Abstract
α4 integrins (including α4β1 and α4β7) are primarily expressed on leukocytes. By interacting with their ligands expressed on high endothelial venules (HEVs), α4 integrins mediate the recruitment of leukocytes from blood circulation to lymphoid organs and inflamed tissues, thereby playing essential roles in immune surveillance and host defense. The function of integrins is dynamically regulated by their activation and signaling. Integrin activation is associated with global conformational rearmament from a bent to extend conformation, mainly triggered by intracellular activation signals, termed “inside-out” signaling. The ligand binding to the integrin can also activate multiple intracellular pathways, which is termed “outside-in” signaling. In this chapter, we summarize the major findings regarding α4 integrins over the last decades, including their structures, extracellular ligands, intracellular adaptor proteins, and functions in homeostasis and diseases, including cancer, multiple sclerosis (MS), inflammatory bowel disease (IBD), and other autoimmune diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keyword
- Integrin
- α4β1
- α4β7
- Structure
- Extracellular ligands
- Intracellular adaptor proteins
- Activation
- Homeostasis
- Disease
1 Introduction
Integrins are a family of α/β heterodimeric cell adhesion molecules, which exist extensively in all multicellular organisms (Hynes 1987; Tamkun et al. 1986). They were named “integrins” because they are integral membrane protein complexes for cell adhesion to the extracellular matrix (ECM) and were first proposed in the 1980s at the molecular level (Hynes 1987; Tamkun et al. 1986). Integrins have been major cell adhesion receptors since the early evolutionary history of the metazoans (Burke 1999; Hughes 2001), and homologous integrin sequences are even found in many prokaryotes (Johnson et al. 2009), suggesting they are a conserved evolutionary process and have pivotal functions in a wide range of scenarios. The vertebrate integrin family originates from homologous domains residing in the protists and prokaryotes, adapting itself to diverse functions within complete immune and closed circulatory systems throughout chordate evolution from lower organisms to individuals of phylum Chordata (Johnson et al. 2009). In vertebrates, 18 integrin α subunits and 8 β subunits form at least 24 different integrins (Hynes 2002). These integrins form a superfamily of cell adhesion receptors that bind to ECM ligands, cell-surface-expressing ligands, and pathogenic ligands and are responsible for mediating cell–matrix attachments, cell–cell and cell–pathogen interactions.
Integrin α4β1, also named very late activation antigen-4 (VLA-4), and CD49d/CD29 were described approximately 30 years ago (Hemler et al. 1987a) as a new member of the VLA antigen proteins that were originally found to appear during late T-cell activation (Hemler et al. 1985). Integrin α4β1 facilitates the recruitment of leukocytes to endothelial cells upon inflammation through the interaction with its ligand, vascular cell adhesion molecule-1 (VCAM-1) (Elices et al. 1990). Furthermore, the α4β1–VCAM-1 axis in different connective tissue cells has fundamental roles in many physiological processes, such as tissue organization, angiogenesis, and heart and skeleton development (Bouvard et al. 2001; Yong and Khwaja 1990). Integrin α4β1 on lymphocytes also recognizes the fibronectin (FN) Type III connecting-segment-1 (CS-1) region during T-cell function execution and immune responses (Wayner et al. 1989b). Soon after the discovery of integrin α4β1, another β integrin subunit named β7 was reported to form heterodimers with the α4 integrin subunit in mice (Holzmann and Weissman 1989; Kilshaw and Murant 1991) and humans (Erle et al. 1991). Integrin α4β7 (lamina propria-associated molecule-1, LPAM-1; CD49d/β7), whose distribution is restricted to subsets of immune cells in peripheral blood, mediates adhesion to mucosal tissues, such as gut-associated lymphoid tissue (GALT) through binding to its primary ligand, mucosal addressin cell adhesion molecule-1 (MAdCAM-1) (von Andrian and Mackay 2000; Yu et al. 2012). α4β1 and α4β7 share some ligands, including VCAM-1 and FN. α4β7 exhibits preferential binding to MAdCAM-1 over the other two ligands (Yu et al. 2012). Moreover, integrin α4β7 can bind to human immunodeficiency virus-1 (HIV-1) envelope glycoprotein gp120 to mediate an HIV–T-cell interaction, thereby participating in HIV-1 infection of T cells (Arthos et al. 2008; Liu and Lusso 2020; Wang et al. 2021).
Overall, α4 integrins play critical roles in multiple biological and pathological processes, including leukocyte recruitment from the bloodstream into lymphoid organs and targeted tissues, immune cells, especially T-cell co-stimulation, and embryonic development.
2 Structure of α4 Integrins
Integrins are α/β heterodimeric type I transmembrane proteins. Both α and β subunits consist of a large extracellular domain, a single transmembrane domain, and a short cytoplasmic domain (Fig. 1a) (Arnaout et al. 2005). In humans, the α4 subunit contains 1032 amino acid residues, and both β1 and β7 subunits contain 798 amino acid residues. Since the first characterization of the integrin α4 subunit in 1989, many studies have shed light on the structure of α4 integrins (Baldini and Cro 1994; Kassner et al. 1992; Wang et al. 2018; Yu et al. 2012).
Schematic of the α4 integrin structure and conformational rearrangements. (a) Domains within the primary structure of α- and β-subunits of α4 integrin are shown. Yellow and red asterisks denote Ca2+- and Mg2+-binding sites, respectively. (b) Conformational rearrangements of the α4 integrin during activation. Broken lines symbolize lower leg flexibility. Redrawn from Zhang and Chen (Zhang and Chen 2012)
2.1 Extracellular Domain
Integrin α4 subunit, which contains five extracellular domains, including a seven-bladed β-propeller, a thigh, a genu, and two calf domains, belongs to the α-I less integrin family because it lacks an I domain inserted between blades 2 and 3 in the β-propeller domain (Fig. 1a) (Larson et al. 1989). For the β1 and β7 subunits, the extracellular domain consists of a βI (βA), hybrid, plexin-semaphorin-integrin (PSI), cysteine-rich integrin epidermal growth factor (I-EGF) 1–4, and β-tail domains (Fig. 1a) (Xiao et al. 2004; Yu et al. 2012).
The conformations and dimensions of several integrin ectodomains (e.g., αXβ2, αVβ3, and αIIbβ3) have been extensively studied by different research groups (Xie et al. 2010; Xiong et al. 2001; Zhu et al. 2008a). The overall shape of the integrin extracellular domain is a large “head” on two long “legs” with flexible “knees” (Fig. 1b). In 2012, the structure of the integrin α4β7 ectodomain was revealed by electron microscopy (EM) and X-ray crystal structure (Yu et al. 2012). The integrin “head piece” contains a β-propeller domain and βI domain, together with the “upper leg,” which contains an α thigh and β hybrid, PSI, and I-EGF1 domains (Yue et al. 2013). The remaining calf-1/2, I-EGFs, and β-tail domains in the ectodomain make up the “lower leg” of the integrin (Fig. 1b) (Yu et al. 2012).
The adhesion between an α4 integrin and its ligand is metal ion-dependent. In the α4 subunit, there are three Ca2+-binding sites located in the loops extending between propeller blades 5 to 7 and one site located at the “genu” (Fig. 1a). The β-propeller Ca2+-binding sites are involved in the regulation of the integrin-ligand binding affinity. Conservative mutations in these sites of the α4 β-propeller significantly decreased the affinity for ligand binding to α4β1 (Masumoto and Hemler 1993).
In the β1 and β7 subunits, the βI domain contains an interlinked linear array of three metal ion-binding sites, with a metal ion-dependent adhesion site (MIDAS) at the center flanked by two other sites: the synergistic metal ion-binding site (SyMBS) and the adjacent to MIDAS (ADMIDAS). Based on the electron density in crystal structures, MIDAS is occupied by Mg2+, but the two flanking sites are loaded with Ca2+ (Zhu et al. 2008b). The divalent cation in the MIDAS site forms a critical interaction with a negatively charged residue, usually Asp, in the integrin ligand. Disruption of the MIDAS site by mutations completely abolished the MAdCAM-1 binding to integrin α4β7 (Chen et al. 2003). SyMBS, also termed ligand-associated metal-binding site (LIMBS), exhibits a positive regulatory effect for integrin-ligand binding, which is required for the activation of α4β7 (Chen et al. 2003). The SyMBS metal ion can form a cation-π interaction with a conserved aromatic residue (Tyr or Phe) in the specificity-determining loop (SDL), which may help to stabilize SyMBS metal ion coordination and maintain the proper conformation of SDL for an integrin high-affinity state (Pan et al. 2010; Zhang and Chen 2012) (Fig. 2). When occupied by Ca2+, ADMIDAS functions as a negative regulatory site responsible for keeping the integrin in the low-affinity state by preventing the downward movement of the βI domain C-terminal α7-helix, a critical step in integrin activation. Mn2+ can compete with Ca2+ to occupy the ADMIDAS site and induce integrin activation by the release of the inhibitory effects of Ca2+ (Chen et al. 2004; Humphries et al. 2003) (Fig. 2). The downward displacement of the βI domain C-terminal α7-helix allosterically alters the geometry of the metal ion clusters in a way that increases the affinity for ligand binding (Zhang and Chen 2012) (Fig. 2).
Metal ion cluster in the βI domain. The linear cluster of the βI domain metal ion-binding sites is shown as SyMBS, MIDAS, and ADMIDAS from left to right. The metal ion-binding sites are colored as follows: blue, SyMBS; red, MIDAS; gray, ADMIDAS. The cation-π interaction between the SyMBS metal ion and the aromatic side chain of Tyr or Phe is shown by a blue dashed line
2.2 Transmembrane Domains
The integrin α and β subunits anchor themselves within the cell plasma membrane via a single short transmembrane domain (TMD) (Fig. 1a). In addition to connecting the integrin extracellular domain and cytoplasmic domain, TMD has an important role in transducing bidirectional signaling across the plasma membrane (Kim et al. 2003). The linkers between the integrin ectodomain and TMD helices are suggested to be quite flexible during integrin activation, facilitating the β hybrid domain swing-out and overall conformational shift of the integrin molecule to a high-affinity conformation (Lau et al. 2009). Acidic phospholipids in the plasma membrane may ionically interact with the integrin intramembrane basic residue (K/R) close to the TMD and cytoplasmic domain border, which is believed to stabilize the integrin transmembrane dimer and hold the integrin in a resting state (Kim et al. 2011; Lu et al. 2016b). Intriguingly, calcium ions (Ca2+) may disrupt the ionic K/R–lipid interaction through its positive charge, which leads to the separation of the integrin α/β TMDs and the subsequent extracellular domain extension to a high-affinity conformation (Guo et al. 2018).
2.3 Cytoplasmic Domains
The integrin cytoplasmic domain is very short. The α4 and β1/β7 subunits have approximately 30 and 50 amino acid residues, respectively. It serves as a vital bond connecting its mechano-sensing ectodomain with its cytoplasmic adaptor proteins within the cell (Legate et al. 2006; Wiesner et al. 2006). The binding proteins for the β subunit cytoplasmic domain have been well characterized (Harburger and Calderwood 2009; Zaidel-Bar et al. 2007). For example, talin binds to the membrane-proximal NPxY motif via its canonical phosphotyrosine-binding (PTB) domain, which is critical for integrin activation (Calderwood et al. 2003; Wegener and Campbell 2008). Kindlin binds to a serine/threonine (S/T) rich motif and the membrane-distal NxxY motif, which functions as an integrin co-activator (Calderwood et al. 2003; Wegener and Campbell 2008). Some other PTB-containing proteins, such as docking protein 1 (DOK1) and integrin cytoplasmic domain associated protein 1 (ICAP1), suppress integrin activation by competition with talin (Liu and Boggon 2013; Wegener et al. 2007). Although filamin has no PTB domain, it also competes with talin/kindlin for binding to the β tail because of the overlapping binding sites in the integrin β tail (Calderwood et al. 2013b). The adaptor proteins for the α4 tail are less well studied. Integrin inhibitors, such as mammary-derived growth inhibitor (MDGI) and SHANK-associated RH domain-interacting protein (SHARPIN), interact with the α4 cytoplasmic domain around the conserved juxtamembrane GFFKR motif (Bouvard et al. 2013). The GFFKR motif serves as an important intrinsic structural component in making a salt bridge between the α/β cytoplasmic tails to keep the integrin inactive (Lu et al. 2001). Paxillin specifically binds to the α4 tail and regulates cell spreading and migration (Liu and Ginsberg 2000; Liu et al. 2002; Liu et al. 1999). Moreover, a study using chimeric α2, α4, and α5 integrins demonstrates that the cytoplasmic tails of different α subunits contribute to the determination of integrin-ligand binding specificity (Chan et al. 1992).
3 Extracellular Ligands for α4 Integrins
3.1 VCAM-1
The cell-surface glycoprotein VCAM-1 belongs to the Ig superfamily (IgSF) and contains seven Ig-like extracellular domains or is alternatively spliced into six or eight Ig-like domains (Renz et al. 1994). VCAM-1 is widely expressed on the stimulated endothelial cells of blood vessels, peripheral lymph nodes (PLNs), and bone marrow (BM) (Berlin-Rufenach et al. 1999). Both integrin α4β1 and α4β7 can bind to VCAM-1. Domain 1 (D1) and domain 4 (D4) of VCAM-1 contribute to α4β1-dependent adhesion (Osborn et al. 1992). The linear sequence for QIDSPL, especially the tripeptide IDS (Ile-Asp-Ser), in the D1 and D4 has been demonstrated to be critical for α4β1 recognition (Baiula et al. 2019; Vonderheide et al. 1994). It is noteworthy that both the resting and activated integrin α4β1 can bind to VCAM-1 D1, whereas only the activated α4β1 can bind to VCAM-1 D4 (Kilger et al. 1995). Similarly, integrin α4β7 can also bind to D1 and D4 of VCAM-1 (Ruegg et al. 1992) but with much less affinity than α4β1.
