Abstract
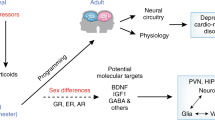
Major depressive disorder (MDD) is the fourth leading cause of disease burden worldwide, and women have approximately two times the risk of onset than men. Thus understanding the pathophysiology of MDD has widespread implications for attenuation and prevention of disease burden, particularly in women. MDD has been historically linked to adrenal and gonadal hormone dysregulation. This review argues the importance of applying prenatal stress models [i.e., fetal disruption of hypothalamic-pituitary-adrenal axis (HPA) circuitry] to understanding the fetal programming of sex differences in MDD. We review the literature on the important roles of HPA and HP-gonadal (HPG) hormones in understanding the comorbidity of MDD and endocrine dysregulation. We further review the literature on the fetal programming of MDD. Integrating these literatures and our current work, we argue the critical importance of investigating the disruption of the development of fetal HPA circuitry, during periods in which the sexual differentiation of the brain occurs, that we hypothesize place the male or female fetus at differential risks for MDD in adulthood. We believe that an understanding of the mechanisms involved in sex differences in the dysregulation of gonadal and adrenal hormones during fetal development in MDD will have etiologic implications and importance for the psychopharmacologic and hormonal treatment and prevention of MDD, particularly in women.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Major Depressive Disorder
- Cortisol Level
- Anterior Cingulate Cortex
- Corticotrophin Release Hormone
- Gonadal Hormone
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Clinical Evidence of Endocrine Disruption Related to Mood Disorders
Major depressive disorder (MDD) is the fourth leading cause of disease burden worldwide (Murray and Lopez 1997; Ustun et al. 2004), and the incidence of MDD in women is twice that of men (Kessler 2003; Kendler et al. 2006). Thus, understanding the pathophysiology of MDD has widespread implications for attenuation and prevention of disease burden (Ustun et al. 2004), particularly in women. Over 40 years of research implicates hormonal dysregulation in mood disorders, with the earliest reports citing elevated cortisol in patients with major depression (Board et al. 1956; Gibbons and McHugh 1962). While in subsequent years a number of hormonal systems have been demonstrated to be associated with depression [i.e., appetite-regulatory, thyroid, and growth hormones (Coplan et al. 2000; Brouwer et al. 2005; Kurt et al. 2007; Barim et al. 2009)], evidence overwhelmingly supports the involvement of the hypothalamic-pituitary-adrenal (HPA) and hypothalamic-pituitary-gonadal (HPG) axes (Plotsky et al. 1998; Young and Korszun 2002; Swaab et al. 2005) in the development of mood dysregulation. In particular, hormonal dysfunctions in women have been found to precede MDD onset (Nemeroff et al. 1984; Harlow et al. 2003), suggesting that hormonal abnormalities are important in female vulnerability to MDD. Despite the important findings stemming from this critical line of investigation, there is a dearth of literature on sex differences in HPA-/HPG-axis functioning. Further, a number of other confounds (illness state versus disorder trait, treatment and medication status, age, and single episode versus recurrent diagnosis of MDD) present challenges to elucidating the role of sex in the co-occurrence of hormonal dysregulation and mood disorders.
HPA Axis and MDD
There is a long history of work characterizing the HPA system as central to understanding the development of MDD (Nemeroff et al. 1984; Holsboer et al. 1987; Plotsky et al. 1998; Arborelius et al. 1999; Heim et al. 2002; Parker et al. 2003; Raison and Miller 2003; Barden 2004; Swaab et al. 2005; Antonijevic 2006). Depressive symptoms can occur in the context of either endogenously elevated cortisol (i.e., Cushing syndrome; Sonino et al. 1998) or exogenously administered corticosteroids (Kelly et al. 1980), and patients treated with corticosteroids can develop MDD (Ling et al. 1981). Animal and human studies demonstrated consistent HPA axis abnormalities associated with MDD, most notably elevated levels of cortisol in plasma, CSF, and 24-h urine, in addition to high CSF fluid corticotrophin releasing hormone (CRH) levels, blunted responses to CRH administration, and nonsupression of cortisol secretion upon dexamethasone suppression test (Carroll et al. 1976a, b, 1981; Jarrett et al. 1983; Nemeroff et al. 1984; Halbreich et al. 1985; Holsboer et al. 1985; Banki et al. 1987; Evans and Nemeroff 1987; Holsboer et al. 1987; Rubin et al. 1987; Nemeroff et al. 1991; Arborelius et al. 1999; Heim and Nemeroff 2001; Heim et al. 2001; Newport et al. 2003; Oquendo et al. 2003; Raison and Miller 2003; Barden 2004). HPA dysregulation has been related to, among other things, age (Nelson et al. 1984a, b; Bremmer et al. 2007), depression subtype (hypercortisolemia in atypical depression and normal cortisol levels in melancholia; Brouwer et al. 2005), and single versus recurrent episodes (Poor et al. 2004).
Several studies have examined the utility of HPA reactivity as an indicator of treatment response in MDD. For example, while the elevation in CRH has been shown to resolve with treatment (Nemeroff et al. 1991; De Bellis et al. 1993; Veith et al. 1993), some studies report an incomplete resolution to normal levels, suggesting that these HPA abnormalities may be part of the vulnerability to MDD (or a trait) and not only state-related. Although decreases following treatment in abnormally elevated pre-treatment cortisol levels have been widely reported (Gibbons and McHugh 1962; Carroll et al. 1976a, b), a recent meta-analysis found that cortisol levels did not change pre- versus post-treatment in over half of subjects with depression (McKay and Zakzanis 2010). An examination of subject characteristics related to changes in cortisol post-treatment revealed the greatest decreases in those with the melancholic subtype. Time of sample collection, inpatient versus outpatient setting, type of treatment or antidepressant, subject sex, and number of past episodes were not associated with cortisol changes following treatment, although the length of the current episode was negatively associated with change in cortisol levels (McKay and Zakzanis 2010). This finding supported the hypothesis that the nature of HPA axis dysregulation shifts dramatically from acute [overall hypersecretion of corticotrophin releasing hormone (CRH), adrenocorticotropin hormone (ACTH), and cortisol] to chronic (reduced ACTH and hypercortisolemia) phases of depression (Parker et al. 2003).
The issues of state versus trait (independent of treatment) and underlying vulnerability to relapse in depression have been examined sparingly, with findings initially pointing to hypercortisolemia as a state (not trait) feature of MDD. In remitted patients compared with controls, cortisol levels were reported to be similar (Trestman et al. 1993) or even decreased (Ahrens et al. 2008), although these studies were small (n/group ~20–30). However, a recent well-powered study examined morning and evening salivary cortisol levels in 308 controls, 579 individuals with remitted MDD, and 701 patients currently in an MDD episode (Vreeburg et al. 2009). Results showed that remitted and current MDD subjects demonstrated significantly higher awakening cortisol levels compared to controls, providing compelling evidence that elevated cortisol is not specific to current state but persists following recovery and may therefore be a trait characteristic (Vreeburg et al. 2009). Although findings held when adjusted for sex (57–71 % female, depending on group) and other demographic variables, specific sex differences were not explored. When tracked longitudinally, baseline cortisol and dexamethasone suppression test abnormalities also predicted vulnerability to relapse, necessity for continued medication to sustain remission, and remission rate following hospitalization in MDD (O’Toole et al. 1997; Zobel et al. 1999; Appelhof et al. 2006; Ising et al. 2007).
Further evidence for the role of the adrenal cortex is suggested by work on dehydroepiandrosterone sulfate (DHEA-S) and MDD. DHEA-S, which is produced by the adrenal gland, is considered a weak androgen and has been significantly associated with MDD, depending on age and sex (Orentreich et al. 1984; Schmidt et al. 2002), illness severity, medication status, and time of sampling. In unmedicated MDD patients, DHEA-S had anti-glucocorticoid action in the brain (Young et al. 2002; van Broekhoven and Verkes 2003). In fact, studies demonstrated lower depressive symptoms and better memory function with increased levels of DHEA-S (Wolkowitz et al. 1999; van Broekhoven and Verkes 2003). A high cortisol:DHEA-S ratio, which is a functional indicator of hypercortisolemia (Gallagher and Young 2002), was significantly associated with MDD, emphasizing anti-glucocorticoid DHEA-S action (Young et al. 2002; van Broekhoven and Verkes 2003).
Despite significant advances in understanding the comorbidity of major depression and HPA axis dysregulation as evidenced above, there is a paucity of data on sex differences in the comorbidity. This is striking for three reasons. First, as mentioned previously, there are well-documented sex differences in MDD incidence and prevalence (Kessler 2003; Kendler et al. 2006). Second, substantial data support sex differences in HPA-HPG axes functioning during stress in healthy control populations (Kudielka and Kirschbaum 2005; Goldstein et al. 2010; Andreano et al. 2011) and in MDD women (Holsen et al. 2011). Finally, as discussed below, there are significant interactions of the HPA axis with the HPG axis, which we know is different between the sexes.
Among the few investigations reporting significant sex differences in HPA axis functioning in MDD, the direction of effects is mixed. Men, but not women, with MDD demonstrate abnormal ACTH pulsatility (Young et al. 2007a). Additionally, elevated cortisol has been documented in depressed men versus depressed women (Bremmer et al. 2007) and versus non-depressed men (Hinkelmann et al. 2011), but also in depressed women versus depressed men (Poor et al. 2004) versus non-depressed women (Young and Altemus 2004; Chopra et al. 2009). These conflicting reports on sex differences in cortisol levels may be related to timing of cortisol assessment across studies and/or genetic factors. Recent data suggest an interaction between sex and adrenoreceptor gene polymorphisms in HPA hyperactivity using a dexamethasone/CRH test pre- and post-treatment (Haefner et al. 2008). Specifically, increased ACTH and cortisol responses were seen in males (but not females) homozygotic for the alpha(2)-adrenoreceptor (ADRA2A) gene and females (but not males) homozygotic for the beta(2)-adrenoreceptor (ADRB2) gene (Haefner et al. 2008). Collectively these findings offer initial evidence of sex differences in the role of HPA axis functioning in MDD pathophysiology.
