Abstract
Epigenetic mechanisms play a key role in regulating gene expression. One of the best-studied epigenetic modifications is DNA methylation at cytosine residues of CpG dinucleotides in gene promoters, transposons and imprinting control regions (ICR). Genomic imprinting refers to the epigenetic marking of genes that results in monoallelic expression, depending on their parental origin. Several hormone genes involved in embryonic and fetal growth are imprinted. There are two critical time periods in epigenetic reprogramming: gametogenesis and early preimplantation development. Major reprogramming takes place in primordial germ cells in which parental imprints are erased and totipotency is restored. Imprint marks are then re-established during spermatogenesis or oogenesis, depending on sex. Upon fertilization, there is genome-wide demethylation followed by a wave of de novo methylation, both of which are resisted by imprinted loci. Disruption of imprinting causes disorders involving growth defects, such as the Beckwith-Wiedemann overgrowth syndrome (BWS) and Silver-Russell syndrome (SRS) with the opposite phenotype, involving intrauterine and postnatal growth retardation. These growth disorders are caused, in most cases, by abnormal DNA methylation at the 11p15 imprinted region that contains many imprinted genes, including Insulin-like Growth Factor 2 (IGF2). Loss of methylation (LOM) on the maternal allele at the centromeric ICR2/KCNQ1OT1 region or gain of methylation (GOM) on the maternal allele at the telomeric ICR1/IGF2/H19 region has been shown in BWS. This latter defect is associated with a higher risk of pediatric tumors, such as nephroblastoma. By contrast, LOM on the paternal allele at the telomeric ICR1 is observed in SRS. There is an abnormally high prevalence of conceptions by assisted reproductive technology (ART) among patients with BWS and SRS, suggesting that ART may favor imprinting alterations at the imprinted centromeric 11p15 locus (LOM at the maternally methylated ICR2 or LOM at the paternally methylated ICR1, respectively). The underlying cause of these imprinting defects (following ART or occurring spontaneously) remains unclear. However, recent data indicate that, in patients with BWS or SRS, including those born following ART for BWS, the methylation defect involves imprinted loci other than 11p15. Moreover, some patients exhibit LOM at both maternally and paternally methylated ICR, which suggests that unfaithful maintenance of DNA methylation marks following fertilization involves the dysregulation of a trans-acting regulatory factor.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Assisted Reproductive Technology
- Imprint Gene
- Imprint Control Region
- Imprint Locus
- Transient Neonatal Diabetes Mellitus
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
The genetic code has been known for decades; in contrast, epigenetic mechanisms controlling gene expression were discovered within the last 30 years. Epigenetic mechanisms are involved in many physiological processes, including during development. Genomic imprinting (also called parental imprinting) refers to the epigenetic marking of genes, resulting in monoallelic expression depending on the parental origin. Several human syndromes are associated with the failure of maintenance and/or establishment of genomic imprinting (Azzi et al. 2013). The fetal overgrowth syndrome, Beckwith-Wiedemann syndrome (BWS), and the intrauterine and postnatal growth retardation syndrome, Silver-Russell syndrome (SRS), are both due to imprinting defects. Here, we review clinical aspects of BWS and SRS, including the relationships between phenotype and (epi)/genotype. We also describe epigenetic and genetic anomalies leading to the imprinting defects (isolated locus or multilocus) involved in these developmental diseases, and we consider the potential role of environmental factors such as assisted reproductive technology (ART) in the occurrence of imprinting defects.
Epigenetics and Genomic Imprinting
Epigenetic modifications of the genome play important roles in the regulation of gene expression in diverse cell lineages. Epigenetic marks are various changes to the chromatin but do not include changes in the nucleotide sequence of the DNA (genetic code). Epigenetic marks are dynamically reprogrammed but, once established, they are stably transmitted to daughter cells during mitosis. Epigenetic modifications regulate the expression of genes and confer cell lineage specificity. The nucleosome is the basic unit of chromatin organization and consists of an octamer of histone proteins around which wraps the strand of DNA (Fig. 1). The best-known epigenetic marks are DNA methylation at CpG islands (DNA domains rich in CG dinucleotides) and various post-translational modifications (notably acetylation and methylation) of histones H3 and H4. In any particular region of chromatin, a combination of post-translational modifications of histones (histone code) and the DNA status (methylated/unmethylated) induces either compaction of the chromatin (repressive form) or decondensation of the chromatin (active form; Reik et al. 2001).
Parental imprinting. These two alleles have different epigenetic modifications (methylation, acetylation) according to their parental origin, resulting in expression or non-expression of a gene. DNA methylation and repressive histone marks (such as H3K9me1 or me3, H3K27me1 and me3, and H4K20me3) are associated with the absence of transcription. Conversely, unmethylated DNA and permissive histone marks (H3K9 ac, H4K20me1, H3K4me1 or me2) are associated with transcription activity
In general, DNA methylation is associated with histone deacetylation in regions where chromatin is compacted and thus gene expression is prevented. However, when the DNA is demethylated and histones acetylated, chromatin is in an open conformation. Thus, two loci can be identical in nucleotide sequence (genetic code) but, due to genomic imprinting, they can be functionally different. Expression is monoallelic: one of the two parental alleles is expressed and the other is silent. The two alleles have different epigenetic modifications (DNA methylation and post-translational histone modifications: including methylation and/or acetylation) according to their parental origin, resulting in the expression or non-expression of a gene (Fig. 1). Parental imprinting was identified in mammals in the 1980s through nuclear transfer experiments that demonstrated the non-equivalence of the two parental genomes: zygotes generated with two maternal genomes (gynogenotes) led to embryo development but no development of the embryonic annexes, whereas the zygotes generated with two paternal genomes (androgenotes) developed embryonic annexes but failed to develop an embryo. These experiments showed the importance of the contribution of both parental genomes to achieve normal development and suggested that some genes are expressed from only the paternal or the maternal allele (McGrath and Solter 1984).
These genes were called imprinted genes. One of the first imprinted genes to be identified by gene inactivation (“knockout”) in mice was Igf-2 (DeChiara et al. 1991).
Mice heterozygous for a deletion of the Igf2 gene exhibited growth retardation at birth only if the deletion had been paternally transmitted; growth was normal if the deleted gene was inherited from the mother. The phenotype of mice homozygous for the mutation was not more severe than that of heterozygous mice carrying the mutation on the paternal allele.
The vast majority of genes are expressed by the two parental alleles, and less than 1 % of genes are subject to parental imprinting. There is dynamic reprogramming of genomic imprinting during development: imprinting marks are first erased in primordial germ cells and thereafter re-established differently depending on the sex of the individual during gamete maturation (Lucifero et al. 2002). After fertilization during the preimplantation period, these epigenetic marks are protected against a wave of demethylation and then a wave of global genome de novo remethylation (Santos and Dean 2004).
Several chromosomal regions have now been identified as being imprinted in several mammalian species. Imprinted genes are organized into clusters throughout the genome and many are regulated by a regulatory element called the imprinting center region (ICR).
Several transacting factors involved in the regulation of DNA methylation and imprinting have been identified. DNA methyltransferases (DNMT; Cheng and Blumenthal 2008) and Methyl CpG Binding Domain proteins (MBDs; Klose and Bird 2006) are well-known regulatory factors of DNA methylation. There are also many other regulatory proteins involved in the regulation of DNA methylation and imprinting and in the regulation of the modifications of histone tails by histone acetyltransferases or deacetylases and by histone methylases or demethylases. All these epigenetic changes affect chromatin structure and are thus determinant for the control of gene expression of the cluster.
There are two main regulatory pathways that govern the monoallelic expression of imprinted genes in a cluster: the “chromatin insulator or boundary” mechanism and the long non-coding RNA mechanism (Ideraabdullah et al. 2008; Wan and Bartolomei 2008).
Fetal Development, Imprinting and the 11p15 Region
The imprinted 11p15 region is organized into two domains: a telomeric domain including the IGF2 and H19 genes and a centromeric domain including the CDKN1C (cyclin-dependent kinase inhibitor 1C), KCNQ1 (potassium voltage-gated channel, subfamily Q, member 1) and KCNQ1OT1 (KCNQ1-overlapping transcript 1) genes. Each domain is controlled by its own ICR: ICR1, for the telomeric domain, controls the allele-specific expression of IGF2 and H19; and ICR2, for the centromeric domain, controls the allele-specific expression of KCNQ1OT1, KCNQ1 and CDKN1C (Fig. 2).
The two imprinted domains of the 11p15 region. The reciprocal imprinting of the maternally (M) expressed H19 and the paternally (P) expressed IGF-2 genes depends on the differentially methylated ICR1 upstream from the H19 gene, which acts as an insulator. CTCF binds to the maternal unmethylated ICR1 and prevents the IGF-2 gene promoter from interacting with enhancers downstream from the H19 gene, resulting in transcriptional silencing of the maternal IGF-2 allele (Bell and Felsenfeld 2000; Hark et al. 2000). On the paternal allele, ICR1 is methylated, preventing CTCF binding and thereby leading to IGF-2 transcription on the paternal allele. The centromeric ICR2 domain functions as a silencer by producing a non-coding RNA (antisense KCNQ1OT1 RNA), which results in paternal silencing of the genes in this domain. The KCNQ1OT1 RNA is probably involved in targeting repressive histone modifications to the flanking genes (Lewis et al. 2004; Umlauf et al. 2004; Monk et al. 2006). Paternally expressed genes are represented as blue boxes, maternally expressed genes as orange boxes, and non-expressed genes as gray boxes
Reciprocal imprinting of the H19 gene (the gene for a maternally expressed noncoding RNA) expressed by the maternal allele (M) and of the IGF2 gene expressed by the paternal allele (P) depends on the differentially methylated ICR1 (upstream from the H19 gene), which acts as an insulator. CTCF binds to the unmethylated maternal ICR1 and prevents IGF2 promoters from interacting with the shared enhancers downstream from the H19 gene, thereby abolishing IGF2 expression. In contrast, on the paternal allele, ICR1 is methylated, which prevents the binding of CTCF, thus leading to the transcription of the paternal IGF2 gene. The centromeric domain ICR2 acts as a “silencer” by producing a long non-coding RNA (KCNQ1OT1) from the unmethylated paternal allele. KCNQ1OT1 in turn silences the neighboring paternal genes of the centromeric domain, in cis, including the CDKN1C gene (Edwards and Ferguson-Smith 2007; Ideraabdullah et al. 2008; Wan and Bartolomei 2008).
This imprinted 11p15 region is extremely important during fetal growth and development.
Indeed, the BWS overgrowth syndrome results from various molecular or chromosomal abnormalities at 11p15 that cause overexpression of the paternally expressed genes or underexpression of the maternally expressed genes (Gaston et al. 2001; Gicquel et al. 2005b; Weksberg et al. 2005). SRS, a fetal growth restriction, is mainly due to an imprinting anomaly affecting the paternal ICR1.
