Abstract
Disruptive behaviors in health care can have a profound effect on staff relationships that can lead to impaired communication, reduced information transfer, and dysfunctional team collaboration that can negatively impact patient care. Recognizing what disruptive behavior is and what it can do is the first step in enabling organizations to develop appropriate programs and effective strategies to reduce its occurrence. Disruptive behaviors occur across all disciplines, but when physicians are involved, by virtue of their role as captain of the ship, it can set off a chain of events that seriously compromises process and flow. By gaining a better understanding of the forces shaping physician attitudes and behaviors, organizations can then provide the necessary assistance and resource support to enhance behavioral adjustments. The ultimate goal is to not only reduce the incidence of disruptive events, but to also improve overall staff relationships, care efficiency, and instill a positive work atmosphere that increases staff morale, physician engagement, and overall satisfaction.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Physicians spend years of training and dedication developing their skills to provide excellent care to their patients. Most of their training focused on improving their knowledge and technical competencies in an effort to master their craft. Until recently, little attention has been paid to improving their interpersonal skills which are necessary for effective leadership, communication efficiency, and team collaboration. Most of the time physicians provide services in a professional manner leading to successful outcomes of care. However, for a variety of different reasons, there are other times when physicians act unprofessionally to the point where it becomes disruptive to staff relationships and can compromise patient safety and quality of care (Rosenstein and O’Daniel 2008; The Joint Commission 2008; Dang et al. 2016). Despite the fact that this is such a significant issue, many organizations still struggle to address disruptive behavior in an effective manner (Rosenstein 2015a). Reducing the incidence of disruptive behaviors will require a multistep approach that includes a combination of education, training, intervention, counseling, and resource support to enhance compliance with expected professional behavioral standards (Rosenstein 2015b).
2 Definition
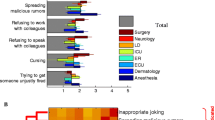
The first step in the process is to raise awareness of what disruptive behavior is. The term disruptive behavior was originally used to describe any inappropriate behavior, confrontation, or conflict ranging from verbal abuse to physical or sexual harassment that can potentially negatively impact patient care (Rosenstein and O’Daniel 2008). The types of offensive behaviors described in this category include yelling; abusive language; condescending, berating, or disrespectful behaviors; overt bullying; or intimidation. Direct physical abuse is reported to occur less than 5% of the time (Fig. 3.1). More recently, The Joint Commission modified the definition to remove the term “disruptive behavior” and to redefine such behaviors as any behavior that can undermine a culture of safety (http://www.jointcommission.org/assets/1/6/Leadership standard_behaviors.pdf). While that is a general definition, each organization should develop its own operational definition of disruptive behavior that is clear and appropriate to their organizational mission and objectives. This is crucial prior to developing appropriate policies (such as a Code of Conduct Policy) and procedures (such as how the organization will respond to alleged disruptive behaviors), which set the expectations for professional behaviors and hold noncompliant individuals accountable for their actions.
3 Causes
The next step is to try to figure out why these types of behavior occur. Nobody intentionally starts the day planning to be disruptive; it’s just that a variety of disturbances can get in the way. In an effort to provide effective strategies to reduce their occurrence, we need to gain a better understanding of the factors affecting physician values, attitudes, and behaviors. Table 3.1 divides these factors into two categories: internal and external forces. We recognize that it is impossible to apply a cause-and-effect relationship to each individual factor; instead, we need to consider the interplay of these factors and their role in influencing emotions and reactions.
3.1 Internal Factors
Age and generational issues are based on the values and perceptions reinforced by the existing status of the social, economic, and political environment at the time in which the individual grew up. Differences in views as to work ethic, commitment, views of authority, and work-personal life balance are different for each of the groups (variously defined such as Millennials <1980–1995>, Generation X or Gen X<1965–1979>, Baby Boomers <1946–1964>, Veterans/Traditionalists <pre 1946>), which under stressful situations may lead to conflict in the workplace environment. Various assumptions are made about generational differences and medical professionalism among millennials and those from Gen X, such as a declining work ethic and commitment, less willingness to work long hours, and a greater focus on lifestyle balance compared to the older generations (Smith 2005). During stressful periods some of these differences can lead to potential conflicts in workplace dynamics. Other differences have been noted between millennials and Gen X medical trainees (Borges et al. 2010). On the other hand, a survey study of 1178 physicians comparing baby boomers to Gen X doctors found no generational differences regarding commitment to medicine, job satisfaction, patient care attitudes, work-home balance, perceptions of work load, or use of harmful coping strategies (Lemaire et al. 2013). Moreover, Gen X physicians did not work fewer hours but were more likely to report burnout than baby boomers. While conclusions cannot rest on a single study, it is important not to stereotype generations based on impressions, which may increase conflict between them, nor to minimize real differences. It’s not that either group is right or wrong, it’s just that they have different ideas and approaches to work responsibilities (Executive Dialogue 2013). As the older workforce retires and the younger workforce moves in, the issue of how to deal with millennials is taking center stage (Thew 2015). Accordingly, many organizations have addressed the issue by offering programs that educate physicians about generational differences and similarities and to provide strategies to help them reach compromises during periods of conflict or disagreement (Roberts et al. 2012).
Gender: Women make up an increasingly larger proportion of physicians in Canada, the USA, Australia, the Netherlands, and the UK (Lemaire et al. 2013). Differences between male and female physicians may affect the way they react in stressful situations. Women are more likely than men to feel overworked and burned out, report work-family conflicts, shoulder child care and household duties, and reduce their work hours after their children are born. Consequently, they have been considered to be less committed to their medical career (Lemaire et al. 2013). In terms of coping responses, women are more likely than men to talk with colleagues about problems and to receive social support from relatives and friends in addition to coworkers. Men are more likely to keep their stress to themselves, dig in, and focus all their attention to the task at hand. They are also more likely to use humor as a way to pacify the situation (Gray 2004). In the past these differences were exacerbated by the predominantly female nursing workforce and the predominantly male physician task force. While the percentages are changing, potential conflicts may still arise. Many organizations have addressed these issues by educating staff on sexual equality and harassment (Jagsi et al. 2015). Other issues related to gender workforce equality and tolerance or discrimination to sexual orientation may also influence individual behaviors.
Culture and ethnicity: As the world situation changes, we are seeing a greater diversity in our patient and staff populations with a greater influx of foreign-born or foreign-trained nursing and medical staff in the USA. They come with their own ethnic, cultural, and religious beliefs that affect values, thoughts, and beliefs as to religion and spirituality, hierarchy, authority, and communication styles. In difficult situations this can lead to misunderstandings in purpose and intent that may negatively affect communication efficiency, expectations, and outcomes. In this regard, there is a big push toward training providers on cultural competency and/or providing diversity training to help individuals better understand individual needs and values, address hidden assumptions or biases, and provide effective solutions for more effective communication (Beach et al. 2005; Williams and Wyatt 2016; Curtis et al. 2007; Holm et al. 2017).
All of these factors combined with genetics, socioeconomic factors, geographic influences, and other individual life experiences help to shape an individual’s personality (McCracken and Hicks 2012).
