Abstract
Interleukin-1 and other IL-1 family members are key players in immunity and inflammation.
The activation of the IL-1 system is tightly regulated, through ligands with antagonistic or anti-inflammatory activity, or decoy and negative regulatory receptors. IL-1R2 and IL-1R8 (also known as SIGIRR) are members of the ILR family acting as negative regulators of the IL-1 system. IL-1R2 binds IL-1 and the accessory protein IL-1RAcP without activating signaling, thus modulating IL-1 availability for the signaling receptor. IL-1R8 dampens IL-1 receptor- and Toll Like Receptor-mediated cell activation and is a component of the receptor complex recognizing the anti-inflammatory cytokine IL-37.
The deregulated activation of the IL-1 system is the potential cause of detrimental local or systemic inflammatory reactions. Here, we summarize our current understanding of the function of IL-1R2 and IL-1R8, focusing on their role in pathological conditions, ranging from infectious and sterile inflammation, to cancer-related inflammation.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Innate and adaptive immunity cells are tightly regulated by a plethora of cytokines and receptors. The Interleukin-1 system plays a crucial role in controlling immune responses and inflammatory processes [1, 2]. IL-1 family ligands include 7 molecules with agonist activity (IL-1α, IL-1β, IL-18, IL-33, IL-36α, β, and γ), three receptor antagonists (IL-1Ra, IL-36Ra and IL-38), and an anti-inflammatory cytokine (IL-37). The IL-1R family members include 11 molecules [IL-1R1, IL-1R2, IL-1R3 (IL-1RAcP), IL-1R4 (ST2), IL-1R5 (IL-18Rα), IL-1R6 (IL-1Rrp2, IL-36R), IL-1R7 (IL-18Rβ), IL-1R8 (TIR8, also known as SIGIRR), IL-1R9 (TIGIRR-2), IL-1R10 (TIGIRR-1)] (Fig. 1) [2].
The IL-1 system
Ligands of the IL-1 receptor (ILR) family are shown (IL-1α, IL-1β, IL-38, IL-33, IL-36α, IL-36β, IL-36γ and IL-18). IL-1R, IL-33R, IL-36R and IL-18R complexes activate signal transduction. IL-R2, sIL-1R2, IL-1Ra, IL-36Ra IL-18BP and IL-1R8 are negative regulators acting with different mechanisms. IL-37 is an anti-inflammatory cytokine, signaling upon the formation of a tripartite complex (IL-37/IL-1R5/IL-1R8). IL-1R3 is an accessory protein for IL-R1, IL-1R2, IL-1R4 and IL-1R6. Ligands for IL-1R8, IL-1R9 and IL-1R10 are still partially defined
ILRs are characterized by an evolutionarily conserved structure which consists of Ig-like extracellular domains and an intracellular Toll-IL-1 resistance (TIR) domain, that is shared with Toll-like receptors (TLRs) [3]. Ligand binding induces the dimerization through the TIR domain of the specific receptor with a second receptor molecule, acting as an accessory protein and establishing an intracellular signaling platform, which recruits one of the adaptor proteins MyD88, MAL, TRIF, TRAM or SARM. In turn, these molecular complexes unleash protein kinases activation (e.g. Tumor necrosis factor receptor-associated factor 6 (TRAF6) and IL-1R associated kinases (IRAKs),) and trigger a cohort of downstream targets such as nuclear factor-κB (NFκB), activator protein-1 (AP-1), c-Jun N-terminal kinase (JNK), p38 mitogen-associated protein kinase, extracellular signal-regulated kinases (ERKs), mitogen-activated protein kinases (MAPKs), and interferon (IFN)-regulatory factors (IRF) [4,5,6]. The modulation of multiple Transcriptional Factors (TFs) orchestrates a robust pro-inflammatory reaction, enforcing both the innate and adaptive immunity [7,8,9].
The fundamental role of ILR family in inflammation is underlined by a broad spectrum of inflammatory, autoimmune and neoplastic diseases correlated to deregulation of the IL-1 system. For instance, several lines of evidence indicate that IL-1 and its regulation play a pivotal role in cancer -related inflammation and progressive tissue damages in chronic inflammatory conditions. This link emphasizes the implications of ILR and cytokine targeting as therapeutic strategy in several pathological conditions associated with acute and chronic inflammation, ranging from cardiovascular and autoimmune diseases to cancer [10,11,12,13,14,15,16].
The IL-1 system includes several extracellular and intracellular endogenous regulators, which tune ILR signaling and are necessary to restore homeostatic conditions. These “caretakers” are anti-inflammatory cytokines (IL-37, IL-38), receptor antagonists (IL-1Ra, IL-36Ra, and IL-38), scavengers and/or decoy or negative regulatory receptors (e.g. IL-1R2, IL-1R8 and IL-18BP), and miRNAs [17] that tune ILR signaling at transcriptional and post-transcriptional level.
Here, we summarize our current understanding of the structure and function of IL-1R2 and IL-1R8, two negative regulators of inflammation and immune responses, describing their relevance in physiology and pathology.
2 The Decoy Receptor IL-1R2
2.1 IL-1R2 Protein and Function
Human IL-1R2 is a highly conserved gene localized in chromosome 2, in a large cluster which includes several ILR members such as the receptors for IL-33, IL-18 and IL-36 [18, 19].
IL-1R2 gene encodes an extensively glycosylated 68 kDa protein composed of 386 amino acids. The IL-1R2 extracellular domain has the canonical ILR Ig-like-structure, and shares 28% amino acid homology with IL-1R1. In contrast, the IL-1R2 intracellular domain is peculiar for the absence of a functional TIR domain, which is substituted by a short 29 amino acid-long cytoplasmic tail [20, 21]. Several enzymes, in particular the metalloproteinase ADAM17, cleave the full-length receptor to generate an IL-1R2 soluble form with decoy activity [22,23,24]. Pro-inflammatory molecules (LPS, TNFα, leukotriene B4, or fMLF) trigger the enzymatic cleavage and the release of soluble IL-1R2 [25,26,27,28], which can be also generated by an alternative splicing isoform of the IL-1R2 transcript [29].
IL-1R2 exerts its decoy activity through different mechanisms. First, IL-1R2 sequesters IL-1R3 to generate a dominant negative receptor complex [30], which competes with IL-1R1 for the formation of a signaling receptor complex [31,32,33]. Second, the IL-1R2/IL-1R3 complex binds IL-1α and IL-1β, without activating the pro-inflammatory signaling cascade [20, 34]. In addition, the soluble form participates in reducing IL-1 availability for the signaling receptor, since soluble IL-1R2 and IL-1R3 are found at high concentration (in the order of ng/ml) in the blood, and their physical interaction increases the affinity for IL-1α and IL-1β [34, 35]. Finally, IL-1R2 is present in the cytoplasm and interacts with pro-IL-1α preventing cleavage and activation by different enzymes (calpain, granzyme B, chymase, and elastase) during necrosis [34,35,36,37].
2.2 IL-1R2 Expression and Regulation
IL-1R2 is the predominant IL-1 receptor in the myeloid compartment, in particular monocytes, macrophages and neutrophils, and it is overexpressed in M2 macrophages [20, 34, 38, 39]. In the lymphoid compartment, IL-1R2 shows a high expression level in B cells and in T regulatory cells (Treg) and it is up-regulated upon TCR stimulation [20, 34, 38, 39]. In colorectal and non-small-cell lung cancers, Treg express higher levels of IL-1R2 compared to Th1 and Th17 tumor infiltrating lymphocytes [40]. Similarly, breast cancer infiltrating Tregs express higher IL-1R2 levels compared to healthy breast resident Tregs and circulating Tregs [41]. The functional activity of IL-1R2 in tumor infiltrating Tregs and the molecular mechanisms regulating its expression are still unknown. Interestingly, IL-1β inhibition significantly reduced the risk of incident lung cancer and lung cancer mortality in a large cohort of atherosclerosis patients, suggesting the relevance of IL-1 regulation in cancer [16].
In the mouse, Il1r2 is widely expressed in innate and adaptive immune cells of myeloid and lymphoid origin [25, 42,43,44,45,46,47,48,49,50], it is up-regulated by several anti-inflammatory stimuli (e.g. IL-4, IL-13, IL-27, IL-10, glucocorticoid hormones and prostaglandins) [20, 38, 51,52,53,54,55,56], and down-regulated by pro-inflammatory and chemotactic molecules (e.g. LPS, IFNγ, TNFα, reactive oxygen intermediates and phorbol myristate acetate) [22, 27, 28, 54, 57].
The regulation of IL-1R2 expression on the myeloid compartment has been associated with the pathogenesis of several inflammatory diseases. Atherosclerosis is associated with vessel wall inflammation and IL-1 has long been known to drive atherosclerosis and its complications. Interestingly, reduced expression of IL-1R2 was observed in atherosclerosis vascular lesions, which suggests defective tuning of IL-1 activity [48]. Based on the role of IL-1 in the pathogenesis of cardiovascular diseases, a large prospective study was conducted using anti-IL-1β (Canakinumab) in high-risk atherosclerosis patients, which showed that treatment led to a significantly lower rate of recurrent cardiovascular events [15].
Up-regulation of IL-1R2 in microglia represents a protective mechanism of the central nervous system suppressing IL-1β-mediated brain inflammation and neurotoxicity [45, 46, 58]. IL-1R2 down-regulation has been associated with type II osteoarthritis [59] and correlated to bone resorption upon IL-1 stimulation [47].
The relevance of decoy receptors as fundamental brakes of the immune response is demonstrated by their exploitation by viruses and bacteria as pathogen evasion strategies. For instance, double strand DNA viruses (Poxviruses and Herpesviruses) have acquired decoy receptor genes through genetic recombination with the host genome [60]. In lethal Listeria monocytogenes infection, IL-1R2 expression is up-regulated in monocytes [42], and protein A of Staphylococcus aureus was shown to induce soluble IL-1R2 by stimulating ADAM17-mediated cleavage, resulting in IL-1β sequestration and decreased bacterial eradication [61].
2.3 IL-1R2 Functional Role In Vivo
Several studies have demonstrated the anti-inflammatory role of IL-1R2 in vivo. IL-1R2 deficiency exacerbates endometriosis [62], autoimmune myocarditis [63] and skin inflammation [64], through the inhibition of IL-1 signaling and therefore Th17 cell activation [65].
IL-1R2 deficient mice were also more susceptible to arthritis. In collagen-induced arthritis, IL-1R2-deficient macrophages increased their responsiveness to IL-1 and governed the pro-inflammatory response [59, 66, 67]. In contrast, in the K/BxN serum transfer-induced arthritis, increased joint degeneration has been attributed to neutrophils, through a not cell autonomous mechanism [68]. IL-1R2-deficiency on neutrophils increased the IL-1-induced response of fibroblasts, suggesting that IL-1R2 acts in trans, as soluble form shed upon IL-1β treatment. However, IL-1R2-deficiency did not affect the acute inflammation induced by systemic administration of IL-1β or LPS [64, 68], in contrast with pleiotropic effects of IL-1Ra-deficiency [69, 70].
Recently, it was shown that IL-1R2 was expressed together with the IL-1 receptor antagonist IL-1Ra, by follicular regulatory T (Tfr) cells, which are responsible for the modulation of follicular helper T (Tfh) cell effector functions and therefore B cell activation in the germinal center. IL-1 treatment induced IL-21 and IL-4 production by Tfh cells and this effect was inhibited in the presence of Tfr cells, possibly because of IL-1 capture by IL-1R2 [71].
2.4 IL-1R2 Like Prognostic and Diagnostic Marker
IL-1R2 shedding in pathological conditions has encouraged the studies of IL-1R2 soluble form as diagnostic and prognostic marker. IL-1R2 is released in plasma in physiological conditions (5–10 ng/ml), but its levels are proportionally increased upon infections (acute meningococcal infection, experimental endotoxemia, trauma, necrotizing enterocolitis, acute respiratory distress syndrome, sepsis) [72]. IL-1R2 soluble form was suggested as biomarker in multiple sclerosis [73] and in Alzheimer’s disease [74], whereas in the synovial fluid and plasma of rheumatoid arthritis patients IL-1R2 was correlated with symptom amelioration [75, 76]. Soluble IL-1R2 has been suggested as good prognostic biomarker in pancreas islet transplantation [77] and in inflammatory bowel disease [78] and as biomarker to monitor the clinical outcome of TNFα blockade with Etanercept [79] and in steroid treatment response [80].
