Abstract
Most of the anticancer drugs affect both the cancerous cells and the normal cells. The most common treatment chemotherapy is always associated with the poor selection of the targeted cancer cells and also the drug resistance. Therefore, to enhance the therapeutic efficacy of anticancer drugs, nano-drug delivery systems have been designed and implemented. To limit the challenges associated with the conventional chemotherapy, there are strategies to combat it. The strategies are functionalising the material, functionalisation with multiple targets, in vivo imaging and dual/multiple drug delivery system. This chapter provides insights about the wide range of polymers which helps to engineer the anticancer molecules. It also emphasises the different mechanisms for releasing the anticancer drugs in an effective manner. The recent advances about the materials used for cancer therapy and commercially available products are also discussed. The effect of engineered biomaterials for treating the cancer patients is mostly expected to increase in the future.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Cancer is the most major disease in the world with huge number of death due to exposure of carcinogenic substances, change in diet, age, suppression in the immune system and other factors [1]. In the recent years, a lot of progress has been taken place in developing a targeted delivery system. By these effective treatments, the survival rate of patients will be increased and still some of the disadvantages occurs. The chemotherapy treatment acts non-specifically in the cancerous cells and also in the normal cells because of the toxic side effects. Moreover, a high dose is required for some of the patients at regular intervals to improve the therapeutic efficacy in the targeted area [2, 3]. The recent advancements of the biomaterials incorporated delivery system provide the specific release of the anticancer agents only in the cancerous cells by subsequently improving the life of patients and its side effects are eliminated [4].
There have been a lot of developments in the recent years for the treatment of cancer are formulations of controlled delivery system, targeted delivery systems and nano-drug delivery system. Formulating a biomaterial with a controlled or targeted release is quite challenging task and needs a multidisciplinary approach [5, 6]. There are certain parameters to develop the formulation and they are incorporating the sufficient drug within the biomaterial for the controlled and prolonged release to achieve better efficacy. Secondly, to protect the drug in the human environment (in vivo) to increase the biological activity. Thirdly, formulating a drug by predicting its release behaviour to improve its therapeutic efficacy which ranges from weeks to years. Fourthly, the drug component and the biomaterials should be biocompatible and nontoxic within the system. Fifthly, the developing material should avoid the discomfort before and during administration. Finally, the drug-biomaterial formulation should be affordable to the patients which are most important factor to taken into account before designing the formulation [7, 8].
There is strong growth in developing biomaterials for the controlled/targeted release of anticancer drugs by imbibing different types of mechanisms which is not confined to diffusion, swelling, magnetic and chemical-based mechanisms [9,10,11]. There are formulations which consist of phospholipids with bilayer structures that lead to the preparation of liposomes and it is one of the nanocarrier delivery systems. This then expanded into many carriers such as micelles, nanospheres, nanomaterials, dendrimers and inorganic nanoparticles in the rapidly increasing field of nano-drug delivery system. The biomaterials and the drug can also be modified by microfabrication technology to formulate patches consisting of microneedles which pierce the skin without pain to deliver the drug. This transdermal delivery system allows the drug to improve the permeability in skin, it should dissolve, should be biodegradable and should not leave any waste. Very recently, there are smart and intelligent biomaterials have been developed which responds to the environmental factors (pH, enzymes, temperature and pressure) for releasing the drug. Likewise, there are biomaterials which can be triggered by UV-Vis light, NIR light, sound, electrical currents and by means of magnetic pulse for delivering the drugs in controllable pace [12,13,14,15,16].
In this chapter, the importance and the need for the incorporation of biomaterials in the drug delivery system are explained. An outline of the natural, synthetic and combination of both natural and synthetic materials used for the development of the targeted delivery system is also highlighted. The recent advancements in the design, development and preparation of hybrid materials are also described. Lastly, the significance of the polymeric materials incorporated in the targeted system and commercially available products are also presented.
2 Classes of Biomaterials for Anticancer Activity
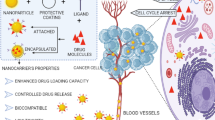
There is a broad array of polymers used as carrier for the anticancer compounds and this includes natural, synthetic and hybrid classes (Fig. 1). In the synthetic class, organic and inorganic materials are used, and this section deals with the physical, chemical properties and mechanisms of drug delivery of individual class of carriers. The natural source of biomaterials comes from both the animals and the plants which includes collagen, alginates, hyaluronic acid, silk fibroin, chitosan and others. The synthetic classes of biomaterials include poly(ethylene glycol) (PEG), polylactides, polyglycolide and its derivatives. Then, the hybrid materials include PEG-alginates, PEG-proteins and others [17].
3 Natural Biomaterials
In the tumour stroma, there are natural proteins which occur in the tumour stroma which increases the formation of tumour in the cancerous cell through interactions of physicochemical properties. Those proteins include fibrin, collagen and laminin, and to improve the biochemical nature of the extracellular matrix (ECM) proteins, these natural biomaterials are used and they are explained below;
3.1 Collagen
The most important biomaterial is hydrogels and they occur in the crosslinked chains of collagen with a high amount of absorption of water and also it facilitates the exchange of nutrients. This is one of the natural proteins found in abundance in the ECM protein which occurs in the tumour stroma and it provides mechanical strength to the tissue [18]. Moreover, the biochemical and mechanical properties of the hydrogels are improved by changing the crosslinking behaviour or the individual polymer chains. The bioactive components, growth factors and metalloproteases are incorporated in the hydrogel matrix for the encapsulation of the drugs. Therefore, these hydrogels are formulated by mechanical, chemical and structural means in particular to change the behaviour of the cells and to provide targeted delivery [19]. The hydrogels were prepared with the collagen which are formed through a physical crosslinking and they are used for the encapsulation of the anticancer drugs. Through enzymatic crosslinking the collagen-based gels have been prepared with the enzyme transglutaminase. These hydrogels are used against the MDA-MB-231 metastatic cells which are breast cancer cells and it forms tissue hypoxia and necrosis. In the case of MCF-7, a non-metastatic breast cancer cells it exhibits epithelial–mesenchymal transition (EMT) markers. Owing to its fibril nature, they have been widely used to study the migration of bioactive moieties through the diameter of fibril, pores and crosslinking density. The elastic modulus and the alignment of the fibres in the collagen matrix are responsible for the release behaviour [20]. For example, an increase in the collagen density leads to mechanical stiffness which leads to invasion of malignant cells. This kind of collagen hydrogels is used against the epithelial organoids and tumour spheroids which invades through adhesion by integrin [21].
3.2 Alginates
They are natural biomaterial which are derived from the seaweeds and it has been used as gel for the controlled delivery of anticancer drugs. They have α-l-guluronic and β-d-mannuronic acid in the structure and it involves in the ion-exchange reaction for the release of the bioactive components. The advantages of using alginates and agarose as carrier are they have high porosity and high water holding capacity [22]. Agarose is also similar to alginates which has d-galactose and 3, 6-anhydro-l-galactopyranose in its structure. The physicochemical properties of these biopolymers such as molecular weight, pH, ionic strength, mechanical strength, porosity can be tuned by modifying the concentration of the two structural units. These two polymeric gel can be used as encapsulating agent for the cancer drugs because of its thermal stability. Alginates incorporated bioactive moieties are used against breast cancer cells, leukaemic cells and squamous cell carcinoma. The alginates have very good mechanical stiffness which ranges from 21 kPa to 105 kPa and this characteristic property destroys the tumourigenic potential of hepatocellular carcinoma. Agarose is used against the renal carcinoma cells and MCF-7 cancer cells [23,24,25].
3.3 Hyaluronic Acid (HA)
It is a high molecular weight biopolymer and it consists of the repeating units of d-glucuronic acid and d-N-acetyl glucosamine. Because of its presence in the ECM matrix, this HA have been widely used as carrier for the anticancer moieties. The molecular weight of hyaluronic acid (0.5–2 MDa) and its interaction with the tissues are the main determining factors for the release of the active moieties in the cells. In a study, the ultra-high molecular weight (6–12 MDa) of HA leads to an invasion of cancer cells due to the decrease in activity of degrading enzymes of HA. The molecular weight of HA is reliant on the comparative activity of HA synthases and they are denoted as HAS1, HAS2 and HAS3 which specifically synthesis HA of different molecular weights [26]. The hyaluronidase activity (HYAL1, HYAL2) is the one in which it breaks the HA high molecular weight into small chains HA in the ECM matrix. In an another study, they have found that the higher levels of HA low molecular weight along with the higher levels of HAS1, HAS2, HYAL1, HYAL2 exhibited an invasion of breast cancer cells [27].
Anticancer drugs encapsulated HA hydrogels (0.5–1.3 MDa) forms a cluster formation by the hyaluronidase enzyme which involves in destroying the cancer cells. HA with the molecular weight of 500 kDa along with the thiol and acrylate groups forms the hydrogel bilayer constructs which were used to invade the prostate cancer cells. HA with molecular weight >1 MDa forms a reticulated hydrogels which is combined with the adipic dihydrazide were used to destroy the primary tumours based on its secretion of hyaluronidase. HA hydrogel with molecular weight ~1.5 MDa along with the tyramine were used to attack CD44 and CD133 of U87 astrocytoma cells. Therefore, for choosing HA, the physicochemical and biological properties should be optimised cautiously to study the cell reaction through tissue-matrix interactions [28,29,30].
3.4 Chitosan
This is obtained from the polymer chitin and they are used for many biomedical applications starting from sutures to implants [31]. The chitosan films were impregnated with the paclitaxel and it is implanted in the tumour site to obtain the sustained release behaviour. The release profile shows an initial burst effect and this chitosan offers a high loading capacity of about 31% W/W. The further release behaviour shows the sustained delivery of paclitaxel and the film lost its integrity by the biodegradation mechanism. There is no inflammatory response of this biopolymer films and its biodegradation behaviour helps in the delivery of implantable anticancer drugs [32]. Chitosan is used in many anticancer treatments and the examples include chitosan-doxorubicin for chemo-immunotherapy [33], chitosan-cisplatin used for pleural mesothelioma [34] and chitosan-letrozole for the breast cancer treatments [35].
3.5 Cellulose
This is another kind of biocompatible biopolymer used as carrier for biomedical applications [36]. In a clinical study, cisplatin was administered for treatment of glioblastoma multiforme. For this, they have used biodegradable carbomethylcellulose biopolymer is incorporated with the cisplatin drug and they have administered as chemotherapy (polymer-drug) for 17 patients. After the removal of the tumour cells, the polymer-drug plates were implanted into the tumour area and they have found that the total survival rate of patients increased (427.5 days), whereas for patients from the control group is 211 days [37]. In another study, cellulose sulphate is encapsulated in the genetically modified cells and they were implanted in the tumour site for the treatment of pancreatic cancer. The cytochrome P450 2B1 enzyme modified the cells and it could able to modify the cancer drug ifosfamide to its toxic metabolites. By this method, the tumour cells were ablated completely and it shows an example of in situ mechanism [38].
3.6 Cyclodextrins (CD)
It consists of 6–8 glucopyranoside unit which are interconnected and they are used as carriers for many bioactive molecules [39, 40]. It contains a hydrophilic part in the outer region and the hydrophobic part in the inner region and this type of shape creates an inclusion complex between the CD and the hydrophobic anticancer drugs. β-CD are covalently linked with the amino acid poly-l-lysine and anticancer drug risedronate which is used for the treatment of bone cancer [41, 42]. Manchun et al. demonstrated about the dextrin nanogels incorporated doxorubicin and they have formulated by an emulsion method. Using a cross-linker glyoxal and formaldehyde, the doxorubicin was bonded (acid labile bond) to the CDs. They have also found that the release of doxorubicin is a pH responsive and it delivers the drug at pH-5 which is the pH of the cancer cells. The obtained nanogels were effective for destroying the colorectal cancer cells nuclei and the side effects were reduced [43, 44].
