Abstract
Costimulatory signals initiated by the interaction between the tumor necrosis factor (TNF) ligand and cognate TNF receptor (TNFR) superfamilies promote clonal expansion, differentiation, and survival of antigen-primed CD4+ and CD8+ T cells and have a pivotal role in T-cell-mediated adaptive immunity and diseases. Accumulating evidence in recent years indicates that costimulatory signals via the subset of the TNFR superfamily molecules, OX40 (TNFRSF4), 4-1BB (TNFRSF9), CD27, DR3 (TNFRSF25), CD30 (TNFRSF8), GITR (TNFRSF18), TNFR2 (TNFRSF1B), and HVEM (TNFRSF14), which are constitutive or inducible on T cells, play important roles in protective immunity, inflammatory and autoimmune diseases, and tumor immunotherapy. In this chapter, we will summarize the findings of recent studies on these TNFR family of co-signaling molecules regarding their function at various stages of the T-cell response in the context of infection, inflammation, and cancer. We will also discuss how these TNFR co-signals are critical for immune regulation and have therapeutic potential for the treatment of T-cell-mediated diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
The tumor necrosis factor (TNF) superfamily (TNFSF) of cytokines engages specific cognate cell surface receptors, the TNF receptor superfamily (TNFRSF). The TNFSF–TNFRSF interactions activate signaling pathways for cell survival, death, and differentiation that control immune function and disease, and several receptor–ligand pairs within TNF family molecules expressed by immune cells play key roles in T-cell immunity (Locksley et al. 2001; Aggarwal 2003; So et al. 2006; Croft 2009; Watts 2005; Ward-Kavanagh et al. 2016). The subset of TNFRSF molecules, 4-1BB, CD27, CD30, DR3 (death receptor 3), GITR (glucocorticoid-induced TNFR family-related protein), HVEM (herpesvirus entry mediator), OX40, and TNFR2 (tumor necrosis factor receptor 2), expressed by T cells, deliver activating signals, which are largely dependent on antigen recognition and participate in activation, clonal expansion, and differentiation of T cells. TNFRSF and TNFSF molecules that contribute to these additional signals in T cells function as a costimulatory receptor and a costimulatory ligand, respectively (Croft 2009; Watts 2005; So and Croft 2013) (Table 3.1, Fig. 3.1).
Protein domain organization in the TNF–TNFR family of co-signaling molecules. Data are based on UniProt (www.uniprot.org). TNF-α, P01375; LT-α, P01374; BTLA, Q7Z6A9; CD160, O95971; LIGHT, O43557; TL1A, O95150; OX40L, P23510; CD70, P32970; CD30L, P32971; 4-1BBL, P41273; GITRL, Q9UNG2; TNFR2, P20333; HVEM, Q92956; DcR3, O95407; DR3, Q93038; OX40, P43489; CD27, P26842; CD30, P28908; 4-1BB, Q07011; GITR, Q9Y5U5. LT-α shows low affinity for HVEM (dashed line)
A dialogue between a naïve T cell and a dendritic cell (DC) plays an essential role for priming of naïve T cells in secondary lymph organs. The expression levels of 4-1BB, CD27, CD30, DR3, GITR, HVEM, OX40, and TNFR2 on T cells are positively or negatively controlled by activating signals through the T-cell receptor (TCR) and the costimulatory receptor CD28. At the same time, after recognition of microbes, immature DCs are activated via pattern recognition receptors and upregulate not only major histocompatibility complex (MHC) and B7 proteins but also TNFSF molecules including 4-1BBL, CD70, CD30L, TL1A (TNF-like ligand 1A), GITRL, LIGHT, OX40L, and TNF-α. The T cell-DC dialogue via each individual TNFSF–TNFRSF interaction provides additional costimulatory signals to antigen-primed naïve T cells, promotes the differentiation of naïve T cells into effector and memory T-cell populations, and supports the survival of these antigen-primed T cells in the periphery (Fig. 3.2).
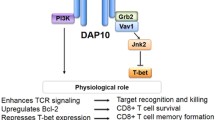
T-cell signaling regulated by the TNF–TNFR family of co-signaling molecules. T cells are activated firstly by recognition of antigen by the T-cell receptor (TCR)/CD3 complex when antigenic peptides are presented by class I or class II molecules of the major histocompatibility complex (MHC) on antigen-presenting cell (APCs), such as dendritic cells, B cells, and macrophages. The second costimulatory signal is delivered via CD28 by interacting its ligands B7.1 (CD80) and/or B7.2 (CD86). After recognition of trimeric TNF ligand superfamily (TNFSF) molecules on APCs, TNF receptor superfamily (TNFRSF) molecules on T cells are trimerized and recruit TNF receptor-associated factors (TRAFs) to their cytoplasmic regions, which results in activation of canonical and noncanonical nuclear factor kappa B (NF-κB) and mitogen-activated protein kinase (MAPK) pathways. The TNFSF–TNFRSF interaction promotes costimulatory signaling pathways, which include phosphoinositide 3-kinase (PI3K)-Akt (protein kinase B), NF-κB, and MAPK pathways, initiated by the TCR and CD28, and plays important roles for T-cell activation, differentiation, and survival, at both early and later stages of the T-cell response. TNFSF and TNFRSF molecules constitutively and inducibly expressed by cells are indicated in blue and red, respectively
In this chapter, we focus on the TNFRSF of costimulatory receptors, 4-1BB, CD27, CD30, DR3, GITR, HVEM, OX40, and TNFR2, and summarize the significance of costimulatory signals mediated by these receptors in terms of protective immunity, autoimmunity and inflammation, and cancer, in which these TNFRSF molecules play critical roles. Administration of agonistic or antagonistic agents (biologics) that can modulate the co-signaling activity of TNFRSF molecules can regulate T-cell functions in vivo, and thus these TNFSF–TNFRSF interactions have been considered as therapeutic targets for intervention in human diseases including autoimmunity and cancer.
2 Structure
2.1 Ligand
The costimulatory ligands of the TNFSF described in this chapter are type II (intracellular N terminus and extracellular C terminus) transmembrane proteins and have a C-terminal TNF homology domain (THD) that is responsible for receptor binding (Bodmer et al. 2002) (Table 3.1, Fig. 3.1). One TNFSF molecule assembles into a trimer on the surface of antigen-presenting cells (APCs), and its cognate monomer TNFRSF molecule on T cells is trimerized through binding to the trimeric configuration of the ligand THDs, resulting in formation of a quaternary organized hexamer complex at the T cell–APC interface (Fig. 3.2). TNFSF molecules can be produced as membrane-bound trimers or be released as soluble trimers from the cell surface after proteolytic processing in the stalk region. The membrane-bound TNFSF molecules that are engaged by their cognate receptors have been defined as inducers of signal transduction. This “reverse” signaling mediated by membrane-bound TNFSF molecules can regulate some cellular functions, such as pro-inflammatory cytokine production and cell maturation (Eissner et al. 2004; Sun and Fink 2007).
2.2 Receptor
The costimulatory receptors of the TNFRSF described in this chapter are type I (extracellular N terminus and intracellular C terminus) transmembrane proteins and have three to six cysteine-rich domains (CRDs) in their extracellular regions (Bodmer et al. 2002) (Table 3.1, Fig. 3.1). After binding to TNFSF timers via CRDs, TNFRSF molecules cluster on the T-cell membrane, which in turn initiates co-signaling cascades in antigen-recognized T cells. The cytoplasmic amino acid sequences divide TNFRSF molecules into three major groups: (1) TNF receptor-associated factor (TRAF) binding TNFRSF molecule, such as 4-1BB, CD27, CD30, DR3, GITR, HVEM, OX40, and TNFR2; (2) death domain (DD) containing TNFRSF molecule, such as DR3; and (3) decoy TNFRSF molecule lacking a functional cytoplasmic domain, such as DcR3 (decoy receptor 3). Upon binding of cognate TNFSF molecules, the TNFRSF of co-signaling molecules on T cells initiate “forward” signaling mediated by the TRAF family molecules, and this TRAF-mediated signaling contributes to activation of co-signaling cascades in antigen-primed T cells (Figs. 3.1 and 3.2). The extracellular domains of membrane-bound TNFRSF molecules can be cleaved to release soluble TNFRSF forms in some contexts.
2.3 TRAF
After binding to cognate ligands of the TNFSF family molecules, the TNFRSF of co-signaling molecules recruits various intracellular TRAF molecules to their cytoplasmic tails, leading to activation of canonical and noncanonical nuclear factor-kappa B (NF-κB), mitogen-activated protein kinase (MAPK), and serine/threonine-protein kinase Akt (protein kinase B) cascades (Brenner et al. 2015; So and Croft 2013; Hayden and Ghosh 2014; Karin and Gallagher 2009) (Fig. 3.2). Thus, TRAFs mediate the link between receptor-proximal and cytosolic signaling events. Six TRAFs, TRAF1 to TRAF6, which share a conserved C-terminal TRAF-C domain, function both as ubiquitin E3 ligases and as adaptor molecules to potentiate signal transduction. Except for TRAF1, the N-terminal of TRAF contains a really interesting new gene (RING) and zinc-finger domains that are responsible for ubiquitin E3 ligase activity to promote the activation of downstream signaling cascades. The C-terminal of TRAF contains a coiled-coil (TRAF-N) domain and a TRAF-C domain that contributes to intermolecular interactions and sequence-specific interactions with receptor cytoplasmic tails, respectively (Ha et al. 2009; So et al. 2015).
3 TNFR Co-signaling
3.1 OX40L-OX40
3.1.1 Expression and Function
Naïve CD4+ and CD8+ T cells do not express OX40. OX40 is induced on activated T cells upon antigen recognition and is downregulated after antigen clearance. Resting and memory T cells rapidly reexpress OX40 after antigen reencounter. CD28 co-signaling and pro-inflammatory cytokines including IL-1, IL-2, IL-4, and TNF-α can promote the expression of OX40. Foxp3+ CD25+ CD4+ regulatory T cells (Treg cells) constitutively express OX40 in mice. OX40L is induced on activated T cells and professional APCs, such as DCs, B cells, and macrophages. Activating signals via CD40, B-cell receptor (BCR), Toll-like receptors (TLRs), and cytokines, such as TSLP, type I IFN, and IL-18, and prostaglandin E2 promote the expression of OX40L on APCs. Mice deficient in Ox40 or Ox40l show no abnormality in organization of lymphoid tissues and early development of the immune system. Upon interaction with OX40L, OX40 recruits TRAF2 and TRAF3 and promotes the activation of NF-κB, PI3K-Akt, and NFAT pathways in antigen-primed T cells (Table 3.1, Figs. 3.1 and 3.2).