Finally, IL-1R2 over-expression has been also observed in psoriatic patients [81] and in several solid tumors such as prostatic cancer, ductal adenocarcinoma [82], benign prostatic hyperplasia [83] and ovarian cancer [84], but the functional implication of IL-1R2 in neoplastic transformation is unknown. In ulcerative colitis, IL-1R2 expression was correlated to remission [78, 85] and to steroid response [80].
3 IL-1R8 (TIR8/SIGIRR)
3.1 IL-1R8 Gene and Protein
IL-1R8 is an antisense gene on human chromosome 11 [86], with three main isoforms that share a common coding DNA sequence. The murine locus is on chromosome 7. The gene is well conserved among vertebrates, and the human IL-1R8 protein has a primary sequence of 414 amino-acid with a high identity score (82%) between human and mouse species [87]. Despite the partial identity with IL-1R1 protein (23%), IL-1R8 has relevant structural differences: the extracellular region of IL-1R8 has only a single Ig domain and the intracellular TIR domain has a long tail of 95 residues. Compared to “canonical” TIR domains, IL-1R8 has two aminoacid substitutions in Ser447 and Tyr536 (switched to Cys222 and Leu305) and the lack of phosphorylation on these two residues influences IL-1R8 signaling activity.
Similarly to IL-1R2, IL-1R8 is N- and O-glycosylated on the extracellular domain, and these post-transcriptional modifications have been described as functionally relevant in a study performed in colon cancer patients (see below) [88].
IL-1R8 is expressed in the majority of epithelial tissues and it is particularly enriched in liver, in kidney and in lymphoid organs. The expression in leukocytes is ubiquitous, showing a higher expression level in NK cells and T lymphocytes, and it is also expressed in platelets [86, 89,90,91] (Fig. 2).
IL-1R8 functions in different cell types
IL-1R8 is widely express in both the hematopoietic and non-hematopoietic compartment and governs cell differentiation and activation. In particular, IL-1R8 modulates NK cell maturation and effector functions; ILC1 activation; T cell activation and polarization; monocyte, macrophage, DC, platelet and epithelium activation, through the negative regulation of IL-1 family members or microbial moieties acting on ILRs and TLRs, respectively
IL-1R8 was shown to be downregulated upon bacterial infections by Pseudomonas aeruginosa [92], or Toxoplasma gondii [93], in pyelonephritis induced by E. coli [94] and in necrotizing enterocolitis [95]. A reduced expression of IL-1R8 was also observed in acute inflammation , in psoriatic arthritis, in asymptomatic bacteriuria [96, 97], in colitis, and after stimulation with flagellin and LPS in vivo and in vitro [91, 98,99,100]. Treatment with LPS was shown to downregulate IL-1R8 in monocytes and neutrophils [98] through the inhibition of SP1 binding on IL-1R8 promoter [98, 101]. However, an increased expression of IL-1R8 was observed in monocytes in sepsis and sterile inflammation and this correlated with a tolerogenic phenotype after LPS and Pam3CysSK4 stimulation [102]. Moreover, amyloid β treatment has been proposed to down-regulate IL-1R8 in microglia and hippocampal tissue through the transcription factor peroxisome proliferator-activated receptor (PPAR)γ [103]. Other stimuli involved in tuning IL-1R8 are the neuropeptide vasoactive intestinal peptide (VIP), Lactobacillus jensenii [104], and bacterial immunogenic molecules [105], which mainly affect myeloid derived cells (macrophages, DC, Langerhans cells).
The deregulation of IL-1R8 has been associated with malignant transformation. In chronic lymphocytic leukemia (CLL) , neoplastic B cells showed lower expression of IL-1R8 compared to B cells from healthy donors [106]. Several genes are downregulated through DNA hypermethylation in CLL, but no difference was observed in IL-1R8 methylation. However, treatment with the hypomethylating drug 5-Azacytidine led to IL-1R8 overexpression, suggesting an indirect regulation of IL-1R8 mediated by 5-Azacytidine [106]. IL-1R8 loss of function has been described in colon tumorigenesis, which has been explained with the existence of a dominant negative isoform of IL-1R8, a truncated protein that was shown to trap the main IL-1R8 protein isoform in the endoplasmic reticulum [88]. Finally, RNAseq data and experiments on tumor cell lines showed that IL-1R8 was upregulated in breast cancer [107].
Other IL-1R8 isoforms are emerging, but their function is unknown. Recently a longer isoform called IL-1R8L1 was characterized in tumor epithelial cell lines (e.g. Hela, HT-29 and PC3), in a neuroblastoma cell line (SK-N-HS), in leukemic cell lines (e.g. Jurkat, MEC1, Ramos, Daudi, and THP1), and in human healthy tissues (e.g. hearth, small intestine, kidney, liver, lung, stomach, spleen, ovary, and testis) [108]. LPS stimulation was shown to downregulate IL-1R8L1 in THP1 cell lines, indicating a common regulatory mechanism shared by IL-1R8 isoforms [108].
3.2 Functional Roles of IL-1R8
IL-1R8-deficient mice have demonstrated the role of IL-1R8 in reducing NFκB and JNK activation, inhibiting ILRs and TLRs (e.g. IL-1R1, IL-1R5/IL-18Rα, IL-1R4/ST2, TLR1, TLR2, TLR4, TLR7, TLR9, TLR3) downstream signaling pathways [90, 91, 109,110,111,112,113,114].
IL-1R8 is recruited to the ligand-receptor complex, and the BB-loop structure of IL-1R8 TIR domain inhibits the dimerization of MyD88 [86, 89, 109, 111, 115, 116]. In silico studies of protein modeling have suggested a regulatory mechanism similar to IRAK-M, in which the Myddosome complex is retained on receptors and cannot drive the pro-inflammatory cascade [117]. Furthermore, IL-1R8 extracellular domain inhibits the reciprocal interaction between IL-1R1 and IL-1R3 [111]. The steric competition exerted by IL-1R8 has been also proposed to explain the IL-1R8-mediated regulation of TLR3 signaling, in which IL-1R8 blocks TRAM homodimerization and TLR4-TRAM and TRIF-TRAM interactions [117,118,119].
The decoy activity of IL-1R8 is also involved in the regulation of JNK and mTOR pathways in lymphoid and not lymphoid cells (e.g. Th17, NK cells and intestinal epithelium) [90, 120, 121].
The deregulation of the IL-1 system is part of pathogen evasion strategies, as mentioned in case of IL-1R2 [122]. Indeed, several bacteria (e.g. Brucella melitensis, E. coli, Salmonella enterica, Pseudomonas denitrificans and P. aeruginosa) [122,123,124,125] have evolved TIR-containing proteins (Tcps) that dampen TIR-related pathway, suggesting that Tcps might be evolutionary linked to IL-1R8.
3.3 IL-1R8 as a Coreceptor of IL-1R5/IL-18Rα for IL-37
In the last decade new anti-inflammatory interleukins involved in controlling TLR pro-inflammatory pathways were identified. In this regard, IL-37 has emerged as a bioactive molecule in leukocytes, in particular in macrophages, and epithelial cells, and IL-37-transgenic mice (IL-37tg mice) were reported to be refractory to inflammation [126]. Intriguingly, the formation of a tripartite complex composed by IL-37, IL-1R8 and IL-1R5 was demonstrated to be required for IL-37 signaling in human PBMCs and murine bone marrow-derived macrophages. This interaction induced an immunosuppressive pathway, inhibiting MAPK, NFκB, mTOR, TAK1 and Fyn, and activating STAT3, Mer, PTEN and p62(dok) signaling [127, 128]. IL-37 mediated protection was abolished by IL-1R8-deficiency in LPS-induced endotoxemia, A. fumigatus pulmonary infection [127, 129], and OVA-induced asthma [130].
IL-37 was also implicated in tuning metabolism and in AMPK activation in adipocytes and macrophages [131], with a significant effects on obesity, insulin response and glucose tolerance. In this context, IL-37 and IL-1R5/IL-1R8 receptor complex led to the inhibition of mTOR signaling and activation of STAT6 and Foxo TF family [127], which triggered a pseudo-starvational state in macrophages and DCs. Furthermore, IL-37 was described as a regulatory molecule in muscle cells, orchestrating AMPK pathway and improving exercise performance [132]. At the cellular level, IL-37 potentiated oxidative phosphorylation in mitochondria modulating redox state in the organelles [132]. Finally, recombinant human IL-37 increased muscular resistance in healthy mice and in models of systemic inflammation (upon LPS administration), and IL-1R8-deficiency abrogated IL-37 effects on fatigue tolerance [132]. These lines of experimental evidence support the potential targeting of IL-37/IL-1R8 axis in patients, in which chronic inflammation leaded muscle degeneration and impaired physical mobility [133].
3.4 IL-1R8 in Infections and Inflammation
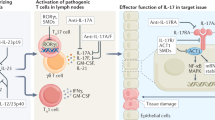
IL-1R8-deficient mice exhibited an overwhelming local and systemic inflammation and tissue damage after infection with several pathogens (Fig. 3). In fungal infection models such as Candida albicans or Aspergillus fumigatus, the absence of IL-1R8 led to enhanced susceptibility to mucosal and disseminated or lung infection, respectively, with increased mortality and fungal burden, increased activation of IL-1 signaling and Th17 cell response and reduced Treg activation [134]. In Mycobacterium tuberculosis infection, IL-1R8-deficiency was associated with exacerbated inflammation , in terms of macrophage and neutrophil lung infiltration and increased systemic levels of inflammatory cytokines. The higher mortality observed in IL-1R8-deficient mice was prevented by IL-1 and TNFα inhibition and was not dependent on the increased mycobacteria load [135]. In acute lung infections with P. aeruginosa, IL-1R8-deficient mice showed deregulation of IL-1 signaling, leading to higher mortality and bacterial load, and increased production of pro-inflammatory cytokines [92]. Moreover, in a model of keratitis induced by P. aeruginosa, IL-1R8 was involved in preventing tissue damage , through the negative regulation of IL-1R1 and TLR4 signaling in Th1 cells [136]. In humans, 3 SNPs (rs10902158, rs7105848, rs7111432) were identified in the IL-1R8 gene, which correlated with the development of both pulmonary tuberculosis and tuberculous meningitis [137]. Increased susceptibility to LPS-induced mortality was described in IL-1R8-deficient mice on a BALB/c background [109], but not in a mixed C57BL/6 × 129/Sv background [110].
Roles of IL-1R8 in pathology
IL-1R8 emerged as a crucial modulator of inflammation, and innate and adaptive immune responses in several pathological contexts and it is also part of the tripartite complex necessary for IL-37 signaling. IL-1R8 plays a fundamental role in models of infections, autoimmunity, allergy, renal inflammation, platelet activation, brain inflammation and neuronal plasticity, intestinal inflammation and cancer (colorectal cancer, CLL and breast cancer). IL-1R8 acts as a checkpoint molecule regulating NK cell antitumor and antiviral activity
In contrast, IL-1R8-deficiency was protective in a model of experimental urinary tract infection (UTI) induced by uropathogenic E. coli, causing reduced renal bacteria outgrowth and renal dysfunction. The initial recruitment of leukocytes in the kidney was increased, in line with increased production of TNFα and chemokines (CXCL1, CCL2 and CCL3) by tubular epithelial cells after stimulation with E. coli [94]. In line with this, in a human bladder epithelial cell line (BECs), IL-1R8 silencing was associated with increased JNK, p38 and ERK1/2 activation and IL-6 and IL-8 production, after stimulation with LPS [100]. Similarly, in Streptococcus pneumoniae pneumonia and sepsis, IL-1R8-deficiency caused reduced mortality, bacterial outgrowth and dissemination [138].
In Citrobacter rodentium infection in mice, that mimics intestinal infections by enteric bacterial pathogens in humans, IL-1R8-deficiency was associated with microbiota depletion, due to enhanced IL-1R1 and MyD88-driven inflammatory and anti-microbial response, and therefore causing exacerbated pathogen colonization [139].
Thus, depending on the effect of inflammatory responses in specific infections , IL-1R8 may play a protective or detrimental role in the innate resistance to pathogens, emerging as a key player in the regulation of the complex and delicate balance between protective immune responses and inflammation and host tissue damage.
