Abstract
The kidney is a main target for drug-and chemical-induced toxicity, and the renal proximal tubule is frequently affected. Many widely-prescribed drugs are nephrotoxic. Reliable renal proximal tubular cell (PTC) models are needed for developing improved in vitro assays for nephrotoxicity prediction. PTC in the human kidney express various transporters for drugs and chemicals, which are often down-regulated in vitro. This renders the cells inactive to nephrotoxicants, which is a main problem in nephrotoxicity testing. Here, I addressed organic anion uptake by three different PTC models: conditionally immortalised proximal tubular epithelial cells (ciPTEC) stably transfected with OAT1 and OAT3 expression constructs (ciPTEC-OAT1 and ciPTEC-OAT3) and human-induced pluripotent stem cell (iPSC)-derived PTC-like cells. In addition, the activity of the renal organic anion transporters OAT1 and OAT3 was assessed. These transporters are important for the cellular uptake of a wide range of nephrotoxicants. The results showed that the cell culture medium has a major impact on organic anion uptake. A proprietary novel medium for PTC-like cells was formulated (Renal Tox Medium) that sustained high organic anion uptake in vitro. Furthermore, the results showed that OAT1 and/or OAT3 activity in PTC-like cells was superior compared to ciPTEC-OAT1 and ciPTEC-OAT3 cells, which are currently the PTC models favoured by the pharmaceutical industry. The results also showed that ciPTEC cell lines consisted of inhomogeneous cell populations. Together, the results suggest that PTC-like cells, in combination with the here developed proprietary Renal Tox Medium, could provide a more suitable solution for industry and academia.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
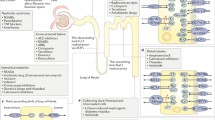
The kidney plays a key role in eliminating drugs and other chemicals from the body and is a main target for chemical-induced toxicity. A major site of damage is the renal proximal tubule, as all compounds are heavily concentrated here due to water reabsorption [1], and the proximal tubular cells (PTC) are very active in the transport, reabsorption and elimination of drugs and other chemicals from the body [2, 3]. Widely-prescribed drugs like antibiotics and immunosuppressants are often nephrotoxic [3, 4] and are the root cause of ~20% of hospital and community acquired cases of acute kidney injury [5,6,7]. Hence, nephrotoxicity assays with improved predictivity would be required for drug development and other applications, and reliable PTC models are needed for such in vitro assays [3, 8,9,10,11]. It is crucial for the respective PTC models to express renal transporters for drugs and other chemicals. Such transporters are often down-regulated in vitro [3, 12,13,14]. This impairs the uptake of drugs and chemicals and renders the cells insensitive to potential nephrotoxicants [14,15,16].
At the basolateral membrane of the PTC in the kidney, organic anion transporters OAT1 (solute carrier family 22 member 6; SLC22A6), OAT3 (SLC22A8) and organic cation transporter OCT2 (SLC22A2) are key transporters which mediate the uptake of anionic and cationic drugs and chemicals from the blood [17,18,19,20]. In the case of human conditionally immortalized proximal tubular epithelial cells (ciPTEC) [21], the problem of transporter downregulation in vitro was addressed by stably transfecting the cells with OAT1 and OAT3 expression constructs. The resulting cell lines are ciPTEC-OAT1 and ciPTEC-OAT3 [22]. These PTC models are currently preferred by pharmaceutical companies such as AstraZeneca and GlaxoSmithKline due to their presumably high OAT1 and 3 activity [10, 23]. Stem cell-based approaches probably also offer a solution to the problems with current renal cell models. Recently, Kandasamy et al. [12] published a simple 1-step protocol for the differentiation of human-induced pluripotent stem cells (iPSC) into PTC-like cells. These cells resemble human primary renal PTC, but larger cell numbers can be more easily obtained [12]. My mentors observed that PTC-like cells had issues with OAT1 and 3 activity (unpublished results), which was probably due to the cell culture media used.
The main goal of this study was to compare the OAT1 and OAT3 activities of three different cell types: ciPTEC-OAT1, ciPTEC-OAT3, and iPSC-derived PTC-like cells. Another goal was to identify cell culture media which sustained high OAT1 and 3 activities in vitro.
