Abstract
The endoscopic middle ear surgery has evolved over the time course. The usage of the endoscope in middle ear surgery gave a wider and clearer anatomy of middle ear spaces due to a better magnification and to the possibility to look into the hidden spaces. The hidden recesses most likely to cause an undetected residual and recurrence are the sinus tympani, the anterior epitympanic space, and the protympanic spaces can now be explored with a good magnification. This advantage enables us to perform a less invasive and more physiologic surgery of middle ear. This chapter gives a detailed description of the endoscopic middle ear anatomy with description of every compartment, with particular attention to ventilation pathways and middle ear folds. The trans canal access to the tympanic cavity with the endoscope and it is hard to reach extensions have given us the privilege to divert the attention from the less critical area like the mastoid proper to the tympanic cavity (Baki et al., Otolaryngol Head Neck Surg 127:158–162, 2002; Thomassin et al., Laryngoscope 103:939–943, 1993; Badr-El-Dine, Otol Neurotol 23:631–635, 2002; Tarabichi, Am J Otol 18:544–549, 1997; Tarabichi, Laryngoscope 114:1157–1162, 2004; Bowdler and Walsh, Clin Otolaryngol Allied Sci 20:418–422, 1995; Bottril and Poe Am J Otol 16:158–163, 1995; Karhuketo et al., Acta Otolaryngol Suppl 529:34–39, 1997).
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Endoscopic Anatomy of the External Auditory Canal
It is important to inspect the anatomy of the external auditory canal (EAC), the tympanic membrane (TM), and the structures visible through the translucent TM. Understanding the anatomy of temporal bone from the CT scan sections prior to the surgery is of paramount importance. An axis drawn through the ear canal will be directing you to the attic. On removal of the scutum seen in between will give us a wide and open access to the attic, which forms the natural cul de sac of the external auditory canal (Fig. 47.1).
Right ear: Coronal CT section through the external auditory canal (EAC) and middle ear. Note that the axis of the EAC slopes upward. The scutum represents the real “bottom of the EAC” rather than the mesotympanum. If the scutum is removed, this would allow direct access to the attic, the area frequently involved in cholesteatoma growth
The blood vessels of the TM originate from the EAC. They supply in a lateral to medial direction. The skin of EAC and the epithelial layer of the TM form the bleeding elements of the external ear (Fig. 47.2). The friable skin and epithelium of the TM can be seen distinctly in the Fig. 47.3.
Enlargement of the Ear Canal
The axis of the external auditory canal is directed superiorly and the scutum forms the medial end of the ear canal. It is also common to find bony over hangings in the EAC. The location and extent of it should be well noted (Figs. 47.1 and 47.4). Anterior or even an inferior overhang are commonly seen in many anatomical specimens. These can be curated out in all directions to achieve a panoramic view of the annulus using the 0° endoscope, keeping in mind the fact that the bony annulus is very variable in relation to the adjacent critical structures. Always consider the possibility of a high jugular bulb, anterior sigmoid sinus, a low lying dura, and the facial nerve (Figs. 47.5 and 47.6).
Fibrous annulus—The glistening white fibrous annulus is anchored in a bony groove. It is incomplete in the upper posterior part of tympanic membrane. The fibrous annulus will be visible inferiorly and is incomplete at its upper end (Figs. 47.2 and 47.3). The annulus serves as a good landmark for the incision for the vascular strip.
Endoscopic Anatomy of the Middle Ear
After detaching the fibrous layer of the TM from the upper part of malleus handle and mobilizing from the bony sulcus, it is deflected inferiorly (Fig. 47.7). Separate the TM from the malleus handle starting from the lateral short process of the malleus and extending toward the umbo. The posterior malleolar ligament can be seen overlying the chorda tympani (Fig. 47.8).
Endoscopic Anatomy of the Retro Tympanum
On removing the bony annulus posteriorly gives a full access to the facial recess and sinus tympani. The posterior canal wall needs to be almost flushed with the pyramidal eminence. The pyramidal eminence accurately marks the level of the vertical segment of the facial nerve. It is safer to curette the bone superficial to that level. The facial recess present as a small depression on the posterior border of tympanic cavity (Fig. 47.9).