3.5 IL-1R8 in Autoimmunity and Allergy
IL-1 family and TLR signaling are involved in the pathogenesis of autoimmune diseases and allergy (Fig. 3). In two different models of arthritis, IL-1R8-deficient mice displayed an higher susceptibility, associated with increased cellular infiltration into the affected joints [140]. In line with this study, IL-1R8 expression was reduced in the peripheral blood of patients with psoriatic arthritis, compared with healthy donors [96]. Moreover, IL-1R8-deficient mice showed enhanced susceptibility to psoriasis, increased infiltration and activation of γδ T cells, and IL-1-driven IL-17A expression by γδ T cells [141]. In experimental autoimmune encephalomyelitis (EAE) IL-1R8-deficient mice developed a more severe disease, due to an increased Th17 infiltrate in the central nervous system (CNS) and enhanced Th17 polarization and pathogenic functions. IL-1R8 was shown to regulate IL-1-dependent Th17 cell differentiation, expansion and effector functions, by controlling IL-1-induced mTOR pathway [120].
In a model of hydrocarbon oil-induced lupus, IL-1R8-deficiency was associated with enhanced TLR7-mediated activation of DCs and expansion of autoreactive lymphocyte clones [142]. In SLE patients, in particular those with nephritis, reduced frequency of IL-1R8+ CD4+ T cells was reported in [143]. The analysis of IL-1R8 gene allelic variants of a single missense SNP (rs3210908) in a large European population showed no correlation between IL-1R8 polymorphisms and SLE [144], whereas the genetic variants of SNP rs7396562 correlated with the susceptibility to SLE in a Chinese population [145]. In C57BL/6lpr/lpr mice, which develop delayed autoimmunity due to impaired Fas-induced apoptosis of autoreactive B and T cells, the absence of IL-1R8 determined a massive lymphoproliferative disorder, increased autoimmune lung disease, lupus nephritis and hypergammaglobulinemia. The phenotype was associated with increased activation of DCs and B cells and production of proinflammatory cytokines (CCL2, IL-6, and IL-12p40) and B cell antiapoptotic mediators (Baff/BlyS and Bcl-2) in response to RNA and DNA immune complexes or other TLR agonists [146].
In the context of IL-33-dependent allergic responses, IL-1R8-deficient mice showed increased lung inflammation, splenomegaly and serum levels of IL-5 and IL-13 and enhanced production of type 2 cytokines in vitro [113]. In contrast, IL-1R8 alleles or haplotypes were not associated with asthma susceptibility or asthma-related conditions in a cohort of Japanese asthma patients [147].
3.6 IL-1R8 in Sterile Inflammation
IL-1R8 is expressed at high levels in the kidney, in particular in tubular epithelial cells, DCs and macrophages [112]. In a postischemic renal failure model, IL-1R8-deficient mice exhibit increased renal injury , caused by a massive activation of myeloid cells, increased intrarenal cytokine and chemokine production and increased leukocyte recruitment [148]. In lupus nephritis, postischemic acute renal failure or kidney transplantation, IL-1R8 expressed by hematopoietic cells was demonstrated to negatively modulate TLR activation by nucleosomes and DAMPs, released during cell necrosis associated with these conditions [142, 146, 148, 149]. In a model of fully mismatched kidney allotransplantation, IL-1R8-deficient grafts were less tolerated compared with control grafts. This phenotype was associated with enhanced allostimulatory activity of DCs and consequently allogeneic adaptive immune responses and increased post transplant kidney inflammatory response, driven by ILR and TLR signaling [149].
3.7 IL-1R8 in the Brain
IL-1R8 is expressed in the brain by neurons, microglia and astrocytes [89, 150, 151] and it regulates LPS- or IL-1-induced neuro-inflammation (Fig. 3). IL-1R8-deficient mice exhibited a massive brain inflammation , in terms of CD40, ICAM, IL-6 and TNFα mRNA expression in microglia and inflammatory cytokine production in hippocampal tissue, upon treatment with LPS [152]. Even in the absence of external stimuli, cognitive and synaptic functions, such as novel object recognition, spatial reference memory, and long-term potentiation (LTP) were impaired. The phenotype was dependent on increased expression of IL-1α and high mobility group box 1 (HMGB1) and enhanced activation of IL-1R1 and TLR4 downstream signaling molecules (IRAK1, c-Jun, JNK and NFκB) [153]. Moreover, IL1R8 negatively regulated the anti-inflammatory activity of IL-36Ra in glial cells [150]. In addition, it was demonstrated that IL-1R8 regulated β-amyloid (Aβ) peptide-induced TLR2 signaling and inflammation in the brain, suggesting a potential role of IL-1R8 in Alzheimer’s disease (AD) and AD-associated neuroinflammation [103].
A recent study elucidated the molecular mechanisms underlying cognitive and synaptic function impairment in absence of IL-1R8 [114]. It was shown that IL-1R8-deficiency and the consequent hyperactivation of the IL-1R pathway affected neuron synapse morphology, plasticity and function. Indeed, IL-1R8-deficient hippocampal neurons displayed an increased number of immature, thin spines and a decreased number of mature, mushroom spines along with a significant reduction of spine width, and reduced amplitude of miniature excitatory postsynaptic currents. Spine morphogenesis and plasticity impairment was caused by the IL-1R1-driven hyperactivation of the PI3K/AKT/mTOR pathway in IL-1R8-deficient neurons, leading to and increased expression of methyl-CpG-binding protein 2 (MeCP2), a synaptopathy protein involved in neurological diseases, such as Rett syndrome and MeCP2 duplication syndrome [154]. Pharmacological inhibition of IL-1R1 with IL-1Ra (Anakinra) or IL-1R1 genetic inactivation normalized MeCP2 expression and cognitive deficits in IL-1R8-deficient mice, revealing the key role of IL-1R8 in the fine tuning of IL-1R1 pathway, which is required for correct long-term potentiation [114]. Importantly, in cryopyrin-associated periodic syndrome (CAPS) patients, pharmacological inhibition of IL-1, reversed mental defects of the patients and reduced signs and symptoms of IL-1-dependent inflammation [155]. These results thus identify IL-1R8 as a key molecule involved in synaptopathies through the modulation of IL-1 activity in neurons.
3.8 IL-1R8 in Intestinal Inflammation and Intestinal Cancer
IL-1R8-deficiency is associated with uncontrolled inflammation in the intestine , leading to a reduced survival, weight loss, intestinal bleeding and local tissue injury in the model of dextran sodium sulfate (DSS)-induced colitis [110, 156] (Fig. 3). The phenotype was associated with increased local leukocyte infiltration and higher level of proinflammatory cytokines (TNFα, IL-6, IL-1β, IL-12p40, IL-17), chemokines (CXCL1, CCL2) and prostaglandins [110, 156], and demonstrated the regulatory function of IL-1R8 in epithelial cells.
IL-1R8 was also shown to inhibit the proliferation and survival signals for intestinal epithelial cells in colon crypts, through the regulation of microflora-induced ILR and TLR activation. Indeed, IL-1R8-deficiency was associated with constitutive NFκB and JNK activation and increased expression of Cyclin D1 and Bcl-xL [156]. This phenotype in healthy mice was not confirmed by other studies [110, 157], probably because of animal house-dependent variation of the microflora.
In agreement with the contribution of inflammation in increasing the risk of cancer , IL-1R8 was shown to act as a negative regulator of cancer-related inflammation and therefore cancer development and progression in different murine models of colon cancer. In a model induced by the procarcinogen Azoxymethane (AOM) followed by DSS, IL-1R8-deficiency was associated with increased susceptibility to cancer development, driven by exacerbated intestinal inflammation, as demonstrated by deregulated intestinal permeability, increased in situ production of proinflammatory cytokines, chemokines and prostaglandin E2 and expression of NFκB-induced genes involved in cell survival and proliferation (Bcl-xL and Cyclin D1) [156, 157]. IL-1R8 overexpression in gut epithelial cells rescued the susceptibility of IL-1R8-deficient mice to colitis-associated cancer development, suggesting that the regulatory activity of IL-1R8 in intestinal epithelial cells plays a central role in this model [156].
In the genetic Apcmin/+ model, which mimics the Familial Adenomatous Polyposis syndrome [158], IL-1R8 deficiency caused increased susceptibility to cancer development, due to a more sustained activation of the Akt/mTOR pathway, which is involved in cell cycle progression and consequent genetic instability [121].
Interestingly, in human colorectal cancer specimens, IL-1R8 expression was shown to be impaired compared with healthy tissues [88]. Zhao et al. identified a dominant negative isoform of IL-1R8 (IL-1R8ΔE8), derived from an alternative splicing causing the skipping of the exon 8. IL-1R8ΔE8 was retained in the cytoplasm, showed reduced N-linked glycosylation, and interacted with full-length IL-1R8, acting as an antagonist and suppressing its function. In agreement, gut epithelium-specific IL-1R8 transgenic mice expressing a mutant form of IL-1R8 (IL-1R8N85/101S) that resembles IL-1R8ΔE8 isoform showed increased susceptibility to colon cancer. This indicates that IL-1R8 full functionality in vivo requires proper post-transcriptional modifications and cell membrane localization [88].
3.9 IL-1R8 in Chronic Lymphocytic Leukemia
TLR and ILR signaling are involved CLL development and progression, together with genetic defects and other microenvironmental contributions [159, 160]. IL-1R8-deficient mice exhibited an earlier and more severe appearance of monoclonal B cell expansion and an increased mortality, in the mouse model of CLL (TCL1), mimicking the aggressive variant of human CLL [161]. In line with these results, human malignant B cells expressed lower levels of IL-1R8 mRNA than normal B cells [160, 162, 163].
3.10 IL-1R8 in Platelets
In a recent study it was shown that both human and murine platelets and megakaryocytes expressed high levels of IL-1R8 , which emerged as a key player in the regulation of platelet activation in inflammation and thromboembolism [91] (Fig. 3). Platelets express functional TLRs and IL-1 family receptors (e.g. IL-1R1 and IL-18Rα) [91, 164, 165] and interestingly, IL-1R8-deficiency caused increased platelet/neutrophil aggregate formation, induced by LPS, IL-1β or IL-18 in vitro and upon systemic treatment with LPS in vivo [91]. IL-1R8-deficient platelets displayed higher active α2bβ3 and P-selectin surface expression in basal conditions, suggesting a hyperactivated phenotype. After in vitro stimulation with pro-thrombotic stimuli, Il1r8−/− platelets showed enhanced aggregation amplitude and higher expression of α2bβ3 [91]. Moreover, IL-1R8-deficient mice were more susceptible to ADP-induced pulmonary thromboembolism, as shown by enhanced occlusion of vessels by fibrin clots and systemic levels of soluble P-selectin. IL-1R8-mediated regulation of IL-1 signaling was shown to be responsible for the hyperactivity of platelets in the absence of IL-1R8, since the phenotype was abrogated in Il1r8−/−/Il1r1−/− mice, in line with the reported role of IL-1β in platelet activation [164]. In addition, commensal flora-derived TLR agonists were shown to be also involved in the phenotype, since microflora depletion abrogated the enhanced platelet activation in IL-1R8-deficient mice [91]. In agreement with these results in the mouse, in SIRS/sepsis patients, which exhibit platelet dysfunction [166], IL-1R8 surface expression was significantly downregulated compared to healthy controls and the downregulation correlated with the severity of the disease. Moreover, IL-1R8 expression was shown to be higher in microparticles released from LPS-stimulated platelets or collected from the serum of septic patients compared to controls, suggesting the shedding of the receptor in inflammatory conditions through microparticle release [91]. These results indicate that IL-1R8 contribute to the modulation of platelet activation, aggregation and hetero-aggregation, both in physiological and pathological conditions in vitro and in vivo, and unveil a novel function of IL-1R8 in the regulation of thrombocyte function.
3.11 IL-1R8 in Breast Tumors
Tumor recognition and eradication mediated by the immune system can be escaped through various strategies developed by tumors [167]. Recently, we characterize IL-1R8 in breast cancer as a crucial immunomodulatory molecule. Transformed breast epithelial cells upregulated IL-1R8 expression, which was associated with impaired innate immune and T cell response [107] (Fig. 3). IL-1R8 upregulation in breast tumor cell lines led to the inhibition of IL-1-dependent NFκB activation and expression of pro-inflammatory molecules. In agreement, in a genetic model of breast cancer (MMTV-neu), IL-1R8-deficiency was associated with protection from the development of breast lesions and the number of lung metastasis was reduced. In vitro and in vivo evidences demonstrated that IL-1R8 in tumor cells was responsible for shaping the tumor microenvironment and IL-1R8-deficiency was associated with higher frequency of DCs, NK cells and CD8+ T cells and lower frequency of TAMs [107]. Importantly, RNA sequencing in 1102 clinical samples of breast cancer patients showed that high IL-1R8 expression was associated with a non-T cell inflamed molecular signature, lower expression level of pro-inflammatory cytokines and chemokines, DC and NK cell metagenes, components of the peptide-presenting machinery, cytolytic enzymes and type I IFN-induced genes. Collectively, these data indicate that IL-1R8 emerges as a novel immunomodulatory molecule in breast tumors, affecting the mobilization and activation of immune cells and therefore tumor growth and metastatization [107]. These findings have important therapeutic implications, since the inhibition of IL-1R8 in this context may represent a way to restore the innate immune response and T cell trafficking and activation in the tumor microenvironment.