Several reports have found no effect of sex on HPA dysfunction in MDD (Carroll et al. 1976a, b; Nelson et al. 1984a; Maes et al. 1987, 1989, 1994; Dahl et al. 1989; Deuschle et al. 1998; Brouwer et al. 2005; Rubin et al. 2006; Vreeburg et al. 2009). However, the majority of these studies cited above (including those reporting sex differences and those with null findings) did not initially design their studies to investigate sex differences but rather analyzed the data by sex post hoc. This approach is problematic, since potential confounding (uncontrolled in the initial designs) is typical. For example, the vast majority of studies of MDD oversample women (Maes et al. 1987; Brouwer et al. 2005; Rubin et al. 2006; Young et al. 2007a; Vreeburg et al. 2009; Hinkelmann et al. 2011). Some have matched on sex whereas some included women using oral contraceptives or estrogen-replacement therapy (Brouwer et al. 2005), which have been shown to affect plasma levels of cortisol (Kirschbaum et al. 1999). Further, only a few mention “matching for menstrual status” (Maes et al. 1987; Rubin et al. 2006), and those that do generally refer to including similar numbers of women who are pre- or post-menopausal rather than actually controlling for menstrual cycle phase (for example, conducting study visits only within certain phases such as early follicular or late luteal). These methodological confounds present significant challenges to understanding the inconsistencies in the literature on sex differences in HPA axis dysregulation and MDD comorbidity.
The importance of HPA axis abnormalities in MDD is underscored by human postmortem studies. One human postmortem study found a 25 % decrease in the density of glucocorticoid receptor (GR) mRNA in MDD compared with healthy brains in frontal cortex, dentate gyrus, and subiculum, suggesting a down-regulation of GRs affecting the negative feedback system of the HPA axis resulting in hypercortisolemia (Webster et al. 2002). CRH action on ACTH is potentiated by arginine vasopressin (AVP), which is co-expressed with CRH in some neurons of the paraventricular nucleus of the hypothalamus (PVN) and was enhanced in MDD (von Bardeleben et al. 1989; Muller and Holsboer 2006). A recent postmortem study reported increased AVP mRNA in the PVN and supraoptic nucleus in MDD, particularly with melancholic features (Meynen et al. 2006). This finding is consistent with an increased number of AVP-immunoreactive neurons in PVN (Purba et al. 1996), particularly those co-localizing with increased CRH in PVN in MDD (Raadsheer et al. 1994a, b). It is also consistent with studies of MDD reporting elevated AVP plasma levels (van Londen et al. 1997; van Amelsvoort et al. 2001; de Winter et al. 2003), positive correlations of plasma AVP with cortisol (De Bellis et al. 1994; Inder et al. 1997; de Winter et al. 2003), and increased ACTH and cortisol in MDD and controls with intravenous administration of AVP (Gispen-de Wied et al. 1992), which are findings that were not due to medication confounds (van Londen et al. 1997; van Amelsvoort et al. 2001; Meynen et al. 2006).
HPG Axis and MDD
The relationship between mood disturbances and gonadal hormones was initially recognized, in part, through developmental endocrine disorders such as polycystic ovarian syndrome (PCOS), which is associated with high levels of comorbid depression (Himelein and Thatcher 2006b). The mechanisms behind this comorbidity are not fully understood, as data do not support an association between depressive symptoms and androgen levels, infertility issues, or hirsutism (Keegan et al. 2003; Rasgon et al. 2003; McCook et al. 2005; Himelein and Thatcher 2006a). Further evidence is derived from the abundant literature relating women’s reproductive system to mood fluctuations and depression (Payne 2003; Spinelli 2005; Payne et al. 2009). For example, pubertal onset (Angold and Costello 2006), late luteal menstrual cycle phase (Steiner 1992), chronic use of oral contraceptives (Young et al. 2007b), the postpartum period (Bloch et al. 2000; Brummelte and Galea 2010), and postmenopause (Graziottin and Serafini 2009) are all associated with vulnerability to MDD. However, the establishment of this relationship in women has not been accompanied by parallel examination of possible hormonal deficits linked to mood dysregulation in men at similar ages.
Human studies of MDD patients have found deficits in gonadal function (Rubinow and Schmidt 1996; Harlow et al. 2003), e.g., androgens (Baischer et al. 1995; Rubinow and Schmidt 1996; Schweiger et al. 1999; Seidman et al. 2001; Weiner et al. 2004) and estradiol (Young et al. 2000), and pituitary function, i.e., low follicle stimulating hormone (FSH; Daly et al. 2003). Women with persistent MDD had two times the risk of earlier perimenopausal transition, and those with a lifetime history of MDD had higher FSH and lower estradiol levels, suggesting an early decline in ovarian function (Young et al. 2000; Harlow et al. 2003). Further reports suggested a relationship between depressive symptom severity and estradiol levels (Baischer et al. 1995) and that ovarian dysfunction preceded the onset of MDD (Harlow et al. 2003). Abnormalities in luteinizing hormone (LH) levels and pulsatility in women with MDD have been consistently documented (Young et al. 2000; Meller et al. 2001; Harlow et al. 2003). LH pulse frequency and testosterone secretion in males with MDD were also lower (Schweiger et al. 1999), although conflicting reports suggested relatively normal HPG axis functioning in MDD males (Rubin et al. 1989).
HPA-HPG Interactions
There is some evidence that inhibition of HPG activity by stress and other factors may be linked to HPA activity (Halbreich and Kahn 2001). CRH inhibits gonadotropin releasing hormone (GnRH) and gonadotropin secretion in model animal studies (Nikolarakis et al. 1986; Olster and Ferin 1987). In fact, the low levels of estradiol seen in MDD premenopausal women may lead to decreased inhibitory feedback of the HPA axis in the presence of increased HPA drive with unopposed progesterone. This may in turn account for elevated levels of cortisol in MDD women compared to MDD men or non-depressed women (Young and Altemus 2004). Although the mood disturbances in premenstrual syndrome do not reach the severity or duration of major depression, transient dysregulation of the HPA axis during the luteal phase has been noted in this population (Rabin et al. 1990; Roca et al. 2003), offering further support for the influence of gonadal steroid hormones on HPA functioning related to mood.
Further, in postmortem studies of MDD, CRH-producing neurons in PVN that co-localized with estrogen receptor alpha (ERα) were enhanced in MDD, again suggesting HPA-HPG interactions in MDD (Bao et al. 2005). In our recent functional imaging study in MDD women, gonadal hormone abnormalities (lower estradiol) were significantly associated with functional brain activity deficits in key regions in the stress response circuitry (e.g., amygdala and hippocampus; Holsen et al. 2011). We are currently testing the hypothesis that the vulnerability for these stress response circuitry deficits and endocrine abnormalities begins during fetal development.
Brain Circuitry Linking MDD, HPA and HPG
The comorbidity between depression and HPA-HPG-axis dysregulation is not surprising from a brain circuitry point of view, given that depression is a disorder that involves hypothalamic nuclei [such as paraventricular (PVN) and ventromedial (VMN)], central amygdala, hippocampus, subgenual anterior cingulate cortex (ACC), and medial and orbitofrontal cortex (mPFC OFC; Dougherty and Rauch 1997; Mayberg 1997; Drevets et al. 2002; Sheline et al. 2002; Rauch et al. 2003), regions that are dense in glucocorticoid and sex steroid hormone receptors (MacLusky et al. 1987; Clark et al. 1988; Handa et al. 1994; Kawata 1995; Tobet and Hanna 1997; Donahue et al. 2000; Östlund et al. 2003). The overlap between these circuitries has been historically noted from behavioral and endocrinological findings but, with the advent of magnetic resonance imaging (MRI) technology, there is a greater focus on the investigation of brain circuitry implicated in the regulation of mood and endocrine functioning. This technology allows for hypothesis-driven in vivo exploration of this shared circuitry.
HPA Axis Hormones Associated with Brain Activity
Over the past 5 years, there has been a rapid increase in studies examining the relationship between HPA hormones (more specifically endogenous and exogenous cortisol) and brain activity in subcortical and cortical stress response regions using a variety of functional MRI (fMRI) paradigms in healthy control subjects (generally comprising mixed-gender samples with age ranges between 18 and 35 years). Amygdala and hippocampal activity in response to stimuli of high negative emotionality was positively associated with pre- versus post-scan (Root et al. 2009) and diurnal amplitude (Cunningham-Bussel et al. 2009) salivary cortisol. This relationship between hyperactivation in the amygdala and increased cortisol is supported by additional evidence suggesting that, when categorized by level of endogenous cortisol, individuals with high cortisol demonstrate greater amygdala activity than those with low cortisol levels (van Stegeren et al. 2007, 2008), an effect that is blocked by administration of a noradrenergic antagonist. Cushing syndrome (CS), which is associated with chronic hypercortisolemia, also appears to be associated with hyperactivity in arousal regions. Adolescents with CS compared with age- and gender-matched controls demonstrated increased activation of the amygdala and hippocampus during successful encoding of emotional faces, despite similar memory performance (Maheu et al. 2008). Further, adults with CS showed hyperactivation in the anterior hippocampus, medial frontal gyrus, ACC, caudate, and superior parietal lobule during identification of emotional facial expressions. Accuracy in CS patients was lower and correlated with brain activity, suggesting these differences could be partially explained by compensatory recruitment of these regions (Langenecker et al. 2012). However, in general, these findings point to a pattern of significantly enhanced activation in the presence of heightened endogenous cortisol levels in healthy controls and CS patients.
In cortical stress response circuitry regions, however, somewhat contrasting results emerge. For example, one study reported a negative correlation between ventromedial prefrontal cortical activation to negative (versus neutral) stimuli and pre- versus post-scan cortisol levels (Root et al. 2009). Further, decreased activations in the ACC and OFC were observed in individuals who demonstrated a significant increase in cortisol levels (i.e., “responders”) during a psychosocial stress paradigm (negative feedback during arithmetic problems), as compared to cortisol non-responders (Pruessner et al. 2008). Interestingly, although several of these studies included sex as a covariate in the analyses, only one focused specifically on sex differences. They reported a lateralized pattern of activations in the frontal cortex in males [i.e., increased cerebral blood flow (CBF) in the right PFC and decreased in left OFC, which were associated with cortisol levels] and activations in the ventral striatum, putamen insula, and ACC (unrelated to cortisol level variation) in females (Wang et al. 2007). Taken together, these findings suggest potentially divergent roles of subcortical versus cortical arousal regions in response to stress and cortisol variation, which may be influenced by gonadal steroid hormones given substantial differences in activation patterns between men and women and the importance of HPA and HPG interactions.
Importantly, the literature on changes in endogenous cortisol levels associated with brain responses to emotional and stressful paradigms highlights the significant variability among even healthy individuals in the psychophysiological reaction to stress, as not all study subjects are ultimately classified as cortisol “responders” (Wust et al. 2000; Muehlhan et al. 2011). One methodological alternative to relying on natural variation in cortisol levels is to observe similar phenomena following administration of exogenous cortisol (i.e., hydrocortisone). In general, the amygdala and hippocampus appear to be most sensitive to hydrocortisone, demonstrating significant decreases in activation in comparison to placebo (Lovallo et al. 2010). Striking sex differences in the neural response to hydrocortisone (versus placebo) during fear conditioning have been observed, with increased activation in the ACC, OFC, and mPFC in response to the conditioned (versus unconditioned) stimulus in females and decreases in these same regions in males (Stark et al. 2006; Merz et al. 2010).