Most known 11p15 defects display a mosaic pattern, where the ratio between cells with defects and normal cells differs between tissues (including kidney, muscle, liver, leucocytes and fibroblasts) and patients; this is probably a main cause of the variability of the BWS and SRS phenotypes.
A particular tissue, the placenta, exhibits some imprinting differences as compared to the tissues of the embryo. The placenta in eutherian mammals is a distinct organ ensuring maternal-fetal nutrient allocation and is, consequently, crucial for fetal growth. Thus, the effectiveness with which the placenta transfers nutrients to the fetus is a determinant of fetal growth. Imprinted genes play an important role in placental development (Coan et al. 2005; Frost and Moore 2010). This was first demonstrated by parthenogenesis experiments that provided evidence for the necessity for both paternal and maternal genomes for correct development of both embryo and annexes (Barton et al. 1984; McGrath and Solter 1984; Surani et al. 1984). A subset of genes is imprinted only in the placenta and some imprinted genes are expressed exclusively in the placenta (Gutierrez-Marcos et al. 2012; Lefebvre 2012). The inactivation of the maternally expressed Cdkn1c, in mice, results in a large placenta weighing 140 % of the normal weight (Takahashi et al. 2000). The inactivation of any of the paternally expressed Igf2, Peg3 and Peg1 genes results in a small placenta (Reik et al. 2003). Igf2 is particularly interesting because it has a variant, Igf2 P0, expressed specifically in the mouse labyrinthine trophoblast (Constância et al. 2002). Inactivation of this variant is associated with reduced expression of Igf2 in the placenta, whereas its expression in the fetus is normal. The placental weight and passive transport of nutrients in Igf2 P0 −/− mice were both lower than those in controls. These experimental models have highlighted the important role of imprinted genes in the control of placental development and function (Coan et al. 2005; Angiolini et al. 2006; Frost and Moore 2010; Fowden et al. 2011; Nelissen et al. 2011; Gutierrez-Marcos et al. 2012).
The placenta is the mediator between the mother and the fetus; it is sensitive to its environment and can adapt its capacity in response to environmental variations to ensure an appropriate nutrient supply to the fetus. This characteristic has been extensively documented by caloric restriction studies in animals, and also in humans (Sibley et al. 2010; Sandovici et al. 2012; Wu et al. 2012). Indeed, most of these studies show that placental development and function are compromised by caloric restriction (Heasman et al. 1998; Fowden et al. 2008), which may also affect DNA methylation of imprinted genes (Lumey 1998; Heijmans et al. 2008).
All these various observations and findings highlight the importance of imprinted genes in the regulation of feto-placental development.
Fetal Growth Disorders and Imprinting Defects: Clinical Aspects
In humans, two syndromes in particular, with opposite and severe fetal growth anomalies, have been associated with dysregulation of imprinted gene expression: BWS and SRS.
BWS
BWS is an overgrowth disorder involving developmental abnormalities and an increased risk of childhood tumors. It has an estimated population incidence of 1 in 13,700 (Thorburn et al. 1970), but this is probably an underestimate because of the existence of mild phenotypes that may not be detected or reported (Sotelo-Avila et al. 1950; Schneid et al. 1993).
Its phenotypic expression is indeed variable and diagnosis is still based on clinical signs, although there is no consensus on the clinical definition of the syndrome (Wiedemann 1969; Pettenati et al. 1986; Elliott et al. 1994; DeBaun and Tucker 1998; Weksberg et al. 2001). It is generally accepted that the diagnosis of BWS requires at least three clinical findings, including at least two major findings: the major clinical criteria are macroglossia, macrosomia, abdominal wall defects (exomphalos, umbilical hernia) and selective visceromegaly (involving kidneys, liver or spleen). Less frequent and minor clinical findings are neonatal hypoglycemia, anterior ear lobe creases and/or posterior helical pits, facial nevus flammeus, hemihyperplasia and polyhydramnios. Diverse molecular defects within the 11p15 region are associated with BWS; it can be the result of various molecular or chromosomal alterations that cause overexpression of paternally expressed genes or impair the expression of maternally expressed genes (Gaston et al. 2001; Gicquel et al. 2005b; Weksberg et al. 2005).
More powerful techniques for the molecular diagnosis of BWS are now available and can confirm the diagnosis in patients with incomplete phenotypes, which suggests that BWS should now be defined molecularly. About 7.5–10 % of BWS patients develop a tumor before the age of 5 years. However, it is now clear that this risk differs very substantially depending on the molecular defect involved (Bliek et al. 2004; Cooper et al. 2005; Rump et al. 2005; Brioude et al. 2013a; Eggermann et al. 2013) (see section “Genotype-Phenotype Relationships”).
SRS
SRS is a clinically heterogeneous syndrome involving severe pre- and postnatal growth retardation. It was first described by Silver et al. (1953) and Russell (Russell and Jackson 1954). Their common findings were short stature without catch-up growth, normal head circumference for age, distinctive triangular face morphology with prominent forehead, low-set ears, clinodactyly of the fifth fingers, and skeletal asymmetry. The clinical presentation of SRS covers a spectrum of manifestations such that it is fairly easy to recognize in extreme cases but can be difficult to diagnose in less severely affected individuals, especially if there is no body asymmetry. Based on reviews of the published data, we and others have proposed a clinical scoring system to overcome these difficulties (Price et al. 1999; Netchine et al. 2007; Abu-Amero et al. 2010; Wakeling et al. 2010). For a diagnosis of SRS under these systems, the patient must be born small for gestational age (SGA: birth weight and/or length ≤−2 SDS for gestational age) and also present at least three of the five following features: postnatal growth retardation (at 2 years of age or at the nearest measure available), relative macrocephaly [arbitrarily defined as a head circumference at birth at least 1.5 SDS above that expected for the birth weight and/or length SDS according to Usher and McLean charts (Usher and McLean 1969)], body asymmetry, prominent forehead and feeding difficulties during early childhood and/or postnatal Body Mass Index (BMI) below −2 SDS (at 2 years of age or at the nearest measure available; Netchine et al. 2007).
Molecular Aspects of BWS and SRS
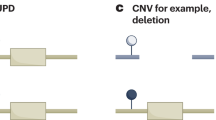
Imprinting disorders may arise in several ways: through copy-number changes for imprinted domains, uniparental isodisomy, disruption of regulatory sequences, and mutation of the active allele or “primary” imprinting defects such as gain or loss of DNA methylation. In BWS, various cytogenetic, genetic and epigenetic defects in 11p15 result in the down-regulation of maternally expressed genes and/or the up-regulation of paternally expressed genes; conversely, in SRS, genetic or epigenetic defects in the 11p15 region result in the down-regulation of paternally expressed genes and/or the up-regulation of maternally expressed genes.
Genetic Defects
Duplications in BWS and SRS Patients
Approximately ten unbalanced translocations involving both imprinted 11p15 domains have been described. Duplications of the whole 11p15 domain (both ICR1 and ICR2) resulting from unbalanced translocations cause an SRS or fetal growth retardation phenotype if they involve the maternal allele and a BWS or overgrowth phenotype if they involve the paternal allele (review in Bliek et al. 2009a; Demars et al. 2011a; Azzi et al. 2013; Soejima and Higashimoto 2013; Table 1).
Cis-duplications confined to one of the two domains are rare and until recently the picture was relatively clear. Cis-duplications involving the whole ICR1 IGF2/H19 domain always result in BWS if the paternal chromosome is involved with no phenotype if the maternal chromosome is involved (Russo et al. 2006; Algar et al. 2007; Bliek et al. 2009a; Demars et al. 2011b; Table 1). On the other hand, cis-duplications involving the whole ICR2 KCNQ1/CDKN1C domain result in SRS if the maternal chromosome is involved with no phenotype if the paternal chromosome is involved (Schönherr et al. 2007; Bonaldi et al. 2011; Table 1). Cis-duplications involving only part of one of the two imprinted domains have recently been described in SRS and BWS cases (Chiesa et al. 2011; Demars et al. 2011b) and provide interesting information on how imprinting control mechanisms normally work and how they can be altered in human imprinting disorders. A cis-duplication involving only part of the ICR1 IGF2/H19 domain (the imprinting control region and the H19 gene) results in a SRS phenotype only if maternally inherited, whereas there is no phenotype upon paternal transmission (Demars et al. 2011b; Table 1). Both the parental transmission pattern and the phenotype in these cases differ from previously reported ICR1 duplications (Russo et al. 2006; Algar et al. 2007; Bliek et al. 2009a; Demars et al. 2011b; Beygo et al. 2013). Hence, a partial maternal cis-duplication of the IGF2/H19 domain results in a SRS phenotype whereas a maternal cis-duplication involving the whole IGF2/H19 domain does not result in any phenotype (Table 1). Two copies of the active maternal H19 gene are expressed in both cases but, in the partial cis-duplication, one maternal H19 gene is not engaged in a cis-effect. We (Demars et al. 2011b) and others (Chiesa et al. 2011; De Crescenzo et al. 2013) have also described partial cis-duplications of the ICR2 KCNQ1/CDKN1C domain; they result in a BWS phenotype only if maternally inherited whereas there is no phenotype upon paternal transmission (Table 1). One of these partial cis-duplications (Demars et al. 2011b) does not involve ICR2 but involves a region displaying CTCF- and cohesin-binding sites, suggesting that cis-regulatory elements other than ICR2 contribute to the establishment/maintenance of imprinting.
Uniparental 11p15 Isodisomy
Uniparental isodisomy (UPiD) is the presence of two copies of the same parental chromosome and results in unbalanced expression of imprinted genes. Paternal isodisomy (patUPiD) of the 11p15 region is a common cause of BWS and is present in 20–25 % of BWS cases (reviewed in Demars et al. 2011a; Azzi et al. 2013; Brioude et al. 2013a).
We recently showed that SNP array analysis is a powerful diagnostic technique for BWS. Such arrays can be used to distinguish patUPiDs from trisomies more precisely than karyotyping and FISH, and they help to determine the size and mosaicism rate of patUPiDs even in cases of low-rate patUPiD mosaicism (Keren et al. 2013).
Maternal isodisomy has been reported in only one SRS case (Bullman et al. 2008). UPiD is the consequence of a postzygotic event due to mitotic recombination in early embryogenesis and therefore results in mosaicism. Postzygotic mitotic recombination produces a mixed population composed of normal cells and cells with maternal UPiD or paternal UPiD. Maternal UPiD is rare, suggesting that cells with paternal UPiD have a selective growth advantage.