2 Materials and Methods
2.1 Cell Culture
Undifferentiated is070a iPSCs were obtained from Dr. Adrian Teo, IMCB, A*STAR and were differentiated into PTC-like cells. ciPTEC-OAT1 and ciPTEC-OAT3 cell lines (Accellerate, Hamburg, Germany) were cultivated according to the manufacturer’s protocol in Assay Medium (AM) provided by the manufacturer. Details about cell cultivation and differentiation are outlined in Sect. 5.
2.2 Determination of 6-carboxyfluorescein (6-CF) Uptake in Various Media
Cellular uptake of the fluorescent organic anion 6-CF was studied in complete medium, assay medium and Renal Tox Medium. Technical details are provided in the supplementary material. A 6-CF is a high-affinity OAT1 and 3 substrate [24] that was chosen as a fluorescent tracer dye to visualize organic anion uptake by the cells. Complete medium refers to renal epithelial cell basal medium supplemented with renal epithelial growth kit (American Type Culture Collection, Manassas, VA, USA). Assay medium was provided by the ciPTEC manufacturer. Renal Tox Medium was formulated by my mentor and myself (composition not disclosed due to confidentiality issues).
2.3 Transporter Assay/Determination of OAT1- and OAT3 Activities
Fluorescent substrate (6-CF) and inhibitor (MK571)-based transporter assays were conducted to determine OAT1 and 3 transporter activity. These assays are explained in greater detail in Sect. 3 and technical details can be found in Sect. 5.
3 Results
3.1 Formulation of Renal Tox Medium
During the first half of my attachment, we worked on formulating a cell culture medium that sustained high 6-CF uptake by iPSC-derived PTC-like cells. We tested 40 different formulations. Highest 6-CF uptake was observed in what is here referred to as the Renal Tox Medium (composition not disclosed due to confidentiality issues).
3.2 Determination of 6-CF Uptake by PTC-Like Cells and CiPTEC-OAT1 and -OAT3 Cells
Next, I compared 6-CF uptake by PTC-like cells and ciPTEC-OAT1 and ciPTEC-OAT3 cell lines in different cell culture media. A 6-CF uptake was measured by flow cytometry, and the results are shown in Fig. 1.
For each condition (as indicated on the x-axis) the intracellular mean fluorescence intensity (MFI) of 10,000 cells was determined by flow cytometry (two technical replicates per experiment). All bars represent the mean MFIs (± standard deviation) of three independent experiments using three independently differentiated batches in the case of PTC-like cells. All data were normalized to 6-CF uptake in PTC-like cells in Renal Tox Medium, which was set to 1. The units on the y-axis indicate the relative normalized 6-CF-specific fluorescence intensity (1 = 6-CF intensity of PTC-like cells in Renal Tox Medium). The colour of each bar in the diagram indicates the medium in which the cells were exposed to 6-CF (labelled on x-axis)
The results showed that ciPTEC-OAT1 and -OAT3 cells have up to ~6- to ~eightfold higher 6-CF uptake compared to PTC-like cells. For ciPTEC-OAT1 and -OAT3, highest 6-CF uptake was observed in Assay Medium that was recommended by the vendor. On the other hand, 6-CF uptake by PTC-like cells was highest in Renal Tox Medium and lowest in Assay Medium. This result suggests that medium conditions need to be carefully selected for each PTC model.
3.3 Functional Activity of OAT1 and OAT3 in Different PTC Models
Next, the OAT1 and OAT3 transporter functionality of each cell model was evaluated using fluorescent substrate- and inhibitor-based transporter assays. These assays work by incubating cells with a transporter-specific fluorescent substrate. Cell samples are either incubated with only the fluorescent substrate, or in addition with an inhibitor for the transporter of interest. If the uptake transporter is active, cells with inhibited transporters would exhibit lower uptake of the fluorescent substrate and therefore display lower fluorescence intensity compared to the non-inhibited cells. This would be represented by a clear leftwards shift of the flow-sorting histogram (x-axis indicates fluorescence intensity) from the uninhibited sample (black histograms in Fig. 2) to the inhibited sample (orange histograms in Fig. 2). Here, we used the OAT1- and 3-specific substrate 6-CF and OAT1- and 3-specific inhibitor MK571.
