Abstract
The weight is an important factor that influences the onset and progression of puberty. The overweight as well as the underweight could influence the development of puberty. Some previous studies suggest that there may be gender differences in development of puberty related to body weight. Most of the authors reported that the adiposity in early childhood appeared to be linked to advanced puberty in girls, but the results in the boys are controversial. In recent years, after the using of more accurate methods for determining the onset of puberty, such as measuring the testicular volume, it became clear that the boys with overweight and obesity start the onset of puberty earlier. Girls and boys with overweight grow faster and reach sexual maturity earlier than normal-weight children, while underweight lagging behind them at every stage of puberty. It is even necessary to reach a certain weight and the presence of an amount of fat to initiation of puberty.
The amount of fat in the body affects the function of the reproductive axis both in the onset of puberty and during its development. Adipose tissue plays a dynamic role in energy homeostasis by acting as an endocrine organ, because in it run very important processes involved in the metabolism of the individuals. In it is secreted a large number adipocytokines, the most important of which is leptin, that can influence sexual development. On the other hand, the impact of energy status on the reproductive axis is realized through a number of neuropeptides and metabolic signals. These neuropeptides have either direct or indirect effects on feeding and metabolism as well as on the secretion of gonadotropin-releasing hormone (GnRH). Some hormones, such as insulin, also have an important effect on the reproductive axis.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
In mammals, reproduction is acutely regulated by metabolic status [1]. The body weight is an important factor that influences on the initiation and progression of puberty . In the childhood the overweight as well as the underweight could influence the development of puberty. In recent years excessive food consumption and sedentary behavior in developed societies are the cause of overweight and obesity . The lower intake of food and increased physical activity induce unfavorable energy balance and underweight, which also may disturb the sexual function.
Globally, about 10 % of school-age children are obese or overweight, and this percentage is highest in the USA (32 %), followed by Europe (20 %) and the Middle East (16 %) [2]. The worldwide prevalence of childhood obesity increased from 4.2 to 6.7 % between 1990 and 2010 [3].
In the USA, the 85th and 95th percentiles of body mass index (BMI) for age and sex based on nationally representative survey data have been recommended as cutoff points to identify overweight and obesity, respectively, which are the same as those, proposed by the Expert Committee [4].
In most publications, the underweight is defined within different limits: 5th or 15th percentile of BMI for given age. According to World Health Organization’s cutoff points, BMI of 18.5 kg/m2 in young adults is equivalent to the 12th percentile in children [5].
Unfortunately, the data on children with underweight and its effect on sexual development are scarce. But underweight can negatively affect both the onset and progression of puberty, and also the reproductive capacity later in adulthood, especially in girls. The publications on this subject are mainly related to patients with anorexia nervosa .
Pubertal maturation consists of two associated processes: adrenarche, the increase of adrenal androgen production, and gonadarche, the pubertal reactivation of hypothalamic-pituitary-gonadal (HPG) axis. The development of breast tissue in girls (thelarche) and testicular growth in boys are signs of the onset of puberty. Typically, adrenarche occurs before gonadarche. Some authors believe that adrenal androgens may be one of the factors necessary for the reactivation of the hypothalamic-pituitary-gonadal axis [6].
The severity of the disturbances in sexual sphere depends on the degree of the variations in body weight as more severe deviations in body weight cause more prominent abnormalities in sexual function.
Body Weight and Puberty in Girls
The adiposity in early childhood is probably linked to advanced puberty in girls [7, 8]. It is generally accepted that overweight and obesity are related with early appearance of menarche [7, 9]. Multiple studies from several continents have demonstrated that levels of childhood obesity in girls are associated with earlier onset of puberty or menarche: in the USA [10–14], in South America [3], in Europe [15, 16], and in Asia [17]. Nevertheless there are some authors who suggested that the population-level shifts in BMI and the timing of menarche are largely independent processes, although sometimes they coincide [18].
Data from several epidemiological studies in the past 30 years present a link between the earlier onset of puberty in girls and increased BMI, which is the most available method for indirectly determining body fat stores [19]. Girls with greater BMI reach breast stage 2 at younger ages. Higher BMI is the strongest predictor of earlier age at breast stage 2 in the study of Biro et al. [14]. Pubertal signs occur before 8.0 years of age in <5 % of the normal BMI female population in the USA [20]. Breast and sexual pubic hair developments are premature before 8 years of age in girls with normal BMI in general population. Girls with excessive BMI have significantly higher prevalence of breast appearance from ages 8.0–9.6 years and pubarche from ages 8.0–10.2 years than those with normal BMI [20]. Menarche is also significantly more likely to occur in preteen girls with an elevated BMI [20]. A study in Denmark found that early-matured girls had higher BMI, but similar body fat percentage, compared with late-matured similarly aged girls [21]. Results of a study in Brazil indicate that early sexual maturation is associated with a higher prevalence of excessive body weight in girls . Compared to the reference group (normal sexual maturation), early-maturing females have higher prevalence of excess body weight and increased height for age [3]. Lee et al. found a strong association between elevated body weight at all ages and the early onset of puberty as determined by breast development and the onset of menstruation [13]. Fat mass at age 8 years is strongly associated with stage and onset of puberty in both sexes. However, by age 11 year, lean mass accretion is more closely associated with more advanced puberty [22]. Four-year longitudinal study in China demonstrated that childhood obesity contributes to an earlier onset of puberty, and the mean estradiol concentration is higher in obese girls in comparison to normal or underweight girls during this period [17].
