Abstract
Traumatic injury around the knee results in articular cartilage damage and leads to posttraumatic arthritis (PTA). The challenges encountered in this situation are knee stiffness, soft tissue compromise, retained hardware, bone defects, malunion and nonunion, and latent infection. Total knee arthroplasty (TKA) in posttraumatic situation provides good functional outcome, but risk of complications is higher when compared to TKA for primary osteoarthritis.
Preoperative planning is critical and of paramount importance for successful outcome and longevity after TKA. Restoration of joint line, reconstruction of bone defect, and ligament balancing should be achieved. The usage of better implant designs, judicious use of stem and augments, proper soft tissue handling, and modern reconstruction techniques may lead to the favorable functional outcome and best long-term results.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Posttraumatic arthritis
- Total knee arthroplasty
- Conversion total knee arthroplasty
- Failed fixations
- Complications
- Soft tissue compromise
- Bone defects
1 Introduction
Posttraumatic arthritis (PTA) develops after post-trauma and failed fixations, around the knee due to articular cartilage damage either by direct injury or secondary to metal protrusion into the joint after a fixation for fractures in the periarticular region. The need for Total Knee Arthroplasty (TKA) after injury or failed fixation is increasing. The challenges we encounter are so complex that it requires lot of systematic approach and careful planning.
The incidence of arthritis following tibial plateau and distal femur fractures is high and estimated to be from 21% to 44% [1,2,3,4]. After osteoarthritis and rheumatoid arthritis, the third most common indication for total knee arthroplasty is PTA [1]. The terminology “conversion TKA” is used by some authors, which require periarticular hardware removal prior or during TKA [5, 6]. High energy trauma is the major cause of posttraumatic arthritis in younger patients [1]. Young patients, high velocity injuries, articular incongruity, bicondylar fractures, residual malalignment, associated soft tissue involvement lead to an increased chance of posttraumatic arthritis [7].
The incidence of tibial plateau fractures leading to end-stage PTA, which requires knee arthroplasty is low. Wasserstein et al. [4] showed 7.3% incidence of TKA at 10 years after operatively treated tibial plateau fractures. TKA for posttraumatic arthritis gives significant improvement in functional outcome but poor results compared to TKA for primary osteoarthritis. Saleh et al. concluded that TKA for posttraumatic arthritis results in pain-free mobility, good range of motion, and better functional outcome scores, but complications are high which includes infection, stiffness, delayed wound healing, extensor apparatus disruption, and polyethylene wear [8]. TKA performed for distal femur fractures is more complicated due to tissue scarring, nonunion, malunion, infection but have good functional outcome compared to tibial plateau fractures [9].
2 Challenges in Post-Trauma Situation
Total knee arthroplasty in the post-trauma situation is technically challenging. Literature reports fair to poor outcome with more complications when TKA is performed for posttraumatic arthritis. The reason behind this can be many like knee stiffness, bone loss, malalignment, joint instability, poor skin condition, broken hardware, and latent infection [10]. Moreover, many studies showed increased need for blood transfusion, increased duration of surgery, risk of perioperative complications, and readmission rate associated with TKA for posttraumatic conditions [1, 3, 5, 6, 11].
3 Preoperative Planning
Preoperative planning is critical and of paramount importance for total knee arthroplasty in PTA. It helps the surgeon to anticipate any potential intraoperative challenges and reduce the risk of complications. The past history is very important in regard to open or closed fractures, any discharging wound, or postoperative complications that has to be considered with lot of attention. The discharge summary should be scrutinized in detail for valuable information. The comorbidities of the patients should be carefully evaluated and optimized. History of chronic smoking and alcoholism increases the wound healing problems and carefully documented.
The clinical examination should be meticulous for decision making. The patient’s gait should carefully be evaluated for the presence of thrust and hyperextension while walking and that suggests joint laxity. The varus and valgus stress assessment of ligament stability is important to find the competence of collateral ligaments. Sometimes, the bone defects give the perception of pseudo-instability [1]. The skin over the knee should be evaluated for any redness, warmth, and swelling indicative of doubtful infection. The previous scar over the knee should be assessed for its location, number and its adherence to the underlying structures.
One of the most common problems with PTA is knee stiffness, which is defined as flexion <90°. Articular damage, hemarthrosis, insufficient fracture reduction will subsequently lead to cartilage destruction resulting in fibrosis and knee stiffness [1]. Evaluating the baseline knee range of motion is essential. The preoperative range of motion has a strong correlation with the postoperative range of motion [1, 12]. Hence, exact documentation of range of motion in the supine and sitting position helps to counsel the patients preoperatively.
The deformities assessed for its magnitude and its location like tibia, femur, or both. The plane of deformity in coronal plane like varus and valgus deformity and in sagittal plane like fixed flexion deformity evaluated at rest and weight-bearing. The status of peripheral pulses and neurology was carefully recorded. The ipsilateral hip and ankle and contralateral limb assessed, which will have a contribution to postoperative rehabilitation [13].
3.1 Radiological Evaluation
The radiographic evaluation includes full-length standing hip-to-ankle radiographs to know the magnitude of the deformity, coronal laxity, and location of the deformity like intraarticular, extraarticular deformity, or both [1]. It also helps to visualize the complete profile of the previous implants and to determine the planning for corrective osteotomy. Sometimes, the previous implants may obscure the degenerative changes in the knee. The lateral view helps to identify the patella position and tibial slope. The skyline view identifies any patellar subluxation with shift or tilt. The stress view helps to quantify the amount of instability and document ligamentous competence. The preoperative CT scan helps to identify the location and degree of the bone deficiency [1]. In rare situations, CT angiography will be required to evaluate the status of vessels in difficult cases.
