Abstract
Helicobacter pylori vacuolating cytotoxin (VacA) is a major virulence factor, with pleiotropic actions on target cells including induction of vacuole formation, mitochondrial dysfunction leading to apoptosis, modulation of signal transduction pathways associated with autophagy, inhibition of T cell proliferation, and production of inflammatory cytokines. Numerous epidemiological studies have indicated that the allelic diversity within four variable regions of the vacA gene might be associated with cell type-specific binding as well as specific clinical outcomes in H. pylori infection. VacA binds to receptors such as receptor protein tyrosine phosphatases (RPTPα and RPTPβ), low-density lipoprotein receptor-related protein-1 (LRP1), fibronectin, CD18, and sphingomyelin to facilitate its action, suggesting the involvement of these receptors in the pathogenesis of H. pylori infection. RPTPβ contributes to ulceration in gastric epithelial cells and LRP1 is involved in the induction of autophagy. Interestingly, it has been suggested that CagA is degraded by VacA-induced autophagy and that the interaction between these two molecules is associated with the pathogenesis of gastric diseases. Therefore, better understanding of the mechanism of VacA toxicity may provide valuable information regarding appropriate medical care for gastroduodenal diseases caused by H. pylori infection.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Helicobacter pylori is a Gram-negative bacterium that causes gastroduodenal diseases including chronic gastritis, peptic ulcers, gastric adenocarcinoma, and gastric lymphoma. A number of virulence factors are involved in the pathogenesis of H. pylori infection. During colonization of the gastric epithelium, H. pylori secretes a potent protein toxin, vacuolating cytotoxin, termed VacA, which is considered to be an important virulence factor associated with peptic ulcer disease, indicating that VacA is critical to the pathogenicity of H. pylori [1–4]. Although vacuolation, a hallmark of VacA function (Fig. 4.1), is readily observed in VacA-intoxicated cells in vitro, its function in vivo in H. pylori infection is unclear.
Vacuolation in the cytoplasm of mammalian cells. Purified VacA (left) or vehicle (right) was added, and cultured mammalian cells were incubated at 37 °C, 5 % CO2 for several hours. Many vacuoles (arrows) were observed in the cytoplasm of cells incubated in the presence of VacA, while vehicle did not cause vacuolation. Thus, VacA is the responsible protein for vacuole formation
In 1988, Leunk et al. reported that the broth culture filtrates of H. pylori caused the generation of large vacuoles in the cytoplasm of cultured mammalian cells [5]. After Cover et al. purified an 87-kDa VacA from culture supernatant [6], the entire nucleotide sequence of the vacA gene and its deduced amino acid sequence were determined, revealing the presence of a protoxin of about 140 kDa that lacked homology to any other protein [7]. Vacuolating activity was enhanced by acidic (<pH 5.5) or alkaline (>pH 9.5) conditions due to conformational changes in the protein [8, 9]. Further, vacuolating activity was also potentiated by weak bases, including ammonium chloride and nicotine [10]. After binding to the cell surface receptors, VacA internalizes into epithelial cells by endocytosis and then induces the formation of vacuoles, which are derived from late endosomes. Maturation of vacuoles involves several host molecules including a small GTPase, Rab7, and vacuolar-type ATPase (V-ATPase) proton pump. Rab7 is essential for the efficient membrane flow from early to late endosome, and V-ATPase is involved in osmotic swelling of the endosomal compartment, resulting in generation of VacA-dependent vacuolation [11–13].
VacA also causes mitochondrial dysfunction, leading eventually to apoptotic cell death through cytochrome c release and caspase activation [14–16]. Furthermore, VacA also modulates membrane potential and signal transduction pathways associated with immune responses, induction of autophagy, and inhibition of T cell proliferation [17–21]. There is some evidence of an antagonistic relationship between VacA and cytotoxin-associated gene A (CagA), another important H. pylori virulence factor [22–24], suggesting that both toxins contribute to the development of gastric disorders in H. pylori infection. In this review, we will discuss the multiple functions of VacA on target host cells and also discuss the latest research on VacA function.
2 Protein Structure and Domains of VacA
All isolated strains of H. pylori contain the vacA gene encoding a 140-kDa precursor protein, which has three major domains, i.e., signal sequence, mature toxin, and autotransporter domains. Proteolytic cleavage of the signal sequence and autotransporter domain from a VacA protoxin results in a mature VacA toxin of about 90-kDa molecular mass, which is secreted into the extracellular space by a type V secretion system (Fig. 4.2a) [1, 6, 7, 25]. Secreted mature VacA forms an oligomeric structure, and the assembled VacA has an expected molecular mass of around 1000 kDa under neutral pH or non-denaturing conditions [6]. Upon imaging analysis by electron microscopy, VacA oligomer is composed of six or seven VacA monomers that form a flower-shaped structure with a central ring. VacA oligomerization leads to the assembly of a double-layered form of a single VacA oligomer (consisting of 12 or 14 VacA monomers), rather than the single-layered oligomer [26–29]. VacA oligomers observed in the lipid bilayer of cell or mitochondrial membrane seem to contribute to anion-selective membrane channel formation [26, 30]. The mature VacA is further cleaved into two fragments by proteolytic digestion and consists of 33-kDa N-terminal (termed p33) and 55-kDa C-terminal fragments (termed p55) [1, 27, 31]. It has been proposed that in the three-dimensional structures of VacA oligomers, p55 represents the peripheral arms and p33, the central core of the complexes [29].
vacA gene allelic and protein structures. (a) Precursor VacA is synthesized in H. pylori with three functional domains (signal sequence, mature toxin, and autotransporter domain). Mature VacA protein, which lacks two fragments (signal sequence and autotransporter domain), is generated by proteolytic digestion and is then secreted by a type V secretion system. The p33 and p55 fragments might be generated from the mature form of VacA. Arrowheads indicate cleavage sites. (b) The vacA gene as four variable regions: s-region (black, s1 and s2), i-region (green, i1, i2, and i3), d-region (red, d1), and m-region (blue, m1 and m2). The vacA gene allele d2 is missing the d1 region (lower figure)
Although many studies about the cellular functions of both p33 and p55 have been performed, their functions are still debated. Several lines of evidence have indicated that p55 is involved in binding to host cells, whereas p33 plays a role in the formation of anion channels in the lipid membrane and is targeted to the inner mitochondrial membrane, leading to the loss of membrane potential [14]. In addition, it has been reported that p33 is crucial in pore formation in lipid bilayers [32]. The N-terminal of p33 is predicted to contain a hydrophobic region, which is required for not only channel formation but also vacuolating activity and trafficking to the inner mitochondrial membrane [33, 34]. Furthermore, the proline residue at position 9 and glycine residue at position 14 in p33 play key roles in these activities [35]. In addition, GXXXG motif at residues 14–18 in p33 is also important for channel formation [34]. However, mutant VacA lacking a part of the hydrophobic region retained channel activity in planar lipid bilayers [32]. Other studies have shown that p33 and p55 are involved in cell binding and channel formation [36, 37]. Thus, further studies to define the molecular basis underlying p33 and p55 activities are required.