The increased incidence of childhood obesity in recent decades may be responsible for dramatic increase in early puberty in girls. From the late nineteenth century, evidence from several European countries shows a decrease in the age of menarche—as a result of the earlier achievement of the required weight for the initiation of menarche [23]. The age of the onset of menses (menarche) declined in North America and Europe from age 17 years in the mid-nineteenth century to less than 14 years in the mid-twentieth century. In a study in Bulgaria, done by the beginning of twentieth century (1904–1906), the mean age of menarche was 15 years, while at the end of the century, it was 12 years [24]. Similar trends also occurred in the age of onset of breast development (thelarche) and pubic hair development (pubarche) [25]. Moreover, in recent years an inverse correlation of BMI was found with the age of onset of menarche [26, 27]. The nutrition in the postnatal period and rapid weight gain can predict the onset of earlier puberty [28, 29].
For the changes in reproductive axis in girls with underweight can be judged mainly on the studies done in adolescents with anorexia nervosa, where the considerable weight reduction causes delay in puberty or its discontinuation. This disease is associated with unfavorable changes in the reproductive axis—hypogonadotropic hypogonadism. The degree of weight loss is associated with the degree of hormonal disturbances in the gonadal axis. The basal levels of gonadotropins are lower, and the responses of luteinizing hormone (LH) to gonadotropin-releasing hormone (GnRH) are diminished, but those of follicle-stimulating hormone (FSH) are exaggerated. The basal levels of LH are significantly correlated with body weight, BMI, and percentage of weight loss [30]. The changes in the gonadal axis are due to disturbances in the hypothalamus, and all hormonal alterations are in relationship with the degree of weight loss . The severe weight loss is mainly associated with the reduced amount of adipose tissue and with considerably decreased leptin levels [31]. Several other hormones and mediators are implicated in this process and can send signals to the hypothalamus that influence on its activity.
Body Weight and Puberty in Boys
Data from studies on the influence of body weight (especially overweight and obesity) on the onset and development of the puberty in boys are controversial. In some studies male obesity was associated with delayed pubertal development [11, 32, 33], while in others earlier start of puberty in overweight boys was found [34, 35]. In a small study Laron has not observed any difference in pubertal development between boys with obesity and those with normal weight [8]. Some authors found that earlier sexual maturation in boys was associated with greater height for age [3, 36], but not with the weight. Others considered that in contrast to the girls, there was no evidence of an association between adiposity and pubarche in boys [20]. The analyses of National Health and Nutrition Examination Survey (NHANES) III data by Karpati et al. [37] and by Wang [11] suggested that overweight and obesity might result in delayed instead of advanced puberty in boys. However, these studies have some limitations as the authors evaluated the genital stages only visually, without measuring the testicular volumes and penis sizes. With these methods the data could be more difficult for interpretation, because of the subjective evaluation of early stages and subsequent physical progression through puberty. It is not possible to define exactly the pubertal events in boys without assessment of testicular volumes. Perhaps for this reason, the influence of body weight and BMI on sexual maturation in males has not been clarified for a long period of time.
A volume of 3 ml is considered the most reliable and valid marker of male pubertal onset generally accepted to date [38–40]. According to Tanner and Whitehouse [41], a mean testicular volume of 12 ml indicates that adolescent is proceeding toward the late stage of pubertal development.
Results from study of Tomova et al. [42], based on objective data obtained by determining testicular volume, found earlier enlargement of the testicular volume in overweight and obese boys as well as earlier pubertal maturation in comparison to normal-weight children. The increase in testicular volume begins initially in boys with obesity, but subsequently overweight children have the fastest pubertal development in comparison to these with obesity and those with normal weight. Delayed pubertal development was observed in underweight boys, who were clearly behind at every stage of puberty relative to the normal-weight children (Fig. 7.1). At the beginning of the puberty at the age of 11 years, the testicular volume of 3 ml has been found in 69.6 % of the boys with overweight and obesity, in 51.5 % of the boys with normal weight and only in 29.7 % in those who were underweight. The results concerning the late stage of puberty (testicular volume ≥12 ml) were similar. At the age 13 the percentage of the boys with overweight and obesity, who had testicular volume of 12 ml or more, was 43.5 %, whereas in the group of underweight children, it was only 2.70 %. An early increase of penis length as well as of penis circumference was found in overweight children, while a significant delay was observed in boys with underweight and obesity [42]. From this data it is clear that the boys with overweight and obesity start puberty development earlier and finished it faster in comparison to those who are underweight [42]. In all investigated groups, it has been established a positive significant correlation of the body weight and BMI with the indices of pubertal development: pubic hair, penis length, and circumference as well as with the volume of the testes. Moreover, according to this study, the onset of puberty is expected at a certain threshold of the body weight (40.17 ± 9.10 kg) (median 39.0 kg) [42].
