Abstract
The sentinel lymph node (SLN) is frequently the first node in the lymphatic basin that receives drainage from an anatomic region and is immunologically responsible for that region. Sentinel lymph node biopsy (SLNB) remains the standard of care for the assessment of clinically negative axillary lymph nodes in patients with invasive breast carcinomas. Accurate diagnosis of a SLNB can direct the surgeon with regard to the need for axillary dissection (AD), and it can affect post-operative treatment decisions, including decisions about radiation therapy. Furthermore, an accurate negative diagnosis on SLNB can spare the patient the increased risk of lymphedema that accompanies AD or post-operative treatments. Its relatively low false negative rate of 5–10% and high sensitive rate of 90–95% in the detection of cancer to the lymph node basin has made this minimally invasive operation a standard. The idea that the SLN serves as a limited target sample of the axillary lymph nodes aroused an interest and trend toward increased inspection of the sentinel lymph node for detection of metastatic carcinoma by the pathologist though serial sections and/or immunohistochemistry.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
The sentinel lymph node (SLN) is frequently the first node in the lymphatic basin that receives drainage from an anatomic region and is immunologically responsible for that region. Sentinel lymph node biopsy (SLNB) remains the standard of care for the assessment of clinically negative axillary lymph nodes in patients with invasive breast carcinomas. Accurate diagnosis of a SLNB can direct the surgeon with regard to the need for axillary dissection (AD), and it can affect post-operative treatment decisions, including decisions about radiation therapy. Furthermore, an accurate negative diagnosis on SLNB can spare the patient the increased risk of lymphedema that accompanies AD or post-operative treatments. Its relatively low false negative rate of 5–10% and high sensitive rate of 90–95% in the detection of cancer to the lymph node basin has made this minimally invasive operation a standard. The idea that the SLN serves as a limited target sample of the axillary lymph nodes aroused an interest and trend toward increased inspection of the sentinel lymph node for detection of metastatic carcinoma by the pathologist though serial sections and/or immunohistochemistry .
22.1 Introduction
Axillary lymph nodes status is an important prognostic factor and determinant of treatment for patients with breast carcinoma . For decades, axillary lymph node dissection (ALND) was the only procedure used for staging axillary lymph nodes in women with invasive breast carcinoma [1]. Axillary lymph node dissection, however, is associated with significant morbidity, including long-term complications such as limitation of shoulder movements, paresthesia and arm numbness, and lymphedema, which can have a significant impact on the patient’s quality of life.
The feasibility of identifying a sentinel lymph node (SLN) intraoperatively in breast cancer was first investigated at the JWCI by Giulano et al. [2]. In October 1991, the group began to investigate the feasibility of lymphatic mapping and sentinel lymphadenectomy with isosulfan blue vital dye in breast cancer as a more accurate and less morbid approach to stage breast cancer. This prospective study demonstrated that sentinel node biopsy of the axilla is technically feasible, safe, and without added complications. With a defined technique and experience, 100% accuracy in predicting the status of axilla was subsequently achieved [2, 3].
The sentinel lymph node (SLN) is frequently the first node in the lymphatic basin that receives drainage from an anatomic region and is immunologically responsible for that region. The sentinel lymph node biopsy (SLNB) has become the standard of care in the assessment of metastatic spread to the lymph node basin. Its relative low false negative rate of 5–10% and high sensitivity rate of 90–95% in the detection of cancer to the lymph node basin has made this minimally invasive operation a standard [4].
Clinical trials have proven that SLN is equivalent to staging of the axilla in patients with clinically node-negative disease (cN0). In addition, recent trials show that ALND may be safely omitted in selected cN0 patients with metastatic carcinomas limited to one or two sentinel lymph nodes . No difference in regional control, disease-free survival, and overall survival have been found between sentinel lymph node biopsy and axillary lymph node dissection in patients with early breast cancer and clinically negative axillary lymph nodes [5, 6].
22.2 Patterns of Regional Nodal Drainage
The axilla is the primary site of drainage in about 95% of breast cancer cases, with isolated internal mammary drainage seen in less than 5% of cases. Primary drainage to other pathways, such as supraclavicular, cervical, or intercostal, and contralateral lymph nodes, is extremely uncommon [7].