HPG Axis Hormones Associated with Brain Activity
Although studies on the HPA hormone-brain relationships occasionally report controlling for menstrual cycle phase in women (Stark et al. 2006), gonadal hormone variation is the primary focus of functional neuroimaging studies of HPG hormone effects on brain activity. A number of investigations have provided evidence of estradiol and progesterone influences on brain activity during cognitive paradigms, including executive functioning (Berman et al. 1997), language processing (Fernandez et al. 2003), and verbal memory (Craig et al. 2008; Konrad et al. 2008) among others (Dietrich et al. 2001; de Leeuw et al. 2006). Here we focus on emotional paradigms, given the role of emotion dysregulation in mood disorders. Activation in stress response circuitry regions has been shown to be modulated across menstrual cycle in healthy women in response to negative arousal images, with greater activation in the anterior hypothalamus, amygdala, hippocampus, ACC, and OFC during the early follicular phase compared with late follicular/midcycle (Goldstein et al. 2005). Further, in healthy women, hyperactivity of the amygdala and hippocampus was present during late luteal compared with early follicular menstrual cycle phase (Andreano and Cahill 2010), with estradiol being negatively associated with amygdala activation (Andreano and Cahill 2010). Direct comparisons between males and females were consistent with these patterns, with greater hyperactivity in men than in women during their late follicular/midcycle compared to when they were in early follicular (Goldstein et al. 2010). Results suggested gonadal hormonal modulation of subcortical arousal by prefrontal circuitry (Goldstein et al. 2005, 2010).
Using paradigms that examine inhibitory control during cognitive and emotional processing, inhibitory responses to negative (versus neutral) emotional stimuli targets during the luteal phase (versus follicular) are associated with greater activation in the medial OFC (Protopopescu et al. 2005), ACC, DLPFC, and putamen (Amin et al. 2006). In contrast, increased OFC activity during follicular rather than luteal phase was observed in response to male faces judged on sexual desirability (Rupp et al. 2009), which may suggest a significant shift in OFC processing and decision-making related to positive and negative stimuli across the menstrual cycle. However, a study utilizing a reward paradigm recently demonstrated greater follicular than luteal phase activation to anticipation of positive reward delivery in the OFC (Dreher et al. 2007). These discrepancies might be related to differences in menstrual phase definition, with follicular phase defined as days 4–8 (Dreher et al. 2007), 8–12 (Protopopescu et al. 2005), or 10–12 after the start of menstruation (Rupp et al. 2009), and luteal phase defined as 19–23 days following the start of menstruation (Rupp et al. 2009), 6–10 days post LH surge (Dreher et al. 2007), or 1–5 days before menses onset (Protopopescu et al. 2005). Although the healthy control women in these samples had regular cycles, this variation in phase definition across studies could have significant effects on estradiol and progesterone levels, leading to substantial differences reported in these studies in brain activity across the menstrual cycle.
Similar to literature (cited above) on exogenous HPA hormone administration and brain activity, a number of investigations have examined effects of exogenous gonadal hormone regulation of neural responses to emotional stimuli. Compared with placebo, progesterone administration (during early follicular phase when progesterone levels are naturally low) is related to increased amygdala reactivity to emotional face processing, increased amygdala-dorsal ACC connectivity, and decreased amygdala-fusiform gyrus connectivity (van Wingen et al. 2008b). Testosterone administration, contrastingly, increased hippocampus and inferior temporal gyrus activation during memory formation and retrieval of male faces in middle-aged women (van Wingen et al. 2008a). Compared with placebo, testosterone increased amygdala responsivity to levels equivalent to those observed in young women (van Wingen et al. 2009) and reduced functional connectivity between the amygdala and OFC (van Wingen et al. 2010). Thus, administration of exogenous gonadal hormones exerts significant influence on amygdala responsivity in general and coupling between the amygdala and other limbic and cortical regions during evaluation of emotionally salient cues.
Recent Findings in Mood Disorders
A few studies recently demonstrated compelling evidence of links between HPA-HPG hormone dysregulation and brain activity deficits in MDD. Hydrocortisone administration to currently depressed women resulted in increased hippocampal activation during encoding of neutral (versus negative or positive) words in comparison to healthy control women, a trend not observed during placebo (Abercrombie et al. 2011). Importantly, this relationship between exogenous cortisol administration and memory formation did not occur in depressed men, suggesting sex differences in the effect of cortisol on memory processing in depression (Abercrombie et al. 2011). Further, we showed that young women with MDD displayed hypoactivation in a number of regions involved in the stress response circuitry that were significantly associated with gonadal hormone deficits (Holsen et al. 2011), including decreased estradiol and increased progesterone levels in MDD women during late follicular/midcycle phase of the menstrual cycle. Finally, hypoactivation to positive stimuli in the nucleus accumbens and hyperactivations in the amygdala and lateral OFC in response to negative stimuli during the luteal phase (versus late follicular) were reported in women with premenstrual dysphoric disorder compared with healthy controls (Protopopescu et al. 2008b). Findings from these initial studies indicate a complex interaction between HPA (cortisol) and HPG (progesterone, estradiol) dysregulation and brain activation during cognitive and emotional processing (respectively) in women with mood disorders, providing support for mechanisms implicating neuroendocrine systems associated with sex differences in depression.
Sexual Dimorphisms in Shared Mood and Endocrine Circuitry
Extant literature suggests that the circuitry shared between mood regulation and endocrine functioning also includes highly sexually dimorphic regions and therefore may help us understand sex differences in MDD. In vivo imaging and postmortem studies have demonstrated sex differences in brain volumes (or nuclei) of regions associated with MDD. In women, relative to cerebrum size, findings support greater relative volumes of hippocampus (Filipek et al. 1994; Giedd et al. 1996; Murphy et al. 1996; Goldstein et al. 2001), ACC (Paus et al. 1996; Goldstein et al. 2001) and OFC (Goldstein et al. 2001). In men, there are greater volumes (relative to cerebrum size) of the amygdala (Giedd et al. 1996; Goldstein et al. 2001), hypothalamus (Swaab and Fliers 1985; Allen et al. 1989; Goldstein et al. 2001), and paracingulate gyrus (Paus et al. 1996; Goldstein et al. 2001). Thus women tend to have relatively larger volumes of hippocampus, OFC, and ACG, whereas men have relatively larger amygdala and hypothalamic volumes. Recent findings offer additional evidence that regional brain volumes in women vary across the menstrual cycle, with hippocampal gray matter volume increased and dorsal basal ganglia gray matter volume decreased during follicular rather than luteal phase (Protopopescu et al. 2008a). Further, estradiol, progesterone, and testosterone levels in young adults explained 13 %, 13 %, and 2 % in the variation of superior parietal gyrus, medial temporal pole, and inferior frontal gyrus gray matter volume, respectively (Witte et al. 2010), suggesting significant associations between gonadal hormone levels and neuroanatomic variation in humans.
One potential factor involved in human sexual dimorphisms may be the role of gonadal hormones on brain development, as seen in particular in model animal work by collaborators Tobet and Handa (McEwen 1983; Simerly et al. 1990; Tobet et al. 1993, 2009; O’Keefe et al. 1995; Park et al. 1996; Tobet and Hanna 1997; Gorski 2000; Chung et al. 2006). Our findings in humans indirectly suggested that this factor might also, in part, contribute to understanding human sexual dimorphisms in adulthood (Goldstein et al. 2001). In animals, nuclei of the corticomedial amygdala, PVN, VMN, hippocampus, OFC, and ACG express high concentrations of gonadal and/or adrenal hormone receptors compared with other brain regions (Handa et al. 1994; Pacak et al. 1995; Koob 1999; Solum and Handa 2002; Tobet 2002; Östlund et al. 2003; Lund et al. 2004, 2006; Suzuki and Handa 2004). These brain regions have been implicated in MDD and HPA function. Our hypotheses are in part based on the premise, supported by our work on sex differences in another disorder with fetal origins, schizophrenia (Goldstein et al. 2002), that normal sexual dimorphisms during fetal development in MDD may go awry in brain regions associated with MDD and HPA function and that mechanisms involved in understanding normal sexual dimorphisms, such as the roles of gonadal and adrenal hormones (in association with genes; Handa et al. 1994; Majdic and Tobet 2011), will contribute to understanding sex differences in MDD in adulthood.
Prenatal Stress Models of Understanding Sex Differences in MDD and Comorbid Endocrine Dysregulation
Preclinical and clinical studies have demonstrated lasting effects of prenatal adverse events on the HPA axis and noradrenergic stress systems (Takahashi et al. 1992; Weinstock et al. 1992; Vallee et al. 1997; Weinstock 1997). These include conditioned stress responses such as heightened glucocorticoid, norepinephrine, and autonomic response to novel stressors and altered dopaminergic, gamma aminobutyric acid (GABA)-ergic, and serotonergic function (Heim et al. 2000; Heim and Nemeroff 2001). Animal studies demonstrated the impact of prenatal stress on hypothalamic and hippocampal structure and function (Takahashi et al. 1992; Matsumoto and Arai 1997; Weinstock 1997), with lasting effects on the HPA axis in adult offspring by programming a “hyperactive” system that was vulnerable to adult depression, anxiety, and autonomic nervous system deficits among others (Weinstock et al. 1992; Henry et al. 1994; Barker 1995; Arborelius et al. 1999; Seckl 2001). Our current work has demonstrated that mid-to-late gestation is a particularly vulnerable time for the impact of prenatal events on sex-specific brain development (Tobet et al. 2009; Majdic and Tobet 2011) and development of the hormonal systems such as HPA (Celsi et al. 1998; Slotkin et al. 1998; Tronche et al. 1999; Sandau and Handa 2007; Zuloaga et al. 2011). Thus preclinical studies, including our own work, have demonstrated the vulnerability of the HPA system to adverse prenatal events with sex-specific effects on HPA function and affect.
Models for investigation of HPA compromise have included prenatal stress and infection during mid-to-late gestation that have demonstrated sex-specific effects in preclinical studies. From preclinical studies, sex effects (i.e., greater in females than males) include (1) greater glucocorticoid transfer across the placenta in female mice (Montano et al. 1993; Fameli et al. 1994); (2) greater immobility in standard tests associated with MDD phenotypic behavior (Alonso et al. 2000); (3) increased ACTH corticosterone and glucocorticoid receptor (GR) binding (Weinstock et al. 1992; McCormick et al. 1995; Regan et al. 2004); (4) increased corticosterone sensitivity (Rhodes and Rubin 1999); (5) greater susceptibility to changes following loss of GABAB receptor function (McClellan et al. 2010; Stratton et al. 2011); (6) greater susceptibility to cell death in the amygdala following developmental exposure to the glucocorticoid agonist dexamethasone (Zuloaga et al. 2011); and (7) greater susceptibility to diet-induced hepatosteatosis and insulin growth factor (IGF)-1 deficits (Carbone et al. 2011). In humans, MDD females compared with MDD males show (1) increased GR and MR mRNA in temporal and PFC regions (Watzka et al. 2000); (2) higher levels of cortisol (Frederiksen et al. 1991; Heuser et al. 1994; Laughlin and Barrett-Connor 2000); and (3) decreased volume of hippocampus and increased amygdala (Vakili et al. 2000; Janssen et al. 2004; Weniger et al. 2006). Thus we have been testing the hypothesis that sex differences in the impact of adverse fetal HPA programming demonstrated in preclinical studies, contribute to sex differences in adult MDD.
