Abstract
Pressure, airflow, and volume waveforms are the graphical representations of how a breath is delivered to a patient. The changes in these parameters over time show the interaction of the ventilator with the respiratory system.
Useful information can be obtained from a clear understanding of these graphics to monitor the ventilated patient and to modify the parameters of the ventilator to best suit the dynamic needs of the patient.
The aim of the monitoring is not to measure fine variations related to the time factor but to alert the clinician about any dyssynchrony between the patient and the ventilator.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Waveform representations of pressure, flow, or volume vs time are the three scalars that we can find on conventional mechanical ventilators.
Each scalar represents the entire breath from the beginning of inspiration to the end of expiration.
Ventilators measure airway pressure and airway flow. Volume is derived from the flow measurement. Pressure and flow provide most of the information necessary to explain the physical interaction between ventilator and patient [1, 2].
The analysis of the waves may allow the clinician to:
-
Identify asynchrony between the patient and the ventilator during inspiratory phase
-
Identify the control variables set
-
Evaluate the correct setting of expiratory trigger
-
Obtain an indirect estimate of the presence of eventual intrinsic PEEP
-
Evaluate the presence of tracheobronchial secretions
-
Evaluate if the patient is under- or over-assisted.
2 Pressure Versus Time Scalar
This curve represents the pressure in the airway as a function of time.
In the typical graphic displayed on the ventilator, the baseline pressure indicates the EPAP (PEEP) and the maximum pressure at the end of the curve indicates the peak of inspiratory pressure. This can be a fixed or variable amount depending on the mode of ventilation [1, 3, 4] (Fig. 13.1).
It is possible to divide a breath into four phases.
-
1.
In the first part of a respiratory act in pressure support, the ventilator recognizes the inspiratory effort by the inspiratory trigger. In this phase, the effort of the respiratory muscles should be able to overcome the configured inspiratory trigger.
-
2.
Then the ventilator delivers an inspiratory flow until the configured pressure is reached (pressurization phase). During pressure control ventilation, when the configured pressure is reached, the pressure delivered is constant and the pressure scalar is square-shaped. In volume control ventilation, the pressure scalar is ascending due to the rise in pressure with a constant flow pattern (Fig. 13.2) [1, 4, 5].
The inspiratory plateau level is the pressure in the airway under static conditions, or when there is no airflow. It gives us information about reaching the limit between the phase variables and inspiratory pressure reached in the airways.
-
3.
When the flow reaches a set value (cycling point), there is cycling from inspiration to expiration, that is, the end of inspiration. Ideally, the ventilator terminates inspiratory flow in synchrony with the patient’s neural timing, but frequently the ventilator terminates inspiration either too early or too late, relative to the patient’s neural timing. During volume-controlled ventilation, we can adjust variables that affect inspiratory time (e.g., peak flow, tidal volume). During pressure-controlled or pressure-support ventilation, we can adjust variables that affect the end of inspiration (e.g., inspiratory time, expiratory sensitivity).
-
4.
Expiratory phase. The pressure returns to baseline.
3 Flow Versus Time Scalar (Fig. 13.3)
This curve represents the flow in the airway as a function of time.
Inspiratory flow is a positive value on the graph, whereas expiratory flow is a negative value. The area under the curve represents the volume involved during the phases of breathing [1, 4, 6].
The shape of the inspiratory limb of the curve depends on the mode of ventilation (see Fig. 13.2).
In pressure-targeted modes, the peak inspiratory pressure (PIP) and inspiratory time are set and the flow is variable. The shape of the inspiratory flow is decreasing at the beginning of the breath, flow is delivered at a high rate but thendecreases during inspiration, resulting in a descending shape of the curve. Decreasing inspiratory flow is the consequence of inspiration with constant pressure. Pressure-supported modes may also have a sinusoidal flow curve.
In volume-targeted mode, the tidal volume, inspiratory time, and inspiratory flow are set, resulting in a constant flow or square shape to the flow scalar. Then there is a constant inspiratory flow and pressure in the airway increases during inspiration.
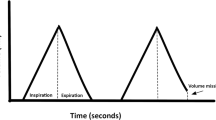
4 Volume Versus Time Scalar (Fig. 13.4)
The volume versus time scalar is the graphical representation of the amount of gas delivered into the lungs by the ventilator over time. It is calculated from the measurement of flow.