A genetic deficiency of Ox40 or Ox40l in mice leads to defective survival of antigen-primed CD4+ and CD8+ T cells during an active immune response and causes decreased accumulation of antigen-specific memory T cells in the later stages of the primary immune response. The interaction between OX40 on a T cell and OX40L on an APC provides critical costimulatory signals to activated T cells and controls not only cell survival but also other functional activities of effector/memory T cells. A number of studies indicate that OX40 has a more dominant role in CD4+ rather than CD8+ T-cell immunity because of its higher expression on CD4+ T cells. OX40–OX40L interactions regulate the expansion, differentiation, and activity of Treg cells in both positive and negative manner depending on the context (Sugamura et al. 2004; Croft et al. 2009; Ishii et al. 2010; Croft 2010) (see Sect. 3.9).
3.1.2 Protective Immunity
Pathogen invasion results in activation of antigen-specific CD4+ and CD8+ T cells, and the OX40 co-signaling in primed T cells plays a key role in establishing protective immunity against infections by promoting the accumulation of antigen-specific effector/memory T cells. The OX40–OX40L interaction enhances pathogen-specific T-cell immunity in various models of infection including lymphocytic choriomeningitis virus (LCMV), influenza virus, vaccinia virus, human immunodeficiency virus, Epstein–Barr virus (EBV), cytomegalovirus (CMV), Listeria monocytogenes, and malaria. Although excessive stimulation of activated T cells with an agonistic monoclonal antibody (mAb) to OX40 induces adverse responses in some contexts, OX40 co-signaling generally augments both primary and memory T-cell responses to bacteria, virus, and parasite infections (Mousavi et al. 2008; Humphreys et al. 2007; Salek-Ardakani et al. 2008; Zander et al. 2015).
The cross talk and counterbalance between OX40 costimulatory and PD-1 (programmed cell death 1, CD279) co-inhibitory pathways play important roles for generation of protective CD4+ T-cell immunity against malaria. OX40 is expressed by malaria-specific CD4+ T cells but not CD8+ T cells, and the expression is sustained after malaria infection. OX40L blockade and OX40 agonism exhibit enhanced and reduced parasite burdens, respectively. OX40 signaling supports the expansion of IFN-γ+ T-bet+ T-helper-1 (Th1) cells and Bcl-6+ T follicular helper (Tfh) cells. OX40 signaling also enhances extra-follicular IgM+ plasmablast formation, sustained Tfh responses, germinal center (GC) reactions, and T-dependent malaria-specific antibody class switching to IgG1. Both OX40 and PD-1 are expressed by malaria-specific CD4+ T cells, and simultaneous PD-1 blockade and OX40 stimulation induce overproduction of IFN-γ, which limits Tfh cell-dependent humoral immunity that requires parasite control. This shows that OX40 co-signaling augments malaria-specific CD4+ T-cell immunity and that PD-1 co-inhibitory signaling counterbalances the OX40 signaling to inhibit Th1 effector responses, which in turn facilitates the generation of optimal Tfh response required for humoral immunity to parasite (Zander et al. 2015).
In vaccinia virus infection in mice, the OX40–OX40L interaction promotes the development of Tfh cells, which is critical for GC development, plasma cell generation, and virus-specific antibody responses. OX40 is expressed by differentiating Tfh cells, and OX40L is expressed by CD11c+ DCs in the periarteriolar lymphoid sheaths and the marginal zone bridging channels and by B220+ B cells in the follicles. OX40L+ DCs and OX40L+ B cells are in contact with OX40+ CD4+ T cells at the T/B borders in the white pulp of the spleen. OX40 and ICOS (inducible T-cell costimulatory, CD278) are co-expressed by CXCR5+ Bcl-6+ Tfh cells in GC, and deficiency in OX40 or OX40L blockade or ICOS blockade significantly inhibits the development of both Tfh cells and GC B cells. This demonstrates that OX40 co-signaling in synergy with ICOS co-signaling maximizes Tfh responses and GC reactions, which are important for humoral immunity against vaccinia virus (Tahiliani et al. 2017).
A case study that reports a nonfunctional OX40 mutant in a patient strongly suggests that OX40 co-signaling plays a critical role in establishing a long-term T-cell immunity to pathogens in humans. The homozygous Arg65Cys missense/loss-of-function mutation in the first of four CRDs of extracellular region in OX40 causes a low level of OX40 expression on the T-cell surface, and this residual OX40 mutant protein does not show any binding activity to OX40L. The peripheral blood from this patient contains a decreased frequency of memory CD4+ T cells. Consistent with this, in vitro recall T-cell responses to encountered antigens, including tuberculin purified protein derivatives (PPD), tetanus toxoid, EBV, CMV, and herpes simplex virus type 1, are severely impaired in this patient (Byun et al. 2013).
3.1.3 Autoimmunity and Inflammation
The OX40–OX40L interaction drives the development of autoimmunity and inflammation in many different animal models of asthma, colitis, graft-versus-host disease (GVHD), diabetes, multiple sclerosis, rheumatoid arthritis, atherosclerosis, and transplantation. Polymorphisms of the OX40L and OX40 genes have been identified as risk factors in human diseases including systemic lupus erythematosus (SLE), rheumatoid arthritis, Sjögren syndrome, systemic sclerosis, cardiovascular disease, and narcolepsy (Table 3.2). Antigen-primed pathogenic T cells, but not naïve T cells, express OX40 or rapidly reexpress OX40 upon antigen reencounter, and thus the blockade of OX40L-OX40 interaction with a mAb or the depletion of OX40+ T cells with a mAb to OX40 has been suggested to be effective for treatment of these T-cell-mediated diseases (Sugamura et al. 2004; Croft et al. 2009; Ishii et al. 2010; Croft 2010
).
One human lupus study shows the correlation between the frequency of circulating OX40L+ myeloid APCs in blood and the disease activity of SLE. OX40L is highly expressed in inflamed tissues including the tonsils, kidney, and skin from SLE patients. Sera from SLE patients contain immune complexes with RNA that can promote OX40L expression through TLR7 in APCs, and this OX40L activates human CD4+ T cells to become Tfh-like cells possessing B-cell-helper activity. This proposes a hypothesis that excessive OX40 co-signaling through OX40L overproduction on APCs causes aberrant Tfh responses that lead to SLE (Jacquemin et al. 2015).
OX40L blockade in conjunction with traditional costimulation blockade is effective in preventing alloreactive T-cell responses that hinder long-term graft function and survival. In a murine allogeneic skin graft model, a blocking mAb to OX40L, but not to ICOSL (ICOS ligand, CD275), CD70, RANKL (receptor activator of NF-κB ligand, TNFSF11, CD254), or 4-1BBL, significantly improves allograft survival when combined with traditional blockade with anti-CD40L and CTLA-4 (cytotoxic T-lymphocyte-associated protein-4, CD152)-immunoglobulin (CTLA-4-Ig). This combined blockade effectively suppresses not only primary but also memory allogeneic T-cell responses. In a nonhuman primate renal transplantation model, treatment with combined humanized anti-OX40L mAb and belatacept (CTLA-4-Ig) exhibits a synergistic suppressive effect in prolonging allograft survival. This demonstrates that successful acceptance of allografts can be achieved by the simultaneous blockade of multiple costimulatory pathways and suggests that in this setting blockade of OX40 co-signaling is effective for dampening memory T-cell responses against allografts (Kitchens et al. 2017).
3.1.4 Cancer
Agonistic agents against OX40, such as anti-OX40 mAb and OX40L-Ig, provide potent costimulatory signals that can augment the expansion and proliferation of CD4+ and CD8+ T cells that recognize tumor antigens. In addition, the transduction of tumor cells or DCs with a vector that expresses OX40L can effectively boost antitumor T-cell responses. Although augmenting OX40 co-signaling can induce tumor regression and delay tumor growth, combination therapies of OX40 agonists with additional immune modulations, such as other mAbs to costimulatory/co-inhibitory receptors, cytokines, vaccination, chemotherapy, and radiotherapy, have been suggested to be more effective in comparison to OX40 monotherapies (Moran et al. 2013; Linch et al. 2015).
OX40 agonism can effectively eradicate tumor cells in the presence of an immune checkpoint inhibitor and vaccination. Combination of mAb treatment of mice with anti-OX40 agonist and anti-CTLA-4 antagonist promotes the expansion and differentiation of tumor antigen-specific effector/memory CD8+ T cells. In murine models of mammary carcinoma and spontaneous prostate adenocarcinoma, additional vaccination targeting to cross-presenting DCs using an anti-DEC205 (CD205) mAb conjugated with HER2, a tumor-associated antigen that is overexpressed in a subset of breast cancers, promotes the induction of IFN-γ-producing CD4+ and CD8+ T cells that infiltrate into the tumor, which leads to extensive tumor destruction and improved mice survival. This demonstrates that OX40 agonism in synergy with checkpoint inhibitor blockade and tumor antigen vaccination augments durable T-cell immunity that is effective for tumor eradication (Linch et al. 2016).
3.2 4-1BBL-4-1BB
3.2.1 Expression and Function
As with OX40, 4-1BB is not expressed by naïve or resting CD4+ and CD8+ T cells but is transiently upregulated on activated T cells upon TCR triggering. 4-1BBL is transiently induced on activated professional APCs by signals from CD40 and TLRs. A genetic deficiency of 4-1bb or 4-1 bbl in mice displays no abnormality in the development of lymphocytes and lymphoid organs. Co-signaling via 4-1BB promotes T-cell proliferation, cytokine production, and cell survival. 4-1BB plays more predominant effects on CD8+ T-cell responses because of its higher expression on CD8+ T cells in comparison with CD4+ T cells. Upon binding with 4-1BBL, 4-1BB recruits TRAF1 and TRAF2, which leads to activation of NF-κB, Akt, and MAPK pathways (Snell et al. 2011; Wortzman et al. 2013a; Croft 2009) (Table 3.1, Figs. 3.1 and 3.2).
