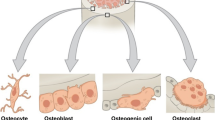
Abstract
Critical-sized bone defects can be repaired by using bone tissue engineering (BTE) procedures which rely on the combined use of cells, scaffolds and biologically active molecules. Based on their bioreactivity, biomaterials can be bioinert or bioactive. Bioinert biomaterials cause fibrous capsule formation upon implantation which favors the appearance of micromovements in the implant-tissue interface so the prosthesis fails. Bioactive biomaterials elicit a specific biological response thus avoiding fibrous layer formation and are able to interact with the biological environment. Bioactive biomaterials can be natural (bovine bone mineral matrix, hyaluronic acid, collagen, gelatin, fibrin, agarose, alginate, chitosan, silk) or synthetic (ceramics, metals, polymers, hydrogels and composites). Ceramics (bioactive glasses, glass–ceramics, calcium phosphates ceramics and cements) are most frequently used among these biomaterials due to similarity with the bone mineral phase. Another advantage from the use of ceramics is the presence of biologically active hydroxycarbonate apatite layer formed on the surface of these biomaterials, which represents the bonding interface with the tissues. Bioactive biomaterials have wide application as medical devices and in drug delivery systems. Since cells cannot survive without an adequate blood supply, future directions in bioactive biomaterials applications lies in the construction of bioactive and biodegradable 3D scaffolds that have osteogenic and angiogenic features. A possible alternative to improve osteogenic and angiogenic potential of the applied biomaterials is to incorporate bioactive biomolecules (e.g. growth factors) into the scaffold. One of the future perspectives in this area is the construction of smart biomaterials that respond to their environment in predetermined way regarding the protein release, thus allowing release initiated by microenvironmental conditions.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction to Bioactive Biomaterials in Medicine
Bone remodeling process occurs through whole life. A bone, highly vascularized and dynamic tissue, has high regenerative capacity which means that majority of the fractures can be healed spontaneously. Nevertheless, when critical-sized defects or nonunions occur, surgical interventions are inevitable (Stevens 2008). Critical-sized defects are wounds within a bone that are of such size that cannot heal spontaneously, or in which pathologic process detain regeneration (Allo et al. 2012).
Large bone defects can be reconstructed by using a gold standard in bone regenerative medicine—autografts (Schroeder and Mosheiff 2011). Autografts are osteoinductive and osteoconductive and have numerous osteogenic cells and adequate blood supply that altogether support graft viability (Schroeder and Mosheiff 2011). To avoid autologous bone harvest procedure, which represents health risks for the patient, alternative is the use of allografts (Bishop and Pelzer 2007). However, allografts lack vascular network (Griffith et al. 2005), osteoinductive growth factors as well as osteogenic cells (Cornejo et al. 2012). The other possibility for regeneration of large bone defects are bone tissue engineering (BTE) procedures which rely on the combined use of cells, scaffolds and biologically active molecules (Healy and Guldberd 2007; O’Keefe and Mao 2011; Najdanović et al. 2016). During bone tissue regeneration, the host cells respond to an osteogenic signal, while three-dimensional (3D) scaffold supports the growth of responsive host cells and allow the formation of extracellular matrix (ECM) and a vascularized host bed (Burg et al. 2000).
Biomaterials for BTE must be able to promote differentiation of progenitor cells into osteoblasts (osteoinductive), support bone growth encourage the ingrowth of the surrounding bone (osteoconductive), and to integrate into existing bone (osseointegration) (Stevens 2008). Any biomaterial applied in BTE must be bioresorbable and replaced with newly regenerated biological tissue in the body (Langer and Vacanti 1993).
The term “osseointegration” was first mentioned in 1965 by Brånemark in order to describe the successful fixation of implant into bone tissue (Brånemark et al. 2001). During osseointegration, osteoblast precursors accumulate, bone matrix forms and biomineral formation can eventually occur. The response of bone to an osseointegrated implant is similar to the response that occurs during bone fracture healing and includes the formation of blood clot upon implantation (Davies 2003). A blood clot is a peculiar scaffold for blood cells and, at the same time, a source of biological signals and differentiation factors inductive for the osteogenic process (Puleo and Nanci 1999). Osteogenic transcription factors regulate osteogenic differentiation of mesenchymal stem cells (MSCs) and regulate expression of the following genes: osteocalcin, osteopontin, bone sialoprotein, alkaline phosphatase and collagen type-I (ALP) (Long 2011). Several days after the implantation, osteoblasts secrete a bone matrix directly onto the implant surface that subsequently develops into immature (woven) bone (Davies 2003). At the end, immature bone is being replaced with the mature bone at the implant site, thus providing biological (mechanical) stability of the implant.
1.1 Implant-Tissue Interactions
Interactions between the implant and tissue can be extracellular and intracellular. Extracellular interaction is dependent on biomaterial’s surface features. Adsorption of non-collagenous proteins and collagen at biomaterials’ surface are influenced by surface nanometer scale porosity, biomaterial surface topographic configurations and negatively charged signals. Protein adsorption depends on various features. Interactions between osteoblast receptors and the corresponding protein ligands on the surface contribute to the cellular adhesion. Also, the adsorbed proteins on the implant surface, e.g. bone growth factors and activated enzymes, have a direct influence on the cell differentiation and proliferation. For example, osteoblast proliferation is favored over fibroblast proliferation on the surface of bioactive ceramics (Seitz et al. 1982).
Intracellular interaction is caused by the release of soluble agents from the biomaterial surface. Keeting and his team reported that soluble silicon released from the glass surface was a potent mitogen for human osteoblast-like cells, and that it also increased DNA synthesis and enhanced alkaline phosphatase activity and osteocalcin release (Keeting et al. 1992). It has been shown that osteoblasts’ proliferation is more rapid on bioactive glass substrates compared to synthetic HA (Vrouwenvelder et al. 1993).
2 Classification of Biomaterials in Medicine
Reactivity of the biomaterial with the native tissues is of key importance for the construction of the implants (Vallet-Regi and Ruiz-Hernandez 2011). In the past, biomaterials for BTE were constructed to be “bioinert”, while biomaterials today are mostly designed to be “bioactive” which refers to ability to interact with the cells and biological molecules and regenerate bone tissue (Langer and Vacanti 1993; Hench and Polak 2002).
2.1 Bioinert Biomaterials
Bioinert biomaterials are used in order to reduce the immune reaction and the reaction to foreign body as much as possible (Hench 1980). After implantation of a bioinert biomaterial, fibrous capsule surrounds the material as an answer to the foreign body (Castner and Ratner 2002). Subsequently, a formed capsule favors the appearance of micromovements in the implant-tissue interface. As a consequence, the prosthesis fails and it must be replaced (Salinas et al. 2013).
To overcome such problems, two approaches have been developed: biological fixation and bioactive fixation (Cao and Hench 1996). Biological fixation represents the construction of materials with rough surfaces and pores larger than 100 µm which allow tissue ingrowth and angiogenesis. During bioactive fixation, intimate biomaterial-bone apposition is established which has a mechanically strong bond as a consequence (Salinas et al. 2013).
In earlier experimental and clinical applications, bioinert biomaterials were thought to be superior over bioactive ones because these biomaterials generate a minimal tissue response. Nevertheless, survivability of bioinert implants decrease in long-term periods (>10 years) so the development of bioactive biomaterials became more attractive in tissue engineering (Hench 1998a).
2.2 Bioactive Biomaterials
The term “bioactivity” relates to all interactions and effects that materials exert on cells thus activating responses or leading to specific cell behaviors (Navarro et al. 2008). Bioactive biomaterials are created in such way that elicit a specific biological response and avoid fibrous layer formation. These biomaterials have interaction with the biological environment thus enhancing the biological response as well as the tissue/surface bonding (Navarro et al. 2008). Bioactive biomaterials provide an environment that is consistent with bone growth. This enables development of mineralizing interface which is a natural bond junction between living and non-living biomaterials (Cao end Hench 1996).
Mineralization and binding between the bone tissue and the implant are one of the most important approaches for increasing bioactivity during the repair (Navarro et al. 2008). Also, mechanical properties of the bioactive biomaterial are important. The structure of bone determines its mechanical properties while mechanical load determines bone structure during repair. Therefore, the perfect bioactive biomaterial should enhance newly formed bone formation which has mechanical properties similar to the normal host bone site (Hench 1998b).
Amongst the crucial factors in the design of bioactive biomaterials are the pore size and interconnection of pores (Davis et al. 2005). Large interconnected pores promote colonization of biomaterials (Karande et al. 2004), but if the pores are extremely large, the consequence is impaired vascularization because endothelial cells cannot bridge the pores larger than a cell diameter (Salem et al. 2002). Integrity of the material is also affected by the size of pores so the cellular effects should be in balance with the mechanical properties of applied biomaterial (Karande et al. 2004). When the pores are smaller than 100 nm, diffusion of nutrients and factors are affected, which lead to the failure of implanted grafts and poor survival of implanted cells (Zimmermann et al. 2004). Pore length and numbers has an influence on the diffusion of nutrients and factors in the polymers (Botchwey et al. 2003). Very small pores in hydrogels constructed from self-assembling peptides support adhesion of endothelial cells and formation of capillary network as well as rapid cell migration (Narmoneva et al. 2005).
Bioactive materials are osteoconductive since they provide the surfaces adequate to support the adhesion and proliferation of osteoblasts (Hench and West 1996). Among them, there are also osteoinductive materials which, besides facilitating bone growth, have a role in conducting bone formation (Hench and West 1996). While osteoconduction is an extracellular response, osteoinduction is an intracellular response induced by the release of large amounts of Si (IV) and Ca2+ ions which stimulate the genes response in order to produce the bone formation (Salinas et al. 2013).
