Abstract
Ventricular fibrillation (VF) has been reported to recur in as many as 80 % of patients during basic and advanced life support care in out-of-hospital cardiac arrest with VF as the initial rhythm. Current ILCOR and American Heart Association Guidelines advocate a period of two minutes following a defibrillation shock committed to cardiopulmonary resuscitation (CPR), without regard to the post-shock rhythm, including recurrent VF. Because VF is a high oxygen-demanding arrhythmia, permitting the heart to remain in VF shortly after a shock is delivered may be problematic. It has also been observed that VF can recur quickly after a shock upon resumption of chest compressions. A protocol revision should consider shocking recurrent VF quickly after the first 2–3 shocks in a witnessed arrest, after which post-shock CPR might be done as currently recommended. There is sufficient evidence and experience to warrant a reassessment of the present recommendation to do CPR for two minutes after a shock even if VF recurs within 30–60 seconds after a shock
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Defibrillation and Resuscitation
We know it when we see it, yet despite decades of experimental and clinical investigations, the mechanisms that evolve and sustain ventricular fibrillation (VF) are still not fully clarified. Defining, describing, and understanding VF continue to be daunting tasks [1, 2]. A description of what we now know as VF was discovered on Egyptian papyri around 1534 BC: “If the heart trembles, has little power and sinks, the disease is advancing….and death is near” [1, 3]. Despite these limitations in our understanding of VF, what we do know is that it can be terminated by delivering electrical current with defined waveform morphologies and timing to fibrillating myocardial cells [4–7]. Because of the inexorable degenerative course untreated VF follows, the timing of defibrillation shock delivery becomes a critical determinant of the likelihood of achieving a favorable outcome [8]. This chapter will discuss some of the areas of controversy in defibrillation.
Defibrillation is an electrophysiologic event that occurs within 100–500 ms of shock delivery (Fig. 5.1). Examination of the rhythm at 5 s after a shock is accepted as a time-point to assess the efficacy of the shock without distortion of the electrocardiogram (ECG) by the voltage offset. Figure 5.2 depicts a successful shock followed by recurrence of VF 9 s later. Resuscitation is a composite of all interventions, and a useful end-point is restoration of a spontaneous circulation (ROSC). This distinction between defibrillation and resuscitation is necessary in order to understand the role and contribution of defibrillation in an overall effort to restore return of ROSC
Progressive degeneration of VF over time. The amplitude, frequency, and VF waveform upstroke velocity all decline. From: Valderrabano [2]
.
2 Cardiopulmonary Resuscitation First or Shock First
Many studies have been reported assessing the question of whether or not defibrillation shocks should be preceded by a period of CPR [9–13]. At this time there is no evidence that supports one approach over the other. A recent detailed review and meta-analysis of randomized trials concluded that deferring the initial shock until a short period of CPR has been performed did not show a survival-to-discharge benefit over immediate defibrillation irrespective of response time. There is no evidence of harm in deferring the first shock until a period of CPR has been done [14]. Most EMS systems will make decisions on this unresolved question with a strong consideration of response time. The definitive resolution of this question will very likely be determined by algorithms capable of analyzing the initial VF with sufficient sensitivity and specificity to predict the outcome of the shock (Figs. 5.3, 5.4).