3.2 Blood Investigations
Preoperative blood investigations are always necessary to identify any quiescent infection. The previous history of open fractures, postoperative persistent wound drainage, and chronic antibiotic therapy should raise the suspicion of occult infection. The blood should be evaluated for erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), and complete blood count preoperatively. Optimal glycemic control with HbA1C <8 is essential in patients with diabetes undergoing TKA to avoid complications. If the blood parameters like ESR and CRP are raised above the cut-off values, joint aspiration should be analyzed for culture and sensitivity.
3.3 Role of Preoperative Knee Aspiration
Some authors used preoperative knee aspiration performed in every knee to rule out infection [8]. There are chances of false-negative results because of prior administration of antibiotics, flaws in obtaining and transporting the samples, and using inadequate culturing techniques [14]. Nevertheless, the aspiration will yield a positive result in infection in many cases. The strategies to improve the yield in the cultures are to delay the aspiration at least 2 weeks after the administration of the last antibiotics. Introduction of bacteriostatic components like saline and local anesthetic should be avoided. The fluid should be immediately transferred into the blood culture bottles and standard containers. Usage of specialized culture medium for atypical organisms is also warranted. To improve the culture yield, an extended period of incubation from 14 to 21 days allows isolation of slow-growing organisms like Propionibacterium acnes and some coagulase-negative staphylococci [14].
4 Surgical Considerations
4.1 Incision and Exposure
The soft tissue defect spectrum ranges from multiple scars, scars that are adherent to the underlying bone to previous skin grafts or flaps (Fig. 16.1). The incision is sometimes dictated by the previous scar and the most recent incision should be used if sufficient exposure is gained. The most lateral usable incision should be selected to avoid devascularization and skin necrosis. This is because the fascial perforators arise from the medial aspect of the knee [8]. The previous horizontal incision can be crossed by a longitudinal incision at the right angle [2]. The plastic surgery consultation should be done in the presence of multiple scars or previous plastic procedures over the incision site to evaluate the risk of skin necrosis. The need for any local flaps should be planned before surgery.
Clinical pictures showing the various spectrum of soft tissue defects (a) previous adherent skin graft and flaps involving the entire knee (b) previous skin graft over the incision area (c) two longitudinal scars after fracture fixation (d) previous horizontal incision can be crossed by a longitudinal incision at the right angle
One of the most common problems with PTA is knee stiffness. This can be addressed by arthrolysis of the suprapatellar pouch, removing the fibrous tissue and clearing the medial and lateral gutters, and retro-patellar fat pad removal. If adequate flexion could not be achieved after these maneuvers, an extended approach like quadriceps snip (Fig. 16.2a), VY turndown (Fig. 16.2b), or tibial tubercle osteotomy (Figs. 16.3 and 16.4) may be needed. Massin et al. used tibial tubercle osteotomy in patients with knee stiffness and patella baja and found no compromise in flexion range of motion postoperatively [12]. In the case of patella baja, tibial tubercle osteotomy allows slight proximal recession. Lateral retinacular release may be needed for facilitating knee exposure or if there is a presence of patellar maltracking.
(a) Picture showing initiation of tibial tubercle osteotomy with saw blade in a stiff knee after posttraumatic arthritis (b) elevation of tibial tubercle osteotomy fragment with stacked osteotomes (c) arrow showing the tibial tubercle fragment (d) after final implantation, tibial tubercle fragment closed with ethibond sutures and augmented with cancellous autograft
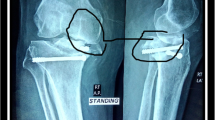
Radiographs of the same patient in Fig. 16.3 showing (a) Posttraumatic arthritis with distal femur plate in situ with stiff knee (b) exposure by tibial tubercle osteotomy and stem augmentation to bypass the screw holes stress riser
4.2 Hardware Removal and Timing of Surgery
Hardware removal can be encountered in three ways.
-
1.
Simultaneous complete hardware removal and TKA. In the presence of normal laboratory parameters like ESR and CRP, good knee range of motion and optimized comorbid conditions, simultaneous implant removal and TKA can be planned. Simultaneous hardware removal and TKA may require more than one incision and may increase the chance of contamination and skin necrosis [15].
-
2.
Partial hardware removal and TKA can be done. Complete removal of the hardware may not be always necessary and only the hardware which hinders the preparation or implantation of the TKA implants can be removed (Fig. 16.5).
-
3.
Two-stage procedure, where hardware removal and TKA in a staged manner. The indications for two-stage removal are long-standing implants with broken screws, long duration procedure with potential soft tissue damage, uncontrolled diabetes, knee stiffness, morbid obesity, and doubtful unhealthy tissue suspicion of infection.
The implants should be assessed for the length of the time that was in situ, because removal may be difficult in remote fixations. In a failed fixation, often the hardware is damaged. Hence, the appropriate and comprehensive implant removal set should be arranged like universal nail extractor, broken screw removal set, high-speed metal cutting burrs, etc. It is necessary to bypass the screw holes left by hardware removal with an intramedullary stem to avoid the risk of refracture. Bergen et al. found the timing of hardware removal not associated with any difference in complication rate [5].
