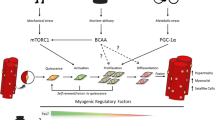
Abstract
Satellite cells are the “currency” for the muscle growth that is critical to meat production in many species, as well as to phenotypic distinctions in development at the level of species or taxa, and for human muscle growth, function and regeneration. Careful research on the activation and behaviour of satellite cells, the stem cells in skeletal muscle, including cross-species comparisons, has potential to reveal the mechanisms underlying pathological conditions in animals and humans, and to anticipate implications of development, evolution and environmental change on muscle function and animal performance.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- c-met receptor
- HGF
- Skeletal muscle
- Growth
- Regeneration
- Nitric oxide
- Muscle atrophy
- Cytoskeleton
- DGC
- Zebrafish
1.1 Introduction
As the building blocks for skeletal muscle during development, growth and regeneration (Anderson 2006; Mauro 1961; Mauro et al. 1970; Yablonka-Reuveni 2011), satellite cells play a fundamental role in muscle biology and animal function. They can respond dramatically and continuously to alterations in physiological demands on muscle, and to injuries and changes in nutritional constraints during adaptation. It is well-established that growth factors and cytokines have important roles in the repair of skeletal muscle (Karalaki et al. 2009), and that they have differential effects at various stages of myogenesis. Hepatocyte growth factor (HGF) for instance, is a protein made in myocytes and myoblasts (Charge and Rudnicki 2004; Sheehan et al. 2000; Tatsumi et al. 1998) and it promotes their proliferation while inhibiting myotube formation and differentiation in culture and regeneration.
HGF binds to the c-met receptor expressed on myoblasts and on satellite cells; that binding inhibits expression of the muscle regulatory genes, MyoD and myogenin, and the structural protein, myosin heavy chain (Anastasi et al. 1997; Gal-Levi et al. 1998; Leshem et al. 2000; Miller et al. 2000). By comparison, other growth factors also promote proliferation of myogenic cells, for example insulin-like growth factor (IGF-1) and fibroblast growth factor (FGF-2) and then promote myotube differentiation (Allen and Boxhorn 1989; Florini and Magri 1989; Hayashi et al. 2004).
Distinctions among growth factors in their activity in skeletal muscle were first explored in now-classic in vitro culture studies of proliferation and differentiation (Allen et al. 1995b; 1979) to understand the regulation of muscle growth. Studies of HGF, FGF and transforming growth factor beta (TGF-β) on proliferation and differentiation (Allen et al. 1995b; Allen and Boxhorn 1989; Allen and Rankin 1990; Johnson and Allen 1993; 1995) opened the field to studies of different stages in the myogenic regulatory program. As revealed at the time, the sequence of regulatory gene expression was delayed in cultures of satellite cells from muscle of old rats, pending a latent period between isolation of the quiescent satellite cells from muscle and their activation and proliferation in culture (Smith et al. 1994). Bischoff used a crushed-muscle extract (CME) preparation to induce activation of satellite cells on isolated fibers prepared for culture, and that extract was also shown to enhance muscle regeneration and satellite cell activity in vivo (Bischoff 1986a, b; Bischoff and Heintz 1994).
Early in situ hybridization experiments demonstrated that HGF was regulated during muscle development and then transiently expressed following ischemia-induced muscle injury and repair (Jennische et al. 1993). However, it was the notion that live and dead muscle fibers have distinctive interactions with their resident satellite cells and that living, intact fibers produce a factor that activates satellite cells and stimulates their transition from G0 to the cell cycle (Bischoff 1990). This was confirmed later, in studies of activation on fibers exposed to CME or the myotoxin, marcaine (Anderson and Pilipowicz 2002); those studies led to the identification of HGF as the activating factor in CME (Tatsumi et al. 1998). Subsequently, HGF-c-met interactions were examined in the context of paracrine signaling (Anastasi et al. 1997). More recently, an engineered high-affinity HGF with two c-met binding sites called Magic-Factor 1, has been shown to stimulate hypertrophy through anti-apoptotic pathways (Cassano et al. 2008). Current literature gives HGF a very prominent profile in processes mediating the balance between the activation of satellite cells and their return to quiescence (bou-Khalil et al. 2010; Chazaud 2010; Yamada et al. 2010), although other gene products and genetic background clearly impact satellite cell populations and their functionality in healthy and diseased muscle (Fukada et al. 2010; 2013).
Satellite cell activation is initiated through a cascade of calcium-dependent signals that release HGF from the extracellular matrix (Hara et al. 2012; Tatsumi et al. 2009b; Tatsumi 2010). Injury-induced activation leads to those processes involved in regeneration of muscle tissue, including angiogenesis, nerve sprouting and innervation, matrix remodelling and myogenesis, itself. All these processes impact directly on the outcome of tissue repair and the level of function attained by that tissue. Since the identification of nitric oxide as a potent mediator of satellite cell activation in mouse muscle (Anderson 2000; Wozniak and Anderson 2007; 2009), many roles of HGF and HGF-mediated signaling during the regeneration of muscle tissue have been reported. However, the scope of differences in HGF-mediated processes during activation and regeneration in different species, and many of the key aspects of chemical, mechanical, growth-factor- and chemokine-mediated signaling that affect muscle plasticity and function are not as well established across species, despite their importance in shaping muscle adaptation and the wide range of life-history challenges met by different species.
Capabilities of research using the single-fiber culture model to study HGF-mediated activation in mammalian and zebrafish muscle provide a strong platform for future exploration of HGF-induced signaling in development and muscle-tissue repair. This chapter provides a focused review of literature that relates to HGF-mediated mechanisms important in muscle growth and regeneration. Many studies demonstrate the interdependence of muscle structure, development and phenotype by modeling their combined impact on the activation of satellite cells. Evolutionary distinctions in activation by nitric oxide signaling (Anderson 2000) and possible species-dependent contributions of satellite cell regulation may contribute to determining the phenotypic pattern of muscle tissue expansion.
1.2 Satellite Cell Activation
The cytoskeletal transmembrane dystroglycan complex (DGC) anchors nitric oxide synthase (NOS)-1 close to the muscle fiber membrane. The DGC stabilizes the membrane of contracting muscle fibers by linking the actin cytoskeleton through the membrane to the surrounding matrix (Barresi and Campbell 2006; Campbell and Stull 2003; Durbeej and Campbell 2002; Ervasti and Campbell 1991; 1993; Matsumura et al. 1993). Changes in dystrophin, NOS-1 and transmembrane β-dystroglycan in the DGC, between muscles of wild-type, dystrophin-deficient and old mice accompany changes in satellite cell activation and cycling in muscle development, atrophy and regeneration (Janke et al. 2013; Leiter et al. 2012; Wozniak et al. 2003; Wozniak and Anderson 2007). We recently identified that the DGC develops in relation to muscle loading (Janke et al. 2013).
Satellite cells are precursor or stem cells on muscle fibers (Anderson 2006; Seale and Rudnicki 2000; Yablonka-Reuveni 2011) and are the source of cells for growth and regeneration (Collins et al. 2005; Collins and Partridge 2005). In adult mice, satellite cells are mitotically quiescent (G0); once activated to cycle, they form myoblasts that commit to the muscle lineage, divide, differentiate and fuse to extend existing fibers or form new ones. By asymmetrical division, some myoblasts return to a satellite position on fibers to renew the stem-cell niche (Collins et al. 2005; Kuang et al. 2007; Rudnicki et al. 2008). As fiber nuclei are post-mitotic, satellite cell activation is critical for muscle regeneration and plasticity.
Satellite cells are activated to cycle via signaling through the potent gaseous signal of nitric oxide release (Anderson 2000). Time-course studies of satellite cell activation using single muscle fibers that were mechanically stretched in culture revealed functional satellite-cell heterogeneity related to mRNA expression of c-met, the receptor for HGF (Fig. 1.1), and that loss of dystrophin appears to deplete particular subpopulations (Anderson and Wozniak 2004; Beauchamp et al. 1999; Collins et al. 2007; Heslop et al. 2000; Wozniak et al. 2003; Wozniak and Anderson 2007; 2009). Changes in NOS-1 expression or activity reduce or delay activation by injury, and then perturb the muscle-regeneration cascade (Anderson 2000; Wozniak and Anderson 2007). NOS-1 down-regulation in dystrophic muscle (Brenman et al. 1995) occurs with muscle loading in development and is not a direct result of the genetic loss of dystrophin (Janke et al. 2013). The mechano-sensitive NOS-1 protein releases nitric oxide after stretch; this liberates HGF from the fiber matrix. HGF binds to the c-met receptor on satellite cells, initiating satellite cell cycling and movement (Siegel et al. 2009; 2011; Tatsumi et al. 1998; 2002; Wozniak et al. 2003; 2005; Wozniak and Anderson 2007; 2009). Satellite cells also express dystrophin (Anderson et al. 1991), loss of which was shown recently to particularly impact satellite cell polarity in mitotic division and disease progression and regeneration in muscular dystrophy (Dumont et al. 2015).