3 Gene Structure of vacA
3.1 Polymorphism of the vacA Gene
Although all H. pylori strains isolated from patients possess a vacA gene, only approximately 50 % of the isolates show vacuolating activity because of allelic diversity within the vacA gene [2, 6]. Nucleotide sequence analyses of the vacA gene have revealed that polymorphisms exist in four variable regions (Fig. 4.2b) [38]. The most characterized allelic diversities are observed within the signal sequence region (s-region) and the mid-region (m-region). The s-region is located at the 5′ end of the vacA gene and includes the signal sequence of VacA (designated s1 and s2). Interestingly, epidemiological studies have shown that strains possessing the s1 type of vacA are linked to the presence of the cagA gene [39, 40]. The s1-type allele is further classified into three subtypes s1a, s1b, and s1c, respectively [41]. Strains possessing the s2 type of vacA allele fail to induce vacuolation in cultured mammalian cells [2]. A hydrophilic segment consisting of 12-amino acids in the s2 type, which the s1 type lacks, suppresses VacA-induced vacuolating activity without any effect on its production [42–44]. Two m-regions (classified as m1 and m2) are located within p55; m2 is further divided into two subtypes, m2a and m2b [2, 41]. The entire m-region composed of m1 and m2 alleles is required for vacuolating activity [45, 46]. However, there is a clear difference in cell specificity between m1 and m2 [47], e.g., m2-type VacA, in contrast to m1-type VacA does not induce vacuole formation in HeLa cells irrespective of acid or alkaline activation [48]. De Guzman et al. have indicated that m2-type VacA does not bind to receptor protein tyrosine phosphatase (RPTP) α, one of the VacA-binding receptors, on membranes of HeLa cells, suggesting that posttranslational modifications of RPTPα of HeLa cells may determine sensitivity to m2 VacA [48]. Combinations of vacA alleles (s1/m1, s1/m2, and s2/m2) are commonly found in clinically isolated strains of H. pylori, but s2/m1 type of vacA gene is rare [2, 49].
Two other variable regions in the vacA gene have been identified. The intermediate region (i-region) has been identified as a third polymorphism region and is located between s- and m-regions (noted as i1, i2, and i3). Rhead et al. has indicated that the s1/m1 allele strains were predominantly i1 type, whereas all s2/m2 allele strains were i2 type and s1/m2 allele strains were variable in the i-region [50]. In addition, there is some evidence that the i-region affects human T cell functions, e.g., i2 type had a diminished capacity to inhibit the activation of nuclear factor of activated T cells (NFAT) and bound to Jurkat cells less avidly than did i1 type [51]. The fourth polymorphism is observed in the deletion region (d-region), which is located between i- and m-regions (noted as d1 and d2) [52]. It has been demonstrated that there is no deletion in the d1 genotype of the vacA gene, but d2 genotype contains a deleted region. However, the effects of the d-regions are still unclear.
3.2 Association Between vacA Gene Alleles and Clinical Outcomes
Many epidemiological studies indicate that a clear functional association between vacA gene alleles and clinical outcome of gastroduodenal diseases has not been found. Generally, s1/m1 vacA is a more toxic genotype than are s1/m2 and s2 types of the vacA alleles [44]. The s1/m1 vacA allele is predominantly isolated from patients, suggesting that strains possessing the s1/m1 vacA allele are more likely to be associated with gastroduodenal disease than other vacA alleles, whereas strains possessing s2 type of vacA are rarely associated with disease. The s1 or s1/m1 vacA allele is associated with duodenal ulceration and gastric cancer in the United States and Western Europe. On the other hand, most of the clinical isolates possess the s1/m1 vacA allele in East Asia including Japan and South Korea, where there is a high incidence of gastric cancer [2, 39, 53–56]. In addition, it has been proposed that i1 genotype is associated with gastric cancer and gastric ulcer in Italian populations, and therefore, the i-region might be a good indicator of the carcinogenic ability of H. pylori strains, while any combinations of three variable regions (s-, m-, and i-regions) in the vacA gene were not disease determinants in East Asian and Southeast Asian countries [50, 57, 58]. From these observations, relationships between vacA genotypes and specific clinical outcomes may be different in different geographic areas.
4 VacA Receptors on Target Cells
It is important to identify specific bacterial toxin receptors on the cell surface. These receptors play a critical role in bacterial toxin binding and entry into cells, followed by intoxication. Thus, interaction between toxin and receptors induce unique signal transduction pathways, leading to effects (e.g., morphological changes, cell damage) on the target cell.
The C-terminal domain of VacA is responsible for binding to cell surface receptors [14, 47]. We identified toxin-binding cultured cell compartments by immunoprecipitation analysis with purified VacA and biotin-labeled cultured cell lysate. In VacA-sensitive cells, we found that biotinylated cell surface proteins of 140 kDa (p140) and 250 kDa (p250) were precipitated with VacA but not inactivated VacA [59]. On the other hand, Seto and colleagues reported that the EGF receptor might be involved in VacA endocytosis, leading to induction of vacuolating activity [60]. Since these VacA-binding proteins, p140 and p250, were modified by N-linked sugar, we purified these proteins using lectin agarose. By LC-MS/MS analysis, RPTPα and RPTPβ were identified as VacA-binding proteins [9, 61].
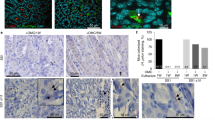
De Bernard et al. reported that phorbol 12-myristate 13-acetate (PMA) induces differentiation of HL-60 cells into macrophage-like cells and induced the susceptibility to VacA [62]. It was found that expression of RPTPβ mRNA and protein was significantly induced during differentiation of HL-60 cells by PMA [63]. Consistently, knockdown of RPTPβ by antisense oligonucleotide resulted in reduction of VacA-induced vacuolation in parallel with suppression of RPTPβ expression [63]. In addition, it is known that acid or alkaline treatment induced conformational changes in VacA, which increased binding, internalization, and cytotoxicity [9, 64]. The activated VacA showed increased binding to RPTPβ, suggesting that conformational changes of VacA promote its interaction with cell surface RPTPβ [9]. Fujikawa et al. demonstrated that oral administration of VacA to wild-type mice, but not RPTPβ knockout mice, resulted in gastric ulcers, indicating that RPTPβ is essential for intoxication by VacA in gastric tissue [65]. These results suggest that VacA binding to RPTPβ has functional effects.