22.3 Indications and Contraindications for Sentinel Lymph Node
Sentinel lymph node biopsy is indicated for staging patients with early T1-T2 invasive breast cancer and clinically negative axillary lymph nodes, irrespective of surgical therapy on the breast. Women with ductal carcinoma in situ undergoing mastectomy are SLNB candidates because the disruption of lymph channels during a mastectomy will prevent accurate subsequent SLNB if invasion is identified. SLNB is absolutely contraindicated in patients with inflammatory breast cancer and patients with clinically positive axillary lymph nodes . These patients require axillary lymph node dissection [8, 9].
22.4 Surgical Techniques
Sentinel lymph node biopsy typically begins with injection of one or two tracers (blue dye or radioactive colloid) into breast skin or parenchyma either in the vicinity of the tumor or under the areolar plexus. These tracers enter the lymphatic channels and passively flow to the draining lymph nodes. Sentinel lymph nodes are then identified as those first receiving drainage from the tumor by the presence of tracer, and are removed [10, 11].
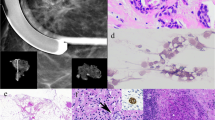
The use of radiocolloids for SLN identification offer several advantages. The colloids are efficiently trapped in the SLN (whereas blue dyes typically pass into second echelon nodes). Radiocolloid enables pre-operative sentinel node imaging (Figs. 22.1 and 22.2). It also facilitates rapid and easy intraoperative detection by the surgeon using a gamma probe (Fig. 22.3). Several studies have shown better sentinel node identification rates, when compared with blue dye alone [12, 13].
Breast lymphatic mapping and sentinel lymph node . The two mapping agents, vital blue dye and radiocolloid, are injected into the subareolar plexus. (a) “Hot” Spots in the axilla can be identified before making the skin incision with the gamma probe. (b) Small incision in axilla, the sentinel lymph node is harvested
22.5 Pathological Axillary Lymph Node Staging
The pathological characterization of regional lymph nodes (pN) for breast carcinoma reflects the cumulative total regional lymph node burden of metastatic disease in the axillary, infraclavicular, supraclavicular, and ipsilateral internal mammary nodes. Pathologic classification (pN) is used only in conjunction with a pathological tumor assignment (surgical resection) (pT), and includes pathological evaluation of excised nodes from a sentinel lymph node biopsy and/ or lymph node dissection. Classification based solely on sentinel lymph node biopsy with fewer than six nodes evaluated and without subsequent axillary lymph node dissection is designated (sn) for “sentinel node” [2,3,4,5,6].
The American Joint Committee on Cancer (AJCC) and the Union for International Cancer Control TNM staging systems recognize three categories of lymph node involvement on the basis of size: isolated tumor cells (ITCs), micrometastasis, and macrometastasis (Table 22.1) [1]:
-
(a)
Isolated Tumor Cells (pN0 [i+]): Isolated tumor cell clusters (ITCs) are defined as small clusters of cells not larger than 0.2 mm, or single tumor cells, or fewer than 200 cells in single histologic cross-section. ITCs may be detected by routine histology or by immunohistochemical methods (Figs. 22.4 and 22.5).
-
(b)
Micrometastasis (pN1mi): Micrometastases are defined as tumor deposits larger than 0.2 mm but not larger than 2.0 mm in the largest dimension (Figs. 22.6, 22.7, 22.8, and 22.9).
-
(c)
Macrometastasis (pN1): For patients who are pathologically node-positive with macrometastasis, at least one node must contain a tumor deposit >2 mm, and all remaining quantified nodes most contain tumor deposits larger than 0.2 mm (at least micrometastasis) (Figs. 22.10, 22.11, and 22.12).
A point that requires clarification pertains to measuring the size of the tumor deposit. When multiple tumor deposits are present in a lymph node with the isolated tumor cells or micrometastasis, the size of only the largest contiguous tumor is used to classify the node. This is regardless of whether the deposit is confined to the lymph node, extends outside the node, or is totally present outside the lymph node and invading adipose tissue. Some authors do not consider lesions purely outside the lymph node (e.g., in afferent lymphatic channels or perinodal fat) as evidence of nodal involvement (Fig. 22.13) [1, 3, 5].