Receptors responsible for the expression and/or regulation of expression of HPA hormones reside in brain regions implicated in MDD. Hypothalamic nuclei (such as PVN and ventromedial nucleus) and hippocampus are involved in the regulation of HPA hormones, as demonstrated in earlier work by Tobet and Handa (Tobet and Hanna 1997; Brown et al. 1999; Lund et al. 2006; Sandau and Handa 2006; Foradori and Handa 2008; McClellan et al. 2010; Stratton et al. 2011). They are dense in CRH and glucocorticoid receptors, vasopressin, GABA receptors, and sex steroid receptors (Keverne 1988; Handa et al. 1994; Pacak et al. 1995; Koob 1999; Tobet et al. 1999; Dellovade et al. 2001; Davis et al. 2002; Solum and Handa 2002; Tobet 2002; Östlund et al. 2003; Lund et al. 2004, 2006; Suzuki and Handa 2004; Weiser and Handa 2009). Studies have argued that the effects of prenatal stressors on the brain are mediated by neurotransmitter systems that interact with glucocorticoids and gonadal steroid receptors such as GABA and glutamate (Tobet et al. 1999; Seckl and Walker 2001; Owen et al. 2005; McClellan et al. 2008, 2010; Zuloaga et al. 2011), which we have demonstrated in our current program project [National Institute of Health Office for Research on Women’s Health-National Institute of Mental Health P50 MH082679].
In Summary
MDD is a major public health problem with substantial economic, social, and disease burden worldwide. Women are approximately two times more likely than men to present with a lifetime history of MDD. Moreover, this sex difference starts in early adolescence and persists through the mid-50s. Thus, understanding the pathophysiology of this disorder, particularly for women, has important implications for attenuation of suffering worldwide. There is substantial literature supporting the notion that MDD (at least some forms) is a disorder whose vulnerability begins during fetal development. A number of potential pathways may connect adverse conditions arising during fetal development and sex differences in MDD in adulthood. We are currently investigating prenatal stress models that focus on disruption of the development of the fetal HPA circuitry―during periods in which the sexual differentiation of the brain occurs―that we hypothesize place the male or female fetus at differential risks for MDD in adulthood. Further, we have been testing the hypothesis that the fetal hormonal programming will be significantly associated with sex differences in brain activity deficits in stress response circuitry and adult HPA and HPG deficits in MDD. Finally, the demonstration of altered neuroendocrine regulation in relation to sex differences in brain activity in MDD may contribute to understanding the higher prevalence of endocrine disorders in MDD than in the general population, thus promoting further inquiry into development of neuroendocrine treatment modalities. We believe that an understanding of the mechanisms involved in sex differences in the dysregulation of gonadal and adrenal hormones during fetal development in MDD will have etiologic implications and importance for the psychopharmacologic, hormonal and immunoregulatory treatment and prevention of MDD, particularly in women.
References
Abercrombie HC, Jahn AL, Davidson RJ, Kern S, Kirschbaum C, Halverson J (2011) Cortisol’s effects on hippocampal activation in depressed patients are related to alterations in memory formation. J Psychiatr Res 45:15–23
Ahrens T, Deuschle M, Krumm B, van der Pompe G, den Boer JA, Lederbogen F (2008) Pituitary-adrenal and sympathetic nervous system responses to stress in women remitted from recurrent major depression. Psychosom Med 70:461–467
Allen LS, Hines M, Shryne JE, Gorski RA (1989) Two sexually dimorphic cell groups in the human brain. J Neurosci 9:497–506
Alonso SJ, Damas C, Navarro E (2000) Behavioral despair in mice after prenatal stress. J Physiol Biochem 56:77–82
Amin Z, Epperson CN, Constable RT, Canli T (2006) Effects of estrogen variation on neural correlates of emotional response inhibition. Neuroimage 32:457–464
Andreano JM, Cahill L (2010) Menstrual cycle modulation of medial temporal activity evoked by negative emotion. Neuroimage 53:1286–1293
Andreano JM, Waisman J, Donley L, Cahill L (2011) Effects of breast cancer treatment on the hormonal and cognitive consequences of acute stress. Psychooncology. doi:10.1002/pon.2006
Angold A, Costello EJ (2006) Puberty and depression. Child Adolesc Psychiatr Clin N Am 15:919–937, ix
Antonijevic IA (2006) Depressive disorders: is it time to endorse different pathophysiologies? Psychoneuroendocrinology 31:1–15
Appelhof BC, Huyser J, Verweij M, Brouwer JP, van Dyck R, Fliers E, Hoogendijk WJ, Tijssen JG, Wiersinga WM, Schene AH (2006) Glucocorticoids and relapse of major depression (dexamethasone/corticotropin-releasing hormone test in relation to relapse of major depression). Biol Psychiatry 59:696–701
Arborelius L, Owens MJ, Plotsky PM, Nemeroff CB (1999) The role of corticotropin-releasing factor in depression and anxiety disorders. J Endocrinol 160:1–12
Baischer W, Koinig G, Hartmann B, Huber J, Langer G (1995) Hypothalamic-pituitary-gonadal axis in depressed premenopausal women: elevated blood testosterone concentrations compared to normal controls. Psychoneuroendocrinology 20:553–559
Banki CM, Bissette G, Arato M, O’Connor L, Nemeroff CB (1987) CSF corticotropin-releasing factor-like immunoreactivity in depression and schizophrenia. Am J Psychiatry 144:873–877
Bao AM, Hestiantoro A, Van Someren EJ, Swaab DF, Zhou JN (2005) Colocalization of corticotropin-releasing hormone and oestrogen receptor-alpha in the paraventricular nucleus of the hypothalamus in mood disorders. Brain 128:1301–1313
Barden N (2004) Implication of the hypothalamic-pituitary-adrenal axis in the physiopathology of depression. J Psychiatry Neurosci 29:185–193
Barim AO, Aydin S, Colak R, Dag E, Deniz O, Sahin I (2009) Ghrelin, paraoxonase and arylesterase levels in depressive patients before and after citalopram treatment. Clin Biochem 42:1076–1081
Barker DJ (1995) Intrauterine programming of adult disease. Mol Med Today 1:418–423
Berman KF, Schmidt PJ, Rubinow DR, Danaceau MA, Van Horn JD, Esposito G, Ostrem JL, Weinberger DR (1997) Modulation of cognition-specific cortical activity by gonadal steroids: a positron-emission tomography study in women. Proc Natl Acad Sci U S A 94:8836–8841
Bloch M, Schmidt PJ, Danaceau M, Murphy J, Nieman L, Rubinow DR (2000) Effects of gonadal steroids in women with a history of postpartum depression. Am J Psychiatry 157:924–930
Board F, Persky H, Hamburg DA (1956) Psychological stress and endocrine functions; blood levels of adrenocortical and thyroid hormones in acutely disturbed patients. Psychosom Med 18:324–333
Bremmer MA, Deeg DJ, Beekman AT, Penninx BW, Lips P, Hoogendijk WJ (2007) Major depression in late life is associated with both hypo- and hypercortisolemia. Biol Psychiatry 62:479–486
Brouwer JP, Appelhof BC, Hoogendijk WJ, Huyser J, Endert E, Zuketto C, Schene AH, Tijssen JG, Van Dyck R, Wiersinga WM, Fliers E (2005) Thyroid and adrenal axis in major depression: a controlled study in outpatients. Eur J Endocrinol 152:185–191
Brown AE, Mani S, Tobet SA (1999) The preoptic area/anterior hypothalamus of different strains of mice: Sex differences and development. Brain Res Dev Brain Res 115:171–182
Brummelte S, Galea LA (2010) Depression during pregnancy and postpartum: contribution of stress and ovarian hormones. Prog Neuropsychopharmacol 34:766–776
Carbone DL, Zuloaga DG, Hiroi R, Foradori CD, Legare ME, Handa RJ (2011) Prenatal dexamethasone exposure potentiates diet-induced hepatosteatosis and decreases plasma IGF-I in a sex-specific fashion. Endocrinology 53:295–306
Carroll BJ, Curtis GC, Mendels J (1976a) Cerebrospinal fluid and plasma free cortisol concentrations in depression. Psychol Med 6:235–244
Carroll BJ, Curtis GC, Davies BM, Mendels J, Sugerman AA (1976b) Urinary free cortisol excretion in depression. Psychol Med 6:43–50
Carroll BJ, Feinberg M, Greden JF, Tarika J, Albala AA, Haskett RF, James NM, Kronfol Z, Lohr N, Steiner M, de Vigne JP, Young E (1981) A specific laboratory test for the diagnosis of melancholia. Standardization, validation, and clinical utility. Arch Gen Psychiatry 38:15–22
Celsi G, Kistner A, Aizman R, Eklof AC, Ceccatelli S, de Santiago A, Jacobson SH (1998) Prenatal dexamethasone causes oligonephronia, sodium retention, and higher blood pressure in the offspring. Pediatr Res 44:317–322
Chopra KK, Ravindran A, Kennedy SH, Mackenzie B, Matthews S, Anisman H, Bagby RM, Farvolden P, Levitan RD (2009) Sex differences in hormonal responses to a social stressor in chronic major depression. Psychoneuroendocrinology 34:1235–1241
Chung WC, Pak TR, Weiser MJ, Hinds LR, Andersen ME, Handa RJ (2006) Progestin receptor expression in the developing rat brain depends upon activation of estrogen receptor alpha and not estrogen receptor beta. Brain Res 1082:50–60
Clark AS, MacLusky NJ, Goldman-Rakic PS (1988) Androgen binding and metabolism in the cerebral cortex of the developing rhesus monkey. Endocrinology 123:932–940
Coplan JD, Wolk SI, Goetz RR, Ryan ND, Dahl RE, Mann JJ, Weissman MM (2000) Nocturnal growth hormone secretion studies in adolescents with or without major depression re-examined: integration of adult clinical follow-up data. Biol Psychiatry 47:594–604