With G401 cells, a human kidney tumor cell line that lacks RPTPβ but forms vacuoles in the presence of VacA, we also identified p140 as RPTPα. The finding that silencing of RPTPα gene by antisense oligonucleotide in G401 cells inhibited VacA binding and induction of vacuolation supports the hypothesis that RPTPα mediates VacA intoxication [61].
Other surface factors appear to interact with VacA and serve as cell surface receptors. By surface plasmon resonance-based biosensor studies, it has been proven that VacA binds to heparin sulfate, a component of the extracellular matrix [66]. Hennig et al. demonstrated that VacA binds to fibronectin of HeLa cells, resulting in inhibition of HeLa cell adhesion, suggesting that VacA affects cytoskeleton organization and cell adhesion via interaction with fibronectin [67]. Further, Gupta et al. also reported that VacA-induced vacuolation in HeLa cells is reduced in the presence of sphingomyelinase [68]. Sewald et al. have reported that β2-integrin subunit CD18 plays an important role in VacA uptake into human T lymphocytes [69]. Through this mechanism, VacA has immunosuppressive effects on cells by inhibiting cell growth and interleukin-2 (IL-2) secretion [69]. They also demonstrated that VacA endocytosis is PKC-dependent and clathrin-independent in primary T cells [70]. Recently, we identified a new VacA receptor, low-density lipoprotein receptor-related protein-1 (LRP1), which is essential for VacA-induced autophagy and apoptosis [19].
5 VacA Uptake Pathway
After binding to its receptors on target cells, VacA is internalized and found in endocytic vesicles. To enter into epithelial cells, VacA associates with lipid rafts [71, 72] and then internalizes via the Cdc42-dependent pinocytic pathway without requirement for dynamin 2, ADP-ribosylation factor 6, or RhoA GTPase. In this process, VacA was associated with detergent-resistant membranes [73]. Gupta et al. also reported that sphingomyelin is important in VacA uptake and intracellular translocation [74]. Furthermore, there is some evidence that VacA is endocytosed via a GPI-anchored protein-enriched early endosomal compartment (GEEC)-dependent pathway. Filamentous actin is involved in VacA translocation from GEECs to late endosomes [75]. In primary T lymphocytes, VacA endocytosis is regulated by PKC-, Cdc42- and Rac1-dependent pathways [70].
6 Biological Activities of VacA
6.1 Vacuolation and Autophagy
The vacuoles induced by interfering with intracellular membrane fusion in VacA-intoxicated cells contain markers of a pre-lysosomal compartment, including Rab7, Lgp110, and LAMP1 [76–78]. Further, various host factors, including dynamin, Rac1 and PIKfyve, are involved in VacA-induced vacuole formation [79–82]. The facts that VacA-induced vacuolation is suppressed by a V-ATPase inhibitor, bafilomycin A1, and V-ATPase colocalized with Rab7 in VacA-induced vacuoles suggest that a pH gradient generated through the activity of V-ATPase proton pump is required for this process (Fig. 4.3a) [83, 84].
Pleiotropic functions of VacA. During H. pylori infection, VacA is internalized into target host cells via its receptors. (a) VacA generates the formation of large vacuoles in the cytoplasm by activation of V-ATPase. (b) After translocation of CagA into gastric epithelial cells, CagA is degraded by VacA-induced autophagy. (c) VacA localizes to the mitochondria and modulates the mitochondrial functions leading to cytochrome c release or caspase activation, resulting in apoptosis. In addition, ER stress is also involved in VacA-induced apoptosis. (d) VacA modulates signal transduction pathways, e.g., VacA activates PI3K/Akt signaling pathway, resulting in phosphorylation of GSK3β, associated with induction of β-catenin release from the GSK3β/β-catenin complex. Resulting β-catenin can translocate from cytoplasm to nucleus to induce expression of genes such as cyclin D1. (e) VacA binds to CD18 and modulates signal transduction pathways, resulting in inhibition of T cell proliferation
Recent studies have reported that VacA induces autophagy, which is different from the large vacuoles formed in VacA-intoxicated cells [85–87]. VacA-induced autophagosomes and autophagolysosomes are dependent on functions of Atg family proteins (e.g., Atg5, Atg12, Atg16L1), with LC3-positive vesicles observed by confocal microscopy [85]. The internalized VacA partially colocalized with LC3 and LRP1 but not mitochondria. Additionally, the channel activity of VacA was also required for autophagosome formation [19, 85]. These findings indicate that VacA associates with autophagosomes and autophagolysosomes. Tsugawa et al. recently demonstrated that CagA is degraded by VacA-induced autophagy, which is regulated by a reactive oxygen species (ROS)-Akt-p53 signaling pathway (Fig. 4.3b) [24]. Interestingly, they found that CD44v9-expressing gastric cancer stem-like cells accumulated CagA by inhibition of VacA-induced autophagy through a mechanism involving cellular increase of glutathione due to stabilization of cystine transporter. A recent study showed that H. pylori have a strategy to avoid clearance by autophagy, i.e., H. pylori infection increased miR30BA, which directly downregulates autophagy regulatory proteins, Atg12 and Beclin1 [88]. Thus, H. pylori use several mechanisms to escape host autophagy, and then the persistent pathogen can produced various virulence factors, which trigger the pathological processes involved in diseases.
6.2 Apoptosis
VacA also induces apoptosis of various cells [11, 89]. It has been suggested that p33 N-terminal fragment of VacA has a unique sequence, which translocates into mitochondria to facilitate intoxication [90]. Apoptosis induced by VacA may proceed by two mechanisms (Fig. 4.3c). After internalization into cytosol, VacA directly moves to mitochondria, followed by modulation of mitochondrial membrane permeability by its channel activity, leading to cytochrome c release and apoptosis [14, 91–93]. Another pathway involves the proapoptotic Bcl-2 family protein in VacA-induced apoptosis, i.e., VacA causes caspase activation and PARP cleavage, subsequent to activation of Bax/Bak on the mitochondria [16, 94, 95]. Calore et al. have demonstrated that VacA-induced apoptosis requires Bax/Bak-dependent juxtaposition of endosomes and mitochondria and accumulation of VacA and Bax in mitochondria [96]. These findings suggest that movements of both VacA and Bax/Bak into mitochondria are important in the apoptotic pathway. Matsumoto et al. reported that VacA downregulates STAT3 expression, followed by reduction of the amounts of Bcl-2 and Bcl-xL, which are anti-apoptotic proteins [97]. Jain et al. reported that VacA-induced activation of dynamin-related protein 1(Drp1), a regulator of mitochondrial fission, is critical to apoptosis and that activation of Drp1-dependent mitochondrial fission requires channel activity of VacA, but not Bax activation, suggesting that cross talk between Drp1 and Bax may be unidirectional in VacA-treated cells [98].
