Abstract
In this chapter, we concentrate on aging as a risk factor for diabetes and diabetes as a risk factor for additional age-related diseases, and provide an overview of the role of insulin signaling/action in the control of mammalian aging. We discuss current knowledge regarding the possible causes of altered glucose homeostasis during aging, including decreased mitochondrial function, lipotoxicity, and inflammation. Also, we review findings from studies that suggest that therapies used to prevent and treat diabetes, such as metformin and physical activity, also may have more global effects to modulate aging, and therefore be used against many aging-related diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Age is a major risk factor for type 2 diabetes mellitus (T2DM), similarly to what is known about the etiology of most chronic diseases. Indeed, before the recent “epidemic” of childhood and adolescent obesity, T2DM was called “adult onset diabetes.” The importance of chronological age as a risk factor for T2DM is only one of many links between diabetes and aging. The genetic and environmental control of the biological process of aging is intertwined with the development and consequences of T2DM in a highly complex network of interactions that are probably unique to diabetes.
Symptoms and diagnosis of T2DM reflect failure of insulin-secreting pancreatic β cells on the background of progressive increase in insulin resistance in target tissues. Insulin resistance commonly accompanies aging, although it is not clear whether insulin resistance is primarily a cause or a consequence of aging and whether it represents a protective/compensatory response to hyperinsulinemia [9]. While controversy persists about the role of aging in insulin resistance, and vice versa, it is widely accepted that maintaining insulin sensitivity through physical activity or pharmacological agents can prevent/delay the development of T2DM in high-risk young and older adults [84].
There is considerable evidence that insulin and homologous hormones in invertebrate species are intricately involved in the control of aging and lifespan [62, 124]. In experimental organisms ranging from yeast to mice, reducing (but not eliminating) insulin/insulin-like growth factor (IGF) signaling by genetic or dietary means can lead to slower aging, reduced susceptibility to age-related disease and significant, often remarkably large, extension of longevity. The increase in longevity can be quite impressive – more than twofold increase in C. elegans and more than 1.5-fold increase in mice. Importantly, a role of insulin/IGF signaling in the control of aging and longevity also applies to primates, including humans [106, 133]. The beneficial effects of reduced insulin/IGF signaling on longevity could be viewed as the first paradox in the relationship between insulin and aging. A severe reduction of the capacity to produce insulin leads to diabetes, a serious, life-threatening disease. In contrast, chronic hypoinsulinemia induced by calorie restriction or mutations related to growth hormone (GH) signaling are associated, most likely causally, with delayed aging and long, healthy life.
The complex interplay between insulin action, diabetes and aging does not end here. Progression of T2DM, with its practically unavoidable deterioration of glucose homeostasis, is associated with the emergence of functional deficits and pathological alterations that typically accompany aging [35]. Indeed, many diabetologists view accelerated aging as a result of T2DM (as well as type 1 diabetes) and believe that patients with T2DM are physiologically older than their chronological age. This difference may be as great as 10 years or, for new patients, approximately 1 year for each year since the diagnosis of their disease. This relationship between T2DM and aging at times has been emphasized by the simple but powerful statement that “diabetes is accelerated aging” [DeFronzo, RA, personal communication]. Although a disease (diabetes) cannot be equated with a physiological process (aging), it is indeed striking that some of their consequences are very similar. Regarding accelerated aging as one of the consequences of diabetes is consistent with many clinical and epidemiological findings. It is also important to remember that diabetes disturbs insulin secretion and its intracellular actions, which are mediated by signaling pathways known to be involved in the control of aging.
In terms of broader relationships between aging and disease as embodied in the concept of geroscience and explored throughout this volume, the suggestion that diabetes may lead to accelerated aging is extremely important. It provides a mechanistic explanation of why diabetes, similarly to chronological age, increases the risk for cardiovascular disease, cancer, frailty and dementia. Uncovering cause:effect relationships between insulin signaling, aging and diabetes is greatly complicated by the fact that circulating insulin concentration and insulin sensitivity are mutually dependent and both are altered in pre-diabetic conditions such as glucose intolerance and the metabolic syndrome, and in patients with T2DM. Although chronic insulin exposure promotes insulin resistance by well-known mechanisms, insulin resistance coexists with insulin deficiency in T2DM; meanwhile long-lived mice with GH-related mutations and offspring of exceptionally long-lived people exhibit reductions in both insulin levels and insulin resistance [8, 133]. These relationships are further complicated by differential alterations in insulin sensitivity and various steps of insulin signaling in different organs of the same individual [19], as well as by the emerging evidence that insulin resistance can be either detrimental or protective [10]. Is this another paradox related to diabetes?
Discussion of the interplay between aging and diabetes would not be complete without a reference to obesity. Aging is associated with progressive changes in the distribution and secretory activity of adipose tissue, as well as adipogenesis and adipocyte senescence, and most often also with a gradual, often very striking increase in adiposity [125]. Obesity is one of the important features of metabolic syndrome and a key risk factor for T2DM. It is also independently associated with an increased risk of cancer and cardiovascular disease, thus resembling the effects of both aging and diabetes. In turn, regulation of lipid metabolism, food intake and adiposity are disturbed in T2DM.
2 Studies in Experimental Animals Link Glucose Homeostasis and Insulin Signaling with Healthy Aging and Longevity
2.1 Animals with Reduced Longevity
Much of the evidence for causal links between glucose homeostasis and aging is derived from mice with genetic or dietary interventions that alter insulin signaling. In this species, obesity induced either by mutations or high-fat diet (HFD) leads to a reduced lifespan, as well as insulin resistance, diabetes and functional deficits resembling those that normally occur during aging [95, 96, 121]. Mice with morbid obesity due to hereditary deficiency of leptin or leptin receptors provide a particularly striking example of these associations [67, 89, 102]. Animals heterozygous for the lethal yellow (AY) mutation at the agouti locus (often referred to as “agouti mice”) are obese, hyperinsulinemic and hyperglycemic and more likely to develop cancer, an aging-related disease [134].
Interestingly, some genetic interventions allow dissociating abnormal glucose homeostasis and accelerated aging from obesity. Transgenic mice overexpressing growth hormone (GH) have reduced adiposity (percent of body fat) during most of their adult life [103], are insulin resistant and hyperinsulinemic, live much shorter than their genetically normal siblings, and exhibit numerous characteristics resembling aging that develop at an inappropriately early chronological age [6]. Pertinent to the subject of this chapter, these “giant mice” are more susceptible to age-related diseases including kidney inflammatory disease, glomerulosclerosis and cancer [129]. Moreover, blood pressure is elevated in these insulin-resistant transgenic mice [78].
2.2 Animals with Extended Longevity
Causal relationships between insulin signaling, glucose homeostasis, age-associated disease and longevity are strongly supported by studies in mice in which somatotropic signaling is suppressed by spontaneous mutations or targeted gene disruptions. Remarkable extension of average and maximal longevity of mice of both sexes lacking GH or GH receptors is associated with enhanced insulin sensitivity, reduced or “low-normal” levels of blood glucose, and resistance to the detrimental impact of high-fat diet on insulin signaling [8, 22, 90]. These characteristics, together with reduced blood pressure [57], could be described as a phenotype opposite to metabolic syndrome or “prediabetes.” Importantly, these animals exhibit numerous features of delayed aging, including improved maintenance of cognitive, immune and neuromuscular function, collagen properties and glucose homeostasis at the age when these parameters exhibit decline in their normal (wild type) siblings [8, 22]. Incidence of cancer and various pathological changes associated with aging are delayed and/or reduced in these insulin-sensitive, long-lived mutants [73, 74].
Our hypothesis that improved insulin signaling/action is one of the key mechanisms responsible for extension of longevity in GH-related mutants was supported by experiments exposing these animals to calorie restriction (CR) throughout most of their post-natal lives. In most strains of mice, CR increases insulin sensitivity, slows aging and extends longevity. In Ames dwarf mice, which lack GH, CR led to a further increase in insulin sensitivity and further extension of their already remarkably long lifespan [7]. In contrast, in GH-resistant GHRKO (a.k.a. “Laron dwarf”) mice, CR did not further increase insulin action (Fig. 1), had no effect on longevity in males and caused a small increase in maximal (but not average) longevity in females [18]. Additional evidence for a cause:effect relationship between insulin signaling and aging was obtained in a recent study in which experimental suppression of insulin sensitivity in long-lived GHRKO mice attenuated phenotypic markers of delayed aging [4]. In contrast to these observations, mice with deletion of insulin receptor substrate 1 (IRS1 −/−) and transgenic mice overexpressing klotho are long-lived in spite of enhanced rather than reduced insulin resistance [86, 116]. It was suggested that insulin resistance may act to reduce the strength of the insulin signals [86] or protect target organs from excessive insulin exposure [9]. Similarly, fat tissue-specific insulin receptor knockout (FIRKO) mice are long-lived in spite of insulin resistance of adipocytes and perhaps also macrophages [16], and rapamycin treatment extends longevity in mice even though it can reduce insulin sensitivity [68]. However, rapamycin’s effects on insulin signaling depend on the dose and duration of treatment [49]. From the data available to date, it is possible to conclude that a combination of reduced insulin levels and enhanced insulin sensitivity might emerge as one of the key mechanisms leading to delayed and healthy aging in mice with GH-related mutations as well as in various species of animals subjected to CR.