3.2 MAdCAM-1
MAdCAM-1, an IgSF type I transmembrane glycoprotein, is the primary ligand for integrin α4β7. MAdCAM-1 is specifically expressed on the endothelium of HEVs in the gut and GALT, such as Peyer’s patches and MLNs, and the venules of the lamina propria (LP) (Berlin et al. 1995; Cox et al. 2011; Springer 1994). The interaction between integrin α4β7 and MAdCAM-1 has an essential role in supporting gut-targeting lymphocyte homing. MAdCAM-1 consists of two Ig-like domains, a mucin-like region, a short TMD, and a cytoplasmic domain (Shyjan et al. 1996). Structural analysis of the MAdCAM-1–α4β7 complex has revealed that α4β7 directly binds to MAdCAM-1 aspartate 42 (Asp42) located on the protruding CD loop in Ig domain 1 through the MIDAS site located in the β7 I domain (Tan et al. 1998; Yu et al. 2012). Moreover, a D strand in the I1 set of MAdCAM-1 Ig domain 2 is also necessary for α4β7 recognition and binding (Newham et al. 1997; Tan et al. 1998). The mucin-like domain, which is a serine/threonine-rich region, leads to a more upright conformation of MAdCAM-1 because of the electrostatic repulsion between negative charges in the extracellular microenvironment and mucin-like region, facilitating α4β7-mediated cell adhesion (Yuan et al. 2020).
A previous study revealed that different chemokines could activate integrin α4β7 in a ligand-specific manner to mediate selective homing of lymphocytes to the gut via its interaction with MAdCAM-1 or to PLNs through binding with VCAM-1 (Sun et al. 2014). In particular, chemokine (C-C motif) ligand 25 (CCL25) enhances the α4β7-mediated lymphocyte adhesion to MAdCAM-1 but suppresses adhesion to VCAM-1, whereas C-X-C motif chemokine 10 (CXCL10) stimulation has the opposite effect. The selective adhesion of α4β7 to MAdCAM-1 and VCAM-1 is determined by the distinct active integrin conformation induced by CCL25 and CXCL10 (Sun et al. 2014; Wang et al. 2018).
3.3 FN
FN is a high-molecular-weight glycoprotein synthesized by hepatocytes and mesenchymal cells (White and Muro 2011). α4 integrins serve as alternative FN receptors in addition to the FN receptor integrin α5β1 (Guan and Hynes 1990; Wayner et al. 1989a). Interestingly, the α4 integrins and α5β1 recognize independent sites in intact FN. Integrin α5β1 recognizes the Arg-Gly-Asp (RGD) containing cell adhesion domain in FN (Pytela et al. 1985), whereas integrin α4β1 recognizes a carboxy-terminal cell adhesion region containing the Heparin II and Type III connecting-segment-1 (CS-1) domains (Guan and Hynes 1990). An acidic motif in CS-1, termed “LDV”, is functionally related to RGD and responsible for α4β1 binding. Integrin α4β7 not only recognizes the same site within the alternatively spliced connecting segment of FN as α4β1 (Ruegg et al. 1992) but also directly binds to FN splice variants containing type III repeats III5 (containing a KLDAPT sequence) and the Extra Domain A (EDA domain, containing an EDGIHEL sequence only in cellular FN) (Pankov and Yamada 2002).
3.4 Gp120
Gp120 is an envelope glycoprotein of HIV-1. Some studies have shown the interaction between integrin α4β7 and gp120 through a conserved tripeptide Leu-Asp-Val/Ile (LDV/I) motif in the V2 loop of gp120 (Peachman et al. 2015; Wang et al. 2021). By mimicking the binding epitopes in MAdCAM-1, gp120 binds to α4β7, which facilitates productive HIV-1 infection of α4β7-expressing CD4+ T cells in GALT (Cicala et al. 2009). However, unlike MAdCAM-1, which can adhere to both inactive and active α4β7, gp120 predominantly binds to α4β7 active conformers with a highly extended conformation (Wang et al. 2021).
3.5 Osteopontin
Osteopontin is a secreted highly acidic glycoprotein originally isolated from bone. Its expression is upregulated at sites of cardiovascular injury, and monocytes and macrophages also synthesized it within injury sites (Bayless et al. 1998). As a ligand for integrin α4β1, osteopontin can promote α4β1-mediated leukocyte adhesion (Bayless et al. 1998). The N-terminal thrombin fragment of osteopontin has been demonstrated to bind to integrin α4β1 (Bayless and Davis 2001).
3.6 Invasin
Another α4β1 ligand is invasin, an outer membrane bacterial protein mediating the attachment of Yersinia pseudotuberculosis to human cells. The α4β1 on T cells binds strongly to purified invasin, facilitating a T-cell proliferative response (Ennis et al. 1993). Direct interactions of T cells with bacterial pathogens such as Yersinia may be relevant to host immune responses to bacterial infection (Ennis et al. 1993).
3.7 Other α4 Extracellular Domain-Binding Proteins
Several membranal proteins have been demonstrated to interact with integrin α4β1, including junctional adhesion molecule-2 (JAM2), A Disintegrin and Metalloproteinase (ADAMs), CD14, and even the α4 subunit itself. The binding of integrin α4β1 to JAM2 is only enabled following prior adhesion of JAM2 with JAM3 and is not detectable in cells where JAM3 expression is absent (Cunningham et al. 2002). The disintegrin domains of ADAM7 and ADAM28 are recognized by α4β1 and α4β7, respectively, and the recognition requires integrin activation (Bridges et al. 2005). The lipopolysaccharide (LPS) receptor, CD14, a GPI-linked cell-surface glycoprotein, is a novel ligand for α4β1, exhibiting similar activation-state dependent binding characteristics (Humphries and Humphries 2007). Additionally, the α4 subunit itself can serve as a ligand. There are three conserved LDV motifs in the extracellular sequence of the α4 subunit. α4β1 and α4β7 exhibited homophilic interactions with α4 subunits in vitro, suggesting that α4 integrins may bind to α4 subunits on adjacent cells (Altevogt et al. 1995).
4 Intracellular Adaptor Proteins for α4 Integrins
4.1 β1 and β7 Cytoplasmic Tail-Binding Proteins
4.1.1 Talin
Talin is a 250 kDa cytoskeletal protein that links integrins and the actin cytoskeleton. Talin comprises a 220 kDa rod domain and a 50 kDa N-terminal head domain (THD). THD harbors four subdomains, including the FERM (Band 4.1, ezrin, radixin, moesin) domain made up of F1, F2, and F3 domains, and the N-terminal F0 domain preceding the FERM domain (Calderwood et al. 1999; Critchley 2009). The F3 subdomain binds to integrin β cytoplasmic tails through its canonical PTB domain. β1 and β7 tails bind to talin via their membrane-proximal NPxY motifs (NPIY motif for β1 and NPLY motif for β7), and the α-helical region lying between the membrane and the NPxY motif (Anthis et al. 2009; Wegener et al. 2007). The binding of talin to the β cytoplasmic domain requires the dephosphorylation of the Tyr in the NPxY motif and is critical for α4 integrin activation (Calderwood et al. 2002). Upon talin binding, integrin β cytoplasmic tails form a stable span between the TMD and cytoplasmic membrane-proximal region, which disrupts the salt bridge between the α/β cytoplasmic tails by forming a non-covalent interaction with a conserved aspartate or glutamate residue at the β subunit membrane-proximal region, and consequently, activates integrin (Calderwood et al. 2013a).
4.1.2 Kindlin
Kindlins also contain the conserved FERM domain and bind to a serine/threonine motif and membrane-distal NxxY motifs (Harburger et al. 2009; Malinin et al. 2010; Sun et al. 2014). In mammals, there are three kinds of kindlins (Lu et al. 2016a; Sun et al. 2014; Sun et al. 2019). Kindlin-1 is mainly expressed in epithelial cells. Kindlin-2 is expressed ubiquitously, except for the hematopoietic system. Kindlin-3 is restricted to hematopoietic cells. Kindlin and talin are indispensable for integrin activation through their crucial functions in connecting surface-expressing integrins with intracellular actomyosin and regulating actin dynamics (Sun et al. 2019).
4.1.3 Filamin
Filamin, a high-molecular-weight actin-cross-linking protein, serves as an important integrin inactivator via interaction with the β subunit membrane-proximal NPxY motif and the subsequent serine/threonine-rich region, which overlaps the talin and kindlin-binding sequences and competes for their association with β tails, thereby inhibiting integrin activation (Calderwood et al. 2001).
4.2 α4 Cytoplasmic Tail-Binding Proteins
4.2.1 SHARPIN
SHARPIN was described as an important inactivator of integrins 10 years ago (Rantala et al. 2011). SHARPIN binds to the α integrin membrane-proximal region that contains the conserved GFFKR motif. SHARPIN binding does not involve the arginine residue in the GFFKR; therefore, it does not interfere with the formation of the clasping salt bridge. Furthermore, SHARPIN bound to the α tail inhibits talin and kindlin binding to the β tail presumably through steric hindrance (Rantala et al. 2011). Therefore, SHARPIN inhibits the activation of both integrin α4β1 and α4β7. Moreover, SHARPIN deficiency has been shown to enhance integrin-mediated cell adhesion and reduce cell migration velocity (Park et al. 2015; Pouwels et al. 2013).
4.2.2 MDGI
Similar to SHARPIN, MDGI also binds directly to the cytoplasmic tail of integrin α subunits, including α4, through a conserved GFFKR sequence. MDGI bound to α tails retains integrin in an inactive conformation attenuating integrin-mediated adhesion, migration, and invasion (Nevo et al. 2010).
4.2.3 Paxillin
Paxillin is the first identified and extensively studied signaling adaptor protein of α4 integrins (Liu et al. 1999). It is widely expressed and comprises five leucine-rich LD motifs in its N-terminus and four LIM domains in its C-terminus (Rose 2006). Paxillin physically associates with α4 integrins, and this association markedly reduces cell spreading, focal adhesions, and stress fiber formation (Liu et al. 1999). A region of nine amino acid residues (Glu983-Tyr991) within the α4 cytoplasmic domain contains a minimal sequence sufficient for paxillin binding. Furthermore, Tyr991 and Glu983 are critical residues, and either a Y991A or E983A substitution disrupts the interaction of α4 integrins with paxillin (Liu and Ginsberg 2000; Liu et al. 1999). In turn, the stretch of amino acid residues Ala176-Asp275 in the LD3 and LD4 repeats of paxillin is sufficient for binding to the α4 tail (Liu et al. 2002). The interactions between LD3 and LD4 of paxillin and the α4 tail have been confirmed by nuclear magnetic resonance (NMR) studies and the docked structures of the α4 tail with these LD repeats, suggesting possible polar and/or salt bridge and non-polar packing interactions (Chua et al. 2013). Paxillin binding to the α4 tail is also regulated by post-translational modification of the latter. Phosphorylation at Ser988 blocks paxillin binding to the α4 tail and reverses the inhibitory effect of α4 on cell spreading (Han et al. 2001). Phosphorylation of α4 is restricted to the leading edge and is absent from the sides and rear of migrating cells (Goldfinger et al. 2003). The binding of paxillin to the α4 integrin subunit in the trailing edge inhibits adhesion-dependent lamellipodium formation by blocking Rac activation (Nishiya et al. 2005).
Transgenic mice homozygous for α4 Y991A have reduced Peyer’s patches and impaired mononuclear leukocyte recruitment to sites of inflammation (Feral et al. 2006). A small molecule that inhibits the interaction of paxillin and α4 integrin inhibits the accumulation of mononuclear leukocytes at sites of inflammation, proving inhibition of α4 integrin signaling as a target for the pharmacological reduction of inflammation (Kummer et al. 2010).
4.2.4 Hsp90
Heat shock proteins (Hsps) are a family of proteins that display enhanced expression in response to thermal stress (Schlesinger 1990). Febrile temperatures (38.5 °C) can efficiently enhance the expression of Hsp90 in T cells and increase α4 integrin-mediated T-cell adhesion and transmigration (Lin et al. 2021; Lin and Chen 2019; Lin et al. 2019). Hsp90 binds to the ENRRDSWSY motif of the α4 cytoplasmic tail and induces association of talin and kindlin-3 with integrin β tails, triggering α4 integrin activation via inside-out signaling. Moreover, the N- and C-terminus of one Hsp90 molecule can simultaneously bind to two α4 tails, resulting in dimerization and clustering of α4 integrins on the plasma membrane and subsequent activation of the FAK-RhoA signaling pathway in T lymphocytes, thereby promoting T lymphocyte adhesion and transmigration. This regulation of α4 integrin function does not require the ATPase activity of Hsp90, suggesting that this function is distinct from the chaperone function of Hsp90, which requires the energy released from ATP hydrolysis (Lin et al. 2019). Abolishing Hsp90-α4 interaction in vivo inhibits whole-body hyperthermia (WBH)-induced T-cell trafficking to draining lymph nodes. Moreover, in a Salmonella typhimurium infection-induced mouse fever model, disruption of the Hsp90-α4 interaction in the mice markedly decreased the number of infiltrated T cells and increased bacterial dissemination in the small intestine, resulting in a significantly increased death rate (Lin et al. 2019). Thus, the fever-induced Hsp90-α4 integrin axis is crucial for promoting immune cell trafficking to inflamed tissues to facilitate the clearance of bacterial infection.
Because other cellular stressors can induce Hsp90 expression, the Hsp90-α4 integrin pathway may also play a role in pathological conditions in allergies, autoimmune diseases, and even cancer. Whether this pathway can be targeted therapeutically to enhance or temper immune trafficking awaits further study (Bird 2019). This pathway might be exploited to make T cells “super-homers” by raising Hsp90 levels in efforts to combat cancer during the administration of cancer immunotherapy (Hampton 2019).
5 Activation of α4 Integrins
5.1 Affinity Regulation
Integrin activation is accompanied by bidirectional signal transduction across the plasma membrane. Both “inside-out” and “outside-in” integrin signaling play important roles in integrin-mediated biological processes. When a cell receives an extracellular stimulus through its cell-surface receptors, such as chemokine receptors or T-cell receptor tyrosine kinases (RTKs), the transduced signals will promote the binding of intracellular integrin activators including talin and kindlins to the integrin β tail, leading to an integrin global conformational change into the active state with enhanced adhesiveness for extracellular ligands. This integrin activation process is termed “inside-out” activation (Kim et al. 2003; Shattil et al. 2010). In addition, integrin can also serve as a classical cell-surface signaling receptor, which transmits signals into cells upon association with its ligands via “outside-in” signaling, thereby mediating cell proliferation, survival, and differentiation (Takagi et al. 2002).