Satellite cell heterogeneity on fibers. Zebrafish fibers were isolated, plated on collagen and incubated with or without cyclical stretching using a FlexCell vacuum-system apparatus. Fibers were fixed after 0 h, 3 of stretching or after 24 h (3 h stretching plus 21 h further incubation) before immunostaining for c-met protein. The number of c-met-positive satellite cells on each fiber was plotted as a frequency distribution for control fibers (without stretch) and fibers immediately or 21 h after stretch (Zhang and Anderson 2014). Graphs show significant heterogeneity for the distribution of c-met-positive satellite cells as a population on fibers (at least 67 fibers per group)
The level of c-met expression in muscle and the number of c-met expressing satellite cells on fibers increases after activating satellite cells in wild-type mouse muscle (Anderson and Wozniak 2004; Wozniak et al. 2003). Interestingly, HGF is expressed in many types of cells in muscle tissue including skeletal, smooth and cardiac muscle cells (Fig. 1.2). HGF is also expressed by infiltrating mononuclear inflammatory cells in regenerating mouse muscle (Sakaguchi et al. 2014) and in human muscle of patients with polymyositis/dermatomyositis (Sugiura et al. 2010). Interestingly, macrophages were reported to activate myogenic cells as early as 1999 (Merly et al. 1999). In cultures of CD56-expressing myoblasts from those patients, the level of HGF was reduced by treatment with TGFβ and anti-inflammatory treatment, and increased by treatment with interleukin-1α (Sugiura et al. 2010). HGF treatment of those cells in culture reduced their synthesis of pro-collagen 1, while interferon-gamma increased the expression of c-met, suggesting the use of HGF to promote regeneration of muscle in inflammatory conditions (Sugiura et al. 2010). HGF-mediated muscle cell proliferation was also suggested as an approach to promoting muscle growth for treatment of urinary incontinence (Sumino et al. 2007). Molecules including miRNA489 (Brack et al. 2009), FoxO1, TGFβ3 and myostatin promote quiescence and inhibit growth and cycling (Argiles et al. 2012; Huang et al. 2012; Reed et al. 2012; Thomas et al. 2000). The balance between quiescence and activation states in myogenic cells is influenced by epigenetic effects of the surrounding matrix that are mediated by signaling through the Wnt pathway and the methylation state of chromatin that is mediated in part by mixed lineage leukemia 5 (MLL5) (Dhawan and Rando 2005; Sebastian et al. 2009; Sellathurai et al. 2013; Srivastava et al. 2010; Subramaniam et al. 2013).
Hepatocyte growth factor (HGF) expression in control and dystrophic muscle. Muscle histology viewed by hematoxylin and eosin staining (a, e) and in situ hybridization for HGF) using digoxigenin-labeled riboprobe to identify mRNA (b–d, f–h) from wild-type C57BL10 mice (a–d) and dystrophin-deficient mdx mice (e–f). (a) Muscle fibers in control diaphragm. (b) Two satellite Fig. 1.2 (continued) cells (arrows) in tibialis anterior muscle contain cytoplasm densely stained for HGF transcript; less intense staining for HGF transcripts is visible around the periphery of myofibers. A nerve bundle is indicated by the crossed vertical arrow. (c) HGF expression is demonstrated in intrafusal fibers of a muscle spindle (arrow) and in smooth muscle around a blood vessel (crossed vertical arrow). (d) A small myotube (vertical arrow) is regenerating between intact fibers in the diaphragm of a control mouse. (e) Regenerating fibers (arrow) within sections of dystrophic tibialis anterior muscle. (f and g) Small regenerating fibers (arrows) are intensely stained for HGF mRNA in an inter-nuclear distribution in longitudinal section (g). (h) Cardiac myocytes from the atrium of a dystrophic mouse are stained for HGF transcripts (arrow). Bar = 10 μm (original magnification X200); bar in panel b applies to b–h (original magnification X400)
1.3 Myogenic Cell Motility
Syndecans, especially syndecan 3 among the heparan sulphate proteoglycans (Casar et al. 2004; Cornelison et al. 2001; 2004; Pisconti et al. 2010; Rapraeger 2000), CD34, Eph-ephrin and Notch-delta interactions, Wnt, FGF2 and possibly Hedgehog (Xie et al. 2013) promote motility and cycling after activation (Alfaro et al. 2011; Ieronimakis et al. 2010; Luo et al. 2005; O’Brien et al. 2004; Stark et al. 2011). Syndecan-3 and dermatan sulfate are required for muscle regeneration and activation signaling (Casar et al. 2004; Villena and Brandan 2004). Interestingly, HGF induces the formation of lamellipodia and cell migration in cultures of C2C12 cells in a 3-dimensional assay. This is reported to occur through a balance of PI3-kinase-dependent signals in the WAVE2 N-WASP pathway that involve the formation of branched actin filaments and polarization of the plasma membrane (Kawamura et al. 2004). Such regulation likely plays a role in the fascinating HGF-dependent travel by activated satellite cells along muscle fibers that can be so beautifully demonstrated in fiber cultures (Siegel et al. 2009; 2011). This HGF-mediated migration may also interact with CD44-dependent regulation of the speed of satellite cell migration (Mylona et al. 2006). Involvement of glypican-1 in stabilizing HGF-c-met interactions via mechanisms related to lipid-raft formation is required for the optimal response of mouse C2C12 cells to HGF signaling and to stabilize CD44 (Gutierrez et al. 2014). HGF also induces expression of caveolin-1 which inhibits cell proliferation, and is proposed to regulate the activity of the ERK pathway in satellite cell mobility and proliferation during regeneration (Volonte et al. 2005).
Another distinction among different growth factor-mediated processes is that HGF appears not to influence fibrinolysis required for invasion of myogenic cells into a matrix, although the migration process is dependent on urokinase plasminogen activator activity which is in turn, regulated by FGF-2 and TGFβ (Fibbi et al. 2002). Possible similarities among different types of cells (e.g., myogenic cells and keratinocytes) suggest that many features of migration, may show distinctions based on the surrounding matrix or particular features of how factors are applied in an experiment (e.g., separately or in combination), as illustrated by use of a wound-assay culture system (Peplow and Chatterjee 2013). In a review of heparanase and syndecan-1 in tumours, the up-regulation of HGF expression by heparanase, and subsequent binding of HGF to syndecan-1 for degradation, was highlighted as a mechanism regulating growth factor activity (Ramani et al. 2013). It is possible that similar interactions during HGF-mediated responses by satellite cells play a role in the timing or dose-response of activation and migration during growth and repair of muscle and could point the way to designing novel therapeutics to promote those processes.
1.4 Zebrafish Single-Fiber Studies of Satellite Cell Activation
Temperature, environment and life-history events such as migratory behaviour in fish and birds and hibernation patterns in mammals, influence muscle plasticity and metabolic adaptation (Corrigan et al. 2011; Johnston 2006; Johnston and Hall 2004; Meyerrochow and Ingram 1993; Price et al. 2011; Wund et al. 2008). For instance, hibernation affects muscle mass or growth in some vertebrates and not in others. Interestingly, hibernation can protect muscle from atrophy that ensues with starvation, disuse/immobilization or even denervation. Hibernation apparently changes the neural regulation of catabolic pathways, such that decreases in muscle mass and fiber cross-sectional area in hibernating bears after denervation are only one third to one half as pronounced as in non-hibernating bears (Lin et al. 2012). Hibernation is also accompanied by down-regulation of autophagic and proteolytic pathways mediated by serum- and glucocorticoid-inducible kinase-1 (GSK1) (Andres-Mateos et al. 2013). Moreover, in studies of the 13-striped ground squirrel, while the level of myostatin, which typically represses satellite cell proliferation in non-hibernating animals and typically increases in starvation and disuse, it is surprising that in hibernating animals, myostatin levels do not change. Myostatin stays at normal pre-hibernation levels well into hibernation, and the marked increase only happens when the animal is beginning to arouse from topor, toward the end of hibernation (Brooks et al. 2011). Regulation of muscle atrophy is clearly overlain by complex metabolic changes somewhat separable from neural and other activity and/or endocrine influences. Such fascinating observations encourage in-depth comparative studies of muscle satellite-cell biology and the impact of various life-history events.
A key distinction in muscle-growth capacity between mammals and teleosts is the regulation of fiber number. In mammals, fiber number does not increase after birth; by comparison, in teleost fish, the number of fibers, especially fast fibers, rises nearly continuously with body size and muscle mass, as part of the process termed indeterminate growth (Hall et al. 2004; Johnston 2006; Johnston and Hall 2004). A leader in the field, IA Johnston, notes the major gap in our understanding of the impact of indeterminate growth and ectothermy on the regulation of muscle growth in teleosts versus mammals (Johnston et al. 2011).
On the basis of the growing body of work on mammalian muscle fibers, and long-standing questions about the regulation of muscle growth in fish, we modified the protocol for isolating mouse-muscle fibers to enable culture studies of zebrafish muscle fibers (Anderson et al. 2012) prepared with careful attention to Bischoff’s technique (Bischoff 1986b). Using single-fiber cultures from zebrafish, experiments revealed that satellite cell activation on zebrafish fibers is mediated by nitric oxide, HGF and mechanical-stretch signals (Zhang and Anderson 2014) (Fig. 1.3a, b), similar to fiber cultures from mouse (Anderson and Pilipowicz 2002; Wozniak et al. 2003; Wozniak and Anderson 2007). However, although the cascade of activation involved similar signals, peak activation in zebrafish fiber cultures occurred at a distinctly higher concentration of nitric oxide and a lower concentration of HGF, than in our earlier findings on activation in mouse-fiber cultures; values in fish vs. mouse fiber experiments were: 1 mM isosorbide dinitrate (2 molar equivalents of nitric oxide released) vs. 100 nM of the NOS substrate L-arginine (1 molar equivalent of nitric oxide produced); and 10 ng/mL vs. 25 ng/mL HGF in medium, respectively (Anderson and Pilipowicz 2002; Wozniak and Anderson 2007; Zhang and Anderson 2014). [Unfortunately, the direction of the comparative fish-mouse difference for response to nitric oxide is reversed in Zhang and Anderson 2014.] While the levels of nitric oxide and HGF extant in the two types of fibers is not known, the relative differences indicate there is a differential “tuning” of activation by the HGF-mediated cascade in mouse and fish fibers. The dose-response of HGF-induced activation is shifted to a lower peak concentration of exogenous HGF by stretching in culture (Fig. 1.3c), due to release of HGF from the low-affinity receptors in the extracellular matrix surrounding fibers (Tatsumi et al. 2001; 2002; Tatsumi and Allen 2004). Activation by exposure to HGF and by mechanical stretching in the fish fibers is additionally mediated by temperature. Results of studies using inhibition of HGF-c-met binding and NOS activity demonstrated that activation of satellite cells on fibers in culture is reduced at 21 °C compared to the level observed at 27 °C, the typical temperature for rearing zebrafish (Zhang and Anderson 2014).