4.3 Joint Reconstruction and Bone Loss Management
The goals in TKA for posttraumatic arthritis are joint line restoration, bone defect reconstruction, and ligament balancing. Recreation of the joint line is essential for the optimal function of the collateral ligaments and extensor mechanism. The various landmarks should be used in the distorted bony anatomy like meniscal scars, tibial tuberosity, fibular head, medial and lateral epicondyles. After defining the joint line, bone loss should be reconstructed appropriately.
Bone loss restoration gives primary stability to the implants [1]. PTA will often result in either contained defect which can be managed with morselized bone grafts or uncontained bone loss. The various options for bone defect management are stems, metal augments, allografts, resected bone, metaphyseal sleeves, and trabecular metal cones. This decision is based on peroperative size of the uncontained defects persisting after the bone cuts.
After reconstituting the bone loss, the competence of the collateral ligaments should be checked. If there is pseudo-instability due to bone defects, ligaments will regain competence after reconstructing the bone loss (Figs. 16.6 and 16.7). Higher level of constraint implant is used if there is compromise in collateral ligaments, which is critical in achieving long-term survivorship [10]. Correcting the extraarticular deformity by extensive intraarticular release may damage the collateral stability, which also necessitates the need for constrained implants. In severe extraarticular deformity, corrective osteotomy will be required either as a simultaneous or staged procedure [16]. The presence of malunion with metaphyseo-diaphyseal mismatch warrants for use of “offset” stems.
(a) Posttraumatic arthritis with a severe bone defect in the lateral tibial condyle and buttress plate in situ (b) Varus and valgus stress view showing the magnitude of bone defect and pseudo-instability (c) hip-to-ankle alignment radiograph showing severe valgus deformity (d) management of bone loss by total knee arthroplasty with metaphyseal sleeves and screw augmentation
Intraoperative pictures of the same patient in Fig. 16.6 showing (a and b) severe lateral tibial and femoral condyle bone defect (c) depth of the defect after proximal tibial cut (d) preparation for the sleeve (e) the defect augmented with both sleeves and screw (f) placement of final tibial component (g and h) anterior and lateral picture showing the final implantation of the components
4.4 Implant Selection
The choice of the implant is decided by the size of the bone loss and competence of the collateral ligaments. In a minimal contained bone loss situation, if the joint stability is achievable by primary cruciate-retaining and posterior stabilized implants, then it will be sufficient. The choice is based on the integrity of the posterior cruciate ligament, surgeon’s expertise and choice [10] (Fig. 16.8). Scott et al. managed primary cruciate-retaining implants in 87% of the patients without augmented tibial stems needed in 35% [17].
The presence of arthrofibrosis and subsequent extensive release may warrant a posterior stabilized implant [10] (Fig. 16.9).
The intramedullary stem augmentation should be done in a compromised metaphyseal bone stock situation to prevent implant subsidence [2] (Figs. 16.4 and 16.10). The stem offloads the stress in the metaphysis and prevents premature failure. It acts as a load-sharing device and bypasses the stress risers resulting from the hardware removal and damaged metaphyseal bone. The stems help to restore the joint alignment and help in aligning the component position.
Epiphyseal bone loss is common in the PTA knees and metaphyseal fixation has several distinct advantages. This region is more vascularized and mostly not affected by bone loss. Martin-Hernandez et al. [18]. used metaphyseal sleeves for PTA and showed 100% survival at a mean follow-up of 79 months. The porous titanium metaphyseal sleeves allow filling of bone defects, improves osseointegration, provides load sharing, reduces stress shielding, and achieves axial and rotational stability (Fig. 16.6). Trabecular metal cones are used for filling the metaphyseal defects and act like structural grafts. The metaphyseal sleeves and cones are indicated in type 3 Anderson Orthopaedic Research Institute (AORI) classification defects.
Often the PTA will be associated with arthrofibrosis, rigid deformities with ligamentous incompetence. About 10% of the PTA patients may have severe ligamentous instability and balancing this knee might involve extensive release which might compromise the collateral ligament stability [15]. The constrained knee prosthesis should be selected to achieve the ligament balance in the event of a ligamentous compromise (Fig. 16.11).
Rai et al. used constrained condylar knee in complex deformities after PTA and showed excellent clinical outcome, regain of function, and survival rate of 94.7% at an average of 6.5 years follow-up [19]. If there is complete ligament disruption, then the option of hinge prosthesis is chosen (Fig. 16.12).
In severe bone loss or acute severe comminuted fracture involving the distal femoral condyle, distal femoral replacement implants may be chosen (Figs. 16.13 and 16.14). The algorithm for the management of posttraumatic arthritis is elucidated in Fig. 16.15.
5 TKA After Intramedullary Nailing
Most diaphyseal fractures of the tibia are treated with intramedullary nailing. There are technical challenges in the placement of the tibial components with the intramedullary nail in situ (Fig. 16.16). As the need for TKA increases, this combination may be encountered more frequently in the future [20, 21]. Kolz et al. showed that the presence of intramedullary nail has not increased the chances of infection and knee stiffness [20]. Preoperative radiographs should be evaluated for possible nail interference with the tibial keel. TKA can be proceeded if the intramedullary nail does not touch the tibial keel.
If there is concern regarding the possible nail interference, one option is that the intramedullary nail can be removed and TKA can be performed in a simultaneous or staged manner (Fig. 16.17).