Flow cytometry was performed with a PTC-like cells, b ciPTEC-OAT1 and c ciPTEC-OAT3 cells as indicated. Cells were incubated with the OAT1 and 3 inhibitor MK571 (orange histograms) or were left uninhibited (black histograms) before incubation with 6-CF for 40 min. 6-CF fluorescence intensity was measured by flow cytometry (scale on x-axis). Cell numbers with a specific level of 6-CF fluorescence intensity are indicated by the scale on the y-axis. The green frames highlight fractions of ciPTEC-OAT1 and ciPTEC-OAT3 cells with high 6-CF fluorescence intensity. The black brackets indicate the size of the shift in fluorescence intensity between inhibited and non-inhibited cells. For each technical replicate, 10,000 cells were analysed (two technical replicates per experiment and cell type). Three independent experiments were performed, and 3 independently differentiate batches of PTC-like cells were used (1 batch per experiment)
We performed this assay with PTC-like cells, ciPTEC-OAT1 and ciPTEC-OAT3 cells. Results are shown in Fig. 2. It should be noted that due to the broadly overlapping substrate specificity of OAT1 and OAT3, this type of assay cannot distinguish between the two transporters. Both transporters could be active in PTC-like cells and so it is not clear whether both transporters or only one of them had contributed to a potentially observed activity in this cell model. However, in ciPTEC-OAT1 and -OAT3 cells, only the transporter with which the cells have been transfected (as indicated by the name of the cell line) would be potentially active, and therefore it is clear in these cases which transporter would contribute to a potentially observed activity.
Typical results as usually observed with this type of assay were obtained with PTC-like cells (Fig. 2). Single-peak, symmetrical histograms suggested a homogenous cell population. The majority of cells had a fluorescence intensity of ~102–103 (inhibited) or ~104 (uninhibited). There was a distinct shift in fluorescence intensity between the inhibited and uninhibited cells (black bracket in Fig. 2). The shift of fluorescence intensity of the entire cell population by more than an order of magnitude showed that almost all PTC-like cells had measurable and relatively high OAT1 and/or OAT3 activity (the larger the shift between the inhibited and non-inhibited samples, the higher the respective transporter activity).
Flow-sorting histograms of ciPTEC-OAT1 and ciPTEC-OAT3 cells exhibited two peaks. In both cell types, the first peak of lower fluorescence intensity was consistently higher than the second (indicating larger cell numbers in this fraction) and was slightly skewed to the right. The presence of two peaks showed that the cell population was inhomogeneous. The majority of cells had low fluorescence intensity, with only a small fraction of cells (indicated by the green frames in Fig. 2) exhibiting much higher uptake activity. The difference in fluorescence intensity between these two sub-populations was nearly 100-fold. As the majority of the ciPTEC cells had in fact low uptake activity, the high intracellular MFI of ciPTEC cells (Fig. 1; yellow bars; Assay Medium) was probably due to this small fraction of cells with very high uptake activity (green frames in Fig. 2). In the case of ciPTEC-OAT1, the main fraction of cells had ~tenfold lower 6-CF uptake than PTC-like cells (histogram of uninhibited ciPTEC-OAT1 peaked at ~103, compared to PTC-like cells where the peak was at ~104). When ciPTEC-OAT1 cells were inhibited, the histogram for the main fraction of cells (orange histogram) flattened out and shifted slightly leftwards, which suggested the presence of some OAT1 activity, albeit at relatively low levels. It is worthy to note that OAT activity here specifically refers to OAT1 activity as ciPTEC-OAT1 cells do not express OAT3 at all. For the high uptake fraction of ciPTEC-OAT1 cells (green box), there was a relatively small shift in fluorescence intensity between the inhibited and uninhibited cells (black bracket in Fig. 2). These results showed that OAT1 was mainly active in the high uptake fraction of ciPTEC-OAT1 cells (green frame in Fig. 2), but at relatively low levels (size of the shift relatively small).