Similar are the observations of Vizmanos and Martí-Henneberg [35] that reveal a positive relationship between BMI and the initiation of sexual development in boys as well as the findings of Juul et al. [43] of the association of prepubertal BMI with earlier age at voice break. The other study in Denmark found that early-matured boys had higher BMI, but similar body fat percentage, compared with late-matured similarly aged boys [21]. Boyne et al. reported that fat mass at age of 8 was strongly associated with the stage and onset of puberty in both sexes. Birth size and growth through infancy and childhood were significantly associated with testicular size. Pooling both sexes together, growth in infancy, late infancy, and childhood is associated with more advanced puberty [22]. Supportive evidence was found also by Fu et al. [44], who observed an earlier activation of the inhibin B/follicle-stimulating hormone axis in boys with obesity during puberty. These authors found significantly greater testicular volume as well as advanced bone age and increased values of dehydroepiandrosterone and dehydroepiandrosterone sulfate (DHEAS) in obese prepubertal boys compared to age-matched controls [44]. Sørensen at al. reported that the mean age at onset of male puberty has declined significantly during period of 15 years, and this decline was associated with the coincident increase in BMI [45]. All these data support the hypothesis for a close relationship between body weight and maturation of the boys .
Links Between Body Weight and Puberty Development
Overweight and Obesity
According to many studies, there are clear associations between childhood obesity and earlier onset of puberty and pubertal development in both sexes.
Puberty is initiated in the late childhood through a cascade of endocrine changes that lead to sexual maturation and reproductive capability [7, 46]. It begins with increasing of GnRH secretion from the hypothalamus, which gains rhythmic, pulsatile character and in turn leads to release of gonadotropins, activation of gonadal axis, and beginning of the puberty. The gonadotropins regulate both steroidogenesis and gametogenesis. The large variability between individuals in the onset and progression of puberty indicates that the timing of puberty is not simply a function of chronological age. The neurotransmitter and neuromodulatory systems that impact upon the GnRH secretory network convey information about metabolic fuels, energy stores, and somatic development [47].
Growth and development are extremely complex processes that are regulated from many humoral and neural factors acting on the genetic basis. The secretion of GnRH is under the control of the so-called hypothalamic pulse generator which is located in the nucleus arcuatus [48, 49]. The physiological mechanisms that trigger activation of the hypothalamic-pituitary gonadal axis are still unknown, but attainment of a set point in growth, body composition, and energy balance seems important [40]. A lot of neurotransmitters, adipocytokines, and hormones, such as leptin, kisspeptin, neuropeptide Y, insulin, and opioids, which control food intake, also have a link to the release of GnRH.
Despite many human and animal studies, it is still unclear how the GnRH pulse generator manages to provoke the onset of puberty in both sexes. However, there are clear evidences that a critical amount of fat during the childhood is necessary to provoke revival of hypothalamic secretory function. Alwis et al. [50] reported that bone mass, lean body, and fat mass, measured by dual-energy X-ray absorptiometry , increased at a constant rate from age 6 until the puberty, when all these indexes showed a rapid increase in both sexes. Total lean body mass increased with 21.2 % in the boys and with 18.4 % in the girls at age 6 to 8 years, while the total amount of fat mass enhanced with 34.5 % in the boys and with 28.6 % in the girls [50]. During the growth spurt at the age of 7 years in both sexes, the rate of fat tissue accumulation was found to be at least 10 % greater than that of the lean mass [50].
After the initiation of this process neurotransmitter systems, which stimulate (neuropeptide Y and noradrenaline) and inhibit (opioids) the gonadal axis, are involve in the control of the GnRH release. During this period gonadal steroids also influence these mechanisms. For the initiation of the puberty, it is necessary to gain a certain “critical” body weight, which is a limiting factor for further processes. The probable messenger between adipose tissue and the nervous system seems to be leptin. There are numerous examples of the relationship between eating behavior, leptin, and sexual maturation. In light of these data, the proposed hypothesis from Frisch and Revelle for “critical body weight ” in girls, according to which a certain minimum body weight or body fat percentage is required for appearance of menarche [51], acquires a completely modern vision.
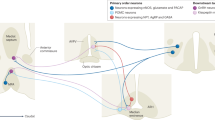
The hypothalamic nucleus arcuatus is a crucial site for the regulation of both reproduction and metabolism. The arcuate nucleus contains proopiomelanocortin/cocaine- and amphetamine-regulated transcript (POMC/CART)-expressing neurons , whose activation suppresses feeding. In contrast, the activation of another population of arcuate neurons, neuropeptide Y/agouti-related protein (NPY/AgRP)-expressing neurons , stimulates feeding [52, 53]. Although much of the cellular and molecular mechanisms associated with the energy balance and reproduction, as well as sites in the brain that mediate these functions are not completely understood, it is well known that the reproductive axis has the ability to respond to changes in the metabolic state of the body.
There are several potential mechanisms by which body fat stores might influence onset of pubertal development as well as the progression of puberty. One is through the direct action of adipocytokines, such as leptin, signaling energy reserves as well as having other direct metabolic effects. In addition, aromatase activity is pronounced in adipose tissue, which increases androgen conversion to estrogens. Adipose tissue is also related to insulin resistance, which increases during puberty, thus lowering sex hormone-binding globulin (SHBG) levels and hence increasing bioavailability of sex steroids [54].
