Abstract
Head and neck squamous cell carcinomas (HNSCC) are the most frequent cancers arising from the squamous epithelia of the aerodigestive tract or skin of the head and neck. Oxidative stress and free radical production from metabolism by host cells and resident microbiota is a continuous process for which cells have protective antioxidant defenses, which usually mitigate damage to prevent or delay development of cancer. In the head and neck, these defenses may be overwhelmed by exposure to carcinogens that cause free radical-mediated or direct DNA damage that results in cancer initiating mutations. Alterations affecting key tumor suppressor genes such as TP53, related oncogene ΔNp63, and PIK3CA, the PI3kinase catalytic subunit alpha, are prevalent. These mutations in turn may activate transcription factor Nuclear Factor-κB to promote host inflammatory responses that further enhance free radical production and cumulative DNA damage, resulting in cancer progression. Mutations in genes such as KEAP1 and NRF2 critical to sensing and inducing antioxidant and survival responses, or the Fanconi/BRCA pathway important in DNA repair enhance susceptibility to HNSCC. Anti-inflammatory drug celecoxib in combination with Epidermal Growth Factor Receptor inhibitor erlotinib has demonstrated activity in premalignant lesions. In genetically engineered experimental animal models with genetic defects in Fanconi D2/TP53 or TGFβ receptor 1/Pten genes that activate PI3K signaling, synthetic antioxidants or PI3K inhibitors may delay onset of cancer and have clinical translational potential.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Head and neck squamous cell carcinoma
- Fanconi anemia
- Oxidative stress
- KEAP1
- NRF2
- NF-kappaB
- Tempol
- Antioxidant
1 Overview
Oxidative stress and free radical production from metabolism by host cells and resident microbiota is a continuous process for which cells have protective antioxidant defenses, which usually mitigate damage to prevent or delay development of cancer (Gorrini et al. 2013). These defenses include sensors of oxidative stress, such as KEAP1, and transcription factor NRF2, that induce detoxification enzymes. In the head and neck, these defenses may be overwhelmed by long-term exposure to tobacco or ultraviolet light carcinogens that cause head and neck squamous cell carcinomas (HNSCC), each arising respectively from the squamous epithelia of the aerodigestive tract or skin. These carcinogens induce free radical-mediated or direct DNA damage that result in cancer initiating mutations (Choudhari et al. 2014). Alterations affecting key tumor suppressor genes such as TP53, related oncogene ΔNp63, and PIK3CA, the PI3kinase catalytic subunit alpha, are prevalent (Walter et al. 2013). These DNA damaging signals and genomic alterations in turn may activate transcription factor Nuclear Factor-κB to promote cell survival and host inflammatory responses (Yang et al. 2011; Vander Broek et al. 2014; Du et al. 2014; Cooks et al. 2013), which further enhance free radical production and cumulative DNA damage, resulting in cancer progression. Mutations in genes such as KEAP1 and NRF2 critical to sensing and inducing antioxidant and survival responses, or the Fanconi/BRCA pathway important in DNA repair, enhance susceptibility to HNSCC (Walter et al. 2013, Van Waes 2005). Anti-inflammatory drug celecoxib in combination with Epidermal Growth Factor Receptor inhibitor erlotinib has demonstrated activity in premalignant lesions. In genetically engineered experimental animal models with genetic defects in Fanconi D2/TP53 or TGFβ receptor 1/Pten genes that activate PI3K signaling, synthetic antioxidants, or PI3K inhibitors may delay onset of cancer, and have clinical translational potential (Zhang et al. 2008; Herzog et al. 2013).
2 Tobacco-Related Free Radical Damage
Development of HNSCC is most frequently associated with exposure to tobacco products, and further enhanced when combined with alcohol. Tobacco smoke and smokeless tobacco contain nitrosamine and polyaromatic hydrocarbon carcinogens whose electrophilic metabolites induce reactive oxygen species (ROS) and reactive nitrogen species (RNS) that modify or disrupt DNA, as well as form direct DNA adducts whose faulty repair cause mutations (Fig. 22.1) (Choudhari et al. 2014; Hecht 2012). One of the major consequences of tobacco and smoke metabolites or induced ROS is increased formation of 8-hydroxy-deoxyguanosine (8-OHdG), which is potentially mutagenic (Hecht 2012). In parallel, chronic nicotine and carcinogen exposure can induce PI3K-Akt and PKA signal activation of transcription factor NF-κB (Fig. 22.1), which promotes cell survival and proliferation, and additional ROS production by infiltrating inflammatory cells, exposing progeny to cumulative mutations (Hecht 2012; West et al. 2004; Tsurutani et al. 2005; Dennis et al. 2005). As a result, tobacco metabolite- and ROS-related mutations across the genome are frequent, and cumulatively affect key tumor suppressor genes and oncogenes, resulting in autonomous loss of growth control, genomic instability, ROS homeostasis, and malignant transformation.