The main fraction of ciPTEC-OAT3 cells showed ~ fivefold lower 6-CF uptake compared to PTC-like cells (Fig. 2, histogram of uninhibited ciPTEC-OAT3 cells showed a main peak between 103 and 104, whereas uninhibited PTC-like cells showed one peak at ~104). The main fraction of ciPTEC-OAT3 shifted toward lower fluorescence intensities upon inhibition (black bracket in Fig. 2), although the shift was smaller compared to PTC-like cells. This indicated the presence of OAT3 transporter functionality in the bulk of the ciPTEC-OAT3 cells (these cells do not express OAT1), although at relatively low levels. On the other hand, no clear shift was observed in case of the high uptake fraction (green box in Fig. 2). This means that 6-CF uptake by these cells was mainly OAT3-independent. Based on these flow cytometry data, we calculated the Multidrug Resistance Affinity Factor (MAF)-values of the respective cell types. MAFs are used to determine transporter activities quantitatively. Results are shown in Fig. 3.
Bars show the Multidrug Resistance Affinity Factor (MAF) values (scale on the y-axis) obtained with each cell type in the respective medium (indicated on x-axis; RTM—Renal Tox Medium, AM—Assay Medium). MAF-values were calculated using the formula: MAFuptake = 100 * ((MFIcontrol − MFIinhibitor)/MFIcontrol), where MFI denotes the mean intracellular fluorescence intensity. MFIs were derived from the results displayed in Fig. 2. The error bars denote the standard deviation. Transporters are considered active if the MAF-value is > 25, as indicated by the dotted line
PTC-like cells had the highest MAF-value of ~55 (Fig. 3). This is well above the threshold level of 25, at which transporters are considered as active. This matches the data shown in Fig. 2, where PTC-like cells exhibited the largest distinct shift between inhibited and uninhibited cells. The results confirm the presence of high OAT1 and/or OAT3 activity in PTC-like cells in Renal Tox Medium.
The lowest MAF-value of ~10 was observed in case of ciPTEC-OAT1 cells (Fig. 3). Here, the value was well below the threshold of 25, which suggests no or only very low OAT1 activity (OAT3 is anyway known to be inactive in these cells). This is consistent with the flow-sorting histograms shown in Fig. 2, where the main fraction of cells exhibited nearly tenfold lower 6-CF uptake than PTC-like cells and no distinct shift was observed after inhibition for the main fraction of cells. Only the high fluorescence intensity fraction of cells displayed a small shift after inhibition, indicating some low level OAT1 activity in a minor fraction of cells.
ciPTEC-OAT3 cells had a MAF-value of ~35 (Fig. 3), which was above the threshold level of 25, but below the MAF value of PTC-like cells. These results are in agreement with the finding that the main fraction of ciPTEC-OAT3 cells had a ~fivefold lower 6-CF uptake compared to PTC-like cells (Fig. 2), and in case of ciPTEC-OAT3 cells the shift after inhibition was relatively small.
Together, the results showed that PTC-like cells displayed the highest OAT1 and/or OAT3 activity and that PTC-like cells represented a homogenous cell population, in contrast to ciPTEC-OAT1 and ciPTEC-OAT3 cells.
4 Conclusion
In the present study, my first mentor and I have formulated a novel cell culture medium for iPSC-derived PTC-like cells. It is planned to file a patent on this so-called Renal Tox Medium, which sustains high OAT1 and/or OAT3 activity in PTC-like cells. Comparison of organic anion uptake of ciPTEC-OAT1, ciPTEC-OAT3 and PTC-like cells in various cell culture media showed the need to select carefully the medium used with each PTC model. The activity of OAT1 and 3 was evaluated by using a fluorescent substrate- and inhibitor-based assay. Transporter activity was quantitated by calculating the MAF values, and PTC-like cells were found to exhibit highest levels of OAT1 and/or 3 transporter activity. ciPTEC-OAT3 cells showed some OAT3 activity above threshold levels (OAT1 is not active in these cells), whereas ciPTEC-OAT1 cells displayed no or only very low levels of OAT1 activity (also OAT3 is not active in these cells). The presence of active, functional drug transporters is particularly important for establishing a reliable in vitro PTC model for nephrotoxicity and drug-drug interaction studies, and OAT1 and 3 are the most important renal uptake transporters for organic anionic drugs like tenofovir or tetracycline [25, 26].
ciPTEC-OAT1 cells have been used in a study by AstraZeneca [10] to establish a novel model for nephrotoxicity prediction, and the pharmaceutical industry is currently most interested in ciPTEC-OAT1 and -OAT3 cells due to their presumably high expression of OAT1 or 3 [10, 23]. However, our results showed that ciPTEC-OAT1 and ciPTEC-OAT3 cells represent inhomogeneous cell populations and have surprisingly low OAT1 or 3 activity, especially in the case of ciPTEC-OAT1. Our flow cytometry results were in agreement with results from Nieskens et al. [22] (Fig. 2c in that publication).
