Abstract
Despite significant advances in surgery, chemotherapy, radiotherapy, endocrine therapy, and molecular-targeted therapy, breast cancer remains the leading cause of death from malignant tumors among women. Immunotherapy has recently become a critical component of breast cancer treatment with encouraging activity and mild safety profiles. CAR-T therapy using genetically modifying T cells with chimeric antigen receptors (CAR) is the most commonly used approach to generate tumor-specific T cells. It has shown good curative effect for a variety of malignant diseases, especially for hematological malignancies. In this review, we briefly introduce the history and the present state of CAR research. Then we discuss the barriers of solid tumors for CARs application and possible strategies to improve therapeutic response with a focus on breast cancer. At last, we outlook the future directions of CAR-T therapy including managing toxicities and developing universal CAR-T cells.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
17.1 Introduction
Breast cancer is the most diagnosed cancer in women. Despite significant advances in surgery, chemotherapy, radiotherapy, endocrine therapy, and now molecular-targeted therapy, breast cancer remains the leading cause of death from malignant tumors among women [1, 2]. After decades of researches and trials, it seems that manipulation and utilization of antitumor properties of the immune system have begun to show promise for a variety of tumors [3, 4]. Through the years, many advances have been made in the immunotherapy of breast cancer. Immunotherapy has become an important part of breast cancer treatment, along with encouraging activity and mild safety.
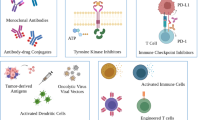
Immunotherapy for breast cancer involves a wide range of therapies including monoclonal antibodies (mAbs), vaccinations, immune checkpoint inhibition, and adoptive T-cell transfer immunotherapy. HER-2/neu monoclonal antibody has been successfully used in treatment for breast cancer patients. However, overexpression of HER-2/neu accounts for only 25–30% of breast cancer patients. Vaccinations induce specific antitumor immunity, but objective tumor regression is rarely observed in clinic [5]. Cytotoxic T cells play a key role in immune-mediated control of cancer [6,7,8,9,10,11,12]. Plenty of studies have proved that the extent of cytotoxic T cell-infiltrating tumors is a key factor in determining the natural progression of a variety of cancers [6,7,8,9, 13,14,15]. Over the past two decades, T-cell-based immune therapy has gained general acceptance with its curative potency for several types of malignant diseases [16]. Current T-cell-based immune therapies are generally based on two methods. The first involves the isolation of antitumor T lymphocytes from the primary tumor tissues of the patients, which is called tumor-infiltrating lymphocytes (TILs). However, due to the difficulties of TIL isolation and culture, TIL therapy is limited to a few types of tumors with high number of TIL [17]. Another way is to generate T cells with a predetermined antitumor specificity via gene therapy-based approaches. There are two gene modification strategies, including TCR gene transfer and chimeric antigen receptor (CAR) gene transfer, which are used to endow polyclonal T cells with an antigen specificity of choice. We highlight the CAR-T cell therapy in this review.
17.2 Present State of CAR-T Therapy
Genetically modifying T cells with CARs is the most common method of producing tumor-specific T cells. CARs usually consist of an extracellular ligand-binding domain of a single-chain antibody (scFv), a hinge, a transmembrane domain, a cytoplasmic signaling chain, and/or costimulatory molecules. CAR-engineered T cells combine the specificity of mAbs with the homing and killing capacity of T cells. Specifically, CAR-T cell therapy is considered to have several advantages when compared with other cellular immunotherapies. Firstly, CAR-T cells are generated using nonspecifically activated polyclonal T cells. Therefore, they overcome the difficulty of isolation and amplification of natural tumor-specific CD4+ and CD8+ T cells [18, 19]. Secondly, CAR-T cells recognize the target antigens in a MHC-independent manner. This property enables CAR-T cells to recognize target cells with reduced HLA expression or antigen processing, which are considered as an important factor in tumor immunological escape [20,21,22]. Thirdly, CAR-T cells can home to tumor sites actively and specifically and possess the capacity to expand and persist over a long term after tumor recognition in vivo. Therefore, CAR-T cells targeted to tumor-associated antigens (TAAs) may be more effective than mAbs in producing long-lasting tumor responses [23]. Another particular advantage of CAR-T cells is the capacity to cross the blood–brain barrier [24]. This characteristic is highly useful for treating malignant tumors that involve in or have been transferred to the central nervous system, though adverse reactions relevant to central nervous system must be considered as well.
