Abstract
We first summarize the course from the initial description of a patient with thrombotic thrombocytopenic purpura (TTP) and the creation of the disease’s name to the diagnostic criteria proposed in 1966. A disease variant, obviously a constitutional form of a TTP-like disease responding to plasma infusions, is presented next. The many pathophysiological hypotheses put forward over the years are outlined with a focus on the detection of von Willebrand factor–cleaving protease, later identified as the metalloprotease ADAMTS13, and its severe deficiency as an important pathogenetic factor for TTP. A more common autoantibody-mediated acquired ADAMTS13 deficiency leading to acquired TTP should be distinguished from the rare hereditary form of the disease which is caused by homozygous or double heterozygous ADAMTS13 mutations. Then, the empirically introduced plasma therapy is reviewed, and the rationale for plasma exchange with fresh frozen plasma replacement in acquired TTP and plasma infusion in hereditary TTP is summarized. Finally, the differential diagnosis between the closely similar diseases TTP and (atypical) hemolytic uremic syndrome is discussed, and the sensitivity and specificity of a severe deficiency of ADAMTS13 activity for diagnosing TTP is evaluated. We conclude that some rare patients with “true” TTP may not be severely deficient in ADAMTS13 activity as measured with currently available methods. However, a severe deficiency of ADAMTS13 is a specific feature for a thrombotic microangiopathy that most clinicians diagnose as TTP.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Hemolytic Uremic Syndrome
- Fresh Freeze Plasma
- Thrombotic Thrombocytopenic Purpura
- ADAMTS13 Activity
- ADAMTS13 Deficiency
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1.1 Thrombotic Thrombocytopenic Purpura: The Initial Case Report, the Name of the Disease, and the Diagnostic Pentad of Clinical and Laboratory Findings
In 1924, Dr. Eli Moschcowitz reported on a 16-year-old previously healthy girl who died after 1 week of hospitalization for an acute illness with high fever, pallor, pain in the arms, a few petechiae on her skin, evolving paralysis of the left arm and leg, and preterminal coma [1]. The autopsy showed multiple “hyaline” thrombi in many arterioles and capillaries of the heart muscle, of the congested spleen, and of the kidneys [1]. At that time, the “hyaline” microvascular thrombi were thought to be caused by red blood cell agglutination, probably brought about by a powerful toxin with hemolytic and agglutinating properties. In an additional report on the same case [2], Moschcowitz mentioned that Dr. Max Lederer of Brooklyn had seen four similar patients and that all of them had recovered after a single blood transfusion.
Singer et al. [3], in 1947, described an 11-year-old white girl hospitalized for weakness, fever, and hemorrhagic tendency following an upper respiratory infection 2 weeks before. Her course rapidly deteriorated; she had high fever, became incoherent, developed transient dizziness and paresthesias, fell into coma, and died. Laboratory findings had shown severe anemia with a high reticulocyte count of 15 % and severe thrombocytopenia of 6000/μL. A sternal puncture had revealed marked erythroid hyperplasia and increased numbers of megakaryocytes, compatible with hemolysis and platelet consumption, respectively. Similar to Moschcowitz’ case, the autopsy showed innumerable thrombi in capillaries, arterioles, and smaller arteries of the heart, lung, liver, spleen, kidneys, brain, and other organs [3]. In this report, the small vessel “hyaline” thrombi were suggested to consist of thrombocytes and some fibrin. Singer et al. found only 11 similar reported cases, including Moschcowitz’ patient, with thrombocytopenia associated with multiple small vessel platelet thrombi. These authors suggested that they were dealing with a specific disease entity and proposed to designate it “thrombotic thrombocytopenic purpura” to highlight the presumed pathogenesis, namely, thrombocytopenia being caused by massive platelet consumption in the microvascular thrombotic process [3].
In 1966, Amorosi and Ultmann [4] reviewed 255 published patients having been diagnosed with thrombotic thrombocytopenic purpura (TTP) and added their own observations in 16 additional cases. They established a diagnostic pentad of clinical and laboratory findings: (1) hemolytic anemia with striking morphologically visible fragmentation of erythrocytes in the blood smear (schistocytes, helmet cells) (Fig. 1.1), (2) thrombocytopenia by consumption, (3) neurologic manifestations, (4) renal dysfunction, and (5) fever. They referred to the typical autopsy findings of microvascular thrombosis in any organ, especially the heart, brain, kidney, pancreas, and adrenals, and noted a striking absence of inflammatory changes in the involved vessels and rather limited areas of infarctions. As opposed to Singer et al. [3] suggesting that the “hyaline” thrombotic material consisted mainly of platelets, Amorosi and Ultmann [4] doubted on its nature. They stressed the unknown pathophysiology and dismal prognosis of TTP, affected patients usually showing a progressive disease course, the majority dying within 3 months.
1.2 A Congenital Form of Microangiopathic Hemolysis and Thrombocytopenia
Dr. Jefferson D. Upshaw, in 1978, described a 29-year-old woman who from the age of 6 months to 12 years had each year about 6–10 episodes of acute illness with fever, petechial rash, severe thrombocytopenia, and hemolytic anemia with microangiopathic changes in the red cell morphology on blood smears [5]. She had been repeatedly hospitalized and treated with antibiotics and blood transfusions with dramatic responses, usually recovering within 48 h. Corticosteroid treatment and splenectomy, performed at the age of 2 years, were not helpful. At the age of 12 years, the frequency of these acute disease episodes decreased to about 3–4 per year with completely asymptomatic intervals varying between 3 weeks and 20 months. Laboratory investigation during an acute attack showed severe thrombocytopenia (e.g., 3000/μL) and anemia (e.g., hematocrit of 19 %, marked reticulocytosis, and schistocytes on the blood smear). After transfusion of 2 units of packed red blood cells, she showed a partial response with platelet count stabilizing at ~50,000/μL and hematocrit at 32 %. One month later, she received, for a similar acute attack, 2 units of fresh whole blood which led to a complete normalization of the platelet count (278,000/μL) and hematocrit (41 %) within 48 h. This observation of a much better response to whole blood as compared to packed red cell concentrates suggested that a plasma factor was responsible for the hematologic correction. When readmitted with the next acute disease flare-up, she received 2 units of fresh platelet-poor plasma and showed a continuous rise of the platelet count, measurable at 20 h and peaking at 9 days with a value of 550,000/μL. During 11 years of consecutive follow-up, this young woman had 32 episodes of thrombocytopenia and microangiopathic hemolysis, sometimes occurring spontaneously but more often being triggered by a precipitating factor, e.g., a preceding (mild) infection, operation, pregnancy, fecal impaction, or pancreatitis. The patient always responded to fresh frozen plasma (FFP) transfusion with normalization of her platelet count and hematocrit and needed only a total of 5 units of red blood cell concentrates during 11 years of observation [5] (Fig. 1.2). Upshaw concluded that his case resembled that reported by Schulman et al. in 1960 [6] but, in contrast to these latter authors’ conclusion, was not due to “thrombopoietin” deficiency but rather to a constitutional deficiency of a factor present in normal plasma that protected from microangiopathic hemolysis and thrombocytopenia by peripheral consumption. Upshaw also noted the similarity of his patient’s hematologic picture with that observed in acute TTP [5].