The other option is placing the tibial component without complete removal of the intramedullary nail. There are a few technical factors that can be considered. They are selecting the implant with a reduced keel length of the tibia or using the uncemented components which will not require deep tibial keel preparation. Opting for posterior stabilized implants is another option that requires less tibial slope preparation such that it will not impinge on the nail as compared to the cruciate-retaining components [21]. The proximal part of the nail can be modified using a metal cutting burr, so that the tibial component can be accommodated [20] (Figs. 16.18 and 16.19).
Intraoperative picture of the same patient in Fig. 16.18 showing (a and b) tibial tubercle osteotomy and exposed intramedullary nail in situ (c) proximal part of the nail exposed (d) arrow showing metal cutting burr used to modify the proximal part of the nail to accommodate the tibial keel (e) cut proximal part of the nail (f) posteromedial bone defect managed with screw augmentation (g and h) implantation of the final components and closure of tibial tubercle osteotomy by ethibond sutures
6 Computer-Assisted Surgery (CAS)
In the presence of hardware in the intramedullary canal, it is not possible to use the conventional instruments with intramedullary jigs. CAS helps to avoid the hardware removal, precludes the stress risers at the screw hole, and improves the component alignment (Fig. 16.20). The presence of angular deformity and canal sclerosis preclude the use of an intramedullary guide and CAS will guide in taking accurate bone cuts [22]. Tani et al. [23]. did a comparative study in patients with extraarticular deformity with and without CAS. They showed the rate of outliers is lower in the navigation group and helps in achieving better clinical and radiological outcomes.
CAS helps to assist in the correct placement of cutting guides and implants in the background of distorted anatomical landmarks. The CAS system has the advantage of reliable component placement in presence of tibial and femoral deformities. It may also reduce blood loss and negates the problems associated with using intramedullary guides. The disadvantages are increased cost and longer operating times [16].
7 Primary Arthroplasty for Acute Fractures Around the Knee
In elderly patients, the incidence of tibial plateau fracture is around 8% [24, 25]. There is renewed interest in primary arthroplasty for acute fractures around the knee. It is because of the high failure rate and poor results associated with internal fixation in this subgroup of patients [26]. The challenges are underlying osteoporosis which makes difficulty in fracture fixation, poor outcome due to preexisting arthritis, delayed weight-bearing leading to medical complications, and morbidity associated with revision surgery [27]. The indications for primary acute TKA are elderly patients with preexisting osteoarthritis of the knee, non-reconstructible articular fractures with underlying severe osteoporosis [28] (Fig. 16.21).
The advantages are early mobilization, immediate weight-bearing, better functional outcomes, eliminating the fracture healing problems, and reduces the reoperation rates [24]. The word of caution is that it should not be performed routinely for all the periarticular fractures. TKA in the acute setting is technically more demanding and should be performed by experienced arthroplasty surgeons considering the severity of metaphyseal bone loss and associated ligamentous injury. There may be disruption of the anatomical landmarks and simulates like performing a revision TKA [25]. It may require constrained implants, stems, sleeves, or cones for filling the metaphyseal defects, hinged components for bony and ligamentous insufficiency, and distal femoral replacement. Even though the functional results are good, the complication rate remains high [24, 25]. Kini et al. suggested computer-assisted navigation helps in accurate component positioning and restoring the mechanical axis [25].
Appleton et al. reported the largest case series of 52 patients undergoing fixed-hinge stemmed total knee replacement for distal femoral fractures with poor preoperative mobility and medically frail patients [27]. They reported high 1-year mortality of 41% and the most common postoperative complication was periprosthetic fractures. Bettin et al. showed good results using cemented modular rotating hinge distal femoral endoprosthesis for acute distal femoral fractures. They concluded that primary arthroplasty allows immediate full weight-bearing and restores the patient’s preoperative functional status in most patients [29]. Haufe et al. used hinge prosthesis in 80% of patients with acute proximal tibial fractures for orthogeriatric patients and showed good clinical results if done with proper indications [30].
The surgical pearls for encountering the TKA are elucidated systematically by Hsu et al. [31]. For the distal femur fractures, a good exposure by medial parapatellar approach and clearing out the medial and lateral gutters are made. After completely exposing the distal femur, cerclage wires are to be placed in the diaphysis to prevent the propagation of the fracture. Then, the integrity of the medial and lateral femoral column is assessed for reconstruction. The fracture fragments are secured with a contoured reconstruction plate and screws and standard arthroplasty is performed. The stems may be used for diaphyseal fixation and sleeves can be used for filling and stabilizing the metaphysis to unload the stress at the fracture site. In case of severe comminuted non-reconstructible articular fractures or complete ligament disruption, distal femur replacement with modular mega-prosthesis should be opted. The joint line, posterior condylar offset, and femoral rotation should be restored by using various anatomical landmarks.
TKA in proximal tibial fractures is still more complex. The prerequisites are to establish a stable tibial platform and reconstitute the joint line. After adequate exposure, the medial and lateral plateau fracture is evaluated for its integrity and reconstructed to provide a solid platform for the tibial prosthesis. Intramedullary guides may help in stabilizing the shaft and taking appropriate cuts. If the fracture fragments are large, it must be stably fixed with internal fixation and can be augmented with the stem. If there is doubt in the ligament integrity, then constrained components should be used. The tibial tubercle involvement leads to chances of nonunion and can be a contraindication for doing TKA [10].
