Abstract
In Korea, prostate cancer incidence has significantly increased in recent years. Prostate-specific antigen (PSA) is a marker for prostate cancer, and elevated serum PSA levels have been associated with prostate intraepithelial neoplasms. Meanwhile, metastasis is a process by which cancer spreads from the place at which it first arose as a primary tumor to distant locations in the body. The so-called tissue inhibitors of metalloproteinases (TIMPs), which are naturally occurring inhibitors of matrix metalloproteinases (MMPs), play an important role in the complex regulation of MMPs. They inhibit the catalytic activity of MMPs by binding to activated MMPs and control breakdown of extracellular matrix. Thus, the balance between MMPs and TIMPs plays a vital role in maintaining the integrity of healthy tissues, and MMP inhibitors, as well as TIMP activators, are expected to be useful chemotherapeutic agents for the treatment of malignancies. In addition, vascular endothelial growth factor (VEGF) plays an important role in prostate cancer invasion. VEGF is a signal protein produced by cells that stimulates vasculogenesis and angiogenesis. In the present study, therefore, we investigated the anti-prostate cancer metastasis effect of taurine, and proved taurine suppressed PSA and several metastasis-related genes in human prostate cancer cells, LNCaP and PC-3. In addition, taurine inhibited migration of LNCaP and PC-3.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
Taurine, 2-aminoethanesulfonic acid was first isolated more than 150 years ago from ox bile in 1827 by German scientists Friedrich Tiedemann and Leopold Gmelin (Tiedemann and Gmelin 1827). Taurine has been implicated in neuro-degenerative disease, antioxidant property, atherosclerosis and coronary heart disease (Olive 2002; Green et al. 1991; Zhang et al. 2004; Choi et al. 2006). Nevertheless, there aren’t many reports on anti-cancer property of taurine (Kirk and Kirk 1993; Yanagita et al. 2008; Chatzakos et al. 2012).
Prostate cancer is the most frequent malignancy in men reaching $8 billion in expenses with an average cost of $81,658 per patient, from diagnosis till death in the US alone (Racioppi et al. 2012; Klein and Thompson 2012) with ~350,000 new cases diagnosed annually in Europe (Siegel et al. 2012; Jemal et al. 2009). Prostate cancer is also the most common cancer in developed world with increasing rates in the developing world (Baade et al. 2009). Over the last 25 years, the number of men diagnosed with prostate cancer each year has increased by 30 % (Wingo et al. 2003). Therefore, a number of agents are currently being investigated for the prevention of prostate cancer (Klein and Thompson 2012).
Prostate specific antigen (PSA), an enzyme of 30 kDa grouped in the kallikrein family and also known as kallikrein-related peptidase 3 (KLK3) is synthesized to high levels by normal and malignant prostate epithelial cells. Therefore, it is the key biomarker currently applied for early diagnosis of prostate cancer (Luigi et al. 2014). The ability of PSA to process a number of growth regulatory proteins that are important in cancer growth and survival (such as insulin-like growth factor binding protein, parathyroid hormone-related protein, latent transforming growth factor-beta 2 as well as extracellular matrix components, like fibronectin and laminin) (Cohen et al. 1992; Iwamura et al. 1996), indeed PSA can facilitate tumor growth and metastasis dissemination (Williams et al. 2007; Webber et al. 1995).
The tumor metastasis is associated with a multigene and multistep process with the participation of various metastasis-related genes. Degradation of the j matrix (ECM) by MMPs is an essential mechanism in tumor metastasis. Studies have revealed that MMPs are the common and crucial target effectors for many oncogenes and tumor suppressor genes facilitating tumor metastasis (Shuman Moss et al. 2012). MMP9, a key member of the MMPs, plays a vital role in cancer metastasis process. In addition, angiogenesis is also required for formation of tumor metastasis. Tumors that have become neovascularized often express increased levels of proangiogenic proteins, such as VEGF. However, to the best of our knowledge, there is no scientific report for PSA, MMP9 and VEGF. In the present study, therefore, we investigated the effects of taurine on PSA, MMPs and VEGF expression in vitro using human prostate cancer cells, LNCaP and PC-3.