Tobacco carcinogen and inflammatory response-induced reactive oxygen species (ROS), bacterial, and viral products mediate inducible and genomic alterations in the PI3K-NF-κB, TP53/63, and KEAP1/NRF2 pathways in HNSCC. (a) Tobacco carcinogen and inflammatory cell-induced ROS cause DNA damage and degrade sensor and ubiquitin ligase KEAP1, inducing activation of the classical Inhibitor-κB kinase (IKK)-NF-κB pathway, which elicits transcription of cancer promoting genes. Carcinogen and ROS-induced genomic mutations in tumor suppressor TP53 and amplifications causing overexpression of oncogenic family member ΔNp63 and PI3-Kinase (PI3K) result in loss of growth control and enhance NF-κB signaling. Classical NF-κB activation may be enhanced by bacterial and viral products, inflammatory and growth factors. (b) Alternative NF-κB pathway activation (and TP53 inactivation) can be directly mediated by HPV E6 and EBV LMP1 oncogenes. ROS-induced KEAP1 and NRF2-mediated transcription of endogenous antioxidants may also be compromised by genomic alterations
3 Activation of NF-κB and Inflammation-Related Free Radical Damage
The NF-κB/REL family transcription factors are aberrantly activated in HNSCC and other cancers, and critically promote cell survival, inflammation, and angiogenesis (Fig. 22.1) (Van Waes 2007). As aforementioned, nicotine and tobacco metabolites can promote PI3K-Akt and PKA signaling, and my laboratory showed that PI3K and PKA contribute to aberrant transactivation of NF-κB observed in HNSCC (Fig. 22.1) (Bancroft et al. 2002; Arun et al. 2009). Additionally, many injury and pathogen inducible signal pathways converge to activate NF-κB (Van Waes 2007). Carcinogen and ROS-induced DNA damage can promote sumoylation and activation of Inhibitor-κB kinases (IKKs), which mediate NF-κB nuclear translocation and activation. Further, ROS can promote degradation of ubiquitin ligase KEAP1, enhancing IKK-mediated signaling (Fig. 22.1). Bacterial, human papilloma virus (HPV) and Epstein Barr Virus (EBV) pathogens have also been implicated in development of HNSCC, and can induce activation of Toll-Like Receptor, IKKs, and alternative pathways that promote NF-κB activation (Van Waes 2007; James et al. 2006; Szczepanski et al. 2004) (Fig. 22.1).
The consequences of such chronic injury-induced signal activation of NF-κB are pathologic. NF-κB promotes expression of Cyclin D1 and BCL-XL genes that promote cell proliferation and survival of HNSCC cells (Van Waes 2007; Lee et al. 2008; Duan et al. 2007). NF-κB also promotes expression of angiogenesis factors IL-6, IL-8, GRO1, and VEGF (Duffey et al. 1999; Bancroft et al. 2001; Loukinova et al. 2001) that recruit and activate monocytic and myeloid inflammatory cells (Loukinova et al. 2000; Young et al. 2001). Activated myeloid-derived cells produce ROS, which likely further exacerbates cell and DNA damage, related signaling and mutations, and compromises immune defenses to malignant cells (Kotsakis et al. 2012; Vasquez-Dunddel et al. 2013).
