Abstract
Osteoarthritis (OA), the most common form of arthritis, is characterized by degradation and loss of articular cartilage, hypertrophic bone changes with osteophyte formation, subchondral bone remodeling, and inflammation of the synovial membrane. This disease can be triggered by external factors (e.g. trauma) and endogenous predisposing factors (e.g. age, genetics, high body mass index). It results in pain, and disability necessitating joint replacement at end-stage disease. Important advances have been made in understanding its pathological processes and promising disease-modifying OA drugs (DMOADs) are being developed that will slow the progression of the disease and improve current symptomatic treatment.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction to Osteoarthritis
Osteoarthritis (OA) is the most common form of arthritis, affecting 13.9 % of US adults aged 25 and older, totaling 26.9 million [1]. OA is characterized by degradation and loss of articular cartilage, hypertrophic bone changes with osteophyte formation (bony projections along the joint margin), subchondral bone remodeling, and inflammation of the synovial membrane. Other tissues of the joint including the muscles and ligaments are also altered during the OA process.
OA can be triggered by external factors such as trauma and endogenous predisposing factors including age, genetics, and high body mass index. It results in pain, reduced quality of life, and disability necessitating joint replacement in end-stage disease.
Important advances have been made in understanding its pathological processes, and promising new disease-modifying OA drugs (DMOADs) are being developed that will slow the progression of the disease and improve the current symptomatic treatment.
Pathophysiology of Osteoarthritis
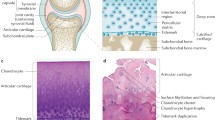
OA is a multifactorial disease resulting in the failure of the articular tissues to maintain a homeostatic balance between matrix synthesis and degradation. An initial phase of cartilage remodeling is characterized by edema, followed by degradation and loss of this tissue. These alterations are associated with synovial inflammation and subchondral bone remodeling (Fig. 1).
A model of global pathophysiology of knee osteoarthritis and of current multimodal management. Osteoarthritis can be triggered by external factors including trauma and endogenous predisposition factors such as age, genetics, and high body mass index (BMI). After an initial phase of cartilage edema, cartilage damage and loss occurs, which is associated with synovial inflammation, osteophyte formation, and subchondral bone remodeling. These structural changes generate pain, disability, and reduced quality of life. Current osteoarthritis management consists of education (on osteoarthritis, its progression, and its risk factors), weight loss (if necessary), prevention of injury, exercise, and pharmacological symptomatic treatment. Common treatments include acetaminophen (paracetamol), nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, intra-articular (IA) administration of hyaluronate and corticosteroids, and symptomatic slow-acting drugs (SYSADOA)
In cartilage, there is only one type of cell, the chondrocyte, which is responsible for the maintenance of this tissue’s extracellular matrix (ECM, see chapter “Overview” under part “Joints”). Early during the OA process, increased biomechanical stress and/or biochemical stimuli can activate the anabolic function of chondrocytes to repair early cartilage damage. Over time, this anabolic attempt fails and leads to an imbalance favoring degradation. This degradation will induce a vicious circle, in which the degradative fragments of ECM proteins (e.g., fibronectin and collagen) induce synovial membrane inflammation, which in turn will produce catabolic and inflammatory factors [2, 3], thus aggravating the OA process. Increasing evidence suggests that in OA there is a cross talk between the cartilage, synovial membrane, and subchondral bone, which sustains the catabolic process [4, 5]. Synovial inflammation, which is suggested to be secondary to the release of cartilage products into the synovial fluid, and subchondral bone remodeling by its release of soluble mediators, affects the cartilage by sustaining its degradation. The chondrocytes (autocrine pathway) and synoviocytes (see chapter “Overview” under part “Joints”) in the synovial membrane (paracrine pathway) release catabolic and proinflammatory substances. These include proteinases, e.g., matrix metalloproteinases (MMPs) and aggrecanases, and inflammatory cytokines, including interleukin (IL)-1β and tumor necrosis factor α (TNFα), which enhance the synthesis of proteinases and other catabolic factors to degrade the ECM of the articular tissues. Soon, these factors overwhelm endogenous inhibitors, such as tissue inhibitors of MMPs (TIMPs) and proinflammatory cytokine inhibitors including the IL-1β receptor antagonist (Fig. 2). Additionally, in OA, the loss of integrity of the osteochondral junction is associated with microcracks and the invasion of articular cartilage by vascular channels originating from the subchondral bone, supporting the molecular cross talk between the subchondral bone and the cartilage. Continued ECM degradation in the articular tissues results, preventing the cartilage from withstanding normal mechanical factors.