2 Methods
2.1 Materials
LNCaP, androgen-dependent human prostate cancer cells were obtained from Korean Cell Line Bank (Seoul, Korea; KCLB numbers: 21740). Taurine and DHT (dihydrotestosterone) were purchased from Sigma (St. Louis, MO, USA). Antibodies for primary antibodies and the peroxidase-conjugated secondary antibodies were purchased from Santa Cruz Biotechnology Inc. (Santa Cruz, CA, USA).
2.2 Cell Culture
The human prostate cancer cell line, LNCaP and PC-3 were cultured in RPMI 1640 medium, supplemented with 10 % FBS, 1 % penicillin/streptomycin in a 5 % CO2 atm at 37 °C. The cells were seeded at a density of 3.5 × 105 cells well in a 13 cm well culture dish. After 24 h, the cells were treated with 0.125, 0.250, 0.500, and 1.000 mM of taurine in medium. Cells were treated with taurine for 24 h and then harvested.
2.3 Cell Viability
Cell viability was determined by 3-(4,5-dimethylthiazol-2yl)-2,5-diphenyl-tetrazolium bromide (MTT) assay in 96-well plates as previously described. Cells were incubated with various concentrations of taurine for 48 h followed by MTT for 4 h, and then 100 μL of isopropanol (in 0.04 N-hydrochloric acid) was added to dissolve the formazan crystals. The absorbance was read at 570 nm using the Anthos 2010 spectrophotometer (Salzburg, Austria). Cell viability was calculated as being the relative absorbance compared to control (Kim et al. 2002).
2.4 Gap Closure Cell Migration Assay
Radius™ 24-well cell migration assay originated from Cell Biolabs, Inc (San Diego, USA). To determine which wells would be assayed, 500 μl of Radius™ gel pretreatment solution was slowly added to each well by careful pipetting down the wall of the well. The plate was covered and incubated at room temperature for 20 min. Radius™ gel pretreatment solution was carefully aspirated from the wells, 500 μl of Radius™ wash solution was added to each well. The cells were harvested and resuspended in culture medium at 0.2 × 106 cell/ml. Radius™ wash solution was carefully aspirated from the wells, 500 μl of the cell suspension was added to each well by careful pipetting down the wall of the well. The plate was transferred the to a cell culture incubator for 24 h to allow firm attachment. After 24 h, the media from each well were aspirated and washed three times with 0.5 ml of fresh medium. Sufficient 1× Radius™ gel removal solution was prepared for all wells by diluting the stock 1:100 in culture medium. The media were aspirated from the wells and 0.5 ml of 1× Radius™ gel removal solution was added to each well and washed three times with 0.5 ml of fresh medium. After the final washing was complete, 1 ml of complete medium and taurine were added to each well, and a photo was taken on 0 h, 8 h, 24 h and 48 h, respectively. To compare the differences in migratory gap, images were captured at the same size, and gap closure was determined after the indicated times (0, 8, 24 and 48 h) using CellProfiler™ software (Broad Institute, MA, USA).