4-1BB is expressed on Treg cells. Divergent expression of 4-1BB and CD40L can distinguish antigen-specific human Treg cells from conventional activated CD4+ T cells. In the course of short-term activation of human peripheral blood mononuclear cells (PBMCs) with antigens in vitro, Treg cells and conventional CD4+ T cells upregulate 4-1BB and CD40L, respectively. Purified 4-1BB+ Treg cells express Treg marker genes including FOXP3, CD25, HELIOS, and CTLA4. 4-1BB+ Treg cells display a complete demethylation of the Treg-specific demethylated region (TSDR) at the FOXP3 gene locus and exhibit a potent antigen-specific suppressive activity. This indicates that the extremely low frequency of antigen-specific Treg cells can be isolated from human PBMCs based on the surface expression of 4-1BB (Bacher et al. 2016).
3.2.2 Protective Immunity
The predominant role for 4-1BB co-signaling in CD8+ T-cell immunity has been demonstrated in various murine infection models including LCMV, influenza virus, CMV, murine gammaherpesvirus 68, vesicular stomatitis virus, and Listeria monocytogenes. The requirement of 4-1BB co-signaling for both CD4+ and CD8+ T-cell responses depends on the antigen load, the persistence of the infection, and the nature of pathogens. The levels of 4-1BB on T cells can be sustained under conditions where the infection persists. In general, mice lacking 4-1bb or 4-1 bbl show defective pathogen clearance and impaired antigen-specific CD8+ T-cell memory formation, especially in chronic or highly infectious disease context with the higher antigenic load. On the other hand, in a situation where antigens are rapidly cleared or the infection induces minimal inflammation, the deficiency in 4-1bb or 4-1 bbl does not display defective antigen-specific T-cell responses (Snell et al. 2011; Wortzman et al. 2013a).
3.2.3 Cancer
Ligation of 4-1BB with agonistic antibodies or engineered 4-1BBL on the surface of tumor cells or DCs promotes 4-1BB co-signaling that leads to expansion of tumor antigen-specific effector CD4+ and CD8+ T cells. Anti-4-1BB agonists can induce significant tumor regressions in various established tumor models, although the associated immunopathology has been reported. The use of anti-4-1BB agonists in combination with other cancer therapeutics, such as checkpoint inhibitors, vaccination, anticancer drugs, radiation, cytokines, and adoptive T-cell therapy, has been shown to exert synergistic antitumor activity (Sanchez-Paulete et al. 2016; Bartkowiak and Curran 2015; Vinay and Kwon 2014).
4-1BB agonism combination with vaccination can induce durable antitumor T-cell immunity against vaginally implanted tumor cells. In a mouse model of human papillomavirus (HPV) syngeneic tumor, mice administered with anti-4-1BB agonistic mAb combination with a peptide vaccine, which is composed of peptides from HPV-16 E6/E7 oncoproteins and α-galactosylceramide, display stronger tumor regression, which is accompanied with expansion of HPV-specific cytotoxic CD4+ and CD8+ T cells and with robust infiltration of these cytotoxic T lymphocytes (CTLs) into the tumor microenvironment. Neither checkpoint inhibitors (anti-CTLA-4 or -PD-1) nor anti-TNFR agonists (anti-OX40, -CD40, or -GITR) cannot recapitulate the therapeutic effect of the 4-1BB agonism. This indicates that 4-1BB co-signaling plays a predominant role for induction of robust antitumor T-cell immunity against cervical neoplasia (Bartkowiak et al. 2015).
The cytoplasmic tail of 4-1BB has been utilized for a critical component of the chimeric antigen receptors (CARs) for adoptive T-cell therapy against B-cell leukemia, lymphoma, and myeloma. A T cell transduced to express a CAR that comprises of an extracellular tumor antigen-binding single-chain antibody fragment and intracellular 4-1BB and TCR CD3ζ signaling domains exhibits a potent cytotoxic activity after recognition of target antigens on the surface of tumor cells. This 4-1BB-CAR, but not CD28-CAR, ameliorates T-cell exhaustion or anergy that is induced by persistent activation of the CD3ζ domain (Long et al. 2015). After recognizing target antigens, human CD8+ T cells expressing 4-1BB-CAR display a phenotype with CD45RO+ CCR7+ central memory T cells that have an enhanced respiratory capacity, increased fatty acid oxidation, and increased mitochondrial biogenesis. In contrast, CD28-CAR promotes the induction of CD45RO+ CCR7− effector memory T cells with an enhanced aerobic glycolysis (Kawalekar et al. 2016). These studies demonstrate that the 4-1BB signaling domain is superior over the CD28 signaling domain in terms of inducing beneficial T-cell signaling activity and suggest that 4-1BB-CAR promotes a better T-cell response that is required for tumor regression.
3.3 CD70–CD27
3.3.1 Expression and Function
Unlike OX40 and 4-1BB, CD27 is constitutively expressed on naïve CD4+ and CD8+ T cells and Treg cells. CD70, the ligand for CD27, is induced on activated DCs and B cells, and signals from TLRs, CD40, and BCR enhance the expression of CD70. Activated T cells also express CD70. Mice deficient in Cd27 or Cd70 show normal development of lymphoid organs and lymphocytes. The CD27–CD70 interaction promotes the expansion of antigen-specific effector/memory CD4+ and CD8+ T cells, which contributes to the establishment of T-cell immunity. Upon binding with CD70, CD27 recruits TRAF2 and TRAF5 to activate NF-κB and MAPK pathways (Nolte et al. 2009; Bullock 2017) (Table 3.1, Figs. 3.1 and 3.2).
3.3.2 Protective Immunity
A population of APCs exclusively localized in the gut lamina propria expresses higher levels of CD70. This CD70+ APC population provides a critical CD27 co-signaling into T cells, which supports proliferation and differentiation of gut mucosal T cells after oral Listeria monocytogenes infection (Laouar et al. 2005).
Optimal CD27 co-signaling plays an important role for protective T-cell immunity against infections. Critical roles for CD27 co-signaling in pathogen clearance have been shown in murine infection models including influenza virus, LCMV, and CMV. Cd27 −/− mice display impaired primary CD4+ and CD8+ T-cell responses to influenza virus, and a memory T-cell response to a secondary challenge with influenza is also greatly attenuated (Hendriks et al. 2000). Mice deficient in Cd70 or injected with an anti-CD70 blocking mAb display diminished primary effector CD8+ T-cell responses to acute LCMV infection and delayed virus clearance (Penaloza-MacMaster et al. 2011; Munitic et al. 2013). By contrast, the prolonged and excessive CD27–CD70 interactions with higher antigenic load during chronic virus infection induce pathological cytokine responses and immunopathology, which promotes activation-induced T-cell death and limits viral clearance. Blockade of this adverse signaling can restore protective CD8+ T-cell responses (Penaloza-MacMaster et al. 2011; Wensveen et al. 2012; Clouthier and Watts 2015). These studies suggest that an optimal level of CD27 co-signaling is required for the differentiation of effector/memory T cells that are important for pathogen clearance.
Loss of function of CD27 or CD70 in humans is associated with higher susceptibility to EBV infection and EBV-related diseases. Homozygous mutations in CD70 in patients abolish surface expression of CD70 on B cells or binding to its cognate receptor CD27 on T cells, which results in impaired T-cell proliferation, cytotoxic responses, and IFN-γ production toward CD70-negative EBV-infected B cells (Izawa et al. 2017; Abolhassani et al. 2017). These studies suggest that CD70–CD27 interactions are important for generating stable T-cell immunity against EBV.
3.3.3 Autoimmunity and Inflammation
CD27 co-signaling promotes intestinal inflammation mediated by CD4+ T cells. Adoptive transfer of CD45RBhigh CD4+ T cells into lymphocyte-deficient Rag −/− recipient mice leads to weight loss, diarrhea, and severe colitis. In this T-cell-dependent murine colitis model, either deficiency of Cd27 in donor CD4+ T cells or administration of a blocking mAb to CD70 into recipient mice prevents the development of colitis and suppresses the differentiation of effector CD4+ T cells producing pro-inflammatory cytokines. CD70 blockade also suppresses Th1 cell-driven trinitrobenzene sulfonic acid (TNBS)-induced colitis, indicating that CD27–CD70 interactions enhance the accumulation of pathogenic T cells in the gut mucosa and play an important role for development of T-cell-driven colitis (Manocha et al. 2009).
CD27–CD70 interactions facilitate allograft rejection mediated by CD8+ T cells. In a murine fully mismatched cardiac allograft model, CD70 blockade inhibits the expansion of alloreactive effector/memory CD8+ T cells and prevents CD8+ T cell-driven allograft rejection. Cardiac allografts can survive longer in Cd28 −/− recipient mice, and this allograft survival is further prolonged in the presence of CD70 blockade, indicating that CD27 co-signaling plays a dominant role for the development of alloimmune responses even in the absence of CD28. Adoptive transfer of allograft-specific memory CD8+ T cells into syngeneic recipient mice lacking secondary lymphoid organs induces rapid rejection of cardiac allografts, and CD70 blockade inhibits this memory recall response. This demonstrates that the CD27–CD70 pathway promotes the development of acute and chronic allograft rejection mediated by alloreactive effector/memory CD8+ T cells (Yamada et al. 2005).
3.3.4 Cancer
Enhancing CD27 signaling via administration of CD27 agonists, transgenic expression of CD70 on APCs, or enforced expression of CD70 on tumor cells is effective for evoking and augmenting antitumor immunity (Bullock 2017).
Ligation of CD27 in combination with PD-1 blockade is effective at eradicating tumor cells expressing HPV antigens. CD4+ T-cell-mediated help is critical for inducing optimal CD8+ T-cell responses against HPV antigens, and CD70 blockade abrogates this helper activity and abolishes the therapeutic effect of tumor vaccination. Contrary to this, CD27 agonism mimics this help and enhances antitumor responses. Although in the absence of help from CD4+ T cells, PD-1 blockade alone cannot improve tumor control, a combination of PD-1 blockade and CD27 agonism augments the therapeutic efficacy of vaccination. Thus, CD27 agonism provides a potent help to the endogenous T-cell immunity against tumor and enhances antitumor immunity either alone or in combination with PD-1 blockade (Ahrends et al. 2016).
Human T cells expressing a tumor antigen-specific CAR, which contains an intracellular TCR CD3ζ and a CD27 signaling domain, produce higher amounts of IFN-γ and exhibit increased cytotoxicity against tumors in vitro. Cognate recognition of tumor antigens supports the expansion of CD27–CAR-expressing T cells in vivo, and adoptive transfer of CD27–CAR T cells into highly immunodeficient mice that have been inoculated with human ovarian cancer cells expressing a specific antigen leads to increased regression of established tumors in recipient mice. This indicates that human T cells bearing CD27 costimulatory module in a CAR can exert enhanced antigen-specific CTL activity toward tumor cells (Song et al. 2012).