Course of platelet count (10−3/μL) over a 10-month period in the patient with chronic relapsing thrombocytopenia and hemolysis reported by J. D. Upshaw in 1978 [5]. Reproducible (often overshooting) normalization of the platelet count occurs within a few days after plasma transfusions (P). From Upshaw JD (1978) N Engl J Med 298:1350–1352, with permission
1.3 Pathophysiological Hypotheses, Discovery of von Willebrand Factor (VWF)–Cleaving Protease, and Its Deficiency in TTP
Many different hypotheses on the etiology and pathogenesis of TTP have been proposed by various researchers over the years (for reviews, the reader is referred to Refs. [7–9]).
Endothelial injury, for instance, by oxidative stress, or reduced fibrinolytic activity of the vessel wall [10] has been described in TTP patients. A putative plasma factor stimulating the endothelial cell synthesis and release of prostacyclin (prostaglandin I2), a potent inhibitor of platelet aggregation, was suggested to be missing in patients with hemolytic uremic syndrome (HUS) and TTP [11]. A 37 kDa protein agglutinating normal platelets [12] or a 59 kDa protein aggregating platelets from healthy donors in the presence of Ca++ and fibrinogen [13] were isolated from the plasma of a few patients with acute TTP. A calcium-dependent cysteine protease was found in the sera of 15 patients during an acute bout of TTP but not during remission and was identified to activate platelets [14]. This protease was later identified to be calpain, associated with platelet microparticles and therefore resistant to plasma inhibitors [15]. Calpain cleaves platelet glycoprotein Ib thereby impairing VWF binding to this receptor and also cleaves the VWF subunit thereby promoting VWF binding to glycoprotein IIb/IIIa on activated platelets, enhancing platelet aggregation [16]. Anti-endothelial cell and, more specifically, anti-glycoprotein IV (CD36) antibodies have been found in plasma samples of most patients diagnosed with acute TTP [17, 18]. CD36 is an integral membrane protein located on microvascular endothelial cells, platelets, as well as some other cells. It has been suggested that anti-glycoprotein IV antibodies could be pathogenetically relevant for acute TTP by causing microvascular endothelial damage as well as platelet activation [17]. A more recent study by Raife et al. [19], however, found only minimal evidence for the presence of circulating endothelial cell- and platelet-reactive antibodies in plasma samples of TTP patients. Another group of researchers reported that plasma of patients with idiopathic TTP as well as human immunodeficiency virus-associated thrombotic microangiopathy (TMA) was able to induce apoptosis of microvascular endothelial cells but not of human umbilical vein endothelial cells [20] and circulating endothelial cells were detected in blood samples of TTP patients [21].
In 1982, Moake et al. reported the presence of unusually large (UL) VWF multimers in the plasma of four patients, including the abovementioned case reported by Upshaw in 1978 [5], with a chronic relapsing form of TTP [22]. The ULVWF multimers, similar in size to those secreted by cultured endothelial cells, were present mainly in plasma samples obtained during remission and tended to disappear during acute disease relapses (Fig. 1.3), probably by consumption of these extremely adhesive multimers during the microvascular platelet clumping process. Moake et al. suggested that the deficiency of an unknown VWF depolymerase, either a protease or a disulfide reductase, was causing the defective VWF processing leading to the relapsing course of TTP due to microvascular platelet thrombosis with ischemic organ manifestations by the extremely adhesive ULVWF multimers [22].
SDS–agarose gel electrophoresis for the analysis of VWF multimer distribution using autoradiography in plasma samples of patient A with chronic relapsing TTP reported by J. L. Moake et al. (1982) N Engl J Med 307:1432–1435 with permission. Patient A displays unusually large VWF multimers during remission (rem, upper part), similar to the endothelial cell culture supernatant (ec). Upon acute TTP relapse (rel), the ULVWF multimers disappeared, presumably by consumption during the microvascular thrombotic process. Normal plasma (n) VWF multimers are shown for comparison
In 1996, Furlan et al. [23] and Tsai [24] simultaneously and independently described a specific VWF–cleaving protease isolated from normal plasma. This isolated protease was not inhibited by inhibitors of serine proteases, cysteine proteases, or metalloproteases. Ca++ or Ba++ ions were needed to “activate” the VWF–cleaving protease isolated from citrated plasma [23], and mild denaturation of VWF by low-ionic-strength buffer containing 1.5 M urea [23] or 1.1–1.2 M guanidinium chloride [24] made the VWF susceptible to proteolytic cleavage by this newly identified protease. Tsai and coworkers [24, 25] further demonstrated that high fluid shear stress enhanced VWF proteolysis. This newly discovered VWF–cleaving protease received considerable interest also for the fact that it cleaved the VWF subunit in vitro at the peptide bond 842 tyrosine–843 methionine (amino acid numbering including the VWF propeptide: 1605 Tyr–1606 Met) [23], the peptide bond earlier reported to be physiologically cleaved during in vivo processing of VWF [26].
This specific VWF–cleaving protease gained widespread attention when we reported four patients, including two brothers (patients A1 and A2) and two unrelated patients (B and C), with a chronic relapsing form of TTP who showed a severe, probably constitutional deficiency of the VWF–cleaving protease activity in 1997 [27] (Fig. 1.4).
(a) VWF multimer analysis by SDS–agarose gel electrophoresis and immunoblotting in two brothers with chronic relapsing TTP (patient, brother), using two plasma samples each (1, 2) obtained several weeks apart. In contrast to samples from family members (mother, father, sister) and normal human plasma (NHP), both patients showed ULVWF multimers (double arrow). (b) VWF–cleaving protease assay using purified plasma-derived VWF substrate that had been incubated overnight with diluted plasma samples of patients (patient, brother), family members (mother, father, sister), or normal plasma (NHP), each preactivated by barium chloride. VWF substrate–plasma mixtures were dialyzed overnight against low-ionic strength buffer containing 1.5 M urea before SDS–agarose gel electrophoresis and immunoblotting. Both plasma samples (1, 2) of the two patients (patient, brother) had a completely lacking VWF–cleaving protease activity; mother and father had a mildly reduced activity (barely visible for father’s plasma samples), whereas sister’s plasma showed normal activity. NHP denotes normal pooled human plasma. Figures (a) and (b) are modified from M. Furlan et al. (1997) Blood 89:3097–3103
Both brothers had a history of recurrent TTP bouts over many years, including severe thrombocytopenia, schistocytic hemolytic anemia, and—in the elder brother—transient severe renal insufficiency and severe neurologic involvement with multiple cerebral infarctions. Both received intermittent plasma exchange (PEX) treatments with FFP replacement which reproducibly led to a transient normalization of the hematologic parameters [27] which is reminiscent of the abovementioned patient described by Upshaw [5]. Mixing the patient plasma samples of patients A1, A2, B, and C, respectively, with normal plasma (1:1, v:v), did not reveal an inhibition of the VWF–cleaving protease in normal plasma, and given that the parents of patients A1 and A2 had a slightly decreased VWF–cleaving protease activity, we suggested that at least patients A1 and A2 might have an inherited severe deficiency of the VWF–cleaving protease and that the resulting hyperadhesive ULVWF multimers were a pathogenetically relevant factor for the recurrent TTP in these patients [27].