2.5 Western Blot
After the indicated treatments, cells were harvested in PBS and lysed in RIPA buffer (150 mM NaCl, 0.5 % deoxycholate, 0.1 % nonidet P-40, 0.1 % SDS and 50 mM Tris) containing protease inhibitors (50 mg/ml phenylmethylsulfonyl fluoride, 10 mg/ml aprotinin, 5 mg/ml leupeptin, 0.1 mg/ml NaF, 1 mM DTT, 0.1 mM sodium orthovanadate and 0.1 mM b-glycerophosphate). Total cellular proteins were quantified by the Bradford procedure and equal amounts of proteins were mixed with loading buffer (25 % glycerol, 0.075 % SDS, 1.25 ml of 14.4 M 2-mercaptoethanol, 10 % bromophenol blue and 3.13 % stacking gel buffer) and fractionated by gel electrophoresis on gradient gels (Novex, CA, USA). Rainbow marker (Novex, CA, USA) was used as the molecular weight standard. Proteins were transferred to nitrocellulose membranes (Novex, CA, USA) and blocked for 1.5 h with clear milk (Thermo Scientific, IL, USA). Blots were subsequently incubated with primary antibodies in 1× TBST for 1.5 h. Goat anti-rabbit or goat anti-mouse horseradish peroxidase conjugated secondary antibodies (Santa Cruz Biotechnology, TX, USA) were used at 1:5,000 dilution in 1× TBST. Blots were treated with Western Lightning Western Blot Chemiluminescence Reagent (Advansta, CA, USA) and the proteins were detected by autoradiography (Fujifilm, Japan). Equal protein loading was ascertained by β-actin bodies.
2.6 Statistical Analysis
All data are presented using the mean ± SE and the data sourced from at least three experiments. Statistical analyses were performed using SAS statistical software (SAS Institute, Cary, NC, USA). Treatment effects were analyzed using one-way analysis of variance, followed by Dunnett’s multiple range tests. For the results p < 0.05 was used to indicate significance.
3 Results
3.1 The Effect of Taurine on Viability of Human Prostate Cancer Cells
The antiproliferative activity of taurine was evaluated using MTT assay. As shown in Fig. 1, taurine significantly stimulated prostate cancer cells death in a dose-dependent manner at concentrations of 0.125–1.0 mM. We omitted 1.0 mM from the results, which showed 30 % below cell viability from the next experiments.
Cell viability analysis of taurine on human prostate cancer cells, LNCaP (a) and PC-3 (b). Prostate cancer cells were incubated with various concentrations of taurine for 48 h followed by MTT for 4 h, and then 100 μl of isopropanol was added to dissolve the formazan crystals. Each value represents the mean ± SEM. Values not sharing a common letter are significantly different at P < 0.05 by Dunnett’s multiple range tests
3.2 The Effect of Taurine on Human Prostate Cancer Cells Migration
To examine the effect of taurine on cell migration, we performed gap closure assay using a Radius™ 24 well. To compare the differences in migratory gap, images were captured at the same size, and gap closure was determined after the indicated times (0, 8, 24 and 48 h) compared to control and DHT group. In LNCaP cells, after 48 h, the gap was closed in approximately 50 % in DHT-treated cells (Fig. 2a). In addition, in PC-3 cells, after 8 h, the gap was closed in approximately 60 % in DHT-treated cells (Fig. 2b). As shown in Fig. 2, taurine significantly reduced cell motility, compared with DHT alone-treated cells in both LNCaP and PC-3 cells.
The effect of taurine on the gap closure ability in human prostate cancer cells, LNCaP (a) and LNCaP (b). Allowed to grow for indicated time in the presence or absence of DHT and different concentrations of taurine. The gap covered by the cells was measured by CellProfiler™. The gap represents the mean of three individual experiments performed in triplicate. *P < 0.05, statistical significance compared with DHT alone-treated cells
3.3 The Effect of Taurine on the Expression of PSA and Migration-Related Genes
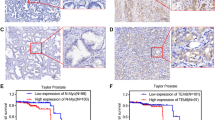
First, protein expression of PSA was investigated by Western blot after treatment with DHT (1 nM) for 48 h. Treatment of LNCaP cells with taurine significantly decreased PSA expression (Fig. 3a, b). Treatment of PC-3 cells with taurine significantly decreased PSA expression (Fig. 3f, g). In addition, migration related genes were also estimated. As shown in Fig. 3a–c, taurine significantly suppressed protein expression of MMP-9 in a dose-dependent fashion in LNCaP cells. Moreover, TIMP-1 and TIMP-2 which are naturally occurring inhibitors of MMP-9, significantly and dose-dependently increased the protein expressions in taurine-treated cells in LNCaP (Fig. 3a, d, e). These data suggest that taurine suppresses the migratory condition by regulating the levels of TIMP-1 and TIMP-2 in androgen-dependent human prostate cancer cells, LNCaP. In addition, Treatment of PC-3 cells with taurine significantly decreased PSA expression (Fig. 3f, g). Moreover, VEGF which is considered to be the main factor promoting angiogenesis was significantly and dose-dependently attenuating the protein expressions in taurine-treated cells (Fig. 3f, h). These data suggest that taurine suppresses the migratory condition by regulating the levels of VEGF in androgen-resistant human prostate cancer cells, PC-3.