3.4 TL1A-DR3
3.4.1 Expression and Function
DR3 is constitutively expressed by naïve or resting CD4+ and CD8+ T cells, and its expression is upregulated following T-cell activation. DR3 is also expressed by Treg cells. TL1A, the ligand for DR3, is expressed on activated T cells and transiently induced on DCs and macrophages by pro-inflammatory stimuli, such as TLR and FcγR signaling. In humans, DcR3 binds to TL1A and inhibits the interaction between DR3 and TL1A. Upon binding to TL1A, DR3 provides costimulatory signals to T cells in concert with TCR signaling, which enhances pro-inflammatory cytokine production and promotes the clonal expansion and differentiation of effector T cells. Although Dr3 −/− mice show a partial impairment in the negative selection of thymocytes, mice deficient in Dr3 or Tl1a show normal development of lymphoid organs and lymphocytes. After interaction with TL1A, DR3 directly binds to TRADD. TRADD then recruits TRAF2 and RIP1 to the DR3 signaling complex and activates NF-κB and MAPK signaling pathways (Meylan et al. 2011; Pobezinskaya et al. 2011) (Table 3.1, Figs. 3.1 and 3.2).
3.4.2 Protective Immunity
DR3 co-signaling is critical for optimal expansion of IFN-γ producing CD4+ T cells that facilitate killing of intracellular bacteria. Infection of mice with Salmonella enterica Typhimurium induces sustained expression of TL1A on F4/80+ macrophages, and TL1A–DR3 interactions expand IFN-γ-producing Th1 cells, which leads to efficient clearance of S. enterica Typhimurium. Clonal expansion of Dr3 −/-CD4+ T cells is significantly impaired, and this reduced T-cell response results in compromised control of the bacterial burden in the spleens of Dr3 −/− mice (Buchan et al. 2012).
DR3 co-signaling is critical for inducing antiviral immunity against murine CMV and vaccinia virus. Dr3 −/− mice cannot mount effective antiviral CD4+ and CD8+ T-cell immunity during acute virus infection, which is associated with impaired control of virus replication and increased morbidity and mortality. The impaired T-cell response in Dr3 −/−mice is caused by defects in the capacity of CD4+ and CD8+ T cells to divide and produce IFN-γ in response to cognate viral antigens (Twohig et al. 2012).
3.4.3 Autoimmunity and Inflammation
TL1A–DR3 interactions enhance immunopathology in a number of T-cell-dependent animal models of multiple sclerosis, rheumatoid arthritis, inflammatory bowel disease, and allergic lung diseases (Richard et al. 2015a; Meylan et al. 2011). Indeed, increased expression of both TL1A and DR3 is observed in patients with ulcerative colitis and Crohn’s disease, and TL1A is one of the definitive susceptible genes to Crohn’s disease in humans (Strober and Fuss 2011) (Table 3.2).
DR3 co-signaling in CD4+ T cells exacerbates inflammatory responses in the target organs of autoimmune and inflammatory diseases. Although CD4+ T cells from the spleen and lymph nodes of antigen-immunized Dr3 −/− mice proliferate normally in response to recall antigen stimulation in vitro, Dr3 −/− mice display reduced inflammation in experimental autoimmune encephalomyelitis (EAE) and allergic airway inflammation with decreased effector CD4+ T-cell accumulation in the local tissues (Meylan et al. 2008).
TL1A expression in DCs supports the expansion and differentiation of inflammatory IL-17-producing helper T cells (Th17 cells), and thus Tl1a −/− mice show reduced clinical severity in EAE that is dependent on autoimmune Th17 cells (Pappu et al. 2008).
TL1A promotes the differentiation of IL-9-producing helper T cells (Th9 cells) by augmenting signals through DR3 on CD4+ T cells, and endogenous TL1A enhances allergic pathology mediated by Th9 cells in murine models of experimental eye inflammation and allergic airway disease (Richard et al. 2015b).
3.4.4 Cancer
DR3 co-signaling augments antitumor CD8+ T-cell immunity. Engagement of DR3 with soluble TL1A enhances both primary and secondary expansion of antigen-specific CD8+ T cells in vivo. Mice inoculated with TL1A-expressing tumor cells generate protective antitumor CD8+ CTL responses and effectively eradicate the tumor cells in a CD8+ T-cell-dependent manner (Slebioda et al. 2011).
3.5 CD30L–CD30
3.5.1 Expression and Function
CD30 is expressed by activated CD4+ and CD8+ T cells and Treg cells. CD30 is also well recognized as a marker for malignant tumors including Hodgkin’s lymphoma and anaplastic large cell lymphoma. CD30L is induced on activated T cells and professional APCs. CD30–CD30L interactions promote the expansion and survival of effector and memory T cells. Cd30 −/− mice have no obvious defects in peripheral T-cell or B-cell lineages. The phenotype of immune homeostasis of Cd30l −/− mice has not been described so far. CD30 utilizes TRAF2 and TRAF3 to activate NF-κB and MAPK pathways (Watts 2005; Ward-Kavanagh et al. 2016) (Table 3.1, Figs. 3.1 and 3.2).
3.5.2 Protective Immunity
CD30–CD30L interactions establish optimal T-cell immunity against Mycobacterium avium. During infection with M. avium, CD30L blockade leads to increased mycobacterial burdens. Cd30 −/− mice display higher susceptibility to M. avium infection, and the defective antibacterial response is associated with a decreased expansion of IFN-γ-producing CD4+ T cells specific for bacterial antigens (Florido et al. 2004). Cd30l −/− mice are susceptible to Mycobacterium bovis Bacillus Calmette–Guérin (BCG) infection and exhibit higher bacterial burden. The numbers of antigen-specific IFN-γ-producing CD4+ T cells in the spleen, lung, and peritoneal cavity of Cd30l −/− mice are greatly diminished after BCG infection (Tang et al. 2008).
CD30 signaling promotes the differentiation of memory CD8+ T cells and is required for protective immunity against Listeria monocytogenes. Following L. monocytogenes infection, Cd30l −/− mice can generate a normal antigen-specific effector CD8+ T-cell response at an early stage of infection but display a defective recall memory CD8+ T-cell response against reinfection (Nishimura et al. 2005).
Double knockout mice deficient in both Cd30 and Ox40 exhibit defective Th1 immunity against Salmonella typhimurium. Antigen-specific Cd30 −/−Ox40 −/− donor CD4+ T cells fail to persist after transfer into infected Rag −/− recipient mice, and these recipient mice exhibit an impaired capacity to control S. typhimurium infection, indicating that both CD30 and OX40 signals promote Th1 immunity against Salmonella (Gaspal et al. 2008).
3.5.3 Autoimmunity and Inflammation
The CD30–CD30L interaction augments allergic airway inflammation mediated by T-helper-2 (Th2) cells. Cd30 −/− or Cd30l −/− mice primed with ovalbumin (OVA) antigen and challenged with OVA display diminished eosinophilic infiltration into the airway and pulmonary inflammation. In these mice, the levels of pro-inflammatory cytokines IL-5 and IL-13 in bronchoalveolar lavage fluids (BALF) are reduced, and lung-draining lymph node CD4+ T cells produce lesser amount of IL-5 and IL-13 in response to OVA in vitro. Thus, CD30 signaling contributes to allergic lung inflammation through accumulation of pathogenic effector/memory Th2 cells during the course of airway inflammation (Polte et al. 2006; Nam et al. 2008; Fuchiwaki et al. 2011).
CD30 signaling in CD4+ T cells enhances the development of pathogenic IL-17- and/or IFN-γ-producing CD4+ T cells in autoimmune neuroinflammation. EAE disease is ameliorated in Cd30 −/− and Cd30l −/− mice. CD4+ T cells from draining lymph node of Cd30 −/− or Cd30l −/− mice exhibit reduced proliferative and cytokine responses to recall antigen in vitro. Infiltration of inflammatory cells including CD4+ T cell, macrophage/microglia, and granulocyte in the spinal cords is significantly attenuated in these knockout mice. CD30 blockade in the course of disease development ameliorates EAE in wild-type mice. Accordingly, adoptive transfer of antigen-specific wild-type CD4+ T cells into Cd30l −/− mice induces significantly attenuated EAE (Shinoda et al. 2015).
Signals through both CD30 and OX40 promote autoimmune tissue damage mediated by effector CD4+ T cells in the context of Foxp3 deficiency. Although Foxp3 −/− mice develop lethal autoimmune disease, mice with combined deficiency in Foxp3, Cd30, and Ox40 develop and grow normally. Pathogenic CD62LlowCD44highCD4+ effector/memory T cells, which reside in Foxp3 −/− mice and secrete higher amounts of IL-4 and IFN-γ, are substantially decreased in Foxp3 −/−Cd30 −/−Ox40 −/− mice. Accordingly, blockade of both CD30 and OX40 signaling can prevent the development of lethal autoimmune responses that are mediated by autoreactive T cells existing in Foxp3 −/− mice (Gaspal et al. 2011).
3.6 GITRL–GITR
3.6.1 Expression and Function
GITR is expressed on naïve or resting CD4+ and CD8+ T cells at basal levels and is upregulated after T-cell activation. GITR is highly expressed by Treg cells. GITRL is expressed at low levels on APCs and is transiently upregulated after cell activation. GITR provides costimulatory signals to CD4+ and CD8+ T cells to enhance proliferation, effector function, and cell survival. Gitr −/− mice show normal development of lymphoid organs and homeostasis of T cells. A study regarding Gitrl −/− mice has not been reported so far. GITR interacts with TRAF2 and TRAF5 and activates NF-κB and MAPK pathways (Snell et al. 2011; Clouthier and Watts 2014) (Table 3.1, Figs. 3.1 and 3.2).
GITR co-signaling plays critical roles in both conventional CD4+ and CD8+ T cells and Treg cells, and the effect of GITR co-signaling on conventional T cells versus Treg cells depends on the context of the immune response (see Sect. 3.9).
3.6.2 Protective Immunity
GITR co-signaling plays a critical role in control of virus infection. GITR is required for primary and recall CD8+ T-cell responses and for survival of antigen-specific CD8+ T cells during viral infection, and GITR signaling protects mice from death during severe respiratory influenza infection (Snell et al. 2010).