Dose-response curves for satellite cell activation on fibers in culture. Muscle fibers were isolated from zebrafish (a, b) and mouse (c) and cultured in basal growth medium containing bromodeoxyuridine (BrdU) for 24 h in the presence of: (a) the NO donor isosorbide dinitrate, ISDN (0–2.5 mM); (b) HGF (0–25 ng/mL); and (c) HGF (0–30 ng/mL) with or without cyclical stretching. After 24 h incubation, fibers were fixed and immunostained for BrdU, the dose-response of satellite cell activation was determined as the number of BrdU-positive satellite cells per fiber. Note that peak activation by HGF occurred at a lower concentration in unstretched zebrafish than mouse fiber cultures (c vs. b), and that HGF-induced activation on mouse fibers shifts to a lower concentration of HGF in the presence of 3 h of stretching
The interesting finding of a novel temperature-sensitive pattern of satellite cell activation on zebrafish fibers was accompanied by observation that the population of satellite cells identified by immunostaining studies for the c-met receptor protein, increased in size only 3 h after stretch (Zhang and Anderson 2014). This finding indicated that c-met is acting as an immediate early gene in satellite cell activation on zebrafish fibers, consistent with findings from mouse-fiber cultures (Wozniak et al. 2003). As well, there were more c-met-positive satellite cells on fish fibers, and they cycled faster than in mouse (Zhang and Anderson 2014). Very recent extension of these fiber-culture studies is now examining developmental aspects of interactions between fibers and their resident satellite cells.
The study demonstrated the sensitivity of the fiber-model system for testing the impact of brief or subtle changes in the fiber environment, on muscle growth and adaptive capacity. While there is clear conservation of regulatory pathways between zebrafish and mouse muscle, at least in the fiber-culture model system, these recent studies provide fresh insights on possible mechanisms of indeterminate muscle growth in fish that utilize fiber hyperplasia and hypertrophy, in comparison to post-natal muscle growth by hypertrophy of fibers in mammalian species. Such information could be a strong asset to aquaculture and food-meat production industries, and assist in further studies of the epigenetic interactions of the fiber cytoskeleton with satellite cell activity as they relate to understanding how the growth and repair of muscle tissue shape functional muscle plasticity.
1.5 Re-defining the Impact of Age on Satellite Cell Activation and Muscle-Growth Capacity
Previous research in this laboratory tracked the concurrent loss of muscle mass, strength, proliferation and fiber size in aging mice, with changes in NOS-1 and β-dystroglycan in the DGC and membrane function. Exercise increased levels of the protein NOS-1 in skeletal muscle and increased the proliferation of satellite cells when the intervention was given at eight but not 18 months-of-age, and the response was muscle-specific rather generalized in all muscles (Leiter et al. 2011). We also found that satellite cells were not activated in old muscle by the level of stretching that effectively activates them when younger muscle is stretched in culture, and this refractoriness to stretching increased with greater age (Leiter and Anderson 2010). The novel finding was that in muscles from old mice, proteins of the DGC were relocated and reduced in concentration (Leiter et al. 2012), and that remarkably, combined treatment with voluntary-running exercise and the nitric oxide-donor compound called isosorbide dinitrate, partly restored the beneficial muscle-building effects of exercise in the old mice, toward effects that are more typical of exercise effects on muscle in younger animals. This was despite the significant decline in the number of satellite cells expressing transcripts for myoD, myogenin or pax7 found in the gastrocnemius muscle of animals at 18 months-of-age, the age at which the combined treatment with ISDN plus exercise had started, compared to muscle at 3, 8 or 12 months-of-age (Fig. 1.4, Leiter & Anderson, unpublished data). Treatment also shifted the subcellular pattern of the β-dystroglycan and NOS-1 in muscle from the old mice, toward the localization pattern seen in muscle from much younger mice. This was concurrent with decreased permeability to serum immunoglobulins in the muscle of old mice; overall, the combined treatment of exercise and the nitric oxide donor resulted in a 25 % increase in muscle mass and increased fiber diameter in the old mice (Leiter et al. 2012). Without the increase in nitric oxide provided by the NO-donor treatment, exercised old mice displayed the typical loss of muscle mass and the distribution of the two proteins in the DGC had the pattern that was observed in muscle of old mice. There may be potential for application of therapy based on nitric oxide, to improve the functional state of muscle growth capacity in aging or to assist in “pre-habilitation” of muscle prior to surgical procedures. This study shows the growth capacity of satellite cells in old muscle is retained. A comprehensive examination of the capacity for muscle regeneration in response to three different types of injury (freeze, crush and myotoxin) in very old mice, showed that the capacity of satellite cells in muscle of old or very old mice to provide fully functional regenerated muscle tissue can be retained if muscle damage has not affected the neurovascular supply (Lee et al. 2013). The possibility of progressive changes in HGF expression and HGF-mediated signaling in satellite cell activation has not been fully explored through the aging process.
Satellite cell populations decline with increasing age. (a) Gastrocnemius muscle from mice aged 3, 8, 12, and 18 months, showing satellite cells stained positive by combined in situ hybridization (ISH) using a cocktail of riboprobes for pax7 (a muscle-specification gene, expressed in quiescent and activated satellite cells), and myoD and myogenin RNA (muscle-regulatory genes Fig. 1.4 (continued) expressed by activated satellite cells). Satellite cells are directly juxtaposed to the sarcolemma of unstained fibers (arrows indicate satellite cells with a prominent nucleus). Insets show a negative-control section (arrow points to an unstained satellite cell) and a satellite cell on an atrophic fiber (at 3 and 18 months, respectively). Bar = 10 μm. (b) Satellite cell density (number of ISH-positive mononuclear cells in the satellite position per field, mean ± SEM, 247–303 fields per group) was highest at 12 months. Brackets indicate significant differences (p < 0.001). (c) The percentage of satellite cells detected by in situ hybridization for each age group, plotted against satellite cell density (the number of ISH+ cells per field). The density of satellite cells expressing at least one of myoD, myogenin or pax7 declined with increasing age (p < 0.01, Chi-square statistics); 18-mo gastrocnemius muscles had the highest frequency of fields without any satellite cells (Leiter and Anderson, unpublished)
1.6 Integrating Growth, Satellite-Cell Behaviour and Cytoskeletal Development
Cytoskeletal NOS-1 and β-dystroglycan develop earlier in mouse diaphragm than limb muscle. This pattern changes with loss of dystrophin from the DGC (Janke et al. 2013). Such findings support the idea that differential muscle loading, which is higher and earlier in diaphragm than in limb muscle, and the structure of the DGC that differs in important but seemingly subtle ways from the DGC in the central nervous system, may explain muscle-specific variations in muscular dystrophy (Janke et al. 2013; Snow et al. 2013a; b). Previous reports on c-met regulation of cell functions, such as migration of invasive tumour cells, limb muscle precursors in development, and tubule formation by epithelial cells, in regeneration of liver and proliferation of liver and placental cells (Trusolino et al. 2010), and the outcome of muscle satellite-cell activation (Leiter et al. 2012; Webster and Fan 2013; Wozniak and Anderson 2007), clearly demonstrate the importance of the cytoskeleton in mediating that regulation.
Semaphorin3A (Sema3A) is a paracrine neuro-repellant protein, novel to muscle biology since 2009 (Tatsumi et al. 2009a). Sema3A is implicated in an axon-guidance role during the regeneration of skeletal muscle. HGF induces Sema3A secretion by activated satellite cells, but interestingly this does not occur through HGF binding to c-met. These findings suggest that satellite cells serve to collect and integrate activating and quiescence factors and the functional capacity for nerve-independent and nerve-dependent repair via Sema3A (Do et al. 2011; 2012; Suzuki et al. 2013). Sema3A is up-regulated by HGF, peaks early in myoblast differentiation and could mediate the timing of axonal ingrowth to regenerating fibers. It is intriguing that Sema3A may act through a receptor in the plexinA2-myogenin pathway that is particularly active in slow muscle (Suzuki et al. 2013; Tatsumi et al. 2009a). This field of study opens exciting new ways to study nerve-muscle interplay during muscle development. For example, it would be fascinating to examine the expression and behaviour of satellite cells on developing fibers at different life-stages from a number of species, as the stage that is particularly critical to organism survival may differ in different species. Satellite cell activity could be explored using an architectural approach, by examining the expression of HGF, Sema3A and other regulatory and structural proteins by satellite cells and their activation status, according to their distance from vessels or nerve-muscle junctions along a fiber in culture or in vivo. Such studies could help identify factors that contribute to producing a heterogeneous population of stem cells in a muscle, and how the behaviour of satellite cells during development and activation in growth, may influence the muscle phenotype that develops in different species.
