Abstract
Small chemical compounds and certain metal ions can activate T cells, resulting in drug hypersensitivity reactions that are a main problem in pharmacology. Mostly, the drugs generate new antigenic epitopes on peptide-major histocompatibility complex (MHC) molecules that are recognized by the T-cell antigen receptor (TCR). In this review we discuss the molecular mechanisms of how the drugs alter self-peptide-MHC, so that neo-antigens are produced. This includes (1) haptens covalently bound to peptides presented by MHC, (2) metal ions and drugs that non-covalently bridge self-pMHC to the TCR, and (3) drugs that allow self-peptides to be presented by MHCs that otherwise are not presented. We also briefly discuss how a second signal—next to the TCR—that naïve T cells require to become activated is generated in the drug hypersensitivity reactions.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Antigen Processing
- Small Chemical Compound
- Drug Hypersensitivity Reaction
- Hapten Recognition
- Hypervariable Loop
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
3.1 Introduction
Adverse drug reactions are a major health problem worldwide, but they are difficult to predict. The propensity for an individual to develop a reaction depends on the chemistry of the drugs or chemicals, on environmental factors, and on the biology of the patient. A good proportion of these reactions are immune mediated, which are also called allergic drug reactions or drug hypersensitivity reactions. These drug hypersensitivity reactions are due to several distinct immune mechanisms, but all types eventually involve stimulation of T cells by the drug.
For a T-cell-dependent immune response to occur, the drug must stimulate the T-cell antigen receptor (TCR). Drugs, which are usually small chemical compounds of low molecular weight (less than 1,000 Da) and metal ions, are thought to be too small to be antigenic per se. How they are able to stimulate an immune response often is an important open question left to answer.
The TCR is composed of the TCRαβ (or TCRγδ), CD3εδ, CD3εγ, and CD3ζζ dimers (Alarcon et al. 2003) (Fig. 3.1a). TCRαβ possesses variable immunoglobulin domains that bind the ligand, an antigenic peptide bound to major histocompatibility complex (pMHC) molecules (Garboczi et al. 1996; Garcia et al. 1996) (Fig. 3.1b). Foreign peptides, such as derived from viruses or bacteria, presented by MHC have a high affinity for their appropriate TCR and thus elicit an immune response. Peptides derived from endogenous proteins (self-peptides) are also presented. However, due to negative selection processes in the thymus, mature T cells only show weak affinity to self-peptide-MHC, so that T cells are not stimulated and autoimmune diseases are prevented. In addition, superantigens can bridge MHC and TCR peptide independently and stimulate T cells (Fig. 3.1c).
The T-cell antigen receptor (TCR). (a) The TCR comprises the pMHC-binding TCRαβ and the signal-transducing CD3εδ, CD3εγ, and CD3ζζ dimers. (b) Foreign peptide-MHC has a high affinity for the responding TCR. The peptide and the MHC molecule have contacts with TCRαβ, triggering intracellular signaling events, such as the activation of PLCγ and other signaling proteins, leading to T-cell activation. (c) Superantigens simultaneously bind to MHC in a peptide-independent manner and to the constant regions of TCRαβ. Thus, pMHC is bridged to the TCR largely independent of pMHC-TCRαβ contacts. Superantigen stimulation leads to the activation of PLCβ and other signaling proteins, resulting in T-cell activation
The CD3 chains contain tyrosine residues in their cytoplasmic tails, that are phosphorylated upon successful ligand binding to TCRαβ and that transmit the signal inside the cell. Phosphorylation of the tyrosines in these cytoplasmic tails is the critical event initiating signaling cascades. Phosphotyrosines serve as binding sites for signaling proteins with Src-homology 2 (SH2) domains.
The molecular mechanism as to how ligand binding induces CD3 phosphorylation is still a matter of debate. In the conformational change models (Aivazian and Stern 2000; DeFord-Watts et al. 2011; Gil et al. 2002; Minguet et al. 2007; Schamel et al. 2006; Xu et al. 2008), pMHC binding induces a structural change in CD3 that enables phosphorylation of the cytoplasmic domains. In other models the kinase-phosphatase equilibrium is disturbed in the vicinity of the TCR by excluding phosphatases (Choudhuri and van der Merwe 2007; Choudhuri et al. 2005; Davis and van der Merwe 2006; James and Vale 2012) or by enhancing the concentration of kinases (Boniface et al. 1998; Cochran et al. 2000; Irvine et al. 2002). These models are discussed in detail in the preceding review “Activation of the TCR complex by peptide-MHC and superantigens.”
Here, we want to discuss models, which have emerged in the recent years to explain how small chemicals or metals can stimulate the TCR.