T-cell-intrinsic GITR co-signaling increases the frequency and number of LCMV-specific CD8+ T cells, which results in decreased viral load. GITRL is transiently induced on APCs at early time points of LCMV infection and is downregulated to below baseline levels thereafter. GITR is also transiently upregulated on CD8+ T cells but is sustained at low but above baseline levels at chronic stages of LCMV infection. Thus, GITR on T cells is not efficiently engaged by endogenously expressed GITRL on APCs at the chronic stage of infection. However, an agonistic mAb to GITR can overcome the insufficiency of GITRL and activates LCMV-specific CD8+ T cells, which leads to lower viral load without causing overt immune pathology (Clouthier et al. 2014).
GITR signaling in CD4+ T cells is required for antiviral CD8+ T-cell responses and humoral immunity that are important for control of chronic LCMV infection. Gitr −/− mice display impaired accumulation of IL-2+ IFN-γ+ Th1 cells as well as Tfh cells and have decreased IgG responses to LCMV. CD8+ T cells from Gitr −/− mice express higher levels of exhaustion markers PD-1 and Tim-3. GITR-mediated priming of Th1 cells promotes cell-mediated immunity as well as humoral immunity to optimally regulate chronic LCMV infection (Clouthier et al. 2015).
3.6.3 Autoimmunity and Inflammation
GITR agonism exacerbates CD4+ T-cell-dependent murine models of autoimmune/inflammatory diseases, such as asthma, collagen-induced arthritis (CIA), diabetes, and EAE. Treatment of mice with an agonistic mAb to GITR promotes migration, proliferation, and activation of diabetogenic T cells within the pancreatic islets and exacerbates T-cell-driven destructive insulitis in nonobese diabetic (NOD) mice (You et al. 2009).
Gitr −/− mice develop significantly attenuated CIA. Draining lymph node CD4+ T cells from type II collagen (CII)-immunized Gitr −/− mice secrete lower amounts of IFN-γ in response to CII in vitro. Donor splenic T cells from CII-immunized Gitr −/−mice fail to induce sufficient disease symptoms of CIA in severe combined immunodeficient (SCID) recipient mice, suggesting that GITR signaling is required for CD4+ T cells to attain full pathogenic potential to promote CIA (Cuzzocrea et al. 2005).
3.6.4 Cancer
GITR signaling boosts antitumor immunity by enhancing effector function of tumor antigen-specific T cells (Schaer et al. 2012).
Although either GITR agonism or PD-1 blockade alone exhibits little antitumor effect, a combination of GITR agonism and PD-1 blockade enhances a potent antitumor immunity against ovarian cancer. Anti-GITR/PD-1 mAbs increase the frequency of IFN-γ-producing CD4+ and CD8+ T cells with cytotoxic activity against tumors. Combined treatment of anti-GITR/PD-1 mAbs and chemotherapeutic drugs further enhances the antitumor responses (Lu et al. 2014). Treatment of mice bearing B16 melanoma with anti-GITR/PD-1 mAbs in combination with tumor antigen vaccination leads to markedly better inhibition of tumor growth and prolonged mice survival. The tumor regression correlates with the induction of tumor-infiltrating antigen-specific effector/memory CD8+ T cells producing IFN-γ and TNF-α, and depletion of these CD8+ T cells abrogates the beneficial effects provided by the therapy (Villarreal et al. 2017).
Anti-GITR agonist facilitates antitumor immunity by promoting the differentiation of IL-9-producing Th9 cells. Administration of anti-GITR mAb into CT26 colon tumor- or B16F10 melanoma-bearing mice inhibits growth of tumors, which is mediated by GITR signal-driven differentiation of Th9 cells. Neutralization of IL-9 prevents the tumor regression, and IL-9 from Th9 cells promotes the development of tumor antigen-specific cytotoxic CD8+ T cells through activation of tumor-associated DCs (Kim et al. 2015).
3.7 TNFα-TNFR2
3.7.1 Expression and Function
A low level of TNFR2 is expressed by resting or naïve CD4+ and CD8+ T cells, and its expression is further upregulated after T-cell activation. TNFR2 binds to cognate ligands TNF-α and LT-α (lymphotoxin-α). TNF-α is produced by activated macrophages, T cells, and many other cell types during inflammation and exists as a transmembrane trimer whose proteolysis by TNF-converting enzyme (TACE or ADAM17) leads to a soluble form. LT-α is produced as a soluble form. TNFR2 is more efficiently engaged by transmembrane TNF-α than by soluble TNF-α. Interaction of TNF-α with TNFR2 is costimulatory to TCR-mediated T-cell activation and promotes the activation, differentiation, and survival of T cells. Tnfr2 −/− mice show normal development of peripheral lymphoid organs and lymphocytes. Unlike TNFR1, TNFR2 lacks an intracellular DD and directly recruits TRAF1, TRAF2, and TRAF3 to activate NF-κB and MAPK pathways (Kim et al. 2006; Calzascia et al. 2007; Faustman and Davis 2010; Mehta et al. 2016) (Table 3.1, Figs. 3.1 and 3.2).
Mutations in TNFR2 that lead to enhanced NF-κB signaling have been found in patients with T-cell lymphoma (Ungewickell et al. 2015).
TNFR2 is expressed on Treg cells. Similar to other TNFRSF molecules, such as GITR and OX40, the effect of TNF-α on conventional CD4+ and CD8+ T cells versus Treg cells depends on the context of inflammatory environments (see Sect. 3.9).
Although the TNF-α-TNFR2 interaction provides costimulatory signals into T cells, signals from TNFR2 limit activity of effector CD8+ T cells in some contexts (Wortzman et al. 2013b; Punit et al. 2015).
3.7.2 Protective Immunity
TNF-α-TNFR2 interactions are critical for generating cytotoxic CD8+ T-cell responses against adenovirus in the liver. Intrahepatic lymphocytes isolated from adenovirus-infected Tnfa −/− or Tnfr2 −/− mice display decreased CTL responses against antigen-expressing target hepatocytes (Kafrouni et al. 2003).
TNFR2 signaling plays an important role for T-cell-mediated immunity against Listeria monocytogenes. After L. monocytogenes infection, Tnfr2 −/− mice display reduced expansion and survival of antigen-specific CD4+ and CD8+ T cells producing IFN-γ and delayed bacterial clearance upon challenge with higher dose of bacteria. Antigen-specific donor Tnfr2 −/− CD8+ T cells display a marked reduction in clonal expansion and survival in infected recipient mice (Kim et al. 2006).
3.7.3 Autoimmunity and Inflammation
In a model of murine GVHD, TNFR2 signaling in both donor CD4+ and CD8+ T cells is required for induction of acute GVHD responses mediated by alloantigen-specific CD8+ CTL. Recipient mice transferred with donor Tnfr2 −/−T cells exhibit a reduced cytotoxic phenotype and a decreased elimination of host spleen cell populations mediated by allo-specific donor CD8+ T cells. Whereas TNFR2 signaling in donor CD4+ T cells is critical for their gaining of optimal helper activity for donor CD8+ T cells, TNFR2 signaling in donor CD8+ T cells promotes the maturation of fully competent KLRG1+ CCR7− CD8+ T cells, termed short-lived effector cells (SLECs). This indicates that induction of optimal donor CD8+ CTL activity requires TNFR2 signaling in both donor CD4+ and CD8+ T-cell populations (Soloviova et al. 2013).
TNF-α blockers are well established for treatment of human inflammatory diseases, such as rheumatoid arthritis and Crohn’s disease. Although T cells might not be the main target cells in the therapy, blockade of TNF-α-TNFR2 interactions promotes apoptosis of mucosal CD4+ T cells from patients with inflammatory bowel disease (IBD). CD14+ macrophages and CD4+ T cells isolated from the lamina propria of IBD patients express higher levels of membrane-bound TNF-α (mTNF-α) and TNFR2, respectively. Clinically effective anti-TNF-α mAbs in IBD induce apoptosis of TNFR2+ CD4+ T cells when these T cells are cocultured with mTNF-α+ CD14+ macrophages, suggesting that disruption of mTNF-α-TNFR2 interactions with anti-TNF-α leads to suppression of gut inflammation in IBD through inducing apoptosis of pathogenic CD4+ T cells in the intestine (Atreya et al. 2011).
TNFR2 signaling in CD4+ T cells expands pathogenic effector T cells that promote colitis in mice. Adoptive transfer of donor naïve CD4+ T cells from Tnfr2 −/− mice fails to induce severe colitis in lymphopenic Rag1 −/− mice. Tnfr2 −/− CD4+ T cells are defective in clonal expansion and differentiation into IFN-γ-producing colitogenic effector T cells in the lymphopenic environment (Chen et al. 2016).
3.8 LIGHT–HVEM
3.8.1 Expression and Function
HVEM, a member of the TNFRSF, binds to four different molecules, TNFSF molecules LIGHT and LT-α and immunoglobulin superfamily molecules BTLA and CD160, in distinct configurations, and these molecular networks activate both inflammatory and anti-inflammatory signaling pathways. Ligation of HVEM on T cells by the canonical TNF-related ligand LIGHT provides costimulatory signals to T cells. HVEM is expressed on naïve or resting CD4+ and CD8+ T cells and Treg cells. LIGHT is expressed on activated lymphoid cells including APC populations and T cells either as a membrane-bound or a soluble form. In human, DcR3 binds to LIGHT and inhibits the interaction between HVEM and LIGHT. HVEM co-signaling promotes the activation, differentiation, and survival of T cells. Hvem −/− and Light −/− mice have no significant abnormalities in the development of lymphoid organs and lymphocytes. HVEM recruits TRAF2 and TRAF3 to activate NF-κB pathway (Ward-Kavanagh et al. 2016) (Table 3.1, Figs. 3.1 and 3.2).
Although ligation of HVEM by BTLA activates pro-survival HVEM signaling pathways in effector and memory T cells after antigen recognition (Steinberg et al. 2013; Flynn et al. 2013; Sakoda et al. 2011), we mainly focus on the canonical HVEM–LIGHT interaction that controls HVEM co-signaling in T cells.
3.8.2 Autoimmunity and Inflammation
HVEM co-signaling promotes the differentiation of pathogenic effector CD4+ T cells that exacerbate experimental autoimmune uveitis (EAU). Pathogenic responses and clinical scores of EAU are significantly decreased in Hvem −/− mice and draining lymph node T cells from Hvem −/− mice display reduced cell proliferation and production of Th1- and Th17-related cytokines in response to antigen restimulation in vitro. Light −/−, Btla −/−, and Light −/-Btla −/− mice also display attenuated EAU disease phenotypes and decreased Th1-/Th17-type responses. A blocking mAb to HVEM that can inhibit both HVEM–LIGHT and HVEM–BTLA interactions ameliorates pathogenic Th1/Th17 responses in EAU (Sakoda et al. 2016).
