Abstract
Focused ultrasound (FUS) is a noninvasive thermal therapy that utilizes energy generated from ultrasound waves to ablate a small target area. The ability of FUS to heat tumors to ablative temperatures in a very precise manner, thereby sparing surrounding tissues, has been equated to surgery with the advantages of reduced tissue trauma and recovery time. FUS may also be used to induce moderate temperature hyperthermia to enhance effects of radiation, chemotherapy, and potentially immunotherapy. The combination of magnetic resonance guidance with FUS (MRgFUS) provides the ability to plan, monitor, and steer treatments in near real-time, further contributing to the safety and effectiveness profile of FUS. Regulatory clearance for noninvasive palliative treatment of bone metastases has been realized. Additional palliative and curative treatments for a wide range of oncologic conditions including prostate, breast, gynecologic, gastrointestinal and brain cancers, and soft tissue tumors are in active development. This chapter provides an overview of MRgFUS including biological effects and physical parameters description. A comprehensive review of all currently approved and evolving oncological applications of MRgFUS then follows. Finally, an overview is provided of wide ranging leading edge research helping to define future applications for the field including the role of MRgFUS in multimodality cancer therapy.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Focused ultrasound
- MR guidance
- Thermal ablation
- Bone metastases
- Prostate cancer
- Breast cancer
- Soft tissue sarcoma
- Brain cancer
- Liver cancer
- Pancreatic cancer
- Colorectal cancer
1 Introduction
Thermal medicine is an emerging field that is based upon therapeutic manipulation of temperature. Thermal therapy may be performed with very cold temperatures—cryotherapy (<−40 °C), or with one of three distinct protocols of elevated temperature: fever-range hyperthermia around 39–41 °C lasting several hours; moderate hyperthermia around 41–45 °C for 30–60 min; and high-temperature thermal ablation, usually 50–85 °C with heat typically applied to each area of the target for several seconds (Stauffer 2005). The biologic effects expected from these different temperature ranges vary widely. At fever-range temperatures, blood perfusion, permeability of tumor microvasculature, and cellular metabolic rate are increased, potentially enhancing drug uptake and local activity as well as stimulation of immune response (Xu et al. 2007; Dewhirst et al. 2012). At moderately higher temperatures of 41–45 °C, the primary goal is to enhance other forms of therapy such as radiation or chemotherapy through a number of overlapping effects on cells, vasculature and tumor physiology. Since higher perfusion improves tissue oxygenation and pH, this increases sensitivity to radiation (Vujaskovic et al. 2000), while the elevated temperature inhibits repair of sub-lethal radiation damage. The radiobiology of heat combinations with radiation are described in detail in numerous publications (Dewhirst et al. 2012, 2005; Sneed et al. 2010; Hall and Giaccia 2006). Combined with chemotherapy, moderate hyperthermia increases cellular metabolism and nutrient consumption, thus enhancing cellular uptake of locally concentrated drug (Dahl 1995; Hahn 1979). In addition to enhancing the local toxicity of systemically administered chemotherapeutics, local hyperthermia has been shown to increase the extravasation of drug out of leaky tumor microvasculature and thereby increase local concentration of bioavailable drug around tumor cells (Dewhirst et al. 2012). This effect may be magnified using nanoparticle drug carriers such as temperature sensitive liposomes that release drug rapidly within the transit time through a heated tumor, potentially increasing total drug delivery by 20–30 fold (Kong et al. 2000). For temperatures above 48 °C, the effects on tissue are more direct, with protein denaturation, coagulation and tissue necrosis following immediately after the heat insult. Besides thermal ablation, mechanical effects such as cavitation and radiation forces may also induce damage (Hectors et al. 2016).
Thermal Oncology concerns the treatment of cancer with heat or cold. Optimum selection of one of the thermal treatment protocols defined above depends on location and extent of the tumor target. For large or irregularly shaped tumors extending out into surrounding host tissues, it may be most appropriate to apply moderate hyperthermia to a large region that encompasses all imageable tumor including a margin, and rely on synergism of heat with radiation and/or chemotherapy to accomplish differential tumor kill over a course of fractionated treatments. For a well-circumscribed lesion in a region of non-critical tissue with some biological reserve (i.e. liver, muscle, fat), an aggressive heating approach may be more appropriate that can ablate the entire tumor target with only a thin rim of surrounding margin. In such cases, focal ablation can accomplish effective thermal surgery in a single treatment session. For this strategy, a high degree of control of power deposition is required to produce ablative temperatures within the target while avoiding overheating of surrounding critical normal tissues.
Numerous reviews clearly describe the capabilities and limitations of available electromagnetic and ultrasonic heating technologies (Stauffer 2005; Diederich and Hynynen 1999; Hynynen 1990; Hynynen and McDannold 2004; Lee 1995; Van Rhoon 2013). Generally, the long wavelength associated with radiofrequency and microwave heating devices prohibits a tight focus in tissue in lieu of a regional concentration of heat. On the contrary, typical clinical ultrasound systems have large multi-transducer arrays on the surface and are able to produce a 1–2 mm diameter by 3–7 mm long focal region at depth in the body. Each focused ultrasound exposure is known as sonication. The high intensity focus quickly ablates tissue (<10–20 s) so that the focal point can be shifted and the process iterated to produce overlapping ablation zones that eventually combine into one large ablated tissue volume (Fig. 1). Because heating only occurs where the ultrasound waves converge, the surrounding tissue remains unaffected. This procedure is known as high-intensity focused ultrasound (HIFU) ablation or simply focused ultrasound (FUS) ablation.
The ability to target tissues deep within the human body depends on the frequency and intensity of the ultrasound wave and the tissue properties through which the wave must travel. Lower frequency acoustic waves are better suited to penetrate deep into tissue, but may require more energy to cause thermal tissue ablation; while higher frequency waves cause heating more easily, but tend to get absorbed more readily and therefore cannot penetrate into deep tissues. Such parameters can be manipulated during FUS treatment to maximize energy delivery to the targeted tissue. Another consideration for planning FUS treatment is the scattering of ultrasound waves when travelling through different mediums. Most human tissues, with the exception of bone and fat, have the same acoustic properties as water: for this reason liquid gel is used to couple extracorporeal ultrasound transducers to human skin. Similarly, bone absorbs a high amount of ultrasound energy, which can lead to unwanted heating along the bone surface while missing the target tissue (Avedian et al. 2011). These factors must be accounted for when planning and implementing FUS treatment.
Because thermal ablation of human soft tissue produces an immediate radical change in tissue properties from the host tissue, the ablation volume can be visualized during treatment via non-invasive imaging. Dependent on location in the body, the most commonly used approaches are ultrasound and magnetic resonance imaging (Copelan et al. 2015). Real time monitoring of lesion formation provides immediate feedback to control movement of the ultrasound focus for successive ablation events and also offers non-invasive verification of the cumulative extent of necrosis. Initially, ultrasound was the primary method for image guided ablation. Due to advances in quality and availability of high resolution MR systems, recent clinical work is shifting quickly to 1.5 and 3 T magnets for higher resolution definition of anatomy, metabolic status, and tissue temperature for real-time guidance of ablation procedures (Copelan et al. 2015; Woodrum et al. 2015; Kim 2015). Images of treatment planning and real-time temperature guidance are provided in Fig. 2.
Examples of treatment planning/guidance systems for MRgFUS. a Treatment planning/guidance for the Exablate Neuro system. Planning screens allow the operator to set treatment parameters, monitor beam path of the transducer array, thermal lesion location, time/temperature graphs, and ultrasound frequency spectrum (Image courtesy of the INSIGHTEC Ltd.) b Treatment guidance for the Sonalleve MR-HIFU system demonstrating the “Therapy Wizard” on the left and monitoring slices in the imaging panel. This system allows the operator to monitor real-time temperature rise at the target, as well as in near-field and far-field regions (Image courtesy of Philips)
Given the wide-ranging applicability of FUS, numerous extracorporeal and intracorporeal devices (e.g. transrectal, transurethral, intravascular, interstitial, etc.) have been designed to optimize application-specific treatment delivery. Today, custom tailored tools for specific organs or clinical situations are available for brain, breast, prostate, abdominal organs, and bone. These approaches take advantage of unique devices in order to achieve the best comfort and positioning of the patient as well as to obtain an effective FUS. At present, three MR-guided systems are available:
-
The Exablate MRgFUS system (INSIGHTEC Ltd., Haifa, Israel), which received the CE Mark and US Food and Drug Administration (FDA) approval for treatment of fibroids in 2002 and 2004, and palliative treatment of bone metastases in 2007 and 2012, respectively. Clinical studies are currently ongoing in prostate (phase I/II), breast (phase II), brain (phase I), soft tissue (phase I/II) and pancreas (phase II).
-
The Sonalleve MR-HIFU system (Koninklijke Philips Electronics N.V., Eindhoven, The Netherlands), received CE Mark for the palliative treatment of bone metastases in 2011. FDA studies for palliative treatment of bone metastases from breast cancer are in phase II/III clinical trials. Clinical studies are currently ongoing in breast (phase I/II), liver (phase I), soft tissue (phase I), rectum (phase II) and gynae metastases (phase I).
-
The TULSA-PRO system (Profound Medical Inc., Toronto ON, Canada) received the CE Mark for treatment of prostate cancer in 2016.
The following sections review the results of ongoing clinical trials (Table 1) in the primary clinical sites of application while describing existing equipment systems for MR-guided FUS (MRgFUS), also known as MR-HIFU. The majority of MRgFUS procedures aim for ablation or thermal surgery, however ultrasound transducers can operate at a lower intensity to produce therapeutic hyperthermia (40–45 °C) in the target, which is an adjuvant technique to enhance the therapeutic response of radiation and/or chemotherapy (De Haas-Kock et al. 2009). The chapter ends with an overview of ongoing research that will help define future applications for the field.
2 Clinical Applications of MRgFUS
2.1 Bone Metastases
Bone metastases are the most common source of pain in cancer patients (Berenson et al. 2006). Autopsy studies have shown that up to 85% of patients with breast, prostate and lung cancer have bone metastases at the time of death, where breast and prostate cancer patients often have survival measured in years. Based on strong clinical evidence from phase I, II and III clinical trials, MRgFUS has received both CE and FDA approvals for management of bone metastases-related pain. The therapeutic goals of such clinical studies included pain palliation, tumor reduction, prevention of impending pathologic fractures, and/or tumor decompression (Rodrigues et al. 2015). The denervation of the periosteum, which contains pain-reporting nerve fibers, is considered a major factor in pain palliation perception (Catane et al. 2007). This explains the rapid relief following FUS treatment which is characterized by significantly higher power deposition in the periosteum and bone relative to surrounding soft tissues. Tumor debulking caused by thermal ablation also plays a role since it diminishes the pressure on the adjacent tissue (Napoli et al. 2013; Hurwitz et al. 2014).
Several hundred patients have been treated who have exhausted, declined, or are unsuitable for other pain palliation methods. The success of the treatment can be evaluated based on changes in pain and quality of life scores, as well as decrease in pain medication usage. These include the Brief Pain Inventory (BPI), a validated 11-point scale for the evaluation of pain (0 = no pain, 10 = unbearable pain) in cancer patients (Cleeland and Ryan 1994), which has two different names: numerical rating scale (NRS) and visual analog scale (VAS). Quality of Life (QoL) is considered an important secondary endpoint in the majority of clinical studies that address painful bone metastases, and is equally evaluated in a 11-point scale (Rosenthal and Callstrom 2012) using tools such as the Brief Pain Inventory (BPI-QoL) (Cleeland and Ryan 1994) or QLQ-BM22, a questionnaire developed by the European Organization for Research and Treatment of Cancer (Chow et al. 2009). The majority of studies associated response with a ≥2-point decrease in pain at the treated site without increase in analgesic intake. Finally, the MD Anderson (MDA) criteria has been used to evaluate treatment efficacy via local tumor control (Costelloe et al. 2010). Quantitatively, these criteria define partial response (PR) as a decrease of ≥50% in the sum of the perpendicular measurements of a lesion, and progressive disease (PD) as an increase of ≥25% in this sum. A secondary measure is change in tumor size.