4 Role TP53 and p63/PI3KCA Genetic Alterations in Genomic Instability and Inflammation in HNSCC
Among genetic alterations, mutation or deletion of TP53 is the most frequent, occurring in over 70 % of 279 HNSCC tumors studied as part of The Cancer Genome Atlas (TCGA) (Fig. 22.2) (TCGA Network 2015). TP53 is a ROS and DNA damage inducible transcription factor that mediates growth arrest and DNA damage repair, or death of cells with irreversibly damaged DNA (Fig. 22.1). Hence, TP53 serves as the “Guardian of the genome,” and its loss leads to uncontrolled proliferation, genomic instability, and progressive genomic alterations (Lane 1992; Stiewe 2007). Among the gains, amplification of the locus containing the gene encoding a TP53 family oncogene ΔNp63, and amplification or activating mutations of PIK3CA, the PI3kinase catalytic subunit alpha, are prevalent (Fig. 22.2) (Walter et al. 2013). In ~20 % cases, ΔNp63 and PIK3CA are included in the same amplicon, while overall, PIK3CA is amplified or mutated in 36 % of cases. Interestingly, these genomic alterations in TP53, ΔNp63, and PIK3CA may contribute to inactivation of TP53-dependent responses, and constitutive activation of transcription factor Nuclear Factor-κB, cell survival, and host inflammatory responses (Fig. 22.1) (Yang et al. 2011; Vander Broek et al. 2014; Du et al. 2014; Cooks et al. 2013), that further enhance free radical production and cumulative DNA damage, resulting in cancer progression.
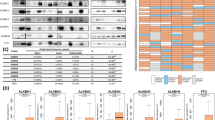
Genomic alterations in TP53, TP63, PIK3CA, KEAP1, and NFE2L2 genes in HNSCC. Publically available data for the genes indicated were queried from 279 head and neck squamous cell carcinomas from The Cancer Genome Atlas (TCGA) using cbioportal (http://www.cbioportal.org/public-portal/). TP53 is mutated in over 70 % of tumors. The adjacent loci containing TP63 and PI3K catalytic subunit PIK3CA are co-amplified in ~20 % of HNSCC, and activating mutations in PIK3CA are observed in additional tumors. Mutations in the oxidative stress pathway including KEAP1 mutations (~5 %) and amplification or mutation of NRF2 (~12 %) are found. Key, red bars, amplifications; blue bars, homozygous deletion; green bars, mutations
5 Role of KEAP1/NRF2 Genetic Alterations in HNSCC Susceptibility
KEAP1 is an important sensor of oxidative stress, and ubiquitin ligase, which in the absence of stress binds and promotes proteasomal degradation of IKKβ proteins, inhibiting NF-κB activation and cell survival, and of transcription factor NRF2, inhibiting antioxidant genes (Fig. 22.1) (Tian et al. 2012). In the presence of ROS, KEAP1 cysteine residues undergo conformational changes that promote IKK-induced NF-κB activation and cell survival, while releasing NRF2 for nuclear translocation and activation of antioxidant genes. The antioxidant genes include glutathione-S-transferases (GSTs), NADP(H) quinone oxidoreductase (NQO1), catalase, and superoxide dismutases (SODs), important in neutralizing ROS. In HNSCC, mutations of KEAP1 are observed in ~5 % and in NRF2 are observed in ~12 % of HNSCC (Fig. 22.2), suggesting genomic alterations affect KEAP1 regulated NF-κB prosurvival signaling and NRF2 antioxidant responses in a subset of HNSCC. Most HNSCC tumors with alterations in KEAP1 and NRF2 also appear to have undergone mutations in TP53 (Fig. 22.2). Studies in transgenic mouse models suggest NRF2 may inhibit initiation of tumorigenesis, but enhance progression of established tumors (Satoh et al. 2013). This observation involving NRF2 and endogenous antioxidants mirrors the cautionary observation that antioxidant β-carotene can inhibit initiation in preclinical models of lung cancer, while enhancing progression and mortality in smokers (ATBC 2003), who could have had premalignant lesions with TP53 mutations.