The extent of isodisomy along chromosome 11 is variable. It can extend to the long arm (10 % of cases) and always involves the two imprinted 11p15 domains (Cooper et al. 2007; Romanelli et al. 2011). Segmental UPiDs confined to the IGF2/H19 or to the KCNQ1OT1/CDKN1C domains do not account for DNA methylation defects restricted to one of the two imprinted 11p15 domains (Demars et al. 2011b).
UPD of Chromosome 7
The molecular cause of SRS has long been unknown (Azzi et al. 2013). Several chromosomal abnormalities were reported to be associated with SRS or SRS-like phenotypes (Hitchins et al. 2001b) but the most relevant abnormality found in a significant number of patients (5–10 % of cases) was UPD of chromosome 7 (mUPD7; Preece 2002). This cytogenetic anomaly implicates imprinted genes on chromosome 7 in the SRS phenotype. Indeed, at least two imprinted domains, located at 7p11.1-p14 and 7q31, have been identified within chromosome 7. These regions harbor at least two imprinted genes involved in the control of growth: the maternally expressed growth factor receptor-binding protein 10 (GRB10 at 7p11.1-p14) and paternally expressed gene 1/mesodermal expressed transcript (PEG1/MEST at 7q31). Because a number of SRS patients with duplications (or inversions) or segmental UPD have been reported (Joyce et al. 1999; Monk et al. 2000; Hannula et al. 2001), these two regions have been the focus of research to identify causative mutations or epimutations. However, screening SRS patients without mUPD7 failed to identify either mutations of GRB10 or PEG1/MEST or epimutations in their DMRs (Riesewijk et al. 1998; Yoshihashi et al. 2000; Hannula et al. 2001; Hitchins et al. 2001a; Kobayashi et al. 2001; McCann et al. 2001; Arnaud et al. 2003). Recently, Kagami and coworkers reported hypermethylation of the PEG1/MEST DMR in a girl with the SRS phenotype born after in vitro fertilization (Kagami et al. 2007); subsequently, Eggermann et al. reported a SRS boy carrying a de novo deletion of 3.7 Mb of the paternal allele on 7q32 causing the loss of 53 genes, including PEG1/MEST (Eggermann et al. 2012). These observations, despite providing evidence of the involvement of imprinted genes in these regions, do not incriminate a particular gene as being causative of SRS.
CDKN1C Mutations
Inactivating mutations in the CDKN1C gene (also known as p57 KIP2), which encodes a maternally expressed cell-cycle inhibitor, are found in approximately 5 % of BWS patients (Choufani et al. 2010) and account for approximately half of familial BWS cases. Mice lacking the imprinted Cdk inhibitor p57 (kip2) show altered cell proliferation and differentiation, leading to abdominal muscle defects and many of the phenotypes seen in patients with BWS (Zhang et al. 1997; Tunster et al. 2011).
Although Cdkn1c transgenic mice display a SRS phenotype (Andrews et al. 2007), no CDKN1C mutations had been found associated with SRS until recently (Obermann et al. 2004). Indeed, maternally transmitted activating mutations of CDKN1C were recently described in cases of the IMAGe syndrome, which shares some phenotypes with SRS, such as fetal growth retardation and facial dysmorphia (Arboleda et al. 2012; Table 1). Then, very recently, an activating mutation was found in a familial case of SRS (Brioude et al. 2013b).
Epigenetic Defects
Isolated DNA Methylation Defects
A large subgroup of BWS and SRS patients displays no obvious genetic defects in a cis-regulatory element or a transacting factor; these cases are identified as ICR1 or ICR2 “primary” DNA methylation defects. However, the prevalence of secondary DNA methylation defects might be underestimated because there is generally no search for mutations in cis-regulatory elements or transacting factors for routine diagnosis of BWS or SRS.
DNA Methylation Defects at ICR2 Result in a BWS Phenotype
Approximately 60 % of BWS patients display ICR2 loss of methylation. In rare cases, the loss of methylation is caused by a deletion involving ICR2 on the maternal allele (Niemitz et al. 2004; Zollino et al. 2010; Algar et al. 2011; Demars et al. 2011a; Azzi et al. 2013; De Crescenzo et al. 2013). At least 25 % of BWS patients with loss of methylation at ICR2 also display loss of methylation at imprinted loci other than 11p15 (see section on “The Multilocus Hypomethylation Disorder”), and this pattern defines the multilocus hypomethylation disorder (MHD). Abnormal methylation of ICR2 DNA (i.e., gain of methylation) has never been identified in SRS patients (Gicquel et al. 2005a; Eggermann et al. 2006; Netchine et al. 2007; Penaherrera et al. 2010).
DNA Methylation Defects at ICR1 Result in Both BWS and SRS Phenotypes
A gain of methylation at ICR1 is found in 10 % of BWS patients and results in biallelic expression of the IGF2 gene. Conversely, a loss of methylation at ICR1 is observed in 50–60 % of SRS patients and results in loss of expression of the IGF2 gene (Gicquel et al. 2005a; Netchine et al. 2007; Azzi et al. 2013). The gain of methylation in BWS is strictly localized at ICR1 and does not involve other imprinted loci (Bliek et al. 2006; Azzi et al. 2009). The situation is different in SRS, with at least 10–17 % of SRS patients displaying loss of DNA methylation at imprinted loci other than 11p15 (Azzi et al. 2009, 2013; Turner et al. 2010; Court et al. 2013; Poole et al. 2013; see section on “The Multilocus Hypomethylation Disorder”).
Dysregulation of the Histone Code in BWS and SRS
Although histone marks are determinant for the regulation of 11p15 genomic imprinting (Henckel et al. 2009), their role in the pathogenesis of BWS and SRS and their link to DNA methylation defects have not been extensively addressed. Very recently, Nativio et al. (2011) showed that trimethylated Lysine 9 of histone H3 and trimethylated Lysine 20 of histone H4 (H3K9me3 and H4K20me3), both repressive histone marks, are associated with the methylated paternal ICR1 allele. In addition, dimethylated Lysine 4 of histone H3 and acetylated Lysine 9 of histone H3 (H3K4me2, H3K9ac), both permissive histone marks, are associated with the non-methylated maternal ICR1 allele. In BWS and SRS patients, the asymmetric distribution of these epigenetic marks is lost: H3K9me3 and H4K20me3 are biallelic in BWS, and H3K4me2 and H3K9ac are biallelic in SRS.
Mechanisms of Imprinting Dysregulation
Genomic imprinting is a multistep process and some specific stages, such as imprint establishment in germ cells or imprint maintenance after fertilization, are critical in the regulation of genomic imprinting. Deregulation of genomic imprinting during one of those stages will result in imprinting disorders.
Evidence for Secondary Imprinting Defects in BWS and SRS
The Prevalence of Mutations in Cis-Regulatory Elements is Probably Underestimated
Investigation of BWS and SRS patients relies mostly on diagnostic techniques, such as MLPA, which identify copy number variants in the kb range but do not recognize small deletions or mutations involving transacting factor-binding sites. The main function of the CTCF protein at ICR1 is to maintain the unmethylated state of the maternal allele. It has therefore been suggested that the loss of some CTCF-binding sites impairs protection by CTCF and results in gain of methylation on the maternal allele. Maternally inherited deletions of between two and six CTCF-binding sites have been identified in several BWS cases (Sparago et al. 2004, 2007; Prawitt et al. 2005; Scott et al. 2008; Demars et al. 2010, 2011b; Beygo et al. 2013) but no such deletions have been found in SRS cases (Bliek et al. 2006; Yamazawa et al. 2008b; Bartholdi et al. 2009; Bruce et al. 2010; Demars et al. 2010). No mutation of CTCF-binding sites has been in BWS (Sparago et al. 2007; Demars et al. 2010) or SRS (Bliek et al. 2006; Yamazawa et al. 2008a; Bruce et al. 2009; Demars et al. 2010).
Novel transacting factors have recently been identified, and there is emerging evidence that CTCF function is modulated by neighboring DNA-binding factors (Weth and Renkawitz 2011). These factors include pluripotency factors that may be involved in the regulation of genomic imprinting. Mutations and small deletions of OCT4- and SOX2-binding sites have been described within ICR1 in BWS patients and are associated with gain of ICR1 methylation (Table 1). In all cases, the BWS phenotype segregated with transmission of the mutation through the female germline, with no phenotype showing paternal transmission (Demars et al. 2010; Poole and Leith 2012; Berland et al. 2013). These observations suggest that loss of binding of pluripotency factors at ICR1 impairs the maintenance of the unmethylated state of the maternal ICR1. Possibly, OCT4 and SOX2 protect the maternal allele from gain of DNA methylation, especially at CTCF-binding sites (Hori et al. 2002). A recent YAC transgenic mouse model confirmed that these OCT4-binding sites are indeed required both for protection of the maternal ICR1 against DNA methylation and during the maintenance stage of the imprinting cycle (Hori et al. 2012; Sakaguchi et al. 2013). This model also suggests that CTCF and OCT4/SOX2 act cooperatively (Sakaguchi et al. 2013). OCT4- and SOX2-binding sites have also been identified at the Angelman imprinting center (Kaufman et al. 2009). The mechanism of action of pluripotency factors is not clear, but OCT4 interacts with CTCF when regulating the X chromosome inactivation process (Donohoe et al. 2009). Very recently, a novel function was attributed to OCT4: negative regulation of chromatin loop formation mediated by cohesin at CTCF-binding sites (Kim et al. 2011). Whether mutations of pluripotency factor-binding sites are also involved at ICR2 is yet to be determined. It is also plausible that mutations/deletions of other transacting factor-binding sites are involved in the pathogenesis of 11p15 imprinting disorders, and this possibility should be further investigated. However, all binding sites for ZFP57 in ICR1 overlap with CTCF-binding sites; such sites have been investigated in cases of SRS and BWS and no mutation has been found (Demars et al. 2010).
Genetic Variants in Cis-Regulatory Elements may Play a Role in Susceptibility to 11p15 Imprinting Disorders
Recent studies clearly show that genetic variants in cis account for allele-specific differences in DNA methylation status (reviewed in Tycko 2010), chromatin status (McDaniell et al. 2010) or transcription factor binding (Kasowski et al. 2010; McDaniell et al. 2010), which result in differences in allele-specific expression. The significance of the parental origin of alleles is also emerging in genetic studies and may be particularly relevant to imprinting disorders. Relatively little research has addressed the nature and effects of allelic diversity at imprinted loci. Zogel et al. (2006) identified preferential maternal transmission of one specific haplotype of the 15q11-13 ICR in a subgroup of Angelman patients with primary imprinting defects. Interestingly, within this haplotype, a polymorphism affects a SOX2-binding site (Kaufman et al. 2009). It would therefore be interesting to determine whether genetic variability in imprinted regions, by affecting the binding of regulatory factors at play in the establishment and/or the maintenance of 11p15 genomic imprinting, has a role in imprinting disorders.