Left ear. Endoscopic view through a transcanal endoscopic access after minor removal of bone; the facial recess (FR) is very shallow and more of a flat depression, superficial to the pyramidal eminence (PE), and the vertical segment of facial nerve (FN). Also note the horizontal segment of the facial nerve
Figures 47.10 and 47.11 shows the retro tympanic anatomy. To see the retro tympanic anatomy clearly, the posterior aspect should face away from you and the axis of the scope’s direction of viewpoints away from you. The presence of a sub pyramidal space and its entry point is to be noted.
The schematic diagram shows the drawing of the sub pyramidal space (sps) (Fig. 47.12) and the variable morphology of the pyramidal eminence (Fig. 47.13) and description.
Variable morphology of the pyramidal eminence (pe) in a right ear demonstrated by two types of perspectives: an anatomic view (a1, b1, c1) and a surgical endoscopic view (a2, b2, c2) through an angled-view scope while looking in the posterior direction. a b c Morphological variations of the pe, sinus tympani (st), and posterior sinus tympani (pts) communicating through the subpyramidal space (sps). Partial morphology of the pe. The subpyramidal space (sps) is communicating with the sinus tympani. Partial morphology of the pe. The subpyramidal space (sps) is communicating with the posterior sinus tympani (pts)
The  refers to the communication of sps; facial nerve (fn); stapes (s); ponticulus (p); promontory (pr); round window (rw); subiculum (su).
refers to the communication of sps; facial nerve (fn); stapes (s); ponticulus (p); promontory (pr); round window (rw); subiculum (su).
The anatomy of the sinus tympani and ponticulus promontorii also varies with each individual. The variable morphology of the sinus tympani and ponticulus promontorii is described with the different types (Figs. 47.14, 47.15, 47.16, and 47.17). The tegmen of the round window niche and anterior and posterior pillars are to be identified on identification of the round window niche (Fig. 47.18).
The variable morphological appearance of the sinus tympani. Facial nerve (fn); posterior sinus tympani (pts); pyramidal eminence (pe); promontory (pr); stapes (s); round window (rw); subiculum (su); jugular bulb (jb); sinus subtympanicus (ss); sinus tympani (st); ridge separating the sinus tympani into two parts (*); superior part of sinus tympani (sts); inferior part of sinus tympani (sti)
Schematic drawing of a “Type C” sinus tympani. The  indicates the posterior extension of the sinus tympani with respect to the third portion of the facial nerve (fn). Chordal ridge (cr); chorda tympani nerve (ctn); lateral tympanic sinus (lts); facial sinus (fs); incus (in); malleus (ma); ponticulus (p); pyramidal eminence (pe); cochlear promontory (pr); posterior sinus tympani (pts); stapedial tendon (st); stapes (s); subiculum (su); round window (rw)
indicates the posterior extension of the sinus tympani with respect to the third portion of the facial nerve (fn). Chordal ridge (cr); chorda tympani nerve (ctn); lateral tympanic sinus (lts); facial sinus (fs); incus (in); malleus (ma); ponticulus (p); pyramidal eminence (pe); cochlear promontory (pr); posterior sinus tympani (pts); stapedial tendon (st); stapes (s); subiculum (su); round window (rw)
(a–c) The variable morphological appearance of the ponticulus promontorii (p). Ridge ponticulus (Type A); incomplete ponticulus (Type B), bridge ponticulus (Type C). Facial nerve (fn); incus (in); ponticulus (p); pyramidal eminence (pe); posterior sinus tympani (pts); cochlear promontory (pr); stapedial tendon (st); stapes (s); subiculum (su); sinus subtympanicus (ss)
Endoscopic Anatomy of the Hypotympanum
In order to view the hypotympanum, a 30° endoscope is preferred with the removal of any inferior bony overhang and enlarging the access to the inferior and the posterior-inferior part of the retro tympanum. The subiculum separates inferior from superior retro tympanum. The subiculum also shows different variations in each specimen (Figs. 47.19, 47.20, and 47.21).