In a T-cell-dependent allergic lung inflammation model, the HVEM–LIGHT interaction plays a dominant role in the survival of pathogenic memory Th2 cells. After antigen recall challenges, adoptively transferred donor OVA-specific Hvem −/− Th2 cells display reduced accumulation in the airways, lungs, and draining mediastinal lymph nodes of recipient mice and induce decreased airway eosinophilia and Th2 cytokine responses. Interruption of HVEM–LIGHT interactions also inhibits the accumulation of inflammatory memory Th2 cells in the lung. Although Light −/− donor CD4+ T cells cannot sustain after antigen exposure in vivo, cotransfer of wild-type and Light −/−donor T cells rescues the survival defect of Light −/−donor T cells, suggesting that HVEM induces cell survival signals into T cells through interacting with LIGHT expressing on neighboring antigen-specific T cells. This demonstrates that HVEM expressed by CD4+ T cells induces cell survival signals and controls T-cell-driven allergic lung inflammation (Soroosh et al. 2011).
In a T-cell-dependent murine colitis model, HVEM signaling in donor CD4+ T cells promotes intestinal inflammation and contributes to the immunopathology mediated by differentiated colitogenic T cells. Rag −/− recipient mice with donor CD45RBhigh CD4+ T cells from Hvem −/− or Light −/− mice display reduced intestinal inflammation, indicating that both HVEM and LIGHT on CD4+ T cells are required for the development of inflammatory T cells within the intestine during colitis development. Rag −/− recipient mice receiving Hvem −/− CD4+ T cells express lesser amounts of IL-6, TNF-α, and IL-12 mRNAs in the colon and have a decreased number of donor T cells producing IFN-γ or IL-17. In the absence of HVEM signaling, donor CD4+ T cells expand normally at early time points but cannot persist at later time points in lymphopenic hosts. These results suggest that T-cell-expressing LIGHT interacting with HVEM expressed by an adjacent T cell plays a critical role for the expansion, differentiation, and survival of gut-homing pathogenic T cells driving colitis (Schaer et al. 2011; Steinberg et al. 2008).
HVEM–LIGHT interactions contribute to GVHD pathogenesis. Adoptive transfer of allogeneic T cells from Hvem −/− or Light −/− mice into recipient mice induces attenuated anti-host CTL responses, which results in prolonged survival of recipient mice. Hvem −/− and Light −/− donor T cells undergo apoptosis after transfer into recipient mice. Accordingly, administration of an anti-HVEM mAb, which interferes with HVEM–LIGHT interactions, ameliorates GVHD responses and prolongs the survival of recipient mice (Xu et al. 2007).
3.8.3 Cancer
HVEM co-signaling via LIGHT plays an important role for establishing robust T-cell immunity against tumors. Mice inoculated with tumor cells expressing an agonistic mAb to HVEM on the cell surface generate protective antitumor immunity in a manner dependent on both CD4+ and CD8+ T cells. The potent antitumor CTL activity is associated with increased IFN-γ production, and mice which have rejected this tumor are resistant to rechallenge of parental tumors, indicating that HVEM signaling facilitates tumor-reactive T-cell responses, induction of long-term antitumor immunity, and tumor regression (Park et al. 2012).
LIGHT expression in the tumor environment elicits potent antitumor immunity leading to tumor regression (Yu and Fu 2008). Combined immunotherapy with LIGHT expression on tumors and antigen-specific vaccination is effective for generating tumor-infiltrating CD8+ T-cell responses that are important for tumor eradication. Adenovirus-mediated forced expression of LIGHT in HPV16-induced tumors results in upregulation of IFN-γ and chemoattractant cytokines in the tumor, which results in induction of antigen-specific CD8+ T cells in the peripheral lymphoid organs and within the tumor. However, antigen-specific T cells induced by LIGHT cannot induce complete tumor regression. More importantly, additional vaccination with HPV16 antigen boosts the frequency of antigen-specific T cells and prevents the outgrowth of tumors. This suggests that LIGHT expressed by tumors expands incoming T cells via HVEM signaling and that these LIGHT–HVEM interactions in the presence of antigenic signals play an important role for generating robust antitumor immunity that can eradicate tumors (Kanodia et al. 2010).
3.9 The Role of TNFRSF Molecules in Immune Regulation Mediated by Treg Cells
Treg cells play important roles for regulation of conventional CD4+ and CD8+ T-cell responses. TNFRSF molecules described in this chapter are all expressed by both Treg cells and conventional T-cell populations, and the cognate TNFSF–TNFRSF interaction regulates the balance between Treg cells and conventional T cells, which is critical for determining all aspects of the immune response. Although the cell-intrinsic effects of the TNFRSF signaling in Treg cells are still unclear (Shevach and Stephens 2006; So et al. 2008; Croft 2014; Mbanwi and Watts 2014), it has been demonstrated that signals from TNFRSF molecules influence the Treg and conventional T-cell balance through (1) promoting the development of natural or thymus-derived Treg cells, (2) antagonizing the development of induced or periphery-derived Treg cells, (3) promoting the expansion and survival of Treg cells, (4) downregulating Treg cell suppressive functions, and (5) enhancing resistance of naïve/effector/memory responder CD4+ and CD8+ T cells to the Treg cell-mediated suppression.
4 Conclusion
Five out of eight TNFRSF molecules, CD27, DR3, HVEM, GITR, and TNFR2, discussed in this chapter are constitutively expressed on most CD4+ and CD8+ T cells, whereas other three TNFRSF molecules, 4-1BB, CD30, and OX40, are upregulated on activated T cells after antigen recognition. Most of the cognate ligands for these TNFRSF molecules are not highly expressed by APC populations or other cell types and are induced by antigen recognition or innate stimuli or inflammation. The co-signaling activated by the cognate TNFSF–TNFRSF interaction quantitatively and/or qualitatively augments signals that are initiated by the TCR and CD28 and controls not only in early phases of T-cell responses to enhance cell proliferation, differentiation, and survival but also in later phases of memory T-cell responses (Fig. 3.2). Thus, TNFRSF molecules expressed by T cells have central roles in infection, immune-mediated diseases, and cancer that are critically regulated by various populations of antigen-primed T cells. Understanding of co-signaling functions of TNFRSF molecules in health and disease has progressed over the past few decades, and biologics or gene engineering technologies that inhibit or stimulate co-signaling functions of TNFRSF molecules have proven to be clinically efficacious for autoimmune and inflammatory diseases and cancer (Sugamura et al. 2004; Croft et al. 2013; Moran et al. 2013; Ward-Kavanagh et al. 2016). However, there are still fundamental questions regarding signaling mechanisms of the TNF–TNFR family of co-signal molecules: (1) qualitative and/or quantitative contribution of the TNFR co-signaling to the TCR, (2) cross talk between TNFR and co-inhibitory molecules, (3) intrinsic TNFR signaling functions in Treg cells, (4) utilization patterns of individual TRAF molecules in each individual TNFR signaling complex that might explain the qualitative difference in co-signaling activity, (5) cross talk of costimulatory signals among TNFRSF molecules, (6) roles of reverse signaling mediated by membrane-bound TNFSF ligands expressed by T cells, and (7) adverse (death) signaling effects of co-stimulatory TNFRSF molecules expressed by T cells. Further research will uncover these unresolved issues and may provide novel information regarding the potential usefulness of blockade or agonism of the TNFR co-signaling pathways in human diseases (Table 3.2).