Craig MC, Fletcher PC, Daly EM, Rymer J, Brammer M, Giampietro V, Maki PM, Murphy DG (2008) Reversibility of the effects of acute ovarian hormone suppression on verbal memory and prefrontal function in pre-menopausal women. Psychoneuroendocrinology 33:1426–1431
Cunningham-Bussel AC, Root JC, Butler T, Tuescher O, Pan H, Epstein J, Weisholtz DS, Pavony M, Silverman ME, Goldstein MS, Altemus M, Cloitre M, Ledoux J, McEwen B, Stern E, Silbersweig D (2009) Diurnal cortisol amplitude and fronto-limbic activity in response to stressful stimuli. Psychoneuroendocrinology 34:694–704
Dahl R, Puig-Antich J, Ryan N, Nelson B, Novacenko H, Twomey J, Williamson D, Goetz R, Ambrosini PJ (1989) Cortisol secretion in adolescents with major depressive disorder. Acta Psychiatr Scand 80:18–26
Daly RC, Danaceau MA, Rubinow DR, Schmidt PJ (2003) Concordant restoration of ovarian function and mood in perimenopausal depression. Am J Psychiatry 160:1842–1846
Davis AM, Henion TR, Tobet SA (2002) Gamma-aminobutyric acidB receptors and the development of the ventromedial nucleus of the hypothalamus. J Comp Neurol 449:270–280
De Bellis MD, Gold PW, Geracioti TD Jr, Listwak SJ, Kling MA (1993) Association of fluoxetine treatment with reductions in CSF concentrations of corticotropin-releasing hormone and arginine vasopressin in patients with major depression. Am J Psychiatry 150:656–657
De Bellis MD, Chrousos GP, Dorn LD, Burke L, Helmers K, Kling MA, Trickett PK, Putnam FW (1994) Hypothalamic-pituitary-adrenal axis dysregulation in sexually abused girls. J Clin Endocrinol Metab 78:249–255
de Leeuw R, Albuquerque RJ, Andersen AH, Carlson CR (2006) Influence of estrogen on brain activation during stimulation with painful heat. J Oral Maxillofac Surg 64:158–166
de Winter RF, van Hemert AM, DeRijk RH, Zwinderman KH, Frankhuijzen-Sierevogel AC, Wiegant VM, Goekoop JG (2003) Anxious-retarded depression: relation with plasma vasopressin and cortisol. Neuropsychopharmacology 28:140–147
Dellovade TL, Davis AM, Ferguson C, Sieghart W, Homanics GE, Tobet SA (2001) GABA influences the development of the ventromedial nucleus of the hypothalamus. J Neurobiol 49:264–276
Deuschle M, Weber B, Colla M, Depner M, Heuser I (1998) Effects of major depression, aging and gender upon calculated diurnal free plasma cortisol concentrations: a re-evaluation study. Stress 2:281–287
Dietrich T, Krings T, Neulen J, Willmes K, Erberich S, Thron A, Sturm W (2001) Effects of blood estrogen level on cortical activation patterns during cognitive activation as measured by functional MRI. Neuroimage 13:425–432
Donahue JE, Stopa EG, Chorsky RL, King JC, Schipper HM, Tobet SA, Blaustein JD, Reichlin S (2000) Cells containing immunoreactive estrogen receptor-alpha in the human basal forebrain. Brain Res 856:142–151
Dougherty D, Rauch SL (1997) Neuroimaging and neurobiological models of depression. Harv Rev Psychiatry 5:138–159
Dreher JC, Schmidt PJ, Kohn P, Furman D, Rubinow D, Berman KF (2007) Menstrual cycle phase modulates reward-related neural function in women. Proc Natl Acad Sci U S A 104:2465–2470
Drevets WC, Price JL, Bardgett ME, Reich T, Todd RD, Raichle ME (2002) Glucose metabolism in the amygdala in depression: relationship to diagnostic subtype and plasma cortisol levels. Pharmacol Biochem Behav 71:431–447
Evans DL, Nemeroff CB (1987) The clinical use of the dexamethasone suppression test in DSM-III affective disorders: correlation with the severe depressive subtypes of melancholia and psychosis. J Psychiatr Res 21:185–194
Fameli M, Kitraki E, Stylianopoulou F (1994) Effects of hyperactivity of the maternal hypothalamic-pituitary-adrenal (HPA) axis during pregnancy on the development of the HPA axis and brain monoamines of the offspring. Int J Dev Neurosci 12:651–659
Fernandez G, Weis S, Stoffel-Wagner B, Tendolkar I, Reuber M, Beyenburg S, Klaver P, Fell J, de Greiff A, Ruhlmann J, Reul J, Elger CE (2003) Menstrual cycle-dependent neural plasticity in the adult human brain is hormone, task, and region specific. J Neurosci 23:3790–3795
Filipek PA, Richelme C, Kennedy DN, Caviness VS Jr (1994) The young adult human brain: an MRI-based morphometric analysis. Cereb Cortex 4:344–360
Foradori CD, Handa RJ (2008) Living or dying in three quarter time: neonatal orchestration of hippocampal cell death pathways by androgens and excitatory GABA. Exp Neurol 213:1–6
Frederiksen SO, Ekman R, Gottfries CG, Widerlov E, Jonsson S (1991) Reduced concentrations of galanin, arginine vasopressin, neuropeptide Y and peptide YY in the temporal cortex but not in the hypothalamus of brains from schizophrenics. Acta Psychiatr Scand 83:273–277
Gallagher P, Young A (2002) Cortisol/DHEA ratios in depression. Neuropsychopharmacology 26:410
Gibbons JL, McHugh PR (1962) Plasma cortisol in depressive illness. J Psychiatr Res 1:162–171
Giedd JN, Vaituzis AC, Hamburger SD, Lange N, Rajapakse JC, Kaysen D, Vauss YC, Rapoport JL (1996) Quantitative MRI of the temporal lobe, amygdala, and hippocampus in normal human development: ages 4–18 years. J Comp Neurol 366:223–230
Gispen-de Wied CC, Westenberg HG, Koppeschaar HP, Thijssen JH, van Ree JM (1992) Stimulation of the pituitary-adrenal axis with a low dose [Arg8]-vasopressin in depressed patients and healthy subjects. Eur Neuropsychopharmacol 2:411–419
Goldstein JM, Seidman LJ, Horton NJ, Makris N, Kennedy DN, Caviness VS Jr, Faraone SV, Tsuang MT (2001) Normal sexual dimorphism of the adult human brain assessed by in vivo magnetic resonance imaging. Cereb Cortex 11:490–497
Goldstein JM, Seidman LJ, O’Brien LM, Horton NJ, Kennedy DN, Makris N, Caviness VS Jr, Faraone SV, Tsuang MT (2002) Impact of normal sexual dimorphisms on sex differences in structural brain abnormalities in schizophrenia assessed by magnetic resonance imaging. Arch Gen Psychiatry 59:154–164
Goldstein JM, Jerram M, Poldrack R, Ahern T, Kennedy DN, Seidman LJ, Makris N (2005) Hormonal cycle modulates arousal circuitry in women using functional magnetic resonance imaging. J Neurosci 25:9309–9316
Goldstein JM, Jerram M, Abbs B, Whitfield-Gabrieli S, Makris N (2010) Sex differences in stress response circuitry activation dependent on female hormonal cycle. J Neurosci 30:431–438
Gorski RA (2000) Sexual differentiation of the nervous system. In: Kandel ER, Schwartz JH, Jessell TM (eds) Principles of neural science, 4th edn. McGraw-Hill Health Professions Division, New York, pp 1131–1146
Graziottin A, Serafini A (2009) Depression and the menopause: why antidepressants are not enough? Menopause Int 15:76–81
Haefner S, Baghai TC, Schule C, Eser D, Spraul M, Zill P, Rupprecht R, Bondy B (2008) Impact of gene-gender effects of adrenergic polymorphisms on hypothalamic-pituitary-adrenal axis activity in depressed patients. Neuropsychobiology 58:154–162
Halbreich U, Kahn LS (2001) Role of estrogen in the aetiology and treatment of mood disorders. CNS Drugs 15:797–817
Halbreich U, Asnis GM, Shindledecker R, Zumoff B, Nathan RS (1985) Cortisol secretion in endogenous depression. I. Basal plasma levels. Arch Gen Psychiatry 42:904–908
Handa RJ, Burgess LH, Kerr JE, O’Keefe JA (1994) Gonadal steroid hormone receptors and sex differences in the hypothalamo-pituitary-adrenal axis. Horm Behav 28:464–476
Harlow BL, Wise LA, Otto MW, Soares CN, Cohen LS (2003) Depression and its influence on reproductive endocrine and menstrual cycle markers associated with perimenopause: the Harvard Study of Moods and Cycles. Arch Gen Psychiatry 60:29–36
Heim C, Nemeroff CB (2001) The role of childhood trauma in the neurobiology of mood and anxiety disorders: preclinical and clinical studies. Biol Psychiatry 49:1023–1039
Heim C, Newport DJ, Heit S, Graham YP, Wilcox M, Bonsall R, Miller AH, Nemeroff CB (2000) Pituitary-adrenal and autonomic responses to stress in women after sexual and physical abuse in childhood. JAMA 284:592–597
Heim C, Newport DJ, Bonsall R, Miller AH, Nemeroff CB (2001) Altered pituitary-adrenal axis responses to provocative challenge tests in adult survivors of childhood abuse. Am J Psychiatry 158:575–581
Heim C, Newport DJ, Wagner D, Wilcox MM, Miller AH, Nemeroff CB (2002) The role of early adverse experience and adulthood stress in the prediction of neuroendocrine stress reactivity in women: a multiple regression analysis. Depress Anxiety 15:117–125
Henry C, Kabbaj M, Simon H, Le Moal M, Maccari S (1994) Prenatal stress increases the hypothalamo-pituitary-adrenal axis response in young and adult rats. J Neuroendocrinol 6:341–345
Heuser IJ, Gotthardt U, Schweiger U, Schmider J, Lammers CH, Dettling M, Holsboer F (1994) Age-associated changes of pituitary-adrenocortical hormone regulation in humans: importance of gender. Neurobiol Aging 15:227–231
Himelein MJ, Thatcher SS (2006a) Depression and body image among women with polycystic ovary syndrome. J Health Psychol 11:613–625
Himelein MJ, Thatcher SS (2006b) Polycystic ovary syndrome and mental health: a review. Obstet Gynecol Surv 61:723–732
Hinkelmann K, Botzenhardt J, Muhtz C, Agorastos A, Wiedemann K, Kellner M, Otte C (2011) Sex differences of salivary cortisol secretion in patients with major depression. Stress 15:105–109
Holsboer F, Gerken A, Stalla GK, Muller OA (1985) ACTH, cortisol, and corticosterone output after ovine corticotropin-releasing factor challenge during depression and after recovery. Biol Psychiatry 20:276–286