Characterization of the satellite cell populations in vivo on adult and developing muscle fibers on non-mammalian species is an important and achievable goal, given the acceleration of the satellite cell field that has resulted in the past three decades of focused research using rodent models of human disease. Understanding how satellite cell populations vary in size and activation state by species, fiber type and through development can now be examined in relation to differences in the environment, function and behaviour of an organism. A good “baseline” understanding is still missing information about cross-species comparisons of satellite cell populations in adult and developing muscle that explain the differential responses by muscle to activating stimuli and environmental change, and the distinctive capacity for nearly life-long formation of new fibers in some species. Studies of the differential growth by fish developing in cold versus warm water, and the genes expressed by muscle tissue or fibers (Johnston 2006; Johnston et al. 2009; Johnston and Hall 2004; Steinbacher et al. 2011) have not fully explained the important biology of muscle satellite cells, the proteins they make or bind and their response to changing conditions. That information is crucial to anticipating animal responses to climate change, toxic habitat or tissue injury.
By studying the regulation of satellite cell activation signaling on single fibers in vitro, experiments could be conducted to examine species-specific differences in the regulation of satellite cell activation and how they may relate to features of the DGC. A synthesis of information on how the DGC and internal cytoskeleton shape nuclear position and development is also missing from the literature, despite the critical roles of those proteins in regulating satellite cell activation (for example, see Janke et al. 2013; Wozniak and Anderson 2007) and muscle fiber integrity.
A further gap in our knowledge relates to understanding the basis for central nucleation in regenerated fibers. Typically in development, as myotubes differentiate and receive innervation, nuclei shift from the central region of myotubes toward the periphery of fibers (just inside the DGC). Nesprin1 may be involved in that relocation. Nesprins are part of a complex that links the outer nuclear envelope with the actin cytoskeleton, and preliminary observations showed nesprin1 distribution differed between the peripheral nuclei in normal adult fibers and those centrally located nuclei in regenerated fibers in the absence of dystrophin (Kaluzny and Anderson, unpublished). The positioning of satellite cells in proximity to in-growing nerves and blood vessels (Duxson and Sheard 1995; Harris et al. 1989), particularly at the nerve-muscle junction or endplate regions, is also reported to relate to the location of giant nesprinG proteins (>1000 kb) (Burke and Roux 2009; Crisp et al. 2006; Roux et al. 2009; Starr and Fischer 2005; Tzur et al. 2006; Zhang et al. 2007). It would be fascinating to examine nerve-muscle junctions on fibers in culture, in relation to the position and activity of the resident satellite cells and myonuclei at important stages in development and regeneration, and also the interaction of satellite cells with angiogenic processes and vascular endothelial growth factor through those processes.
Since muscle stem-cell activity on fibers is so strongly linked with the ultimate outcome of muscle growth, physiology and adaption to neurovascular regulation (Allen et al. 1995a), it will be important to take new advantage from the fiber-model system to interrogate the relationship between satellite cell activation, behaviour and muscle phenotype. Fiber cultures could be used to study whether growth factors such as HGF or cytokines derived from the many tissue types in a muscle belly, direct satellite cell populations toward regenerating fibers that take up a particular fast or slower phenotype after the repair. Alternatively, satellite cells may be the prime organizers of key stages in the regenerative response through their integration of incoming signals and subsequent release of factors that actively signal to the local or systemic environment. For example, an interesting report examined systemic interactions mediating HGF expression, and found that within an hour of a muscle injury, both liver and spleen had up-regulated HGF expression and production of the inactive 90 kDa form of HGF protein. Serum from rats undergoing muscle regeneration was also able to induce expression of HGF transcripts in cells cultured from rat spleen, suggesting a role for an endocrine-level regulation of satellite cell behaviour (Suzuki et al. 2002). Fiber cultures could be used to screen for myogenic or growth-promoting effects of a range of compounds or extracts from natural or engineered tissues. Another report noted the importance of HGF in recruiting myogenic cells into injured muscle by mediating their interactions with vascular endothelial cells (Corti et al. 2001). With the recent discovery that satellite cells make Sema3A during activation and regeneration (Do et al. 2011; Suzuki et al. 2013; Tatsumi et al. 2009a), it is time to open the window wide for study of this novel aspect of muscle biology and nerve-muscle interaction.
Experiments on HGF-induced Sema3A production by satellite cells on single fibers, classified by immunostaining (Anderson et al. 1988; Merrifield and Atkinson 2000) and structure from mouse and zebrafish could be designed to manipulate satellite cell activation by HGF and nitric oxide, inhibit NOS-1 or block c-met and other cytokine and growth-factor receptors. Time-course studies such as those that tracked repair (Anderson et al. 1998; Grounds 1987; Grounds et al. 1992; Grounds and McGeachie 1987; 1992; McGeachie and Grounds 1987; McIntosh et al. 1998a, b, c; Moor et al. 2000; Smythe et al. 2008) may identify further fiber-type (Suzuki et al. 2013) or differential species effects on activation and Sema3A synthesis. Studies of larval muscle development in various fish species may identify species-specific patterns of HGF and Sema3A signaling that influence receptor clustering at nerve-muscle junctions (Lomo 2003), motor synapse elimination (Busetto et al. 2003; Jansen and Fladby 1990; Missias et al. 1996) and satellite cell positioning near synapses and vessels (Duxson et al. 1986; Duxson and Sheard 1995; Paul et al. 2004). HGF is known to increase blood vessel formation if it is incorporated in local-release acellular grafts after nerve sectioning (Li et al. 2008; Watanabe and Okada 1967). HGF also promotes angiogenesis and muscle-fascicle organization, as studied in a gel matrix around engrafted myoblasts (Barbero et al. 2001), and HGF expression increases during hyperbaric oxygen treatment to improve muscle repair after severe ischemia (Asano et al. 2007). Both findings are consistent with a recent report on the impact of oxygen levels on HGF-promoter activity and satellite cell-mediated angiogenesis (Flann et al. 2014).
Interestingly, acetylcholine receptors cluster on the muscle membrane before, not after developing fibers are innervated, so the pattern of fiber formation may influence the growth of motor axons and synapse formation (Arber et al. 2002). There are also distinct innervation patterns in parasitic and free-living lamprey (Atkins and Pezzementi 1993; Pezzementi and Chatonnet 2010) that have not been studied in relation to satellite cells on those muscle fibers. Such research could pursue the impact of satellite cell-derived factors such as HGF on driving angiogenesis (Ferrara et al. 2003; Williams and Annex 2004) or axon-guidance, and provide an exciting revision of classical thinking that is untested at the level of satellite-cell biology on fibers.
The precise state of satellite cells in a particular model system during assay, is critically important in interpreting findings. Satellite cells can be examined in many model systems: single-cell primary cultures, cell homogenates after expansion or differential plating, myoblasts derived from bulk cultures of mixed muscle cells, fibers cultured either free-floating or attached to a substrate, and in sections of normal, developing or regenerating muscle. In each system, the previous activities of those cells, the experimental conditions, and the way satellite cells or fibers are isolated as reagents for use in each assay all affect research findings and their interpretation. For instance, the mechanism of fiber isolation impacts the activation status of their resident satellite cells. Isolation to study satellite cell motility in response to HGF can effectively use cultures in which the preparation protocol activates the satellite cells (Siegel et al. 2009). By comparison, studies of the transition from quiescence to activation need preparations that avoid shaking or other activating stimuli (Anderson et al. 2012; Wozniak and Anderson 2005). The status of satellite cells, quiescent, activated, mobile and/or proliferative, needs to be verified in a control group under the same conditions (Wozniak et al. 2003; Wozniak and Anderson 2007). An understanding the status of satellite cells, such as their expression of muscle-regulatory genes (therefore activated), genes such as pax7 that specify muscle (Seale et al. 2000) or identify satellite cells (e.g., c-met, CD44, or CD56/NCAM) and their proliferation state, is as critical as experimental design in interpreting in vivo experiments. A recent report suggesting that HGF-c-met signaling may not be required for activation or proliferation of satellite cells (Webster and Fan 2013) did not control for a number of important features of experimental design: the interval between tamoxifen-knockdown of c-met gene activity and experimental assay; the possibility of residual c-met in satellite cells that were most stem-like or quiescent; satellite cell activation in different-aged mice at the time of injury; uncertain half-life of c-met; the activity of c-met as an immediate early gene (Wozniak and Anderson 2007; Zhang and Anderson 2014); and the complex implications of satellite-cell heterogeneity. Thus, the conclusions of that report regarding satellite cell activation are not well founded. Satellite cell behaviour following injury, stretching and isolation reflects the events of activation, including entry into the cell cycle and mobilization (Anderson 2000); the many molecular-genetic pathways and epigenetic and feedback mechanisms that regulate activation and/or are impacted by it, are yet to be fully established.
1.7 Conclusion
HGF activates satellite cells; its release from the muscle extracellular matrix is initially mediated via nitric oxide release, calcium-calmodulin signaling and matrix metalloproteinase activity after mechanical or injury-induced signals. Satellite cells respond by proliferating and making HGF and Sema3A; they also underpin the multi-directional signaling process between muscle fibers and proteins and cells in the large volume of tissue outside the endomysium. By using the single-fiber model system, single-cell physiology is accessible to comparative study and can give insights into the integral role of a heterogeneous population of satellite cells. Such research has potential to improve our ability to promote human muscle growth and repair, to prevent conditions such as age-related atrophy and to improve management and treatment of neuromuscular diseases. For animal and comparative physiologists, such basic muscle-cell biology studies could test new approaches to aquaculture and species conservation.