Both of these events lead to integrin affinity regulation along with striking conformational changes in the integrin molecule (Beglova et al. 2002; Luo et al. 2007; Takagi et al. 2001; Takagi et al. 2002). α4 integrins consist of a globular ligand-binding head domain involving an α and β subunit interface localized within the α4-β propeller and β1/β7-βI domains, two long legs connected to the TMD and the cytoplasmic tail of each subunit (Yu et al. 2012). It behaves in at least three overall conformational states, including the bent conformation low-affinity state, the extended conformation with a closed or intermediate headpiece intermediate affinity state, and the extended conformation with an open headpiece high-affinity state (Fig. 1b) (Carman and Springer 2003; Luo et al. 2007).
The activation of α4 integrins is associated with an integrin molecule extension coupled with a β subunit hybrid domain swing-out and separation of the α/β leg domains (Fig. 1b) (Chigaev et al. 2009; Takagi et al. 2002). Separation of the α/β subunit transmembrane domains and cytoplasmic tails has been defined as the crucial initiator of the inside-out signaling cascade, which has been widely verified using fluorescence resonance energy transfer (FRET)-based studies (Kim et al. 2003; Wang et al. 2018). A ~ 62° hybrid domain swing-out with respect to the βI domain is thought to drive the downward movement of the α7 helix within the I domain and shift the ligand-binding MIDAS site into the open conformation, thereby facilitating high ligand-binding affinity (Liu et al. 2014; Wang et al. 2018; Xiao et al. 2004). This high-affinity integrin conformation can exist independently of ligand binding (Carman and Springer 2003). In the presence of its binding ligand, integrin rearranges its headpiece conformation to an open orientation with an ~ 80° β subunit hybrid domain swing-out (Takagi et al. 2002; Takagi et al. 2003), followed by conformational changes in the tailpiece, which lead to “outside-in” signal transduction.
It is noteworthy that α4β7 can be activated into distinct intermediate- and high-affinity states, which exhibit selective ligand-binding preferences for MAdCAM-1 and VCAM-1 (Sun et al. 2014; Wang et al. 2018). Chemokines CCL25 and CXCL10 can stabilize the α4β7 integrin in two intermediate open conformations via triggering the p38α MAPK/PKCα and c-Src/Syk pathways, respectively, leading to different phosphorylation states of the β7 tail and distinct talin and kindlin-3 binding patterns. The two intermediate open conformers of α4β7 show selective adhesion to either MAdCAM-1 or VCAM-1, which results in selective homing of lymphocytes to distinct tissues in mice.
5.2 Avidity Regulation
Cells treated with a certain stimulus represent an obvious adhesive phenotype to the ligand-coated surface while no high-affinity soluble ligand binding is observed (Stewart et al. 1998; van Kooyk and Figdor 2000), suggesting that another regulatory pathway than “affinity regulation” contributes to integrin activation. Indeed, an integrin binding to its ligands not only changes its global conformation but also leads to clustering or patching of integrin-receptor complexes on the cell surface where cell–cell or cell–matrix contact exists, which is termed “avidity regulation” or “valency regulation” (Carman and Springer 2003; Schurpf and Springer 2011). Diverse patterns of α4 integrins clustering on living cells have been reported (Carman and Springer 2003; Shamri et al. 2002; Sun et al. 2014; Zhang et al. 2013) and can be classified into two types based on the presence of extrinsic ligands or not. In the absence of ligands, integrins redistribute to form active clusters via intrinsic signals and are transported to the cell–matrix contact surface or cell leading edge, facilitating cell adhesion and migration (Sun et al. 2014; Wang et al. 2021; Zhang et al. 2013). The cytoplasmic tail of α4 integrins makes strong positive contributions to integrin-mediated cell adhesion by upregulating integrin clustering and increasing the overall avidity of integrins (Yauch et al. 1997). Hsp90 has recently been identified as a novel α4 intracellular binding protein (Lin et al. 2019). The N-terminal domain (NTD) and C-terminal domain (CTD) of Hsp90 can directly bind to the α4 tail. Thus, one Hsp90 molecule simultaneously associates with two α4 subunits, which induces α4 integrin dimerization and clustering on the cell membrane and subsequent activation of integrin downstream signaling. Redistribution of α4 integrins on the cell surface also occurs in a ligand-dependent manner. This is probably caused by the multivalent property of integrin-binding ligands, such as FN.
6 Expression and Physiological Functions of α4 Integrins
6.1 Expression of Integrin α4β1 and α4β7
Integrin α4β1 is constitutively expressed on most leukocytes (Luster et al. 2005). In general, neutrophils are assumed not to express α4 integrins. However, α4 integrins have been demonstrated to play a role in mediating neutrophil adhesion and migration (Johnston and Kubes 1999), suggesting that low levels of α4 integrins on neutrophils suffice for functional activity. Moreover, α4β1 expression occurs in hematopoietic stem cells (HSCs) (Williams et al. 1991) and non-hematopoietic cells in multiple embryonic tissues, including somites, heart, vascular smooth muscle and skeletal muscle, the neuroepithelium of the embryonic retina, and neural crest-derived cells, such as melanoblasts (Sheppard et al. 1994; Stepp et al. 1994; Yang et al. 1995). α4β1 is also expressed in various tumor cells, including metastatic melanoma and gastric cancer cells (Mould et al. 1994; Park et al. 2004; Rebhun et al. 2010), indicating vital roles in both physiological and pathological processes.
The expression of integrin α4β7 is restricted on hematopoietic cells. A group of immune cells has been reported to express integrin α4β7 constitutively, including lymphocytes, NK cells, mast cells, basophils, eosinophils, macrophages, and monocytes (von Andrian and Mackay 2000). Under a steady-state, naïve lymphocytes exhibit a relatively low expression level of integrin α4β7 (Erle et al. 1994). Among them, most B lymphocytes show relatively high expression of integrin α4β7 compared with most T lymphocytes in the peripheral lymphoid organs, including the spleen, Peyer’s patches, and lymph nodes (Andrew et al. 1996). Intestinal dendritic cells (DCs)-derived retinoic acid (RA) has been shown to upregulate α4β7 expression on memory or activated gut-tropic lymphocytes, promoting lymphocyte homing to mucosal tissues or GALT effectively during intestinal immune responses (Hao et al. 2021; Iwata et al. 2004; Mora et al. 2006). In contrast, the majority of naïve or memory T cells, which lack α4β7 expression in circulation, express α4β1 instead (DeNucci et al. 2010). These cells prefer to home to non-mucosal tissues via binding to VCAM-1 (Rott et al. 1996; Rott et al. 1997). Interleukin-7 (IL-7) can potently induce α4β7 expression on naïve T cells and is closely related to α4β7 activation, resulting in intestinal homing of lymphocytes and immunologic reconstitution in lymphopenic hosts (Cimbro et al. 2012). As observed in hypereosinophilic patients, eosinophils characterized with high α4β7 expression exhibit preferential gut homing rather than trafficking to the lungs (Brandt et al. 2006). Moreover, integrin α4β7 is significantly upregulated on both peripheral naïve and memory T-cell subsets in intestinal graft-versus-host disease (GvHD) patients (Chen et al. 2009; Chen et al. 2013), suggesting integrin α4β7 serves as a crucial regulator in both homeostatic and pathologic conditions.
6.2 Integrin α4β1 and α4β7 in Leukocyte Homing
The recruitment of leukocytes from blood circulation to lymphoid organs and inflamed tissues is regulated by the sequential interactions of adhesion and signaling molecules on leukocytes and blood vessels, essential to immune surveillance and host defense (Butcher and Picker 1996). This recruitment process consists of a highly ordered adhesion cascade that includes tethering and rolling leukocytes along vessel walls of HEVs, chemokine-induced activation, firm arrest, and transendothelial migration (von Andrian and Mempel 2003). The initial transient contact of the circulating leukocytes with the vascular endothelium leads to leukocytes rolling along the vascular wall with greatly reduced velocity. The interaction mainly mediates this process between selectins and their ligands. In addition, inactive α4β1 and α4β7 integrins are also able to support lymphocyte rolling via binding to their endothelial ligands, VCAM-1 and MAdCAM-1 (Ley et al. 2007), respectively. After chemokine-induced activation of lymphocytes on the endothelium, α4 and β2 integrins are activated to mediate cell arrest. During this process, chemokines activate integrins through the rapid triggering of the signaling network that regulates the binding of intracellular effector proteins (e.g., talin or kindlin) to the cytoplasmic domains of integrins, which induces integrin activation (Hogg et al. 2011). The final transmigration step across HEVs involves multiple adhesion molecules, including α4β1, αLβ2, VCAM-1, intercellular adhesion molecule-1 (ICAM-1), ICAM-2, platelet endothelial cell adhesion molecule-1 (PECAM-1), junctional adhesion molecule-1 (JAM-1), and JAM-2 (Carman and Springer 2004). Notably, α4 integrins are involved in each step of leukocyte homing, and thus, have essential roles in regulating lymphocyte trafficking to lymphoid organs and inflamed tissues (Lin et al. 2019).
6.3 Integrin α4β7 in Lymphocyte Gut-Tropic Trafficking and GALT Formation
Integrin α4β7 is the most important gut-homing adhesion molecule in targeting lymphocytes trafficking to mucosal lymphoid tissues, such as Peyer’s patches and mesenteric lymph nodes (MLNs) (Habtezion et al. 2016). Naïve and central memory lymphocytes in circulation are recruited to enter the mucosal lymphoid tissues via interaction between surface-expressing α4β7 and its ligand MAdCAM-1 expressed on the HEVs localized in these tissues (Laudanna et al. 2002). Along with priming in the GALT, gut-homing lymphocytes undergo α4β7 and CCR9 upregulation by RA produced by DCs and/or stromal cells in the MLN, which imprints them with gut tropism and directs these cells to the LP of the small intestine (Agace 2010; Agace and Persson 2012). The conventional intraepithelial lymphocytes (IELs) derived from circulating T cells work similarly as LP lymphocytes (LPLs) (Habtezion et al. 2016), whereas the unconventional IELs originate from CD8+ thymocytes, which already express α4β7 and CCR9 in the thymus, bypassing the imprinting process in GALT (Guy-Grand et al. 2013; Staton et al. 2006).
Integrin α4β7 deficiency shows no defect in T and B cell development in mice, suggesting it is not required for lymphocyte development. However, in β7−/− mice, the failure of α4β7-induced lymphocyte homing results in a large reduction in gut-tropic lymphocytes within the intestinal tissue, which eventually leads to abnormal development of GALT (Wagner et al. 1996). In addition, an integrin α4β7 mutation, which fails to transmit talin-induced TMD topology and blocks lymphocyte gut homing, results in GALT development disruption (Sun et al. 2018). These data suggest a vital role of α4β7 in the development of GALT architecture.
6.4 Role of Integrin α4β7 in Innate Immune Cells
Integrin α4β7 has also been reported to regulate innate immune cell tolerogenic functions in the mucosal immune system beyond lymphocyte trafficking (Kempster and Kaser 2014; Villablanca et al. 2014). A subset of α4β7-expressing LinnegLy6Clow BM cell progenitors give rise to RA-producing DCs, which are required to imprint gut-homing T cells. Moreover, integrin α4β7 is indispensable for the localization and reconstitution of these tolerogenic gut mononuclear phagocytes with the ability to induce Foxp3+ regulatory T cells and IL-10-producing T cells (Villablanca et al. 2014).
6.5 Integrin α4β1 in T-Cell Proliferation, Activation, and Survival
Integrin α4β1 can influence T cells in different ways. Anti-CD3 plus the integrin α4β1 ligand (CS1) can induce significant proliferation of CD4+ cells (Engelhardt et al. 1998; Nojima et al. 1990). Certain antibodies against integrin α4β1 block the effector activity of class I- and II-specific cytotoxic T lymphocytes (CTLs) in vitro (Clayberger et al. 1987; Takada et al. 1989). Integrin α4β1 also plays a regulatory role for T lymphocyte-antigen presenting cell cognate immune interactions by concentrating at the peripheral supramolecular activation complex (pSMAC) of the immune synapse and driving Th1 responses (Mittelbrunn et al. 2004). Furthermore, adhesion mediated by α4β1–VCAM-1 interaction promotes both T and B cell survival. Blockade of the interaction via monoclonal antibodies (mAbs) causes increased cell apoptosis (Koopman et al. 1994; Leussink et al. 2002).
6.6 Integrin α4β1 in Hematopoietic Stem Cell Maintenance and Hematopoiesis
Integrin α4β1 also plays an important role in developing and maintaining HSCs and hematopoiesis. Disturbing progenitor cell interaction with stromal cells by blocking α4 integrin inhibits lymphopoiesis in vitro (Miyake et al. 1991). Analyzing hematopoiesis in integrin α4- and β1-deficient somatic chimeric mice demonstrated a requirement of α4β1 in HSC homing to the fetal liver (Arroyo et al. 1999). α4 integrins are also required for hematopoietic precursor cell interactions with BM stromal cells and act as a retention signal for hematopoietic progenitors to remain in the BM compartment (Arroyo et al. 1996). Lack of α4 integrins leads to premature detachment of hematopoietic progenitors and low yields of mature cells in peripheral tissues (Arroyo et al. 1999). It is noteworthy that all detected requirements for α4 integrins in hematopoiesis result from α4-deficient mice. However, the lack of α4 integrins solely on hematopoietic cells in the adult does not hamper hematopoiesis, suggesting α4 integrins in non-hematopoietic cells may involve hematopoiesis (Brakebusch et al. 2002; Bungartz et al. 2006; Scott et al. 2003).