The low OAT1 and 3 activity of respective ciPTEC lines was surprising in the light of the high 6-CF uptake (Fig. 1, yellow bars, Assay Medium). This can be explained by two different mechanisms, which are not mutually exclusive. Firstly, ciPTEC-OAT1 and -OAT3 are inhomogeneous cell populations, which include a minor fraction of cells with very high 6-CF uptake (green frames in Fig. 2). If the mean uptake of the entire cell population is determined, this high-uptake subpopulation would shift the mean values toward higher values. Secondly, 6-CF uptake does not necessarily reflect OAT 1 and 3 activity. PTC express various other organic anion transporters, which may have contributed to 6-CF uptake. These include OAT2 (SLC22A7), OAT4 (SLC22A11) and OATP4C1 (SLCO4C1) [27, 28]. The idea that other organic anion transporters also contributed to 6-CF uptake is supported by the finding that the flow-sorting histograms in Fig. 2 continued to display substantial fluorescence intensity in the cells inhibited with OAT1 and 3 inhibitor MK571. If 6-CF was only transported into the cells by OAT1 and 3 there would be little to no fluorescence in such cells. Also, the high uptake fraction of ciPTEC-OAT3 cells displays essentially no shift upon inhibition of OAT1 and 3 (Fig. 2, green frame). This suggests that high 6-CF uptake in this fraction of cells was mediated by other transporters. Nevertheless, although uptake of 6-CF might not only be mediated by OAT1 and 3, the assays based on the OAT1- and 3-specific inhibitor MK571 still allowed to determine the activity of these two transporters.
Overall, the results revealed that the industry-preferred cell lines ciPTEC-OAT1 and -OAT3 showed surprisingly poor performance. Apart from the low OAT1 or OAT3 activity, the different subpopulations of cells is a problem in toxicity or drug-drug interaction studies. The behaviour of the entire cell population is typically determined in these studies, and the presence of various subpopulations comprises the interpretation of results. Findings obtained here also show that PTC-like cells, in combination with the here developed proprietary Renal Tox Medium, could provide a more suitable solution for academia and industry.
5 Supplementary Material
5.1 Details of Cell Culture
Undifferentiated is070a iPSCs (obtained from Dr. Adrian Teo, IMCB, A*STAR) were expanded in multi-well plates coated with growth factor-reduced Matrigel (Corning, Bedford, MA, USA). Cells were incubated at 37 ℃ with 5% CO2. For differentiation into PTC-like cells, renal epithelium cell growth medium (REGM, Thermo Fisher Scientific, Singapore) supplemented with bone morphogenetic protein (BMP)2 and BMP7 (Merck/Sigma-Aldrich, Singapore) was added to the undifferentiated iPSCs as described by Kandasamy et al. [12]. This previously published protocol [12] was modified in the following way: cells were cryopreserved and stored in liquid nitrogen on day 6 after adding REGM supplemented with BMP2 and BMP7. Before usage cells were thawed and cultivated for 2 days in REGM without BMP2 and BMP7, followed by cultivation for another 2 days in REGM supplemented with BMP2 and BMP7. After this, 4-day cultivation period PTC-like cells were ready to use. Conditionally immortalized proximal tubular epithelial cells (ciPTEC)-OAT1 and ciPTEC-OAT3 cell lines (Accellerate, Hamburg, Germany) were cultivated according to the manufacturer’s protocol in Assay Medium (AM) provided by the manufacturer. Cells were seeded at 62,500 cells/cm2 and grown for 1 day in Assay Medium provided by the manufacturer at 37 ℃ in 5% CO2 before the cells were applied in the assays performed here.