Adipose tissue should be considered as an endocrine organ . A wide range of different active products are released from it into blood stream. Some of them are synthesized de novo, while others are converted from already existing substances. All factors might act locally in auto-/paracrine manner or may exert metabolic, immunologic, and endocrine effects [55]. Through them the link between adipose tissue and hypothalamic-pituitary system is realized, which modulates the function of other endocrine glands. Some of these adipocytokines are actively involved in the function of the reproductive axis.
Leptin , an adipocyte-secreted hormone, is a metabolic factor that bridges the regulation of the fat mass with reproduction [56]. Its levels are elevated in individuals with overweight and obesity and decreased in persons with underweight. Moreover, leptin concentrations correlate with amount of fat mass, and for the timing of puberty, certain levels of this hormone are required [19]. Matkovic et al. found an inverse relation between menarche and serum leptin. An increase of 1 ng/mL in serum leptin level lowers the timing of menarche by 1 month, and a gain in body fat of 1 kg is associated with an earlier onset of menarche by approximately 13 days [57]. Sex differences are also observed in the concentrations of leptin , LH, and FSH before and during the puberty. In girls, a peak in leptin concentrations was observed at Tanner stage 2, followed by a peak in LH and FSH concentrations at Tanner stage 3. In boys, no peak in leptin levels was observed at Tanner stage 2, as leptin decreased from Tanner stage 2 onward and LH and FSH concentrations increased from Tanner stage 1–4 [58]. In girls leptin levels rise during the age, according to the changes in body weight, and this trend is maintained with age. In boys leptin concentrations are as a rule lower than in girls, but the pattern of gradual increase at an early age is similar. After 10 years of age, leptin levels decrease, and this could be coupled with a concomitant increase of testosterone [48, 59]. Testosterone inhibits differentiation of preadipocytes into mature adipocytes [60]. The net result of these androgen actions at multiple sites in the adipogenic processes is a reduction in fat mass [60]. Testosterone stimulates the weight gain through increased muscle mass but reduces the percentage of body fat, resulting in decrease levels of leptin. It is possible that in boys after the initial onset of puberty, this hormone is not more needed for the pubertal development. In girls, however, it is necessary that a certain threshold level of leptin to be maintained. Perhaps leptin signals the presence of a sufficient amount of adipose tissue, i.e., energy resources, that is necessary for the normal reproductive function [59]. In that regard, leptin may be a factor which allows the start of puberty. This thesis is supported by the fact that leptin is increased years before any other hormone associated with pubertal development [58].
The administration of leptin stimulates the growth of cells from cartilaginous tissue, which can result in epiphyseal cartilage growth in long bones [3]. Fat mass is an important determinant of bone density, and leptin acts directly on bone, influencing both osteoblasts and osteoclasts. The direct bone effects of leptin tend to reduce bone fragility and contribute to the high bone mass and low fracture rates of obesity [61]. Peripheral leptin is essential for normal bone resorption and enhances bone formation. The results indicate that leptin acting primarily through peripheral pathways increases osteoblast number and activity in mice [62].
The absence of signaling-competent leptin receptor expression on GnRH neurons strongly suggests that intermediary factor or pathway mediates the essential effects of leptin on activation of GnRH neurons [56]. The kisspeptin appears to play a role in reproductive effects of leptin. Kisspeptin stimulates the secretion of LH, after binding with the receptor GPR 54, which is located on the surface of the GnRH neurons. Inactivating gene mutations are associated with hypogonadotropic hypogonadism. In such patients, puberty does not occur. It is assumed that the system kisspeptin-GPR 54 is absolutely necessary to the activation of gonadotropin secretion in early sexual maturation and maintenance of reproductive function in adults [63–65]. It is believed that leptin stimulates expression of kisspeptin 1 (KISS-1) and thereby initiates the production of kisspeptin and subsequently stimulation of GnRH release [53]. Thus, the increased levels of leptin in obese and overweight children can be the cause of an earlier puberty start. Some authors consider that leptin serves as a metabolic signal for puberty to progress and appears to be a permissive factor rather than the trigger of the onset of puberty [66].
Discovered in 1999 galanin-like peptide (GALP) shows close structural similarity with galanin and specifically stimulates GnRH-mediated LH secretion. GALP-expressing cells are mainly found in the arcuate nucleus of the hypothalamus and the posterior pituitary, where they appear to be in contact with multiple neuromodulators, which are involved in the regulation of energy homeostasis and reproduction. GALP gene expression is regulated by several factors that reflect metabolic state including the metabolic hormones leptin and insulin, thyroid hormones, and blood glucose. Since the onset of puberty is so tightly regulated by metabolic status, it is possible that GALP plays a role in the onset of puberty [67].
Insulin is an important nutritional signal from periphery that may regulate the reproductive axis by direct effects on the GnRH neurons and specifically by stimulating GnRH gene expression [1]. Furthermore, there is clear evidence that insulin can act directly on the ovaries, since they have receptors for insulin and insulin-like growth factor (IGF) [68].