Recently, it was demonstrated that VacA activates PERK, an endoplasmic reticulum (ER) stress sensor protein, and stimulates phosphorylation of eIF2α, followed by induction of C/EBP homologous protein (CHOP), a key protein of ER stress-induced apoptosis [99], suggesting that ER stress is also involved in VacA-induced apoptosis in AZ-521 and dendritic cells. More recently, Radin et al. have reported that connexin 43 (Cx43), a major component of the gap junction, in AZ-521 cells contributes to VacA-induced cell death [100].
On the other hand, in eosinophils, VacA induced apoptosis via p38 mitogen-activated protein kinase (MAPK) activation, leading to Bax translocation and cytochrome c release, although VacA promotes inhibitor of apoptosis protein (c-IAP)-2 expression at an early step in the process [94].
6.3 Immunosuppressive Activity of VacA
VacA might contribute to chronic infection of H. pylori in the stomach by preventing protective immunity [51, 94, 101]. Molinari et al. have reported that VacA inhibits the Ii-dependent process of antigen presentation through MHC class II [102]. Other groups also indicated that VacA could not only interfere with T cell activation by preventing NFAT activity, resulting in suppression of IL-2 expression, but also activate MAPK kinase (MKK) 3/6 and Vav/Rac1, leading to massive actin reorganization in T cells (Fig. 4.3e) [103, 104]. In addition, Kim et al. reported that VacA treatment inhibits LPS-induced dendritic cell maturation, suggesting that VacA negatively regulates dendritic cell maturation through the restoration of E2F1 [105].
ROS also plays important roles in host defense [106]. In macrophages, VacA inhibits ROS production by interfering with expression of integrin-linked kinase (ILK), followed by suppression of endothelial nitric oxygen synthase (eNOS), resulting in increased survival of VacA-positive H. pylori [107].
6.4 Cell Signal Transduction by VacA
VacA has diverse roles in signal transduction including proliferation, apoptosis, and host defense [18, 108]. Nakayama et al. reported that in AZ-521 cells, VacA activates p38 MAPK/activating transcription factor 2 (ATF-2) signaling pathway, which requires interaction with an unknown GPI-anchored membrane protein in lipid rafts [72]. Furthermore, VacA induced phosphoinositide-3-kinase activation, leading to phosphorylation of Akt and glycogen synthase kinase-3β (GSK3β). This signal transduction pathway interfered with β-catenin translocation from cytoplasm to nucleus by inhibiting β-catenin release from GSK3β/β-catenin complex (Fig. 4.3d) [109]. Another study showed that VacA treatment activates prostaglandin E2 production through induction of cyclooxygenase 2 (COX-2) expression via the p38 MAPK/ATF-2 pathway, leading to stimulation of cis-acting replication element (CRE) site in the COX-2 promoter [110].
In T cells and monocytic cell line U937, VacA enhanced NF-κB activation [111, 112]. In U937 cells, VacA induced IL-8 production via activation of p38 MAPK through intracellular Ca2+ release, leading to stimulation of IL-8 promoter activation by binding of transcription factors, ATF-2, CRE-binding protein (CREB), and NF-κB [112]. These results indicate that H. pylori VacA is a pleiotropic toxin, able to affect various signaling transduction pathways and disrupt cell homeostasis.
7 Conclusion
VacA has pleiotropic actions in vitro and is considered to be one of the most important virulence factors of H. pylori. In addition to the findings related to VacA toxicity, it is interesting to note that the biological activities of VacA and the prevalence of some types of gastroduodenal disease caused by H. pylori infection are strongly associated with specific vacA gene alleles, suggesting that the vacA gene allele is a putative genetic biomarker of H. pylori-induced gastric diseases. Although many studies have demonstrated more clearly the importance of VacA in H. pylori infection, current investigations are focused on understanding the mechanisms by which VacA causes the pathogenesis of gastroduodenal diseases. Therefore, research on VacA may lead to a better understanding of its role in the development of gastric disorders and modulation of host immune defense in H. pylori infection. Thus, further studies may provide new insights into the role of VacA as a factor that promotes gastric diseases.
References
Telford JL, Ghiara P, Dell’Orco M, Comanducci M, Burroni D, Bugnoli M, et al. Gene structure of the Helicobacter pylori cytotoxin and evidence of its key role in gastric disease. J Exp Med. 1994;179:1653–8.
Atherton JC, Cao P, Peek Jr RM, Tummuru MK, Blaser MJ, Cover TL. Mosaicism in vacuolating cytotoxin alleles of Helicobacter pylori. Association of specific vacA types with cytotoxin production and peptic ulceration. J Biol Chem. 1995;270:17771–7.
Tee W, Lambert JR, Dwyer B. Cytotoxin production by Helicobacter pylori from patients with upper gastrointestinal tract diseases. J Clin Microbiol. 1995;33:1203–5.
Memon AA, Hussein NR, Miendje Deyi VY, Burette A, Atherton JC. Vacuolating cytotoxin genotypes are strong markers of gastric cancer and duodenal ulcer-associated Helicobacter pylori strains: a matched case–control study. J Clin Microbiol. 2014;52:2984–9.
Leunk RD, Johnson PT, David BC, Kraft WG, Morgan DR. Cytotoxic activity in broth-culture filtrates of Campylobacter pylori. J Med Microbiol. 1988;26:93–9.
Cover TL, Blaser MJ. Purification and characterization of the vacuolating toxin from Helicobacter pylori. J Biol Chem. 1992;267:10570–5.
Cover TL, Tummuru MK, Cao P, Thompson SA, Blaser MJ. Divergence of genetic sequences for the vacuolating cytotoxin among Helicobacter pylori strains. J Biol Chem. 1994;269:10566–73.
de Bernard M, Papini E, de Filippis V, Gottardi E, Telford J, Manetti R, et al. Low pH activates the vacuolating toxin of Helicobacter pylori, which becomes acid and pepsin resistant. J Biol Chem. 1995;270:23937–40.
Yahiro K, Niidome T, Kimura M, Hatakeyama T, Aoyagi H, Kurazono H, et al. Activation of Helicobacter pylori VacA toxin by alkaline or acid conditions increases its binding to a 250-kDa receptor protein-tyrosine phosphatase beta. J Biol Chem. 1999;274:36693–9.