5.2 Details of Determining of 6-CF Uptake
The various PTC models tested here were incubated in cell culture medium containing 6-CF (25 μM, Merck, Singapore) for 40 min at 37 ℃. Subsequently, cells were dislodged with accutase (Merck, Singapore), neutralized with 1 ml of warm phosphate-buffered saline (PBS) and transferred to flow cytometer tubes. The cell solution was centrifuged at 200 g for 1 min and the supernatant was discarded. Cells were resuspended in 500 μl ice-cold Hank’s balanced buffer solution (HBSS, Gibco Life Technologies, Waltham, MA, USA) and kept on ice, until flow cytometry was conducted to analyze 6-CF uptake. In all experiments, flow cytometry was conducted using a BD FACSCelesta™ flow cytometer (BD Biosciences, Singapore).
5.3 Details of Determining of OAT1 and OAT3 Activities
Cells were first incubated with the OAT1- and 3-specific inhibitor MK571 [28] or were left untreated (non-inhibited). Cells were then incubated with the fluorescent anion 6-CF. Quantitative cellular uptake of 6-CF was determined by flow cytometry, where fluorescence-activated cell sorting would detect the 6-CF accumulated within the cells. The difference in 6-CF uptake between inhibited and non-inhibited samples shows the combined activity of OAT1 and three transporters. If the transporters were not active there would be no difference between inhibited and non-inhibited samples. Due to the broadly overlapping substrate specificity of OAT1 and OAT3 this type of assay cannot distinguish between OAT1 and OAT3 activity.
To perform the assay, cells were cultured in BD Falcon 24-well plates according to their respective protocols (see paragraph “Cell Culture”). Cells were either pre-incubated with inhibitor MK571 (50 μM, Selleck Chemicals, Houston, TX, USA) or were left untreated for 10 min at 37ºC. The cell culture medium for the respective cell type containing 6-CF (25 μM, Merck, Singapore) was then added to each well, and cells were incubated for another 40 min at 37 ℃. During the last 5 min of incubation, DAPI dye (4′,6-diamidino-2-phenylindole; Thermo Fisher Scientific, Singapore) was added in a 1:1250 dilution to allow for the exclusion of dead cells from the flow analysis. The reaction was stopped by washing cells with 500 μl PBS. Cells were dislodged with accutase, neutralized with 1 ml of warm PBS and transferred to flow cytometer tubes. The cell solution was centrifuged at 200 g for 1 min and the supernatant was discarded. Cells were resuspended in 500 μl ice-cold HBSS and kept on ice, until flow cytometry was conducted to analyse 6-CF uptake.
References
Curthoys, N. P., & Moe, O. W. (2014). Proximal tubule function and response to acidosis. Clinical Journal of the American Society of Nephrology., 9, 1627–1638. https://doi.org/10.2215/CJN.10391012
Morrissey, K. M., Stocker, S. L., Wittwer, M. B., Xu, L., & Giacomini, K. M. (2013). Renal transporters in drug development. Annual Review of Pharmacology and Toxicology, 53, 503–529. https://doi.org/10.1146/annurev-pharmtox-011112-140317
Tiong, H. Y., Huang, P., Xiong, S., Li, Y., Vathsala, A., & Zink, D. (2014). Drug-induced nephrotoxicity: Clinical impact and preclinical in vitro models. Molecular Pharmaceutics, 11, 1933–1948. https://doi.org/10.1021/mp400720w
Naughton, C. A. (2008). Drug-induced nephrotoxicity. American Family Physician, 78, 743–750. https://pubmed.ncbi.nlm.nih.gov/18819242/
Kaufman, J., Dhakal, M., Patel, B., & Hamburger, R. (1991). Community-acquired acute renal failure. American Journal of Kidney Diseases, 17(2), 191–198. https://doi.org/10.1016/S0272-6386(12)81128-0
Nash, K., Hafeez, A., & Hou, S. (2002). Hospital-acquired renal insufficiency. American Journal of Kidney Diseases, 39(5), 930–936. https://doi.org/10.1053/ajkd.2002.32766