6 Role of Alterations in Fanconi/BRCA DNA Damage Response in HNSCC Susceptibility
The Fanconi Anemia (FANC) and Breast/ovarian cancer (BRCA) genes and proteins are now known to comprise a pathway critical in mediating repair of ROS-mediated DNA damage by nonhomologous recombination (Kee and D’Andrea 2012). Overall, the pathway includes 15 FANC genes, BRCA1 and BRCA2. Mutations in FANCA, FANCB, FANCC, FANCE, FANCF, FANCG, FANCL, and FANCM account for approximately 90 % of patients. These result in loss of FANCD2 and FANCI monoubiquitylation, the key regulatory event in the FA pathway. Besides loss of DNA repair, FANCD2 activates transcription of a TP53 homologue TAp63 that suppresses tumorigenesis (Park et al. 2013). Patients with FANC mutations are prone to bone marrow failure with anemia and leukemia in childhood, or development of HNSCC and genitourinary tract SCCs in young adulthood. While BRCA gene mutations predispose to breast and ovarian cancer, they have also been detected in patients with HNSCC. Overall, genomic alterations in FANC and BRCA genes are detected in 86/279 (~31 %) of HNSCC tumors in TCGA (Fig. 22.3). The HNSCC that arise in patients with FA patients in their 20–40 s frequently occur in the absence of tobacco use, and occur in the oral cavity in the tongue and mucosa adjacent to areas of exposure to dental trauma and microbiota (Van Waes 2005). The FA pathway has recently been shown to limit human papilloma virus replication and transformation by the HPV E7 gene (Hoskins et al. 2012; Park et al. 2010). However, the extent of the role of HPV in FA HNSCC remains unclear, as others report that the mutational spectrum in HNSCC in FA includes genes such as TP53, similar to that in tobacco-related HNSCC (van Zeeburg et al. 2008). Increased oxidative stress and potential for mutations and malignant transformation has been detected in FA cells (Du et al. 2008), and is enhanced by inflammatory signaling and induction of ROS by TNFα (Li et al. 2007).
Genomic alterations in Fanconi and BRCA genes in HNSCC. Publically available data for the genes indicated were queried from 279 head and neck squamous cell carcinomas from The Cancer Genome Atlas (TCGA) using cbioportal (http://www.cbioportal.org/public-portal/). Fanconi genes include named FANC, and other genes listed. Most genes exhibit deletions or inactivating mutations, but FANCG is more often amplified, which could enhance or repair of ROS-mediated genomic instability, respectively. Key, red bars, amplifications; blue bars, homozygous deletion; green bars, mutations
7 Potential of Anti-inflammatory Agents, Antioxidants, and PI3K-mTOR Inhibitors to Delay Malignant Progression and for Clinical Translation
Based on the potential role of HNSCC-associated inflammation and ROS in promoting HNSCC, anti-inflammatory drugs have been of interest. Many anti-inflammatory drugs inhibit NF-κB or NF-κB targets such as Cyclooxygenases, responsible for inflammatory prostaglandins (Van Waes 2007). Proteasome inhibitors preventing IκB degradation and NF-κB activation and inflammation yielded incomplete and transient responses in preclinical and clinical trials, which were found to be due to compensatory activation of other prosurvival signaling pathways (Allen et al. 2008; Chen et al. 2008). Cyclooxygenase inhibitor ketorolac inhibited inflammatory cells in response to HNSCC in preclinical studies, but showed a similar 30 % response rate as placebo in reducing leukoplakia (Hong et al. 2000; Mulshine et al. 2004). However, Cyclooxygenase 2 plus Epidermal Growth Factor Receptor inhibitors were found to synergistically inhibit head and neck squamous cell carcinoma tumorigenesis in preclinical and clinical studies (Saba et al. 2014). In a phase I study with a combination of COX2 inhibitor celecoxib and EGFR inhibitor erlotinib in patients with advanced premalignant lesions, the overall histologic response rate was 63 % (complete response 43 %, partial response 14 %, stable disease 29 %, disease progression 14 %). With median follow-up of 36 months, mean time to progression to higher-grade dysplasia or carcinoma was 25.4 months. Encouraging responses to the celecoxib and erlotinib combination correlated with EGFR pathway inhibition, where downregulation of EGFR and p-ERK in follow-up biopsies correlated with response to treatment (Vander Broek et al. 2013).
With evidence for a relatively high prevalence of PI3K-mTOR pathway alterations HNSCC, and their importance in activation of NF-κB and inflammatory responses (Vander Broek et al. 2013), PI3K and mTOR inhibitors have been the subject of preclinical and clinical investigation. In genetically engineered experimental animal models with genetic defects in TGFβ receptor 1/Pten genes and activated PI3K signaling, a synthetic PI3K-mTOR inhibitor delayed onset of HNSCC, demonstrating clinical translational potential (Herzog et al. 2013). In a clinical trial of mTOR inhibitor rapamycin underway at NIH, clinical responses have been observed in patients with stage II–IV oral and oropharyngeal cancers [C. Van Waes, unpublished observations].