A model of cross talk between cartilage, synovial membrane, and subchondral bone leading to an imbalance favoring articular tissue degradation in knee osteoarthritis. Excessive production of proteases such as matrix metalloproteinases (MMPs) and aggrecanases, nitric oxide (NO), and inflammatory cytokines, such as interleukin-1β (IL-1β) and tumor necrosis factor α (TNFα) by the chondrocyte contributes to the degradation of articular tissue including the cartilage. This induces a vicious circle in which the cartilage fragments activate synoviocytes (see chapter “Overview” under part “Joints”), resulting in enhanced cartilage degradation and synovial inflammation. The attempt to repair, which could occur via growth factors such as bone morphogenetic proteins (BMPs) and transforming growth factor β (TGF-β), fails to achieve a complete repair of the extracellular matrix. Disease-modifying osteoarthritis drugs, such as inhibitors of MMPs and aggrecanases, anti-cytokine therapy, anti-bone remodeling, anti-nuclear factor-κB (NF-κB), and anti-mitogen-activated protein kinase (MAPK), have been developed, which aim to inhibit these factors and pathways. BML bone marrow lesion, IGF-1 insulin-like growth factor 1, IL-1Ra interleukin-1β receptor antagonist, TIMPs tissue inhibitors of metalloproteinases
Osteoarthritis Management
A multimodal approach combining non-pharmacological and pharmacological treatment (Fig. 1) [6] is at present the best option for OA management. However, current options are symptomatic treatments, which mostly aim at reducing joint pain. They are classified into rapid- or slow-acting symptomatic agents, and some of the slow-acting symptomatic drugs may contribute to slow the natural progression of joint structural damage. When combined approaches are unsuccessful, surgical treatments may be considered.
Non-pharmacological Treatment
The combination of education, improvement of muscle strength, and weight loss (if overweight) are reported to be joint protective and recommended [7], as are orthotic (joint-stabilizing) devices and prevention of injury.
Pharmacological Treatment: Rapid-Acting Symptomatic Agents
The rapid-acting symptomatic treatments for OA consist mainly of analgesics and nonsteroidal anti-inflammatory drugs (NSAIDs).
Acetaminophen (paracetamol) remains the first-line therapeutic agent for OA [6] because of its low cost, efficacy, and safety profile. Opioids have become more widely prescribed (often in combination with acetaminophen), especially for OA patients who experience lack of efficacy, contraindications, or intolerance to NSAIDs [6] and those who cannot undergo total joint arthroplasty because of comorbidities contraindicating surgery and anesthesia [7]. However, opioids show several, sometimes severe, adverse events, resulting from binding of opioids to δ, κ, and μ receptors that also cause analgesia, including sedation, vomiting, and respiratory depression. Another analgesic, duloxetine, may improve knee pain as well as function [8]. Duloxetine is a selective serotonin and norepinephrine reuptake inhibitor. These neurotransmitters are involved in the mediation of endogenous descending inhibitory pain pathways and central sensitization; in chronic pain states, their inhibitory effect is reduced or lost and duloxetine increases their availability and activity [9]. The main adverse events include nausea, constipation, and hyperhidrosis (increased sweating).
A second class of rapid symptomatic treatments that aim to block or reduce joint inflammation is nonselective NSAIDs (such as diclofenac) and cyclooxygenase-2 (COX-2) inhibitors, also named coxibs (such as celecoxib). These are recommended for patients who are unresponsive to acetaminophen, preferentially during inflammatory flares [6]. The use of NSAIDs is limited by gastrointestinal, renal, and cardiovascular side effects, which increase with age due to comorbidities. Coxibs demonstrate fewer gastrointestinal complications than nonselective NSAIDs but pose a potential cardiovascular risk [10]. Coxibs inhibit prostacyclin production (by COX-2), but do not inhibit thromboxane A2 release (from platelets, formed by COX-1). This potentially explains the coxib-related cardiovascular risk as such an imbalance could create continued thromboxane A2 production, thus increasing the risk of thrombosis. Another explanation could be that some coxibs have been found to increase blood pressure. NSAIDs can be used orally or topically with similar efficacy [11]; however, topical application shows fewer gastrointestinal complications but possible local skin reactions.