The effect of taurine on PSA and migration-related genes in human prostate cancer cells, LNCaP (a–e) and PC-3 (f–h). Cells were treated with or without DHA and various concentrations of taurine for 48 h. The protein levels from whole-cell lysates were analyzed by Western blot. β-actin was used as a loading control. The blot represents the mean of three individual experiments performed in triplicate. *P < 0.05, statistical significance compared with DHT alone-treated cells
4 Discussion
The sulfur-containing -amino acid, taurine, is the most plentiful free amino acid in cardiac and skeletal muscle. Recently, several studies have investigated that taurine exhibits anti-proliferative and antineoplastic effects in prostate cancer cells (Chatzakos et al. 2012; Darnowski et al. 2004; Zhang et al. 2008). The regulation of cell growth is a homeostatic balance between stimulatory and inhibitory signals. The negative growth control by tumor suppressor genes, differentiation factors, and programmed cell death (apoptosis) is commonly targeted mechanism exploited for strategies in the treatment of malignancies and other diseases. Among them, apoptosis is a highly attractive and widely studied area to search for more effective agents for treatment of human cancers. A wide variety of in vivo and in vitro studies published in recent years suggested that many chemotherapeutic agents could induce apoptotic cell death in different cancer cells (McCloskey et al. 1996). For this reason, the anticancer activity of taurine was evaluated for apoptosis using MTT assay. As shown in Fig. 1, taurine stimulated apoptosis in a dose-dependent manner. From the results, we decided upon the concentrations of taurine for the next experiments.
Cellular adhesion and migration are important features of cancer progression and therefore a potential target for cancer interception (Elgass et al. 2014). In this study we have examined the in vitro effect of taurine on these processes. The migratory potential was assessed using gap closure assay. As shown in Fig. 2, taurine significantly suppressed the migratory movement of human prostate cancer cells, LNCaP at 48 h and PC-3 at 8 h, respectively.
Meanwhile, there is no scientific report for PSA and migration-related genes. Therefore, we also elucidated the effect of taurine on the expression of PSA and migration-related genes such as MMP-9, TIMP-1, TIMP-2, and VEGF. Prostate cancer can increase the amount of PSA released into the blood stream. Notably, PSA present in the extracellular fluid, surrounding prostate epithelial cells, has been reported to be enzymatically active, suggesting that its proteolytic activity plays a role in the physiopathology of prostate cancer (Tomao et al. 2014; Denmeade et al. 2001). MMPs are essential for extracellular matrix remodelling and may contribute to the development of endometriosis (Osteen et al. 2003). It is known that MMP-2 and MMP-9 play important roles in the ectopic adhesion, invasion, and implantation and neovascularisation of the endometrium (Chen et al. 2009). Firstly, we conducted gap closure assay, and found that taurine significantly suppressed the movement of androgen-dependent human prostate cancer cell (Fig. 2). Western blot for the estimation of protein expression of PSA, MMP-2, MMP-9, TIMP-1, TIMP-2, and VEGF was also performed. As shown in Fig. 3, we proved taurine attenuated PSA, MMP-9, and VEGF. However we didn’t obtain any evidence of the effect of taurine on MMP-2 protein level in LNCaP and PC-3 cells (data not shown).