The concept of the CAR was put forward by Gross and colleagues in 1989, who fused the antibody-binding domain Fab with the TCR signaling domain CD3ζ and named it as T body. Since then, different generations of CAR-T cells have been claimed with confusing definition. In our opinion, based on the three signals required for T-cell activation, which are TCR, costimulation, and cytokine, CAR-T cells could be divided into three generations (Fig. 17.1). The first generation of CARs contained scFv and only a single signaling domain derived from CD3ζ [25]. However, the effect of the first-generation CAR trials was disappointing. Both complete T-cell activation and prevention of apoptosis required a costimulatory signal [26]. The second-generation CARs were subsequently developed, which contained two or three costimulatory signal domains of CD28 and/or 4-1BB, or other costimulatory molecules, to complete the activation signal of the CAR-T cells [27, 28]. The third-generation CARs were embedded into a cytokine cassette which endowed the CAR-T cells with a better function or survival environment. Other features such as migration, homeostatic proliferation, suppression resistance, etc. were subsequently embedded into CAR-T cells, which were described as TRUCK CAR-T cells [29, 30]. For example, the transgenic cytokine IL-12 produced by TRUCK T cells not only improves T-cell activation and modulates the immunological environment but also recruits other immune cells for the fight against those antigen-negative cancer cells that are not recognized by CAR-T cells. Other cytokines like IL-23, IL-27, and IL-15 are alternative payload for TRUCK T cells. In treatment for solid cancer, such TRUCK T cells might have an advantage to modulate the tumor environment, thus enhancing the T-cell antitumor response [31, 32].
T cells engrafted with CAR recognize a wide variety of TAAs expressed on a broad range of tumors, representing both solid and hematologic malignancies. One of the most impressive clinical results ever achieved by CAR-T cells is that polyclonal T cells express CD19-specific CARs with CD28-CD3ζ or 41BB-CD3ζ as signaling domains [24, 33,34,35,36,37]. Complete responses were achieved after infusion of 2nd generation CAR-T cells in patients with CD19+ hematological malignancies including NHL, acute lymphoblastic leukemia (ALL) and chronic lymphocytic leukemia (CLL). There are also clinical studies with 2nd generation CAR-T cells specific for the κ-light chain of human immunoglobulin or for CD30. Clinical responses including CRs have been observed [38, 39]. In contrast to B-cell malignancies, clinical experiences of CARs in treatment of T-cell or myeloid-derived malignancies are limited.
17.3 CAR-T Therapy for Breast Cancer: Problems and Solutions
CAR-based therapy for solid tumors involves the use of CARs targeting colorectal cancer [40, 41], ovarian cancer [42], prostate cancer [43], metastatic renal cell carcinoma, and so on [44]. There are also studies targeting HER-2, Lewis Y, mesothelin, folate receptor alpha (FR-α), and Muc1 for breast cancer in vitro and in animal models [28, 40, 45,46,47,48,49,50,51,52,53,54,55]. HER-2 expression is known to impact breast cancer recurrence and ultimately survival [56]. The use of anti-HER2 mAbs has significantly improved breast cancer prognosis. HER-2-targeted therapies are now a main component of HER-2 overexpressing breast cancer treatment [57, 58]. There are several clinical trials of CAR-T cells targeting HER-2 in progress, such as a phase I/II study of HER-2-targeted CAR-T cells in chemotherapy or HER-2 antibody inhibitor therapy for refractory HER-2-advanced breast cancer (NCT01935843) and a phase II study of anti-CD3 x anti-HER2/Neu-armed activated T cells after second-line chemotherapy in women with HER2/Neu (0, 1+ or 2+) metastatic breast cancer (NCT01022138). Moreover, clinical trials of CAR-T-cell therapy targeting other antigens for patients with breast cancer are ongoing, including a phase I study of CAR-T cells targeting cMet, which is aberrant activation in cancer and correlates with poor prognosis, in metastatic breast cancer refractory to at least one standard treatment or newly diagnosed patients with operable triple-negative breast cancer (TNBC) (NCT03060356), and a phase I study of CAR-T cells targeting mesothelin, a tumor antigen associated with TNBC, in metastatic HER2-negative breast cancer (NCT02580747). Despite the successes in treating hematological malignancies, CAR-T cells have encountered significant challenges for treatment of solid tumors [44, 59,60,61,62]. Some of the key problems are the rarity of target antigens, limited persistence of the CAR-T cells, inefficient homing of T cells to tumor sites, and less cytotoxicity in the local tumor immunosuppressive microenvironment [63]. The preclinical and clinical studies on treatment for breast cancer with CAR-T therapy are summarized in Table 17.1.