Based on the hypothesis that FA cells are more prone to oxidative damage, we examined and demonstrated an increase in ROS DNA marker 8-OHdG in human FA fibroblast lines relative to control cell lines (Zhang et al. 2008). A synthetic nitrosamine antioxidant tempol reduced 8-OHdG similar to normal levels in these FA cells, and cells from Fancd2 knockout mice. Fancd2−/− Trp53+/− mice on a tempol diet showed a significantly longer mean tumor-free survival (mean = 390 days) than the mice on placebo diet (mean = 308 days) (P < 0.01). After early deaths due to leukemias, statistical analysis revealed that tempol treatment significantly increased the mean epithelial tumor-free survival time by 38 % in Fancd2−/− Trp53+/− mice (P < 0.0001). These data suggest that tempol may have a role in reducing oxidative DNA damage and malignant transformation in FA (Zhang et al. 2008), although naturally occurring antioxidant resveratrol or n-acetylcysteine did not have significant chemopreventive effects in the same model (Zhang et al. 2014).
In conclusion, anti-inflammatory, antioxidants, and PI3K-mTOR inhibitors targeting specific genetic alterations have preclinical or clinical activity and potential for further clinical investigation in prevention of HNSCC.
References
Allen C, Saigal K, Nottingham L, Arun P, Chen Z, Van Waes C (2008) Bortezomib-induced apoptosis with limited clinical response is accompanied by inhibition of canonical but not alternative nuclear factor-{kappa}B subunits in head and neck cancer. Clin Cancer Res 14:4175–4185. doi:10.1158/1078-0432.CCR-07-4470
Arun P, Brown MS, Ehsanian R, Chen Z, Van Waes C (2009) Nuclear NF-kappaB p65 phosphorylation at serine 276 by protein kinase A contributes to the malignant phenotype of head and neck cancer. Clin Cancer Res 15:5974–5984. doi:10.1158/1078-0432.CCR-09-1352
Bancroft CC, Chen Z, Dong G, Sunwoo JB, Yeh N, Park C, Van Waes C (2001) Coexpression of proangiogenic factors IL-8 and VEGF by human head and neck squamous cell carcinoma involves coactivation by MEK-MAPK and IKK-NF-kappaB signal pathways. Clin Cancer Res 7:435–442
Bancroft CC, Chen Z, Yeh J, Sunwoo JB, Yeh NT, Jackson S, Jackson C, Van Waes C (2002) Effects of pharmacologic antagonists of epidermal growth factor receptor, PI3K and MEK signal kinases on NF-kappaB and AP-1 activation and IL-8 and VEGF expression in human head and neck squamous cell carcinoma lines. Int J Cancer 99:538–548
Chen Z, Ricker JL, Malhotra PS, Nottingham L, Bagain L, Lee TL, Yeh NT, Van Waes C (2008) Differential bortezomib sensitivity in head and neck cancer lines corresponds to proteasome, nuclear factor-kappaB and activator protein-1 related mechanisms. Mol Cancer Ther 7:1949–1960. doi:10.1158/1535-7163.MCT-07-2046
Choudhari SK, Chaudhary M, Gadbail AR, Sharma A, Tekade S (2014) Oxidative and antioxidative mechanisms in oral cancer and precancer: a review. Oral Oncol 50:10–18. doi:10.1016/j.oraloncology.2013.09.011
Cooks T, Pateras IS, Tarcic O, Solomon H, Schetter AJ, Wilder S, Lozano G, Pikarsky E, Forshew T, Rosenfeld N, Harpaz N, Itzkowitz S, Harris CC, Rotter V, Gorgoulis VG, Oren M (2013) Mutant p53 prolongs NF-κB activation and promotes chronic inflammation and inflammation-associated colorectal cancer. Cancer Cell 23:634–646. doi:10.1016/j.ccr.2013.03.022
Dennis PA, Van Waes C, Gutkind JS, Kellar KJ, Vinson C, Mukhin AG, Spitz MR, Bailey-Wilson JE, Yeh GC, Anderson LM, Wiest JS (2005) The biology of tobacco and nicotine: bench to bedside. Cancer Epidemiol Biomarkers Prev 14:764–767