References
Alfaro LA, Dick SA, Siegel AL, Anonuevo AS, McNagny KM, Megeney LA, Cornelison DD, Rossi FM (2011) CD34 promotes satellite cell motility and entry into proliferation to facilitate efficient skeletal muscle regeneration. Stem Cells 29(12):2030–2041
Allen RE, Boxhorn LK (1989) Regulation of skeletal muscle satellite cell proliferation and differentiation by transforming growth factor-beta, insulin-like growth factor I, and fibroblast growth factor. J Cell Physiol 138(2):311–315
Allen RE, Rankin LL (1990) Regulation of satellite cells during skeletal muscle growth and development. Proc Soc Exp Biol Med 194(2):81–86
Allen RE, Merkel RA, Young RB (1979) Cellular aspects of muscle growth: myogenic cell proliferation. J Anim Sci 49(1):115–127
Allen DL, Monke SR, Talmadge RJ, Roy RR, Edgerton VR (1995a) Plasticity of myonuclear number in hypertrophied and atrophied mammalian skeletal muscle fibers. J Appl Physiol 78(5):1969–1976
Allen RE, Sheehan SM, Taylor RG, Kendall TL, Rice GM (1995b) Hepatocyte growth factor activates quiescent skeletal muscle satellite cells in vitro. J Cell Physiol 165(2):307–312
Anastasi S, Giordano S, Sthandier O, Gambarotta G, Maione R, Comoglio P, Amati P (1997) A natural hepatocyte growth factor/scatter factor autocrine loop in myoblast cells and the effect of the constitutive Met kinase activation on myogenic differentiation. J Cell Biol 137(5):1057–1068
Anderson JE (2000) A role for nitric oxide in muscle repair: nitric oxide-mediated activation of muscle satellite cells. Mol Biol Cell 11(5):1859–1874
Anderson JE (2006) The satellite cell as a companion in skeletal muscle plasticity: currency, conveyance, clue, connector and colander. J Exp Biol 209(Pt 12):2276–2292
Anderson J, Pilipowicz O (2002) Activation of muscle satellite cells in single-fiber cultures. Nitric Oxide 7(1):36–41
Anderson JE, Wozniak AC (2004) Satellite cell activation on fibers: modeling events in vivo – an invited review. Can J Physiol Pharmacol 82(5):300–310
Anderson JE, Bressler BH, Ovalle WK (1988) Functional regeneration in the hindlimb skeletal muscle of the mdx mouse. J Muscle Res Cell Motil 9(6):499–515
Anderson JE, Liu L, Kardami E (1991) Distinctive patterns of basic fibroblast growth factor (bFGF) distribution in degenerating and regenerating areas of dystrophic (mdx) striated muscles. Dev Biol 147(1):96–109
Anderson JE, McIntosh LM, Moor AN, Yablonka-Reuveni Z (1998) Levels of MyoD protein expression following injury of mdx and normal limb muscle are modified by thyroid hormone. J Histochem Cytochem 46(1):59–67
Anderson JE, Wozniak AC, Mizunoya W (2012) Single muscle-fiber isolation and culture for cellular, molecular, pharmacological, and evolutionary studies. Methods Mol Biol 798:85–102
Andres-Mateos E, Brinkmeier H, Burks TN, Mejias R, Files DC, Steinberger M, Soleimani A, Marx R, Simmers JL, Lin B, Hedderick EF, Marr TG, Lin BM, Hourde C, Leinwand LA, Kuhl D, Foller M, Vogelsang S, Hernandez-Diaz I, Vaughan DK, de la Rosa DA, Lang F, Cohn RD (2013) Activation of serum/glucocorticoid-induced kinase 1 (SGK1) is important to maintain skeletal muscle homeostasis and prevent atrophy. EMBO Mol Med 5(1):80–91
Arber S, Burden SJ, Harris AJ (2002) Patterning of skeletal muscle. Curr Opin Neurobiol 12(1):100–103
Argiles JM, Orpi M, Busquets S, Lopez-Soriano FJ (2012) Myostatin: more than just a regulator of muscle mass. Drug Discov Today 17(13–14):702–709
Asano T, Kaneko E, Shinozaki S, Imai Y, Shibayama M, Chiba T, Ai M, Kawakami A, Asaoka H, Nakayama T, Mano Y, Shimokado K (2007) Hyperbaric oxygen induces basic fibroblast growth factor and hepatocyte growth factor expression, and enhances blood perfusion and muscle regeneration in mouse ischemic hind limbs. Circ J 71(3):405–411
Atkins C, Pezzementi L (1993) Developmental changes in the molecular forms of acetylcholinesterase during the life-cycle of the lamprey Petromyzon marinus. Comp Biochem Physiol B: Biochem Mol Biol 106:369–372
Barbero A, Benelli R, Minghelli S, Tosetti F, Dorcaratto A, Ponzetto C, Wernig A, Cullen MJ, Albini A, Noonan DM (2001) Growth factor supplemented matrigel improves ectopic skeletal muscle formation–a cell therapy approach. J Cell Physiol 186(2):183–192
Barresi R, Campbell KP (2006) Dystroglycan: from biosynthesis to pathogenesis of human disease. J Cell Sci 119(Pt 2):199–207
Beauchamp JR, Morgan JE, Pagel CN, Partridge TA (1999) Dynamics of myoblast transplantation reveal a discrete minority of precursors with stem cell-like properties as the myogenic source. J Cell Biol 144(6):1113–1122
Bischoff R (1986a) A satellite cell mitogen from crushed adult muscle. Dev Biol 115(1):140–147
Bischoff R (1986b) Proliferation of muscle satellite cells on intact myofibers in culture. Dev Biol 115(1):129–139
Bischoff R (1990) Cell cycle commitment of rat muscle satellite cells. J Cell Biol 111(1):201–207
Bischoff R, Heintz C (1994) Enhancement of skeletal muscle regeneration. Dev Dyn 201(1):41–54
bou-Khalil R, Mounier R, Chazaud B (2010) Regulation of myogenic stem cell behavior by vessel cells: the “menage a trois” of satellite cells, periendothelial cells and endothelial cells. Cell Cycle 9(5):892–896
Brack AS, Murphy-Seiler F, Hanifi J, Deka J, Eyckerman S, Keller C, Aguet M, Rando TA (2009) BCL9 is an essential component of canonical Wnt signaling that mediates the differentiation of myogenic progenitors during muscle regeneration. Dev Biol 335(1):93–105
Brenman JE, Chao DS, Xia H, Aldape K, Bredt DS (1995) Nitric oxide synthase complexed with dystrophin and absent from skeletal muscle sarcolemma in Duchenne muscular dystrophy. Cell 82(5):743–752
Brooks NE, Myburgh KH, Storey KB (2011) Myostatin levels in skeletal muscle of hibernating ground squirrels. J Exp Biol 214(15):2522–2527
Burke B, Roux KJ (2009) Nuclei take a position: managing nuclear location. Dev Cell 17(5):587–597
Busetto G, Buffelli M, Cangiano L, Cangiano A (2003) Effects of evoked and spontaneous motoneuronal firing on synapse competition and elimination in skeletal muscle. J Neurocytol 32(5–8):795–802
Campbell KP, Stull JT (2003) Skeletal muscle basement membrane-sarcolemma-cytoskeleton interaction minireview series. J Biol Chem 278(15):12599–12600
Casar JC, Cabello-Verrugio C, Olguin H, Aldunate R, Inestrosa NC, Brandan E (2004) Heparan sulfate proteoglycans are increased during skeletal muscle regeneration: requirement of syndecan-3 for successful fiber formation. J Cell Sci 117(Pt 1):73–84
Cassano M, Biressi S, Finan A, Benedetti L, Omes C, Boratto R, Martin F, Allegretti M, Broccoli V, Cusella De AG, Comoglio PM, Basilico C, Torrente Y, Michieli P, Cossu G, Sampaolesi M (2008) Magic-factor 1, a partial agonist of Met, induces muscle hypertrophy by protecting myogenic progenitors from apoptosis. Plos One 3(9):e3223
Charge SB, Rudnicki MA (2004) Cellular and molecular regulation of muscle regeneration. Physiol Rev 84(1):209–238
Chazaud B (2010) Dual effect of HGF on satellite/myogenic cell quiescence. Focus on “High concentrations of HGF inhibit skeletal muscle satellite cell proliferation in vitro by inducing expression of myostatin: a possible mechanism for reestablishing satellite cell quiescence in vivo”. Am J Physiol Cell Physiol 298(3):C448–C449
Collins CA, Partridge TA (2005) Self-renewal of the adult skeletal muscle satellite cell. Cell Cycle 4(10):1338–1341
Collins CA, Olsen I, Zammit PS, Heslop L, Petrie A, Partridge TA, Morgan JE (2005) Stem cell function, self-renewal, and behavioral heterogeneity of cells from the adult muscle satellite cell niche. Cell 122(2):289–301
Collins CA, Zammit PS, Perez RA, Morgan JE, Partridge TA (2007) A population of myogenic stem cells that survives skeletal muscle aging. Stem Cells 25:885–894
Cornelison DD, Filla MS, Stanley HM, Rapraeger AC, Olwin BB (2001) Syndecan-3 and syndecan-4 specifically mark skeletal muscle satellite cells and are implicated in satellite cell maintenance and muscle regeneration. Dev Biol 239(1):79–94