Relationship management: Given the multidimensional influences contributing to attitudes and behaviors, key strategies for improvement should focus on introducing a variety of different training programs designed to enhance personality and relationship management. These programs might include such topics as sensitivity training, diversity management, cultural competency, mindfulness, generational gap values, personality traits, conflict management, stress management, anger management, sexual harassment training, customer satisfaction, and improving overall communication and collaboration skills. Some organizations have added a more in-depth focus by providing training in emotional intelligence to enhance staff and patient relationships (Rosenstein and Stark 2015; Goleman 1995). The process includes a four step approach designed to (a) enable the individual to gain a better understanding of their own individual perceptions, values, biases, and trigger points, (b) raise social awareness by enabling the individual to better recognize the perceptions, needs, and values of others, (c) learn how to modify their own behaviors, and (d) be more sensitive to the cues and reactions needed to foster a positive relationship and positive outcome. Each of these programs have value, but success will depend on the specific situation, underlying organizational dynamics, culture, leadership commitment, and individual motivation.
All of these internal factors have a deep-seated impact on a person’s mood, disposition, character, and personality, and may be more difficult to address than some of the external factors to be discussed in the next section.
3.2 External Factors
Training environment: The external factors include current day circumstances that influence present state perceptions. For physicians one of the key factors starts with the training environment. Some equate this training to a fraternity/sorority hazing type environment where individuals are harassed to the point of losing self-esteem. In some cases, this can lead to severe cases of stress, burnout, depression, and suicidal ideation (Karim and Duchcherer 2014; Mata et al. 2015; Dyrbye et al. 2010). In response, trainees try to develop knowledge and technical competencies through exhaustive independent study. As a consequence, there is less focus on developing personal and team collaboration skills, which leads to a lower degree of sensitivity and emotional intelligence. This presents a definite liability in today’s complex multi-spectrum health care environment so dependent on multidisciplinary collaboration and full spectrum care. The problem is further exacerbated by the traditional hierarchal health care structure with dedicated roles and responsibilities and set boundaries between the different health care disciplines. This is further accentuated by the different incentives and priorities of administrative management. Fortunately, there are movements in place to try and deal with these training hazards. Many medical schools are now looking for more “well-rounded” and “better adjusted” students who are majoring in something other than the traditional math and science tracks (Schwartzstein 2015; Rappleye 2015). The MCAT (Medical College Admission Test) now includes questions on sociology and humanities (Schwartzstein et al. 2013). Some of the more progressive medical schools are adding programs that focus on improving emotional intelligence and communication skill efficiencies, in some cases pairing medical students with nursing students, pharmacy students, and individuals from other disciplines during their freshman year to learn about the different perspectives on care management responsibilities (Lutfiyya et al. 2016; Muller 2013; Reeves et al. 2015; Brock et al. 2013). The overall goal is to build personal relationships and develop team competencies along with clinical expertise.
Health Care Reform has added another level of stress to the work environment. Whereas physicians used to pride themselves on their ability to provide excellent care with autonomy and control, the introduction of new regulations, utilization controls, changing incentives, and performance/accountability metrics has forced many physicians to reassess their positions and change models of care. In addition, the growing complexity of health care management, frustrations of dealing with electronic documentation and other administrative requirements, less time spent on direct face-to-face patient care with increasing productivity demands, and medical school debt can have a significant negative impact on physician attitudes and behaviors (Shanafelt et al. 2016). Furthermore, many physicians fear adverse outcomes, malpractice litigation, and having to share bad news with families. During tense moments in the operating room, emergency department, and critical care units, a physician’s perception of non-responsiveness or incompetence on the part of other team members may fuel disruptive behavior. Ironically, such behavior can increase the risk of adverse events and litigation (Hickson and Entman 2008; Rosenstein 2013). As far as a remedy, it’s unlikely that we’ll be able to change the system, although physicians can hopefully expect that electronic health record software will evolve to better facilitate physician work-flow (Ratwani et al. 2015). We can also provide more education to help the physician better understand why this is occurring, the intent, what the projected service impact will be, and then provide the necessary support to help physicians adapt in meeting these new objectives. Dealing with stress and burnout has the greatest potential for success.
Stress and Burnout: Stress and burnout can often provide the tipping force for the onset of disruptive behaviors (Rosenstein 2016a). Recent studies have shown that more than 50% of physicians report a significant amount of stress and burnout that has led to increasing irritability, cynicism, apathy, fatigue, disillusionment, dissatisfaction, and in some cases more serious depression, behavioral disorders, and even suicidal ideation (Shanafelt et al. 2015a; Privitera et al. 2014; Danielson et al. 2013; Rosenstein 2012a). As a result, there has been a significant drop in physician morale and a growing amount of physician dissatisfaction, and many physicians have either changed practice settings, joined different groups, or moved into salaried positions (The Physicians Foundation 2016). Others have either left the profession entirely or chose early retirement. Not a good situation particularly with the looming physician shortage.
So how should physicians deal with stress and burnout? The first issue is physician awareness. Many physicians are unaware that they are working under stress and the physical and emotional toll it’s taking on their livelihood. If they do admit that they are under stress, they accept it as being part of the job and rationalize that they have been working under stress all their lives. Even if they think they may need some outside help, they are reluctant to ask in fear of concerns about their competency, confidentiality, discoverability, or being stigmatized (Kay et al. 2008; O’Reilly 2012). These are significant barriers that need to be addressed before moving forward. If physicians are reluctant to admit their distress or receive assistance, we need to look for the organizations that they are associated with to take a more proactive role in trying to encourage and provide support.
Where to begin? As mentioned previously, there is a growing amount of evidence suggesting that high levels of stress, burnout, depression, and even suicidal ideation start during the first year of medical school (Schwenk et al. 2010). This probably results from a combination of factors of having individuals driven by a strong, competitive, and egocentric personality being dropped into an intensely complex and bewildering hierarchal system without direction and a sense of nowhere to go. These problems are further exacerbated by a sense of physical and emotional exhaustion, stress, and fatigue, which can take a toll on physical and mental well-being. One of the major barriers is the student’s as well as physicians’ reluctance to seek help for issues related to stigma and/or time (Gold et al. 2016). Fortunately, many organizations are making a concerted effort to provide resources to help trainees adjust to the pressures in the academic environment (Salles et al. 2015).
Once a physician gets out into practice, there are other day-to-day pressures that promote a stressful environment. As mentioned previously, many physicians are either unaware or reluctant to admit that they are under stress, and even if they do recognize it, they won’t take any action on their own. In this case, physicians need to look for outside assistance from friends, peers, or the organizations with which they are associated to help. The most consistent approach is to provide proactive support at the organizational level. Unfortunately, many physicians feel that their organizations don’t support them. In a recent study conducted by Cejka Search and VITAL WorkLife, when asked if their organization did anything currently to help physicians deal more effectively with stress and/or burnout, 85% of the respondents said no (2014). Another study conducted by InCrowd showed similar findings reporting that 75% of surveyed physicians did not feel that their organization was doing anything to address burnout (Rappleye 2016). So, in an effort to better address the issue of physician stress and burnout, we need to (1) raise awareness, (2) motivate effective physician responses, and (3) have organizations take a more active role in providing support services to help physicians better adjust to the stress and pressures of today’s health care environment.
Support can come from a variety of different directions and a variety of individual and organizational interventions demonstrate effectiveness (West et al. 2016). At one level the organization can provide training in stress management, time management, conflict management, business management, and other appropriate programs to teach basic skill sets on stress reduction. On a deeper level the organization can provide more personalized support services through Physician Wellness Programs, Wellness Committees, Physician EAPs (Employee Assistance Programs), or through individualized coaching or counseling. Some physicians may require more in-depth behavioral modification programs. Organizations need to approach these programs with greater empathy and understanding of the physician’s world, show that they respect and value the physician’s time and what physicians do, and reinforce the point that they are here to help. They need to make an effort to promote individualized support and be responsive to physician resistance, time constraints, and fears of confidentiality. To motivate physician action, the focus needs to be on the goal of helping the physician do what they want to do, which is to practice good medical care.