The ascending curve is the inspiratory volume and the descending curve is the expiratory volume [1, 3]. In a ventilation pattern without problems, inspiratory and expiratory volumes should be similar.
5 Monitoring Noninvasive Mechanical Ventilation Using Ventilator Waveforms
The pressure and flow scalars provide the clinician with a wealth of information to identify problems with the phases of the ventilation. Following the sequential phases of the respiratory act, different problems can be encountered [2, 7, 8].
5.1 Ineffective Triggering or Ineffective Effort
It is possible to obtain much important information about the critical phase of the supported ventilatory act, that is, the activation of the inspiratory trigger by the patient.
An ineffective triggering is a decrease of pressure with an increase in flow not followed by a ventilatory cycle. In this case, the respiratory rate detected by the ventilator is lower than the real respiratory rate of the patient that is under and poorly attended [9,10,11] (Fig. 13.5).
Ineffective triggering
Cause:
• Intrinsic PEEP if the inspiratory trigger is correct
• Incorrect settings: inspiratory trigger, cycling… If we set an inspiratory trigger too strong we will ask the patient for a hard muscular effort that he/she will not be able to sustain and there will be ineffective inspiratory efforts
• Excessive inspiratory support: the high tidal volume generated does not allow a complete emptying of accumulated air
5.2 Autotriggering
In this case, the ventilator perceives the inspiratory trigger threshold is satisfied even when it is not due to inspiratory efforts but to artifacts. The respiratory rate of the ventilator is higher than the real respiratory rate of the patient that is poorly attended [12] (Fig. 13.6).
5.3 Double Trigger
In this situation, there is a sustained inspiration followed by another sustained inspiration after a very short time (<500 ms) [13] (Fig. 13.7).
5.4 Rise Time
Once the inspiratory trigger is started, it begins the phase of pressurization of the airway. During this time, it is possible to modify the “pressure rise time” In acute respiratory failure, most patients need to be supported in the ventilatory act with the lowest possible latency and as fast as possible modifying the ramp before increasing inspiratory support [11] (Fig. 13.8).
5.5 Hang-Up
Another classical problem with NIV is hang-up, that is, a prolonged inspiration due to leaks of the circuit. In the flow wave, there is an initial fall of the flow and then a plateau where the patient does not reach the fixed expiratory flow point to move to expiration.
Cause:
5.6 Expiratory Cycling
At the end of inspiration, the analysis of waveforms can provide information about the correct configuration of expiratory cycling.
Cycle asynchrony usually occurs when there is a mismatch between the patient’s inspiratory time (i.e., neural time) and the ventilator’s inspiratory time.
If we set a percentage of expiratory flow too high, the neural time could be greater than the ventilator’s inspiratory time (Fig. 13.10).
Consequently the ventilator ends flow delivery, but the patient’s inspiratory effort continues. Premature cycling leads to a transient inversion of flow in the expiratory portion of the flow waveform. If the patient’s effort exceeds the trigger threshold, it can activate another breath, generating a double trigger. The risk is the fall of tidal expiratory volume because of an excessive reduction of inspiratory time (Fig. 13.11).
If we set a percentage of expiratory flow too low, the patient initiates the exhalation while the ventilator is still delivering flow (prolonged or delayed cycling). Delayed cycling leads to a spike in pressure in late inspiration on the pressure scalar waveform. The airway of the patient remains pressurized for too long with side effects on comfort and expiratory time and dynamic hyperinflation [11, 14, 15].
5.7 Hyperdynamic Inflation
The shape of expiratory limb of the flow curve is affected by the resistance to airflow and the compliance of the lung. Under normal conditions, the expiratory limb of the curve returns to a baseline of zero flow prior to the next breath being initiated. However, if expiration of air is still ongoing when inspiration starts, then the lungs are not emptying completely and air trapping occurs. The persistence of flow at the end of the expiration shows that the pulmonary system is above the residual functional capacity and the flow is generated by positive elastic return of the respiratory system at the end of the exhalation (PEEPi). The analysis of the waves does not allow measuring PEEPi but provides an estimation of the possible presence of PEEPi [16] (Fig. 13.12).
5.8 Volume Scalar
The analysis of volume scalar is a completion of the analysis of pressure and flow scalar. It can be used to evaluate the volume of a patient’s spontaneous breath and the effect that our adjustment of the ventilator settings can produce on volume.
