Abstract
Abdominal aortic aneurysms (AAA) are defined as dilatations of the aorta to a diameter 1.5 times the expected normal aortic diameter. Although they are responsible for a variety of symptomatic presentations, from embolism to frank rupture, the most common presentation is one of an incidental finding in an asymptomatic patient. History and physical exam should be focused on elucidating symptoms, as well as risk factors, and potentially palpating a pulsatile abdominal mass, although the positive predictive value of physical exam in identifying and predicting size of a AAA is notoriously poor. The preoperative imaging of choice is computed tomographic angiography. Based on imaging characteristics and preoperative risk stratification, either an endovascular or open surgical modality should be used for repair. No statistically significant differences in long-term mortality have been found between the two modalities. Postoperative surveillance is imperative following both types of repair, although necessarily more frequent following endovascular interventions.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Algorithmic Approach
-
A.
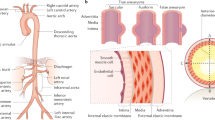
Definitions: An aneurysm is defined as a focal dilatation of an artery to a diameter of at least 1.5 times larger than the expected normal diameter. As this pertains to the infrarenal abdominal aorta, a diameter of 3 cm or greater typically qualifies as aneurysmal.
-
B.
Evaluation/history: With the widespread use of cross-sectional imaging, many abdominal aortic aneurysms are discovered incidentally. Others are found on screening exams, as the US Preventative Services Task Force recommends that men aged 65–75 years who have ever smoked undergo screening ultrasound [1]. A small proportion of patients present with symptomatic AAA, with abdominal and/or back pain and a palpable pulsatile abdominal mass, which is widely believed to represent an impending aneurysmal rupture [2].
-
C.
Evaluation/physical examination: Risk factors for development of AAA include advanced age, male gender, and a history of smoking. The positive predictive value of physical exam for detection and diagnosis of AAA is only 15% [3]. Physical examination should also focus on identifying factors that may impact intervention, such as surgical scars on the abdominal wall, hernias, and body habitus.
-
D.
Imaging: Screening and monitoring of AAA typically use duplex ultrasonography as it is low risk and the least invasive. In the setting of preoperative planning, computed tomographic angiography (CTA) provides greater accuracy and more reliable measurements.
-
E.
Indications and management: Any patient with a reasonable life expectancy and an AAA >5 cm, or aortic expansion of 1 cm or more in 1 year, is a candidate to be considered for surgical repair. Surgical operations for the treatment of AAA include open surgical repair (OSR) and endovascular aortic repair (EVAR) . The character of the aortic neck bears great influence over the suitability for endovascular repair, as length, angulation, diameter, and shape will impact the ability to obtain an adequate proximal seal. Both OSR and EVAR must remain in the armamentarium of the vascular surgeon as conversion to open repair may be necessary when safe execution of EVAR is not possible; moreover, long-term outcomes demonstrate that no differences in long-term mortality exist between the two modalities [4].
-
F.
Postoperative complications: Depending on the circumstances of the presentation and of the repair, common complications following AAA repair include cardiac ischemia, renal failure, and ischemia of the sigmoid colon, lower extremities, or spinal cord. Graft-related complications following EVAR include endoleaks. Ischemic colitis can present with bloody diarrhea, abdominal pain, distension, fever, leukocytosis, or metabolic acidosis.
-
G.
Long-term follow-up: Following EVAR , contrast-enhanced CT scanning should be undertaken at 1 and 12 months; alternatively, duplex ultrasound combined with non-contrast CT serves as a viable option in patients with renal insufficiency. An endoleak, a complication unique to EVAR , occurs due to persistent blood flow into the aneurysmal sac and if seen at 1 month would necessitate a CTA at 6 months to determine need for re-intervention. There are five types of endoleaks: Type 1 (incomplete seal between the stent and native vessel – Immediate repair required), type 2 (blood flow into aneurysm sac via branch vessels of the intrarenal abdominal aorta), type 3 (blood flow between the separate components of the graft), type 4 (blood flow through the graft fabric), and type 5 (persistently elevated pressure within the aneurysm sac). Thereafter, surveillance following EVAR should be continued at least on an annual basis. Following open repair, imaging should be obtained at least every 5 years.

Algorithm 135.1
References
US Preventive Services Task Force: Abdominal Aortic Aneurysm. Web address: https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/abdominal-aortic-aneurysm-screening. Accessed 25 Aug 2017.
Sullivan CA, Rohrer MJ, Cutler BS. Clinical management of symptomatic but unruptured abdominal aortic aneurysm. J Vasc Surg. 1990;11(6):799–803.
Beede SD, Ballard DJ, James EM, Ilstrup DM, Hallet JW Jr. Positive predictive value of clinical suspicion of abdominal aortic aneurysm. Implications for effective use of abdominal ultrasonography. Arch Intern Med. 1990;150(3):549–51.
Schermerhorn M, Dominique B, O’Malley J, Curran T, McCallum J, Darling J, Landon BE. Long term outcomes of abdominal aortic aneurysm in the medicare population. N Engl J Med. 2015;373:328–38.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Greenleaf, E.K., Aziz, F. (2019). Abdominal Aortic Aneurysm. In: Docimo Jr., S., Pauli, E. (eds) Clinical Algorithms in General Surgery . Springer, Cham. https://doi.org/10.1007/978-3-319-98497-1_135
Download citation
DOI: https://doi.org/10.1007/978-3-319-98497-1_135
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-98496-4
Online ISBN: 978-3-319-98497-1
eBook Packages: MedicineMedicine (R0)