Abstract
Fetal glucocorticoid exposure is a key mechanism involved in adverse programming outcomes in the adult. Impairment of fetal growth has predominantly been attributed to direct effects of glucocorticoids on the fetus, prematurely shifting tissue development from a proliferative to a more functionally mature state. However, fetal growth is dependent on a complex interplay of maternal, placental, and fetal endocrine signals, and glucocorticoid-mediated fetal growth retardation is likely also to relate to disturbances in placental growth and function. Regulation of fetal glucocorticoid exposure is achieved by the placental glucocorticoid barrier, which involves glucocorticoid inactivation within the labyrinth zone of the murine placenta by 11β-hydroxysteroid dehydrogenase type 2 (11β-HSD2). Overexposure to glucocorticoids or depletion of 11β-HSD2 has a dramatic effect on placental development and function, with a reduction in capillary networks and alterations in nutrient transport. This work highlights the finding that adverse programming effects of glucocorticoids are not exclusively due to direct actions on the fetus but are also a consequence of changes in placental development and function.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Developmental Programming
Low birth-weight and other indicators of reduced fetal growth are associated with adult cardio-metabolic and psychiatric disease. This association is the result of “developmental programming,” whereby a stimulus during a sensitive period of early development exerts permanent effects on structure, physiology or metabolism (Cottrell and Seckl 2009). The environmental mechanisms of developmental programming identified so far can be simplified into two major groups: fetal stress exposure and maternal nutrition, although changes in glucocorticoids appear to underpin the programming effects of both (Langley-Evans et al. 1996; Gardner et al. 2007; Harris and Seckl 2010). In many animals, including mice and humans, there is an increased exposure of the developing fetus to glucocorticoids late in pregnancy, as they have a crucial role in the structural development and functional maturation of fetal organs. However, glucocorticoid overexposure of the fetus can be detrimental, as glucocorticoids cause a shift from cell proliferation to differentiation. Therefore, exposure to excess glucocorticoids in utero alters fetal organ growth and maturation patterns, which can result in adverse consequences in later life. In humans, the actions of glucocorticoids are exploited for preterm births to advance fetal lung maturation (Roberts and Dalziel 2006), although this may set the stage for adverse effects in later life (Benediktsson et al. 1993; Brown et al. 1996a; Levitt et al. 1996; Lindsay et al. 1996; Dodic et al. 1998, 1999, 2002a, b; Gatford et al. 2000; Langdown and Sugden 2001; Jensen et al. 2002).
The Feto-Placental Glucocorticoid Barrier: 11β-HSD2
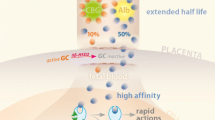
As glucocorticoids are highly lipophilic, they readily diffuse across biological membranes and, therefore, control of intracellular levels of bioactive glucocorticoid is critical. This control arises from the enzyme 11β-hydroxysteroid dehydrogenase (11β-HSD), which interconverts the active glucocorticoids cortisol and corticosterone with their biologically inactive forms, cortisone and 11-dehydrocorticosterone (DHC), respectively. There are two distinct forms of 11β-HSD: 11β-HSD1, which is a low affinity, NADP(H)-dependent bidirectional enzyme, although in vivo it appears to act predominantly as an 11β-oxoreductase to enhance glucocorticoid activity; and 11β-HSD2, which is a high affinity NAD-dependent enzyme that exhibits exclusive 11β-dehydrogenase activity (conversion of corticosterone to DHC) to reduce glucocorticoid potency. 11β-HSD2 is highly expressed in aldosterone-selective target tissues such as the distal nephron (Roland et al. 1995), colon (Whorwood et al. 1994), salivary glands (Roland and Funder 1996) and skin (Kenouch et al. 1994), thus serving to confer aldosterone specificity on the mineralocorticoid receptor (MR) to which both corticosterone and aldosterone can bind. Importantly, 11β-HSD2 does not always colocalize with MR, such as within placental and fetal tissues, and so its function has expanded beyond involvement in electrolyte transport to include regulation of corticosteroid action.
