Abstract
In this chapter we will review the structural and functional neuroimaging correlates of anhedonia.
Regions associated with anhedonia range from the reward processing circuits of the medial orbitofrontal cortex in healthy subjects to the fear processing neurocircuitry of amygdala in patients with schizophrenia. The emerging picture of the hedonic brain imaging literature is one of a hedonic continuum, with a remarkable continuity between healthy and across affected individuals, suggesting that anhedonia might be a useful endophenotype or potential trait marker related to vulnerability to major psychiatric disorders such as depression and schizophrenia. However, the relatively small number of brain imaging studies to date, lack of precision in the definition of anhedonia, diagnostic heterogeneity of the study populations and heterogeneity of study methods indicate that this remains an incipient field of research. We conclude that the evidence to date about the brain correlates of anhedonia is preliminary and further research is indicated.
“For it is then that we have need of pleasure, when we feel pain owing to the absence of pleasure.” Epicurus (341–270 B.C.)
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Accumbens
- Amygdala
- Anhedonia
- Anterior cingulate cortex
- Depression
- fMRI
- Insula
- Mesolimbic reward system
- MRS
- Orbitofrontal cortex
- PET
- [ventromedial/dorsolateral] Prefrontal cortex
- Raphe Nuclei
- Reward
- Schizophrenia
- Striatum
- Substantia Nigra
- Ventral striatum
- Ventral tegmental area
2 The Neuroimaging of Anhedonia: Challenges and Opportunities
When compared to clinical syndromes such as depression and schizophrenia anhedonia would arguably make for a better neuroimaging target: anhedonia presents more homogeneity than clinical syndromes such as depression or schizophrenia; in addition, one can argue that measurements of anhedonia are less confounded than measurements of psychiatric clinical syndromes. Further, anhedonia has been conceptualized as a neurobiological endophenotype possibly mediating the occurrence of major neuropsychiatric disorders such as schizophrenia and depression [3, 4]. Accordingly, understanding the neural correlates of anhedonia can illuminate the neuropathological correlates of major psychiatric and neurological disorders as well as help identify individuals at risk.
At the same time, the ability to perceive pleasure is the result of a complex set of processes involving processing of sensorial stimuli, mitigated by higher cognitive inputs associated with perceived costs and rewards, including effort, resolving cognitive dissonance, and decision making. As each of these processes has a putative different neurocircuitry basis, separating the neural foundation of anhedonia is not a straightforward proposal.
Further, while the neural correlates of pleasure and reward are fairly well studied [5] the number of studies directly correlating brain structure and function with anhedonia severity is surprisingly low. A brief review of the specific challenges that any neuroimaging study of anhedonia faces will help understand this rather paradoxical and disconcerting state of affairs.
2.1 Anhedonia Lacks Diagnostic Specificity
Most clinical brain imaging studies compare affected subjects with a control group. As anhedonia is not a disorder per se data from brain imaging studies are limited to comparisons between patients diagnosed with a disorder where anhedonia is one of the many manifesting symptoms [6, 7]. An immediate limitation of any topographical location of anhedonia defined this way is that associated symptoms will be unaccounted for variables that could greatly affect the accuracy of the mapping. For example, the associated symptoms of anhedonia differ in patients with depression:schizophrenia which may affect the brain signature of anhedonia in these different patient groups [7].
2.2 Anhedonia Is a Poorly Defined Neuroimaging Target
Ideal functional neuroimaging targets are clearly and objectively defined states. That is not the case with anhedonia, an essentially subjective state which interpretation is to a good extent subject-dependent [8]. Is the intense negative emotion experienced by the depressed patient who is no longer able to enjoy anything [9] the same with the lack of emotion experienced by the patient with schizophrenia who finds himself indifferent to almost everything [10]? Both patients will likely score high on any given anhedonia scale but it is debatable if the same concept is measured all along.
