Abstract
The human γD crystallins is one of the most abundant protein of the lens nucleus and it is believed that their main function is to help maintaining the optical properties of the lens during the life span. Human γ-D crystallins is a 173 residues protein that fold into two homologousdomains (N-terminal and C-terminal), each containing two Greek key motifs. Although, this protein is extremely stable, over the years the protection mechanism loses efficiency and the protein accumulates damages, resulting in protein aggregation which is associated with cataracts formation. At present, cataracts is the main cause of blindness in the world and surgical removal of the lens remains the only treatment. This review summarizes the current knowledge on cataracts risk factors, in vivo studies, unfolding and inhibition associated with human γD crystallins.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
- Human γD crystallin
- Cataracts
- Blindness
- Protein unfolding
- Aggregates
- Inhibition
- Greek key motifs
- Protein damage
- Blindness
- In vivo studies
Introduction
The main function of the eye lens is to produce the refractive power to focus the light onto the retina [1]. Lens is an avascular tissue composed of a single layer of epithelial cells, which has to maintain the transparency to allow the passage of light [2]. During the lens formation, the epithelial cells elongate to become fiber cells. In this process of differentiation, the cells produce large quantities of proteins. After this elongation, in order to avoid any potential light scattering structure, the organelles are removed from the fiber cells by a programmed proteolytic process (Fig. 1) [3, 4]. Even though this process continues throughout life, it does at a minimal pace, and the older fibers are pushed to the center of the lens by the newer fiber cells (Fig. 1) [2]. Therefore, fully differentiated lens cells consist of a high concentration of proteins without nuclei or any other organelles and do not produce or degrade proteins [1]. Human lens has the highest protein content within the body [5] and, as a direct consequence of the missing repair mechanisms, the proteins in the lens have to be stable and soluble for the organism lifetime.
Most of the refractive power of the lens is conferred by high concentrations of three types of proteins: α, β and γ-crystallins, which count for more than 90 % of the proteins in the lens [6, 7]. In normal lenses, these proteins are found in concentrations higher than 300 mg/mL in order to have a high refractive index [6], and while they still scatter light, they do it in a specific manner. The correlation in the position of pairs of proteins reduces the scattering; this is due to the fact that the fluctuation in the number of protein molecules over a short space is small, resulting in transparency [8]. This is known as short-range spatial order. Any microscopic fluctuation will induce light scattering, these fluctuations could be produced by molecules of large molecular weight formed, for example, by protein aggregation or polymerization [8]. Such protein aggregation leads to the development of opacities known as cataracts .
Cataracts Risk Factors
The cataracts are an opacification of the lens of the eyes due to the accumulation of aggregates of crystallins. At present, cataracts formation is the main cause of blindness in the world [9]. The formation of cataracts is highly related to aging, and it is generally accepted that proteins modifications have to occur to promote the aggregation and then the cataracts. Some of the modifications that have been observed with aging, include oxidation of the tryptophans, cysteines and methionines [10], deamidation of arginines and glutamines [11, 12], glycosylation of lysine residues [13], and peptide fragmentation [14]. Most of these modifications are believed to be induced by environmental factors such as ultraviolet light exposure [15, 16], and oxidative stress [10, 17, 18]; the consequence for all of them is the formation of insoluble aggregates resulting in lens opacity and then loss of vision for cataracts (Table 1).
In the human eye, the cornea absorbs most of the UV radiation (240–400 nm) [27], and there is also low-molecular weight UV-filter molecules in the human lens, the most abundant are kynurenine, 3-hydroxykynurenine glucoside (3OHKG), and 4-(2-amino-3-hydroxyphenyl)-4-oxybutanoic acid O-glucoside, which absorb in the UV-B (280–330 nm) and UV-C ranges (100–280 nm) [28]. However, throughout the years, significant radiation reaches the lens, producing proteins UV radiation damage, which has been correlated manly to structural changes in different residues that destabilize the proteins and accelerate their unfolding [16].
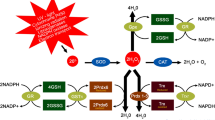
On the other hand, the oxidative stress becomes more important with aging, due to the decline of the levels of glutathione (GSH) and antioxidant enzymes as the superoxide dismutase and catalase activity [29, 30]. The decrease of GSH levels lead to crosslinking, aggregation, insolubility, and fragmentation of crystallin, which then result in the formation of cataracts [31]. Moreover, aging may also reduce the functionality of the chaperon α-crystallins to rescue the unfold β and γ-crystallins [32].
As well as aging, diabetes, malnutrition, hypertension and ionic imbalance have been correlated with cataracts formation. For instance, in diabetes, the hyperglycemia produced the diffusion of extracellular glucose to lens which produced then post-translational modification in the proteins of the lenses [33]. Also, the glucose is metabolized by the sorbitol-aldose reductase pathway and, as a result, the lens accumulates sorbitol. Then the sorbitol produces osmotic swelling, leakage of glutathione, myo-inositol changes in the membrane permeability, and generation of free radicals [34, 35]. Another factor, associated with cataracts is the ionic imbalance in the lens. An increase in the concentrations of calcium produces the activation of calpain serine-proteases that will degrade crystallins [36, 37], while a magnesium concentration decrease has been associated with an increase in the oxidative stress [38].
Finally, an intrinsically different group of cataracts are the hereditary cataracts which, unlike the other types, occur at early ages. The congenital cataracts are caused by a single-gene disorder that induces the substitution of one amino-acid, and the estimated frequency is between 1 and 6 per 10,000 of new born babies [39]. Some of these mutations are listed in Table 1; the mutation can cause protein insolubility, crystallization, changes in charge, or destabilization.