3.12 IL-1R8 as a Novel Checkpoint in NK Cells
Our group has recently described that IL-1R8 is expressed at high levels in murine and human NK cells and that IL-1R8 expression level increased during NK cell maturation, both in terms of mRNA and protein [90]. IL-1R8-deficient mice displayed a higher frequency and absolute number of NK cells in peripheral blood, higher frequency of mature NK cells (CD11b+CD27− and KLRG1+) in blood, spleen, bone marrow and liver. Moreover, IL-1R8-deficient NK cells showed a more active phenotype, in terms of activating receptor expression (NKG2D, DNAM-1, Ly49H), interferon-γ (IFNγ) and granzyme B production, Fas ligand expression and degranulation [90]. Bone marrow chimeric mice and IL-18 depletion experiments demonstrated that IL-1R8 directly acts on NK cells regulating IL-18, which is a key cytokine involved in NK cell activation [168, 169]. RNASeq and protein phosphorylation analysis showed that IL-18 responsiveness was dramatically different in IL-1R8-deficient NK cells, affecting pathways involved in NK cell activation, degranulation, cytokine production and anti-viral response. Moreover, IL-18-dependent activation of mTOR and JNK pathways was enhanced in IL-1R8-deficient NK cells. In contrast, other candidate pathways (i.e. IL-1 and microflora-driven TLR activation) potentially regulated by IL-1R8 in NK cells were not involved in the IL-1R8-deficient NK cell phenotype. In models of DEN-induced hepatocellular carcinoma, MCA-induced lung metastasis and colon cancer-derived liver metastasis, the disease severity and the number and dimension of metastasis were significantly reduced in Il1r8−/− mice. The protection was dependent on IL-1R8-mediated regulation of IL-18 in NK cells, since depletion of NK cells or IL-18-deficiency totally abrogated the phenotype. Finally, in a model of MCMV infection, Il1r8−/− mice controlled the virus more efficiently and the protection was dependent on enhanced NK cell degranulation and IFNγ production . Importantly, the adoptive transfer of Il1r8−/− NK cells was protective in the metastasis and viral infection models, compared to the treatment with Il1r8+/+ NK cells. Partial silencing of the molecule demonstrated that also in human IL-1R8 regulates NK cell activation, in terms of IFNγ production and CD69 expression [90].
NK cells are generally not credited to play a major role in the control of solid tumors, whereas evidences suggest that they are involved in the control of metastasis [170,171,172]. These results indicate that in addition to metastasis, NK cells have the potential to restrain solid tumors upon checkpoint blockade and in NK cell-enriched sites, such as the liver. Thus, IL-1R8 plays a non-redundant role in the regulation of NK cell development and effector functions, by tuning IL-18 signaling and emerges as a novel checkpoint molecule of NK cell antitumoral and antiviral potential [90] (Fig. 4 ).
IL-1R8 as a novel checkpoint of NK cell anti-tumor and anti-viral activity
IL-1R8 plays a key role in the regulation of NK cell maturation and effector functions, through the modulation of IL-18-induced signaling pathway. IL-1R8 genetic blockade leads to enhanced NK cell anti-tumor, anti-metastatic and anti-viral activity
4 Concluding Remarks
IL-1 family members are central mediators of the inflammatory process and play a key role in both homeostatic differentiation and activation of immune cells. ILR and TLR pathway activation is crucial for the immune surveillance against infectious agents and sterile damages, but given its broad inflammatory potential it needs to be tightly regulated at different levels. Indeed, the balance of positive and negative regulators, accelerators and brakes is a fundamental concept that governs the delicate equilibrium between host defense and detrimental inflammation leading to tissue damage.
IL-1R8 and IL-1R2 emerge as important regulators in various physiological and pathological conditions and the impairment of their function is an escape mechanism developed by pathogens and tumors. Dissecting their cell-specific and context-specific role is essential for the development and improvement of therapeutic strategies.
Fundings
The contribution of the European Commission (TIMER, HEALTH-F4-2011-281608; ESA/ITN, H2020-MSCA-ITN-2015-676129), Ministero dell’Istruzione, dell’Università e della Ricerca (MIUR) (project FIRB RBAP11H2R9; project PRIN2015YYKPNN), and Associazione Italiana Ricerca sul Cancro (AIRC IG-19014 and AIRC 5x1000-9962), CARIPLO (project 2015-0564), is gratefully acknowledged.
References
Dinarello CA (2010) Anti-inflammatory agents: present and future. Cell 140(6):935–950. https://doi.org/10.1016/j.cell.2010.02.043
Garlanda C, Dinarello CA, Mantovani A (2013) The interleukin-1 family: back to the future. Immunity 39(6):1003–1018. https://doi.org/10.1016/j.immuni.2013.11.010
Kang JY, Lee JO (2011) Structural biology of the Toll-like receptor family. Annu Rev Biochem 80:917–941. https://doi.org/10.1146/annurev-biochem-052909-141507
O’Neill LA (2006) How Toll-like receptors signal: what we know and what we don’t know. Curr Opin Immunol 18(1):3–9. https://doi.org/10.1016/j.coi.2005.11.012
O’Neill LA (2008) The interleukin-1 receptor/Toll-like receptor superfamily: 10 years of progress. Immunol Rev 226:10–18. https://doi.org/10.1111/j.1600-065X.2008.00701.x
Dinarello CA (2009) Immunological and inflammatory functions of the interleukin-1 family. Annu Rev Immunol 27:519–550. https://doi.org/10.1146/annurev.immunol.021908.132612
Towne JE, Garka KE, Renshaw BR, Virca GD, Sims JE (2004) Interleukin (IL)-1F6, IL-1F8, and IL-1F9 signal through IL-1Rrp2 and IL-1RAcP to activate the pathway leading to NF-kappaB and MAPKs. J Biol Chem 279(14):13677–13688
Arend WP, Palmer G, Gabay C (2008) IL-1, IL-18, and IL-33 families of cytokines. Immunol Rev 223:20–38
Dinarello C, Arend W, Sims J, Smith D, Blumberg H, O’Neill L, Goldbach-Mansky R, Pizarro T, Hoffman H, Bufler P, Nold M, Ghezzi P, Mantovani A, Garlanda C, Boraschi D, Rubartelli A, Netea M, van der Meer J, Joosten L, Mandrup-Poulsen T, Donath M, Lewis E, Pfeilschifter J, Martin M, Kracht M, Muehl H, Novick D, Lukic M, Conti B, Solinger A, Kelk P, van de Veerdonk F, Gabel C (2010) IL-1 family nomenclature. Nat Immunol 11(11):973. https://doi.org/10.1038/ni1110-973
Krelin Y, Voronov E, Dotan S, Elkabets M, Reich E, Fogel M, Huszar M, Iwakura Y, Segal S, Dinarello CA, Apte RN (2007) Interleukin-1beta-driven inflammation promotes the development and invasiveness of chemical carcinogen-induced tumors. Cancer Res 67(3):1062–1071. https://doi.org/10.1158/0008-5472.CAN-06-2956
Liew FY, Pitman NI, McInnes IB (2010) Disease-associated functions of IL-33: the new kid in the IL-1 family. Nat Rev Immunol 10(2):103–110. https://doi.org/10.1038/nri2692
Dinarello CA (2011) Interleukin-1 in the pathogenesis and treatment of inflammatory diseases. Blood 117(14):3720–3732. https://doi.org/10.1182/blood-2010-07-273417
Towne JE, Sims JE (2012) IL-36 in psoriasis. Curr Opin Pharmacol 12(4):486–490. https://doi.org/10.1016/j.coph.2012.02.009
Dinarello CA, Simon A, van der Meer JW (2012) Treating inflammation by blocking interleukin-1 in a broad spectrum of diseases. Nat Rev Drug Discov 11(8):633–652. https://doi.org/10.1038/nrd3800
Ridker PM, Everett BM, Thuren T, MacFadyen JG, Chang WH, Ballantyne C, Fonseca F, Nicolau J, Koenig W, Anker SD, Kastelein JJP, Cornel JH, Pais P, Pella D, Genest J, Cifkova R, Lorenzatti A, Forster T, Kobalava Z, Vida-Simiti L, Flather M, Shimokawa H, Ogawa H, Dellborg M, Rossi PRF, Troquay RPT, Libby P, Glynn RJ, CANTOS Trial Group (2017) Antiiflammatory therapy with canakinumab for atherosclerotic disease. N Engl J Med 377(12):1119–1131. https://doi.org/10.1056/NEJMoa1707914
Ridker PM, MacFadyen JG, Thuren T, Everett BM, Libby P, Glynn RJ, CANTOS Trial Group (2017) Effect of interleukin-1beta inhibition with canakinumab on incident lung cancer in patients with atherosclerosis: exploratory results from a randomised, double-blind, placebo-controlled trial. Lancet 390(10105):1833–1842. https://doi.org/10.1016/S0140-6736(17)32247-X
O’Neill LA, Sheedy FJ, McCoy CE (2011) MicroRNAs: the fine-tuners of Toll-like receptor signalling. Nat Rev Immunol 11(3):163–175. https://doi.org/10.1038/nri2957
Copeland NG, Silan CM, Kingsley DM, Jenkins NA, Cannizzaro LA, Croce CM, Huebner K, Sims JE (1991) Chromosomal location of murine and human IL-1 receptor genes. Genomics 9(1):44–50
Morrison RN, Young ND, Nowak BF (2012) Description of an Atlantic salmon (Salmo salar L.) type II interleukin-1 receptor cDNA and analysis of interleukin-1 receptor expression in amoebic gill disease-affected fish. Fish Shellfish Immunol 32(6):1185–1190. https://doi.org/10.1016/j.fsi.2012.03.005
Colotta F, Re F, Muzio M, Bertini R, Polentarutti N, Sironi M, Giri JG, Dower SK, Sims JE, Mantovani A (1993) Interleukin-1 type II receptor: a decoy target for IL-1 that is regulated by IL-4. Science 261(5120):472–475
McMahan CJ, Slack JL, Mosley B, Cosman D, Lupton SD, Brunton LL, Grubin CE, Wignall JM, Jenkins NA, Brannan CI et al (1991) A novel IL-1 receptor, cloned from B cells by mammalian expression, is expressed in many cell types. EMBO J 10(10):2821–2832
Orlando S, Sironi M, Bianchi G, Drummond AH, Boraschi D, Yabes D, Mantovani A (1997) Role of metalloproteases in the release of the IL-1 type II decoy receptor. J Biol Chem 272(50):31764–31769
Lorenzen I, Lokau J, Dusterhoft S, Trad A, Garbers C, Scheller J, Rose-John S, Grotzinger J (2012) The membrane-proximal domain of A Disintegrin and Metalloprotease 17 (ADAM17) is responsible for recognition of the interleukin-6 receptor and interleukin-1 receptor II. FEBS Lett 586(8):1093–1100. https://doi.org/10.1016/j.febslet.2012.03.012
Uchikawa S, Yoda M, Tohmonda T, Kanaji A, Matsumoto M, Toyama Y, Horiuchi K (2015) ADAM17 regulates IL-1 signaling by selectively releasing IL-1 receptor type 2 from the cell surface. Cytokine 71(2):238–245. https://doi.org/10.1016/j.cyto.2014.10.032
Martin P, Palmer G, Vigne S, Lamacchia C, Rodriguez E, Talabot-Ayer D, Rose-John S, Chalaris A, Gabay C (2013) Mouse neutrophils express the decoy type 2 interleukin-1 receptor (IL-1R2) constitutively and in acute inflammatory conditions. J Leuk Biol 94(4):791–802. https://doi.org/10.1189/jlb.0113035
