synaptic strength and plasticity. This novel mechanism involving astrocytic MOR has been shown to participate in hippocampus-dependent conditioned place preference. Furthermore, the signaling of hippocampal MOR, whose action is sexually dimorphic, is engaged in adult neurogenesis, seizure, and stress-induced memory impairment. In this review, we focus on the two profoundly different hippocampal opioid signaling pathways through either GABAergic interneuronal or astrocytic MOR. We further compare and contrast their molecular and cellular mechanisms and their possible roles in opioid-associated conditioned place preference and other hippocampus-dependent behaviors.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Opioids such as morphine have been widely used for effective treatment of severe pain. Opioids are also frequently used non-medically for their euphoric effects, and the recreational use of opioids typically results in addiction [1, 2]. The opioids act upon their specific opioid receptors, i.e., μ-opioid receptor (MOR), δ-opioid receptor (DOR), κ-opioid receptor (KOR), and nociceptin receptors (NOR) [3]. Among these four types of opioid receptors, the prototypical agonist of MOR is morphine [4]. The identity of opioid receptors including MOR was first revealed in the 1970s [5, 6], whereas opiates have been conventionally used for remedial and recreational purposes for the past several thousand years. Furthermore, the crystal structure of G-protein-coupled MOR was elucidated very recently [7, 8], which gave significant insights into the design of new MOR ligands with improved pharmacological properties targeting the MOR. There are several well-known exogenous MOR agonists, including morphine, oxycodone, and oxymorphone, which are widely used as analgesics and are also highly addictive substances [9]. In addition to these exogenous agonists, there are endogenous MOR agonists such as beta-endorphin and enkephalin [10, 11], which were firstly isolated by groups led by Chung and Morris, respectively [12,13,14,15,16]. MOR has a widespread but selective distribution in the major circuits of pain, reward, and addiction, particularly in the periaqueductal gray region, nucleus accumbens, amygdala, and hippocampus [17, 18].
In the hippocampus, MOR is broadly expressed on GABAergic interneurons [10, 19,20,21,22]. MOR is a Gαi-protein-coupled receptor (Gi-GPCR), which is classically regarded as an inhibitory GPCR. Therefore, MOR activation by exogenous opioids of small molecular structures (e.g., morphine and oxycodone) and opioid peptides called exorphins (e.g., casomorphine and soymorphine) has been believed to excite neurons via suppression of presynaptic release of γ-aminobutyric acid (GABA) [23,24,25]. In addition to this traditional view, it has been recently demonstrated that a new surprising player of astrocytes in the CA1 hippocampus exhibits high expression of MOR [26], the activation of which elicits a significant release of glutamate from astrocytes through two-pore potassium (K2P) channels containing tandem of pore domains in a weak inward rectifying K+ channel-1 (TWIK-1) and TWIK-related K+ channel-1 (TREK-1) [27, 28]. These new findings suggest that astrocytic glutamate by MOR activation exerts a non-canonical excitatory effect of Gi-GPCR onto neighboring neurons.
In addition to the classical analgesic effect of opioids, several recent studies have focused on the relationship between MOR and diverse hippocampal functions. For example, MOR agonists affect cognitive performance such as spatial learning and memory by modulating the excitatory synaptic transmission in the hippocampus [29,30,31]. Moreover, MOR agonists are known to be engaged in adult hippocampal neurogenesis [32, 33], seizure [34,35,36], and stress-induced hippocampal changes [37, 38]. These studies allude to the possibility that hippocampal MOR plays key roles in many cognitive processes and pathological conditions, which might be under-appreciated and needs to be highlighted. However, there is not yet a comprehensive review on this important topic. Therefore, we have reviewed previous literature on the cellular localization of MOR, signaling pathways in interneurons and astrocytes, its role in synaptic transmission and plasticity, and the behavioral and cognitive functions of hippocampal MOR.
Cellular localization of MOR in the hippocampus
Four major subtypes of opioid receptors, three classical and one new subtype, have been characterized, which are MOR, DOR, KOR, and NOR, respectively [3]. Each subtype of opioid receptors has distinct functional differences with varying preferences for endogenous opioid peptides and exogenous ligands. Among them, MOR has a high affinity for beta-endorphin and enkephalin. Early immunohistochemical studies have reported that enkephalin is abundant in the hippocampus [39, 40], while beta-endorphin level has been inconclusive [41,42,43]. The presence of beta-endorphin needs to be confirmed by advanced sensor techniques such as G-protein-coupled receptor-based (GRAB) genetically encoded fluorescent sensor or fluorescence resonance energy transfer (FRET) sensor [44, 45].
Unlike the μ-opioid peptides, the localization of MOR has been established extensively. In the hippocampus, several early studies have demonstrated a relatively abundant expression of MOR in the pyramidal cell layer, stratum lacunosum-moleculare, and the molecular and granular cell layers of the ventral dentate gyrus [17, 46]. Subsequent immunocytochemistry and electron microscopy studies have shown that MOR is localized in the somatodendritic and axonal compartments of GABAergic neurons in rat hippocampal formation [22]. Among many types of GABAergic interneurons, MOR is expressed in most of the parvalbumin (PV)-containing basket cells and some of the somatostatin-, neuropeptide Y-, vasoactive intestinal peptide-, and calretinin-containing interneurons in the CA1 hippocampus [19,20,21]. In the dentate gyrus, MOR is extensively co-localized with PV, but not with somatostatin [21]. Consistently, a recent study using MOR-mCherry transgenic mice has clearly demonstrated that the expression of MOR in the CA1 pyramidal layer belongs to the presynaptic terminals of GABAergic interneurons, but not likely to the pyramidal neurons [26]. Taken together, these previous findings have suggested that MORs are most frequently found in the GABAergic interneurons, especially in PV-containing interneurons, which phasically inhibit the activities of granule cells and pyramidal neurons (Table 1 and Fig. 1).
Schematic diagrams of the MOR distribution in hippocampus region (CA1, CA3, and DG). Color of cell indicates cell types: gold, inhibitory neuron; green, pyramidal neuron; blue, granule cell; yellow, astrocyte. MOR is indicated in brown. DG dentate gyrus, SO stratum oriens, SP stratum pyramidale, SR stratum radiatum, SLM stratum lacunosum-moleculare, Slu stratum lucidum, ML molecular layer, GCL granule cell layer
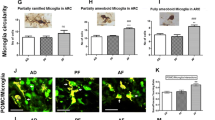
Meanwhile, whether non-neuronal cells, such as astrocytes, express MOR has been a controversial issue. A research group led by Hauser reported that primary cultured hippocampal astrocytes exhibit only little amounts of MOR [47]. Three years later, the same group demonstrated that primary cultured astrocytes from various brain regions, including cortex and hippocampus, express MOR [48]. Although in vivo evidence of astrocytic MOR in the hippocampus had been lacking, recent lines of evidence have clearly demonstrated the expression of MOR on astrocytes in the hippocampus, ventral tegmental area, and the nucleus accumbens by utilizing MOR-mCherry, MOR-knock-out transgenic mice, and two different antibodies validated with MOR specific-short hairpin RNA (shRNA) [26, 49] (Table 1). An ultrastructural investigation with electron microscopy further revealed that MOR is mainly localized in the soma and processes, but rarely in the microdomains of hippocampal astrocytes [26]. In addition to astrocytes, microglia are also reported to express MOR in the murine cerebral cortex, hippocampus, and striatum (Table 1) [50]. These findings have raised a possibility of neglected role of glial, especially astrocytic, MOR in various behavioral and cognitive functions including conditioned place preference (CPP) and opioid addiction, which had been attributed solely to interneuronal MOR in the hippocampus.