Based on the type of effect exerted on bone tissue, bioactive biomaterials divide into two classes—Class A and Class B. The bioactive glasses that enhance bone proliferation and differentiation of progenitors (osteoproduction) due to reactivity at a cellular level in the body has a Class A bioactivity. In contrast to that, Class B bioactive biomaterials, such as synthetic HA, lead only to bone growth along the implant surface—osteoconduction (Hench and West 1996). It has been shown that bone proliferation in vivo is enhanced in the presence of bioactive glasses with the same or even greater growth rate compared to an autogeneous bone applied for same defect (Hench and West 1996). As a consequence of the enhanced osteogenic behavior, production of biological growth factors is also enhanced and therefore, cell proliferation and the formation of newly organized tissues are stimulated (Hench 1998a).
Class A bioactive materials are able to form a biologically active hydroxycarbonate apatite (HCA) layer on their surfaces in vivo within a few minutes to a few hours (Cao and Hench 1996; Hench and West 1996), while well-crystallized HCA layer onto Class B bioactive materials need more than one week to be formed (Hench and West 1996). Sol–gel chemistry can be used to synthesize HCA coatings on various types of substrates which are formed probably by the mechanism of heterogeneous nucleation of HCA crystals within the nanometer-sized pores that create supersaturated Ca–P solutions (Pereira and Hench 1996).
It is thought that the biomaterials which will enhance tissue regeneration should have higher molecular control of interfacial reactions than the one in Class A bioactive biomaterials. The molecular control comprises the release control of the elements and chemical compounds which activate the genes important for mitosis and cell differentiation. Resorption of bioactive materials is also important and it is controlled at molecular level by the metabolic processes of the tissue which is being replaced. The genetic activation of the enzymes and growth factors synthesis and the ability to adsorb and desorb biologically active molecules without losing the conformation and biological function are also important. Sol–gel processing provides the chemical control of a biomaterial’s dissolution rate and surface chemical binding sites (Hench 1998a).
Class A bioactive biomaterials can form a biologically active, hydrated silica-gel layer on their surfaces a few minutes after exposure to the body fluids either in vivo or in vitro. This hydrated silica-gel layer is highly porous three-dimensional network which is totally interpenetrated with pore liquid (Hench 1998a). Pore-liquid networks can be enriched by incorporation of various organic and biological molecules (Avnir et al. 1997). A spectrum of differing volume fraction and size distributions of porosities can be accomplished in films (Brinker et al. 1995) and porous matrices (Hench and Orefice 1997) by changing the production conditions.
3 Bioactive Biomaterials in Bone Regenerative Medicine
The clinical survivability of the biomaterials such as bioactive glasses, ceramics, glass-ceramics, and composites is higher than in the case of bioinert biomaterials (Cao and Hench 1996; Hench and West 1996). Among the successful clinical applications of bioactive biomaterials are bioactive synthetic hydroxyapatite coatings and filling of bone defects (Ratner et al. 2004), bioactive glass middle-ear prostheses, endosseous alveolar ridge maintenance implants (Cao and Hench 1996) and bioactive A/W glass-ceramic in iliac crest donor site repair and replacement of vertebrae (Cao and Hench 1996).
Hydroxyapatite, in bulk and granular forms, was used as bone spacers and fillers (Shores and Holmes 1993). Glass-ceramic A–W, due to its high mechanical strength and good bone-bonding ability, has been used as artificial vertebrae, intervertebral discs, and iliac crests in dense bulk form (Yamamuro 1993).
The success was made in the application of BG particulate in the 6-mm defect in a rabbit femur by Oonishi et al. (1997). New trabecular bone was formed within one week, while after three weeks regenerated trabecular bone formed around the bioactive glass particles throughout the defect and bonded the particles together. Synthetic HA particulate did not succeed to fill the same defect even after twelve weeks of the surgical procedure. In this later case, the bridges between bone ends did not grow in thickness and only a small amount of bone were found between HA particles (Oonishi et al. 1997).
Wheeler et al. demonstrated that the accelerated bone formation was accompanied by resorption of the gel glass particles in 3 months. Active mineralization occurred throughout the grafted bone defects, with osteoblasts lining the new bone, formed around the gel-glass particulates. All grafted defects had significantly more bone within the area than the unfilled controls (Wheeler and Stokes 1997).
Wheeler and his associates (Wheeler et al. 1998) examined bone regeneration in cancellous skeletal defects of rabbits distal femur augmented with USB (90–710-µm particle size) or OV (300–355-µm particle size) bioactive glass particles and compared it with normal cancellous bone. Statistically higher bone quantity was found in the defect filled with USB and NORM than in the defect with OV (p < 0.05) at both observation points (4 and 12 weeks). This can be explained by the larger mean particle size of the OV than the USB particles combined with more numerous particles within the USB-grafted defects. Greater particles number in combination with the smaller particle size caused greater surface area of bioactive glass in the USB-filled defects, which further provided more sites for osteoblast adhesion and osseous formation than in the defects filled with OV.
Bioactive calcium phosphates and silica-based glasses are suitable for small bone defects filling (Yuan et al. 2010) where the bone regeneration kinetics is preferable over mechanical properties (Salinas and Vallet-Regı 2013). Due to their fragility and low resistance to fatigue, these types of bioactive biomaterials are inappropriate choice for large bone defects repair.
Bioactive biomaterials that have application in bone regenerative medicine could be classified as natural and synthetic bone substitutes (Fig. 1). Nanomaterials belong to a special class of bioactive biomaterials that comprises both natural and synthetic biomaterials (Fig. 1).
3.1 Natural Bone Substitutes
In our laboratory, we are dealing with bone biology and bone regeneration in animal models. For this purpose, various biomaterials as bone substitutes and scaffolds for cells, growth factors and drugs are exploited. Commercial, hydroxyapatite-based bone mineral matrix (BMM) Bio-Oss® (Geistlich-Pharma, Wolhusen, Switzerland) combined with platelet-rich plasma (PRP) as a source of growth factors and adipose-derived stem cells (ADSCs) in vitro induced towards endothelial cells (ECs) were used to provide “biological triad” principle in subcutaneous implants (Fig. 2). Such combination caused increased vascularization in bioengineered implants and more pronounced osteogenic process (Najdanović et al. 2015). Also, in vitro osteoinduced ADSCs delivered with PRP on BMM as a carrier (Fig. 2) induced formation of osteocalcin-positive callus-like tissue in ectopic implants and intensive resorption of BMM granules (Cvetković et al. 2015).
In a simulated intraoperative procedure, we have shown that subcutaneous implants composed of BMM as a carrier, PRP and freshly isolated adipose derived stromal vascular fraction cells, rapidly triggered osteogenic process and had excellent osteogenic capacity (Najman et al. 2016). The same BMM combined with blood diluted with inflammatory macrophages has shown a favorable effect on the process of angiogenesis and synthesis of an organic fraction of bone matrix (Živković et al. 2015). Bio-Oss granules supplemented with PRP have also served as carriers for different forms of vitamin D which is utilized in the regeneration of osteoporotic bone (Fig. 3). Cholecalciferol and alfacalcidol, locally applied with this bioactive carrier/scaffold in the area of femoral defect, decrease the resorption of Bio-Oss particles, delay early bone regeneration and induce the formation of new healthy bone tissue in the case of alfacalcidol or high amount of the well mineralized bone tissue in the case of cholecalciferol (Rajković et al. 2015).
An important bioactive effect in various tissues, including bone and cartilage, has been shown by using some natural polymers: hyaluronic acid, collagen, gelatin, fibrin, agarose, alginate, chitosan, silk.
Hyaluronic acid has been applied for surgical adhesions, knee pain (Furth et al. 2007), cartilage regeneration (Jazayeri et al. 2017).
Although collagen is mostly used in soft tissue regeneration (Furth et al. 2007), it has been found that collagen-based osteochondral grafts have consistently integrated layer structure and good porosity as well as mechanical properties (Levingstone et al. 2014).
Main use of gelatin is cartilage tissue regeneration, while fibrin is a potential scaffold for stem cell cultures which could be further used in bone and cartilage tissue engineering (Jazayeri et al. 2017).
It has been shown that agarose scaffolds increase stem cells’ differentiation into chondocytes (Awad et al. 2004). These scaffolds are the versatile ones for the application in bone tissue engineering (Jazayeri et al. 2017).
Alginate can be used in the form of hydrogels that bears cell-adhesion ligands (Langer and Tirrell 2004). These biomaterials have been applied as scaffolds for cell encapsulation and transplantation, which brought good results regarding engineering such bone tissue that can grow out of modest numbers of implanted cells (Alsberg et al. 2002) and in drug delivery (Tonnesen and Karlsen 2002).
Chitosan-based injectable materials and its derivatives could be applied as osteogenic bone substitutes (Shi et al. 2006). Ge and his associates found that combinations of chemically modificated hyaluronic acid and also chitin-chitosan-HA biomaterial promoted neovascularization, had osteoinductive effects and rapidly degraded in vivo (Ge et al. 2004). The other advantage of chitosan application in bone regenerative medicine is the ability to induce recruitment and attachment of osteogenic cells (Kim et al. 2002). It was also found that scaffolds composed of chitosan/alginate/hydroxyapatite, which was the carrier for recombinant BMP-2 and mesenchymal stem cells, had excellent effect on formation of new bone that resulted in almost completed repair of critical sized bone defects in rats 12 weeks after implantations (He et al. 2014).
Due to its biocompatibility and slow degradation rate (Hege and Schiller 2015), silk is good candidate for application in bone regenerative medicine. In spite of that, silk lacks osteoinductivity, so the addition of osteoinductive factors to silk is necessary (Huang et al. 2014). Huang and associates examined the effect of osteoinductive-nanoscaled silk/HA composite scaffolds and found that the addition of hydroxyapatite to silk enhanced biocompatibility and mechanical strength of the scaffolds (Huang et al. 2014).
One of the most attractive directions in bone regenerative medicine is the use of bioinspired biomaterials. Construction of such biomaterials is based on mimicking natural biological design in order to construct synthetic biomaterials (Green et al. 2016). For example, this mechanism has been applied for the construction of boundary between bone replacements and natural bone in a rat calvarial defect. The boundary was made out of glue substrate that was secreted by Phragmatopoma californica, a sandcastle worm (Winslow et al. 2010). The glue was moderately resorbed and replaced by new lamellar bone.