Cover TL, Vaughn SG, Cao P, Blaser MJ. Potentiation of Helicobacter pylori vacuolating toxin activity by nicotine and other weak bases. J Infect Dis. 1992;166:1073–8.
Rassow J. Helicobacter pylori vacuolating toxin A and apoptosis. Cell Commun Signal. 2011;9:26.
Papini E, Satin B, Bucc C, de Bernard M, Telford JL, Manetti R, et al. The small GTP binding protein rab7 is essential for cellular vacuolation induced by Helicobacter pylori cytotoxin. EMBO J. 1997;16:15–24.
Genisset C, Puhar A, Calore F, de Bernard M, Dell’Antone P, Montecucco C. The concerted action of the Helicobacter pylori cytotoxin VacA and of the v-ATPase proton pump induces swelling of isolated endosomes. Cell Microbiol. 2007;9:1481–90.
Galmiche A, Rassow J, Doye A, Cagnol S, Chambard JC, Contamin S, et al. The N-terminal 34 kDa fragment of Helicobacter pylori vacuolating cytotoxin targets mitochondria and induces cytochrome c release. EMBO J. 2000;19:6361–70.
Kimura M, Goto S, Wada A, Yahiro K, Niidome T, Hatakeyama T, et al. Vacuolating cytotoxin purified from Helicobacter pylori causes mitochondrial damage in human gastric cells. Microb Pathog. 1999;26:45–52.
Yamasaki E, Wada A, Kumatori A, Nakagawa I, Funao J, Nakayama M, et al. Helicobacter pylori vacuolating cytotoxin induces activation of the proapoptotic proteins Bax and Bak, leading to cytochrome c release and cell death, independent of vacuolation. J Biol Chem. 2006;281:11250–9.
Cover TL, Blanke SR. Helicobacter pylori VacA, a paradigm for toxin multifunctionality. Nat Rev Microbiol. 2005;3:320–32.
Isomoto H, Moss J, Hirayama T. Pleiotropic actions of Helicobacter pylori vacuolating cytotoxin, VacA. Tohoku J Exp Med. 2010;220:3–14.
Yahiro K, Satoh M, Nakano M, Hisatsune J, Isomoto H, Sap J, et al. Low-density lipoprotein receptor-related protein-1 (LRP1) mediates autophagy and apoptosis caused by Helicobacter pylori VacA. J Biol Chem. 2012;287:31104–15.
Kim IJ, Blanke SR. Remodeling the host environment: modulation of the gastric epithelium by the Helicobacter pylori vacuolating toxin (VacA). Front Cell Infect Microbiol. 2012;2:37.
Greenfield LK, Jones NL. Modulation of autophagy by Helicobacter pylori and its role in gastric carcinogenesis. Trends Microbiol. 2013;21:602–12.
Oldani A, Cormont M, Hofman V, Chiozzi V, Oregioni O, Canonici A, et al. Helicobacter pylori counteracts the apoptotic action of its VacA toxin by injecting the CagA protein into gastric epithelial cells. PLoS Pathog. 2009;5, e1000603.
Akada JK, Aoki H, Torigoe Y, Kitagawa T, Kurazono H, Hoshida H, et al. Helicobacter pylori CagA inhibits endocytosis of cytotoxin VacA in host cells. Dis Model Mech. 2010;3:605–17.
Tsugawa H, Suzuki H, Saya H, Hatakeyama M, Hirayama T, Hirata K, et al. Reactive oxygen species-induced autophagic degradation of Helicobacter pylori CagA is specifically suppressed in cancer stem-like cells. Cell Host Microbe. 2012;12:764–77.
Fischer W, Buhrdorf R, Gerland E, Haas R. Outer membrane targeting of passenger proteins by the vacuolating cytotoxin autotransporter of Helicobacter pylori. Infect Immun. 2001;69:6769–75.
Adrian M, Cover TL, Dubochet J, Heuser JE. Multiple oligomeric states of the Helicobacter pylori vacuolating toxin demonstrated by cryo-electron microscopy. J Mol Biol. 2002;318:121–33.
Cover TL, Hanson PI, Heuser JE. Acid-induced dissociation of VacA, the Helicobacter pylori vacuolating cytotoxin, reveals its pattern of assembly. J Cell Biol. 1997;138:759–69.
El-Bez C, Adrian M, Dubochet J, Cover TL. High resolution structural analysis of Helicobacter pylori VacA toxin oligomers by cryo-negative staining electron microscopy. J Struct Biol. 2005;151:215–28.
Chambers MG, Pyburn TM, González-Rivera C, Collier SE, Eli I, Yip CK, et al. Structural analysis of the oligomeric states of Helicobacter pylori VacA toxin. J Mol Biol. 2013;425:524–35.
Iwamoto H, Czajkowsky DM, Cover TL, Szabo G, Shao Z. VacA from Helicobacter pylori: a hexameric chloride channel. FEBS Lett. 1999;450:101–4.
Torres VJ, McClain MS, Cover TL. Interactions between p-33 and p-55 domains of the Helicobacter pylori vacuolating cytotoxin (VacA). J Biol Chem. 2004;279:2324–31.
Torres VJ, McClain MS, Cover TL. Mapping of a domain required for protein-protein interactions and inhibitory activity of a Helicobacter pylori dominant-negative VacA mutant protein. Infect Immun. 2006;74:2093–101.
Vinion-Dubiel AD, McClain MS, Czajkowsky DM, Iwamoto H, Ye D, Cao P, et al. A dominant negative mutant of Helicobacter pylori vacuolating toxin (VacA) inhibits VacA-induced cell vacuolation. J Biol Chem. 1999;274:37736–42.
McClain MS, Iwamoto H, Cao P, Vinion-Dubiel AD, Li Y, Szabo G, et al. Essential role of a GXXXG motif for membrane channel formation by Helicobacter pylori vacuolating toxin. J Biol Chem. 2003;278:12101–8.
Boquet P, Ricci V. Intoxication strategy of Helicobacter pylori VacA toxin. Trends Microbiol. 2012;20:165–74.
Torres VJ, Ivie SE, McClain MS, Cover TL. Functional properties of the p33 and p55 domains of the Helicobacter pylori vacuolating cytotoxin. J Biol Chem. 2005;280:21107–14.
Ivie SE, McClain MS, Torres VJ, Algood HM, Lacy DB, Yang R, et al. Helicobacter pylori VacA subdomain required for intracellular toxin activity and assembly of functional oligomeric complexes. Infect Immun. 2008;76:2843–51.