Even tough there are several factors related to cataract formation, the only effective treatment is still surgical removal of the lens. This procedure has become routine in many clinics, but nevertheless cataracts remain as the main cause of blindness in the world. This is due to the fact that this surgical procedure is expensive and is often inaccessible in low and middle-income countries. Also, it has been argued that the artificial lens doesn’t have all the optical properties of the “normal” lens [40, 41].
In Vivo Studies
The use of in vivo studies allows to conduct essential investigations in the characteristic physiological environment of the disease, providing a deeper understanding of the mechanisms involved in the appearance and progression of cataracts . Therefore, several different animals models have been developed, capable of reproducing the characteristics of the disease seen in humans, mainly to study the different factors that give rise to cataracts and some potential treatment molecules. These studies would contribute decisively to the possible development of future preventive treatments.
Some of the earliest studies focused on radiation damage induced in lenses. Rabbit lenses were subjected to X-rays, and by electronic microscopy, it was possible to observe very high molecular aggregates in irradiated cortex while in normal cortex only relatively small aggregates were visible [119]. Later, some studies of UV radiation effects in rodents lenses were done, demonstrating by histological analysis that the first target tissue of UV radiation was the epithelium [42]. Also it was found that the level of glutathione (GSH) suffers modification [43]. With these types of experiments, it has been generally accepted that the long term effect of UV-radiation is cataract formation probably by protein damage [44].
Studies focusing in oxidative stress have made extensive use of specific mouse models with known alterations for oxidative damage, and were then able to reproduce some of the features of human aged related cataracts [45, 46]. For instance, the OXXYS strain exhibits premature aging and significantly shortened life span associated with oxidative damage, and therefore the status of the lens can be characterized due to the inherent over-generation of ROS (Radical Oxygen Species) [47]. In a different methodology, oxidative stress can be induced in rats trough a galactose diet, and then induce the depletion of levels of GSH [48].
Cataract has also been studied in animal model using other inducers. Selenite has been commonly used, causing alteration of the epithelial metabolism, calcium accumulation, calpain-induced proteolysis, crystallins precipitation and cytoskeletal [49, 50]. Galactose-induced cataracts produce the accumulation of osmolytes causing ocular lens swelling of fiber cells and then disruption of the native state of lens proteins [51]. Cataracts have also been studied by using genetics mouse models [45, 52, 53].
In a different type of studies, the specific aim of using animal models has been to test routes of administration of compounds, like intraperitoneal [29, 30, 54], subcutaneous [55] or as a supplementary diet [56, 57].
Crystallins Family
Crystallins are the main constituent of the lens and are separated into three types in vertebrates: α, β and γ-crystallins [6, 7]. α-Crystallin is the predominant and biggest type of crystallins, with a molecular weight around 800 kDa [6]. It is formed by the non-covalent association of two subunits (A and B), in a molar ratio around 3:1 to 2:1 [58, 59]. Subunits A and B are homologue and form part of the small heat shock proteins family (sHSPs). Their secondary structure is primarily β-sheets [60], and the subunits seem to be in equilibrium between dissociating and re-associating constantly, which makes the protein a dynamic oligomer [61]. The main function of the native α-crystallin complex in the lens is its chaperone function [60, 62–65], but also, some experimental evidence suggests that α-crystallin is involved in remodeling and protection of the cytoskeleton, inhibition of apoptosis and the resistance to stress [66].
The β and γ-crystallins are members of the same family; they have 30 % sequence identity [67, 68], consisting mainly of β-sheets that form two domains each formed for two Greek Key motif. The β-crystallins are multimeric and contain N-terminal extensions, while the γ-crystallins are monomeric in solution [6]. The β-crystallins family is constituted by four acidic proteins (βA1, βA2, βA3, and βA4) and three basic (βB1, βB2, βB3) [69, 70]. The βB1, βB3 and βA4 crystallins are homo-oligomers [71, 72] while the βB2-crystallin forms dimers by domain swapping, and hetero-oligomers with βA1, βA2 and βA3-crystallin. The domain swapped dimer is thermodynamically unstable [67, 73], but has been proposed to act as a chaperon to stabilize or to assemble other β-crystallins [74]. The γ-crystallins are encoded by seven different genes, γA, γB, γC, γD, γE, γF, and γS, all encoding proteins of about 20 kDa. Nevertheless, only the γD, γC and γS crystallins are expressed at an appreciable concentration in human lenses [66].
Human γD-Crystallin Structure and Function
The human γD-crystallin (HγD) is the second most abundant protein of the lens nucleus (Ji 2013), and it is believed that their main function is to help maintaining the optical properties of the lens during the life span. Consequently, the γD-crystallins have evolved to be stable, soluble at elevated concentrations and damage tolerant.
HγD is a monomeric protein with 173 amino acids. It is composed of two domains: N and C-terminal domain connected by a short linker (Fig. 2). Its structure has been resolved by X-ray diffraction [75]. It folds into two Greek key motifs with eight β-strands characterized by an unusual folded β-hairpin (Fig. 2).
Some of the features that seem to confer stability to the protein include six pair of aromatic residues distributed all over the protein (F11/Y6, Y16/Y28, Y50/Y45, Y92/Y97, Y138/y133, F117/F115) [76], a group of hydrophobic and polar residues in the inter-face of the two domains [77] and two “tyrosine corners”, a classic characteristic of the Greek key motifs [78]. This motif is formed in the N-terminal domain with tyrosine 62 and in the C-terminal domain with tyrosine 150, and it connects two β-strands by a hydrogen bond between the hydroxyl group of the tyrosine and a carboxyl group [79]. Interestingly, HγD have six cysteines, more than any of the α and β-crystallins, but does not have any disulphide bond [80].