Compared with the VF in Fig. 5.3 the VF here is of relatively low and varying amplitude but the frequency is sufficient to warrant a shock, which was followed by an organized rhythm during post-shock CPR
3 Termination of Recurrent VF
Recurrence of VF after a successful shock is common. Recurrence at least once was observed in 52–61 % of patients while in the care of Basic Life Support First Responders [15, 16]. In patients during both Basic and Advanced Life Support, VF was observed to occur in 74–80 % of patients [17–19]. Frequent refibrillation was also observed in 67 % of patients in an earlier study describing post-shock rhythms [20]. The 2005 Guidelines recommended immediate resumption of CPR after a shock without regard to the post-shock rhythm and continuation of the CPR for 2 min before re-analysis of the rhythm [21]. With this approach persistent or recurrent VF can continue for at least 2 min after a shock (Fig. 5.5); the implications of this post-shock CPR period warrant a reconsideration. (1) A recent experimental study documented the high oxygen demands of VF [22]. In that study VF was shown to impair restoration of creatine-phosphate levels during simulated CPR. (2) It is assumed that CPR will be performed with such high quality that this high oxygen demand will be met for periods of two or more minutes. (3) The median duration of VF was shorter with shocks that were followed by ROSC. This observation was applied to both initial and recurrent VF [23]. These investigators concluded that detection of VF during ongoing chest compressions might be helpful because of this relationship between shorter duration of VF episodes and ROSC. Their recommendation was that recurring VF should be shocked as soon as possible. (4) Chest compressions can induce VF quickly after resumption of post-shock chest compressions and thus permit VF to continue for nearly 2 min before re-analysis of the rhythm and delivery of a shock [24–27]. Berdowski and colleagues reported that time in recurrent VF is associated with worse outcomes and it is thus desirable to terminate recurrent VF as soon as possible because survival decreases with every minute that the next shock is postponed [24]. An analysis of the performance of the amplitude spectral area and slope to predict defibrillation in out-of-hospital cardiac arrest concluded that for recurrent VF a shock should be delivered immediately upon detection [28]. What then can be considered for modification in terminating recurrent VF? Certainly the well-established benefit of minimally interrupted CPR must be weighed against any modification of the 2 min CPR period after a shock. As resuscitation progresses in time the role of CPR becomes increasingly crucial. (Figs. 5.6, 5.7).
At A, rhythm analysis was commenced, followed by CPR (sCPR). The first shock terminated VF but VF resumed after a few chest compressions. Two minutes of CPR then continued with ongoing VF before the next rhythm analysis. Adapted from: Berdowski et al. [24]
Red arrows indicate chest compressions in two patients (a and b). In both patients VF resumed at the asterisk, shortly after compressions were resumed. In the patient depicted in (a) the third compression occurred during ventricular repolarization. From: Osorio et al. [27]
In 2001 Blouin and colleagues reported their experience with recurrent VF [29]. Using tape-recorded ECG data in 376 shocks, in 96 patients there were 22 shocks with recurrence of VF in 3 min or less. In their experience VF recurred within 6 s after a shock in only 20 % of recurrences, and in 73 % at 60 s. They suggested performing CPR for 30 s after a shock in order to capture the largest number of recurrences. Yet their conclusion was that recurring VF should be acted on rapidly [29].
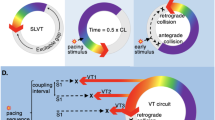
An action plan proposal to confront recurrent VF was described and illustrated in an editorial in response to the Blouin study [30]. Amplification of that approach might be a basis for change. During the first several minutes of intervention in VF, recurrent VF should be recognized by the algorithm or operator quickly after onset and a shock delivered as soon as possible (Fig. 5.8). After 2–3 shocks, if VF continues to recur, other measures, including minimally interrupted CPR and anti-arrhythmic therapy, will be necessary. Advances in algorithm design and function will provide accurate recognition of shockable VF without distortion of ECG interpretation by chest compression artifact. Already major improvements in algorithm performance are being reported, such as faster times to a shock advisory following cessation of chest compressions and the optimal timing of defibrillation by waveform analysis during CPR [3–32]. Sensitivity of over 90 % has been shown to be feasible in recognition of noise-free VF during CPR [33]. Suppression of CPR artifacts using the chest compression rate extracted from the thoracic impedance recording acquired from the defibrillation pads has been demonstrated to be as accurate as methods based on information acquired from CPR feedback data [34]. Continued enhancement of sensitivity and specificity is needed to separate CPR artifact from the ECG to eliminate unacceptable interruptions in CPR. These very recent studies make it evident that we are moving rapidly in that direction. Then prolonged periods of recurrent VF will be minimized with the prospect of more frequent return of an organized rhythm and probably ROSC [13].