The Multilocus Hypomethylation Disorder Indicates Abnormal Expression of a Transacting Regulatory Factor
The involvement of transacting factors in the pathogenesis of imprinting disorders was first suggested in 2006: we and others showed that a subset of BWS and transient neonatal diabetes mellitus (TNDM) patients displayed a loss of DNA methylation at loci other than the causal locus (i.e., ICR2 and ZAC1, respectively; Mackay et al. 2006; Rossignol et al. 2006). This finding has since been confirmed by other studies in BWS (Bliek et al. 2006; Azzi et al. 2009; Lim et al. 2009; Meyer et al. 2009; Court et al. 2013; Poole et al. 2013), SRS (Bliek et al. 2006; Azzi et al. 2009; Turner et al. 2010; Kannenberg et al. 2012; Court et al. 2013; Poole et al. 2013), TNDM (Mackay et al. 2006; Court et al. 2013) and pseudohypoparathyroidism 1B (PHP1B) (Perez-Nanclares et al. 2012; Court et al. 2013; Maupetit-Mehouas et al. 2013), but not in Prader-Willi or Angelman syndromes (Court et al. 2013; Table 2). This finding defines a new entity of imprinting disorders, now called the multilocus hypomethylation disorder (MHD). Multilocus imprinting disorder (MID) is not restricted to multilocus hypomethylation and, indeed, both hypo and hypermethylation at numerous imprinted genes may coexist in the same SRS (Kannenberg et al. 2012) or PHP1B (Maupetit-Mehouas et al. 2013) patient. This observation adds an additional layer of complexity to the issue of imprinting regulation and MID occurrence. MID displays mosaicism and involves both maternally and paternally imprinted ICRs, except in TNDM where only maternal loci are affected (Table 2).
Although MID is relatively frequent, mutation analyses of recently identified transacting regulatory factors, including ZFP57, TRIM28 (KAP1), NLRP2, NLRP7 and C6ORF221, are rare. ZFP57 mutations (a maternal-effect gene involved in both the establishment and maintenance of imprints) have only been identified in cases of TNDM with MHD (Mackay et al. 2008; Court et al. 2013), and a NLRP2 (member of the NLRP family of CATERPILLER proteins) mutation has been identified in a case of BWS with MHD (Meyer et al. 2009; Table 2).
Another interesting concept that emerged recently is the imprinted gene network: groups of imprinted genes can be co-regulated as parts of networks. For example, ICR1 at 11p15 interacts physically with several chromosomal regions as part of an epigenetically regulated network operating both intra- and interchromosomally (Varrault et al. 2006; Gabory et al. 2009). The existence of this network suggests that a defect of one imprinted locus might induce perturbation at other imprinted loci. Further work is needed to assess the contribution, if any, of imprinted gene networks to the pathogenesis of MHD/MID.
Genotype-Phenotype Relationships
BWS
Various molecular and chromosomal alterations can lead to BWS (Gaston et al. 2001; Gicquel et al. 2005b; Weksberg et al. 2005; Demars et al. 2011a); only about 25 % of cases are caused by genetic defects. UPids of paternal origin (patUPiD, 20 % of cases) are segmental and always include the 11p15 region but the proximal breakpoints are diverse (Nyström et al. 1992; Henry et al. 1993; Cooper et al. 2007; Romanelli et al. 2011). Genetic mutations on the maternal allele of CDKN1C account only for 5 % of cases overall but are found in more than 70 % of familial cases. The most frequent mechanism is clearly epigenetic (70 % of cases): LOM at ICR2 explains more than half BWS cases (50–60 %) whereas GOM at ICR1 is less common (10 % of cases). PatUPiD and both epigenetic defects always display variable mosaicism, presumably explaining the substantial variability of the phenotype. Some of the phenotypic features of BWS can be directly correlated to particular molecular alterations (Gaston et al. 2001; Cooper et al. 2005; Weksberg et al. 2005; Brioude et al. 2013a; Table 3). Hemihyperplasia is more frequent in patients with patUPiD11p15, whereas the abdominal wall defect is strongly associated with abnormalities mapping in the centromeric domain. Moreover, exomphalos are almost constant in CDKN1C mutations. An important finding is that tumor risk differs substantially between molecular subtypes. The tumor risk is high (around 30 %) in patients with ICR1 GOM who only develop nephroblastoma (Wilms Tumor: WT); around 20 % of patients with patUPD11p15 develop a childhood tumor, especially nephroblastoma, hepatoblastoma and adrenocortical tumor. Fortunately, less than 5 % of patients with ICR2 LOM, the situation for the majority of BWS cases, develop a tumor and no nephroblastoma has yet been reported in these patients. It is also important that physicians be careful with patients with a positive clinical diagnosis of BWS without known molecular anomaly or isolated severe hemihyperplasia or organomegalies, because the risk of WT is high in such cases. These observations and findings can help the physician in the follow-up of patients, as diverse factors need to be considered: the type of transmission (maternal or paternal); the risk of false negative findings due to the variability of the percentage of mosaic abnormality between tissues; and the possibility of a multilocus disorder involving any of the ICR2, SNRPN, ZAC, IGF-2R, DLK1/GTL2 IG-DMR and GNAS loci (Rossignol et al. 2006; Azzi et al. 2009). These findings also allow better genetic counseling for families (Brioude et al. 2013a). Abdominal ultrasound scans every 3 months are recommended for patients with a telomeric defect (ICR1 GOM and patUPiD11p15), associated with regular physical examinations. For patients with a centromeric defect, regular physical examination seems to be sufficient.
Two observations related to BWS suggest that the preimplantation embryo is particularly prone to imprinting errors. First, the incidence of monozygotic twinning in BWS is very much higher than normal, with an unusually high proportion of female monozygotic twins. These twins are always discordant for the BWS phenotype and the only molecular defect is, in all cases, an ICR2 LOM. Weksberg’s group showed that the imprinted defect is found in blood leucocytes of both twins but only in fibroblasts of the affected twin (Weksberg et al. 2002; Gicquel et al. 2005a). This is probably due to the sharing of the blood circulation, which is a common feature of monozygotic twins. Discordance between monozygotic twins may result from a failure of maintenance of methylation during a single cell cycle at or just prior to the twinning event, caused by an error in the nucleocytoplasmic trafficking of a transacting factors involved in the process (Bestor 2003; Weksberg et al. 2005). The X-inactivation process takes place at the same time and presumably involves common factors, and this may explain the female vulnerability. A second line of evidence that preimplantation is a critical period is the large proportion of BWS (DeBaun et al. 2003; Gicquel et al. 2003; Maher et al. 2003; Halliday et al. 2004), SRS (Svensson et al. 2005; Wakeling et al. 2010) and also Angelman syndrome (Ludwig et al. 2005) patients who were conceived by ART. Again, the molecular defect is a LOM at maternally (BWS, AS) or paternally (SRS) imprinted loci, implicating a factor involved in the maintenance of methylation. The underlying cause of this association remains unclear, and no particular procedure or cause of infertility has been found to be specifically associated with these abnormalities.
SRS
Most (over 50 % of) SRS patients display hypomethylation of the telomeric ICR1 domain of the 11p15 region (Gicquel et al. 2005a; Netchine et al. 2007). SRS and BWS mirror each other, both clinically and at the molecular level. In SRS patients, the paternal allele switches to a maternal epigenotype resulting in biallelic expression of H19 and decreased IGF2 expression. In most of these cases, the hypomethylation is partial, reflecting the mosaic distribution of the epimutation and explaining at least in part the variability of the SRS phenotype.
mUPD7, where at least two imprinted domains are located (7p11.1-p14 and 7q31), is present in about 5–10 % of SRS cases (Preece 2002). However, in around 40 % of SRS cases with a typical clinical phenotype, no abnormality is found.
Many SRS patients carrying ICR1 LOM display a more severely abnormal growth phenotype than other SRS patients, and this may be associated with typical dysmorphy (relative macrocephaly, prominent forehead) and the highly evocative body asymmetry. They also more frequently have associated malformations (Netchine et al. 2007; Wakeling et al. 2010; Binder et al. 2011; Ghanim et al. 2013).
The specific features of mUPD7 SRS patients are mild developmental delay, mainly consisting of speech difficulties, predisposition to myoclonus dystonia and a putative susceptibility to developing autism traits (Hitchins et al. 2001b; Guettard et al. 2008; Binder et al. 2011). All these features are thought to be related to disruption of the expression of particular imprinted genes on chromosome 7. However, it should be noted that there is no discontinuity of the phenotypic presentation between these subgroups of patients; similarly, there is variability within subpopulations of patients with the same molecular abnormalities (Bliek et al. 2006; Murphy et al. 2012).
No molecular anomalies have been identified in about 40 % of SRS patients studied, and these cases can therefore be called “idiopathic” SRS. However, this diagnosis should be made only by clinicians with substantial experience of SRS and after various differential diagnoses have been ruled out (notably 3M syndrome, Mullibrey Syndrome, Bloom syndrome and other chromosome breakage susceptibility syndromes, and IGF-1R molecular anomalies). This group of patients is of particular interest because further investigations may identify new molecular etiologies of SRS, and the same follow-up and treatment guidelines used for other SRS patients may also be appropriate for this subgroup.
Conclusion and Outlook
The regulation of gene expression is under the control of the genetic codes but also of epigenetic phenomena. Abnormalities affecting epigenetic, and especially imprinting, mechanisms can result in abnormal gene expression, leading to various developmental pathologies and tumors. The BWS and the SRS syndromes are some of the most characteristic pediatric diseases involving abnormalities of imprinting, in both cases involving the 11p15 region. These human imprinting disorders have helped to identify key cis-regulatory elements in imprinting centers, as well as various transacting regulatory factors. Work on these 11p15 imprinting disorders has focused mainly on DNA methylation. However, other epigenetic marks and factors, such as histone acetylation and methylation, long non-coding RNAs, small RNAs and miRNA, and genetic variations (SNP, CNV involved in chromatin organization) should be explored for their involvement in the pathogenesis of 11p15 imprinting disorders. Genetic analysis with high-throughput techniques should speed the discovery of new factors in cis and trans associated with 11p15 genomic imprinting controls. Finally, it is important to elucidate the role of environmental factors (ART, undernutrition) in the pathogenesis of BWS and SRS.
Progress in these fields should provide new diagnostic and predictive tools, but such tools must be appropriate for these diseases in which there is a high risk of false negative results; the percentage of mosaic abnormalities can differ very substantially between tissues. Progress will also allow improved genetic counseling to be provided to families.