3.2 Synthetic Bone Substitutes
3.2.1 Ceramics
Ceramic materials, which include bioactive glasses (BGs), glass–ceramics, calcium phosphates ceramics (CaPs) and cements (Navarro et al. 2008), are mostly used as bone defect fillers (Vogel et al. 2001). These biomaterials are similar to the bone mineral phase and have structural and surface features which enable binding to the bone without forming an interface that consists of fibrous connective tissue (Schepers et al. 1991).
Simultaneously with the implantation procedure, time-dependent kinetic modification of the ceramics surface begins. Hydroxycarbonate apatite (HCA) layer developed at the biomaterial surface is bioactive and represents the bonding interface with tissues due to its similarity with the mineral bone phase (Hench 1998b). Bioactive glasses applied in BTE are able to induce bone tissue growth processes—enzyme activity (Aksay and Weiner 1998), revascularization (Keshaw et al. 2005) as well as osteoblast differentiation from mesenchymal stem cells and osteoblast adhesion (Lu et al. 2005; Schepers et al. 1991).
During the early implantation period, apatite layer formation on the ceramic surface precede bone matrix integration into apatite (Kokubo 1990). This apatite layer contains nano-crystals of carbonate-ion-containing apatite with structure and crystallinity similar to the one in bone mineral phase (Kokubo 1990). Osteoblasts that proliferate on the apatite form a biological apatite/collagen extracellular matrix (Loty et al. 2000), thus enabling direct contact between surface of the apatite layer and surrounding bone (Kokubo et al. 2003).
Immersion of bioactive biomaterials into a simulated body fluid (SBF), an aqueous solution with mostly the same ingredients as human extracellular fluid, is another approach applied to achieve a bone-like apatite layer formation. SBF is cell-free and protein-free, so the apatite layer is formed due to the chemical reaction between bioactive ceramics and the surrounding fluid. Thanks to such features of SBF, new types of biomaterials that are bioactive have been designed—glass-ceramics, organic–inorganic hybrids, coatings as well as bioresorbable ceramics (Ohtsuki et al. 2009).
Some of the most frequently used ceramics in medicine are: Bioglasss in the Na2O–CaO–SiO2–P2O5 system (Hench et al. 1971), hydroxyapatite (HA) (Ca10(PO4)6(OH)2 (Jarcho et al. 1977), β-tricalcium phosphate (TCP) (Ca3(PO4)2 (Rejda et al. 1977), HA/TCP bi-phase ceramic (Daculsi et al. 1990), glass ceramic A–W containing crystalline oxyfluoroapatite (Ca10(PO4)6(O, F2)) and β-wollastonite (CaO × SiO2) in an MgO–CaO–SiO2 glassy matrix (Kokubo et al. 1982).
In 1971, Hench and associates made the first bioactive glass Bioglass® by the conventional melt-derived process (Hench et al. 1971). Nowadays, it exists in the particulate form of following commercial products: Perioglas® (periodontal bone filler), Novabone® (orthopedic bone filler), Novamin (additive for toothpaste), but its disadvantage is that it cannot be made into a scaffold because it crystallizes on sintering and forms a glass-ceramic. A Sol–gel derived glass is a procedure for production of scaffolds from bioactive glasses. It is developed as an alternative to the traditional melt processing in order to ensure an interconnected nanoporous structure through the whole glass (Jones 2009). Nanoporosity influence cell response, especially osteoblast response (Biggs et al. 2007). Nevertheless, the greatest advantage of bioglass prepared by sol–gel method is the introduced foaming step that creates porous scaffolds with interconnected macropore networks.
45S5 Bioglasst (USB) is an effective graft material for the use in oral and maxillofacial bone surgery (Oguntebi et al. 1993), mostly because of its bioactivity based on the following composition −45% SiO2, 24.5% CaO, 24.5% Na2O, and 6% P2O5. Such composition of USB stimulates apatite gel layer formation on the surface of the particles, which attracts osteoprogenitor cells and osteoblasts, thus stimulating formation of bone (Hench et al. 1991). USB has a wide range of particle size (from 90 to 710 mm) which was shown as an optimal feature for bone tissue regeneration of critical-sized calvaria defects (Bergman and Litkowski 1995). Numerous studies have proved the potential of 45S5 bioactive glass for skeletal applications (Piotrowski et al. 1975).
Bioactive gel-glasses are advantageous over bioactive glasses, such as 45S5 Bioglasst (BG), for several reasons. Among these reasons is the absence of Na2O in the Bioactive gel-glasses structure, which ensures that there is no rapid increase in interfacial pH following the surface reactions. Also, a large surface silanols-rich area can be obtained in situ in the gel-glasses by controlling the ultrastructure processing, aging, and stabilization treatments. Therefore, bioactive gel-glasses can nucleate a biologically active HCA layer within minutes more rapidly than bioactive melt glasses with much lower contents of silica. Thanks to sol–gel processing, bioactive compositions can obtain wide range of silica content and variable levels of CaO and P2O5 (Pereira et al. 1994).
Bioactive glasses can also be designed to deliver ions which activate complex gene transduction pathways and thus enhance cell differentiation and osteogenesis (Hench and Polak 2002; Tsigkou et al. 2007). Crystalline HA can be used for the adjustment of resorption rate of bioactive glasses and bioceramics. Other calcium phosphates possess a greater capacity to be resorbed but their strength for sustaining load is lower (Oonishi et al. 1995).
Biologically relevant levels of soluble ions of Si, Ca, P, and Na can be released by bioactive glass surfaces. These ions further promote intra- and extra-cellular responses (Xynos et al. 2001). Bioactive glasses based on borate support cell proliferation and differentiation in vitro (Fu et al. 2010a; Marion et al. 2005) as well as the tissue infiltration in vivo (Fu et al. 2010b), while bioactive glasses which have Cu, Zn or S as components favors bone growth (Fu et al. 2010a; Wang et al. 2011; Zheng et al. 2012).
3.2.2 Metals
Since none of the orthopedic metallic biomaterials is bioactive by itself, there are two methods to make them bioactive: coating implants’ surface with a bioactive ceramic and chemical modification of the biomaterials’ surface. The second procedure is used in order to accomplish deposition of a bioactive ceramic in vivo or to promote adhesion of cells and proteins and other interactions between tissue and biomaterial (Navarro et al. 2008).
Some metals may become bioactive due to ceramic component formed on their surfaces by chemical etching process. For example, as a result of the chemical reaction of TiO2 with NaOH, a sodium hydrogen titanate gel layer is formed. Subsequently, the thermal treatment produces amorphous sodium titanate which displays a bioactive response (Salinas and Vallet-Regı 2013).
Osseointegration of an implant can be improved by coating the implants with inorganic and organic components that are similar to the ones in physiological extracellular bone matrix (ECM) (de Jonge et al. 2005). These depositions of bioactive biomaterials enable direct implant–bone bonding and enhance implant osseointegration due to the accelerated speed and amount of new bone formed at the interface (de Jonge et al. 2005). Described cell-biomaterial interactions are mediated by integrins which also probably cooperate with osteogenic factors that accumulate on the implant surface thus regulating proliferation and differentiation of osteoblasts (Siebers et al. 2005). The coating which had the successful application in BTE are nano-CaP/collagen and CaP/ALP composite coating onto titanium surfaces (de Jonge et al. 2009), growth factors loaded on collagen or CaP-coated implants (Li et al. 2010) and DNA-based coating onto titanium implants using the layer-by-layer (LbL) deposition technique (Schouten et al. 2010).
3.2.3 Polymers
Polymers can be either biological or synthetic. Biological polymers contain inherent biological informations that are necessary for induction of chemotactic responses as well as cell attachment. The alterative for biological polymers are synthetic ones which can be produced into various three-dimensional scaffolds with different porosities and surface characteristics (Stevens 2008).
Biological polymers physodic (P2) and 3-hydroxy physodic acid (P3), that are main compounds of methanol extracts (ME) isolated from the lichen Hypogymnia physodes, induced a significant decrease in the HeLa cells viability and proliferation in vitro (Stojanović et al. 2014). Obtained data are interesting for further investigation of biological activity of these biopolymers. It has been shown that lichen derivates have pro-apoptotic effects on tissues around bone implants which might be a mechanism for protection from cancer development in different tissues (Odabasoglu et al. 2012). This could be a possible future direction for examination of physodic (P2), 3-hydroxy physodic acid (P3) and ME of the H. physodes as bioactive agents in BTE.
Synthetic hydroxyapatite (sHA, Ca10(PO4)6(OH)2) is one of the most applied materials for bone defect reparation due to its similarity to the bone mineral, as well as its bioactivity and osteoconductivity (LeGeros 2002). Various commercial porous forms of sHA are in use (e.g. ApaPore® (Apatech Ltd., Elstree, UK)), but their resorption rate is low so they can be only used for bone augmentation (mechanical support of diseased bone), and not for regeneration. Silicon or carbonate substituted apatites can be used for increasing their resorption rate which is still slow (Jones 2009).
Functional groups and binding sites at the polymers surface influence their bioactivity. In order to achieve bioactivity, polymer surface can be modified usually by physisorption of proteins and peptides on the surface, dipcoating and amino- and carboxyl-directed immobilization of biomolecules (Ma et al. 2002) or biochemically in order to induce mineralization with HA layers (Kato et al. 1996).
3.2.4 Hydrogels
In order to supply three-dimensional cellular microenvironment with high content of water, hydrogels can be obtained by using minimally invasive techniques and gelled in situ by photocrosslinking or ionically (Stevens 2008). Due to viscoelasticity, hydrogels could be applicable in regeneration of cartilage (Stevens et al. 2004) and bone (Lutolf et al. 2003). Our team have shown that although 2-hydroxyethyl methacrylate, poly(alkylene glycol) (meth)acrylates and itaconic acid are able to swell in phosphate buffer, physical integrity and soft and rubbery consistency of these biomaterials are maintained even when swelling experiments were performed for a long time after reaching the equilibrium state (Takić-Miladinov et al. 2016). Also, the tested hydrogels induce genotoxic effects, which intensity depend on chemical composition, extract concentration and degree of crosslinking of these hydrogels.