3.1.1 Chemicals Acting as Haptens
The term “hapten” was introduced by Landsteiner and Jacobs in 1935. Haptens are chemically reactive compounds that form a covalent bond with endogenous proteins. In 1992 it was demonstrated that hapten recognition by T cells required covalent hapten attachment to MHC-associated peptides (Ortmann et al. 1992). In general hapten-modified proteins are processed by the antigen-presenting machineries and haptenated peptides displayed on MHC class I or II to T cells. In contrast to self-pMHC, which only weakly binds to the TCR and does not stimulate T cells (Fig. 3.2a), haptenated self-pMHC can possess strong binding to an appropriate TCR, and the T cell is stimulated (Fig. 3.2b). These haptenated self-pMHCs were absent during thymocyte development and negative selection, so that the specific TCRs reacting to these haptenated self-pMHCs were not removed from the T-cell population. One example for haptens are β-lactam antibiotics, such as penicillin, which covalently bind to lysine residues of many proteins, such as serum albumin (Batchelor et al. 1965; Jenkins et al. 2009; Levine and Ovary 1961; Schneider and De Weck 1965). One study, using the synthetic penicillin Flucloxacillin, showed that the modification of the lysine residues in human serum albumin occurs in a dose-, time-, and site-dependent manner (Jenkins et al. 2009). However, the exact mechanisms for the immune responses to penicillin are still not clear and create difficulties in the development of effective diagnostics methods (Blanca et al. 2009).
pMHC-TCRαβ interactions mediated by small chemical compounds I. (a) Negative selection in the thymus ensures that self-peptide-MHC only has a weak affinity for TCRs in peripheral T cells. Self-pMHC does not perfectly fit to TCRαβ, thus not triggering their TCR. (b) Haptens bind covalently to endogenous proteins, thus generating haptenated self-peptides that together with MHC can form high affinity ligands for the TCR. (c) Transitional metal ions or drugs can non-covalently bind to the common self-peptide-MHC surface and thus potentially generate a high affinity ligand for the TCR. (d) Metal ions or drugs might also non-covalently bind to the MHC only. This could also form a complementary structure to some TCRαβ, forming a high affinity ligand. (e) Similar to superantigens, Fig. 3.1c, metal ions or drugs might bridge MHC with TCRαβ with high affinity without the involvement of the peptide. Thus, a large fraction of MHC might become competent in stimulation of TCRs. The stimulation of PLCγ (or PLCβ in case of superantigen-like ions/drugs) and other intracellular signaling molecules induced by high affinity TCR binding is indicated. This leads to activation of the T cell
3.1.2 Chemicals Acting as Prohaptens
Prohaptens are chemicals that only become active after a metabolic reaction. Often bioactivation of prohaptens involves oxidative processes, with the cytochrome P450-dependent metabolism playing a major role. In the liver, for example, sulfamethoxazole is converted by P450 to sulfamethoxazole hydroxylamine (Cribb and Spielberg 1992), and autooxidation of the latter compound generates the metabolite nitroso sulfamethoxazole (SMX-NO), which reacts with cysteine residues of proteins (Callan et al. 2009). Indeed, the peptides derived from the SMX-NO-modified proteins after antigen processing can possess high affinity for the appropriate TCR and thus are potent antigens to the specific T cells (Castrejon et al. 2010). Prohaptens are a major problem for drug development as the different metabolic systems in a whole organism have to be investigated to make sure that an initially nonreactive drug does not become reactive upon metabolism.
3.1.3 Haptens as Tools in Basic Research
Traditionally haptens have been an important tool in studying the immune response. For example, trinitrophenol and dinitrophenol have been used to demonstrate the exquisite specificity of the immune system (Weltzien et al. 1996). More recently, haptenated peptides were synthesized to generate TCR antigens with defined properties. For example, photoreactive 4-azidobenzoic acid on the lysine of the peptide SYIPSAEKI was used and the haptenated peptide bound to MHC class I. Specific TCRs could bind, and using a short pulse of UV light, a covalent link between the peptide-MHC molecule and the bound TCR was made, thus “freezing” the otherwise transient peptide-MHC-TCR interaction (Gregoire et al. 1996; Luescher et al. 1995). Using this system we could show that bivalent peptide-MHC binding was required to induce an activatory conformational change in the CD3 subunits of the TCR (Minguet et al. 2007).
3.1.4 Transitional Metal Ions
Nickel (Ni) allergy is the most common and best studied of all metal hypersensitivities, again stimulating T cells. Reactions to other metals such as cobalt (Co), chromium (Cr), platinum (Pt), beryllium (Be), mercury (Hg), and gold (Au) are also reported. These transitional metals are only active as ions (e.g., Ni2+) after their oxidation that can take place on the skin. Metal ions cannot form covalent bonds to peptides and thus are not classical haptens. Instead, metal ions form geometrically highly defined non-covalent coordination bonds with four or six electron donors. The electron donors are mainly nitrogen or oxygen in the amino acid side chains of proteins (Zhang and Wilcox 2002). Thus, metal ions can form very specific complexes with proteins. Ni is studied best (Thierse et al. 2005) and thus serves as an example here.
T-cell activation by Ni-treated APCs did not require antigen processing in some cases (Moulon et al. 1995), being in contrast to the classical haptens. In some cases, Ni bound to the MHC molecule and the peptide, thus forming a new surface to be recognized by the TCR (Fig. 3.2c) (Lu et al. 2003). This might require a certain MHC haplotype, a limited set of peptides and some specific TCR. However, if the hypervariable regions of the TCR are not required to make the contact, then a large number of different TCRs (e.g., those containing a certain Vα and/or Vβ segment) might be stimulated (Vollmer et al. 1997). Unfortunately, a crystal structure of a pMHC-Ni-TCRαβ complex does not exist. However, mimotopic peptides have been used to substitute for the Ni and the self-peptide. The structure shows that the same diagonal orientation of the pMHC-TCRαβ interaction as for the classical pMHC-TCRαβ exists (Yin et al. 2012). This might suggest that the canonical PLCγ pathway is used (Fig. 3.2c). Unfortunately, it is unknown whether metal ions also allow other orientations than the diagonal one. In this case the interaction might resemble more the one of superantigen-mediated TCR activation and thus also activate PLCβ (Bueno et al. 2006, 2007).