Giri JG, Wells J, Dower SK, McCall CE, Guzman RN, Slack J, Bird TA, Shanebeck K, Grabstein KH, Sims JE et al (1994) Elevated levels of shed type II IL-1 receptor in sepsis. Potential role for type II receptor in regulation of IL-1 responses. J Immunol 153(12):5802–5809
Colotta F, Orlando S, Fadlon EJ, Sozzani S, Matteucci C, Mantovani A (1995) Chemoattractants induce rapid release of the interleukin 1 type II decoy receptor in human polymorphonuclear cells. J Exp Med 181(6):2181–2186
Orlando S, Matteucci C, Fadlon EJ, Buurman WA, Bardella MT, Colotta F, Introna M, Mantovani A (1997) TNF-alpha, unlike other pro- and anti-inflammatory cytokines, induces rapid release of the IL-1 type II decoy receptor in human myelomonocytic cells. J Immunol 158(8):3861–3868
Liu C, Hart RP, Liu XJ, Clevenger W, Maki RA, De Souza EB (1996) Cloning and characterization of an alternatively processed human type II interleukin-1 receptor mRNA. J Biol Chem 271(34):20965–20972
Wang D, Zhang S, Li L, Liu X, Mei K, Wang X (2010) Structural insights into the assembly and activation of IL-1beta with its receptors. Nat Immunol 11(10):905–911. https://doi.org/10.1038/ni.1925
Lang D, Knop J, Wesche H, Raffetseder U, Kurrle R, Boraschi D, Martin MU (1998) The type II IL-1 receptor interacts with the IL-1 receptor accessory protein: a novel mechanism of regulation of IL-1 responsiveness. J Immunol 161(12):6871–6877
Malinowsky D, Lundkvist J, Laye S, Bartfai T (1998) Interleukin-1 receptor accessory protein interacts with the type II interleukin-1 receptor. FEBS Lett 429(3):299–302
Laye S, Lundkvist J, Bartfai T (1998) Human/mouse interleukin-1 receptor/receptor accessory protein interactions in IL-1beta-induced NFkappaB activation. FEBS Lett 429(3):307–311
Re F, Sironi M, Muzio M, Matteucci C, Introna M, Orlando S, Penton-Rol G, Dower SK, Sims JE, Colotta F, Mantovani A (1996) Inhibition of interleukin-1 responsiveness by type II receptor gene transfer: a surface “receptor” with anti-interleukin-1 function. J Exp Med 183(4):1841–1850
Smith DE, Hanna R, Della F, Moore H, Chen H, Farese AM, MacVittie TJ, Virca GD, Sims JE (2003) The soluble form of IL-1 receptor accessory protein enhances the ability of soluble type II IL-1 receptor to inhibit IL-1 action. Immunity 18(1):87–96
Kawaguchi Y, Nishimagi E, Tochimoto A, Kawamoto M, Katsumata Y, Soejima M, Kanno T, Kamatani N, Hara M (2006) Intracellular IL-1alpha-binding proteins contribute to biological functions of endogenous IL-1alpha in systemic sclerosis fibroblasts. Proc Natl Acad Sci U S A 103(39):14501–14506. https://doi.org/10.1073/pnas.0603545103
Zheng Y, Humphry M, Maguire JJ, Bennett MR, Clarke MC (2013) Intracellular interleukin-1 receptor 2 binding prevents cleavage and activity of interleukin-1alpha, controlling necrosis-induced sterile inflammation. Immunity 38(2):285–295. https://doi.org/10.1016/j.immuni.2013.01.008
Colotta F, Saccani S, Giri JG, Dower SK, Sims JE, Introna M, Mantovani A (1996) Regulated expression and release of the IL-1 decoy receptor in human mononuclear phagocytes. J Immunol 156(7):2534–2541
Martinez FO, Gordon S, Locati M, Mantovani A (2006) Transcriptional profiling of the human monocyte-to-macrophage differentiation and polarization: new molecules and patterns of gene expression. J Immunol 177(10):7303–7311
De Simone M, Arrigoni A, Rossetti G, Gruarin P, Ranzani V, Politano C, Bonnal RJ, Provasi E, Sarnicola ML, Panzeri I, Moro M, Crosti M, Mazzara S, Vaira V, Bosari S, Palleschi A, Santambrogio L, Bovo G, Zucchini N, Totis M, Gianotti L, Cesana G, Perego RA, Maroni N, Pisani Ceretti A, Opocher E, De Francesco R, Geginat J, Stunnenberg HG, Abrignani S, Pagani M (2016) Transcriptional landscape of human tissue lymphocytes unveils uniqueness of tumor-infiltrating T regulatory cells. Immunity 45(5):1135–1147. https://doi.org/10.1016/j.immuni.2016.10.021
Plitas G, Konopacki C, Wu K, Bos PD, Morrow M, Putintseva EV, Chudakov DM, Rudensky AY (2016) Regulatory T cells exhibit distinct features in human breast cancer. Immunity 45(5):1122–1134. https://doi.org/10.1016/j.immuni.2016.10.032
Drevets DA, Schawang JE, Mandava VK, Dillon MJ, Leenen PJ (2010) Severe Listeria monocytogenes infection induces development of monocytes with distinct phenotypic and functional features. J Immunol 185(4):2432–2441. https://doi.org/10.4049/jimmunol.1000486
Hofkens W, Schelbergen R, Storm G, van den Berg WB, van Lent PL (2013) Liposomal targeting of prednisolone phosphate to synovial lining macrophages during experimental arthritis inhibits M1 activation but does not favor M2 differentiation. PLoS One 8(2):e54016. https://doi.org/10.1371/journal.pone.0054016
Fettelschoss A, Kistowska M, LeibundGut-Landmann S, Beer HD, Johansen P, Senti G, Contassot E, Bachmann MF, French LE, Oxenius A, Kundig TM (2011) Inflammasome activation and IL-1beta target IL-1alpha for secretion as opposed to surface expression. Proc Natl Acad Sci U S A 108(44):18055–18060. https://doi.org/10.1073/pnas.1109176108
Pinteaux E, Parker LC, Rothwell NJ, Luheshi GN (2002) Expression of interleukin-1 receptors and their role in interleukin-1 actions in murine microglial cells. J Neurochem 83(4):754–763
McNamee EN, Ryan KM, Kilroy D, Connor TJ (2010) Noradrenaline induces IL-1ra and IL-1 type II receptor expression in primary glial cells and protects against IL-1beta-induced neurotoxicity. Eur J Pharmacol 626(2–3):219–228. https://doi.org/10.1016/j.ejphar.2009.09.054
Trebec DP, Chandra D, Gramoun A, Li K, Heersche JN, Manolson MF (2007) Increased expression of activating factors in large osteoclasts could explain their excessive activity in osteolytic diseases. J Cell Biochem 101(1):205–220. https://doi.org/10.1002/jcb.21171
Pou J, Martinez-Gonzalez J, Rebollo A, Rodriguez C, Rodriguez-Calvo R, Martin-Fuentes P, Cenarro A, Civeira F, Laguna JC, Alegret M (2011) Type II interleukin-1 receptor expression is reduced in monocytes/macrophages and atherosclerotic lesions. Biochim Biophys Acta 1811(9):556–563. https://doi.org/10.1016/j.bbalip.2011.05.014
Iwai H, Inaba M (2012) Fetal thymus graft prevents age-related hearing loss and up regulation of the IL-1 receptor type II gene in CD4(+) T cells. J Neuroimmunol 250(1–2):1–8. https://doi.org/10.1016/j.jneuroim.2012.05.007
Tran DQ, Andersson J, Hardwick D, Bebris L, Illei GG, Shevach EM (2009) Selective expression of latency-associated peptide (LAP) and IL-1 receptor type I/II (CD121a/CD121b) on activated human FOXP3+ regulatory T cells allows for their purification from expansion cultures. Blood 113(21):5125–5133. https://doi.org/10.1182/blood-2009-01-199950
Spriggs MK, Nevens PJ, Grabstein K, Dower SK, Cosman D, Armitage RJ, McMahan CJ, Sims JE (1992) Molecular characterization of the interleukin-1 receptor (IL-1R) on monocytes and polymorphonuclear cells. Cytokine 4(2):90–95
Re F, Muzio M, De Rossi M, Polentarutti N, Giri JG, Mantovani A, Colotta F (1994) The type II “receptor” as a decoy target for interleukin 1 in polymorphonuclear leukocytes: characterization of induction by dexamethasone and ligand binding properties of the released decoy receptor. J Exp Med 179(2):739–743
Colotta F, Re F, Muzio M, Polentarutti N, Minty A, Caput D, Ferrara P, Mantovani A (1994) Interleukin-13 induces expression and release of interleukin-1 decoy receptor in human polymorphonuclear cells. J Biol Chem 269(17):12403–12406
Dickensheets HL, Donnelly RP (1997) IFN-gamma and IL-10 inhibit induction of IL-1 receptor type I and type II gene expression by IL-4 and IL-13 in human monocytes. J Immunol 159(12):6226–6233
Kalliolias GD, Gordon RA, Ivashkiv LB (2010) Suppression of TNF-alpha and IL-1 signaling identifies a mechanism of homeostatic regulation of macrophages by IL-27. J Immunol 185(11):7047–7056. https://doi.org/10.4049/jimmunol.1001290
Daun JM, Ball RW, Burger HR, Cannon JG (1999) Aspirin-induced increases in soluble IL-1 receptor type II concentrations in vitro and in vivo. J Leukoc Biol 65(6):863–866
Penton-Rol G, Orlando S, Polentarutti N, Bernasconi S, Muzio M, Introna M, Mantovani A (1999) Bacterial lipopolysaccharide causes rapid shedding, followed by inhibition of mRNA expression, of the IL-1 type II receptor, with concomitant up-regulation of the type I receptor and induction of incompletely spliced transcripts. J Immunol 162(5):2931–2938
Docagne F, Campbell SJ, Bristow AF, Poole S, Vigues S, Guaza C, Perry VH, Anthony DC (2005) Differential regulation of type I and type II interleukin-1 receptors in focal brain inflammation. Eur J Neurosci 21(5):1205–1214. https://doi.org/10.1111/j.1460-9568.2005.03965.x
Attur MG, Dave M, Cipolletta C, Kang P, Goldring MB, Patel IR, Abramson SB, Amin AR (2000) Reversal of autocrine and paracrine effects of interleukin 1 (IL-1) in human arthritis by type II IL-1 decoy receptor. Potential for pharmacological intervention. J Biol Chem 275(51):40307–40315. https://doi.org/10.1074/jbc.M002721200
Alcami A, Koszinowski UH (2000) Viral mechanisms of immune evasion. Immunol Today 21(9):447–455
Giai C, Gonzalez CD, Sabbione F, Garofalo A, Ojeda D, Sordelli DO, Trevani AS, Gomez MI (2016) Staphylococcus aureus induces shedding of IL-1RII in monocytes and neutrophils. J Innate Immun 8(3):284–298. https://doi.org/10.1159/000443663
Khoufache K, Bondza PK, Harir N, Daris M, Leboeuf M, Mailloux J, Lemyre M, Foster W, Akoum A (2012) Soluble human IL-1 receptor type 2 inhibits ectopic endometrial tissue implantation and growth: identification of a novel potential target for endometriosis treatment. Am J Pathol 181(4):1197–1205. https://doi.org/10.1016/j.ajpath.2012.06.022
Simeoni E, Dudler J, Fleury S, Li J, Pagnotta M, Pascual M, von Segesser LK, Vassalli G (2007) Gene transfer of a soluble IL-1 type 2 receptor-Ig fusion protein improves cardiac allograft survival in rats. Eur J Cardiothorac Surg 31(2):222–228. https://doi.org/10.1016/j.ejcts.2006.10.042
Rauschmayr T, Groves RW, Kupper TS (1997) Keratinocyte expression of the type 2 interleukin 1 receptor mediates local and specific inhibition of interleukin 1-mediated inflammation. Proc Natl Acad Sci U S A 94(11):5814–5819