3.2.5 Composites
Inorganic-organic composites “mimic” the composite nature of the native bone regarding to combined toughness of a polymer phase and compressive strength of an inorganic phase. Nanosized inorganic component are probably more bioactive than the micro-sized components (Stevens 2008). Since cell’s transmembrane integrin receptors bind biologically active peptide motifs, e.g. arginine-glycine-aspartic acid (RGD), implementation of such motifs is among most applied methods for enhancing functionality of these biomaterials (Bökel and Brown 2002). Optimization of biodegradability of the applied biomaterial with the one specific for remodeling and regeneration of native bone tissue can be achieved with proteolytically degradable peptide motifs that are recognized by cell-secreted matrix metalloproteases (Lutolf et al. 2003).
Biodegradable polymers can be combined with bioactive inorganic materials in order to construct nanocomposites and organic-inorganic (O/I) hybrids (Allo et al. 2012). Better cell attachment and responses could be achieved by modification of the surface of nanocomposites or O/I hybrids via changing functional groups present at the surface of these biomaterials. As a consequence, vascularization is successful and mineralization occurs in the scaffolds. The limitation of porous 3D nanocomposites and O/I hybrids scaffolds are unknown long-term in vivo behavior regarding angiogenic stimulus, degradation and ion release kinetics (Allo et al. 2012).
3.3 Nanomaterials
Nanomaterials represent a special type of biomaterials that can be found in nature but also can be synthetic (Adlakha-Hutcheon et al. 2009). Nanomaterial-based scaffolds have significant application both in tissue engineering and in drug delivery. Due to biodegradability, these biomaterials support cell growth and infiltration in a manner that natural replacement with new biological tissue occurs, which is of significance in bone regenerative medine (Marchesan and Prato 2013). Since smart nanodevices target site of the certain disease, an external signal induce controlled release of multiple agents, which is powerful mechanism for drug delivery. Graphene-based nanomaterials are applicable in bone tissue engineering (Shin et al. 2016). For example, the beneficial effect of graphene-based biomaterials on enhancement of adherence, proliferation, and differentiation of osteogenic cells was estimated (Shi et al. 2012; Venkatesan et al. 2014). In addition, graphene can be used to replace the effect of BMP-2 as an inductive factor for cell differentiation (Nayak et al. 2011) or in order to boost osteoconductivity via stimulation of osteogenic cells differentiation and biomineralization process (Kim et al. 2011).
4 Bioactive Biomaterials in Dentistry
Bioactive biomaterials play a key role in dentistry where they are used for a dental treatment, in the therapy of the pulp and root canal as well as in dental surgery (Goldberg and Smith 2004; Mauth et al. 2007; Grotra and Subbarao 2012). They are essential in restoring impaired teeth and jaw bone structure. A wide range of biomaterials is used in dentistry including inorganic salt, polymers, ceramics, metals and composites. Bioceramics and bioglasses have a wide spread application in dentistry and medicine because they interact with and induce regeneration of the surrounded tissue which is important for successful regeneration.
Biocompatible white powder, which consists of ceramics particles, can be used in root canal repair due to the ability to stimulate cementogenesis and form a hermetic seal in the root canal (Sharma et al. 2013). Portland cement or Mineral trioxide aggregate (MTA) is a type of the bioactive material, composed of calcium and silicate, which maintains pulp and periodontal tissue vitality (Roberts et al. 2008) and has characteristic of apatite formation.
Calcium phosphates are good choice for both craniofacial and dental applications (Thein-Han et al. 2012). Likewise, hydroxyapatite was applied for the production of HA-based (n-HA/polyamide (PA)) biomaterials by using CAD/CAM technology and implanted into a fracture of mandibular condyle. The results of the treatment showed that patients gained a jaw contour that had proper temporomandibular joint activity (Li et al. 2011).
Bioglass and Bioglass-type glasses particulates were used with success in periodontal bone repair (Wilson et al. 1993). Bioactive glass BaG 45S5 is very reliable at the sites of tooth extraction for the tooth roots treatment and maintaining a solid ridge for dentures (Jazayeri et al. 2017). Biosilicate is a bioactive glass-ceramic used for open dentinal tubules of a vital tooth. These bioactive glass-ceramic induce HCA (hydroxyl carbonate apatite) deposition in open dentinal tubules thus offering a new opportunity for treating dentine hypersensitivity (Tirapelli et al. 2010).
For maxillofacial and craniofacial surgery, synthetic bone materials and freeze-dried bone are in use, while β-Tricalciumphosphate (β-TCP) and histoacryl are good filling materials for the bone defects treatments (Sharma et al. 2013).
Poly (lactid) acid/hydroxyapatite (PLLA/HA) is a polymer matrix composite material that has been successfully used as anosteochondral construct for mandible bone regeneration (Schek et al. 2005) and Ceramic Matrix Composites are used in order to increase mechanical strength of the construct to resist load-bearing applications, chiefly in the jaw compression (Friedman et al. 1991). For the necessary step in oral and maxillofacial surgery—guided tissue regeneration, polymers including tissue-derived collagen (Karfeld-Sulzer and Weber 2012; Wang and Carroll 2001) and synthetic polyesters (Karfeld-Sulzer and Weber 2012; Gentile et al. 2011) are frequently used.
Dentin extracellular matrix proteins (ECMPs) and Dentonin (peptide) are amongst the most promising biomolecules for application in pulp repair and regeneration (Goldberg et al. 2006). ECMPs can stimulate proliferation and differentiation of dental pulp stem cell and their migration to sites of injury, while Dentonin activates reparative mineralization of the cornal pulp and root canal lumen.
Emdogain, a biomaterial composed of porcine proteins, can be applied in periodontal regeneration after gum disease and injuries.
Among the metals, most frequently used biodegradable metals (BMs) are Mg-based BMs due to efficacy in maxillofacial bone defects treatment (Li et al. 2014).
In the field of prosthetics, due to low cytotoxicity, silicone oral tissue conditioners are suitable for daily dental practice (Krunić et al. 2011).
5 Bioactive Biomaterials in Drug Delivery Systems
The application of biomaterials as carriers for sustained and controlled drug delivery has become a very popular approach in the treatment of different diseases. By using drug delivery systems, target sites in the body can obtain an effective concentration of drug avoiding the side effects of systemic treatment.
In the case of impaired bone regeneration associated with bone metabolic disorders, local delivery of anti-osteoporotic drugs and anabolic agents (e.g. growth factors) using bone substitutes causes more rapid bone “answer” to the treatment and provide a better osseointegration of implants (Kyllönen et al. 2015).
Besides the good choice of anabolic drug, an adequate selection of delivery system is essential. In order to be used as systems for the drug delivery, biomaterial should be synthesized as a biocompatible and should provide long and gradual drug release. Most of the biomaterials used in tissue engineering are biodegradable and this feature is particularly important for local drug releasement.
Different synthetic and natural polymers, bioceramics and biocomposites that are widely used as scaffolds for tissue engineering may serve as carriers for drug delivery. After the incorporation or absorption, obtained bioactive implants release drugs in their surroundings affecting the bone regeneration and osseointegration.
Biomaterials based on calcium and phosphates are often used for bone regeneration as a bone substitutes and, therefore, represent good candidates as bioactive local drug delivery carriers. Because of the similarity with an inorganic bone phase, these biomaterials exhibit osteoconductive properties and may be resorbed by osteoclasts thus enabling sustained drug release (Kyllönen et al. 2015; Verron et al. 2010). CaPs based biomaterials are available in the form of powders, granules, ceramic, cement and coatings.
The potential ways for the local drug delivery in bone disorders involve implants coating, the application of injectable forms of bone cements and gels and, in the cases of large bone defects, application of bioactive scaffolds for tissue regeneration (Kyllönen et al. 2015).
Calcium phosphate cements (CPC) are suitable carriers for the local drug delivery due to their osteoconductivity, good protein absorbability and gradual release of different agents (Guo et al. 2005; van de Watering et al. 2012; Wu et al. 2012; Ginebra et al. 2006). During the system designing, a chosen drug or growth factor may be incorporated into the solid or liquid phase of the cement or first incorporated in the microparticles that can be inserted into the delivery system. Using cements in combination with growth factors showed a favorable impact on bone regeneration, especially in osteoporotic conditions (Blom et al. 2001; van de Watering et al. 2012).
Disadvantage of this system is a need for enough space in the bone fracture area, in order to deliver required amount of the chosen drug (Kyllönen et al. 2015). Also, CPCs are slowly biodegradable in vivo and suffer of the lack of porosity which may be improved with various modifications (Xu et al. 2004).
Utilization of bone cement as a carrier for antimicrobial drugs is particularly recommended against infection associated with implant application (Neut et al. 2005).
Heat produced during the polymerization and postpolymerization treatments in cold-polymerized PMMA (Kostić et al. 2011), a non-biodegradable acrylic cements which is commonly used for implant fixation in orthopedics and dental surgery, restrict the range of drugs to deliver but they found to be very effective in delivering antibiotics (Minelli and Benini 2007).
Implant coatings is strategy of particular importance for metallic inert materials that are often used for hard tissue repair (Goodman et al. 2013). Drug insertion in coatings represents a good strategy in bone fracture healing due to the capability of the delivered agents to influence on implant osseointegration. Metal implants can be coated with the suitable drug directly, but the better results in the treating of bone fractures can be achieved by absorption or incorporation of the drug onto the CaP materials which can be used as coatings around the implant (Liu et al. 2007). Hydroxyapatite coatings can be the way to deliver growth factors, DNA or various bioactive molecules (Sachse et al. 2005; Yu et al. 2012; Goodman et al. 2013). This approach enabled gradual releasement of the applied drug and enhanced osseointegration of the implant in experimental animals. Using anti-osteoporotic drugs as components of the coatings may improve bone microarchitecture around the titanium implant in osteoporotic rat tibiae (Pyo et al. 2014). The lack of this strategy is the possibility of the drug releasement only in near vicinity of the implant and the general resistance of the coating (Kyllönen et al. 2015).