Cornelison DD, Wilcox-Adelman SA, Goetinck PF, Rauvala H, Rapraeger AC, Olwin BB (2004) Essential and separable roles for Syndecan-3 and Syndecan-4 in skeletal muscle development and regeneration. Genes Dev 18(18):2231–2236
Corrigan LJ, Lucas MC, Winfield IJ, Hoelzel AR (2011) Environmental factors associated with genetic and phenotypic divergence among sympatric populations of Arctic charr (Salvelinus alpinus). J Evol Biol 24:1906–1917
Corti S, Salani S, Del BR, Sironi M, Strazzer S, D’Angelo MG, Comi GP, Bresolin N, Scarlato G (2001) Chemotactic factors enhance myogenic cell migration across an endothelial monolayer. Exp Cell Res 268(1):36–44
Crisp M, Liu Q, Roux K, Rattner JB, Shanahan C, Burke B, Stahl PD, Hodzic D (2006) Coupling of the nucleus and cytoplasm: role of the LINC complex. J Cell Biol 172(1):41–53
Dhawan J, Rando TA (2005) Stem cells in postnatal myogenesis: molecular mechanisms of satellite cell quiescence, activation and replenishment. Trends Cell Biol 15(12):666–673
Do MK, Sato Y, Shimizu N, Suzuki T, Shono J, Mizunoya W, Nakamura M, Ikeuchi Y, Anderson JE, Tatsumi R (2011) Growth factor regulation of neural chemorepellent Sema3A expression in satellite cell cultures. Am J Physiol Cell Physiol 301(5):C1270–C1279
Do MK, Suzuki T, Gerelt B, Sato Y, Mizunoya W, Nakamura M, Ikeuchi Y, Anderson JE, Tatsumi R (2012) Time-coordinated prevalence of extracellular HGF, FGF2 and TGF-beta3 in crush-injured skeletal muscle. Anim Sci J 83(10):712–717
Dumont NA, Wang YX, von Maltazahn J, Pasut A, Bentzinger CF, Brun CE, Rudnicki MA (2015) Dystrophin expression in muscle stem cells regulates their polarity and asymmetric division. Nat Med 21(12):1455–1463
Durbeej M, Campbell KP (2002) Muscular dystrophies involving the dystrophin-glycoprotein complex: an overview of current mouse models. Curr Opin Genet Dev 12(3):349–361
Duxson MJ, Sheard PW (1995) Formation of new myotubes occurs exclusively at the multiple innervation zones of an embryonic large muscle. Dev Dyn 204(4):391–405
Duxson MJ, Ross JJ, Harris AJ (1986) Transfer of differentiated synaptic terminals from primary myotubes to new-formed muscle cells during embryonic development in the rat. Neurosci Lett 71(2):147–152
Ervasti JM, Campbell KP (1991) Membrane organization of the dystrophin-glycoprotein complex. Cell 66(6):1121–1131
Ervasti JM, Campbell KP (1993) A role for the dystrophin-glycoprotein complex as a transmembrane linker between laminin and actin. J Cell Biol 122(4):809–823
Ferrara N, Gerber HP, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9(6):669–676
Fibbi G, D’Alessio S, Pucci M, Cerletti M, Del RM (2002) Growth factor-dependent proliferation and invasion of muscle satellite cells require the cell-associated fibrinolytic system. Biol Chem 383(1):127–136
Flann KL, Rathbone CR, Cole LC, Liu X, Allen RE, Rhoads RP (2014) Hypoxia simultaneously alters satellite cell-mediated angiogenesis and hepatocyte growth factor expression. J Cell Physiol 229(5):572–579
Florini JR, Magri KA (1989) Effects of growth factors on myogenic differentiation. Am J Physiol 256(4) Pt 1:C701–C711
Fukada S, Morikawa D, Yamamoto Y, Yoshida T, Sumie N, Yamaguchi M, Ito T, Miyagoe-Suzuki Y, Takeda S, Tsujikawa K, Yamamoto H (2010) Genetic background affects properties of satellite cells and mdx phenotypes. Am J Pathol 176(5):2414–2424
Fukada S, Ma Y, Ohtani T, Watanabe Y, Murakami S, Yamaguchi M (2013) Isolation, characterization, and molecular regulation of muscle stem cells. Front Physiol 4:317
Gal-Levi R, Leshem Y, Aoki S, Nakamura T, Halevy O (1998) Hepatocyte growth factor plays a dual role in regulating skeletal muscle satellite cell proliferation and differentiation. Biochim Biophys Acta 1402(1):39–51
Grounds MD (1987) Phagocytosis of necrotic muscle in muscle isografts is influenced by the strain, age, and sex of host mice. J Pathol 153(1):71–82
Grounds MD, McGeachie JK (1987) A model of myogenesis in vivo, derived from detailed autoradiographic studies of regenerating skeletal muscle, challenges the concept of quantal mitosis. Cell Tissue Res 250(3):563–569
Grounds MD, McGeachie JK (1992) Skeletal muscle regeneration after crush injury in dystrophic mdx mice: an autoradiographic study. Muscle Nerve 15(5):580–586
Grounds MD, Garrett KL, Lai MC, Wright WE, Beilharz MW (1992) Identification of skeletal muscle precursor cells in vivo by use of MyoD1 and myogenin probes. Cell Tissue Res 267(1):99–104
Gutierrez J, Cabrera D, Brandan E (2014) Glypican-1 regulates myoblast response to HGF via Met in a lipid raft-dependent mechanism: effect on migration of skeletal muscle precursor cells. Skelet Muscle 4(1):5
Hall TE, Smith P, Johnston IA (2004) Stages of embryonic development in the Atlantic cod Gadus morhua. J Morphol 259(3):255–270
Hara M, Tabata K, Suzuki T, Do MK, Mizunoya W, Nakamura M, Nishimura S, Tabata S, Ikeuchi Y, Sunagawa K, Anderson JE, Allen RE, Tatsumi R (2012) Calcium influx through a possible coupling of cation channels impacts skeletal muscle satellite cell activation in response to mechanical stretch. Am J Physiol Cell Physiol 302(12):C1741–C1750
Harris AJ, Duxson MJ, Fitzsimons RB, Rieger F (1989) Myonuclear birthdates distinguish the origins of primary and secondary myotubes in embryonic mammalian skeletal muscles. Development 107(4):771–784
Hayashi S, Aso H, Watanabe K, Nara H, Rose MT, Ohwada S, Yamaguchi T (2004) Sequence of IGF-I, IGF-II, and HGF expression in regenerating skeletal muscle. Histochem Cell Biol 122(5):427–434
Heslop L, Morgan JE, Partridge TA (2000) Evidence for a myogenic stem cell that is exhausted in dystrophic muscle. J Cell Sci 113(Pt 12):2299–2308
Huang Z, Chen X, Yu B, He J, Chen D (2012) MicroRNA-27a promotes myoblast proliferation by targeting myostatin. Biochem Biophys Res Commun 423(2):265–269
Ieronimakis N, Balasundaram G, Rainey S, Srirangam K, Yablonka-Reuveni Z, Reyes M (2010) Absence of CD34 on murine skeletal muscle satellite cells marks a reversible state of activation during acute injury. PLoS One 5(6):e10920
Janke A, Upadhaya R, Snow WM, Anderson JE (2013) A new look at cytoskeletal NOS-1 and â-dystroglycan changes in developing muscle and brain in control and mdx dystrophic mice. Dev Dyn 242(12):1369–1381. doi:10.1002/dvdy.24031
Jansen JK, Fladby T (1990) The perinatal reorganization of the innervation of skeletal muscle in mammals. Prog Neurobiol 34(1):39–90
Jennische E, Ekberg S, Matejka GL (1993) Expression of hepatocyte growth factor in growing and regenerating rat skeletal muscle. Am J Physiol 265(1) Pt 1;C122–C128
Johnson SE, Allen RE (1993) Proliferating cell nuclear antigen (PCNA) is expressed in activated rat skeletal muscle satellite cells. J Cell Physiol 154(1):39–43
Johnson SE, Allen RE (1995) Activation of skeletal muscle satellite cells and the role of fibroblast growth factor receptors. Exp Cell Res 219(2):449–453
Johnston IA (2006) Environment and plasticity of myogenesis in teleost fish. J Exp Biol 209(Pt 12):2249–2264
Johnston IA, Hall TE (2004) Mechanisms of muscle development and responses to temperature change in fish larvae. In: Govoni JJ (ed) Development of form and function in fishes and the question of larval adaptation [40], pp 85–116. American Fisheries Society Symposium. Ref Type: Serial (Book, Monograph)
Johnston IA, Lee HT, Macqueen DJ, Paranthaman K, Kawashima C, Anwar A, Kinghorn JR, Dalmay T (2009) Embryonic temperature affects muscle fibre recruitment in adult zebrafish: genome-wide changes in gene and microRNA expression associated with the transition from hyperplastic to hypertrophic growth phenotypes. J Exp Biol 212(Pt 12):1781–1793
Johnston IA, Bower NI, Macqueen DJ (2011) Growth and the regulation of myotomal muscle mass in teleost fish. J Exp Biol 214(Pt 10):1617–1628
Karalaki M, Fili S, Philippou A, Koutsilieris M (2009) Muscle regeneration: cellular and molecular events. In Vivo 23(5):779–796
Kawamura K, Takano K, Suetsugu S, Kurisu S, Yamazaki D, Miki H, Takenawa T, Endo T (2004) N-WASP and WAVE2 acting downstream of phosphatidylinositol 3-kinase are required for myogenic cell migration induced by hepatocyte growth factor. J Biol Chem 279(52):54862–54871