Corticosteroids are potent anti-inflammatory drugs that inhibit, among other factors, phospholipase A2, reducing the release of proinflammatory phospholipids. Intra-articular corticosteroid injection is recommended for OA inflammatory flares [6].
Hyaluronic acid is a glycosaminoglycan component of ECM and synovial fluid. It is involved in the maintenance of joint homeostasis and its concentration is reduced in OA patients. Intra-articular hyaluronic acid injection (viscosupplementation) is recommended for knee OA patients with an inadequate response to initial therapy [7], despite possible induced transient pain and swelling at the injection site [12]. Compared with intra-articular corticosteroids, viscosupplementation has a delayed but prolonged effect [12].
Pharmacological Treatment: Slow-Acting Symptomatic Drugs
Among the symptomatic slow-acting drugs for OA are glucosamine and chondroitin sulfate, which demonstrate a pain relief effect. Glucosamine sulfate is a substrate for the formation of glycosaminoglycans and shows a protective structural effect [13]. Chondroitin sulfate, a sulfated glycosaminoglycan, improves joint swelling and delays disease progression [13, 14].
Diacerein, an inhibitor of IL-1β and some proteases, is effective in knee [15] and hip OA [16]. Diarrhea is the most frequent adverse event, which likely occurs due to prostaglandin synthesis induced by rhein, the active metabolite of diacerein, leading to an increase in gut motility.
Treatment with avocado-soybean unsaponifiables reduces pain in knee and hip OA persistently, and the effect is prolonged even after treatment discontinuation [17, 18]. Inhibition of IL-1β and MMPs has been proposed as potential mechanisms of action.
Disease-Modifying Osteoarthritis Drugs
Currently, several classes of DMOADs are in development or tested in clinical trials (Fig. 2).
Targeting Cartilage Catabolism and Anabolism
MMP inhibitors aim to block ECM degradation. One such drug, doxycycline, showed only a minimal structural benefit and no effect on pain in a clinical trial [19]. An inhibitor of inducible NO synthase (cindunistat) revealed a reduction in joint space narrowing in mild OA in the first year [20]. Finally, intra-articular injection of growth factors such as bone morphogenetic protein 7 (BMP7) aims to repair OA cartilage.
Targeting Synovial Inflammation by Anti-cytokine Therapy
Blockade of inflammatory cytokines focuses on IL-1β and TNFα. Other potential targets include IL-6, nuclear factor-κB (NF-κB), and mitogen-activated protein kinase (MAPK), as they are part of the inflammation cascade in OA. Intra-articular administration of the IL-1β receptor antagonist anakinra shows controversial results with regard to symptoms [21], probably due to the short half-life of the drug and the protocol used for the clinical studies so far. Moreover, two antibodies against TNFα (adalimumab, infliximab) were shown to relieve symptoms of hand [22] and knee OA [23], but the results are still controversial [24].
Targeting Subchondral Bone Remodeling
Strontium ranelate inhibits bone resorption in subchondral bone [25]. This results from decreased differentiation and resorptive activity of osteoclasts and increased osteoclast apoptosis [26]. Strontium ranelate reduces the progression of spinal [27] and knee OA, as assessed in a Phase III trial by both X-rays [28] and MRI [29].
Risedronate, a bisphosphonate with anti-resorptive properties, preserves the structural integrity of the subchondral bone [30], but in a Phase III clinical trial, no significant effect was found on the Western Ontario and McMaster Universities Arthritis Index (WOMAC) or radiographic progression in knee OA [31].
In vitro, calcitonin reduces collagen degradation by inhibiting the expression and activity of MMPs in chondrocytes [32]. Oral and nasal applications of this thyroid hormone involved in calcium homeostasis are currently being tested [33]. Recently, a Phase III clinical trial was terminated early, probably due to an imbalance in prostate cancer events in male subjects [34].