Phosphorylation of Akt1 and Akt2 in response to acute insulin stimulation in the skeletal muscle of long-lived growth hormone receptor deleted (GHRKO; KO) and normal (N) male mice fed ad libitum (AL) or subjected to chronic 30 % calorie restriction (CR). Results indicate that GHRKO mice are more insulin sensitive than N (control animals). CR produces the expected increase in insulin sensitivity of N mice but no further increase in the GHRKO mutants. Importantly, this CR regimen extends longevity in N but not in GHRKO males [19]
3 Role of Adiposity
Interestingly, studies in long-lived mutant mice allowed dissociation of the effects of insulin signaling on aging from the effects of obesity. In contrast to animals subjected to CR, long-lived GH-related mutants have increased rather than reduced adiposity [13]. Examination of the adipose tissue expression of pro- and anti-inflammatory cytokines and their circulating levels along with the effects of surgical removal of most of the intra-abdominal (visceral) fat in these animals provided evidence suggesting that insulin resistance is not determined by the amount of adipose tissue but by its secretory profile [94]. Long-lived mice with GH-related mutations have unexpectedly increased levels of adiponectin and reduced expression of IL-6 and TNFα in spite of their increased adiposity [91, 94]. It is well documented that in addition to its anti-inflammatory and anti-atherogenic effects, adiponectin increases insulin sensitivity [12, 127, 137]. It is possible that increased adiponectin levels, together with reduced levels of pro-inflammatory cytokines and suppressed mechanistic target of rapamycin (mTOR) signaling, provide a likely explanation for increased insulin sensitivity in corpulent or obese GH-deficient and GH-resistant mice.
4 Pathophysiology and Natural History of Type 2 Diabetes
In young and middle-aged individuals, T2DM occurs as a consequence of two pathophysiologic alterations, insulin resistance and β-cell failure. Both genetic and environmental factors (obesity, physical inactivity) contribute to the development of insulin resistance. Resistance to the actions of insulin in skeletal muscle, liver, and adipose tissue appears early in the natural history of the disease. In muscle, insulin resistance is manifested as decreased insulin-mediated glucose disposal; in the liver it is manifested as impaired suppression of hepatic glucose output; and in adipose tissue insulin resistance manifests as increased lipolysis rates, resulting in increased plasma free fatty acid concentration that further impairs insulin action in muscle and liver (i.e. lipotoxicity). During the early stages of insulin resistance, β-cells can compensate by augmenting insulin secretion to maintain normal glucose tolerance. However, in subjects destined to develop diabetes (~10–20 % of all insulin-resistant individuals), the β-cells eventually will fail, leading to the onset of overt diabetes. The resultant hyperglycemia causes a further decline in insulin sensitivity (i.e. glucotoxicity), but it is the progressive β-cell failure that determines the rate of disease progression [44].
5 Aging as a Risk Factor for Type 2 Diabetes
Substantial evidence has demonstrated that increasing age is associated with impaired glucose homeostasis [2, 43, 107]. The Baltimore Longitudinal Study of Aging showed a progressive decline in glucose tolerance from the third through the ninth decade of life [118]. During an oral glucose tolerance test, the mean fasting plasma glucose increased ~1 mg/dl per decade, and the 2 h glucose increased ~5 mg/dl per decade. This decline in glucose tolerance was also evident in the National Health and Nutrition Examination Survey (NHANES) III, which showed that the percentage of physician-diagnosed diabetes (fasting glucose ≥126 mg/dl) is 3.9 % in subjects aged 40–49 years, whereas prevalence increases to 13.2 % in subjects ≥75 years of age [66]. The percentage of subjects with undiagnosed diabetes also increases from 7.1 to 14.1 % within these age groups. Approximately 50–60 % of subjects aged ≥65 have diabetes or impaired glucose tolerance (IGT), and ~25–50 % (depending upon the population) of subjects with IGT will ultimately convert to type 2 diabetes [47], Other than chronological age, the factors responsible for such high prevalence of IGT and T2DM in the aging population are not clear. However, age-dependent decreases in (i) insulin sensitivity and (ii) β cell function are thought to play important roles in the deterioration of glucose homeostasis that occurs with advancing age.
5.1 Molecular Basis for Peripheral Insulin Resistance
As mentioned above, insulin resistance is characteristic of peripheral tissues (i.e. muscle, adipose) from obese and T2DM subjects [43]. The first step in the insulin signaling transduction pathway is binding of insulin to the α subunits of the insulin receptor in the cell surface. The activated insulin receptor then tyrosine phosphorylates and activates downstream insulin receptor substrate (IRS) proteins, such as IRS-1 (IRS-1). Tyrosine phosphorylation of IRS-1 leads to its association with the p85 subunit of phosphatidylinositol 3-kinase (PI-3 kinase) [132]. Activation of PI-3 kinase leads to the phosphorylation/activation of a series of enzymes and proteins, such as phosphoinositide-dependent kinase (PDK)-1, protein kinase C (PKC) λ/ζ, Akt, and the RabGAP protein AS160 [50, 142, 143]. The phosphorylation/activation of these signaling intermediaries results in the translocation of GLUT4 glucose transporters to the cell membrane and the uptake of glucose [50, 142, 143]. A wide array of abnormalities distinguish insulin-resistant muscle from normal muscle, including decreased insulin receptor tyrosine kinase activity, decreased IRS-1-associated tyrosine phosphorylation, and decreased insulin-stimulated PI 3-kinase activation [28, 41, 145]. Other defects reported in insulin-resistant muscle include decreases in insulin-stimulated PKC activity [50], and AS160 phosphorylation [80]. Insulin-mediated GLUT4 translocation also is reduced in insulin resistant subjects [54], due in part to impairments in insulin signaling described above. These molecular abnormalities are strongly correlated with decreased insulin-stimulated glucose disposal in muscle [41, 145]. Some of these cellular processes will be further discussed in Sect. 5.2
Insulin-stimulated glucose transport in muscles from nondiabetic rodents decreases with age [58, 61]. The majority of reports that have examined the effect of age on insulin sensitivity in humans also have demonstrated reduced insulin sensitivity [48]. Some studies have reported that decreased insulin sensitivity with aging is not apparent when results are expressed by lean body mass. However, when glucose disposal is measured using the hyperinsulinemic euglycemic clamp technique over a range of insulin doses, the plasma insulin concentration required to achieve half-maximal glucose disposal is considerably lower in younger compared with older subjects (shift to the right) [112]. This decrease in insulin-stimulated glucose disposal is evident whether glucose disposal rates are plotted per kg of whole body weight or lean body mass. Other dose-response studies using the euglycemic clamp also have shown impaired insulin sensitivity in older subjects [51, 105]. Petersen et al. demonstrated that, in response to physiologic hyperinsulinemia (20 mU/kg.min insulin clamp), older subjects have a ~40 % reduction in peripheral glucose disposal compared to younger subjects who were matched for body mass index (BMI) and lean body mass [105]. Importantly, the impairment in insulin sensitivity in older subjects was still evident when glucose disposal was expressed per lean mass [77]. In addition, peripheral insulin resistance in aging has been demonstrated using other techniques, such as forearm glucose uptake and the frequently sampled intravenous glucose tolerance test (minimal model) [32]. Studies in rodents and human subjects from various groups also have shown that skeletal muscle from aging animals has defects in the insulin transduction pathway as described above [55, 75, 85, 87].
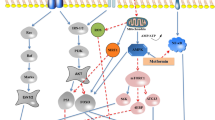
The underlying pathogenic mechanism responsible for the reduction in insulin action that occurs with aging is unclear. Probable factors contributing to age-associated insulin resistance include adiposity/lipotoxicity, inflammation, and mitochondrial dysfunction. These are discussed below and illustrated in Fig. 2.