Liberman et al. in (2009) published the first multicenter clinical study on the use of MRgFUS for pain palliation of bone metastases. This report incorporated previously reported results (Catane et al. 2007) and (Gianfelice et al. 2008), and comprised of 31 patients with 32 bone lesions. Three-month follow-up was available for 25 out of 31 patients. A significant reduction in pain (>2 points) was reported by 72% of patients, with 36% reporting a VAS score of 0. The average VAS score decreased from 5.9 prior to treatment to 1.8 at the three-month follow-up, with 52% of patients reporting substantial pain relief within three days. 24% of patients had no response and one patient experienced worsened pain levels. A reduction in opioid usage was reported in 67% of patients with recorded medication data. No major complications were noted.
In 2013, Napoli et al. reported a prospective, single-arm research study with 18 patients treated with MRgFUS for painful bone metastases (Napoli et al. 2013). The pain severity score changed significantly from a baseline average of 7.1–1.1 at three-month follow-up. A score of 0 for pain severity, without medication intake, was reported by 72% of patients at final follow-up, consistent with a complete response to treatment. Computed tomography (CT) examinations demonstrated increased bone density with restoration of cortical borders in five patients (28%). According to the MDA criteria (Costelloe et al. 2010), a complete response to treatment was observed in two patients (11%), a partial response in four patients (22%), stable disease in 10 patients (56%) and progressive disease in two patients (11%). No treatment-related adverse events were recorded during the study.
The results of a multicenter phase III clinical trial on bone tumors were published by Hurwitz et al. (2014). 147 patients with metastatic bone pain, refractory to other pain interventions often including radiation, were randomized to MRgFUS treatment or placebo treatment. Patients randomized to placebo underwent the same procedure as those receiving MRgFUS treatment but without energy deposition. The pain response rates three months after treatment were 64% in the MRgFUS treated arm versus 20% in the placebo arm. Complete pain relief was observed in 23% of treated patients, compared to 6% of patients who received placebo treatment. Approximately two-thirds of responders experienced significant pain relief—as defined by a decrease in worst NRS score of 2 points or more—within three days of treatment, establishing the ability of MRgFUS to induce fast pain response. This response was accompanied by a similarly rapid improvement in patient function scores. The most common complication was pain during MRgFUS treatment (32%) and major complications occurred in 3% of treated patients: two patients had pathological fractures and one patient had third-degree skin burn. However, one fracture was outside the treated area, and the skin burn was due to a violation of the inclusion criteria protocol. Furthermore, the majority of adverse events (60%) were transient and resolved on the treatment day and 51 patients (46%) had no adverse events.
The phase III trial as reported by Hurwitz et al. was subject to a retrospective analysis of the safety of combination MRgFUS with active systemic chemotherapy (Meyer et al. 2014). Chemotherapy data were available for 104 patients and patients were followed for three months. Ninety patients were treated without chemotherapy, and 14 were treated with chemotherapy. There was no significant difference between the response rates of the chemotherapy group (71%) and the non-chemotherapy group (68%) with p = 0.78. The overall adverse event rates were 57% for chemotherapy patients and 45% for non-chemotherapy patients (p = 0.38), whereas the sonication pain was 50% and 28% for the same groups (p = 0.11), respectively. Remaining adverse event rates were not significantly different (p = 0.17).
Several single-arm trials have since been published supporting the safety and efficacy demonstrated in the phase III clinical trial. A prospective multicenter study with 72 patients was performed to evaluate the efficacy of MRgFUS for pain palliation of bone metastasis in patients who had exhausted radiotherapy or refused other therapeutic options (Zaccagna et al. 2014). Thirty four patients (47%) reported complete response to treatment and discontinued medications. Twenty nine patients (40%) experienced a pain score reduction >2 points, consistent with partial response. The remaining 9 patients (13%) had recurrence after treatment. Significant differences between baseline (VAS = 6) and follow-up (VAS = 2) average values and medication intake were observed. Similarly, a significant difference was found for QLQ-BM22 between baseline and follow-up. No treatment-related adverse events were recorded. Bazzocchi et al. (2015) evaluated the clinical outcome of 64 patients (90 lesions) with painful bone metastases that were treated with MRgFUS. The treated lesions ranged between 1 and 14 cm. On a lesion-based approach, average VAS score at baseline was 5.3 decreasing to 2.7 at one month, and to 1.8 after 12 months. Two treatment-related adverse events (3%) were reported: a single case of small skin burn and one case of prostate inflammation in a patient treated to the ischiopubic ramus. More recently, Gu et al. treated 23 patients with painful bone metastases with NRS ≥4 and that have not received radiotherapy or chemotherapy for pain palliation at least two weeks prior to MRgFUS treatment (Gu et al. 2015). Adverse events included pain in therapeutic area (13%), which relieved spontaneous within one week and numbness in lower limb (4%) that relieved after physiotherapy. Before treatment the average NRS was 6.0, which decreased to 3.7 and 2.2 at the one-week and three-month follow up, respectively. In the same timeframe, the average BPI-QoL score decreased from 39 to 27 and 21; and the QLQ-BM22 score decreased from 52 to 44 and 39, respectively. The clinical benefits of pain palliation and patient’s quality of life improved and were sustained after treatment at least to three months.
Further studies have introduced innovative approaches to treatment delivery. In 2014, Huisman and colleagues reported the first experience with volumetric MRgFUS for palliative treatment of painful bone metastases in 11 patients, a technique intended to reduce treatment time (Huisman et al. 2014). Three days after treatment, the pain score NRS decreased significantly from baseline median of 8 to 6 correlating with a response in six patients (55%). At one-month follow-up, which was available for nine patients, there was no pain recurrence, pain scores decreased significantly compared to baseline, and six patients (67%) obtained pain response. No treatment-related major complications were observed. More recently, Joo et al. (2015) evaluated the safety and effectiveness of a novel MRgFUS Conformal Bone System for the palliation of painful bone metastases. As opposed to table mounted systems, this applicator can be positioned on the target area with the patient in any position thereby optimizing patient comfort. Six painful metastatic bone lesions in five patients were treated and all patients showed significant pain relief within two weeks. Two patients experienced complete pain reduction that lasted for one year. The size of the enhancing soft tissue mass in metastatic lesions decreased, and new bone formation was seen on follow-up images (Fig. 3). No severe adverse events occurred.
Patient imaging before and after MRgFUS treatment for bone metastases. Comparison of a DCE-MRI before treatment and b at 90 days after treatment—note the decrease in size of the enhancing mass. Comparison of c CT before treatment and d at 90 days after treatment—note the new bone formation (arrow). e Further new bone formation (arrow) was seen on CT at one year post-treatment. Adapted with permission from Joo et al. (2015)
In summary, MRgFUS provides fast and durable relief of painful bone metastases as well as improved function in patients who failed or who are not candidates for radiation (Table 2). Given the impact of these clinically significant results, coupled with a favorable side effect profile, MRgFUS can now be considered a viable treatment option for painful bone metastases. Further studies are underway to assess the role of MRgFUS as a first-line therapy for patients with bone metastases (Table 1).
2.2 Breast Cancer
The first feasibility studies for use of MRgFUS in treatment of breast cancer date back over 15 years. Initial rates of complete or near complete ablation were 20–50%, but with ongoing refinement of the technique, more impressive results are now being reported. The first case report of MRgFUS for treatment of breast cancer was reported by Huber and colleagues (2001). The investigators described their experience with a patient who underwent MRgFUS five days prior to breast conservation surgery. Gianfelice and colleagues were the first to report on the accuracy of MRgFUS for treatment of a series of breast cancer patients, according to a treat-and-resect protocol. Twelve patients with invasive breast cancer were treated with two MRgFUS systems prior to surgery (Gianfelice et al. 2003). Histopathological analysis of resected tumor revealed a mean of 88% of cancer tissue necrosed in nine patients treated with the second generation system. However, residual tumor was noted at the periphery of the tumor in all patients, indicating the need for larger ablation margins in the range of 5 mm around the MR defined tumor. The complete list of studies can be found in Table 3.
Noting the importance of defining treatment effect with imaging, these investigators subsequently assessed the value of DCE-MRI parameters to monitor residual tumor following MRgFUS treatment of breast tumors. DCE-MRI data were acquired before and after the MRgFUS treatment of 17 patients with breast tumors <3.5 cm. Tumors were surgically resected and the presence of residual tumor was determined by histopathological analysis. The percentage of residual tumor was correlated with three DCE-MRI parameters measured at the maximally enhancing site of each tumor. Notably, complete necrosis or less than 10% residual tumor was observed in 76% lesions at the time of surgery including 23% with complete response. Allowing for a seven day post-treatment delay, a good correlation was found between the DCE-MRI parameters and the percentage of residual viable tumor determined by histopathology. The authors concluded the results suggest that parameters from DCE-MRI data can provide a reliable non-invasive method for assessing residual tumor following MRgFUS treatment of breast tumors (Gianfelice et al. 2003).
In a follow-up report on 24 women with a single biopsy proven breast carcinoma who were not surgical candidates, MRgFUS was used as an adjunct to tamoxifen. Biopsy was performed after six month follow-up and retreatment with MRgFUS was performed if residual tumor was present, in which case a second biopsy was performed one month later. Treatment was well tolerated with only one second-degree skin burn associated with treatment. Overall, 79% had negative biopsy results after one or two treatment sessions. The presence of enhancement or lack thereof on follow-up MR imaging appeared to correlate well with biopsy findings (Gianfelice et al. 2003). Zippel et al. reported the results of a phase I trial with use of the same MRgFUS system with similar results (Zippel and Papa 2005). They treated 10 patients followed by lumpectomy one week later with complete necrosis noted in two patients. Khiat et al. (2006) further assessed tumor eradication and the effect of post-treatment delay for evaluation of MR images on the presence of residual cancer. Twenty-five patients with 26 tumors underwent histopathological analyses following MRgFUS showed no residual cancer in eight lesions (31%) and <10% residual cancer in 11 lesions (42%). They too recommended an interval of approximately seven days to determine the effectiveness of MRgFUS. More recently Napoli have reported a complete response rate of 90% and partial response rate of 10% in 10 patients treated with a 3 T system (Napoli et al. 2013), with a successful example shown in Fig. 4.
Patient with breast cancer. a Gadolinium-enhanced T1 gradient recalled echo fat-saturated axial image shows the malignant highly vascular nodule. b After MRgFUS treatment, no residual enhancement of ablated lesion is detectable. Reprinted with permission from Napoli et al. (2013)
In follow-up to an initial feasibility report (Furusawa et al. 2006), Furusawa and colleagues published their experience with 21 cases of biopsy-proven invasive and noninvasive ductal carcinoma of the breast treated by MRgFUS. Median tumor size was 15 mm ranging from 5 to 50 mm. Seventeen patients received a single treatment and four patients were treated twice. With median follow-up of 14 months, one patient experienced local recurrence, with the remaining patients demonstrating no evidence of radiographic recurrence. Treatment was well tolerated, with skin burns in two patients (Furusawa et al. 2007). Furusawa subsequently has reported an update on an expanded cohort of 87 patients treated since 2005. The main inclusion criteria were biopsy-proven breast cancer up to 15 mm in size and well-demarcated mass seen in DCE-MRI. Postoperative needle biopsy was performed again within three weeks after ablation. The median age was 56 years and the average tumor size was 11 mm. With a median follow-up period of 68 months, no severe adverse events were noted. Local recurrence developed seven years after the initial treatment in only one invasive breast cancer case. There were no distant recurrences noted (Furusawa et al. 2015).
MRgFUS appears to be a promising method for replacing some surgical breast procedures with potential cosmetic benefits in very carefully selected patients. Two phase I/II clinical trials are current accruing patients for further confirmation of safety and effectiveness of this noninvasive procedure (Table 1).
2.3 Prostate Cancer
The most extensive clinical use of FUS has been for prostate cancer. Techniques include transrectal and transurethral approaches, with either whole gland or focal ablation. Of the tens of thousands of patients treated to date, almost all have been treated using ultrasound guidance, with regulatory approvals achieved in Europe, Asia, and recently in the United States. Although only a small fraction of prostate patients have been treated with MR guidance (Table 4), MR offers significant advantages over ultrasound guidance. These advantages include much better defined targeting with DCE-MRI and real-time temperature guidance to ensure adequate tumor ablation while protecting critical normal tissues such as urethra, bladder neck, rectum, and neurovascular bundles.