It could also be possible that the metal ion only contacts MHC and TCR (Fig. 3.2d).
In another case, Ni activated the TCR with the correct MHC haplotype, but independent of any peptide (Gamerdinger et al. 2003). Thus, it was proposed that Ni acted in a similar manner as superantigens (Fig. 3.2e). However, in this case the hypervariable regions of the TCR were used as a contact site; thus, only very few TCRs might be activated. This is in contrast to superantigens that can activate all TCRs of a given Vβ region (Fraser and Proft 2008; Petersson et al. 2004). It was suggested that self-pMHC first binds to the TCR and that Ni then stabilizes the complex, in order to generate a high affinity interaction (Thierse et al. 2005). Whether in these cases PLCβ is simulated is unknown.
3.1.5 The “Pharmacological Interaction of Drugs with Immune Receptors (p-i) Concept”
The mechanisms of generating high affinity pMHC ligands for the TCR that we have just discussed for metal ions (Fig. 3.2) might also hold true for small organic compounds that do not covalently bind to peptides but still activate T-cell responses. These mechanisms were proposed in the “pharmacological interaction of drugs with immune receptors (p-i) concept” (Adam et al. 2011; Pichler 2005) and have gained much experimental support in the last years.
This model accounts for the observation that T cells could be activated, in an MHC-dependent mechanism, even in the presence of glutaraldehyde-fixed APCs (unable to process antigens) and the nonreactive drug (Schnyder et al. 1997; Zanni et al. 1998). Furthermore, the speed in which T cells could be activated (visualized by calcium influx) after introduction of the drug was too fast for antigen processing to have occurred (Zanni et al. 1998). Thus, these chemicals form reversible, non-covalent bonds (electric, van der Waals, hydrophobic, and hydrogen bonding forces) with pMHC and TCRαβ.
3.1.6 Drugs Binding Non-covalently to pMHC
Strong associations between drug hypersensitivity reactions and specific HLA alleles (human leukocyte antigen, HLA, is the name for human MHC) have been described, although the exact mechanisms for the TCR-stimulating activity of the drugs are often unclear. For example, strong associations between HLA-B*5801 and allopurinol-induced or HLA-B*1502 and carbamazepine-induced Stevens-Johnson syndrome or between HLA-B*5701 and flucloxacillin-induced reactions have been reported (Chung et al. 2004; Daly et al. 2009; Tassaneeyakul et al. 2009). In fact, carbamazepine seems to bind directly but non-covalently to endogenous peptide-loaded HLA-B*1502 (Wei et al. 2012; Yang et al. 2007). Thus, the pMHC-binding mechanisms shown in Fig. 3.2c, d might hold true. The 5-carboxamide chemical moiety of carbamazepine was seen to be required for presentation with HLA-B*1502, and three key residues in the peptide-binding groove of HLA-B*1502 were identified (Wei et al. 2012).
3.1.7 Drugs Altering the Self-Peptide Repertoire Bound to MHC
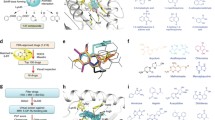
The antiviral drug abacavir causes severe adverse reactions exclusively in HIV-infected individuals expressing HLA-B*5701. As one example for personalized medicine, it is now common practice to genotype a patient for HLA-B*5701 before prescribing abacavir. The adverse reactions are mediated by the activation of cytokine-producing cytotoxic CD8+T cells, and the specificity of the abacavir-HLA interaction was mapped to the F pocket of the peptide-binding cleft of the MHC molecule (Chessman et al. 2008). Several groups showed recently that abacavir binds non-covalently to amino acid residues within the F pocket and thus changes the shape and chemistry of the cleft (Illing et al. 2012; Ostrov et al. 2012), changing the repertoire of self-peptides bound to and presented by HLA-B*5701 (Fig. 3.3a). The X-ray crystal structure of HLA-B*5701 bound to pep-V in the presence of abacavir suggests that the peptide is bound in the MHC molecule in a normal antigen conformation allowing for conventional pMHC-TCR interaction (Ostrov et al. 2012). So, self-peptides, that can bind to HLA-B*5701 only in the presence of abacavir, will then form new pMHC complexes not present in the thymus during negative selection of T cells. Thus, the abacavir hypersensitivity syndrome is a model of drug-induced autoimmunity in which the drug alters the self-peptide repertoire presented by MHC and so drives responses of T cells recognizing these neo-self epitopes (Illing et al. 2012; Norcross et al. 2012; Ostrov et al. 2012).