3.7 Silk
Silk fibroin is used as a suitable biomaterial since long time for biomedical applications [45, 46]. There are a lot of advantages and some of them are it has extremely good mechanical and elastic properties, good immune behaviour, biocompatible, biodegradable and very low adherence to bacterial cells. These proteins can be developed into films without any difficulty, and the films act as a carrier for the anticancer moieties. In a study, they have prepared silk fibroin hydrogels and doxorubicin was incorporated into it and they observed a good loading efficiency. The self-assembling nature of the silk showed extraordinary anticancer activity [47, 48]. One of the reported works suggests that the cell-specific and site-specific delivery of doxorubicin was achieved by the silk-doxorubicin matrix films. These films are used for the treatment of advanced stage of breast cancer and their results of the in vivo studies proves that it showed an exceptional improvement in inhibiting the cell growth when compared to the control. In addition, they have also identified huge reduction in the tumour cells weight and the tumour spread was also reduced with no toxic effects in the normal cells [49,50,51]. For treating the not resectable neuroblastoma cells, the silk fibroin films were loaded with doxorubicin and crizotinib. It forms a crosslinking between the drug and the film which showed an outstanding results in treating the unresectable neuroblastoma cells. It is also reported that it exhibited an excellent activity in the in vitro and in vivo studies when compared to the intravenous dose of drugs. Moreover, it also displayed a good release profile with desirable kinetics and can be directly placed over the tumour surface [52,53,54]. It was also reported in a study that they have combined the surgery along with the drug loaded silk films to treat the neuroblastoma cancer cells. It was stated that the drug release was observed in the sustained manner, and thereby during shrinkage of cells, it was removed surgically. Recently, silk fibroin nanospheres were fabricated along with the incorporation of floxuridine for the prevention and treatment of cancer cells. Nanogels silk elastin was loaded with floxuridine for the treatment of hepatocellular carcinoma [55, 56].
4 Inorganic Biomaterials
4.1 Titanium and Selenium
The titanium is one of the most used metals in the development of implants owing to its many advantages like good mechanical strength [57], resistant to corrosion properties, biocompatible and time-dependent biodegradable behaviour [58]. The implant consists of a layers of titanium oxide and it is implanted over the surface of the cancerous bone. The orthopaedic implant will replace the cancerous bone cells and it is the common method adopted to treat bone cancer. The titanium alone cannot able to prevent the cancer cells, and hence the anticancer drugs are incorporated in the titanium dioxide layers by surface modification technique [59,60,61]. For supporting the above-said statement, Perla et al. found two strategies to develop the new type of bone implants. The first one is modifying the surface of the implants by using nanosize range of particles particularly to improve the adhesion and growth rate. The second one modifying the surface through chemical means by using metal particles exhibiting anticancer properties. The one such inorganic material which has anticarcinogenic potential is selenium. They observed improved adhesion of osteoblasts cells in the surface modified selenium and nanoparticles matrix. It was reported that selenium nanoparticles found to be a promising material for the anticancer orthopaedic implants [62].
Tran et al. used nanoselenium along with the titanium and found that it inhibits the growth of cancerous cells from recurrence simultaneously improving the growth of bone. In the in vivo experimentation, the Se-coated Ti nanoparticles were observed to be a promising material for the tumourous bone cells and also for the healthy cells [63,64,65]. Chen et al. came up with a new modification in the surface of the titanium. They have formulated a chitosan coated over the surface of nano-titania tubes and deposited selenium on the surface of nanotubes. They have studied its efficacy by implanting this material and observed that it prevents the growth of cancerous cells and improves the proliferation of healthy cells. In addition, they have also shown that selenium exhibits sustained release behaviour of about twenty-one days. Titanium nanowires and titanium nanotubes are incorporated with doxorubicin drug for treatment of brain cancer (doxorubicin implants) [66]. Gulati et al. demonstrated that this novel nano-metal-drug conjugates were successful in the prevention of brain tumour. The loading efficiency and the release profile of the doxorubicin showed better characteristics. The added advantage of this method was it could able to bypass the blood-brain barrier which actually prevents the release of doxorubicin from the blood and thereby releases the drug in the brain [67].
4.2 Calcium Phosphate
The calcium phosphate biomaterial is very similar to the bone mineral in its composition and this biomaterial itself acts as an anticancer agent. This biomineral also offers several advantages and they are osteoconductive, biocompatible and biodegradable based on its porosity, bioactive, nontoxic and stable. The most commonly used calcium phosphate-based biomaterials are tricalcium phosphate, hydroxyapatite and amorphous calcium phosphate [68,69,70,71,72]. Cisplatin is incorporated in the bone mineral and studied its release behaviour. The release pattern followed the sustained release behaviour and it was observed for nearly 12 week period under in vitro conditions. The in vivo behaviour of this implanted material of about 3 months shows good compatibility and better release profile [73]. Then, in another study, they have used hydroxyapatite material which is incorporated with adriamycin and it was found that hydroxyapatite (2 mm diameter) can load about 0.08 of adriamycin. The in vivo studies revealed that the implanted composites exhibited sustained release behaviour and used in the treatment of early stage hepatic cancer whereas for the late stage it was unresectable. After resection of tumour, the bone mineral containing high concentration of anticancer drug was placed in the tumour site for improving the cells present in the site. Likewise, the calcium phosphate mineral loaded with cis-diaminedichloroplatinum and the release profile was observed to be 0.1 mg/day. After implantation of over six weeks, the platinum release was 3200 μg/g tissue which was found accumulated in bone marrow whereas it was not present in other organs. When the platinum is administered intravenously, the concentration of platinum is very low in bone marrow 0.2 μg/g tissue and it was lower than that of liver 3.5 μg/g tissue and kidneys 3.5 μg/g tissue [74]. The composites showed that the concentration of platinum at the tumour site is higher than that of other tissues and organs. This idea was taken by Tanzwa et al. prepared a composite containing calcium phosphate loaded with caffeine and the cisplatin. Here, the cisplatin release was improved in the tumour site because of the presence of caffeine which holds the cisplatin in the tumour site [75]. Recently, Chen et al. developed a polycaprolactone scaffold along with chitosan, nanoclay and β-tricalcium phosphate loaded with doxorubicin for the controlled delivery of the drug in the tumour site [76].
4.3 Silica
This biomaterial is related with the breast implants and they are also used for drug delivery applications. They are hydrophobic material which are used as membrane-based reservoir systems [77]. The first work on silicone-based anticancer drug delivery was introduced by Ueno. The selected anticancer drug 1,3-bis(2-chloroethyl)-1-nitrosourea (BCNU) is incorporated in the different types of silica, silicone and silicone-nylon refillable systems. In this work, they have selected silicone balloons as a reservoir for the drug and it is used for the treatment of ocular malignancies [78].
Nanoporous silica was developed by Bell et al. and he reported that because of its solubility, biocompatibility, biodegradability and low toxicity, and it has very wide range of biomedical applications [79]. The applications include biosensors [80], chemical sensors [81], radiotherapy [82], drug delivery and biotechnological applications [83,84,85,86]. The porous silica nanoparticles are used for delivering anticancer drugs like doxorubicin [87, 88], cisplatin [89], celastrol [90] and camptothecin [91]. Therefore, the biodegradation pathway of nanosilica particles paves the way to remove safely from the body [92]. Tzur et al. investigated the porous nanosilica films loaded with the anticancer agent mitoxantrone dihydrochloride for the local drug delivery. The drug was loaded into the nanostructured silica by means of alkylation and thermal hydrosilylation using undecylenic acid and dodecene. And the drug was adsorbed and covalently linked to the porous nanosilica scaffold. The release pattern exhibited no burst effect initially followed by the sustained delivery of mitoxantrone in the breast cancer site. They have also denoted that it can be further developed either into injectable nanosilica particles or implantable material [93, 94].
5 Synthetic Biomaterials
5.1 Carbon Nanotubes (CNTs)
There has been extensive research in using the carbon nanotubes structures as a nanocarrier for numerous biomedical applications. The CNTs are said to be a universal carrier for a large number of bioactive molecules [95]. The CNTs containing immobilised drug can be combined with the nanoparticles containing magnetic properties and this hybrid structures releases the drug via the external magnetic field for targeting the cancer cells [96]. Functionalising the CNTs and surface modifications are another way of releasing the drug in the target site. The oxidised CNTs are difunctionalised using folic acid and iron nanoparticles which are useful in dual targeting [97, 98]. Doxorubicin drug is incorporated into the dual targeted nanocarrier CNTs and found the controlled release behaviour. The in vitro studies prove that the difunctionalised CNTs-doxorubicin act against the HeLa cells. It was also reported that CNTs exhibit improved doxorubicin loading capacity and it provides 6 times better release profile than the free drug. When the CNTs functionalised with folic acid and it is particularly useful in targeting the lymphatic systems through the external stimuli magnetic field. The externally place magnet will target the lymph nodes and releases the drug cisplatin and 5-fluorouracil in a controlled fashion [99, 100]. The natural bioactive compound quercetin is incorporated in the CNTs nanocarrier and they are formulated by polymerisation of methacrylic acid around CNTs. Then, the quercetin drug was found to be covalently conjugated which showed a better release profile. The in vitro studies proved that it acts against the HeLa cells effectively than the free quercetin. The quercetin was particularly loaded in nanocarrier CNTs particularly to improve the stability and release profile [101].
5.2 Graphene
An interesting nanomaterial which provides many advantages since its inception and they are graphene-based materials (GBMs) and in particular graphene oxide (GO) and reduced graphene oxide (rGO) [102]. The GO and rGO attracted much interest in the last few years for the development of drug delivery systems and in many biomedical applications [103]. There are lot of studies reported that it has toxic potential based on its size and amount used. But the side effects produced from GBMs are very low compared to the chemical molecules. Huge number of reports studied that GBMs was used as nanocarrier for many anticancer drugs [104,105,106,107]. Zhang et al. study reported that GO functionalised with folic acid in particular to target the MCF-7 cells. Doxorubicin and camptothecin are loaded in the GO through hydrophobic and π–π interactions. The effects showed that it targets specifically to the cancer cells with higher loading and better release properties [108]. Wu et al. studied the effects of doxorubicin-GO-Adramycin complex and found a good loading capacity of about 93.6%. They revealed that doxorubicin undergoes a pH mediated release in a controlled fashion and found effective in killing breast cancer cells. The pH mediated release is that the hydrogen bonding between the GO and doxorubicin is dissociated and protonated –NH2 groups in the doxorubicin molecule [109].
5.3 Poly(Lactic Acid) (PLA)
PLA has a lot of advantages and they are biocompatible, biodegradable, easily processable and nontoxic. PLA and its product poly(d,l-lactide-coglycolide) (PLGA) have been used since its inception in many pharmaceutical products for biomedical applications and these polymers are approved by FDA [110]. Zhao et al. used recombinant drug interleukin-2 and it is conjugated with PLA/PLGA microspheres along with dextran. The microspheres were prepared with a core/shell morphology with the loaded drug and this was used for the treatment of paracrine cancer. When the interleukin-2 was administered multiple injections, it has been proved that the rate of growth inhibition of the cancer cells was higher. The l-lactide and g-lactide with the dextran molecules form the stereocomplex which undergoes gelation and releases the drug in controlled fashion [111]. PLA nanofibres along with sodium dichloroacetane and diisopropylamine dichloroacetate loaded with the oxaliplatin and studied its release profile. It was reported that it has good loading efficiency and release profile. The in vivo studies showed that prolonged release behaviour of oxaliplatin in tumour site and it also completely inhibit the growth and limits the recurrence of tumour in the liver. The suppression rate of the tumour was observed to be 95% and its asymmetric structure enables in diffusion of oxaliplatin in normal cells and other tissues [112, 113].
5.4 Poly(Ethylene Glycol) (PEG)
Mostly, the anticancer drugs are incorporated in the PEG as hydrogel formulation [114,115,116]. Hydrogels are powerful structures and are widely used in smart drug delivery systems because its delivers the drug inside the system through the changes in the pH, light, temperature and sound. They also have all the advantages in which the carrier molecules should possess and they biocompatible, biodegradable and nontoxic. When the drug is incorporated in the system, it changes from the liquid state to gel state by means of chemical interactions such as hydrogen bonding, crosslinking, hydrophobic–hydrophilic, charge, sterocomplexation, photo-polymerisation and molecular recognition. When the drug loaded hydrogels are implanted in the tumour site, it releases the drug via diffusion coefficient mechanism. PEG are formulated into a hydrogel delivery system for many biomedical applications [117,118,119,120]. 5-fluorouracil is loaded into the PEG hydrogels which are used to prevent the growth the malignant tumours. The in vivo studies shows that when the drug was administered via bolus injection, the release rate was very poor and leads to short half-life. Whereas the hydrogel formulation showed that it increases the drug residence time and half-life of the drug was observed to be satisfactory [121]. In order to increase the desired properties of PEG, it is to be copolymerised with the other molecules such as poly(methyl methacrylate)(PMMA) [122], poly(vinyl ether) [123], poly(styrene) [124]. In a study, they have incorporated polycaprolactone (PCL), PLGA into the PEG system and it undergoes crosslinking through gelation process. The crosslinking takes place when the temperature is increased and resulted in aggregation of the hydrophobic portion of the molecule [120]. In a study by Cheng et al., they have formulated hydrogels composed of triblock copolymers consists of poly(γ-ethyl-l-glutamate)–poly(ethylene glycol)–poly(γ-ethyl-l-glutamate) and incorporated the drug paclitaxel. The in vivo studies demonstrated that within 3 weeks of time, it completely prevents the growth of tumour without damaging the other tissues and cells [125]. In another study, PEG was formulated in the micellar structures along with the 2,2-bis(methylo)propionic acid loaded with the drug paclitaxel. The in vivo experimentation showed that it inhibits the growth of tumour cells. Nanoparticle delivery system was developed by combining PEG and poly(propylene succinate). Then, it is loaded with the drug cisplatin and it was found to be controlled delivery of drug in the tumour site and thereby preventing the growth of malignant cells [126].