Right ear. Schematic anatomical survey drawing of the retrotympanum and hypotympanum. The finiculus (fi) appears as a bony ridge which arises from the anterior and inferior lip of the round window and separates the inferior retrotympanum from the hypotympanum. The subiculum (su) marks the boundary between the superior and inferior retrotympanum. Right side. Facial nerve (fn); pyramidal eminence (pe); oval window (ow); cochleariform process (cp); sinus tympani (st); ponticulus (p); subiculum (su); posterior pillar (pp); tegmen of round window niche (te); cochlear promontory (pr); Eustachian tube (et); round window (rw); styloid eminence (sty); sinus subtympanicus (ss); anterior pillar (ap); finiculus (fi); jugular bulb (jb)
(a–c) Right ear: Anatomic variations of the subiculum. (A) Ridge subiculum. (B) Bridge subiculum. (C) Absent subiculum, Key to abbreviations: Facial nerve (fn); pyramidal eminence (pe); oval window (ow); cochleariform process (cp); sinus tympani (st); ponticulus (p); subiculum (su); cochlear bridge subiculum (Type B). promontory (pr); sinus subtympanicus (sst); round window (rw); Eustachian tube (et); styloid eminence (sty); ponticulus (p). Absent subiculum (Type C), in which the sinus subtympanicus is confluent with the sinus tympani
Finiculus is a ridge of bone from the anterior and inferior slip of the round window separating the inferior retro tympanum from hypotympanum (Fig. 47.22). The styloid eminence, jugular bulb including the curvature of the basal turn of cochlea can be seen in a well pneumatised infracochlear space.
Anatomical variations of the finiculus (fi). Right side. Ridge finiculus (Type A); Bridge finiculus (Type B). Absent finiculus (Type C). Key to abbreviations: facial nerve (fn); pyramidal eminence (pe); oval window (ow); cochleariform process (cp); sinus tympani (st); ponticulus (p); subiculum (su); round window (r w); cochlear promontory (pr); Eustachian tube (et); styloid eminence (sty); sinus subtympanicus (sst); finiculus (fi); jugular bulb (jb); styloid eminence (sty); ponticulus (p); hypotympanic air cell (hc)
Endoscopic Anatomy of the Epitympanum
After a careful limited atticotomy meticulously, preserving the lateral incudo malleolar ligament and the lateral malleolar ligament on the medial aspect of the scutum. These are two friable ligaments along with the neck of malleus forms the roof and medial aspect of the Prussak’s space Fig. 47.23).
These suspensory ligaments separates the area between scutum and ossicles by forming the lateral part of the epitympanic diaphragm. These ligaments act as the gateway for the spread of attic cholesteatoma (Fig. 47.24).
On extending the atticotomy, the anterior epitympanic space can be seen. The epitympanic space is separated from the supratubal space by the Sheehy’s cog. The tensor fold is seen spreading across the cog and the tensor tympani (TT) (Figs. 47.25, 47.26, 47.27, 47.28, 47.29, and 47.30).