17.3.1 Target Antigen
Antigens currently targeted in clinical studies include HER2, mesothelin, CEA, carbonic anhydrase IX (CAIX), FR-α, CD171, GD2, EGFRvIII, fibroblast activation protein (FAP), and vascular endothelial growth factor receptor 2 (VEGF-R2) [64]. Like other forms of cancer immunotherapy, CARs should ideally target antigens that are expressed only on cancer cells but not on normal tissues. Besides, unlike the native TCR, the CARs containing scFv only recognize target antigens expressed on the cell surface, rather than internal antigens which are processed and rendered by the cells’ MHC. Consequently, only few solid tumor antigens are available, though numerous antigens are being actively explored for CAR-T cell therapy. An alternative approach is to target antigen-MHC complex, which could make intracellular antigens available, though the generation of this kind of antibody is quite difficult. Conventional T cells only recognize single antigens, but CAR-T cells could be genetically modified to recognize multiple antigens, which should allow the recognition of unique antigen expression patterns on tumor cells. One example is the “split signal CARs,” which limit full T-cell activation to tumors that express multiple antigens [43, 65, 66]. Other strategies for recognizing multiple antigens include tandem CARs, ectodomains of which are 2 scFvs [67], and so-called universal ectodomain CARs that incorporate avidin or a fluorescein isothiocyanate-specific scFv to identify tumor cells incubated with labeled monoclonal antibodies [43, 65, 68, 69]. Another possible concern is immune escape. Antigenic shift may cause tumor cells to produce new tumor antigens that may not be identified by the original CAR-T cells. Such escape variants are not rare because most of the cancer cells are genetically unstable [70]. Immune escape, previously described as a drug resistance mechanism in chemotherapy, may become a dilemma in cell-based therapies. The risk of immune escape can be reduced by targeting multiple antigens. Another solution is to target antigens that are expressed on the tumor stroma. The tumor stromal compartment supports tumor growth directly by secreting cytokines and growth factors, providing nutrients, and contributing to tumor-induced immunosuppression [71]. Moreover, tumor stroma is demonstrated to be genetically more stable by studies targeting FAP expressed on cancer-associated fibroblasts or VEGFR-2 expressed on the endothelial cells of the tumor vasculature [72,73,74,75].
17.3.2 Persistence
It is important to achieve high levels of CAR-T cells persisting in the peripheral circulation of patients, in order to ensure sufficient cells are available to penetrate into tumor sites. Early trials using the first generation of CAR-T cells targeting ovarian [76] and renal cell antigens [44] indicated that the lack of persistence might be induced by lack of patient preconditioning or anti-CAR immune responses. CARs were then added with costimulatory signals to improve persistence in vivo, particularly when administered to lymphodepleted hosts [36, 77, 78]. Another effort to improve the persistence of CAR-T cells focuses on the range of cytokines that are used to culture the T cells. IL-2 has been selected as an essential cytokine to drive the expansion of T cells in vitro. There are other cytokines including IL-15, IL-7, and IL-21 that can result in cultured T cells preferential to IL-2-expanded T cells. Studies show that IL-15 can promote the proliferation of T lymphocytes, prevent apoptosis and exhaustion [79, 80], reverse anergy [79], stimulate long-lasting antigen-experienced memory cells [81], and overcome Treg-mediated inhibition [82,83,84,85]. IL-7 plays an important role in maintaining the homeostasis of mature T cells and the maintenance of memory T cells [86]. Meanwhile, CAR-T cells can be genetically modified to produce cytokines to improve the expansion and persistence in vivo while avoiding systemic toxicity [30, 82, 84, 87]. The function of CAR-T cells may be enhanced not only by adding stimulatory signals (costimulation, cytokines/cytokine receptors) but also by blocking down regulatory signals. Antibodies that block the programmed death-1 (PD-1) receptor or the PD-L1 ligand or the cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4) have produced encouraging clinical results as single agents [3, 88]. Convincing evidence also demonstrates their benefit for triple-negative breast cancer [89]. The combination of these antibodies with CAR-T cells prolongs the effector function of CAR-T cells at tumor sites, which is a logical evolution of current clinical strategies.
Besides, the source and phenotype of T cells used to generate CAR-T cells will affect the latter’s persistence. Selecting T cells that express naive markers such as CD62L before the genetic modification may produce CAR-T cells that possess better persistence ability than effector or more differentiated T cells [90]. Alternatively, virus-specific cytotoxic T lymphocytes (CTLs) have the potential for life-long persistence, and the CTLs contain both CD4+ and CD8+ subsets, with the latter being a critical compartment for the former’s long-term persistence [91, 92]. Virus-specific CTLs also feature expression of homing/chemokines receptors commensurate with their capacity for trafficking to and residing in the designated lymphoid or non-lymphoid tissues [93]. Memory T-stem cell could differentiate into memory T cells, leading to a continuous supply of CAR-T cells. On the other hand, hematopoietic stem cells could be engineered with CARs to produce CAR-T cells in a sustained way [94].
17.3.3 Homing
Since the direct binding of tumor antigen is the primary condition of CAR to display its function, the efficient migration of CAR-T cells into tumor sites is essential to the success of the CAR-based therapeutic approach. The success of CAR-T cell therapy for B-cell malignancies is probably caused by the fact that the target B cells are readily accessible to CAR-T cells and express a variety of costimulatory receptor ligands that can promote CAR-T cell function [95]. Chemokines play an important role in the migration of lymphocytes [96], as typified by recent studies [97,98,99]. However, the chemokine system is complex. Therefore, it is important to develop a strategy to make use of the important homing chemokines and avoid the potential regulatory effect of other tumor-expressed chemokines, in order to achieve efficient targeting of CAR-T cells [17].