Kuang S, Kuroda K, Le GF, Rudnicki MA (2007) Asymmetric self-renewal and commitment of satellite stem cells in muscle. Cell 129(5):999–1010
Lee AS, Anderson JE, Joya JE, Head SI, Pather N, Kee AJ, Gunning PW, Hardeman EC (2013) Aged skeletal muscle retains the ability to fully regenerate functional architecture. Bioarchitecture 3(2):25–37
Leiter JR, Anderson JE (2010) Satellite cells are increasingly refractory to activation by nitric oxide and stretch in aged mouse-muscle cultures. Int J Biochem Cell Biol 42:132–136
Leiter JR, Peeler J, Anderson JE (2011) Exercise-induced muscle growth is muscle-specific and age-dependent. Muscle Nerve 43(6):828–838
Leiter JR, Upadhaya R, Anderson JE (2012) Nitric oxide and voluntary exercise together promote quadriceps hypertrophy and increase vascular density in female 18-mo-old mice. Am J Physiol Cell Physiol 302(9):C1306–C1315
Leshem Y, Spicer DB, Gal-Levi R, Halevy O (2000) Hepatocyte growth factor (HGF) inhibits skeletal muscle cell differentiation: a role for the bHLH protein twist and the cdk inhibitor p27. J Cell Physiol 184(1):101–109
Li Z, Peng J, Wang G, Yang Q, Yu H, Guo Q, Wang A, Zhao B, Lu S (2008) Effects of local release of hepatocyte growth factor on peripheral nerve regeneration in acellular nerve grafts. Exp Neurol 214(1):47–54
Lin DC, Hershey JD, Mattoon JS, Robbins CT (2012) Skeletal muscles of hibernating brown bears are unusually resistant to effects of denervation. J Exp Biol 215(12):2081–2087
Lomo T (2003) What controls the position, number, size, and distribution of neuromuscular junctions on rat muscle fibers? J Neurocytol 32(5–8):835–848
Luo D, Renault VM, Rando TA (2005) The regulation of Notch signaling in muscle stem cell activation and postnatal myogenesis. Semin Cell Dev Biol 16(4-5):612–622
Matsumura K, Ohlendieck K, Ionasescu VV, Tome FM, Nonaka I, Burghes AH, Mora M, Kaplan JC, Fardeau M, Campbell KP (1993) The role of the dystrophin-glycoprotein complex in the molecular pathogenesis of muscular dystrophies. Neuromuscul Disord 3(5–6):533–535
Mauro A (1961) Satellite cell of skeletal muscle fibers. J Biophys Biochem Cytol 9:493–495
Mauro A, Shafiq SA, Milhorat AT (1970) Regeneration of striated muscle, and myogenesis. Ekcerpta Medica, Amsterdam
McGeachie JK, Grounds MD (1987) Initiation and duration of muscle precursor replication after mild and severe injury to skeletal muscle of mice. An autoradiographic study. Cell Tissue Res 248(1):125–130
McIntosh L, Granberg KE, Briere KM, Anderson JE (1998a) Nuclear magnetic resonance spectroscopy study of muscle growth, mdx dystrophy and glucocorticoid treatments: correlation with repair. NMR Biomed 11(1):1–10
McIntosh LM, Baker RE, Anderson JE (1998b) Magnetic resonance imaging of regenerating and dystrophic mouse muscle. Biochem Cell Biol 76(2–3):532–541
McIntosh LM, Garrett KL, Megeney L, Rudnicki MA, Anderson JE (1998c) Regeneration and myogenic cell proliferation correlate with taurine levels in dystrophin- and MyoD-deficient muscles. Anat Rec 252(2):311–324
Merly F, Lescaudron L, Rouaud T, Crossin F, Gardahaut MF (1999) Macrophages enhance muscle satellite cell proliferation and delay their differentiation. Muscle Nerve 22(6):724–732
Merrifield P, Atkinson BG (2000) Phylogenetic diversity of myosin expression in muscle. Microsc Res Tech 50(6):425–429
Meyerrochow VB, Ingram JR (1993) Red white muscle distribution and fiber growth dynamics – a comparison between Lacustrine and Riverine populations of the Southern smelt Retropinna-Retropinna Richardson. Proc Biol Sci 252(1334):85–92
Miller KJ, Thaloor D, Matteson S, Pavlath GK (2000) Hepatocyte growth factor affects satellite cell activation and differentiation in regenerating skeletal muscle. Am J Physiol Cell Physiol 278(1):C174–C181
Missias AC, Chu GC, Klocke BJ, Sanes JR, Merlie JP (1996) Maturation of the acetylcholine receptor in skeletal muscle: regulation of the AChR gamma-to-epsilon switch. Dev Biol 179(1):223–238
Moor AN, Rector ES, Anderson JE (2000) Cell cycle behavior and MyoD expression in response to T3 differ in normal and mdx dystrophic primary muscle cell cultures. Microsc Res Tech 48(3–4):204–212
Mylona E, Jones KA, Mills ST, Pavlath GK (2006) CD44 regulates myoblast migration and differentiation. J Cell Physiol 209(2):314–321
O’Brien LE, Tang K, Kats ES, Schutz-Geschwender A, Lipschutz JH, Mostov KE (2004) ERK and MMPs sequentially regulate distinct stages of epithelial tubule development. Dev Cell 7(1):21–32
Paul AC, Sheard PW, Duxson MJ (2004) Development of a mammalian series-fibered muscle. Anat Rec A Discov Mol Cell Evol Biol 278(2):571–578
Peplow PV, Chatterjee MP (2013) A review of the influence of growth factors and cytokines in in vitro human keratinocyte migration. Cytokine 62(1):1–21
Pezzementi L, Chatonnet A (2010) Evolution of cholinesterases in the animal kingdom. Chem Biol Interact 187:27–33. Ref Type: Journal (Full)
Pisconti A, Cornelison DD, Olguin HC, Antwine TL, Olwin BB (2010) Syndecan-3 and Notch cooperate in regulating adult myogenesis. J Cell Biol 190(3):427–441
Price ER, Bauchinger U, Zajac DM, Cerasale DJ, McFarlan JT, Gerson AR, McWilliams SR, Guglielmo CG (2011) Migration- and exercise-induced changes to flight muscle size in migratory birds and association with IGF1 and myostatin mRNA expression. J Exp Biol 214(17):2823–2831
Ramani VC, Purushothaman A, Stewart MD, Thompson CA, Vlodavsky I, Au JL, Sanderson RD (2013) The heparanase/syndecan-1 axis in cancer: mechanisms and therapies. FEBS J 280(10):2294–2306
Rapraeger AC (2000) Syndecan-regulated receptor signaling. J Cell Biol 149(5):995–998
Reed SA, Sandesara PB, Senf SM, Judge AR (2012) Inhibition of FoxO transcriptional activity prevents muscle fiber atrophy during cachexia and induces hypertrophy. FASEB J 26(3):987–1000
Roux KJ, Crisp ML, Liu Q, Kim D, Kozlov S, Stewart CL, Burke B (2009) Nesprin 4 is an outer nuclear membrane protein that can induce kinesin-mediated cell polarization. Proc Natl Acad Sci U S A 106(7):2194–2199
Rudnicki MA, Le GF, McKinnell I, Kuang S (2008) The molecular regulation of muscle stem cell function. Cold Spring Harb Symp Quant Biol 73:323–331
Sakaguchi S, Shono JI, Suzuki T, Sawano S, Anderson JE, Do MK, Ohtsubo H, Mizunoya W, Sato Y, Nakamura M, Furuse M, Yamada K, Ikeuchi Y, Tatsumi R (2014) Implication of anti-inflammatory macrophages in regenerative moto-neuritogenesis: promotion of myoblast migration and neural chemorepellent semaphorin 3A expression in injured muscle. Int J Biochem Cell Biol 54:272–285
Seale P, Rudnicki MA (2000) A new look at the origin, function, and “stem-cell” status of muscle satellite cells. Dev Biol 218(2):115–124
Seale P, Sabourin LA, Girgis-Gabardo A, Mansouri A, Gruss P, Rudnicki MA (2000) Pax7 is required for the specification of myogenic satellite cells. Cell 102(6):777–786
Sebastian S, Sreenivas P, Sambasivan R, Cheedipudi S, Kandalla P, Pavlath GK, Dhawan J (2009) MLL5, a trithorax homolog, indirectly regulates H3K4 methylation, represses cyclin A2 expression, and promotes myogenic differentiation. Proc Natl Acad Sci U S A 106(12):4719–4724
Sellathurai J, Cheedipudi S, Dhawan J, Schroder HD (2013) A novel in vitro model for studying quiescence and activation of primary isolated human myoblasts. Plos One 8(5):e64067
Sheehan SM, Tatsumi R, Temm-Grove CJ, Allen RE (2000) HGF is an autocrine growth factor for skeletal muscle satellite cells in vitro. Muscle Nerve 23(2):239–245
Siegel AL, Atchison K, Fisher KE, Davis GE, Cornelison DD (2009) 3D timelapse analysis of muscle satellite cell motility. Stem Cells 27(10):2527–2538
Siegel AL, Kuhlmann PK, Cornelison DD (2011) Muscle satellite cell proliferation and association: new insights from myofiber time-lapse imaging. Skelet Muscle 1(1):1–7
Smith CK, Janney MJ, Allen RE (1994) Temporal expression of myogenic regulatory genes during activation, proliferation, and differentiation of rat skeletal muscle satellite cells. J Cell Physiol 159(2):379–385