During much of normal pregnancy, circulating levels of glucocorticoids in the fetus are substantially lower than in the mother. This difference arises in part from the high expression of 11β-HSD2 in both the placenta and fetus, and this 11β-HSD2 expression serves as a “glucocorticoid barrier,” enabling tight regulation of materno-fetal glucocorticoid transfer. Within the placenta, 11β-HSD2 is highly expressed at the interface between maternal and fetal circulations, in the syncytiotrophoblast in humans (Brown et al. 1996a,b) and the labyrinthine zone in rodents (Waddell et al. 1998). In the rodent, 11β-HSD2 expression within the labyrinthine zone of the placenta falls during late gestation, which may facilitate glucocorticoid passage to the fetus and thus lung maturation (Brown et al. 1996a, b; Burton et al. 1996).
The high expression of 11β-HSD2 in placenta and fetal tissues and the growth-retarding and maturational effects of glucocorticoids upon the fetus (Meyer 1983) have lead to the proposal that variations in feto-placental 11β-HSD2 may underlie developmental programming. Thus, placental 11β-HSD2 activity correlates with birth parameters in rodents and, less consistently, in humans (Benediktsson et al. 1993; Stewart et al. 1995; Murphy et al. 2002), suggesting that normal variation in fetal exposure to maternal glucocorticoids has an impact on fetal growth. Numerous studies have shown that inhibition, deficiency or by-pass (poor substrate steroids such as dexamethasone or betamethasone) of 11β-HSD2 in gestation in rodents and humans associates with alterations in pregnancy duration, birth weight and programmed outcomes in the offspring (Benediktsson et al. 1993; Burton and Waddell 1994; Mune et al. 1995; Lindsay et al. 1996; Dave-Sharma et al. 1998; Nyirenda et al. 1998; Smith and Waddell 2000; Welberg et al. 2000, 2001; O'Regan et al. 2004; Holmes et al. 2006; Wyrwoll et al. 2006, 2007; Newnham and Jobe 2009). Furthermore, maternal stress in rodents during pregnancy has been associated with decreased expression of placental 11β-HSD2 (Mairesse et al. 2007; Lucassen et al. 2009; Pankevich et al. 2009). Interestingly, programming models involving maternal low-protein diet show an increase in maternal and fetal glucocorticoid levels (Lesage et al. 2001; Guzmán et al. 2006) in addition to a decrease in placental 11β-HSD2 activity and/or expression (Langley-Evans et al. 1996; Lesage et al. 2001; Stocker et al. 2004). Moreover, dexamethasone administration during pregnancy decreases food intake (Woods and Weeks 2005). Consequently, there seems to be considerable overlap in mechanisms by which maternal undernutrition and fetal glucocorticoid overexposure elicit developmental programming.