In the following year, we reported another patient with recurrent episodes of TTP who was followed for 400 days with repeated laboratory analyses [28]. During his first acute TTP episode, he had a severe deficiency of the VWF–cleaving protease. After prolonged treatment with daily PEX sessions, FFP replacement, and corticosteroid, vincristine, and iloprost treatment, the platelet count finally normalized after more than 1 month, and in parallel, the VWF–cleaving protease activity progressively normalized. During the further course, VWF–cleaving protease activity redisappeared completely about 4 months after disease onset, and the patient suffered from an acute TTP relapse on day 221 which necessitated resumption of PEX and corticosteroid therapy. A second relapse with resumption of plasma therapy occurred on day 330. In the meantime, we had identified a circulating inhibitor of the VWF–cleaving protease in the plasma obtained at onset of the first TTP bout and in the plasma samples obtained when the protease redisappeared 4 months after the initial episode. This inhibitor was identified to be an IgG autoantibody, strongly inhibiting VWF proteolysis by VWF–cleaving protease in vitro. At this time point, we decided to perform a splenectomy on day 365 which led to the disappearance of the IgG inhibitor, normalization of the VWF–cleaving protease activity, and persistent normalization of platelets and hemoglobin [28]. At the time of this writing, the patient is in continuing remission without any therapy about 18 years after his initial disease bout.
In 1998, two independent studies, published in the same issue of the New England Journal of Medicine, demonstrated that a severe deficiency of the VWF–cleaving protease activity was not an anecdotal finding but a rather general feature of patients diagnosed with acute idiopathic TTP [29, 30]. Furlan et al. found a severe VWF–cleaving protease deficiency in 20 of 24 patients with acute nonfamilial TTP and moderate deficiency in the remaining four subjects. An inhibitor was identified in 20 of these patients. In addition, 6 patients (3 pairs of siblings) with a familial TTP had a severe VWF–cleaving protease deficiency without inhibitor, whereas all 23 patients diagnosed with familial (n = 10) or nonfamilial (n = 13) atypical hemolytic uremic syndrome had normal (in 2 instances slightly decreased) VWF–cleaving protease activity [29]. Tsai and Lian similarly found a severe VWF–cleaving protease deficiency in all 37 patients with acute TTP, whereas no deficiency was found in remission samples and a series of hospital control samples. IgG inhibitors were detected in 26 of the 39 plasma samples obtained from 37 patients with acute TTP [30].
These findings of a severe VWF–cleaving protease deficiency in acute TTP have been heavily criticized as completely unspecific [31] or as also occurring in various inflammatory conditions, liver cirrhosis, and uremia, in later stages of pregnancy, or in newborns [32], but the methodology of measuring this enzyme was not using a proper standard curve [31], or the authors considered samples with mildly or moderately decreased VWF–cleaving protease as “deficient” samples [32]. In a prospective study on 68 hospitalized patients with thrombocytopenia of various causes (except TMAs), we found 12 of the 68 patients having VWF–cleaving protease activity ≤30 % of the normal, but none with a severe deficiency of <5 % [33]. Therefore, a severely deficient VWF–cleaving protease activity was considered to be a rather specific feature of TTP.
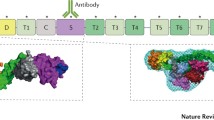
In 2001, 5 years after the initial isolation of VWF–cleaving protease from plasma [23, 24], three research teams had succeeded in purifying the protease from plasma to homogeneity and performed N-terminal amino acid sequence analysis [34–36]. Based on the partial amino acid sequence, Zheng et al. were able to identify VWF–cleaving protease as a new member of the ADAMTS (a disintegrin and metalloprotease with thrombospondin type 1 motifs) family of metalloproteases, denoted as ADAMTS13, and to locate the respective gene to chromosome 9q34 [37]. At the same time, Levy et al. reported their genome-wide linkage analysis in four pedigrees with patients suffering from a constitutional TTP and severe VWF–cleaving protease deficiency [38]. They identified the same gene on chromosome 9q34, belonging to the ADAMTS family of zinc metalloproteases, ADAMTS13. In their investigated families, the authors studied patients with a severe ADAMTS13 deficiency, asymptomatic carriers with about half-normal activity, and subjects with normal VWF–cleaving protease activity and were able to identify 12 different putative ADAMTS13 mutations explaining 14 of the 15 disease alleles [38] (Fig. 1.5).
ADAMTS13 gene structure (a), protein domain structure (b), and ADAMTS13 mutations (c) identified in patients with hereditary TTP by G. G. Levy et al. (2001) Nature 413:488–494. The 29 vertical bars in panel a denote exons. In panel b, S denotes signal peptide, P propeptide, Dis disintegrin domain, 1 first thrombospondin type 1 domain, Cys cysteine-rich domain, 2–8 seven additional thrombospondin type 1 domains, CUB Cub domain. In panel c, missense, splice site, and frameshift mutations located over the whole gene are shown, exchanges of amino acids labeled in single-letter code. Figure reproduced by courtesy from X.L. Zheng et al. (2002) Current Opinion in Hematology 9:389–394, with permission
Thus, the missing plasma factor in Upshaw’s patient suffering from chronic relapsing constitutional TTP [5] was identified as ADAMTS13 23 years later. Plaimauer et al. expressed a functionally active human ADAMTS13 in mammalian cells in 2002 [39] which corrected the lacking VWF proteolytic processing when added to the plasma of the abovementioned two brothers with severe constitutional VWF–cleaving protease deficiency identified in 1997 [27, 40].
For further insights into the fascinating discovery of the VWF proteolytic processing and its defect as a main pathogenetic factor in TTP, the reader is referred to historical sketches and personal annotations of three protagonists in the field, Drs. Miha Furlan, Han-Mou Tsai, and Joel Moake [41–43].