Holsboer F, Gerken A, Stalla GK, Muller OA (1987) Blunted aldosterone and ACTH release after human CRH administration in depressed patients. Am J Psychiatry 144:229–231
Holsen LM, Spaeth SB, Lee JH, Ogden LA, Klibanski A, Whitfield-Gabrieli S, Goldstein JM (2011) Stress response circuitry hypoactivation related to hormonal dysfunction in women with major depression. J Affect Disord 131:379–387
Inder WJ, Donald RA, Prickett TC, Frampton CM, Sullivan PF, Mulder RT, Joyce PR (1997) Arginine vasopressin is associated with hypercortisolemia and suicide attempts in depression. Biol Psychiatry 42:744–747
Ising M, Horstmann S, Kloiber S, Lucae S, Binder EB, Kern N, Kunzel HE, Pfennig A, Uhr M, Holsboer F (2007) Combined dexamethasone/corticotropin releasing hormone test predicts treatment response in major depression - a potential biomarker? Biol Psychiatry 62:47–54
Janssen J, Hulshoff Pol HE, Lampe IK, Schnack HG, de Leeuw FE, Kahn RS, Heeren TJ (2004) Hippocampal changes and white matter lesions in early-onset depression. Biol Psychiatry 56:825–831
Jarrett DB, Coble PA, Kupfer DJ (1983) Reduced cortisol latency in depressive illness. Arch Gen Psychiatry 40:506–511
Kawata M (1995) Roles of steroid hormones and their receptors in structural organization in the nervous system. Neurosci Res 24:1–46
Keegan A, Liao LM, Boyle M (2003) ‘Hirsutism’: a psychological analysis. J Health Psychol 8:327–345
Kelly WF, Checkley SA, Bender DA (1980) Cushing’s syndrome, tryptophan and depression. Br J Psychiatry 136:125–132
Kendler KS, Gatz M, Gardner CO, Pedersen NL (2006) A Swedish national twin study of lifetime major depression. Am J Psychiatry 163:109–114
Kessler RC (2003) Epidemiology of women and depression. J Affect Disord 74:5–13
Keverne EB (1988) Central mechanisms underlying the neural and neuroendocrine determinants of maternal behaviour. Psychoneuroendocrinology 13:127–141
Kirschbaum C, Kudielka BM, Gaab J, Schommer NC, Hellhammer DH (1999) Impact of gender, menstrual cycle phase, and oral contraceptives on the activity of the hypothalamus-pituitary-adrenal axis. Psychosom Med 61:154–162
Konrad C, Engelien A, Schoning S, Zwitserlood P, Jansen A, Pletziger E, Beizai P, Kersting A, Ohrmann P, Luders E, Greb RR, Heindel W, Arolt V, Kugel H (2008) The functional anatomy of semantic retrieval is influenced by gender, menstrual cycle, and sex hormones. J Neural Transm 115:1327–1337
Koob GF (1999) Corticotropin-releasing factor, norepinephrine, and stress. Biol Psychiatry 46:1167–1180
Kudielka BM, Kirschbaum C (2005) Sex differences in HPA axis responses to stress: a review. Biol Psychol 69:113–132
Kurt E, Guler O, Serteser M, Cansel N, Ozbulut O, Altinbas K, Alatas G, Savas H, Gecici O (2007) The effects of electroconvulsive therapy on ghrelin, leptin and cholesterol levels in patients with mood disorders. Neurosci Lett 426:49–53
Langenecker SA, Weisenbach SL, Giordani B, Briceno EM, Guidotti Breting LM, Schallmo MP, Leon HM, Noll DC, Zubieta JK, Schteingart DE, Starkman MN (2012) Impact of chronic hypercortisolemia on affective processing. Neuropharmacology 62:217–225
Laughlin GA, Barrett-Connor E (2000) Sexual dimorphism in the influence of advanced aging on adrenal hormone levels: the Rancho Bernardo Study. J Clin Endocrinol Metab 85:3561–3568
Ling MH, Perry PJ, Tsuang MT (1981) Side effects of corticosteroid therapy. Psychiatric aspects. Arch Gen Psychiatry 38:471–477
Lovallo WR, Robinson JL, Glahn DC, Fox PT (2010) Acute effects of hydrocortisone on the human brain: an fMRI study. Psychoneuroendocrinology 35:15–20
Lund TD, Munson DJ, Haldy ME, Handa RJ (2004) Androgen inhibits, while oestrogen enhances, restraint-induced activation of neuropeptide neurones in the paraventricular nucleus of the hypothalamus. J Neuroendocrinol 16:272–278
Lund TD, Hinds LR, Handa RJ (2006) The androgen 5alpha-dihydrotestosterone and its metabolite 5alpha-androstan-3beta, 17beta-diol inhibit the hypothalamo-pituitary-adrenal response to stress by acting through estrogen receptor beta-expressing neurons in the hypothalamus. J Neurosci 26:1448–1456
MacLusky NJ, Clark AS, Naftolin F, Goldman-Rakic PS (1987) Estrogen formation in the mammalian brain: possible role of aromatase in sexual differentiation of the hippocampus and neocortex. Steroids 50:459–474
Maes M, De Ruyter M, Claes R, Bosma G, Suy E (1987) The cortisol responses to 5-hydroxytryptophan, orally, in depressive inpatients. J Affect Disord 13:23–30
Maes M, De Ruyter M, Suy E (1989) Use of the dexamethasone suppression test in an inpatient setting: a replication and new findings. Psychoneuroendocrinology 14:231–239
Maes M, Calabrese J, Meltzer HY (1994) The relevance of the in- versus outpatient status for studies on HPA-axis in depression: spontaneous hypercortisolism is a feature of major depressed inpatients and not of major depression per se. Prog Neuropsychopharmacol Biol Psychiatry 18:503–517
Maheu FS, Mazzone L, Merke DP, Keil MF, Stratakis CA, Pine DS, Ernst M (2008) Altered amygdala and hippocampus function in adolescents with hypercortisolemia: a functional magnetic resonance imaging study of Cushing syndrome. Dev Psychopathol 20:1177–1189
Majdic G, Tobet S (2011) Cooperation of sex chromosomal genes and endocrine influences for hypothalamic sexual differentiation. Front Neuroendocrinol 32:137–145
Matsumoto A, Arai Y (1997) Sexual differentiation of neuronal circuitry in the neuroendocrine hypothalamus. Biomed Rev 7:5–15
Mayberg HS (1997) Limbic-cortical dysregulation: a proposed model of depression. J Neuropsychiatry Clin Neurosci 9:471–481
McClellan KM, Calver AR, Tobet SA (2008) GABAB receptors role in cell migration and positioning within the ventromedial nucleus of the hypothalamus. Neuroscience 151:1119–1131
McClellan KM, Stratton MS, Tobet SA (2010) Roles for gamma-aminobutyric acid in the development of the paraventricular nucleus of the hypothalamus. J Comp Neurol 518:2710–2728
McCook JG, Reame NE, Thatcher SS (2005) Health-related quality of life issues in women with polycystic ovary syndrome. J Obstet Gynecol Neonatal Nurs 34:12–20
McCormick CM, Smythe JW, Sharma S, Meaney MJ (1995) Sex-specific effects of prenatal stress on hypothalamic-pituitary-adrenal responses to stress and brain glucocorticoid receptor density in adult rats. Brain Res Dev Brain Res 84:55–61
McEwen BS (1983) Gonadal steroid influences on brain development and sexual differentiation. In: Green R (ed) Reproductive physiology IV. University Park, Baltimore, pp 99–145
McKay MS, Zakzanis KK (2010) The impact of treatment on HPA axis activity in unipolar major depression. J Psychiatr Res 44:183–192
Meller WH, Grambsch PL, Bingham C, Tagatz GE (2001) Hypothalamic pituitary gonadal axis dysregulation in depressed women. Psychoneuroendocrinology 26:253–259
Merz CJ, Tabbert K, Schweckendiek J, Klucken T, Vaitl D, Stark R, Wolf OT (2010) Investigating the impact of sex and cortisol on implicit fear conditioning with fMRI. Psychoneuroendocrinology 35:33–46
Meynen G, Unmehopa UA, Heerikhuize JJ, Hofman MA, Swaab DF, Hoogendijk WJ (2006) Increased arginine vasopressin mRNA expression in the human hypothalamus in depression: a preliminary report. Biol Psychiatry 60:892–895
Montano MM, Wang MH, vom Saal FS (1993) Sex differences in plasma corticosterone in mouse fetuses are mediated by differential placental transport from the mother and eliminated by maternal adrenalectomy or stress. J Reprod Fertil 99:283–290
Muehlhan M, Lueken U, Wittchen HU, Kirschbaum C (2011) The scanner as a stressor: evidence from subjective and neuroendocrine stress parameters in the time course of a functional magnetic resonance imaging session. Int J Psychophysiol 79:118–126
Muller MB, Holsboer F (2006) Mice with mutations in the HPA-system as models for symptoms of depression. Biol Psychiatry 59:1104–1115
Murphy DG, DeCarli C, McIntosh AR, Daly E, Mentis MJ, Pietrini P, Szczepanik J, Schapiro MB, Grady CL, Horwitz B, Rapoport SI (1996) Sex differences in human brain morphometry and metabolism: an in vivo quantitative magnetic resonance imaging and positron emission tomography study on the effect of aging. Arch Gen Psychiatry 53:585–594
Murray CJ, Lopez AD (1997) Mortality by cause for eight regions of the world: Global Burden of Disease Study. Lancet 349:1269–1276
Nelson WH, Orr WW Jr, Shane SR, Stevenson JM (1984a) Hypothalamic-pituitary-adrenal axis activity and age in major depression. J Clin Psychiatry 45:120–121
Nelson WH, Khan A, Orr WW Jr, Tamragouri RN (1984b) The dexamethasone suppression test: interaction of diagnosis, sex, and age in psychiatric inpatients. Biol Psychiatry 19:1293–1304
Nemeroff CB, Widerlov E, Bissette G, Walleus H, Karlsson I, Eklund K, Kilts CD, Loosen PT, Vale W (1984) Elevated concentrations of CSF corticotropin-releasing factor-like immunoreactivity in depressed patients. Science 226:1342–1344
Nemeroff CB, Bissette G, Akil H, Fink M (1991) Neuropeptide concentrations in the cerebrospinal fluid of depressed patients treated with electroconvulsive therapy. Corticotrophin-releasing factor, beta-endorphin and somatostatin. Br J Psychiatry 158:59–63
Newport DJ, Heim C, Owens MJ, Ritchie JC, Ramsey CH, Bonsall R, Miller AH, Nemeroff CB (2003) Cerebrospinal fluid corticotropin-releasing factor (CRF) and vasopressin concentrations predict pituitary response in the CRF stimulation test: a multiple regression analysis. Neuropsychopharmacology 28:569–576