17.3.4 Tumor Microenvironment
The tumor microenvironment possesses a variety of pro-tumorigenic and immunosuppressive qualities that are consistent with supporting tumor growth and proliferation and with preventing the antitumor effects of the immune system. The tumor microenvironment comprises several factors such as immunosuppressive cytokines, regulatory modulators, and coinhibitory receptors [100]. The immunosuppressive cell populations include regulatory T cells, immature myeloid cell populations, and tumor-associated macrophages [9, 101,102,103]. As highly complex interactions among different components in the tumor microenvironment contribute to clinical outcomes, CAR-T cells must be armed and thrive in the environment. Genetically engineering of the CAR vector to include dominant negative TGFβ receptors to overcome the adverse effects of tumor-derived TGFβ [104], and to adopt knockdown strategies to avoid apoptosis mediated by Fas/Fas ligand [105] or the expression of survival genes such as BCL-XL [106], may protect the CAR-T cells against the tumor immunosuppressive microenvironment. Besides, transgenic expression of cytokines such as IL-15 or IL-12 can reverse the immunosuppressive tumor environment. In an alternate strategy, silencing of genes that inhibit the function of T cells in the tumor microenvironment or the transgenic expression of constitutively active signaling molecules may improve CAR-T cell function [105, 107]. Lastly, a combined treatment of agents that propagate cell-based immunotherapies and agents that circumvent antitumor mechanisms may be beneficial for CAR-T cells to overcome the tumor microenvironment.
17.4 Toxicities and Management
As the potency of CARs was enhanced, toxicity induced by this immunotherapeutic approach was unfortunately observed. The continued expansion of CAR-T cells implies that the associated toxicities may show corresponding persistence and deterioration with time. “On target, off tumor” toxicity is currently a major concern, which results from the activation of CAR-T cells by targeting antigen within healthy tissues. This is a well-recognized phenomenon and has led to several different side effects. Prevention of on-target toxicity requires accurate selection of antigens that are more restricted in their expression. Another approach is to infuse CAR-T cells with transient expression of the CARs only. Thus, the expression level decreases with the cell division, and the transcription becomes diluted gradually [108,109,110]. Another well-documented clinical side effect is systemic inflammatory response syndrome (SIRS) or cytokine storm, which is driven by a variety of cytokines, including IFN-γ, TNF-α, IL-2 [33, 77], and the most important IL-6 [24]. To reduce the onset or severity of SIRS, researchers are modifying the dose escalation of T cells and have introduced the prompt use of antibodies that block the effects of IL-6. In addition, there are genetically modified T cells expressing a suicide or safety switch along with the CAR. These cells would retain their long-term expansion and expression capacity, but could be eliminated by activating the suicide genes once toxicity occurs [111,112,113]. Although the expression of multiple CARs in T cells is likely to increase safety [43, 65, 66], it remains to be proved whether the benefits can be summarized within heterogeneous human malignancies, as the patterns and levels of antigen expression may vary between different malignancies.
17.5 Universal CAR-T Cells
The current standard CAR-T cell therapy requires autologous adoptive cell transfer, which is expensive and time-consuming. For newborns and elder patients, it is often difficult to obtain enough T cells with good quality to generate patient-specific CAR-T cells. To make CAR-T therapy more accessible, it is highly desirable to develop an allogeneic adoptive transfer strategy, in which universal CAR-T cells derived from healthy donors can be applied to treat multiple patients circumventing the inherent variability of individualized patient. For this strategy to work, human leukocyte antigens class I (HLA-Is) on CAR-T cells need to be removed to minimize their immunogenicity, and the T-cell receptor (TCR) on allogeneic CAR-T cells needs to be eliminated to avoid graft-versus-host disease (GVHD) [114]. There have been studies to efficiently generate CAR-T cells with TCRα subunit constant (TRAC) and beta-2 microglobulin (β2M) genes disrupted. However, these TRAC/β2M-negative CAR-T cells need to be further tested for their efficacy and safety in clinical studies [114,115,116].
17.6 Combinatorial CAR-T Cell Therapy
It may be better to fight a war with a well-orchestrated army than a “single bullet,” so combining CAR-T cells with other therapies offers the potential to improve antitumor effects. For example, combining blocking antibodies (CTLA-4, PD-1, and PD-L1) to the coinhibitory receptors, epigenetic modifiers that upregulate the expression of TAA [117], or targeted therapies that inhibit tumor cell growth without impairing T cells may be beneficial [118]. In the future, experimental treatment will be needed to determine how the CAR-T cell approach will be combined with other therapies for solid tumors, such as breast cancer.
17.7 Conclusions
The general concept of CAR-T cell was invented about 20 years ago. CAR-T cells are changing from being simply “promising” to being “effective” regimens for treating hematological malignancies. As we continue to improve the function of CAR-T cells in tumor microenvironment, broader application can be expected beyond hematological tumors and into solid tumors. Clinical trials comparing different genetic modification strategies will be important in the future for optimizing CAR-T cell therapy, which would be a potentially effective method to cure breast cancer disease.