To date, five preliminary feasibility studies of MRgFUS for treatment of prostate cancer have been published, all involving eight or fewer patients treated with transurethral (Siddiqui et al. 2010; Chopra et al. 2012) or transrectal approach (Lindner et al. 2012; Napoli et al. 2013; Ghai et al. 2015). Taken together, these studies have demonstrated the ability of MRgFUS to effectively treat the intended targeted areas with few or no adverse effects. More recently, Chin et al. reported a series of 30 patients treated with a 3T MR guided transurethral system (Fig. 5). At the 12-months follow-up, a 14% complete and 55% partial response rates were noted with median PSA declining from 5.8 ng/ml pre-treatment to 0.8 ng/ml at 12 months. Urinary IPSS score improved slightly from 8 to 5 over the same period with no change in sexual function as measured by the IIEF. One major adverse event (epididymitis) was noted with all other toxicities scored as minor including 50% hematuria, 33% urinary tract infections, and 27% acute urinary retention (Chin et al. 2016).
Example MRI findings through the prostate mid-gland. a Treatment planning transverse MR image, showing the TULSA-PRO device in a patient: transurethral Ultrasound Applicator (UA) and Endorectal Cooling Device (ECD). b Maximum temperature measured during ultrasound treatment using real-time MR thermometry; the acute cell kill target temperature (≥55 °C) was shaped accurately and precisely to the treatment plan (black contour). c DCE-MRI image acquired immediately after treatment, demonstrating the hypointense region of non-perfused prostate tissue concordant with the acute ablative temperatures on MR thermometry. d Corresponding location in the prostate at 12-month follow-up, showing 85% reduced prostate volume. Image courtesy of Profound Medical Inc
At present, two phase I and one multi-institutional phase II study have been opened to assess the use of MRgFUS partial gland ablation in subjects with low or low-intermediate risk prostate cancer (Table 1). In the latter (NCT01226576), 80 patients with cT1c and cT2a, N0, M0, PSA ≤10 ng/ml and Gleason score 6 or 7 who may currently be on watchful waiting or active surveillance and not in need of imminent radical therapy are eligible. Up to two cancerous lesions may be identified for MRgFUS ablation in the prostate with each tumor not exceeding more than 10 mm in maximal linear dimension.
2.4 Brain Cancer
MRgFUS has great potential for treating brain tumors, because the technique could be used to ablate targeted tissue without injuring the normal brain. The main challenge for FUS in the brain is the high energy absorption in bone, which leads to excessive heating in the skull and adjacent brain parenchyma (Kobus and McDannold 2015). In addition, local variations in the skull thickness acts as defocusing lens (Hynynen 2010). Despite these challenges, several advances have now accelerated the development of transcranial MRgFUS. First, it was discovered that a relatively sharp focus can be produced through intact skull using a low frequency phased array (Sun and Hynynen 1998; Hynynen and Jolesz 1998) coupled with software that compensates for skull-induced distortions of FUS (Aubry et al. 2003). The skull heating problem can be overcome using a phased array applicator with large surface areas that spread the ultrasound energy over much of the skull (Sun and Hynynen 1999; Clement et al. 2000). Second, modern medical imaging can provide enough information to allow precise focusing noninvasively (Clement and Hynynen 2002; Pernot et al. 2003). The development of sophisticated MR imaging sequences permit high-resolution visualization of brain targets, as well as real-time tissue temperature maps, thus allowing real-time monitoring and guidance for FUS (McDannold and Jolesz 2000; Hynynen et al. 2000; Ishihara et al. 1995; Odeen et al. 2014).
In 2006, Ram and colleagues reported a phase I clinical study to treat three patients with recurrent glioblastoma multiforme (Ram et al. 2006). Prior to MRgFUS treatment, patients underwent a standard craniotomy over the tumor area to create the bony window necessary for penetration of the ultrasound waves. Histological analysis in one patient showed sharp delineation between viable tumor and thermocoagulated tumor at the treated site. One patient made an uneventful recovery, but nine months later showed evidence of tumor progression and died of her disease 10 months after the MRgFUS treatment. The remaining two patients were still alive after 33 and 38 months. Two adverse events were reported, a mild left hemiparesis that developed three days after treatment in one patient and mild transient worsening of preexisting dysphasia in another patient.
McDannold et al. (2010) published their experience with a dedicated MRgFUS system for brain applications (512 elements, 670 kHz) in three patients with high-grade glioma. All patients underwent the procedure under conscious sedation and tolerated the procedure well. Their results suggest that it is feasible to heat tumors in the brain without overheating the tissue at the brain surface and without performing a craniotomy. However, the targetable regions may be limited to deep and central locations in the brain. Nonetheless, these are precisely the locations where surgery is challenging or not an option. After this experience several technical adjustments were implemented (Lipsman et al. 2014), leading to an improved system with a conformal hemispherical shape (Fig. 6). This system has now been used to treat more than 200 patients with a range of neurological disorders through precise thermal ablation. No severe adverse events have been observed and the device has received regulatory approvals for treatment of movement disorders (essential tremor and Parkinson’s tremor) and neuropathic pain in several countries (Foley et al. 2015).
a Commercially available transcranial MRgFUS system, which integrates a 650 kHz hemispheric array with 1024 ultrasound transducers into a clinical MRI system. The patient’s head is fixed to the system in a stereotactic frame and a diaphragm placed around the patient’s scalp before filling the transducer with degassed water to allow ultrasound waves to propagate into the head (Courtesy of INSIGHTEC Ltd.). b Treatment planning is based on initial MRI scans, with modelling to plan the dynamic scanning of heat focus for contiguous heating of large tissue volumes (Courtesy of IT’IS Foundation, Zürich, Switzerland)
Motivated by the excellent results in non-oncological applications, Coluccia and colleagues reported a case report to demonstrate feasibility and safety in a patient with recurrent glioblastoma (Coluccia et al. 2014). The patient received local anesthesia for the positioning of a stereotactic frame. Post-operative MR images showed well circumscribed areas of non-enhancing volumes at the location of sonicated tumor tissue. No adverse events were reported. While the total ablation volume is substantial (0.7 cc), it is still relatively small, i.e., 10% of the enhancing tumor volume (6.5 cc), and not sufficient for significant cytoreduction as is the key for sustained tumor control. Nonetheless, this result demonstrated, for the first time, the feasibility of using noninvasive transcranial MRgFUS to safely ablate brain tumor tissue.
2.5 Liver Cancer
Invasive thermal ablations with radio frequency (RF) or laser-probes have been shown to increase local tumor control and survival in patients with primary or metastatic liver tumors (Lin 2009). The use of FUS to ablate tumors deep in the liver offers the first completely noninvasive alternative to these techniques and it has been widely tested with US imaging guidance (USgFUS), mostly in China (Wu 2006; Wu et al. 2004). In a clinical trial with 55 patients with large (average 8 cm) hepatocellular carcinoma (HCC), Wu et al. demonstrated a complete ablation rate up to 69% without major complications, overall survival rates of 62% at 12 months and 35% at 18 months (Wu et al. 2004). Leslie et al. (2008) reported a phase II efficacy trial that showed USgFUS to be feasible. Using USgFUS, Xu et al. (2011) reported a two-year survival rate of 80% in patients with stage Ib HCC, 51% in stage IIa, and 47% in stage IIIa. In patients with unresectable HCC receiving USgFUS, it was demonstrated one- and three-year survival rates of 88% and 62%, respectively (Ng et al. 2011). Chan and colleagues evaluated the feasibility of USgFUS and patient survival in 27 patients with recurrent HCC (average tumor size of 1.8 cm) after first-line therapy with either hepatectomy or RF ablation at a median follow-up of 28 months. Complete tumor ablation was obtained in 85% of the patients. The three-year overall survival rate was 70% (Chan et al. 2013).
The principal feasibility of USgFUS ablation has been proven and extensively validated for parenchymal abdominal organs; introduction of MR-guidance in this field should thus be considered a natural evolution of this modality. There are only occasional reports of MRgFUS ablation in abdominal organs, mostly on animal models of liver tissue (Kopelman et al. 2006; Courivaud et al. 2014), with clinical trials in humans still ongoing (Table 1). Human treatments have been implemented so far with suspended respiration, which requires intubation and anesthesia. This respiratory gating approach overcomes liver motion during MR temperature measurement and also allows accurate targeting (Okada et al. 2006; Tokuda et al. 2008). More recently, real-time liver motion compensation has been developed and tested both in animal models (Quesson et al. 2011; Zachiu et al. 2015; Wijlemans et al. 2015; Holbrook et al. 2014) and in healthy volunteers (Napoli et al. 2013), potentially providing a chance for more accurate MRI guidance of liver ablation. Another difficulty in using FUS for abdominal targets is the presence of intervening anatomy such as ribs and bowel, which limit the acoustic window. To overcome this problem, sonications are delivered only between the ribs (Quesson et al. 2010; Zhou 2011).
So far, only single case reports were documented on the use of MRgFUS for treatment of liver cancer for a patient with HCC that refused RF ablation (Okada et al. 2006). The tumor measured about 15 mm in diameter and was located in the lateral segment of the liver, where there was no rib or bowel loop in the path of the ultrasound beam. Using respiratory gating, the tumor was completely ablated. In 2013, Napoli et al. performed a successful MRgFUS ablation in one patient with unifocal HCC, who was not eligible for other treatment options (Napoli et al. 2013). Post-treatment follow-up revealed a decrease of α-fetoprotein compared to baseline levels. Treatment efficacy was evaluated with DCE-MRI, revealing an extensive decrease of contrast uptake from tumor after MRgFUS ablation compared to baseline examination, correlating with significant reduction of symptom severity. More recently, Anzidei et al. (2014) presented a study designed to evaluate the feasibility and safety of MRgFUS for treatment of solid tumors in the upper abdomen, including one patient with HCC. Treatment response was evaluated by assessing the non-perfused volume (NPV) of ablated tissue at MR and the degree of pain severity. Immediately after treatment and at one-month follow-up, the lesion showed complete ablation (100% NPV); six-month follow-up images showed a small focus of recurrent tumor tissue along the lateral edge of the ablation zone, with a NPV of 85%. Histological analysis after liver transplantation showed fibrosis in the ablated area with minimal local tumor recurrence.
In summary, MRgFUS for liver lesions is still at an early stage due to the limited therapeutic window through the ribcage and complications from respiratory motion. Nonetheless, the aforementioned case studies indicate that MRgFUS for liver ablation is feasible. The integration of recent technology will allow the use of a higher number of phased-array elements and MRI-based tracking and gating, which will permit the acoustic beams to be synchronized with the moving organ to allow treatment of freely breathing patients.
2.6 Pancreatic Cancer
Anzidei and colleagues have reported the results of a pilot study with six patients assessing feasibility, safety, pain palliation, and potential for local tumor control with MRgFUS for pancreatic cancer (Anzidei et al. 2014). Outcome assessments with a follow-up between three and six months were based on imaging for response, yielding a 83% complete and 17% partial response rates. The VAS scale was used to assess pain and it decreased from an average of 7.3 pre-treatment to 3.8 one month post-treatment, which was consistent with a clinically meaningful improvement in pain. More recently, Jove-Vidal and colleagues reported encouraging results with USgFUS in 45 patients with unresected tumors treated between 2008 and 2015 with 83% overall response rate as assessed at eight weeks, with an encouraging median survival of 16 months and overall survival of 34% at five-year follow-up. The toxicity profile included the following major complications: severe pancreatitis (4%), third-degree skin burn that required plastic surgery (4%), and duodenal perforation (2%). These early results with USgFUS await validation including with use of MR-guided techniques (Vidal-Jove et al. 2016).
2.7 Soft Tissue Tumors
MRgFUS clinical studies for soft-tissue tumors are limited. In 2015, Ghanouni and colleagues reported a clinical study with seven patients with desmoid tumors, two patients with arteriovenous malformation (AVM) and one patient with a sarcoma in the thigh (Ghanouni et al. 2015). The average NPV for desmoid tumors (42–1010 cc) was 58%, whereas the sarcoma (20 cc) was 97%. Five of the desmoid tumor patients were included in a subsequent multicenter trial with 15 patients (Ghanouni et al. 2016). The median viable targeted tumor volume decreased 63%, corresponding to a decrease from 105 to 54 ml in volume. Pain response was also assessed, with a significant pain reduction (NRS) from 6 to 1 after MRgFUS treatment. Only minor complications were observed. The authors concluded that MRgFUS may safely and effectively treat extra-abdominal desmoid tumors.