There are several reports describing MMP-9 and its specific inhibitor, TIMPs, that are closely correlated with physiological and pathological processes by degradation and accumulation of the ECM (Roderfeld et al. 2007; Goldberg et al. 1989). With the exception of neutrophil granulocytes, MMP-9 is usually secreted together with variable amounts of its specific inhibitor, TIMP-1 and TIMP-2 (Van den Steen et al. 2002). Interestingly, TIMP-1 has been found not only in separated localization, but also in co-localization with pro-MMP-9 in neutrophil organelles, which resemble secretory vesicles (Price et al. 2000). Accordingly, we ascertained the protein level of TIMP-1 and TIMP-2. Figure 3a, d, e show taurine enhance the protein level of TIMP-1 and TIMP-2 in a dose-dependent fashion. Meanwhile, VEGF induces endothelial cell proliferation, promotes cell migration, and inhibits apoptosis (Neufeld et al. 1999). Accordingly, the VEGF expression was also assessed by Western blot. Figure 3e–g showed that taurine suppressed the expression of VEGF, as well as the expression of PSA which is a marker for prostate cancer.
These results of the present study suggest that taurine has a beneficial effect on the cell death and the expression of PSA, MMP-9, TIMP-1, and TIMP-2 in LNCaP, androgen-dependent human prostate cancer cells.
5 Conclusion
In the present study, taurine improved the apoptosis, the expression of PSA and modulated migration related genes. Although the mechanism for inducing apoptosis and PSA in tumor cells needs further investigation, taurine presents a potential chemotherapy agent.
Abbreviations
- MMPs:
-
Matrix metalloproteinases
- PSA:
-
Prostate-specific antigen
- TIMPs:
-
Tissue inhibitors of metalloproteinases
- VEGF:
-
Vascular endothelial growth factor
References
Baade PD, Youlden DR, Krnjacki LJ (2009) International epidemiology of prostate cancer: geographical distribution and secular trends. Mol Nutri Food Res 53:171–184. doi:10.1002/mnfr.200700511
Chatzakos V, Slatis K, Djureinovic T, Helleday T, Hunt MC (2012) N-acyl taurines are anti-proliferative in prostate cancer cells. Lipids 47:355–361. doi:10.1007/s11745-011-3639-9
Chen JS, Wang Q, Fu XH, Huang XH, Chen XL, Cao LQ, Chen LZ, Tan HX, Li W, Bi J, Zhang LJ (2009) Involvement of PI3 K/PTEN/AKT/mTOR pathway in invasion and metastasis in hepatocellular carcinoma: association with MMP-9. Hepatol Res 39:177–186. doi:10.1111/j.1872-034X.2008
Choi MJ, Kim JH, Chang KJ (2006) The effect of dietary taurine supplementation on plasma and liver lipid concentrations and free amino acid concentrations in rats fed a high-cholesterol diet. Adv Exp Med Biol 583:235–242. doi:10.1007/978-0-387-33504-9_25
Cohen P, Graves HC, Peehl DM, Kamarei M, Giudice LC, Rosenfeld RG (1992) Prostate-specific antigen (PSA) is an insulin-like growth factor binding protein-3 protease found in seminal plasma. J Clin Endocrinol Metab 75: 1046–1053. http://dx.doi.org/10.1210/jcem.75.4.1383255
Darnowski JW, Goulette FA, Cousens LP, Chatterjee D, Calabresi P (2004) Mechanistic and antineoplastic evaluation of taurolidine in the DU145 model of human prostate cancer. Cancer Chemother Pharmacol 54:249–258. doi:10.1007/s00280-004-0806-1