5.5 Poly(ɛ-Caprolactone) (PCL)
This polymer also possesses many advantages like biocompatible, biodegradable, nontoxic and no side effects [127, 128]. This is widely used in situ forming drug delivery system and this polymer along with its copolymer poly(ɛ-caprolactone fumarate) loaded with tamoxifen is formulated into injectable preparation. The in vitro studies show that it shows a higher loading efficiency, excellent release rate and it prevents the growth of breast cancer cells against MCF-7 cells. They have also reported that the composites do not display no toxicity, no cytotoxicity in normal cells and tissues [129]. PCL was also formulated into implants together with its copolymers such as derivative poly(ethylene glycol)-block-poly(ε-caprolactone). This PCL and copolymer nanoparticles were loaded with hydroxypropyl-β-cyclodextrin and docetaxel drugs. These implants were placed over the patients having breast adenocarcinoma and found outstanding anticancer activity. Therefore, these PCL-based nanoparticle implants were proven to be suitable for the anticancer therapy [130]. Pereira et al. developed PCL incorporated methotrexate and found it effective for the treatment of Ehrlich solid tumour cells [131]. PCL was formulated into nanofibres and the natural bioactive compound curcumin was incorporated into it. This curcumin loaded PCL fibres were tested against MCF-7 and A459 cells and found better entrapment efficiency which leads to be effective in killing the breast cancer cells and lung cancer cells [132]. PCL along with curcumin was developed into micellar formulation and both the in vitro and in vivo studies displays that they are very effective in treating colon cancer cells [133]. Recently, Wong et al. developed a formulation containing dual functions in which it serves in treating the cancer cells and as well as in tissue regeneration. In this study, PCL was loaded with doxorubicin where it acts in dual functions such as locally delivering the drug in the tumour site and cells get attached for generating new tissues. They have suggested that this kind of drug loaded nanofibres formulation will be very useful in post-surgery of the limb salvage process for repairing the tissues [134].
5.6 Polyanhydrides
This polymer is one perfect example in the category of surface eroding polymers owing to its high water content of the anhydride bonds over the surface and highly hydrophobic in the bulk of the polymer [135]. In this type of polymers, the release of the drug is directly proportional to the erosion rate of the polymer. So, to achieve the control in release of a drug is possible only when the surface of the biomaterial starts degrading. The in vivo experiments suggest that polyanhydride can be easily excreted from the body via urine and faeces as CO2 [136]. This biomaterial was together mixed with its copolymer poly[bis(pcarboxypenoxy) propanesebacic acid] for the local delivery of cancer drugs which was also approved by the FDA. In this matrix, the drug camptothecin was incorporated to study the effects in treating gliosarcoma. The results showed that the release rate was prolonged for about 1000 h [137]. Poly(ester anhydride) along with oligomers of poly(sebacic acid) and ricinoleic acid was studied for its possibility of selecting as drug carrier. To the above polymers, the cisplatin drug was loaded and studied that it was very effecting in inhibiting the growth of cancer cells. The above-said polymers are incorporated with 5-fluorouracil, paclitaxel and methotrexate to find out the release rate. The release profile was found to be very effecting and showed prolonged release [138,139,140]. Recently, curcumin was loaded in the poly(anhydrides) for the prevention of growth against breast cancer cells, osteoblasts cells and HeLa cells. This polymer has also been used for improving the immune response inside the body by the vaccine delivery formulation [141].
5.7 Polyurethanes (PU)
This is one of the synthetic polymers which also has good biocompatibility, biodegradability, good mechanical strength and nontoxic [142, 143]. Chen et al. developed polyurethanes nanocomposite implants loaded with the drug paclitaxel. It releases the drug with tunable on and off switching mechanism for delivering to the tumour site. The temperature-responsive PU nanocomposite membrane releases the drug by heating at 44 ℃ (switching on) and drops at 37 ℃ (switching off) results in temperature-responsive release [144]. Another work reported about the solvent casted PU along with paclitaxel drug to make stent-based delivery system for the treatment of tumours in the gastrointestinal area. The PU-paclitaxel stent could able to inhibit the growth of tumour in a better way and its release was inversely proportional to the paclitaxel loading. The major threat to a patient who underwent tumour removal surgery is that it increases the growth in other normal cells [145]. To cure this problem, Manabe et al. came with a new device, i.e. infusion pump with elastomeric tube which delivers the drug gemcitabine directly into the resected tumour site and the tube is used for reloading the drug. The controlled delivery of the gemcitabine drug inhibits the growth, slows down the growth and also prevents regrowth of the tumour [146].
5.8 Conducting Polymers
Mostly, these kinds of polymers are used in electronics, but these kinds of polymers also used as fascinating materials for the drug delivery system [147, 148]. The conducting polymers are not biodegradable and its degradability is increased by chemical modification. So that the polymers become biodegradable with the in vivo enzymes reaction. These polymers are biocompatible, which allows ion-exchange reactions, electrically conductive which undergoes charging and discharging process [149, 150]. With the help of electric potential, the drugs with anionic charge get immobilised during the process of oxidation and the drugs get released during reduction process which is called as charging-discharging potential of polymer [151]. There are many reported works of this kind of polymer as reservoir for many drugs (ibuprofen [150], salicylate [152], dexamethasone [153] and ciprofloxacin [154, 155]) where they get released inside the system with the help of electrical stimuli. Few years back, scientists have started using this type of polymers as reservoirs for delivering anticancer drugs. They have used a conducting polymer polypyrrole loaded with methotrexate along with oleanolic acid making the system electrochemically active. The kinetic analysis exhibited that methotrexate release was sustained by means of both temperature and electrical stimuli [4]. In another study, authors have used a different type of conducting polymer poly(3,4-ethylenedioxythiophene) as reservoir for releasing methotrexate drug. The in vitro experimentation proved that it acts against the A-549, HeLa and KB cell lines and it showed a controlled release profile. Therefore, these kinds of polymers are used as promising material for the development of formulation containing anticancer drugs [156].
6 Hybrid Materials
By combining two polymers HA and methylcellulose, it forms injectable gel-like structures. This mixed polymers go through the process of gelation technique through hydrogen bonding interactions [157]. Another example is that mixing of sodium carboxymethyl cellulose along with chitosan to encapsulate doxorubicin which can be formulated into microspheres or hydrogels. Because of the porous nature of carboxymethyl chitosan (oxidised hydrogel) shows no cytotoxicity in the umbilical endothelial cells, compatible in the blood and degraded by the lysozyme. This behaviour enables the doxorubicin delivery as an advantageous method for broad spectrum of vascular embolisation. In the microsphere formulation, owing to its porous nature doxorubicin were easily loaded. The in vitro and the in vivo studies proved that doxorubicin was delivered by enzyme degradation [158].
Haupt et al. studied the treatment for colorectal cancer using chitosan and guar gum. Celecoxib as an individual component delivers with the increased side effects with most majorly complications in the gastrointestinal tract (GIT). Along with the hybrid polymers, the celecoxib delivery results in the decrease in the growth of tumour cells and simultaneously reduces the toxic reactions [159, 160].
The CD complexes were combined with the polyelectrolytes in a multilayer fashion for the effective covering of bone implants and this is said to be an in situ prevention of bone tumour. The CD is combined with hydroxyapatite (HA) for the prolonged delivery of chemotherapeutic agent for the treatment of bone reformation. Chai et al. also revealed that there is improvement in the loading of cisplatin and it is due to the presence of CDs over the surface of HA. It is also noted that it undergoes a prolonged release of cisplatin in the bone defects to reconstruct the bone structure which also exhibits good biocompatibility [42].
The recent studies showed that the nanosilica material can be used as implantable electronic delivery systems. Li et al. fabricated silica wafers incorporated with anticancer moieties cisplatin, carboplatin and platinum. The silica wafers consist of hydroxyapatite, silica and calcium phosphate impregnated with anticancer moiety for the treatment of bone cancer. The implanted material in the tumour site reveals that it delivers the drug via pulsatile delivery with the application of external stimuli involving electric current/radiation [161].
Kakran et al. developed a system containing GO combined with other polymers such as Tween 80, Pluronic F38, maltodextrin. They are loaded with the natural bioactive component ellagic acid via π–π stacking and identified its release kinetics. The cytotoxicity of the formulation is tested against MCF-7 and HT-29 cells and found good anticancer activity because of the antioxidant nature of drug ellagic acid [162]. In a study by Zhang et al., GO was conjugated with the dextran and the anticancer drug was incorporated into the system. They have proved that the GO-drug conjugates exhibited a reduction in the tumour site against cervical cancer cells. And also found that the GO was gradually cleared from the system without causing toxicity [108]. Liu et al. found that GO when combined with polymer polyethylene glycol (PEG) proves to be a promising material for delivering anticancer drugs. GO-PEG conjugates provide very good stability under physiological conditions and the drug molecule camptothecin along with SN38 were attached via π–π stacking. They have reported that this conjugate PEG-GO-SN38-Camptothecin is highly efficient than the FDA approved water soluble pro-drug used for the treatment of colon cancer [163].
Hydrogels were prepared using PLGA, PLA and PEG which is loaded with the anticancer drug topotecan. There are hydrophobic interactions between the polymer and the drug was observed which increases the pKa value of carboxylate group present in the topotecan. Because of this property, the loading percentage of drug was increased and its efficacy is also increased. The in vivo studies proved that when the hydrogels placed as implants in the tumour site it completely inhibits the growth and recurrence [164].
PCL along with chitosan was prepared in the form of core-shell nanoparticles to load the drug. The drug loaded in this formulation was mitomycin-C and they were very effective in treating bladder tumours. PCL along with the PEG diacrylate microneedles loaded with the drug were useful in obtaining the membranes with different structural surface design. They found that the drug release was very slow and delivered in controlled manner for about 112 days. The in vitro studies were studied against the human dermal fibroblasts cells and observed that scaffolds served as platform for attachment of cells [165].
7 Triggerable Biomaterials
There are biomaterials which are responsive to the different triggers and release the drugs effectively (Fig. 2). The triggers can respond to the stimulus such as physical, chemical and biological agents in which the biological and chemical stimuli are present within the body, whereas the physical ones present externally. By this way, the delivery of drugs can be controlled effectively and targeted to the particular site [17]. The following part briefs about the different classes of responsive biomaterials and its use in anticancer drug delivery.
7.1 Magnetic Responsive Biomaterials
The magnetic properties of the material act as a triggering agent for the controlled delivery of drugs. This idea has been extended to design a system for releasing the active moieties to specific organs by combining two techniques [166]. The magnetic resonance imaging techniques and the drug loaded polymers were paired together for the therapeutic treatment and active targeting. In a study, the doxorubicin loaded alginates were taken and incorporated magnetic beads into the material for targeting the diseased organ. This triggering agent can be combined with pH-responsive materials to offer double benefits in delivering the drugs. In a work, they have combined the magnetic particles in the polymeric matrix which contains drug molecules. Then, they have used MRI imaging to correctly identify the exact location in which the drug was delivered [167,168,169].
The advantage of including a magnetic material within polymer-drug matrix will be more beneficial because of its easy recovery. When an implant is inserted in a patient, it is necessary to determine the response of the implant. If there is any weak immune response or undesired rejection, to remove the implant from the patient/living system becomes critical. In such a case, this magnetic pulsing technique could be helpful in removing the material from the organ or from the blood circulation. Therefore, drug-polymer with the magnetic particles in the system expands the scope to develop a value-added formulation. It is important to note that some of the magnetic responsive polymer systems have been approved by FDA [170, 171].