In fact, several types of anhedonia have been described, including sensorial or physical anhedonia as distinct from interpersonal or social anhedonia [11], as well as anticipatory anhedonia as distinct from consummatory anhedonia [12]. Further, it is not clear if patients reporting anhedonia experience a deficit in their ability to experience pleasure [a predominantly emotional deficit] or rather an undervaluation of reward stimuli (a predominantly cognitive deficit) [13].
Secondly, ideal functional imaging targets are circumscribed states that can be easily, reliably and rapidly turned on and off. This unfortunately is not the case with anhedonia, a rather persistent and lingering state : trait, without clear modifying factors [7, 14].
Lastly, both the intensity and quality of any hedonic occurrence are essentially subjective experiences; as such, difficult targets for any scientific, i.e. objective data-driven, investigation.
A way of overcoming the stated challenges is to investigate the hedonic:anhedonic spectrum in non-clinical populations. As mentioned, the very nature of anhedonia allows its conceptualization not only as a state (associated with other clinical symptoms) but also as a trait; as such, present to some extent in all people. However, with the exception of resting state studies, neuroimaging trait studies are limited by the fact that trait severity neural correlates cannot be directly assessed. The alternative is to estimate trait severity correlates via surrogate state-dependent measures, with the added inherent limitation of any indirect measurement.
Considering these important limitations we decided to review the brain imaging correlates of anhedonia within the boundaries of predefined functional neural correlates of reward-hedonic capacity processing, specifically:
-
1.
Hedonic Appraisal: Orbitofrontal Cortex (OFC) and Ventral Striatum (VS)
-
2.
Reward Appraisal and Executive-Decision Making: the Prefrontal Cortex (PFC) and the Anterior Cingulate Cortex (ACC)
-
3.
(The Mesolimbic) Reward Detection System: Nucleus Accumbens (NAc) and the Ventral Tegmental Area/Substantia Nigra (VTA/SN)
-
4.
Emotional Context: the Insula Cortex and Amygdala
-
5.
Other Regions of Interest: Cerebellum, Raphe Nuclei
Of note, as a number of brain regions belong to more than one reward/hedonic neurocircuits, we will attempt to sketch a functionally driven (as opposed to a structurally driven) map of the territory.
Thus our brain mapping review will follow a cross-diagnostic function-based neuroimaging strategy [15]. For each specific region of interest we will discuss findings from a variety of neuroimaging studies, including studies of anhedonia:hedonic capacity in clinical:non-clinical populations.
Last but not least, as a way of overcoming some of the mentioned difficulties, we will also review reward/pleasure based neuroimaging data under the assumption that the neural substrates of anhedonia and reward/pleasure overlap to a good extent [15].
3 Hedonic Appraisal: Orbitofrontal Cortex (OFC)
The OFC is a major information integration hub providing support for a variety of cognitive processes from decision making to sensory, reward and hedonic processing [16]. From a neural connectivity perspective, the OFC is an important center for integrating sensory-autonomic input with visceral-motor systems output [16]; as such an important hedonic focal point.
From the perspective of neuroimaging studies the OFC however is not the easiest target to investigate. Due to its proximity to the air-filled sinuses the quality of OFC MRI findings can be diminished by signal dropout, geometric distortion or susceptibility artifacts [17, 18]. Hence negative findings of fMRI OFC studies need to be considered with caution [16].
Limitations considered, the medial OFC activation has been consistently correlated with reinforcers pleasantness for a variety of gustative and olfactory stimuli (for review see Ref. [16]).
Quite a few studies focused on finding the hedonia “spot” in the OFC; however, very few studies approached the subject of anhedonia relationship to OFC.
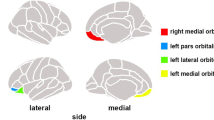
In their comprehensive meta-analysis of neuroimaging and neuropsychological studies focused on the OFC Kringelbach and Rolls found that the OFC specializes in different types of hedonic processing along its medial-lateral and antero-posterior axes [19]. Specifically, reward-based processing correlates with activity in the medial while punishment processing correlates mostly with activity in the lateral OFC. Also, abstract/complex reinforcers associations (e.g. financial incentives) appear to be based in the anterior OFC, while more concrete/simple reinforcers associations are mostly based in the posterior OFC.