Vitamin D supplementation in one study did not show any symptom or DMOAD benefits [35]. However, another clinical trial evaluating whether vitamin D supplementation can slow knee OA progression is ongoing [36].
A Phase III study evaluating the recombinant human FGF-18 in patients with knee OA is also currently underway [37].
Perspectives
OA management is based on a wide spectrum of therapeutic options to relieve pain and to try to delay progression. The focus is now on the development of DMOADs that could be associated with conventional therapy to provide a more effective treatment, which remains a huge unmet medical need worldwide given that OA prevalence is likely to increase with the aging population.
References
Lawrence RC, Felson DT, Helmick CG, Arnold LM, Choi H, Deyo RA, Gabriel S, Hirsch R, Hochberg MC, Hunder GG, Jordan JM, Katz JN, Kremers HM, Wolfe F (2008) Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part II. Arthritis Rheum 58:26–35
Martel-Pelletier J, Lajeunesse D, Pelletier JP (2005) Etiopathogenesis of osteoarthritis. In: Koopman WJ, Moreland LW (eds) Arthritis & allied conditions a textbook of rheumatology, 15th edn. Lippincott, Williams & Wilkins, Baltimore, pp 2199–2226
Martel-Pelletier J, Boileau C, Pelletier JP, Roughley P (2008) Cartilage in normal and osteoarthritis conditions. In: Pap T (ed) Best practice & research clinical rheumatology, vol 22. Rapid Medical Media, East Sussex, pp 351–384
Martel-Pelletier J, Lajeunesse D, Pelletier JP (2007) Subchondral bone and osteoarthritis progression: a very significant role. In: Buckwalter JA, Lotz M, Stoltz JF (eds) Osteoarthritis, inflammation and degradation: a continuum, 1st edn. IOS Press, Amsterdam, pp 206–218
Martel-Pelletier J, Pelletier JP (2010) Is osteoarthritis a disease involving only cartilage or other articular tissues? Eklem Hastalik Cerrahisi 21:2–14
Zhang W, Moskowitz RW, Nuki G, Abramson S, Altman RD, Arden N, Bierma-Zeinstra S, Brandt KD, Croft P, Doherty M, Dougados M, Hochberg M, Hunter DJ, Kwoh K, Lohmander LS, Tugwell P (2008) OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines. Osteoarthritis Cartilage 16:137–162
Hochberg MC, Altman RD, April KT, Benkhalti M, Guyatt G, McGowan J, Towheed T, Welch V, Wells G, Tugwell P (2012) American College of Rheumatology 2012 recommendations for the use of nonpharmacologic and pharmacologic therapies in osteoarthritis of the hand, hip, and knee. Arthritis Care Res (Hoboken) 64:455–474
Hochberg MC, Wohlreich M, Gaynor P, Hanna S, Risser R (2012) Clinically relevant outcomes based on analysis of pooled data from 2 trials of duloxetine in patients with knee osteoarthritis. J Rheumatol 39:352–358
Skljarevski V, Zhang S, Iyengar S, D’Souza D, Alaka K, Chappell A, Wernicke J (2011) Efficacy of duloxetine in patients with chronic pain conditions. Curr Drug Ther 6:296–303
Trelle S, Reichenbach S, Wandel S, Hildebrand P, Tschannen B, Villiger PM, Egger M, Juni P (2011) Cardiovascular safety of non-steroidal anti-inflammatory drugs: network meta-analysis. BMJ 342:c7086
Underwood M, Ashby D, Cross P, Hennessy E, Letley L, Martin J, Mt-Isa S, Parsons S, Vickers M, Whyte K (2008) Advice to use topical or oral ibuprofen for chronic knee pain in older people: randomised controlled trial and patient preference study. BMJ 336:138–142
Bellamy N, Campbell J, Robinson V, Gee T, Bourne R, Wells G (2005) Viscosupplementation for the treatment of osteoarthritis of the knee. Cochrane Database Syst Rev (2):CD005321
Lee YH, Woo JH, Choi SJ, Ji JD, Song GG (2010) Effect of glucosamine or chondroitin sulfate on the osteoarthritis progression: a meta-analysis. Rheumatol Int 30:357–363