Further studies are required to assess the role of MRgFUS as first-line therapy in patients with soft tissue tumors. There are currently three clinical trials open for accrual, including a phase I/II study to determine the safety and efficacy of MRgFUS in the treatment of soft tissue tumors of the extremities (NCT01965002) and a phase I study to determine if MRgFUS is safe and feasible for treatment of children with refractory or relapsed solid tumors (NCT02076906). The last clinical study is a multimodality approach that aims to determine whether Doxil (liposomal doxorubicin) given prior to MRgFUS hyperthermia is safe for the treatment of pediatric and young adult patients with recurrent and refractory solid tumors (NCT02557854). A preliminary report of this trial included seven tumors in six patients with osteosarcoma (n = 3), Ewing sarcoma (n = 3) and neurofibrosarcoma (n = 1). The MR thermometry (MRT) quality results of lower extremities was sufficient to control MRgFUS hyperthermia, but motion compensation or breath may be required to achieve reliable MRT in pelvic and abdominal tumors in pediatric patients (Laetsch et al. 2016).
2.8 Cervical Cancer
The first MRgFUS application to receive clinical certification was the treatment of uterine fibroids that received CE Mark in 2002 and FDA approval in 2004 (Dick and Gedroyc 2010). Despite the success in treating these benign neoplasms of the uterus (Clark et al. 2014), only one clinical case of treating cervical carcinoma with MRgFUS has been reported. Machtinger et al. (2008) presented a case report for pain relief in a 29-year-old patient suffering from recurrent cervical carcinoma. This patient failed traditional treatments and underwent two MRgFUS treatments two weeks apart, resulting in a substantial decrease in pelvic pain. No adverse events were reported during the procedure or during the follow-up. The patient remained free of pain for four months after treatment. A 35 patient pilot study started in 2016 to determine whether or not it is feasible to use MRgFUS to treat symptomatic pain and bleeding from recurrent gynecological malignancies with an acceptable safety profile (NCT02714621).
2.9 Colorectal Cancer
The colon and rectum sites are particularly difficult to heat with noninvasive focused ultrasound due to the shadowing effect of the sacral bone. In 2004, researchers in China published a study suggesting that USgFUS ablation combined with radiation could be safe and effective in patients with rectal carcinoma (Jun-Qun et al. 2004). Later, in 2011, researchers in London reported a single case of advanced, recurrent rectal carcinoma treated with transrectal focused ultrasound (Monzon et al. 2011). These limited clinical results have been supplemented with promising preclinical studies. A recent preclinical study showed that FUS along with gold nanoparticles and pulsed light, could shrink tumors (Sazgarnia et al. 2013), and another preclinical study suggested that FUS can enhance the targeted delivery of chemotherapy (Park et al. 2013).
Clearly, recurrent rectal cancer is a vexing clinical problem and current retreatment protocols have limited efficacy (Ahmed et al. 2014). With this in mind, a clinical trial was designed to test the hypothesis that MRgFUS hyperthermia is technically feasible and can be safely used in combination with concurrent reirradiation and chemotherapy for the treatment of recurrent rectal cancer without increased side-effects (NCT02528175). The first report from this trial includes a patient with rectal recurrence in the pelvic sidewall. During MRgFUS, the patient was under conscious sedation, and provided verbal feedback to the physician to decide when to pause the treatment. The patient did not report pain, and has no adverse effects after 90 days of follow-up. Therapeutic temperatures were achieved with no treatment-related toxicity (Chu et al. 2016).
2.10 Emerging Clinical Applications of MRgFUS
MRgFUS treatment of renal disease must overcome many similar challenges as reported for treatment of liver cancer due to their similar location in the ribcage (Quesson et al. 2011). For this reason, the clinical trial NCT01197820 addressed the technical feasibility of MRgFUS for treatment of both liver and kidney with a focus on challenges related to organ motion. The safety and feasibility of USgFUS was previously established in 2003 (Wu et al. 2003) and later in 2005 (Illing et al. 2005), but the ablation of liver tumors was achieved more consistently than for kidney tumors: 100% versus 67%, assessed radiologically. The primary reason relates to higher blood perfusion in kidneys, which carries away heat more efficiently than in liver (Quesson et al. 2011). A recent preclinical study reported the use of MRgFUS to create renal lesions on six mechanically-ventilated pigs (Saeed et al. 2016). Histopathology examinations and DCE-MRI showed presence of coagulative necrosis, interstitial hemorrhage and vascular damage in the renal target lesions. The authors suggested that in order to address the high blood perfusion in kidneys, the MRgFUS could be used to mediate vascular occlusion prior to targeting the tumor.
One of the most recent target applications for MRgFUS is head and neck cancer. Although there are no current clinical results, Lee and colleagues published the clinical protocol of a pilot study to assess safety, toxicity and feasibility of MRgFUS in the head and neck region (Lee et al. 2016). This prospective trial plans to recruit 10 patients to undergo MRgFUS prior to palliative radiotherapy. The authors hypothesize that treatment will cause de-vascularization and necrosis of the targeted lesion by heating the tissue to 55–90 °C during approximately 30 s. Also, a margin of 1 cm will be left between the ablation zone and neighboring critical structures. Serious adverse events and toxicity will be evaluated at 1, 7, 14, 30, 90 days follow-up, and post-MR imaging will be performed. In addition, clinical studies are under consideration to examine the use of MRgFUS to enhance standard chemo-radiotherapy treatments of locally advanced, unresectable head and neck tumors.
Pre-clinical work has been completed or is ongoing for several additional clinical applications. Because of diaphragm movement and air content of ventilated lungs, lung tumors have never been treated with FUS (Wolfram et al. 2014). However, Lesser et al. proposed flooding one lung to produce a suitable acoustic pathway to treat lung tumors with MRgFUS. This approach was investigated in in vivo pig models and in ex vivo human tissues (Wolfram et al. 2014; Lesser et al. 2016). In other site, Karakitosis et al. presented a feasibility study to induce thermal ablation in the vertebral body and intervertebral discs using MRgFUS. The study demonstrated that the heating pattern could induce thermal ablation in the target, with no damage in adjacent critical structures such as nerves (Karakitsios et al. 2016). The feasibility of esophageal thermal ablation using intraluminal MRgFUS has also been demonstrated in a preclinical setting (Melodelima et al. 2005).
3 Future Directions
Increasing clinical interest in MRgFUS has fueled continued development of the modality for a variety of clinical applications. Future directions within the field are expected to utilize ongoing research in both the MR and ultrasound fields to further leverage current advancements. These advancements are in various stages of development or early clinical adoption and are expected to benefit the field of MRgFUS for oncological applications.
3.1 Targeted Drug Delivery
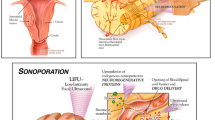
A variety of applications using MRgFUS for targeted drug delivery have recently been presented in the literature. The applications generally focus on areas that are amenable to both MR and US imaging, and that have also presented historical challenges for delivery of therapeutics. One such area is the localized delivery of therapeutic agents across the blood brain barrier (BBB). Delivery of therapeutics from the vasculature to brain extracellular fluid is greatly limited by the presence of tight junctions, which restrict passage of molecules larger than 400 Da or those that form greater than eight hydrogen bonds with water. These exclusions rule out direct passage of over 99% of therapeutic drugs (Pardridge 2005). However, as ultrasound waves propagate through tissue, they interact with dissolved gases in a process known as cavitation, leading to the formation of gas-filled microbubbles that has been shown to temporarily increase BBB permeability (De Smet et al. 2013; Liu et al. 2012; Diaz et al. 2014; Nance et al. 2014; Marquet et al. 2011). Using this approach, Nance et al. (2014) demonstrated in rats that MRgFUS enables delivery of 60 nm nanoparticles across the BBB when disrupted by microbubble cavitation, making localized delivery of drugs to the brain feasible. This approach has also been demonstrated in non-human primates (Marquet et al. 2011), and a first-in-humans clinical trial is currently underway for the delivery of doxorubicin to solid brain tumors (NCT02343991). In addition, it has been shown in a preclinical setting (via both MRI and histological analyses) that the BBB reverts to its original structure without permanent damage within four hours after the end of the sonication (Tung et al. 2011).
Targeted drug delivery can be achieved using MRgFUS by encapsulating the drug of choice within either a temperature or acoustic pressure sensitive carrier. These carriers can be injected systemically, but release their contents only when triggered within the targeted area. Temperature-sensitive liposomes have been fabricated to deliver anticancer drugs at moderate temperatures (Ponce et al. 2006; Escoffre et al. 2013; Zagar et al. 2014). After systemic injection, these liposomes aggregate within the tumor space either as a function of the enhanced permeation and retention effect, or through passive targeting with the conjugation of tumor-specific peptides on the surface of the carrier (Ponce et al. 2006). Localized hyperthermia using MRgFUS can then be used to generate localized release of the chemotherapeutics. Similarly, drugs can be conjugated or encapsulated within ultrasound-sensitive microbubbles or nanoemulsions, and their localized release triggered with focused ultrasound (Rapoport et al. 2013; Eisenbrey et al. 2010, 2015). These results have demonstrated significant advantages in preclinical cancer models (Cochran et al. 2011; Zhu et al. 2016), and eventual clinical trials are expected.
Similar approaches using the combination of MRgFUS and microbubble cavitation have been used in gene transfection applications. Gene therapy translation has generally suffered from low overall delivery and transfection efficiencies (Al-Dosari and Gao 2009). Using the bioeffects described above, different groups have shown improved delivery and transfection efficiencies using the combination MRgFUS and microbubble cavitation. This work is currently in preclinical stages and covers a wide range of applications including improved gene transfection in the spinal cord (Weber-Adrian et al. 2015), treatment of cardiovascular disease (Chen et al. 2013), and solid tumors (Carson et al. 2011). These encouraging results are expected to translate to pilot clinical trials in the near future.
3.2 Image Optimization
3.2.1 Image Fusion
As imaging modalities, the inherent strengths and limitations of MR and ultrasound make them natural adjuncts in diagnostic imaging. MR suffers from relatively low temporal resolution making guidance difficult in soft tissues prone to respiratory motion such as the liver and kidneys (Napoli et al. 2013). USgFUS for liver and renal tumors is more prevalent in the literature in part due to the favorable cost and ability of ultrasound image guidance to effectively deal with organ motion (Schlesinger et al. 2013). However, hepatic lesions visible on MR may not be seen on ultrasound imaging, particularly lesions less than 2 cm and those closer to the diaphragm (Lee et al. 2010), limiting the ability to ablate these masses with USgFUS. Image fusion systems may be an alternative to these limitations. These systems use co-registration of MR or CT image stacks with real-time ultrasound data using magnetic sensors attached to the ultrasound transducer and a stationary reference center stationed near the patient (Ewertsen et al. 2013). Electromagnetic needle tracking systems can also be implemented for MR/US fusion guided procedures and have been used for a variety of interventions including liver and kidney mass biopsy and ablation and targeted prostate biopsy (Ewertsen et al. 2013). These approaches have improved confidence in targeting technically challenging lesions (Kang and Rhim 2015) and should be applicable to FUS therapies in the future. As an alternative, but similar approach, MR compatible ultrasound transducers have also been developed enabling real-time MR/US hybrid guidance (Petrusca et al. 2013). This approach would benefit from the inclusion of both the real-time motion compensation of ultrasound guidance and MR-thermometry treatment monitoring.
3.2.2 Synergistic MR and US Contrast Agents
Multimodality contrast agents are expected to be useful for MRgFUS. These agents will enable better image guidance and monitoring by improving visualization of targeted regions on both modalities. Additionally, inclusion of ultrasound contrast agents or nanoemulsions have been shown to lower cavitation thresholds in FUS, thereby selectively sensitizing areas of interest to tissue heating (Kopechek et al. 2014; Farny et al. 2010). Multimodality contrast agents for ultrasound and MR imaging have been developed consisting of microbubbles with either iron oxide or gadolinium in the shell (Teraphongphom et al. 2015). More recently, these particles have been modified to include doxorubicin for potential targeted cancer therapy (Teraphongphom 2016). An example of this work is provided in Fig. 7, showing attachment of iron oxide nanoparticles conjugated to a poly-lactic acid microbubble on transmission electron microscopy, and these same multi-modality agents on fluorescence microscopy showing the presence of doxorubicin (in red) within the shell of the microbubble. While these particles are still in early preclinical studies, their potential clinical impact may be significant in that they combine both the therapeutic and imaging benefits described above.