Chang H, Wang Y, Wu W, Li G, Hanawa H, Zou J (2013) Hydrodynamics-based delivery of an interleukin-1 receptor II fusion gene ameliorates rat autoimmune myocarditis by inhibiting IL-1 and Th17 cell polarization. Int J Mol Med 31(4):833–840. https://doi.org/10.3892/ijmm.2013.1276
Bessis N, Guery L, Mantovani A, Vecchi A, Sims JE, Fradelizi D, Boissier MC (2000) The type II decoy receptor of IL-1 inhibits murine collagen-induced arthritis. Eur J Immunol 30(3):867–875. https://doi.org/10.1002/1521-4141(200003)30:3<867::AID-IMMU867>3.0.CO;2-M
Dawson J, Engelhardt P, Kastelic T, Cheneval D, MacKenzie A, Ramage P (1999) Effects of soluble interleukin-1 type II receptor on rabbit antigen-induced arthritis: clinical, biochemical and histological assessment. Rheumatology (Oxford) 38(5):401–406
Martin P, Palmer G, Rodriguez E, Seemayer CA, Palomo J, Talabot-Ayer D, Gabay C (2017) Deficiency in IL-1 receptor type 2 aggravates K/BxN serum transfer-induced arthritis in mice but has no impact on systemic inflammatory responses. J Immunol 198(7):2916–2926. https://doi.org/10.4049/jimmunol.1600855
Lamacchia C, Palmer G, Bischoff L, Rodriguez E, Talabot-Ayer D, Gabay C (2010) Distinct roles of hepatocyte- and myeloid cell-derived IL-1 receptor antagonist during endotoxemia and sterile inflammation in mice. J Immunol 185(4):2516–2524. https://doi.org/10.4049/jimmunol.1000872
Hirsch E, Irikura VM, Paul SM, Hirsh D (1996) Functions of interleukin 1 receptor antagonist in gene knockout and overproducing mice. Proc Natl Acad Sci U S A 93(20):11008–11013
Ritvo PG, Churlaud G, Quiniou V, Florez L, Brimaud F, Fourcade G, Mariotti-Ferrandiz E, Klatzmann D (2017) Tfr cells lack IL-2Ralpha but express decoy IL-1R2 and IL-1Ra and suppress the IL-1-dependent activation of Tfh cells. Sci Immunol 2(15). https://doi.org/10.1126/sciimmunol.aan0368
Kovach MA, Stringer KA, Bunting R, Wu X, San Mateo L, Newstead MW, Paine R, Standiford TJ (2015) Microarray analysis identifies IL-1 receptor type 2 as a novel candidate biomarker in patients with acute respiratory distress syndrome. Respir Res 16:29. https://doi.org/10.1186/s12931-015-0190-x
Dujmovic I, Mangano K, Pekmezovic T, Quattrocchi C, Mesaros S, Stojsavljevic N, Nicoletti F, Drulovic J (2009) The analysis of IL-1 beta and its naturally occurring inhibitors in multiple sclerosis: the elevation of IL-1 receptor antagonist and IL-1 receptor type II after steroid therapy. J Neuroimmunol 207(1–2):101–106. https://doi.org/10.1016/j.jneuroim.2008.11.004
Garlind A, Brauner A, Hojeberg B, Basun H, Schultzberg M (1999) Soluble interleukin-1 receptor type II levels are elevated in cerebrospinal fluid in Alzheimer’s disease patients. Brain Res 826(1):112–116
Arend WP, Malyak M, Smith MF Jr, Whisenand TD, Slack JL, Sims JE, Giri JG, Dower SK (1994) Binding of IL-1 alpha, IL-1 beta, and IL-1 receptor antagonist by soluble IL-1 receptors and levels of soluble IL-1 receptors in synovial fluids. J Immunol 153(10):4766–4774
Jouvenne P, Vannier E, Dinarello CA, Miossec P (1998) Elevated levels of soluble interleukin-1 receptor type II and interleukin-1 receptor antagonist in patients with chronic arthritis: correlations with markers of inflammation and joint destruction. Arthritis Rheum 41(6):1083–1089. https://doi.org/10.1002/1529-0131(199806)41:6<1083::AID-ART15>3.0.CO;2-9
van der Torren CR, Verrijn Stuart AA, Lee D, Meerding J, van de Velde U, Pipeleers D, Gillard P, Keymeulen B, de Jager W, Roep BO (2016) Serum cytokines as biomarkers in islet cell transplantation for type 1 diabetes. PLoS One 11(1):e0146649. https://doi.org/10.1371/journal.pone.0146649
Mora-Buch R, Dotti I, Planell N, Calderon-Gomez E, Jung P, Masamunt MC, Llach J, Ricart E, Batlle E, Panes J, Salas A (2015) Epithelial IL-1R2 acts as a homeostatic regulator during remission of ulcerative colitis. Mucosal Immunol. https://doi.org/10.1038/mi.2015.108
Meusch U, Klingner M, Baerwald C, Rossol M, Wagner U (2013) Deficient spontaneous in vitro apoptosis and increased tmTNF reverse signaling-induced apoptosis of monocytes predict suboptimal therapeutic response of rheumatoid arthritis to TNF inhibition. Arthritis Res Ther 15(6):R219. https://doi.org/10.1186/ar4416
Kuznetsov NV, Zargari A, Gielen AW, von Stein OD, Musch E, Befrits R, Lofberg R, von Stein P (2014) Biomarkers can predict potential clinical responders to DIMS0150 a Toll-like receptor 9 agonist in ulcerative colitis patients. BMC Gastroenterol 14:79. https://doi.org/10.1186/1471-230X-14-79
Debets R, Hegmans JP, Croughs P, Troost RJ, Prins JB, Benner R, Prens EP (1997) The IL-1 system in psoriatic skin: IL-1 antagonist sphere of influence in lesional psoriatic epidermis. J Immunol 158(6):2955–2963
Ruckert F, Dawelbait G, Winter C, Hartmann A, Denz A, Ammerpohl O, Schroeder M, Schackert HK, Sipos B, Kloppel G, Kalthoff H, Saeger HD, Pilarsky C, Grutzmann R (2010) Examination of apoptosis signaling in pancreatic cancer by computational signal transduction analysis. PLoS One 5(8):e12243. https://doi.org/10.1371/journal.pone.0012243
Ricote M, Garcia-Tunon I, Bethencourt FR, Fraile B, Paniagua R, Royuela M (2004) Interleukin-1 (IL-1alpha and IL-1beta) and its receptors (IL-1RI, IL-1RII, and IL-1Ra) in prostate carcinoma. Cancer 100(7):1388–1396. https://doi.org/10.1002/cncr.20142
Laios A, O’Toole SA, Flavin R, Martin C, Ring M, Gleeson N, D’Arcy T, McGuinness EP, Sheils O, Sheppard BL, O’ Leary JJ (2008) An integrative model for recurrence in ovarian cancer. Mol Cancer 7:8. https://doi.org/10.1186/1476-4598-7-8
Keita M, AinMelk Y, Pelmus M, Bessette P, Aris A (2011) Endometrioid ovarian cancer and endometriotic cells exhibit the same alteration in the expression of interleukin-1 receptor II: to a link between endometriosis and endometrioid ovarian cancer. J Obstet Gynaecol Res 37(2):99–107. https://doi.org/10.1111/j.1447-0756.2010.01320.x
Thomassen E, Renshaw BR, Sims JE (1999) Identification and characterization of SIGIRR, a molecule representing a novel subtype of the IL-1R superfamily. Cytokine 11(6):389–399. https://doi.org/10.1006/cyto.1998.0452
Riva F, Polentarutti N, Tribbioli G, Mantovani A, Garlanda C, Turin L (2009) The expression pattern of TIR8 is conserved among vertebrates. Vet Immunol Immunopathol 131(1–2):44–49. https://doi.org/10.1016/j.vetimm.2009.03.009
Zhao J, Bulek K, Gulen MF, Zepp JA, Karagkounis G, Martin BN, Zhou H, Yu M, Liu X, Huang E, Fox PL, Kalady MF, Markowitz SD, Li X (2015) Human colon tumors express a dominant-negative form of SIGIRR that promotes inflammation and colitis-associated colon cancer in mice. Gastroenterology 149(7):1860–1871.e1868. https://doi.org/10.1053/j.gastro.2015.08.051
Polentarutti N, Rol GP, Muzio M, Bosisio D, Camnasio M, Riva F, Zoja C, Benigni A, Tomasoni S, Vecchi A, Garlanda C, Mantovani A (2003) Unique pattern of expression and inhibition of IL-1 signaling by the IL-1 receptor family member TIR8/SIGIRR. Eur Cytokine Netw 14(4):211–218
Molgora M, Bonavita E, Ponzetta A, Riva F, Barbagallo M, Jaillon S, Popovic B, Bernardini G, Magrini E, Gianni F, Zelenay S, Jonjic S, Santoni A, Garlanda C, Mantovani A (2017) IL-1R8 is a checkpoint in NK cells regulating anti-tumour and anti-viral activity. Nature 551(7678):110–114. https://doi.org/10.1038/nature24293
Anselmo A, Riva F, Gentile S, Soldani C, Barbagallo M, Mazzon C, Feruglio F, Polentarutti N, Somma P, Carullo P, Angelini C, Bacci M, Mendolicchio GL, Voza A, Nebuloni M, Mantovani A, Garlanda C (2016) Expression and function of IL-1R8 (TIR8/SIGIRR): a regulatory member of the IL-1 receptor family in platelets. Cardiovasc Res 111(4):373–384. https://doi.org/10.1093/cvr/cvw162
Veliz Rodriguez T, Moalli F, Polentarutti N, Paroni M, Bonavita E, Anselmo A, Nebuloni M, Mantero S, Jaillon S, Bragonzi A, Mantovani A, Riva F, Garlanda C (2012) Role of Toll interleukin-1 receptor (IL-1R) 8, a negative regulator of IL-1R/Toll-like receptor signaling, in resistance to acute Pseudomonas aeruginosa lung infection. Infect Immun 80(1):100–109. https://doi.org/10.1128/IAI.05695-11
Gopal R, Birdsell D, Monroy FP (2008) Regulation of Toll-like receptors in intestinal epithelial cells by stress and Toxoplasma gondii infection. Parasite Immunol 30(11–12):563–576. https://doi.org/10.1111/j.1365-3024.2008.01055.x
Leemans JC, Butter LM, Teske GJ, Stroo I, Pulskens WP, Florquin S (2012) The Toll interleukin-1 receptor (IL-1R) 8/single Ig domain IL-1R-related molecule modulates the renal response to bacterial infection. Infect Immun 80(11):3812–3820. https://doi.org/10.1128/IAI.00422-12
Nanthakumar N, Meng D, Goldstein AM, Zhu W, Lu L, Uauy R, Llanos A, Claud EC, Walker WA (2011) The mechanism of excessive intestinal inflammation in necrotizing enterocolitis: an immature innate immune response. PLoS One 6(3):e17776. https://doi.org/10.1371/journal.pone.0017776
Batliwalla FM, Li W, Ritchlin CT, Xiao X, Brenner M, Laragione T, Shao T, Durham R, Kemshetti S, Schwarz E, Coe R, Kern M, Baechler EC, Behrens TW, Gregersen PK, Gulko PS (2005) Microarray analyses of peripheral blood cells identifies unique gene expression signature in psoriatic arthritis. Mol Med 11(1–12):21–29. https://doi.org/10.2119/2006-00003.Gulko
Ragnarsdottir B, Samuelsson M, Gustafsson MC, Leijonhufvud I, Karpman D, Svanborg C (2007) Reduced Toll-like receptor 4 expression in children with asymptomatic bacteriuria. J Infect Dis 196(3):475–484. https://doi.org/10.1086/518893
Kadota C, Ishihara S, Aziz MM, Rumi MA, Oshima N, Mishima Y, Moriyama I, Yuki T, Amano Y, Kinoshita Y (2010) Down-regulation of single immunoglobulin interleukin-1R-related molecule (SIGIRR)/TIR8 expression in intestinal epithelial cells during inflammation. Clin Exp Immunol 162(2):348–361
Khan MA, Steiner TS, Sham HP, Bergstrom KS, Huang JT, Assi K, Salh B, Tai IT, Li X, Vallance BA (2010) The single IgG IL-1-related receptor controls TLR responses in differentiated human intestinal epithelial cells. J Immunol 184(5):2305–2313. https://doi.org/10.4049/jimmunol.0900021
Li D, Zhang X, Chen B (2015) SIGIRR participates in negative regulation of LPS response and tolerance in human bladder epithelial cells. BMC Immunol 16:73. https://doi.org/10.1186/s12865-015-0137-5