6.7 Integrin α4β1 and Embryonic Development
α4β1 is crucial in embryonic development. Deficiency of the α4 integrin subunit leads to embryonic lethality because of a failure in cell–cell adhesion events in placental and cardiac development (Yang et al. 1995). The early defect in α4-null embryos is characterized by a failure of the allantois to fuse with the chorion during placental development, and these embryos die by approximately embryonic day 11 (Yang et al. 1995). Although in a few cases, the fusion of the allantois and the chorion is successful, those embryos still die at approximately embryonic day 11.5 because of severe hemorrhage in the heart region caused by a failure in the epicardium-myocardium attachment during cardiac development (Yang et al. 1995). As a major counter-receptor of the α4β1 integrin, VCAM-1–deficient embryos show the same placental and cardiac defects, suggesting that these defects are probably caused by α4β1/VCAM-1–mediated adhesive interactions during embryonic development (Gurtner et al. 1995; Kwee et al. 1995). Whether α4β1 and VCAM-1 are involved in skeletal muscle development is controversial (Rosen et al. 1992; Yang et al. 1996).
7 α4 Integrins in Disease
7.1 α4 Integrins in Cancer
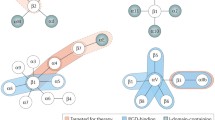
Altered integrin expression and function have been comprehensively reported in many types of human cancer and are tightly correlated with different stages of tumor progression, patient responses to antineoplastic therapy, and survival rates of patients with cancer (Table 1) (Hamidi and Ivaska 2019). Integrin α4β1 has been detected on both benign and malignant cells of the melanocytic lineage and suppresses metastasis formation in some experimental tumor models (Gazitt and Akay 2004). However, in the MYCNlow neuroblastoma, integrin α4 expression enhances experimental metastasis in a syngeneic tumor model, reconstituting a pattern of organ involvement similar to that seen in patients. Accordingly, antagonism of α4β1 (P1H4, antibody against integrins α4) blocks metastasis, suggesting the adhesive function of α4β1 is required during neuroblastoma metastasis (Young et al. 2015).
A previous study documented the crucial role of integrin α4β7 in the pathogenesis and development of multiple myeloma (MM), also called Kahler’s disease, a blood cancer that forms from the abnormal aggregation of antibody-producing plasma cells (Hosen 2020). In MM patients, cancerous plasma cells preferentially accumulate in the BM microenvironment, which crowds out healthy leukocytes and generates superfluous invalid immunoglobulins into blood circulation and bones, thereby causing severe complications. MM cells selectively adhere to either the BM microenvironment ECM components or multiple cell types residing in the BM, including hematopoietic cells, stromal cells, endothelial cells, and osteocytes, through interactions between adhesion molecules, such as integrins α4β1, α4β7, αLβ2, and their ligands VCAM-1, FN, and ICAM-1 (Shishido et al. 2014). In particular, integrin α4β7 is a central mediator in orchestrating MM cell adhesion, migration, aggregation, and extraversion during cancer progression (Neri et al. 2011). The expression of integrin β7 subunit could be upregulated by overexpression of c-maf gene (Hurt et al. 2004). The upregulated expression of integrin β7 in MM is inversely correlated with patient survival outcomes (Neri et al. 2011). Depletion of β7 expression in MM cells impairs the adhesion between cancer cells and ECM ligands, such as FN. It weakens its transwell migration induced by the BM-homing chemokine, CXCL12 (stromal cell-derived factor-1, SDF-1), reducing MM cells assembling in the BM microenvironment and subsequently alleviating cancer progression in the mouse model (Hosen 2020; Neri et al. 2011). Moreover, the integrin β7 subunit is primarily associated with the α4 subunit on MM cells rather than the αE subunit (Hosen et al. 2017), underlining the dominating effects of α4β7 in regulating MM pathogenesis. It is noteworthy that integrin β7 on MM cells has been unexpectedly detected to adopt a constitutively active conformation in the process of MM-specific cell-surface antigen screening (Hosen 2020; Hosen et al. 2017). The MM-specific mAb MMG49, which only recognizes the highly-activated conformation of the integrin β7 chain, specifically targets constitutively activated β7 expressed on MM cells instead of other CD45+ normal leukocytes in the BM. Usage of MMG49-derived chimeric antigen receptor (CAR)-T cells significantly dampens MM progression and prolongs the survival of tumor-bearing mice without damaging normal hematopoietic cells in the mouse model (Hosen et al. 2017). This suggests promising results from targeting a specific active conformer of α4β7 in anti-MM therapy in the future.
Integrin α4β7 is involved in abnormal lymphocyte trafficking to the hyperplastic thymus, characterized by an increased number of medullary blood vessels showing prominent HEV morphology and MAdCAM-1 expression, leading to thymic lymphoma development (Michie et al. 1995). Importantly, as a gut-tropic molecule, integrin α4β7 plays a profound role in regulating the progression of colorectal cancer (CRC). α4β7 mediates the recruitment of IFN-γ-producing CD4+ T cells, cytotoxic CD8+ T cells, and NK cells to the CRC tissue where they exert effective anti-tumor immune responses (West et al. 2015). A recent study showed that β7 expression decreased in tumor-derived compared to normal tissue-derived CD8+ T cells (Zhang et al. 2021). Higher β7 expression levels are correlated with longer patient survival, higher cytotoxic immune cell infiltration, lower somatic copy number alterations, decreased mutation frequency of APC and TP53, and better response to immunotherapy. β7 deficiency led to exaggerated tumorigenesis and progression in both Apcmin/+ spontaneous and MC38 orthotopic models of CRC, which could have been caused by the reduced infiltration of activated CD8+ T cells, effector memory CD8+ T cells, IFNγ+ CD8+ T cells, and other immune cell subsets that are essential players in anti-tumor immunity.
7.2 Integrin α4β1 in Multiple Sclerosis (MS)
The integrin α4β1/VCAM-1 axis plays an essential role in the homing of inflammatory leukocyte cells into the central nervous system (CNS) in different experimental autoimmune encephalomyelitis (EAE) models (Table 1) (Engelhardt et al. 1998; Kent et al. 1995a; Kerfoot and Kubes 2002; Yednock et al. 1992). Although encephalitogenic T cells express both α4β1 and α4β7 at similar levels, neutralizing α4β7 with antibodies does not inhibit EAE development (Engelhardt et al. 1998). It has been reported that antibodies to VCAM-1 inhibit the pathogenicity of encephalitogenic Th1 cells in vivo (Baron et al. 1993). The mouse mAb AN100226m, a potent antibody blocking α4 integrin-mediated binding to FN and VCAM-1, has been demonstrated to inhibit lymphocyte adhesion to tumor necrosis factor (TNF)-stimulated brain endothelium and is shown to reverse disease progression in the EAE model (Kent et al. 1995b). The humanized antibody AN100226, natalizumab, can reduce the risk of the sustained progression of disability and the rate of clinical relapse in patients with relapsing MS (Polman et al. 2006). It is noteworthy that few patients undergoing natalizumab therapy in combination with other immunoregulatory and immunosuppressive agents were diagnosed with progressive multifocal leukoencephalopathy (PML) after its initial approval, therefore the usage of the agent is restricted to monotherapy in patients with relapsing forms of MS (Warnke et al. 2010). Furthermore, the combination of natalizumab with interferon-β 1α (IFN-β 1α) is significantly more effective than IFN-β 1α alone in patients with relapsing MS (Radue et al. 2010; Rudick et al. 2006). Thus, adhesion-molecule inhibitors hold promise as an effective treatment for relapsing MS.
7.3 Integrin α4β7 in Inflammatory Bowel Disease (IBD)
IBD is a chronic and prejudicial inflammation of the gastrointestinal (GI) tract, including Crohn’s disease (CD) and ulcerative colitis (UC). The former is diagnosed with intermittent transmural inflammation that occurs mostly on the terminal ileum of the small intestine before the large intestine (colon) but can also affect other sites in the GI tract from the mouth to the anus. Unlike CD, UC primarily occurs in the large intestine (colon) and the rectum, with pathological features characterized by continuous inflammation in the superficial mucosa starting from the rectum and extending further into the large intestine (Gorfu et al. 2009). CD and UC share common clinical symptoms, including persistent diarrhea, abdominal pain, rectal bleeding, bloody stools, body weight loss, and fatigue, seriously hindering the quality of life of the patient (Waljee et al. 2009).
Activation of the immune response generally occurs in IBD patients, manifested by various alterations in inflammatory cytokines and Ig family protein production (de Souza and Fiocchi 2016). During the progression of IBD, the chronic inflammation is accompanied by the accumulation of macrophages, CD4+ and CD8+ T cells, B cells, and other leukocytes in the LP, and crypt abscesses with a high production of cytokines, including TNF-α, IFN-γ, IL-12, IL-13, and IL-5 (de Souza and Fiocchi 2016; Strober et al. 2007; Xavier and Podolsky 2007). Of note, integrin α4β7-mediated lymphocyte trafficking to intestinal tissues is deemed the most significant inducement in IBD etiopathogenesis (Table 1) (Neurath 2014; Zhang et al. 2016), whose inhibitors show promising therapeutic effects in clinical implications of IBD patients. Natalizumab, which targets the integrin α4 subunit to block α4β7 binding to VCAM-1/MAdCAM-1 and α4β1–VCAM-1 binding, provides favorable effects in treating CD patients who are refractory to standard therapy (Mezu-Ndubuisi and Maheshwari 2021). Unfortunately, PML, a rare and often fatal side effect of natalizumab in IBD patients, restricts the use of this drug during treatment (Li et al. 2018b). Vedolizumab, an integrin α4β7 blocking mAb, came on the market for IBD treatment in 2014 from Takeda. It specifically inhibits the interaction between α4β7 and MAdCAM-1 without affecting α4β1 function; thus, it avoids the PML-associated side effects of natalizumab and other systemic immunosuppression influences (Sandborn et al. 2013).
The successful use of vedolizumab in IBD highlights the research and development of therapeutic targets aiming at the gut-tropic molecule α4β7. Recently, abrilumab (Amgen), also called AMG-181, targeting the α4β7 integrin heterodimer, shows encouraging results in a phase II study on moderate to severe CD and UC (Pan et al. 2013). In addition, etrolizumab from Genentech, mAb specifically targets the β7 subunit to block both α4β7- and αEβ7-mediated adhesion, is now in an ongoing robust phase II study on UC and phase III study on CD (Selinger et al. 2018).
7.4 Integrin α4β7 in Acquired Immunodeficiency Syndrome (AIDS)
Acute HIV infection features high virus replication within the GALT, accompanied by a remarkable reduction in CD4+ T cells, especially the gut-homing integrin α4β7-expressing CD4+ T cells (Table 1) (Cicala et al. 2009; Guadalupe et al. 2003). It has been demonstrated that the HIV-1 envelope glycoprotein gp120 can bind α4β7 through its key residues localized in the V2 domain (V2-loop) (Richardson et al. 2015), facilitating the HIV virion-α4β7+CD4+ T-cell complex recruitment to intestinal tissues via an α4β7 interaction with MAdCAM-1 (Liu and Lusso 2020). During acute HIV infection, the α4β7high memory CD4+ T cells are thought to be the early and primary targets of HIV (Cicala et al. 2011; Pena-Cruz et al. 2013).
Integrin α4β7-gp120 binding and further incorporation of α4β7 in HIV virions exist in a selective manner (Guzzo et al. 2017; Wang et al. 2021). It was recently reported that gp120 only binds to α4β7 active conformers with highly extended conformations, which can be induced by particular chemokines, such as CCL19 and CCL25, and the binding of gp120 to α4β7 induces the activation of multiple signal pathways in T cells (Wang et al. 2021). The α4β7-directed virus gut-tropic distribution subsequently leads to HIV colonization and replication in gut-related tissues in the early stage of HIV infection, further resulting in massive depletion of CD4+ T cells and structural damage of the GI tract (Brenchley et al. 2004; Cicala et al. 2009).
The α4β7 blocking mAb vedolizumab and β7 blocking mAb etrolizumab have shown efficient inhibition of gp120 binding to α4β7 (Wang et al. 2021), supporting the inhibitory effects of α4β7 neutralization in HIV infection (Li et al. 2018a). To date, several open-label, single-arm clinical trials with vedolizumab are being conducted with HIV-infected individuals in the USA, Spain, Canada, and France to better evaluate the effects of the α4β7 inhibitor in anti-HIV therapy (Burnie and Guzzo 2019; Sneller et al. 2019).
7.5 Integrin α4β7 in Graft-Versus-Host Disease
GvHD is identified as two distinct entities: acute and chronic GvHD (Martinez-Cibrian et al. 2021). Acute GvHD (aGvHD) is an immune syndrome induced by activated donor effector T cells, which are CTLs, recognizing host antigens and initiating immune responses to attack host organs, such as the GI tract, skin, and liver (Table 1) (Welniak et al. 2007). It frequently occurs in patients adopting allogeneic HSCT, whose grade of aGvHD is negatively correlated with prognosis and is considered the major cause of mortality post-HSCT surgery (Deeg 2007; Martin et al. 2012).
During aGvHD, donor T cells migrate to intestinal tissues, such as MLN and Peyer’s patches utilizing the integrin α4β7–MAdCAM-1 interaction (Dutt et al. 2007). It has been shown that depletion of α4β7 (Petrovic et al. 2004) or β7 (Waldman et al. 2006) on donor T cells and interception of the α4β7–MAdCAM-1 interaction (Ueha et al. 2007) can alleviate aGvHD-induced gut damage in murine allogeneic BM transplantation (BMT) models. Promising data obtained from murine transplant models suggests the usage of integrin α4β7 blocking mAb that prevents α4β7–MAdCAM-1 binding in the treatment of intestinal aGvHD. Integrin α4β7 mAb vedolizumab has now been evaluated to treat steroid-refractory (SR) GI aGvHD in phase I trials and showed a reduced incidence of high-grade aGvHD without generating adverse effects (Chen et al. 2019; Danylesko et al. 2019). However, these results need to be further validated in prospective clinical trials.