Poly-lactic acid ultrasound contrast agents loaded with iron oxide nanoparticles which are visible on transmission electron microscopy (a) and doxorubicin which is visible on fluorescence microscopy (b) for targeted drug delivery with MRgFUS (Courtesy of Dr. Nutte Teraphongphom). c Schematic representation of substance delivery using ultrasound-targeted microbubble destruction. An ultrasound contrast agent with an attached or incorporated bioactive substance is administered into the vasculature and will distribute throughout the capillaries. Ultrasound can then destroy microbubbles in the target region, thus releasing the transported substance into the surrounding tissue [Reprinted with permission (Bekeredjian et al. 2005)]
3.3 Multimodality MRgFUS Treatments
Perhaps the greatest benefits of MRgFUS in oncology remain to be realized through its integration in multimodality oncologic care. Many cancer patients are treated with combinations of surgery, radiation, and chemotherapy; yet there is a paucity of research exploring the integration of ablative therapies such as MRgFUS with other anti-cancer therapies. Beyond the utility of MRgFUS for targeted drug delivery and opening the blood brain barrier, MRgFUS may also augment effects of standard approaches to chemotherapy through enhanced effects mediated at the heated—but non-ablated—rim of tissue adjacent to the ablation zone. Moderate temperature elevation in this tumor margin should significantly enhance the effects of radiotherapy, including complementary tumor cell killing based on stage of the cell cycle, pH, degree of hypoxia, and repair inhibition of radiation induced DNA damage (Hurwitz and Stauffer 2014). Benefits seen in randomized studies combining hyperthermia and radiation or chemotherapy for many tumor types point to the promise of similar benefits with thermal therapy induced with MRgFUS (Hurwitz and Stauffer 2014). Likewise, hyperthermia has been shown in preclinical models to have multiple anti-tumor effects mediated through augmentation of immune response across the cancer-immunity cycle (Toraya-Brown and Fiering 2014). Tumor antigen spillage with MRgFUS ablation is one of many ways this modality may work across the therapeutic temperature profile to make immunotherapy more effective. In addition, the aforementioned mechanical effects combined with thermal effects can induce vasoconstriction or even hemostasis. This strategy is being considered as a noninvasive method to cut off the blood supply to tumors, effectively starving them of vital nutrients and making them more vulnerable to other treatments (Goertz 2015).
Finally, new techniques are in development that should shorten treatment time. Strategies to accomplish this important goal include the injection of microbubbles to increase the absorption of acoustic energy, optimized scanning algorithms, and also the use of spiral sonications; all techniques that should reduce the time of MRgFUS treatments.
4 Concluding Remarks
Without doubt, the next decade will see rapid advances in both clinical and technological application of MR-guided focused ultrasound. As results from preclinical models translate to clinical trials, clinicians will have a powerful new tool for expand treatment capabilities for their cancer patients who may not want or cannot tolerate an operation. MRgFUS may also serve as a powerful adjuvant or enhancer to other treatments, including gene therapy, radiation therapy, chemotherapy, and immunotherapy. Larger studies with longer follow-up will help characterize the long-term clinical and radiological effects, allowing better comparisons with approved modalities. Despite impressive temperature (0.1 °C) and spatial (1 mm diameter) accuracy, the most dramatic advances for MRgFUS will be technical. Currently, the typical procedure length for MRgFUS is of the order of 2–4 h. With evolving software, off-line analysis of tumor anatomy and its surroundings, as well as experience, procedure length will be significantly shortened. In summary, MRgFUS is a rapidly emerging technology offering a non-invasive treatment option either as monotherapy or in combination with other anti-neoplastic modalities.
Abbreviations
- AE:
-
Adverse events
- AVM:
-
Arteriovenous malformation
- BBB:
-
Blood brain barrier
- BPI:
-
Brief pain inventory
- BPI-QoL:
-
Brief pain inventory-Quality of life
- CE:
-
European conformity
- CR:
-
Complete response
- CT:
-
Computed tomography
- DCE-MRI:
-
Dynamic contrast-enhanced magnetic resonance imaging
- DNA:
-
Deoxyribonucleic acid
- ECD:
-
Endorectal cooling device
- FDA:
-
Food and drug administration
- FUS:
-
Focused ultrasound
- HCC:
-
Hepatocellular carcinoma
- HIFU:
-
High-intensity focused ultrasound
- IBMCWP:
-
International bone metastasis consensus working party
- IIEF:
-
International index of erectile function
- IPSS:
-
International prostate symptom score
- MDA:
-
MD Anderson criteria
- MR:
-
Magnetic resonance
- MRgFUS:
-
Magnetic resonance guided focused ultrasound
- MR-HIFU:
-
Magnetic resonance high-intensity focused ultrasound
- MRT:
-
MR thermometry
- NPV:
-
Non-perfused volume
- NR:
-
No response
- NRS:
-
Numerical rating scale
- OMED:
-
Changes in analgesic intake
- OR:
-
Overall response
- PD:
-
Progressive disease
- PP:
-
Pain progression
- PR:
-
Partial response
- PSA:
-
Prostate specific antigen
- QLQ-BM22:
-
European Organization for Research and Treatment of Cancer—Quality of life questionnaire for patients with bone metastases
- QoL:
-
Quality of life
- RF:
-
Radio frequency
- RR:
-
Recurrence
- UA:
-
Ultrasound applicator
- USgFUS:
-
Ultrasound guided focused ultrasound
- VAS:
-
Visual analog scale
References
Ahmed S, Johnson K, Ahmed O, Iqbal N (2014) Advances in the management of colorectal cancer: from biology to treatment. Int J Colorectal Dis 29(9):1031–1042. doi:10.1007/s00384-014-1928-5
Al-Dosari MS, Gao X (2009) Nonviral gene delivery: principle, limitations, and recent progress. AAPS J 11(4):671–681. doi:10.1208/s12248-009-9143-y
Anzidei M, Napoli A, Sandolo F, Marincola BC, Di Martino M, Berloco P, Bosco S, Bezzi M, Catalano C (2014a) Magnetic resonance-guided focused ultrasound ablation in abdominal moving organs: a feasibility study in selected cases of pancreatic and liver cancer. Cardiovasc Intervent Radiol 37(6):1611–1617. doi:10.1007/s00270-014-0861-x
Anzidei M, Marincola BC, Bezzi M, Brachetti G, Nudo F, Cortesi E, Berloco P, Catalano C, Napoli A (2014b) Magnetic resonance-guided high-intensity focused ultrasound treatment of locally advanced pancreatic adenocarcinoma: preliminary experience for pain palliation and local tumor control. Invest Radiol 49(12):759–765. doi:10.1097/RLI.0000000000000080
Aubry JF, Tanter M, Pernot M, Thomas JL, Fink M (2003) Experimental demonstration of noninvasive transskull adaptive focusing based on prior computed tomography scans. J Acoust Soc Am 113(1):84–93. doi:10.1121/1.1529663
Avedian RS, Gold G, Ghanouni P, Pauly KB (2011) Magnetic resonance guided high-intensity focused ultrasound ablation of musculoskeletal tumors. Curr Orthop Pract 22(4):303–308. doi:10.1097/BCO.0b013e318220dad5
Bazzocchi A, Facchini G, Spinnato P, Donatiello S, Diano D, Rimondi E, Battaglia M, Albisinni U (2015) Palliation of painful bone metastases: the “Rizzoli” experience. In: Annual congress of the European society of musculoskeletal radiology, York, UK, 18–20 June 2015. pp P-0136. doi:10.1594/essr2015/P-0136
Bekeredjian R, Grayburn PA, Shohet RV (2005) Use of ultrasound contrast agents for gene or drug delivery in cardiovascular medicine. J Am Coll Cardiol 45(3):329–335. doi:10.1016/j.jacc.2004.08.067
Berenson JR, Rajdev L, Broder M (2006) Cancer biology and therapy. J Am Coll Radiol 5(9):1078–1081. doi:10.4161/cbt.5.9.3306
Carson AR, McTiernan CF, Lavery L, Hodnick A, Grata M, Leng XP, Wang JJ, Chen XC, Modzelewski RA, Villanueva FS (2011) Gene therapy of carcinoma using ultrasound-targeted microbubble destruction. Ultrasound Med Biol 37(3):393–402. doi:10.1016/j.ultrasmedbio.2010.11.011
Catane R, Beck A, Inbar Y, Rabin T, Shabshin N, Hengst S, Pfeffer RM, Hanannel A, Dogadkin O, Liberman B, Kopelman D (2007) MR-guided focused ultrasound surgery (MRgFUS) for the palliation of pain in patients with bone metastases - preliminary clinical experience. Ann Oncol 18(1):163–167. doi:10.1093/annonc/mdl335
Chan AC, Cheung TT, Fan ST, Chok KS, Chan SC, Poon RT, Lo CM (2013) Survival analysis of high-intensity focused ultrasound therapy versus radiofrequency ablation in the treatment of recurrent hepatocellular carcinoma. Ann Surg 257(4):686–692. doi:10.1097/SLA.0b013e3182822c02
Chen ZY, Lin Y, Yang F, Jiang L, Ge S (2013) Gene therapy for cardiovascular disease mediated by ultrasound and microbubbles. Cardiovasc Ultrasound 11:11. doi:10.1186/1476-7120-11-11
Chin JL, Billia M, Relle J, Roethke MC, Popeneciu IV, Kuru TH, Hatiboglu G, Mueller-Wolf MB, Motsch J, Romagnoli C, Kassam Z, Harle CC, Hafron J, Nandalur KR, Chronik BA, Burtnyk M, Schlemmer HP, Pahernik S (2016) Magnetic resonance imaging-guided transurethral ultrasound ablation of prostate tissue in patients with localized prostate cancer: a prospective phase 1 clinical trial. Eur Urol S0302-2838 (15):01238-01235. doi:10.1016/j.eururo.2015.12.029
Chopra R, Colquhoun A, Burtnyk M, N’Djin WA, Kobelevskiy I, Boyes A, Siddiqui K, Foster H, Sugar L, Haider MA, Bronskill M, Klotz L (2012) MR imaging-controlled transurethral ultrasound therapy for conformal treatment of prostate tissue: initial feasibility in humans. Radiology 265(1):303–313. doi:10.1148/radiol.12112263
Chow E, Hird A, Velikova G, Johnson C, Dewolf L, Bezjak A, Wu J, Shafiq J, Sezer O, Kardamakis D, van der Linden Y, Ma B, Castro M, Foro Arnalot P, Ahmedzai S, Clemons M, Hoskin P, Yee A, Brundaye M, Bottomley A, Grp EQL (2009) The European organisation for research and treatment of cancer quality of life questionnaire for patients with bone metastases: the EORTC QLQ-BM22. Eur J Cancer 45(7):1146–1152. doi:10.1016/j.ejca.2008.11.013
Chu W, Staruch R, Pichardo S, Huang Y, Mougenot C, Tillander M, Köhler M, Ylihautala M, McGuffin M, Czarnota G, Hynynen K (2016) MR-HIFU mild hyperthermia for locally recurrent rectal cancer: temperature mapping and heating quality in first patient. In: 12th International congress of hyperthermic oncology (ICHO 2016), New Orleans, LA, 11–15 April 2016, p 144