Recurrent VF was detected quickly after the first shock and 12 s after onset of recurrent VF a shock restored an immediate organized rhythm. From: (2001) Ann Emerg Med 38(3):278–281 [30]
4 Conclusions
Advances in the treatment of VF, both in defibrillation waveform design and in clinical practice, have contributed significantly to improved outcomes from out-of-hospital cardiac arrest with VF as the initial rhythm. Areas of uncertainty and controversy remain and continue to be subject to ongoing discussion and study. These areas include the appropriate application of CPR first or defibrillation first. For this decision it is very likely that algorithms with high sensitivity and specificity will continue to evolve that will separate VF likely to benefit from a shock first or from CPR first. Because of the very high incidence of recurrent VF and the high oxygen demand of this arrhythmia there is considerable agreement that recurrent VF should be terminated as soon as it is recognized. Again, algorithms that separate chest compression artifact from the underlying rhythm will enable this to occur without unduly compromising ongoing CPR. This is most likely to be clinically applicable in the first several minutes of resuscitation when VF recurs frequently.
References
Karagueuzian HS (2004) Ventricular fibrillation: an organized delirium or uncoordinated reason? Heart Rhythm 1:24–26
Valderrabano M (2011) Deciphering the electrogram in ventricular fibrillation to extract physiological information. Heart Rhythm 8(5):750–751
Breasted JH (1930) The Edwin Smith surgical papyrus. University of Chicago Press, Chicago
White RD (2002) New concepts in transthoracic defibrillation. Emerg Med Clin N Am 20:785–807
Chen B, Yin C, Ristagno G, Quan W, Tan Q, Freeman G, Li Y et al (2012) Retrospective evaluation of current-based impedance compensation defibrillation in out-of-hospital cardiac arrest. Resuscitation doi:10.1016/j.resuscitation.2012.09.017 (Epub ahead of print)
Daubert JP, Sheu SS (2008) Mystery of biphasic defibrillation waveform efficacy. JACC 52(10):836–838
Darragh KM, Manoharan G, Maio R et al (2012) A low tilt waveform in the transthoracic defibrillation of ventricular arrhythmias during cardiac arrest. Resuscitation 83:1438–1443
Chen PS, Wu TJ, Ting CT et al (2003) A tale to two fibrillations. Circulation 108:2298–2303
Cobb LA, Fahrenbruch CE, Walsh TR et al (1999) Influence of cardiopulmonary resuscitation prior to defibrillation in patients with out-of-hospital ventricular fibrillation. JAMA 281(13):1182–1188
Wik L, Hansen TB, Fylling F et al (2003) Delaying defibrillation to give basic cardiopulmonary resuscitation to patients with out-of-hospital ventricular fibrillation. JAMA 289(11):1389–1395
Jacobs IG, Finn JC, Oxer HF, Jelinek GA (2005) CPR before difibrillation in out-of-hospital cardiac arrest: A randomized trial. Emerg Med Australas 17:39–45
Baker PW, Conway J, Cotton C et al (2008) Defibrillation or cardiopulmonary resuscitation first for patient with out-of-hospital cardiac arrests found by paramedics to be in ventricular fibrillation? A randomized control trial. Resuscitation 79:424–431
Koike S, Tanabe S, Ogawa T et al (2011) Immediate defibrillation or defibrillation after cardiopulmonary resuscitation. Prehosp Emerg Care 15:393–400
Simpson PM, Goodger MS, Bendall JC (2010) Delayed versus immediate defibrillation for out-of-hospital cardiac arrest due to ventricular fibrillation: a systematic review and meta-analysis of randomized controlled trials. Resuscitation 81:925–931
White RD, Russell JK (2002) Refibrillation, resuscitation and survival in out-of-hospital sudden cardiac arrest victims treated with biphasic automated external defibrillators. Resuscitation 55:17–23
Hess EP, White RD (2004) Recurrent ventricular fibrillation in out-of-hospital cardiac arrest after defibrillation by police and firefighters: implications for automated external defibrillator users. Crit Care Med 32(9) Suppl:S436-S439