Bellomo, R. (2006). The epidemiology of acute renal failure: 1975 versus 2005. Current Opinion in Critical Care, 12(6), 557–560. https://doi.org/10.1097/01.ccx.0000247443.86628.68
Guengerich, F. P. (2011). Mechanisms of drug toxicity and relevance to pharmaceutical development. Drug Metabolism and Pharmacokinetics, 26(1), 3–14. https://doi.org/10.2133/dmpk.dmpk-10-rv-062
Soo, J. Y., Jansen, J., Masereeuw, R., & Little, M. H. (2018). Advances in predictive in vitro models of drug-induced nephrotoxicity. Nature Reviews Nephrology, 14(6), 378–393. https://doi.org/10.1038/s41581-018-0003-9
Sjogren, A. K., Breitholtz, K., Ahlberg, E., et al. (2018). A novel multi-parametric high content screening assay in ciPTEC-OAT1 to predict drug-induced nephrotoxicity during drug discovery. Archives of Toxicology, 92(10), 3175–3190. https://doi.org/10.1007/s00204-018-2284-y
Li, S., Zhao, J., Huang, R., Steiner, T., Bourner, M., Mitchell, M., Thompson, D. C., Zhao, B., & Xia, M. (2017). Development and application of human renal proximal tubule epithelial cells for assessment of compound toxicity. Current Chemical Genomics and Translational Medicine, 11, 19–30. https://doi.org/10.2174/2213988501711010019
Kandasamy, K., Chuah, J. K., Su, R., Huang, P., Eng, K. G., Xiong, S., Li, Y., Chia, C. S., Loo, L. H., & Zink, D. (2015). Prediction of drug-induced nephrotoxicity and injury mechanisms with human induced pluripotent stem cell-derived cells and machine learning methods. Scientific Reports, 5, 12337. https://doi.org/10.1038/srep12337
Chuah, J., & Zink, D. (2017). Stem cell-derived kidney cells and organoids: Recent breakthroughs and emerging applications. Biotechnology Advances, 35(2), 150–167. https://doi.org/10.1016/j.biotechadv.2016.12.001
Zink, D., Chuah, J., & Ying, J. Y. (2020). Assessing toxicity with human cell-based in vitro methods. Trends in Molecular Medicine, 26(6), 570–582. https://doi.org/10.1016/j.molmed.2020.01.008
Jenkinson, S. E., Chung, G. W., van Loon, E., Bakar, N. S., Dalzell, A. M., & Brown, C. D. (2012). The limitations of renal epithelial cell line HK-2 as amodel of drug transporter expression and function in the proximal tubule. Pflugers Archiv—European Journal of Physiology, 464, 601–611. https://doi.org/10.1007/s00424-012-1163-2
Weiland, C., Ahr, H. J., Vohr, H. W., & Ellinger-Ziegelbauer, H. (2007). Characterization of primary rat proximal tubular cells by gene expression analysis. Toxicology in Vitro, 21, 466–491. https://doi.org/10.1016/j.tiv.2006.10.008
Wang, L., & Sweet, D. H. (2013). Renal organic anion transporters (SLC22 family): Expression, regulation, roles in toxicity, and impact on injury and disease. The AAPS Journal, 15(1), 53–69. https://doi.org/10.1208/s12248-012-9413-y
Nigam, S. K., Bush, K. T., Martovetsky, G., Ahn, S. Y., Liu, H. C., Richard, E., Bhatnagar, V., & Wu, W. (2015). The organic anion transporter (OAT) family: A systems biology perspective. Physiological Reviews, 95(1), 83–123. https://doi.org/10.1152/physrev.00025.2013
Zeng, Y., Zhang, R., Wu, J., Liu, M., Peng, W., Yu, X., & Yang, X. (2012). Organic anion transporter 1 (OAT1) involved in renal cell transport of aristolochic acid I. Human & Experimental Toxicology, 31(8), 759–770. https://doi.org/10.1177/0960327111424302
Motohashi, H., Sakurai, Y., Saito, H., Masuda, S., Urakami, Y., Goto, M., Fukatsu, A., Ogawa, O., & Inui, K. I. (2002). Gene expression levels and immunolocalization of organic ion transporters in the human kidney. Journal of the American Society of Nephrology: JASN, 13(4), 866–874. https://doi.org/10.1681/ASN.V134866