Bridge DR, Merrell DS. Polymorphism in the Helicobacter pylori CagA and VacA toxins and disease. Gut Microbes. 2013;4:101–17.
Miehlke S, Kirsch C, Agha-Amiri K, Günther T, Lehn N, Malfertheiner P, et al. The Helicobacter pylori vacA s1, m1 genotype and cagA is associated with gastric carcinoma in Germany. Int J Cancer. 2000;87:322–7.
Yamaoka Y, Kodama T, Kita M, Imanishi J, Kashima K, Graham DY. Relationship of vacA genotypes of Helicobacter pylori to cagA status, cytotoxin production, and clinical outcome. Helicobacter. 1998;3:241–53.
van Doorn LJ, Figueiredo C, Sanna R, Pena S, Midolo P, Ng EK, et al. Expanding allelic diversity of Helicobacter pylori vacA. J Clin Microbiol. 1998;36:2597–603.
Letley DP, Atherton JC. Natural diversity in the N terminus of the mature vacuolating cytotoxin of Helicobacter pylori determines cytotoxin activity. J Bacteriol. 2000;182:3278–80.
McClain MS, Cao P, Iwamoto H, Vinion-Dubiel AD, Szabo G, Shao Z, et al. A 12-amino-acid segment, present in type s2 but not type s1 Helicobacter pylori VacA proteins, abolishes cytotoxin activity and alters membrane channel formation. J Bacteriol. 2001;183:6499–508.
Letley DP, Rhead JL, Twells RJ, Dove B, Atherton JC. Determinants of non-toxicity in the gastric pathogen Helicobacter pylori. J Biol Chem. 2003;278:26734–41.
Ji X, Fernandez T, Burroni D, Pagliaccia C, Atherton JC, Reyrat J, et al. Cell specificity of Helicobacter pylori cytotoxin is determined by a short region in the polymorphic midregion. Infect Immun. 2000;68:3754–57.
Skibinski DA, Genisset C, Barone S, Telford JL. The cell-specific phenotype of the polymorphic vacA midregion is independent of the appearance of the cell surface receptor protein tyrosine phosphatase beta. Infect Immun. 2006;74:49–55.
Pagliaccia C, de Bernard M, Lupetti P, Ji X, Burroni D, Cover TL, et al. The m2 form of the Helicobacter pylori cytotoxin has cell type-specific vacuolating activity. Proc Natl Acad Sci USA. 1998;95:10212–17.
De Guzman BB, Hisatsune J, Nakayama M, Yahiro K, Wada A, Yamasaki E, et al. Cytotoxicity and recognition of receptor-like protein tyrosine phosphatases, RPTPalpha and RPTPbeta, by Helicobacter pylori m2VacA. Cell Microbiol. 2005;7:1285–93.
Bindayna KM, Al Mahmeed A. vacA genotypes in Helicobacter pylori strains isolated from patients with and without duodenal ulcer in Bahrain. Indian J Gastroenterol. 2009;28:175–9.
Rhead JL, Letley DP, Mohammadi M, Hussein N, Mohagheghi MA, Eshagh Hosseini M, et al. A new Helicobacter pylori vacuolating cytotoxin determinant, the intermediate region, is associated with gastric cancer. Gastroenterology. 2007;133:926–36.
González-Rivera C, Algood HM, Radin JN, McClain MS, Cover TL. The intermediate region of Helicobacter pylori VacA is a determinant of toxin potency in a Jurkat T cell assay. Infect Immun. 2012;80:2578–88.
Ogiwara H, Sugimoto M, Ohno T, Vilaichone RK, Mahachai V, Graham DY, et al. Role of deletion located between the intermediate and middle regions of the Helicobacter pylori vacA gene in cases of gastroduodenal diseases. J Clin Microbiol. 2009;47:3493–500.
Kidd M, Lastovica AJ, Atherton JC, Louw JA. Heterogeneity in the Helicobacter pylori vacA and cagA genes: association with gastroduodenal disease in South Africa? Gut. 1999;45:499–502.
Atherton JC, Peek Jr RM, Tham KT, Cover TL, Blaser MJ. Clinical and pathological importance of heterogeneity in vacA, the vacuolating cytotoxin gene of Helicobacter pylori. Gastroenterology. 1997;112:92–9.
Shimoyama T, Yoshimura T, Mikami T, Fukuda S, Crabtree JE, Munakata A. Evaluation of Helicobacter pylori vacA genotype in Japanese patients with gastric cancer. J Clin Pathol. 1998;51:299–301.
Yamaoka Y, Kodama T, Gutierrez O, Kim JG, Kashima K, Graham DY. Relationship between Helicobacter pylori iceA, cagA, and vacA status and clinical outcome: studies in four different countries. J Clin Microbiol. 1999;37:2274–9.
Basso D, Zambon CF, Letley DP, Stranges A, Marchet A, Rhead JL, et al. Clinical relevance of Helicobacter pylori cagA and vacA gene polymorphisms. Gastroenterology. 2008;135:91–9.
Ogiwara H, Graham DY, Yamaoka Y. vacA i-region subtyping. Gastroenterology. 2008;134:1267.
Yahiro K, Niidome T, Hatakeyama T, Aoyagi H, Kurazono H, Padilla PI, et al. Helicobacter pylori vacuolating cytotoxin binds to the 140-kDa protein in human gastric cancer cell lines, AZ-521 and AGS. Biochem Biophys Res Comm. 1997;238:629–32.
Seto K, Hayashi-Kuwabara Y, Yoneta T, Suda H, Tamaki H. Vacuolation induced by cytotoxin from Helicobacter pylori is mediated by the EGF receptor in HeLa cells. FEBS Lett. 1998;431:347–50.
Yahiro K, Wada A, Nakayama M, Kimura T, Ogushi K, Niidome T, et al. Protein-tyrosine phosphatase alpha, RPTP alpha, is a Helicobacter pylori VacA receptor. J Biol Chem. 2003;278:19183–9.
de Bernard M, Moschioni M, Papini E, Telford JL, Rappuoli R, Montecucco C. TPA and butyrate increase cell sensitivity to the vacuolating toxin of Helicobacter pylori. FEBS Lett. 1998;436:218–22.
Padilla PI, Wada A, Yahiro K, Kimura M, Niidome T, Aoyagi H, et al. Morphologic differentiation of HL-60 cells is associated with appearance of RPTPbeta and induction of Helicobacter pylori VacA sensitivity. J Bio Chem. 2000;275:15200–6.
McClain MS, Schraw W, Ricci V, Boquet P, Cover TL. Acid activation of Helicobacter pylori vacuolating cytotoxin (VacA) results in toxin internalization by eukaryotic cells. Mol Microbiol. 2000;37:433–42.