Children normally experience transient insulin resistance at puberty. Insulin resistance is increased immediately at the onset of puberty (Tanner 2) but returns to near prepubertal levels by the end of puberty (Tanner 5). The peak of insulin resistance occurs at Tanner 3 in both sexes, and girls are more insulin resistant than boys at all Tanner stages [69]. Insulin resistance is associated with compensatory hyperinsulinemia and decreased SHBG concentrations, which in turn causes increase in the bioavailability of sex steroids. In addition, hyperinsulinemia decreases hepatic production of SHBG. Insulin resistance is strongly related to BMI and waist circumference [69]. Obesity appears to be linked with marked insulin resistance, and the higher levels of insulin during this period may have more pronounced stimulatory effect on the reproductive axis. It may also increase the bioavailability of IGF-1, which is positively correlated to the level of obesity [70].
The increased amount of adipose tissue may play a crucial role also for the release of suprarenal androgens and consequently of adrenarche, which precedes the activation of gonadal axis. The role of adipocytes and their hormone leptin in the pubertal processes is shown in Fig. 7.2.
Other factor that has been implicated in the accelerated growth of obese children includes increased adipose tissue aromatization of androgens into estrogens [70]. Recently it was reported that maternal obesity before pregnancy may be related to earlier timing of pubertal milestones among sons [71]. The formula milk feeding may also have an impact on pubertal development, because it is more energy dense than breast milk, and this could explain the differences in rate of early weight gain between formula-fed and breastfed infants [29, 72]. Earlier beginning of artificial feeding of infants may be relevant to the earlier onset of puberty and to be a risk factor for childhood obesity. Exposure to other environmental agents such as phytoestrogens and endocrine disruptive chemicals can cause early pubertal development and early onset of menarche [54, 73].
Underweight
Underweight status may be related to genetic factors, acute or chronic undernutrition, or chronic diseases. It is a result of negative energy balance, which is most often due to reduced food intake, increased energy expenditure, or both together. Typically this occurs in patients with anorexia nervosa or in certain diseases which are associated with malnutrition. In recent years excessive exercise alone may be another cause of weight loss. Underweight status has been associated with higher rates of morbidity and mortality, although to a lesser extent that obesity.
Changes in reproductive axis in underweight children are poorly understood. The observations are mainly in patients with anorexia nervosa. Nutritional deprivation has a suppressive effect on gonadotropin secretion and gonads, regardless of its etiology. The main mechanism of gonadotropin suppression is inhibition of the secretion of GnRH. Severe malnutrition leads to decreased levels of gonadotropins [30, 74], which can be increased with normalization of food imports, and this can cause a temporary increase in estrogen production [74] with the development of gynecomastia in boys (see Chap. 13). It is assumed that the decreased response of the pituitary is due to the dysfunction of the hypothalamus and the changes in the levels of certain neurotransmitters and neuropeptides. Also, some studies have found a decrease in insulin [75] and leptin [31, 74] levels and increase of SHBG concentrations [75], which may lead to disturbances in the function of gonadal axis in adolescents. Leptin stimulates the secretion of GnRH, and its lowering in conditions of negative energy balance leads to the diminish effect on the cells expressing GnRH. However, after a rise of leptin to physiological levels, its impact on GnRH is not recovered [76]. Other hormonal changes as increased levels of GH and cortisol are well described. The disturbances in patients with anorexia nervosa and malnutrition can be seen as adaptive mechanism in conditions of energy insufficiency. Increased cortisol levels intensify proteolysis in muscles to amino acids that are necessary for gluconeogenesis and for the synthesis of essential functional proteins in the liver. The increased GH on the background of reduced levels of IGF-1 does not have an anabolic effect and leads to cessation of the growth. However, lipolytic effect of GH is preserved. Gonadal axis in this extreme situation returns to prepubertal levels to keep the individual, and the reproductive function is discontinued.
Consequences of the Disturbances in Body Weight for the Pubertal Development
In girls as well as in boys, there is a positive relationship between body weight and the pubertal development. In the overweight children puberty begins and progresses earlier in comparison with the normal-weight individuals, whereas the underweight in adolescents is related to later onset and development of puberty. Early onset of puberty could have serious health and social consequences, such as increased rates of cancer in reproductive organs later in life and engagement in early sexual activity and alcohol use [34]. Overnutrition between 2 and 8 years of age will not be beneficial from a final height point of view, as the temporary increase in height gain in childhood will be compensated by an earlier maturity and subnormal height gain in adolescence. Each increased unit of BMI gained in childhood reduces the height gain in adolescence with 0.88 cm for boys and 0.51 cm for girls [77]. In recent years, the efforts have mainly focused on obesity prevention, since there is a greater risk for developing cardiovascular disease and diabetes in later life, but little attention is paid to underweight in children, which, especially in girls, can cause severe disturbances in function of gonadal axis and may affect the processes of reproduction. These data support the need of wide promotion activities regarding the optimal and healthy nutrition in children and regular physical activity.
References
Kim HH, DiVall SA, Deneau RM, Wolfe A. Insulin regulation of GnRH gene expression through MAP kinase signaling pathways. Mol Cell Endocrinol. 2005;242(1–2):42–9.