Placental 11β-HSD2 Is More than Just a Glucocorticoid Barrier
As described above, placental 11β-HSD2 may underpin aspects of developmental programming by allowing excess glucocorticoid passage from the “high” glucocorticoid maternal circulation to the “low” glucocorticoid fetal environment (Edwards et al. 1993), thus impairing fetal growth by direct effects of glucocorticoids on the fetus. Fetal growth is, however, dependent on a complex array of maternal, placental and fetal endocrine signals, and glucocorticoid-mediated fetal growth retardation must also relate, at least in part, to disturbances in placental growth and function. Indeed, treatment of rats with glucocorticoids such as dexamethasone, which are poor substrates for 11β-HSD2, restricts placental vascular development, via inhibition of the endothelial cell-specific mitogen, vascular endothelial growth factor-A (VEGF-A), and peroxisome proliferators-activated receptor gamma (PPARγ), which regulates VEGF-A expression (Hewitt et al. 2006a,b). Impaired vascular arborization within key areas of the placenta that are involved in nutrient exchange between the maternal and fetal circulations is likely to have effects on placental function. However, glucocorticoid effects on placental function have been discordant. Thus, chronic restraint stress during late gestation in rats reduces placental 11ß-HSD2 expression and expression of GLUT1, with an associated reduction in fetal plasma glucose (Mairesse et al. 2007), whereas late gestation dexamethasone increases placental GLUT1 and 3 expression (Langdown and Sugden 2001), and another synthetic glucocorticoid, triamcinolone, down-regulates placental GLUT1 and 3 protein and mRNA (Hahn et al. 1999). Any physiological relevance of these manipulations is unresolved. Furthermore, while system A amino acid transporter (SNAT) activity and expression are upregulated by cortisol exposure in BeWo cells (Jones et al. 2006), they are unaltered in human placental villous fragments exposed to cortisol (Jansson et al. 2003; Ericsson et al. 2005). Importantly, it is unknown whether the above observations of altered placental function in whole animal experiments are a direct effect of glucocorticoids on the placenta or occur via indirect effects on the dam. Thus, recent work utilizing 11β-HSD2+/− mice sought to demonstrate a direct effect of increased glucocorticoid exposure on placental function. This model of 11β-HSD2 heterozygous matings, whereby 11β-HSD2+/+, +/− and −/− fetuses are generated by the same mother, clearly demonstrates a direct effect of increased glucocorticoid exposure on placental development and function.
Absence of Placental 11β-HSD2 Alters Placental Function and Development
Depletion of 11β-HSD2 in mice (generated by 11β-HSD2+/− matings) has been recently shown to compromise not only fetal but also placental growth (Wyrwoll et al. 2009) and to increase placental and fetal exposure to glucocorticoids (Cottrell et al. 2012). In this model, as 11β-HSD2 is expressed in the labyrinth zone of the placenta (which originates from fetal tissue), the genotype of the fetus is also the genotype of the placenta with regard to 11β-HSD2. At E15, despite a reduction in placental size, fetal weight is maintained, generating an increase in fetal/placental ratio that is indicative of enhanced placental function (Wyrwoll et al. 2009). Indeed, placental amino acid transport of 11β -HSD2−/− fetuses was upregulated at E15 alongside increased expression of the amino acid transporters Slc38a2 and Slc38a4 (Wyrwoll et al. 2009). Later in pregnancy, at E18, the smaller placenta of the 11β-HSD2−/− fetus appears unable to maintain normal fetal growth, and fetal weight falls behind control littermates (Wyrwoll et al. 2009). At this time, the transplacental transfer of glucose and plasma glucose levels was reduced in 11β-HSD2−/− fetuses (Wyrwoll et al. 2009). Glucose is a primary nutrient required for fetal development and is transported across the placenta by facilitated diffusion, primarily via GLUT1 and GLUT3 (Uldry and Thorens 2004). The reduced Slc2a3 expression we observed in the labyrinth zone of placentas from 11β-HSD2−/− fetuses most likely accounts for the reduction in the transplacental transfer of glucose.
This altered placental function is further associated with reduced capillary networks (Wyrwoll et al. 2009). Thus, 11β-HSD2−/− placentas have significantly reduced fetal capillary development within the labyrinth zone, the zone regulating nutrient exchange, accompanied by a decline in VEGF-A and PPARγ mRNA expression, which are factors known to regulate angiogenesis (Wyrwoll et al. 2009). The decrease in fetal capillary vascularity in the 11β-HSD2−/− placentas may have implications for blood flow within the placenta and the umbilical cord. Indeed, ultrasound measures of blood flow have revealed decreased blood flow in the 11β-HSD2−/− placenta towards the end of gestation (Wyrwoll, unpublished data). Furthermore, umbilical vein flow in 11β-HSD2−/− fetuses does not undergo the normal gestational increase that occurs in wild-type littermates (Wyrwoll, unpublished data).