pMHC-TCRαβ interactions mediated by small chemical compounds II. (a) In at least one documented case, the drug binds to the peptide-binding cleft of the MHC molecule. This allows peptides that otherwise cannot bind to the MHC, to bind and be presented. Since these new self-peptides are not presented in the thymus, reactive T cells are present in the periphery. (b) A drug or metal ion might influence proteins of the antigen processing pathways, such that new self-peptides are made and presented on MHC. (c) As seen in Fig. 3.2, metal ions or drugs can bind to pMHC and thus create a high affinity docking site for specific TCRs. (d) The same pMHC-drug-TCRαβ complex as in (c) can be accomplished, if the drug (or metal ion) binds to TCRαβ. TCR-induced downstream signaling via PLCγ and other pathways is indicated
A different mechanism for the presentation of new self-peptides was suggested for metal ions, in cases where antigen processing was required to stimulate Ni-specific T cells by APCs. It was suggested that the presence of Ni altered antigen processing, so that new self-peptides are presented (Fig. 3.3b). Thus, the T cells might recognize these Ni-induced cryptic self-peptides, but not Ni itself (Griem et al. 1998).
3.1.8 Drugs Binding to TCRαβ
In principle drugs that bridge pMHC and TCRαβ (Fig. 3.2c, d, e) could have a higher affinity for pMHC or a higher affinity for TCRαβ, thus either first binding to pMHC or to TCRαβ before the pMHC-drug-TCRαβ complex forms. At first sight, it might seem irrelevant for the complex, and thus for T-cell activation, whether pMHC or TCRαβ binds first (Fig. 3.3c, d). However, the flexibility of the large TCRαβ hypervariable loops reduces the on-rate of the pMHC-TCR interaction and thus might act negatively on T-cell activation (Aleksic et al. 2010). If the drug binds first to TCRαβ and thereby fixes the conformation of the hypervariable loops in the pMHC-permissive binding state, then the on-rate would be enhanced and T-cell activation would be favored. Thus, although hypothetical, drug binding to TCRαβ first might have different effects than binding to pMHC first.
The antibacterial sulfonamide sulfamethoxazole (SMX) is one of the drugs suggested to bind mainly or firstly to the TCR (in addition, to be a prohapten). TCRs from several SMX-specific T-cell clones isolated from patients with hypersensitivity to SMX reacted to SMX only in the presence of APCs indicating that the TCR stimulation by the drug was MHC dependent but antigen processing independent (Depta et al. 2004). Recent modeling of the drug-TCRαβ interaction suggested several candidate SMX binding sites on the CDR2 and CDR3 hypervariable loops of the TCRα and TCRβ chains (Pichler et al. 2011). Thus, SMX might be one example in which the drug binds stably to TCRαβ (Fig. 3.3d). Since the MHC-bound peptide did not affect the reactivity of SMX-specific T cells (Burkhart et al. 2002), the drug-TCRαβ complex might bind to the MHC molecule without the involvement of the peptide, thus resembling the way that superantigens use to bride TCRs to MHCs (Figs. 3.1c and 3.2e) with the difference that superantigens do not bind to the CDR loops of TCRαβ.
3.1.9 Drug-Induced MHC-Independent TCR Triggering
TCRs can be activated independently of pMHC, such as multivalent anti-TCRαβ and anti-CD3 antibodies (Chang et al. 1981; Kaye and Janeway 1984) or activation of a chimeric TCR by artificial ligands (Minguet et al. 2007). Even in vivo MHC-independent TCR activation was shown. In mice deficient for MHC class I, MHC class II, the coreceptors CD4 and CD8 thymocyte selection produced mature αβ T cells recognizing ligands independently of MHC (Van Laethem et al. 2007). The TCRs of two T-cell clones derived from these mice recognized glycosylation-dependent epitopes of the self-protein CD155 (Tikhonova et al. 2012). Thus, it is possible that drugs could bind to some endogenous proteins that are not pMHC, thereby creating new ligands for the TCRαβ or CD3 that could stimulate T cells in an MHC-independent manner.
3.1.10 The Second Signal of T-Cell Activation
The theory stipulating that an immune cell needs two signals to be activated was first developed in 1970 (Bretscher and Cohn 1970). TCR triggering is an important step in naïve T-cell activation, but it is usually not sufficient to release the T cells (αβ T cells) from their quiescent state. If TCR triggering (signal 1) is the only signal, the naïve cells usually become anergic and cannot be stimulated further (Jenkins et al. 1990; Schwartz 2003). To avoid the anergic, nonresponsive state, naïve T cells require signal 2, provided by a costimulatory receptor such as CD28 (Rudd et al. 2009). In addition, other members of this family (CD2, ICOS) or of the tumor necrosis factor receptor family (including OX40 and 4-1BB) have been shown to be critical as stimulatory co-signals for T-cell activation (Sharpe 2009). So, a small chemical should require the presence of a costimulatory signal, in order to stimulate naïve T cells inducing proliferation and effector functions. Very often, in drug/metal hypersensitivities, the drug or metal also activates the innate immune system leading to the expression of costimulatory ligands by the APCs. Alternatively, the second signal could come from an ongoing infection or autoimmune reaction that takes place at the same time.