The canonical signaling pathway of MOR via inhibitory neurons
MOR is found in all portions of PV-positive inhibitory interneurons, especially in axonal processes and terminals. A previous study has demonstrated that many MOR-positive terminals contact NMDAR-positive dendrites and form inhibitory synapses with each other [51]. This finding has raised a possibility that endogenous or exogenous MOR agonists (e.g., beta-endorphin, morphine, or some exorphins targeting MOR such as casomorphine) may activate MOR to suppress GABAergic activity, thus boosting excitatory action of dentate granule cells or pyramidal neurons by GABAergic disinhibition. Indeed, whole-cell patch clamp recordings of dentate granule cells showed that MOR activation reduced the amplitude of inhibitory post-synaptic currents evoked by electrical stimulation (eIPSCs) [52].
How does MOR activation suppress the GABAergic activity on the inhibitory interneurons? The activation of neuronal MOR is well documented to cause presynaptic depression through inhibition of N- and P/Q-type voltage-gated calcium channels [23]. In addition, activation of MOR causes dissociation of G-protein βγ-subunits (Gβγ) from an inactive heterotrimeric G-protein complexes (Gαβγ), and the Gβγ binds to and opens G-protein-coupled inwardly-rectifying potassium (GIRK) channels [53] (Fig. 2a, b). MOR also activates voltage-gated potassium channels [54] and increases the conductance of M-type potassium channels in hippocampus [55]. Through the potassium channels, potassium efflux leads to hyperpolarization of the cell membrane, which reduces the inhibitory action of interneurons [56]. Indeed, an endogenous MOR agonist, enkephalin was reported to hyperpolarize GABAergic interneurons [24]. This is how MOR has been thought to increase the activity of excitatory neurons through disinhibition. Furthermore, opioids are also known to exert analgesic effects through MOR-mediated disinhibition [57, 58].
Cellular mechanisms underlying how hippocampal MOR activation enhances synaptic transmission and plasticity. a Schematic diagram of hippocampal synapses. b Schematic diagram of interneuronal MOR signaling through disinhibition via membrane hyperpolarization of GABAergic interneuron. MOR activation in the interneurons dissociates Gβγ from heterotrimeric G-protein complex, leading to the opening of GIRK by Gβγ binding. Potassium efflux through GIRK causes hyperpolarization of the interneurons, which decreases GABA release and causes GABAergic disinhibition. c Schematic diagram of astrocytic MOR signaling through glutamate release. MOR activation in the astrocytes dissociates Gβγ from heterotrimeric G-protein complex, leading to the opening of TREK-1 by Gβγ binding. Glutamate release through TREK-1 binds to mGluR1, which is localized in the axonal process of presynaptic neurons, causing glutamatergic axonal excitability. d Schematic diagram of the alteration of glutamatergic synaptic transmission at SC-CA1 synapses. CA1 cornu ammonis 1, CA3 cornu ammonis 3, DG dentate gyrus, SC Schaffer collateral, MF mossy fiber, MOR μ-opioid receptor, Gαi G-protein alpha I subunit. Gβγ G-protein beta gamma complex, GIRK G-protein-coupled inwardly-rectifying potassium channel, GABAA GABAA receptor, GABAB GABAB receptor, Glu glutamate, mGluR1 metabotropic glutamate receptor 1, TREK-1 TWIK-related potassium channel, AMPAR α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor, NMDAR N-methyl-D-aspartate receptor
The MOR-mediated reduction in GABA release causes a suppression of both GABAA and GABAB receptor-mediated inhibitory signaling. MOR activation is also reported to facilitate the propagation of excitatory activity in CA1 hippocampus of a rat by disinhibition of all anatomical layers through a suppression of GABAA receptor signaling [59]. In addition to GABAA receptor signaling, it is also suggested that MOR activation hinders GABAB-mediated hyperpolarization in CA1 hippocampus to boost the excitatory activity [60]. These findings together indicate that MOR activation in the GABAergic interneurons causes a suppression of GABAergic interneuronal activity, which in turn disinhibits the excitatory neurons in the hippocampus. So far, this mechanism, i.e. disinhibition through interneuronal MOR, has been accepted as the sole contributor of the MOR-mediated excitation in the hippocampus.
The novel signaling pathway of MOR involving astrocytes
In addition to GABAergic interneurons, MOR is highly expressed in astrocytes of the hippocampus [26]. Astrocytic MOR is mainly localized in the soma and processes, but rarely in the microdomains which form a tripartite synapse [26, 28]. This subcellular distribution of MOR in the hippocampal astrocytes is coinciding with TREK-1- and TWIK-1-containing K2P channels, which is known to be a glutamate-releasing channel in the astrocytes [27, 28]. The TREK-1- and TWIK-1-containing K2P channels can be opened upon the activation of astrocytic MOR and other Gi-GPCRs (GABABR, CB1R, and A1R) through dissociation of Gβγ which binds to N-terminus of TREK-1 (Fig. 2a, c) [27, 28]. Subsequently, intracellular glutamate is released through TREK-1- and TWIK-1-containing K2P channels in a Ca2+-independent manner [27, 28].
The glutamate released upon the activation of astrocytic MOR exerts an excitatory action through binding to group I metabotropic glutamate receptors (mGluRs), especially mGluR1 [61, 62]. mGluR1 is predominantly expressed on the axon strands of presynaptic neurons [62]. The astrocytic glutamate released upon MOR activation binds to axonal mGluR1, leading to an enhancement of the axonal excitability and subsequent increase in the probability of presynaptic glutamate release at the Schaffer collateral-CA1 (SC-CA1) synapses of the hippocampus [62] (Fig. 2c, d). Finally, the activation of astrocytic MOR, a classical inhibitory Gi-GPCR, exerts a paradoxical excitatory action through astrocytic glutamate release and this mechanism is entirely distinct from the action of interneuronal MOR. Based on these recent studies, the novel mechanism involving astrocytic MOR has made a debut as an alternative contributor to the MOR’s ability to boost excitatory signaling in the hippocampus.
Synaptic transmission enhancement through two distinct MOR signaling pathways
Since 1990s, several reports demonstrated that activation of MOR enhances glutamatergic synaptic transmission and plasticity at the hippocampal mossy fiber-CA3 synapses [63, 64], SC-CA1 synapses [62, 65], and the perforant path-dentate granule cell synapses [66, 67]. In the early 1990s, Martinez group has demonstrated that opioid receptors, especially MORs, are involved in the induction of long-term potentiation (LTP) at hippocampal mossy fiber-CA3 synapses [63, 64, 68, 69], which was also validated by other groups [70, 71]. A few years later, McQuiston group utilized voltage sensor imaging for an in-depth study of the layer-specific actions of MOR activation. They have demonstrated that MOR activation facilitates the excitatory activity more sensitively in stratum pyramidale, oriens, and radiatum, but less in stratum lacunosum-moleculare [59, 72]. Another group has also proposed that acute treatment of fentanyl, which is a strong agonist of MOR, dose-dependently increases the field excitatory post-synaptic potentials (fEPSPs) at the Schaffer collateral-CA1 (SC-CA1) synapses [73]. In addition to LTP, hippocampal MOR has been also implicated in the induction of long-term depression (LTD) at SC-CA1 synapses [38, 74].