Fujikawa A, Shirasaka D, Yamamoto S, Ota H, Yahiro K, Fukada M, et al. Mice deficient in protein tyrosine phosphatase receptor type Z are resistant to gastric ulcer induction by VacA of Helicobacter pylori. Nat Genet. 2003;33:375–81.
Utt M, Danielsson B, Wadstrom T. Helicobacter pylori vacuolating cytotoxin binding to a putative cell surface receptor, heparan sulfate, studied by surface plasmon resonance. FEMS Immunol Med Microbiol. 2001;30:109–13.
Hennig EE, Godlewski MM, Butruk E, Ostrowski J. Helicobacter pylori VacA cytotoxin interacts with fibronectin and alters HeLa cell adhesion and cytoskeletal organization in vitro. FEMS Immunol Med Microbiol. 2005;44:143–50.
Gupta VR, Patel HK, Kostolansky SS, Ballivian RA, Eichberg J, Blanke SR. Sphingomyelin functions as a novel receptor for Helicobacter pylori VacA. PLoS Pathog. 2008;4, e1000073.
Sewald X, Gebert-Vogl B, Prassl S, Barwig I, Weiss E, Fabbri M, et al. Integrin subunit CD18 is the T-lymphocyte receptor for the Helicobacter pylori vacuolating cytotoxin. Cell Host Microbe. 2008;3:20–9.
Sewald X, Jimenez-Soto L, Haas R. PKC-dependent endocytosis of the Helicobacter pylori vacuolating cytotoxin in primary T lymphocytes. Cell Microbiol. 2011;13:482–96.
Schraw W, Li Y, McClain MS, van der Goot FG, Cover TL. Association of Helicobacter pylori vacuolating toxin (VacA) with lipid rafts. J Biol Chem. 2002;277:34642–50.
Nakayama M, Hisatsune J, Yamasaki E, Nishi Y, Wada A, Kurazono H, et al. Clustering of Helicobacter pylori VacA in lipid rafts, mediated by its receptor, receptor-like protein tyrosine phosphatase beta, is required for intoxication in AZ-521 cells. Infect Immun. 2006;74:6571–80.
Gauthier NC, Monzo P, Kaddai V, Doye A, Ricci V, Boquet P. Helicobacter pylori VacA cytotoxin: a probe for a clathrin-independent and Cdc42-dependent pinocytic pathway routed to late endosomes. Mol Biol Cell. 2005;16:4852–66.
Gupta VR, Wilson BA, Blanke SR. Sphingomyelin is important for the cellular entry and intracellular localization of Helicobacter pylori VacA. Cell Microbiol. 2010;12:1517–33.
Gauthier NC, Monzo P, Gonzalez T, Doye A, Oldani A, Gounon P, et al. Early endosomes associated with dynamic F-actin structures are required for late trafficking of H. pylori VacA toxin. J Cell Biol. 2007;177:343–54.
Li Y, Wandinger-Ness A, Goldenring JR, Cover TL. Clustering and redistribution of late endocytic compartments in response to Helicobacter pylori vacuolating toxin. Mol Biol Cell. 2004;15:1946–59.
Molinari M, Galli C, Norais N, Telford JL, Rappuoli R, Luzio JP, et al. Vacuoles induced by Helicobacter pylori toxin contain both late endosomal and lysosomal markers. J Biol Chem. 1997;272:25339–44.
Papini E, de Bernard M, Milia E, Bugnoli M, Zerial M, Rappuoli R, et al. Cellular vacuoles induced by Helicobacter pylori originate from late endosomal compartments. Proc Natl Acad Sci USA. 1994;91:9720–4.
Ikonomov OC, Sbrissa D, Yoshimori T, Cover TL, Shisheva A. PIKfyve Kinase and SKD1 AAA ATPase define distinct endocytic compartments. Only PIKfyve expression inhibits the cell-vacoulating activity of Helicobacter pylori VacA toxin. J Biol Chem. 2002;277:46785–90.
Suzuki J, Ohnsihi H, Shibata H, Wada A, Hirayama T, Iiri T, et al. Dynamin is involved in human epithelial cell vacuolation caused by the Helicobacter pylori-produced cytotoxin VacA. J Clin Invest. 2001;107:363–70.
Hotchin NA, Cover TL, Akhtar N. Cell vacuolation induced by the VacA cytotoxin of Helicobacter pylori is regulated by the Rac1 GTPase. J Biol Chem. 2000;275:14009–12.
Suzuki J, Ohnishi H, Wada A, Hirayama T, Ohno H, Ueda N, et al. Involvement of syntaxin 7 in human gastric epithelial cell vacuolation induced by the Helicobacter pylori-produced cytotoxin VacA. J Biol Chem. 2003;278:25585–90.
Papini E, Bugnoli M, de Bernard M, Figura N, Rappuoli R, Montecucco C. Bafilomycin A1 inhibits Helicobacter pylori-induced vacuolization of HeLa cells. Mol Microbiol. 1993;7:323–7.
Papini E, Gottardi E, Satin B, de Bernard M, Massari P, Telford J, et al. The vacuolar ATPase proton pump is present on intracellular vacuoles induced by Helicobacter pylori. J Med Microbiol. 1996;45:84–9.
Terebiznik MR, Raju D, Vazquez CL, Torbricki K, Kulkarni R, Blanke SR, et al. Effect of Helicobacter pylori’s vacuolating cytotoxin on the autophagy pathway in gastric epithelial cells. Autophagy. 2009;5:370–9.
Raju D, Jones NL. Methods to monitor autophagy in H. pylori vacuolating cytotoxin A (VacA)-treated cells. Autophagy. 2010;6:138–43.
Raju D, Hussey S, Ang M, Terebiznik MR, Sibony M, Galindo-Mata E, et al. Vacuolating cytotoxin and variants in Atg16L1 that disrupt autophagy promote Helicobacter pylori infection in humans. Gastroenterology. 2012;142:1160–71.
Tang B, Li N, Gu J, Zhuang Y, Li Q, Wang HG, et al. Compromised autophagy by MIR30B benefits the intracellular survival of Helicobacter pylori. Autophagy. 2012;8:1045–57.
Kuck D, Kolmerer B, Iking-Konert C, Krammer PH, Stremmel W, Rudi J. Vacuolating cytotoxin of Helicobacter pylori induces apoptosis in the human gastric epithelial cell line AGS. Infect Immun. 2001;69:5080–7.
Galmiche A, Rassow J. Targeting of Helicobacter pylori VacA to mitochondria. Gut microbes. 2010;1:392–5.