Left ear: The ossicles have been fully exposed within the attic allowing to clearly visualize the incudo-mallear articulation line. Incudo-mallear joint (IMJ); anterior epitympanic space (AES); Sheehy’s cog (COG) separating the supratubal recess from the anterior epitympanic space; tensor tympani fold (TF), partially visible and preventing the attic from direct ventilation via the supratubal recess and the Eustachian tube
Left ear: handle of malleus (HM); supratubal recess (STS); anterior surface of Sheehy’s cog (COG) separating the attic from the supra-tubal recess; vertical segment of the tensor tympani fold (TFV), which—given its entire integrity—closes off the attic from the Eustachian tube; horizontal segment of the tensor tympani fold (TFH) which partially contributes to the floor of the supratubal recess anteriorly; bony encasement of the tensor tympani muscles (TTM); bony annulus (BA); carotid artery (CA)
Endoscopic View down the Eustachian Tube
An angled endoscope is used to look further down into the eustachian tube. The relationship between the carotid artery and the bony canal for TT muscle (Fig. 47.29). The size and depth of the supra tubal recess vary considerably. On rotating further superiorly and posteriorly, the TT fold can be seen separating the supratubal recess from the anterior attic. The position and shape of the TT fold are also highly variable and are related to the size of the supra tubal recess (Fig. 47.30). The TT fold is almost a horizontal structure that closes the anterior attic and separates it from the eustachian tube when the supratubal recess is poorly developed. It begins with the tendon of TT and inserts along a bony ridge formed by the encasement of the TT muscle and extends into the anterior epitympanic spine (Figs. 47.31, 47.32, and 47.33).
Histologic section through a dome-shaped supratubal recess ( ). The outermost plate (
). The outermost plate ( ) of the petrosa; a spur (
) of the petrosa; a spur ( ) projecting toward the mallear head, to which attaches a mucosal fold that stems from the anterior mallear ligament; sheehy’s cog (
) projecting toward the mallear head, to which attaches a mucosal fold that stems from the anterior mallear ligament; sheehy’s cog ( ); tensor tympani folds (
); tensor tympani folds ( ); geniculate ganglion (G); cochlea (C); lateral semicircular canal (L)
); geniculate ganglion (G); cochlea (C); lateral semicircular canal (L)
Left ear: Endoscopic anatomy of the tensor tympani fold in a specimen with a well-developed supratubal recess (STS). The tensor tympani folds are composed of two segments, a vertical part (TFV) that attaches to Sheehy’s cog (COG), and a horizontal part (TFH) that partly contributes to the floor of the supratubal recess anteriorly; bony encasement of the tensor tympani muscle (TTM)
Right ear: Unlike the anatomic specimen shown in Fig. 47.31, this is a poorly developed supratubal recess in a surgical case. View through a 70°-scope, upward and backward. The tensor tympani fold (TF) here, different from the one shown in Fig. 47.31, is almost a horizontal structure. Handle of malleus (HM); tensor tympani muscle (TTM), anterior bony annulus (ABA)
If the supratubal recess is well developed as in this specimen, the tensor tympani then holds two parts. The vertical part attaches to the cog and forms the wall separating the anterior attic from the supratubal recess. The horizontal segment attaches to the TT tendon and the most anterior part of the bony ridge which is formed by the bony canal for the TT muscle. The horizontal part of TT fold also contributes to the floor of the supratubal recess if it is well developed (Figs. 47.31, 47.32, 47.33, and 47.34).
Right ear: Endoscopic close-up view of the tensor tympani fold (TF) shown in Fig. 47.32. Bony encasement of the tensor tympani muscle (TTM); tensor tympani tendon (TTT) inserting on the neck of the malleus. Funnel-shaped entrance to the Eustachian tube ( )
)
The epitympanic ventilation is maintained through the tympanic isthmus formed between the incudo stapedial joint and the TT tendon. A complete TT fold and a closed lateral attic space prevents the ventilation through the anterior attic (Fig. 47.35).
The Incus is removed here to visualize the articular facet with malleus and stapes (Figs. 47.36 and 47.37). The horizontal segment of the facial nerve and the second genu, the lateral semi-circular canal, and remnant of the superior incudal ligament can be seen in the picture (Fig. 47.38).