This effect of hippocampal MOR in excitatory synaptic potentiation can be attributed to either GABAergic disinhibition or glutamate release from astrocyte or both. Until now, the excitatory action exerted upon MOR activation has been mostly ascribed to GABA-mediated disinhibition [73, 75, 76] based upon previous reports of the exclusive expression of MOR in the inhibitory interneurons [22]. In detail, MORs are known to act exclusively by hyperpolarizing inhibitory interneurons and suppressing inhibitory synaptic transmission, which translates into an increase in excitatory activity in the hippocampus. This was coincident with the findings that MOR-dependent augmentation of excitatory synaptic transmission is mediated by a suppression of both GABAA [59] and GABAB receptor-mediated hyperpolarization [60].
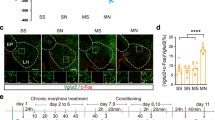
On the other hand, some contradictory data from electrophysiological experiments have been reported. A recent study reported that the enhancement of evoked EPSC (eEPSC) and evoked EPSP (eEPSP) by DAMGO ([D-Ala2, N-MePhe4, Gly-ol]-enkephalin), the MOR agonist, was observed even in the presence of GABAA and GABAB blockers, bicuculline and CGP55845, respectively, in the CA1 hippocampus [62]. This surprising result suggested that the disinhibitory action of MOR might be a minor contributor to the enhancement of eEPSC and eEPSP. In an attempt to resolve this conflict, we performed an additional experiment of whole-cell patch clamp recording to measure eEPSC in the presence or absence of bicuculline and CGP55845 (Fig. 3). Surprisingly, we were able to recapitulate that the DAMGO-induced enhancement of eEPSC was indistinguishable between the absence and presence of bicuculline and CGP55845 (Fig. 3). These additional findings indicate that, in addition to GABAergic disinhibition, there is another critical player in the excitatory action of MOR, the astrocytic MOR [26, 28, 62]. These results raise a surprising possibility that the astrocytic MOR could be the major contributor to the excitatory action of MOR in the CA1 hippocampus.
DAMGO enhances eEPSC at SC-CA1 synapse, which is not mediated by GABAergic disinhibition. DAMGO-mediated enhancement of eEPSC amplitude was not further increased by treatment with bicuculline and CGP55845, which are blockers against GABAA and GABAB receptors, respectively. Orange trace is originated from Nam et al. Cell Reports (2019). DAMGO [D-Ala2, N-MePhe4, Gly-ol]-enkephalin, Bic bicuculline, CGP CGP55845, EPSC excitatory post-synaptic current, ns non-significant
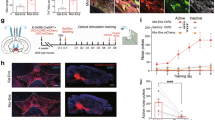
The activation of astrocytic MOR in the dorsal hippocampus can induce a fast glutamate release through TREK-1- and TWIK-1-containing K2P channels, as revealed by sniffer patch technique [28] and astrocytic glutamate sensor (iGluSnFr) imaging in CA1 hippocampus [62]. An investigation with whole-cell patch clamp of CA1 pyramidal neurons has demonstrated that astrocytic MOR activation also causes a significant decrease in the paired pulse ratio and a dramatic increase in the frequency of spontaneous excitatory post-synaptic currents (sEPSCs) without affecting sEPSC amplitude, indicating an increased presynaptic release at the glutamatergic SC-CA1 synapses. Moreover, this enhancement of synaptic transmission by MOR activation further led to an induction of the NMDAR-dependent LTP with subthreshold stimulation at SC-CA1 synapses of the hippocampus [62]. The astrocytic MOR-dependent enhancements of synaptic transmission and LTP induction were dependent on presynaptic mGluR1. More importantly, DAMGO-induced enhancements of synaptic transmission and LTP in the hippocampal slices were not attributed to GABAergic disinhibition, as most of the experiments were performed in the presence of GABAA and GABAB blockers [62]. Furthermore, the study also revealed that DAMGO’s action was much more potent in increasing the frequency of sEPSC (EC50 = 0.49 nM) than in reducing the frequency of sIPSC (IC50 = 50.67 nM) [62]. These findings indicate that DAMGO-induced enhancement of glutamatergic transmission is less likely mediated by the suppression of GABAergic transmission. Taken together, the recent lines of evidence suggest that the astrocytic glutamate release upon MOR activation is a more predominant contributor to the excitatory action of MOR agonists, compared to the disinhibitory action of interneuronal MOR.
Opioid-associated contextual memory formation by hippocampal astrocytic MOR
The MOR agonists, such as morphine and DAMGO, are well known to induce CPP through the disinhibition of mesocorticolimbic dopamine system by suppressing GABAergic transmission [77]. Although mesocorticolimbic dopamine system is critical for wanting/motivational aspect of CPP, there is another major aspect to CPP: spatial learning and memory. The precise mechanism of spatial learning and memory in CPP is not very well understood.
The hippocampus is critical to the formation of contextual memory, especially to the opioid-associated contextual memory. Several studies have demonstrated the causal relationship between the hippocampus and MOR-induced CPP. A lesion study previously demonstrated that the hippocampus is necessary for systemically administered morphine-induced CPP [78]. The necessity of hippocampal MOR for opioid-induced CPP was also demonstrated by pharmacological blockade of MOR through intra-hippocampal infusion of a specific antagonist of MOR, D-Phe-Cys-Tyr-D-Trp-Orn-Thr-Pen-Thr-NH2 (CTOP) [62]. In addition to the necessity of hippocampal MOR, the sufficiency was also demonstrated by intra-hippocampal injection of morphine, which was sufficient to induce CPP in rats [79]. These reports have suggested that the hippocampus is sufficient and necessary for morphine-induced CPP. However, to date, there has been no study using cell-type specific gene-modulation of MOR, possibly due to the strong belief that MOR is exclusively expressed in GABAergic interneurons.
In 2019, a study utilizing the genetic strategy of cell-type specific gene-silencing of MOR systematically tested the possible contribution of MORs of pyramidal neurons, GABAergic interneurons, or astrocytes in the CA1 hippocampus to the DAMGO-induced CPP [62]. The study demonstrated that astrocytic MOR, but not of pyramidal neurons and interneurons, was necessary for CPP by both intra-CA1 infusion and systemic administration of DAMGO [62]. Moreover, this study also demonstrated that astrocyte-specific expression of MOR in the CA1 hippocampus recovered systemic DAMGO or morphine-induced CPP in the MOR-deficient mice [62]. These findings indicate that the astrocytic MOR in CA1 hippocampus is sufficient and necessary for CPP, establishing a causal relationship between the two.
Consistently, several other previous reports have alluded to the idea that another player besides GABAergic disinhibition is required for CPP. Subcutaneous administration of morphine (1 mg/kg) is well documented as sufficient to induce CPP in rats [80]. If this CPP is induced by GABAergic disinhibition, the concentration of morphine in the brain should be enough to inhibit sIPSCs. However, previous pharmacokinetics reports point to the fact that the concentration of morphine in the brain after subcutaneous administration may not be enough to inhibit sIPSCs. It has been reported that after intravenous injection of morphine (10 mg/kg), the maximum concentration of morphine in the brain is ~ 120 ng/mL, which is equivalent to 0.42 μM [81]. The subcutaneous administration of morphine (1 mg/kg) can be assumed to reach the brain with the concentration of under 0.042 μM after accounting for the fact that subcutaneous administration is generally less effective to reach the brain compared to intravenous administration. Another report demonstrated that such a low dose of morphine (under 0.1 μM) merely inhibits sIPSC frequency (~ 20%), and the IC50 of morphine to inhibit sIPSC frequency is about 2 μM [25]. Taken together, these findings suggest that low dosage morphine-induced CPP is less likely to be mediated by GABAergic disinhibition, but more likely mediated by other players such as astrocytic MOR.