Model of pathogenesis of muscle insulin resistance with aging. During aging, there is a pro-inflammatory state evidenced by increased expression and activity of mediators such as NFκB and MAP-kinases, caused by elevated levels of inflammatory stimuli, including plasma free fatty acids and endotoxin (which signal via TLR4), intracellular lipids (e.g. ceramides, diacylglycerol), cytokines (e.g. TNFα) and ROS. Decreases in mitochondrial function also contribute by promoting accumulation of intracellular lipids and increased ROS production. The activation of NFκB and MAP-kinases impair insulin action at the Akt and IRS levels, which eventually result in decreased insulin-mediated glucose disposal
5.2 Role of Adiposity/Lipotoxicity on Insulin Resistance
Approximately 30–40 % of older U.S. adults are obese (CDC/NHANES). The high prevalence of obesity in this population is multifactorial, including decreased physical activity, lower oxidative capacity, and muscle wasting. Obesity is associated with impaired glucose metabolism, although the mechanism by which excess adipose tissue alters glucose homeostasis is unclear. Plasma concentration of free fatty acids (FFA) is commonly elevated in older subjects, and several lines of evidence implicate a deleterious effect of elevated plasma FFA level on muscle insulin sensitivity. For example, an experimental elevation of FFA induces muscle insulin resistance in normal glucose-tolerant subjects [17], whereas a reduction in plasma FFA concentrations rapidly ameliorates insulin resistance in insulin-resistant individuals [113]. In addition to the circulation, a variety of approaches has confirmed the existence of increased lipid content in insulin-resistant skeletal muscle [5, 60, 128]. Triglycerides account for most intramyocellular lipids. While triglycerides probably do not impair insulin action per se, metabolites of triglycerides/FFA, particularly diacylglycerol and ceramides, have been shown to have a deleterious effect on insulin action [63, 141]. The cause for the accumulation of intracellular lipids in insulin-resistant muscle is unknown, although one possibility is a reduction in mitochondrial oxidative capacity [105], which appears as a major hallmark of aging (see below). This elevation in intramyocellular lipids is thought to initiate a reverberating negative feedback cycle by decreasing insulin signaling and aggravating the insulin resistance that is already present. Specifically, these intracellular lipid metabolites activate kinases, such as inhibitor κB kinase, protein kinase C, and c-jun N-terminal kinase (JNK), which in turn serine phosphorylate IRS-1, resulting in decreased activation of PI-3 kinase [1, 26, 76].
Numerous studies have examined whether intracellular lipid content varies with normal age. A study in rats found elevated intramyocellular lipid content in aging animals [126]. In humans, studies employing magnetic resonance spectroscopy (MRS) have shown that older subjects also have higher intracellular lipid levels in muscle and liver than younger individuals, and that intramyocellular lipid content correlates closely with peripheral insulin resistance [40, 105]. As in the case for insulin-resistant muscle, the molecular basis for the age-dependent accumulation of intramyocellular fat is also yet to be determined; however, it likely results from an imbalance between the rate of uptake of fatty acids and fat oxidation. Indeed, studies performed in older, nondiabetic subjects have demonstrated that aging is associated with a reduction in basal fat oxidation rates [27, 122].
5.3 Role of Decreased Mitochondrial Function
As mentioned above, aging is accompanied by alterations in various parameters of mitochondrial function and structure. In the context of metabolic diseases such as obesity and type 2 diabetes, particularly relevant are mitochondrial alterations described in skeletal muscle, which is a key tissue responsible for substrate (glucose, FFA) uptake and oxidation. Mitochondrial alterations described in aging muscle include reductions in mitochondrial number, ATP production, and respiration, abnormal structure, and, in some cases, elevated reactive oxygen species generation [reviewed in [79].
The cause for the reduction in mitochondrial function observed with aging is not clear. According to the free radical and mitochondrial theories of aging the decreases in mitochondrial function are the result of cumulative oxidative damage to mitochondrial molecules (mtDNA, proteins, and lipids) [65, 97]. Consistent with this theory, studies performed in human muscle have shown that aging is associated with oxidative damage to mtDNA and proteins [reviewed in 79]. Some [130], albeit not all [55], studies also have found increased lipid peroxidation in muscle from older subjects. Concerning the age-related reductions in oxidative capacity, various studies [88, 100, 110] have reported that aging is accompanied by a reduction in the activity of the energy-sensing enzyme AMP-activated protein kinase (AMPK). AMPK works as a fuel gauge, being activated robustly by energy-consuming stimuli such as muscle contraction, hypoxia, and ischemia [70, 135]. Upon stimulation, AMPK functions to restore cellular ATP by modifying diverse metabolic and cellular pathways, including increased fat oxidation and glucose transport. AMPK promotes fat oxidation in tissues by phosphorylating and inactivating acetyl CoA carboxylase (ACC), resulting in decreased synthesis of malonyl-CoA, an inhibitor of carnitine palmitoyltransferase I (CPT-1). The reduction in malonyl CoA relieves the inhibition of CPT-1 and promotes CPT-1 mediated transport of fatty acids into the mitochondria for oxidation. Because the end result of AMPK activation is an increase in fat oxidation, decreases in AMPK activity, as seen with aging, could lead to an excessive accumulation of intramyocelular lipids, which in turn would impair insulin action/sensitivity. Other key regulators of mitochondrial biogenesis and oxidative capacity reported to be altered with aging are the transcriptional coactivator peroxisome proliferator-activated receptor γ coactivator (PGC)-1α and the NAD-dependent deacetylase sirtuin-1. PGC-1α controls mitochondrial biogenesis and cellular metabolism by regulating the expression of numerous proteins involved in the Krebs cycle, oxidative phosphorylation, and mtDNA replication/transcription [64]. AMPK increases PGC-1α gene expression, and sirtuin-1 enhances PGC-1α activity through deacetylation on lysine residues. Similar to AMPK, the expression of both PGC-1α [55] and sirtuin-1 [31] are reduced in aging tissues, suggesting that a coordinated downregulation of the AMPK-PGC-1α-sirtuin 1 axis may play a role in the reductions of mitochondrial number, oxidative capacity, and cellular metabolic functions that occur with aging.
While, in general there is agreement with the notion that aging is associated with alterations in mitochondrial number, structure, and function, it is debated whether primary mitochondrial abnormalities (independent of aging) are sufficient to induce insulin resistance [59, 72]. Conflicting results about the role of mitochondrial dysfunction on the pathogenesis of insulin resistance, obesity, and type diabetes are due in part to differences in animal species, tissues, and human populations studied, and in the conditions and methods employed to assess mitochondrial function [79, 104]. Despite the ongoing debate, it is probable that increasing mitochondrial oxidative capacity via lifestyle interventions (i.e. physical activity) or pharmacological agents would result in improved metabolic outcomes during aging.
5.4 Role of Inflammation
Aging may be considered a state of low-grade “sterile” inflammation that could play a role in the high prevalence of glucose metabolism abnormalities in older subjects [24, 30, 37]. Increased low-grade inflammatory activity in older subjects could either cause age-related diseases or be a marker of diseases that occur with aging. Bruunsgaard et al. determined that low-grade increases in the levels of pro-inflammatory cytokines in older subjects were independent of the presence of medical disorders [23], although medical disorders can exacerbate this phenomenon.
The source for the elevated cytokine levels with aging is not clear. Cytokine levels in the circulation reflect production from many tissues including inflammatory cells (monocytes/macrophages, T cells, etc.), senescent cells and adipose tissue. In the young, approximately 25 % of IL-6 is derived from fat tissue [98], and adipocytes can secrete TNFα in addition to IL-6. Aging is associated with increases in abdominal fat mass and visceral obesity is associated with increased circulating levels of these cytokines [42, 52, 81]. There is some evidence suggesting that omental fat produces more cytokines than subcutaneous fat tissue [52], and this may explain why visceral obesity has a greater detrimental effect on insulin sensitivity [53]. The production of cytokines by adipose tissue can also be modulated by the interaction between adipocytes and macrophages within the adipose tissue [82]. The number of macrophages in adipose tissue directly correlates with adiposity [131, 136] and insulin resistance [46], and adipose tissue expansion correlates with the accumulation of macrophages and the proinflammatory phenotype [20, 92]. Another potential source of inflammation with aging is the accumulation of senescent preadipocytes [125]. Senescent cells typically have a pro-inflammatory secretory profile, termed the senescence-associated secretory phenotype (SASP), that may propagate the inflammatory adipose tissue microenvironment as well as promote inflammation throughout the whole body.