Abbreviations
- APC:
-
antigen-presenting cell;
- CAR:
-
chimeric antigen receptor
- CMV:
-
cytomegalovirus
- CTL:
-
cytotoxic T lymphocyte
- CTLA-4:
-
cytotoxic T-lymphocyte-associated protein-4
- DC:
-
dendritic cell
- DcR3:
-
decoy receptor 3
- DR3:
-
death receptor 3
- EAE:
-
experimental autoimmune encephalomyelitis
- EBV:
-
Epstein–Barr virus
- GC:
-
germinal center
- GITR:
-
glucocorticoid-induced TNFR family-related protein
- GVHD:
-
graft-versus-host disease
- HPV:
-
human papillomavirus
- HVEM:
-
herpesvirus entry mediator
- ICOS:
-
inducible T-cell costimulator
- LCMV:
-
lymphocytic choriomeningitis virus
- LIGHT:
-
homologous to lymphotoxins (LTs), inducible expression, which competes with herpes simplex virus glycoprotein D (HSV gD) for HVEM, a receptor expressed on T lymphocytes
- mAb:
-
monoclonal antibody
- MAPK:
-
mitogen-activated protein kinase
- NF-κB:
-
nuclear factor-kappa B
- PD-1:
-
programmed cell death-1
- SLE:
-
systemic lupus erythematosus
- TCR:
-
T-cell receptor
- Tfh:
-
T follicular helper
- Th1:
-
T-helper-1
- Th17:
-
T-helper-17
- Th2:
-
T-helper-2
- Th9:
-
T-helper-9
- TL1A:
-
TNF-like ligand 1A
- TLR:
-
Toll-like receptor
- TNF:
-
tumor necrosis factor
- TNFR2:
-
tumor necrosis factor receptor 2
- TNFRSF:
-
TNF receptor superfamily
- TNFSF:
-
TNF superfamily
- TRAF:
-
TNF receptor-associated factor
- Treg cells:
-
Foxp3+ CD25+ CD4+ regulatory T cells
References
Abolhassani H, Edwards ES, Ikinciogullari A et al (2017) Combined immunodeficiency and Epstein-Barr virus-induced B cell malignancy in humans with inherited CD70 deficiency. J Exp Med 214:91–106
Aggarwal BB (2003) Signalling pathways of the TNF superfamily: a double-edged sword. Nat Rev Immunol 3:745–756
Ahrends T, Babala N, Xiao Y et al (2016) CD27 Agonism plus PD-1 blockade recapitulates CD4+ T-cell help in therapeutic anticancer vaccination. Cancer Res 76:2921–2931
Atreya R, Zimmer M, Bartsch B et al (2011) Antibodies against tumor necrosis factor (TNF) induce T-cell apoptosis in patients with inflammatory bowel diseases via TNF receptor 2 and intestinal CD14(+) macrophages. Gastroenterology 141:2026–2038
Bacher P, Heinrich F, Stervbo U et al (2016) Regulatory T cell specificity directs tolerance versus allergy against Aeroantigens in humans. Cell 167:1067–1078
Bartkowiak T, Curran MA (2015) 4-1BB agonists: multi-potent Potentiators of tumor immunity. Front Oncol 5:117
Bartkowiak T, Singh S, Yang G et al (2015) Unique potential of 4-1BB agonist antibody to promote durable regression of HPV+ tumors when combined with an E6/E7 peptide vaccine. Proc Natl Acad Sci U S A 112:E5290–E5299
Bodmer JL, Schneider P, Tschopp J (2002) The molecular architecture of the TNF superfamily. Trends Biochem Sci 27:19–26
Brenner D, Blaser H, Mak TW (2015) Regulation of tumour necrosis factor signalling: live or let die. Nat Rev Immunol 15:362–374
Brown GR, Thiele DL (2000) Enhancement of MHC class I-stimulated alloresponses by TNF/TNF receptor (TNFR)1 interactions and of MHC class II-stimulated alloresponses by TNF/TNFR2 interactions. Eur J Immunol 30:2900–2907
Buchan SL, Taraban VY, Slebioda TJ et al (2012) Death receptor 3 is essential for generating optimal protective CD4(+) T-cell immunity against Salmonella. Eur J Immunol 42:580–588
Bullock TN (2017) Stimulating CD27 to quantitatively and qualitatively shape adaptive immunity to cancer. Curr Opin Immunol 45:82–88
Byun M, Ma CS, Akcay A et al (2013) Inherited human OX40 deficiency underlying classic Kaposi sarcoma of childhood. J Exp Med 210:1743–1759
Calzascia T, Pellegrini M, Hall H et al (2007) TNF-alpha is critical for antitumor but not antiviral T cell immunity in mice. J Clin Invest 117:3833–3845
Chen X, Nie Y, Xiao H et al (2016) TNFR2 expression by CD4 effector T cells is required to induce full-fledged experimental colitis. Sci Rep 6:32834
Clouthier DL, Watts TH (2014) Cell-specific and context-dependent effects of GITR in cancer, autoimmunity, and infection. Cytokine Growth Factor Rev 25:91–106
Clouthier DL, Watts TH (2015) TNFRs and control of chronic LCMV infection: implications for therapy. Trends Immunol 36:697–708
Clouthier DL, Zhou AC, Watts TH (2014) Anti-GITR agonist therapy intrinsically enhances CD8 T cell responses to chronic lymphocytic choriomeningitis virus (LCMV), thereby circumventing LCMV-induced downregulation of costimulatory GITR ligand on APC. J Immunol 193:5033–5043
Clouthier DL, Zhou AC, Wortzman ME et al (2015) GITR intrinsically sustains early type 1 and late follicular helper CD4 T cell accumulation to control a chronic viral infection. PLoS Pathog 11:e1004517
Croft M (2009) The role of TNF superfamily members in T-cell function and diseases. Nat Rev Immunol 9:271–285
Croft M (2010) Control of immunity by the TNFR-related molecule OX40 (CD134). Annu Rev Immunol 28:57–78
Croft M (2014) The TNF family in T cell differentiation and function-unanswered questions and future directions. Semin Immunol 26:183–190
Croft M, So T, Duan W et al (2009) The significance of OX40 and OX40L to T-cell biology and immune disease. Immunol Rev 229:173–191
Croft M, Benedict CA, Ware CF (2013) Clinical targeting of the TNF and TNFR superfamilies. Nat Rev Drug Discov 12:147–168
Cuzzocrea S, Ayroldi E, Di Paola R et al (2005) Role of glucocorticoid-induced TNF receptor family gene (GITR) in collagen-induced arthritis. FASEB J 19:1253–1265
Eissner G, Kolch W, Scheurich P (2004) Ligands working as receptors: reverse signaling by members of the TNF superfamily enhance the plasticity of the immune system. Cytokine Growth Factor Rev 15:353–366
Faustman D, Davis M (2010) TNF receptor 2 pathway: drug target for autoimmune diseases. Nat Rev Drug Discov 9:482–493
Florido M, Borges M, Yagita H et al (2004) Contribution of CD30/CD153 but not of CD27/CD70, CD134/OX40L, or CD137/4-1BBL to the optimal induction of protective immunity to Mycobacterium avium. J Leukoc Biol 76:1039–1046
Flynn R, Hutchinson T, Murphy KM et al (2013) CD8 T cell memory to a viral pathogen requires trans Cosignaling between HVEM and BTLA. PLoS One 8:e77991
Fuchiwaki T, Sun X, Fujimura K et al (2011) The central role of CD30L/CD30 interactions in allergic rhinitis pathogenesis in mice. Eur J Immunol 41:2947–2954
Gaspal F, Bekiaris V, Kim MY et al (2008) Critical synergy of CD30 and OX40 signals in CD4 T cell homeostasis and Th1 immunity to Salmonella. J Immunol 180:2824–2829
Gaspal F, Withers D, Saini M et al (2011) Abrogation of CD30 and OX40 signals prevents autoimmune disease in FoxP3-deficient mice. J Exp Med 208:1579–1584
Ha H, Han D, Choi Y (2009) TRAF-mediated TNFR-family signaling. Curr Protoc Immunol Suppl.87:Unit11.9D.1–Unit 11.9D.19
Hayden MS, Ghosh S (2014) Regulation of NF-kappaB by TNF family cytokines. Semin Immunol 26:253–266
Hendriks J, Gravestein LA, Tesselaar K et al (2000) CD27 is required for generation and long-term maintenance of T cell immunity. Nat Immunol 1:433–440
Humphreys IR, de Trez C, Kinkade A et al (2007) Cytomegalovirus exploits IL-10-mediated immune regulation in the salivary glands. J Exp Med 204:1217–1225
Ishii N, Takahashi T, Soroosh P et al (2010) OX40-OX40 ligand interaction in T-cell-mediated immunity and immunopathology. Adv Immunol 105:63–98
Izawa K, Martin E, Soudais C et al (2017) Inherited CD70 deficiency in humans reveals a critical role for the CD70-CD27 pathway in immunity to Epstein-Barr virus infection. J Exp Med 214:73–89
Jacquemin C, Schmitt N, Contin-Bordes C et al (2015) OX40 ligand contributes to human lupus pathogenesis by promoting T follicular helper response. Immunity 42:1159–1170
Kafrouni MI, Brown GR, Thiele DL (2003) The role of TNF-TNFR2 interactions in generation of CTL responses and clearance of hepatic adenovirus infection. J Leukoc Biol 74:564–571
Kanodia S, Da Silva DM, Karamanukyan T et al (2010) Expression of LIGHT/TNFSF14 combined with vaccination against human papillomavirus type 16 E7 induces significant tumor regression. Cancer Res 70:3955–3964
Karin M, Gallagher E (2009) TNFR signaling: ubiquitin-conjugated TRAFfic signals control stop-and-go for MAPK signaling complexes. Immunol Rev 228:225–240
Kawalekar OU, O’Connor RS, Fraietta JA et al (2016) Distinct signaling of coreceptors regulates specific metabolism pathways and impacts memory development in CAR T cells. Immunity 44:380–390
Kim EY, Priatel JJ, Teh SJ et al (2006) TNF receptor type 2 (p75) functions as a costimulator for antigen-driven T cell responses in vivo. J Immunol 176:1026–1035
Kim IK, Kim BS, Koh CH et al (2015) Glucocorticoid-induced tumor necrosis factor receptor-related protein co-stimulation facilitates tumor regression by inducing IL-9-producing helper T cells. Nat Med 21:1010–1017
Kitchens WH, Dong Y, Mathews DV et al (2017) Interruption of OX40L signaling prevents costimulation blockade-resistant allograft rejection. JCI Insight 2:e90317
Laouar A, Haridas V, Vargas D et al (2005) CD70+ antigen-presenting cells control the proliferation and differentiation of T cells in the intestinal mucosa. Nat Immunol 6:698–706
Linch SN, McNamara MJ, Redmond WL (2015) OX40 agonists and combination immunotherapy: putting the pedal to the metal. Front Oncol 5:34
Linch SN, Kasiewicz MJ, McNamara MJ et al (2016) Combination OX40 agonism/CTLA-4 blockade with HER2 vaccination reverses T-cell anergy and promotes survival in tumor-bearing mice. Proc Natl Acad Sci U S A 113:E319–E327
Locksley RM, Killeen N, Lenardo MJ (2001) The TNF and TNF receptor superfamilies: integrating mammalian biology. Cell 104:487–501
Long AH, Haso WM, Shern JF et al (2015) 4-1BB costimulation ameliorates T cell exhaustion induced by tonic signaling of chimeric antigen receptors. Nat Med 21:581–590
Lu L, Xu X, Zhang B et al (2014) Combined PD-1 blockade and GITR triggering induce a potent antitumor immunity in murine cancer models and synergizes with chemotherapeutic drugs. J Transl Med 12:36
Manocha M, Rietdijk S, Laouar A et al (2009) Blocking CD27-CD70 costimulatory pathway suppresses experimental colitis. J Immunol 183:270–276
Mbanwi AN, Watts TH (2014) Costimulatory TNFR family members in control of viral infection: outstanding questions. Semin Immunol 26:210–219