References
Abu-Amero S, Wakeling EL, Preece M, Whittaker J, Stanier P, Moore GE (2010) Epigenetic signatures of Silver-Russell syndrome. J Med Genet 47:150–154
Algar E, Dagar V, Sebaj M, Pachter N (2011) An 11p15 imprinting centre region 2 deletion in a family with Beckwith Wiedemann syndrome provides insights into imprinting control at CDKN1C. PLoS One 6:e29034. doi:10.1371/journal.pone.0029034
Algar EM, St Heaps L, Darmanian A, Dagar V, Prawitt D, Peters GB, Collins F (2007) Paternally inherited submicroscopic duplication at 11p15.5 implicates insulin-like growth factor II in overgrowth and Wilms’ tumorigenesis. Cancer Res 67:2360–2365
Andrews SC, Wood MD, Tunster SJ, Barton SC, Surani MA, John RM (2007) Cdkn1c (p57Kip2) is the major regulator of embryonic growth within its imprinted domain on mouse distal chromosome 7. BMC Dev Biol 7:53
Angiolini E, Fowden A, Coan P, Sandovici I, Smith P, Dean W, Burton G, Tycko B, Reik W, Sibley C, Constância M (2006) Regulation of placental efficiency for nutrient transport by imprinted genes. Placenta 27(Suppl A):S98–S102
Arboleda VA, Lee H, Parnaik R, Fleming A, Banerjee A, Ferraz-de-Souza B, Délot EC, Rodriguez-Fernandez IA, Braslavsky D, Bergadá I, Dell’Angelica EC, Nelson SF, Martinez-Agosto JA, Achermann JC, Vilain E (2012) Mutations in the PCNA-binding domain of CDKN1C cause IMAGe syndrome. Nat Genet 44:788–792
Arnaud P, Monk D, Hitchins M, Gordon E, Dean W, Beechey CV, Peters J, Craigen W, Preece M, Stanier P, Moore GE, Kelsey G (2003) Conserved methylation imprints in the human and mouse GRB10 genes with divergent allelic expression suggests differential reading of the same mark. Hum Mol Genet 12:1005–1019
Azzi S, Rossignol S, Steunou V, Sas T, Thibaud N, Danton F, Le Jule M, Heinrichs C, Cabrol S, Gicquel C, Le Bouc Y (2009) Multilocus methylation analysis in a large cohort of 11p15-related foetal growth disorders (Russell Silver and Beckwith Wiedemann syndromes) reveals simultaneous loss of methylation at paternal and maternal imprinted loci. Hum Mol Genet 18:4724–4733
Azzi S, Rossignol S, Le Bouc Y, Netchine I (2010) Lessons from imprinted multilocus loss of methylation in human syndromes: a step toward understanding the mechanisms underlying these complex diseases. Epigenetics 5:373–377
Azzi S, Brioude F, Le Bouc Y, Netchine I (2013) Human imprinting anomalies in fetal and childhood growth disorders: clinical implications and molecular mechanisms. Curr Pharm Des, 2013 Jul 19. [Epub ahead of print] PMID: 23888961
Bartholdi D, Krajewska-Walasek M, Ounap K, Gaspar H, Chrzanowska KH, Ilyana H, Kayserili H, Lurie IW, Schinzel A, Baumer A (2009) Epigenetic mutations of the imprinted IGF2-H19 domain in Silver-Russell syndrome (SRS): results from a large cohort of patients with SRS and SRS-like phenotypes. J Med Genet 46:192–197
Barton SC, Surani MA, Norris ML (1984) Role of paternal and maternal genomes in mouse development. Nature 311:374–376
Bell AC, Felsenfeld G (2000) Methylation of a CTCF-dependent boundary controls imprinted expression of the Igf2 gene. Nature 405:482–485
Berland S, Appelback M, Bruland O, Beygo J, Buiting K, Mackay DJ, Karen Temple I, Houge G (2013) Evidence for anticipation in Beckwith-Wiedemann syndrome. Eur J Hum Genet 21(12):1344–1348. doi:10.1038/ejhg.2013.71
Bestor TH (2003) Imprinting errors and developmental asymmetry. Philos Trans R Soc Lond B Biol Sci 358(1436):1411–1415
Beygo J, Citro V, Sparago A, De Crescenzo A, Cerrato F, Heitmann M, Rademacher K, Guala A, Enklaar T, Anichini C, Cirillo Silengo M, Graf N, Prawitt D, Cubellis MV, Horsthemke B, Buiting K, Riccio A (2013) The molecular function and clinical phenotype of partial deletions of the IGF2/H19 imprinting control region depends on the spatial arrangement of the remaining CTCF-binding sites. Hum Mol Genet 22:544–557
Binder G, Begemann M, Eggermann T, Kannenberg K (2011) Silver-Russell syndrome. Best Pract Res Clin Endocrinol Metab 25:153–160
Bliek J, Gicquel C, Maas S, Gaston V, Le Bouc Y, Mannens M (2004) Epigenotyping as a tool for the prediction of tumor risk and tumor type in patients with Beckwith-Wiedemann syndrome (BWS). J Pediatr 145:796–799
Bliek J, Terhal P, van den Bogaard MJ, Maas S, Hamel B, Salieb-Beugelaar G, Simon M, Letteboer T, van der Smagt J, Kroes H, Mannens M (2006) Hypomethylation of the H19 gene causes not only Silver-Russell syndrome (SRS) but also isolated asymmetry or an SRS-like phenotype. Am J Hum Genet 78:604–614
Bliek J, Snijder S, Maas SM, Polstra A, van der Lip K, Alders M, Knegt AC, Mannens MM (2009a) Phenotypic discordance upon paternal or maternal transmission of duplications of the 11p15 imprinted regions. Eur J Med Genet 52:404–408
Bliek J, Verde G, Callaway J, Maas SM, De Crescenzo A, Sparago A, Cerrato F, Russo S, Ferraiuolo S, Rinaldi MM, Fischetto R, Lalatta F, Giordano L, Ferrari P, Cubellis MV, Larizza L, Temple IK, Mannens MM, Mackay DJ, Riccio A (2009b) Hypomethylation at multiple maternally methylated imprinted regions including PLAGL1 and GNAS loci in Beckwith-Wiedemann syndrome. Eur J Hum Genet 17:611–619
Bonaldi A, Mazzeu JF, Costa SS, Honjo RS, Bertola DR, Albano LM, Furquim IM, Kim CA, Vianna-Morgante AM (2011) Microduplication of the ICR2 domain at chromosome 11p15 and familial Silver-Russell syndrome. Am J Med Genet A 155A(10):2479–2483
Brioude F, Lacoste A, Netchine I, Vazquez MP, Auber F, Audry G, Gauthier-Villars M, Brugieres L, Gicquel C, Le Bouc Y, Rossignol S.(2013a) Beckwith-Wiedemann syndrome: growth pattern and tumor risk according to molecular mechanism, and guidelines for tumor surveillance. Horm Res Paediatr 80(6):457–465
Brioude F, Oliver-Petit I, Blaise A, Praz F, Rossignol S, Jule ML, Thibaud N, Faussat AM, Tauber M, Bouc YL, Netchine I (2013b) CDKN1C mutation affecting the PCNA binding domain as a cause M of familial Russell Silver Syndrome. J Med Genet 50(12):823–830
Bruce S, Hannula-Jouppi K, Peltonen J, Kere J, Lipsanen-Nyman M (2009) Clinically distinct epigenetic subgroups in Silver-Russell syndrome: the degree of H19 hypomethylation associates with phenotype severity and genital and skeletal anomalies. J Clin Endocrinol Metab 94:579–587
Bruce S, Hannula-Jouppi K, Puoskari M, Fransson I, Simola KO, Lipsanen-Nyman M, Kere J (2010) Submicroscopic genomic alterations in Silver-Russell syndrome and Silver-Russell-like patients. J Med Genet 47:816–822
Bullman H, Lever M, Robinson DO, Mackay DJ, Holder SE, Wakeling EL (2008) Mosaic maternal uniparental disomy of chromosome 11 in a patient with Silver-Russell syndrome. J Med Genet 45:396–399
Cheng X, Blumenthal RM (2008) Mammalian DNA methyltransferases: a structural perspective. Structure 16:341–350
Chiesa N, De Crescenzo A, Mishra K, Perone L, Carella M, Palumbo O, Mussa A, Sparago A, Cerrato F, Russo S, Lapi E, Cubellis MV, Kanduri C, Cirillo Silengo M, Riccio A, Ferrero GB (2011) The KCNQ1OT1 Imprinting Control Region and non-coding RNA: new properties derived from the study of Beckwith-Wiedemann syndrome and Silver-Russell syndrome cases. Hum Mol Genet 21:10–25
Choufani S, Shuman C, Weksberg R (2010) Beckwith-Wiedemann syndrome. Am J Med Genet C Semin Med Genet 154C:343–354
Coan PM, Burton GJ, Ferguson-Smith AC (2005) Imprinted genes in the placenta—a review. Placenta 26(4):S10–S20
Constância M, Hemberger M, Hughes J, Dean W, Ferguson-Smith A, Fundele R, Stewart F, Kelsey G, Fowden A, Sibley C, Reik W (2002) Placental-specific IGF-II is a major modulator of placental and fetal growth. Nature 417:945–948
Cooper WN, Luharia A, Evans GA, Raza H, Haire AC, Grundy R, Bowdin SC, Riccio A, Sebastio G, Bliek J, Schofield PN, Reik W, Macdonald F, Maher ER (2005) Molecular subtypes and phenotypic expression of Beckwith-Wiedemann syndrome. Eur J Hum Genet 13:1025–1032
Cooper WN, Curley R, Macdonald F, Maher ER (2007) Mitotic recombination and uniparental disomy in Beckwith-Wiedemann syndrome. Genomics 89:613–617
Court F, Martin-Trujillo A, Romanelli V, Garin I, Iglesias-Platas I, Salafsky I, Guitart M, Perez de Nanclares G, Lapunzina P, Monk D (2013) Genome-wide allelic methylation analysis reveals disease-specific susceptibility to multiple methylation defects in imprinting syndromes. Hum Mutat 34:595–602
DeBaun MR, Niemitz EL, Feinberg AP (2003) Association of in vitro fertilization with Beckwith-Wiedemann syndrome and epigenetic alterations of LIT1 and H19. Am J Hum Genet 72(1):156–160
DeBaun MR, Tucker MA (1998) Risk of cancer during the first four years of life in children from The Beckwith-Wiedemann Syndrome registry. J Pediatr 132(3 Pt 1):398–400
De Crescenzo A, Coppola F, Falco P, Bernardo I, Ausanio G, Cerrato F, Falco L, Riccio A (2011) A novel microdeletion in the IGF2/H19 imprinting centre region defines a recurrent mutation mechanism in familial Beckwith-Wiedemann syndrome. Eur J Med Genet 54:e451–e454