7.2 pH-Responsive Biomaterials
There are pH values that exist within the human body and they are different for tissues, organelles and fluids. For example, acidic pH exists in stomach and vaginal areas (pH < 7). The neutral pH occurs in the ocular surface (pH 7.1) and in the blood (pH 7.4). In addition, pH values will differ in disease environment and in the barriers of organ. Therefore, a good approach to increase the efficacy of cancer drugs which involves in the polymeric delivery system which can react at particular pH [172]. To develop a pH sensitive product, functional groups to be included which can protonate or deprotonate in the polymeric matrix. Mostly, amine containing polymers which are derived from dimethyl aminoethylmethacrylate will be protonated to yield a cationic group of materials. Another example in this case is carboxylate containing polymers which includes poly(acrylic acid) will be deprotonated to yield anionic materials under basic environment. Therefore, the charge of these polymers could be easily changed and these materials can react to changes in the pH in the form of swelling, shrinkage, dissociated or degraded. By these strategies, these type of polymeric materials can release the drug moieties in the target organs and tissues [9, 173]. There are various pH-responsive polymers which are used for masking the taste, delivery nucleic acid and doxorubicin delivery (Fig. 3). Most commonly this pH-responsive materials have been used for targeting the tumour environment because they exist at lower pH (5.7). And the surrounding environment occurs at pH of 6.8–7 because of acidosis in the area. Hence, polymeric multifunctional nanocomposites (acid sensitive) were used for the controlled delivery of anticancer drugs. In the cancer environments, the folic acid receptors will be overexpressed and it can be used for functionalising the molecule for improved targeting. The acid-responsive polymer diaminoketal with the drug increases the cellular uptake compared to the free drug alone. A well-known example poly(ethylene glycol) has been used for the controlled delivery of drugs for tumour targeting. These pH-responsive polymeric materials continue to be an area of interest for delivering the anticancer drugs [174, 175].
7.3 Temperature-Responsive Biomaterials
These kinds of polymers can be used for delivering and targeting the tissues and organs. Our human body exists in a temperature of 37 ℃, and the room temperature is 25 ℃ [176]. This difference is advantageous in case of temperature-responsive polymers because these materials flow at ambient temperature and it gels at body temperature. These kinds of polymeric materials were developed by sol-gel techniques for the improved targeting. Examples of these type of polymers are cellulose, chitosan, poly(N-vinylcaprolactam), poly(N-alkyl acrylamides), poloxamers and xyloglucan. The strategies for formulating this type of materials are modifying the end group molecules, varying the post polymerisation process and changing the concentration of monomers. These strategies could be useful for the controlled delivery and for improved targeting [177,178,179].
7.4 Redox Responsive Biomaterials
The human body consists of reducing and oxidising agent which differs in organs, cells and tissues. Glutathione, a reducing agent found at higher concentration in cells than the surroundings. Hydrogen peroxide, oxidising agent found in the inflamed and injured tissues. The differences in these redox reactions between the cells/tissues and the surrounding environment develop a diseased state. Therefore, it is important to formulate a materials which should balance the redox potential of the body [180].
The materials obtained from disulphides are used to stabilise the reduction trigger in the body. Inside the cells, it is mediated by glutathione molecule in which the disulphide bridges are reduced to form analogues of dithiol (Fig. 4). This interchange of dithiol and disulphide is a reversible reaction which is best suited for anticancer activity. Another example of this kind is that the sulphur-based materials have been used to balance the oxidation triggers. Sulphur exists in many oxidation states and in particular the sulphur-based block copolymers are used for cancer drug delivery, protein and gene delivery [181, 182].
Interestingly, materials with dual activation capacity can balance both of the oxidation and reduction triggers have been explored. The common functional group used are diselenides in which it has the similar chemical structure as that of disulphides. These diselenides can be incorporated into the bioresponsive polymeric system which prevents the triggers caused by the oxidation and reduction process [183].
7.5 Enzymes and Hydrolysis Sensitive Polymers
The enzymatic and hydrolytically responsive polymers have been designed and formulated for cancer drug delivery. Hydrolytic susceptible materials are the ones which are degraded by water. The degradation process happens by the nucleophilic addition of water into the functional group (electrophile) of the polymer [184]. The most commonly used electrophilic functional group of the polymers are esters and anhydrides. An example for such kinds of bioresponsive formulation available in the market is Gliadel wafer. This product consists of chemotherapeutic drug carmustine impregnated on the polymer polyanhydride. The Gliadel wafer shows the influence of hydrolysis responsive materials. This chemotherapeutic formulation could also be implanted into brain for the controlled delivery of carmustine to the tumours. Gliadel wafer can also be used in patients with glioblastoma multiforme and it improves the survival rate for about six months [7].
Enzyme sensitive polymers have been developed for tumour imaging and delivering the drugs (Fig. 5). With the disease pathology, some of the enzymes differ from the normal values and they are hyaluronidases, phospholipases, matrix metalloproteins, etc. For the colon tumour treatment, the enzyme responsive polymer along with the drug doxorubicin was developed. It was also found that it minimises the inflammation in the colon than any other systems developed [173, 185].
7.6 Light Responsive Biomaterials
Light-induced drug delivery has been used to target the cancerous cells by releasing the drugs through the source of light. This is one of the painless and non-invasive technique act as an external stimulus for delivering the cancer drugs [186]. This light stimulation system tuned into a non-invasive trigger for controlling the temporal and spatial delivery of drugs. UV-Visible light irradiation at a particular wavelength will release the drug in the targeted site and this acts as a remote activated system. There are some of the challenges to control the light activation system and they are drug degradation of during light exposure, distance of the light from the polymer-drug system and the thickness of the tissue and the penetration of the light [187]. The important mechanism for the light stimulated delivery is that it undergoes either a ring opening reaction or cis-trans isomerisation through the light source. In one of the study, they have used a light sensitive modified azobenzene block copolymer for targeting the melanoma cells. During irradiation, it undergoes a molecular conformation in the azobenzene molecule and by this means it alters the structure to release the drug [188, 189].
7.7 Electrically Responsive Biomaterials
There are various types of electrically sensitive polymers were developed and they have been used for many biomedical applications in particular for targeted delivery of anticancer drugs [190]. Our body is supplied with electrical stimulus, whereas the neurons act as a neurotransmitters for transmitting the information through electrical signals. The electrically responsive polymers are highly conjugated aromatic materials and they will directly form a boundary with the cells when the electrical stimulus is applied. One such example is polypyrrole and they are widely used for electronic applications, bioimaging and targeting the cells. The polypyrrole nanoparticles have also been developed and they have studied its biocompatility in mice. This kind of electrically sensitive polymers has also been combined with temperature sensitive polymers for the dual responsive systems [191, 192].
7.8 Sound Responsive Biomaterials
This is another way to release the drug in the targeted site via auditory stimuli. The challenges associated with this system to release the drug are tuning the properties of materials and functionalising the materials to optimise the release [193]. A study shows that to optimise the release, they have incorporated growth promoting molecules in the ultrasound responsive scaffolds through acoustic responsive polymer. In another study, the drug is impregnated in the fibrin scaffolds and to control the release, and they have prepared a double layer emulsion using a microfluidiser. Through this microfluidic device, the multilayer delivery systems were created which includes microbubbles and an array of nanoparticle designs [171].
7.9 Swelling and Shrinking Biomaterials
Some of the polymers or biopolymers undergo swelling and contraction with respect to the exterior stimulus. Most common example of biopolymer releasing the anticancer drug is alginates. The anticancer drugs are encapsulated using the alginates by controlling the release profile. Alginates also functionalised by vascular endothelial growth factor (VEGF) to target the specific site in the body. These materials also used for sensing the specific region and the injectable was also prepared using alginates. Many applications are there for using alginates as biopolymer for delivering the drugs [194].
8 Commercially Available Products
There are many products which have been transferred from clinic, approved by FDA and they are commercially available in the market. Most of the formulations are available as ideas in the literature and not executed in commercial market for medical applications (Table 1). Lupron Depot is a commercially available drug which contains PLGA microsphere loaded with leuprolide which is used for the treatment of prostate cancer. PLA and PLGA are used in many products because of its versatility, biocompatibility and biodegradability nature which will be degraded into lactides and glycolides [195]. Doxil which contains PEGylated (PEG) liposomal formulation encapsulated with doxorubucin was approved by FDA for the treatment and prevention of regrowth of ovarian cancer and Kaposi’s sarcoma [196]. Marqibo is a recently approved nanoparticle liposomal formulation containing vincristine for the treatment of leukaemia [197]. Abraxane, a nanoparticle formulation useful for the treatment of breast cancer [198]. Zoladex, a product containing PLGA and drug goserelin acetate for treating prostate and breast cancer cells. This implants duration of action was found to be 3 months and they are in 10 mm length and 1 mm in diameter [199]. Eligard, it is an injectable implant containing leuprolide acetate used for the treatment of prostate and breast cancer cells. This implant consists of 2 syringes one is filled with PLGA along with methyl pyrrolidone and the other with the drug. Before injecting at the site, it should be mixed together and injected into the tumour site and it forms implants [200]. InGell Delta, PLGA containing dextran and interleukin-2and it forms a stereocomplex which preserves it three-dimensional structure. They exhibit very low initial burst release with good biocompatibility and useful for the treatment of lymphoma [201]. OncoGel is a product containing PLGA, PEG loaded with paclitaxel drug and it turns into gel form at body temperature. It delivers the drug paclitaxel directly into the brain tumour cells through intralesional injection into the tumour cavity [202]. Viadur, osmotic implant which is made up of titanium, PU, elastomeric piston and polyethylene (PE) moderator which provides sustained delivery of drug for about one year in the implant site [203]. Gliadel wafer consists of wafers with dime shape and it contains poly(carboxyphenoxy-propane/sebacic acid) loaded with the drug carmustine. They are useful during the post-surgery of the brain tumour, glioblastoma multiforme and release is driven by two types of mechanisms one is surface erosion of biomaterial and drug releases by diffusion [204].
9 Conclusions
The biomaterials (natural, inorganic, organic and hybrid) act as reservoir for delivering the anticancer drugs is the most promising approach to improve the delivery of drugs to the tumour site and thereby reducing its side effects. This approach is advantageous in treating all types of tumour and it can be called as regional chemotherapy. With the expanding research on cancer treatment, the biomaterials have the potential to deliver the drugs to the targeted site through functionalisation, surface modification, combined delivery and controlled release mechanisms. Hence, the biomaterials mediated drug delivery operate in these three mechanisms such as it inhibits the growth, slows down the growth and also prevents regrowth of the tumour. Moreover, it minimises the harm caused by traditional methods of delivery and it owns the broad spectrum of advantages in the biomedical field. In the last few years, a responsive drug delivery system has been widely considered for the improved permeability, treatment and prevention of cancer growth.