1.4 Therapeutic Efforts in TTP
Here, we present some important aspects on the development of the therapeutic strategies in TTP and refer the reader to some earlier reviews highlighting various aspects of treatment of this devastating disease [44–48]. Until the 1960s and early 1970s, TTP was almost universally fatal, and patients usually died out of good general health after a progressive disease course over days to a few weeks [4]. In 1959, Rubinstein et al. reported “an unusual remission in a case of thrombotic thrombocytopenic purpura syndrome following fresh blood exchange transfusions” [49]. In the late 1970s, reports on a few patients suggested a beneficial effect of exchange transfusions, PEX, and replacement using FFP [50, 51]. This largely empirical treatment was based on the assumption that either a toxic substance needed to be removed from the plasma or alternatively a missing substance was to be replaced by infusion of fresh plasma. Despite a lacking pathophysiologic basis underlying plasma therapy, the clinically evident drastically improved survival of patients with acute TTP led to a rather widespread use of PEX and/or FFP infusion. In 1987, Shepard and Bukowski reviewed the accumulated experience with exchange transfusions, FFP infusions, and PEX in TTP patients and concluded that a randomized clinical trial comparing various forms of plasma therapy would be highly desirable but difficult to perform and that at the present time they favored the initial use of PEX with FFP replacement [52]. In 1991, the Canadian Apheresis Study Group published such a randomized controlled trial comparing PEX with FFP replacement versus simple FFP infusion in TTP patients [53]. In this landmark study on 102 patients, Rock et al. demonstrated that PEX of 1.5 plasma volumes daily for 3 days, followed by PEX of 1 volume daily and FFP replacement, was superior to FFP infusion alone, response rates after the first treatment cycle and at 6 months being 47 and 78 %, respectively, for PEX/FFP versus 25 and 49 %, respectively, for FFP infusion. The mortality at 6 months was 22 % in the PEX/FFP group versus 37 % in the FFP infusion group which was significantly different [53]. These findings were supported by an accompanying single-center/single-protocol cohort study that suggested, in addition, that corticosteroid treatment may be an important adjunct to PEX/FFP and sometimes be effective if given alone without any plasma therapy in milder cases of TTP [54].
Evidently, the discovery of autoantibody-mediated severe ADAMTS13 deficiency in acquired TTP [9, 29, 30, 55] and of homozygous or double heterozygous ADAMTS13 mutations in hereditary TTP [38, 40, 56] as the relevant pathogenetic factors gave some rationale to the various forms of plasma therapy. Thus, for the rare patients suffering from a hereditary TTP, also denoted as Upshaw–Schulman syndrome, caused by biallelic ADAMTS13 mutations, simple FFP infusion may be effective therapeutically and prophylactically when given every 2–3 weeks [9, 57], sometimes over many years without any attacks of TTP [58]. Erroneous diagnoses of immune thrombocytopenic purpura or Evans syndrome in children with Upshaw–Schulman syndrome are common [59] and may lead to wrong therapeutic measures such as steroid therapy or even splenectomy as was already performed in the index case without any benefit [5]. Missing a timely diagnosis in a seemingly “hyperactive child” was associated with severe neurological deficits and multiple cerebral infarctions at the time of diagnosis in a 3-year-old boy [60]. In another instance, we diagnosed hereditary TTP postmortem in a 7-year-old boy who had suffered from hemolytic anemia and thrombocytopenia since birth [61].
For the more common patients with acquired TTP, large-volume PEX with replacement of FFP may both remove IgG autoantibodies and replace ADAMTS13 [46], and corticosteroids may suppress autoantibody production. Splenectomy had been empirically performed in earlier years before plasma therapy was recognized to be useful and also later in plasma-resistant or relapsing TTP patients [62]. Thirty-three patients with acquired TTP, subjected to splenectomy because of plasma refractoriness (n = 9) or because of TTP relapse (n = 24) from 1982 to 2002, seemed to benefit substantially from this procedure: Splenectomy generated prompt remissions in all but 5 patients, and in those with relapsing TTP the relapse rate decreased from 0.74 relapses/patient-year before to 0.10 relapses/patient-year after splenectomy with long-term observation over many years before and after the procedure [62].
Many other treatment strategies have been used, including vincristine; the anti-CD20 monoclonal antibody rituximab with the intent to inhibit autoantibody production by B-lymphocytes [63]; protein A immunoadsorption, either empirically [64] or intending to remove anti-ADAMTS13 autoantibodies [46]; cyclosporin instead of corticosteroids for autoantibody suppression [65]; an aptamer [66] or a nanobody [67] binding to the “activated” A1 domain of VWF and thereby inhibiting VWF–platelet glycoprotein Ib interaction; and, very recently, N-acetylcysteine, intended to disulfide-reduce ULVWF multimers [68]. It is out of the scope of this chapter to discuss these therapeutic means in more detail.
1.5 Differential Diagnosis of TTP, HUS, and Other TMAs
Today, various tentative entities of TMAs are recognized; a categorization of the most common forms is shown in Table 1.1.
Here, we do not discuss the historical aspects of all these TMAs but ask the question whether TTP and HUS, first described by Gasser et al. in 1955 [69], are different disease entities or mere variants of the same disease process (see also Refs. [45, 48]). Furthermore, we try to assess the sensitivity and specificity of the laboratory finding of a severe ADAMTS13 deficiency for the clinical diagnosis of TTP. When Furlan et al. [29] and Tsai and Lian [30] reported severe VWF–cleaving protease deficiency in 26/30 patients [29] and 37/37 patients [30] with acute TTP but normal (or mildly reduced) VWF–cleaving protease activity in 23/23 patients with a diagnosis of (atypical) HUS [29], a rather strict segregation of TTP with severe ADAMTS13 deficiency and (atypical) HUS with normal (or mildly decreased) ADAMTS13 deficiency was apparent. This was rather surprising given the often difficult clinical distinction in individual patients. Table 1.2 summarizes some earlier cohort studies from different centers on patients having been clinically diagnosed with acute TTP [29, 30, 70–76].
It is evident from these case series that only about 60–70 % (range 33–100 %) of the patients with a clinical diagnosis of TTP had a severely deficient ADAMTS13 activity [55]. Therefore, the sensitivity of finding a severely decreased ADAMTS13 activity for the clinical diagnosis of TTP may not be 100 %, and one has to admit that there may be cases with clinically apparent TTP without severely deficient ADAMTS13 activity using currently available in vitro assays. Tsai [77] disagreed with this statement reporting that all 127 cases of TTP investigated by him had an ADAMTS13 activity lower than 10 % and that the diagnosis of TTP should not be made without severe ADAMTS13 deficiency. We tend to suggest that a diagnosis of TTP should not be strictly excluded in the absence of severely deficient ADAMTS13 activity. Observing a patient with recurring acquired TTP bouts over 8 years, each bout characterized by severe hemolytic anemia, thrombocytopenia, and various clinical signs suggesting TTP, we found a low normal ADAMTS13 activity using three different assays, no functional inhibitor, and only borderline-positive anti-ADAMTS13 autoantibodies by ELISA at his first disease bout [78]. During subsequent acute TTP episodes, the situation changed, and at his fifth and sixth bouts, all three ADAMTS13 activity assays (VWF multimer degradation assay, FRETS-VWF73 assay, and flow-based assay) congruently revealed a severe ADAMTS13 deficiency. In addition, a circulating ADAMTS13 inhibitor and autoantibodies directed against ADAMTS13 by ELISA were now present [78]. It is unlikely that this patient who ultimately died from another TTP bout had acute episodes of different diseases. Rather, all his acute disease attacks should be considered as “TTP,” and one may question whether our currently available ADAMTS13 assays may miss an “in vivo defect” of the ADAMTS13–VWF interaction in some rare instances. From the Oklahoma TTP–HUS registry, we also learned that the response to PEX in patients with clinically diagnosed idiopathic TTP was similar in the 32 without severe ADAMTS13 deficiency as in the 16 severely deficient patients [72]. Therefore, we should probably accept that at least some patients with a “bona fide” TTP may not have a lacking ADAMTS13 activity as assessed with our currently available methodology.