One excellent case example is the approach taken by the Center for Professionalism and Peer Support at Brigham and Woman’s Hospital in Boston (Shapiro and Galowitz 2016). Recognizing the impact of physician burnout and the emotional stress it has on physicians and organizational culture, the hospital started its peer support program in 2008 in an effort to provide resources to support physician well-being and resilience. Through a multistep process that includes education, proactive outreach, peer training, peer support, and individualized coaching, the organization has led the way in developing programs that have now been replicated across the country. Many other examples from the Mayo Clinic, Stanford University, Case Western, and other hospital centers across the country provide a variety of different innovative approaches designed to reduce physician stress and burnout (Shulte 2015; Snowbeck 2016; Rovner 2016).
4 Consequences
Despite all the evidence and concern about physician behavioral turmoil, in many cases it goes unresolved. Depending on the circumstances, the combination of internal and external factors can result in inappropriate actions that lead to disruptive behaviors. Unfortunately, many disruptive events either go unrecognized, go unreported, or are ignored for a variety of different reasons (MacDonald 2014). The problem with this personal and organizational reluctance is the potential for bad things to happen to patients and staff (see Table 3.2).
One of the issues raised earlier was the importance of defining what disruptive behavior is and holding individuals accountable for their actions. Many individuals who act “disruptively” are not aware that they are acting in an inappropriate nonprofessional manner. This is particularly true for physicians who are used to taking control and “giving orders.” Under times of stress they may yell and intimidate others and not even realize they are doing it. Even if they are aware, they justify their behaviors as being necessary to direct patient care. The problem is that they are oblivious to the downstream negative consequences this may cause on care relationships, communication efficiency, task accountability, and patient care.
A second big concern is the issue of organizational tolerance. Many of the events involve very prominent physicians who bring a large number of patients and revenue into the organization. Many organizations are reluctant to address the issue in fear of antagonizing a physician to the point where they worry that the physician will not bring their patients into the facility. This is particularly true for smaller organizations where there may be a shortage in supply of certain specialties. There is also the concern about traditional hierarchy and crossing boundaries. Physicians work autonomously and in many organizational cultures physicians are viewed as “sacred saints” impeding the willingness to intervene. There is often a hidden “code of silence” where health care workers are reluctant to report disruptive behaviors (Boothman 2016). This lack of reporting is accentuated by potential conflicts of interest, concerns about lack of confidentiality, uncertainty about how to report problems, skepticism that the organization will respond, and/or fears of retaliation. Many who do report are frustrated by the lack of administrative support and the fact that despite reporting, the perception is that nothing ever changes, so why bother.
And lastly is the structure and skill set to deal with behavioral problems. Organizations have policies and procedures in place to address clinical competency but may not be well equipped to deal with behavioral problems. They need to have the right structure in place supported by individuals skilled in facilitation and negotiation techniques. Turning matters over to the Chief or Chairman of the Department may not lead to an effective resolution. At one end individuals need to be trained, empowered, and feel comfortable in speaking up when they are involved in a disruptive event. These skills can be reinforced through assertiveness training or through training in how to conduct crucial conversations as taught by Vital Smarts (Patterson et al. 2002). At the other end is to develop appropriate skill sets in dealing effectively with conflict resolution (Rosenstein et al. 2014). The importance of speaking up and resolving conflict in a professional respectful manner is a crucial step for maintaining workplace integrity and assuring optimal care efficiency.
5 The Risks of Inaction
The risk of inaction can lead to dangerous downstream consequences that affect morale, culture, workplace atmosphere, and reputation, and/or lead to medical mishaps that have significant direct or indirect patient safety and quality defects with associated financial penalties (Rosenstein 2011) (see Tables 3.2 and 3.3).
On one level disruptive behaviors have been shown to have a significant negative impact on nurse satisfaction and retention (Rosenstein 2002). Replacing a nurse can cost the organization anywhere from $60,000 to $100,000 for recruitment, training, and secondary opportunity costs (Moss et al. 2016). When it occurs in a public arena disruptive events can also lead to patient dissatisfaction which can negatively impact Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) scores and other patient satisfaction pay for performance initiatives which can have a negative effect on reimbursement. Then there is the spillover effect on hospital reputation which may negatively impact market share and contracting negotiations.
From a patient care perspective, the biggest concern is safety and the occurrence of preventable medical errors or adverse events (The Joint Commission 2008; Dang et al. 2016; Rosenstein 2013). In addition to waste, duplication, and inefficiencies in management, lack of communication and collaboration can lead to task failures that result in medication errors, infections, delays in treatment, and other serious medical conditions, which can increase lengths of stay and accrue significant non-reimbursable costs of care. To illustrate the point a little more dramatically, listed below are some of the comments made as part of our survey linking disruptive behaviors to the occurrence of adverse patient outcomes (The Joint Commission 2008; Rosenstein and O’Daniel 2006) (see Table 3.4).
The Joint Commission states that more than 50% of adverse sentinel events can be traced back to human factor issues and/or failures in communication (http://www.jointcommission.org/assets/1/18/Root_Causes_by_Event_Type_2004-2014.pdf). The relationship between human factor contributions and bad outcomes is a well-known cause of preventable medical errors (Rosenstein 2009a, 2016a). Communication problems are costly (Agarwal et al. 2010). In response to the concerns about the impact of disruptive behaviors on patient safety in 2010, The Joint Commission added a new leadership standard requiring hospitals to have a disruptive behavior policy in place and to supply support for its intent as part of the leadership accreditation standards (http://www.jointcommission.org/assets/1/6/Leadership_standard_behaviors.pdf). In order for hospitals to receive Medicare reimbursements, they need to pass the accreditation survey requirements (Spok Inc. 2013).
From a compliance perspective, noncompliant behaviors that adversely impact process flow, coding and documentation requirements, non-adherence to case management utilization protocols, and/or not following best practice guidelines, policies, and procedures can all have a significant negative economic and quality impact on reported patient care outcomes.
From a risk management perspective issues can arise from not only the occurrence of medical errors or adverse events, but also to poor compliance, poor communication and collaboration, impeded information transfer, neglect, failure to respond, and/or poor patient satisfaction. It is estimated that the average yearly cost for a midsize hospital due to communication deficiencies is $400,000 (Agarwal et al. 2010).
More egregious cases can lead to litigation. Time, preparation, and malpractice awards can result in significant dollar amounts with average malpractice settlements averaging above a half-million dollars (Hickson and Entman 2008; Crico Strategies 2015; Hickson et al. 2002; Beaulieu-Volk 2013; Lindro 2013). In California there is the additional penalty of hospital fines (ranging from $25,000 to $100,000) for the occurrence of significant adverse events (Seipel 2015).
6 Addressing Disruptive Behaviors
Recognizing the multidimensional cause, nature, and extent of disruptive behaviors, it is clear that there is no one solution to resolve the problem. The ultimate objective is to prevent disruptive behaviors from occurring. If they do occur, the organization and staff need to take immediate action to lessen the likelihood of any adverse event on staff or patient care. Depending on the nature and frequency of events, further interventions may be required to prevent repeated incidents. Table 3.5 provides a list of recommended strategies. In addition to its focus on reducing the incidence of disruptive behaviors, this approach can also improve overall organizational culture, staff relationships, team collaboration, communication efficiency, physician engagement, and physician well-being.