While the UV-damage protection is conferred by four buried tryptophan: W42 and W68 in the N-terminal domain, and W130 and W156 in the C-terminal domain, these tryptophan are highly conserved among vertebrates [6] and are important in the stability of the protein by dispersing the UV radiation [16, 81]. The conformation of the tryptophans seems to enable the lens to be a very effective UV filter, and their efficient quenching of the radiation provides an excellent mechanism to prevent photochemical degradation [82].
Although, this protein is extremely stable, over the years the protection mechanism loses efficiency and the protein accumulates damages. Some of the post-translational modifications of γD-crystallins include deamidation of Q12, N49 and N160 [83, 84], Y45 and W156 oxidation [83, 85], C110 methylation [20], G1 carbamylation [20, 84], and C18-C32 and C108-C110 disulfide binding [11]. All of these major modifications become more important with aging, and are considered to be the first step in cataract development [12].
Unfolding: Aggregation
As in many other protein folding diseases, it is believed that a partially unfolded intermediate produces the formation of the aggregates that lead to cataracts . Consequently, the aggregation pathway for the HγD-crystallin has been extensively studied. By using equilibrium temperature and chemical unfolding, it was found that the HγD-crystallin is stable to 8 M urea and has a Tm close to 80 °C. In order to unfold the protein it was necessary to use GuHCI at 37 °C [86]. A very useful feature of the HγD is that the florescence is shifted between the native fold at 325 nm and the unfolded state at 348 nm. Mostly, the unfolded experiments were done going from a native conditions to a high level of denaturant, usually 5.5 M GuHCL at 37 °C. For the native protein the unfolding curve showed, apparently, a single major unfolding transition [86]; later it was found by kinetic analysis in triple mutants the existence of a partially unfolded intermediate [87], and it was confirmed that the native unfolding curve was better adjusted by a three state model [88]. The first unfolding event consists in the unfolding of the N-terminal domain, intermediately followed by the unfolding of the C-terminal domain. Even though the state with one domain structured and the other one unfolded is a short live state in the native, it has been proposed as a good candidate for the aggregation intermediate in the cataract formation (Fig. 3).
There has been several stability/unfolding studies of mutants proteins, mainly divided in two types: mutations to change the stability elements of the protein and mutations that mimic some protein damage observed in in vivo experiments. In the first group, there are reports for the mutations of the conserved aromatic pairs in the protein F11/Y6, Y16/Y28, Y50/Y45, Y92/Y97, Y138/Y133, F117/F115 [76], mutations of the four internal tryptophans W42,W68/W130/W156, mutations of residues in the protein interface (Q54, Q143, and R79, M147) [88] among others. Meanwhile, in the second group, most of the mutations evaluated have been a single mutation that has been reported in cataracts studies. For instance, the genetic studies of families exhibiting juvenile-onset cataracts R114, R38, and R36 [24, 25], possible glutamine deamidation sites Q54, Q143 [89], deletion mutant W156X [90], R140, A36 [91], among others.
Most of the mutations can be classified according to where the mutation occurred: the N-domain, the interface or the C-domain. In general, N-terminal domain mutations shifted the first transition to lower denaturan concentration without affecting the C-terminal domain. The lower stability of the first unfolding event, in many cases, populated more this intermediate state and clearly presented a three unfolding curve [76], whereas mutation in the C-domain did not usually affect the first unfolding event or the shape of the curve. The mutations seems to destabilize the two domains in a more cooperative way [76].
Finally, the mutations in the interface produce a destabilization of the N-terminal and reveal a clear plateau in the unfolding curves [88, 89]. And, at the same time, they affect the N-terminal domain folding but not the C-terminal domain, suggesting that the interface could function as a scaffold for the folding of the N-terminal domain [88]. Many of these mutations studied would, consequently, effectively increase the life span of the partially unfolded conformer. Interestingly, many of the observed cataract point mutations in vivo cluster in the N-terminal domain.
It has been also studied the unfolding of the protein due to external factors. For instance, by using UV radiation, depending on the exposition time, protein aggregation has been observed [1, 92], as well as several damages from affecting specific residues to complete cleavage of the backbone [93]. It is worth to notice that out of the four internal tryptophan, it was reported that W42 is the more easily affected by UV radiations [94]. As a different external factor, the protein has been exposed to acidic pHs, and the formation of amyloid fibril was observed in these conditions (Fig. 3) [95].
Ultimately, the unfolding processes have been studied by molecular simulation in silico. In this type of studies, it has also been observed the preferential unfolding of the N-terminal domain, due to urea, temperature or mutations [96, 97]. Also it was proposed that the N-terminal domain stability is regulated by the inter-domain interaction. In simulations were the four internal tryptophan were changed to kynurenine simulating UV damage, it was found that both domain unfold faster and not sequentially. This suggests that, if the UV radiation is such that it makes this damage to any of the four tryptophans, the domain is going to unfold [16]. Also by simulation, the formation of a swap dimer was observed (Fig. 3) [96].
Inhibition
As mentioned before, cataracts is the main cause of blindness in the world [9], and while surgical removal of lens is effective, it is also expensive and is not available for all persons in developing countries. Hence, a search of a preventive treatment remains a key aspect in the research related to this disease.
Many different compounds have been studied in order to measure their anti-cataractogenic ability (Fig. 4). Several small molecules have been tested to prevent cataract formation due to external factors. For instance, caffeine was reported as an effective compound to prevent damage of lens by UV radiation [48]. The synthesis of bifunctional antioxidant with radical scavenging and chelation ability was found to delay the opacity of lenses exposed to gamma radiation and delay reactive oxygen species [56].