In a PET study using musical dissonance as an anhedonic-equivalent, OFC activity was correlated with the level of consonance/hedonic experience [20]. A more recent fMRI study, using an anhedonic stimulus in the form of a reinforcer devaluation paradigm found that the mid-anterior OFC and amygdala activity decreased in parallel with the reinforcer perceived hedonic value [21].
Trait-anhedonia negatively correlated with OFC activity in healthy subjects [22].
Consistent with the OFC and ventral striatum (VS) role in hedonic experiences, anhedonic patients with major depressive disorder (MDD) [23, 24] and schizophrenia [25, 26] usually present with lower than expected activity in both the OFC and. Of note, task-dependent increased or decreased OFC activation correlated with anhedonia severity in depressed patients [24].
4 Reward Appraisal and Executive-Decision Making: The Prefrontal Cortex (PFC) and the Anterior Cingulate Cortex (ACC)
The prefrontal cortex has long been known for its executive role including decision making, reward appraisal, and cost-benefit analysis as distinct functions contributing to normal cognitive processes such as learning and motivation, or pathological dysfunction such as addiction [27], negative symptoms in schizophrenia [28], or impaired decision making in depression [29].
Based on different connectivity patterns, the PFC is usually divided in two regions: the ventromedial PFC (vmPFC) and dorsolateral PFC (dlPFC), with the vmPFC traditionally seen as underlying emotional/affective processing (“what” function), while the dlPFC providing support for cognitive/executive processing (“how” function) [30].
In non-clinical subjects physical anhedonia inversely correlated with vmPFC and ACC activity [25, 31], anterior PFC activity [31], as well as with ACC and dlPFC resting state activity [32]. High levels of social anhedonia inversely correlated with medial PFC activity during emotional discrimination tasks [33]. However, vmPFC activity has also been reported to positively correlate with the level of anhedonia-trait severity in both healthy individuals [34] and depressed patients [24].
In patients addicted to opioids anhedonia severity negatively correlated with activity in PFC and ACC [31].
In MDD patients anhedonia severity correlated with ventrolateral PFC and dorsal cingulate gyrus responses to sad stimuli but inversely correlated with ventral ACC activation to happy stimuli [24].
Anterior cingulate cortex GABA levels, as measured by proton magnetic resonance spectroscopy, negatively correlated with the severity of anhedonia in adolescents with MDD [35]. Emotional intensity ratings, an anhedonia surrogate, correlated with glutamate and N-acetylaspartate concentrations and inversely correlated with glutamine concentration and pregenual anterior cingulate activation in highly anhedonic depressed patients [36].
In patients with schizophrenia, in addition to an inverse correlation with activity in the OFC and VS [25] physical anhedonia has also been correlated with decreased activity in the vmPFC [25]. Structural and functional MRI as well as PET studies also suggest that in patients with schizophrenia physical anhedonia might be associated with volume deficits and hypo-activity in the default-mode neurocircuitry including the ventromedial prefrontal cortex [37].
In conclusion, decreased activity in the both the vmPFC and dlPFC as well as the ACC appear to contribute to anhedonia in affected and healthy individuals. This importance of this circuit in the genesis of anhedonia is emphasized by the fact that clinical findings have been consistent in both adolescent and adult samples.
5 (The Mesolimbic) Reward Detection System (MRDS): Nucleus Accumbens (NAc) and the Ventral Tegmental Area/Substantia Nigra (VTA/SN)
The ventral striatum (VS), and especially nucleus accumbens, with its strong OFC input, has been long associated with the pathology of addiction and reward [38].