Ueno-Shuto K, Kato K, Tasaki Y, Sato M, Sato K, Uchida Y, Sakai H, Ono T, Suico MA, Mitsutake K, Tokutomi N, Kai H, Shuto T (2014) Lipopolysaccharide decreases single immunoglobulin interleukin-1 receptor-related molecule (SIGIRR) expression by suppressing specificity protein 1 (Sp1) via the Toll-like receptor 4 (TLR4)-p38 pathway in monocytes and neutrophils. J Biol Chem 289(26):18097–18109. https://doi.org/10.1074/jbc.M113.532093
Adib-Conquy M, Adrie C, Fitting C, Gattolliat O, Beyaert R, Cavaillon JM (2006) Up-regulation of MyD88s and SIGIRR, molecules inhibiting Toll-like receptor signaling, in monocytes from septic patients. Crit Care Med 34(9):2377–2385. https://doi.org/10.1097/01.CCM.0000233875.93866.88
Costello DA, Carney DG, Lynch MA (2015) Alpha-TLR2 antibody attenuates the Abeta-mediated inflammatory response in microglia through enhanced expression of SIGIRR. Brain Behav Immun 46:70–79. https://doi.org/10.1016/j.bbi.2015.01.005
Villena J, Suzuki R, Fujie H, Chiba E, Takahashi T, Tomosada Y, Shimazu T, Aso H, Ohwada S, Suda Y, Ikegami S, Itoh H, Alvarez S, Saito T, Kitazawa H (2012) Immunobiotic Lactobacillus jensenii modulates the Toll-like receptor 4-induced inflammatory response via negative regulation in porcine antigen-presenting cells. Clin Vaccine Immunol 19(7):1038–1053. https://doi.org/10.1128/CVI.00199-12
Davies JM, MacSharry J, Shanahan F (2010) Differential regulation of Toll-like receptor signalling in spleen and Peyer’s patch dendritic cells. Immunology 131(3):438–448. https://doi.org/10.1111/j.1365-2567.2010.03317.x
Vilia MG, Fonte E, Veliz Rodriguez T, Tocchetti M, Ranghetti P, Scarfo L, Papakonstantinou N, Ntoufa S, Stamatopoulos K, Ghia P, Muzio M (2017) The inhibitory receptor Toll interleukin-1R 8 (TIR8/IL-1R8/SIGIRR) is downregulated in chronic lymphocytic leukemia. Leuk Lymphoma 58(10):2419–2425. https://doi.org/10.1080/10428194.2017.1295142
Campesato LF, Silva APM, Cordeiro L, Correa BR, Navarro FCP, Zanin RF, Marcola M, Inoue LT, Duarte ML, Molgora M, Pasqualini F, Massara M, Galante P, Barroso-Sousa R, Polentarutti N, Riva F, Costa ET, Mantovani A, Garlanda C, Camargo AA (2017) High IL-1R8 expression in breast tumors promotes tumor growth and contributes to impaired antitumor immunity. Oncotarget 8(30):49470–49483. https://doi.org/10.18632/oncotarget.17713
Vilia MG, Tocchetti M, Fonte E, Sana I, Muzio M (2017) Characterization of a long isoform of IL-1R8 (TIR8/SIGIRR). Eur Cytokine Netw 28(2):63–69. https://doi.org/10.1684/ecn.2017.0395
Wald D, Qin J, Zhao Z, Qian Y, Naramura M, Tian L, Towne J, Sims JE, Stark GR, Li X (2003) SIGIRR, a negative regulator of Toll-like receptor-interleukin 1 receptor signaling. Nat Immunol 4(9):920–927. https://doi.org/10.1038/ni968
Garlanda C, Riva F, Polentarutti N, Buracchi C, Sironi M, De Bortoli M, Muzio M, Bergottini R, Scanziani E, Vecchi A, Hirsch E, Mantovani A (2004) Intestinal inflammation in mice deficient in Tir8, an inhibitory member of the IL-1 receptor family. Proc Natl Acad Sci U S A 101(10):3522–3526. https://doi.org/10.1073/pnas.0308680101
Qin J, Qian Y, Yao J, Grace C, Li X (2005) SIGIRR inhibits interleukin-1 receptor- and Toll-like receptor 4-mediated signaling through different mechanisms. J Biol Chem 280(26):25233–25241. https://doi.org/10.1074/jbc.M501363200
Lech M, Garlanda C, Mantovani A, Kirschning CJ, Schlondorff D, Anders HJ (2007) Different roles of TiR8/Sigirr on Toll-like receptor signaling in intrarenal antigen-presenting cells and tubular epithelial cells. Kidney Int 72(2):182–192. https://doi.org/10.1038/sj.ki.5002293
Bulek K, Swaidani S, Qin J, Lu Y, Gulen MF, Herjan T, Min B, Kastelein RA, Aronica M, Kosz-Vnenchak M, Li X (2009) The essential role of single Ig IL-1 receptor-related molecule/Toll IL-1R8 in regulation of Th2 immune response. J Immunol 182(5):2601–2609. https://doi.org/10.4049/jimmunol.0802729
Tomasoni R, Morini R, Lopez-Atalaya JP, Corradini I, Canzi A, Rasile M, Mantovani C, Pozzi D, Garlanda C, Mantovani A, Menna E, Barco A, Matteoli M (2017) Lack of IL-1R8 in neurons causes hyperactivation of IL-1 receptor pathway and induces MECP2-dependent synaptic defects. Elife 6. https://doi.org/10.7554/eLife.21735
Li X, Qin J (2005) Modulation of Toll-interleukin 1 receptor mediated signaling. J Mol Med (Berl) 83(4):258–266. https://doi.org/10.1007/s00109-004-0622-4
Gong J, Wei T, Stark RW, Jamitzky F, Heckl WM, Anders HJ, Lech M, Rossle SC (2010) Inhibition of Toll-like receptors TLR4 and 7 signaling pathways by SIGIRR: a computational approach. J Struct Biol 169(3):323–330. https://doi.org/10.1016/j.jsb.2009.12.007
Guven-Maiorov E, Keskin O, Gursoy A, Nussinov R (2015) A structural view of negative regulation of the Toll-like receptor-mediated inflammatory pathway. Biophys J 109(6):1214–1226. https://doi.org/10.1016/j.bpj.2015.06.048
Garlanda C, Anders HJ, Mantovani A (2009) TIR8/SIGIRR: an IL-1R/TLR family member with regulatory functions in inflammation and T cell polarization. Trends Immunol 30(9):439–446. https://doi.org/10.1016/j.it.2009.06.001
Drexler SK, Kong P, Inglis J, Williams RO, Garlanda C, Mantovani A, Yazdi AS, Brennan F, Feldmann M, Foxwell BM (2010) SIGIRR/TIR-8 is an inhibitor of Toll-like receptor signaling in primary human cells and regulates inflammation in models of rheumatoid arthritis. Arthritis Rheum 62(8):2249–2261. https://doi.org/10.1002/art.27517
Gulen MF, Kang Z, Bulek K, Youzhong W, Kim TW, Chen Y, Altuntas CZ, Sass Bak-Jensen K, McGeachy MJ, Do JS, Xiao H, Delgoffe GM, Min B, Powell JD, Tuohy VK, Cua DJ, Li X (2010) The receptor SIGIRR suppresses Th17 cell proliferation via inhibition of the interleukin-1 receptor pathway and mTOR kinase activation. Immunity 32(1):54–66. https://doi.org/10.1016/j.immuni.2009.12.003
Xiao H, Yin W, Khan MA, Gulen MF, Zhou H, Sham HP, Jacobson K, Vallance BA, Li X (2010) Loss of single immunoglobulin interlukin-1 receptor-related molecule leads to enhanced colonic polyposis in Apc(min) mice. Gastroenterology 139(2):574–585. https://doi.org/10.1053/j.gastro.2010.04.043
Patterson NJ, Werling D (2013) To con protection: TIR-domain containing proteins (Tcp) and innate immune evasion. Vet Immunol Immunopathol 155(3):147–154. https://doi.org/10.1016/j.vetimm.2013.06.017
Newman RM, Salunkhe P, Godzik A, Reed JC (2006) Identification and characterization of a novel bacterial virulence factor that shares homology with mammalian Toll/interleukin-1 receptor family proteins. Infect Immun 74(1):594–601. https://doi.org/10.1128/IAI.74.1.594-601.2006
Low LY, Mukasa T, Reed JC, Pascual J (2007) Characterization of a TIR-like protein from Paracoccus denitrificans. Biochem Biophys Res Commun 356(2):481–486. https://doi.org/10.1016/j.bbrc.2007.03.003
Imbert PR, Louche A, Luizet JB, Grandjean T, Bigot S, Wood TE, Gagne S, Blanco A, Wunderley L, Terradot L, Woodman P, Garvis S, Filloux A, Guery B, Salcedo SP (2017) A Pseudomonas aeruginosa TIR effector mediates immune evasion by targeting UBAP1 and TLR adaptors. EMBO J 36(13):1869–1887. https://doi.org/10.15252/embj.201695343
Nold MF, Nold-Petry CA, Zepp JA, Palmer BE, Bufler P, Dinarello CA (2010) IL-37 is a fundamental inhibitor of innate immunity. Nat Immunol 11(11):1014–1022. https://doi.org/10.1038/ni.1944
Nold-Petry CA, Lo CY, Rudloff I, Elgass KD, Li S, Gantier MP, Lotz-Havla AS, Gersting SW, Cho SX, Lao JC, Ellisdon AM, Rotter B, Azam T, Mangan NE, Rossello FJ, Whisstock JC, Bufler P, Garlanda C, Mantovani A, Dinarello CA, Nold MF (2015) IL-37 requires the receptors IL-18Ralpha and IL-1R8 (SIGIRR) to carry out its multifaceted anti-inflammatory program upon innate signal transduction. Nat Immunol 16(4):354–365. https://doi.org/10.1038/ni.3103
Li S, Neff CP, Barber K, Hong J, Luo Y, Azam T, Palmer BE, Fujita M, Garlanda C, Mantovani A, Kim S, Dinarello CA (2015) Extracellular forms of IL-37 inhibit innate inflammation in vitro and in vivo but require the IL-1 family decoy receptor IL-1R8. Proc Natl Acad Sci U S A 112(8):2497–2502. https://doi.org/10.1073/pnas.1424626112
Moretti S, Bozza S, Oikonomou V, Renga G, Casagrande A, Iannitti RG, Puccetti M, Garlanda C, Kim S, Li S, van de Veerdonk FL, Dinarello CA, Romani L (2014) IL-37 inhibits inflammasome activation and disease severity in murine aspergillosis. PLoS Pathog 10(11):e1004462. https://doi.org/10.1371/journal.ppat.1004462
Lunding L, Webering S, Vock C, Schroder A, Raedler D, Schaub B, Fehrenbach H, Wegmann M (2015) IL-37 requires IL-18Ralpha and SIGIRR/IL-1R8 to diminish allergic airway inflammation in mice. Allergy 70(4):366–373. https://doi.org/10.1111/all.12566
Ballak DB, van Diepen JA, Moschen AR, Jansen HJ, Hijmans A, Groenhof GJ, Leenders F, Bufler P, Boekschoten MV, Muller M, Kersten S, Li S, Kim S, Eini H, Lewis EC, Joosten LA, Tilg H, Netea MG, Tack CJ, Dinarello CA, Stienstra R (2014) IL-37 protects against obesity-induced inflammation and insulin resistance. Nat Commun 5:4711. https://doi.org/10.1038/ncomms5711
Cavalli G, Justice JN, Boyle KE, D’Alessandro A, Eisenmesser EZ, Herrera JJ, Hansen KC, Nemkov T, Stienstra R, Garlanda C, Mantovani A, Seals DR, Dagna L, Joosten LA, Ballak DB, Dinarello CA (2017) Interleukin 37 reverses the metabolic cost of inflammation, increases oxidative respiration, and improves exercise tolerance. Proc Natl Acad Sci U S A 114(9):2313–2318. https://doi.org/10.1073/pnas.1619011114
Dantzer R, O’Connor JC, Freund GG, Johnson RW, Kelley KW (2008) From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci 9(1):46–56. https://doi.org/10.1038/nrn2297
Bozza S, Zelante T, Moretti S, Bonifazi P, DeLuca A, D’Angelo C, Giovannini G, Garlanda C, Boon L, Bistoni F, Puccetti P, Mantovani A, Romani L (2008) Lack of Toll IL-1R8 exacerbates Th17 cell responses in fungal infection. J Immunol 180(6):4022–4031
Garlanda C, Di Liberto D, Vecchi A, La Manna MP, Buracchi C, Caccamo N, Salerno A, Dieli F, Mantovani A (2007) Damping excessive inflammation and tissue damage in Mycobacterium tuberculosis infection by Toll IL-1 receptor 8/single Ig IL-1-related receptor, a negative regulator of IL-1/TLR signaling. J Immunol 179(5):3119–3125
Huang X, Hazlett LD, Du W, Barrett RP (2006) SIGIRR promotes resistance against Pseudomonas aeruginosa keratitis by down-regulating type-1 immunity and IL-1R1 and TLR4 signaling. J Immunol 177(1):548–556