Nikolarakis KE, Almeida OF, Herz A (1986) Corticotropin-releasing factor (CRF) inhibits gonadotropin-releasing hormone (GnRH) release from superfused rat hypothalami in vitro. Brain Res 377:388–390
O’Keefe JA, Li Y, Burgess LH, Handa RJ (1995) Estrogen receptor mRNA alterations in the developing rat hippocampus. Brain Res Mol Brain Res 30:115–124
O’Toole SM, Sekula LK, Rubin RT (1997) Pituitary-adrenal cortical axis measures as predictors of sustained remission in major depression. Biol Psychiatry 42:85–89
Olster DH, Ferin M (1987) Corticotropin-releasing hormone inhibits gonadotropin secretion in the ovariectomized rhesus monkey. J Clin Endocrinol Metab 65:262–267
Oquendo MA, Echavarria G, Galfalvy HC, Grunebaum MF, Burke A, Barrera A, Cooper TB, Malone KM, John Mann J (2003) Lower cortisol levels in depressed patients with comorbid post-traumatic stress disorder. Neuropsychopharmacology 28:591–598
Orentreich N, Brind JL, Rizer RL, Vogelman JH (1984) Age changes and sex differences in serum dehydroepiandrosterone sulfate concentrations throughout adulthood. J Clin Endocrinol Metab 59:551–555
Östlund H, Keller E, Hurd YL (2003) Estrogen receptor gene expression in relation to neuropsychiatric disorders. Ann N Y Acad Sci 1007:54–63
Owen D, Andrews MH, Matthews SG (2005) Maternal adversity, glucocorticoids and programming of neuroendocrine function and behaviour. Neurosci Biobehav Rev 29:209–226
Pacak K, Palkovits M, Kopin IJ, Goldstein DS (1995) Stress-induced norepinephrine release in the hypothalamic paraventricular nucleus and pituitary-adrenocortical and sympathoadrenal activity: In vivo microdialysis studies. Front Neuroendocrinol 16:89–150
Park J-J, Baum MJ, Paredes RG, Tobet SA (1996) Neurogenesis and cell migration into the sexually dimorphic preoptic area/anterior hypothalamus of the fetal ferret. J Neurobiol 30:315–328
Parker KJ, Schatzberg AF, Lyons DM (2003) Neuroendocrine aspects of hypercortisolism in major depression. Horm Behav 43:60–66
Paus T, Otaky N, Caramanos Z, MacDonald D, Zijdenbos A, D’Avirro D, Gutmans D, Holmes C, Tomaiuolo F, Evans AC (1996) In vivo morphometry of the intrasulcal gray matter in the human cingulate, paracingulate, and superior-rostral sulci: hemispheric asymmetries, gender differences and probability maps. J Comp Neurol 376:664–673
Payne JL (2003) The role of estrogen in mood disorders in women. Int Rev Psychiatry 15:280–290
Payne JL, Palmer JT, Joffe H (2009) A reproductive subtype of depression: conceptualizing models and moving toward etiology. Harv Rev Psychiatry 17:72–86
Plotsky PM, Owens MJ, Nemeroff CB (1998) Psychoneuroendocrinology of depression. Hypothalamic-pituitary-adrenal axis. Psychiatr Clin North Am 21:293–307
Poor V, Juricskay S, Gati A, Osvath P, Tenyi T (2004) Urinary steroid metabolites and 11beta-hydroxysteroid dehydrogenase activity in patients with unipolar recurrent major depression. J Affect Disord 81:55–59
Protopopescu X, Pan H, Altemus M, Tuescher O, Polanecsky M, McEwen B, Silbersweig D, Stern E (2005) Orbitofrontal cortex activity related to emotional processing changes across the menstrual cycle. Proc Natl Acad Sci U S A 102:16060–16065
Protopopescu X, Butler T, Pan H, Root J, Altemus M, Polanecsky M, McEwen B, Silbersweig D, Stern E (2008a) Hippocampal structural changes across the menstrual cycle. Hippocampus 18:985–988
Protopopescu X, Tuescher O, Pan H, Epstein J, Root J, Chang L, Altemus M, Polanecsky M, McEwen B, Stern E, Silbersweig D (2008b) Toward a functional neuroanatomy of premenstrual dysphoric disorder. J Affect Disord 108:87–94
Pruessner JC, Dedovic K, Khalili-Mahani N, Engert V, Pruessner M, Buss C, Renwick R, Dagher A, Meaney MJ, Lupien S (2008) Deactivation of the limbic system during acute psychosocial stress: evidence from positron emission tomography and functional magnetic resonance imaging studies. Biol Psychiatry 63:234–240
Purba JS, Hoogendijk WJ, Hofman MA, Swaab DF (1996) Increased number of vasopressin- and oxytocin-expressing neurons in the paraventricular nucleus of the hypothalamus in depression. Arch Gen Psychiatry 53:137–143
Raadsheer FC, Oorschot DE, Verwer RW, Tilders FJ, Swaab DF (1994a) Age-related increase in the total number of corticotropin-releasing hormone neurons in the human paraventricular nucleus in controls and Alzheimer’s disease: comparison of the disector with an unfolding method. J Comp Neurol 339:447–457
Raadsheer FC, Hoogendijk WJ, Stam FC, Tilders FJ, Swaab DF (1994b) Increased numbers of corticotropin-releasing hormone expressing neurons in the hypothalamic paraventricular nucleus of depressed patients. Neuroendocrinology 60:436–444
Rabin DS, Schmidt PJ, Campbell G, Gold PW, Jensvold M, Rubinow DR, Chrousos GP (1990) Hypothalamic-pituitary-adrenal function in patients with the premenstrual syndrome. J Clin Endocrinol Metab 71:1158–1162
Raison CL, Miller AH (2003) When not enough is too much: the role of insufficient glucocorticoid signaling in the pathophysiology of stress-related disorders. Am J Psychiatry 160:1554–1565
Rasgon NL, Rao RC, Hwang S, Altshuler LL, Elman S, Zuckerbrow-Miller J, Korenman SG (2003) Depression in women with polycystic ovary syndrome: clinical and biochemical correlates. J Affect Disord 74:299–304
Rauch SL, Shin LM, Wright CI (2003) Neuroimaging studies of amygdala function in anxiety disorders. Ann N Y Acad Sci 985:389–410
Regan J, Wagner D, Hamer G, Wright A, White C (2004) Latinos and their mental health. Tenn Med 97:218–219
Rhodes ME, Rubin RT (1999) Functional sex differences (‘sexual diergism’) of central nervous system cholinergic systems, vasopressin, and hypothalamic-pituitary-adrenal axis activity in mammals: A selective review. Brain Res Brain Res Rev 30:135–152
Roca CA, Schmidt PJ, Altemus M, Deuster P, Danaceau MA, Putnam K, Rubinow DR (2003) Differential menstrual cycle regulation of hypothalamic-pituitary-adrenal axis in women with premenstrual syndrome and controls. J Clin Endocrinol Metab 88:3057–3063
Root JC, Tuescher O, Cunningham-Bussel A, Pan H, Epstein J, Altemus M, Cloitre M, Goldstein M, Silverman M, Furman D, Ledoux J, McEwen B, Stern E, Silbersweig D (2009) Frontolimbic function and cortisol reactivity in response to emotional stimuli. Neuroreport 20:429–434
Rubin RT, Poland RE, Lesser IM, Winston RA, Blodgett AL (1987) Neuroendocrine aspects of primary endogenous depression. I. Cortisol secretory dynamics in patients and matched controls. Arch Gen Psychiatry 44:328–336
Rubin RT, Poland RE, Lesser IM (1989) Neuroendocrine aspects of primary endogenous depression VIII. Pituitary-gonadal axis activity in male patients and matched control subjects. Psychoneuroendocrinology 14:217–229
Rubin RT, Miller TH, Rhodes ME, Czambel RK (2006) Adrenal cortical responses to low- and high-dose ACTH(1–24) administration in major depressives vs. matched controls. Psychiatry Res 143:43–50
Rubinow DR, Schmidt PJ (1996) Androgens, brain, and behavior. Am J Psychiatry 153:974–984
Rupp HA, James TW, Ketterson ED, Sengelaub DR, Janssen E, Heiman JR (2009) Neural activation in the orbitofrontal cortex in response to male faces increases during the follicular phase. Horm Behav 56:66–72
Sandau US, Handa RJ (2006) Localization and developmental ontogeny of the pro-apoptotic Bnip3 mRNA in the postnatal rat cortex and hippocampus. Brain Res 1100:55–63
Sandau US, Handa RJ (2007) Glucocorticoids exacerbate hypoxia-induced expression of the pro-apoptotic gene Bnip3 in the developing cortex. Neuroscience 144:482–494
Schmidt PJ, Murphy JH, Haq N, Danaceau MA, St Clair L (2002) Basal plasma hormone levels in depressed perimenopausal women. Psychoneuroendocrinology 27:907–920
Schweiger U, Deuschle M, Weber B, Korner A, Lammers CH, Schmider J, Gotthardt U, Heuser I (1999) Testosterone, gonadotropin, and cortisol secretion in male patients with major depression. Psychosom Med 61:292–296
Seckl JR (2001) Glucocorticoid programming of the fetus; adult phenotypes and molecular mechanisms. Mol Cell Endocrinol 185:61–71
Seckl JR, Walker BR (2001) Minireview: 11beta-hydroxysteroid dehydrogenase type 1- a tissue-specific amplifier of glucocorticoid action. Endocrinology 142:1371–1376
Seidman SN, Araujo AB, Roose SP, McKinlay JB (2001) Testosterone level, androgen receptor polymorphism, and depressive symptoms in middle-aged men. Biol Psychiatry 50:371–376
Sheline YI, Mittler BL, Mintun MA (2002) The hippocampus and depression. Eur Psychiatry 17(Suppl 3):300–305
Simerly RB, Chang C, Muramatsu M, Swanson LW (1990) Distribution of androgen and estrogen receptor mRNA-containing cells in the rat brain: an in situ hybridization study. J Comp Neurol 294:76–95
Slotkin TA, Zhang J, McCook EC, Seidler FJ (1998) Glucocorticoid administration alters nuclear transcription factors in fetal rat brain: Implications for the use of antenatal steroids. Brain Res Dev Brain Res 111:11–24
Solum DT, Handa RJ (2002) Estrogen regulates the development of brain-derived neurotrophic factor mRNA and protein in the rat hippocampus. J Neurosci 22:2650–2659
Sonino N, Fava GA, Raffi AR, Boscaro M, Fallo F (1998) Clinical correlates of major depression in Cushing’s disease. Psychopathology 31:302–306
Spinelli MG (2005) Neuroendocrine effects on mood. Rev Endocr Metab Disord 6:109–115
Stark R, Wolf OT, Tabbert K, Kagerer S, Zimmermann M, Kirsch P, Schienle A, Vaitl D (2006) Influence of the stress hormone cortisol on fear conditioning in humans: evidence for sex differences in the response of the prefrontal cortex. Neuroimage 32:1290–1298
