Abstract
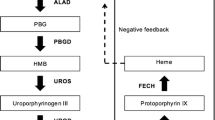
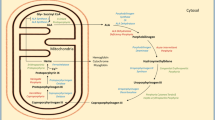
The porphyrias are a clinically, biochemically, and genetically heterogeneous group of metabolic diseases. They result from a predominantly hereditary, rarely acquired dysfunction of one of the eight enzymes along the heme biosynthetic pathway. Although the majority of the different variants of porphyria manifest with cutaneous symptoms, other forms exclusively show acute, potentially life-threatening neurovisceral porphyria attacks. In all porphyrias, inner organ complications can occur, mainly in the liver and kidneys. Therefore, affected patients should be cared for interdisciplinarily, if possible. This article provides an up-to-date overview of the clinic, diagnostics, and therapy of the various forms of porphyria.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Bickers DR, Frank J (2012) The porphyrias. In: Wolff K, Goldsmit LA, Katz SI et al (eds) Fitzpatrick’s dermatology in general medicine, 8th edn. McGraw-Hill, New York, pp 1538–1573
Biolcati G, Marchesini E, Sorge F et al (2015) Long-term observational study of afamelanotide in 115 patients with erythropoietic protoporphyria. Br J Dermatol 172:1601–1612
Fontanellas A, Ávila MA, Berraondo (2016) Emerging therapies for acute intermittent porphyria. Expert Rev Mol Med 18:e17. 1–13
Frank J, Poblete-Gutiérrez P (2010) Porphyria cutanea tarda – when skin meets liver. Best Pract Res Clin Gastroenterol 24:735–745
Gouya L, Puy H, Robreau AM et al (2002) The penetrance of dominant erythropoietic protoporphyria is modulated by expression of wildtype FECH. Nat Genet 30:27–28
Hift RJ, Thunell S, Brun A (2011) Drugs in porphyria: from observation to a modern algorithm-based system for the prediction of porphyrogenicity. Pharmacol Ther 132:158–169
Holme SA, Whatley SD, Roberts AG et al (2009) Seasonal palmar keratoderma in erythropoietic protoporphyria indicates autosomal recessive inheritance. J Invest Dermatol 129:599–605
James MF, Hift RJ (2000) Porphyrias. Br J Anaesth 85:143–153
Karim Z, Lyoumi S, Nicolas G et al (2015) Porphyrias: a 2015 update. Clin Res Hepatol Gastroenterol 39:412–425
Kunitz O, Frank J (2001) Anästhesiologisches Management bei Patienten mit akuten Porphyrien. Anaesthesist 50:957–969
Langendonk JG, Balwani M, Anderson KE et al (2015) Afamelanotide for erythropoietic protoporphyria. N Engl J Med 373:48–59
Ramanujam VM, Anderson KE (2015) Porphyria diagnostics-Part 1: a brief overview of the porphyrias. Curr Protoc Hum Genet 86:17.20.1–17.20.26
van Serooskerken AM, Poblete-Gutiérrez P, Frank J (2010) The porphyrias: clinic, diagnostics, novel investigative tools and evolving molecular therapeutic strategies. Skin Pharmacol Physiol 23:18–28
Whatley SD, Badminton MN (2013) Role of genetic testing in the management of patients with inherited porphyria and their families. Ann Clin Biochem 50:204–216
First Describer
Barnes HD (1945) A note on porphyrinuria with a resumé of eleven South African cases. Clin Proc 4:269–287
Doss M, by Tiepermann R, Schneider J et al (1979) New type of hepatic porphyria with porphobilinogen synthase defect and intermittent acute clinical manifestation. Klin Wochenschr 57:1123–1127
Günther H (1911) Die Hämatoporphyrie. Dtsch Arch Klin Med 105:89–146
Ippen H (1977) Treatment of porphyria cutanea tarda by phlebotomy. Semin Hematol 14:253–259
Kosenow W, Treibs A (1953) Lichtüberempfindlichkeit und Porphyrinämie. Z Kinderkrankh 73:82–92
Magnus IA, Jarrett A, Pankered TAJ et al (1961) Erythropoietic protoporphyria: a new porphyria syndrome with solar urticaria due to protoporphyrinemia. Lancet 2:448–451
Pinol Aquade J, Herrero C, Almeida J et al (1969) A case of biochemically unclassifiable hepatic porphyria. Br J Dermatol 81:270–275
Poh-Fitzpatrick MB (1980) A plasma porphyrin fluorescence marker for variegate porphyria. Arch Dermatol 116:543–547
Simon N, Kocsis GY, Nagy GY et al (1967) Über das familiäre Vorkommen der Porphyria cutanea. Wissenschaftlicher Vortrag auf der Sitzung der Hamburger Dermatologischen Gesellschaft im Gedenken an Alfred Marchionini. 21. Mai 1966. Hamburg. Dermatol Wochenschr 153:452
Waldenström J (1937) Studien über Porphyrie. Acta Medica Scand Suppl 82:84–90
Watson CJ, Schwartz S, Schultze W et al (1949) Studies of coporphyrin III: idiopathic coporphyrinuria, a hitherto unrecognized form characterized by lack of symptoms in spite of the excretion of large amounts of coporphyrin. J Clin Invest 28:465–482
Whatley SD, Ducamp S, Gouya L et al (2008) C-terminal deletions in the ALAS2 gene lead to gain of function and cause X-linked dominant protoporphyria without anemia or iron overload. Am J Hum Genet 83:408–414
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Section Editor information
Rights and permissions
Copyright information
© 2022 Springer-Verlag GmbH Germany, part of Springer Nature
About this entry
Cite this entry
Frank, J. (2022). Porphyrias. In: Plewig, G., French, L., Ruzicka, T., Kaufmann, R., Hertl, M. (eds) Braun-Falco´s Dermatology. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-63709-8_94
Download citation
DOI: https://doi.org/10.1007/978-3-662-63709-8_94
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-63708-1
Online ISBN: 978-3-662-63709-8
eBook Packages: MedicineReference Module Medicine