However, it is quite possible to imagine that some chemicals would directly stimulate effector or memory T cells where the requirement for a costimulatory signal is smaller (Boesteanu and Katsikis 2009; Kannan et al. 2012), thus overcoming the requirement for simultaneous stimulation of the innate immune system. In addition, effector or memory T cells have a lower affinity threshold for activation than naïve T cells (Bachmann et al. 1999; Cho et al. 1999; Iezzi et al. 1998; Kedl and Mescher 1998; Zimmermann et al. 1999) and respond to lower amounts of antigen than naïve T cells (Kimachi et al. 1997; London et al. 2000; Pihlgren et al. 1996; Rogers et al. 2000). The increased sensitivity to antigenic stimulation by effector and memory cells is partly caused by enhanced pre-clustering of the TCR (Kumar et al. 2011). This pre-clustering increases the avidity towards pMHC (Molnar et al. 2010, 2012). So an effector or memory T cell could be activated by a chemical without the need for a high affinity pMHC interaction with the TCR or even the need for costimulation.
3.2 Conclusion
The molecular mechanisms that small chemical compounds or metal ions use, in order to generate novel peptide-MHC surfaces that can bind with high affinity to TCRs, is an important topic in pharmacologic research. Beginning with the discovery that haptens can covalently bind to proteins whose peptides are presented by MHC in the last century, up to the recent demonstration that a drug altered the kind of self-peptides that are presented by a certain MHC haplotype, a number of different mechanisms have emerged. We believe that novel mechanisms will be discovered in the next years and decades. Detailed insight into these mechanisms might help in treating drug hypersensitivity reactions.
References
Adam J, Pichler WJ, Yerly D (2011) Delayed drug hypersensitivity: models of T-cell stimulation. Br J Clin Pharmacol 71:701–707
Aivazian D, Stern LJ (2000) Phosphorylation of T cell receptor zeta is regulated by a lipid dependent folding transition. Nat Struct Biol 7:1023–1026
Alarcon B, Gil D, Delgado P, Schamel WW (2003) Initiation of TCR signaling: regulation within CD3 dimers. Immunol Rev 191:38–46
Aleksic M, Dushek O, Zhang H, Shenderov E, Chen JL, Cerundolo V, Coombs D, van der Merwe PA (2010) Dependence of T cell antigen recognition on T cell receptor-peptide MHC confinement time. Immunity 32:163–174
Bachmann MF, Barner M, Viola A, Kopf M (1999) Distinct kinetics of cytokine production and cytolysis in effector and memory T cells after viral infection. Eur J Immunol 29:291–299
Batchelor FR, Dewdney JM, Gazzard D (1965) Penicillin allergy: the formation of the penicilloyl determinant. Nature 206:362–364
Blanca M, Romano A, Torres MJ, Fernandez J, Mayorga C, Rodriguez J, Demoly P, Bousquet PJ, Merk HF, Sanz ML, Ott H, Atanaskovic-Markovic M (2009) Update on the evaluation of hypersensitivity reactions to betalactams. Allergy 64:183–193
Boesteanu AC, Katsikis PD (2009) Memory T cells need CD28 costimulation to remember. Semin Immunol 21:69–77
Boniface JJ, Rabinowitz JD, Wülfing C, Hampl J, Reich Z, Altman JD, Kantor RM, Beeson C, McConnell HM, Davis MM (1998) Initiation of signal transduction through the T cell receptor requires the peptide multivalent engagement of MHC ligands. Immunity 9:459–466
Bretscher P, Cohn M (1970) A theory of self-nonself discrimination. Science 169:1042–1049
Bueno C, Lemke CD, Criado G, Baroja ML, Ferguson SS, Nur-Ur Rahman AK, Tsoukas CD, McCormick JK, Madrenas J (2006) Bacterial superantigens bypass Lck-dependent T cell receptor signaling by activating a Ga11-dependent, PLC-b-mediated pathway. Immunity 25:67–78
Bueno C, Criado G, McCormick JK, Madrenas J (2007) T cell signalling induced by bacterial superantigens. Chem Immunol Allergy 93:161–180
Burkhart C, Britschgi M, Strasser I, Depta JP, von Greyerz S, Barnaba V, Pichler WJ (2002) Non-covalent presentation of sulfamethoxazole to human CD4+ T cells is independent of distinct human leucocyte antigen-bound peptides. Clin Exp Allergy 32:1635–1643
Callan HE, Jenkins RE, Maggs JL, Lavergne SN, Clarke SE, Naisbitt DJ, Park BK (2009) Multiple adduction reactions of nitroso sulfamethoxazole with cysteinyl residues of peptides and proteins: implications for hapten formation. Chem Res Toxicol 22:937–948
Castrejon JL, Berry N, El-Ghaiesh S, Gerber B, Pichler WJ, Park BK, Naisbitt DJ (2010) Stimulation of human T cells with sulfonamides and sulfonamide metabolites. J Allergy Clin Immunol 125(411–418):e414