22.6 Occult Metastatic Disease
An occult metastasis is defined as any metastasis that is not identified on initial examination with a “standard” evaluation protocol. In one study, more intensive pathologic evaluation of the nodes by deeper sectioning and immunohistochemical staining increased the yield of occult metastases and led to an overall case conversion rate of 10.3% in patients who had an initial negative sentinel lymph node [14]. Occult metastases have no significance in terms of surgical management and patient outcomes. Routine immunohistochemical and reverse transcriptase polymerase chain reaction (PCR) are therefore not recommended for the evaluation of SLN [15].
22.7 Intraoperative Evaluation
Intraoperative detection of metastatic carcinoma in sentinel lymph nodes leads to immediate axillary lymph node dissection, avoiding the need for a delayed second surgical procedure. Intraoperative evaluation (IOE) of SLN at the time of primary breast surgery may be reserved for patients with clinically and radiologically negative axillae or suspicious intraoperative findings. The disadvantages of IOE of SLN include an increase in operation time and possible false-positive results. It is helpful for pathologists to be aware of the histologic type of carcinoma ; metastatic invasive lobular carcinoma can be very difficult to diagnose in frozen sections [16, 17].
Frozen section (FS), imprint cytology (IC), or cytological smear (CS) can be used to evaluate sentinel lymph nodes intraoperatively. Cytological techniques are faster than FS, and do not cause significant loss of nodal tissue, but it may be difficult to confirm findings limited to the cytology material, and not present in H&E-stained sections (Fig. 22.14). FS is time-consuming (all slides should be frozen), freezing introduces artefactual tissue distortion, and sectioning of the frozen tissue block could potentially lead to the loss of critical tissue [17].
Recent studies have called the need for intraoperative sentinel lymph node assessment in situations where additional axillary dissection (AD) is unlikely to be performed even if metastasis is detected in the SLN. The ACOSOG Z0011 study showed no difference in local or regional recurrence between patients with 1–2 positive sentinel lymph nodes who were randomly treated with either SLNB-alone or SLNB plus axillary dissection. By applying the Z0011 criteria, it is estimated that approximately 75% of patients undergoing breast-conservation surgery could avoid additional AD [18]. Finally, intraoperative evaluations of SLN continue to be performed routinely at many hospitals for cN0 patients undergoing mastectomy, and pathologists should use the method (FS, IC, CS) that they are most comfortable with to avoid false-positive results [19].
22.7.1 Pathologic Evaluation
Despite specific recommendations from the College of American Pathologists (CAP) and ASCO, considerable heterogeneity remains among pathologists in the evaluation of sentinel lymph node pertaining to grossing, sectioning, cutting intervals, and use of immunohistochemistry or RT-PCR [20].
22.7.2 Gross Evaluation
First, we must inspect the node and any adherent fat. If any dimension is larger than 2.0 mm, the node must be sectioned. Most lymph nodes take the form of an asymmetric ellipsoid, or are bean shaped, with one long axis and two shorter axes. Most authors recommend cutting the node parallel to the long axis even though this is harder than sectioning perpendicular to this axis. Cutting parallel to the long axis produces fewer 2.0 mm slices to examine, and there is data that suggest afferent lymphatics are more likely to enter the node in this plane. The two opposing cut faces should be placed down in the cassette and full-face sections should be examined microscopically (Fig. 22.15) [20, 21].
22.7.3 Histologic Evaluation
Standard histopathologic evaluation of SLN has a sensitivity for the detection of both micrometastasis and macrometastasis at a rate of 83.4%. The assessment of levels in SLN is highly inconsistent among institutions, ranging from the performance of 1 H&E as advocated by CAP to 2–5–100 levels separated by intervals ranging from 2 to 500 μm, to a more labor-intensive and cost-intensive protocol with exhaustive sampling of the entire paraffin block at 50 μm. ASCO has endorsed limited step sections cut at 200–500 μm, to enhance detection of micrometastases [22].
22.8 Extracapsular Extension
Metastatic carcinoma can invade through the lymph node (LN) capsule into the surrounding axillary fibroadipose tissue (Fig. 22.16). According to CAP, the presence of extracapsular extension (ECE) should be reported and the area of invasion outside of the LN capsule should be included when measuring the largest span of the LN metastasis .
The presence of tumor outside the lymph node is a prognostic parameter in breast cancer. It has also been shown to be associated with increased likelihood of non-sentinel lymph node involvement. Extranodal invasion is often further classified into minimal (if less than 1 mm beyond the capsule) or prominent (if greater than 1 mm) (Fig. 22.17).