Du W, Adam Z, Rani R, Zhang X, Pang Q (2008) Oxidative stress in Fanconi anemia hematopoiesis and disease progression. Antioxid Redox Signal 10:1909–1921
Du J, Romano RA, Si H, Mattox A, Bian Y, Yang X, Sinha S, Van Waes C, Chen Z (2014) Epidermal overexpression of transgenic ΔNp63 promotes type 2 immune and myeloid inflammatory responses and hyperplasia via NF-κB activation. J Pathol 232:356–368. doi:10.1002/path.4302
Duan J, Friedman J, Nottingham L, Chen Z, Ara G, Van Waes C (2007) Nuclear factor-kappaB p65 small interfering RNA or proteasome inhibitor bortezomib sensitizes head and neck squamous cell carcinomas to classic histone deacetylase inhibitors and novel histone deacetylase inhibitor PXD101. Mol Cancer Ther 6:37–50
Duffey DC, Chen Z, Dong G, Ondrey FG, Wolf JS, Brown K, Siebenlist U, Van Waes C (1999) Expression of a dominant-negative mutant inhibitor-kappaBalpha of nuclear factor-kappaB in human head and neck squamous cell carcinoma inhibits survival, proinflammatory cytokine expression, and tumor growth in vivo. Cancer Res 59:3468–3474
Gorrini C, Harris IS, Mak TW (2013) Modulation of oxidative stress as an anticancer strategy. Nat Rev Drug Discov 12:931–947. doi:10.1038/nrd4002
Hecht SS (2012) Lung carcinogenesis by tobacco smoke. Int J Cancer 131:2724–2732. doi:10.1002/ijc.27816
Herzog A, Bian Y, Vander Broek R, Hall B, Coupar J, Cheng H, Sowers AL, Cook JD, Mitchell JB, Chen Z, Kulkarni AB, Van Waes C (2013) PI3K/mTOR inhibitor PF-04691502 antitumor activity is enhanced with induction of wild-type TP53 in human xenograft and murine knockout models of head and neck cancer. Clin Cancer Res 19:3808–3819. doi:10.1158/1078-0432.CCR-12-2716
Hong SH, Ondrey FG, Avis IM, Chen Z, Loukinova E, Cavanaugh PF Jr, Van Waes C, Mulshine JL (2000) Cyclooxygenase regulates human oropharyngeal carcinomas via the proinflammatory cytokine IL-6: a general role for inflammation? FASEB J 14:1499–1507
Hoskins EE, Morreale RJ, Werner SP, Higginbotham JM, Laimins LA, Lambert PF, Brown DR, Gillison ML, Nuovo GJ, Witte DP, Kim MO, Davies SM, Mehta PA, Butsch Kovacic M, Wikenheiser-Brokamp KA, Wells SI (2012) The Fanconi anemia pathway limits human papillomavirus replication. J Virol 86:8131–8138. doi:10.1128/JVI.00408-12
James MA, Lee JH, Klingelhutz AJ (2006) Human papillomavirus type 16 E6 activates NF-kappaB, induces cIAP-2 expression, and protects against apoptosis in a PDZ binding motif-dependent manner. J Virol 80:5301–5307
Kee Y, D’Andrea AD (2012) Molecular pathogenesis and clinical management of Fanconi anemia. J Clin Invest 122:3799–3806. doi:10.1172/JCI58321
Kotsakis A, Harasymczuk M, Schilling B, Georgoulias V, Argiris A, Whiteside TL (2012) Myeloid-derived suppressor cell measurements in fresh and cryopreserved blood samples. J Immunol Methods 381:14–22. doi:10.1016/j.jim.2012.04.004
Lane DP (1992) p53, Guardian of the genome. Nature 358:15–16
Lee TL, Yeh J, Friedman J, Yan B, Yang X, Yeh NT, Van Waes C, Chen Z (2008) A signal network involving coactivated NF-kappaB and STAT3 and altered p53 modulates BAX/BCL-XL expression and promotes cell survival of head and neck squamous cell carcinomas. Int J Cancer 122:1987–1998. doi:10.1002/ijc.23324
Li J, Sejas DP, Zhang X, Qiu Y, Nattamai KJ, Rani R, Rathbun KR, Geiger H, Williams DA, Bagby GC, Pang Q (2007) TNF-alpha induces leukemic clonal evolution ex vivo in Fanconi anemia group C murine stem cells. J Clin Invest 117:3283–3295