References
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics, 2017. CA Cancer J Clin 67(1):7–30
Chen W et al (2016) Cancer statistics in China, 2015. CA Cancer J Clin 66(2):115–132
Brahmer JR et al (2012) Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med 366(26):2455–2465
Topalian SL et al (2012) Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 366(26):2443–2454
Zhou J, Zhong Y (2004) Breast cancer immunotherapy. Cell Mol Immunol 1(4):247–255
Galon J et al (2006) Type, density, and location of immune cells within human colorectal tumors predict clinical outcome. Science 313(5795):1960–1964
Hamanishi J et al (2007) Programmed cell death 1 ligand 1 and tumor-infiltrating CD8+ T lymphocytes are prognostic factors of human ovarian cancer. Proc Natl Acad Sci U S A 104(9):3360–3365
Mahmoud SM et al (2011) Tumor-infiltrating CD8+ lymphocytes predict clinical outcome in breast cancer. J Clin Oncol 29(15):1949–1955
Bindea G et al (2013) Spatiotemporal dynamics of intratumoral immune cells reveal the immune landscape in human cancer. Immunity 39(4):782–795
Matsushita H et al (2012) Cancer exome analysis reveals a T-cell-dependent mechanism of cancer immunoediting. Nature 482(7385):400–404
Oble DA et al (2009) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human melanoma. Cancer Immun 9:3
DuPage M et al (2012) Expression of tumour-specific antigens underlies cancer immunoediting. Nature 482(7385):405–409
Pages F et al (2009) In situ cytotoxic and memory T cells predict outcome in patients with early-stage colorectal cancer. J Clin Oncol 27(35):5944–5951
Rusakiewicz S et al (2013) Immune infiltrates are prognostic factors in localized gastrointestinal stromal tumors. Cancer Res 73(12):3499–3510
Stumpf M et al (2009) Intraepithelial CD8-positive T lymphocytes predict survival for patients with serous stage III ovarian carcinomas: relevance of clonal selection of T lymphocytes. Br J Cancer 101(9):1513–1521
Dotti G et al (2001) Adenovector-induced expression of human-CD40-ligand (hCD40L) by multiple myeloma cells. A model for immunotherapy. Exp Hematol 29(8):952–961
Cheadle EJ et al (2014) CAR T cells: driving the road from the laboratory to the clinic. Immunol Rev 257(1):91–106
Pittet MJ et al (2001) Expansion and functional maturation of human tumor antigen-specific CD8+ T cells after vaccination with antigenic peptide. Clin Cancer Res 7(3 Suppl): 796s–803s
Valmori D et al (2000) Naturally occurring human lymphocyte antigen-A2 restricted CD8+ T-cell response to the cancer testis antigen NY-ESO-1 in melanoma patients. Cancer Res 60(16):4499–4506
Jakobsen MK et al (1995) Defective major histocompatibility complex class I expression in a sarcomatoid renal cell carcinoma cell line. J Immunother Emphasis Tumor Immunol 17(4):222–228
Lou Y et al (2008) Combining the antigen processing components TAP and Tapasin elicits enhanced tumor-free survival. Clin Cancer Res 14(5):1494–1501
Singh R, Paterson Y (2007) Immunoediting sculpts tumor epitopes during immunotherapy. Cancer Res 67(5):1887–1892
Sun M et al (2014) Construction and evaluation of a novel humanized HER2-specific chimeric receptor. Breast Cancer Res 16(3):R61
Grupp SA et al (2013) Chimeric antigen receptor-modified T cells for acute lymphoid leukemia. N Engl J Med 368(16):1509–1518
Eshhar Z et al (2001) Functional expression of chimeric receptor genes in human T cells. J Immunol Methods 248(1–2):67–76
Lenschow DJ, Walunas TL, Bluestone JA (1996) CD28/B7 system of T cell costimulation. Annu Rev Immunol 14:233–258
Carpenito C et al (2009) Control of large, established tumor xenografts with genetically retargeted human T cells containing CD28 and CD137 domains. Proc Natl Acad Sci U S A 106(9):3360–3365
Song DG et al (2012) CD27 costimulation augments the survival and antitumor activity of redirected human T cells in vivo. Blood 119(3):696–706
Chmielewski M et al (2011) IL-12 release by engineered T cells expressing chimeric antigen receptors can effectively muster an antigen-independent macrophage response on tumor cells that have shut down tumor antigen expression. Cancer Res 71(17):5697–5706
Zhang L et al (2011) Improving adoptive T cell therapy by targeting and controlling IL-12 expression to the tumor environment. Mol Ther 19(4):751–759
Hunter CA (2005) New IL-12-family members: IL-23 and IL-27, cytokines with divergent functions. Nat Rev Immunol 5(7):521–531
Tamzalit F et al (2014) IL-15.IL-15Ralpha complex shedding following trans-presentation is essential for the survival of IL-15 responding NK and T cells. Proc Natl Acad Sci U S A 111(23):8565–8570