Denmeade SR, Sokoll LJ, Chan DW, Khan SR, Isaacs JT (2001) Concentration of enzymatically active prostate-specific antigen (PSA) in the extracellular fluid of primary human prostate cancers and human prostate cancer xenograft models. Prostate 48:1–6. doi:10.1002/pros.1075
Elgass S, Cooper A, Chopra M (2014) Lycopene treatment of prostate cancer cell lines inhibits adhesion and migration properties of the cells. Int J Med Sci 11(9):948–954. doi:10.7150/ijms.9137
Goldberg GI, Marmer BL, Grant GA, Eisen AZ, Wilhelm S, He CS (1989) Human 72-kilodalton type IV collagenase forms a complex with a tissue inhibitor of metalloproteases designated TIMP-2. Proc Natl Acad Sci USA 86:8207–8211. http://www.pnas.org/content/86/21/8207.full.pdf+html?sid=3b5e5d64-219a-4d50-8042-99f1d6236bd3
Green TR, Fellman JH, Eicher AL, Pratt KL (1991) Antioxidant role and subcellular location of hypotaurine and taurine in human neutrophils. Biochim Biophys Acta 1073:91–97. doi:10.1016/0304-4165(91)90187-L
Iwamura M, Hellman J, Cockett AT, Lilja H, Gershagen S (1996) Alteration of the hormonal bioactivity of parathyroid hormone-related protein (PTHrP) as a result of limited proteolysis by prostate-specific antigen. Urology 48:317–325. doi:10.1016/S0090-4295(96)00182-3
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics, 2009. CA Cancer J Clin 59:225–249. doi:10.3322/caac.20006
Kim SH, Johnson VJ, Sharma RP (2002) Mercury inhibits nitric oxide production but activates proinflammatory cytokine expression in murine macrophage: differential modulation of NF-kappaB and p38 MAPK signaling pathways. Nitric Oxide 7:67–74. doi:10.1016/S1089-8603(02)00008-3
Kirk K, Kirk J (1993) Volume-regulatory taurine release from a human heart cancer cell line. FEBS Lett 336:153–158. doi:10.1016/0014-5793(93)81630-I
Klein EA, Thompson IM (2012) Chemoprevention of prostate cancer: an updated view. World J Urol 30:189–194. doi:10.1007/s00345-011-0822-9
Luigi M, Nunzi E, Giovannozzi S, Lepri L, Lolli C, Giannantoni A (2014) Urodynamic evaluation after high-intensity focused ultrasound for patients with prostate cancer. Prostate Cancer ID: 462153. http://dx.doi.org/10.1155/2014/462153
McCloskey DE, Kaufmann SH, Prestigiacomo LJ, Davidson NE (1996) Paclitaxel induces programmed cell death in MDA-MB-468 human breast cancer cells. Clin Cancer Res 2:847–854. http://clincancerres.aacrjournals.org/content/2/5/847.full.pdf+html
Neufeld G, Cohen T, Gengrinovitch S, Poltorak Z (1999) Vascular endothelial growth factor (VEGF) and its receptors. FASEB J 13:9–22. doi:10.1096/fj.1530-6860
Olive MF (2002) Interactions between taurine and ethanol in the central nervous system. Amino Acids 23:345–357. doi:10.1007/s00726-002-0203-1
Osteen KG, Yeaman GR, Bruner-Tran KL (2003) Matrix metalloproteinases and endometriosis. Semin Reprod Med 21:155–164. doi:10.1055/s-2003-41322
Price B, Dennison C, Tschesche H, Elliott E (2000) Neutrophil tissue inhibitor of matrix metalloproteinases-1 occurs in novel vesicles that do not fuse with the phagosome. J Biol Chem 275:28308–28315. doi:10.1074/jbc.M002263200
Racioppi M, Palermo G, D’Addessi A, Pinto F, Sacco E, D’Agostino D, Vittori M, Bassi PF (2012) Hot topics in urological health economics. A mini review. Arch Ital Urol Androl 84:47–52. http://www.unboundmedicine.com/medline/citation/22908771/Hot_topics_in_urological_health_economics__A_mini_review_