Ultrasound measures have also revealed altered cardiac function in 11β-HSD2−/− fetuses. Thus, the normal increase in E/A wave ratio [the E wave represents passive filling of the left ventricle (LV) and the A wave represents LV filling due to contraction of the atria] over gestation as the fetal heart becomes more compliant is not apparent in 11β-HSD2−/− hearts (Wyrwoll, unpublished data). Furthermore, the resistance index [RI = systole/(systole + diastole); systole being blood flow during maximal contraction of the heart and diastole being maximal relaxation] in the umbilical artery does not undergo the normal gestational decline as blood flow from the fetus to placenta increases (Wyrwoll, unpublished data).
These novel ultrasound data have lead to the proposal that impaired placental hemodynamics in the 11β-HSD2−/− fetus may have direct implications for fetal cardiac function. As the site of gaseous exchange in the fetus is the placenta, fetal circulation is distinct from the postnatal period. Thus oxygenated blood from the placenta travels through the umbilical vein and enters the fetal circulation either through the ductus venosus (a fetal shunt that bypasses the hepatic circulation such that blood is directly delivered into the inferior vena cava) or, after perfusing the liver, enters the inferior vena cava via the hepatic veins. Once circulated, blood returns to the placenta via the umbilical artery. Therefore, given that both the fetal heart and liver are the immediate organs exposed to blood leaving the placenta, the placenta is uniquely placed to have a direct influence on these particular organs. Indeed, epidemiological studies have revealed associations between placental size and the shape and incidence of cardiovascular disease in later life (Barker et al. 2010).
However, the results discussed above provide only indirect evidence of changes in placental blood flow and vascularity impacting on fetal heart development and function. What is required to provide a conclusive link in this relationship is to produce an amelioration of the compromised fetal capillary development in 11β-HSD2−/− placentas and to then investigate how this alters placental and fetal hemodynamics. Indeed, restoration of angiogenic balance in mouse models of preeclampsia has striking effects. Thus, administration of pravastatin (one of a class of lipid-lowering compounds, the HMG-CoA reductase inhibitors, that reduce cholesterol biosynthesis) in various mouse models of preeclampsia appears to ameliorate preeclamptic pathology (Ahmed et al. 2010 , Kumasawa et al. 2011), The precise mechanisms by which this improvement transpires is unclear but there was marked restoration of vasculogenesis in the preeclamptic placentas which has been variously attributed to stimulation of placental VEGF release (Ahmed et al. 2010) or placental growth factor (Kumasawa et al. 2011). The previous finding that VEGF is decreased in the placentas of 11β-HSD2−/− fetuses and thus presumably accounts for the observed decline in normal fetal capillary development is notable (Wyrwoll et al. 2009).
Therefore, recent work has sought to establish the effects of pravastatin on placental blood flow and fetal heart function of 11β-HSD2−/− fetuses. Administration of pravastatin to 11β-HSD2+/− dams from E6 of gestation onwards had marked effects on placental blood flow and fetal heart measures. Thus, both placental blood flow and the fetal cardiac E/A ratio of 11β-HSD2−/− fetuses remained comparable to those in wild-type fetuses in the pravastatin-treated pregnancies (Wyrwoll, unpublished data). Strikingly, gene expression of placental VEGF-A is upregulated in the pravastatin-treated pregnancies, which would presumably enhance angiogenesis within the placenta, with consequent ramifications for blood flow (Wyrwoll, unpublished data). Characterization of vascularity within these placentas is currently being undertaken to establish if this is indeed the case.
Optimal Placental Function, Optimal Health in Later Life?