Prominent extranodal invasion is often used by radiation oncologists to guide therapy, although there is no hard evidence that this makes a difference to the outcomes [22,23,24].
22.9 Sentinel Lymph Node Biopsy After Neoadjuvant Chemotherapy
Neoadjuvant chemotherapy (NAC) is a common treatment used for patients with locally advanced and lymph-positive breast cancer to reduce tumor size, increase the rate of breast-conserving surgery, and acquire information regarding chemotherapy sensitivity. The use of sentinel lymph node biopsy after NAC is controversial. A meta-analysis of studies in which SLNB was performed after NAC in patients with clinically node-negative cancer showed acceptable accuracy (Fig. 22.18) [25].
22.10 Immunohistochemistry
Immunohistochemical stains are commonly performed to increase the likelihood of detection of micrometastases. A number of different broad-spectrum or low-molecular-weight cytokeratin antibodies, including AE1/AE3, MNF 116, and CAM 5.2, have been used for this purpose. The results of two randomized trials (NSABP-B32 and ACOSOG Z0010) [15] have raised questions about the clinical significance of micrometastasis and isolated tumor cells. As a result, it has been suggested that routine evaluation of sentinel lymph node with cytokeratin immunostains should be abandoned. Immunohistochemistry is more commonly performed for evaluation of lymph nodes from a patient with lobular carcinoma (Fig. 22.19).
Immunostaining for cytokeratin does have a role in the evaluation of both sentinel and nonsentinel lymph nodes when there are cells identified on H&E-stained sections that are suspicious for, but not diagnostic of, tumor cells (Fig. 22.20). If cytokeratin staining is to be performed in this setting, it is important to recognize that other cell types in lymph nodes , particularly interstitial reticulum cells, demonstrate cytokeratin reactivity with some antibodies (especially antibody CAM 5.2); these cells much less frequently stain with cytokeratin AE1/AE3. Therefore, AE1/AE3 is preferable to CAM 5.2 for the confirmation of carcinoma cells in lymph nodes [26].
References
Amin M, Edge S, Greene F, Byrd DR, Brookland RK, Washington MK, et al., editors. The AJCC cancer staging manual. 8th ed. New York, NY: Springer International Publishing; 2017.
Giuliano AE, Kirgan DM, Guenther JM, Morton DL. Lymphatic mapping and sentinel lymphadenectomy for breast cancer. Ann Surg. 1994;220:391–8.
Lyman GH, Giulano AE, Somerfield MR, Benson AB 3rd, Bodurka DC, Burstein HJ, et al. American Society of Clinical Oncology guideline recommendations for sentinel lymph node biopsy in early-stage breast cancer. J Clin Oncol. 2005;23:7703–20.
McMaster KM, Tuttle TM, Carlson DJ, Brown CM, Noyes RD, Glaser RL, et al. Sentinel lymph node biopsy for breast cancer: a suitable alternative to routine axillary dissection in multi-institutional practice when optimal technique is used. J Clin Oncol. 2000;18:2560–6.
Veronesi U, Viale G, Paganelly G, Zurrida S, Luini A, Galimberti V, et al. Sentinel lymph node biopsy in breast cancer: ten-year results of a randomized controlled study. Ann Surg. 2010;25:595–600.
Giuliano AE, Ballman K, Mc Call L, Beitsch P, Whitworth PW, Blumencranz P, et al. Locoregional recurrence after sentinel lymph node dissection with or without axillary dissection in patients with sentinel lymph node metastases: long-term follow-up from the American College of Surgeons oncology group (alliance) ACOSOG Z 011 randomized trial. Ann Surg. 2016;264:413–20.
Chatterjee A, Serniak N, Czerniecki BJ. Sentinel lymph node biopsy in breast cancer: a work in progress. Cancer J. 2015;21:7–10.
Apple SK. Sentinel lymph node in breast cancer: review article from a pathologist’s point of view. J Pathol Transl Med. 2016;50:83–95.
Hansen NM, Grube BJ, Giulano AE. The time has come to change the algorithm for the surgical management of early breast cancer. Arch Surg. 2002;137:1131–5.
Somasundaram SK, Chicken DW, Keshtgar M. Detection of the sentinel lymph node in breast cancer. Br Med Bull. 2007;84:117–31.