Reilly J. Obesity in childhood and adolescence: evidence based clinical and public health perspectives. Postgrad Med J. 2006;82:429–37.
Benedet J, da Silva Lopes A, Adami F, de Fragas Hinnig P, de Vasconcelos FA. Association of sexual maturation with excess body weight and height in children and adolescents. BMC Pediatr. 2014;14:72–8.
Barlow SE. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics. 2007;120 Suppl 4:S164–92.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240–5.
Biro FM, Huang B, Daniels SR, Lucky AW. Pubarche as well as thelarche may be a marker for the onset of puberty. J Pediatr Adolesc Gynecol. 2008;21(6):323–8.
Burt Solorzano CM, McCartney CR. Obesity and the pubertal transition in girls and boys. Reproduction. 2010;140:399–410.
Laron Z. Is obesity associated with early sexual maturation? Pediatrics. 2004;113:171–2.
Styne DM. Puberty, obesity and ethnicity. Trends Endocrinol Metab. 2004;15(10):472–78.
Kaplowitz PB, Slora EJ, Wasserman RC, Pedlow SE, Herman-Giddens ME. Earlier onset of puberty in girls: relation to increased body mass index and race. Pediatrics. 2001;108(2):347–53.
Wang Y. Is obesity associated with early sexual maturation? A comparison of the association in American boys versus girls. Pediatrics. 2002;110:903–10.
Anderson SE, Dallal GE, Must A. Relative weight and race influence average age at menarche: results from two nationally representative surveys of US girls studied 25 years apart. Pediatrics. 2003;111(4 Pt 1):844–50.
Lee JM, Appugliese D, Kaciroti N, Corwyn RF, Bradley RH, Lumering JC. Weight status in young girls and the onset of puberty. Pediatrics. 2007;119(3):e624–30. Erratum in: Pediatrics 2007;120(1):251.
Biro FM, Greenspan LC, Galvez MP, Pinney SM, Teitelbaum S, Windham GC, et al. Onset of breast development in a longitudinal cohort. Pediatrics. 2013;132(5):1–9.
de Muinck Keizer-Schrama SMPF, Mul D. Trends in pubertal development in Europe. Hum Reprod Update. 2001;7(3):287–91.
Aksglaede L, Sørensen K, Petersen JH, Skakkebaek NE, Juul A. Recent decline in age at breast development: the Copenhagen Puberty Study. Pediatrics. 2009;123(5):e932–9.
Zhai L, Liu J, Zhao J, Liu J, Bai Y, Jia L, et al. Association of obesity with onset of puberty and sex hormones in Chinese girls: a 4-year longitudinal study. PLoS One. 2015;10(8), e0134656.
Demerath EW, Towne B, Chumlea WC, Sun SS, Czerwinski SA, Remsberg KE, et al. Recent decline in age at menarche: the Fels Longitudinal Study. Am J Hum Biol. 2004;16:453–7.
Kaplowitz PB. Link between body fat and the timing of puberty. Pediatrics. 2008;121 Suppl 3:S208–17.
Rosenfeld RL, Lipton RB, Drum ML. Thelarche, pubarche, and menarche attainment in children with normal and elevated body mass index. Pediatrics. 2009;123(1):84–8. Erratum in: Pediatrics. 2009;123(4):1255.
Sørensen K, Juul A. BMI percentile-for-age overestimates adiposity in early compared with late maturing pubertal children. Eur J Endocrinol. 2015;173(2):227–35.
Boyne MS, Thame M, Osmond C, Fraser RA, Gabay L, Reid M, et al. Growth, body composition, and the onset of puberty: longitudinal observations in Afro-Caribbean children. J Clin Endocrinol Metab. 2010;95:3194–200.
Ong KK, Ahmed ML, Dunger DB. Lessons from large population studies on timing and tempo of puberty (secular trends and relation to body size): the European trend. Mol Cell Endocrinol. 2006;254–255:8–12.
Tomova A, Lalabonova C, Robeva RN, Kumanov PT. Timing of pubertal maturation according to the age at first conscious ejaculation. Andrologia. 2011;43:163–6.
Parent AS, Teilmann G, Jull A, Skakkebaek NE, Toppari J, Bourguignon JP. The timing of normal puberty and the age limits of sexual precocity: variation around the world, secular trend, and changes after migration. Endocr Rev. 2003;24:668–93.
Bau AM, Ernert A, Schenk L, Wiegand S, Martus P, Grutrs A, et al. Is there a further acceleration in the age at onset of menarche? A cross-sectional study in 1840 school children focusing on age and bodyweight at the onset of menarche. Eur J Endocrinol. 2009;160(1):107–13.
Hernandez MI, Unanue N, Gaete X, Cassorla F, Codner E. Age of menarche and its relationship with body mass index and socioeconomic status. Rev Med Chil. 2008;135(11):1429–36.
Dos Santos Silva I, De Stavola BL, Mann V, Kuh D, Hardy R, Wadsworth ME. Prenatal factors, childhood growth trajectories and age at menarche. Int J Epidemiol. 2002;31(2):405–12.
Dunger DB, Ahmed ML, Ong KK. Early and late weight gain and the timing of puberty. Mol Cell Endocrinol. 2006;254–255:140–5.