6.1 Training Redesign
One of the earliest steps is to improve the process and criteria for medical school selection. As discussed earlier, many medical schools are looking for more “well-rounded,” medical school applicants who majored in something other than pure science and mathematics (Schwartzstein 2015). The new MCAT (Medical College Admission Test) is now introducing more questions on humanities and social sciences (Schwartzstein et al. 2013). The goal is to look for individuals with more highly developed social and personal skills rather than only technical skill sets. Many medical schools in the USA, supported by large grants from the American Medical Association (AMA) and Robert Wood Johnson Foundation, are in the process of revising their curriculum to focus more on the importance of developing strong individual communication and team collaboration skills early in the education process (Frieden 2015; Vassar 2015).
6.2 Organizational Culture and Work Environment
From an organizational perspective, hiring and retaining the right people is key to success. Many organizations are recognizing the importance of the right “cultural fit” and are using more selective interviewing techniques to assure that new hires will work well with the mission and operational needs of the work environment (Byington 2013; Stark et al. 2014; White and Burroughs 2010). Once hired, there should be a comprehensive on-boarding process to first welcome the physician, explain organizational priorities and incentives working under the complexities of today’s health care environment, and then emphasize the support available to help physicians negotiate through the maze of medical requirements (Wagner 2014; Hobson 2016). Recognizing administrative concerns for financial viability, and clinical staff concerns about quality and safety, there needs to be discussions around the business side of medicine ending in a mutually agreed upon rallying point and alignment around best patient care.
Organizational culture sets the tone. Strong and supportive organizational cultures have been shown to significantly enhance staff morale, satisfaction, motivation, and engagement which leads to behaviors that result in the best patient care outcomes (Shanafelt et al. 2015b). Having a strong, committed, and respectful leadership, an effective structure and process in place covered by skilled individuals, a willingness to address and respond to individual concerns and barriers that pose a potential disturbance in the workforce, establishing priorities, and enlisting the help of key individuals who act as champions and catalysts to help promote a positive work environment are the key ingredients to a successful culture. In today’s multitasking and pressure-filled “here’s what you need to do world,” always remember to take a step back and take time to involve, thank, and recognize physicians and staff for their efforts and a job well done.
6.3 Education
Another crucial step is to make an effort to educate staff about healthcare reform, what we need to do in response, and how it might impact individual roles and responsibilities. Providing educational sessions on the evolving healthcare environment, value-based care, system redesign, performance-based accountabilities, and the business implications of clinical practice will help set realistic expectations by giving physicians a better understanding of current trends and how it might affect their individual practice.
6.4 Relationship Training
Providing training to enhance relationship management is crucial. Under an umbrella of increasing complexity and accountability, more segmentation between specialty and discipline-specific tasks and responsibilities, and a greater focus on care responsibilities that extend across the entire spectrum of care, it is crucial for all members of the health care team to work well together to achieve best patient care outcomes. In order to accomplish this, we need to gain a better understanding of the factors affecting individual values, perceptions, and behaviors.
As discussed above, disruptive behaviors derive from a number of different internal and external factors influencing one’s personality, mood, and demeanor. Providing specific training programs to address some of these specific factors are beneficial in gaining a better understanding of contributing circumstances and how individuals can deal more effectively with complicated issues. These programs might include training in diversity management, cultural competency, emotional intelligence, generational values, personality assessments, and patient satisfaction. Additional programs on conflict management, anger management, and stress management may also be of value.
6.5 Communication and Team Collaboration
Beyond addressing disruptive behaviors is the need to improve overall communication and team collaboration skills. Physicians are typically not the best communicators. There are many barriers that get in the way (Rosenstein 2012b). First, many physicians approach patient management through a one-way dictatorial process. They are trained to work autonomously, to take control, and give orders. Communication gaps are further accentuated by a bureaucratic health care hierarchy; a teaching focus on gaining knowledge and technical competency rather than personal skill development; segmented, siloed, and discipline-specific priorities which focus more on the organ or disease rather than overall patient needs; and an overriding strong ego that resists outside advice, interference, or involvement. In today’s complex healthcare world, improving communication skill sets should be a number one priority.
There are many different types of communication skills training programs available. At one level is the SBAR (Situation/Background/Assessment/Recommendation) script available to help nurses more effectively organize their thoughts in presenting patient information to the physician (De Meester et al. 2013). At a deeper level are the basic communication techniques taught by a number of different programs such as the AIDET, BAYER, and STARS programs. The focus is to get the physician more in synch with the values of two-way communication. Crucial points emphasized include a proper introduction and acknowledgement, making time and patience, exhibiting positive body language and verbal tone, enabling trust, avoiding distractions or conflict, reflective listening, being sensitive to the other’s values, needs, and desires, providing clarification and understanding, and setting appropriate expectations. In a demanding hectic environment, taking the time to listen, understand, respond, discuss, and explain are the keys to gaining cooperation and a successful interaction and outcome (Joshi 2015; Wen and Kosowsky 2012).
A further extension of communication is to teach team collaboration. One of the most effective programs in health care is the TeamSTEPPS program (2016; Helfner et al. 2016). Based on the crew resource management techniques used by the aviation and race car industries, the focus of the training program is to teach team members how to (a) anticipate and assist, (b) build trust, respect, and commitment, (c) understand one’s own role and the roles of others, (d) reinforce accountability and task responsibilities, (e) avoid/manage conflict or confusion, (f) be assertive and speak up, (g) have follow-up discussions, and (h) give thanks for a job well done. Assertiveness training is a crucial part of the process reinforcing the need to speak up when there is a question of patient safety. In addition to the TeamStepps program is the training offered through the VitalSmarts Crucial Conversations program (Patterson et al. 2002).
6.6 Behavioral Policies and Procedures
In order to hold individuals accountable for their behaviors, the organization needs to have a code of conduct policy in place that outlines unprofessional behaviors and the ramifications of non-compliance (Rosenstein and O’Daniel 2005; Shapiro et al. 2014). The policy must be backed by an effective incident reporting system where each complaint is evaluated on its individual merits with recommendations given for appropriate follow-up action. In order for the program be effective, individuals need to be willing to report. Barriers to reporting include fear of whistleblower retaliation, a double standard of reluctance to apply consistent reprimands when it involves physicians, and the sense that people report and report and nothing ever changes. On the incident evaluation side, determinations need to be made by trained individuals functioning without personal bias or conflicts of interest, with recommendations passed on to an individual or committee who has the appropriate facilitation skills to foster accountability and resolution. When patient quality or safety is of concern, many of these issues fall under a risk management protocol.
6.7 Intervention
When it comes to intervention, the first intervention is prevention. As discussed previously, taking a proactive approach in trying to get a better understanding of behavioral characteristics, and teaching basic principles about behavioral management can certainly reduce the predilection for behavioral problems. For recurring issues, early intervention has a much greater potential for success than waiting until a bad incident occurs where the interactions take on more of a remedial tone (Rosenstein 2009b).
Interventions can occur at several different levels. In all cases it is crucial to intervene at the appropriate time and place with the intervention conducted by someone skilled in the arts of facilitation and conflict management.
The first intervention is real time. If somebody is acting inappropriately, the recipient needs to be assertive in addressing their concerns in a respectful professional manner. Assertiveness and Crucial Conversations training can help reinforce these capabilities. In some organizations they will call a “code white” or a “code lavender” where a group of trained individuals are paged to the scene in an effort to provide emotional support to diffuse a difficult situation (Advisory Board 2013).