De Crescenzo A, Sparago A, Cerrato F, Palumbo O, Carella M, Miceli M, Bronshtein M, Riccio A, Yaron Y (2013) Paternal deletion of the 11p15.5 centromeric-imprinting control region is associated with alteration of imprinted gene expression and recurrent severe intrauterine growth restriction. J Med Genet 50:99–103
DeChiara TM, Robertson EJ, Efstratiadis A (1991) Parental imprinting of the mouse insulin-like growth factor II gene. Cell 64:849–859
Demars J, Shmela ME, Rossignol S, Okabe J, Netchine I, Azzi S, Cabrol S, Le Caignec C, David A, Le Bouc Y, El-Osta A, Gicquel C (2010) Analysis of the IGF2/H19 imprinting control region uncovers new genetic defects, including mutations of OCT-binding sequences, in patients with 11p15 fetal growth disorders. Hum Mol Genet 19:803–814
Demars J, Le Bouc Y, El-Osta A, Gicquel C (2011a) Epigenetic and genetic mechanisms of abnormal 11p15 genomic imprinting in Silver-Russell and Beckwith-Wiedemann syndromes. Curr Med Chem 18:1740–1750
Demars J, Rossignol S, Netchine I, Lee KS, Shmela M, Faivre L, Weill J, Odent S, Azzi S, Callier P, Lucas J, Dubourg C, Andrieux J, Le Bouc Y, El-Osta A, Gicquel C (2011b) New insights into the pathogenesis of Beckwith-Wiedemann and Silver-Russell syndromes: contribution of small copy number variations to 11p15 imprinting defects. Hum Mutat 32:1171–1182
Donohoe ME, Silva SS, Pinter SF, Xu N, Lee JT (2009) The pluripotency factor Oct4 interacts with Ctcf and also controls X-chromosome pairing and counting. Nature 460:128–132
Edwards CA, Ferguson-Smith AC (2007) Mechanisms regulating imprinted genes in clusters. Curr Opin Cell Biol 19:281–289
Eggermann T, Schonherr N, Meyer E, Obermann C, Mavany M, Eggermann K, Ranke MB, Wollmann HA (2006) Epigenetic mutations in 11p15 in Silver-Russell syndrome are restricted to the telomeric imprinting domain. J Med Genet 43:615–616
Eggermann T, Spengler S, Begemann M, Binder G, Buiting K, Albrecht B, Spranger S (2012) Deletion of the paternal allele of the imprinted MEST/PEG1 region in a patient with Silver-Russell syndrome features. Clin Genet 81:298–300
Eggermann T, Algar E, Lapunzina P, Mackay D, Maher ER, Mannens M, Netchine I, Prawitt D, Riccio A, Temple IK, Weksberg R (2013) Clinical utility gene card for: Beckwith-Wiedemann syndrome. Eur J Hum Genet. doi:10.1038/ejhg.2013.132
Elliott M, Bayly R, Cole T, Temple IK, Maher ER (1994) Clinical features and natural history of Beckwith-Wiedemann syndrome: presentation of 74 new cases. Clin Genet 46(2):168–174
Fowden AL, Coan PM, Angiolini E, Burton GJ, Constancia M (2011) Imprinted genes and the epigenetic regulation of placental phenotype. Prog Biophys Mol Biol 106(1):281–288
Fowden AL, Forhead AJ, Coan PM, Burton GJ (2008) The placenta and intrauterine programming. J Neuroendocrinol 20(4):439–450
Frost JM, Moore GE (2010) The importance of imprinting in the human placenta. PLoS Genet 6(7):e1001015
Gabory A, Ripoche MA, Le Digarcher A, Watrin F, Ziyyat A, Forné T, Jammes H, Ainscough JF, Surani MA, Journot L, Dandolo L (2009) H19 acts as a trans regulator of the imprinted gene network controlling growth in mice. Development 136(20):3413–3421
Gaston V, Le Bouc Y, Soupre V, Burglen L, Donadieu J, Oro H, Audry G, Vazquez MP, Gicquel C (2001) Analysis of the methylation status of the KCNQ1OT and H19 genes in leukocyte DNA for the diagnosis and prognosis of Beckwith-Wiedemann syndrome. Eur J Hum Genet 9:409–418
Ghanim M, Rossignol S, Delobel B, Irving M, Miller O, Devisme L, Plennevaux JL, Lucidarme-Rossi S, Manouvrier S, Salah A, Chivu O, Netchine I, Vincent-Delorme C (2013) Possible association between complex congenital heart defects and 11p15 hypomethylation in three patients with severe Silver-Russell syndrome. Am J Med Genet A 161A:572–577
Gicquel C, Gaston V, Mandelbaum J, Siffroi JP, Flahault A, Le Bouc Y (2003) In vitro fertilization may increase the risk of Beckwith-Wiedemann syndrome related to the abnormal imprinting of the KCN1OT gene. Am J Hum Genet 72(5):1338–1341
Gicquel C, Rossignol S, Cabrol S, Houang M, Steunou V, Barbu V, Danton F, Thibaud N, Le Merrer M, Burglen L, Bertrand AM, Nechine I, Le Bouc Y (2005a) Epimutation of the telomeric imprinting center region on chromosome 11p15 in Silver-Russell syndrome. Nat Genet 37:1003–1007
Gicquel C, Rossignol S, Le Bouc Y (2005b) Beckwith-Wiedemann syndrome. Orphanet Encyclopedia, http://www.orpha.net/data/patho/GB/uk-BWS05.pdf
Grønskov K, Poole RL, Hahnemann JM, Thomson J, Tümer Z, Brøndum-Nielsen K, Murphy R, Ravn K, Melchior L, Dedic A, Dolmer B, Temple IK, Boonen SE, Mackay DJ (2011) Deletions and rearrangements of the H19/IGF2 enhancer region in patients with Silver-Russell syndrome and growth retardation. J Med Genet 48(5):308–311
Guettard E, Portnoi MF, Lohmann-Hedrich K, Keren B, Rossignol S, Winkler S, El Kamel I, Leu S, Apartis E, Vidailhet M, Klein C, Roze E (2008) Myoclonus-dystonia due to maternal uniparental disomy. Arch Neurol 65(10):1380–1385
Gutierrez-Marcos JF, Constância M, Burton GJ (2012) Maternal to offspring resource allocation in plants and mammals. Placenta 33(Suppl 2):e3–e10
Halliday J, Oke K, Breheny S, Algar E, J Amor D (2004) Beckwith-Wiedemann syndrome and IVF: a case–control study. Am J Hum Genet 75(3):526–528
Hannula K, Lipsanen-Nyman M, Kontiokari T, Kere J (2001) A narrow segment of maternal uniparental disomy of chromosome 7q31-qter in Silver-Russell syndrome delimits a candidate gene region. Am J Hum Genet 68:247–253
Hark AT, Schoenherr CJ, Ingram RS, Levorse JM, Tilghman SM (2000) CTCF mediates methylation-sensitive enhancer-blocking activity at the H19/Igf2 locus. Nature 405:486–489
Heasman L, Clarke L, Firth K, Stephenson T, Symonds ME (1998) Influence of restricted maternal nutrition in early to mid gestation on placental and fetal development at term in sheep. Pediatr Res 44(4):546–551
Heijmans BT, Tobi EW, Stein AD, Putter H, Blauw GJ, Susser ES, Slagboom PE, Lumey LH (2008) Persistent epigenetic differences associated with prenatal exposure to famine in humans. Proc Natl Acad Sci U S A 105(44):17046–17049
Henckel A, Nakabayashi K, Sanz LA, Feil R, Hata K, Arnaud P (2009) Histone methylation is mechanistically linked to DNA methylation at imprinting control regions in mammals. Hum Mol Genet 18(18):3375–3383
Henry I, Puech A, Riesewijk A, Ahnine L, Mannens M, Beldjord C, Bitoun P, Tournade MF, Landrieu P, Junien C (1993) Somatic mosaicism for partial paternal isodisomy in Wiedemann-Beckwith syndrome: a post-fertilization event. Eur J Hum Genet 1(1):19–29
Hitchins MP, Monk D, Bell GM, Ali Z, Preece MA, Stanier P, Moore GE (2001a) Maternal repression of the human GRB10 gene in the developing central nervous system; evaluation of the role for GRB10 in Silver-Russell syndrome. Eur J Hum Genet 9:82–90
Hitchins MP, Stanier P, Preece MA, Moore GE (2001b) Silver-Russell syndrome: a dissection of the genetic aetiology and candidate chromosomal regions. J Med Genet 38:810–819
Hori N, Nakano H, Takeuchi T, Kato H, Hamaguchi S, Oshimura M, Sato K (2002) A dyad oct-binding sequence functions as a maintenance sequence for the unmethylated state within the H19/Igf2-imprinted control region. J Biol Chem 277:27960–27967
Hori N, Yamane M, Kouno K, Sato K (2012) Induction of DNA demethylation depending on two sets of Sox2 and adjacent Oct3/4 binding sites (Sox-Oct motifs) within the mouse H19/insulin-like growth factor 2 (Igf2) imprinted control region. J Biol Chem 287:44006–44016
Ideraabdullah FY, Vigneau S, Bartolomei MS (2008) Genomic imprinting mechanisms in mammals. Mutat Res 647:77–85
Joyce CA, Sharp A, Walker JM, Bullman H, Temple IK (1999) Duplication of 7p12.1-p13, including GRB10 and IGFBP1, in a mother and daughter with features of Silver-Russell syndrome. Hum Genet 105:273–280
Kagami M, Nagai T, Fukami M, Yamazawa K, Ogata T (2007) Silver-Russell syndrome in a girl born after in vitro fertilization: partial hypermethylation at the differentially methylated region of PEG1/MEST. J Assist Reprod Genet 24:131–136
Kannenberg K, Urban C, Binder G (2012) Increased incidence of aberrant DNA methylation within diverse imprinted gene loci outside of IGF2/H19 in Silver-Russell syndrome. Clin Genet 81:366–377
Kasowski M, Grubert F, Heffelfinger C, Hariharan M, Asabere A, Waszak SM, Habegger L, Rozowsky J, Shi M, Urban AE, Hong MY, Karczewski KJ, Huber W, Weissman SM, Gerstein MB, Korbel JO, Snyder M (2010) Variation in transcription factor binding among humans. Science 328(5975):232–235
Kaufman Y, Heled M, Perk J, Razin A, Shemer R (2009) Protein-binding elements establish in the oocyte the primary imprint of the Prader-Willi/Angelman syndromes domain. Proc Natl Acad Sci U S A 106(25):10242–10247