Loukinova E, Dong G, Enamorado-Ayalya I, Thomas GR, Chen Z, Schreiber H, Van Waes C (2000) Growth regulated oncogene-alpha expression by murine squamous cell carcinoma promotes tumor growth, metastasis, leukocyte infiltration and angiogenesis by a host CXC receptor-2 dependent mechanism. Oncogene 19:3477–3486
Loukinova E, Chen Z, Van Waes C, Dong G (2001) Expression of proangiogenic chemokine Gro 1 in low and high metastatic variants of Pam murine squamous cell carcinoma is differentially regulated by IL-1alpha, EGF and TGF-beta1 through NF-kappaB dependent and independent mechanisms. Int J Cancer 94:637–644
Mulshine JL, Atkinson JC, Greer RO, Papadimitrakopoulou VA, Van Waes C, Rudy S, Martin JW, Steinberg SM, Liewehr DJ, Avis I, Linnoila RI, Hewitt S, Lippman SM, Frye R, Cavanaugh PF Jr (2004) Randomized, double-blind, placebo-controlled phase IIb trial of the cyclooxygenase inhibitor ketorolac as an oral rinse in oropharyngeal leukoplakia. Clin Cancer Res 10:1565–1573
Park JW, Pitot HC, Strati K, Spardy N, Duensing S, Grompe M, Lambert PF (2010) Deficiencies in the Fanconi anemia DNA damage response pathway increase sensitivity to HPV-associated head and neck cancer. Cancer Res 70:9959–9968. doi:10.1158/0008-5472.CAN-10-1291
Park E, Kim H, Kim JM, Primack B, Vidal-Cardenas S, Xu Y, Price BD, Mills AA, D'Andrea AD (2013) FANCD2 activates transcription of TAp63 and suppresses tumorigenesis. Mol Cell 50:908–918. doi:10.1016/j.molcel.2013.05.017
Saba N, Hurwitz SJ, Kono S, Yang CS, Zhao Y, Chen Z, Sica GL, Muller S, Moreno-Williams R, Lewis M, Grist W, Chen AY, Moore CE, Owonikoko TK, Ramalingam SS, Beitler JJ, Nannapaneni S, Shin HJ, Grandis JR, Khuri FR, Chen ZG, Shin DM (2014) Chemoprevention of head and neck cancer with celecoxib and erlotinib: results of a phase 1b and pharmacokinetic study. Cancer Prev Res (Phila) 7:283–291
Satoh H, Moriguchi T, Takai J, Ebina M, Yamamoto M (2013) Nrf2 prevents initiation but accelerates progression through the Kras signaling pathway during lung carcinogenesis. Cancer Res 73:4158–4168. doi:10.1158/0008-5472.CAN-12-4499
Stiewe T (2007) The p53 family in differentiation and tumorigenesis. Nat Rev Cancer 7:165–167. doi:10.1038/nrc2072
Szczepanski MJ, Czystowska M, Szajnik M, Harasymczuk M, Boyiadzis M, Kruk-Zagajewska A, Szyfter W, Zeromski J, Whiteside TL (2004) Triggering of Toll-like receptor 4 expressed on human head and neck squamous cell carcinoma promotes tumor development and protects the tumor from immune attack. Cancer Res 69:3105–3113. doi:10.1158/0008-5472.CAN-08-3838
The ATBC Study Group (2003) Incidence of cancer and mortality following α-tocopherol and β-carotene supplementation: a postintervention follow-up. JAMA 290:476–485
The Cancer Genome Atlas Network (2015) Comprehensive genomic characterization of head and neck squamous cell carcinomas. Nature 517:576–582
Tian H, Zhang B, Di J, Jiang G, Chen F, Li H, Li L, Pei D, Zheng J (2012) Keap1: one stone kills three birds Nrf2, IKKβ and Bcl-2/Bcl-xL. Cancer Lett 325:26–34. doi:10.1016/j.canlet.2012.06.007
Tsurutani J, Castillo SS, Brognard J, Granville CA, Zhang C, Gills JJ, Sayyah J, Dennis PA (2005) Tobacco components stimulate Akt-dependent proliferation and NFkappaB-dependent survival in lung cancer cells. Carcinogenesis 26:1182–1195
Vander Broek R, Mohan S, Eytan DF, Chen Z, Van Waes C (2013) The PI3K/Akt/mTOR axis in head and neck cancer: functions, aberrations, crosstalk, and therapies. Oral Dis. doi:10.1111/odi.12206, Epub ahead of print