A wide range of synthetic and natural polymers, ceramics and metals are available in the forms of micro- and nano-particles which represent very important systems for the delivery and sustained release of various agents for the treatment of a broad spectrum of diseases (Chau et al. 2008).
Particulated forms of biomaterials may adsorb or encapsulate drugs and deliver them to the place of releasement. Particles can be used alone, combined within cements, hydrogels and scaffolds or even form a coatings on implants. In any of these cases, the selected drug is being physically or chemically incorporated in/onto the particles and thus protected from degradation until its release begins in the target tissue. Different scaffolds with incorporated drug-loaded particles found to be more effective in enhancing osteogenesis in comparison with the scaffold alone with adsorbed BMP-2 (Wei et al. 2007). Controlled drug releasement depends on particle size, material properties, their degradability and formulation of delivery systems (Kim and Pack 2006). Pharmacokinetics of the applied drug is of a key importance for the selection of suitable system for their delivery.
Biodegradable polymer microparticles are the most common particulated biomaterial that has been used for controlled drug delivery due to biocompatibility and degradation mechanisms (Makadia and Siegel 2011). In bone therapy, PLGA based particles in combination with growth factors showed to stimulate osteogenic cell differentiation (Kirby et al. 2011).
Ca- and P-based particles have advantage over the other materials in bone regeneration, because of the similarity with the inorganic bone composition and high osteoconductivity as well as biocompatibility and bioactivity. Hydroxyapatite particles have a high affinity for proteins and other bioactive molecules and can be used with high efficiency to load and deliver drugs such as bisphosphonates (BP), growth factors etc. which are used in osteoporotic bone therapies (Lee et al. 2011). Combination with bioresorbable polymers such as PLGA, provide better systems for drug delivery because of slow PLGA degradation under physiological conditions. Sustained release of BP from PLGA/hydroxyapatite composite or from hydroxyaptite microsphere, reduces local osteoclastic activities (Boanini et al. 2008; Seshima et al. 2006).
HA/PLGA or HA alone nanoparticles that have been used as bioactive systems for vitamin D delivery have also showed to improve regeneration of osteoporotic bone (Ignjatović et al. 2013)
In addition to bone therapy, nanostructures are attractive biomaterials for other biomedical application because of their small sizes and an ability to deliver drugs inside target cells. They represent an effective approach in tumor therapy due to the possibility of targeting tumor cells, and avoiding side effects of conventional chemotherapy. Cell-specific targeting can be achieved by active mechanism, by applying functionalized NPs, or passive mechanisms, which refers to the effect of enhanced permeability and retention effect (EPR) (Acharya and Sahoo 2011; Steichen et al. 2013). Different nanostructures, such are liposomes, dendrimers, polymers, silicon or carbon materials, magnetic and gold nanoparticles, can serve as carriers for local drug delivery (De Jong and Borm 2008; Wilczewska et al. 2012). PLGA particles are widely in use as drug delivery systems due to low toxicity, biodegradability, biocompatibility and possibility for controlled and constant release of carried agents (Bala et al. 2004; Sadat et al. 2014). So far, they have been used for delivery of anti-cancer therapy, immunomodulatory agents, anti-hypertensive drugs and hormones. Carbon nanomaterials are widely examined as chemotherapy, carriers for genes and proteins, designed for potential applications in the cancer treatment (Liu et al. 2008, 2011). We have demonstrated that carbon nanotubes functionalized with a Toll-like receptor 7 agonist have immunomodulatory effects on human dendritic cells which can be applied in therapies (Čolić et al. 2014).
In cancer diagnostic and therapy, gold nanoparticles (GNPs) are also found as perspective carriers and agents for drug delivery because of their specific physical and chemical properties (Huang et al. 2007). Beside their tunable size and shape which enable controlled plasmon resonance for photo thermal therapeutic treatments by conversion of near-infrared light into thermal energy, they are biocompatible, not toxic and capable for drug delivery due to small dimensions and large surface area for functionalization with drugs, genes and biomolecules (Han et al. 2007). In our study, we investigated the effect of differently sized GNPs on functions of immune, dendritic, cells and found that 10 nm-sized GNPs have more powerful inhibitory effects on antitumor functions as well as maturation of DCs, in comparison with larger 50 nm-sized GNPs (Tomić et al. 2014).
Biomaterials used in medicine as medical devices are associated with risk of microbial infection. Bacteria growth made biofilms on their surfaces that are resistant to antibiotics and host immunity and may cause implant failure.
The approach of biomaterial coating with antimicrobial agents such as antimicrobial polymers, antibiotics, plant extracts etc. was found to be effective in obtaining therapeutically bioactive materials for the infection prevention. Plant extracts have shown great success in combating the various strains of bacteria. Staphylococcus aureus is the most frequent causer of biofilm formation on the material surfaces and therefore the coatings which prevent its colonization and biofilm growth are favorable. In addition to the biomaterials testing, we are dealing with antimicrobial, antioxidant and cytotoxic effects of different plant extracts often used in Ethnomedicine. Inula helenium and Carlinae radix essential oils showed significant antimicrobial effect against Staphylococcus aureus (Stojanović-Radić et al. 2012a, b). The potential use of these plant extracts as coatings on biomaterials, in order to prevent infection, is subjected to our further research.
6 Future Directions and Perspectives
Biomaterials from the so-called “third-generation” were constructed in the way so that, at the molecular level, are able to trigger specific cellular responses (Hench and Polak 2002) and to integrate the biodegradability and bioactivity concepts. Also, these biomaterials must be able to promote specific cellular actions and performances. The bioactivation of the biomaterials’ surface induced with biomolecules guide and stimulate cell migration, adhesion, proliferation as well as differentiation towards the certain cell line (Navarro et al. 2008).
Injectable cement composite mixed with living cells was obtained by involving undifferentiated bone marrow stromal cells into a hydrogel containing CaP particles. This kind of biomaterials are well vascularized and integrated into the host tissue upon implantation which has been shown on the mouse model (Trojani et al. 2006).
Development of bioactive and biodegradable 3D scaffolds with osteogenic and angiogenic potential is a major challenge, because cells cannot survive without an adequate blood supply. A possible alternative to improve osteogenic and angiogenic potential of the materials is incorporation of the active biomolecules such as growth factors into the scaffold (Allo et al. 2012).
Since shape, architecture and mechanical support are not enough for providing long-lasting structure for developing scaffold (Furth et al. 2007), designing of the smart biomaterials became one of the most important future directions in construction of bioactive materials (Davis et al. 2005). Smart biomaterials actively participate in functional tissue development (Furth et al. 2007). These biomaterials respond to their environment in previously determined manner which includes protein release. Consequently, delayed release as well as release stimulated by microenvironmental factors is possible (Anderson et al. 2004). Since microenvironmental factors have the influence on progenitor and stem cells differentiation, modification of bioactive injectable materials by using peptide-like nanofibers may be one of the key solutions in future cell therapies (Davis et al. 2005).