Since the hippocampus contains a high density of endogenous MOR agonists such as enkephalin [40], it is possible that the hippocampal MORs contribute to the acquisition and retrieval of spatial memory. Indeed, MOR null knock-out mice showed an impaired spatial memory in eight-arm radial maze and Morris water maze tests with impaired LTP at mossy fiber to CA3 synapses [71, 82]. A few years later, another report insisted that the impaired task performance in the Morris water maze test was attributed to a motivational deficit (namely, a deficit in dopamine signaling), but not a learning deficit [83]. However, there was a report showing that the CA3-specific pharmacological blockade of MOR by β-funaltrexamine (β-FNA) caused a significant impairment in the acquisition and retrieval of spatial learning [84]. On the other hand, a recent study reported a normal spatial memory of MOR null knock-out mice in the passive avoidance test [62]. Taken together, unlike opioid-associated spatial memory, the contribution of hippocampal MOR to the non-opioid-associated spatial memory is still controversial. Future investigations are needed to establish the precise role of MOR in the acquisition of spatial memory in the hippocampus.
Other behavioral roles of hippocampal MOR
Adult neurogenesis Several previous studies have revealed that the chronic administration of opioids negatively influences adult hippocampal neurogenesis [85,86,87], which is correlated to the hippocampus-dependent learning ability [88, 89]. Among the multi-stage process of neurogenesis (i.e., proliferation, differentiation, migration, and maturation), the chronic exposure to morphine is reported to negatively affect proliferation [85, 90, 91], decrease the survival of newborn cells [86] and interrupt maturation [85]. Moreover, MOR null knock-out mice show an increase in the survival rate of newborn cells without affecting proliferation rate, leading to the increased number of granule cells and increased layer volume in the granule cell layer of the dentate gyrus [92]. Nonetheless, the precise mechanism of how MOR negatively influences hippocampal neurogenesis has not been fully elucidated. Meanwhile, MOR was recently reported to be expressed in hippocampal astrocytes [26, 62], with close contact with neural stem cells and an ability to affect their proliferation and differentiation [93]. Moreover, astrocytic glutamate uptake is reported to be critical for adult neurogenesis [94], implying that astrocytic glutamate release might also affect adult neurogenesis. To sum up, the role of astrocytic MOR in the adult hippocampal neurogenesis needs to be investigated in the future.
Seizure Seizures are known to modify hippocampal distribution of MORs and vice versa. The protein density, mRNA level, and basal binding affinity of MOR are higher in the hippocampus of human post-mortem brains with epilepsy [95]. Seizures increase the MOR immunoreactivities in the inner molecular layer where GABAergic interneurons are mostly located, but lower than in the granule cell layer and hilus of DG where excitatory neurons are mostly located [11, 34, 35]. In addition to the alteration of the receptor, the mRNA and hormone levels of enkephalin are increased in the hippocampus of human epileptics and the hippocampus of several epileptic rodent models [39, 96,97,98,99,100]. Increased MOR signaling could contribute to seizure development by altering excitation/inhibition (E/I) balance towards excitation, possibly through MOR-mediated enhanced disinhibition. In contrast, several reports have demonstrated that MOR agonists such as morphine and beta-endorphin also increased the susceptibility to seizures [101, 102], while only few studies reported that systemic application of MOR agonist results in an anti-convulsant effect [103]. These results strongly suggest an interesting possibility of MOR involvement in epilepsy. In addition to MOR, KOR, and DOR are also highly implicated in seizure pathology [11]. It will be of great interest to determine whether the disinhibitory action or astrocytic MOR is critical to the role of MOR in seizures.
Stress-induced memory impairment Learning and memory is strongly affected by stress, which is known to facilitate LTD in CA1 hippocampus [104, 105]. Two recent studies have demonstrated that acute stress-induced memory impairment is mediated by GABAergic interneuronal MOR, but not by astrocytic or excitatory neuronal MOR [37, 38]. The authors showed that an acute elevated platform (EP) stress caused the activation of the GABAergic interneuronal MOR in the hippocampus, possibly by upregulation of endogenous MOR agonists [37, 38, 106]. In turn, GABAergic feedforward and feedback inhibition of CA1 pyramidal neurons is attenuated and LTD at SC-CA1 glutamatergic synapses is facilitated [38]. These results implicate the engagement of GABAergic interneuronal MOR in acute stress-induced memory impairment. As stress-induced upregulation of endogenous MOR agonists can also affect astrocytic MOR in the hippocampus, future investigations on the alteration of astrocytic MOR signaling under stressful condition could be of interest.
Sexual dimorphism of hippocampal MOR A recent study reported that the MOR-mediated response to stress is sex-dependent due to the sexual dimorphic phenotype of MOR [107]. Indeed, the MOR trafficking in PV-positive neurons and enkephalin level are positively regulated by gonadal hormones, especially ovarian hormones [108, 109]. In detail, MOR trafficking in the hippocampal PV-positive interneurons is increased in the proestrus phase (relatively high estrogens) of a female rat, as compared to diestrus phase [109]. This sexual dimorphism of hippocampal μ-opioid signaling leads to sex-dependent behavior of MOR. For example, MOR-mediated regulation of mossy fiber transmission is distinct only in females [110]. More interestingly, acute immobilization stress increased the immunoreactivity of phosphorylated MOR in the hippocampus of male, did not alter it in the diestrus female, and significantly decreased it in proestrus female rats [111]. Not only the protein level, but also the MOR trafficking is sex-differentially altered by acute stress: decreased in females and increased in males [107, 109]. These previous findings have proposed the estrogen-dependent sexual dimorphism of hippocampal μ-opioid signaling, which affects its response to acute stress. All the current studies on sexual dimorphism of MOR have only focused on MOR of GABAergic interneurons. Based on recent evidence of astrocytic MOR [26, 62], the possible sex-dimorphic alteration of the expression and trafficking of astrocytic MOR requires further investigation.
Summary
We have comprehensively reviewed the cellular expression of MOR, its signaling pathways, and its behavioral and cognitive function in the hippocampus. While MOR in the GABAergic interneurons has long been focused on, the presence and function of MOR in the astrocytes have only recently been investigated. Activation of interneuronal MOR causes membrane hyperpolarization and suppresses GABAergic synaptic transmission leading to disinhibition of pyramidal neurons in the CA1 and granule cells in the dentate gyrus. Therefore, MORs of the GABAergic interneurons are considered as the major contributors of hippocampal MOR signaling. However, recent studies have revealed that hippocampal astrocytes express MOR, and the activation of the astrocytic MOR causes glutamate release to enhance glutamatergic synaptic transmission at SC-CA1 synapses. Furthermore, astrocytic MOR activation, but not interneuronal MOR activation, mainly contributes to MOR-mediated enhancement of synaptic transmission in the hippocampus and opioid-mediated contextual memory. Lastly, hippocampal MOR signaling is engaged in hippocampal neurogenesis, seizure, and stress-induced memory impairment, which are reportedly dependent on MOR-mediated disinhibition of principal hippocampal cells. Further investigations are needed to determine the contribution of astrocytic MOR to these pathophysiological functions.