The next series of interventions are post-event interactions. Hickson and his group at Vanderbilt University have come up with a four-phase process for intervention that includes informal, awareness, authority, and disciplinary actions (Hickson et al. 2007). The informal interaction is often described as the “cup of coffee” approach where you take the physician aside, describe the series of events, and ask for their opinion. The usual response is that they were not aware of any problem and question how someone could think that they were acting in a disruptive manner. The next thought is justifying their need to take control during a period of uncertainty or crisis. Following that is rationalization and/or blaming someone or something else for their behavior without taking any responsibility for their own actions. A good facilitator will listen to what the physician has to say, ask if they thought that their action was appropriate and address their concerns; but then bring the focus back to their behaviors, reframe the issue to bring it into context, ask them to think about the impact it had on the other person(s) involved, and what they could have done differently to ease the angst of the situation. When the situation is addressed under the guise of raised awareness and care improvement, most physicians will self-correct.
For repeated offenders, or when the incident is of a serious nature, there needs to be a more formal intervention. The physician needs to recognize the ramifications of non-compliance with the code of behavioral standards and the organization needs to reinforce the importance of a zero tolerance policy with the potential of disciplinary action. In some cases, the recommendations may be made for anger management, stress management, conflict management, or diversity training, and in more serious cases the need for individualized counseling and/or coaching. Always keep in mind the underlying possibility of a psychiatric illness or a substance use disorder that may contribute to disruptive behaviors and require a psychiatric evaluation. Depending on the nature of the problem, some physicians may be required to attend an outside behavioral therapy program offered through state-sponsored physician health programs (PHPs) (see Chap. 12), university-sponsored programs and workshops or private outside resources (Vanderbilt University Medical Center 2017; UC San Diego PACE Program 2016; Boyd 2016).
In the more extreme cases where physicians are resistant to follow recommended actions, the only recourse may be sanctions or termination of privileges. Having served as an expert witness on both sides of the picture (representing hospitals, representing individual physicians) termination cases stir up a lot of legal entanglement and organizational aggravation. Most physicians will fight and appeal termination decisions based on failure of the hospital to follow due process, breach of contract, anti-trust issues, bad faith, malice or discrimination, defamation of character, or undue harassment and retaliation. In their defense hospitals need to have a clear line of documentation as to the issues, follow due process, adhere to the bylaws and Health Care Quality Improvement Act (HCQIA) requirements, be consistent with similar types of cases, document follow-up discussions, comply with the rights of the physician to be heard, provide specific recommendations designed to resolve problems, and state the ability to reapply once the issues are addressed and resolved. Hospitals win more than 80% of the appeals (Rosenstein et al. 2016).
6.8 Physician Support
When possible the focus of any intervention should be on trying to help the physician better adjust to the situation by offering assistance and career guidance rather than punishment. The primary focus should be on positive physician support.As mentioned previously, physicians are overwhelmed by administrative requirements and time constraints and are being asked to take on more and more responsibilities that take them away from direct patient care. There are several ways in which the organization can help. From an administrative and logistical perspective, having the organization be more sensitive to on-call schedules, workflow dynamics, productivity requirements, and meeting or committee attendance will help reduce some of the administrative load. Offering administrative assistance by providing more help with documentation and compliance with electronic medical records through additional training, staff support staff, or “scribes” will help ease physician frustrations in this area (Schultz and Holmstrom 2015).
From a clinical perspective, using physician assistants, nurse practitioners, or case coordinators to help cover some basic medical necessities will free the physician to concentrate on more complex patient management issues.
From a behavioral perspective, providing services to help the physician better adjust to the pressures of medical practice, organizations can offer services through wellness committees, employee assistance programs, individualized coaching and counseling sessions, or other services offered though Human Resources, Medical Staff Services, or outside referral services.
6.9 Physician Well-Being
As mentioned previously, stress and burnout are a major problem affecting physician satisfaction and overall well-being (Rosenstein 2015c; Ariely and Lanier 2015). Both organizational support and individual resilience and wellness strategies are important. Unfortunately, motivation for change can be challenging and there is often a significant gap between intentions and action (Saddawi-Konefka et al. 2016). Achieving a proper balance between intrinsic and extrinsic motivators can be helpful in this regard (Judson et al. 2015).
Motivation for physician well-being needs to be linked with the physician’s primary goal and aspirations to provide best practice care. They need to recognize, understand, and accept the fact that emotional and physical well-being affects their levels of energy and the joy of being a physician. Many recent studies have documented that emotional and physical wellness is a strong contributor to physician satisfaction, improved care relationships, and improved patient outcomes of care (West et al. 2014; Friedberg 2016). This all starts by understanding the importance of good health and the negative consequences of ill-health on performance that impacts family, friends, colleagues, staff, and ultimately patients. Physicians understand the importance of relaxation and recreation, adequate sleep, regular exercise, and good nutrition but have difficulty integrating such self-care activities into their own lives. Avoiding stressful situations, setting limits, learning to comfortably say no, and willingness to accept outside advice are necessary components of well-being. Most importantly, teaching techniques to support self-awareness, reflection, and self-preservation as well as taking time off for relaxation and energy restoration help to achieve inner peace. Most physicians recognize that these activities are important, but they become a secondary priority to the daily grind. Currently, professional culture supports self-sacrifice in the interest of patients and organizational culture focuses on productivity and reimbursement. To aggressively promote and support the importance of physician well-being will require commitment at the individual, professional, and organizational levels (Rosenstein 2015d, 2016b).
There are now a growing number of different initiatives being introduced to support this point. From a health care policy perspective, the Institute of Healthcare Improvement (IHI), the AMA, and other health care societies are promoting the extension of the Triple Aim (enhancing the patient experience, improving population health, reducing costs) to the Quadruple Aim, adding to these goals the importance of improving the work life of health care providers (Bodenheimer and Sinsky 2014; Wallace and Lemaire 2009). Many organizations are introducing the concepts of mindfulness and meditation training programs for physicians as a way to promote self-refection, purpose, and fulfillment (Krasner et al. 2009; Beach et al. 2013). Mindfulness activities help to reinforce purpose and meaning by focusing on the benefits of the current activity or task. It incorporates many of the ideals of meditation and relaxation techniques with the goal of providing a more productive and fulfilling interaction. Many organizations have successfully used these techniques to improve overall physician satisfaction, well-being, and engagement (Beckman et al. 2012). The term resilience is used to describe the capacity to “bounce back” and respond to stressful situations in a successful manner (Epstein and Krasner 2013; Beckman 2015). Positive organizational and social support, mindfulness, relaxation, self-care, and setting limits can all help to facilitate resilience.
6.10 Physician Engagement
The final phase is to enhance physician engagement. The key steps include establishing an underlying culture of positive support for physician livelihood, giving physicians an opportunity for input and discussion, and responding to their needs and concerns (Rosenstein 2015e, 2015f, 2015g; Whitlock and Stark 2014; Lister et al. 2015; Henson 2016).
Physicians are a precious resource. All they really want to do is to practice good medical care. But growing frustrations arise from outside intrusions and other forces unidirectionally telling them what they need to do. Morale is at an all-time low (The Physicians Foundation 2016). Part of their frustration is the lack of physician input. Physicians want to have a voice particularly when it involves issues affecting patient care. Input can be gathered from several different sources. These include surveys, discussions at Town Hall or Department meetings, specialized task forces, or better yet, one-on-one conversations with administrative and clinical leaders. Allowing input diffuses some of the frustrations particularly if there are expressions of empathy and understanding of the physician world. Input must be followed by responsiveness. This may include administrative, logistical, clinical, or behavioral support. Not every problem can be solved, but at least leaders can provide an explanation and coordinate next steps on achieving mutually aligned objectives. There is a strong correlation between physician engagement, physician alignment, physician well-being, physician satisfaction, physician motivation, improved relationships, and improved outcomes of care. At the end, always remember to visibly show respect and thank physicians for what they do. Physicians are a precious resource and excellent healthcare cannot do what it does without them.