Concerning the specificity of a severely decreased ADAMTS13 activity for TTP, there have been early claims that this finding was largely unspecific [31, 32] (see above, Sect. 1.3). Bianchi et al. [33], however, confirmed the specificity of a strongly depressed VWF–cleaving protease activity for a TMA most clinicians would diagnose as TTP. On the contrary, Remuzzi et al. maintained that a severely deficient VWF–cleaving protease was also found in some patients with HUS, at least in familial and recurrent cases [79], and Remuzzi concluded, therefore, that this laboratory feature was not specific for TTP [80]. Similarly, in the excellent prospective cohort study on patients with acute TMA by Veyradier et al., there were a few cases clinically diagnosed as HUS that had a lacking VWF–cleaving protease, whereas the majority of those with HUS had a normal or subnormal activity [70]. We believe that there may be clinical overlap, mainly in cases with hereditary TTP caused by biallelic ADAMTS13 mutations, and several cases with severe constitutional ADAMTS13 deficiency, including the abovementioned index case A1 [27], had (transient) severe kidney failure making it likely that they could be diagnosed as “HUS” instead of hereditary TTP. In this context, the report by Noris et al. on two sisters with severe hereditary ADAMTS13 deficiency caused by double heterozygous ADAMTS13 mutations is of interest [81]. Both sisters had phenotypically different disease episodes, and it was found that only the one developing chronic renal failure had, in addition, a heterozygous complement factor H mutation characteristic of atypical HUS [82]. Thus, modifying genetic and possibly environmental factors may alter the phenotype of acute disease episodes in hereditary and possibly also in acquired TTP which may then preclude to clearly categorize these cases as TTP or atypical HUS.
Tsai and collaborators carefully investigated 16 children with typical HUS after Escherichia coli O157:H7 infection and noted normal VWF–cleaving protease activity and a loss of large VWF multimers in all of them [83]. They also highlighted the different composition of microthrombi in postmortem histologic preparations. Glomerular microthrombi in typical HUS were fibrin rich but did not contain VWF. In contrast, postmortem brain sections of a TTP patient revealed microthrombi that were mainly composed of platelets and VWF [83]. Hosler et al. performed a retrospective autopsy review on 56 cases and concluded that TTP and HUS were distinct pathologic entities. The 25 patients diagnosed with TTP demonstrated platelet-rich thrombi in the heart, pancreas, kidney, adrenal gland, and brain, whereas the 31 with a diagnosis of HUS had fibrin-/red cell-rich thrombi, largely confined to the kidney [84]. Most physicians are reluctant, however, to perform diagnostic biopsies in patients admitted with acute TMA, having severe thrombocytopenia. Therefore, in most centers, no diagnostic biopsies are performed. Similar to Tsai et al. [83], we performed a study in 29 children diagnosed with enterohemorrhagic E. coli-associated HUS diagnosed at two centers in London [85]. Whereas 28/29 children had a normal (in 2 instances subnormal) VWF–cleaving protease activity, one 18-month-old toddler had a severely decreased protease activity and an inhibitor. Stool cultures obtained on admission had grown E. coli O157. Follow-up investigations 3 years later showed normal renal function, and VWF–cleaving protease assay gave a normal value, also in his parents and his sister [85]. It is difficult to interpret this situation in retrospect, but one may hypothesize that this toddler in fact had a transient autoantibody-mediated ADAMTS13 deficiency and the superimposed enterohemorrhagic E. coli infection triggered an acute TMA disease bout which is somewhat reminiscent to the animal TTP model reported by Motto et al. in which Shiga toxin injection was the best identified trigger to bring about an acute TTP-like disease in susceptible ADAMTS13 knockout mice [86].
In conclusion, severe ADAMTS13 deficiency is a rather specific finding for a TMA which most clinicians tend to diagnose as TTP, but there may be some cases clinically presenting as classical TTP in which our current diagnostic tests do not show a lacking ADAMTS13.
1.6 Conclusions
These historical considerations show the fascinating evolution of our knowledge on TTP and other TMAs during the past decades. Even though new insights into disease mechanisms were obtained and a defective proteolytic regulation of the newly synthesized and secreted extremely adhesive unusually large VWF multimers has been recognized as an important pathogenetic factor, many questions remain and new ones are raised. We refer to the other chapters of this book highlighting various state-of-the-art aspects of TTP and ADAMTS13. We believe that these historical annotations should be kept in mind, also for further research, because it is not excluded that some earlier pathophysiologic hypotheses may be shown to contribute to the complex pathogenesis of the various forms of TMAs.
References
Moschcowitz E. Hyaline thrombosis of the terminal arterioles and capillaries: a hitherto undescribed disease. Proc N Y Pathol Soc. 1924;24:21–4.
Moschcowitz E. An acute febrile pleiochromic anemia with hyaline thrombosis of the terminal arterioles and capillaries. An undescribed disease. Arch Intern Med. 1925;36:89–93.
Singer K, Bornstein FP, Wile SA. Thrombotic thrombocytopenic purpura: hemorrhagic diathesis with generalized platelet thromboses. Blood. 1947;2:542–54.
Amorosi EL, Ultmann JE. Thrombotic thrombocytopenic purpura: report of 16 cases and review of the literature. Medicine. 1966;45:139–59.
Upshaw JD. Congenital deficiency of a factor in normal plasma that reverses microangiopathic hemolysis and thrombocytopenia. N Engl J Med. 1978;298:1350–2.
Schulman I, Pierce M, Lukens A, Currimbhoy Z. Studies on thrombopoiesis. I. A factor in normal human plasma required for platelet production; chronic thrombocytopenia due to its deficiency. Blood. 1960;16:943–57.
Ruggenenti P, Remuzzi G. The pathophysiology and management of thrombotic thrombocytopenic purpura. Eur J Haematol. 1996;56:191–207.
Moake JL, Chow TW. Thrombotic thrombocytopenic purpura: understanding a disease no longer rare. Am J Med Sci. 1998;316:105–19.