Domanska G, Motz C, Meinecke M, Harsman A, Papatheodorou P, Reljic B, et al. Helicobacter pylori VacA toxin/subunit p34: targeting of an anion channel to the inner mitochondrial membrane. PLoS Pathog. 2010:6:e1000878.
Willhite DC, Blanke SR. Helicobacter pylori vacuolating cytotoxin enters cells, localizes to the mitochondria, and induces mitochondrial membrane permeability changes correlated to toxin channel activity. Cell Microbiol. 2004;6:143–54.
Foo JH, Culvenor JG, Ferrero RL, Kwok T, Lithgow T, Gabriel K. Both the p33 and p55 subunits of the Helicobacter pylori VacA toxin are targeted to mammalian mitochondria. J Mol Biol. 2010;401:792–8.
Kim JM, Kim JS, Lee JY, Sim YS, Kim YJ, Oh YK, et al. Dual effects of Helicobacter pylori vacuolating cytotoxin on human eosinophil apoptosis in early and late periods of stimulation. Eur J Immunol. 2010;40:1651–62.
Lan CH, Sheng JQ, Fang DC, Meng QZ, Fan LL, Huang ZR. Involvement of VDAC1 and Bcl-2 family of proteins in VacA-induced cytochrome c release and apoptosis of gastric epithelial carcinoma cells. J Dig Dis. 2010;11:43–9.
Calore F, Genisset C, Casellato A, Rossato M, Codolo G, Esposti MD, et al. Endosome-mitochondria juxtaposition during apoptosis induced by H. pylori VacA. Cell Death Differ. 2010;17:1707–16.
Matsumoto A, Isomoto H, Nakayama M, Hisatsune J, Nishi Y, Nakashima Y, et al. Helicobacter pylori VacA reduces the cellular expression of STAT3 and pro-survival Bcl-2 family proteins, Bcl-2 and Bcl-XL, leading to apoptosis in gastric epithelial cells. Dig Dis Sci. 2011;56:999–1006.
Jain P, Luo ZQ, Blanke SR. Helicobacter pylori vacuolating cytotoxin A (VacA) engages the mitochondrial fission machinery to induce host cell death. Proc Natl Acad Sci USA. 2011;108:16032–7.
Akazawa Y, Isomoto H, Matsushima K, Kanda T, Minami H, Yamaghchi N, et al. Endoplasmic reticulum stress contributes to Helicobacter pylori VacA-induced apoptosis. PLoS One. 2013:8:e82322.
Radin JN, Gonzalez-Rivera C, Frick-Cheng AE, Sheng J, Gaddy JA, Rubin DH, et al. Role of connexin 43 in Helicobacter pylori VacA-induced cell death. Infect Immun. 2014;82:423–32.
Schmees C, Gerhard M, Treptau T, Voland P, Schwendy S, Rad R, et al. VacA-associated inhibition of T-cell function: reviewed and reconsidered. Helicobacter. 2006;11:144–6.
Molinari M, Salio M, Galli C, Norais N, Rappuoli R, Lanzavecchia A, et al. Selective inhibition of Ii-dependent antigen presentation by Helicobacter pylori toxin VacA. J Exp Med. 1998;187:135–40.
Gebert B, Fischer W, Weiss E, Hoffmann R, Haas R. Helicobacter pylori vacuolating cytotoxin inhibits T lymphocyte activation. Science. 2003;301:1099–102.
Boncristiano M, Paccani SR, Barone S, Ulivieri C, Patrussi L, Ilver D, et al. The Helicobacter pylori vacuolating toxin inhibits T cell activation by two independent mechanisms. J Exp Med. 2003;198:1887–97.
Kim JM, Kim JS, Yoo DY, Ko SH, Kim N, Kim H, et al. Stimulation of dendritic cells with Helicobacter pylori vacuolating cytotoxin negatively regulates their maturation via the restoration of E2F1. Clin Exp Immunol. 2011;166:34–45.
Geiszt M, Leto TL. The Nox family of NAD(P)H oxidases: host defense and beyond. J Biol Chem. 2004;2798:51715–8.
Yuan J, Li P, Tao J, Shi X, Hu B, Chen H, et al. H. pylori escape host immunoreaction through inhibiting ILK expression by VacA. Cell Mol Immunol. 2009;6:191–7.
Backert S, Tegtmeyer N. The versatility of the Helicobacter pylori vacuolating cytotoxin vacA in signal transduction and molecular crosstalk. Toxins. 2010;2:69–92.
Nakayama M, Hisatsune J, Yamasaki E, Isomoto H, Kurazono H, Hatakeyama M, et al. Helicobacter pylori VacA-induced inhibition of GSK3 through the PI3K/Akt signaling pathway. J Bio Chem. 2009;284:1612–9.
Hisatsune J, Yamasaki E, Nakayama M, Shirasaka D, Kurazono H, Katagata Y, et al. Helicobacter pylori VacA enhances prostaglandin E2 production through induction of cyclooxygenase 2 expression via a p38 mitogen-activated protein kinase/activating transcription factor 2 cascade in AZ-521 cells. Infect Immun. 2007;75:4472–81.
Takeshima E, Tomimori K, Takamatsu R, Ishikawa C, Kinjo F, Hirayama T, et al. Helicobacter pylori VacA activates NF-kappaB in T cells via the classical but not alternative pathway. Helicobacter. 2009;14:271–9.
Hisatsune J, Nakayama M, Isomoto H, Kurazono H, Mukaida N, Mukhopadhyay AK, et al. Molecular characterization of Helicobacter pylori VacA induction of IL-8 in U937 cells reveals a prominent role for p38MAPK in activating transcription factor-2, cAMP response element binding protein, and NF-kappaB activation. J Immunol. 2008;180:5017–27.
Acknowledgments
MN was supported by Takeda Science Foundation. TH and KY were supported by the Cooperative Research Grant of the Institute of Tropical Medicine, Nagasaki University, 2012 and 2014. JM was supported by the Intramural Research Program, National Institutes of Health, and National Heart, Lung, and Blood Institute. KY was also supported by Grants-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan and Improvement of Research Environment for Young Researchers from the Japan Science and Technology Agency.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Japan
About this chapter
Cite this chapter
Nakano, M., Hirayama, T., Moss, J., Yahiro, K. (2016). Helicobacter pylori VacA Exhibits Pleiotropic Actions in Host Cells. In: Suzuki, H., Warren, R., Marshall, B. (eds) Helicobacter pylori. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55705-0_4
Download citation
DOI: https://doi.org/10.1007/978-4-431-55705-0_4
Published:
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55704-3
Online ISBN: 978-4-431-55705-0
eBook Packages: MedicineMedicine (R0)