Chang TW, Kung PC, Gingras SP, Goldstein G (1981) Does OKT3 monoclonal antibody react with an antigen-recognition structure on human T cells? Proc Natl Acad Sci U S A 78:1805–1808
Chessman D, Kostenko L, Lethborg T, Purcell AW, Williamson NA, Chen Z, Kjer-Nielsen L, Mifsud NA, Tait BD, Holdsworth R, Almeida CA, Nolan D, Macdonald WA, Archbold JK, Kellerher AD, Marriott D, Mallal S, Bharadwaj M, Rossjohn J, McCluskey J (2008) Human leukocyte antigen class I-restricted activation of CD8+ T cells provides the immunogenetic basis of a systemic drug hypersensitivity. Immunity 28:822–832
Cho BK, Wang C, Sugawa S, Eisen HN, Chen J (1999) Functional differences between memory and naive CD8 T cells. Proc Natl Acad Sci U S A 96:2976–2981
Choudhuri K, van der Merwe PA (2007) Molecular mechanisms involved in T cell receptor triggering. Semin Immunol 19:255–261
Choudhuri K, Wiseman D, Brown MH, Gould K, van der Merwe PA (2005) T-cell receptor triggering is critically dependent on the dimensions of its peptide-MHC ligand. Nature 436:578–582
Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, Wu JY, Chen YT (2004) Medical genetics: a marker for Stevens-Johnson syndrome. Nature 428:486
Cochran JR, Cameron TO, Stern LJ (2000) The relationship of MHC-peptide binding and T cell activation probed using chemically defined MHC class II oligomers. Immunity 12:241–250
Cribb AE, Spielberg SP (1992) Sulfamethoxazole is metabolized to the hydroxylamine in humans. Clin Pharmacol Therap 51:522–526
Daly AK, Donaldson PT, Bhatnagar P, Shen Y, Pe'er I, Floratos A, Daly MJ, Goldstein DB, John S, Nelson MR, Graham J, Park BK, Dillon JF, Bernal W, Cordell HJ, Pirmohamed M, Aithal GP, Day CP (2009) HLA-B*5701 genotype is a major determinant of drug-induced liver injury due to flucloxacillin. Nat Genet 41:816–819
Davis SJ, van der Merwe PA (2006) The kinetic-segregation model: TCR triggering and beyond. Nat Immunol 7:803–809
DeFord-Watts LM, Dougall DS, Belkaya S, Johnson BA, Eitson JL, Roybal KT, Barylko B, Albanesi JP, Wulfing C, Van Oers NS (2011) The CD3 zeta subunit contains a phosphoinositide-binding motif that is required for the stable accumulation of TCR-CD3 complex at the immunological synapse. J Immunol 186:6839–6847
Depta JP, Altznauer F, Gamerdinger K, Burkhart C, Weltzien HU, Pichler WJ (2004) Drug interaction with T-cell receptors: T-cell receptor density determines degree of cross-reactivity. J Allergy Clin Immunol 113:519–527
Fraser JD, Proft T (2008) The bacterial superantigen and superantigen-like proteins. Immunol Rev 225:226–243
Gamerdinger K, Moulon C, Karp DR, Van Bergen J, Koning F, Wild D, Pflugfelder U, Weltzien HU (2003) A new type of metal recognition by human T cells: contact residues for peptide-independent bridging of T cell receptor and major histocompatibility complex by nickel. J Exp Med 197:1345–1353
Garboczi DN, Ghosh P, Utz U, Fan QR, Biddison WE, Wiley DC (1996) Structure of the complex between human T-cell receptor, viral peptide and HLA-A2. Nature 384:134–141
Garcia KC, Degano M, Stanfield RL, Brunmark A, Jackson MR, Peterson PA, Teyton L, Wilson IA (1996) An alphabeta T cell receptor structure at 2.5 A and its orientation in the TCR-MHC complex. Science 274:209–219
Gil D, Schamel WW, Montoya M, Sanchez-Madrid F, Alarcon B (2002) Recruitment of Nck by CD3 epsilon reveals a ligand-induced conformational change essential for T cell receptor signaling and synapse formation. Cell 109:901–912
Gregoire C, Lin SY, Mazza G, Rebai N, Luescher IF, Malissen B (1996) Covalent assembly of a soluble T cell receptor-peptide-major histocompatibility class I complex. Proc Natl Acad Sci U S A 93:7184–7189
Griem P, von Vultee C, Panthel K, Best SL, Sadler PJ, Shaw CF 3rd (1998) T cell cross-reactivity to heavy metals: identical cryptic peptides may be presented from protein exposed to different metals. Eur J Immunol 28:1941–1947
Iezzi G, Karjalainen K, Lanzavecchia A (1998) The duration of antigenic stimulation determines the fate of naive and effector T cells. Immunity 8:89–95
Illing PT, Vivian JP, Dudek NL, Kostenko L, Chen Z, Bharadwaj M, Miles JJ, Kjer-Nielsen L, Gras S, Williamson NA, Burrows SR, Purcell AW, Rossjohn J, McCluskey J (2012) Immune self-reactivity triggered by drug-modified HLA-peptide repertoire. Nature 486:554–558
Irvine DJ, Purbhoo MA, Krogsgaard M, Davis MM (2002) Direct observation of ligand recognition by T cells. Nature 419:845–849
James JR, Vale RD (2012) Biophysical mechanism of T-cell receptor triggering in a reconstituted system. Nature 487:64–69