References
de Vita VT, Chu E (2008) A history of cancer chemotherapy. Cancer Res 68:8643–8653. https://doi.org/10.1158/0008-5472.CAN-07-6611
Krishnamurthy S, Ng VWL, Gao S, Tan MH, Yang YY (2014) Phenformin-loaded polymeric micelles for targeting both cancer cells and cancer stem cells invitro and invivo. Biomaterials 35:9177–9186. https://doi.org/10.1016/j.biomaterials.2014.07.018
Sun CC, Bodurka DC, Weaver CB, Rasu R, Wolf JK, Bevers MW et al (2005) Rankings and symptom assessments of side effects from chemotherapy: insights from experienced patients with ovarian cancer. Support Care Cancer 13:219–227. https://doi.org/10.1007/s00520-004-0710-6
Krukiewicz K, Jarosz T, Zak JK, Lapkowski M, Ruszkowski P, Bobkiewicz-Kozlowska T et al (2015) Advancing the delivery of anticancer drugs: conjugated polymer/triterpenoid composite. Acta Biomater 19:158–165. https://doi.org/10.1016/j.actbio.2015.03.006
Anselmo AC, Mitragotri S (2014) An overview of clinical and commercial impact of drug delivery systems. J Control Release 190:15–28. https://doi.org/10.1016/j.jconrel.2014.03.053
Peer D, Karp JM, Hong S, Farokhzad OC, Margalit R, Langer R (2007) Nanocarriers as an emerging platform for cancer therapy. Nat Nanotechnol 2:751–760. https://doi.org/10.1038/nnano.2007.387
Mitchell MJ, Jain RK, Langer R (2017) Engineering and physical sciences in oncology: challenges and opportunities. Nat Rev Cancer 17:659–675. https://doi.org/10.1038/nrc.2017.83
De Souza R, Zahedi P, Allen CJ, Piquette-Miller M (2010) Polymeric drug delivery systems for localized cancer chemotherapy. Drug Deliv 17:365–375. https://doi.org/10.3109/10717541003762854
Kanamala M, Wilson WR, Yang M, Palmer BD, Wu Z (2016) Mechanisms and biomaterials in pH-responsive tumour targeted drug delivery: a review. Biomaterials 85:152–167. https://doi.org/10.1016/j.biomaterials.2016.01.061
Li M, Tang Z, Zhang Y, Lv S, Li Q, Chen X (2015) Targeted delivery of cisplatin by LHRH-peptide conjugated dextran nanoparticles suppresses breast cancer growth and metastasis. Acta Biomater 18:132–143. https://doi.org/10.1016/j.actbio.2015.02.022
Lu Y, Aimetti AA, Langer R, Gu Z (2016) Bioresponsive materials. Nat Rev Mater 2:1–17. https://doi.org/10.1038/natrevmats.2016.75
Liu J, Huang Y, Kumar A, Tan A, Jin S, Mozhi A et al (2014) PH-sensitive nano-systems for drug delivery in cancer therapy. Biotechnol Adv 32:693–710. https://doi.org/10.1016/j.biotechadv.2013.11.009
Schmaljohann D (2006) Thermo- and pH-responsive polymers in drug delivery. Adv Drug Deliv Rev 58:1655–1670. https://doi.org/10.1016/j.addr.2006.09.020
Tietze R, Zaloga J, Unterweger H, Lyer S, Friedrich RP, Janko C et al (2015) Magnetic nanoparticle-based drug delivery for cancer therapy. Biochem Biophys Res Commun 468:463–470. https://doi.org/10.1016/j.bbrc.2015.08.022
Schneider C, Langer R, Loveday D, Hair D (2017) Applications of ethylene vinyl acetate copolymers (EVA) in drug delivery systems. J Control Release 262:284–295. https://doi.org/10.1016/j.jconrel.2017.08.004
Stewart SA, Domínguez-Robles J, Donnelly RF, Larrañeta E (2018) Implantable polymeric drug delivery devices: classification, manufacture, materials, and clinical applications. Polymers (Basel) 10. https://doi.org/10.3390/polym10121379
Liqun Yang ZH (2018) Application of responsive nano-drug delivery system in cancer therapy. J Nanomed 1:2–5
Jeyanthi R, Rae KP (1990) Controlled release of anticancer poly(hema) hydrogel matrices drugs from collagen. J Control Release 13:91–98
Transl J, Xu S, Xu H, Wang W, Li S, Li H et al (2019) The role of collagen in cancer: from bench to bedside. J Transl Med:1–22. https://doi.org/10.1186/s12967-019-2058-1
Sasaki K, Ishihara J, Ishihara A, Miura R, Mansurov A (2019) Engineered collagen-binding serum albumin as a drug conjugate carrier for cancer therapy. Sci Adv 5:1–13
Ahmednagar D, Zambare SP (2015) Effect of anticancer drugs cisplatin and 5-fluorouracil on collagen contents in fresh water bivalve, Parreysia corrugata (M). Biology (Basel) 5:20–22
Kim C, Kim H, Park H, Yong K (2019) Controlling the porous structure of alginate ferrogel for anticancer drug delivery under magnetic stimulation. Carbohydr Polym 223:115045. https://doi.org/10.1016/j.carbpol.2019.115045
Manatunga DC, de Silva RM, de Silva KMN, de Silva N, Bhandari S, Yap YK et al (2017) pH responsive controlled release of anti-cancer hydrophobic drugs from sodium alginate and hydroxyapatite bi-coated iron oxide nanoparticles. Eur J Pharm Biopharm. https://doi.org/10.1016/j.ejpb.2017.03.014
Pourjavadi A, Amin SS, Hosseini SH (2018) Delivery of hydrophobic anticancer drugs by hydrophobically modified alginate based magnetic nanocarrier. Ind Eng Chem Res 5:1–31. https://doi.org/10.1021/acs.iecr.7b04050
Prabha G, Raj V (2017) Sodium alginate–polyvinyl alcohol–bovin serum albumin coated Fe3O4 nanoparticles as anticancer drug delivery vehicle: Doxorubicin loading and in vitro release study and cytotoxicity to HepG2 and L02 cells G. Mater Sci Eng, C 4:1–54. https://doi.org/10.1016/j.msec.2017.04.075
Dosio F, Arpicco S, Stella B, Fattal E (2015) Hyaluronic acid for anticancer drug and nucleic acid delivery. Adv Drug Deliv Rev 2:1–71. https://doi.org/10.1016/j.addr.2015.11.011
Cadete A, Olivera A, Besev M, Dhal PK, Gonçalves L, Almeida AJ et al (2019) Self-assembled hyaluronan nanocapsules for the intracellular delivery of anticancer drugs. Sci Rep 9:1–11. https://doi.org/10.1038/s41598-019-47995-8
Shanmugam G, Varadharajan RS, Prabakar D, Mohammed S, Renganathan S, Erminio M et al (2018) Molecular insights of hyaluronic acid as potential source of polymer-drug conjugate in the target-mediated treatment of cancer. Nat Prod Commun 13:813–819. https://doi.org/10.1177/1934578X1801300501
Park S, Park H, Jeong S, Yi BG, Park K (2019) Hyaluronic acid-conjugated mesoporous silica nanoparticles loaded with dual anticancer agents for chemophotodynamic cancer therapy. J Nanomater 2019:1–11
Kim JH, Moon MJ, Kim DY, Heo SH, Jeong YY (2018) Hyaluronic acid-based nanomaterials for cancer therapy. Polymers (Basel) 10:1–15. https://doi.org/10.3390/polym10101133
Croisier F, Jérôme C (2013) Chitosan-based biomaterials for tissue engineering. Euro Polym J 49:780–792
Dhanikula AB, Panchagnula R (2004) Development and characterization of biodegradable chitosan films for local delivery of paclitaxel. AAPS J 6
Dong H, Kil C, Sung Y, Hee K, Hee J, Hwang T et al (2008) A chitosan hydrogel-based cancer drug delivery system exhibits synergistic antitumor effects by combining with a vaccinia viral vaccine. Int J Pharm 350:27–34. https://doi.org/10.1016/j.ijpharm.2007.08.014
Ampollini L, Sonvico F, Barocelli E, Cavazzoni A, Bilancia R, Mucchino C et al (2010) Intrapleural polymeric films containing cisplatin for malignant pleural mesothelioma in a rat tumour model : a preliminary study. Eur J Cardiothorac Surg 37:557–565. https://doi.org/10.1016/j.ejcts.2009.08.012
Reza M, Tabatabaie RM, Maharramov A, Ali M (2011) Synthesis and in vitro studies of biodegradable thiolated chitosan hydrogels for breast cancer therapy. Int J Biol Macromol 48:747–752. https://doi.org/10.1016/j.ijbiomac.2011.02.020
Rokhade AP, Agnihotri SA, Patil SA, Mallikarjuna NN, Kulkarni PV, Aminabhavi TM (2006) Semi-interpenetrating polymer network microspheres of gelatin and sodium carboxymethyl cellulose for controlled release of ketorolac tromethamine. Carbohydr Polym 65:243–252. https://doi.org/10.1016/j.carbpol.2006.01.013
Sheleg SV, Korotkevich EA, Zhavrid EA, Muravskaya GV, Smeyanovich AF, Shanko YG et al (2002) Local chemotherapy with cisplatin-depot for glioblastoma multiforme. J Neurooncol 60:53–59. https://doi.org/10.1023/a:1020288015457
Löhr M, Müller P, Karle P, Stange J, Mitzner S, Jesnowski R et al (1998) Targeted chemotherapy by intratumour injection of encapsulated cells engineered to produce CYP2B1, an ifosfamide activating cytochrome P450. Gene Ther 5:1070–1078. https://doi.org/10.1038/sj.gt.3300671
Shimpi S, Chauhan B, Shimpi P (2005) Cyclodextrins: application in different routes of drug administration. Acta Pharm 55:139–156
Loftsson T, Duch D (2007) Cyclodextrins and their pharmaceutical applications. Int J Pharm 329:1–11. https://doi.org/10.1016/j.ijpharm.2006.10.044
Cortial D, Ladam G, Atmani H, Haı Y, Daubine F, Benkirane-Jessel N et al (2009) Biomaterials Nanostructured polyelectrolyte multilayer drug delivery systems for bone metastasis prevention. Biomaterials 30:6367–6373. https://doi.org/10.1016/j.biomaterials.2009.08.002
Chai F, Abdelkarim M, Laurent T, Tabary N, Degoutin S, Simon N et al (2014) Poly-cyclodextrin functionalized porous bioceramics for local chemotherapy and anticancer bone reconstruction. J Biomed Mater Res, Part B:1–10. https://doi.org/10.1002/jbm.b.33094
Manchun S, Cheewatanakornkool K, Dass CR, Sriamornsak P (2014) Novel pH-responsive dextrin nanogels for doxorubicin delivery to cancer cells with reduced cytotoxicity to cardiomyocytes and stem cells. Carbohydr Polym 4:1–32. https://doi.org/10.1016/j.carbpol.2014.08.002
Manchun S, Dass CR, Cheewatanakornkool K, Sriamornsak P (2015) Enhanced anti-tumor effect of pH-responsive dextrin nanogels delivering doxorubicin on colorectal cancer. Carbohydr Polym. https://doi.org/10.1016/j.carbpol.2015.03.018
Yucel T, Lovett ML, Kaplan DL (2014) Silk-based biomaterials for sustained drug delivery. J Control Release 5:1–66. https://doi.org/10.1016/j.jconrel.2014.05.059
Scheibel T, Leal-Egana A (2010) Silk-based materials for biomedical applications. Biotechnol Appl Biochem 167:155–167. https://doi.org/10.1042/ba20090229
Hofmann S, Po CTW, Rossetti F, Textor M, Vunjak-Novakovic G (2006) Silk fibroin as an organic polymer for controlled drug delivery. J Control Release 111:219–227. https://doi.org/10.1016/j.jconrel.2005.12.009
Rockwood DN, Preda RC, Yücel T, Wang X, Lovett ML, Kaplan DL (2011) Materials fabrication from Bombyx mori silk fibroin. Nat Protoc. https://doi.org/10.1038/nprot.2011.379
Hines DJ, Kaplan DL (2011) Mechanisms of controlled release from silk fibroin films. Biomacromolecules:804–812
Seib FP, Kaplan DL (2012) Biomaterials Doxorubicin-loaded silk films: drug-silk interactions and in vivo performance in human orthotopic breast cancer. Biomaterials 33:8442–8450. https://doi.org/10.1016/j.biomaterials.2012.08.004
Lu Q, Wang X, Hu X, Cebe P, Omenetto F, Kaplan DL (2010) Stabilization and release of enzymes from silk films. Macromol Biosci:359–368. https://doi.org/10.1002/mabi.200900388
Seib FP, Pritchard EM, Kaplan DL (2012) Self-assembling doxorubicin silk hydrogels for the focal treatment of primary breast cancer. Adv Func Mater:1–8. https://doi.org/10.1002/adfm.201201238