7 Conclusion
Increasing complexities in today’s healthcare environment have introduced a number of different factors distracting physicians from their primary goal to provide the best possible care. At times the resulting levels of frustration, dissatisfaction, stress, and burnout can affect their attitudes and behaviors to a point where they become disruptive and their actions can negatively impact relationships that adversely affect patient care outcomes. With this in mind, we need to do what we can to help physicians better adjust to the pressures of medical practice. To do this, we must first get a better understanding of the contributing factors that impact their world, give them an opportunity to discuss their concerns, and then provide proactive support to help them thrive. This will require a multistep process that includes raising levels of awareness and accountability; education; advanced training to enhance work relationships, improve communication, conflict, and stress management skills; and providing the necessary logistical, clinical, and behavioral support to help them deal with the day-to-day operations and distractions. In some cases more in-depth support needs to be provided to help reduce the effects of stress and burnout. More difficult cases may require more comprehensive individualized coaching or counseling. Many of these services can be provided through a physician wellness committee, a physician EAP, or other internal or outsourced professional resources. At the same time we need to support physician health and well-being by limiting their stress and providing appropriate relaxation, mindfulness, and coping skills to enhance their resilience and endurance. When more serious behavioral problems occur, the organization needs to take the necessary steps to address the issue head-on before it can compromise care. Organizations need to have the right policies and procedures in place, provide the necessary intervention protocols to hold the physician accountable for their actions, and implement the appropriate recommendations for improvement. To better motivate and engage physicians, we need to listen to their concerns, address the barriers, overcome resistance, and emphasize the value of change by buffering their reluctance from “what’s in it for me.” We need to provide a supportive culture that makes an effort to better understand their world and motivate engagement by giving them an opportunity for input and discussion and reminding them of the pride and joy of who they are and what they do. In the end always treat them with respect and thank them for a job well done. Recognize that most physicians will not act on their own. We all need to take a proactive role in trying to help them better adjust to the pressures of today’s medical world.
References
Advisory Board. When Cleveland clinic staff are troubled they file code lavender advisory board. 2013. https://www.advisory.com/daily-briefing/2013/12/03/when-cleveland-clinic-staff-are-troubled-they-file-code-lavender
Agarwal R, Sands DZ, Schneider JD, Smaltz Detlev H. Quantifying the economic impact of communication inefficiencies in US hospitals. J Healthc Manag. 2010;55(4):265.
Ariely D, Lanier W. Disturbing trends in physician burnout and satisfaction with work-life balance: dealing with the malady among Nation’s leaders. Mayo Clin Proc. 2015;90(12):1593–6.
Beach M, Price E, Gary T, Robinson K, et al. Cultural competency: a systematic review of health care provider educational interventions. Med Care. 2005;43(4):356–73.
Beach M, Roter D, Korthuis P, Epstein R, et al. A multicenter study of physician mindfulness and health care quality. Ann Fam Med. 2013;11(5):421–8.
Beaulieu-Volk D. Poor communication ups risk of malpractice suits, patient non-adherence. FierceHealthcare; 2013. http://www.fiercehealthcare.com/practices/poor-communication-ups-risk-malpractice-suits-patient-nonadherence
Beckman R. The role of medical culture in the journey to resilience. Acad Med. 2015;90(6):710–2.
Beckman H, Wendland M, Mooney C, Krasner M, et al. The impact of a program in mindful communication on primary care physicians. Acad Med. 2012;87(6):1–5.
Bodenheimer T, Sinsky C. From triple to quadruple aim: care of the patient requires care of the provider. Ann Fam Med. 2014;12(6):573–6.
Boothman R. Breaking through dangerous silence to tap an organization’s richest source of information: its own staff. Jt Comm J Qual Patient Saf. 2016;42(4):147–8.
Borges NJ, Manuel RS, Elam CL, Jones BJ. Differences in motives between Millennial and Generation X medical students. Med Educ. 2010;44(6):570–6.
Boyd J. State physician health programs: what you need to know. Quantia MD; 2016. https://quantiamd.com/player/ycnipdwzy?cid=1818
Brock D, Abu-Rish E, Chiu C, Hammer D, et al. Interprofessional education in team communication: working together to improve patient safety. Post Grad Med J. 2013;89(1057):642–51.
Byington M. Hiring for cultural fit at your medical practice. Physicians Practice; 2013. http://www.physicianspractice.com/blog/hiring-cultural-fit-your-medical-practice
Crico Strategies. Malpractice risks in communication failures: 2015 annual benchmark report. Crico Strategies Risk Management Foundation of the Harvard Medical Institutions, Boston, MA; 2015.
Curtis E, Dreachslin J, Sinioris M. Diversity and cultural competence training in health care organizations: hallmarks of success. Health Care Manag. 2007;26(3):255–62.
Dang D, Sung-Heui B, Karlowicz K, Kim M. Do clinician disruptive behaviors make an unsafe environment for patients? J Nurs Care Qual. 2016;31(2):115–24.
Danielson D, Ketterling R, Rosenstein A. M.D physician stress and burnout: causes, effects, and impact on performance and behavior. AMGA Group Pract J. 2013;62(3):38–41.
De Meester K, Verspuy M, Monsieurs K, Van Bogaert P. SBAR improves nurse–physician communication and reduces unexpected death: a pre and post intervention study. Resuscitation. 2013;84(9):1192–6.
Dyrbye AL, Massie F, Eacker A, Harper W, et al. Relationship between burnout and professional conduct and attitudes among U.S. medical students. JAMA. 2010;304(11):1173–80.
Rappleye E. Why Vanderbilt’s medical school is dropping science requirement. Beckers Hospital Review; 2015. http://www.beckershospitalreview.com/hospital-physician-relationships/why-vanderbilt-s-medical-school-is-dropping-science-requirements.html
Epstein R, Krasner M. Physician resilience: what it means, why it matters, and how to promote it. Acad Med. 2013;88(3):301–3.
Executive Dialogue. Executive dialogue: the multigenerational workforce: management implications and best practices. Hospitals and Health Networks; 2013. http://www.hhnmag.com/articles/5899-executive-dialogue-the-multigenerational-workforce
Friedberg M. Relationships between physician professional satisfaction and patient safety. PSNet; 2016. https://psnet.ahrq.gov/perspectives/perspective/193
Frieden R. AMA increases investment in medical education reform. MedpageToday; 2015. http://www.medpagetoday.com/publichealthpolicy/medicaleducation/52852
Gold KJ, Andrew LB, Goldman EB, Schwenk TL. “I would never want to have a mental health diagnosis on my record”: a survey of female physicians on mental health diagnosis, treatment, and reporting. Gen Hosp Psychiatry. 2016;43:51–7.
Goleman D. Emotional intelligence. New York: Bantam Books; 1995.
Gray J. Men are from Mars women are from Venus. New York: Harper Collins Publishers; 2004.
Helfner J, Hilligoss B, Knupp A, Bournique J, et al. Cultural transformation after implementation of crew resource management: is it really possible? Am J Med Qual. 2016;15:1–10. http://ajm.sagepub.com/content/early/2016/07/11/1062860616655424.full.pdf+html
Henson J. Reducing physician burnout through engagement. J Healthc Manag. 2016;61(1):86–9.
Hickson GB, Entman SS. Physician practice behavior and litigation risk: evidence and opportunity. Clin Obstet Gynecol. 2008;51(4):688–99.