More specifically, nucleus accumbens is an important reward-contingent as well as reward-independent pleasure processing center. NAc forms a functional unit with the VTA/SN via the medial forebrain bundle connection [39]. The NAc-VTA circuit is essential in detecting rewards and thus modulating responses to natural rewards such as food, sexual, and social intercourse. The activation of this circuit results increases the likelihood that a certain activity [labeled as pleasurable] will be repeated in the future. As such the MRDS plays in important role in the control of hedonic experiences and putatively MRDS dysfunctions may result in anhedonia.
Consistent with this understanding of the MRDS role, Wacker et al. [32] found that in a non-clinical sample anhedonia was inversely correlated with both NAcc volume and NAcc responses to reward feedback. In contrast to an initial finding of a lack of correlation between anhedonia-trait and NAc activity [34] in a recent fMRI study healthy subjects activation in response to a musical stimulus in the right NAc, basal forebrain and bilateral hypothalamus was negatively correlated with trait anhedonia [22].
In depressed patients anhedonia severity did not correlate with NAc volume [40]. Blood et al. [41]. found that MDD patients have microstructural VTA abnormalities compared to health subjects; however, they also reported that in their sample anhedonia did not correlate with the severity of VTA abnormalities.
Lee et al. reported a significant percent signal change in NAc and hippocampus activity correlated with physical anhedonia severity in patients with schizophrenia compared to healthy controls, indicating that specific parts of the limbic and reward circuitry may be associated with physical anhedonia in schizophrenia [42].
Patients with schizophrenia differ from healthy individuals in that their anhedonia level inversely correlated with VS response to positive stimuli compared to negative and neutral stimuli [43].
In summary, decreased volume and activity in the (MRDS) appears to contribute to anhedonia in healthy and affected individuals. However, the relationship between the MDRS and anhedonia in clinical populations is less clear than in healthy individuals; this lack of clarity may be in part due the difficulties in higher level of confounding as well as more difficulties in reliably measuring primary:secondary anhedonia in clinical samples.
6 Emotional Context: The Insula Cortex and Amygdala
Alongside with the orbitofrontal, cingulate, and medial prefrontal the insular cortices complete the who’s who list of hedonic hotspots [44].
In an fMRI study of healthy subjects Keller et al. [22] found that trait-anhedonia negatively correlated with activity in the anterior insula.
In a study of healthy individuals with high:low social anhedonia Germine et al. [33] reported that social anhedonia severity did not correlate with amygdala activity; however the study findings might be limited by amygdala’s rapid habituation in the context of the study’s rapid block-design, continuous presentation of faces, and emotion labeling demands, that might have resulted in a low signal:noise ratio.
In an early PET schizophrenia study Crespo-Facorro et al. [45] found that patients with schizophrenia had decreased activity in the insular cortex in response to unpleasant odors only. Of note, the patients showed impairment in the experience of pleasant odors when compared to healthy controls – consistent with an anhedonic presentation – but this experiential difference did not result in PET activity differences; on the contrary, it was their response to the unpleasant odors, which was experientially similar to healthy volunteers, that resulted in PET differences. It appears that the insular cortex functional abnormalities may contribute to anhedonia in schizophrenia; however further studies are recommended to clarify the directionality of this relationship.
In a recent PET resting-state paradigm study Park et al. [37] reported that in patients with schizophrenia physical anhedonia correlated with hypo-activity in the default-mode neurocircuitry including the insular cortex.
Dowd et al. [43] reported that physical anhedonia correlated with decreased bilateral amygdala activation to positive versus negative stimuli in patients with schizophrenia.
7 Other Regions of Interest: Cerebellum, Raphe Nuclei (RN)
In a recently published meta-analysis Kuhn et al. [46] found both positive and negative correlates of subjective pleasantness in the right cerebellum.
Using PET Park et al. [37] reported that cerebellum activity did not correlate with trait physical anhedonia severity in patients with schizophrenia.
In summary, the evidence to date does not support the hypothesis that cerebellum plays a significant role in the pathology of anhedonia.