8 Conclusion and Future Perspectives
Integrin α4β1 and α4β7 are constitutively expressed on some leukocyte populations. Upon stimulation, α4 integrin expression can be induced on the surface of some leukocytes (Hemler et al. 1987b; Kirveskari et al. 2000). The α4 integrin-mediated aberrant homing of leukocytes to the CNS or gut plays a critical role in MS or IBD, respectively. Blocking antibodies targeting α4 integrins, including natalizumab and vedolizumab, have been used clinically and show efficacy in treating MS and IBD. It is noteworthy that natalizumab treatment may induce PML. Moreover, some UC patients exhibited aggravated colitis after vedolizumab, which the aberrant innate immune response may cause after fully blocking α4β7. Therefore, instead of fully blocking α4 integrins, more precise regulation of α4 integrin function, such as blocking the aberrant integrin activation, could be a better strategy for managing MS and IBD. Screening small molecule compounds or mAbs for blocking the activation of α4 integrins could lead to discovering next-generation MS/IBD drugs with fewer adverse effects (Baiula et al. 2019).
The interaction between integrins and different ligands enables the targeting of lymphocytes to different tissues. Each leukocyte integrin can recognize multiple ligands, which makes the tissue-specific leukocyte homing complicated. Some studies have revealed that different chemokines can induce ligand-specific activation of integrin α4β7, which allows the selective binding of α4β7 to either MAdCAM-1 or VCAM-1 to ensure a tissue-specific homing of lymphocytes (Sun et al. 2014; Wang et al. 2018). Notably, when chemokines promote α4β7 to one ligand, it inhibits α4β7 binding to the other ligand. The chemokine-induced inhibition of α4β7 binding to its ligands may be involved in the selective recruitment of different immune cells into tissues under pathological conditions, which deserves further investigation.
Although integrin α4β7 has been characterized in-depth as a gut-homing molecule expressed on the surface of lymphocytes, it also plays a role in several innate immune cell subtypes, including the BM precursor cells, which differentiate into tolerogenic, RA-secreting DCs, and NK cells and monocytes (Bouchentouf et al. 2010; Picarella et al. 1997; Schleier et al. 2020; Villablanca et al. 2014). The regulatory function of α4β7 appears disparate among different cell types and may be more complex than originally speculated. More precise studies need to be conducted to investigate the distinct functions in specific immune cell subsets during both homeostatic and pathologic processes.
References
Agace W (2010) Generation of gut-homing T cells and their localization to the small intestinal mucosa. Immunol Lett 128:21–23
Agace WW, Persson EK (2012) How vitamin a metabolizing dendritic cells are generated in the gut mucosa. Trends Immunol 33:42–48
Altevogt P, Hubbe M, Ruppert M, Lohr J, von Hoegen P, Sammar M, Andrew DP, McEvoy L, Humphries MJ, Butcher EC (1995) The alpha 4 integrin chain is a ligand for alpha 4 beta 7 and alpha 4 beta 1. J Exp Med 182:345–355
Andrew DP, Rott LS, Kilshaw PJ, Butcher EC (1996) Distribution of alpha 4 beta 7 and alpha E beta 7 integrins on thymocytes, intestinal epithelial lymphocytes and peripheral lymphocytes. Eur J Immunol 26:897–905
Anthis NJ, Haling JR, Oxley CL, Memo M, Wegener KL, Lim CJ, Ginsberg MH, Campbell ID (2009) Beta integrin tyrosine phosphorylation is a conserved mechanism for regulating Talin-induced integrin activation. J Biol Chem 284:36700–36710
Arnaout MA, Mahalingam B, Xiong JP (2005) Integrin structure, allostery, and bidirectional signaling. Annu Rev Cell Dev Bi 21:381–410
Arroyo AG, Yang JT, Rayburn H, Hynes RO (1996) Differential requirements for alpha4 integrins during fetal and adult hematopoiesis. Cell 85:997–1008
Arroyo AG, Yang JT, Rayburn H, Hynes RO (1999) Alpha4 integrins regulate the proliferation/differentiation balance of multilineage hematopoietic progenitors in vivo. Immunity 11:555–566
Arthos J, Cicala C, Martinelli E, Macleod K, Van Ryk D, Wei D, Xiao Z, Veenstra TD, Conrad TP, Lempicki RA et al (2008) HIV-1 envelope protein binds to and signals through integrin alpha(4)beta(7), the gut mucosal homing receptor for peripheral T cells. Nat Immunol 9:301–309
Baiula M, Spampinato S, Gentilucci L, Tolomelli A (2019) Novel ligands targeting alpha4beta1 integrin: therapeutic applications and perspectives. Front Chem 7:489
Baldini LG, Cro LM (1994) Structure and function of VLA integrins: differential expression in B-cell leukemia/lymphoma. Leuk Lymphoma 12:197–203
Baron JL, Madri JA, Ruddle NH, Hashim G, Janeway CA (1993) Surface expression of Alpha-4 integrin by Cd4 T-cells is required for their entry into brain parenchyma. J Exp Med 177:57–68
Bayless KJ, Davis GE (2001) Identification of dual alpha 4beta1 integrin binding sites within a 38 amino acid domain in the N-terminal thrombin fragment of human osteopontin. J Biol Chem 276:13483–13489
Bayless KJ, Meininger GA, Scholtz JM, Davis GE (1998) Osteopontin is a ligand for the alpha4beta1 integrin. J Cell Sci 111(Pt 9):1165–1174
Beglova N, Blacklow SC, Takagi J, Springer TA (2002) Cysteine-rich module structure reveals a fulcrum for integrin rearrangement upon activation. Nat Struct Biol 9:282–287
Berlin C, Bargatze RF, Campbell JJ, von Andrian UH, Szabo MC, Hasslen SR, Nelson RD, Berg EL, Erlandsen SL, Butcher EC (1995) Alpha 4 integrins mediate lymphocyte attachment and rolling under physiologic flow. Cell 80:413–422
Berlin-Rufenach C, Otto F, Mathies M, Westermann J, Owen MJ, Hamann A, Hogg N (1999) Lymphocyte migration in lymphocyte function-associated antigen (LFA)-1-deficient mice. J Exp Med 189:1467–1478
Bird L (2019) T cells feel the heat. Nat Rev Immunol 19:139
Bouchentouf M, Forner KA, Cuerquis J, Michaud V, Zheng JM, Paradis P, Schiffrin EL, Galipeau J (2010) Induction of cardiac angiogenesis requires killer cell lectin-like receptor 1 and alpha 4 beta 7 integrin expression by NK cells. J Immunol 185:7014–7025
Bouvard D, Brakebusch C, Gustafsson E, Aszodi A, Bengtsson T, Berna A, Fassler R (2001) Functional consequences of integrin gene mutations in mice. Circ Res 89:211–223
Bouvard D, Pouwels J, De Franceschi N, Ivaska J (2013) Integrin inactivators: balancing cellular functions in vitro and in vivo. Nat Rev Mol Cell Biol 14:430–442
Brakebusch C, Fillatreau S, Potocnik AJ, Bungartz G, Wilhelm P, Svensson M, Kearney P, Korner H, Gray D, Fassler R (2002) Beta1 integrin is not essential for hematopoiesis but is necessary for the T cell-dependent IgM antibody response. Immunity 16:465–477
Brandt EB, Zimmermann N, Muntel EE, Yamada Y, Pope SM, Mishra A, Hogan SP, Rothenberg ME (2006) The alpha 4 beta 7-integrin is dynamically expressed on murine eosinophils and involved in eosinophil trafficking to the intestine. Clin Exp Allergy 36:543–553
Brenchley JM, Schacker TW, Ruff LE, Price DA, Taylor JH, Beilman GJ, Nguyen PL, Khoruts A, Larson M, Haase AT et al (2004) CD4(+) T cell depletion during all stages of HIV disease occurs predominantly in the gastrointestinal tract. J Exp Med 200:749–759
Bridges LC, Sheppard D, Bowditch RD (2005) ADAM disintegrin-like domain recognition by the lymphocyte integrins alpha4beta1 and alpha4beta7. Biochem J 387:101–108
Bungartz G, Stiller S, Bauer M, Muller W, Schippers A, Wagner N, Fassler R, Brakebusch C (2006) Adult murine hematopoiesis can proceed without beta1 and beta7 integrins. Blood 108:1857–1864
Burke RD (1999) Invertebrate integrins: structure, function, and evolution. Int Rev Cytol 191:257–284
Burnie J, Guzzo C (2019) The incorporation of host proteins into the external HIV-1 envelope. Viruses-Basel 11(1):85
Butcher EC, Picker LJ (1996) Lymphocyte homing and homeostasis. Science 272:60–66
Calderwood DA, Zent R, Grant R, Rees DJG, Hynes RO, Ginsberg MH (1999) The Talin head domain binds to integrin beta subunit cytoplasmic tails and regulates integrin activation. J Biol Chem 274:28071–28074
Calderwood DA, Huttenlocher A, Kiosses WB, Rose DM, Woodside DG, Schwartz MA, Ginsberg MH (2001) Increased filamin binding to beta-integrin cytoplasmic domains inhibits cell migration. Nat Cell Biol 3:1060–1068
Calderwood DA, Yan BX, de Pereda JM, Alvarez BG, Fujioka Y, Liddington RC, Ginsberg MH (2002) The phosphotyrosine binding-like domain of Talin activates Integrins. J Biol Chem 277:21749–21758
Calderwood DA, Fujioka Y, de Pereda JM, Garcia-Alvarez B, Nakamoto T, Margolis B, McGlade CJ, Liddington RC, Ginsberg MH (2003) Integrin beta cytoplasmic domain interactions with phosphotyrosine-binding domains: a structural prototype for diversity in integrin signaling. Proc Natl Acad Sci U S A 100:2272–2277
Calderwood DA, Campbell ID, Critchley DR (2013a) Talins and kindlins: partners in integrin-mediated adhesion. Nat Rev Mol Cell Bio 14:503–517
Calderwood DA, Campbell ID, Critchley DR (2013b) Talins and kindlins: partners in integrin-mediated adhesion. Nat Rev Mol Cell Biol 14:503–517
Carman CV, Springer TA (2003) Integrin avidity regulation: are changes in affinity and conformation underemphasized? Curr Opin Cell Biol 15:547–556
Carman CV, Springer TA (2004) A transmigratory cup in leukocyte diapedesis both through individual vascular endothelial cells and between them. J Cell Biol 167:377–388
Chan BM, Kassner PD, Schiro JA, Byers HR, Kupper TS, Hemler ME (1992) Distinct cellular functions mediated by different VLA integrin alpha subunit cytoplasmic domains. Cell 68:1051–1060
Chen JF, Salas A, Springer TA (2003) Bistable regulation of integrin adhesiveness by a bipolar metal ion cluster. Nat Struct Biol 10:995–1001
Chen J, Takagi J, Xie C, Xiao T, Luo BH, Springer TA (2004) The relative influence of metal ion binding sites in the I-like domain and the interface with the hybrid domain on rolling and firm adhesion by integrin alpha4beta7. J Biol Chem 279:55556–55561
Chen YB, Kim HT, McDonough S, Odze RD, Yao XP, Lazo-Kallanian S, Spitzer TR, Soiffer R, Antin JH, Ritz J (2009) Up-regulation of alpha 4 beta 7 integrin on peripheral T cell subsets correlates with the development of acute intestinal graft-versus-host disease following allogeneic stem cell transplantation. Biol Blood Marrow Tr 15:1066–1076
Chen YB, McDonough S, Chen H, Kennedy J, Illiano C, Attar EC, Ballen KK, Dey BR, McAfee SL, Jagasia M et al (2013) Expression of alpha 4 beta 7 integrin on memory CD8(+) T cells at the presentation of acute intestinal GVHD. Bone Marrow Transpl 48:598–603
Chen YB, Shah NN, Renteria AS, Cutler C, Jansson J, Akbari M, Chen CL, Quadri S, Parfionovas A, Devine SM (2019) Vedolizumab for prevention of graft-versus-host disease after allogeneic hematopoietic stem cell transplantation. Blood Adv 3:4136–4146
Chigaev A, Waller A, Amit O, Halip L, Bologa CG, Sklar LA (2009) Real-time analysis of conformation-sensitive antibody binding provides new insights into integrin conformational regulation. J Biol Chem 284:14337–14346
Chua GL, Patra AT, Tan SM, Bhattacharjya S (2013) NMR structure of integrin alpha4 cytosolic tail and its interactions with paxillin. PLoS One 8:e55184
Cicala C, Martinelli E, McNally JP, Goode DJ, Gopaul R, Hiatt J, Jelicic K, Kottilil S, Macleod K, O’Shea A et al (2009) The integrin alpha(4)beta(7) forms a complex with cell-surface CD4 and defines a T-cell subset that is highly susceptible to infection by HIV-1. P Natl Acad Sci USA 106:20877–20882
Cicala C, Arthos J, Fauci AS (2011) HIV-1 envelope, integrins and co-receptor use in mucosal transmission of HIV. J Transl Med 9(Suppl 1):S2
Cimbro R, Vassena L, Arthos J, Cicala C, Kehrl JH, Park C, Sereti I, Lederman MM, Fauci AS, Lusso P (2012) IL-7 induces expression and activation of integrin alpha 4 beta 7 promoting naive T-cell homing to the intestinal mucosa. Blood 120:2610–2619