Clark NA, Mumford SL, Segars JH (2014) Reproductive impact of MRI-guided focused ultrasound surgery for fibroids: a systematic review of the evidence. Curr Opin Obstet Gynecol 26(3):151–161. doi:10.1097/GCO.0000000000000070
Cleeland CS, Ryan KM (1994) Pain assessment: global use of the brief pain inventory. Ann Acad Med Singapore 23(2):129–138
Clement GT, Hynynen K (2002) A non-invasive method for focusing ultrasound through the human skull. Phys Med Biol 47(8):1219–1236. doi:10.1088/0031-9155/47/8/301
Clement GT, Sun J, Giesecke T, Hynynen K (2000) A hemisphere array for non-invasive ultrasound brain therapy and surgery. Phys Med Biol 45(12):3707–3719. doi:10.1088/0031-9155/45/12/314
Cochran MC, Eisenbrey JR, Soulen MC, Schultz SM, Ouma RO, White SB, Furth EE, Wheatley MA (2011) Disposition of ultrasound sensitive polymeric drug carrier in a rat hepatocellular carcinoma model. Acad Radiol 18(11):1341–1348. doi:10.1016/j.acra.2011.06.013
Coluccia D, Fandino J, Schwyzer L, O’Gorman R, Remonda L, Anon J, Martin E, Werner B (2014) First noninvasive thermal ablation of a brain tumor with MR-guided focused ultrasound. J Ther Ultrasound 2:17. doi:10.1186/2050-5736-2-17
Copelan A, Hartman J, Chehab M, Venkatesan AM (2015) High-Intensity focused ultrasound: current status for image-guided therapy. Semin Intervent Radiol 32(4):398–415. doi:10.1055/s-0035-1564793
Costelloe CM, Chuang HH, Madewell JE, Ueno NT (2010) Cancer response criteria and bone metastases: RECIST 1.1, MDA and PERCIST. J Cancer 1:80–92
Courivaud F, Kazaryan AM, Lund A, Orszagh VC, Svindland A, Marangos IP, Halvorsen PS, Jebsen P, Fosse E, Hol PK, Edwin B (2014) Thermal fixation of swine liver tissue after magnetic resonance-guided high-intensity focused ultrasound ablation. Ultrasound Med Biol 40(7):1564–1577. doi:10.1016/j.ultrasmedbio.2014.02.007
Dahl O (1995) Interaction of heat and drugs in vitro and in vivo. In: Seegenschmiedt MH, Fessenden P, Vernon CC (eds) Thermoradiotherapy and thermochemotherapy: volume 1, biology, physiology and physics. Springer-Verlag, Berlin, pp 103–121
De Haas-Kock DFM, Buijsen J, Pijls-Johannesma M, Lutgens L, Lammering G, van Mastrigt GAPG, De Ruysscher DKM, Lambin P, van der Zee J (2009) Concomitant hyperthermia and radiation therapy for treating locally advanced rectal cancer. Cochrane Database Syst Rev (3):CD006269. doi:10.1002/14651858.CD006269.pub2
De Smet M, Hijnen NM, Langereis S, Elevelt A, Heijman E, Dubois L, Lambin P, Grull H (2013) Magnetic resonance guided high-intensity focused ultrasound mediated hyperthermia improves the intratumoral distribution of temperature-sensitive liposomal doxorubicin. Invest Radiol 48(6):395–405. doi:10.1097/RLI.0b013e3182806940
Dewhirst MW, Vujaskovic Z, Jones E, Thrall D (2005) Re-setting the biologic rationale for thermal therapy. Int J Hyperthermia 21(8):779–790. doi:10.1080/02656730500271668
Dewhirst MW, Das SK, Stauffer PR, Craciunescu OA, Vujaskovic Z, Thrall D (2012) Hyperthermia. In: Gunderson LL, Tepper JE (eds) Clinical radiation oncology, 3rd edn. Elsevier, Philladelphia, pp 385–403
Diaz RJ, McVeigh PZ, O’Reilly MA, Burrell K, Bebenek M, Smith C, Etame AB, Zadeh G, Hynynen K, Wilson BC, Rutka JT (2014) Focused ultrasound delivery of Raman nanoparticles across the blood-brain barrier: potential for targeting experimental brain tumors. Nanomedicine 10(5):1075–1087. doi:10.1016/j.nano.2013.12.006
Dick EA, Gedroyc WM (2010) ExAblate magnetic resonance-guided focused ultrasound system in multiple body applications. Expert Rev Med Devices 7(5):589–597. doi:10.1586/erd.10.38
Diederich CJ, Hynynen K (1999) Ultrasound technology for hyperthermia. Ultrasound Med Biol 25(6):871–887. doi:10.1016/S0301-5629(99)00048-4
Eisenbrey JR, Burstein OM, Kambhampati R, Forsberg F, Liu JB, Wheatley MA (2010) Development and optimization of a doxorubicin loaded poly(lactic acid) contrast agent for ultrasound directed drug delivery. J Control Release 143(1):38–44. doi:10.1016/j.jconrel.2009.12.021
Eisenbrey JR, Albala L, Kramer MR, Daroshefski N, Brown D, Liu JB, Stanczak M, O’Kane P, Forsberg F, Wheatley MA (2015) Development of an ultrasound sensitive oxygen carrier for oxygen delivery to hypoxic tissue. Int J Pharm 478(1):361–367. doi:10.1016/j.ijpharm.2014.11.023
Escoffre JM, Novell A, de Smet M, Bouakaz A (2013) Focused ultrasound mediated drug delivery from temperature-sensitive liposomes: in-vitro characterization and validation. Phys Med Biol 58(22):8135–8151. doi:10.1088/0031-9155/58/22/8135
Ewertsen C, Saftoiu A, Gruionu LG, Karstrup S, Nielsen MB (2013) Real-time image fusion involving diagnostic ultrasound. AJR Am J Roentgenol 200(3):W249–W255. doi:10.2214/AJR.12.8904
Farny CH, Holt RG, Roy RA (2010) The correlation between bubble-enhanced HIFU heating and cavitation power. IEEE Trans Biomed Eng 57(1):175–184. doi:10.1109/Tbme.2009.2028133
Foley J, Kassell N, LeBlang S, Weber P, Snell JEM, Paeng DK (2015) Moore D workshop summary. In: Focused ultrasound for glioblastoma workshop, Charlottesville, VA, 9–10 Nov 2015. Focused Ultrasound Foundation, pp 4–6
Furusawa H, Namba K, Thomsen S, Akiyama F, Bendet A, Tanaka C, Yasuda Y, Nakahara H (2006) Magnetic resonance-guided focused ultrasound surgery of breast cancer: reliability and effectiveness. J Am Coll Surg 203(1):54–63. doi:10.1016/j.jamcollsurg.2006.04.002
Furusawa H, Namba K, Nakahara H, Tanaka C, Yasuda Y, Hirabara E, Imahariyama M, Komaki K (2007) The evolving non-surgical ablation of breast cancer: MR guided focused ultrasound (MRgFUS). Breast Cancer 14(1):55–58. doi:10.2325/jbcs.14.55
Furusawa H, Shidooka J, Inomata M, Hirabara E, Nakahara H, Ymaguchi Y (2015) MRgFUS of small breast cancer: what should be learned from a case of local recurrence. J Ther Ultrasound 3(Suppl 1):O75–O75. doi:10.1186/2050-5736-3-S1-O75
Ghai S, Louis AS, Van Vliet M, Lindner U, Haider MA, Hlasny E, Spensieri P, Van Der Kwast TH, McCluskey SA, Kucharczyk W, Trachtenberg J (2015) Real-time MRI-guided focused ultrasound for focal therapy of locally confined low-risk prostate cancer: feasibility and preliminary outcomes. AJR Am J Roentgenol 205(2):W177–W184. doi:10.2214/AJR.14.13098
Ghanouni P, Pauly KB, Bitton R, Avedian R, Bucknor M, Gold G (2015) MR guided focused ultrasound treatment of soft tissue tumors of the extremities—preliminary experience. J Ther Ultrasound 3(Suppl 1):O69–O69. doi:10.1186/2050-5736-3-S1-O69
Ghanouni P, Dobrotwir A, Bazzocchi A, Bucknor M, Bitton R, Rosenberg J, Telischak K, Busacca M, Ferrari S, Albisinni U, Walters S, Gold G, Ganjoo K, Napoli A, Pauly KB, Avedian R (2016) Magnetic resonance-guided focused ultrasound treatment of extra-abdominal desmoid tumors: a retrospective multicenter study. Eur Radiol In press. doi:10.1007/s00330-016-4376-5
Gianfelice D, Khiat A, Amara M, Belblidia A, Boulanger Y (2003a) MR imaging-guided focused US ablation of breast cancer: histopathologic assessment of effectiveness—initial experience. Radiology 227(3):849–855. doi:10.1148/radiol.2281012163
Gianfelice D, Khiat A, Amara M, Belblidia A, Boulanger Y (2003b) MR imaging-guided focused ultrasound surgery of breast cancer: correlation of dynamic contrast-enhanced MRI with histopathologic findings. Breast Cancer Res Treat 82(2):93–101. doi:10.1023/B:BREA.0000003956.11376.5b
Gianfelice D, Khiat A, Boulanger Y, Amara M, Belblidia A (2003c) Feasibility of magnetic resonance imaging-guided focused ultrasound surgery as an adjunct to tamoxifen therapy in high-risk surgical patients with breast carcinoma. J Vasc Interv Radiol 14(10):1275–1282. doi:10.1097/01.RVL.0000092900.73329.A2
Gianfelice D, Gupta C, Kucharczyk W, Bret P, Havill D, Clemons M (2008) Palliative treatment of painful bone metastases with MR imaging-guided focused ultrasound. Radiology 249(1):355–363. doi:10.1148/radiol.2491071523
Goertz DE (2015) An overview of the influence of therapeutic ultrasound exposures on the vasculature: high intensity ultrasound and microbubble-mediated bioeffects. Int J Hyperth 31(2):134–144. doi:10.3109/02656736.2015.1009179
Gu J, Wang H, Tang N, Hua Y, Yang H, Qiu Y, Ge R, Zhou Y, Wang W, Zhang G (2015) Magnetic resonance guided focused ultrasound surgery for pain palliation of bone metastases: early experience of clinical application in China. Zhonghua Yi Xue Za Zhi 95(41):3328–3332
Hahn GM (1979) Potential for therapy of drugs and hyperthermia. Cancer Res 39:2264–2268
Hall EJ, Giaccia AJ (2006) Radiobiology for the radiologist, 6th edn. Lippincott Williams & Wilkins, Philadelphia
Hectors SJ, Jacobs I, Moonen CT, Strijkers GJ, Nicolay K (2016) MRI methods for the evaluation of high intensity focused ultrasound tumor treatment: current status and future needs. Magn Reson Med 75(1):302–317. doi:10.1002/mrm.25758
Holbrook AB, Ghanouni P, Santos JM, Dumoulin C, Medan Y, Pauly KB (2014) Respiration based steering for high intensity focused ultrasound liver ablation. Magn Reson Med 71(2):797–806. doi:10.1002/mrm.24695
Huber PE, Jenne JW, Rastert R, Simiantonakis I, Sinn HP, Strittmatter HJ, von Fournier D, Wannenmacher MF, Debus J (2001) A new noninvasive approach in breast cancer therapy using magnetic resonance imaging-guided focused ultrasound surgery. Cancer Res 61(23):8441–8447
Huisman M, Lam MK, Bartels LW, Nijenhuis RJ, Moonen CT, Knuttel FM, Verkooijen HM, van Vulpen M, van den Bosch MA (2014) Feasibility of volumetric MRI-guided high intensity focused ultrasound (MR-HIFU) for painful bone metastases. J Ther Ultrasound 2:16. doi:10.1186/2050-5736-2-16
Hurwitz M, Stauffer P (2014) Hyperthermia, radiation and chemotherapy: the role of heat in multidisciplinary cancer care. Semin Oncol 41(6):714–729. doi:10.1053/j.seminoncol.2014.09.014
Hurwitz MD, Ghanouni P, Kanaev SV, Iozeffi D, Gianfelice D, Fennessy FM, Kuten A, Meyer JE, LeBlang SD, Roberts A, Choi J, Larner JM, Napoli A, Turkevich VG, Inbar Y, Tempany CM, Pfeffer RM (2014) Magnetic resonance-guided focused ultrasound for patients with painful bone metastases: phase III trial results. J Natl Cancer Inst 106 (5). doi:10.1093/jnci/dju082
Hynynen K (1990) Biophysics and technology of ultrasound hyperthermia. In: Gautherie M (ed) Methods of external hyperthermia heating. Clinical thermology, subseries thermotherapy. Springer, Berlin, Heidelberg, pp 61–115
Hynynen K (2010) MRI-guided focused ultrasound treatments. Ultra 50(2):221–229. doi:10.1016/j.ultras.2009.08.015
Hynynen K, Jolesz FA (1998) Demonstration of potential noninvasive ultrasound brain therapy through an intact skull. Ultrasound Med Biol 24(2):275–283. doi:10.1016/S0301-5629(97)00269-X