In addition to cytokines produced by adipose tissue and inflammatory cells, another potential source of inflammation during aging is the microbiome and its products. Studies in flies [109], rodents [21] and humans [56] have shown that aging is accompanied by alterations in intestinal microbiota composition and intestinal barrier integrity. In line with these findings, our group recently showed that older subjects have increased plasma concentration of endotoxin (a marker of altered barrier integrity) in association with insulin resistance, sarcopenia, and increased inflammatory signaling (toll like-receptor 4, NFκB, MAPK) in muscle [56]. Thus, it is possible that endotoxin, and other yet unidentified microbial products, could be involved in the inflammatory state and consequent metabolic alterations of aging.
A potential mechanism linking aging, inflammation, and metabolic disease is immune sensing through the NLRP3 inflammasome [140]. The NLRP3 inflammasome is a multiprotein cytoplasmic complex composed of NLRP3, the adaptor molecule ASC, and the cysteine protease caspase-1. Stimulation of the inflammasome by pathogen-associated molecular patterns (PAMPs) leads to the activation of caspase-1, which cleaves the pro-forms of the cytokines IL-1β, IL-18 and IL-33 to their active and secreted forms. A role of the inflammasome in aging-related inflammation and associated pathologies is suggested by findings that NLRP3 ablation protects against glucose intolerance, bone loss, and thymic involution in aged mice [140].
6 Aging, Diabetes and Insulin Signaling in the Brain
The well-documented association of diabetes with chronic age-related disease and geriatric conditions [35] includes increased risk of cognitive impairment, dementia, brain atrophy and Alzheimer’s disease [35, 38, 99]. Potential mechanisms of these associations include several well-recognized hallmarks of aging, including increased accumulation of advanced glycation end-products (AGEs), oxidative stress, inflammation, defective proteostasis and metabolic abnormalities, as well as altered insulin signaling within the brain [38, 83].
Insulin receptors, as well as various proteins involved in the intra-cellular transmission of insulin signals, are expressed in various brain regions [83]. However, the role of insulin in the control of glucose metabolism in the central nervous system has been questioned. The controversy surrounding this issue is likely related to the fact that, in healthy subjects, glucose uptake by the brain is already maximally stimulated by normal insulin levels and therefore does not respond to further insulin stimulation [71]. In the context of Alzheimer’s disease, some investigators refer to the brain insulin resistance as “type III diabetes” [34, 123]. Recent studies in obese patients suggest that iron overload in the brain may be caused by local insulin resistance and could represent yet another potential mechanism of the detrimental influence of diabetes on cognitive performance [15] and risk for Alzheimer’s and Parkinson’s disease [115].
Complex relationships between brain function and obesity, insulin resistance, diabetes and its complications also involve the role of hypothalamic function in the control of peripheral metabolism and aging. High-fat diet and obesity promote hypothalamic inflammation and insulin resistance [96, 111], and the hypothalamus controls multiple facets of peripheral metabolism [11, 14, 101]. Insulin signaling within the hypothalamus influences hepatic gluconeogenesis [25], lipogenesis and lipolysis in the adipose tissue [117], as well as circulating levels of branch chain amino acids, which are known to be elevated in T2DM [119]. Recent elegant studies in the Cai laboratory [144] linked hypothalamic inflammation with the control of aging. Interestingly, ongoing studies in our laboratory [69, Bartke unpublished] indicate that expression of IL-1β and other pro-inflammatory cytokines is reduced in the hypothalamus of long-lived mutant mice. Further studies will be necessary to elucidate the role of hypothalamic inflammation and insulin resistance in the development of whole-body metabolic abnormalities that lead to diabetes.
More work will also be needed to identify mechanisms responsible for the increased risk of cognitive decline and Alzheimer’s disease in patients with diabetes. Epidemiological studies provide evidence that the risk of dementia in diabetic patients is reduced by treatment with metformin [33]. Metformin and related drugs have also been shown to reduce the risk of cancer and to extend longevity of experimental animals [3, 93]. These findings imply that drugs of this class can slow down and/or delay the aging process. The apparent “anti-aging” action of metformin could have contributed to its beneficial effects on cognition in diabetes patients. However, regardless of the mechanisms involved, evidence for cognitive benefits of diabetes treatment strengthens the suggestion for etiological links between diabetes and dementia. These findings also generate interest in the exciting possibility that diabetes drugs could be useful for prevention and/or treatment of Alzheimer’s disease [139]. Consistent with this notion, animal studies and early clinical trials suggest that intranasal administration of insulin in order to overcome insulin resistance and enhanced brain metabolism leads to reductions in β amyoloid and tauopathy, as well as improvements in brain function and cognition in Alzheimer’s disease [36, 108, 138].
7 Prevention of Diabetes Versus Anti-aging Interventions
The prevalence of pre-diabetes (IGT) among older adults is increasing [29]. Because life expectancy is also increasing, the number of older individuals with diabetes and/or at risk of developing its complications (blindness, kidney failure, amputations, neuropathic pain, cardiovascular disease, etc.) will be substantial. Therefore, strategies for diabetes prevention are urgently needed. Since physical inactivity and obesity are common in older subjects, lifestyle interventions are a logical diabetes preventative strategy. In addition, exercise improves mitochondrial and vascular function, which are reduced/impaired with aging [55, 114, 120]. Physical activity is effective in improving insulin action in older subjects [55]. In line with these findings, the Diabetes Prevention Program (DPP) clinical trial, conducted in pre-diabetic (IGT) subjects showed that lifestyle intervention proved exceptionally effective in preventing diabetes in older individuals [39].
Pharmacological interventions with insulin-sensitizing agents also have been evaluated for diabetes prevention in older subjects. In parallel to lifestyle changes, the DPP also tested the effect of metformin on diabetes prevention. In contrast to lifestyle modification, metformin seemed to be less effective in preventing conversion to diabetes in older subjects versus middle-aged individuals [39]. Our group conducted a multi-center diabetes prevention trial in pre-diabetic subjects using pioglitazone [45], a potent insulin-sensitizer. Pioglitazone was highly effective in preventing diabetes conversion (72 % overall reduction), and it was as effective in older (mean age = 66 years) as in middle-aged (mean age = 46 years) individuals in improving insulin sensitivity and in preventing diabetes (Espinoza S, Tripathy D, Defronzo RA, Musi N, unpublished, 2015).
Since the glucose metabolism alterations seen in older subjects may be caused by “primary” aging-mediated cellular changes (mitochondrial dysfunction, oxidative damage, cellular senescence, inflammation), another strategy for diabetes prevention is to target the aging process instead of “secondary” metabolic/endocrine perturbations (β cell dysfunction, insulin resistance). This approach would have the added benefit of potentially preventing other aging-related diseases such as cardiovascular disease, cancer, neurodegeneration and arthritis at the same time. This is in fact the central tenet of the Geroscience Hypothesis, which is awaiting experimental testing. The apparent beneficial effects of metformin and physical activity on many of these diseases, exemplifies the possibility of preventing/treating them through modifying basic mechanisms of aging. As research in aging biology advances and novel molecular targets are identified, trials using agents that modify these targets should be conducted for the testing of interventions to prevent diabetes and other diseases of aging in the elderly.
8 Closing Remarks
Aging is accompanied by various changes in metabolic processes at the cellular, tissue and whole body levels, including decreases in oxidative capacity, intracellular lipid accumulation, insulin resistance, and β cell dysfunction. These metabolic changes contribute to the higher prevalence of obesity and T2DM that are important causes of disability and death in older people. A better understanding of the molecular basis for the age-induced metabolic alterations will help design strategies to preserve metabolic homeostasis and prevent these diseases that affect millions of people around the world.