Kochenderfer JN et al (2012) B-cell depletion and remissions of malignancy along with cytokine-associated toxicity in a clinical trial of anti-CD19 chimeric-antigen-receptor-transduced T cells. Blood 119(12):2709–2720
Brentjens RJ et al (2011) Safety and persistence of adoptively transferred autologous CD19-targeted T cells in patients with relapsed or chemotherapy refractory B-cell leukemias. Blood 118(18):4817–4828
Porter DL et al (2011) Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N Engl J Med 365(8):725–733
Kalos M et al (2011) T cells with chimeric antigen receptors have potent antitumor effects and can establish memory in patients with advanced leukemia. Sci Transl Med 3(95): 95ra73
Brentjens RJ et al (2013) CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci Transl Med 5(177):177ra38
Savoldo B et al (2007) Epstein Barr virus specific cytotoxic T lymphocytes expressing the anti-CD30zeta artificial chimeric T-cell receptor for immunotherapy of Hodgkin disease. Blood 110(7):2620–2630
Ramos CA et al (2016) Clinical responses with T lymphocytes targeting malignancy-associated kappa light chains. J Clin Invest 126(7):2588–2596
Morgan RA et al (2010) Case report of a serious adverse event following the administration of T cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol Ther 18(4):843–851
Schlimper C et al (2012) Improved activation toward primary colorectal cancer cells by antigen-specific targeting autologous cytokine-induced killer cells. Clin Dev Immunol 2012:238924
Kandalaft LE, Powell DJ, Coukos G (2012) A phase I clinical trial of adoptive transfer of folate receptor-alpha redirected autologous T cells for recurrent ovarian cancer. J Transl Med 10:157
Kloss CC et al (2013) Combinatorial antigen recognition with balanced signaling promotes selective tumor eradication by engineered T cells. Nat Biotechnol 31(1):71–75
Lamers CH et al (2013) Treatment of metastatic renal cell carcinoma with CAIX CAR-engineered T cells: clinical evaluation and management of on-target toxicity. Mol Ther 21(4):904–912
Davies DM et al (2012) Flexible targeting of ErbB dimers that drive tumorigenesis by using genetically engineered T cells. Mol Med 18:565–576
Zhao Y et al (2009) A herceptin-based chimeric antigen receptor with modified signaling domains leads to enhanced survival of transduced T lymphocytes and antitumor activity. J Immunol 183(9):5563–5574
Teng MW et al (2004) Immunotherapy of cancer using systemically delivered gene-modified human T lymphocytes. Hum Gene Ther 15(7):699–708
Stancovski I et al (1993) Targeting of T lymphocytes to Neu/HER2-expressing cells using chimeric single chain Fv receptors. J Immunol 151(11):6577–6582
Moritz D et al (1994) Cytotoxic T lymphocytes with a grafted recognition specificity for ERBB2-expressing tumor cells. Proc Natl Acad Sci U S A 91(10):4318–4322
Altenschmidt U et al (1996) Cytolysis of tumor cells expressing the Neu/erbB-2, erbB-3, and erbB-4 receptors by genetically targeted naive T lymphocytes. Clin Cancer Res 2(6):1001–1008
Lanitis E et al (2012) Redirected antitumor activity of primary human lymphocytes transduced with a fully human anti-mesothelin chimeric receptor. Mol Ther 20(3):633–643
Westwood JA et al (2005) Adoptive transfer of T cells modified with a humanized chimeric receptor gene inhibits growth of Lewis-Y-expressing tumors in mice. Proc Natl Acad Sci U S A 102(52):19051–19056
Mezzanzanica D et al (1998) Transfer of chimeric receptor gene made of variable regions of tumor-specific antibody confers anticarbohydrate specificity on T cells. Cancer Gene Ther 5(6):401–407
Moon EK et al (2011) Expression of a functional CCR2 receptor enhances tumor localization and tumor eradication by retargeted human T cells expressing a mesothelin-specific chimeric antibody receptor. Clin Cancer Res 17(14):4719–4730
Wilkie S et al (2008) Retargeting of human T cells to tumor-associated MUC1: the evolution of a chimeric antigen receptor. J Immunol 180(7):4901–4909
O’Shaughnessy JA (2006) Molecular signatures predict outcomes of breast cancer. N Engl J Med 355(6):615–617
Slamon DJ et al (2001) Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N Engl J Med 344(11):783–792
Baselga J et al (2012) Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N Engl J Med 366(2):109–119
Lipowska-Bhalla G et al (2012) Targeted immunotherapy of cancer with CAR T cells: achievements and challenges. Cancer Immunol Immunother 61(7):953–962
Gilham DE et al (2012) CAR-T cells and solid tumors: tuning T cells to challenge an inveterate foe. Trends Mol Med 18(7):377–384