Reward/castigatory stimuli correlated with neural activation within the dorsal RN indicative of a change in serotonergic transmission elicited by hedonic processing [47].
8 Conclusions and Future Directions
In summary, anhedonia is associated with decreased reactivity and connectivity in the neural substrates underlying sensing and appraisal of pleasant stimuli and rewards (OFC and VS/NAc), cost/benefit analysis and decision making (ACC, vmPFC and dlPFC), reward processing and consolidation (the mesolimbic system: VS/NAc, VTA/SN, and hippocampus connections), salience labeling (amygdala), as well as related limbic and paralimbic regions (Table 14.1).
A clear interpretation of the literature is limited by a lack of coherence in approaching the topic of anhedonia. Despite a wealth of studies on the neural substrates of reward and hedonia, there are relatively few studies addressing the subject of anhedonia per se. Moreover, the relationships between state:trait anhedonia or the different specific types of anhedonia (e.g. physical:social, anticipatory:consumatory) is yet to be explored in a well-articulated manner.
Despite the evidence to date shortcomings, the emerging picture of the hedonic brain imaging literature is one of a hedonic continuum, with a remarkable continuity between healthy and affected individuals.
This emerging theme of a linked set of neural hedonic circuits supports the view that anhedonia might be a useful endophenotype or potential trait marker related to vulnerability to major psychiatric disorders such as depression and schizophrenia.
In light of the relatively small number of brain imaging studies of anhedonia to date, lack of precision in the definition of anhedonia, diagnostic heterogeneity of the study populations and heterogeneity of study methods, the brain imaging of anhedonia remains an incipient field of research at this time.
The evidence to date about the brain correlates of anhedonia while promising, remains preliminary. Further research is indicated.
Abbreviations
- ACC:
-
Anterior Cingulate Cortex
- fMRI:
-
functional MRI
- MRS:
-
Magnetic Resonance Spectroscopy
- OFC:
-
Orbitofrontal cortex
- NAc:
-
Nucleus Accumbens
- [vm/dl]PFC:
-
[ventromedial/dorsolateral] Prefrontal cortex
- PET:
-
Positron Emission Tomography
- SN:
-
Substantia Nigra
- VS:
-
Ventral striatum
References
Loas G, Pierson A. Anhedonia in psychiatry: a review. Ann Medicopsychol. 1989;147:705–17.
Gorwood P. Neurobiological mechanisms of anhedonia. Dialogues Clin Neurosci. 2008;10(3):291–9.
Meehl PE. Hedonic capacity: some conjectures. Bull Menninger Clin. 1975;39(4):295–307.
Bogdan R, Pizzagalli DA. The heritability of hedonic capacity and perceived stress: a twin study evaluation of candidate depressive phenotypes. Psychol Med. 2009;39(2):211–18.
Haber SN, Knutson B. The reward circuit: linking primate anatomy and human imaging. Neuropsychopharmacology. 2010;35:4–26.
Kaji Y, Hirata K. Apathy and anhedonia in Parkinson’s disease. ISRN Neurol. 2011;2011:219427.
Pelizza L, Ferrari A. Anhedonia in schizophrenia and major depression: state or trait? Ann Gen Psychiatry. 2009;8:22.
Loas G, Perot JM, Boyer P, Gayant C, Fremaux D. Evaluation of the subjective component of emotions in normal subjects: relation between anhedonia and the capacity to perceive unpleasant feelings in a population of 221 normal subjects. Ann Medicopsychol. 1995;153:143–5.
Snaith P. Anhedonia: a neglected symptom of psychopathology. Psychol Med. 1993;23:957–66.
Kirkpatrick B, Buchanan RW. Anhedonia and the deficit syndrome of schizophrenia. Psychiatry Res. 1990;31:25–30.
Kerns JG, Docherty AR, Martin EA. Social and physical anhedonia and valence and arousal aspects of emotional experience. J Abnorm Psychol. 2008;117:735–46.