References
Aguirre V, Uchida T, Yenush L, Davis R, White MF (2000) The c-Jun NH(2)-terminal kinase promotes insulin resistance during association with insulin receptor substrate-1 and phosphorylation of Ser(307). J Biol Chem 275:9047–9054
Andres R (1971) Aging and diabetes. Med Clin North Am 55:835–846
Anisimov VN, Bartke A (2013) The key role of growth hormone-insulin-IGF-1 signaling in aging and cancer. Crit Rev Oncol Hematol 87(3):201–223
Arum O, Boparai RK, Saleh JK, Wang F, Dirks AL, Turner JG, Kopchick JJ, Liu JL, Khardori RK, Bartke A (2014) Specific suppression of insulin sensitivity in growth hormone receptor gene-disrupted (GHR-KO) mice attenuates phenotypic features of slow aging. Aging Cell 13:981–1000
Bachmann OP, Dahl DB, Brechtel K, Machann J, Haap M, Maier T, Loviscach M, Stumvoll M, Claussen CD, Schick F, Haring HU, Jacob S (2001) Effects of intravenous and dietary lipid challenge on intramyocellular lipid content and the relation with insulin sensitivity in humans. Diabetes 50:2579–2584
Bartke A (2003) Can growth hormone (GH) accelerate aging? Evidence from GH-transgenic mice. Neuroendocrinology 78:210–216
Bartke A, Wright JC, Mattison JA, Ingram DK, Miller RA, Roth GS (2001) Extending the lifespan of long-lived mice. Nature 414:412
Bartke A, Sun LY, Longo V (2013) Somatotropic signaling: trade-offs between growth, reproductive development, and longevity. Physiol Rev 93:571–598
Barzilai N, Ferrucci L (2012) Insulin resistance and aging: a cause or a protective response? J Gerontol A Biol Sci Med Sci 67:1329–1331
Barzilai N, Huffman DM, Muzumdar RH, Bartke A (2012) The critical role of metabolic pathways in aging. Diabetes 61(6):1315–1322. http://doi.org/10.2337/db11-1300
Belgardt BF, Mauer J, Wunderlich FT, Ernst MB, Pal M, Spohn G, Brönneke HS, Brodesser S, Hampel B, Schauss AC, Brüning JC (2010) Hypothalamic and pituitary c-Jun N-terminal kinase 1 signaling coordinately regulates glucose metabolism. Proc Natl Acad Sci U S A 107(13):6028–6033
Berg AH, Combs TP, Du X, Brownlee M, Scherer PE (2001) The adipocyte-secreted protein Acrp30 enhances hepatic insulin action. Nat Med 7:947–953
Berryman DE, List EO, Palmer AJ, Chung MY, Wright-Piekarski J, Lubbers E, O’Connor P, Okada S, Kopchick JJ (2010) Two-year body composition analyses of long-lived GHR null mice. J Gerontol A Biol Sci Med Sci 65:31–40
Martínez B, de Morentin P, González CR, Saha AK, Martins L, Diéguez C, Vidal-Puig A, Tena-Sempere M, López M (2011) Hypothalamic AMP-activated protein kinase as a mediator of whole body energy balance. Rev Endocr Metab Disord 12(3):127–140
Blasco G, Puig J, Daunis-i-Estradella J, Molina X, Xifra G, Fernádez-Aranda F, Pedraza S, Wifredo R, Portero-Otín M, Fernádez-Real JM (2014) Brain iron overload, insulin resistance and cognitive performance in obese subjects: a preliminary MRI case-control study. Diabetes Care 37:3076–3083
Blüher M, Kahn B, Kahn CR (2003) Extended longevity in mice lacking the insulin receptor in adipose tissue. Science 299:572–574
Boden G, Chen X (1995) Effects of fat on glucose uptake and utilization in patients with non-insulin-dependent diabetes. J Clin Invest 96:1261–1268
Bonkowski MS, Rocha JS, Masternak MM, Al Regaiey KA, Bartke A (2006) Targeted disruption of growth hormone receptor interferes with the beneficial actions of calorie restriction. Proc Natl Acad Sci U S A 103:7901–7905
Bonkowski MS, Dominici FP, Arum O, Rocha JS, Al Regaiey KA, Westbrook R, Spong A, Panici J, Masternak MM, Kopchick JJ, Bartke A (2009) Disruption of growth hormone receptor prevents calorie restriction from improving insulin action and longevity. PLoS One 4:e4567
Bourlier V, Zakaroff-Girard A, Miranville A, De Barros S, Maumus M, Sengenes C, Galitzky J, Lafontan M, Karpe F, Frayn KN, Bouloumie A (2008) Remodeling phenotype of human subcutaneous adipose tissue macrophages. Circulation 117:806–815
Brasili E, Mengheri E, Tomassini A, Capuani G, Roselli M, Finamore A, Sciubba F, Marini F, Miccheli A (2013) Lactobacillus acidophilus La5 and Bifidobacterium lactis Bb12 induce different age-related metabolic profiles revealed by 1H-NMR spectroscopy in urine and feces of mice. J Nutr 143:1549–1557
Brown-Borg HM, Bartke A (2012) GH and IGF1: roles in energy metabolism of long-living GH mutant mice. J Gerontol A Biol Sci Med Sci 67:652–660
Bruunsgaard H, Ladelund S, Pedersen AN, Schroll M, Jorgensen T, Pedersen BK (2003) Predicting death from tumour necrosis factor-alpha and interleukin-6 in 80-year-old people. Clin Exp Immunol 132:24–31
Bruunsgaard H, Pedersen M, Pedersen BK (2001) Aging and proinflammatory cytokines. Curr Opin Hematol 8:131–136
Buettner C, Camacho RC (2008) Hypothalamic control of hepatic glucose production and its potential role in insulin resistance. Endocrinol Metab Clin North Am 37(4):825–840
Cai D, Yuan M, Frantz DF, Melendez PA, Hansen L, Lee J, Shoelson SE (2005) Local and systemic insulin resistance resulting from hepatic activation of IKK-beta and NF-kappaB. Nat Med 11:183–190
Calles-Escandon J, Poehlman ET (1997) Aging, fat oxidation and exercise. Aging (Milano) 9:57–63
Caro JF, Sinha MK, Raju SM, Ittoop O, Pories WJ, Flickinger EG, Meelheim D, Dohm GL (1987) Insulin receptor kinase in human skeletal muscle from obese subjects with and without noninsulin dependent diabetes. J Clin Invest 79:1330–1337
Caspersen CJ, Thomas GD, Beckles GL, Bullard KM (2015) Secular changes in prediabetes indicators among older-adult Americans, 1999–2010. Am J Prev Med 48:253–263
Catania A, Airaghi L, Motta P, Manfredi MG, Annoni G, Pettenati C, Brambilla F, Lipton JM (1997) Cytokine antagonists in aged subjects and their relation with cellular immunity. J Gerontol A Biol Sci Med Sci 52:B93–B97
Chang HC, Guarente L (2013) SIRT1 mediates central circadian control in the SCN by a mechanism that decays with aging. Cell 153:1448–1460
Chen M, Bergman RN, Pacini G, Porte D Jr (1985) Pathogenesis of age-related glucose intolerance in man: Insulin resistance and decreased beta-cell function. J Clin Endocrinol Metab 60:13–20
Cheng C, Lin CH, Tsai YW, Tsai CJ, Chou PH, Lan TH (2014) Type 2 diabetes and antidiabetic medications in relations to dementia and diagnosis. J Gerontol A Biol Sci Med Sci 69(10):1299–1305
Cholerton B, Baker LD, Craft S (2011) Insulin resistance and pathological brain ageing. Diabet Med 28:1463–1475
Cigolle CT, Lee PG, Langa KM, Lee YY, Tian Z, Blaum CS (2011) Geriatric conditions develop in middle-aged adults with diabetes. J Gen Intern Med 26:272–279
Claxton A, Baker LD, Hanson A, Trittschuh EH, Cholerton B, Morgan A, Callaghan M, Arbuckle M, Behl C, Craft S (2015) Long-acting intranasal insulin detemir improves cognition for adults with mild cognitive impairment or early-stage Alzheimer’s disease dementia. J Alzheimers Dis 44:897–906
Cohen HJ, Pieper CF, Harris T, Rao KM, Currie MS (1997) The association of plasma IL-6 levels with functional disability in community-dwelling elderly. J Gerontol A Biol Sci Med Sci 52:M201–M208
Craft S (2009) The role of metabolic disorders in Alzheimer’s disease and vascular dementia: two roads converged. Arch Neurol 66(3):300–305
Crandall J, Schade D, Ma Y, Fujimoto WY, Barrett-Connor E, Fowler S, Dagogo-Jack S, Andres R (2006) The influence of age on the effects of lifestyle modification and metformin in prevention of diabetes. J Gerontol A Biol Sci Med Sci 61:1075–1081