Lamers CH et al (2006) Treatment of metastatic renal cell carcinoma with autologous T-lymphocytes genetically retargeted against carbonic anhydrase IX: first clinical experience. J Clin Oncol 24(13):e20–e22
Park JR et al (2007) Adoptive transfer of chimeric antigen receptor re-directed cytolytic T lymphocyte clones in patients with neuroblastoma. Mol Ther 15(4):825–833
Han EQ et al (2013) Chimeric antigen receptor-engineered T cells for cancer immunotherapy: progress and challenges. J Hematol Oncol 6:47
Kakarla S, Gottschalk S (2014) CAR T cells for solid tumors: armed and ready to go? Cancer J 20(2):151–155
Wilkie S et al (2012) Dual targeting of ErbB2 and MUC1 in breast cancer using chimeric antigen receptors engineered to provide complementary signaling. J Clin Immunol 32(5):1059–1070
Lanitis E et al (2013) Chimeric antigen receptor T cells with dissociated signaling domains exhibit focused antitumor activity with reduced potential for toxicity in vivo. Cancer Immunol Res 1(1):43–53
Grada Z et al (2013) TanCAR: a novel Bispecific chimeric antigen receptor for cancer immunotherapy. Mol Ther Nucleic Acids 2:e105
Urbanska K et al (2012) A universal strategy for adoptive immunotherapy of cancer through use of a novel T-cell antigen receptor. Cancer Res 72(7):1844–1852
Tamada K et al (2012) Redirecting gene-modified T cells toward various cancer types using tagged antibodies. Clin Cancer Res 18(23):6436–6445
Janssen A, Medema RH (2013) Genetic instability: tipping the balance. Oncogene 32(38):4459–4470
Rabinovich GA, Gabrilovich D, Sotomayor EM (2007) Immunosuppressive strategies that are mediated by tumor cells. Annu Rev Immunol 25:267–296
Kakarla S et al (2013) Antitumor effects of chimeric receptor engineered human T cells directed to tumor stroma. Mol Ther 21(8):1611–1620
Roberts EW et al (2013) Depletion of stromal cells expressing fibroblast activation protein-alpha from skeletal muscle and bone marrow results in cachexia and anemia. J Exp Med 210(6):1137–1151
Niederman TM et al (2002) Antitumor activity of cytotoxic T lymphocytes engineered to target vascular endothelial growth factor receptors. Proc Natl Acad Sci U S A 99(10):7009–7014
Tran E et al (2013) Immune targeting of fibroblast activation protein triggers recognition of multipotent bone marrow stromal cells and cachexia. J Exp Med 210(6):1125–1135
Kershaw MH et al (2006) A phase I study on adoptive immunotherapy using gene-modified T cells for ovarian cancer. Clin Cancer Res 12(20 Pt 1):6106–6115
Brentjens R et al (2010) Treatment of chronic lymphocytic leukemia with genetically targeted autologous T cells: case report of an unforeseen adverse event in a phase I clinical trial. Mol Ther 18(4):666–668
Savoldo B et al (2011) CD28 costimulation improves expansion and persistence of chimeric antigen receptor-modified T cells in lymphoma patients. J Clin Invest 121(5):1822–1826
Li XC et al (2001) IL-15 and IL-2: a matter of life and death for T cells in vivo. Nat Med 7(1):114–118
Mueller K, Schweier O, Pircher H (2008) Efficacy of IL-2- versus IL-15-stimulated CD8 T cells in adoptive immunotherapy. Eur J Immunol 38(10):2874–2885
Ochoa MC et al (2013) Interleukin-15 in gene therapy of cancer. Curr Gene Ther 13(1):15–30
Perna SK et al (2013) Interleukin 15 provides relief to CTLs from regulatory T cell-mediated inhibition: implications for adoptive T cell-based therapies for lymphoma. Clin Cancer Res 19(1):106–117
Quintarelli C et al (2007) Co-expression of cytokine and suicide genes to enhance the activity and safety of tumor-specific cytotoxic T lymphocytes. Blood 110(8):2793–2802
Hoyos V et al (2010) Engineering CD19-specific T lymphocytes with interleukin-15 and a suicide gene to enhance their anti-lymphoma/leukemia effects and safety. Leukemia 24(6):1160–1170
Hsu C et al (2005) Primary human T lymphocytes engineered with a codon-optimized IL-15 gene resist cytokine withdrawal-induced apoptosis and persist long-term in the absence of exogenous cytokine. J Immunol 175(11):7226–7234
Carrette F, Surh CD (2012) IL-7 signaling and CD127 receptor regulation in the control of T cell homeostasis. Semin Immunol 24(3):209–217
Pegram HJ et al (2012) Tumor-targeted T cells modified to secrete IL-12 eradicate systemic tumors without need for prior conditioning. Blood 119(18):4133–4141
Hodi FS et al (2010) Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med 363(8):711–723
Flies DB et al (2014) Coinhibitory receptor PD-1H preferentially suppresses CD4(+) T cell-mediated immunity. J Clin Invest 124(5):1966–1975
Wang X et al (2012) Phenotypic and functional attributes of lentivirus-modified CD19-specific human CD8+ central memory T cells manufactured at clinical scale. J Immunother 35(9):689–701