Nevertheless, most of the studies have focused in the inhibition of the factor responsible of producing cataracts . For instance, it has been reported that byakangelicin, the principal component of roots of Angelica dahurics, suppress sorbitol accumulation and galactose-induced cataract [98], citric acid inhibits the progression of cataracts in diabetics rat [99], and caffeine inhibits the oxidative stress in the lens [48].
In diabetic mouse models, there has been several reports of molecules studied to prevent cataracts . It was first tested the inhibitory effect of aspirin [100], then better results were obtained by combining aspirin and carnosine eye drops [101]. Vitamin K was showed to be effective to keep Ca2+ ATPase activity and lens calcium homeostasis resulting in an inhibition of diabetic cataractogenesis [57]. Similarly, magnesium taurate treatment to galactose diabetic rats showed its ability for correcting the lenticular Ca2+/Mg2+ ratio [55]. Also, the aldose reductase has been a target for anticataract drug [31, 33].
There have been studies on inhibition of cataract formation by using several natural products, which are known to contain anti-oxidants (Table 2). The crude extract of plants Ocimum sanctum [110], Ginkgo biloba [112], and Adhatoda vasica [102], have been tested to inhibit the polyol accumulations, oxidative stress and aldose reductase activity in animal models. Flavonoid fractions of Vitex negundo present an increase effect in the enzymatic activity of superoxide dismutase, glutathione peroxidase and catalase [29]. Other molecules tested include flavonoids isolated from honey [113] and egalic acid [30].
Meanwhile, in studies in vitro, the search of cataract inhibition focuses in molecules that present an effect in the native γ-crystallin or the partially folded intermediaries. Making use of spectroscopic techniques, the ability of sodium citrate to interact with human wild type and mutants γD-crystallin was tested, showing that the molecule interacts with unfolding intermediates, and promotes stabilizing interactions [114]. While sodium 4-phenyl butyrate increments the solubility of a truncated γD-crystallin mutant [115] and pantethine stops the aggregation in solution and reduces the phase separation temperature [116]. For aggregation induced by UV light, resveratrol inhibits the aggregation [117] and carnosine inhibits the induced degradation [118].
Perspectives
Crystallins are not regenerated in the lens during the organism lifetime, therefore, they have to remain unchanged during aging in order to not affect the lens transparency. When different factors affect the protein, cataracts are formed. The understanding of the conformational changes that γ-crystallins suffer during the cataracts development is necessary in order to get structural information that would allow the development of treatment strategies different than the surgical removal. In spite of the multiple compounds that have been studied as potential drugs for cataracts, there is not a potential preventive molecule for the inhibition of aggregation of crystallins. The study of inhibitors previously related to or associated with other misfolding protein aggregation diseases may be a (valuable) option for testing new compounds.
References
Schafheimer N, Wang Z, Schey K, King J (2014) Tyrosine/cysteine cluster sensitizing human γD-crystallin to ultraviolet radiation-induced photoaggregation in vitro. Biochemistry 53:979–990. doi:10.1021/bi401397g
Sharma KK, Santhoshkumar P (2009) Lens aging: effects of crystallins. Biochim Biophys Acta 1790:1095–1108. doi:10.1016/j.bbagen.2009.05.008
Bassnett S (2002) Lens organelle degradation. Exp Eye Res 74:1–6. doi:10.1006/exer.2001.1111
Bassnett S (2009) On the mechanism of organelle degradation in the vertebrate lens. Exp Eye Res 88:133–139. doi:10.1016/j.exer.2008.08.017
Kyselova Z (2011) Mass spectrometry-based proteomics approaches applied in cataract research. Mass Spectrom Rev 30:1173–1184. doi:10.1002/mas.20317
Bloemendal H, de Jong W, Jaenicke R et al (2004) Ageing and vision: structure, stability and function of lens crystallins. Prog Biophys Mol Biol 86:407–485. doi:10.1016/j.pbiomolbio.2003.11.012
Slingsby C, Wistow GJ, Clark AR (2013) Evolution of crystallins for a role in the vertebrate eye lens. Protein Sci 22:367–380. doi:10.1002/pro.2229
Benedek GB (1971) Theory of transparency of the eye. Appl Opt 10:459–473. doi:10.1364/AO.10.000459
Fraile García E (2014) Causas de Ceguera en el Mundo: distribución geográfica y relación con el medio socio-económico
Hains PG, Truscott RJW (2007) Post-translational modifications in the nuclear region of young, aged, and cataract human lenses. J Proteome Res 6:3935–3943. doi:10.1021/pr070138h
Hanson SR, Hasan A, Smith DL, Smith JB (2000) The major in vivo modifications of the human water-insoluble lens crystallins are disulfide bonds, deamidation, methionine oxidation and backbone cleavage. Exp Eye Res 71:195–207. doi:http://dx.doi.org/10.1006/exer.2000.0868