Clayberger C, Krensky AM, McIntyre BW, Koller TD, Parham P, Brodsky F, Linn DJ, Evans EL (1987) Identification and characterization of two novel lymphocyte function-associated antigens, L24 and L25. J Immunol 138:1510–1514
Cox D, Brennan M, Moran N (2011) Integrins as therapeutic targets: lessons and opportunities. Nat Rev Drug Discov 9:804–820
Critchley DR (2009) Biochemical and structural properties of the integrin-associated cytoskeletal protein Talin. Annu Rev Biophys 38:235–254
Cunningham SA, Rodriguez JM, Arrate MP, Tran TM, Brock TA (2002) JAM2 interacts with alpha4beta1. Facilitation by JAM3. J Biol Chem 277:27589–27592
Danylesko I, Bukauskas A, Paulson M, Peceliunas V, Gedde-Dahl T, Shimoni A, Shouval R, Griskevicius L, Floisand Y, Nagler A (2019) Anti-a4 beta 7 integrin monoclonal antibody (vedolizumab) for the treatment of steroid-resistant severe intestinal acute graft-versus-host disease. Bone Marrow Transpl 54:987–993
de Souza HSP, Fiocchi C (2016) Immunopathogenesis of IBD: current state of the art. Nat Rev Gastro Hepat 13:13–27
Deeg HJ (2007) How I treat refractory acute GVHD. Blood 109:4119–4126
DeNucci CC, Pagan AJ, Mitchell JS, Shimizu Y (2010) Control of alpha 4 beta 7 integrin expression and CD4 T cell homing by the beta 1 integrin subunit. J Immunol 184:2458–2467
Dutt S, Tseng D, Ermann J, George TI, Liu YP, Davis CR, Fathman CG, Strober S (2007) Naive and memory T cells induce different types of graft-versus-host disease. J Immunol 179:6547–6554
Elices MJ, Osborn L, Takada Y, Crouse C, Luhowskyj S, Hemler ME, Lobb RR (1990) Vcam-1 on activated endothelium interacts with the leukocyte integrin Vla-4 at a site distinct from the Vla-4 fibronectin binding-site. Cell 60:577–584
Engelhardt B, Laschinger M, Schulz M, Samulowitz U, Vestweber D, Hoch G (1998) The development of experimental autoimmune encephalomyelitis in the mouse requires alpha4-integrin but not alpha4beta7-integrin. J Clin Invest 102:2096–2105
Ennis E, Isberg RR, Shimizu Y (1993) Very late antigen 4-dependent adhesion and costimulation of resting human T cells by the bacterial beta 1 integrin ligand invasin. J Exp Med 177:207–212
Erle DJ, Ruegg C, Sheppard D, Pytela R (1991) Complete amino acid sequence of an integrin beta subunit (beta 7) identified in leukocytes. J Biol Chem 266:11009–11016
Erle DJ, Briskin MJ, Butcher EC, Garcia-Pardo A, Lazarovits AI, Tidswell M (1994) Expression and function of the MAdCAM-1 receptor, integrin alpha 4 beta 7, on human leukocytes. J Immunol 153:517–528
Feral CC, Rose DM, Han J, Fox N, Silverman GJ, Kaushansky K, Ginsberg MH (2006) Blocking the alpha 4 integrin-paxillin interaction selectively impairs mononuclear leukocyte recruitment to an inflammatory site. J Clin Invest 116:715–723
Gazitt Y, Akay C (2004) Mobilization of myeloma cells involves SDF-1/CXCR4 signaling and downregulation of VLA-4. Stem Cells 22:65–73
Goldfinger LE, Han J, Kiosses WB, Howe AK, Ginsberg MH (2003) Spatial restriction of alpha4 integrin phosphorylation regulates lamellipodial stability and alpha4beta1-dependent cell migration. J Cell Biol 162:731–741
Gorfu G, Rivera-Nieves J, Ley K (2009) Role of beta(7) Integrins in intestinal lymphocyte homing and retention. Curr Mol Med 9:836–850
Guadalupe M, Reay E, Sankaran S, Prindiville T, Flamm J, McNeil A, Dandekar S (2003) Severe CD4(+) T-cell depletion in gut lymphoid tissue during primary human immunodeficiency virus type 1 infection and substantial delay in restoration following highly active antiretroviral therapy. J Virol 77:11708–11717
Guan JL, Hynes RO (1990) Lymphoid cells recognize an alternatively spliced segment of fibronectin via the integrin receptor alpha 4 beta 1. Cell 60:53–61
Guo J, Zhang Y, Li H, Chu H, Wang Q, Jiang S, Li Y, Shen H, Li G, Chen J et al (2018) Intramembrane ionic protein-lipid interaction regulates integrin structure and function. PLoS Biol 16:e2006525
Gurtner GC, Davis V, Li H, McCoy MJ, Sharpe A, Cybulsky MI (1995) Targeted disruption of the murine VCAM1 gene: essential role of VCAM-1 in chorioallantoic fusion and placentation. Genes Dev 9:1–14
Guy-Grand D, Vassalli P, Eberl G, Pereira P, Burlen-Defranoux O, Lemaitre F, Di Santo JP, Freitas AA, Cumano A, Bandeira A (2013) Origin, trafficking, and intraepithelial fate of gut-tropic T cells (vol 210, pg 1839, 2013). J Exp Med 210:2493–2493
Guzzo C, Ichikawa D, Park C, Phillips D, Liu QB, Zhang P, Kwon A, Miao HY, Lu J, Rehm C et al (2017) Virion incorporation of integrin alpha 4 beta 7 facilitates HIV-1 infection and intestinal homing. Sci Immunol 2(11):eaam7341
Habtezion A, Nguyen LP, Hadeiba H, Butcher EC (2016) Leukocyte trafficking to the small intestine and colon. Gastroenterology 150:340–354
Hamidi H, Ivaska J (2019) Every step of the way: integrins in cancer progression and metastasis (vol 18, pg 533, 2018). Nat Rev Cancer 19:179–179
Hampton T (2019) Fever induces a molecular homing response in immune cells during infection. JAMA 321:1657–1658
Han J, Liu S, Rose DM, Schlaepfer DD, McDonald H, Ginsberg MH (2001) Phosphorylation of the integrin alpha 4 cytoplasmic domain regulates paxillin binding. J Biol Chem 276:40903–40909
Hao XY, Zhong XF, Sun X (2021) The effects of all-trans retinoic acid on immune cells and its formulation design for vaccines. AAPS J 23(2):32
Harburger DS, Calderwood DA (2009) Integrin signalling at a glance. J Cell Sci 122:159–163
Harburger DS, Bouaouina M, Calderwood DA (2009) Kindlin-1 and -2 directly bind the C-terminal region of beta integrin cytoplasmic tails and exert integrin-specific activation effects. J Biol Chem 284:11485–11497
Hemler ME, Jacobson JG, Brenner MB, Mann D, Strominger JL (1985) Vla-1 - a T-cell surface-antigen which defines a novel late stage of human T-cell activation. Eur J Immunol 15:502–508
Hemler ME, Huang C, Schwarz L (1987a) The Vla protein family - characterization of 5 distinct cell-surface heterodimers each with a common 130,000 molecular-weight Beta-subunit. J Biol Chem 262:3300–3309
Hemler ME, Huang C, Takada Y, Schwarz L, Strominger JL, Clabby ML (1987b) Characterization of the cell surface heterodimer VLA-4 and related peptides. J Biol Chem 262:11478–11485
Hogg N, Patzak I, Willenbrock F (2011) The insider’s guide to leukocyte integrin signalling and function. Nat Rev Immunol 11:416–426
Holzmann B, Weissman IL (1989) Peyers patch-specific lymphocyte homing receptors consist of a Vla-4-like alpha-chain associated with either of 2 integrin Beta-chains, one of which is novel. EMBO J 8:1735–1741
Hosen N (2020) Integrins in multiple myeloma. Inflamm Regen 40:4
Hosen N, Matsunaga Y, Hasegawa K, Matsuno H, Nakamura Y, Makita M, Watanabe K, Yoshida M, Satoh K, Morimoto S et al (2017) The activated conformation of integrin beta(7) is a novel multiple myeloma-specific target for CAR T cell therapy. Nat Med 23:1436-+
Hughes AL (2001) Evolution of the integrin alpha and beta protein families. J Mol Evol 52:63–72
Humphries JD, Humphries MJ (2007) CD14 is a ligand for the integrin alpha4beta1. FEBS Lett 581:757–763
Humphries MJ, Symonds EJ, Mould AP (2003) Mapping functional residues onto integrin crystal structures. Curr Opin Struct Biol 13:236–243
Hurt EM, Wiestner A, Rosenwald A, Shaffer AL, Campo E, Grogan T, Bergsagel PL, Kuehl WM, Staudt LM (2004) Overexpression of c-maf is a frequent oncogenic event in multiple myeloma that promotes proliferation and pathological interactions with bone marrow stroma. Cancer Cell 5:191–199
Hynes RO (1987) Integrins - a family of cell-surface receptors. Cell 48:549–554
Hynes RO (2002) Integrins: bidirectional, allosteric signaling machines. Cell 110:673–687
Iwata M, Hirakiyama A, Eshima Y, Kagechika H, Kato C, Song SY (2004) Retinoic acid imprints gut-homing specificity on T cells. Immunity 21:527–538
Johnson MS, Lu N, Denessiouk K, Heino J, Gullberg D (2009) Integrins during evolution: evolutionary trees and model organisms. Biochim Biophys Acta 1788:779–789
Johnston B, Kubes P (1999) The alpha4-integrin: an alternative pathway for neutrophil recruitment? Immunol Today 20:545–550
Kassner PD, Teixido J, Chan BM, Parker CM, Hemler ME (1992) Analyses of VLA-4 structure and function. Adv Exp Med Biol 323:163–170
Kempster SL, Kaser A (2014) Alpha(4)beta(7) integrin: beyond T cell trafficking. Gut 63:1377–U1330
Kent SJ, Karlik SJ, Cannon C, Hines DK, Yednock TA, Fritz LC, Horner HC (1995a) A monoclonal antibody to alpha 4 integrin suppresses and reverses active experimental allergic encephalomyelitis. J Neuroimmunol 58:1–10
Kent SJ, Karlik SJ, Cannon C, Hines DK, Yednock TA, Fritz LC, Horner HC (1995b) A monoclonal-antibody to Alpha-4 integrin suppresses and reverses active experimental allergic encephalomyelitis. J Neuroimmunol 58:1–10
Kerfoot SM, Kubes P (2002) Overlapping roles of P-selectin and alpha 4 integrin to recruit leukocytes to the central nervous system in experimental autoimmune encephalomyelitis. J Immunol 169:1000–1006
Kilger G, Needham LA, Nielsen PJ, Clements J, Vestweber D, Holzmann B (1995) Differential regulation of alpha 4 integrin-dependent binding to domains 1 and 4 of vascular cell adhesion molecule-1. J Biol Chem 270:5979–5984
Kilshaw PJ, Murant SJ (1991) Expression and regulation of beta 7(beta p) integrins on mouse lymphocytes: relevance to the mucosal immune system. Eur J Immunol 21:2591–2597
Kim M, Carman CV, Springer TA (2003) Bidirectional transmembrane signaling by cytoplasmic domain separation in integrins. Science 301:1720–1725
Kim C, Schmidt T, Cho EG, Ye F, Ulmer TS, Ginsberg MH (2011) Basic amino-acid side chains regulate transmembrane integrin signalling. Nature 481:209–213
Kirveskari J, Bono P, Granfors K, Leirisalo-Repo M, Jalkanen S, Salmi M (2000) Expression of alpha4-integrins on human neutrophils. J Leukoc Biol 68:243–250
Koopman G, Keehnen RM, Lindhout E, Newman W, Shimizu Y, van Seventer GA, de Groot C, Pals ST (1994) Adhesion through the LFA-1 (CD11a/CD18)-ICAM-1 (CD54) and the VLA-4 (CD49d)-VCAM-1 (CD106) pathways prevents apoptosis of germinal center B cells. J Immunol 152:3760–3767
Kummer C, Petrich BG, Rose DM, Ginsberg MH (2010) A small molecule that inhibits the interaction of Paxillin and alpha 4 integrin inhibits accumulation of mononuclear leukocytes at a site of inflammation. J Biol Chem 285:9462–9469
Kwee L, Baldwin HS, Shen HM, Stewart CL, Buck C, Buck CA, Labow MA (1995) Defective development of the embryonic and extraembryonic circulatory systems in vascular cell adhesion molecule (VCAM-1) deficient mice. Development 121:489–503
Larson RS, Corbi AL, Berman L, Springer T (1989) Primary structure of the leukocyte function-associated molecule-1 alpha subunit: an integrin with an embedded domain defining a protein superfamily. J Cell Biol 108:703–712
Lau TL, Kim C, Ginsberg MH, Ulmer TS (2009) The structure of the integrin alpha IIb beta 3 transmembrane complex explains integrin transmembrane signalling. EMBO J 28:1351–1361
Laudanna C, Kim JY, Constantin G, Butcher EC (2002) Rapid leukocyte integrin activation by chemokines. Immunol Rev 186:37–46
Legate KR, Montanez E, Kudlacek O, Fassler R (2006) ILK, PINCH and parvin: the tIPP of integrin signalling. Nat Rev Mol Cell Biol 7:20–31
Leussink VI, Zettl UK, Jander S, Pepinsky RB, Lobb RR, Stoll G, Toyka KV, Gold R (2002) Blockade of signaling via the very late antigen (VLA-4) and its counterligand vascular cell adhesion molecule-1 (VCAM-1) causes increased T cell apoptosis in experimental autoimmune neuritis. Acta Neuropathol 103:131–136
Ley K, Laudanna C, Cybulsky MI, Nourshargh S (2007) Getting to the site of inflammation: the leukocyte adhesion cascade updated. Nat Rev Immunol 7:678–689
Li H, Huang SY, Shi FH, Gu ZC, Zhang SG, Wei JF (2018a) Alpha(4)beta(7) integrin inhibitors: a patent review. Expert Opin Ther Pat 28:903–917
Li H, Shi FH, Huang SY, Zhang SG, Chen ML (2018b) A review on clinical pharmacokinetics, pharmacodynamics, and pharmacogenomics of Natalizumab: a humanized anti-alpha 4 integrin monoclonal antibody. Curr Drug Metab 19:1213–1223