8 Complications: How to Avoid and Tackle Them?
TKA for posttraumatic arthritis have shown high rate of complications between 26% and 60% in the literature [2, 8, 9, 17, 32, 33]. PTA knees have complex joint deformities, previous multiple procedures leading to soft tissue compromise and associated arthrofibrosis [7]. These factors lead to an increased chance of complications in the PTA group when compared with the primary osteoarthritis group. The various preoperative risk factors associated with unsatisfactory outcomes are complex deformities like combined tibial and femoral involvement [34], compromise of soft tissue envelope [34], patella baja [22], multiple previous surgeries [35], collateral ligament insufficiency and arthrofibrosis [36]. The impact of PTA on postoperative outcome after TKA shows that higher incidence of periprosthetic joint infection, wound complications, knee stiffness, and decreased implant survivorship [7, 37].
The study from Mayo clinic with 15 years follow-up of TKA for previous proximal tibial fractures reported more than 90% of complications occurred within 2 years after TKA [38]. In a national database study comparing 674 posttraumatic TKA with 67,675 primary TKA, Kester et al. reported an increased need for transfusion, length of hospital stays, and 30-day readmission rate in the posttraumatic arthritis group [6, 39]. Ge et al. showed that the post-fracture TKA cohort has an increased complication rate like surgical site infection and a 6.7-fold increase in 90-day readmission rate compared to the previous soft tissue trauma cohort [35].
8.1 Infection
Prosthetic joint infection is the most worrisome complication following TKA. The complex deformities, previous multiple procedures, presence of prior hardware, increased operative time contribute to surgical site infection. The overall infection rate secondary to PTA ranges between 3.4 and 9.6% in the literature [19]. Infection is the most common cause of revision in patients undergoing TKA for PTA [40, 41]. A recent comparative study on a large national database also shows PTA patients having a statistically significant increase in the incidence of superficial and deep wound infection when compared with the osteoarthritis group [42].
A high index of suspicion is needed for a possibility of hidden infection in a previously operated knee with retained hardware. Preoperative antibiotics should be given after taking the intraoperative cultures. If there is suspicion of infection, then two-stage revision should be opted. The antibiotic-impregnated cement can be used in patients with higher risk of infection [8]. Saleh et al. reported a 20% infection rate and recommended intraoperative frozen section analysis even if the preoperative cultures are negative [8].
8.2 Skin Problems
The arteriole plexus over the knee gets damages in the previous knee surgeries. Wound healing complications are a significant issue in a compromised soft tissue envelope. Principles in soft tissue handling are making adequate skin bridges between the previous scars, sharp dissection with full-thickness flaps without undermining, and carefully avoiding forceful retraction. Meticulous hemostasis and tension-free wound closure are also recommended for avoiding wound necrosis and dehiscence [43].
8.3 Postoperative Knee Stiffness
Scott et al. [17]. reported about 13% of patients (4 out of 31) developed knee stiffness and required manipulation under anesthesia. Knee stiffness is a frequent complication and needs proper preoperative counseling [44]. Rai et al. found significant improvement in the postoperative range of motion. They suggested the proper intraoperative balancing of the knee along with postoperative rehabilitation helps to improve the postoperative range of knee motion [19].
8.4 Instability
El-Galaly et al. [45]. showed instability is the major cause of revision in the posttraumatic group. This can be attributed to the preceding injury and ligament damage during hardware removal. The authors cautioned the intraoperative meticulous ligament balancing and choosing the optimal implants to address the instability.
8.5 Extensor Mechanism Disruption
This is a catastrophic complication that can affect the functional outcome after TKA and the incidence is as high as 8 to 13% [15, 46]. It can occur either intraoperatively or postoperatively. Exposure in a previous stiff knee with quadriceps contracture can lead to disruption of the patellar tendon. Extensile approaches like tibial tubercle osteotomy, V-Y quadricepsplasty, or rectus snip may be necessary to avoid those complications. A smooth pin placed at the patellar tendon also helps in preventing the avulsion. Massin et al. reported that about 75% of patients with severe stiff knees had postoperative complications like patellar tendon avulsion and infection [12].
Performing the systematic lateral retinacular release and avoiding patellar eversion are also described to reduce its incidence [15]. Postoperatively, tendon ruptures occur in patients on long-term steroids, diabetes, after extensive lateral release leading to devascularization and sudden hyperflexion from acute trauma [8]. It can be managed by direct repair augmented with patella-tibial cerclage protection or reconstructed with autologous graft or allograft.
8.6 Malalignment
The critical factor to ensure the longevity of the implant is achieving proper mechanical alignment [16]. Malalignment is an important concern when TKA is performed with conventional instruments. Lonner et al. [2]. reported 26% aseptic failures and poor outcomes due to malalignment. This is because of the distortion of the anatomical landmarks. Papadopoulos et al. [33]. noted over half of their patients had suboptimal positioning of the components and residual deformity. The computer-assisted navigation may help to achieve proper alignment in distorted anatomy. The stemmed tibial implants are recommended to avoid malalignment and subsidence [2].
9 Clinical Outcomes and Survivorship
Overall the literature shows TKA is an effective treatment in terms of improvement in the quality of life, functional parameters, pain reduction, and improvement in the knee range of motion. Although patients have significant improvement compared to the preoperative disability, the overall postoperative scores remained low compared to osteoarthritis patients. This difference can be primarily attributed to the poorer preoperative scores due to unstable knees when compared with non-PTA patients [7, 47].