Keren B, Chantot-Bastaraud S, Brioude F, Mach C, Fonteneau E, Azzi S, Depienne C, Brice A, Netchine I, Le Bouc Y, Siffroi JP, Rossignol S (2013) SNP arrays in Beckwith-Wiedemann syndrome: an improved diagnostic strategy. Eur J Med Genet 56(10):546–550. doi:10.1016/j.ejmg.2013.06.005, pii: S1769-7212(13)00134-1
Kim YJ, Cecchini KR, Kim TH (2011) Conserved, developmentally regulated mechanism couples chromosomal looping and heterochromatin barrier activity at the homeobox gene A locus. Proc Natl Acad Sci U S A 108(18):7391–7396
Klose RJ, Bird AP (2006) Genomic DNA methylation: the mark and its mediators. Trends Biochem Sci 31:89–97
Kobayashi S, Uemura H, Kohda T, Nagai T, Chinen Y, Naritomi K (2001) No evidence of PEG1/MEST gene mutations in Silver-Russell syndrome patients. Am J Med Genet 104:225–231
Lefebvre L (2012) The placental imprintome and imprinted gene function in the trophoblast glycogen cell lineage. Reprod Biomed Online 25(1):44–57
Lewis A, Mitsuya K, Umlauf D, Smith P, Dean W, Walter J, Higgins M, Feil R, Reik W (2004) Imprinting on distal chromosome 7 in the placenta involves repressive histone methylation independent of DNA methylation. Nat Genet 36:1291–1295
Lim D, Bowdin SC, Tee L, Kirby GA, Blair E, Fryer A, Lam W, Oley C, Cole T, Brueton LA, Reik W, Macdonald F, Maher ER (2009) Clinical and molecular genetic features of Beckwith-Wiedemann syndrome associated with assisted reproductive technologies. Hum Reprod 24:741–747
Lucifero D, Mertineit C, Clarke HJ, Bestor TH, Trasler JM (2002) Methylation dynamics of imprinted genes in mouse germ cells. Genomics 79:530–538
Ludwig M, Katalinic A, Gross S, Sutcliffe A, Varon R, Horsthemke B (2005) Increased prevalence of imprinting defects in patients with Angelman syndrome born to subfertile couples. J Med Genet 42:289–291
Lumey LH (1998) Compensatory placental growth after restricted maternal nutrition in early pregnancy. Placenta 19(1):105–111
Mackay DJ, Boonen SE, Clayton-Smith J, Goodship J, Hahnemann JM, Kant SG, Njølstad PR, Robin NH, Robinson DO, Siebert R, Shield JP, White HE, Temple IK (2006) A maternal hypomethylation syndrome presenting as transient neonatal diabetes mellitus. Hum Genet 120:262–269
Mackay DJ, Callaway JL, Marks SM, White HE, Acerini CL, Boonen SE, Dayanikli P, Firth HV, Goodship JA, Haemers AP, Hahnemann JM, Kordonouri O, Masoud AF, Oestergaard E, Storr J, Ellard S, Hattersley AT, Robinson DO, Temple IK (2008) Hypomethylation of multiple imprinted loci in individuals with transient neonatal diabetes is associated with mutations in ZFP57. Nat Genet 40:949–951
Maher ER, Brueton LA, Bowdin SC, Luharia A, Cooper W, Cole TR, Macdonald F, Sampson JR, Barratt CL, Reik W, Hawkins MM (2003) Beckwith-Wiedemann syndrome and assisted reproduction technology (ART). J Med Genet 40(1):62–64
Maupetit-Mehouas S, Azzi S, Steunou V, Sakakini N, Silve C, Reynes C, Perez de Nanclares G, Keren B, Chantot S, Barlier A, Linglart A, Netchine I (2013) Simultaneous hyper- and hypomethylation at imprinted loci in a subset of patients with GNAS epimutations underlies a complex and different mechanism of multilocus methylation defect in pseudohypoparathyroidism Type 1b. Hum Mutat 34:1172–1180
McCann JA, Zheng H, Islam A, Goodyer CG, Polychronakos C (2001) Evidence against GRB10 as the gene responsible for Silver-Russell syndrome. Biochem Biophys Res Commun 286:943–948
McDaniell R, Lee BK, Song L, Liu Z, Boyle AP, Erdos MR, Scott LJ, Morken MA, Kucera KS, Battenhouse A, Keefe D, Collins FS, Willard HF, Lieb JD, Furey TS, Crawford GE, Iyer VR, Birney E (2010) Heritable individual-specific and allele-specific chromatin signatures in humans. Science 328(5975):235–239
McGrath J, Solter D (1984) Completion of mouse embryogenesis requires both the maternal and paternal genomes. Cell 37:179–183
Meyer E, Lim D, Pasha S, Tee LJ, Rahman F, Yates JR, Woods CG, Reik W, Maher ER (2009) Germline mutation in NLRP2 (NALP2) in a familial imprinting disorder (Beckwith-Wiedemann Syndrome). PLoS Genet 5:e1000423. doi:10.1371/journal.pgen.1000423
Monk DE, Wakeling EL, Proud V, Hitchins M, Abu-Amero SN, Stanier P, Preece MA, Moore GE (2000) Duplication of 7p11.2-p13, including GRB10, in Silver-Russell syndrome. Am J Hum Genet 66:36–46
Monk D, Arnaud P, Apostolidou S, Hills FA, Kelsey G, Stanier P, Feil R, Moore GE (2006) Limited evolutionary conservation of imprinting in the human placenta. Proc Natl Acad Sci U S A 103:6623–6628
Murphy R, Ibanez L, Hattersley A, Tost J (2012) IGF2/H19 hypomethylation in a patient with very low birthweight, preocious pubarche and insulin resistance. BMC Med Genet 13:42
Nativio R, Sparago A, Ito Y, Weksberg R, Riccio A, Murrell A (2011) Disruption of genomic neighbourhood at the imprinted IGF2-H19 locus in Beckwith-Wiedemann syndrome and Silver-Russell syndrome. Hum Mol Genet 20(7):1363–1374
Nelissen EC, van Montfoort AP, Dumoulin JC, Evers JL (2011) Epigenetics and the placenta. Hum Reprod Update 17(3):397–417
Netchine I, Rossignol S, Dufourg MN, Azzi S, Rousseau A, Perin L, Houang M, Steunou V, Esteva B, Thibaud N, Demay MC, Danton F, Petriczko E, Bertrand AM, Heinrichs C, Carel JC, Loeuille GA, Pinto G, Jacquemont ML, Gicquel C, Cabrol S, Le Bouc Y (2007) 11p15 imprinting center region 1 loss of methylation is a common and specific cause of typical Russell-Silver syndrome: clinical scoring system and epigenetic-phenotypic correlations. J Clin Endocrinol Metab 92:3148–3154
Niemitz EL, DeBaun MR, Fallon J, Murakami K, Kugoh H, Oshimura M, Feinberg AP (2004) Microdeletion of LIT1 in familial Beckwith-Wiedemann syndrome. Am J Hum Genet 75:844–849
Nyström A, Cheetham JE, Engström W, Schofield PN (1992) Molecular analysis of patients with Wiedemann-Beckwith syndrome. II. Paternally derived disomies of chromosome 11. Eur J Pediatr 151(7):511–514
Obermann C, Meyer E, Prager S, Tomiuk J, Wollmann HA, Eggermann T (2004) Searching for genomic variants in IGF2 and CDKN1C in Silver-Russell syndrome patients. Mol Genet Metab 82:246–250
Penaherrera MS, Weindler S, Van Allen MI, Yong S-L, Metzger DL, McGillivray B, Boerkoel C, Langlois S, Robinson WP (2010) Methylation profiling in individuals with Russell-Silver syndrome. Am J Med Genet A 152A:347–355
Perez-Nanclares G, Romanelli V, Mayo S, Garin I, Zazo C, Fernandez-Rebollo E, Martínez F, Lapunzina P, de Nanclares GP (2012) Detection of hypomethylation syndrome among patients with epigenetic alterations at the GNAS locus. J Clin Endocrinol Metab 97:E1060–E1067
Pettenati MJ, Haines JL, Higgins RR, Wappner RS, Palmer CG, Weaver DD (1986) Wiedemann-Beckwith syndrome: presentation of clinical and cytogenetic data on 22 new cases and review of the literature. Hum Genet 74(2):143–154
Poole RL, Leith DJ (2012) Beckwith-Wiedemann syndrome caused by maternally inherited mutation of an OCT-binding motif in the IGF2/H19-imprinting control region, ICR1. Eur J Hum Genet 20:240–243
Poole RL, Docherty LE, Al Sayegh A, Caliebe A, Turner C, Baple E, Wakeling E, Harrison L, Lehmann A, Temple IK, Mackay DJ (2013) Targeted methylation testing of a patient cohort broadens the epigenetic and clinical description of imprinting disorders. Am J Med Genet A 161:2174–2182
Prawitt D, Enklaar T, Gärtner-Rupprecht B, Spangenberg C, Oswald M, Lausch E, Schmidtke P, Reutzel D, Fees S, Lucito R, Korzon M, Brozek I, Limon J, Pelletier J, Housman DE, Zabel B (2005) Microdeletion of target sites for insulator protein CTCF in a chromosome 11p15 imprinting center in Beckwith-Wiedemann syndrome and Wilms’ tumor. Proc Natl Acad Sci U S A 102:4085–4090
Preece MA (2002) The genetics of the Silver-Russell syndrome. Rev Endocr Metab Disord 3:369–379
Price SM, Stanhope R, Garrett C, Preece MA, Trembath RC (1999) The spectrum of Silver-Russell syndrome: a clinical and molecular genetic study and new diagnostic criteria. J Med Genet 36:837–842
Reik W, Dean W, Walter J (2001) Epigenetic reprogramming in mammalian development. Science 293:1089–1093
Reik W, Constância M, Fowden A, Anderson N, Dean W, Ferguson-Smith A, Tycko B, Sibley C (2003) Regulation of supply and demand for maternal nutrients in mammals by imprinted genes. J Physiol 547:35–44
Riesewijk AM, Blagitko N, Schinzel AA, Hu L, Schulz U, Hamel BC, Ropers HH, Kalscheuer VM (1998) Evidence against a major role of PEG1/MEST in Silver-Russell syndrome. Eur J Hum Genet 6:114–120
Romanelli V, Meneses HN, Fernández L, Martínez-Glez V, Gracia-Bouthelier R, Fraga M, Guillén E, Nevado J, Gean E, Martorell L, Marfil VE, García-Miñaur S, Lapunzina P (2011) Beckwith-Wiedemann syndrome and uniparental disomy 11p: fine mapping of the recombination breakpoints and evaluation of several techniques. Eur J Hum Genet 19:416–421
Rossignol S, Steunou V, Chalas C, Kerjean A, Rigolet M, Viegas-Pequignot E, Jouannet P, Le Bouc Y, Gicquel C (2006) The epigenetic imprinting defect of patients with Beckwith-Wiedemann syndrome born after assisted reproductive technology is not restricted to the 11p15 region. J Med Genet 43:902–907