References
Acharya S, Sahoo SK (2011) PLGA nanoparticles containing various anticancer agents and tumour delivery by EPR effect. Adv Drug Deliv Rev 63(3):170–183
Aksay IA, Weiner S (1998) Biomaterials-is this really a field of research? Curr Opin Solid State Mater Sci 3(3):219–220
Allo BA, Costa DO, Dixon SJ et al (2012) Bioactive and biodegradable nanocomposites and hybrid biomaterials for bone regeneration. J Funct Biomater 3(2):432–463
Alsberg E, Anderson KW, Albeiruti A et al (2002) Engineering growing tissues. Proc Natl Acad Sci USA 99:12025–12030
Anderson DG, Burdick JA, Langer R (2004) Materials science. Smart biomaterials. Science 305(5692):1923–1924
Avnir D, Klein LC, Levy D et al (1997) Organo-silica Sol–gel materials. In: Apeloig Y, Rappoport Z (eds) The chemistry of organosilicon compounds—part 2. Wiley& Sons, Chichester
Awad HA, Wickham MQ, Leddy HA et al (2004) Chondrogenic differentiation of adipose-derived adult stem cells in agarose, alginate, and gelatin scaffolds. Biomaterials 25(16):3211–3222
Bala I, Hariharan S, Kumar MR (2004) PLGA nanoparticles in drug delivery: the state of the art. Crit Rev Ther Drug Carrier Syst 21(5):387–422
Bergman S, Litkowski L (1995) Bone in-fill of non-healing calvarial defects using particulate bioglass and autogenous bone. In: Wilson J, Hench LL, Greenspan D (eds) Bioceramics. Elsevier Science, Tarrytown, New York, pp 17–21
Biggs MJ, Richards RG, Gadegaard N et al (2007) The effects of nanoscale pits on primary human osteoblast adhesion formation and cellular spreading. J Mater Sci Mater Med 18(2):399–404
Bishop AT, Pelzer M (2007) Vascularized bone allotransplantation: current state and implications for future reconstructive surgery. Orthop Clin North Am 38(1):109–122
Blom EJ, Klein-Nulend J, Yin L et al (2001) Transforming growth factor-β1 incorporated in calcium phosphate cement stimulates osteotransductivity in rat calvarial bone defects. Clin Oral Implants Res 12(6):609–616
Boanini E, Torricelli P, Gazzano M et al (2008) Alendronate–hydroxyapatite nanocomposites and their interaction with osteoclasts and osteoblast-like cells. Biomaterials 29(7):790–796
Bökel C, Brown NH (2002) Integrins in development: moving on, responding to, and sticking to the extracellular matrix. Dev Cell 3(3):311–321
Botchwey EA, Dupree MA, Pollack SR et al (2003) Tissue engineered bone: measurement of nutrient transport in threedimensional matrices. J Biomed Mater Res A 67(1):357–367
Brånemark R, Brånemark PI, Rydevik B et al (2001) Osseointegration in skeletal reconstruction and rehabilitation: a review. J Rehabil Res Dev 38(2):175–181
Brinker CJ, Raman NK, Logan MN et al (1995) Structure-property relationships in thin films and membranes. J Sol–Gel Sci Technol 4(2):117–135
Burg KJ, Porter S, Kellam JF (2000) Biomaterial developments for bone tissue engineering. Biomaterials 21(23):2347–2359
Cao W, Hench LL (1996) Bioactive Materials. Ceram Int 22:493–507
Castner DG, Ratner BD (2002) Biomedical surface science: foundations to frontiers. Surf Sci 500(1):28–60
Chau D, Agashi K, Shakesheff K (2008) Microparticles as tissue engineering scaffolds: manufacture, modification and manipulation. Mater Sci Technol 24(9):1031–1044
Cornejo A, Sahar DE, Stephenson SM et al (2012) Effect of adipose tissue-derived osteogenic and endothelial cells on bone allograft osteogenesis and vascularization in critical-sized calvarial defects. Tissue Eng Part A 18(15–16):1552–1561
Cvetković VJ, Najdanović JG, Vukelić-Nikolić MĐ et al (2015) Osteogenic potential of in vitro osteoinduced adipose-derived mesenchymal stem cells combined with platelet-rich plasma in ectopic model. Int Orthop 39(11):2173–2180
Čolić M, Džopalić T, Tomić S et al (2014) Immunomodulatory effects of carbon nanotubes functionalized with a toll-like receptor 7 agonist on human dendritic cells. Carbon 67:273–287
Daculsi G, LeGeros RZ, Heughebaert M et al (1990) Formation of carbonateapatite crystals after implantation of calciumphosphate ceramics. Calcif Tissue Int 46(1):20–27
Davies JE (2003) Understanding peri-implant endosseous healing. J Dent Educ 67(8):932–949
Davis ME, Hsieh PCH, Grodzinsky AJ et al (2005) Custom design of the cardiac microenvironment with biomaterials. Circ Res 97(1):8–15
De Jong WH, Borm PJ (2008) Drug delivery and nanoparticles: applications and hazards. Int J Nanomed 3(2):133–149
De Jonge LT, van den Beucken JJ, Leeuwenburgh SC et al (2009) In vitro responses to electrosprayed alkaline phosphatase/calcium phosphate composite coatings. Acta Biomater 5(7):2773–2782
Friedman CD, Costantino PD, Jones K et al (1991) Hydroxyapatite cement. II. Obliteration and reconstruction of the cat frontal sinus. Arch Otolaryngol Head Neck Surg 117(4):385–389
Fu Q, Rahaman MN, Bal BS et al (2010a) Silicate, borosilicate, and borate bioactive glass scaffolds with controllable degradation rate for bone tissue engineering applications. II. In vitro and in vivo biological evaluation. J Biomed Mater Res A 95(1):172–179
Fu Q, Rahaman MN, Fu H et al (2010b) Silicate, borosilicate, and borate bioactive glass scaffolds with controllable degradation rate for bone tissue engineering applications. I. Preparation and in vitro degradation. J Biomed Mater Res A 95(1):164–171
Furth ME, Atala A, Van Dyke ME (2007) Smart biomaterials design for tissue engineering and regenerative medicine. Biomaterials 28(34):5068–5073
Ge Z, Baguenard S, Lim LY et al (2004) Hydroxyapatitechitin materials as potential tissue engineered bone substitutes. Biomaterials 25:1049
Gentile P, Chiono V, Tonda-Turo C et al (2011) Polymeric membranes for guided bone regeneration. Biotechnol J 6(10):1187–1197
Ginebra MP, Traykova T, Planell J (2006) Calcium phosphate cements as bone drug delivery systems: a review. J Controlled Release 113(2):102–110
Goldberg M, Smith AJ (2004) Cells and extracellular matrices of dentin and pulp: a biological basis for repair and tissue engineering. Crit Rev Oral Biol Med 15(1):13–27
Goldberg M, Lacerda-Pinheiro S, Jegat N et al (2006) The impact of bioactive molecules to stimulate tooth repair and regeneration as part of restorative dentistry. Dent Clin North Am 50(2):277–298
Goodman SB, Yao Z, Keeney M et al (2013) The future of biologic coatings for orthopaedic implants. Biomaterials 34(13):3174–3183
Green DW, Ben-Nissan B, Yoon K-S et al (2016) Bioinspired materials for regenerative medicine: going beyond the human archetypes. J Mater Chem B 4(14):2396–2406
Griffith CK, Miller C, Sainson RC et al (2005) Diffusion limits of an in vitro thick prevascularized tissue. Tissue Eng 11(1–2):257–266
Grotra D, Subbarao CV (2012) Bioactive materials used in endodontics. Rec Res Sci Tech 4(6):25–27
Guo D, Xu K, Zhao X et al (2005) Development of a strontium-containing hydroxyapatite bone cement. Biomaterials 26(19):4073–4083
Han G, Ghosh P, Rotello VM (2007) Multi-functional gold nanoparticles for drug delivery. Adv Exp Med Biol 620:48–56
He X, Liu Y, Yuan X et al (2014) Enhanced healing of rat calvarial defects with MSCs loaded on BMP-2 releasing chitosan/alginate/hydroxyapatite scaffolds. PLoS ONE 9:e104061. doi:10.1371/journal.pone.0104061
Healy KE, Guldberg RE (2007) Bone tissue engineering. J Musculoskelet Neuronal Interact 7(4):328–330
Hege CS, Schiller SM (2015) New bioinspired materials for regenerative medicine. Curr Mol Bio Rep 1(2):77–86
Hench LL (1980) Biomaterials. Science 208(4446):826–831
Hench LL (1998a) Bioactive materials: the potential for tissue regeneration. J Biomed Mater Res 41(4):511–518
Hench LL (1998b) Bioceramics. J Am Ceram Soc 81(7):1705–1728
Hench LL, Orefice R (1997) Sol–gel technology. In: Kirk-Othmer encyclopedia of chemical technology, 4th edn, vol 22. Wiley, New York, p 497
Hench LL, Polak JM (2002) Third-generation biomedical materials. Science 295(5557):1014–1107
Hench LL, West JK (1996) Biological applications of bioactive glasses. Life Chem Rep 13:187–241
Hench LL, Splinter RJ, Allen WC et al (1971) Bonding mechanisms at the interface of ceramic prosthetic materials. J Biomed Mater Res 5(6):117–141
Hench LL, Andersson OH, LaTorre GP (1991) The kinetics of bioactive ceramics part III: surface reactions for bioactive glasses compared with an inactive glass. Bioceramics 4:156–162
Huang X, Bai S, Lu Q et al (2014) Osteoinductive-nanoscaled silk/HA composite scaffolds for bone tissue engineering application. J Biomed Mater Res B Appl Biomater 103(7):1–13
Huang X, Jain PK, El-Sayed IH et al (2007) Gold nanoparticles: interesting optical properties and recent applications in cancer diagnostics and therapy. Nanomedicine (Lond) 2(5):681–693
Ignjatović N, Uskoković V, Ajduković Z et al (2013) Multifunctional hydroxyapatite and poly (D, L-lactide-co-glycolide) nanoparticles for the local delivery of cholecalciferol. Mater Sci Eng C Mater Biol Appl 33(2):943–950
Jarcho M, Kay JL, Gumaer RH et al (1977) Tissue, cellular and subcellular events at bone–ceramic hydroxyapatite interface. J Bioeng 1(2):79–92
Jazayeri HE, Tahriri M, Razavi M et al (2017) A current overview of materials and strategies for potential use in maxillofacial tissue regeneration. Mater Sci Eng C Mater Biol Appl 70(Pt 1):913–929
Jones JR (2009) New trends in bioactive scaffolds: the importance of nanostructure. J Eur Ceram Soc 29(7):1275–1281
Karande TS, Ong JL, Agrawal CM (2004) Diffusion in musculoskeletal tissue engineering scaffolds: design issues related to porosity, permeability, architecture, and nutrient mixing. Ann Biomed Eng 32(12):1728–1743