Seib FP, Coburn J, Konrad I, Klebanov N, Jones GT, Blackwood B et al (2015) Acta Biomaterialia focal therapy of neuroblastoma using silk films to deliver kinase and chemotherapeutic agents in vivo. Acta Biomater 20:32–38. https://doi.org/10.1016/j.actbio.2015.04.003
Chiu B, Coburn J, Pilichowska M, Holcroft C, Seib FP, Charest A et al (2014) Surgery combined with controlled-release doxorubicin silk films as a treatment strategy in an orthotopic neuroblastoma mouse model. Br J Cancer 111:708–715. https://doi.org/10.1038/bjc.2014.324
Poursaid A, Price R, Tiede A, Olson E, Huo E, Mcgill L et al (2015) Biomaterials In situ gelling silk-elastinlike protein polymer for transarterial chemoembolization. Biomaterials 57:142–152. https://doi.org/10.1016/j.biomaterials.2015.04.015
Yu S, Yang W, Chen S, Chen M, Liu Y, Shao Z et al (2014) Floxuridine-loaded silk fibroin nanospheres. RSC Adv 4:18171–18177. https://doi.org/10.1039/c4ra02113d
Yang W, Lan M, Lee S, Chang J, Huang H (2015) Primary human nasal epithelial cell response to titanium surface with a nanonetwork structure in nasal implant applications. Nanoscale Res Lett 10:167–179. https://doi.org/10.1186/s11671-015-0849-8
Kazek-Kęsik A, Dercz G, Kalemba I, Suchanek K, Kukharenko AI, Korotin DM et al (2014) Surface characterisation of Ti–15Mo alloy modified by a PEO process in various suspensions. Mater Sci Eng, C 39:259–272. https://doi.org/10.1016/j.msec.2014.03.008
Muñoz S, Pavón J, Civantos A, Allain JP, Torres Y (2015) On the influence of space holder in the development of porous titanium implants: mechanical, computational and biological evaluation. Mater Charact 2:1–49. https://doi.org/10.1016/j.matchar.2015.08.019
Słu K, Widziołek M, Szade J, Winiarski A, Dercz G, Kazek A et al (2013) Electrochimica acta formation of bioactive coatings on a Ti–6Al–7Nb alloy by plasma electrolytic oxidation. Electrochim Acta 104:407–424. https://doi.org/10.1016/j.electacta.2012.07.075
Att W, Hori N, Takeuchi M, Ouyang J, Yang Y, Anpo M et al (2009) Biomaterials Time-dependent degradation of titanium osteoconductivity: an implication of biological aging of implant materials. Biomaterials 30:5352–5363. https://doi.org/10.1016/j.biomaterials.2009.06.040
Perla V, Webster TJ (2005) Better osteoblast adhesion on nanoparticulate selenium—a promising orthopedic implant material. Wiley Period 2022:356–364. https://doi.org/10.1002/jbm.a.30423
Phong Tran TJW (2008) Enhanced osteoblast adhesion on nanostructured selenium compacts for anti-cancer orthopedic applications. Int J Nan 3:391–396
Tran PA, Taylor E, Sarin L, Hurt RH, Webster TJ (2009) Novel anti-cancer, anti-bacterial coatings for biomaterial applications: selenium nanoclusters. MRS Online Proc Libr Arch 1209
Tran PA, Sarin L, Hurt RH, Webster TJ (2009) Titanium surfaces with adherent selenium nanoclusters as a novel anticancer orthopedic material. J Biomed Res Part A: An Official J Soc Biomater, Aus Soc Biomater, Korean Soc Biomater. https://doi.org/10.1002/jbm.a.32631
Chen X, Cai K, Fang J, Lai M, Hou Y, Li J et al (2013) Fabrication of selenium-deposited and chitosan-coated titania nanotubes with anticancer and antibacterial properties. Coll Surf, B 103:149–157. https://doi.org/10.1016/j.colsurfb.2012.10.022
Gulati K, Aw MS, Losic D (2012) Nanoengineered drug-releasing Ti wires as an alternative for local delivery of chemotherapeutics in the brain. Int J Nanomedicine 7:2069–2076
Hong Y, Fan H, Li B, Guo B, Liu M, Zhang X (2010) Fabrication, biological effects, and medical applications of calcium phosphate nanoceramics. Mater Sci Eng, R: Rep 70:225–242. https://doi.org/10.1016/j.mser.2010.06.010
Aoki H, Ogaki M, Kano S (1993) Effects of adriacin-absorbing hydroxyapatite-sol on Ca-9 cell growth. Rep Inst Med Dent Eng 27:39–44
Yuan H, Kurashina K, de Bruijn JD, Li Y, de Groot K, Zhang X (1999) A preliminary study on osteoinduction of two kinds of calcium phosphate ceramics. Biomaterials 20:1799–1806
Pardun K, Treccani L, Volkmann E, Streckbein P, Heiss C, Li G et al (2015) Mixed zirconia calcium phosphate coatings for dental implants: tailoring coating stability and bioactivity potential ☆. Mater Sci Eng, C 48:337–346. https://doi.org/10.1016/j.msec.2014.12.031
Klein CPAT, Driessen AA, de Groot K (1983) Biodegradation behavior of various calcium phosphate materials in bone tissue. J Biomed Mater Res 17:769–784
Uchida A, Shinto Y, Araki N, Ono K (1992) Slow release of anticancer drugs from porous calcium hydroxyapatite ceramic. J Orthop Res:440–445
Yasuhisa Tahara YI (2001) Apatite cement containing cis-diamminedichloroplatinum implanted in rabbit femur for sustained release of the anticancer drug and bone formation. J Orthop Sci 6:556–565
Tanzawa Y, Tsuchiya H, Shirai T (2011) Potentiation of the antitumor effect of calcium phosphate cement containing anticancer drug and caffeine on rat osteosarcoma. J Orthop Sci:77–84. https://doi.org/10.1007/s00776-011-0045-3
Chen M, Le DQS, Hein S, Li P, Nygaard JV, Kassem M et al (2012) Fabrication and characterization of a rapid prototyped tissue engineering scaffold with embedded multicomponent matrix for controlled drug release. Int J Nanomed 7:4285
Yasin MN, Svirskis D, Seyfoddin A, Rupenthal ID (2014) Implants for drug delivery to the posterior segment of the eye: a focus on stimuli-responsive and tunable release systems. J Control Release 2:1–15. https://doi.org/10.1016/j.jconrel.2014.09.030
Ueno N (1982) Controlled release rate of a lipophilic drug (BCNU) from a refillable silicone rubber device. J Biomed Mater Res 16:669–677
Uhlir BA (1955) Electrolytic shaping of germanium. Bell Syst Tech J:333–348
Ko PJ, Ishikawa R, Takamura T, Morimoto Y, Cho B, Sohn H et al (2011) Porous-silicon photonic-crystal platform for the rapid detection of nano-sized superparamagnetic beads for biosensing applications. Nanosci Nanotechnol Lett:612–616. https://doi.org/10.1166/nnl.2011.1236
Gabouze N, Belhousse S, Cheraga H, Ghellai N, Ouadah Y (2006) CO2 and H2 detection with a CHx/porous silicon-based sensor. Vacuum 80:986–989. https://doi.org/10.1016/j.vacuum.2006.01.004
Talamonti C, Bruzzi M, Marrazzo L, Menichelli D, Scaringella M, Bucciolini M et al (2011) Bidimensional silicon dosimeter: development and characterization. Nucl Inst Methods Phys Res A 658:84–89. https://doi.org/10.1016/j.nima.2011.05.044
Bogaerts W, de Heyn P, van Vaerenbergh T, de Vos K, Kumar S (2012) Silicon microring resonators. Laser Photon Rev 73:47–73. https://doi.org/10.1002/lpor.201100017
Park J, Gu L, Von Maltzahn G, Ruoslahti E, Bhatia SN, Sailor MJ (2009) Biodegradable luminescent porous silicon nanoparticles for in vivo applications. Nat Mater 8:331–336. https://doi.org/10.1038/nmat2398
Anglin EJ, Cheng L, Freeman WR, Sailor MJ (2008) Porous silicon in drug delivery devices and materials ☆. Adv Drug Deliv Rev 60:1266–1277. https://doi.org/10.1016/j.addr.2008.03.017
Ali NK, Haidary SM, Emma PC (2012) Nanoporous silicon as drug delivery systems for cancer therapies. J Nanomater 2012. https://doi.org/10.1155/2012/830503
Bum S, Joo Y, Kim H, Ryu W, Park Y (2015) Biodegradation-tunable mesoporous silica nanorods for controlled drug delivery. Mater Sci Eng, C 50:64–73. https://doi.org/10.1016/j.msec.2015.01.073
Xia B, Wang B, Zhang W, Shi J (2015) High loading of doxorubicin into styrene- terminated porous silicon nanoparticles via p-stacking for cancer treatments in vitro †. RSC Adv 5:44660–44665. https://doi.org/10.1039/C5RA04843E
Park JS, Kinsella JM, Jandial DD, Howell SB, Sailor MJ (2011) Cisplatin-loaded porous Si microparticles capped by electroless deposition of platinum. Small:2061–2069. https://doi.org/10.1002/smll.201100438
Niemelä E, Desai D, Nkizinkiko Y, Eriksson JE, Jessica M (2015) Sugar-decorated mesoporous silica nanoparticles as delivery vehicles for the poorly soluble drug celastrol enables targeted induction of apoptosis in cancer cells. Eur J Pharm Biopharm. https://doi.org/10.1016/j.ejpb.2015.07.009
Alhmoud H, Delalat B, Elnathan R, Cifuentes-rius A, Chaix A, Rogers M et al (2014) Porous silicon nanodiscs for targeted drug delivery. Adv Funct Mater 2:1–9. https://doi.org/10.1002/adfm.201403414
Hon NK, Shaposhnik Z, Diebold ED, Tamanoi F, Jalali B (2012) Tailoring the biodegradability of porous silicon nanoparticles. J Biomed Mater Res Part A:1–6. https://doi.org/10.1002/jbm.a.34294
Tzur-Balter A, Shatsberg Z, Beckerman M, Segal E, Artzi N (2015) Mechanism of erosion of nanostructured porous silicon drug carriers in neoplastic tissues. Nat Commun 6:6208
Tzur-balter A, Gilert A, Massad-ivanir N, Segal E (2013) Engineering porous silicon nanostructures as tunable carriers for mitoxantrone dihydrochloride. Acta Biomater 9:6208–6217. https://doi.org/10.1016/j.actbio.2012.12.010
Kumar S, Zheng D, Pastorin G, Al-rubeaan K, Luong JHT, Sheu F (2011) Delivery of drugs and biomolecules using carbon nanotubes. Carbon N Y 49:4077–4097. https://doi.org/10.1016/j.carbon.2011.05.049
Kostarelos K, Bianco A (2015) Multifunctional carbon nanomaterial hybrids for magnetic manipulation and targeting. Biochem Biophys Res Commun 1:1–9. https://doi.org/10.1016/j.bbrc.2015.06.131
Boncel S, Zając P, Koziol KKK (2013) Liberation of drugs from multi-wall carbon nanotube carriers. J Control Release 3:1–50. https://doi.org/10.1016/j.jconrel.2013.04.009
Yang X, Chen Y, Yuan R, Chen G, Blanco E, Gao J et al (2008) Folate-encoded and Fe3O4-loaded polymeric micelles for dual targeting of cancer cells. Polymer 49:3477–3485. https://doi.org/10.1016/j.polymer.2008.06.005
Yang F, Fu DL, Long J, Ni QX (2008) Magnetic lymphatic targeting drug delivery system using carbon nanotubes. Med Hypotheses:765–767. https://doi.org/10.1016/j.mehy.2007.07.045
Li R, Wu R, Zou H (2011) Folate and iron difunctionalized multiwall carbon nanotubes as dual-targeted drug nanocarrier to cancer cells. Carbon N Y 49:1797–1805. https://doi.org/10.1016/j.carbon.2011.01.003
Cirillo G, Vittorio O, Hampel S, Iemma F, Cecchini M, Puoci F et al (2013) Quercetin nanocomposite as novel anticancer therapeutic: improved efficiency and reduced toxicity. Eur J Pharm Sci. https://doi.org/10.1016/j.ejps.2013.04.008
Bai S, Shen X (2012) Graphene-inorganic nanocomposites. RSC Adv 2:64–98. https://doi.org/10.1039/C1RA00260K
Akhavan O, Ghaderi E, Akhavan A (2012) Biomaterials size-dependent genotoxicity of graphene nanoplatelets in human stem cells. Biomaterials 33:8017–8025. https://doi.org/10.1016/j.biomaterials.2012.07.040
Hashemi E, Akhavan O, Shamsara M, Valimehr S, Rahighi R (2014) DNA and RNA extractions from eukaryotic and prokaryotic cells by graphene nanoplatelets. RSC Adv 4:60720–60728