Weiss et al. suggested that the important factor which influences the outcome after TKA is the initial fracture treatment like proper soft tissue handling, minimal periosteal stripping, anatomic reduction, and restoring the alignment [46]. Patients with instability needed earlier TKA than those patients with malunion. Scott et al. concluded that postoperative patient-reported outcome measures were comparable to patients with primary osteoarthritis, although a higher rate of intra-and-postoperative complications is noted in the PTA group [17].
Historically, TKA for posttraumatic arthritis showed overall inferior survival results in the literature. In a registry-based study on 52,518 patients, El-Galaly et al. [45]. showed TKA for posttraumatic arthritis has an increased risk of early and medium-term revision. But, after 5 years, there is no significant difference in the risk of revision when compared to TKA for osteoarthritis. Lunebourg et al. reported lower ten-year survival of 79% at 10 years for posttraumatic arthritis compared to 99% in the primary osteoarthritis group [3]. The posttraumatic arthritis group had poor clinical results in terms of quality of life, but there is an equal subjective and functional improvement from the baseline scores compared to the primary osteoarthritis group. About one-fifth of the patient required reoperation within 2 years from the index surgery [3]. Houdek et al. concluded that TKA for the posttraumatic condition has a worse outcome and 1 in 4 patients tend to have revision by 15 years [43].
On contrary, recent studies found no difference in the functional outcome in patients with prior tibial plateau fracture at an average of 6.7 years in a prospective matched control study [15]. The long-term study from Mayo clinic shows survival free of revision for aseptic loosening is 96% at 15 years for TKA after tibial plateau fractures. They suggested excellent long-term survivorship similar to TKA for degenerative arthritis [38]. The survival rate of 89% at 10 years and a 60% satisfaction rate of reported in a multicenter nationwide study among 263 patients [48]. Khoshbin et al. [41]. concluded significant improvement in patient-related outcome measures comparable to TKA for osteoarthritis. The modern reconstruction techniques using better implant designs, judicious use of stem and augments, and proper soft tissue handling can be attributed to improvement in functional outcome and implant survivorship.
10 Summary
Total knee arthroplasty in post-trauma and failed fixations is demanding and challenging, for which preoperative planning is essential to manage and achieve a good functional outcome. Stiffness, bone loss, instability, and retained hardware are major challenges encountered, hence caution and high-level expertise are warranted. Chances of latent infection should be considered, investigated and patients thoroughly counseled for potential postoperative complication. The bone defect and ligament stability should be adequately managed with proper implants and constraint level should be appropriately selected. However, total knee arthroplasty in these situation gives significant improvement in the functional outcome. Therefore, proper surgical execution is necessary for best long-term results.
References
Benazzo F, Rossi SMP, Combi A, Meena S, Ghiara M. Knee replacement in chronic post-traumatic cases. EFORT Open Rev. 2016;1(5):211–8. https://doi.org/10.1302/2058-5241.1.000025.
Lonner JH, Pedlow FX, Siliski JM. Total knee arthroplasty for post-traumatic arthrosis. J Arthroplast. 1999;14(8):969–75.
Lunebourg A, Parratte S, Gay A, Ollivier M, Garcia-Parra K, Argenson J-N. Lower function, quality of life, and survival rate after total knee arthroplasty for posttraumatic arthritis than for primary arthritis. Acta Orthop. 2015;86(2):189–94. https://doi.org/10.3109/17453674.2014.979723.
Wasserstein D, Henry P, Paterson JM, Kreder HJ, Jenkinson R. Risk of total knee arthroplasty after operatively treated tibial plateau fracture: a matched-population-based cohort study. J Bone Joint Surg Am Vol. 2014;96(2):144–50. https://doi.org/10.2106/JBJS.L.01691.
Bergen MA, Ryan SP, Hong CS, Bolognesi MP, Seyler TM. Conversion total knee arthroplasty: a distinct surgical procedure with increased resource utilization. J Arthroplast. 2019;34(7):S114–20. https://doi.org/10.1016/j.arth.2019.01.070.
Kreitz TM, Deirmengian CA, Penny GS, Maltenfort MG, Deirmengian GK. A current procedural terminology code for “knee conversion” is needed to account for the additional surgical time required compared to total knee arthroplasty. J Arthroplast. 2017;32(1):20–3. https://doi.org/10.1016/j.arth.2016.06.040.
Liu Y, Zhao X-D, Zou C. Lingering risk: a meta-analysis of outcomes following primary total knee arthroplasty for patients with post-traumatic arthritis. Int J Surg. 2020;77:163–72. https://doi.org/10.1016/j.ijsu.2020.03.053.
Saleh KJ, Sherman P, Katkin P, et al. Total knee arthroplasty after open reduction and internal fixation of fractures of the tibial plateau: a minimum five-year follow-up study. J Bone Joint Surg Am Vol. 2001;83(8):1144–8. https://doi.org/10.2106/00004623-200108000-00002.
Weiss NG, Parvizi J, Hanssen AD, Trousdale RT, Lewallen DG. Total knee arthroplasty in post-traumatic arthrosis of the knee. J Arthroplast. 2003;18(3):23–6. https://doi.org/10.1054/arth.2003.50068.
Benazzo F, Rossi SMP, Ghiara M, Zanardi A, Perticarini L, Combi A. Total knee replacement in acute and chronic traumatic events. Injury. 2014;45:S98–S104. https://doi.org/10.1016/j.injury.2014.10.031.