Mehta AK, Gracias DT, Croft M (2016) TNF activity and T cells. Cytokine 101:14–18
Meylan F, Davidson TS, Kahle E et al (2008) The TNF-family receptor DR3 is essential for diverse T cell-mediated inflammatory diseases. Immunity 29:79–89
Meylan F, Richard AC, Siegel RM (2011) TL1A and DR3, a TNF family ligand-receptor pair that promotes lymphocyte costimulation, mucosal hyperplasia, and autoimmune inflammation. Immunol Rev 244:188–196
Moran AE, Kovacsovics-Bankowski M, Weinberg AD (2013) The TNFRs OX40, 4-1BB, and CD40 as targets for cancer immunotherapy. Curr Opin Immunol 25:230–237
Mousavi SF, Soroosh P, Takahashi T et al (2008) OX40 costimulatory signals potentiate the memory commitment of effector CD8+ T cells. J Immunol 181:5990–6001
Munitic I, Kuka M, Allam A et al (2013) CD70 deficiency impairs effector CD8 T cell generation and viral clearance but is dispensable for the recall response to lymphocytic choriomeningitis virus. J Immunol 190:1169–1179
Nam SY, Kim YH, Do JS et al (2008) CD30 supports lung inflammation. Int Immunol 20:177–184
Nishimura H, Yajima T, Muta H et al (2005) A novel role of CD30/CD30 ligand signaling in the generation of long-lived memory CD8+ T cells. J Immunol 175:4627–4634
Nolte MA, van Olffen RW, van Gisbergen KP et al (2009) Timing and tuning of CD27-CD70 interactions: the impact of signal strength in setting the balance between adaptive responses and immunopathology. Immunol Rev 229:216–231
Pappu BP, Borodovsky A, Zheng TS et al (2008) TL1A-DR3 interaction regulates Th17 cell function and Th17-mediated autoimmune disease. J Exp Med 205:1049–1062
Park JJ, Anand S, Zhao Y et al (2012) Expression of anti-HVEM single-chain antibody on tumor cells induces tumor-specific immunity with long-term memory. Cancer Immunol Immunother 61:203–214
Penaloza-MacMaster P, Ur Rasheed A, Iyer SS et al (2011) Opposing effects of CD70 costimulation during acute and chronic lymphocytic choriomeningitis virus infection of mice. J Virol 85:6168–6174
Pobezinskaya YL, Choksi S, Morgan MJ et al (2011) The adaptor protein TRADD is essential for TNF-like ligand 1A/death receptor 3 signaling. J Immunol 186:5212–5216
Polte T, Behrendt AK, Hansen G (2006) Direct evidence for a critical role of CD30 in the development of allergic asthma. J Allergy Clin Immunol 118:942–948
Punit S, Dube PE, Liu CY et al (2015) Tumor necrosis factor receptor 2 restricts the pathogenicity of CD8(+) T cells in mice with colitis. Gastroenterology 149:993–1005
Richard AC, Ferdinand JR, Meylan F et al (2015a) The TNF-family cytokine TL1A: from lymphocyte costimulator to disease co-conspirator. J Leukoc Biol 98:333–345
Richard AC, Tan C, Hawley ET et al (2015b) The TNF-family ligand TL1A and its receptor DR3 promote T cell-mediated allergic immunopathology by enhancing differentiation and pathogenicity of IL-9-producing T cells. J Immunol 194:3567–3582
Sakoda Y, Park JJ, Zhao Y et al (2011) Dichotomous regulation of GVHD through bidirectional functions of the BTLA-HVEM pathway. Blood 117:2506–2514
Sakoda Y, Nagai T, Murata S et al (2016) Pathogenic function of herpesvirus entry mediator in experimental autoimmune uveitis by induction of Th1-and Th17-type T cell responses. J Immunol 196:2947–2954
Salek-Ardakani S, Moutaftsi M, Crotty S et al (2008) OX40 drives protective vaccinia virus-specific CD8 T cells. J Immunol 181:7969–7976
Sanchez-Paulete AR, Labiano S, Rodriguez-Ruiz ME et al (2016) Deciphering CD137 (4-1BB) signaling in T-cell costimulation for translation into successful cancer immunotherapy. Eur J Immunol 46:513–522
Schaer C, Hiltbrunner S, Ernst B et al (2011) HVEM signalling promotes colitis. PLoS One 6:e18495
Schaer DA, Murphy JT, Wolchok JD (2012) Modulation of GITR for cancer immunotherapy. Curr Opin Immunol 24:217–224
Shevach EM, Stephens GL (2006) The GITR-GITRL interaction: co-stimulation or contrasuppression of regulatory activity? Nat Rev Immunol 6:613–618
Shinoda K, Sun X, Oyamada A et al (2015) CD30 ligand is a new therapeutic target for central nervous system autoimmunity. J Autoimmun 57:14–23
Slebioda TJ, Rowley TF, Ferdinand JR et al (2011) Triggering of TNFRSF25 promotes CD8(+) T-cell responses and anti-tumor immunity. Eur J Immunol 41:2606–2611
Snell LM, McPherson AJ, Lin GH et al (2010) CD8 T cell-intrinsic GITR is required for T cell clonal expansion and mouse survival following severe influenza infection. J Immunol 185:7223–7234
Snell LM, Lin GH, McPherson AJ et al (2011) T-cell intrinsic effects of GITR and 4-1BB during viral infection and cancer immunotherapy. Immunol Rev 244:197–217
So T, Croft M (2013) Regulation of PI-3-kinase and Akt signaling in T lymphocytes and other cells by TNFR family molecules. Front Immunol 4:139
So T, Lee SW, Croft M (2006) Tumor necrosis factor/tumor necrosis factor receptor family members that positively regulate immunity. Int J Hematol 83:1–11
So T, Lee SW, Croft M (2008) Immune regulation and control of regulatory T cells by OX40 and 4-1BB. Cytokine Growth Factor Rev 19:253–262
So T, Nagashima H, Ishii N (2015) TNF receptor-associated factor (TRAF) signaling network in CD4(+) T-lymphocytes. Tohoku J Exp Med 236:139–154
Soloviova K, Puliaiev M, Haas M et al (2013) In vivo maturation of Allo-specific CD8 CTL and prevention of lupus-like graft-versus-host disease is critically dependent on T cell signaling through the TNF p75 receptor but not the TNF p55 receptor. J Immunol 190:4562–4572
Song DG, Ye Q, Poussin M et al (2012) CD27 costimulation augments the survival and antitumor activity of redirected human T cells in vivo. Blood 119:696–706
Soroosh P, Doherty TA, So T et al (2011) Herpesvirus entry mediator (TNFRSF14) regulates the persistence of T helper memory cell populations. J Exp Med 208:797–809
Steinberg MW, Turovskaya O, Shaikh RB et al (2008) A crucial role for HVEM and BTLA in preventing intestinal inflammation. J Exp Med 205:1463–1476
Steinberg MW, Huang YJ, Wang-Zhu Y et al (2013) BTLA interaction with HVEM expressed on CD8(+) T cells promotes survival and memory generation in response to a bacterial infection. PLoS One 8:e77992
Strober W, Fuss IJ (2011) Proinflammatory cytokines in the pathogenesis of inflammatory bowel diseases. Gastroenterology 140:1756–1767
Sugamura K, Ishii N, Weinberg AD (2004) Therapeutic targeting of the effector T-cell co-stimulatory molecule OX40. Nat Rev Immunol 4:420–431
Sun M, Fink PJ (2007) A new class of reverse signaling costimulators belongs to the TNF family. J Immunol 179:4307–4312
Tahiliani V, Hutchinson TE, Abboud G et al (2017) OX40 cooperates with ICOS to amplify follicular Th cell development and germinal center reactions during infection. J Immunol 198:218–228
Tang C, Yamada H, Shibata K et al (2008) A novel role of CD30L/CD30 signaling by T-T cell interaction in Th1 response against mycobacterial infection. J Immunol 181:6316–6327
Twohig JP, Marsden M, Cuff SM et al (2012) The death receptor 3/TL1A pathway is essential for efficient development of antiviral CD4(+) and CD8(+) T-cell immunity. FASEB J 26:3575–3586
Ungewickell A, Bhaduri A, Rios E et al (2015) Genomic analysis of mycosis fungoides and Sezary syndrome identifies recurrent alterations in TNFR2. Nat Genet 47:1056–1060
Villarreal DO, Chin D, Smith MA et al (2017) Combination GITR targeting/PD-1 blockade with vaccination drives robust antigen-specific antitumor immunity. Oncotarget 8:39117–39130
Vinay DS, Kwon BS (2014) 4-1BB (CD137), an inducible costimulatory receptor, as a specific target for cancer therapy. BMB Rep 47:122–129
Ward-Kavanagh LK, Lin WW, Sedy JR et al (2016) The TNF receptor superfamily in co-stimulating and co-inhibitory responses. Immunity 44:1005–1019
Watts TH (2005) TNF/TNFR family members in costimulation of T cell responses. Annu Rev Immunol 23:23–68
Wensveen FM, Unger PP, Kragten NA et al (2012) CD70-driven costimulation induces survival or Fas-mediated apoptosis of T cells depending on antigenic load. J Immunol 188:4256–4267
Wortzman ME, Clouthier DL, McPherson AJ et al (2013a) The contextual role of TNFR family members in CD8(+) T-cell control of viral infections. Immunol Rev 255:125–148
Wortzman ME, Lin GH, Watts TH (2013b) Intrinsic TNF/TNFR2 interactions fine-tune the CD8 T cell response to respiratory influenza virus infection in mice. PLoS One 8:e68911
Xu Y, Flies AS, Flies DB et al (2007) Selective targeting of the LIGHT-HVEM costimulatory system for the treatment of graft-versus-host disease. Blood 109:4097–4104
Yamada A, Salama AD, Sho M et al (2005) CD70 signaling is critical for CD28-independent CD8+ T cell-mediated alloimmune responses in vivo. J Immunol 174:1357–1364
You S, Poulton L, Cobbold S et al (2009) Key role of the GITR/GITRLigand pathway in the development of murine autoimmune diabetes: a potential therapeutic target. PLoS One 4:e7848
Yu P, Fu YX (2008) Targeting tumors with LIGHT to generate metastasis-clearing immunity. Cytokine Growth Factor Rev 19:285–294
Zander RA, Obeng-Adjei N, Guthmiller JJ et al (2015) PD-1 co-inhibitory and OX40 co-stimulatory crosstalk regulates helper T cell differentiation and anti-plasmodium humoral immunity. Cell Host Microbe 17:628–641
Acknowledgments
This work was supported by JSPS KAKENHI Grant Numbers 24590571 (to T.S.), 15H04640 (to T.S.), 18H02572 (to T.S.), 24390118 (to N.I.), 15H04742 (to N.I.), and 16K15508 (to N.I.), as well as by grants from the Takeda Science Foundation (to T.S.), the Suzuken Memorial Foundation (to T.S.), the SENSHIN Medical Research Foundation (to T.S.), the Astellas Foundation for Research on Metabolic Disorders (to T.S.), the Yamaguchi Educational and Scholarship Foundation (to T.S.), and the Daiichi-Sankyo Foundation of Life Science (to N.I. and T.S.).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
So, T., Ishii, N. (2019). The TNF–TNFR Family of Co-signal Molecules. In: Azuma, M., Yagita, H. (eds) Co-signal Molecules in T Cell Activation. Advances in Experimental Medicine and Biology, vol 1189. Springer, Singapore. https://doi.org/10.1007/978-981-32-9717-3_3
Download citation
DOI: https://doi.org/10.1007/978-981-32-9717-3_3
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-32-9716-6
Online ISBN: 978-981-32-9717-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)