Smythe GM, Shavlakadze T, Roberts P, Davies MJ, McGeachie JK, Grounds MD (2008) Age influences the early events of skeletal muscle regeneration: studies of whole muscle grafts transplanted between young (8 weeks) and old (13–21 months) mice. Exp Gerontol 43(6):550–562
Snow WM, Anderson JE, Jakobson LS (2013a) Neuropsychological and neurobehavioral functioning in Duchenne muscular dystrophy: a review. Neurosci Biobehav Rev 37(5):743–752
Snow WM, Fry M, Anderson JE (2013b) Increased density of dystrophin protein in the lateral versus the vermal mouse cerebellum. Cell Mol Neurobiol 33(4):513–520
Srivastava S, Mishra RK, Dhawan J (2010) Regulation of cellular chromatin state: insights from quiescence and differentiation. Organogenesis 6(1):37–47
Stark DA, Karvas RM, Siegel AL, Cornelison DD (2011) Eph/ephrin interactions modulate muscle satellite cell motility and patterning. Development 138(24):5279–5289
Starr DA, Fischer JA (2005) KASH ’n Karry: the KASH domain family of cargo-specific cytoskeletal adaptor proteins. Bioessays 27(11):1136–1146
Steinbacher P, Marschallinger J, Obermayer A, Neuhofer A, Sanger AM, Stoiber W (2011) Temperature-dependent modification of muscle precursor cell behaviour is an underlying reason for lasting effects on muscle cellularity and body growth of teleost fish. J Exp Biol 214(Pt 11):1791–1801
Subramaniam S, Sreenivas P, Cheedipudi S, Reddy VR, Shashidhara LS, Chilukoti RK, Mylavarapu M, Dhawan J (2013) Distinct transcriptional networks in quiescent myoblasts: a role for Wnt signaling in reversible vs. irreversible arrest. Plos One 8(6):e65097
Sugiura T, Kawaguchi Y, Soejima M, Katsumata Y, Gono T, Baba S, Kawamoto M, Murakawa Y, Yamanaka H, Hara M (2010) Increased HGF and c-Met in muscle tissues of polymyositis and dermatomyositis patients: beneficial roles of HGF in muscle regeneration. Clin Immunol 136(3):387–399
Sumino Y, Hirata Y, Sato F, Mimata H (2007) Growth mechanism of satellite cells in human urethral rhabdosphincter. Neurourol Urodyn 26(4):552–561
Suzuki S, Yamanouchi K, Soeta C, Katakai Y, Harada R, Naito K, Tojo H (2002) Skeletal muscle injury induces hepatocyte growth factor expression in spleen. Biochem Biophys Res Commun 292(3):709–714
Suzuki T, Do MK, Sato Y, Ojima K, Hara M, Mizunoya W, Nakamura M, Furuse M, Ikeuchi Y, Anderson JE, Tatsumi R (2013) Comparative analysis of semaphorin 3A in soleus and EDL muscle satellite cells in vitro toward understanding its role in modulating myogenin expression. Int J Biochem Cell Biol 45(2):476–482
Tatsumi R (2010) Mechano-biology of skeletal muscle hypertrophy and regeneration: possible mechanism of stretch-induced activation of resident myogenic stem cells. Anim Sci J 81(1):11–20
Tatsumi R, Allen RE (2004) Active hepatocyte growth factor is present in skeletal muscle extracellular matrix. Muscle Nerve 30(5):654–658
Tatsumi R, Anderson JE, Nevoret CJ, Halevy O, Allen RE (1998) HGF/SF is present in normal adult skeletal muscle and is capable of activating satellite cells. Dev Biol 194(1):114–128
Tatsumi R, Sheehan SM, Iwasaki H, Hattori A, Allen RE (2001) Mechanical stretch induces activation of skeletal muscle satellite cells in vitro. Exp Cell Res 267(1):107–114
Tatsumi R, Hattori A, Ikeuchi Y, Anderson JE, Allen RE (2002) Release of hepatocyte growth factor from mechanically stretched skeletal muscle satellite cells and role of pH and nitric oxide. Mol Biol Cell 13(8):2909–2918
Tatsumi R, Sankoda Y, Anderson JE, Sato Y, Mizunoya W, Shimizu N, Suzuki T, Yamada M, Rhoads RP Jr, Ikeuchi Y, Allen RE (2009a) Possible implication of satellite cells in regenerative motoneuritogenesis: HGF upregulates neural chemorepellent Sema3A during myogenic differentiation. Am J Physiol Cell Physiol 297(2):C238–C252
Tatsumi R, Wuollet al, Tabata K, Nishimura S, Tabata S, Mizunoya W, Ikeuchi Y, Allen RE (2009b) A role for calcium-calmodulin in regulating nitric oxide production during skeletal muscle satellite cell activation. Am J Physiol Cell Physiol 296(4):C922–C929
Thomas M, Langley B, Berry C, Sharma M, Kirk S, Bass J, Kambadur R (2000) Myostatin, a negative regulator of muscle growth, functions by inhibiting myoblast proliferation. J Biol Chem 275(51):40235–40243
Trusolino L, Bertotti A, Comoglio PM (2010) MET signalling: principles and functions in development, organ regeneration and cancer. Nat Rev Mol Cell Biol 11(12):834–848
Tzur YB, Wilson KL, Gruenbaum Y (2006) SUN-domain proteins: ‘Velcro’ that links the nucleoskeleton to the cytoskeleton. Nat Rev Mol Cell Biol 7(10):782–788
Villena J, Brandan E (2004) Dermatan sulfate exerts an enhanced growth factor response on skeletal muscle satellite cell proliferation and migration. J Cell Physiol 198(2):169–178
Volonte D, Liu Y, Galbiati F (2005) The modulation of caveolin-1 expression controls satellite cell activation during muscle repair. FASEB J 19(2):237–239
Watanabe I, Okada S (1967) Stationary phase of cultured mammalian cells (L5178Y). J Cell Biol 35(2):285–294
Webster MT, Fan CM (2013) c-MET regulates myoblast motility and myocyte fusion during adult skeletal muscle regeneration. PLoS One 8(11):e81757
Williams RS, Annex BH (2004) Plasticity of myocytes and capillaries: a possible coordinating role for VEGF. Circ Res 95(1):7–8
Wozniak AC, Anderson JE (2005) Single-fiber isolation and maintenance of satellite cell quiescence. Biochem Cell Biol 83(5):674–676
Wozniak AC, Anderson JE (2007) Nitric oxide-dependence of satellite stem cell activation and quiescence on normal skeletal muscle fibers. Dev Dyn 236(1):240–250
Wozniak AC, Anderson JE (2009) The dynamics of the nitric oxide release-transient from stretched muscle cells. Int J Biochem Cell Biol 41(3):625–631
Wozniak AC, Pilipowicz O, Yablonka-Reuveni Z, Greenway S, Craven S, Scott E, Anderson JE (2003) C-met expression and mechanical activation of satellite cells on cultured muscle fibers. J Histochem Cytochem 51(11):1437–1445
Wozniak AC, Kong J, Bock E, Pilipowicz O, Anderson JE (2005) Signaling satellite-cell activation in skeletal muscle: markers, models, stretch, and potential alternate pathways. Muscle Nerve 31(3):283–300
Wund MA, Baker JA, Clancy B, Golub JL, Foster SA (2008) A test of the “Flexible stem” model of evolution: ancestral plasticity, genetic accommodation, and morphological divergence in the threespine stickleback radiation. Am Nat 172:449–462
Xie G, Karaca G, Swiderska-Syn M, Michelotti GA, Kruger L, Chen Y, Premont RT, Choi SS, Diehl AM (2013) Cross-talk between notch and hedgehog regulates hepatic stellate cell fate. Hepatology 58(5):1801–1813
Yablonka-Reuveni Z (2011) The skeletal muscle satellite cell: still young and fascinating at 50. J Histochem Cytochem 59(12):1041–1059
Yamada M, Tatsumi R, Yamanouchi K, Hosoyama T, Shiratsuchi S, Sato A, Mizunoya W, Ikeuchi Y, Furuse M, Allen RE (2010) High concentrations of HGF inhibit skeletal muscle satellite cell proliferation in vitro by inducing expression of myostatin: a possible mechanism for reestablishing satellite cell quiescence in vivo. Am J Physiol Cell Physiol 298(3):C465–C476
Zhang H, Anderson JE (2014) Satellite cell activation and populations on single muscle-fiber cultures from adult zebrafish (Danio rerio). J Exp Biol 217(Pt 11):1910–1917
Zhang X, Xu R, Zhu B, Yang X, Ding X, Duan S, Xu T, Zhuang Y, Han M (2007) Syne-1 and Syne-2 play crucial roles in myonuclear anchorage and motor neuron innervation. Development 134(5):901–908
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Anderson, J.E. (2016). Hepatocyte Growth Factor and Satellite Cell Activation. In: White, J., Smythe, G. (eds) Growth Factors and Cytokines in Skeletal Muscle Development, Growth, Regeneration and Disease. Advances in Experimental Medicine and Biology, vol 900. Springer, Cham. https://doi.org/10.1007/978-3-319-27511-6_1
Download citation
DOI: https://doi.org/10.1007/978-3-319-27511-6_1
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-27509-3
Online ISBN: 978-3-319-27511-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)