Karfeld-Sulzer LS, Weber FE (2012) Biomaterial development for oral and maxillofacial bone regeneration. J Korean Assoc Oral Maxillofac Surg 38(5):264–270
Kato K, Eika Y, Ikada Y (1996) Deposition of hydroxiapatite thin layer onto a polymer surface carrying grafted phosphate polymer chains. J Biomed Mater Res 32(4):687–691
Keeting PE, Oursler MJ, Wiegand KE et al (1992) Zeolite A increases proliferation, differentiation, and transforming growth factor beta production in normal adult human osteoblast-like cells in vitro. J Bone Mineral Res 7(11):1281–1289
Keshaw H, Forbes A, Day RM (2005) Release of angiogenic growth factors from cells encapsulated in alginate beads with bioactive glass. Biomaterials 26(19):4171–4179
Kim IS, Park JW, Kwon IC et al (2002) Role of BMP, betaig-h3, and chitosan in early bony consolidation in distraction osteogenesis in a dog model. Plast Reconstr Surg 109:1966
Kim KK, Pack DW (2006) Microspheres for drug delivery. In: Ferrari M, Lee AP, Lee LJ (eds) BioMEMS and Biomed Nanotechnol. Springer, New York, pp 19–50
Kim S, Ku SH, Lim SY et al (2011) Graphene–biomineral hybridmaterials. Adv Mater 23(17):2009–2014
Kirby GT, White LJ, Rahman CV et al (2011) PLGA-based microparticles for the sustained release of BMP-2. Polymers 3(1):571–586
Kostic M, Krunic N, Nikolic L et al (2011) Influence of residual monomer reduction on acrylic denture base resins quality. Hemijska industrija 65(2):171–177
Kokubo T (1990) Surface chemistry of bioactive glass-ceramics. J Non-Cryst Solids 120(1–3):138–151
Kokubo T, Shigematsu M, Nagashima Y et al (1982) Apatite- and wollastonite-containing glass-ceramics for prosthetic application. Bull Inst Chem Res Kyoto Univ 60(3–4):260–268
Kokubo T, Kim HM, Kawashita M (2003) Novel bioactive materials with different mechanical properties. Biomaterials 24(13):2161–2175
Krunić N, Lj Nikolić, Kostić M et al (2011) In vitro examination of oral tissue conditioners potential toxicity. Chem Ind 65(6):697–706
Kyllönen L, D’Este M, Alini M et al (2015) Local drug delivery for enhancing fracture healing in osteoporotic bone. Acta Biomater 11:412–434
Langer R, Tirrell DA (2004) Designing materials for biology and medicine. Nature 428:487–492
Langer R, Vacanti JP (1993) Tissue engineering. Science 260(5110):920–926
Lee JH, Ko IH, Jeon SH et al (2011) Localized drugs delivery hydroxyapatite microspheres for osteoporosis therapy. In: Proceedings of SPIE, biosens nanomed IV: 8099 of 80990K, San Diego, Calif, USA
LeGeros RZ (2002) Properties of osteoconductive biomaterials: calcium phosphates. Clin Orthopaed Related Res 395:81–98
Levingstone TJ, Matsiko A, Dickson GR et al (2014) biomimetic multi-layered collagen-based scaffold for osteochondral repair. Acta Biomater 10(5):1996–2004
Li H, Zheng Y, Qin L (2014) Progress of biodegradable metals. Prog Nat Sci Mater Int 24(5):414–422
Li J, Hsu Y, Luo E et al (2011) Computer-aided design and manufacturing and rapid prototyped nanoscale hydroxyapatite/polyamide (n-HA/PA) construction for condylar defect caused by mandibular angle ostectomy. Aesthet Plast Surg 35(4):636–640
Li M, Liu X, Ge B (2010) Calcium phosphate cement with BMP-2-loaded gelatin microspheres enhances bone healing in osteoporosis: a pilot study. Clin Orthop Relat Res 468(7):1978–1985
Liu Y, Enggist L, Kuffer AF et al (2007) The influence of BMP-2 and its mode of delivery on the osteoconductivity of implant surfaces during the early phase of osseointegration. Biomaterials 28(16):2677–2686
Liu Z, Chen K, Davis C et al (2008) Drug delivery with carbon nanotubes for in vivo cancer treatment. Cancer Res 68(16):6652–6660
Liu Z, Robinson JT, Tabakman SM et al (2011) Carbon materials for drug delivery & cancer therapy. Mater Today 14(7–8):316–323
Long F (2011) Building strong bones: molecular regulation of the osteoblast lineage. Nat Rev Mol Cell Biol 13(1):27–38
Loty C, Sautier JM, Boulekbache H et al (2000) In vitro bone formation on a bonelike apatite layer prepared by a biomimetic process on a bioactive glass-ceramic. J Biomed Mater Res 49(4):423–434
Lu HH, Tang A, Oh SC et al (2005) Compositional effects on the formation of a calcium phosphate layer and the response of osteoblast-like cells on polymer-bioactive glass composites. Biomaterials 26(32):6323–6334
Lutolf MP, Weber FE, Schmoekel HG et al (2003) Repair of bone defects using synthetic mimetics of collagenous extracellular matrices. Nat Biotechnol 21(5):513–518
Ma Z, Gao C, Gong Y et al (2002) Immobilization of natural macromolecules on poly-L-lactic acid membrane surface in order to improve its cytocompatibility. J Biomed Mater Res 63(6):838–847
Makadia HK, Siegel SJ (2011) Poly lactic-co-glycolic acid (PLGA) as biodegradable controlled drug delivery carrier. Polymers (Basel) 3(3):1377–1397
Marchesan S, Prato M (2013) Nanomaterials for (Nano)medicine. ACS Med Chem Lett 4(2):147–149
Marion NW, Liang W, Reilly GC et al (2005) Borate glass supports the in vitro osteogenic differentiation of human mesenchymal stem cells. Mech Adv Mater Struct 12(3):239–246
Mauth C, Huwig A, Graf-Hausner U et al (2007) Restorative applications for dental pulp therapy. In: Ashammakhi N, Reis RL, Chiellini (eds) Topics in tissue engineering, vol 3, pp 1–30
Minelli EB, Benini A (2007) PMMA as drug delivery system and in vivo release from spacers. In: Romano C, Crosby L, Hofmann G, Meani E (eds) Infection and local treatment in orthopedic surgery. Springer, New York, pp 79–91
Najdanović JG, Cvetković VJ, Stojanović S et al (2015) The influence of adipose-derived stem cells induced into endothelial cells on ectopic vasculogenesis and osteogenesis. Cell Mol Bioeng 8(4):577–590
Najdanović JG, Cvetković VJ, Stojanović S et al (2016) Effects of bone tissue engineering triad components on vascularization process: comparative gene expression and histological evaluation in an ectopic bone-forming model. Biotechnol Biotechnol Equip 30(6):1122–1131
Najman SJ, Cvetković VJ, Najdanović JG et al (2016) Ectopic osteogenic capacity of freshly isolated adipose-derived stromal vascular fraction cells supported with platelet-rich plasma: a simulation of intraoperative procedure. J Craniomaxillofac Surg 44(10):1750–1760
Narmoneva DA, Oni O, Sieminski AL et al (2005) Self-assembling short oligopeptides and the promotion of angiogenesis. Biomaterials 26(23):4837–4846
Navarro M, Michiardi A, Castaño O et al (2008) Biomaterials in orthopaedics. J R Soc Interface 5(27):1137–1158
Nayak TR, Andersen H, Makam VS et al (2011) Graphene for controlled and accelerated osteogenic differentiation of human mesenchymal stem cells. ACS Nano 5(6):4670–4678
Neut D, Hendriks JG, van Horn JR et al (2005) Pseudomonas aeruginosa biofilm formation and slime excretion on antibiotic-loaded bone cement. Acta Orthop 76(1):109–114
Odabasoglu F, Yildirim OS, Aygun H et al (2012) Diffractaic acid, a novel proapoptotic agent, induces with olive oil both apoptosis and antioxidative systems in Ti-implanted rabbits. Eur J Pharmacol 674(2–3):171–178
Oguntebi B, Clark A, Wilson J (1993) Pulp capping with bioglass and autologous demineralized dentin in miniature swine. J Dent Res 72(2):484–489
Ohtsuki C, Kamitakahara M, Miyazaki T (2009) Bioactive ceramic-based materials with designed reactivity for bone tissue regeneration. J R Soc Interface 6(Suppl 3):S349–S360
O’Keefe RJ, Mao J (2011) Bone tissue engineering and regeneration: from discovery to the clinicean overview. Tissue Eng Part B Rev 17(6):389–392
Oonishi H, Kushitani S, Iwaki H (1995) Comparative bone formation in several kinds of bioceramic granules. In: Wilson J, Hench LL, Greenspan D (eds) Eighth international symposium on ceramics in medicine. Elsevier Science Ltd, Tokyo, pp 137–144
Oonishi H, Kushitani S, Yasukawa E et al (1997) Particulate bioglass compared with hydroxyapatite as a bone g raft substitute. J Clin Orthop Rel Res 334:316–325
Pereira MM, Hench LL (1996) Mechanisms of hydroxyapatite formation on porous gel-silica matrices. J Sol–Gel Sci Technol 7(1):59–64
Pereira MM, Clark AE, Hench LL (1994) Calcium phosphate formation on sol–gel derived bioactive glasses in vitro. J Biomed Mater Res 28(6):693–698
Piotrowski G, Hench LL, Allen WC et al (1975) Mechanical studies of the bone bioglass interfacial bond. J Biomed Mater Res 9(4):47–61
Puleo DA, Nanci A (1999) Understanding and controlling the bone–implant interface. Biomaterials 20(23–24):2311–2321
Pyo SW, Kim YM, Kim CS et al (2014) Bone formation on biomimetic calcium phosphate-coated and zoledronate-immobilized titanium implants in osteoporotic rat tibiae. Int J Oral Maxillofac Implants 29(2):478–484
Rajković J, Stojanović S, Đorđević L et al (2015) Locally applied cholecalciferol and alfacalcidol act differently on healing of femur defects filled with bone mineral matrix and platelet-rich plasma in ovariectomized rats. Biotechnol Biotechnol Equip 29(5):963–969
Ratner BD, Hoffman AS, Schoen FJ et al (2004) Biomaterials science: an introduction to materials in medicine, 2nd edn. Academic Press, New York
Rejda BV, Peelen JGJ, de Groot K (1977) Tricalcium phosphate as a bone substitute. J Bioeng 1(2):93–97
Roberts HW, Toth JM, Berzins DW et al (2008) Mineral trioxide aggregate material use in endodontic treatment: a review of the literature. Dent Mater 24(2):149–164
Sachse A, Wagner A, Keller M et al (2005) Osteointegration of hydroxyapatite-titanium implants coated with nonglycosylated recombinant human bone morphogenetic protein-2(BMP-2) in aged sheep. Bone 37(5):699–710