Suzuki G, Saito S, Ishii T, Motojima S, Tokuhashi Y, Ryu J. Previous fracture surgery is a major risk factor of infection after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2011;19(12):2040–4. https://doi.org/10.1007/s00167-011-1525-x.
Massin P, Bonnin M, Paratte S, Vargas R, Piriou P, Deschamps G. Total knee replacement in post-traumatic arthritic knees with limitation of flexion. Orthop Traumatol Surg Res. 2011;97(1):28–33. https://doi.org/10.1016/j.otsr.2010.06.016.
Tanzer M, Makhdom AM. Preoperative planning in primary total knee arthroplasty. J Am Acad Orthop Surg. 2016;24(4):220–30. https://doi.org/10.5435/JAAOS-D-14-00332.
Parvizi J, Erkocak OF, Della Valle CJ. Culture-negative periprosthetic joint infection. J Bone Joint Surg Am Vol. 2014;96(5):430–6. https://doi.org/10.2106/JBJS.L.01793.
Lizaur-Utrilla A, Collados-Maestre I, Miralles-Muñoz FA, Lopez-Prats FA. Total knee arthroplasty for osteoarthritis secondary to fracture of the tibial plateau. A prospective matched cohort study. J Arthroplast. 2015;30(8):1328–32. https://doi.org/10.1016/j.arth.2015.02.032.
Dexel J, Beyer F, Lützner C, Kleber C, Lützner J. TKA for posttraumatic osteoarthritis is more complex and needs more surgical resources. Orthopedics. 2016;39(3):S36–40. https://doi.org/10.3928/01477447-20160509-11.
Scott CEH, Davidson E, MacDonald DJ, White TO, Keating JF. Total knee arthroplasty following tibial plateau fracture: a matched cohort study. Bone Joint J. 2015;97-B(4):532–8. https://doi.org/10.1302/0301-620X.97B4.34789.
Martín-Hernández C, Floría-Arnal LJ, Gómez-Blasco A, et al. Metaphyseal sleeves as the primary implant for the management of bone defects in total knee arthroplasty after post-traumatic knee arthritis. Knee. 2018;25(4):669–75. https://doi.org/10.1016/j.knee.2018.05.009.
Rai S, Liu X, Feng X, Rai B, Tamang N, Wang J, Ye S, Yang S. Primary total knee arthroplasty using constrained condylar knee design for severe deformity and stiffness of knee secondary to post-traumatic arthritis. J Orthop Surg Res. 2018;13(1):67.
Kolz JM, Stuart MB, Taunton MJ, Berry DJ, Yuan BJ, Abdel MP. Total knee arthroplasty after intramedullary tibial nail: a matched cohort study. J Arthroplast. 2020;35(7):1847–51. https://doi.org/10.1016/j.arth.2020.02.052.
Smith EJ, Heng M, Bedair HS, Melnic CM. Total knee arthroplasty following intramedullary tibial nailing. Knee Surg Relat Res. 2020;32(1):35. https://doi.org/10.1186/s43019-020-00055-2.
Wang XS, Zhou YX, Shao HY, Yang DJ, Huang Y, Duan FF. Total knee arthroplasty in patients with prior femoral and tibial fractures: outcomes and risk factors for surgical site complications and reoperations. Orthop Surg. 2020 Feb;12(1):210–7.
Tani I, Nakano N, Takayama K, Ishida K, Kuroda R, Matsumoto T. Navigated total knee arthroplasty for osteoarthritis with extra-articular deformity. Acta Ortop Bras. 2018;26(3):170–4. https://doi.org/10.1590/1413-785220182603178367.
Wong MT, Bourget-Murray J, Johnston K, Desy NM. Understanding the role of total knee arthroplasty for primary treatment of tibial plateau fracture: a systematic review of the literature. J Orthop Traumatol. 2020;21(1):7. https://doi.org/10.1186/s10195-020-00546-8.
Kini SG, Sathappan SS. Role of navigated total knee arthroplasty for acute tibial fractures in the elderly. Arch Orthop Trauma Surg. 2013;133(8):1149–54. https://doi.org/10.1007/s00402-013-1792-8.
Wui NB, Anuar MAA, Wahid AMA. Short-term outcome of early primary total knee arthroplasty for fractures around the knee in the elderly population: the experience of a secondary healthcare centre in Malaysia. Malays J Med Sci. 2020;27(4):64.
Appleton P, Moran M, Houshian S, Robinson CM. Distal femoral fractures treated by hinged total knee replacement in elderly patients. J Bone Joint Surg. 2006;88-B(8):1065–70. https://doi.org/10.1302/0301-620X.88B8.17878.
Davis JT, Rudloff MI. Posttraumatic arthritis after intra-articular distal femur and proximal tibia fractures. Orthop Clin N Am. 2019;50(4):445–59. https://doi.org/10.1016/j.ocl.2019.06.002.
Bettin CC, Weinlein JC, Toy PC, Heck RK. Distal femoral replacement for acute distal femoral fractures in elderly patients. J Orthop Trauma. 2016;30(9):503–9. https://doi.org/10.1097/BOT.0000000000000600.
Haufe T, Förch S, Müller P, Plath J, Mayr E. The role of a primary arthroplasty in the treatment of proximal tibia fractures in orthogeriatric patients. Biomed Res Int. 2016;2016:1–5. https://doi.org/10.1155/2016/6047876.
Lee G-C. A systematic approach to primary non-hinged knee replacement in patients with comminuted periarticular fractures about the knee. Univ Pa Orthop J. 2010;20:88–91.