In a ventilation pattern without problems, inspiratory and expiratory volumes should be similar. If there are differences between inspiratory and expiratory volume, there can be:
-
Air leaks in the system
-
Intrinsic positive end-expiratory pressure (i.e., auto-PEEP or air trapping). In this case, the downslope representing expiration decreases as expected but never reaches the baseline of zero volume before the next breath (see Fig. 13.4) [4, 11].
Key Major Recommendations
-
The analysis of flow/pressure and volume waveforms is important to properly monitor the ventilated patient, to modify parameters of the ventilator, and reduce patient–ventilator asynchrony.
-
At first, evaluate pressure and flow scalar; the analysis of volume scalar is a completion.
-
The clinician should evaluate:
-
if respiratory acts are preceded by a normal activation of inspiratory trigger
-
if there are ineffective efforts or double efforts
-
if the ventilator generates autotrigger
-
if the pressure rises up properly
-
if the pressure is maintained properly or if there are signs of leaks
-
if cycling from inspiration to expiration is correctly configured
-
if there are signs of hyperdynamic inflation.
-
References
Elizabeth Emrath. The basics of ventilator waveforms. In: Giuliano J, Mack E, section editors. Current pediatrics reports, critical care, vol 9; 2021. pp. 11–19.
Owens W. Guida alla Ventilazione meccanica. Piccin; 2016.
Prabhakaran P, Sasser WC, Kalra Y, Rutledge C, Tofil NM. Ventilator graphics. Minerva Pediatr. 2016;68(6):456–69. Epub 2016 Jul 8.
Nava S, Fanfulla F. Ventilazione meccanica non invasiva. Come, quando e perché. Springer Italia.
L’insufficienza respiratoria: basi razionali dell’ossigenoterapia e della ventilazione meccanica. Mattioli.
Gruppo NIV SIMEU. Insufficienza respiratoria acuta: dalla CPAP alla NIV. C.G. Edizioni Medico scientifiche.
Nilsestuen JO, Hargett KD. Using ventilator graphics to identify patient-ventilator asynchrony. Respir Care. 2005;50(2):202–34; discussion 232–4.
Basics AJ-M. Monitoring mechanical ventilation using ventilator waveforms. Cham: Springer International Publishing; 2018. p. 1–28.
Thille AW, Rodriguez P, Cabello B, Lellouche F, Brochard L. Patient-ventilator asynchrony during assisted mechanical ventilation. Intensive Care Med. 2006;32(10):1515–22. https://doi.org/10.1007/s00134-006-0301-8. Epub 2006 Aug 1.
Bulleri E, Fusi C, Bambi S, Pisani L, Petraglia A. Patient-ventilator asynchronies: types, outcomes and nursing detection skills. Acta Biomed. 2018;89(7-S):6–18.
Restrepo R, Khusid F. Essentials of ventilator graphics. Indian J Respir Care. 2014;3(1):396–404.
Subirà C, de Haro C, Magrans R, Fernández R, Blanch L. Minimizing asynchronies in mechanical ventilation: current and future trends. Respir Care. 2018;63(4):464–78.
Sheehy RD, Duce B, Edwards TP, Churton JA, Sharma R, Hukins CA. Double-triggering during noninvasive ventilation in a simulated lung model. Respir Care. 2020;65(9):1333–8.
Tassaux D, Gainnier M, Battisti A, Jolliet P. Impact of expiratory trigger setting on delayed cycling and inspiratory muscle workload. Am J Respir Crit Care Med. 2005;172(10):1283–9.
Gentile MA. Cycling of the mechanical ventilator breath. Respir Care. 2011;56(1):52–60.
Venu Gopal Reddy. Auto-PEEP: how to detect and how to prevent—a review. Middle East J Anaesthesiol. 2005;18(2):293–312.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Fagetti, L. (2023). Pressure/Airflow and Volume Waveforms. In: Esquinas, A.M. (eds) Noninvasive Mechanical Ventilation. Springer, Cham. https://doi.org/10.1007/978-3-031-28963-7_13
Download citation
DOI: https://doi.org/10.1007/978-3-031-28963-7_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-28962-0
Online ISBN: 978-3-031-28963-7
eBook Packages: MedicineMedicine (R0)