Jenkins MK, Chen CA, Jung G, Mueller DL, Schwartz RH (1990) Inhibition of antigen-specific proliferation of type 1 murine T cell clones after stimulation with immobilized anti-CD3 monoclonal antibody. J Immunol 144:16–22
Jenkins RE, Meng X, Elliott VL, Kitteringham NR, Pirmohamed M, Park BK (2009) Characterisation of flucloxacillin and 5-hydroxymethyl flucloxacillin haptenated HSA in vitro and in vivo. Proteomics Clin Appl 3:720–729
Kannan A, Huang W, Huang F, August A (2012) Signal transduction via the T cell antigen receptor in naive and effector/memory T cells. Int J Biochem Cell Biol 44:2129–2134
Kaye J, Janeway CA Jr (1984) The Fab fragment of a directly activating monoclonal antibody that precipitates a disulfide-linked heterodimer from a helper T cell clone blocks activation by either allogeneic Ia or antigen and self-Ia. J Exp Med 159:1397–1412
Kedl RM, Mescher MF (1998) Qualitative differences between naive and memory T cells make a major contribution to the more rapid and efficient memory CD8+ T cell response. J Immunol 161:674–683
Kimachi K, Croft M, Grey HM (1997) The minimal number of antigen-major histocompatibility complex class II complexes required for activation of naive and primed T cells. Eur J Immunol 27:3310–3317
Kumar R, Ferez M, Swamy M, Arechaga I, Rejas MT, Valpuesta JM, Schamel WW, Alarcon B, van Santen HM (2011) Increased sensitivity of antigen-experienced T cells through the enrichment of oligomeric T cell receptor complexes. Immunity 35:375–387
Landsteiner K, Jacobs J (1935) Studies on the sensitization of animals with simple chemical compounds. J Exp Med 61:643–656
Levine BB, Ovary Z (1961) Studies on the mechanism of the formation of the penicillin antigen. III. The N-(D-alpha-benzylpenicilloyl) group as an antigenic determinant responsible for hypersensitivity to penicillin G. J Exp Med 114:875–904
London CA, Lodge MP, Abbas AK (2000) Functional responses and costimulator dependence of memory CD4+ T cells. J Immunol 164:265–272
Lu L, Vollmer J, Moulon C, Weltzien HU, Marrack P, Kappler J (2003) Components of the ligand for a Ni++ reactive human T cell clone. J Exp Med 197:567–574
Luescher IF, Vivier E, Layer A, Mahiou J, Godeau F, Malissen B, Romero P (1995) CD8 modulation of T-cell antigen receptor-ligand interactions on living cytotoxic T lymphocytes. Nature 373:353–356
Minguet S, Swamy M, Alarcon B, Luescher IF, Schamel WW (2007) Full activation of the T cell receptor requires both clustering and conformational changes at CD3. Immunity 26:43–54
Molnar E, Deswal S, Schamel WW (2010) Pre-clustered TCR complexes. FEBS Lett 584:4832–4837
Molnar E, Swamy M, Holzer M, Beck-Garcia K, Worch R, Thiele C, Guigas G, Boye K, Luescher IF, Schwille P, Schubert R, Schamel WW (2012) Cholesterol and sphingomyelin drive ligand-independent T-cell antigen receptor nanoclustering. J Biol Chem 287:42664–42674
Moulon C, Vollmer J, Weltzien HU (1995) Characterization of processing requirements and metal cross-reactivities in T cell clones from patients with allergic contact dermatitis to nickel. Eur J Immunol 25:3308–3315
Norcross MA, Luo S, Lu L, Boyne MT, Gomarteli M, Rennels AD, Woodcock J, Margulies DH, McMurtrey C, Vernon S, Hildebrand WH, Buchli R (2012) Abacavir induces loading of novel self-peptides into HLA-B*57: 01: an autoimmune model for HLA-associated drug hypersensitivity. AIDS 26:F21–F29
Ortmann B, Martin S, von Bonin A, Schiltz E, Hoschutzky H, Weltzien HU (1992) Synthetic peptides anchor T cell-specific TNP epitopes to MHC antigens. J Immunol 148:1445–1450
Ostrov DA, Grant BJ, Pompeu YA, Sidney J, Harndahl M, Southwood S, Oseroff C, Lu S, Jakoncic J, de Oliveira CA, Yang L, Mei H, Shi L, Shabanowitz J, English AM, Wriston A, Lucas A, Phillips E, Mallal S, Grey HM, Sette A, Hunt DF, Buus S, Peters B (2012) Drug hypersensitivity caused by alteration of the MHC-presented self-peptide repertoire. Proc Natl Acad Sci U S A 109:9959–9964
Petersson K, Forsberg G, Walse B (2004) Interplay between superantigens and immunoreceptors. Scand J Immunol 59:345–355
Pichler WJ (2005) Direct T-cell stimulations by drugs–bypassing the innate immune system. Toxicology 209:95–100
Pichler WJ, Naisbitt DJ, Park BK (2011) Immune pathomechanism of drug hypersensitivity reactions. J Allergy Clin Immunol 127:S74–S81
Pihlgren M, Dubois PM, Tomkowiak M, Sjogren T, Marvel J (1996) Resting memory CD8+ T cells are hyperreactive to antigenic challenge in vitro. J Exp Med 184:2141–2151
Rogers PR, Dubey C, Swain SL (2000) Qualitative changes accompany memory T cell generation: faster, more effective responses at lower doses of antigen. J Immunol 164:2338–2346