Roderfeld M, Graf J, Giese B, Salguero-Palacios R, Tschuschner A, Müller-Newen G, Roeb E (2007) Latent MMP-9 is bound to TIMP-1 before secretion. Biol Chem 388:1227–1234. doi:10.1515/BC.2007.123
Shuman Moss LA, Jensen-Taubman S, Stetler-Stevenson WG (2012) Matrix metalloproteinases: changing roles in tumor progression and metastasis. Am J Pathol 181:1895–1899. doi:10.1016/j.ajpath
Siegel R, Naishadham D, Jemal A (2012) Cancer statistics. CA Cancer J Clin 62:10–29. doi:10.3322/caac.20138
Tiedemann F, Gmelin L (1827) Einige neue Bestandtheile der Galle des Ochsen. Ann Phys 85:326–337. doi:10.1002/andp.18270850214
Tomao L, Sbardella D, Gioia M, Di Masi A, Marini S, Ascenzi P, Coletta M (2014) Characterization of the Prostate-Specific Antigen (PSA) catalytic mechanism: a pre-steady-state and steady-state study. PLoS One 9:e102470. doi:10.1371/journal.pone.0102470
Van den Steen PE, Dubois B, Nelissen I, Rudd PM, Dwek RA, Opdenakker G (2002) Biochemistry and molecular biology of gelatinase B or matrix metalloproteinase-9 (MMP-9). Crit Rev Biochem Mol Biol 37:375–536. doi:10.1080/10409230290771546
Webber MM, Waghray A, Bello D (1995) Prostate-specific antigen, a serine protease, facilitates human prostate cancer cell invasion. Clin Cancer Res 1:1089–1094. http://clincancerres.aacrjournals.org/content/1/10/1089.full.pdf+html
Williams SA, Singh P, Isaacs JT, Denmeade SR (2007) Does PSA play a role as a promoting agent during the initiation and/or progression of prostate cancer? Prostate 67:312–329. doi:10.1002/pros.20531
Wingo PA, Cardinez CJ, Landis SH, Greenlee RT, Ries LA, Anderson RN, Thun MJ (2003) Long-term trends in cancer mortality in the United States, 1930–1998. Cancer 97:3133–3275. doi:10.1002/cncr.11380
Yanagita T, Han SY, Hu Y, Nagao K, Kitajima H, Murakami S (2008) Taurine reduces the secretion of apolipoprotein B100 and lipids in HepG2 cells. Lipids Health Dis 7:38–43. doi:10.1186/1476-511X-7-38
Zhang M, Bi LF, Fang JH, Su XL, Da GL, Kuwamori T, Kagamimori S (2004) Beneficial effects of taurine on serum lipids in overweight or obese non-diabetic subjects. Amino Acids 26:267–271. doi:10.1007/s00726-003-0059-z
Zhang X, Bi C, Fan Y, Cui Q, Chen D, Xiao Y, Dou QP (2008) Induction of tumor cell apoptosis by taurine Schiff base copper complex is associated with the inhibition of proteasomal activity. Int J Mol Med 22:677–682. doi:10.3892/ijmm_00000072
Acknowledgements
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (2013R1A1A3006958) and by “Cooperative Research Program for Agriculture Science & Technology Development (Project NO. PJ010181)” Rural Development Administration, Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this paper
Cite this paper
Tang, Y. et al. (2015). Effect of Taurine on Prostate-Specific Antigen Level and Migration in Human Prostate Cancer Cells. In: Marcinkiewicz, J., Schaffer, S. (eds) Taurine 9. Advances in Experimental Medicine and Biology, vol 803. Springer, Cham. https://doi.org/10.1007/978-3-319-15126-7_18
Download citation
DOI: https://doi.org/10.1007/978-3-319-15126-7_18
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-15125-0
Online ISBN: 978-3-319-15126-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)