Hickson G, Federspiel G, Pichert J, Miller C, et al. Patient complaints and malpractice risks. JAMA. 2002;287(22):2951–7.
Hickson G, Pichert J, Webb L, Gabbe S. A complementary approach to promoting professionalism: identifying, measuring, and addressing unprofessional behaviors. Acad Med. 2007;82(11):1040–8.
Hobson S. Best practices for effective physician on-boarding CHC Community. Hospital Blog; 2016. http://www.communityhospitalcorp.com/community-hospital-blog/~best-practices-for-effective-physician-on-boarding
Holm A, Gorosh M, Brady M, White-Perkins D. Recognizing privilege and bias: an interactive exercise to expand health care providers’ personal awareness. Acad Med. 2017;92:360–4. http://journals.lww.com/academicmedicine/Abstract/publishahead/Recognizing_Privilege_and_Bias___An_Interactive.98457.aspx
MacDonald I. Why hospitals turn a blind eye to misbehaving physicians. FierceHealthcare; 2014. http://www.fiercehealthcare.com/healthcare/why-hospitals-turn-a-blind-eye-to-misbehaving-docs
Jagsi R, Griffin K, Jones R, Perumalswami C, et al. Sexual harassment and discrimination experiences of an academic facility. JAMA. 2015;6:555–6.
Joshi N. Doctor, shut up and listen. New York Times; 2015. http://www.nytimes.com/2015/01/05/opinion/doctor-shut-up-and-listen.html?_r=0
Judson TJ, Volpp KG, Detsky AS. Harnessing the right combination of extrinsic and intrinsic motivation to change physician behavior. JAMA. 2015;314:2233–4.
O’Reilly K. Stressed physicians reluctant to seek support. amednews.com; 2012. http:www.amednews.com/apps/pbcs.dll/personalia?ID=koreilly
Karim S, Duchcherer M. Intimidation and harassment in residency: a review of the literature and results of the 2012 Canadian Association of Interns and Residents National Survey. Canad Med Educ J. 2014;5(1):e50.
Kay M, Mitchell G, Clavarino A, Doust J. Doctors as patients: a systematic review of doctors’ health access and the barriers they experience. Br J Gen Pract. 2008;58(552):501–8.
Krasner M, Epstein R, Beckman H, Suchman A, et al. Association of an educational program in mindful communication with burnout, empathy, and attitudes among primary care physicians. JAMA. 2009;302(12):1284–93.
Lemaire JB, Wallace JE, Jovanovic A. Stress and coping: generational and gender similarities and differences. In: Figley C, Huggard P, Rees C, editors. First do no self-harm: understanding and promoting physician stress resilience. New York, NY: Oxford University Press; 2013. p. 216–46.
Lister E, Ledbetter T, Warren A. The engaged physician. Mayo Clin Proc. 2015;90(4):425–7.
Lutfiyya MN, Brandt BF, Cerra F. Reflections from the intersection of health professions education and clinical practice: the state of the science of interprofessional education and collaborative practice. Acad Med. 2016;91(6):766–71.
Mata D, Ramos M, Bansai N, Khan R, et al. Prevalence of depression and depressive symptoms among medical residents: a systematic review and meta-analysis. JAMA. 2015;314(22):2373–83.
McCracken J, Hicks R. Personality traits of a disruptive physician. Physician Exec. 2012;38(5):66–8.
Moss M, Good V, Gozal D, Kleinpell R, et al. An official critical care societies collaborative statement-burnout syndrome in critical care health-care professions: a call for action. Chest. 2016;150(1):17–26.
Muller D. Reforming pre-medical education: out with the old, in with the new. N Engl J Med. 2013;368(17):1567–9.
Patterson K, Grenny J, McMillan R, Switzer AI. Crucial conversations: tools for talking when the stakes are high. New York: McGraw-Hill; 2002.
Privitera M, Rosenstein A, Plessow F, LoCastro T. Physician burnout and occupational stress: an inconvenient truth with unintended consequences. J Hosp Adm. 2014;4(1):27–35.
Rappleye E. 3 in 4 Physicians say their organization is not addressing burnout. Becker Hospital Review; 2016. http://www.beckershospitalreview.com/hospital-physician-relationships/3-in-4-physicians-say-their-organization-is-not-addressing-burnout.html
Ratwani RM, Fairbanks RJ, Hettinger AZ, Benda NC. Electronic health record usability: analysis of the user-centered design processes of eleven electronic health record vendors. J Am Med Inform Assoc. 2015;22(6):1179–82.
Reeves S, Palaganas J, Zierler B. Measuring the impact of interprofessional education on collaborative practice and patient outcomes. Washington, DC: The National Academies Press; 2015.
Roberts DH, Newman LR, Schwartzstein RM. Twelve tips for facilitating Millennials’ learning. Med Teach. 2012;34:274–8.
Rosenstein A. The impact of nurse-physician relationships on nurse satisfaction and retention. Am J Nurs. 2002;102(6):26–34.
Rosenstein A. Physician and nurse behaviors and their impact on communication efficiency and patient care. J Commun Healthc. 2009a;2(4):328–40.
Rosenstein A. Early intervention can help prevent disruptive behavior. Am Coll Physician Exec J. 2009b;37(6):14–5.
Rosenstein A. The economic impact of disruptive behaviors: the risks of non-effective intervention. Am J Med Qual. 2011;26(5):372–9.
Rosenstein A. Physician stress and burnout: what can we do? Physician Exec J. 2012a;38(6):22–30.
Rosenstein A. Physician communication and care management: the good, the bad, and the ugly. Physician Exec J. 2012b;38(4):34–7.
Rosenstein A. Bad medicine: managing the risks of disruptive behaviors in health care settings. Risk Manag. 2013;60(10):38–42.
Rosenstein A. Physician disruptive behaviors: five year progress report. World J Clin Cases. 2015a;3(11):930–4.
Rosenstein A. Taking a new approach to reduce the incidence of physician disruptive behaviors. Hosp Pract. 2015b;43(4):221–5.
Rosenstein A. A multistep approach to improving well –being and purpose. Patient Saf Qual Healthcare. 2015c;12(4):14–7.
Rosenstein A. Meeting the physician’s needs: the road to organizational-physician engagement. Trustee; 2015d. p. 19–22. http://www.trusteemag.com/articles/887-meeting-the-physicians-needs-the-road-to-organization-physician-engagement
Rosenstein A. Strategies to enhance physician engagement. J Med Pract Manag. 2015e;31(2):113–6.
Rosenstein, A. True physician engagement. Hosp Health Netw Vol.85 No.3 March 2015f p.14
Rosenstein A. Human factors affecting disruptive physician behaviors and its impact on the business of medicine. J Bus Hum Resour Dev. 2016a;2(2):1–10.
Rosenstein A. Understanding the psychology behind physician attitudes, behaviors, and engagement as the pathway to physician well-being. J Psychol Clin Psychiatry. 2016b;5(6):1–4.
Rosenstein A, O’Daniel M. Addressing disruptive nurse-physician behaviors: developing programs and policies to improve relationships that improve outcomes of care. Harv Health Policy Rev. 2005;7(1):86–97.
Rosenstein A, O’Daniel M. Impact and implications of disruptive behavior in the peri-operative arena. JACS. 2006;203(1):96–105.
Rosenstein A, O’Daniel M. A survey of the impact of disruptive behaviors and communication defects on patient safety. Jt Comm J Qual Patient Saf. 2008;34(8):464–71.