Rudd CE, Taylor A, Schneider H (2009) CD28 and CTLA-4 coreceptor expression and signal transduction. Immunol Rev 229:12–26
Schamel WW, Risueno RM, Minguet S, Ortiz AR, Alarcon B (2006) A conformation- and avidity-based proofreading mechanism for the TCR-CD3 complex. Trends Immunol 27:176–182
Schneider CH, De Weck AL (1965) A new chemical spect of penicillin allergy: the direct reaction of penicillin with epsilon-amino-groups. Nature 208:57–59
Schnyder B, Mauri-Hellweg D, Zanni M, Bettens F, Pichler WJ (1997) Direct, MHC-dependent presentation of the drug sulfamethoxazole to human alphabeta T cell clones. J Clin Investig 100:136–141
Schwartz RH (2003) T cell anergy. Annu Rev Immunol 21:305–334
Sharpe AH (2009) Mechanisms of costimulation. Immunol Rev 229:5–11
Tassaneeyakul W, Jantararoungtong T, Chen P, Lin PY, Tiamkao S, Khunarkornsiri U, Chucherd P, Konyoung P, Vannaprasaht S, Choonhakarn C, Pisuttimarn P, Sangviroon A (2009) Strong association between HLA-B*5801 and allopurinol-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in a Thai population. Pharmacogenet Genom 19:704–709
Thierse HJ, Gamerdinger K, Junkes C, Guerreiro N, Weltzien HU (2005) T cell receptor (TCR) interaction with haptens: metal ions as non-classical haptens. Toxicology 209:101–107
Tikhonova AN, Van Laethem F, Hanada K, Lu J, Pobezinsky LA, Hong C, Guinter TI, Jeurling SK, Bernhardt G, Park JH, Yang JC, Sun PD, Singer A (2012) alphabeta T cell receptors that do not undergo major histocompatibility complex-specific thymic selection possess antibody-like recognition specificities. Immunity 36:79–91
Van Laethem F, Sarafova SD, Park JH, Tai X, Pobezinsky L, Guinter TI, Adoro S, Adams A, Sharrow SO, Feigenbaum L, Singer A (2007) Deletion of CD4 and CD8 coreceptors permits generation of alphabetaT cells that recognize antigens independently of the MHC. Immunity 27:735–750
Vollmer J, Fritz M, Dormoy A, Weltzien HU, Moulon C (1997) Dominance of the BV17 element in nickel-specific human T cell receptors relates to severity of contact sensitivity. Eur J Immunol 27:1865–1874
Wei CY, Chung WH, Huang HW, Chen YT, Hung SI (2012) Direct interaction between HLA-B and carbamazepine activates T cells in patients with Stevens-Johnson syndrome. J Allergy Clin Immunol 129(1562–1569):e1565
Weltzien HU, Moulon C, Martin S, Padovan E, Hartmann U, Kohler J (1996) T cell immune responses to haptens. Structural models for allergic and autoimmune reactions. Toxicology 107:141–151
Xu C, Gagnon E, Call ME, Schnell JR, Schwieters CD, Carman CV, Chou JJ, Wucherpfennig KW (2008) Regulation of T cell receptor activation by dynamic membrane binding of the CD3epsilon cytoplasmic tyrosine-based motif. Cell 135:702–713
Yang CW, Hung SI, Juo CG, Lin YP, Fang WH, Lu IH, Chen ST, Chen YT (2007) HLA-B*1502-bound peptides: implications for the pathogenesis of carbamazepine-induced Stevens-Johnson syndrome. J Allergy Clin Immunol 120:870–877
Yin L, Crawford F, Marrack P, Kappler JW, Dai S (2012) T-cell receptor (TCR) interaction with peptides that mimic nickel offers insight into nickel contact allergy. Proc Natl Acad Sci U S A 109:18517–18522
Zanni MP, von Greyerz S, Schnyder B, Brander KA, Frutig K, Hari Y, Valitutti S, Pichler WJ (1998) HLA-restricted, processing- and metabolism-independent pathway of drug recognition by human alpha beta T lymphocytes. J Clin Invest 102:1591–1598
Zhang Y, Wilcox DE (2002) Thermodynamic and spectroscopic study of Cu(II) and Ni(II) binding to bovine serum albumin. J Biol Inorg Chem 7:327–337
Zimmermann C, Prevost-Blondel A, Blaser C, Pircher H (1999) Kinetics of the response of naive and memory CD8 T cells to antigen: similarities and differences. Eur J Immunol 29:284–290
Acknowledgements
We thank Stefan Martin for discussions on this topic. This work was funded by the EU through grant FP7/2007–2013 (SYBILLA) and the Deutsche-Forschungsgemeinschaft (DFG) through EXC294 (the Center for Biological Signalling Studies, BIOSS).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Basel
About this chapter
Cite this chapter
Louis-Dit-Sully, C., Schamel, W.W.A. (2014). Activation of the TCR Complex by Small Chemical Compounds. In: Martin, S. (eds) T Lymphocytes as Tools in Diagnostics and Immunotoxicology. Experientia Supplementum, vol 104. Springer, Basel. https://doi.org/10.1007/978-3-0348-0726-5_3
Download citation
DOI: https://doi.org/10.1007/978-3-0348-0726-5_3
Published:
Publisher Name: Springer, Basel
Print ISBN: 978-3-0348-0725-8
Online ISBN: 978-3-0348-0726-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)