Horne DJ, Randhawa AK, Chau TT, Bang ND, Yen NT, Farrar JJ, Dunstan SJ, Hawn TR (2012) Common polymorphisms in the PKP3-SIGIRR-TMEM16J gene region are associated with susceptibility to tuberculosis. J Infect Dis 205(4):586–594. https://doi.org/10.1093/infdis/jir785
Blok DC, van Lieshout MH, Hoogendijk AJ, Florquin S, de Boer OJ, Garlanda C, Mantovani A, van’t Veer C, de Vos AF, van der Poll T (2014) Single immunoglobulin interleukin-1 receptor-related molecule impairs host defense during pneumonia and sepsis caused by Streptococcus pneumoniae. J Innate Immun 6(4):542–552. https://doi.org/10.1159/000358239
Sham HP, Yu EY, Gulen MF, Bhinder G, Stahl M, Chan JM, Brewster L, Morampudi V, Gibson DL, Hughes MR, McNagny KM, Li X, Vallance BA (2013) SIGIRR, a negative regulator of TLR/IL-1R signalling promotes microbiota dependent resistance to colonization by enteric bacterial pathogens. PLoS Pathog 9(8):e1003539. https://doi.org/10.1371/journal.ppat.1003539
Drexler SK, Foxwell BM (2010) The role of Toll-like receptors in chronic inflammation. Int J Biochem Cell Biol 42(4):506–518. https://doi.org/10.1016/j.biocel.2009.10.009
Russell SE, Stefanska AM, Kubica M, Horan RM, Mantovani A, Garlanda C, Fallon PG, Walsh PT (2013) Toll IL-1R8/single Ig IL-1-related receptor regulates psoriasiform inflammation through direct inhibition of innate IL-17A expression by gammadelta T cells. J Immunol 191(6):3337–3346. https://doi.org/10.4049/jimmunol.1300828
Lech M, Skuginna V, Kulkarni OP, Gong J, Wei T, Stark RW, Garlanda C, Mantovani A, Anders HJ (2010) Lack of SIGIRR/TIR8 aggravates hydrocarbon oil-induced lupus nephritis. J Pathol 220(5):596–607. https://doi.org/10.1002/path.2678
Wang DY, Su C, Chen GM, Pan HF, Wang FM, Liu GL, Hao L, Wang DG, Ye DQ (2015) The decreased frequency of SIGIRR-positive CD4+ T cells in peripheral blood of patients with SLE and its correlation with disease activity. Mol Biol Rep 42(2):423–430. https://doi.org/10.1007/s11033-014-3783-4
Sanchez E, Garcia-Bermudez M, Jimenez-Alonso J, de Ramon E, Sanchez-Roman J, Ortego-Centeno N, Witte T, D'Alfonso S, Pons-Estel B, Anders HJ, Alarcon-Riquelme ME, Martin J (2012) Association study of IRAK-M and SIGIRR genes with SLE in a large European-descent population. Lupus 21(11):1166–1171. https://doi.org/10.1177/0961203312449494
Zhu Y, Wang DG, Yang XK, Tao SS, Huang Q, Pan HF, Feng CC, Ye DQ (2014) Emerging role of SIGIRR rs7396562(T/G) polymorphism in systemic lupus erythematosus in a Chinese population. Inflammation 37(5):1847–1851. https://doi.org/10.1007/s10753-014-9916-z
Lech M, Kulkarni OP, Pfeiffer S, Savarese E, Krug A, Garlanda C, Mantovani A, Anders HJ (2008) Tir8/Sigirr prevents murine lupus by suppressing the immunostimulatory effects of lupus autoantigens. J Exp Med 205(8):1879–1888. https://doi.org/10.1084/jem.20072646
Nakashima K, Hirota T, Obara K, Shimizu M, Jodo A, Kameda M, Doi S, Fujita K, Shirakawa T, Enomoto T, Kishi F, Yoshihara S, Matsumoto K, Saito H, Suzuki Y, Nakamura Y, Tamari M (2006) An association study of asthma and related phenotypes with polymorphisms in negative regulator molecules of the TLR signaling pathway. J Hum Genet 51(4):284–291. https://doi.org/10.1007/s10038-005-0358-1
Lech M, Avila-Ferrufino A, Allam R, Segerer S, Khandoga A, Krombach F, Garlanda C, Mantovani A, Anders HJ (2009) Resident dendritic cells prevent postischemic acute renal failure by help of single Ig IL-1 receptor-related protein. J Immunol 183(6):4109–4118. https://doi.org/10.4049/jimmunol.0900118
Noris M, Cassis P, Azzollini N, Cavinato R, Cugini D, Casiraghi F, Aiello S, Solini S, Cassis L, Mister M, Todeschini M, Abbate M, Benigni A, Trionfini P, Tomasoni S, Mele C, Garlanda C, Polentarutti N, Mantovani A, Remuzzi G (2009) The Toll-IL-1R member Tir8/SIGIRR negatively regulates adaptive immunity against kidney grafts. J Immunol 183(7):4249–4260. https://doi.org/10.4049/jimmunol.0803549
Costelloe C, Watson M, Murphy A, McQuillan K, Loscher C, Armstrong ME, Garlanda C, Mantovani A, O'Neill LA, Mills KH, Lynch MA (2008) IL-1F5 mediates anti-inflammatory activity in the brain through induction of IL-4 following interaction with SIGIRR/TIR8. J Neurochem 105(5):1960–1969. https://doi.org/10.1111/j.1471-4159.2008.05304.x
Andre R, Lerouet D, Kimber I, Pinteaux E, Rothwell NJ (2005) Regulation of expression of the novel IL-1 receptor family members in the mouse brain. J Neurochem 95(2):324–330. https://doi.org/10.1111/j.1471-4159.2005.03364.x
Watson MB, Costello DA, Carney DG, McQuillan K, Lynch MA (2010) SIGIRR modulates the inflammatory response in the brain. Brain Behav Immun 24(6):985–995. https://doi.org/10.1016/j.bbi.2010.04.002
Costello DA, Watson MB, Cowley TR, Murphy N, Murphy Royal C, Garlanda C, Lynch MA (2011) Interleukin-1alpha and HMGB1 mediate hippocampal dysfunction in SIGIRR-deficient mice. J Neurosci 31(10):3871–3879. https://doi.org/10.1523/JNEUROSCI.6676-10.2011
Na ES, Nelson ED, Kavalali ET, Monteggia LM (2013) The impact of MeCP2 loss- or gain-of-function on synaptic plasticity. Neuropsychopharmacology 38(1):212–219. https://doi.org/10.1038/npp.2012.116
Goldbach-Mansky R, Dailey NJ, Canna SW, Gelabert A, Jones J, Rubin BI, Kim HJ, Brewer C, Zalewski C, Wiggs E, Hill S, Turner ML, Karp BI, Aksentijevich I, Pucino F, Penzak SR, Haverkamp MH, Stein L, Adams BS, Moore TL, Fuhlbrigge RC, Shaham B, Jarvis JN, O'Neil K, Vehe RK, Beitz LO, Gardner G, Hannan WP, Warren RW, Horn W, Cole JL, Paul SM, Hawkins PN, Pham TH, Snyder C, Wesley RA, Hoffmann SC, Holland SM, Butman JA, Kastner DL (2006) Neonatal-onset multisystem inflammatory disease responsive to interleukin-1beta inhibition. N Engl J Med 355(6):581–592. https://doi.org/10.1056/NEJMoa055137
Xiao H, Gulen MF, Qin J, Yao J, Bulek K, Kish D, Altuntas CZ, Wald D, Ma C, Zhou H, Tuohy VK, Fairchild RL, de la Motte C, Cua D, Vallance BA, Li X (2007) The Toll-interleukin-1 receptor member SIGIRR regulates colonic epithelial homeostasis, inflammation, and tumorigenesis. Immunity 26(4):461–475. https://doi.org/10.1016/j.immuni.2007.02.012
Garlanda C, Riva F, Veliz T, Polentarutti N, Pasqualini F, Radaelli E, Sironi M, Nebuloni M, Zorini EO, Scanziani E, Mantovani A (2007) Increased susceptibility to colitis-associated cancer of mice lacking TIR8, an inhibitory member of the interleukin-1 receptor family. Cancer Res 67(13):6017–6021. https://doi.org/10.1158/0008-5472.CAN-07-0560
Yamada Y, Hata K, Hirose Y, Hara A, Sugie S, Kuno T, Yoshimi N, Tanaka T, Mori H (2002) Microadenomatous lesions involving loss of Apc heterozygosity in the colon of adult Apc(Min/+) mice. Cancer Res 62(22):6367–6370
Muzio M, Bertilaccio MT, Simonetti G, Frenquelli M, Caligaris-Cappio F (2009) The role of Toll-like receptors in chronic B-cell malignancies. Leuk Lymphoma 50(10):1573–1580. https://doi.org/10.1080/10428190903115410
Muzio M, Scielzo C, Bertilaccio MT, Frenquelli M, Ghia P, Caligaris-Cappio F (2009) Expression and function of Toll like receptors in chronic lymphocytic leukaemia cells. Br J Haematol 144(4):507–516. https://doi.org/10.1111/j.1365-2141.2008.07475.x
Bertilaccio MT, Simonetti G, Dagklis A, Rocchi M, Rodriguez TV, Apollonio B, Mantovani A, Ponzoni M, Ghia P, Garlanda C, Caligaris-Cappio F, Muzio M (2011) Lack of TIR8/SIGIRR triggers progression of chronic lymphocytic leukemia in mouse models. Blood 118(3):660–669. https://doi.org/10.1182/blood-2011-01-329870
Arvaniti E, Ntoufa S, Papakonstantinou N, Touloumenidou T, Laoutaris N, Anagnostopoulos A, Lamnissou K, Caligaris-Cappio F, Stamatopoulos K, Ghia P, Muzio M, Belessi C (2011) Toll-like receptor signaling pathway in chronic lymphocytic leukemia: distinct gene expression profiles of potential pathogenic significance in specific subsets of patients. Haematologica 96(11):1644–1652. https://doi.org/10.3324/haematol.2011.044792
Bichi R, Shinton SA, Martin ES, Koval A, Calin GA, Cesari R, Russo G, Hardy RR, Croce CM (2002) Human chronic lymphocytic leukemia modeled in mouse by targeted TCL1 expression. Proc Natl Acad Sci U S A 99(10):6955–6960. https://doi.org/10.1073/pnas.102181599
Brown GT, Narayanan P, Li W, Silverstein RL, McIntyre TM (2013) Lipopolysaccharide stimulates platelets through an IL-1beta autocrine loop. J Immunol 191(10):5196–5203. https://doi.org/10.4049/jimmunol.1300354
Beaulieu LM, Freedman JE (2010) The role of inflammation in regulating platelet production and function: Toll-like receptors in platelets and megakaryocytes. Thromb Res 125(3):205–209. https://doi.org/10.1016/j.thromres.2009.11.004
Levi M, Lowenberg EC (2008) Thrombocytopenia in critically ill patients. Semin Thromb Hemost 34(5):417–424. https://doi.org/10.1055/s-0028-1092871
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454(7203):436–444. https://doi.org/10.1038/nature07205
Chaix J, Tessmer MS, Hoebe K, Fuseri N, Ryffel B, Dalod M, Alexopoulou L, Beutler B, Brossay L, Vivier E, Walzer T (2008) Cutting edge: priming of NK cells by IL-18. J Immunol 181(3):1627–1631
Dupaul-Chicoine J, Arabzadeh A, Dagenais M, Douglas T, Champagne C, Morizot A, Rodrigue-Gervais IG, Breton V, Colpitts SL, Beauchemin N, Saleh M (2015) The Nlrp3 inflammasome suppresses colorectal cancer metastatic growth in the liver by promoting natural killer cell tumoricidal activity. Immunity 43(4):751–763. https://doi.org/10.1016/j.immuni.2015.08.013
Guillerey C, Huntington ND, Smyth MJ (2016) Targeting natural killer cells in cancer immunotherapy. Nat Immunol 17(9):1025–1036. https://doi.org/10.1038/ni.3518
Morvan MG, Lanier LL (2016) NK cells and cancer: you can teach innate cells new tricks. Nat Rev Cancer 16(1):7–19. https://doi.org/10.1038/nrc.2015.5
Stojanovic A, Cerwenka A (2011) Natural killer cells and solid tumors. J Innate Immun 3(4):355–364. https://doi.org/10.1159/000325465
Conflicts of Interest
The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Molgora, M., Supino, D., Garlanda, C. (2018). Regulation of Immunity and Disease by the IL-1 Receptor Family Members IL-1R2 and IL-1R8. In: Riccardi, C., Levi-Schaffer, F., Tiligada, E. (eds) Immunopharmacology and Inflammation. Springer, Cham. https://doi.org/10.1007/978-3-319-77658-3_10
Download citation
DOI: https://doi.org/10.1007/978-3-319-77658-3_10
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-77657-6
Online ISBN: 978-3-319-77658-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)