Rosenstein A, Privitera M. Recognizing and addressing physician stress and burnout to improve physician satisfaction. AHA Physician Leadership Forum; 2015c. https://ahaphysicianforum.wordpress.com/2015/03/
Rosenstein A, Stark D. Emotional intelligence: a critical tool to understand and improve behaviors that impact patient care. J Psychol Clin Psychiatry. 2015;2(1):1–4.
Rosenstein A, Dinkin S, Munro J. Conflict resolution: unlocking the key to success. Nurs Manag. 2014;45(10):34–9.
Rosenstein A, Karwaki T, Smith K. Legal process and outcome success in addressing disruptive behaviors: getting it right. Physician Leaders J. 2016;3(3):46–51.
Rovner J. Teaching medical teamwork right from the start. Kaiser Health News; 2016. http://khn.org/news/teaching-medical-teamwork-right-from-the-start/
Saddawi-Konefka D, Schumacher D, Baker K, Charnin J, Gollwitzer P. Changing physician behavior with implementation intentions: closing the gap between intentions and actions. Acad Med. 2016;91:211–6.https://www.researchgate.net/publication/299395724_Changing_Physician_Behavior_With_Implementation_Intentions_Closing_the_Gap_Between_Intentions_and_Actions
Salles A, Liebert C, Greco R. Promoting balance in the lives of resident physicians: a call to action. JAMA. 2015;150(7):607–8.
Schultz C, Holmstrom H. The use of medical scribes in health care settings: a systematic review and future directions. J Am Board of Fam Med. 2015;28(3):371–81.
Schwartzstein R. Getting the right medical students: nature versus nurture. N Engl J Med. 2015;372(17):1586–7.
Schwartzstein R, Rosenfeld G, Hilborn R, Oyewole S, et al. Redesigning the MCAT Exam: balancing multiple perspectives. Acad Med. 2013;88(5):560–7.
Schwenk TL, Davis L, Wimsatt LA. Depression, stigma, and suicidal ideation in medical students. JAMA. 2010;304(11):1181–90.
Seipel T. 212 California hospitals fined by state health officials. The Mercury News; 2015. http://www.mercurynews.com/health/ci_28174132/12-california-hospitals-fined-by-state-health-officials
Shanafelt T, Hasan O, Lotte N, Drybye N, et al. Changes in burnout and satisfaction with work-life balance and the general US working population between 2011–2014. Mayo Clin Proc. 2015a;90(12):1600–13.
Shanafelt T, Gorringe G, Menaker R, Storz K, et al. Impact of organizational leadership on physician burnout and satisfaction. Mayo Clin Proc. 2015b;90(4):432–40.
Shanafelt T, Dyrbye L, Sinsky C, Hasan O, et al. Relationship between clerical burden and characteristics of the electronic environment with physician burnout and professional satisfaction. Mayo Clin Proc. 2016;91(7):836–48.
Shapiro J, Galowitz P. Peer support for clinicians: a programmatic approach. Acad Med. 2016;91(9):1–5.
Shapiro J, Whittmore A, Tsen L. Instituting a culture of professionalism: the establishment of a center for professionalism and peer support. Jt Comm J Qual Patient Saf. 2014;40(4):168–78.
Shulte B. Time in the bank: a Stanford plan to save doctors from burnout. The Washington Post; 2015. https://www.washingtonpost.com/news/inspired-life/wp/2015/08/20/the-innovative-stanford-program-thats-saving-emergency-room-doctors-from-burnout/
Smith LG. Medical professionalism and the generation gap. Am J Med. 2005;118:439–42.
Spok Inc. Getting right with the Joint Commission: The Hospital Communication Bill of Rights. White paper. Spok Inc; 2013. http://cloud.amcomsoftware.com/WP-AMER-Joint-Commission.pdf.
Stark R, Whitlock D, Cornett D. Addressing satisfaction gaps around cultural fit. Physician Exec J. 2014;40:22–6.
TeamSTEPPS®. TeamSTEPPS®: strategies and tools to enhance performance and patient safety. Agency for Healthcare Research and Quality, Rockville, MD; 2016. http://www.ahrq.gov/professionals/education/curriculum-tools/teamstepps/index.html
Lindro L. The Talking cure for health care: improving the ways doctors communicate with their patients can lead to better care—and lower costs. The Wall Street Journal; 2013. http://www.wsj.com/articles/SB10001424127887323628804578346223960774296
The Joint Commission. Joint Commission Sentinel Event 40. 2008. dhttp://www.jointcommission.org/assets/1/18/SEA_40.PDF
The Physicians Foundation. Survey of American Physicians. 2016. http://www.physiciansfoundation.org/uploads/default/Biennial_Physician_Survey_2016.pdf
Thew J., Millennials, boomers, gen Xers - can they all get along? HealthLeaders Media; 2015. http://www.healthleadersmedia.com/nurse-leaders/millennials-boomers-gen-xerscan-they-all-get-along
UC San Diego PACE Program. UC San Diego Physician Assessment and Clinical Evaluation (PACE) Program. 2016. http://www.paceprogram.ucsd.edu/Documents/PACE_Program_Detail_Printable.pdf
Vanderbilt University Medical Center. Vanderbilt University Disruptive Behavior and Professional Health Center. 2017. https://www.mc.vanderbilt.edu/root/vumc.php?site=cph&doc=22631
Vassar L. 21 More schools tapped to transform physician training. AMA Wire; 2015. http://www.ama-assn.org/ama/ama-wire/post/20-schools-tapped-transform-physician-training
VITAL WorkLife. Physician Stress and Burnout Survey Cejka Search and VITAL WorkLife; 2014. www.VITALWorkLife.com/survey/Stress
Wagner R. 7 keys to successful doctor on-boarding. Health Care Finance; 2014. http://www.healthcarefinancenews.com/news/7-keys-successful-doctor-onboarding
Wallace J, Lemaire W. Physician wellness: a missing quality indicator. Lancet. 2009;374(9702):1714–21. http://www.thelancet.com/pdfs/journals/lancet/PIIS0140673609614240.pdf
Wen J, Kosowsky J. When doctors don’t listen. New York: Thomas Dunne Books St. Martin’s Press; 2012.
West C, Dyrbye L, Rabatin J, Call T, et al. Intervention to promote physician well-being, job satisfaction, and professionalism: a randomized clinical trial. JAMA Int Med. 2014;174(4):527–33.
West CP, Dyrbye LN, Erwin PJ, Shanafelt TD. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet. 2016;388:10057.
White RD, Burroughs JH. Credentialing: stopping disruptive behavior at the door (chapter 2). In: A practical guide to managing disruptive and impaired physicians. Danvers, MA: HC Pro; 2010. p. 29–41.
Whitlock DJ, Stark R. Understanding physician engagement--and how to increase it. Physician Leaders J. 2014;1(1):8–13.
Williams D, Wyatt R. Racial bias in health care and health: challenges and opportunities. JAMA. 2016;315(19):2120–1.
Snowbeck C. Minnesota hospitals ramp up efforts to battle physician burnout. Star Tribune; 2016. http://www.startribune.com/minnesota-hospitals-ramp-up-efforts-to-battle-physician-burnout/389385481
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Rosenstein, A. (2017). Disruptive and Unprofessional Behaviors. In: Brower, K., Riba, M. (eds) Physician Mental Health and Well-Being. Integrating Psychiatry and Primary Care. Springer, Cham. https://doi.org/10.1007/978-3-319-55583-6_3
Download citation
DOI: https://doi.org/10.1007/978-3-319-55583-6_3
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-55582-9
Online ISBN: 978-3-319-55583-6
eBook Packages: MedicineMedicine (R0)