Wildi LM, Raynauld JP, Martel-Pelletier J, Beaulieu A, Bessette L, Morin F, Abram F, Dorais M, Pelletier JP (2011) Chondroitin sulphate reduces both cartilage volume loss and bone marrow lesions in knee osteoarthritis patients starting as early as 6 months after initiation of therapy: a randomised, double-blind, placebo-controlled pilot study using MRI. Ann Rheum Dis 70:982–989
Pelletier JP, Yaron M, Haraoui B, Cohen P, Nahir MA, Choquette D, Wigler I, Rosner IA, Beaulieu AD (2000) Efficacy and safety of diacerein in osteoarthritis of the knee: a double-blind, placebo-controlled trial. The Diacerein Study Group. Arthritis Rheum 43:2339–2348
Dougados M, Nguyen M, Berdah L, Mazieres B, Vignon E, Lequesne M, ECHODIAH Investigators Study Group (2001) Evaluation of the structure-modifying effects of diacerein in hip osteoarthritis: ECHODIAH, a three-year, placebo-controlled trial. Evaluation of the Chondromodulating Effect of Diacerein in OA of the Hip. Arthritis Rheum 44:2539–2547
Maheu E, Mazieres B, Valat JP, Loyau G, Le Loet X, Bourgeois P, Grouin JM, Rozenberg S (1998) Symptomatic efficacy of avocado/soybean unsaponifiables in the treatment of osteoarthritis of the knee and hip: a prospective, randomized, double-blind, placebo-controlled, multicenter clinical trial with a six-month treatment period and a two-month followup demonstrating a persistent effect. Arthritis Rheum 41:81–91
Maheu E, Cadet C, Marty M, Moyse D, Kerloch I, Coste P, Dougados M, Mazieres B, Spector TD, Halhol H, Grouin JM, Lequesne M (2014) Randomised, controlled trial of avocado-soybean unsaponifiable (Piascledine) effect on structure modification in hip osteoarthritis: the ERADIAS study. Ann Rheum Dis 73:376–384
Nuesch E, Rutjes AW, Trelle S, Reichenbach S, Juni P (2009) Doxycycline for osteoarthritis of the knee or hip. Cochrane Database Syst Rev (4):CD007323
Hellio le Graverand MP, Clemmer RS, Redifer P, Brunell RM, Hayes CW, Brandt KD, Abramson SB, Manning PT, Miller CG, Vignon E (2013) A 2-year randomised, double-blind, placebo-controlled, multicentre study of oral selective iNOS inhibitor, cindunistat (SD-6010), in patients with symptomatic osteoarthritis of the knee. Ann Rheum Dis 72:187–195
Chevalier X, Goupille P, Beaulieu AD, Burch FX, Bensen WG, Conrozier T, Loeuille D, Kivitz AJ, Silver D, Appleton BE (2009) Intraarticular injection of anakinra in osteoarthritis of the knee: a multicenter, randomized, double-blind, placebo-controlled study. Arthritis Rheum 61:344–352
Fioravanti A, Fabbroni M, Cerase A, Galeazzi M (2009) Treatment of erosive osteoarthritis of the hands by intra-articular infliximab injections: a pilot study. Rheumatol Int 29:961–965
Maksymowych WP, Russell AS, Chiu P, Yan A, Jones N, Clare T, Lambert RG (2012) Targeting tumour necrosis factor alleviates signs and symptoms of inflammatory osteoarthritis of the knee. Arthritis Res Ther 14:R206
Verbruggen G, Wittoek R, Vander Cruyssen B, Elewaut D (2012) Tumour necrosis factor blockade for the treatment of erosive osteoarthritis of the interphalangeal finger joints: a double blind, randomised trial on structure modification. Ann Rheum Dis 71:891–898
Tat SK, Pelletier JP, Mineau F, Caron J, Martel-Pelletier J (2011) Strontium ranelate inhibits key factors affecting bone remodeling in human osteoarthritic subchondral bone osteoblasts. Bone 49:559–567
Martel-Pelletier J, Wildi LM, Pelletier JP (2012) Future therapeutics for osteoarthritis. Bone 51:297–311
Bruyere O, Delferriere D, Roux C, Wark JD, Spector T, Devogelaer JP, Brixen K, Adami S, Fechtenbaum J, Kolta S, Reginster JY (2008) Effects of strontium ranelate on spinal osteoarthritis progression. Ann Rheum Dis 67:335–339