References
Wang S (2019) Historical review: opiate addiction and opioid receptors. Cell Transp 28(3):233–238. https://doi.org/10.1177/0963689718811060
Green J (2017) Epidemiology of opioid abuse and addiction. J Emerg Nurs 43(2):106–113. https://doi.org/10.1016/j.jen.2016.09.004
Corbett AD, Henderson G, McKnight AT, Paterson SJ (2006) 75 years of opioid research: the exciting but vain quest for the Holy Grail. Br J Pharmacol 147(Suppl 1):S153–162. https://doi.org/10.1038/sj.bjp.0706435
Stefano GB, Ptacek R, Kuzelova H, Kream RM (2012) Endogenous morphine: up-to-date review 2011. Folia Biol (Praha) 58(2):49–56
Pert CB, Snyder SH (1973) Opiate receptor: demonstration in nervous tissue. Science 179(4077):1011–1014. https://doi.org/10.1126/science.179.4077.1011
Goldstein A, Lowney LI, Pal BK (1971) Stereospecific and nonspecific interactions of the morphine congener levorphanol in subcellular fractions of mouse brain. Proc Natl Acad Sci U S A 68(8):1742–1747. https://doi.org/10.1073/pnas.68.8.1742
Huang W, Manglik A, Venkatakrishnan AJ, Laeremans T, Feinberg EN, Sanborn AL, Kato HE, Livingston KE, Thorsen TS, Kling RC, Granier S, Gmeiner P, Husbands SM, Traynor JR, Weis WI, Steyaert J, Dror RO, Kobilka BK (2015) Structural insights into micro-opioid receptor activation. Nature 524(7565):315–321. https://doi.org/10.1038/nature14886
Manglik A, Kruse AC, Kobilka TS, Thian FS, Mathiesen JM, Sunahara RK, Pardo L, Weis WI, Kobilka BK, Granier S (2012) Crystal structure of the micro-opioid receptor bound to a morphinan antagonist. Nature 485(7398):321–326. https://doi.org/10.1038/nature10954
Babalonis S, Lofwall MR, Nuzzo PA, Walsh SL (2016) Pharmacodynamic effects of oral oxymorphone: abuse liability, analgesic profile and direct physiologic effects in humans. Addict Biol 21(1):146–158. https://doi.org/10.1111/adb.12173
Drake CT, Chavkin C, Milner TA (2007) Opioid systems in the dentate gyrus. Prog Brain Res 163:245–263. https://doi.org/10.1016/S0079-6123(07)63015-5
Burtscher J, Schwarzer C (2017) The opioid system in temporal lobe epilepsy: functional role and therapeutic potential. Front Mol Neurosci 10:245. https://doi.org/10.3389/fnmol.2017.00245
Li CH, Barnafi L, Chretien M, Chung D (1965) Isolation and amino-acid sequence of beta-LPH from sheep pituitary glands. Nature 208(5015):1093–1094. https://doi.org/10.1038/2081093b0
Li CH, Chung D (1976) Isolation and structure of an untriakontapeptide with opiate activity from camel pituitary glands. Proc Natl Acad Sci U S A 73(4):1145–1148. https://doi.org/10.1073/pnas.73.4.1145
Hughes J, Smith TW, Kosterlitz HW, Fothergill LA, Morgan BA, Morris HR (1975) Identification of two related pentapeptides from the brain with potent opiate agonist activity. Nature 258(5536):577–580. https://doi.org/10.1038/258577a0
Hughes J (1975) Isolation of an endogenous compound from the brain with pharmacological properties similar to morphine. Brain Res 88(2):295–308. https://doi.org/10.1016/0006-8993(75)90391-1
Fricker LD, Margolis E, Gomes I, Devi LA (2020) Five decades of research on opioid peptides: Current knowledge and unanswered questions. Mol Pharmacol. https://doi.org/10.1124/mol.120.119388
Arvidsson U, Riedl M, Chakrabarti S, Lee JH, Nakano AH, Dado RJ, Loh HH, Law PY, Wessendorf MW, Elde R (1995) Distribution and targeting of a mu-opioid receptor (MOR1) in brain and spinal cord. J Neurosci 15(5 Pt 1):3328–3341
Garzon M, Pickel VM (2001) Plasmalemmal mu-opioid receptor distribution mainly in nondopaminergic neurons in the rat ventral tegmental area. Synapse 41(4):311–328. https://doi.org/10.1002/syn.1088
Drake CT, Milner TA (2002) Mu opioid receptors are in discrete hippocampal interneuron subpopulations. Hippocampus 12(2):119–136. https://doi.org/10.1002/hipo.1107
Stumm RK, Zhou C, Schulz S, Hollt V (2004) Neuronal types expressing mu- and delta-opioid receptor mRNA in the rat hippocampal formation. J Comp Neurol 469(1):107–118. https://doi.org/10.1002/cne.10997
Drake CT, Milner TA (2006) Mu opioid receptors are extensively co-localized with parvalbumin, but not somatostatin, in the dentate gyrus. Neurosci Lett 403(1–2):176–180. https://doi.org/10.1016/j.neulet.2006.04.047
Drake CT, Milner TA (1999) Mu opioid receptors are in somatodendritic and axonal compartments of GABAergic neurons in rat hippocampal formation. Brain Res 849(1–2):203–215
Heinke B, Gingl E, Sandkuhler J (2011) Multiple targets of mu-opioid receptor-mediated presynaptic inhibition at primary afferent Adelta- and C-fibers. J Neurosci 31(4):1313–1322. https://doi.org/10.1523/JNEUROSCI.4060-10.2011
Madison DV, Nicoll RA (1988) Enkephalin hyperpolarizes interneurons in the rat hippocampus. J Physiol 398:123–130
Bull FA, Baptista-Hon DT, Lambert JJ, Walwyn W, Hales TG (2017) Morphine activation of mu opioid receptors causes disinhibition of neurons in the ventral tegmental area mediated by beta-arrestin2 and c-Src. Sci Rep 7(1):9969. https://doi.org/10.1038/s41598-017-10360-8
Nam MH, Han KS, Lee J, Bae JY, An H, Park S, Oh SJ, Kim E, Hwang E, Bae YC, Lee CJ (2018) Expression of µ-opioid receptor in CA1 hippocampal astrocytes. Experimental Neurobiology 27(2):120–128
Woo DH, Han KS, Shim JW, Yoon BE, Kim E, Bae JY, Oh SJ, Hwang EM, Marmorstein AD, Bae YC, Park JY, Lee CJ (2012) TREK-1 and Best1 channels mediate fast and slow glutamate release in astrocytes upon GPCR activation. Cell 151(1):25–40. https://doi.org/10.1016/j.cell.2012.09.005
Woo DH, Bae JY, Nam M-H, An H, Ju YH, Won J, Choi JH, Hwang EM, Han K-S, Bae YC, Lee CJ (2018) Activation of astrocytic μ-opioid receptor elicits fast glutamate release through TREK-1-containing K2P channel in hippocampal astrocytes. Front Cell Neurosci. https://doi.org/10.3389/fncel.2018.00319
Bramham CR (1992) Opioid receptor dependent long-term potentiation: peptidergic regulation of synaptic plasticity in the hippocampus. Neurochem Int 20(4):441–455. https://doi.org/10.1016/0197-0186(92)90021-i
Pu L, Bao GB, Xu NJ, Ma L, Pei G (2002) Hippocampal long-term potentiation is reduced by chronic opiate treatment and can be restored by re-exposure to opiates. J Neurosci 22(5):1914–1921
Robbins TW, Ersche KD, Everitt BJ (2008) Drug addiction and the memory systems of the brain. Ann N Y Acad Sci 1141:1–21. https://doi.org/10.1196/annals.1441.020