Tomova A, Makker K, Kirilov G, Agarwal A, Kumanov P. Disturbances in gonadal axis in women with anorexia nervosa. Eat Weight Disord. 2007;12(4):e92–7.
Tolle V, Kadem M, Bluet-Pajot MT, Frere D, Foulon C, Bossu C, et al. Balance in ghrelin and leptin plasma levels in anorexia nervosa patients and constitutionally thin women. J Clin Endocrinol Metab. 2003;88(1):109–16.
Karlberg J. Secular trends in pubertal development. Horm Res. 2002;57 Suppl 2:19–30.
Lee JM, Kaciroti N, Appugliese D, Corwyn RF, Bradley RH, Lumeng JC. Body mass index and timing of pubertal initiation in boys. Arch Pediatr Adolesc Med. 2010;164:139–44.
Herman-Giddens ME, Steffes J, Harris D, Slora E, Hussey M, Dowshen SA, et al. Secondary sexual characteristics in boys: data from the pediatric research in office settings network. Pediatrics. 2012;130:e1058–1068.
Vizmanos B, Martí-Henneberg C. Puberty begins with a characteristic subcutaneous body fat mass in each sex. Eur J Clin Nutr. 2000;54:203–8.
Tinggaard J, Aksglaede L, Sørensen K, Mouritsen A, Wohlfahrt-Veje C, Hagen CP, et al. The 2014 Danish references from birth to 20 years for height, weight and body mass index. Acta Paediatr. 2014;103:214–24.
Karpati AM, Rubin CH, Kieszak SM, Marcus M, Troiano RP. Stature and pubertal stage assessment in American boys: the 1988–1994 Third National Health and Nutrition Examination Survey. J Adolesc Health. 2002;30:205–12.
Ankarberg-Lindgren C, Norjavaara E. Changes of diurnal rhythm and levels of total and free testosterone secretion from pre to late puberty in boys: testis size of 3 ml is a transition stage to puberty. Eur J Endocrinol. 2004;151:747–57.
Palmert MR, Dunkel L. Delayed puberty. N Engl J Med. 2012;366:443–53.
Tinggaard J, Mieritz MG, Sørensen K, Mouritsen A, Hagen CP, Aksglaede L, et al. The physiology and timing of male puberty. Curr Opin Endocrinol Diabetes Obes. 2012;19:197–203.
Tanner JM, Whitehouse RH. Clinical longitudinal standards for height, weight, height velocity, weight velocity, and stages of puberty. Arch Dis Child. 1976;51:170–9.
Tomova A, Robeva R, Kumanov P. Influence of the body weight on the onset and progression of puberty in boys. J Pediatr Endocrinol Metab. 2015;28(7–8):859–65.
Juul A, Magnusdottirs S, Scheike T, Prytz S, Skakebaek NE. Age at voice break in Danish boys: effects of pre-pubertal body mass index and secular trend. Int J Androl. 2007;30(6):537–42.
Fu JF, Dong GP, Liang L, Jiang YJ, Chen LQ, Dayan C. Early activation of the inhibin B/FSH axis in obese Tanner stage G1PH1 boys. Clin Endocrinol (Oxf). 2006;65:327–32.
Sørensen K, Aksglaede L, Petersen JH, Juul A. Recent changes in pubertal timing in healthy Danish boys: association with body mass index. J Clin Endocrinol Metab. 2010;95:263–70.
Patton GC, Viner R. Pubertal transitions in health. Lancet. 2007;369:1130–39.
Ebling FJ. The neuroendocrine timing of puberty. Reproduction. 2005;129:675–83.
Styne D. Puberty. In: Gardner DG, Shoback D, editors. Greenspan’s basic and clinical endocrinology. New York, Chicago, San Francisco: McGraw Hill; 2007. p. 611–40.
Araujo AB, Wittert GA. Endocrinology of the aging male. Best Pract Res Clin Endocrinol Metab. 2011;25(2):303–19.
Alwis G, Rosengren B, Stenevi-Lundgren S, Düppe H, Sernbo I, Karlsson MK. Normative dual energy X-ray absorptiometry data in Swedish children and adolescents. Acta Paediatr. 2010;99:1091–9.
Frisch RF, Revelle R. Height and weight at menarche and hypothesis of menarche. Arch Dis Child. 1971;46:695–701.
Baskin DG, Breininger JF, Schwartz MW. SOCS-3 expression in leptin-sensitive neurons of the hypothalamus of fed and fasted rats. Regul Pept. 2000;92(1–3):9–15.
Hill JW, Elmquist JK, Elias CF. Hypothalamic pathways linking energy balance and reproduction. Am J Physiol Endocrinol Metab. 2008;294:E827–32.
Biro FM, Greenspan LC, Galvezl MP. Puberty in girls of the 21st century. J Pediatr Adolesc Gynecol. 2012;25(5):289–94.
Fischer-Posovszky P, Wabitsch M, Hochberg Z. Endocrinology of adipose tissue: an update. Horm Metab Res. 2007;39:314–21.
Chehab FF. Leptin and reproduction: past milestones, present undertakings and future endeavors. J Endocrinol. 2014;223:T37–48.