Hynynen K, McDannold N (2004) MRI guided and monitored focused ultrasound thermal ablation methods: a review of progress. Int J Hyperthermia 20(7):725–737. doi:10.1080/02656730410001716597
Hynynen K, McDannold N, Mulkern RV, Jolesz FA (2000) Temperature monitoring in fat with MRI. Magn Reson Med 43(6):901–904. doi:10.1002/1522-2594(200006)43:6<901:AID-MRM18>3.0.CO;2-A
Illing RO, Kennedy JE, Wu F, ter Haar GR, Protheroe AS, Friend PJ, Gleeson FV, Cranston DW, Phillips RR, Middleton MR (2005) The safety and feasibility of extracorporeal high-intensity focused ultrasound (HIFU) for the treatment of liver and kidney tumours in a Western population. Br J Cancer 93(8):890–895. doi:10.1038/sj.bjc.6602803
Ishihara Y, Calderon A, Watanabe H, Okamoto K, Suzuki Y, Kuroda K, Suzuki Y (1995) A precise and fast temperature mapping using water proton chemical shift. Magn Reson Med 34(6):814–823. doi:10.1002/mrm.1910340606
Joo B, Park MS, Lee SH, Choi HJ, Lim ST, Rha SY, Rachmilevitch I, Lee YH, Suh JS (2015) Pain palliation in patients with bone metastases using magnetic resonance-guided focused ultrasound with conformal bone system: a preliminary report. Yonsei Med J 56(2):503–509. doi:10.3349/ymj.2015.56.2.503
Jun-Qun Z, Guo-Min W, Bo Y, Gong-Xian W, Shen-Xu H (2004) Short-term results of 89 cases of rectal carcinoma treated with high-intensity focused ultrasound and low-dose radiotherapy. Ultrasound Med Biol 30(1):57–60. doi:10.1016/j.ultrasmedbio.2003.08.014
Kang TW, Rhim H (2015) Recent advances in tumor ablation for hepatocellular carcinoma. Liver Cancer 4(3):176–187. doi:10.1159/000367740
Karakitsios I, Mihcin S, Saliev T, Melzer A (2016) Feasibility study of pre-clinical thiel embalmed human cadaver for MR-guided focused ultrasound of the spine. Minim Invasive Ther Allied Technol 25(3):154–161. doi:10.3109/13645706.2016.1150297
Khiat A, Gianfelice D, Amara M, Boulanger Y (2006) Influence of post-treatment delay on the evaluation of the response to focused ultrasound surgery of breast cancer by dynamic contrast enhanced MRI. Br J Radiol 79(940):308–314. doi:10.1259/bjr/23046051
Kim YS (2015) Advances in MR image-guided high-intensity focused ultrasound therapy. Int J Hyperth 31(3):225–232. doi:10.3109/02656736.2014.976773
Kobus T, McDannold N (2015) Update on clinical magnetic resonance-guided focused ultrasound applications. Magn Reson Imaging Clin N Am 23(4):657–667. doi:10.1016/j.mric.2015.05.013
Kong G, Anyarambhatla G, Petros WP, Braun RD, Colvin OM, Needham D, Dewhirst MW (2000) Efficacy of liposomes and hyperthermia in a human tumor xenograft model: importance of triggered drug release. Cancer Res 60(24):6950–6957
Kopechek JA, Park EJ, Zhang YZ, Vykhodtseva NI, McDannold NJ, Porter TM (2014) Cavitation-enhanced MR-guided focused ultrasound ablation of rabbit tumors in vivo using phase shift nanoemulsions. Phys Med Biol 59(13):3465–3481. doi:10.1088/0031-9155/59/13/3465
Kopelman D, Inbar Y, Hanannel A, Freundlich D, Castel D, Perel A, Greenfeld A, Salamon T, Sareli M, Valeanu A, Papa M (2006) Magnetic resonance-guided focused ultrasound surgery (MRgFUS): ablation of liver tissue in a porcine model. Eur J Radiol 59(2):157–162. doi:10.1016/j.ejrad.2006.04.008
Laetsch T, Staruch R, Koral K, Chopra R (2016) Prospective imaging study of magnetic resonance thermometry quality in pediatric solid tumors. In: 12th international congress of hyperthermic oncology (ICHO 2016), New Orleans, LA, 11–15 April 2016, p 144
Lee ER (1995) Electromagnetic superficial heating technology. In: Seegenschmiedt MH, Fessenden P, Vernon CC (eds) Thermoradiotherapy and thermochemotherapy, vol 1, chapter 10. Springer, Berlin, Heidelberg, pp 193–217
Lee MW, Kim YJ, Park HS, Yu NC, Jung SI, Ko SY, Jeon HJ (2010) Targeted sonography for small hepatocellular carcinoma discovered by CT or MRI: factors affecting sonographic detection. AJR Am J Roentgenol 194(5):W396–W400. doi:10.2214/AJR.09.3171
Lee J, Farha G, Poon I, Karam I, Higgins K, Pichardo S, Hynynen K, Enepekides D (2016) Magnetic resonance-guided high-intensity focused ultrasound combined with radiotherapy for palliation of head and neck cancer-a pilot study. J Ther Ultrasound 4:12. doi:10.1186/s40349-016-0055-x
Leslie TA, Kennedy JE, Illing RO, Ter Haar GR, Wu F, Phillips RR, Friend PJ, Roberts IS, Cranston DW, Middleton MR (2008) High-intensity focused ultrasound ablation of liver tumours: can radiological assessment predict the histological response? Br J Radiol 81(967):564–571. doi:10.1259/bjr/27118953
Lesser TG, Schubert H, Gullmar D, Reichenbach JR, Wolfram F (2016) One-lung flooding reduces the ipsilateral diaphragm motion during mechanical ventilation. Eur J Med Res 21(1):9. doi:10.1186/s40001-016-0205-1
Liberman B, Gianfelice D, Inbar Y, Beck A, Rabin T, Shabshin N, Chander G, Hengst S, Pfeffer R, Chechick A, Hanannel A, Dogadkin O, Catane R (2009) Pain palliation in patients with bone metastases using MR-guided focused ultrasound surgery: a multicenter study. Ann Surg Oncol 16(1):140–146. doi:10.1245/s10434-008-0011-2
Lin SM (2009) Recent advances in radiofrequency ablation in the treatment of hepatocellular carcinoma and metastatic liver cancers. Chang Gung Med J 32(1):22–32
Lindner U, Ghai S, Spensieri P, Hlasny E, Van Der Kwast TH, McCluskey SA, Haider MA, Kucharczyk W, Trachtenberg J (2012) Focal magnetic resonance guided focused ultrasound for prostate cancer: initial North American experience. Can Urol Assoc J 6(6):E283–E286. doi:10.5489/cuaj.12218
Lipsman N, Mainprize TG, Schwartz ML, Hynynen K, Lozano AM (2014) Intracranial applications of magnetic resonance-guided focused ultrasound. Neurother: J Am Soc Exp NeuroTher 11(3):593–605. doi:10.1007/s13311-014-0281-2
Liu HL, Yang HW, Hua MY, Wei KC (2012) Enhanced therapeutic agent delivery through magnetic resonance imaging-monitored focused ultrasound blood-brain barrier disruption for brain tumor treatment: an overview of the current preclinical status. Neurosurg Focus 32(1). doi:10.3171/2011.10.Focus11238
Machtinger R, Inbar Y, Ben-Baruch G, Korach J, Rabinovici J (2008) MRgFUS for pain relief as palliative treatment in recurrent cervical carcinoma: a case report. Gynecol Oncol 108(1):241–243. doi:10.1016/j.ygyno.2007.08.079
Marquet F, Tung YS, Teichert T, Ferrera VP, Konofagou EE (2011) Noninvasive, transient and selective blood-brain barrier opening in non-human primates in vivo. PLoS ONE 6(7):e22598. doi:10.1371/journal.pone.0022598
McDannold NJ, Jolesz FA (2000) Magnetic resonance image-guided thermal ablations. Top Magn Reson Imaging 11(3):191–202. doi:10.1097/00002142-200006000-00005
McDannold N, Clement GT, Black P, Jolesz F, Hynynen K (2010) Transcranial magnetic resonance imaging- guided focused ultrasound surgery of brain tumors: initial findings in 3 patients. Neurosurgery 66(2):323–332; discussion 332. doi:10.1227/01.NEU.0000360379.95800.2F
Melodelima D, Salomir R, Chapelon JY, Theillere Y, Moonen C, Cathignol D (2005) Intraluminal high intensity ultrasound treatment in the esophagus under fast MR temperature mapping: in vivo studies. Magn Reson Med 54(4):975–982. doi:10.1002/mrm.20638
Merckel LG, Knuttel FM, Deckers R, van Dalen T, Schubert G, Peters NH, Weits T, van Diest PJ, Mali WP, Vaessen PH, van Gorp JM, Moonen CT, Bartels LW, van den Bosch MA (2016) First clinical experience with a dedicated MRI-guided high-intensity focused ultrasound system for breast cancer ablation. Eur Radiol In Press. doi:10.1007/s00330-016-4222-9
Meyer J, Pfeffer R, Kanaev S, Iozeffi D, Gianfelice D, Ghanouni P, Militianu D, Hurwitz M (2014) MR-guided focused ultrasound for painful bone metastases: safety when combined with chemotherapy. In: 4th International focused ultrasound symposium, Bethesda, 12–16 Oct 2014. pp 50–BM
Monzon L, Wasan H, Leen E, Ahmed H, Dawson PM, Harvey C, Muhamed A, Hand J, Price P, Abel PD (2011) Transrectal high-intensity focused ultrasonography is feasible as a new therapeutic option for advanced recurrent rectal cancer: report on the first case worldwide. Ann R Coll Surg Engl 93(6):e119–e121. doi:10.1308/147870811X592458
Nance E, Timbie K, Miller GW, Song J, Louttit C, Klibanov AL, Shih TY, Swaminathan G, Tamargo RJ, Woodworth GF, Hanes J, Price RJ (2014) Non-invasive delivery of stealth, brain-penetrating nanoparticles across the blood—brain barrier using MRI-guided focused ultrasound. J Control Release 189:123–132. doi:10.1016/j.jconrel.2014.06.031
Napoli A, Anzidei M, Marincola BC, Brachetti G, Ciolina F, Cartocci G, Marsecano C, Zaccagna F, Marchetti L, Cortesi E, Catalano C (2013a) Primary pain palliation and local tumor control in bone metastases treated with magnetic resonance-guided focused ultrasound. Invest Radiol 48(6):351–358. doi:10.1097/RLI.0b013e318285bbab
Napoli A, Anzidei M, Ciolina F, Marotta E, Cavallo Marincola B, Brachetti G, Di Mare L, Cartocci G, Boni F, Noce V, Bertaccini L, Catalano C (2013b) MR-guided high-intensity focused ultrasound: current status of an emerging technology. Cardiovasc Intervent Radiol 36(5):1190–1203. doi:10.1007/s00270-013-0592-4
Napoli A, Anzidei M, De Nunzio C, Cartocci G, Panebianco V, De Dominicis C, Catalano C, Petrucci F, Leonardo C (2013c) Real-time magnetic resonance-guided high-intensity focused ultrasound focal therapy for localised prostate cancer: preliminary experience. Eur Urol 63(2):395–398. doi:10.1016/j.eururo.2012.11.002
Ng KK, Poon RT, Chan SC, Chok KS, Cheung TT, Tung H, Chu F, Tso WK, Yu WC, Lo CM, Fan ST (2011) High-intensity focused ultrasound for hepatocellular carcinoma: a single-center experience. Ann Surg 253(5):981–987. doi:10.1097/SLA.0b013e3182128a8b
Odeen H, de Bever J, Almquist S, Farrer A, Todd N, Payne A, Snell JW, Christensen DA, Parker DL (2014) Treatment envelope evaluation in transcranial magnetic resonance-guided focused ultrasound utilizing 3D MR thermometry. J Ther Ultrasound 2:19. doi:10.1186/2050-5736-2-19
Okada A, Murakami T, Mikami K, Onishi H, Tanigawa N, Marukawa T, Nakamura H (2006) A case of hepatocellular carcinoma treated by MR-guided focused ultrasound ablation with respiratory gating. Magn Reson Med Sci 5(3):167–171. doi:10.2463/mrms.5.167
Pardridge WM (2005) The blood-brain barrier: bottleneck in brain drug development. NeuroRx 2(1):3–14. doi:10.1602/neurorx.2.1.3