Persson AI, Thorlin T, Bull C, Zarnegar P, Ekman R, Terenius L, Eriksson PS (2003) Mu- and delta-opioid receptor antagonists decrease proliferation and increase neurogenesis in cultures of rat adult hippocampal progenitors. Eur J Neurosci 17(6):1159–1172. https://doi.org/10.1046/j.1460-9568.2003.02538.x
Cominski TP, Ansonoff MA, Turchin CE, Pintar JE (2014) Loss of the mu opioid receptor induces strain-specific alterations in hippocampal neurogenesis and spatial learning. Neuroscience 278:11–19. https://doi.org/10.1016/j.neuroscience.2014.07.039
Skyers PS, Einheber S, Pierce JP, Milner TA (2003) Increased mu-opioid receptor labeling is found on inner molecular layer terminals of the dentate gyrus following seizures. Exp Neurol 179(2):200–209. https://doi.org/10.1016/s0014-4886(02)00018-3
Bausch SB, Chavkin C (1997) Changes in hippocampal circuitry after pilocarpine-induced seizures as revealed by opioid receptor distribution and activation. J Neurosci 17(1):477–492
French ED, Siggins GR (1980) An iontophoretic survey of opioid peptide actions in the rat limbic system: in search of opiate epileptogenic mechanisms. Regul Pept 1(2):127–146. https://doi.org/10.1016/0167-0115(80)90016-6
Shi MM, Fan KM, Qiao YN, Xu JH, Qiu LJ, Li X, Liu Y, Qian ZQ, Wei CL, Han J, Fan J, Tian YF, Ren W, Liu ZQ (2019) Hippocampal mu-opioid receptors on GABAergic neurons mediate stress-induced impairment of memory retrieval. Mol Psychiatry. https://doi.org/10.1038/s41380-019-0435-z
Fan KM, Qiu LJ, Ma N, Du YN, Qian ZQ, Wei CL, Han J, Ren W, Shi MM, Liu ZQ (2019) Acute stress facilitates LTD induction at glutamatergic synapses in the hippocampal CA1 region by activating mu-opioid receptors on GABAergic neurons. Front Neurosci 13:71. https://doi.org/10.3389/fnins.2019.00071
Hong JS, Wood PL, Gillin JC, Yang HY, Costa E (1980) Changes of hippocampal Met-enkephalin content after recurrent motor seizures. Nature 285(5762):231–232. https://doi.org/10.1038/285231a0
Gall C, Brecha N, Karten HJ, Chang KJ (1981) Localization of enkephalin-like immunoreactivity to identified axonal and neuronal populations of the rat hippocampus. J Comp Neurol 198(2):335–350. https://doi.org/10.1002/cne.901980211
Zakarian S, Smyth D (1979) Distribution of active and inactive forms of endorphins in rat pituitary and brain. Proc Natl Acad Sci U S A 76(11):5972–5976. https://doi.org/10.1073/pnas.76.11.5972
Zakarian S, Smyth DG (1982) Distribution of beta-endorphin-related peptides in rat pituitary and brain. Biochem J 202(3):561–571. https://doi.org/10.1042/bj2020561
Chavkin C, Shoemaker WJ, McGinty JF, Bayon A, Bloom FE (1985) Characterization of the prodynorphin and proenkephalin neuropeptide systems in rat hippocampus. J Neurosci 5(3):808–816
Sun F, Zeng J, Jing M, Zhou J, Feng J, Owen SF, Luo Y, Li F, Wang H, Yamaguchi T, Yong Z, Gao Y, Peng W, Wang L, Zhang S, Du J, Lin D, Xu M, Kreitzer AC, Cui G, Li Y (2018) A genetically encoded fluorescent sensor enables rapid and specific detection of dopamine in flies, fish, and mice. Cell 174(2):481–496. https://doi.org/10.1016/j.cell.2018.06.042
Patriarchi T, Cho JR, Merten K, Howe MW, Marley A, Xiong WH, Folk RW, Broussard GJ, Liang R, Jang MJ, Zhong H, Dombeck D, von Zastrow M, Nimmerjahn A, Gradinaru V, Williams JT, Tian L (2018) Ultrafast neuronal imaging of dopamine dynamics with designed genetically encoded sensors. Science. https://doi.org/10.1126/science.aat4422
Mansour A, Khachaturian H, Lewis ME, Akil H, Watson SJ (1988) Anatomy of CNS opioid receptors. Trends Neurosci 11(7):308–314. https://doi.org/10.1016/0166-2236(88)90093-8
Stiene-Martin A, Zhou R, Hauser KF (1998) Regional, developmental, and cell cycle-dependent differences in mu, delta, and kappa-opioid receptor expression among cultured mouse astrocytes. Glia 22(3):249–259
Ruzicka BB, Fox CA, Thompson RC, Meng F, Watson SJ, Akil H (1995) Primary astroglial cultures derived from several rat brain regions differentially express mu, delta and kappa opioid receptor mRNA. Brain Res Mol Brain Res 34(2):209–220
Corkrum M, Rothwell PE, Thomas MJ, Kofuji P, Araque A (2019) Opioid-mediated astrocyte-neuron signaling in the nucleus accumbens. Cells. https://doi.org/10.3390/cells8060586
Maduna T, Audouard E, Dembele D, Mouzaoui N, Reiss D, Massotte D, Gaveriaux-Ruff C (2018) Microglia express mu opioid receptor: insights from transcriptomics and fluorescent reporter mice. Front Psychiatry 9:726. https://doi.org/10.3389/fpsyt.2018.00726
Milner TA, Drake CT (2001) Ultrastructural evidence for presynaptic mu opioid receptor modulation of synaptic plasticity in NMDA-receptor-containing dendrites in the dentate gyrus. Brain Res Bull 54(2):131–140. https://doi.org/10.1016/s0361-9230(00)00415-9
Xie CW, Morrisett RA, Lewis DV (1992) Mu opioid receptor-mediated modulation of synaptic currents in dentate granule cells of rat hippocampus. J Neurophysiol 68(4):1113–1120. https://doi.org/10.1152/jn.1992.68.4.1113
Lober RM, Pereira MA, Lambert NA (2006) Rapid activation of inwardly rectifying potassium channels by immobile G-protein-coupled receptors. J Neurosci 26(48):12602–12608. https://doi.org/10.1523/JNEUROSCI.4020-06.2006
Wimpey TL, Chavkin C (1991) Opioids activate both an inward rectifier and a novel voltage-gated potassium conductance in the hippocampal formation. Neuron 6(2):281–289. https://doi.org/10.1016/0896-6273(91)90363-5
Moore SD, Madamba SG, Schweitzer P, Siggins GR (1994) Voltage-dependent effects of opioid peptides on hippocampal CA3 pyramidal neurons in vitro. J Neurosci 14(2):809–820
Hoang QV, Bajic D, Yanagisawa M, Nakajima S, Nakajima Y (2003) Effects of orexin (hypocretin) on GIRK channels. J Neurophysiol 90(2):693–702. https://doi.org/10.1152/jn.00001.2003
Stein C, Schafer M, Machelska H (2003) Attacking pain at its source: new perspectives on opioids. Nat Med 9(8):1003–1008. https://doi.org/10.1038/nm908
Millan MJ (1999) The induction of pain: an integrative review. Prog Neurobiol 57(1):1–164. https://doi.org/10.1016/s0301-0082(98)00048-3
McQuiston AR, Saggau P (2003) Mu-opioid receptors facilitate the propagation of excitatory activity in rat hippocampal area CA1 by disinhibition of all anatomical layers. J Neurophysiol 90(3):1936–1948. https://doi.org/10.1152/jn.01150.2002
McQuiston AR (2007) Effects of mu-opioid receptor modulation on GABAB receptor synaptic function in hippocampal CA1. J Neurophysiol 97(3):2301–2311. https://doi.org/10.1152/jn.01179.2006