Matkovic V, Ilich JZ, Skugor M, Badenhop NE, Goel P, Clairmont A, et al. Leptin is inversely related to age at menarche in human females. J Clin Endocrinol Metab. 1997;82(10):3239–45.
Rutters F, Nieuwenhuizen AG, Verhoef SP, Lemmens SG, Vogels N, Westerterp-Plantenga MS. The relationship between leptin, gonadotropic hormones, and body composition during puberty in a Dutch children cohort. Eur J Endocrinol. 2009;160(6):973–8.
Blum W, Englaro P, Hanitsch S, Juul A, Hertel NT, Muller G, et al. Plasma leptin levels in healthy children and adolescent: dependence on body mass index, body fat mass, gender, pubertal stage and testosterone. J Clin Endocrinol Metab. 1997;82(9):2904–10.
Singh R, Artaza JN, Taylor WE, Braga M, Yuan X, Gonzalez-Cadavid NF, et al. Testosterone inhibits adipogenic differentiation in 3T3 L1 cells: nuclear translocation of androgen receptor complex with β-catenin and T-cell factor 4 may bypass canonical Wnt signalling to down-regulate adipogenic transcription factors. Endocrinology. 2006;147:141–54.
Cornish J, Callon KE, Bava U, Lin C, Naot D, Hill BL, et al. Leptin directly regulates bone cell function in vitro and reduces bone fragility in vivo. J Endocrinol. 2002;175(2):405–15.
Turner RT, Kalra SP, Wong CP, Philbrick KA, Lindenmaier LB, Boghossian S, et al. Peripheral leptin regulates bone formation. J Bone Miner Res. 2013;28(1):22–34.
Shahab M, Mastronardi C, Seminara S, Crowley WF, Ojeda SR, Plant TM. Increased hypothalamic GPR54 signaling: a potential mechanism for initiation of puberty in primates. Proc Natl Acad Sci U S A. 2005;102(6):2129–34.
Plant T. The role of KISS-1 in the regulation of puberty in higher primates. Eur J Endocrinol. 2006;155:S11–6.
Zhang C, Bosch MA, Rønnekleiv OK, Kelly MJ. Gamma-aminobutyric acid B receptor mediated inhibition of gonadotropin-releasing hormone neurons is suppressed by kisspeptin-G protein-coupled receptor 54 signaling. Endocrinology. 2009;150(5):2388–94.
Ahmed ML, Ong KK, Dunger D. Childhood obesity and the timing of puberty. Trends Endocrinol Metab. 2009;20(5):237–42.
Lawrence C, Fraley GS. Galanin-like peptide (GALP) is a hypothalamic regulator of energy homeostasis and reproduction. Front Neuroendocrinol. 2011;32(1):1–9.
Rosen MP, Cedars MI. Female reproductive endocrinology and infertility. In: Gardner DG, Shoback D, editors. Greenspan’s basic and clinical endocrinology. New York, Chicago, San Francisco etc: McGraw Hill comp; 2007. p. 502–61.
Moran A, Jacobs DR, Steinberger J, Hong CP, Prineas R, Luepker R, et al. Insulin resistance during puberty: results from clamp studies in 357 children. Diabetes. 1999;48(10):2039–44.
Marcovecchio ML, Chiarelli F. Obesity and growth during childhood and puberty. World Rev Nutr Diet. 2013;106:135–41.
Hounsgaard ML, Håkonsen LB, Vested A, Thulstrup AM, Olsen J, Bonde JP, et al. Maternal pre-pregnancy body mass index and pubertal development among sons. Andrology. 2014;2:198–204.
Novotny R, Daida YG, Grove JS, Acharya S, Vogt TM. Formula feeding in infancy is associated with adolescent body fat and earlier menarche. Cell Mol Biol (Noisy-le-grand). 2003;49(8):1289–93.
Den Hond E, Schoeters G. Endocrine disrupters and human puberty. Int J Androl. 2006;29:264–71.
Djurovic M, Pekic S, Petakov M, Damjanovic S, Doknic M, Dieguez C, et al. Gonadotropin response to clomiphene and plasma leptin levels in weight recovered but amenorrhoeic patients with anorexia nervosa. J Endocrinol Invest. 2004;27(6):523–7.
Tomova A, Kumanov P, Kirilov G. Factors related to sex hormone binding globulin concentrations in women with anorexia nervosa. Horm Metab Res. 1995;27(11):508–10.
True C, Grove KL, Smith MS. Beyond leptin: emerging candidates for the integration of metabolic and reproductive function during negative energy balance. Front Endocrinol. 2011;2:1–12.
He Q, Karlberg J. BMI in childhood and its association with height gain, timing of puberty, and final height. Pediatr Res. 2001;49:244–51.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Tomova, A. (2016). Body Weight and Puberty. In: Kumanov, P., Agarwal, A. (eds) Puberty. Springer, Cham. https://doi.org/10.1007/978-3-319-32122-6_7
Download citation
DOI: https://doi.org/10.1007/978-3-319-32122-6_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-32120-2
Online ISBN: 978-3-319-32122-6
eBook Packages: MedicineMedicine (R0)