Reginster JY, Badurski J, Bellamy N, Bensen W, Chapurlat R, Chevalier X, Christiansen C, Genant H, Navarro F, Nasonov E, Sambrook PN, Spector TD, Cooper C (2013) Efficacy and safety of strontium ranelate in the treatment of knee osteoarthritis: results of a double-blind, randomised placebo-controlled trial. Ann Rheum Dis 72:179–186
Pelletier J-P, Roubille C, Raynauld JP, Abram F, Dorais M, Delorme P, Martel-Pelletier J (2013) Disease modifying effect of strontium ranelate in the Phase III knee osteoarthritis study SEKOIA using quantitative magnetic resonance imaging: reduction in bone marrow lesions protects against cartilage loss. Ann Rheum Dis. doi: 10.1136/annrheumdis-2013-203989
Buckland-Wright JC, Messent EA, Bingham CO 3rd, Ward RJ, Tonkin C (2007) A 2 yr longitudinal radiographic study examining the effect of a bisphosphonate (risedronate) upon subchondral bone loss in osteoarthritic knee patients. Rheumatology (Oxford) 46:257–264
Bingham CO 3rd, Buckland-Wright JC, Garnero P, Cohen SB, Dougados M, Adami S, Clauw DJ, Spector TD, Pelletier JP, Raynauld JP, Strand V, Simon LS, Meyer JM, Cline GA, Beary JF (2006) Risedronate decreases biochemical markers of cartilage degradation but does not decrease symptoms or slow radiographic progression in patients with medial compartment osteoarthritis of the knee: results of the two-year multinational knee osteoarthritis structural arthritis study. Arthritis Rheum 54:3494–3507
Sondergaard BC, Wulf H, Henriksen K, Schaller S, Oestergaard S, Qvist P, Tanko LB, Bagger YZ, Christiansen C, Karsdal MA (2006) Calcitonin directly attenuates collagen type II degradation by inhibition of matrix metalloproteinase expression and activity in articular chondrocytes. Osteoarthritis Cartilage 14:759–768
Esenyel M, Icagasioglu A, Esenyel CZ (2013) Effects of calcitonin on knee osteoarthritis and quality of life. Rheumatol Int 33:423–427
Nordic Bioscience A/S; Novartis. Efficacy and safety of oral salmon calcitonin in patients with knee osteoarthritis (OA 2 Study). In: ClinicalTrials.gov [Internet]. Bethesda (MD): National Library of Medicine (US). 2000- [cited 2014 Mar 5]. Available from http://clinicaltrials.gov/show/NCT00704847NLMIdentifier:NCT00704847
McAlindon T, LaValley M, Schneider E, Nuite M, Lee JY, Price LL, Lo G, Dawson-Hughes B (2013) Effect of vitamin D supplementation on progression of knee pain and cartilage volume loss in patients with symptomatic osteoarthritis: a randomized controlled trial. JAMA 309:155–162
Cao Y, Jones G, Cicuttini F, Winzenberg T, Wluka A, Sharman J, Nguo K, Ding C (2012) Vitamin D supplementation in the management of knee osteoarthritis: study protocol for a randomized controlled trial. Trials 13:131
EMD Serono; Nordic Bioscience Clinical Development AS, Herlev Denmark. A study to investigate the safety and effectiveness of different doses of sprifermin (AS902330) in patients with osteoarthritis of the knee (FORWARD). In: ClinicalTrials.gov [Internet]. Bethesda (MD): National Library of Medicine (US). 2000- [cited 2014 Mar 5]. Available from http://clinicaltrials.gov/show/NCT01919164NLMIdentifier:NCT01919164
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag Wien
About this chapter
Cite this chapter
Roubille, C., Martel-Pelletier, J., Pelletier, JP. (2014). Osteoarthritis. In: Lammert, E., Zeeb, M. (eds) Metabolism of Human Diseases. Springer, Vienna. https://doi.org/10.1007/978-3-7091-0715-7_18
Download citation
DOI: https://doi.org/10.1007/978-3-7091-0715-7_18
Published:
Publisher Name: Springer, Vienna
Print ISBN: 978-3-7091-0714-0
Online ISBN: 978-3-7091-0715-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)