Perea G, Araque A (2007) Astrocytes potentiate transmitter release at single hippocampal synapses. Science 317(5841):1083–1086. https://doi.org/10.1126/science.1144640
Nam MH, Han KS, Lee J, Won W, Koh W, Bae JY, Woo J, Kim J, Kwong E, Choi TY, Chun H, Lee SE, Kim SB, Park KD, Choi SY, Bae YC, Lee CJ (2019) Activation of astrocytic mu-opioid receptor causes conditioned place preference. Cell Rep 28(5):1154–1166. https://doi.org/10.1016/j.celrep.2019.06.071
Derrick BE, Martinez JL Jr (1994) Frequency-dependent associative long-term potentiation at the hippocampal mossy fiber-CA3 synapse. Proc Natl Acad Sci U S A 91(22):10290–10294. https://doi.org/10.1073/pnas.91.22.10290
Derrick BE, Martinez JL Jr (1994) Opioid receptor activation is one factor underlying the frequency dependence of mossy fiber LTP induction. J Neurosci 14(7):4359–4367
SanMartin S, Menendez L, Gutierrez M, Hidalgo A, Baamonde A (2000) Effects of DAGO on the rodent hippocampal evoked potentials using different perfusion solutions. Acta Neurobiol Exp (Wars) 60(2):187–193
Xie CW, Lewis DV (1991) Opioid-mediated facilitation of long-term potentiation at the lateral perforant path-dentate granule cell synapse. J Pharmacol Exp Ther 256(1):289–296
Jin W, Chavkin C (1999) Mu opioids enhance mossy fiber synaptic transmission indirectly by reducing GABAB receptor activation. Brain Res 821(2):286–293. https://doi.org/10.1016/s0006-8993(99)01089-6
Derrick BE, Rodriguez SB, Lieberman DN, Martinez JL Jr (1992) Mu opioid receptors are associated with the induction of hippocampal mossy fiber long-term potentiation. J Pharmacol Exp Ther 263(2):725–733
Derrick BE, Weinberger SB, Martinez JL Jr (1991) Opioid receptors are involved in an NMDA receptor-independent mechanism of LTP induction at hippocampal mossy fiber-CA3 synapses. Brain Res Bull 27(2):219–223. https://doi.org/10.1016/0361-9230(91)90071-q
Matthies H, Schroeder H, Becker A, Loh H, Hollt V, Krug M (2000) Lack of expression of long-term potentiation in the dentate gyrus but not in the CA1 region of the hippocampus of mu-opioid receptor-deficient mice. Neuropharmacology 39(6):952–960. https://doi.org/10.1016/s0028-3908(99)00203-8
Jamot L, Matthes HW, Simonin F, Kieffer BL, Roder JC (2003) Differential involvement of the mu and kappa opioid receptors in spatial learning. Genes Brain Behav 2(2):80–92. https://doi.org/10.1034/j.1601-183x.2003.00013.x
McQuiston AR (2008) Layer selective presynaptic modulation of excitatory inputs to hippocampal cornu Ammon 1 by mu-opioid receptor activation. Neuroscience 151(1):209–221. https://doi.org/10.1016/j.neuroscience.2007.09.077
Tian H, Xu Y, Liu F, Wang G, Hu S (2015) Effect of acute fentanyl treatment on synaptic plasticity in the hippocampal CA1 region in rats. Front Pharmacol 6:251. https://doi.org/10.3389/fphar.2015.00251
Wagner JJ, Etemad LR, Thompson AM (2001) Opioid-mediated facilitation of long-term depression in rat hippocampus. J Pharmacol Exp Ther 296(3):776–781
Xie CW, Lewis DV (1995) Depression of LTP in rat dentate gyrus by naloxone is reversed by GABAA blockade. Brain Res 688(1–2):56–60. https://doi.org/10.1016/0006-8993(95)00510-w
Zieglgansberger W, French ED, Siggins GR, Bloom FE (1979) Opioid peptides may excite hippocampal pyramidal neurons by inhibiting adjacent inhibitory interneurons. Science 205(4404):415–417
Fields HL, Margolis EB (2015) Understanding opioid reward. Trends Neurosci 38(4):217–225. https://doi.org/10.1016/j.tins.2015.01.002
Olmstead MC, Franklin KB (1997) The development of a conditioned place preference to morphine: effects of lesions of various CNS sites. Behav Neurosci 111(6):1313–1323. https://doi.org/10.1037//0735-7044.111.6.1313
Corrigall WA, Linseman MA (1988) Conditioned place preference produced by intra-hippocampal morphine. Pharmacol Biochem Behav 30(3):787–789
Mueller D, Perdikaris D, Stewart J (2002) Persistence and drug-induced reinstatement of a morphine-induced conditioned place preference. Behav Brain Res 136(2):389–397. https://doi.org/10.1016/s0166-4328(02)00297-8
Zakaria Z, Badhan R (2018) Development of a region-specific physiologically based pharmacokinetic brain model to assess hippocampus and frontal cortex pharmacokinetics. Pharmaceutics. https://doi.org/10.3390/pharmaceutics10010014
Jang CG, Lee SY, Yoo JH, Yan JJ, Song DK, Loh HH, Ho IK (2003) Impaired water maze learning performance in mu-opioid receptor knockout mice. Brain Res Mol Brain Res 117(1):68–72. https://doi.org/10.1016/s0169-328x(03)00291-2
Lubbers ME, van den Bos R, Spruijt BM (2007) Mu opioid receptor knockout mice in the Morris water maze: a learning or motivation deficit? Behav Brain Res 180(1):107–111. https://doi.org/10.1016/j.bbr.2007.02.021
Meilandt WJ, Barea-Rodriguez E, Harvey SA, Martinez JL Jr (2004) Role of hippocampal CA3 mu-opioid receptors in spatial learning and memory. J Neurosci 24(12):2953–2962. https://doi.org/10.1523/JNEUROSCI.5569-03.2004
Arguello AA, Harburg GC, Schonborn JR, Mandyam CD, Yamaguchi M, Eisch AJ (2008) Time course of morphine's effects on adult hippocampal subgranular zone reveals preferential inhibition of cells in S phase of the cell cycle and a subpopulation of immature neurons. Neuroscience 157(1):70–79. https://doi.org/10.1016/j.neuroscience.2008.08.064
Eisch AJ, Barrot M, Schad CA, Self DW, Nestler EJ (2000) Opiates inhibit neurogenesis in the adult rat hippocampus. Proc Natl Acad Sci U S A 97(13):7579–7584. https://doi.org/10.1073/pnas.120552597
Zhang Y, Xu C, Zheng H, Loh HH, Law PY (2016) Morphine modulates adult neurogenesis and contextual memory by impeding the maturation of neural progenitors. PLoS ONE 11(4):e0153628. https://doi.org/10.1371/journal.pone.0153628
Aimone JB, Li Y, Lee SW, Clemenson GD, Deng W, Gage FH (2014) Regulation and function of adult neurogenesis: from genes to cognition. Physiol Rev 94(4):991–1026. https://doi.org/10.1152/physrev.00004.2014
Eisch AJ (2002) Adult neurogenesis: implications for psychiatry. Prog Brain Res 138:315–342. https://doi.org/10.1016/S0079-6123(02)38085-3
Arguello AA, Fischer SJ, Schonborn JR, Markus RW, Brekken RA, Eisch AJ (2009) Effect of chronic morphine on the dentate gyrus neurogenic microenvironment. Neuroscience 159(3):1003–1010. https://doi.org/10.1016/j.neuroscience.2009.01.020