Buechel FF. Knee arthroplasty in post-traumatic arthritis. J Arthroplast. 2002;17(4):63–8. https://doi.org/10.1054/arth.2002.32809.
Papadopoulos EC, Parvizi J, Lai CH, Lewallen DG. Total knee arthroplasty following prior distal femoral fracture. Knee. 2002;9(4):267–74. https://doi.org/10.1016/S0968-0160(02)00046-7.
Shearer DW, Chow V, Bozic KJ, Liu J, Ries MD. The predictors of outcome in total knee arthroplasty for post-traumatic arthritis. Knee. 2013;20(6):432–6. https://doi.org/10.1016/j.knee.2012.12.010.
Ge DH, Anoushiravani AA, Kester BS, Vigdorchik JM, Schwarzkopf R. Preoperative diagnosis can predict conversion total knee arthroplasty outcomes. J Arthroplast. 2018;33(1):124–129.e1. https://doi.org/10.1016/j.arth.2017.08.019.
Parratte S, Bonnevialle P, Pietu G, Saragaglia D, Cherrier B, Lafosse JM. Primary total knee arthroplasty in the management of epiphyseal fracture around the knee. Orthop Traumatol Surg Res. 2011;97(6):S87–94. https://doi.org/10.1016/j.otsr.2011.06.008.
Bala A, Penrose CT, Seyler TM, Mather RC, Wellman SS, Bolognesi MP. Outcomes after total knee arthroplasty for post-traumatic arthritis. Knee. 2015;22(6):630–9. https://doi.org/10.1016/j.knee.2015.10.004.
Abdel MP, von Roth P, Cross WW, Berry DJ, Trousdale RT, Lewallen DG. Total knee arthroplasty in patients with a prior Tibial plateau fracture: a long-term report at 15 years. J Arthroplast. 2015;30(12):2170–2. https://doi.org/10.1016/j.arth.2015.06.032.
Kester BS, Minhas SV, Vigdorchik JM, Schwarzkopf R. Total knee arthroplasty for posttraumatic osteoarthritis: is it time for a new classification? J Arthroplast. 2016;31(8):1649–1653.e1. https://doi.org/10.1016/j.arth.2016.02.001.
Saleh H, Yu S, Vigdorchik J, Schwarzkopf R. Total knee arthroplasty for treatment of post-traumatic arthritis: systematic review. WJO. 2016;7(9):584. https://doi.org/10.5312/wjo.v7.i9.584.
Khoshbin A, Stavrakis A, Sharma A, et al. Patient-reported outcome measures of total knee arthroplasties for post-traumatic arthritis versus osteoarthritis: a short-term (5- to 10-year) retrospective matched cohort study. J Arthroplast. 2019;34(5):872–876.e1. https://doi.org/10.1016/j.arth.2019.01.022.
Brockman BS, Maupin JJ, Thompson SF, Hollabaugh KM, Thakral R. Complication rates in total knee arthroplasty performed for osteoarthritis and post-traumatic arthritis: a comparison study. J Arthroplast. 2020;35(2):371–4. https://doi.org/10.1016/j.arth.2019.09.022.
Houdek MT, Watts CD, Shannon SF, Wagner ER, Sems SA, Sierra RJ. Posttraumatic total knee arthroplasty continues to have worse outcome than total knee arthroplasty for osteoarthritis. J Arthroplast. 2016;31(1):118–23. https://doi.org/10.1016/j.arth.2015.07.022.
Stevenson I, McMillan TE, Baliga S, Schemitsch EH. Primary and secondary total knee arthroplasty for tibial plateau fractures. J Am Acad Orthop Surg. 2018;26(11):386–95. https://doi.org/10.5435/JAAOS-D-16-00565.
El-Galaly A, Haldrup S, Pedersen AB, Kappel A, Jensen MU, Nielsen PT. Increased risk of early and medium-term revision after post-fracture total knee arthroplasty: results from the Danish Knee Arthroplasty Register. Acta Orthop. 2017;88(3):263–8. https://doi.org/10.1080/17453674.2017.1290479.
Weiss NG, Parvizi J, Trousdale RT, Bryce RD, Lewallen DG. Total knee arthroplasty in patients with a prior fracture of the tibial plateau. J Bone Joint Surg Am Vol. 2003;85(2):218–21. https://doi.org/10.2106/00004623-200302000-00006.
Kornah BA, Safwat HM, Abdel-hameed SK, et al. Managing of post-traumatic knee arthritis by total knee arthroplasty: case series of 15 patients and literature review. J Orthop Surg Res. 2019;14(1):168. https://doi.org/10.1186/s13018-019-1180-3.
Putman S, Argenson J-N, Bonnevialle P, et al. Ten-year survival and complications of total knee arthroplasty for osteoarthritis secondary to trauma or surgery: a French multicentre study of 263 patients. Orthop Traumatol Surg Res. 2018;104(2):161–4. https://doi.org/10.1016/j.otsr.2017.11.019.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Natesan, R., Dhanasekaran, S. (2022). TKA in Post-Trauma and Failed Fixations. In: Sharma, M. (eds) Knee Arthroplasty. Springer, Singapore. https://doi.org/10.1007/978-981-16-8591-0_16
Download citation
DOI: https://doi.org/10.1007/978-981-16-8591-0_16
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-16-8590-3
Online ISBN: 978-981-16-8591-0
eBook Packages: MedicineMedicine (R0)