Cree MG, Newcomer BR, Katsanos CS, Sheffield-Moore M, Chinkes D, Aarsland A, Urban R, Wolfe RR (2004) Intramuscular and liver triglycerides are increased in the elderly. J Clin Endocrinol Metab 89:3864–3871
Cusi K, Maezono K, Osman A, Pendergrass M, Patti ME, Pratipanawatr T, DeFronzo RA, Kahn CR, Mandarino LJ (2000) Insulin resistance differentially affects the PI 3-kinase- and MAP kinase-mediated signaling in human muscle. J Clin Invest 105:311–320
Dandona P, Weinstock R, Thusu K, Abdel-Rahman E, Aljada A, Wadden T (1998) Tumor necrosis factor-alpha in sera of obese patients: fall with weight loss. J Clin Endocrinol Metab 83:2907–2910
DeFronzo RA (1981) Glucose intolerance and aging. Diabetes Care 4:493–501
DeFronzo RA (2009) Banting lecture. From the triumvirate to the ominous octet: a new paradigm for the treatment of type 2 diabetes mellitus. Diabetes 58:773–795
DeFronzo RA, Tripathy D, Schwenke DC, Banerji M, Bray GA, Buchanan TA, Clement SC, Henry RR, Hodis HN, Kitabchi AE, Mack WJ, Mudaliar S, Ratner RE, Williams K, Stentz FB, Musi N, Reaven PD (2011) Pioglitazone for diabetes prevention in impaired glucose tolerance. N Engl J Med 364:1104–1115
Di Gregorio GB, Yao-Borengasser A, Rasouli N, Varma V, Lu T, Miles LM, Ranganathan G, Peterson CA, McGehee RE, Kern P (2005) Expression of CD68 and macrophage chemoattractant protein-1 genes in human adipose and muscle tissues: association with cytokine expression, insulin resistance, and reduction by pioglitazone. Diabetes 54:2305–2313
Edelstein SL, Knowler WC, Bain RP, Andres R, Barrett-Connor EL, Dowse GK, Haffner SM, Pettitt DJ, Sorkin JD, Muller DC, Collins VR, Hamman RF (1997) Predictors of progression from impaired glucose tolerance to NIDDM: an analysis of six prospective studies. Diabetes 46(4):701–710
Elahi D, Muller DC (2000) Carbohydrate metabolism in the elderly. Eur J Clin Nutr 54(Suppl 3):S112–S120
Fang Y, Westbrook R, Hill C, Boparai RK, Arum O, Spong A, Wang F, Javors MA, Chen J, Sun LY, Bartke A (2013) Duration of rapamycin treatment has differential effects on metabolism in mice. Cell Metab 17:456–462
Farese RV, Sajan MP, Standaert ML (2005) Insulin-sensitive protein kinases (atypical protein kinase C and protein kinase B/Akt): actions and defects in obesity and type II diabetes. Exp Biol Med (Maywood) 230:593–605
Fink RI, Kolterman OG, Griffin J, Olefsky JM (1983) Mechanisms of insulin resistance in aging. J Clin Invest 71:1523–1535
Fried SK, Bunkin DA, Greenberg AS (1998) Omental and subcutaneous adipose tissues of obese subjects release interleukin-6: depot difference and regulation by glucocorticoid. J Clin Endocrinol Metab 83:847–850
Gastaldelli A, Miyazaki Y, Pettiti M, Matsuda M, Mahankali S, Santini E, DeFronzo RA, Ferrannini E (2002) Metabolic effects of visceral fat accumulation in type 2 diabetes. J Clin Endocrinol Metab 87:5098–5103
Garvey WT, Maianu L, Zhu JH, Brechtel-Hook G, Wallace P, Baron AD (1998) Evidence for defects in the trafficking and translocation of GLUT4 glucose transporters in skeletal muscle as a cause of human insulin resistance. J Clin Invest 101:2377–2386
Ghosh S, Lertwattanarak R, Lefort N, Molina-Carrion M, Joya-Galeana J, Bowen BP, Garduno-Garcia Jde J, Abdul-Ghani M, Richardson A, DeFronzo RA, Mandarino L, Van Remmen H, Musi N (2011) Reduction in reactive oxygen species production by mitochondria from elderly subjects with normal and impaired glucose tolerance. Diabetes 60:2051–2060
Ghosh S, Lertwattanarak R, Garduno Jde J, Galeana JJ, Li J, Zamarripa F, Lancaster JL, Mohan S, Hussey S, Musi N (2015) Elevated muscle TLR4 expression and metabolic endotoxemia in human aging. J Gerontol A Biol Sci Med Sci 70:232–246
Giani JF, Miquet JG, Munoz MC et al (2012) Upregulation of the angiotensin-converting enzyme 2/angiotensin-(1–7)/mas receptor axis in the heart and the kidney of growth hormone receptor knock-out mice. Growth Horm IGF Res 22:224–233
Goodman MN, Dluz SM, McElaney MA, Belur E, Ruderman NB (1983) Glucose uptake and insulin sensitivity in rat muscle: changes during 3–96 weeks of age. Am J Physiol 244:E93–E100
Goodpaster BH (2013) Mitochondrial deficiency is associated with insulin resistance. Diabetes 62(4):1032–1035
Goodpaster BH, Theriault R, Watkins SC, Kelley DE (2000) Intramuscular lipid content is increased in obesity and decreased by weight loss. Metabolism 49:467–472
Guarente L, Kenyon C (2000) Genetic pathways that regulate ageing in model organisms. Nature 408(6809):255–262
Grundleger ML, Godbole VY, Thenen SW (1980) Age-dependent development of insulin resistance of soleus muscle in genetically obese (ob/ob) mice. Am J Physiol 239:E363–E371
Hajduch E, Balendran A, Batty IH, Litherland GJ, Blair AS, Downes CP, Hundal HS (2001) Ceramide impairs the insulin-dependent membrane recruitment of protein kinase B leading to a loss in downstream signalling in L6 skeletal muscle cells. Diabetologia 44:173–183
Handschin C, Speigelman BM (2006) Peroxisome proliferator-activated receptor gamma coactivator 1 coactivators, energy homeostasis, and metabolism. Endocr Rev 27(7):728–735
Harman D (1972) Free radical theory of aging: dietary implications. Am J Clin Nutr 25(8):839–843
Harris MI, Flegal KM, Cowie CC, Eberhardt MS, Goldstein DE, Little RR, Wiedmeyer HM, Byrd-Holt DD (1998) Prevalence of diabetes, impaired fasting glucose, and impaired glucose tolerance in U.S. adults. The third national health and nutrition examination survey, 1988–1994. Diabetes Care 21:518–524
Harrison DE, Archer JR, Astle CM (1984) Effects of food restriction on aging: separation of food intake and adiposity. Proc Natl Acad Sci U S A 81:1835–1838
Harrison DE, Strong R, Sharp ZD, Nelson JF, Astle CM, Flurkey K, Nadon NL, Wilkinson JE, Frenkel K, Carter CS, Pahor M, Javors MA, Fernandez E, Miller RA (2009) Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature 460:392–395
Hascup ER, Wang F, Kopchick JJ, Bartke A (2015) Inflammatory and glutamatergic homeostasis are involved in successful aging. J Gerontol A Biol Sci Med Sci Pii: doi: 10.1093/gerona/glv010. PubMed PMID: 25711529
Hayashi T, Hirshman MF, Kurth EJ, Winder WW, Goodyear LJ (1998) Evidence for 5’ amp-activated protein kinase mediation of the effect of muscle contraction on glucose transport. Diabetes 47:1369–1373
Hirvonen J, Virtanen KA, Nummenmaa L, Hannukainen JC, Honka MJ, Bucci M, Nesterov SV, Parkkola R, Rinne J, Iozzo P, Nuutila P (2011) Effects of insulin on brain glucose metabolism in impaired glucose tolerance. Diabetes 60:443–447
Holloszy JO (2013) “Deficiency” of mitochondria in muscle does not cause insulin resistance. Diabetes 62(4):1036–1040
Ikeno Y, Hubbard GB, Lee S et al (2009) Reduced incidence and delayed occurrence of fatal neoplastic diseases in growth hormone receptor/binding protein knockout mice. J Gerontol A Biol Sci Med Sci 64:522–529
Ikeno Y, Hubbard GB, Lee S et al (2013) Do Ames dwarf and calorie-restricted mice share common effects on age-related pathology? Pathobiol Aging Age Relat Dis 3. http://www.pathobiologyofaging.net/index.php/pba/article/view/20833
Iossa S, Mollica MP, Lionetti L, Crescenzo R, Tasso R, Liverini G (2004) A possible link between skeletal muscle mitochondrial efficiency and age-induced insulin resistance. Diabetes 53:2861–2866
Itani SI, Zhou Q, Pories WJ, MacDonald KG, Dohm GL (2000) Involvement of protein kinase C in human skeletal muscle insulin resistance and obesity. Diabetes 49:1353–1358