McMasters KM, Wong SL, Martin RC 2nd, Chao C, Tuttle TM, Noyes RD, et al. Dermal injection of radioactive colloid is superior to peritumoral injection for breast cancer sentinel lymph node biopsy: results of a multiinstitutional study. Ann Surg. 2001;233:676–87.
Maguire A, Brogi E. Sentinel lymph nodes for breast carcinoma. A paradigm shift. Arch Pathol Lab Med. 2016;140:791–8.
Weaver DL. Sentinel lymph nodes and breast carcinoma: which micrometastases are clinically significant? Am J Surg Pathol. 2003;27:842–7.
Weaver DL, Ashikaga T, Krag DN, Skelly JM, Anderson SJ, Harlow SP, et al. Effect of occult metastases on survival in node-negative breast cancer. N Engl J Med. 2011;364:412–21.
Weaver DL, Le UP, Harlow SP, Ashikaga T, Krag DN, Dupuis SL, et al. Metastasis detection in sentinel lymph nodes comparison of a limited widely spaced (NSABP protocol B-32) and a comprehensive narrowly spaced paraffin block sectioning strategy. Am J Surg Pathol. 2009;33:1583–9.
Van der Noordaa MEM, MTFD V-P, EJT R. The intraoperative assessment of sentinel nodes—standards and controversies. Breast. 2017;34:S64–9.
Barroso-Bravo S, Zarco-Espinoza G, Alvarado-Cabrero I, Valenzuela-Flores AG, Pichardo-Romero P, Rodríguez-Cuevas S. Lymphatic mapping and sentinel lymph node biopsies in order to avoid axillary dissection in early breast cancer. Cir Cir. 2005;73:437–41.
Cox C, Centeno B, Dickson D, Clark J, Nicosia S, Dupont E, et al. Accuracy of Intraoperative imprint cytology for sentinel lymph node evaluation in the treatment of breast carcinoma. Cancer. 2005;105:13–20.
Brogi E, Torres-Matundan E, Tan LK, Cody HS III. The results of frozen section, touch preparation, and cytological smear are comparable for intraoperative examination of sentinel lymph nodes: a study in 133 breast cancer patients. Ann Surg Oncol. 2005;12:173–80.
Weaver DL. Pathology evaluation on sentinel lymph nodes in breast cancer: protocol recommendations and rationale. Mod Pathol. 2010;23:S26–32.
Diaz LK, Hunt K, Ames F, Meric F, Kuerer H, Babiera G, et al. Histologic localization of sentinel lymph node metastases in breast cancer. Am J Surg Pathol. 2003;27:385–9.
Association of Directors of Anatomic and surgical Pathology. ADASP recommendations for processing and reporting lymph node specimens submitted for evaluation of metastatic disease. Am J Surg Pathol. 2001;25:961–3.
Aziz S, Wik E, Knutsuik G, Klingen TA, Chen Y, Davidsen B, et al. Extra-nodal extension is a significant prognostic factor in lymph node positive breast cancer. PLoS One. 2017;15:e0171853.
Cserni G. Axillary sentinel lymph node micrometastases with extracapsular extension: a distinct pattern of breast cancer metastasis? J Clin Pathol. 2008;61:115–8.
Xing Y, Foy M, Cox DD, Kuerer HM, Hunt KK, Cormier JN. Meta-analysis of sentinel lymph node biopsy after preoperative chemotherapy in patients with breast cancer. Br J Surg. 2006;93:539–46.
Lyman GH, Temin S, Edge SB, Newman LA, Turner RR, Weaver DL, et al. Sentinel lymph node biopsy for patients with early-breast cancer: American Society of Clinical Oncology. Clinical practice guideline update. J Clin Oncol. 2014;32:1365–83.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Alvarado-Cabrero, I., Rodríguez-Cuevas, S.A. (2018). Sentinel Lymph Node: Clinicopathologic Features. In: Stolnicu, S., Alvarado-Cabrero, I. (eds) Practical Atlas of Breast Pathology . Springer, Cham. https://doi.org/10.1007/978-3-319-93257-6_22
Download citation
DOI: https://doi.org/10.1007/978-3-319-93257-6_22
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-93256-9
Online ISBN: 978-3-319-93257-6
eBook Packages: MedicineMedicine (R0)