Lin CD, Chen JF (2019) Regulation of immune cell trafficking by febrile temperatures. Int J Hyperth 36:17–21
Lin CD, Zhang YH, Zhang K, Zheng YJ, Lu L, Chang HS, Yang H, Yang YR, Wan YY, Wang SH et al (2019) Fever promotes T lymphocyte trafficking via a thermal sensory pathway involving heat shock protein 90 and alpha 4 Integrins. Immunity 50:137-+
Lin C, Liu Z, Li Y, Chen J (2021) Protocol for fever-range whole-body hyperthermia (WBH) in mice to study febrile effect on T-cell adhesion and migration. STAR Protoc 2:100720
Liu W, Boggon TJ (2013) Cocrystal structure of the ICAP1 PTB domain in complex with a KRIT1 peptide. Acta Crystallogr Sect F Struct Biol Cryst Commun 69:494–498
Liu S, Ginsberg MH (2000) Paxillin binding to a conserved sequence motif in the alpha 4 integrin cytoplasmic domain. J Biol Chem 275:22736–22742
Liu QB, Lusso P (2020) Integrin alpha 4 beta 7 in HIV-1 infection: a critical review. J Leukoc Biol 108:627–632
Liu S, Thomas SM, Woodside DG, Rose DM, Kiosses WB, Pfaff M, Ginsberg MH (1999) Binding of paxillin to alpha4 integrins modifies integrin-dependent biological responses. Nature 402:676–681
Liu S, Kiosses WB, Rose DM, Slepak M, Salgia R, Griffin JD, Turner CE, Schwartz MA, Ginsberg MH (2002) A fragment of paxillin binds the alpha 4 integrin cytoplasmic domain (tail) and selectively inhibits alpha 4-mediated cell migration. J Biol Chem 277:20887–20894
Liu J, Fu T, Peng B, Sun H, Chu H, Li G, Chen J (2014) The hydrophobic contacts between the center of the betaI domain and the alpha1/alpha7 helices are crucial for the low-affinity state of integrin alpha4 beta7. FEBS J 281:2915–2926
Lu CF, Takagi J, Springer TA (2001) Association of the membrane proximal regions of the alpha and beta subunit cytoplasmic domains constrains an integrin in the inactive state. J Biol Chem 276:14642–14648
Lu L, Lin C, Yan Z, Wang S, Zhang Y, Wang S, Wang J, Liu C, Chen J (2016a) Kindlin-3 is essential for the resting alpha4beta1 integrin-mediated firm cell adhesion under shear flow conditions. J Biol Chem 291:10363–10371
Lu Z, Mathew S, Chen J, Hadziselimovic A, Palamuttam R, Hudson BG, Fassler R, Pozzi A, Sanders CR, Zent R (2016b) Implications of the differing roles of the beta1 and beta3 transmembrane and cytoplasmic domains for integrin function. elife 5:e18633
Luo BH, Carman CV, Springer TA (2007) Structural basis of integrin regulation and signaling. Annu Rev Immunol 25:619–647
Luster AD, Alon R, von Andrian UH (2005) Immune cell migration in inflammation: present and future therapeutic targets. Nat Immunol 6:1182–1190
Malinin NL, Plow EF, Byzova TV (2010) Kindlins in FERM adhesion. Blood 115:4011–4017
Martin PJ, Rizzo JD, Wingard JR, Ballen K, Curtin PT, Cutler C, Litzow MR, Nieto Y, Savani BN, Schriber JR et al (2012) First- and second-line systemic treatment of acute graft-versus-host disease: recommendations of the American Society of Blood and Marrow Transplantation. Biol Blood Marrow Tr 18:1150–1163
Martinez-Cibrian N, Zeiser R, Perez-Simon JA (2021) Graft-versus-host disease prophylaxis: pathophysiology-based review on current approaches and future directions. Blood Rev 48:100792
Masumoto A, Hemler ME (1993) Mutation of putative divalent-cation sites in the alpha(4) subunit of the integrin Vla-4 - distinct effects on adhesion to Cs1/fibronectin, Vcam-1, and Invasin. J Cell Biol 123:245–253
Mezu-Ndubuisi OJ, Maheshwari A (2021) The role of integrins in inflammation and angiogenesis. Pediatr Res 89:1619–1626
Michie SA, Streeter PR, Butcher EC, Rouse RV (1995) L-selectin and alpha(4)Beta(7) integrin homing receptor pathways mediate peripheral lymphocyte traffic to Akr mouse hyperplastic thymus. Am J Pathol 147:412–421
Mittelbrunn M, Molina A, Escribese MM, Yanez-Mo M, Escudero E, Ursa A, Tejedor R, Mampaso F, Sanchez-Madrid F (2004) VLA-4 integrin concentrates at the peripheral supramolecular activation complex of the immune synapse and drives T helper 1 responses. Proc Natl Acad Sci U S A 101:11058–11063
Miyake K, Weissman IL, Greenberger JS, Kincade PW (1991) Evidence for a role of the integrin VLA-4 in lympho-hemopoiesis. J Exp Med 173:599–607
Mora JR, Iwata M, Eksteen B, Song SY, Junt T, Senman B, Otipoby KL, Yokota A, Takeuchi H, Ricciardi-Castagnoli P et al (2006) Generation of gut-homing IgA-secreting B cells by intestinal dendritic cells. Science 314:1157–1160
Mould AP, Askari JA, Craig SE, Garratt AN, Clements J, Humphries MJ (1994) Integrin alpha 4 beta 1-mediated melanoma cell adhesion and migration on vascular cell adhesion molecule-1 (VCAM-1) and the alternatively spliced IIICS region of fibronectin. J Biol Chem 269:27224–27230
Neri P, Ren L, Azab AK, Brentnall M, Gratton K, Klimowicz AC, Lin C, Duggan P, Tassone P, Mansoor A et al (2011) Integrin beta 7-mediated regulation of multiple myeloma cell adhesion, migration, and invasion. Blood 117:6202–6213
Neurath MF (2014) Cytokines in inflammatory bowel disease. Nat Rev Immunol 14:329–342
Nevo J, Mai A, Tuomi S, Pellinen T, Pentikainen OT, Heikkila P, Lundin J, Joensuu H, Bono P, Ivaska J (2010) Mammary-derived growth inhibitor (MDGI) interacts with integrin alpha-subunits and suppresses integrin activity and invasion. Oncogene 29:6452–6463
Newham P, Craig SE, Seddon GN, Schofield NR, Rees A, Edwards RM, Jones EY, Humphries MJ (1997) Alpha 4 integrin binding interfaces on VCAM-1 and MAdCAM-1 - integrin binding footprints identify accessory binding sites that play a role in integrin specificity. J Biol Chem 272:19429–19440
Nishiya N, Kiosses WB, Han J, Ginsberg MH (2005) An alpha4 integrin-paxillin-Arf-GAP complex restricts Rac activation to the leading edge of migrating cells. Nat Cell Biol 7:343–352
Nojima Y, Humphries MJ, Mould AP, Komoriya A, Yamada KM, Schlossman SF, Morimoto C (1990) VLA-4 mediates CD3-dependent CD4+ T cell activation via the CS1 alternatively spliced domain of fibronectin. J Exp Med 172:1185–1192
Osborn L, Vassallo C, Benjamin CD (1992) Activated endothelium binds lymphocytes through a novel binding site in the alternately spliced domain of vascular cell adhesion molecule-1. J Exp Med 176:99–107
Pan Y, Zhang K, Qi J, Yue J, Springer TA, Chen J (2010) Cation-pi interaction regulates ligand-binding affinity and signaling of integrin alpha4beta7. Proc Natl Acad Sci U S A 107:21388–21393
Pan WJ, Hsu H, Rees WA, Lear SP, Lee F, Foltz IN, Rathanaswami P, Manchulenko K, Chan BM, Zhang M et al (2013) Pharmacology of AMG 181, a human anti-alpha(4)beta(7) antibody that specifically alters trafficking of gut-homing T cells. Brit J Pharmacol 169:51–68
Pankov R, Yamada KM (2002) Fibronectin at a glance. J Cell Sci 115:3861–3863
Park J, Song SH, Kim TY, Choi MC, Jong HS, Kim TY, Lee JW, Kim NK, Kim WH, Bang YJ (2004) Aberrant methylation of integrin alpha4 gene in human gastric cancer cells. Oncogene 23:3474–3480
Park EJ, Yuki Y, Kiyono H, Shimaoka M (2015) Structural basis of blocking integrin activation and deactivation for anti-inflammation. J Biomed Sci 22:51
Peachman KK, Karasavvas N, Chenine AL, McLinden R, Rerks-Ngarm S, Jaranit K, Nitayaphan S, Pitisuttithum P, Tovanabutra S, Zolla-Pazner S et al (2015) Identification of new regions in HIV-1 gp120 variable 2 and 3 loops that bind to alpha4beta7 integrin receptor. PLoS One 10:e0143895
Pena-Cruz V, Etemad B, Chatziandreou N, Nyein PH, Stock S, Reynolds SJ, Laeyendecker O, Gray RH, Serwadda D, Lee SJ et al (2013) HIV-1 envelope replication and alpha 4 beta 7 utilization among newly infected subjects and their corresponding heterosexual partners. Retrovirology 10:162
Petrovic A, Alpdogan O, Willis LM, Eng JM, Greenberg AS, Kappel BJ, Liu C, Murphy GJ, Heller G, van den Brink MRM (2004) LPAM(alpha(4)beta(7) integrin) is an important homing integrin on alloreactive T cells in the development of intestinal graft-versus-host disease. Blood 103:1542–1547
Picarella D, Hurlbut P, Rottman J, Shi XJ, Butcher E, Ringler DJ (1997) Monoclonal antibodies specific for beta(7) integrin and mucosal addressin cell adhesion molecule-1 (MAdCAM-1) reduce inflammation in the colon of scid mice reconstituted with CD45RB(high) CD4(+) T cells. J Immunol 158:2099–2106
Polman CH, O’Connor PW, Havrdova E, Hutchinson M, Kappos L, Miller DH, Phillips JT, Lublin FD, Giovannoni G, Wajgt A et al (2006) A randomized, placebo-controlled trial of natalizumab for relapsing multiple sclerosis. N Engl J Med 354:899–910
Pouwels J, De Franceschi N, Rantakari P, Auvinen K, Karikoski M, Mattila E, Potter C, Sundberg JP, Hogg N, Gahmberg CG et al (2013) SHARPIN regulates uropod detachment in migrating lymphocytes. Cell Rep 5:619–628
Pytela R, Pierschbacher MD, Ruoslahti E (1985) Identification and isolation of a 140 kd cell surface glycoprotein with properties expected of a fibronectin receptor. Cell 40:191–198
Radue EW, Stuart WH, Calabresi PA, Confavreux C, Galetta SL, Rudick RA, Lublin FD, Weinstock-Guttman B, Wynn DR, Fisher E et al (2010) Natalizumab plus interferon beta-1a reduces lesion formation in relapsing multiple sclerosis. J Neurol Sci 292:28–35
Rantala JK, Pouwels J, Pellinen T, Veltel S, Laasola P, Mattila E, Potter CS, Duffy T, Sundberg JP, Kallioniemi O et al (2011) SHARPIN is an endogenous inhibitor of beta1-integrin activation. Nat Cell Biol 13:1315–1324
Rebhun RB, Cheng H, Gershenwald JE, Fan D, Fidler IJ, Langley RR (2010) Constitutive expression of the alpha4 integrin correlates with tumorigenicity and lymph node metastasis of the B16 murine melanoma. Neoplasia 12:173–182
Renz ME, Chin HH, Jones S, Fox J, Kim KJ, Presta LG, Fong S (1994) Structural requirements for adhesion of soluble recombinant murine vascular cell-adhesion Molecule-1 to Alpha-4-Beta-1. J Cell Biol 125:1395–1406
Richardson SI, Gray ES, Mkhize NN, Sheward DJ, Lambson BE, Wibmer CK, Masson L, Werner L, Garrett N, Passmore JAS et al (2015) South African HIV-1 subtype C transmitted variants with a specific V2 motif show higher dependence on alpha 4 beta 7 for replication. Retrovirology 12:54
Rose DM (2006) The role of the alpha4 integrin-paxillin interaction in regulating leukocyte trafficking. Exp Mol Med 38:191–195
Rosen GD, Sanes JR, LaChance R, Cunningham JM, Roman J, Dean DC (1992) Roles for the integrin VLA-4 and its counter receptor VCAM-1 in myogenesis. Cell 69:1107–1119
Rott LS, Briskin MJ, Andrew DP, Berg EL, Butcher EC (1996) A fundamental subdivision of circulating lymphocytes defined by adhesion to mucosal addressin cell adhesion molecule-1. Comparison with vascular cell adhesion molecule-1 and correlation with beta 7 integrins and memory differentiation. J Immunol 156:3727–3736
Rott LS, Rose JR, Bass D, Williams MB, Greenberg HB, Butcher EC (1997) Expression of mucosal homing receptor alpha4beta7 by circulating CD4+ cells with memory for intestinal rotavirus. J Clin Invest 100:1204–1208
Rudick RA, Stuart WH, Calabresi PA, Confavreux C, Galetta SL, Radue EW, Lublin FD, Weinstock-Guttman B, Wynn DR, Lynn F et al (2006) Natalizumab plus interferon beta-1a for relapsing multiple sclerosis. N Engl J Med 354:911–923
Ruegg C, Postigo AA, Sikorski EE, Butcher EC, Pytela R, Erle DJ (1992) Role of integrin alpha 4 beta 7/alpha 4 beta P in lymphocyte adherence to fibronectin and VCAM-1 and in homotypic cell clustering. J Cell Biol 117:179–189
Sandborn WJ, Feagan BG, Rutgeerts P, Hanauer S, Colombel JF, Sands BE, Lukas M, Fedorak RN, Lee S, Bressler B et al (2013) Vedolizumab as induction and maintenance therapy for Crohn’s disease. New Engl J Med 369:711–721
Schleier L, Wiendl M, Heidbreder K, Binder MT, Atreya R, Rath T, Becker E, Schulz-Kuhnt A, Stahl A, Schulze LL et al (2020) Non-classical monocyte homing to the gut via alpha 4 beta 7 integrin mediates macrophage-dependent intestinal wound healing. Gut 69:252–263
Schlesinger MJ (1990) Heat shock proteins. J Biol Chem 265:12111–12114
Schurpf T, Springer TA (2011) Regulation of integrin affinity on cell surfaces. EMBO J 30:4712–4727