Jackson RA, Blix PM, Matthews JA, Hamling JB, Din BM, Brown DC, Belin J, Rubenstein AH, Nabarro JD (1982) Influence of ageing on glucose homeostasis. J Clin Endocrinol Metab 55:840–848
Jara A, Benner CM, Sim D, Liu X, List EO, Householder LA, Berryman DE, Kopchick JJ (2014) Elevated systolic blood pressure in male GH transgenic mice is age dependent. Endocrinology 155(3):975–986. doi:10.1210/en.2013-1899
Johnson ML, Robinson MM, Nair KS (2013) Skeletal muscle aging and the mitochondrion. Trends Endocrinol Metab 24(5):247–256
Karlsson HK, Zierath JR, Kane S, Krook A, Lienhard GE, Wallberg-Henriksson H (2005) Insulin-stimulated phosphorylation of the Akt substrate AS160 is impaired in skeletal muscle of type 2 diabetic subjects. Diabetes 54:1692–1697
Kern PA, Ranganathan S, Li C, Wood L, Ranganathan G (2001) Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance. Am J Physiol Endocrinol Metab 280:E745–E751
Klaus S, Keijer J (2004) Gene expression profiling of adipose tissue: Individual, depot-dependent, and sex-dependent variabilities. Nutrition 20:115–120
Kleinridders A, Ferris Ham Cai W, Kahn CR (2014) Insulin action on brain regulates systemic metabolism and brain function. Diabetes 63(7):2232–2243
Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, Nathan DM (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346:393–403
Korach-Andre M, Gounarides J, Deacon R, Beil M, Sun D, Gao J, Laurent D (2005) Age and muscle-type modulated role of intramyocellular lipids in the progression of insulin resistance in nondiabetic Zucker rats. Metabolism 54:522–528
Kurosu H, Yamamoto M, Clark JD, Pastor JV, Nandi A, Gurnani P, McGuinness OP, Chikuda H, Yamaguchi M, Kawaguchi H, Shimomura I, Takayama Y, Herz J, Kahn CR, Rosenblatt KP, Kuro-o M (2005) Suppression of aging in mice by the hormone Klotho. Science 309:1829–1833
Larkin LM, Reynolds TH, Supiano MA, Kahn BB, Halter JB (2001) Effect of aging and obesity on insulin responsiveness and GLUT-4 glucose transporter content in skeletal muscle of Fischer 344 x brown Norway rats. J Gerontol A Biol Sci Med Sci 56:B486–B492
Li M, Verdijk LB, Sakamoto K, Ely B, van Loon LJ, Musi N (2012) Reduced AMPK-ACC and mTOR signaling in muscle from older men, and effect of resistance exercise. Mech Ageing Dev 133:655–664
Lindstrom P (2007) The physiology of obese-hyperglycemic mice [ob/ob mice]. ScientificWorldJournal 7:666–685
List EO, Sackmann-Sala L, Berryman DE, Funk K, Kelder B, Gosney ES, Okada S, Ding J, Cruz-Topete D, Kopchick JJ (2011) Endocrine parameters and phenotypes of the growth hormone receptor gene disrupted (GHR−/−) mouse. Endocr Rev 32:356–386
Lubbers ER, List EO, Jara A, Sackman-Sala L et al (2013) Adiponectin in mice with altered GH action: links to insulin sensitivity and longevity? J Endocrinol 216:363–374
Lumeng CN, DelProposto JB, Westcott DJ, Saltiel AR (2008) Phenotypic switching of adipose tissue macrophages with obesity is generated by spatiotemporal differences in macrophage subtypes. Diabetes 57:3239–3246
Martin-Montalvo A, Mercken EM, Mitchell SJ, Palacios HH, Mote PL, Scheibye-Knudsen M, Gomes AP, Ward TM, Minor RK, Blouin MJ, Schwab M, Pollak M, Zhang Y, Yu Y, Becker KG, Bohr VA, Ingram DK, Sinclair DA, Wolf NS, Spindler SR, Bernier M, de Cabo R (2013) Metformin improves healthspan and lifespan in mice. Nat Commun 4:2192
Masternak MM, Bartke A, Wang F, Spong A, Gesing A, Fang Y, Salmon AB, Hughes LF, Liberati T, Boparai R, Kopchick JJ, Westbrook R (2012) Metabolic effects of intra-abdominal fat in GHRKO mice. Aging Cell 11:73–81
McArdle MA, Finucane OM, Connaughton RM, McMorrow AM, Roche HM (2013) Mechanisms of obesity-induced inflammation and insulin resistance: insights into the emerging role of nutritional strategies. Front Endocrinol 4:52
Milanski M, Arruda AP, Coope A, Ignacio-Souza LM, Nunez CE, Roman EA, Romanatto T, Pascoal LB, Caricilli AM, Torsoni MA, Prada PO, Saad MJ, Velloso LA (2012) Inhibition of hypothalamic inflammation reverses diet-induced insulin resistance in the liver. Diabetes 61:1455–1462
Miquel J, Economos AC, Flemming J, Johnson JE Jr (1980) Mitochondrial role in cell aging. Exp Gerontol 15(6):575–591
Mohamed-Ali V, Goodrick S, Rawesh A, Katz DR, Miles JM, Yudkin JS, Klein S, Coppack SW (1997) Subcutaneous adipose tissue releases interleukin-6, but not tumor necrosis factor-alpha, in vivo. J Clin Endocrinol Metab 82:4196–4200
Moran C, Phan TG, Chen J, Blizzard L, Beare R, Venn A, Münch G, Wood AG, Forbes J, Greenaway TM, Pearson S, Srikanth V (2013) Brain atrophy in type 2 diabetes: regional distribution and influence on cognition. Diabetes Care 36(12):4036–4042
Mortensen B, Poulsen P, Wegner L, Stender-Petersen KL, Ribel-Madsen R, Friedrichsen M, Birk JB, Vaag A, Wojtaszewski JF (2009) Genetic and metabolic effects on skeletal muscle AMPK in young and older twins. Am J Physiol Endocrinol Metab 297:E956–E964
Obici S, Feng Z, Morgan K, Stein D, Karkanias G, Rossetti L (2002) Central administration of oleic acid inhibits glucose production and food intake. Diabetes 51(2):271–275
Okada-Iwabu M, Yamauchi T, Iwabu M, Honma T, Hamagami K, Matsuda K, Yamaguchi M, Tanabe H, Kimura-Someya T, Shirouzu M, Ogata H, Tokuyama K, Ueki K, Nagano T, Tanaka A, Yokoyama S, Kadowaki T (2013) A small-molecule AdipoR agonist for type 2 diabetes and short life in obesity. Nature 503:493–499
Palmer AJ, Chung MY, List EO, Walker J, Okada S, Kopchick JJ, Berryman DE (2009) Age-related changes in body composition of bovine growth hormone transgenic mice. Endocrinology 150:1353–1360
Perry CG, Kane DA, Lanza IR, Neufer PD (2013) Methods for assessing mitochondrial function in diabetes. Diabetes 62(4):1041–1053
Petersen KF, Befroy D, Dufour S, Dziura J, Ariyan C, Rothman DL, DiPietro L, Cline GW, Shulman GI (2003) Mitochondrial dysfunction in the elderly: possible role in insulin resistance. Science 300:1140–1142
Paolisso G, Fambardella A, Ammendola S, D’Amore A, Balbi V, Varricchio M, M’Onofrio F (1996) Glucose tolerance and insulin action in healthy centenarians. Am J Physiol 270(5 Pt 1):E890–E894
Reaven GM, Chen N, Hollenbeck C, Chen YD (1989) Effect of age on glucose tolerance and glucose uptake in healthy individuals. J Am Geriatr Soc 37:735–740
Reger MA, Watson GS, Green PS, Wilkinson CW, Baker LD, Cholerton B, Fishel MA, Plymate SR, Breitner JC, DeGroodt W, Mehta P, Craft S (2008) Intranasal insulin improves cognition and modulates beta-amyloid in early AD. Neurology 70:440–448
Rera M, Clark RI, Walker DW (2012) Intestinal barrier dysfunction links metabolic and inflammatory markers of aging to death in Drosophila. Proc Natl Acad Sci U S A 109:21528–21533
Reznick RM, Zong H, Li J, Morino K, Moore IK, Yu HJ, Liu ZX, Dong J, Mustard KJ, Hawley SA, Befroy D, Pypaert M, Hardie DG, Young LH, Shulman GI (2007) Aging-associated reductions in AMP-activated protein kinase activity and mitochondrial biogenesis. Cell Metab 5:151–156
Rother E, Kuschewski R, Alcazar MA, Oberthuer A, Bae-Gart I, Vohlen C, Roth B, Dötsch J (2012) Hypothalamic JNK1 and IKKβ activation and impaired early postnatal glucose metabolism after maternal perinatal high-fat feeding. Endocrinology 153(2):770–781
Rowe JW, Minaker KL, Pallotta JA, Flier JS (1983) Characterization of the insulin resistance of aging. J Clin Invest 71:1581–1587