Rump P, Zeegers MP, van Essen AJ (2005) Tumor risk in Beckwith-Wiedemann syndrome: a review and meta-analysis. Am J Med Genet A 136:95–104
Russell AS, Jackson C (1954) Fetal mortality conference; an interdepartmental approach to neonatal and fetal mortality. Curr Res Anesth Analg 33:277–281
Russo S, Finelli P, Recalcati MP, Ferraiuolo S, Cogliati F, Dalla Bernardina B, Tibiletti MG, Agosti M, Sala M, Bonati MT, Larizza L (2006) Molecular and genomic characterisation of cryptic chromosomal alterations leading to paternal duplication of the 11p15.5 Beckwith-Wiedemann region. J Med Genet 43:e39
Sakaguchi R, Okamura E, Matsuzaki H, Fukamizu A, Tanimoto K (2013) Sox-Oct motifs contribute to maintenance of the unmethylated H19 ICR in YAC transgenic mice. Hum Mol Genet 22(22):4627–4637. doi:10.1093/hmg/ddt311
Sandovici I, Hoelle K, Angiolini E, Constância M (2012) Placental adaptations to the maternal-fetal environment: implications for fetal growth and developmental programming. Reprod Biomed Online 25:68–89
Santos F, Dean W (2004) Epigenetic reprogramming during early development in mammals. Reproduction 127:643–651
Schneid H, Seurin D, Vazquez MP, Gourmelen M, Cabrol S, Le Bouc Y (1993) Parental allele specific methylation of the human insulin-like growth factor II gene and Beckwith-Wiedemann syndrome. J Med Genet 30(5):353–362
Schönherr N, Meyer E, Roos A, Schmidt A, Wollmann HA, Eggermann T (2007) The centromeric 11p15 imprinting centre is also involved in Silver-Russell syndrome. J Med Genet 44(1):59–63
Scott RH, Douglas J, Baskcomb L, Huxter N, Barker K, Hanks S, Craft A, Gerrard M, Kohler JA, Levitt GA, Picton S, Pizer B, Ronghe MD, Williams D, Factors Associated with Childhood Tumours (FACT) Collaboration, Cook JA, Pujol P, Maher ER, Birch JM, Stiller CA, Pritchard-Jones K, Rahman N (2008) Constitutional 11p15 abnormalities, including heritable imprinting center mutations, cause nonsyndromic Wilms tumor. Nat Genet 40:1329–1334
Sibley CP, Brownbill P, Dilworth M, Glazier JD (2010) Review: adaptation in placental nutrient supply to meet fetal growth demand: implications for programming. Placenta 31:S70–S74
Silver HK, Kiyasu W, George J, Deamer WC (1953) Syndrome of congenital hemihypertrophy, shortness of stature, and elevated urinary gonadotropins. Pediatrics 12:368–376
Soejima H, Higashimoto K (2013) Epigenetic and genetic alterations of the imprinting disorder Beckwith-Wiedemann syndrome and related disorders. J Hum Genet 58:402–409
Sotelo-Avila C, Gonzalez-Crussi F, Fowler JW (1980) Complete and incomplete forms of Beckwith-Wiedemann syndrome: their oncogenic potential. J Pediatr 96(1):47–50
Sparago A, Cerrato F, Vernucci M, Ferrero GB, Silengo MC, Riccio A (2004) Microdeletions in the human H19 DMR result in loss of IGF2 imprinting and Beckwith-Wiedemann syndrome. Nat Genet 36:958–960
Sparago A, Russo S, Cerrato F, Ferraiuolo S, Castorina P, Selicorni A, Schwienbacher C, Negrini M, Ferrero GB, Silengo MC, Anichini C, Larizza L, Riccio A (2007) Mechanisms causing imprinting defects in familial Beckwith-Wiedemann syndrome with Wilms’ tumour. Hum Mol Genet 16:254–264
Surani MA, Barton SC, Norris ML (1984) Development of reconstituted mouse eggs suggests imprinting of the genome during gametogenesis. Nature 308:548–550
Svensson J, Björnståhl A, Ivarsson SA (2005) Increased risk of Silver-Russell syndrome after in vitro fertilization? Acta Paediatr 94(8):1163–1165
Takahashi K, Kobayashi T, Kanayama N (2000) p57(Kip2) regulates the proper development of labyrinthine and spongiotrophoblasts. Mol Hum Reprod 6:1019–1025
Thorburn MJ, Wright ES, Miller CG, Smith-Read EH (1970) Exomphalos-macroglossia-gigantism syndrome in Jamaican infants. Am J Dis Child 119:316–321
Tunster SJ, Van de Pette M, John RM (2011) Fetal overgrowth in the Cdkn1c mouse model of Beckwith-Wiedemann syndrome. Dis Model Mech 4:814–821
Turner CL, Mackay DM, Callaway JL, Docherty LE, Poole RL, Bullman H, Lever M, Castle BM, Kivuva EC, Turnpenny PD, Mehta SG, Mansour S, Wakeling EL, Mathew V, Madden J, Davies JH, Temple IK (2010) Methylation analysis of 79 patients with growth restriction reveals novel patterns of methylation change at imprinted loci. Eur J Hum Genet 18:648–655
Tycko B (2010) Allele-specific DNA methylation: beyond imprinting. Hum Mol Genet 19:R210–R220
Umlauf D, Goto Y, Cao R, Cerqueira F, Wagschal A, Zhang Y, Feil R (2004) Imprinting along the Kcnq1 domain on mouse chromosome 7 involves repressive histone methylation and recruitment of Polycomb group complexes. Nat Genet 36:1296–1300
Usher R, McLean F (1969) Intrauterine growth of live-born Caucasian infants at sea level: standards obtained from measurements in 7 dimensions of infants born between 25 and 44 weeks of gestation. J Pediatr 74:901–910
Varrault A, Gueydan C, Delalbre A, Bellmann A, Houssami S, Aknin C, Severac D, Chotard L, Kahli M, Le Digarcher A, Pavlidis P, Journot L (2006) Zac1 regulates an imprinted gene network critically involved in the control of embryonic growth. Dev Cell 11(5):711–722
Wakeling EL, Amero SA, Alders M, Bliek J, Forsythe E, Kumar S, Lim DH, MacDonald F, Mackay DJ, Maher ER, Moore GE, Poole RL, Price SM, Tangeraas T, Turner CL, Van Haelst MM, Willoughby C, Temple IK, Cobben JM (2010) Epigenotype-phenotype correlations in Silver-Russell syndrome. J Med Genet 47:760–768
Wan LB, Bartolomei MS (2008) Regulation of imprinting in clusters: noncoding RNAs versus insulators. Adv Genet 61:207–223
Weksberg R, Nishikawa J, Caluseriu O, Fei YL, Shuman C, Wei C, Steele L, Cameron J, Smith A, Ambus I, Li M, Ray PN, Sadowski P, Squire J (2001) Tumor development in the Beckwith-Wiedemann syndrome is associated with a variety of constitutional molecular 11p15 alterations including imprinting defects of KCNQ1OT1. Hum Mol Genet 10(26):2989–3000
Weksberg R, Shuman C, Caluseriu O, Smith AC, Fei YL, Nishikawa J, Stockley TL, Best L, Chitayat D, Olney A, Ives E, Schneider A, Bestor TH, Li M, Sadowski P, Squire J (2002) Discordant KCNQ1OT1 imprinting in sets of monozygotic twins discordant for Beckwith-Wiedemann syndrome. Hum Mol Genet 11:1317–1325
Weksberg R, Shuman C, Smith AC (2005) Beckwith-Wiedemann syndrome. Am J Med Genet C Semin Med Genet 137C:12–23
Weth O, Renkawitz R (2011) CTCF function is modulated by neighboring DNA binding factors. Biochem Cell Biol 89(5):459–468
Wiedemann HR (1969) The EMG-syndrome: exomphalos, macroglossia, gigantism and disturbed carbohydrate metabolism. Z Kinderheilkd 106(3):171–185
Wu G, Imhoff-Kunsch B, Girard AW (2012) Biological mechanisms for nutritional regulation of maternal health and fetal development. Paediatr Perinat Epidemiol 26:4–26
Yamazawa K, Kagami M, Fukami M, Matsubara K, Ogata T (2008a) Monozygotic female twins discordant for Silver-Russell syndrome and hypomethylation of the H19-DMR. J Hum Genet 53:950–955
Yamazawa K, Kagami M, Nagai T, Kondoh T, Onigata K, Maeyama K, Hasegawa T, Hasegawa Y, Yamazaki T, Mizuno S, Miyoshi Y, Miyagawa S, Horikawa R, Matsuoka K, Ogata T (2008b) Molecular and clinical findings and their correlations in Silver-Russell syndrome: implications for a positive role of IGF2 in growth determination and differential imprinting regulation of the IGF2-H19 domain in bodies and placentas. J Mol Med (Berl) 86:1171–1181
Yoshihashi H, Maeyama K, Kosaki R, Ogata T, Tsukahara M, Goto Y, Hata J, Matsuo N, Smith RJ, Kosaki K (2000) Imprinting of human GRB10 and its mutations in two patients with Russell-Silver syndrome. Am J Hum Genet 67:476–482
Zhang P, Liegeois NJ, Wong C, Finegold M, Hou H, Thompson JC, Silverman A, Harper JW, DePinho RA, Elledge SJ (1997) Altered cell differentiation and proliferation in mice lacking p57KIP2 indicates a role in Beckwith-Wiedemann syndrome. Nature 387:151–158
Zogel C, Bohringer S, Gross S, Varon R, Buiting K, Horsthemke B (2006) Identification of cis- and trans-acting factors possibly modifying the risk of epimutations on chromosome 15. Eur J Hum Genet 14:752–758
Zollino M, Orteschi D, Marangi G, De Crescenzo A, Pecile V, Riccio A, Neri G (2010) A case of Beckwith-Wiedemann syndrome caused by a cryptic 11p15 deletion encompassing the centromeric imprinted domain of the BWS locus. J Med Genet 47:429–432
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Gicquel, C. et al. (2014). Human Fetal Growth Disorders and Imprinting Anomalies. In: Seckl, J., Christen, Y. (eds) Hormones, Intrauterine Health and Programming. Research and Perspectives in Endocrine Interactions, vol 12. Springer, Cham. https://doi.org/10.1007/978-3-319-02591-9_8
Download citation
DOI: https://doi.org/10.1007/978-3-319-02591-9_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-02590-2
Online ISBN: 978-3-319-02591-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)