Rooney CM et al (1998) Infusion of cytotoxic T cells for the prevention and treatment of Epstein-Barr virus-induced lymphoma in allogeneic transplant recipients. Blood 92(5):1549–1555
Heslop HE et al (2010) Long-term outcome of EBV-specific T-cell infusions to prevent or treat EBV-related lymphoproliferative disease in transplant recipients. Blood 115(5):925–935
Hislop AD et al (2007) Cellular responses to viral infection in humans: lessons from Epstein-Barr virus. Annu Rev Immunol 25:587–617
Gschweng E, De Oliveira S, Kohn DB (2014) Hematopoietic stem cells for cancer immunotherapy. Immunol Rev 257(1):237–249
Cheadle EJ et al (2012) Ligation of the CD2 co-stimulatory receptor enhances IL-2 production from first-generation chimeric antigen receptor T cells. Gene Ther 19(11):1114–1120
Bromley SK, Mempel TR, Luster AD (2008) Orchestrating the orchestrators: chemokines in control of T cell traffic. Nat Immunol 9(9):970–980
Kershaw MH et al (2002) Redirecting migration of T cells to chemokine secreted from tumors by genetic modification with CXCR2. Hum Gene Ther 13(16):1971–1980
Di Stasi A et al (2009) T lymphocytes coexpressing CCR4 and a chimeric antigen receptor targeting CD30 have improved homing and antitumor activity in a Hodgkin tumor model. Blood 113(25):6392–6402
Craddock JA et al (2010) Enhanced tumor trafficking of GD2 chimeric antigen receptor T cells by expression of the chemokine receptor CCR2b. J Immunother 33(8):780–788
Gajewski TF et al (2006) Immune resistance orchestrated by the tumor microenvironment. Immunol Rev 213:131–145
Gabrilovich DI, Nagaraj S (2009) Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol 9(3):162–174
Shiao SL et al (2011) Immune microenvironments in solid tumors: new targets for therapy. Genes Dev 25(24):2559–2572
Tanchot C et al (2013) Tumor-infiltrating regulatory T cells: phenotype, role, mechanism of expansion in situ and clinical significance. Cancer Microenviron 6(2):147–157
Foster AE et al (2008) Antitumor activity of EBV-specific T lymphocytes transduced with a dominant negative TGF-beta receptor. J Immunother 31(5):500–505
Dotti G et al (2005) Human cytotoxic T lymphocytes with reduced sensitivity to Fas-induced apoptosis. Blood 105(12):4677–4684
Eaton D et al (2002) Retroviral transduction of human peripheral blood lymphocytes with Bcl-X(L) promotes in vitro lymphocyte survival in pro-apoptotic conditions. Gene Ther 9(8):527–535
Sun J et al (2010) T cells expressing constitutively active Akt resist multiple tumor-associated inhibitory mechanisms. Mol Ther 18(11):2006–2017
Zhao Y et al (2010) Multiple injections of electroporated autologous T cells expressing a chimeric antigen receptor mediate regression of human disseminated tumor. Cancer Res 70(22):9053–9061
Barrett DM et al (2011) Treatment of advanced leukemia in mice with mRNA engineered T cells. Hum Gene Ther 22(12):1575–1586
Almasbak H et al (2011) Transiently redirected T cells for adoptive transfer. Cytotherapy 13(5):629–640
Straathof KC et al (2005) An inducible caspase 9 safety switch for T-cell therapy. Blood 105(11):4247–4254
Di Stasi A et al (2011) Inducible apoptosis as a safety switch for adoptive cell therapy. N Engl J Med 365(18):1673–1683
Arber C et al (2013) The immunogenicity of virus-derived 2A sequences in immunocompetent individuals. Gene Ther 20(9):958–962
Liu X et al (2017) CRISPR-Cas9-mediated multiplex gene editing in CAR-T cells. Cell Res 27(1):154–157
Torikai H et al (2012) A foundation for universal T-cell based immunotherapy: T cells engineered to express a CD19-specific chimeric-antigen-receptor and eliminate expression of endogenous TCR. Blood 119(24):5697–5705
Riolobos L et al (2013) HLA engineering of human pluripotent stem cells. Mol Ther 21(6):1232–1241
Chou J et al (2012) Epigenetic modulation to enable antigen-specific T-cell therapy of colorectal cancer. J Immunother 35(2):131–141
Liu C et al (2013) BRAF inhibition increases tumor infiltration by T cells and enhances the antitumor activity of adoptive immunotherapy in mice. Clin Cancer Res 19(2):393–403
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Wang, J., Zhou, P. (2017). New Approaches in CAR-T Cell Immunotherapy for Breast Cancer. In: Song, E., Hu, H. (eds) Translational Research in Breast Cancer. Advances in Experimental Medicine and Biology, vol 1026. Springer, Singapore. https://doi.org/10.1007/978-981-10-6020-5_17
Download citation
DOI: https://doi.org/10.1007/978-981-10-6020-5_17
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-10-6019-9
Online ISBN: 978-981-10-6020-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)