Furlan M, Lämmle B. Aetiology and pathogenesis of thrombotic thrombocytopenic purpura and haemolytic uraemic syndrome: the role of von Willebrand factor-cleaving protease. Best Pract Res Clin Haematol. 2001;14:437–54.
Kwaan HC. Role of fibrinolysis in thrombotic thrombocytopenic purpura. Semin Thromb Hemost. 1979;6:395–400.
Remuzzi G, Misiani R, Marchesi D, Livio M, Mecca G, De Gaetano G, Donati MB. Haemolytic-uraemic syndrome: deficiency of plasma factor(s) regulating prostacyclin activity? Lancet. 1978;2:871–2.
Siddiqui FA, Lian ECY. Novel platelet-agglutinating protein from a thrombotic thrombocytopenic purpura plasma. J Clin Invest. 1985;76:1330–7.
Lian ECY, Siddiqui FA, Chen SH, Feng LM. Platelet-agglutinating/aggregating proteins from the plasma of patients with thrombotic thrombocytopenic purpura. In: Kaplan BS, Trompeter RS, Moake JL, editors. HUS and TTP. New York: Marcel Dekker, Inc; 1992. p. 473–81.
Murphy WG, Moore JC, Kelton JG. Calcium-dependent cysteine protease activity in the sera of patients with thrombotic thrombocytopenic purpura. Blood. 1987;70:1683–7.
Kelton JG, Warkentin TE, Hayward CPM, Murphy WG, Moore JC. Calpain activity in patients with thrombotic thrombocytopenic purpura is associated with platelet microparticles. Blood. 1992;80:2246–51.
Moore JC, Murphy WG, Kelton JG. Calpain proteolysis of von Willebrand factor enhances its binding to platelet membrane glycoprotein IIb/IIIa: an explanation for platelet aggregation in thrombotic thrombocytopenic purpura. Br J Haematol. 1990;74:457–64.
Tandon NN, Rock G, Jamieson GA. Anti-CD36 antibodies in thrombotic thrombocytopenic purpura. Br J Haematol. 1994;88:816–25.
Schultz DR, Arnold PI, Jy W, et al. Anti-CD36 autoantibodies in thrombotic thrombocytopenic purpura and other thrombotic disorders: identification of an 85 kD form of CD36 as a target antigen. Br J Haematol. 1998;103:849–57.
Raife TJ, Atkinson B, Aster RH, et al. Minimal evidence of platelet and endothelial cell reactive antibodies in thrombotic thrombocytopenic purpura. Am J Hematol. 1999;62:82–7.
Laurence J, Mitra D, Steiner M, et al. Plasma from patients with idiopathic and human immunodeficiency virus-associated thrombotic thrombocytopenic purpura induces apoptosis in microvascular endothelial cells. Blood. 1996;87:3245–54.
Lefevre P, George F, Durand JM, et al. Detection of circulating endothelial cells in thrombotic thrombocytopenic purpura. Thromb Haemost. 1993;69:522.
Moake JL, Rudy CK, Troll JH, Weinstein MJ, Colannino NM, Azocar J, Seder RH, Hong SL, Deykin D. Unusually large plasma factor VIII: Von Willebrand factor multimers in chronic relapsing thrombotic thrombocytopenic purpura. N Engl J Med. 1982;307:1432–5.
Furlan M, Robles R, Lämmle B. Partial purification and characterization of a protease from human plasma cleaving von Willebrand factor to fragments produced by in vivo proteolysis. Blood. 1996;87:4223–34.
Tsai HM. Physiologic cleavage of von Willebrand factor by a plasma protease is dependent on its conformation and requires calcium ion. Blood. 1996;87:4235–44.
Tsai HM, Sussman II, Nagel RL. Shear stress enhances the proteolysis of von Willebrand factor in normal plasma. Blood. 1994;83:2171–9.
Dent JA, Berkowitz SD, Ware J, Kasper CK, Ruggeri ZM. Identification of a cleavage site directing the immunochemical detection of molecular abnormalities in type IIA von Willebrand factor. Proc Natl Acad Sci U S A. 1990;87:6306–10.
Furlan M, Robles R, Solenthaler M, Wassmer M, Sandoz P, Lämmle B. Deficient activity of von Willebrand factor-cleaving protease in chronic relapsing thrombotic thrombocytopenic purpura. Blood. 1997;89:3097–103.
Furlan M, Robles R, Solenthaler M, Lämmle B. Acquired deficiency of von Willebrand factor-cleaving protease in a patient with thrombotic thrombocytopenic purpura. Blood. 1998;91:2839–46.
Furlan M, Robles R, Galbusera M, Remuzzi G, Kyrle PA, Brenner B, Krause M, Scharrer I, Aumann V, Mittler U, Solenthaler M, Lämmle B. Von Willebrand factor-cleaving protease in thrombotic thrombocytopenic purpura and the hemolytic-uremic syndrome. N Engl J Med. 1998;339:1578–84.
Tsai HM, Lian ECY. Antibodies to von Willebrand factor-cleaving protease in acute thrombotic thrombocytopenic purpura. N Engl J Med. 1998;339:1585–94.
Moore JC, Hayward CPM, Warkentin TE, Kelton JG. Decreased von Willebrand factor protease activity associated with thrombocytopenic disorders. Blood. 2001;98:1842–6.
Mannucci PM, Canciani MT, Forza I, Lussana F, Lattuada A, Rossi E. Changes in health and disease of the metalloprotease that cleaves von Willebrand factor. Blood. 2001;98:2730–5.
Bianchi V, Robles R, Alberio L, Furlan M, Lämmle B. Von Willebrand factor-cleaving protease (ADAMTS-13) in thrombocytopenic disorders: a severely deficient activity is specific for thrombotic thrombocytopenic purpura. Blood. 2002;100:710–3.
Gerritsen HE, Robles R, Lämmle B, Furlan M. Partial amino acid sequence analysis of purified von Willebrand factor-cleaving protease. Blood. 2001;98:1654–61.
Fujikawa K, Suzuki H, McMullen B, Chung D. Purification of human von Willebrand factor-cleaving protease and its identification as a new member of the metalloproteinase family. Blood. 2001;98:1662–6.
Soejima K, Mimura N, Hirashima M, Maeda H, Hamamoto T, Nakagaki T, Nozaki C. A novel human metalloprotease synthesized in the liver and secreted into the blood: possibly, the von Willebrand factor-cleaving protease? J Biochem. 2001;130:475–80.
Zheng XL, Chung D, Takayama TK, Majerus EM, Sadler JE, Fujikawa K. Structure of von Willebrand factor-cleaving protease (ADAMTS13), a metalloprotease involved in thrombotic thrombocytopenic purpura. J Biol Chem. 2001;276:41059–63.
Levy GG, Nichols WC, Lian EC, Foroud T, McClintick JN, McGee BM, Yang AY, Siemieniak DR, Stark KR, Gruppo R, Sarode R, Shurin SB, Chandrasekaran V, Stabler SP, Sabio H, Bouhassira EE, Upshaw Jr JD, Ginsburg D, Tsai HM. Mutations in a member of the ADAMTS gene family cause thrombotic thrombocytopenic purpura. Nature. 2001;413:488–94.