Hanson SR, Smith DL, Smith JB (1998) Deamidation and disulfide bonding in human lens gamma-crystallins. Exp Eye Res 67:301–312. doi:10.1006/exer.1998.0530
Chiou SH, Chylack LT, Tung WH, Bunn HF (1981) Nonenzymatic glycosylation of bovine lens crystallins. Effect of aging. J Biol Chem 256:5176–5180
Ajaz MS, Ma Z, Smith DL, Smith JB (1997) Size of human lens β-crystallin aggregates are distinguished by N-terminal truncation of βB1. J Biol Chem 272:11250–11255. doi:10.1074/jbc.272.17.11250
Wang SS-S, Wen W-S (2010) Examining the influence of ultraviolet C irradiation on recombinant human γD-crystallin. Mol Vis 16:2777–2790
Xia Z, Yang Z, Huynh T et al (2013) UV-radiation induced disruption of dry-cavities in human γD-crystallin results in decreased stability and faster unfolding. Sci Rep 3:1560. doi:10.1038/srep01560
Moreau KL, King JA (2012) Cataract-causing defect of a mutant γ-crystallin proceeds through an aggregation pathway which bypasses recognition by the α-crystallin chaperone. PLoS One 7(5):e37256. doi:10.1371/journal.pone.0037256
Truscott RJW (2005) Age-related nuclear cataract-oxidation is the key. Exp Eye Res 80:709–725. doi:10.1016/j.exer.2004.12.007
Stacy RAH, David LS, Smith JB (1998) Deamidation and disulfide bonding in human lens γ-crystallins. Exp Eye Res 67:301–312
Lapko VN, Smith DL, Smith JB (2003) Methylation and carbamylation of human gamma-crystallins. Protein Sci 12:1762–1774. doi:10.1110/ps.0305403
Borkman F (1990) Mechanism of photochemically protein produced solutions in lens. Exp Eye Res 51:663–669
Stephan DA, Gillanders E, Vanderveen D et al (1999) Progressive juvenile-onset punctate cataracts caused by mutation of the γD-crystallin gene. Proc Natl Acad Sci U S A 96:1008–1012
Mackay DS, Andley UP, Shiels A (2004) A missense mutation in the γD crystallin gene (CRYGD) associated with autosomal dominant “coral-like” cataract linked to chromosome 2q. Mol Vis 10:155–162
Kmoch S, Brynda J, Asfaw B et al (2000) Link between a novel human gammaD-crystallin allele and a unique cataract phenotype explained by protein crystallography. Hum Mol Genet 9:1779–1786. doi:10.1093/hmg/9.12.1779
Héon E, Priston M, Schorderet DF et al (1999) The γ-crystallins and human cataracts: a puzzle made clearer. Am J Hum Genet 65:1261–1267. doi:10.1086/302619
Gopinath PM, Löster J, Graw J (2002) Novel mutations in the γ-crystallin genes cause autosomal dominant congenital cataracts. J Med Genet 39:352–358
Kolozsvári L, Nógrádi A, Hopp B, Bor Z (2002) UV absorbance of the human cornea in the 240- to 400-nm range. Invest Ophthalmol Vis Sci 43:2165–2168
Truscott RJ, Wood AM, Carver JA et al (1994) A new UV-filter compound in human lenses. FEBS Lett 348:173–176. doi:10.1016/0014-5793(94)00601-6
Rooban BN, Lija Y, Biju PG et al (2009) Vitex negundo attenuates calpain activation and cataractogenesis in selenite models. Exp Eye Res 88:575–582. doi:10.1016/j.exer.2008.11.020
Sakthivel M, Elanchezhian R, Ramesh E et al (2008) Prevention of selenite-induced cataractogenesis in Wistar rats by the polyphenol, ellagic acid. Exp Eye Res 86:251–259. doi:10.1016/j.exer.2007.10.016
Patel PM, Jivani N, Malaviya S et al (2012) Cataract: a major secondary diabetic complication. Int Curr Pharm J 1:180–185. doi:10.3329/icpj.v1i7.10813
Ponce A, Sorensen C, Takemoto L (2006) Role of short-range protein interactions in lens opacifications. Mol Vis 12:879–884. doi:v12/a99 [pii]
Esteves JF, Dal Pizzol MM, Sccoco CA et al (2008) Cataract and type 1 diabetes mellitus. Diabetes Res Clin Pract 82:324–328. doi:10.1016/j.diabres.2008.08.023
Jung HA, Islam MDN, Kwon YS et al (2011) Extraction and identification of three major aldose reductase inhibitors from Artemisia montana. Food Chem Toxicol 49:376–384. doi:10.1016/j.fct.2010.11.012
Stefek M (2011) Natural flavonoids as potential multifunctional agents in prevention of diabetic cataract. Interdiscip Toxicol 4:69–77. doi:10.2478/v10102-011-0013-y
Biswas S, Harris F, Dennison S et al (2004) Calpains: targets of cataract prevention? Trends Mol Med 10:78–84. doi:10.1016/j.molmed.2003.12.007
Dilsiz N, Olcucu ALI, Atas M (1999) Determination of calcium, sodium, potassium and magnesium concentrations in human senile cataractous lenses. Cell Biochem Funct 18:259–262
Nagai N, Fukuhata T, Ito Y (2007) Effect of magnesium deficiency on intracellular ATP levels in human lens epithelial cells. Biol Pharm Bull 30:6–10. doi:10.1248/bpb.30.6
Ji F, Jung J, Gronenborn AM (2012) Structural and biochemical characterization of the childhood cataract-associated R76S mutant of human γD-crystallin. Biochemistry 51:2588–2596. doi:10.1021/bi300199d
Hirsch RP, Schwartz B (1983) Increased mortality among elderly patients undergoing cataract extraction. Arch Ophthalmol 101:1034–1037. doi:10.1001/archopht.1983.01040020036004
Toh T, Morton J, Coxon J, Elder MJ (2007) Medical treatment of cataract. Clin Experiment Ophthalmol 35:664–671. doi:10.1111/j.1442-9071.2007.01559.x