van Alem AP, Post J, Koster RW (2003) VF recurrence: characteristics and patient outcome in out-of-hospital cardiac arrest. Resuscitation 59:181–188
Koster RW, Walker RG, Chapman FW (2008) Recurrent ventricular fibrillation during advanced life support care of patients with prehospital cardiac arrest. Resuscitation 78:252–257
Hess EP, Agarwal D, Myers LA et al (2011) Performance of a rectilinear biphasic waveform in defibrillation of presenting and recurrent ventricular fibrillation: a prospective multicenter study. Resuscitation 82:685–689
Gliner BE, White RD (1999) Electrocardiographic evaluation of defibrillation shocks delivered to out-of-hospital sudden cardiac arrest patients. Resuscitation 41:133–144
American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care, part 3: defibrillation. 2005 Circulation 112:III17–III24
Hoogendijk MG, Schumacher CA, Belterman CNW et al (2012) Ventricular fibrillation hampers the restoration of creatine-phosphate levels during simulated cardiopulmonary resuscitations. Europace 14:1518–1523
Eilevstjonn J, Kramer-Johansen J, Sunde K (2007) Shock outcome is related to prior rhythm and duration of ventricular fibrillation. Resuscitation 75:60–67
Berdowski J, Tijssen JGP, Koster RW (2010) Chest compressions cause recurrence of ventricular fibrillation after the first successful conversion by defibrillation in out-of-hospital cardiac arrest. Circ Arrhythm Electrophysiol 3:72–78
Berdowski J, ten Haaf M, Tijssen JGP et al (2010) Time in recurrent ventricular fibrillation and survival after out-of-hospital cardiac arrest. Circulation 122:1101–1108
Osorio J, Dosdall DJ, Robichaux RP Jr et al (2008) In a swine model, chest compressions cause ventricular capture and, by means of a long-short sequence, ventricular fibrillation. Circ Arrhythmia Electrophysiol 2008:282–289
Osorio J, Dosdall DJ, Tabereaux PB et al (2012) Effect of chest compressions on ventricular activation. Am J Cardiol 109:670–674
Shanmugasundaram M, Valles A, Kellum MJ et al (2012) Analysis of amplitude spectral area and slope to predict defibrillation in out of hospital cardiac arrest due to ventricular fibrillation (VF) according to VF type: recurrent versus shock-resistant. Resuscitation 83:1242–1247
Blouin D, Topping C, Moore S et al (2001) Out-of-hospital defibrillation with automated external defibrillations: postshock analysis should be delayed. Ann Emerg Med 38(3):256–261
White RD (2001) To shock or not to shock: that is the question. Ann Emerg med 38(3):278–281
Didon JP, Krasteva V, Menetre S (2011) Shock advisory system with minimal delay triggering after end of chest compressions: accuracy and gained hands-off time. Resuscitation 82S:S8–S15
Li Y, Tang W (2012) Optimizing the timing of defibrillation: the role of ventricular fibrillation waveform analysis during cardiopulmonary resuscitation. Crit Care Clin 28:199–210
Krasteva V, Jekova I, Dotsinsky I, Didon JP (2010) Shock advisory system for heart rhythm analysis during cardiopulmonary resuscitation using a single ECG input of automated external defibrillators. Ann Biomed Eng 38(4):1326–1336
Aramendi E, Ayala U, Irusta U et al (2012) Suppression of the cardiopulmonary resuscitation artifacts using the instantaneous chest compression rate extracted from the thoracic impedance. Resuscitation 83:692–698
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag Italia
About this chapter
Cite this chapter
White, R.D. (2014). Ventricular Fibrillation and Defibrillation: State of Our Knowledge and Uncertainities. In: Gullo, A., Ristagno, G. (eds) Resuscitation. Springer, Milano. https://doi.org/10.1007/978-88-470-5507-0_5
Download citation
DOI: https://doi.org/10.1007/978-88-470-5507-0_5
Published:
Publisher Name: Springer, Milano
Print ISBN: 978-88-470-5506-3
Online ISBN: 978-88-470-5507-0
eBook Packages: MedicineMedicine (R0)