Plaimauer B, Zimmermann K, Völkel D, Antoine G, Kerschbaumer R, Jenab P, Furlan M, Gerritsen H, Lämmle B, Schwarz HP, Scheiflinger F. Cloning, expression, and functional characterization of the von Willebrand factor-cleaving protease (ADAMTS13). Blood. 2002;100:3626–32.
Antoine G, Zimmermann K, Plaimauer B, Grillowitzer M, Studt JD, Lämmle B, Scheiflinger F. ADAMTS13 gene defects in two brothers with constitutional thrombotic thrombocytopenic purpura and normalization of von Willebrand factor-cleaving protease activity by recombinant human ADAMTS13. Br J Haematol. 2003;120:821–4.
Furlan M. Proteolytic cleavage of von Willebrand factor by ADAMTS-13 prevents uninvited clumping of blood platelets. J Thromb Haemost. 2004;2:1505–9.
Tsai HM. A journey from sickle cell anemia to ADAMTS13. J Thromb Haemost. 2004;2:1510–4.
Moake JL. Defective processing of unusually large von Willebrand factor multimers and thrombotic thrombocytopenic purpura. J Thromb Haemost. 2004;2:1515–21.
Rock GA. Management of thrombotic thrombocytopenic purpura. Br J Haematol. 2000;109:496–507.
George JN. How I treat patients with thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Blood. 2000;96:1223–9.
Fontana S, Kremer Hovinga JA, Studt JD, Alberio L, Lämmle B, Mansouri Taleghani B. Plasma therapy in thrombotic thrombocytopenic purpura: review of the literature and the Bern experience in a subgroup of patients with severe acquired ADAMTS-13 deficiency. Semin Hematol. 2004;41:48–59.
George JN. Thrombotic thrombocytopenic purpura. N Engl J Med. 2006;354:1927–35.
George JN. How I treat patients with thrombotic thrombocytopenic purpura: 2010. Blood. 2010;116:4060–9.
Rubinstein MA, Kagan BM, MacGillviray MH, Merliss R, Sacks H. Unusual remission in a case of thrombotic thrombocytopenic purpura syndrome following fresh blood exchange transfusions. Arch Intern Med. 1959;51:1409–19.
Bukowski RM, King JW, Hewlett JS. Plasmapheresis in the treatment of thrombotic thrombocytopenic purpura. Blood. 1977;50:413–7.
Byrnes JJ, Khurana M. Treatment of thrombotic thrombocytopenic purpura with plasma. N Engl J Med. 1977;297:1386–9.
Shepard KV, Bukowski RM. The treatment of thrombotic thrombocytopenic purpura with exchange transfusions, plasma infusions, and plasma exchange. Semin Hematol. 1987;24:178–93.
Rock GA, Shumak KH, Buskard NA, Blanchette VS, Kelton JG, Nair RC, Spasoff RA. Comparison of plasma exchange with plasma infusion in the treatment of thrombotic thrombocytopenic purpura. Canadian Apheresis Study Group. N Engl J Med. 1991;325:393–7.
Bell WR, Braine HG, Ness PM, Kickler TS. Improved survival in thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Clinical experience in 108 patients. N Engl J Med. 1991;325:398–403.
Lämmle B, Kremer Hovinga JA, Alberio L. Thrombotic thrombocytopenic purpura. J Thromb Haemost. 2005;3:1663–75.
Kokame K, Matsumoto M, Soejima K, Yagi H, Ishizashi H, Funato M, Tamai H, Konno M, Kamide K, Kawano Y, Miyata T, Fujimura Y. Mutations and common polymorphisms in ADAMTS13 gene responsible for von Willebrand factor-cleaving protease activity. Proc Natl Acad Sci U S A. 2002;99:11902–7.
Kinoshita S, Yoshioka A, Park YD, Ishizashi H, Konno M, Funato M, Matsui T, Titani K, Yagi H, Matsumoto M, Fujimura Y. Upshaw–Schulman syndrome revisited: a concept of congenital thrombotic thrombocytopenic purpura. Int J Hematol. 2001;74:101–8.
Barbot J, Costa E, Guerra M, Barreirinho MS, Isvarlal P, Robles R, Gerritsen HE, Lämmle B, Furlan M. Ten years of prophylactic treatment with fresh-frozen plasma in a child with chronic relapsing thrombotic thrombocytopenic purpura as a result of a congenital deficiency of von Willebrand factor-cleaving protease. Br J Haematol. 2001;113:649–51.
Schneppenheim R, Budde U, Oyen F, Angerhaus D, Aumann V, Drewke E, Hassenpflug W, Häberle J, Kentouche K, Kohne E, Kumik K, Mueller-Wiefel D, Obser T, Santer R, Sykora KW. Von Willebrand factor cleaving protease and ADAMTS13 mutations in childhood TTP. Blood. 2003;101:1845–50.
Häberle J, Kehrel B, Ritter J, Jürgens H, Lämmle B, Furlan M. New strategies in diagnosis and treatment of thrombotic thrombocytopenic purpura: case report and review. Eur J Pediatr. 1999;158:883–7.
Studt JD, Kremer Hovinga JA, Antoine G, Hermann M, Rieger M, Scheiflinger F, Lämmle B. Fatal congenital thrombotic thrombocytopenic purpura with apparent ADAMTS13 inhibitor: in vitro inhibition of ADAMTS13 activity by hemoglobin. Blood. 2005;105:542–4.
Kappers-Klunne MC, Wijermans P, Fijnheer R, Croockewit AJ, van der Holt B, de Wolf JTM, Löwenberg B, Brand A. Splenectomy for the treatment of thrombotic thrombocytopenic purpura. Br J Haematol. 2005;130:768–76.
Fakhouri F, Vernant JP, Veyradier A, Wolf M, Kaplanski G, Binaut R, Rieger M, Scheiflinger F, Poulin P, Deroure B, Delarue R, Lesavre P, Vanhille P, Hermine O, Remuzzi G, Grünfeld JP. Efficiency of curative and prophylactic treatment with rituximab in ADAMTS13-deficient thrombotic thrombocytopenic purpura: a study of 11 cases. Blood. 2005;106:1932–7.
Gaddis TG, Guthrie TH, Drew MJ, Sahud M, Howe RB, Mittelman A. Treatment of plasma refractory thrombotic thrombocytopenic purpura with protein A immunoabsorption. Am J Hematol. 1997;55:55–8.
Cataland SR, Jin M, Lin S, Kennedy MS, Kraut EH, George JN, Wu HM. Cyclosporin and plasma exchange in thrombotic thrombocytopenic purpura: long-term follow-up with serial analysis of ADAMTS13 activity. Br J Haematol. 2007;139:486–93.