Wilmer, M. J., Saleem, M. A., Masereeuw, R., Ni, L., van der Velden, T. J., Russel, F. G., Mathieson, P. W., Monnens, L. A., van den Heuvel, L. P., & Levtchenko, E. N. (2010). Novel conditionally immortalized human proximal tubule cell line expressing functional influx and efflux transporters. Cell and Tissue Research, 339(2), 449–457. https://doi.org/10.1007/s00441-009-0882-y
Nieskens, T. T., Peters, J. G., Schreurs, M. J., Smits, N., Woestenenk, R., Jansen, K., van der Made, T. K., Röring, M., Hilgendorf, C., Wilmer, M. J., & Masereeuw, R. (2016). A human renal proximal tubule cell line with stable organic anion transporter 1 and 3 expression predictive for antiviral-induced toxicity. The AAPS Journal, 18(2), 465–475. https://doi.org/10.1208/s12248-016-9871-8
Vormann, M. K., Vriend, J., Lanz, H. L., Gijzen, L., van den Heuvel, A., Hutter, S., Joore, J., Trietsch, S. J., Stuut, C., Nieskens, T., Peters, J., Ramp, D., Caj, M., Russel, F., Jacobsen, B., Roth, A., Lu, S., Polli, J. W., Naidoo, A. A., & Vulto, P., et al. (2021). Implementation of a human renal proximal tubule on a chip for nephrotoxicity and drug interaction studies. Journal of Pharmaceutical Sciences, 110(4), 1601–1614.https://doi.org/10.1016/j.xphs.2021.01.028
Truong, D. M., Kaler, G., Khandelwal, A., Swaan, P. W., & Nigam, S. K. (2008). Multi-level analysis of organic anion transporters 1, 3, and 6 reveals major differences in structural determinants of antiviral discrimination. The Journal of Biological Chemistry, 283(13), 8654–8663. https://doi.org/10.1074/jbc.M708615200
Moss, D. M., Neary, M., & Owen, A. (2014). The role of drug transporters in the kidney: Lessons from tenofovir. Frontiers in Pharmacology, 5, 248. https://doi.org/10.3389/fphar.2014.00248
Zhu, L., Lu, L., Wang, S., Wu, J., Shi, J., Yan, T., Xie, C., Li, Q., Hu, M., & Liu, Z. (2017). Oral absorption basics: Pathways and physicochemical and biological factors affecting absorption. In Developing solid oral dosage forms (2nd edn). Academic Press. https://doi.org/10.1016/B978-0-12-802447-8.00011-X
Yohannes Hagos, Daniel Stein, Bernhard Ugele, Gerhard Burckhardt, Andrew Bahn, 2007. Human Renal Organic Anion Transporter 4 Operates as an Asymmetric Urate Transporter. JASN, 18 (2) 430–439; https://doi.org/10.1681/ASN.2006040415
Henjakovic, M., Hagos, Y., Krick, W., Burckhardt, G., & Burckhardt, B. C. (2015). Human organic anion transporter 2 is distinct from organic anion transporters 1 and 3 with respect to transport function. American Journal of Physiology. Renal Physiology, 309(10), F843–F851. https://doi.org/10.1152/ajprenal.00140.2015
Acknowledgements
I’d like to thank my two mentors, Dr. Riga Tawo (NBL-SIFBI, A*STAR) and Team Leader and Principal Research Scientist Dr. Daniele Zink (NBL-SIFBI, A*STAR) for their unwavering support, invaluable guidance and utmost dedication. I also express my deepest gratitude to A*STAR Senior Fellow Professor Jackie Y. Ying, and NBL Director and YRP Chair Ms Noreena AbuBakar for this incredible experience. They have all inspired me in immeasurable ways. This work was supported by the NanoBioLab (NBL), Biomedical Research Council, A*STAR and the Singapore Institute of Food and Biotechnology Innovation (SIFBI), Biomedical Research Council, A*STAR.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this paper
Cite this paper
Kylin, T.A., Tawo, R., Zink, D. (2023). Analysis of Chemical Transport by IPSC-Derived Proximal Tubular Cell (PTC)-Like Cells and Other Emerging Human Kidney Cell Models for Drug Toxicity Screening. In: Guo, H., et al. IRC-SET 2022. Springer, Singapore. https://doi.org/10.1007/978-981-19-7222-5_26
Download citation
DOI: https://doi.org/10.1007/978-981-19-7222-5_26
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-19-7221-8
Online ISBN: 978-981-19-7222-5
eBook Packages: Physics and AstronomyPhysics and Astronomy (R0)