The work conducted over the last few years on placental function and development of 11β-HSD2−/− fetuses provides a convincing argument that, while maternal glucocorticoids could play a direct role in programming the fetus, placental development and function also play key roles. Thus, the observations of altered placental transport of nutrients may have important ramifications for “setting” fetal metabolism and, thus, adult health in later life. Furthermore, the possibility that placental hemodynamics have the potential to alter fetal cardiac development and function opens up a novel research avenue. Additionally, placental function may shape health outcomes beyond cardio-metabolic disease. Indeed, there is growing recognition that the placenta generates hormones that are critical for neural function prior to the time such hormones are produced by the fetal brain itself, raising the possibility that the placenta may have a significant role in fetal neurodevelopment (Bonnin et al. 2011). Therefore, the placenta is key in influencing fetal development and shaping health outcomes in later life.
References
Ahmed A, Singh J, Ahmed A, Singh J, Khan Y, Seshan SV, Girardi G (2010) A new mouse model to explore therapies for preeclampsia. PLoS One 5:13663
Barker DJ, Thornburg KL, Osmond C, Kajantie E, Eriksson JG (2010) The surface area of the placenta and hypertension in the offspring in later life. Int J Dev Biol 54:525–530
Benediktsson R, Lindsay RS, Noble J, Seckl JR, Edwards CR (1993) Glucocorticoid exposure in utero: new model for adult hypertension. Lancet 341:339–341
Bonnin A, Goeden N, Chen K, Wilson ML, King J, Shih JC, Blakely RD, Deneris ES, Levitt P (2011) A transient placental source of serotonin for the fetal forebrain. Nature 472:347–350
Brown RW, Diaz R, Robson AC, Kotelevtsev YV, Mullins JJ, Kaufman MH, Seckl JR (1996a) The ontogeny of 11 beta-hydroxysteroid dehydrogenase type 2 and mineralocorticoid receptor gene expression reveal intricate control of glucocorticoid action in development. Endocrinology 137:794–797
Brown RW, Chapman KE, Kotelevtsev Y, Yau JL, Lindsay RS, Brett L, Leckie C, Murad P, Lyons V, Mullins JJ, Edwards CR, Seckl JR (1996b) Cloning and production of antisera to human placental 11 beta-hydroxysteroid dehydrogenase type 2. Biochem J 313:1007–1017
Burton PJ, Waddell BJ (1994) 11 β-Hydroxysteroid dehydrogenase in the rat placenta: developmental changes and the effects of altered glucocorticoid exposure. J Endocrinol 143:505–513
Burton PJ, Smith RE, Krozowski ZS, Waddell BJ (1996) Zonal distribution of 11 beta-hydroxysteroid dehydrogenase types 1 and 2 messenger ribonucleic acid expression in the rat placenta and decidua during late pregnancy. Biol Reprod 55:1023–1028
Cottrell EC, Seckl JR (2009) Prenatal stress, glucocorticoids and the programming of adult disease. Front Behav Neurosci 3:19
Cottrell EC, Holmes MC, Livingstone DE, Kenyon CJ, Seckl JR (2012) Reconciling the nutritional and glucocorticoid hypotheses of fetal programming. FASEB J 26:1866–1874
Dave-Sharma S, Wilson RC, Harbison MD, Newfield R, Azar MR, Krozowski ZS, Funder JW, Shackleton CH, Bradlow HL, Wei JQ, Hertecant J, Moran A, Neiberger RE, Balfe JW, Fattah A, Daneman D, Akkurt HI, De Santis C, New MI (1998) Examination of genotype and phenotype relationships in 14 patients with apparent mineralocorticoid excess. J Clin Endocrinol Metab 83:2244–2254
Dodic M, May CN, Wintour EM, Coghlan JP (1998) An early prenatal exposure to excess glucocorticoid leads to hypertensive offspring in sheep. Clin Sci 94:149–155