Wu K, Shui YB, Kojima M et al (1997) Location and severity of UVB irradiation damage in the rat lens. Jpn J Ophthalmol 41:381–387
Wegener AR (1994) In vivo studies on the effect of UV-radiation on the eye lens in animals. Doc Ophthalmol 88:221–232. doi:10.1007/BF01203676
Zhang J, Yan H, Löfgren S et al (2012) Ultraviolet radiation-induced cataract in mice: the effect of age and the potential biochemical mechanism. Invest Ophthalmol Vis Sci 53:7276–7285. doi:10.1167/iovs.12-10482
Graw J (2009) Mouse models of cataract. J Genet 88:469–486. doi:10.1007/s12041-009-0066-2
Wolf N, Penn P, Pendergrass W et al (2005) Age-related cataract progression in five mouse models for anti-oxidant protection or hormonal influence. Exp Eye Res 81:276–285. doi:10.1016/j.exer.2005.01.024
Marsili S, Salganik RI, Albright CD et al (2004) Cataract formation in a strain of rats selected for high oxidative stress. Exp Eye Res 79:595–612. doi:10.1016/j.exer.2004.06.008
Varma SD, Hegde KR, Kovtun S (2010) Inhibition of selenite-induced cataract by caffeine. Acta Ophthalmol 88:245–249. doi:10.1111/j.1755-3768.2010.02014.x
Ostadalova I, Babický A, Odenberger J (1978) Cataract induced by administration of a single dose of sodium selenite to suckling rats. Experientia 15:222–223
Shearer TR, Ma H, Fukiage C, Azuma M (1997) Selenite nuclear cataract: review of the model. Mol Vis 3:8
Srivastava SK, Ramana KV, Bhatnagar A (2005) Role of aldose reductase and oxidative damage in diabetes and the consequent potential for therapeutic options. Endocr Rev 26:380–392. doi:10.1210/er.2004-0028
Liu XY, Dangel AW, Kelley RI et al (1999) The gene mutated in bare patches and striated mice encodes a novel 3β-hydroxysteroid dehydrogenase. Nat Genet 22:182–187
Sheets NL, Chauhan BK, Wawrousek E et al (2002) Cataract and lens specific upregulation of ARK receptor tyrosine kinase in emory mouse cataract. Invest Ophthalmol Vis Sci 43:1870–1875
Gao X, Wang W, Wei S, Li W (2009) Review of pharmacological effects of Glycyrrhiza radix and its bioactive compounds. Zhongguo Zhong Yao Za Zhi 34:2695–2700. doi:10.1002/ptr
Agarwal R, Iezhitsa I, Awaludin NA et al (2013) Effects of magnesium taurate on the onset and progression of galactose-induced experimental cataract: in vivo and in vitro evaluation. Exp Eye Res 110:35–43. doi:10.1016/j.exer.2013.02.011
Randazzo J, Zhang P, Makita J et al (2011) Orally active multi-functional antioxidants delay cataract formation in streptozotocin (type 1) diabetic and gamma-irradiated rats. PLoS One 6:e18980. doi:10.1371/journal.pone.0018980
Sai Varsha MKN, Raman T, Manikandan R (2014) Inhibition of diabetic-cataract by vitamin K1 involves modulation of hyperglycemia-induced alterations to lens calcium homeostasis. Exp Eye Res 128:73–82. doi:10.1016/j.exer.2014.09.007
Bloemendal H (1982) Lens proteins. CRC Crit Rev Biochem 12:1–38
Graw J (2009) Genetics of crystallins: cataract and beyond. Exp Eye Res 88:173–189. doi:10.1016/j.exer.2008.10.011
Groenen PJTA, Merck KB, De Jong WW, Bloemendal H (1994) Structure and modifications of the junior chaperone γ-crystallin—from lens transparency to molecular pathology. Eur J Biochem 225:1–19. doi:10.1111/j.1432-1033.1994.00001.x
Sun TX, Liang JJN (1998) Intermolecular exchange and stabilization of recombinant human αA- and αB-crystallin. J Biol Chem 273:286–290. doi:10.1074/jbc.273.1.286
Derham BK, Harding JJ (1999) Alpha-crystallin as a molecular chaperone. Prog Retin Eye Res 18:463–509. doi:S1350946298000305
Horwitz J (1992) Alpha-crystallin can function as a molecular chaperone. Proc Natl Acad Sci U S A 89:10449–10453. doi:10.1073/pnas.89.21.10449
Horwitz J (2003) Alpha-crystallin. Exp Eye Res 76:145–153. doi:10.1016/S0014-4835(02)00278-6
Sun Y, MacRae TH (2005) Small heat shock proteins: molecular structure and chaperone function. Cell Mol Life Sci 62:2460–2476. doi:10.1007/s00018-005-5190-4
Andley UP (2007) Crystallins in the eye: function and pathology. Prog Retin Eye Res 26:78–98. doi:10.1016/j.preteyeres.2006.10.003
Bateman OA, Sarra R, Van Genesen ST et al (2003) The stability of human acidic β-crystallin oligomers and hetero-oligomers. Exp Eye Res 77:409–422. doi:10.1016/S0014-4835(03)00173-8
Fu L, Liang JJ-N (2002) Unfolding of human lens recombinant βB2- and γC-crystallins. J Struct Biol 139:191–198. doi:S1047847702005452
Berbers GA, Hoekman WA, Bloemendal H et al (1984) Homology between the primary structures of the major bovine beta-crystallin chains. Eur J Biochem 139:467–479. doi:10.1111/j.1432-1033.1984.tb08029.x
Lampi KJ, Ma Z, Shih M et al (1997) Sequence analysis of betaA3, betaB3, and betaA4 crystallins completes the identification of the major proteins in young human lens. J Biol Chem 272:2268–2275
Downard KM, Kokabu Y, Ikeguchi M, Akashi S (2011) Homology-modelled structure of the βb2B3-crystallin heterodimer studied by ion mobility and radical probe MS. FEBS J 278:4044–4054. doi:10.1111/j.1742-4658.2011.08309.x
Van Montfort RLM, Bateman OA, Lubsen NH, Slingsby C (2003) Crystal structure of truncated human betaB1-crystallin. Protein Sci 12:2606–2612. doi:10.1110/ps.03265903.The