Mandyam CD, Norris RD, Eisch AJ (2004) Chronic morphine induces premature mitosis of proliferating cells in the adult mouse subgranular zone. J Neurosci Res 76(6):783–794. https://doi.org/10.1002/jnr.20090
Harburg GC, Hall FS, Harrist AV, Sora I, Uhl GR, Eisch AJ (2007) Knockout of the mu opioid receptor enhances the survival of adult-generated hippocampal granule cell neurons. Neuroscience 144(1):77–87. https://doi.org/10.1016/j.neuroscience.2006.09.018
Casse F, Richetin K, Toni N (2018) Astrocytes' contribution to adult neurogenesis in physiology and alzheimer's disease. Front Cell Neurosci 12:432. https://doi.org/10.3389/fncel.2018.00432
Guo Y, Wei Q, Huang Y, Xia W, Zhou Y, Wang S (2013) The effects of astrocytes on differentiation of neural stem cells are influenced by knock-down of the glutamate transporter, GLT-1. Neurochem Int 63(5):498–506. https://doi.org/10.1016/j.neuint.2013.08.003
Cuellar-Herrera M, Velasco AL, Velasco F, Chavez L, Orozco-Suarez S, Armagan G, Turunc E, Bojnik E, Yalcin A, Benyhe S, Borsodi A, Alonso-Vanegas M, Rocha L (2012) Mu opioid receptor mRNA expression, binding, and functional coupling to G-proteins in human epileptic hippocampus. Hippocampus 22(2):122–127. https://doi.org/10.1002/hipo.20891
Hong JS, McGinty JF, Grimes L, Kanamatsu T, Obie J, Mitchell CL (1988) Seizure-induced alterations in the metabolism of hippocampal opioid peptides suggest opioid modulation of seizure-related behaviors. NIDA Res Monogr 82:48–66
Houser CR, Miyashiro JE, Swartz BE, Walsh GO, Rich JR, Delgado-Escueta AV (1990) Altered patterns of dynorphin immunoreactivity suggest mossy fiber reorganization in human hippocampal epilepsy. J Neurosci 10(1):267–282
Pierce JP, Milner TA (2001) Parallel increases in the synaptic and surface areas of mossy fiber terminals following seizure induction. Synapse 39(3):249–256. https://doi.org/10.1002/1098-2396(20010301)39:3<249:AID-SYN1006>3.0.CO;2-5
Rees H, Ang LC, Shul DD, George DH, Begley H, McConnell T (1994) Increase in enkephalin-like immunoreactivity in hippocampi of adults with generalized epilepsy. Brain Res 652(1):113–119. https://doi.org/10.1016/0006-8993(94)90324-7
Hong JS, McGinty JF, Lee PH, Xie CW, Mitchell CL (1993) Relationship between hippocampal opioid peptides and seizures. Prog Neurobiol 40(4):507–528. https://doi.org/10.1016/0301-0082(93)90020-s
Rocha L, Ackermann RF, Engel J Jr (1996) Effects of chronic morphine pretreatment on amygdaloid kindling development, postictal seizure and suppression and benzodiazepine receptor binding in rats. Epilepsy Res 23(3):225–233. https://doi.org/10.1016/0920-1211(95)00103-4
Cain DP, Boon F, Corcoran ME (1990) Involvement of multiple opiate receptors in opioid kindling. Brain Res 517(1–2):236–244. https://doi.org/10.1016/0006-8993(90)91032-c
Simmons ML, Chavkin C (1996) k-Opioid receptor activation of a dendrotoxin-sensitive potassium channel mediates presynaptic inhibition of mossy fiber neurotransmitter release. Mol Pharmacol 50(1):80–85
Wong TP, Howland JG, Robillard JM, Ge Y, Yu W, Titterness AK, Brebner K, Liu L, Weinberg J, Christie BR, Phillips AG, Wang YT (2007) Hippocampal long-term depression mediates acute stress-induced spatial memory retrieval impairment. Proc Natl Acad Sci U S A 104(27):11471–11476. https://doi.org/10.1073/pnas.0702308104
Xu L, Anwyl R, Rowan MJ (1997) Behavioural stress facilitates the induction of long-term depression in the hippocampus. Nature 387(6632):497–500. https://doi.org/10.1038/387497a0
Li W, Papilloud A, Lozano-Montes L, Zhao N, Ye X, Zhang X, Sandi C, Rainer G (2018) Stress impacts the regulation neuropeptides in the rat hippocampus and prefrontal cortex. Proteomics 18(7):e1700408. https://doi.org/10.1002/pmic.201700408
Milner TA, Burstein SR, Marrone GF, Khalid S, Gonzalez AD, Williams TJ, Schierberl KC, Torres-Reveron A, Gonzales KL, McEwen BS, Waters EM (2013) Stress differentially alters mu opioid receptor density and trafficking in parvalbumin-containing interneurons in the female and male rat hippocampus. Synapse 67(11):757–772. https://doi.org/10.1002/syn.21683
Torres-Reveron A, Khalid S, Williams TJ, Waters EM, Drake CT, McEwen BS, Milner TA (2008) Ovarian steroids modulate leu-enkephalin levels and target leu-enkephalinergic profiles in the female hippocampal mossy fiber pathway. Brain Res 1232:70–84. https://doi.org/10.1016/j.brainres.2008.07.058
Torres-Reveron A, Williams TJ, Chapleau JD, Waters EM, McEwen BS, Drake CT, Milner TA (2009) Ovarian steroids alter mu opioid receptor trafficking in hippocampal parvalbumin GABAergic interneurons. Exp Neurol 219(1):319–327. https://doi.org/10.1016/j.expneurol.2009.06.001
Harte-Hargrove LC, Varga-Wesson A, Duffy AM, Milner TA, Scharfman HE (2015) Opioid receptor-dependent sex differences in synaptic plasticity in the hippocampal mossy fiber pathway of the adult rat. J Neurosci 35(4):1723–1738. https://doi.org/10.1523/JNEUROSCI.0820-14.2015
Gonzales KL, Chapleau JD, Pierce JP, Kelter DT, Williams TJ, Torres-Reveron A, McEwen BS, Waters EM, Milner TA (2011) The influences of reproductive status and acute stress on the levels of phosphorylated mu opioid receptor immunoreactivity in rat hippocampus. Front Endocrinol (Lausanne). https://doi.org/10.3389/fendo.2011.00018
Breindl A, Derrick BE, Rodriguez SB, Martinez JL Jr (1994) Opioid receptor-dependent long-term potentiation at the lateral perforant path-CA3 synapse in rat hippocampus. Brain Res Bull 33(1):17–24. https://doi.org/10.1016/0361-9230(94)90045-0
Kaplan TJ, Skyers PR, Tabori NE, Drake CT, Milner TA (2004) Ultrastructural evidence for mu-opioid modulation of cholinergic pathways in rat dentate gyrus. Brain Res 1019(1–2):28–38. https://doi.org/10.1016/j.brainres.2004.05.050
Zhang H, Jia M, Wang XW, Ye C, Li Y, Wang N, Elefant F, Ma H, Cui C (2019) Dentate gyrus mu-opioid receptor-mediated neurogenic processes are associated with alterations in morphine self-administration. Sci Rep 9(1):1471. https://doi.org/10.1038/s41598-018-37083-8
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nam, MH., Won, W., Han, KS. et al. Signaling mechanisms of μ-opioid receptor (MOR) in the hippocampus: disinhibition versus astrocytic glutamate regulation. Cell. Mol. Life Sci. 78, 415–426 (2021). https://doi.org/10.1007/s00018-020-03595-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00018-020-03595-8