Gard D, Gard M, Kring A, John O. Anticipatory and consummatory components of the experience of pleasure: a scale development study. J Res Pers. 2006;40:1086–102.
Berridge KC, Kringelbach ML. Affective neuroscience of pleasure: reward in humans and animals. Psychopharmacology (Berl). 2008;199(3):457–80.
Loas G, Monestes JL, Ingelaere A, Noisette C, Herbener ES. Stability and relationships between trait or state anhedonia and schizophrenic symptoms in schizophrenia: a 13-year follow-up study. Psychiatry Res. 2009;166:132–40.
Der-Avakian A, Markou A. The neurobiology of anhedonia and other reward-related deficits. Trends Neurosci. 2012;35(1):68–77.
Kringelbach ML. The human orbitofrontal cortex: linking reward to hedonic experience. Nat Rev Neurosci. 2005;6(9):691–702.
Wilson JL, Jenkinson M, de Araujo I, Kringelbach ML, Rolls ET, Jezzard P. Fast, fully automated global and local magnetic field optimization for fMRI of the human brain. Neuroimage. 2002;17(2):967–76.
Deichmann R, Josephs O, Hutton C, Corfield DR, Turner R. Compensation of susceptibility-induced BOLD sensitivity losses in echo-planar fMRI imaging. Neuroimage. 2002;15(1):120–35.
Kringelbach ML, Rolls ET. The functional neuroanatomy of the human orbitofrontal cortex: evidence from neuroimaging and neuropsychology. Prog Neurobiol. 2004;72(5):341–72.
Blood AJ, Zatorre RJ, Bermudez P, Evans AC. Emotional responses to pleasant and unpleasant music correlate with activity in paralimbic brain regions. Nat Neurosci. 1999;2(4):382–7.
Gottfried JA, O’Doherty J, Dolan RJ. Encoding predictive reward value in human amygdala and orbitofrontal cortex. Science. 2003;301(5636):1104–7.
Keller J, Young CB, Kelley E, Prater K, Levitin DJ, Menon V. Trait anhedonia is associated with reduced reactivity and connectivity of mesolimbic and paralimbic reward pathways. J Psychiatr Res. 2013;47(10):1319–28.
Epstein J, Pan H, Kocsis JH, et al. Lack of ventral striatal response to positive stimuli in depressed versus normal subjects. Am J Psychiatry. 2006;163(10):1784–90.
Keedwell PA, Andrew C, Williams SCR, Brammer MJ, Phillips ML. The neural correlates of anhedonia in major depressive disorder. Biol Psychiatry. 2005;58(11):843–53.
Harvey P-O, Armony J, Malla A, Lepage M. Functional neural substrates of self-reported physical anhedonia in non-clinical individuals and in patients with schizophrenia. J Psychiatr Res. 2010;44(11):707–16.
Dowd EC, Barch DM. Pavlovian reward prediction and receipt in schizophrenia: relationship to anhedonia. Hashimoto K, ed. PLoS One. 2012;7(5):e35622.
Koob GF, Volkow ND. Neurocircuitry of addiction. Neuropsychopharmacology. 2010;35(1):217–38.
Wolkin A, Sanfilipo M, Wolf AP, Angrist B, Brodie JD, Rotrosen J. Negative symptoms and hypofrontality in chronic schizophrenia. Arch Gen Psychiatry. 1992;49(12):959–65.
Koenigs M, Grafman J. The functional neuroanatomy of depression: distinct roles for ventromedial and dorsolateral prefrontal cortex. Behav Brain Res. 2009;201(2):239–43.
O’Reilly RC. The What and How of prefrontal cortical organization. Trends Neurosci. 2010;33(8):355–61.
Zijlstra F, Veltman DJ, Booij J, van den Brink W, Franken IHA. Neurobiological substrates of cue-elicited craving and anhedonia in recently abstinent opioid-dependent males. Drug Alcohol Depend. 2009;99(1):183–92.