Left ear: Endoscopic view after transection of the tensor tympani tendon and removal of the malleus handle, the anterior tympanic spine, anterior mallear ligament, and the chorda tympani. Sheehy’s cog (COG); remnant of the tensor tympani fold (TM); insertion point ( ) of the partially removed vertical segment of the tensor tympani fold; insertion point (
) of the partially removed vertical segment of the tensor tympani fold; insertion point ( ) of the completely removed horizontal segment of the tensor tympani fold; supratubal recess (STR); Eustachian tube (ET); cochleariform process (CP); first genu (1G) of the facial nerve and neighbouring geniculate ganglion; lateral semicircular canal (LC)
) of the completely removed horizontal segment of the tensor tympani fold; supratubal recess (STR); Eustachian tube (ET); cochleariform process (CP); first genu (1G) of the facial nerve and neighbouring geniculate ganglion; lateral semicircular canal (LC)
The malleus is nipped above the neck at a superior level to preserve the anterior mallear ligament and the TT tendon. The TT tendon is seen attached to the handle and neck of the malleus (Fig. 47.39) The head of malleus is removed by preserving the suspensory ligaments and mobilizing the handle anteriorly. We can now observe the TT tendon attaching to the neck of malleus, course of chorda tympani (CT) nerve, anterior aperture of the bony canal into which the CT nerve runs into. Note the topographical relationship of the CT nerve to the AML, the anterior tympanic spine, and the attachment of the anterior mallear ligament (Fig. 47.40).
Left ear: The handle of malleus has been mobilized anteriorly to expose the tensor tympani fold which is released from its attachments; the starting point of the white arrows indicate the original position of the fold and the tips show the current point following lateralization of the malleus handle. Tensor tympani tendon (TT); chorda tympani (CT); tensor tympani fold (TF) after dislocation from its original position; anterior mallear ligament (AML)
Upon transecting the TT tendon and the malleus handle, we can very well see the fibers of the horizontal segment of the facial nerve, its first genu after arising from the IAC, relationship of geniculate ganglion (GG), relation of the second genu, the lateral semi-circular canal, and the remnant of TT fold.
References
Baki FA, El Dine MB, El Said L, et al. Sinus tympani endoscopic anatomy. Otolaryngol Head Neck Surg. 2002;127:158–62.
Thomassin JM, Korchia D, Doris JM. Endoscopic guided otosurgery in the prevention of residual cholesteatomas. Laryngoscope. 1993;103:939–43.
Badr-El-Dine M. Value of ear endoscopy in cholesteatoma surgery. Otol Neurotol. 2002;23:631–5.
Tarabichi M. Endoscopic management of acquired cholesteatoma. Am J Otol. 1997;18:544–9.
Tarabichi M. Endoscopic management of limited attic cholesteatoma. Laryngoscope. 2004;114:1157–62.
Bowdler DA, Walsh RM. Comparison of the otoendoscopic and microscopic anatomy of the middle ear cleft in canal wall-up and canal wall-down temporal bone dissections. Clin Otolaryngol Allied Sci. 1995;20:418–22.
Bottril ID, Poe DS. Endoscope-assisted ear surgery. Am J Otol. 1995;16:158–63.
Karhuketo TS, Puhakka HJ, Laippala PJ. Endoscopy of the middle ear structures. Acta Otolaryngol Suppl. 1997;529:34–9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Tarabichi, M., Ansar, A., Kapadia, M., Marchioni, D. (2023). The Endoscopic Anatomy of Temporal Bone. In: Goycoolea, M.V., Selaimen da Costa, S., de Souza, C., Paparella, M.M. (eds) Textbook of Otitis Media. Springer, Cham. https://doi.org/10.1007/978-3-031-40949-3_47
Download citation
DOI: https://doi.org/10.1007/978-3-031-40949-3_47
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-40948-6
Online ISBN: 978-3-031-40949-3
eBook Packages: MedicineMedicine (R0)


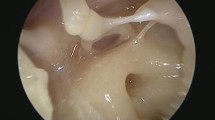













 ) of this specimen are a specific feature of ‘type A’, connecting both the sinus tympani (ST) and posterior tympanic sinus (PTS). Pyramidal eminence (PE)
) of this specimen are a specific feature of ‘type A’, connecting both the sinus tympani (ST) and posterior tympanic sinus (PTS). Pyramidal eminence (PE)






 )
)




