Park MJ, Kim YS, Yang J, Sun WC, Park H, Chae SY, Namgung MS, Choi KS (2013) Pulsed high-intensity focused ultrasound therapy enhances targeted delivery of cetuximab to colon cancer xenograft model in mice. Ultrasound Med Biol 39(2):292–299. doi:10.1016/j.ultrasmedbio.2012.10.008
Pernot M, Aubry JF, Tanter M, Thomas JL, Fink M (2003) High power transcranial beam steering for ultrasonic brain therapy. Phys Med Biol 48(16):2577–2589. doi:10.1088/0031-9155/48/16/301
Petrusca L, Cattin P, De Luca V, Preiswerk F, Celicanin Z, Auboiroux V, Viallon M, Arnold P, Santini F, Terraz S, Scheffler K, Becker CD, Salomir R (2013) Hybrid ultrasound/magnetic resonance simultaneous acquisition and image fusion for motion monitoring in the upper abdomen. Invest Radiol 48(5):333–340. doi:10.1097/RLI.0b013e31828236c3
Ponce AM, Vujaskovic Z, Yuan F, Needham D, Dewhirst MW (2006) Hyperthermia mediated liposomal drug delivery. Int J Hyperth 22(3):205–213. doi:10.1080/02656730600582956
Quesson B, Merle M, Kohler MO, Mougenot C, Roujol S, de Senneville BD, Moonen CT (2010) A method for MRI guidance of intercostal high intensity focused ultrasound ablation in the liver. Med Phys 37(6):2533–2540. doi:10.1118/1.3413996
Quesson B, Laurent C, Maclair G, de Senneville BD, Mougenot C, Ries M, Carteret T, Rullier A, Moonen CT (2011) Real-time volumetric MRI thermometry of focused ultrasound ablation in vivo: a feasibility study in pig liver and kidney. NMR Biomed 24(2):145–153. doi:10.1002/nbm.1563
Ram Z, Cohen ZR, Harnof S, Tal S, Faibel M, Nass D, Maier SE, Hadani M, Mardor Y (2006) Magnetic resonance imaging-guided, high-intensity focused ultrasound for brain tumor therapy. Neurosurgery 59(5):949–955; discussion 955–946. doi:10.1227/01.NEU.0000254439.02736.D8
Rapoport N, Payne A, Dillon C, Shea J, Scaife C, Gupta R (2013) Focused ultrasound-mediated drug delivery to pancreatic cancer in a mouse model. J Ther Ultrasound 1:11. doi:10.1186/2050-5736-1-11
Rodrigues DB, Stauffer PR, Vrba D, Hurwitz MD (2015) Focused ultrasound for treatment of bone tumours. Int J Hyperth 31(3):260–271. doi:10.3109/02656736.2015.1006690
Rosenthal D, Callstrom MR (2012) Critical review and state of the art in interventional oncology: benign and metastatic disease involving bone. Radiology 262(3):765–780. doi:10.1148/radiol.11101384
Saeed M, Krug R, Do L, Hetts SW, Wilson MW (2016) Renal ablation using magnetic resonance-guided high intensity focused ultrasound: Magnetic resonance imaging and histopathology assessment. World J Radiol 8(3):298–307. doi:10.4329/wjr.v8.i3.298
Sazgarnia A, Shanei A, Taheri AR, Meibodi NT, Eshghi H, Attaran N, Shanei MM (2013) Therapeutic effects of acoustic cavitation in the presence of gold nanoparticles on a colon tumor model. J Ultrasound Med 32(3):475–483
Schlesinger D, Benedict S, Diederich C, Gedroyc W, Klibanov A, Larner J (2013) MR-guided focused ultrasound surgery, present and future. Med Phys 40(8):080901. doi:10.1118/1.4811136
Siddiqui K, Chopra R, Vedula S, Sugar L, Haider M, Boyes A, Musquera M, Bronskill M, Klotz L (2010) MRI-guided transurethral ultrasound therapy of the prostate gland using real-time thermal mapping: initial studies. Urology 76(6):1506–1511. doi:10.1016/j.urology.2010.04.046
Sneed PK, Stauffer PR, Li G, Sun X, Myerson R (2010) Hyperthermia. In: Phillips T, Hoppe R, Roach M (eds) Textbook of radiation oncology, 3rd edn. Elsevier, Philadelphia, pp 1564–1593
Stauffer PR (2005) Evolving technology for thermal therapy of cancer. Int J Hyperth 21(8):731–744. doi:10.1080/02656730500331868
Sun J, Hynynen K (1998) Focusing of therapeutic ultrasound through a human skull: a numerical study. J Acoust Soc Am 104(3 Pt 1):1705–1715. doi:10.1121/1.424383
Sun J, Hynynen K (1999) The potential of transskull ultrasound therapy and surgery using the maximum available skull surface area. J Acoust Soc Am 105(4):2519–2527. doi:10.1121/1.426863
Teraphongphom N (2016) Theranostic nanoparticle and drug loaded contrast agents and their biomedical applications. PhD thesis, Drexel University, Philadelphia
Teraphongphom N, Chhour P, Eisenbrey JR, Naha PC, Witschey WRT, Opasanont B, Jablonowski L, Cormode DP, Wheatley MA (2015) Nanoparticle loaded polymeric microbubbles as contrast agents for multimodal imaging. Langmuir 31(43):11858–11867. doi:10.1021/acs.langmuir.5b03473
Tokuda J, Morikawa S, Haque HA, Tsukamoto T, Matsumiya K, Liao H, Masamune K, Dohi T (2008) Adaptive 4D MR imaging using navigator-based respiratory signal for MRI-guided therapy. Magn Reson Med 59(5):1051–1061. doi:10.1002/mrm.21436
Toraya-Brown S, Fiering S (2014) Local tumour hyperthermia as immunotherapy for metastatic cancer. Int J Hyperth 30(8):531–539. doi:10.3109/02656736.2014.968640
Tung YS, Vlachos F, Feshitan JA, Borden MA, Konofagou EE (2011) The mechanism of interaction between focused ultrasound and microbubbles in blood-brain barrier opening in mice. J Acoust Soc Am 130(5):3059–3067. doi:10.1121/1.3646905
Van Rhoon GC (2013) External electromagnetic methods and devices. In: Moros EG (ed) Physics of thermal therapy: fundamentals and clincial applications. Taylor and Francis, Boca Ratan, pp 139–158
Vidal-Jove J, Eres N, Perich E, Jaen A, del Castillo MA (2016) Interventional oncology: role of focused ultrasound (USgHIFU) in pancreatic cancer. Five years experience and tumor ablation considerations in the Western stage. In: 12th International congress of hyperthermic oncology (ICHO 2016), New Orleans, LA, 11–15 April 2016. p 210
Vujaskovic Z, Poulson JM, Gaskin AA, Thrall DE, Page RL, Charles HC, MacFall JR, Brizel DM, Meyer RE, Prescott DM, Samulski TV, Dewhirst MW (2000) Temperature-dependent changes in physiologic parameters of spontaneous canine soft tissue sarcomas after combined radiotherapy and hyperthermia treatment. Int J Radiat Oncol Biol Phys 46(1):179–185. doi:10.1016/S0360-3016(99)00362-4
Weber-Adrian D, Thevenot E, O’Reilly MA, Oakden W, Akens MK, Ellens N, Markham-Coultes K, Burgess A, Finkelstein J, Yee AJM, Whyne CM, Foust KD, Kaspar BK, Stanisz GJ, Chopra R, Hynynen K, Aubert I (2015) Gene delivery to the spinal cord using MRI-guided focused ultrasound. Gene Ther 22(7):568–577. doi:10.1038/gt.2015.25
Wijlemans JW, de Greef M, Schubert G, Bartels LW, Moonen CT, van den Bosch MA, Ries M (2015) A clinically feasible treatment protocol for magnetic resonance-guided high-intensity focused ultrasound ablation in the liver. Invest Radiol 50(1):24–31. doi:10.1097/RLI.0000000000000091
Wolfram F, Boltze C, Schubert H, Bischoff S, Lesser TG (2014) Effect of lung flooding and high-intensity focused ultrasound on lung tumours: an experimental study in an ex vivo human cancer model and simulated in vivo tumours in pigs. Eur J Med Res 19:1. doi:10.1186/2047-783X-19-1
Woodrum DA, Kawashima A, Gorny KR, Mynderse LA (2015) Magnetic resonance-guided thermal therapy for localized and recurrent prostate cancer. Magn Reson Imaging Clin N Am 23(4):607–619. doi:10.1016/j.mric.2015.05.014
Wu F (2006) Extracorporeal high intensity focused ultrasound in the treatment of patients with solid malignancy. Minim Invasive Ther Allied Technol 15(1):26–35. doi:10.1080/13645700500470124
Wu F, Wang ZB, Chen WZ, Bai J, Zhu H, Qiao TY (2003) Preliminary experience using high intensity focused ultrasound for the treatment of patients with advanced stage renal malignancy. J Urol 170(6 Pt 1):2237–2240. doi:10.1097/01.ju.0000097123.34790.70
Wu F, Wang ZB, Chen WZ, Zhu H, Bai J, Zou JZ, Li KQ, Jin CB, Xie FL, Su HB (2004) Extracorporeal high intensity focused ultrasound ablation in the treatment of patients with large hepatocellular carcinoma. Ann Surg Oncol 11(12):1061–1069. doi:10.1245/ASO.2004.02.026
Xu Y, Choi J, Hylander B, Sen A, Evans SS, Kraybill WG, Repasky EA (2007) Fever-range whole body hyperthermia increases the number of perfused tumor blood vessels and therapeutic efficacy of liposomally encapsulated doxorubicin. Int J Hyperth 23(6):513–527. doi:10.1080/02656730701666112
Xu G, Luo G, He L, Li J, Shan H, Zhang R, Li Y, Gao X, Lin S, Wang G (2011) Follow-up of high-intensity focused ultrasound treatment for patients with hepatocellular carcinoma. Ultrasound Med Biol 37(12):1993–1999. doi:10.1016/j.ultrasmedbio.2011.08.011
Yuh B, Liu A, Beatty R, Jung A, Wong JY (2016) Focal therapy using magnetic resonance image-guided focused ultrasound in patients with localized prostate cancer. J Ther Ultrasound 4:8. doi:10.1186/s40349-016-0054-y
Zaccagna F, Giulia B, Bazzocchi A, Spinnato P, Albisinni U, Napoli A, Catalano C (2014) Palliative treatment of painful bone metastases with MR imaging–guided focused ultrasound surgery: a two-centre study. In: 4th international focused ultrasound symposium, Bethesda, 12–16 Oct 2014. pp 51–BM
Zachiu C, Papadakis N, Ries M, Moonen C, Denis de Senneville B (2015) An improved optical flow tracking technique for real-time MR-guided beam therapies in moving organs. Phys Med Biol 60(23):9003–9029. doi:10.1088/0031-9155/60/23/9003
Zagar TM, Vujaskovic Z, Formenti S, Rugo H, Muggia F, O’Connor B, Myerson R, Stauffer P, Hsu IC, Diederich C, Straube W, Boss MK, Boico A, Craciunescu O, Maccarini P, Needham D, Borys N, Blackwell KL, Dewhirst MW (2014) Two phase I dose-escalation/pharmacokinetics studies of low temperature liposomal doxorubicin (LTLD) and mild local hyperthermia in heavily pretreated patients with local regionally recurrent breast cancer. Int J Hyperth 30(5):285–294. doi:10.3109/02656736.2014.936049
Zhou YF (2011) High intensity focused ultrasound in clinical tumor ablation. World J Clin Oncol 2(1):8–27. doi:10.5306/wjco.v2.i1.8
Zhu X, Guo J, He C, Geng H, Yu G, Li J, Zheng H, Ji X, Yan F (2016) Ultrasound triggered image-guided drug delivery to inhibit vascular reconstruction via paclitaxel-loaded microbubbles. Sci Rep 6:21683. doi:10.1038/srep21683
Zippel DB, Papa MZ (2005) The use of MR imaging guided focused ultrasound in breast cancer patients; a preliminary phase one study and review. Breast Cancer 12(1):32–38. doi:10.2325/jbcs.12.32
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Rodrigues, D.B., Stauffer, P.R., Eisenbrey, J., Beckhoff, V., Hurwitz, M.D. (2017). Oncologic Applications of Magnetic Resonance Guided Focused Ultrasound. In: Wong, J., Schultheiss, T., Radany, E. (eds) Advances in Radiation Oncology. Cancer Treatment and Research. Springer, Cham. https://doi.org/10.1007/978-3-319-53235-6_4
Download citation
DOI: https://doi.org/10.1007/978-3-319-53235-6_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-53233-2
Online ISBN: 978-3-319-53235-6
eBook Packages: MedicineMedicine (R0)