Steiner M (1992) Female-specific mood disorders. Clin Obstet Gynecol 35:599–611
Stratton MS, Searcy BT, Tobet SA (2011) GABA regulates corticotropin releasing hormone levels in the paraventricular nucleus of the hypothalamus in newborn mice. Physiol Behav 104:327–333
Suzuki S, Handa RJ (2004) Regulation of estrogen receptor-beta expression in the female rat hypothalamus: Differential effects of dexamethasone and estradiol. Endocrinology 145:3658–3670
Swaab DF, Fliers E (1985) A sexually dimorphic nucleus in the human brain. Science 228:1112–1115
Swaab DF, Bao AM, Lucassen PJ (2005) The stress system in the human brain in depression and neurodegeneration. Ageing Res Rev 4:141–194
Takahashi A, Sudo M, Minokoshi Y, Shimazu T (1992) Effects of ventromedial hypothalamic stimulation on glucose transport system in rat tissues. Am J Physiol 263:R1228–R1234
Tobet SA (2002) Genes controlling hypothalamic development and sexual differentiation. Eur J Neurosci 16:373–376
Tobet SA, Hanna IK (1997) Ontogeny of sex differences in the mammalian hypothalamus and preoptic area. Cell Mol Neurobiol 17:565–601
Tobet SA, Basham ME, Baum MJ (1993) Estrogen receptor immunoreactive neurons in the fetal ferret forebrain. Brain Res Dev Brain Res 72:167–180
Tobet SA, Henderson RG, Whiting PJ, Sieghart W (1999) Special relationship of g-aminobutyric acid to the ventromedial nucleus of the hypothalamus during embryonic development. J Comp Neurol 405:88–98
Tobet S, Knoll JG, Hartshorn C, Aurand E, Stratton M, Kumar P, Searcy B, McClellan K (2009) Brain sex differences and hormone influences: a moving experience? J Neuroendocrinol 21:387–392
Trestman RL, Coccaro EF, Mitropoulou V, Gabriel SM, Horvath T, Siever LJ (1993) The cortisol response to clonidine in acute and remitted depressed men. Biol Psychiatry 34:373–379
Tronche F, Kellendonk C, Kretz O, Gass P, Anlag K, Orban PC, Bock R, Klein R, Schutz G (1999) Disruption of the glucocorticoid receptor gene in the nervous system results in reduced anxiety. Nat Genet 23:99–103
Ustun TB, Ayuso-Mateos JL, Chatterji S, Mathers C, Murray CJ (2004) Global burden of depressive disorders in the year 2000. Br J Psychiatry 184:386–392
Vakili K, Pillay SS, Lafer B, Fava M, Renshaw PF, Bonello-Cintron CM, Yurgelun-Todd DA (2000) Hippocampal volume in primary unipolar major depression: a magnetic resonance imaging study. Biol Psychiatry 47:1087–1090
Vallee M, Mayo W, Dellu F, Le Moal M, Simon H, Maccari S (1997) Prenatal stress induces high anxiety and postnatal handling induces low anxiety in adult offspring: correlation with stress-induced corticosterone secretion. J Neurosci 17:2626–2636
van Amelsvoort TAMJ, Abel KM, Robertson DMR, Daly E, Critchley H, Whitehead M, Murphy DGM (2001) Prolactin response to d-fenfluramine in postmenopausal women on and off ERT: comparison with young women. Psychoneuroendocrinology 26:493–502
van Broekhoven F, Verkes RJ (2003) Neurosteroids in depression: a review. Psychopharmacology (Berl) 165:97–110
van Londen L, Goekoop JG, van Kempen GM, Frankhuijzen-Sierevogel AC, Wiegant VM, van der Velde EA, De Wied D (1997) Plasma levels of arginine vasopressin elevated in patients with major depression. Neuropsychopharmacology 17:284–292
van Stegeren AH, Wolf OT, Everaerd W, Scheltens P, Barkhof F, Rombouts SA (2007) Endogenous cortisol level interacts with noradrenergic activation in the human amygdala. Neurobiol Learn Mem 87:57–66
van Stegeren AH, Wolf OT, Everaerd W, Rombouts SA (2008) Interaction of endogenous cortisol and noradrenaline in the human amygdala. Prog Brain Res 167:263–268
van Wingen G, Mattern C, Verkes RJ, Buitelaar J, Fernandez G (2008a) Testosterone biases automatic memory processes in women towards potential mates. Neuroimage 43:114–120
van Wingen GA, van Broekhoven F, Verkes RJ, Petersson KM, Backstrom T, Buitelaar JK, Fernandez G (2008b) Progesterone selectively increases amygdala reactivity in women. Mol Psychiatry 13:325–333
van Wingen GA, Zylicz SA, Pieters S, Mattern C, Verkes RJ, Buitelaar JK, Fernandez G (2009) Testosterone increases amygdala reactivity in middle-aged women to a young adulthood level. Neuropsychopharmacology 34:539–547
van Wingen G, Mattern C, Verkes RJ, Buitelaar J, Fernandez G (2010) Testosterone reduces amygdala-orbitofrontal cortex coupling. Psychoneuroendocrinology 35:105–113
Veith RC, Lewis N, Langohr JI, Murburg MM, Ashleigh EA, Castillo S, Peskind ER, Pascualy M, Bissette G, Nemeroff CB et al (1993) Effect of desipramine on cerebrospinal fluid concentrations of corticotropin-releasing factor in human subjects. Psychiatr Res 46:1–8
von Bardeleben U, Holsboer F, Gerken A, Benkert O (1989) Mood elevating effect of fluoxetine in a diagnostically homogeneous inpatient population with major depressive disorder. Int Clin Psychopharmacol 4(Suppl 1):31–35
Vreeburg SA, Hoogendijk WJ, van Pelt J, Derijk RH, Verhagen JC, van Dyck R, Smit JH, Zitman FG, Penninx BW (2009) Major depressive disorder and hypothalamic-pituitary-adrenal axis activity: results from a large cohort study. Arch Gen Psychiatry 66:617–626
Wang J, Korczykowski M, Rao H, Fan Y, Pluta J, Gur RC, McEwen BS, Detre JA (2007) Gender difference in neural response to psychological stress. Soc Cogn Affect Neurosci 2:227–239
Watzka M, Beyenburg S, Blumcke I, Elger CE, Bidlingmaier F, Stoffel-Wagner B (2000) Expression of mineralocorticoid and glucocorticoid receptor mRNA in the human hippocampus. Neurosci Lett 290:121–124
Webster MJ, Knable MB, O’Grady J, Orthmann J, Weickert CS (2002) Regional specificity of brain glucocorticoid receptor mRNA alterations in subjects with schizophrenia and mood disorders. Mol Psychiatry 7(985–994):924
Weiner CL, Primeau M, Ehrmann DA (2004) Androgens and mood dysfunction in women: comparison of women with polycystic ovarian syndrome to healthy controls. Psychosom Med 66:356–362
Weinstock M (1997) Does prenatal stress impair coping and regulation of hypothalamic-pituitary-adrenal axis? Neurosci Biobehav Rev 21:1–10
Weinstock M, Matlina E, Maor GI, Rosen H, McEwen BS (1992) Prenatal stress selectively alters the reactivity of the hypothalamic-pituitary adrenal system in the female rat. Brain Res 595:195–200
Weiser MJ, Handa RJ (2009) Estrogen impairs glucocorticoid dependent negative feedback on the hypothalamic-pituitary-adrenal axis via estrogen receptor alpha within the hypothalamus. Neuroscience 159:883–895
Weniger G, Lange C, Irle E (2006) Abnormal size of the amygdala predicts impaired emotional memory in major depressive disorder. J Affect Disord 94:219–229
Witte AV, Savli M, Holik A, Kasper S, Lanzenberger R (2010) Regional sex differences in grey matter volume are associated with sex hormones in the young adult human brain. Neuroimage 49:1205–1212
Wolkowitz OM, Reus VI, Keebler A, Nelson N, Friedland M, Brizendine L, Roberts E (1999) Double-blind treatment of major depression with dehydroepiandrosterone. Am J Psychiatry 156:646–649
Wust S, Wolf J, Hellhammer DH, Federenko I, Schommer N, Kirschbaum C (2000) The cortisol awakening response - normal values and confounds. Noise Health 2:79–88
Young EA, Altemus M (2004) Puberty, ovarian steroids, and stress. Ann N Y Acad Sci 1021:124–133
Young EA, Korszun A (2002) The hypothalamic-pituitary-gonadal axis in mood disorders. Endocrinol Metab Clin North Am 31:63–78
Young EA, Midgley AR, Carlson NE, Brown MB (2000) Alteration in the hypothalamic-pituitary-ovarian axis in depressed women. Arch Gen Psychiatry 57:1157–1162
Young AH, Gallagher P, Porter RJ (2002) Elevation of the cortisol-dehydroepiandrosterone ratio in drug-free depressed patients. Am J Psychiatry 159:1237–1239
Young EA, Ribeiro SC, Ye W (2007a) Sex differences in ACTH pulsatility following metyrapone blockade in patients with major depression. Psychoneuroendocrinology 32:503–507
Young EA, Kornstein SG, Harvey AT, Wisniewski SR, Barkin J, Fava M, Trivedi MH, Rush AJ (2007b) Influences of hormone-based contraception on depressive symptoms in premenopausal women with major depression. Psychoneuroendocrinology 32:843–853
Zobel AW, Yassouridis A, Frieboes RM, Holsboer F (1999) Prediction of medium-term outcome by cortisol response to the combined dexamethasone-CRH test in patients with remitted depression. Am J Psychiatry 156:949–951
Zuloaga DG, Carbone DL, Hiroi R, Chong DL, Handa RJ (2011) Dexamethasone induces apoptosis in the developing rat amygdala in an age-, region-, and sex-specific manner. Neuroscience 199:535–547
Acknowledgments
This work was supported by the National Institutes of Mental Health, Office of Research on Women’s Health (ORWH-NIMH) P50 MH082679 (Goldstein, P.I.).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Goldstein, J.M., Holsen, L.M., Handa, R., Tobet, S. (2013). Sex Differences in HPA and HPG Axes Dysregulation in Major Depressive Disorder: The Role of Shared Brain Circuitry Between Hormones and Mood. In: Pfaff, D., Christen, Y. (eds) Multiple Origins of Sex Differences in Brain. Research and Perspectives in Endocrine Interactions. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-33721-5_10
Download citation
DOI: https://doi.org/10.1007/978-3-642-33721-5_10
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-33720-8
Online ISBN: 978-3-642-33721-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)