Abstract
We behold a 78-year-old male patient with a history of arthrosis and a chronic use of oral NSAID’s and opiates. He had been evaluated at the emergency room because of abdominal pain lasting 72 h. At examination, the patient was hypotensive with a good reaction to fluid therapy. Clinical examination showed signs of generalized peritonitis, being confirmed by CT scan with abundant intra-abdominal fluid collections, submesocolic pneumoperitoneum, and air bubbles at the level of the hepatoduodenal ligament. The history was compatible with a perforated duodenal ulcer secondary to NSAID’s use, and subsequently a diagnostic laparoscopy was performed. After abdominal lavage the perforation was closed with surures and an ometoplasty was added. At the fifth postoperative day the patient had severe abdominal pain with tachycardia and hypotension.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Diagnosis and Indication for Surgery
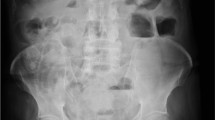
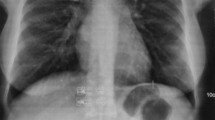
We behold a 78-year-old male patient with a history of arthrosis and a chronic use of oral NSAID’s and opiates. He had been evaluated at the emergency room because of abdominal pain lasting 72 h. At examination, the patient was hypotensive with a good reaction to fluid therapy. Clinical examination showed signs of generalized peritonitis, being confirmed by CT scan with abundant intra-abdominal fluid collections, submesocolic pneumoperitoneum, and air bubbles at the level of the hepatoduodenal ligament. The history was compatible with a perforated duodenal ulcer secondary to NSAID’s use, and subsequently a diagnostic laparoscopy was performed.
Operation
A generalized peritonitis with a perforation larger than 1 cm at the level of the duodenal bulb was found. After abdominal lavage, the perforation was closed with sutures and an omentoplasty was added. Moreover, the subhepatic space was drained.
Postoperative Course: Identification and Treatment of the Complication
At the fifth postoperative day, the patient had severe abdominal pain with a tachycardia and hypotension. The complete blood count showed 23,000 leucocytes, 98 % of them segmented, a hemoglobin of 14 g/dL, and mild coagulation alterations. The abdominal CT scan with oral contrast (gastrographin) showed leakage of contrast at the duodenal level (Fig. 16.1).
A supra-umbilical laparotomy found a dehiscence of the primary suture with an important generalized peritonitis. The antrum of the stomach and the duodenal bulb were resected with use of a stapler, and both the gastric and duodenal stump staple lines were reinforced with PDS continuous sutures. A reconstruction by means of a Roux-Y gastrojejunostomy was performed. The patient recovered slowly on the Intensive Care Unit and could start with oral feeding and medication progressively after 3 weeks.
Discussion
Perforated duodenal ulcers (Illustration 16.1) that cover more than 1/3 of the circumference are not suitable to primary suture reparation due to the high risk of leakage. Moreover the first choice is the horizontal closure and omentum plasty with adequate use of drains. Gastric resection will be used only exceptionally. Perforations equal or shorter than 1/3 of the circumference are suitable for primary suture and omentoplasty.
Perforated duodenal ulcers that cover more than 1/3 of the circumference are not suitable to primary suture reparation due to the high risk of leakage. Perforations equal or shorter than 1/3 of the circumference are suitable for primary suture and omentoplasty. In the case of leakage a partial gastrectomy should be done with a Roux-en-Y anastomosis and adequate drainage
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Sabrido, J.L.G., Jimenez, W.V. (2014). Case on Leakage After Closure of a Duodenal Perforation. In: Cuesta, M., Bonjer, H. (eds) Case Studies of Postoperative Complications after Digestive Surgery. Springer, Cham. https://doi.org/10.1007/978-3-319-01613-9_16
Download citation
DOI: https://doi.org/10.1007/978-3-319-01613-9_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-01612-2
Online ISBN: 978-3-319-01613-9
eBook Packages: MedicineMedicine (R0)