Park YH, Park SY, In I (2015) Direct noncovalent conjugation of folic acid on reduced graphene oxide as anticancer drug carrier. J Ind Eng Chem 3:1–23. https://doi.org/10.1016/j.jiec.2015.05.021
Pourjavadi A, Tehrani ZM, Jokar S (2015) Chitosan based supramolecular polypseudorotaxane as a pH-responsive polymer and their hybridization with mesoporous silica-coated magnetic graphene oxide for triggered anticancer drug delivery. Polymer (Guildf):1–34. https://doi.org/10.1016/j.polymer.2015.08.050
Yang K, Wan J, Zhang S, Tian B, Zhang Y, Liu Z (2012) The influence of surface chemistry and size of nanoscale graphene oxide on photothermal therapy of cancer using ultra-low laser power. Biomaterials 33:2206–2214. https://doi.org/10.1016/j.biomaterials.2011.11.064
Zhang L, Xia J, Zhao Q, Liu L, Zhang Z (2010) Functional graphene oxide as a nanocarrier for controlled loading and targeted delivery of mixed anticancer drugs. Small 6:537–544
Wu SY, An SSA, Hulme J (2015) Current applications of graphene oxide in nanomedicine. Int J Nanomed 10:9–24. https://doi.org/10.2147/IJN.S88285
Khang G, Rhee JM, Jeong JK, Lee JS, Kim MS, Cho SH et al (2003) Local drug delivery system using biodegradable polymers. Macromol Res 11:207–223
Zhao H, Chen Y, Cai Y, Wu F, Wei L, Liu Z et al (2013) Local antitumor effects of intratumoral delivery of rlL-2 loaded sustained-release dextran/PLGA–PLA core/shell microspheres. Int J Pharm:2–7. https://doi.org/10.1016/j.ijpharm.2013.04.051
Liu D, Wang F, Yue J, Jing X, Huang Y (2013) Metabolism targeting therapy of dichloroacetate-loaded electrospun mats on colorectal cancer. Drug Deliv 7544:1–8. https://doi.org/10.3109/10717544.2013.870258
Liu S, Wang X, Zhang Z, Zhang Y (2015) Use of asymmetric multilayer polylactide nanofiber mats in controlled release of drugs and prevention of liver cancer recurrence after surgery in mice. Nanomed Nanotechnol Biol Med 11:1047–1056. https://doi.org/10.1016/j.nano.2015.03.001
Gonçalves C, Pereira P, Gama M (2010) Self-assembled hydrogel nanoparticles for drug delivery applications. Materials (Basel) 3:1420–1460. https://doi.org/10.3390/ma3021420
Liu L, Wu Q, Ma X, Xiong D, Gong C, Qian Z (2013) Camptothecine encapsulated composite drug delivery system for colorectal peritoneal carcinomatosis therapy: biodegradable microsphere in thermosensitive hydrogel. Coll Surf B 106:93–101. https://doi.org/10.1016/j.colsurfb.2013.01.047
Costa D, Queiroz J, Grac M, Lindman B (2012) Swelling behavior of a new biocompatible plasmid DNA hydrogel. Coll Surf B 92:106–112. https://doi.org/10.1016/j.colsurfb.2011.11.038
Wang Z, Xing L, Li J, Li B, Xu M, Liao Y et al (2015) Trimethyl borate as an electrolyte additive for high potential layered cathode with concurrent improvement of rate capability and cyclic stability. Electrochim Acta 184:40–46. https://doi.org/10.1016/j.electacta.2015.10.044
Truong VX, Barker IA, Tan M, Mespouille L, Dubois P, Dove AP (2013) Preparation of in situ-forming poly(5-methyl-5-allyloxycarbonyl-1, 3-dioxan-2-one)-poly(ethylene glycol) hydrogels with tuneable swelling, mechanical strength and degradability. J Mater Chem B 1:221–229
Selvam S, Pithapuram MV, Victor SP, Muthu J (2015) Injectable in situ forming xylitol—PEG-based hydrogels for cell encapsulation and delivery. Coll Surf B 126:35–43. https://doi.org/10.1016/j.colsurfb.2014.11.043
Hoare TR, Kohane DS (2008) Hydrogels in drug delivery: progress and challenges*. Polymer 49:1993–2007. https://doi.org/10.1016/j.polymer.2008.01.027
Yi H, Cho H-J, Cho S-M, Lee D-G, El-Aty AMA, Yoon S-J et al (2010) Pharmacokinetic properties and antitumor efficacy of the 5-fluorouracil loaded PEG-hydrogel. BMC Cancer 10:211
Han S, Hagiwara M, Ishizone T (2003) Synthesis of thermally sensitive water-soluble polymethacrylates by living anionic polymerizations of oligo (ethylene glycol) methyl ether methacrylates. Macromolecules 36:8312–8319
Sugihara S, Kanaoka S, Aoshima S (2005) Double thermosensitive diblock copolymers of vinyl ethers with pendant oxyethylene groups: unique physical gelation. Macromolecules 38:1919–1927
Zhao B, Li D, Hua F, Green DR. Synthesis of thermosensitive water-soluble polystyrenics with pendant methoxyoligo (ethylene glycol) groups by nitroxide-mediated radical polymerization. Macromolecules:9509–9517
Cheng Y, He C, Ding J, Xiao C, Zhuang X, Chen X (2013) Thermosensitive hydrogels based on polypeptides for localized and sustained delivery of anticancer drugs. Biomaterials 3:1–10. https://doi.org/10.1016/j.biomaterials.2013.09.064
Ho S, Tan JPK, Fukushima K, Nederberg F, Yan Y, Waymouth RM et al (2011) Thermoresponsive nanostructured polycarbonate block copolymers as biodegradable therapeutic delivery carriers. Biomaterials 32:5505–5514. https://doi.org/10.1016/j.biomaterials.2011.04.017
Gou M, Zheng X, Men K, Zhang J, Zheng L, Wang X, Luo F, Zhao Y, Zhao X, Wei Y, Qian Z (2009) Poly(ε-caprolactone)-poly(ethylene glycol)-poly(ε-caprolactone)Nanoparticles.pdf. J Phys Chem B 113:12928–12933
Mkhabela V, Ray SS (2015) Biodegradation and bioresorption of poly (ɛ-caprolactone) nanocomposite scaffolds. Int J Biol Macromol 79:186–192
Sharifi S, Mirzadeh H, Imani M, Rong Z (2009) Injectable in situ forming drug delivery system based on poly (e-caprolactone fumarate) for tamoxifen citrate delivery: gelation characteristics, in vitro drug release and anti-cancer evaluation. Acta Biomater 5:1966–1978. https://doi.org/10.1016/j.actbio.2009.02.004
Varan C, Bilensoy E (2014) Development of implantable hydroxypropyl-b-cyclodextrin coated polycaprolactone nanoparticles for the controlled delivery of docetaxel to solid tumors. J Incl Phenom Macrocycl Chem 3:1–7. https://doi.org/10.1007/s10847-014-0422-6
Pereira ADF, Pereira LGR, Barbosa LADO, Fialho SL, Pereira BG, Patricio PSDO et al (2013) Efficacy of methotrexate-loaded poly(ε-caprolactone) implants in Ehrlich solid tumor-bearing mice. Drug Deliv 20:168–179
Sridhar R, Ravanan S, Reddy J (2014) Curcumin- and natural extract-loaded nanofibres for potential treatment of lung and breast cancer: in vitro efficacy evaluation. J Biomater Sci 25:985–998. https://doi.org/10.1080/09205063.2014.917039
Gou M, Men K, Shi H, Xiang M, Zhang J, Song J et al (2011) Nanoscale Curcumin-loaded biodegradable polymeric micelles for colon cancer therapy in vitro and in vivo. Nanoscale 3:1558–1567. https://doi.org/10.1039/c0nr00758g
Wong BS, Teoh S, Kang L (2012) Polycaprolactone scaffold as targeted drug delivery system and cell attachment scaffold for postsurgical care of limb salvage. Drug Deliv Transl Res 2:272–283. https://doi.org/10.1007/s13346-012-0096-9
Prakash J, Modi S, Domb AJ, Kumar N (2005) Role of polyanhydrides as localized drug carriers. J Control Release 103:541–563. https://doi.org/10.1016/j.jconrel.2004.12.021
Katti DS, Lakshmi S, Langer R, Laurencin CT (2002) Toxicity, biodegradation and elimination of polyanhydrides. Adv Drug Deliv Rev 54:933–961
Storm PB, Moriarity JL, Tyler B, Burger PC, Brem H, Weingart J (2002) Polymer delivery of camptothecin against 9L gliosarcoma: release, distribution, and efficacy. J Neurooncol 56:209–217
Krasko MY, Shikanov A, Ezra A, Domb AJ (2003) Poly(ester anhydride) s prepared by the insertion of ricinoleic acid into poly (sebacic acid). J Polym Sci, Part A: Polym Chem 41:1059–1069
Shikanov A, Shikanov A, Vaisman B, Krasko MY, Nyska A, Domb AJ (2014) Poly (sebacic acid-co-ricinoleic acid) biodegradable carrier for paclitaxel: in vitro release and in vivo toxicity. J Biomed Res Part A: An Official J Soc Biomater, Aus Soc Biomater, Korean Soc Biomater. https://doi.org/10.1002/jbm.a.20101
Jain JP, Modi S, Kumar N (2007) Hydroxy fatty acid based polyanhydride as drug delivery system : synthesis, characterization, in vitro degradation, drug release, and biocompatibility. J Biomed Res Part A: An Official J Soc Biomater, Aus Soc Biomater, Korean Soc Biomater. https://doi.org/10.1002/jbm.a
Wang J, Yang G, Guo X, Tang Z, Zhong Z, Zhou S (2013) Biomaterials redox-responsive polyanhydride micelles for cancer therapy. Biomaterials. https://doi.org/10.1016/j.biomaterials.2013.12.025
Zia KM, Zia F, Zuber M, Rehman S, Ahmad MN (2015) Alginate based polyurethanes: a review of recent advances and perspective. Int J Biol Macromol 2:1–47. https://doi.org/10.1016/j.ijbiomac.2015.04.076
Barrioni BR, de Carvalho SM, Lambert R, Aline A, de Oliveira R, Pereira MDM (2015) Synthesis and characterization of biodegradable polyurethane films based on HDI with hydrolyzable crosslinked bonds and a homogeneous structure for biomedical applications. Mater Sci Eng, C 52:22–30. https://doi.org/10.1016/j.msec.2015.03.027
Chen Y, Wang R, Zhou J, Fan H, Shi B (2011) On-demand drug delivery from temperature-responsive polyurethane membrane. React Funct Polym 71:525–535. https://doi.org/10.1016/j.reactfunctpolym.2011.01.010
Kang S, Lee SC, Kim M (2010) Paclitaxel-polyurethane film for anti-cancer drug delivery: film characterization and preliminary in vivo study. Macromol Res 18:680–685. https://doi.org/10.1007/s13233-010-0715-6
Manabe T, Okino H, Maeyama R, Mizumoto K, Tanaka M, Matsuda T (2004) Short communication new infusion device for trans-tissue, sustained local delivery of anticancer agent to surgically resected tissue : potential use for suppression of local recurrence of pancreatic cancer. Wiley Period:203–207. https://doi.org/10.1002/jbm.b.30186
Nalwa HS (2008) Handbook of organic electronics and photonics. American Scientific Publication
Balint R, Cassidy NJ, Cartmell SH (2014) conductive polymers: towards a smart biomaterial for tissue engineering. Acta Biomater. https://doi.org/10.1016/j.actbio.2014.02.015
Rivers BTJ, Hudson TW, Schmidt CE (2002) Synthesis of a novel, biodegradable electrically conducting polymer for biomedical applications**. Adv Func Mater:33–37
Krukiewicz K, Zak JK (2014) Conjugated polymers as robust carriers for controlled delivery of anti-inflammatory drugs. J Mater Sci:5738–5745. https://doi.org/10.1007/s10853-014-8292-2
Svirskis D, Travas-sejdic J, Rodgers A, Garg S (2010) Electrochemically controlled drug delivery based on intrinsically conducting polymers. J Control Release 146:6–15. https://doi.org/10.1016/j.jconrel.2010.03.023
Shamaeli E, Alizadeh N (2013) Kinetic studies of electrochemically controlled release of salicylate from nanostructure conducting molecularly imprinted polymer. Electrochim Acta 114:409–415. https://doi.org/10.1016/j.electacta.2013.10.119
Wadhwa R, Lagenaur CF, Tracy X (2006) Electrochemically controlled release of dexamethasone from conducting polymer polypyrrole coated electrode. J Control Release 110:531–541. https://doi.org/10.1016/j.jconrel.2005.10.027