Dolinska MB, Sergeev YV, Chan MP et al (2009) N-terminal extension of βB1-crystallin: identification of a critical region that modulates protein interaction with βA3-crystallin. Biochemistry 48:9684–9695. doi:10.1021/bi9013984
Marín-Vinader L, Onnekink C, Van Genesen ST et al (2006) In vivo heteromer formation. Expression of soluble βA4-crystallin requires coexpression of a heteromeric partner. FEBS J 273:3172–3182. doi:10.1111/j.1742-4658.2006.05326.x
Basak A, Bateman O, Slingsby C et al (2003) High-resolution X-ray crystal structures of human γD crystallin (1.25Å) and the R58H mutant (1.15Å) associated with aculeiform cataract. J Mol Biol 328:1137–1147. doi:10.1016/S0022-2836(03)00375-9
Kong F, King J (2011) Contributions of aromatic pairs to the folding and stability of long-lived human γD-crystallin. Protein Sci 20:513–518. doi:10.1002/pro.583
Slingsby C, Wistow GJ (2014) Functions of crystallins in and out of lens: roles in elongated and post-mitotic cells. Prog Biophys Mol Biol 115:52–67. doi:10.1016/j.pbiomolbio.2014.02.006
Hemmingsen JM, Gernert KM, Richardson JS, Richardson DC (1994) The tyrosine corner: a feature of most Greek key beta-barrel proteins. Protein Sci 3:1927–1937. doi:10.1002/pro.5560031104
Hamill SJ, Cota E, Chothia C, Clarke J (2000) Conservation of folding and stability within a protein family: the tyrosine corner as an evolutionary cul-de-sac. J Mol Biol 295:641–649. doi:10.1006/jmbi.1999.3360
Spector A, Roy D (1978) Disulfide-linked high molecular weight protein associated with human cataract. Proc Natl Acad Sci U S A 75:3244–3248
Chen J, Flaugh SL, Callis PR, King J (2006) Mechanism of the highly efficient quenching of tryptophan fluorescence in human γD-crystallin. Biochemistry 45:11552–11563. doi:10.1021/bi060988v
Chen J, Toptygin D, Brand L, King JA (2008) Mechanism of the efficient tryptophan fluorescence quenching in human gammaD-crystallin studied by time-resolved fluorescence. Biochemistry 47(40):10705–10721
Searle BC, Dasari S, Wilmarth PA et al (2005) Identification of protein modifications using MS/MS de novo sequencing and the OpenSea alignment algorithm. J Proteome Res 4:546–554. doi:10.1021/pr049781j
Wilmarth PA, Tanner S, Dasari S et al (2006) Age-related changes in human crystalline determined from comparative analysis of post-translational modifications in young and aged lens: does deamidation contribute to crystallin insolubility? J Proteome Res 5:2554–2566. doi:10.1021/pr050473a
MacCoss MJ, McDonald WH, Saraf A et al (2002) Shotgun identification of protein modifications from protein complexes and lens tissue. Proc Natl Acad Sci U S A 99:7900–7905. doi:10.1073/pnas.122231399
Kosinski-Collins MS, King JA (2003) In vitro unfolding, refolding, and polymerization of human gammaD crystallin, a protein involved in cataract formation. Protein Sci 12:480–490. doi:10.1110/ps.0225503
Kosinski-collins MS, Flaugh SL (2004) Probing folding and fluorescence quenching in human γD crystallin Greek key domains using triple tryptophan mutant proteins. Protein Sci 13(8):2223–2235. doi:10.1110/ps.04627004
Flaugh SL, Kosinski-Collins MS, King JA (2005) Interdomain side-chain interactions in human gammaD crystallin influencing folding and stability. Protein Sci 14:2030–2043. doi:10.1110/ps.051460505
Flaugh SL, Mills IA, King J (2006) Glutamine deamidation destabilizes human γD-crystallin and lowers the kinetic barrier to unfolding. J Biol Chem 281:30782–30793. doi:10.1074/jbc.M603882200
Talla V, Srinivasan N, Balasubramanian D (2008) Visualization of in situ intracellular aggregation of two cataract-associated human γ-crystallin mutants: lose a tail, lose transparency. Invest Ophthalmol Vis Sci 49:3483–3490. doi:10.1167/iovs.07-1114
Vendra VPR, Balasubramanian D (2010) Structural and aggregation behavior of the human γD-crystallin mutant E107A, associated with congenital nuclear cataract. Mol Vis 16:2822–2828
Schafheimer N, King J (2013) Tryptophan cluster protects human γD-crystallin from ultraviolet radiation-induced photoaggregation in vitro. Photochem Photobiol 89:1106–1115. doi:10.1111/php.12096
Moran SD, Zhang TO, Decatur SM, Zanni MT (2013) Amyloid fiber formation in human γ D-crystallin induced by UV-B photodamage. Biochemistry 52(36):6169–6181
Ji F, Jung J, Koharudin LMI, Gronenborn AM (2013) The human W42R γD-crystallin mutant structure provides a link between congenital and age-related cataracts. J Biol Chem 288:99–109. doi:10.1074/jbc.M112.416354
Wu JW, Chen M, Wen W et al (2014) Comparative analysis of human γD-crystallin aggregation under physiological and low pH conditions. PLoS One 9(11):e112309. doi:10.1371/journal.pone.0112309
Das P, King JA, Zhou R (2011) Aggregation of γ-crystallins associated with human cataracts via domain swapping at the C-terminal β-strands. Proc Natl Acad Sci U S A 108:10514–10519. doi:10.1073/pnas.1019152108
Das P, King JA, Zhou R (2010) β-strand interactions at the domain interface critical for the stability of human lens γD-crystallin. Protein Sci 19:131–140. doi:10.1002/pro.296