Dodic M, Peers A, Coghlan JP, May CN, Lumbers E, Yu Z, Wintour EM (1999) Altered cardiovascular haemodynamics and baroreceptor-heart rate reflex in adult sheep after prenatal exposure to dexamethasone. Clin Sci 97:103–109
Dodic M, Hantzis V, Duncan J, Rees S, Koukoulas I, Johnson K, Wintour EM, Moritz K (2002a) Programming effects of short prenatal exposure to cortisol. FASEB J 16:1017–1026
Dodic M, Moritz K, Koukoulas I, Wintour EM (2002b) Programmed hypertension: kidney, brain or both? Trends Endocrinol Metab 13:403–408
Edwards CR, Benediktsson R, Lindsay RS, Seckl JR (1993) Dysfunction of placental glucocorticoid barrier: link between fetal environment and adult hypertension? Lancet 341:355–357
Ericsson A, Hamark B, Jansson N, Johansson BR, Powell TL, Jansson T (2005) Hormonal regulation of glucose and system A amino acid transport in first trimester placental villous fragments. Am J Physiol Regul Integr Comp Physiol 288:R656–R662
Gardner DS, Bell RC, Symonds ME (2007) Fetal mechanisms that lead to later hypertension. Curr Drug Targets 8:894–905
Gatford KL, Wintour EM, De Blasio MJ, Owens JA, Dodic M (2000) Differential timing for programming of glucose homoeostasis, sensitivity to insulin and blood pressure by in utero exposure to dexamethasone in sheep. Clin Sci 98:553–560
Guzmán C, Cabrera R, Cárdenas M, Larrea F, Nathanielsz PW, Zambrano E (2006) Protein restriction during fetal and neonatal development in the rat alters reproductive function and accelerates reproductive ageing in female progeny. J Physiol 572:97–108
Hahn T, Barth S, Graf R, Engelmann M, Beslagic D, Reul JM, Holsboer F, Dohr G, Desoye G (1999) Placental glucose transporter expression is regulated by glucocorticoids. J Clin Endocrinol Metab 84:1445–1452
Harris A, Seckl J (2010) Glucocorticoids, prenatal stress and the programming of disease. Horm Behav 59:279–289
Hewitt DP, Mark PJ, Waddell BJ (2006a) Glucocorticoids prevent the normal increase in placental vascular endothelial growth factor expression and placental vascularity during late pregnancy in the rat. Endocrinology 147:5568–5574
Hewitt DP, Mark PJ, Waddell BJ (2006b) Placental expression of peroxisome proliferator-activated receptors in rat pregnancy and the effect of increased glucocorticoid exposure. Biol Reprod 74:23–28
Holmes MC, Abrahamsen CT, French KL, Paterson JM, Mullins JJ, Seckl JR (2006) The mother or the fetus? 11beta-hydroxysteroid dehydrogenase type 2 null mice provide evidence for direct fetal programming of behavior by endogenous glucocorticoids. J Neurosci 26:3840–3844
Jansson N, Greenwood SL, Johansson BR, Powell TL, Jansson T (2003) Leptin stimulates the activity of the system A amino acid transporter in human placental villous fragments. J Clin Endocrinol Metab 88:1205–1211
Jensen EC, Gallaher BW, Breier BH, Harding JE (2002) The effect of a chronic maternal cortisol infusion on the late-gestation fetal sheep. J Endocrinol 174:27–36
Jones HN, Ashworth CJ, Page KR, McArdle HJ (2006) Cortisol stimulates system A amino acid transport and SNAT2 expression in a human placental cell line (BeWo). Am J Physiol Endocrinol Metab 291:E596–E603
Kenouch S, Lombes M, Delahaye F, Eugene E, Bonvalet JP, Farman N (1994) Human skin as target for aldosterone: coexpression of mineralocorticoid receptors and 11 beta-hydroxysteroid dehydrogenase. J Clin Endocrinol Metab 79:1334–1341