Cataland SR, Peyvandi F, Mannucci PM, Lämmle B, Kremer Hovinga JA, Machin SJ, Scully M, Rock G, Gilbert JC, Yang S, Wu H, Jilma B, Knoebl P. Initial experience from a double-blind, placebo-controlled, clinical outcome study of ARC1779 in patients with thrombotic thrombocytopenic purpura. Am J Hematol. 2012;87:430–2.
Hulstein JJ, de Groot PG, Silence K, Veyradier A, Fijnheer R, Lenting PJ. A novel nanobody that detects the gain-of-function phenotype of von Willebrand factor in ADAMTS13 deficiency and von Willebrand disease type 2B. Blood. 2005;106:3035–42.
Li GW, Rambally S, Kamboj J, Reilly S, Moake JL, Udden MM, Mims MP. Treatment of refractory thrombotic thrombocytopenic purpura with N-acetylcysteine: a case report. Transfusion. 2014;54:1221–4.
Gasser C, Gautier E, Steck A, Siebenmann RE, Oechslin R. Hämolytisch-urämische Syndrome: Bilaterale Nierenrindennekrosen bei akuten erworbenen hämolytischen Anämien. Schweiz Med Wochenschr. 1955;85:905–9.
Veyradier A, Obert B, Houllier A, Meyer D, Girma JP. Specific von Willebrand factor-cleaving protease in thrombotic microangiopathies: a study of 111 cases. Blood. 2001;98:1765–72.
Mori Y, Wada H, Gabazza EC, Minami N, Nobori T, Shiku H, Yagi H, Ishizashi H, Matsumoto M, Fujimura Y. Predicting response to plasma exchange in patients with thrombotic thrombocytopenic purpura with measurement of VWF-cleaving protease activity. Transfusion. 2002;42:572–80.
Vesely SK, George JN, Lämmle B, Studt JD, Alberio L, El-Harake MA, Raskob GE. ADAMTS-13 activity in thrombotic thrombocytopenic purpura-hemolytic uremic syndrome: relation to presenting features and clinical outcomes in a prospective cohort of 142 patients. Blood. 2003;102:60–8.
Matsumoto M, Yagi H, Ishizashi H, Wada H, Fujimura Y. The Japanese experience with thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Semin Hematol. 2004;41:68–74.
Kremer Hovinga JA, Studt JD, Alberio L, Lämmle B. Von Willebrand factor-cleaving protease (ADAMTS-13) activity determination in the diagnosis of thrombotic microangiopathies: the Swiss experience. Semin Hematol. 2004;41:75–82.
Zheng XL, Kaufmann RM, Goodnough LT, Sadler JE. Effect of plasma exchange on plasma ADAMTS-13 metalloprotease activity, inhibitor level, and clinical outcome in patients with idiopathic and nonidiopathic thrombotic thrombocytopenic purpura. Blood. 2004;103:4043–9.
Peyvandi F, Ferrari S, Lavoretano S, Canciani MT, Mannucci PM. Willebrand factor cleaving protease (ADAMTS-13) and ADAMTS-13 neutralizing autoantibodies in 100 patients with thrombotic thrombocytopenic purpura. Br J Haematol. 2004;127:433–9.
Tsai HM. Is severe deficiency of ADAMTS-13 specific for thrombotic thrombocytopenic purpura? Yes. J Thromb Haemost. 2003;1:625–31.
Froehlich-Zahnd R, George JN, Vesely SK, Terrell DR, Aboulfatova K, Dong JF, Luken BM, Voorberg J, Budde U, Sulzer I, Lämmle B, Kremer Hovinga JA. Evidence for a role of anti-ADAMTS13 autoantibodies despite normal ADAMTS13 activity in recurrent thrombotic thrombocytopenic purpura. Haematologica. 2012;97:297–303.
Remuzzi G, Galbusera M, Noris M, Canciani MT, Daina E, Bresin E, Contaretti S, Caprioli J, Gamba S, Ruggenenti P, Perico N, Mannucci PM. Von Willebrand factor cleaving protease (ADAMTS13) is deficient in recurrent and familial thrombotic thrombocytopenic purpura and hemolytic uremic syndrome. Blood. 2002;100:778–85.
Remuzzi G. Is ADAMTS-13 deficiency specific for thrombotic thrombocytopenic purpura? No. J Thromb Haemost. 2003;1:632–4.
Noris M, Bucchioni S, Galbusera M, Donadelli R, Bresin E, Castelletti F, Caprioli J, Brioschi S, Scheiflinger F, Remuzzi G. Complement factor H mutation in familial thrombotic thrombocytopenic purpura with ADAMTS13 deficiency and renal involvement. J Am Soc Nephrol. 2005;16:1177–83.
Noris M, Remuzzi G. Atypical hemolytic-uremic syndrome. N Engl J Med. 2009;361:1676–87.
Tsai HM, Chandler WL, Sarode R, Hoffman R, Jelacic S, Habeeb RL, Watkins SL, Wong CS, Williams GD, Tarr PI. Von Willebrand factor and von Willebrand factor-cleaving metalloprotease activity in Escherichia coli O157:H7-associated hemolytic uremic syndrome. Pediatr Res. 2001;49:653–9.
Hosler GA, Cusumano AM, Hutchins GM. Thrombotic thrombocytopenic purpura and hemolytic uremic syndrome are distinct pathologic entities. A review of 56 autopsy cases. Arch Pathol Lab Med. 2003;127:834–9.
Hunt BJ, Lämmle B, Nevard CHF, Haycock GB, Furlan M. Von Willebrand factor-cleaving protease in childhood diarrhoea-associated haemolytic uraemic syndrome. Thromb Haemost. 2001;85:975–8.
Motto DG, Chauhan AK, Zhu G, Homeister J, Lamb CB, Desch KC, Zhang W, Tsai HM, Wagner DD, Ginsburg D. Shigatoxin triggers thrombotic thrombocytopenic purpura in genetically susceptible ADAMTS13-deficient mice. J Clin Invest. 2005;115:2752–61.
Acknowledgments
We thank the many clinicians and researchers with whom BL collaborated clinically and scientifically over many years and especially Prof. Miha Furlan, his longtime colleague and friend for almost 30 years. We also thank the TTP research team in Mainz where we intend to set up a prospective acquired TTP cohort study and the Bundesministerium für Bildung und Forschung (BMBF) for supporting our research project at the Center for Thrombosis and Hemostasis, University Medical Center, Mainz, Germany.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Lämmle, B., von Auer, C. (2015). History of Thrombotic Thrombocytopenic Purpura and the von Willebrand Factor–Cleaving Protease, ADAMTS13. In: Rodgers, G. (eds) ADAMTS13. Springer, Cham. https://doi.org/10.1007/978-3-319-08717-7_1
Download citation
DOI: https://doi.org/10.1007/978-3-319-08717-7_1
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-08716-0
Online ISBN: 978-3-319-08717-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)