Sadat Tabatabaei Mirakabad F, Nejati-Koshki K, Akbarzadeh A et al (2014) PLGA-based nanoparticles as cancer drug delivery systems. Asian Pac J Cancer Prev 15(2):517–535
Salem AK, Stevens R, Pearson RG et al (2002) Interactions of 3T3 fibroblasts and endothelial cells with defined pore features. J Biomed Mater Res 61(2):212–217
Salinas AJ, Vallet-Regı M (2013) Bioactive ceramics: from bone grafts to tissue engineering. RSC Advances 3(28):1116–1131
Salinas AJ, Esbrit P, Vallet-Regí M (2013) A tissue engineering approach based on the use of bioceramics for bone repair. Biomater Sci 1(1):40–51
Schek RM, Taboas JM, Hollister SJ et al (2005) Tissue engineering osteochondral implants for temporomandibular joint repair. Orthod Craniofacial Res 8(4):313–319
Schepers E, de Clercq M, Ducheyne P et al (1991) Bioactive glass particulate material as a filler for bone lesions. J Oral Rehabil 18(5):439–452
Schouten C, van den Beucken JJ, Meijer GJ et al (2010) In vivo bioactivity of DNA-based coatings: an experimental study in rats. J Biomed Mater Res A 92(3):931–941
Schroeder JE, Mosheiff R (2011) Tissue engineering approaches for bone repair: concepts and evidence. Injury 42(5):609–613
Seitz TL, Noonan KD, Hench LL et al (1982) Effect of fibronectin on the adhesion of an established cell line to a surface reactive biomaterial. J Biomed Mater Res 16(3):195–207
Seshima H, Yoshinari M, Takemoto S et al (2006) Control of bisphosphonate release using hydroxyapatite granules. J Biomed Mater Res B Appl Biomater 78(2):215–221
Sharma M, Murray PE, Sharma D (2013) Modern approaches to use bioactive materials and molecules in medical and dental treatments. Int J Curr Microbiol App Sci 2(11):429–439
Shi C, Zhu Y, Ran X et al (2006) Therapeutic potential of chitosan and its derivatives in regenerative medicine. J Surg Res 133(2):185–192
Shi X, Chang H, Chen S et al (2012) Regulating cellular behavior on few-layer reduced graphene oxide films with well-controlled reduction states. Adv Funct Mater 22(4):751–759
Shin SR, Li YC, Jang HL et al (2016) Graphene-based materials for tissue engineering. Adv Drug Deliv Rev 105(Pt B):255–274
Shores EC, Holmes RE (1993) Porous hydroxyapatite. In: Hench LL, Wilson J (eds) An introduction to bioceramics. World Scientific, Singapore, pp 181–198
Siebers M, Ter Brugge P, Walboomers X et al (2005) Integrins as linker proteins between osteoblasts and bone replacing materials. A critical review. Biomaterials 26(2):137–146
Steichen SD, Caldorera-Moore M, Peppas NA (2013) A review of current nanoparticle and targeting moieties for the delivery of cancer therapeutics. Eur J Pharm Sci 48(3):416–427
Stevens MM (2008) Biomaterials for bone tissue engineering. Mater Today 11(5):18–25
Stevens MM, Qanadilo HF, Langer R et al (2004) A rapid-curing alginate gel system: utility in periosteum-derived cartilage tissue engineering. Biomaterials 25(5):887–894
Stojanović IŽ, Najman S, Jovanović O et al (2014) Effects of depsidones from Hypogymnia physodes on HeLa cells viability and growth. Folia Biol (Praha) 60(2):89–94
Stojanović-Radić Z, Čomić L, Radulović N et al (2012a) Antistaphylococcal activity of Inula helenium L. root essential oil: eudesmane sesquiterpene lactones induce cell membrane damage. Eur J Clin Microbiol Infect Dis 31(6):1015–1025
Stojanović-Radić Z, Čomić L, Radulović N et al (2012b) Commercial Carlinae radix herbal drug: Botanical identity, chemical composition and antimicrobial properties. Pharmaceutical biology 50(8):933–940
Takić-Miladinov D, Tomić S, Stojanović S et al (2016) Synthesis, swelling properties and evaluation of genotoxicity of hydrogels based on (Meth)acrylates and Itaconic Acid. Mat Res 19(5):1070–1079
Thein-Han W, Liu J, Xu HH (2012) Calciumphosphate cement with biofunctional agents and stem cell seeding for dental and craniofacial bone repair. Dent Mater 28(10):1059–1070
Tirapelli C, Panzeri H, Soares RG et al (2010) A novel bioactive glass-ceramic for treating dentin hypersensitivity. Braz Oral Res 24(4):381–387
Tomić S, Đokić J, Vasilijić S et al (2014) Size-dependent effects of gold nanoparticles uptake on maturation and antitumor functions of human dendritic cells in vitro. PLoS ONE 9(5):e96584. doi:10.1371/journal.pone.0096584
Tonnesen HH, Karlsen J (2002) Alginate in drug delivery systems. Drug Dev Ind Pharm 28(6):621–630
Trojani C, Boukhechba F, Scimeca JC et al (2006) Ectopic bone formation using an injectable biphasic calcium phosphate/Si-HPMC hydrogel composite loaded with undifferentiated bone marrow stromal cells. Biomaterials 27(17):3256–3264
Tsigkou O, Hench LL, Boccaccini AR et al (2007) Enhanced differentiation and mineralization of human fetal osteoblasts on PDLLA containing Bioglass® composite films in the absence of osteogenic supplements. J Biomed Mater Res A 80(4):837–852
Vallet-Regi M, Ruiz-Hernandez E (2011) Bioceramics: from bone regeneration to cancer nanomedicine. Adv Mater 23(44):5177–5218
van de Watering FC, Molkenboer-Kuenen JD, Boerman OC et al (2012) Differential loading methods for BMP-2 within injectable calcium phosphate cement. J Control Release 164(3):283–290
Venkatesan J, Pallela R, Kim S-K (2014) Applications of carbon nanomaterials in bone tissue engineering. J Biomed Nanotechnol 10(10):3105–3123
Verron E, Khairoun I, Guicheux J et al (2010) Calcium phosphate biomaterials as bone drug delivery systems: a review. Drug Discov Today 15(13–14):547–552
Vogel M, Voigt C, Gross U et al (2001) In vivo comparison of bioactive glass particles in rabbits. Biomaterials 22(4):357–362
Vrouwenvelder CA, Groot CG, de Groot KJ (1993) Histological and biochemical evaluation of osteoblasts cultured on bioactive glass, hydroxylapatite, titanium alloy, and stainless steel. J Biomed Mater Res 27(4):465–475
Wang H-L, Carroll WJ (2001) Guided bone regeneration using bone grafts and collagen membranes. Quintessence Int 32(7):504–515
Wang XP, Li X, Ito A et al (2011) Synthesis and characterization of hierarchically macroporous and mesoporous CaO–MO–SiO(2)–P(2)O(5) (M = Mg, Zn, Sr) bioactive glass scaffolds. Acta Biomater 7(10):3638–3644
Wei G, Jin Q, Giannobile WV et al (2007) The enhancement of osteogenesis by nano-fibrous scaffolds incorporating rhBMP-7 nanospheres. Biomaterials 28(12):2087–2096
Wheeler DL, Stokes KE (1997) In vivo evaluation of sol–gel bioglasst: part I: histological findings. In: Transactions of the 23rd annual meeting of the society for biomaterials, New Orleans, LA
Wheeler DL, Stokes KE, Hoellrich RG et al (1998) Effect of bioactive glass particle size on osseous regeneration of cancellous defects. J Biomed Mater Res 41(4):527–533
Wilczewska AZ, Niemirowicz K, Markiewicz KH et al (2012) Nanoparticles as drug delivery systems. Pharmacol Rep 64(5):1020–1037
Wilson J, Yli-Urpo A, Risto-Pekka H (1993) Bioactive glasses: clinical applications. In: Hench LL, Wilson J (eds) An introduction to bioceramics. World Scientific, Singapore, pp 63–74
Winslow BD, Shao H, Stewart RJ et al (2010) Biocompatibility of adhesive complex coacervates modeled after the Sandcastle glue of P. californica for craniofacial reconstruction. Biomaterials 31(36):9373–9381
Wu CC, Wang CC, Lu DH et al (2012) Calcium phosphate cement delivering zoledronate decreases bone turnover rate and restores bone architecture in ovariectomized rats. Biomed Mater 7(3):035009
Xu HH, Takagi S, Quinn JB et al (2004) Fast-setting calcium phosphate scaffolds with tailored macropore formation rates for bone regeneration. J Biomed Mater Res A 68(4):725–734
Xynos ID, Edgar AJ, Buttery LDK et al (2001) Gene-expression profiling of human osteoblasts following treatment with the ionic products of BioglassW 45S5 dissolution. J Biomed Mater Res 55(2):151–157
Yamamuro T (1993) A/W glass-ceramic: clinical applications. In: Hench LL, Wilson J (eds) An introduction to bioceramics. World Scientific, Singapore, pp 89–104
Yu X, Wang L, Jiang X et al (2012) Biomimetic CaP coating incorporated with parathyroid hormone improves the osseointegration of titanium implant. J Mater Sci Mater Med 23(9):2177–2186
Yuan H, Fernandes H, Habibovic P et al (2010) Osteoinductive ceramics as a synthetic alternative to autologous bone grafting. Proc Natl Acad Sci USA 107(31):13614–13619
Zheng K, Yang SB, Wang JJ et al (2012) Characteristics and biocompatibility of Na(2)O–K(2)O–CaO–MgO–SrO–B(2)O(3)–P(2)O(5) borophosphate glass fibers. J Non-Cryst Solids 358(2):387–391
Zimmermann WH, Melnychenko I, Eschenhagen T (2004) Engineered heart tissue for regeneration of diseased hearts. Biomaterials 25(9):1639–1647
Živković J, Najman S, Vukelić M et al (2015) Osteogenic effect of inflammatory macrophages loaded onto mineral bone substitute in subcutaneous implants. Arch Biol Sci 67(1):173–186
Acknowledgements
This work was supported by the Ministry of Education, Science and Technological Development of the Republic of Serbia [grant number III 41017].
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Najdanović, J., Rajković, J., Najman, S. (2018). Bioactive Biomaterials: Potential for Application in Bone Regenerative Medicine. In: Zivic, F., Affatato, S., Trajanovic, M., Schnabelrauch, M., Grujovic, N., Choy, K. (eds) Biomaterials in Clinical Practice . Springer, Cham. https://doi.org/10.1007/978-3-319-68025-5_12
Download citation
DOI: https://doi.org/10.1007/978-3-319-68025-5_12
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-68024-8
Online ISBN: 978-3-319-68025-5
eBook Packages: EngineeringEngineering (R0)