Wacker J, Dillon DG, Pizzagalli DA. The role of the nucleus accumbens and rostral anterior cingulate cortex in anhedonia: integration of resting EEG, fMRI, and volumetric techniques. Neuroimage. 2009;46(1):327–37.
Germine LT, Garrido L, Bruce L, Hooker C. Social anhedonia is associated with neural abnormalities during face emotion processing. Neuroimage. 2011;58(3):935–45.
Harvey P-O, Pruessner J, Czechowska Y, Lepage M. Individual differences in trait anhedonia: a structural and functional magnetic resonance imaging study in non-clinical subjects. Mol Psychiatry. 2007;12(8):703. 767–75.
Gabbay V, Mao X, Klein RG, et al. Anterior cingulate cortex γ-aminobutyric acid in depressed adolescents: relationship to anhedonia. Arch Gen Psychiatry. 2012;69(2):139–49.
Walter M, Henning A, Grimm S, et al. The relationship between aberrant neuronal activation in the pregenual anterior cingulate, altered glutamatergic metabolism, and anhedonia in major depression. Arch Gen Psychiatry. 2009;66(5):478–86.
Park IH, Kim J-J, Chun J, et al. Medial prefrontal default-mode hypoactivity affecting trait physical anhedonia in schizophrenia. Psychiatry Res Neuroimaging. 2009;171(3):155–65.
Olds J, Milner P. Positive reinforcement produced by electrical stimulation of septal area and other regions of rat brain. J Comp Physiol Psychol. 1954;47(6):419–27.
Yun IA, Wakabayashi KT, Fields HL, Nicola SM. The ventral tegmental area is required for the behavioral and nucleus accumbens neuronal firing responses to incentive cues. J Neurosci. 2004;24(12):2923–33.
Pizzagalli DA, Holmes AJ, Dillon DG, et al. Reduced caudate and nucleus accumbens response to rewards in unmedicated individuals with major depressive disorder. Am J Psychiatry. 2009;166(6):702–10.
Blood AJ, Iosifescu DV, Makris N, et al. Microstructural abnormalities in subcortical reward circuitry of subjects with major depressive disorder. Bartolomucci A, ed. PLoS One. 2010;5(11):e13945.
Lee JS, Park H-J, Chun JW. Neuroanatomical correlates of trait anhedonia in patients with schizophrenia: A voxel-based morphometric study. Neurosci Lett. 2013;489(2):110–14.
Dowd EC, Barch DM. Anhedonia and emotional experience in schizophrenia: neural and behavioral indicators. Biol Psychiatry. 2010;67(10):902–11.
Kringelbach ML, Berridge KC. The neuroscience of happiness and pleasure. Soc Res (New York). 2010;77((2):659–78.
Crespo-Facorro B. Neural mechanisms of anhedonia in schizophrenia. A PET study of response to unpleasant and pleasant odors. JAMA. 2001;286(4):427.
Kühn S, Gallinat J. The neural correlates of subjective pleasantness. Neuroimage. 2012;61(1):289–94.
Lanzenberger R, Hahn A, Windischberger C, et al. Serotonin-1A receptor binding and Reward-dependent Activation are associated within the Human Dorsal Raphe Nucleus as revealed by PET-fMRI. Neuroimage. 2009;47.
Gaillard R, Gourion D, Llorca PM. Anhedonia in depression. Encéphale. 2013;39(4):296–305.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Science+Business Media Dordrecht
About this chapter
Cite this chapter
Preda, A. (2014). Brain Imaging Correlates of Anhedonia. In: Ritsner, M. (eds) Anhedonia: A Comprehensive Handbook Volume I. Springer, Dordrecht. https://doi.org/10.1007/978-94-017-8591-4_14
Download citation
DOI: https://doi.org/10.1007/978-94-017-8591-4_14
Published:
Publisher Name: Springer, Dordrecht
Print ISBN: 978-94-017-8590-7
Online ISBN: 978-94-017-8591-4
eBook Packages: MedicineMedicine (R0)