Kumasawa K, Ikawa M, Kidoya H, Hasuwa H, Saito-Fujita T, Morioka Y, Takakura N, Kimura T, Okabe M (2011) Pravastatin induces placental growth factor (PGF) and ameliorates preeclampsia in a mouse model. Proc Natl Acad Sci U S A 108:1451–1455
Langdown ML, Sugden MC (2001) Enhanced placental GLUT1 and GLUT3 expression in dexamethasone-induced fetal growth retardation. Mol Cell Endocrinol 185:109–117
Langley-Evans SC, Philips GJ, Benediktsson R, Gardner DS, Edwards CR, Jackson AA, Seckl JR (1996) Protein intake in pregnancy, placental glucocorticoid metabolism and the programming of hypertension in the rat. Placenta 17:169–172
Lesage J, Blondeau B, Grino M, Bréant B, Dupouy JP (2001) Maternal undernutrition during late gestation induces fetal overexposure to glucocorticoids and intrauterine growth retardation, and disturbs the hypothalamo-pituitary adrenal axis in the newborn rat. Endocrinology 142:1692–1702
Levitt S, Lindsay RS, Holmes MC, Seckl JR (1996) Dexamethasone in the last week of pregnancy attenuates hippocampal glucocorticoid receptor gene expression and elevates blood pressure in the adult offspring in the rat. Neuroendocrinology 64:412–418
Lindsay RS, Lindsay RM, Edwards CR, Seckl JR (1996) Inhibition of 11-beta-hydroxysteroid dehydrogenase in pregnant rats and the programming of blood pressure in the offspring. Hypertension 27:1200–1204
Lucassen PJ, Bosch OJ, Jousma E, Krömer SA, Andrew R, Seckl JR, Neumann ID (2009) Prenatal stress reduces postnatal neurogenesis in rats selectively bred for high, but not low, anxiety: possible key role of placental 11beta-hydroxysteroid dehydrogenase type 2. Eur J Neurosci 29:97–103
Mairesse J, Lesage J, Breton C, Bréant B, Hahn T, Darnaudéry M, Dickson SL, Seckl J, Blondeau B, Vieau D, Maccari S, Viltart O (2007) Maternal stress alters endocrine function of the feto-placental unit in rats. Am J Physiol Endocrinol Metab 292:E1526–E1533
Meyer JS (1983) Early adrenalectomy stimulates subsequent growth and development of the rat brain. Exp Neurol 82:432–446
Mune T, Rogerson FM, Nikkilä H, Agarwal AK, White PC (1995) Human hypertension caused by mutations in the kidney isozyme of 11 beta-hydroxysteroid dehydrogenase. Nat Genet 10:394–399
Murphy VE, Zakar T, Smith R, Giles WB, Gibson PG, Clifton VL (2002) Reduced 11beta-hydroxysteroid dehydrogenase type 2 activity is associated with decreased birth weight centile in pregnancies complicated by asthma. J Clin Endocrinol Metab 87:1660–1668
Newnham JP, Jobe AH (2009) Should we be prescribing repeated courses of antenatal corticosteroids? Semin Fetal Neonatal Med 14:157–163
Nyirenda MJ, Lindsay RS, Nyirenda MJ, Lindsay RS, Kenyon CJ, Burchell A, Seckl JR (1998) Glucocorticoid exposure in late gestation permanently programs rat hepatic phosphoenolpyruvate carboxykinase and glucocorticoid receptor expression and causes glucose intolerance in adult offspring. J Clin Invest 101:2174–2181
O'Regan D, Kenyon CJ, Seckl JR, Holmes MC (2004) Glucocorticoid exposure in late gestation in the rat permanently programs gender-specific differences in adult cardiovascular and metabolic physiology. Am J Physiol Endocrinol Metab 287:E863–E870
Pankevich DE, Mueller BR, Brockel B, Bale TL (2009) Prenatal stress programming of offspring feeding behavior and energy balance begins early in pregnancy. Physiol Behav 98:94–102
Roberts D, Dalziel S (2006) Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev 3, CD004454
Roland BL, Funder JW (1996) Localization of 11beta-hydroxysteroid dehydrogenase type 2 in rat tissues: in situ studies. Endocrinology 137:1123–1128