Santomauro AT, Boden G, Silva ME, Rocha DM, Santos RF, Ursich MJ, Strassmann PG, Wajchenberg BL (1999) Overnight lowering of free fatty acids with Acipimox improves insulin resistance and glucose tolerance in obese diabetic and nondiabetic subjects. Diabetes 48(9):1836–1841
Santos-Parker JR, LaRocca TJ, Seals DR (2014) Aerobic exercise and other healthy lifestyle factors that influence vascular aging. Adv Physiol Educ 38:296–307
Schipper HM, Song W (2015) A heme oxygenase-1 transducer model of degenerative and developmental brain disorders. Int J Mol Sci 16(3):5400–5419
Selman C, Lingard S, Choudhury AI et al (2008) Evidence for lifespan extension and delayed age-related biomarkers in insulin receptor substrate 1 null mice. FASEB J 22:807–818
Scherer T, O’Hare J, Diggs-Andrews K, Schweiger M, Cheng B, Lindtner C, Zielinski E, Vempati P, Su K, Dighe S, Milsom T, Puchowicz M, Scheja L, Zechner R, Fisher SJ, Previs SF, Buettner C (2011) Brain insulin controls adipose tissue lipolysis and lipogenesis. Cell Metab 13:183–194
Shimokata H, Muller DC, Fleg JL, Sorkin J, Ziemba AW, Andres R (1991) Age as independent determinant of glucose tolerance. Diabetes 40:44–51
Shin AC, Fasshauer M, Filatova N, Grundell LA, Zielinski E, Zhou JY, Scherer T, Lindtner C, White PJ, Lapworth AL, Ilkayeva O, Knippschild U, Wolf AM, Scheja L, Grove KL, Smith RD, Qian WJ, Lynch CJ, Newgard CB, Buettner C (2014) Brain insulin lowers circulating bcaa levels by inducing hepatic bcaa catabolism. Cell Metab 20:898–909
Short KR, Vittone JL, Bigelow ML, Proctor DN, Rizza RA, Coenen-Schimke JM, Nair KS (2003) Impact of aerobic exercise training on age-related changes in insulin sensitivity and muscle oxidative capacity. Diabetes 52:1888–1896
Smith BA, Edwards MS, Ballachey BE, Cramer DA, Sutherland TM (1991) Body weight and longevity in genetically obese and non-obese mice fed fat-modified diets. Growth Dev Aging 55:81–89
Solomon TP, Marchetti CM, Krishnan RK, Gonzalez F, Kirwan JP (2008) Effects of aging on basal fat oxidation in obese humans. Metabolism 57:1141–1147
Talbot K, Han L, Schneider JA, Wilson RS, Bennett DA, Arnold SE (2006) Expression of pIRS-1 (S312 and S616) is elevated in MCI and AD and correlates with cognitive impairment and neurofibrillary pathology. Alzheimers Dement 2:S54
Tartar M, Barke A, Antebi A (2003) The endocrine regulation of aging by insulin-like signals. Science 299(5611):1346–1351
Tchkonia T, Morbeck DE, Von Zglinicki T, Van Deursen J, Lustgarten J, Scrable H, Khosla S, Jensen MD, Kirkland JL (2010) Fat tissue, aging, and cellular senescence. Aging Cell 9:667–684
Tucker MZ, Turcotte LP (2003) Aging is associated with elevated muscle triglyceride content and increased insulin-stimulated fatty acid uptake. Am J Physiol Endocrinol Metab 285:E827–E835
Villarreal-Molina MT, Antuna-Puente B (2012) Adiponectin: anti-inflammatory and cardioprotective effects. Biochimie 94:2143–2149
Virkamaki A, Korsheninnikova E, Seppala-Lindroos A, Vehkavaara S, Goto T, Halavaara J, Hakkinen AM, Yki-Jarvinen H (2001) Intramyocellular lipid is associated with resistance to in vivo insulin actions on glucose uptake, antilipolysis, and early insulin signaling pathways in human skeletal muscle. Diabetes 50:2337–2343
Wanke R, Wolf E, Hermanns W, Folger S, Buchmüller T, Brem G (1992) The GH-transgenic mouse as an experimental model for growth research: clinical and pathological studies. Horm Res 37:74–87
Wei YH, Kao SH, Lee HC (1996) Simultaneous increase of mitochondrial DNA deletions and lipid peroxidation in human aging. Ann N Y Acad Sci 786:24–43
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW Jr (2003) Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 112:1796–1808
White MF (1998) The IRS-signalling system: a network of docking proteins that mediate insulin action. Mol Cell Biochem 182:3–11
Wijsman CA, Rozing MP, Streefland TC, le Cessie S, Mooijaart SP, Slagboom PE, Westendorp RG, Pijl H, van Heemst D, Leiden Logevity Study group (2011) Familial longevity is marked by enhanced insulin sensitivity. Aging Cell 10(1):114–121
Wolff GL, Roberts DW, Mountjoy KG (1999) Physiological consequences of ectopic agouti gene expression: the yellow obese mouse syndrome. Physiol Genomics 1:151–163
Xing Y, Musi N, Fujii N, Zou L, Luptak I, Hirshman MF, Goodyear LJ, Tian R (2003) Glucose metabolism and energy homeostasis in mouse hearts overexpressing dominant negative alpha2 subunit of AMP-activated protein kinase. J Biol Chem 278:28372–28377
Xu H, Barnes GT, Yang Q, Tan G, Yang D, Chou CJ, Sole J, Nichols A, Ross JS, Tartaglia LA, Chen H (2003) Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112(12):1821–1830. 1821-1830. doi:10.1172/JCI19451
Yamauchi T, Kamon J, Waki H, Terauchi Y, Kubota N, Hara K, Mori Y, Ide T, Murakami K, Tsuboyama-Kasaoka N, Ezaki O, Akanuma Y, Gavrilova O, Vinson C, Reitman ML, Kagechika H, Shudo K, Yoda M, Nakano Y, Tobe K, Nagai R, Kimura S, Tomita M, Froguel P, Kadowaki T (2001) The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat Med 7:941–946
Yang Y, Ma D, Wang Y, Jiang T, Hu S, Zhang M, Yu X, Gong CX (2013) Intranasal insulin ameliorates tau hyperphosphorylation in a rat model of type 2 diabetes. J Alzheimers Dis 33:329–338
Yarchoan M, Arnold SE (2014) Repurposing diabetes drugs for brain insulin resistance in alzheimer disease. Diabetes 63:2253–2261
Youm YH, Grant RW, McCabe LR, Albarado DC, Nguyen KY, Ravussin A, Pistell P, Newman S, Carter R, Laque A, Munzberg H, Rosen CJ, Ingram DK, Salbaum JM, Dixit VD (2013) Canonical NIrp3 inflammasome links systemic low-grade inflammation to functional decline in aging. Cell Metab 18:519–532
Yu C, Chen Y, Cline GW, Zhang D, Zong H, Wang Y, Bergeron R, Kim JK, Cushman SW, Cooney GJ, Atcheson B, White MF, Kraegen EW, Shulman GI (2002) Mechanism by which fatty acids inhibit insulin activation of insulin receptor substrate-1 (irs-1)-associated phosphatidylinositol 3-kinase activity in muscle. J Biol Chem 277:50230–50236
Zaid H, Antonescu CN, Randhawa VK, Klip A (2008) Insulin action on glucose transporters through molecular switches, tracks and tethers. Biochem J 413(2):201–215
Zeigerer A, McBrayer MK, McGraw TE (2004) Insulin stimulation of GLUT4 exocytosis, but not its inhibition of endocytosis, is dependent on RabGAP AS160. Mol Biol Cell 15:4406–4415
Zhang G, Li J, Purkayastha S, Tang Y, Zhang H, Yin Y, Li B, Liu G, Cai D (2013) Hypothalamic programming of systemic ageing involving IKKβ, NF-kB and GnRH. Nature 497(7448):211–216
Zierath JR, Krook A, Wallberg-Henriksson H (1998) Insulin action in skeletal muscle from patients with NIDDM. Mol Cell Biochem 182:153–160
Acknowledgments
N.M. has been supported by grants from the American Diabetes Association, the National Institutes of Health (DK-80157, DK-089229 and AG-030979), and by the San Antonio Nathan Shock Center (AG-013319). A.B has been supported by grants from the National Institute on Aging (AG-019899 and AG-031736), and by the SIU Geriatrics Research Initiative.
Editor: Aaron Pawlik, National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), NIH.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing
About this chapter
Cite this chapter
Musi, N., Bartke, A. (2016). Diabetes and Aging. In: Sierra, F., Kohanski, R. (eds) Advances in Geroscience. Springer, Cham. https://doi.org/10.1007/978-3-319-23246-1_12
Download citation
DOI: https://doi.org/10.1007/978-3-319-23246-1_12
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-23245-4
Online ISBN: 978-3-319-23246-1
eBook Packages: MedicineMedicine (R0)