Shin KHH, Lim SSS, Kim DKK (1998) Effect of byakangelicin, an aldose reductase inhibitor, on galactosemic cataracts, the polyol contents and Na+, K+ATPase activity in sciatic nerves of streptozotocin-induced diabetic rats. Phytomedicine 5:121–127. doi:10.1016/S0944-7113(98)80008-1
Nagai R, Nagai M, Shimasaki S et al (2010) Citric acid inhibits development of cataracts, proteinuria and ketosis in streptozotocin (type 1) diabetic rats. Biochem Biophys Res Commun 393:118–122. doi:10.1016/j.bbrc.2010.01.095
Swamy MS, Abraham EC (1989) Inhibition of lens crystallin glycation and high molecular weight aggregate formation by aspirin in vitro and in vivo. Invest Ophthalmol Vis Sci 30:1120–1126
Shi Q, Yan H, Li M, Harding JJ (2009) Effect of a combination of carnosine and aspirin eye drops on streptozotocin-induced diabetic cataract in rats. Mol Vis 15:2129–2138
Gacche RN, Dhole NA (2011) Aldose reductase inhibitory, anti-cataract and antioxidant potential of selected medicinal plants from the Marathwada region, India. Nat Prod Res 25:760–763. doi:10.1080/14786419.2010.536951
Dongare V, Kulkarni C, Kondawar M et al (2012) Inhibition of aldose reductase and anti-cataract action of trans-anethole isolated from Foeniculum vulgare Mill. fruits. Food Chem 132:385–390. doi:10.1016/j.foodchem.2011.11.005
Rathi SS, Grover JK, Vikrant V, Biswas NR (2002) Prevention of experimental diabetic cataract by Indian ayurvedic plant extracts. Phytother Res 777:774–777
Pastene E, Avello M, Letelier ME et al (2007) Preliminary studies on antioxidant and anti-cataract activities of Cheilanthes glauca (Cav.) Mett. through various in vitro models. Electron J Food Plants Chem 2:1–8
Vibin M, Siva Priya SG, N Rooban B et al (2010) Broccoli regulates protein alterations and cataractogenesis in selenite models. Curr Eye Res 35:99–107. doi:10.3109/02713680903428991
Suryanarayana P, Petrash JM (2004) Inhibition of aldose reductase by tannoid principles of Emblica officinalis: implications for the prevention of sugar cataract. Mol Vis 10:148–154
Shin KH, Chung MS, Cho TS (1994) Effects of Furanocoumarins from Angelica dahurica on aldose reductase and galactosemic cataract formation in rats. Arch Pharm Res 5:331–336
Lija Y, Biju PG, Reeni A et al (2006) Modulation of selenite cataract by the flavonoid fraction of Emilia sonchifolia in experimental animal models. Phytother Res 20(12):1091–1095. doi:10.1002/ptr
Halder N, Joshi S, Gupta SK (2003) Lens aldose reductase inhibiting potential of some indigenous plants. J Ethnopharmacol 86:113–116. doi:10.1016/S0378-8741(03)00052-7
Devi VG, Rooban BN, Sasikala V et al (2009) Toxicology in vitro Isorhamnetin-3-glucoside alleviates oxidative stress and opacification in selenite cataract in vitro. Toxicol In Vitro 24:1662–1669. doi:10.1016/j.tiv.2010.05.021
Ertekin MV, Koçer I, Karslioǧlu I et al (2004) Effects of oral Ginkgo biloba supplementation on cataract formation and oxidative stress occurring in lenses of rats exposed to total cranium radiotherapy. Jpn J Ophthalmol 48:499–502. doi:10.1007/s10384-004-0101-z
Vit P, Jacob TJ (2008) Putative anticataract properties of honey studied by the action of flavonoids on a lens culture model. J Heat Sci 54:196–202. doi:10.1248/jhs.54.196
Goulet DR, Knee KM, King JA (2011) Inhibition of unfolding and aggregation of lens protein human gamma D crystallin by sodium citrate. Exp Eye Res 93:371–381. doi:10.1016/j.exer.2011.04.011
Gong B, Zhang L, Lam DS et al (2010) Sodium 4-phenylbutyrate ameliorates the effects of cataract-causing mutant gammaD-crystallin in cultured cells. Mol Vis 16:997–1003
Friberg G, Pande J, Ogun O, Benedek GB (1996) Pantethine inhibits the formation of high-Tc protein aggregates in gamma B crystallin solutions. Curr Eye Res 15:1182–1190
Wu JW-RR, Kao C-YY, Lin LT-WW et al (2013) Human γD-crystallin aggregation induced by ultraviolet C irradiation is suppressed by resveratrol. Biochem Eng J 78:189–197. doi:10.1016/j.bej.2013.03.014
Liao J, Lin I, Huang K et al (2014) Carnosine ameliorates lens protein turbidity formations by inhibiting calpain proteolysis and ultraviolet C—induced degradation. J Agric Food Chem 62:5932–5938. doi:10.1021/jf5017708
Liem-The KN, Stols AL, Jap PH, Hoenders HJ (1975) X-ray induced cataract in rabbit lens. Exp Eye Res 20:317–328. doi:10.1016/0014-4835(75)90114-1
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this paper
Cite this paper
Rivillas-Acevedo, L., Fernández-Silva, A., Amero, C. (2015). Function, Structure and Stability of Human Gamma D Crystallins: A Review. In: Olivares-Quiroz, L., Guzmán-López, O., Jardón-Valadez, H. (eds) Physical Biology of Proteins and Peptides. Springer, Cham. https://doi.org/10.1007/978-3-319-21687-4_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-21687-4_5
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-21686-7
Online ISBN: 978-3-319-21687-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)