Roland BL, Krozowski ZS, Funder JW (1995) Glucocorticoid receptor, mineralocorticoid receptors, 11 beta-hydroxysteroid dehydrogenase-1 and -2 expression in rat brain and kidney: in situ studies. Mol Cell Endocrinol 111:1–7
Smith JT, Waddell BJ (2000) Increased fetal glucocorticoid exposure delays puberty onset in postnatal life. Endocrinology 141:2422–2428
Stewart PM, Rogerson FM, Mason JI (1995) Type 2 11 beta-hydroxysteroid dehydrogenase messenger ribonucleic acid and activity in human placenta and fetal membranes: its relationship to birth weight and putative role in fetal adrenal steroidogenesis. J Clin Endocrinol Metab 80:885–890
Stocker C, O'Dowd J, Morton NM, Wargent E, Sennitt MV, Hislop D, Glund S, Seckl JR, Arch JR, Cawthorne MA (2004) Modulation of susceptibility to weight gain and insulin resistance in low birthweight rats by treatment of their mothers with leptin during pregnancy and lactation. Int J Obes Relat Metab Disord 28:129–136
Uldry M, Thorens B (2004) The SLC2 family of facilitated hexose and polyol transporters. Pflugers Arch 447:480–489
Waddell BJ, Benediktsson R, Brown RW, Seckl JR (1998) Tissue-specific messenger ribonucleic acid expression of 11beta-hydroxysteroid dehydrogenase types 1 and 2 and the glucocorticoid receptor within rat placenta suggests exquisite local control of glucocorticoid action. Endocrinology 139:1517–1523
Welberg LA, Seckl JR, Brown RW, Seckl JR (2000) Inhibition of 11beta-hydroxysteroid dehydrogenase, the foeto-placental barrier to maternal glucocorticoids, permanently programs amygdala GR mRNA expression and anxiety-like behaviour in the offspring. Eur J Neurosci 12:1047–1054
Welberg LA, Seckl JR, Holmes MC (2001) Prenatal glucocorticoid programming of brain corticosteroid receptors and corticotrophin-releasing hormone: possible implications for behaviour. Neuroscience 104:71–79
Whorwood CB, Ricketts ML, Stewart PM (1994) Epithelial cell localization of type 2 11 beta-hydroxysteroid dehydrogenase in rat and human colon. Endocrinology 135:2533–2541
Woods LL, Weeks DA (2005) Prenatal programming of adult blood pressure: role of maternal corticosteroids. Am J Physiol Regul Integr Comp Physiol 289:R955–R962
Wyrwoll CS, Mark PJ, Mori TA, Puddey IB, Waddell BJ (2006) Prevention of programmed hyperleptinemia and hypertension by postnatal dietary omega-3 fatty acids. Endocrinology 147:599–606
Wyrwoll CS, Mark PJ, Waddell BJ (2007) Developmental programming of renal glucocorticoid sensitivity and the renin-angiotensin system. Hypertension 50:579–584
Wyrwoll CS, Seckl JR, Holmes MC (2009) Altered placental function of 11beta-hydroxysteroid dehydrogenase 2 knockout mice. Endocrinology 150:1287–1293
Acknowledgments
This work was supported by a Wellcome Trust project grant (WT079009; MCH, JLP, JJM, JRS). We acknowledge the support of the BHF Centre of Research Excellence.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Wyrwoll, C.S. (2014). Developmental Programming and the Placenta: Focusing in on Glucocorticoids. In: Seckl, J., Christen, Y. (eds) Hormones, Intrauterine Health and Programming. Research and Perspectives in Endocrine Interactions, vol 12. Springer, Cham. https://doi.org/10.1007/978-3-319-02591-9_2
Download citation
DOI: https://doi.org/10.1007/978-3-319-02591-9_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-02590-2
Online ISBN: 978-3-319-02591-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)