Van Waes C (2005) Head and neck squamous cell carcinoma in patients with Fanconi anemia. Arch Otolaryngol Head Neck Surg 131:640–641
Van Waes C (2007) Nuclear factor-kappaB in development, prevention, and therapy of cancer. Clin Cancer Res 13:1076–1082
van Zeeburg HJ, Snijders PJ, Wu T, Gluckman E, Soulier J, Surralles J, Castella M, van der Wal JE, Wennerberg J, Califano J, Velleuer E, Dietrich R, Ebell W, Bloemena E, Joenje H, Leemans CR, Brakenhoff RH (2008) Clinical and molecular characteristics of squamous cell carcinomas from Fanconi anemia patients. J Natl Cancer Inst 100:1649–1653. doi:10.1093/jnci/djn366
Vander Broek R, Snow GE, Chen Z, Van Waes C (2014) Chemoprevention of head and neck squamous cell carcinoma through inhibition of NF-κB signaling. Oral Oncol 50:930–941. doi:10.1016/j.oraloncology.2013.10.005, pii: S1368-8375(13)00714-8
Vasquez-Dunddel D, Pan F, Zeng Q, Gorbounov M, Albesiano E, Fu J, Blosser RL, Tam AJ, Bruno T, Zhang H, Pardoll D, Kim Y (2013) STAT3 regulates arginase-I in myeloid-derived suppressor cells from cancer patients. J Clin Invest 123:1580–1589
Walter V, Yin X, Wilkerson MD, Cabanski CR, Zhao N, Du Y, Ang MK, Hayward MC, Salazar AH, Hoadley KA, Fritchie K, Sailey CJ, Weissler MC, Shockley WW, Zanation AM, Hackman T, Thorne LB, Funkhouser WD, Muldrew KL, Olshan AF, Randell SH, Wright FA, Shores CG, Hayes DN (2013) Molecular subtypes in head and neck cancer exhibit distinct patterns of chromosomal gain and loss of canonical cancer genes. PLoS One 8:e56823. doi:10.1371/journal.pone.0056823
West KA, Linnoila IR, Belinsky SA, Harris CC, Dennis PA (2004) Tobacco carcinogen-induced cellular transformation increases activation of the phosphatidylinositol 3′-kinase/Akt pathway in vitro and in vivo. Cancer Res 64:446–451
Yang X, Lu H, Yan B, Romano RA, Bian Y, Friedman J, Duggal P, Allen C, Chuang R, Ehsanian R, Si H, Sinha S, Van Waes C, Chen Z (2011) ΔNp63 versatilely regulates a Broad NF-κB gene program and promotes squamous epithelial proliferation, migration, and inflammation. Cancer Res 71:3688–3700. doi:10.1158/0008-5472.CAN-10-3445
Young MR, Petruzzelli GJ, Kolesiak K, Achille N, Lathers DM, Gabrilovich DI (2001) Human squamous cell carcinomas of the head and neck chemoattract immune suppressive CD34(+) progenitor cells. Hum Immunol 62:332–341
Zhang QS, Eaton L, Snyder ER, Houghtaling S, Mitchell JB, Finegold M, Van Waes C, Grompe M (2008) Tempol protects against oxidative damage and delays epithelial tumor onset in Fanconi anemia mice. Cancer Res 68:1601–1608. doi:10.1158/0008-5472.CAN-07-5186
Zhang QS, Marquez-Loza L, Sheehan AM, Watanabe-Smith K, Eaton L, Benedetti E, Major A, Schubert K, Deater M, Joseph E, Grompe M (2014) Evaluation of resveratrol and N-acetylcysteine for cancer chemoprevention in a Fanconi anemia murine model. Pediatr Blood Cancer 61(4):740–742. doi:10.1002/pbc.24780
Acknowledgement
Supported by NIDCD intramural research projects ZIA-DC-000016, -73, and -74.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Van Waes, C. (2015). Role of Free Radicals in Head and Neck Cancer. In: Miller, J., Le Prell, C., Rybak, L. (eds) Free Radicals in ENT Pathology. Oxidative Stress in Applied Basic Research and Clinical Practice. Humana Press, Cham. https://doi.org/10.1007/978-3-319-13473-4_22
Download citation
DOI: https://doi.org/10.1007/978-3-319-13473-4_22
Publisher Name: Humana Press, Cham
Print ISBN: 978-3-319-13472-7
Online ISBN: 978-3-319-13473-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)