Krukiewicz K, Stok A, Zak JK (2015) Two approaches to the model drug immobilization into conjugated polymer matrix. Mater Sci Eng, C 54:176–181. https://doi.org/10.1016/j.msec.2015.05.017
Esra D, Razal JM, Moulton SE, Stewart EM, Wallace GG (2013) Multifunctional conducting fi bres with electrically controlled release of cipro floxacin. J Control Rel. https://doi.org/10.1016/j.jconrel.2013.01.022
Alizadeh N, Shamaeli E (2014) Electrochemically controlled release of anticancer drug methotrexate using nanostructured polypyrrole modified with cetylpyridinium: release kinetics investigation. Electrochim Acta 130:488–496. https://doi.org/10.1016/j.electacta.2014.03.055
Hoare TR, Kohane DS (2008) Hydrogels in drug delivery: progress and challenges. Polymer (Guildf) 49:1993–2007. https://doi.org/10.1016/j.polymer.2008.01.027
Weng L, Rostambeigi N, Zantek ND, Rostamzadeh P, Bravo M, Carey J, Golzarian J (2013) An in situ forming biodegradable hydrogel-based embolic agent for interventional therapies.pdf. Acta Biomater 3:1–36
Bhala N, Emberson J, Merhi A, Abramson S, Arber N et al (2013) Vascular and upper gastrointestinal eff ects of non-steroidal anti-inflammatory drugs: meta-analyses of individual. Lancet 6736:1–11. https://doi.org/10.1016/s0140-6736(13)60900-9
Haupt S, Zioni T, Gati I, Kleinstern J, Rubinstein A (2006) Luminal delivery and dosing considerations of local celecoxib administration to colorectal cancer. Eur J Pharm Sci 8:204–211. https://doi.org/10.1016/j.ejps.2006.02.001
Coffer J, Canham L (2000) Porosified silicon wafer structures impregnated with platinum anti-tumor compounds : fabrication, characterization, and diffusion studies. Biomed Microdevices 2:265–272. https://doi.org/10.1023/A:1009951121205
Kakran M, Sahoo NG, Bao H, Pan Y, Li L (2011) Functionalized graphene oxide as nanocarrier for loading and delivery of ellagic Acid. Curr Med Chem 18:4503–4512. https://doi.org/10.2174/092986711797287548
Liu J, Guo S, Han L, Wang T, Hong W, Wang E (2012) Synthesis of phospholipid monolayer membrane functionalized graphene for drug delivery†. J Mater Chem 22:20634–20640. https://doi.org/10.1039/c2jm34494g
Chang G, Ci T, Yu L, Ding J (2011) Enhancement of the fraction of the active form of an antitumor drug topotecan via an injectable hydrogel. J Control Release 156:21–27. https://doi.org/10.1016/j.jconrel.2011.07.008
Erdogar N, Iskit AB, Eroglu H, Sargon MF, Mungan NA, Bilensoy E (2014) Cationic core-shell nanoparticles for intravesical chemotherapy in tumor-induced rat model: safety and efficacy. Int J Pharm 471:1–9. https://doi.org/10.1016/j.ijpharm.2014.05.014
Mi P, Kokuryo D, Cabral H, Wu H, Terada Y, Saga T et al (2016) A pH-activatable nanoparticle with signal-amplification capabilities for non-invasive imaging of tumour malignancy. Nat Nanotechnol 11:724
Sharma S, Chockalingam S, Sanpui P, Chattopadhyay A, Ghosh SS (2014) Silver nanoparticles impregnated alginate–chitosan-blended nanocarrier induces apoptosis in human glioblastoma cells. Adv Healthc Mater 3:106–114
Mir M, Ishtiaq S, Rabia S, Khatoon M, Zeb A, Khan GM et al (2017) Nanotechnology: from in vivo imaging system to controlled drug delivery. Nanoscale Res Lett 12:500
Anselmo AC, Mitragotri S (2016) Nanoparticles in the clinic. Bioeng Transl Med 1:10–29
Ye F, Barrefelt Å, Asem H, Abedi-Valugerdi M, El-Serafi I, Saghafian M et al (2014) Biodegradable polymeric vesicles containing magnetic nanoparticles, quantum dots and anticancer drugs for drug delivery and imaging. Biomaterials 35:3885–3894
Zakrewsky M, Mitragotri S (2016) Therapeutic RNAi robed with ionic liquid moieties as a simple, scalable prodrug platform for treating skin disease. J Control Release 242:80–88
Fu Q, Xu J, Ladewig K, Henderson TMA, Qiao GG (2015) Degradable cross-linked polymer vesicles for the efficient delivery of platinum drugs. Polym Chem 6:35–43
Ulery BD, Nair LS, Laurencin CT (2011) Biomedical applications of biodegradable polymers. J Polym Sci, Part B: Polym Phys 49:832–864
Yang S, Chen D, Li N, Mei X, Qi X, Li H et al (2012) A facile preparation of targetable pH-sensitive polymeric nanocarriers with encapsulated magnetic nanoparticles for controlled drug release. J Mater Chem 22:25354–25361
Wang S, Wang H, Liu Z, Wang L, Wang X, Su L et al (2014) Smart pH-and reduction-dual-responsive folate–PEG-coated polymeric lipid vesicles for tumor-triggered targeted drug delivery. Nanoscale 6:7635–7642
Gandhi A, Paul A, Sen SO, Sen KK (2015) Studies on thermoresponsive polymers: Phase behaviour, drug delivery and biomedical applications. Asian J Pharm Sci 10:99–107
Wiltsey C, Christiani T, Williams J, Scaramazza J, Van Sciver C, Toomer K et al (2015) Thermogelling bioadhesive scaffolds for intervertebral disk tissue engineering: preliminary in vitro comparison of aldehyde-based versus alginate microparticle-mediated adhesion. Acta Biomater 16:71–80
Supper S, Anton N, Boisclair J, Seidel N, Riemenschnitter M, Curdy C et al (2014) Chitosan/glucose 1-phosphate as new stable in situ forming depot system for controlled drug delivery. Eur J Pharm Biopharm 88:361–373
Kakkar A, Traverso G, Farokhzad OC, Weissleder R, Langer R (2017) Evolution of macromolecular complexity in drug delivery systems. Nat Rev Chem 1:63
Cao W, Wang L, Xu H (2015) Selenium/tellurium containing polymer materials in nanobiotechnology. Nano Today 10:717–736
Meng F, Hennink WE, Zhong Z (2009) Reduction-sensitive polymers and bioconjugates for biomedical applications. Biomaterials 30:2180–2198
Cheng G, He Y, Xie L, Nie Y, He B, Zhang Z et al (2012) Development of a reduction-sensitive diselenide-conjugated oligoethylenimine nanoparticulate system as a gene carrier. Int J Nanomedicine 7:3991
Zhao M, Biswas A, Hu B, Joo K-I, Wang P, Gu Z et al (2011) Redox-responsive nanocapsules for intracellular protein delivery. Biomaterials 32:5223–5230
Gajanayake T, Olariu R, Leclère FM, Dhayani A, Yang Z, Bongoni AK et al (2014) A single localized dose of enzyme-responsive hydrogel improves long-term survival of a vascularized composite allograft. Sci Transl Med 6:249ra110
Kim H-J, Zhang K, Moore L, Ho D (2014) Diamond nanogel-embedded contact lenses mediate lysozyme-dependent therapeutic release. ACS Nano 8:2998–3005
Lee TT, García JR, Paez JI, Singh A, Phelps EA, Weis S et al (2015) Light-triggered in vivo activation of adhesive peptides regulates cell adhesion, inflammation and vascularization of biomaterials. Nat Mater 14:352
Marturano V, Cerruti P, Giamberini M, Tylkowski B, Ambrogi V (2017) Light-responsive polymer micro-and nano-capsules. Polymers (Basel) 9:8
Timko BP, Arruebo M, Shankarappa SA, McAlvin JB, Okonkwo OS, Mizrahi B et al (2014) Near-infrared–actuated devices for remotely controlled drug delivery. Proc Natl Acad Sci 111:1349–1354
Pearson S, Vitucci D, Khine YY, Dag A, Lu H, Save M et al (2015) Light-responsive azobenzene-based glycopolymer micelles for targeted drug delivery to melanoma cells. Eur Polym J 69:616–627
Qazi TH, Rai R, Boccaccini AR (2014) Tissue engineering of electrically responsive tissues using polyaniline based polymers: a review. Biomaterials 35:9068–9086
Ge J, Neofytou E, Cahill TJ III, Beygui RE, Zare RN (2011) Drug release from electric-field-responsive nanoparticles. ACS Nano 6:227–233
Balogh D, Tel-Vered R, Freeman R, Willner I (2011) Photochemically and electrochemically triggered Au nanoparticles “sponges”. J Am Chem Soc 133:6533–6536
Liu H-L, Fan C-H, Ting C-Y, Yeh C-K (2014) Combining microbubbles and ultrasound for drug delivery to brain tumors: current progress and overview. Theranostics 4:432
Campbell KT, Hadley DJ, Kukis DL, Silva EA (2017) Alginate hydrogels allow for bioactive and sustained release of VEGF-C and VEGF-D for lymphangiogenic therapeutic applications. PLoS One 12:e0181484
Odeyemi I, Abou-setta AM (2013) Leuprolide acetate 1-, 3- and 6-monthly depot formulations in androgen deprivation therapy for prostate cancer in nine European countries: evidence review and economic evaluation. Clin Econ Outcomes Res 5:257–269
Zhao Y, Alakhova DY, Kim JO, Bronich TK, Kabanov AV (2014) A simple way to enhance doxil® therapy: drug release from liposomes at the tumor site by amphiphilic block copolymer. J Control Release 168:61–69. https://doi.org/10.1016/j.jconrel.2013.02.026.A
Douer D (2016) Efficacy and safety of vincristine sulfate liposome injection in the treatment of adult acute lymphocytic leukemia. Oncologist 3:840–847
Zhao M, Lei C, Yang Y, Bu X, Ma H, Gong H (2015) Abraxane, the nanoparticle formulation of paclitaxel can induce drug resistance by upregulation of P-gp. PLoS One 3:1–19. https://doi.org/10.1371/journal.pone.0131429
Bahl A, Challapalli A, Greenwood R, Hurley K, Persad R (2017) Quality of life evaluation of the effect of decapeptyl compared with zoladex preradiotherapy: final results of randomised controlled trial. J Clin Oncol 35:62. https://doi.org/10.1200/JCO.2017.35.6_suppl.62
Saltzstein D, Shore ND, Moul JW, Chu F, Concepcion R, De Motte S et al (2018) Pharmacokinetic and pharmacodynamic comparison of subcutaneous versus intramuscular leuprolide acetate formulations in male subjects. Ther Adv Urol 10:43–50. https://doi.org/10.1177/1756287217738150
Bhullar KS, Lagarón NO, Mcgowan EM, Parmar I, Jha A, Hubbard BP et al (2018) Kinase-targeted cancer therapies: progress, challenges and future directions. Mol Cancer 17:48–68
Wang F, Porter M, Konstantopoulos A, Zhang P, Cui H (2018) Preclinical development of drug delivery systems for paclitaxel-based cancer chemotherapy. J Control Release 10:100–118. https://doi.org/10.1016/j.jconrel.2017.09.026.preclinical
Dahms J, Carr JP, Lautenbach SD (2008) DUROS® technology delivers peptides and proteins at consistent rate continuously for 3 to 12 months. J Diabetes Sci Technol 2:461–467
Ashby LS, Smith KA, Stea B (2016) Gliadel wafer implantation combined with standard radiotherapy and concurrent followed by adjuvant temozolomide for treatment of newly diagnosed high-grade glioma: a systematic literature review. World J Surg Oncol:1–15. https://doi.org/10.1186/s12957-016-0975-5
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Rajakumari, R., Thomas, S., Kalarikkal, N. (2021). Biomaterials and Its Advances for Delivering Anticancer Drugs. In: Joshy, K.S., Thomas, S., Thakur, V.K. (eds) Nanoparticles for Drug Delivery. Gels Horizons: From Science to Smart Materials. Springer, Singapore. https://doi.org/10.1007/978-981-16-2119-2_2
Download citation
DOI: https://doi.org/10.1007/978-981-16-2119-2_2
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-16-2118-5
Online ISBN: 978-981-16-2119-2
eBook Packages: Chemistry and Materials ScienceChemistry and Material Science (R0)