Scott LM, Priestley GV, Papayannopoulou T (2003) Deletion of alpha4 integrins from adult hematopoietic cells reveals roles in homeostasis, regeneration, and homing. Mol Cell Biol 23:9349–9360
Selinger C, Sandborn W, Panes J, Jones J, Hassanali A, Jacob R, Sharafali Z, Oh Y, Tole S (2018) Etrolizumab as induction therapy in moderate to severe Crohn’s disease: results from bergamot cohort 1. Gut 67:A53–A53
Shamri R, Grabovsky V, Feigelson SW, Dwir O, Van Kooyk Y, Alon R (2002) Chemokine stimulation of lymphocyte alpha 4 integrin avidity but not of leukocyte function-associated antigen-1 avidity to endothelial ligands under shear flow requires cholesterol membrane rafts. J Biol Chem 277:40027–40035
Shattil SJ, Kim C, Ginsberg MH (2010) The final steps of integrin activation: the end game. Nat Rev Mol Cell Bio 11:288–300
Sheppard AM, Onken MD, Rosen GD, Noakes PG, Dean DC (1994) Expanding roles for alpha 4 integrin and its ligands in development. Cell Adhes Commun 2:27–43
Shishido S, Bonig H, Kim YM (2014) Role of integrin alpha4 in drug resistance of leukemia. Front Oncol 4:99
Shyjan AM, Bertagnolli M, Kenney CJ, Briskin MJ (1996) Human mucosal addressin cell adhesion molecule-1 (MAdCAM-1) demonstrates structural and functional similarities to the alpha 4 beta 7-integrin binding domains of murine MAdCAM-1, but extreme divergence of mucin-like sequences. J Immunol 156:2851–2857
Sneller MC, Clarridge KE, Seamon C, Shi V, Zorawski MD, Justement JS, Blazkova J, Huiting ED, Proschan MA, Mora JR et al (2019) An open-label phase 1 clinical trial of the anti-alpha(4)beta(7) monoclonal antibody vedolizumab in HIV-infected individuals. Sci Transl Med 11:eaax3447
Springer TA (1994) Traffic signals for lymphocyte recirculation and leukocyte emigration: the multistep paradigm. Cell 76:301–314
Staton TL, Habtezion A, Winslow MM, Sato T, Love PE, Butcher EC (2006) CD8(+) recent thymic emigrants home to and efficiently repopulate the small intestine epithelium (vol 7, pg 482, 2005). Nat Immunol 7:672
Stepp MA, Urry LA, Hynes RO (1994) Expression of alpha 4 integrin mRNA and protein and fibronectin in the early chicken embryo. Cell Adhes Commun 2:359–375
Stewart MP, McDowall A, Hogg N (1998) LFA-1-mediated adhesion is regulated by cytoskeletal restraint and by a Ca2+−dependent protease, calpain. J Cell Biol 140:699–707
Strober W, Fuss I, Mannon P (2007) The fundamental basis of inflammatory bowel disease. J Clin Investig 117:514–521
Sun H, Liu J, Zheng Y, Pan Y, Zhang K, Chen J (2014) Distinct chemokine signaling regulates integrin ligand specificity to dictate tissue-specific lymphocyte homing. Dev Cell 30:61–70
Sun H, Lagarrigue F, Gingras AR, Fan ZC, Ley K, Ginsberg MH (2018) Transmission of integrin beta 7 transmembrane domain topology enables gut lymphoid tissue development. J Cell Biol 217:1453–1465
Sun ZQ, Costell M, Fassler R (2019) Integrin activation by Talin, kindlin and mechanical forces. Nat Cell Biol 21:25–31
Takada Y, Elices MJ, Crouse C, Hemler ME (1989) The primary structure of the alpha 4 subunit of VLA-4: homology to other integrins and a possible cell-cell adhesion function. EMBO J 8:1361–1368
Takagi J, Erickson HP, Springer TA (2001) C-terminal opening mimics ‘inside-out’ activation of integrin alpha 5 beta 1. Nat Struct Biol 8:412–416
Takagi J, Petre BM, Walz T, Springer TA (2002) Global conformational rearrangements in integrin extracellular domains in outside-in and inside-out signaling. Cell 110:599–511
Takagi J, Strokovich K, Springer TA, Walz T (2003) Structure of integrin alpha(5)beta(1) in complex with fibronectin. EMBO J 22:4607–4615
Tamkun JW, DeSimone DW, Fonda D, Patel RS, Buck C, Horwitz AF, Hynes RO (1986) Structure of integrin, a glycoprotein involved in the transmembrane linkage between fibronectin and actin. Cell 46:271–282
Tan K, Casasnovas JM, Liu JH, Briskin MJ, Springer TA, Wang JH (1998) The structure of immunoglobulin superfamily domains 1 and 2 of MAdCAM-1 reveals novel features important for integrin recognition. Structure 6:793–801
Ueha S, Murai M, Yoneyama H, Kitabatake M, Imai T, Shimaoka T, Yonehara S, Ishikawa S, Matsushima K (2007) Intervention of MAdCAM-1 or fractalkine alleviates graft-versus-host reaction associated intestinal injury while preserving graft-versus-tumor effects. J Leukoc Biol 81:176–185
van Kooyk Y, Figdor CG (2000) Avidity regulation of integrins: the driving force in leukocyte adhesion. Curr Opin Cell Biol 12:542–547
Villablanca EJ, De Calisto J, Paredes PT, Cassani B, Nguyen DD, Gabrielsson S, Mora JR (2014) Beta 7 integrins are required to give rise to intestinal mononuclear phagocytes with tolerogenic potential. Gut 63:1431–1440
von Andrian UH, Mackay CR (2000) Advances in immunology: T-cell function and migration - two sides of the same coin. New Engl J Med 343:1020–1033
von Andrian UH, Mempel TR (2003) Homing and cellular traffic in lymph nodes. Nat Rev Immunol 3:867–878
Vonderheide RH, Tedder TF, Springer TA, Staunton DE (1994) Residues within a conserved amino acid motif of domains 1 and 4 of VCAM-1 are required for binding to VLA-4. J Cell Biol 125:215–222
Wagner N, Lohler J, Kunkel EJ, Ley K, Leung E, Krissansen G, Rajewsky K, Muller W (1996) Critical role for beta 7 integrins in formation of the gut-associated lymphoid tissue. Nature 382:366–370
Waldman E, Lu SX, Hubbard VM, Kochman AA, Eng JM, Terwey TH, Muriglan SJ, Kim TD, Heller G, Murphy GF et al (2006) Absence of beta 7 integrin results in less graft-versus-host disease because of decreased homing of alloreactive T cells to intestine. Blood 107:1703–1711
Waljee AK, Joyce JC, Wren PA, Khan TM, Higgins PDR (2009) Patient reported symptoms during an ulcerative colitis flare: a qualitative focus group study. Eur J Gastroen Hepat 21:558–564
Wang SH, Wu CY, Zhang YB, Zhong QL, Sun H, Cao WP, Ge GX, Li GH, Zhang XF, Chen JF (2018) Integrin alpha 4 beta 7 switches its ligand specificity via distinct conformer-specific activation. J Cell Biol 217:2799–2812
Wang S, Lin C, Li Y, Liu Z, Wang J, Zhang Y, Yan Z, Zhang Y, Li G, Chen J (2021) Distinct chemokines selectively induce HIV-1 gp120-integrin alpha4beta7 binding via triggering conformer-specific activation of alpha4beta7. Signal Transduct Target Ther 6:265
Warnke C, Menge T, Hartung HP, Racke MK, Cravens PD, Bennett JL, Frohman EM, Greenberg BM, Zamvil SS, Gold R et al (2010) Natalizumab and progressive multifocal leukoencephalopathy: what are the causal factors and can it be avoided? Arch Neurol 67:923–930
Wayner EA, Garcia-Pardo A, Humphries MJ, McDonald JA, Carter WG (1989a) Identification and characterization of the T lymphocyte adhesion receptor for an alternative cell attachment domain (CS-1) in plasma fibronectin. J Cell Biol 109:1321–1330
Wayner EA, Garciapardo A, Humphries MJ, Mcdonald JA, Carter WG (1989b) Identification and characterization of the lymphocyte-T adhesion receptor for an alternative cell attachment domain (Cs-1) in plasma fibronectin. J Cell Biol 109:1321–1330
Wegener KL, Campbell ID (2008) Transmembrane and cytoplasmic domains in integrin activation and protein-protein interactions (review). Mol Membr Biol 25:376–387
Wegener KL, Partridge AW, Han J, Pickford AR, Liddington RC, Ginsberg MH, Campbell ID (2007) Structural basis of integrin activation by Talin. Cell 128:171–182
Welniak LA, Blazar BR, Murphy WJ (2007) Immunobiology of allogeneic hematopoietic stem cell transplantation. Annu Rev Immunol 25:139–170
West NR, McCuaig S, Franchini F, Powrie F (2015) Emerging cytokine networks in colorectal cancer. Nat Rev Immunol 15:615–629
White ES, Muro AF (2011) Fibronectin splice variants: understanding their multiple roles in health and disease using engineered mouse models. IUBMB Life 63:538–546
Wiesner S, Lange A, Fassler R (2006) Local call: from integrins to actin assembly. Trends Cell Biol 16:327–329
Williams DA, Rios M, Stephens C, Patel VP (1991) Fibronectin and VLA-4 in haematopoietic stem cell-microenvironment interactions. Nature 352:438–441
Xavier RJ, Podolsky DK (2007) Unravelling the pathogenesis of inflammatory bowel disease. Nature 448:427–434
Xiao T, Takagi J, Coller BS, Wang JH, Springer TA (2004) Structural basis for allostery in integrins and binding to fibrinogen-mimetic therapeutics. Nature 432:59–67
Xie C, Zhu J, Chen X, Mi L, Nishida N, Springer TA (2010) Structure of an integrin with an alphaI domain, complement receptor type 4. EMBO J 29:666–679
Xiong JP, Stehle T, Diefenbach B, Zhang RG, Dunker R, Scott DL, Joachimiak A, Goodman SL, Arnaout MA (2001) Crystal structure of the extracellular segment of integrin alpha V beta 3. Science 294:339–345
Yang JT, Rayburn H, Hynes RO (1995) Cell adhesion events mediated by alpha 4 integrins are essential in placental and cardiac development. Development 121:549–560
Yang JT, Rando TA, Mohler WA, Rayburn H, Blau HM, Hynes RO (1996) Genetic analysis of alpha 4 integrin functions in the development of mouse skeletal muscle. J Cell Biol 135:829–835
Yauch RL, Felsenfeld DP, Kraeft SK, Chen LB, Sheetz MP, Hemler ME (1997) Mutational evidence for control of cell adhesion through integrin diffusion/clustering, independent of ligand binding. J Exp Med 186:1347–1355
Yednock TA, Cannon C, Fritz LC, Sanchez-Madrid F, Steinman L, Karin N (1992) Prevention of experimental autoimmune encephalomyelitis by antibodies against alpha 4 beta 1 integrin. Nature 356:63–66
Yong K, Khwaja A (1990) Leucocyte cellular adhesion molecules. Blood Rev 4:211–225
Young SA, McCabe KE, Bartakova A, Delaney J, Pizzo DP, Newbury RO, Varner JA, Schlaepfer DD, Stupack DG (2015) Integrin alpha 4 enhances metastasis and may be associated with poor prognosis in MYCNlow neuroblastoma. PLoS One 10:e0120815
Yu YM, Zhu JH, Mi LZ, Walz T, Sun H, Chen JF, Springer TA (2012) Structural specializations of alpha(4)beta(7), an integrin that mediates rolling adhesion. J Cell Biol 196:131–146
Yuan MY, Yang YR, Li Y, Yan ZJ, Lin CD, Chen JF (2020) Mucin-like domain of mucosal Addressin cell adhesion Molecule-1 facilitates integrin alpha 4 beta 7-mediated cell adhesion through electrostatic repulsion. Front Cell Dev Biol 8:603148
Yue J, Pan Y, Sun L, Zhang K, Liu J, Lu L, Chen J (2013) The unique disulfide bond-stabilized W1 beta4-beta1 loop in the alpha4 beta-propeller domain regulates integrin alpha4beta7 affinity and signaling. J Biol Chem 288:14228–14237
Zaidel-Bar R, Itzkovitz S, Ma’ayan A, Iyengar R, Geiger B (2007) Functional atlas of the integrin adhesome. Nat Cell Biol 9:858–867
Zhang K, Chen J (2012) The regulation of integrin function by divalent cations. Cell Adhes Migr 6:20–29
Zhang K, Pan YD, Qi JP, Yue J, Zhang MB, Xu CQ, Li GH, Chen JF (2013) Disruption of disulfide restriction at integrin knees induces activation and ligand-independent signaling of alpha(4)beta(7). J Cell Sci 126:5030–5041
Zhang HL, Zheng YJ, Pan YD, Xie C, Sun H, Zhang YH, Yuan MY, Song BL, Chen JF (2016) Regulatory T-cell depletion in the gut caused by integrin beta7 deficiency exacerbates DSS colitis by evoking aberrant innate immunity. Mucosal Immunol 9:391–400
Zhang, Y., Xie, R., Zhang, H., Zheng, Y., Lin, C., Yang, L., Huang, M., Li, M., Song, F., Lu, L., et al. (2021). Integrin β7 inhibits colorectal cancer pathogenesis via maintaining anti-tumor immunity. Cancer Immunol Res 9(8):967-980
Zhu J, Luo BH, Xiao T, Zhang C, Nishida N, Springer TA (2008a) Structure of a complete integrin ectodomain in a physiologic resting state and activation and deactivation by applied forces. Mol Cell 32:849–861
Zhu JH, Luo BH, Xiao T, Zhang CZ, Nishida N, Springer TA (2008b) Structure of a complete integrin Ectodomain in a physiologic resting state and activation and deactivation by applied forces. Mol Cell 32:849–861
Acknowledgments
This work was supported by grants from the National Key Research and Development Program of China (2020YFA0509102), National Natural Science Foundation of China (32030024, 31830112, 31525016 to J.F.C., 32170769, 31970702 to C.D.L., 31900536 to S.H.W.), Shanghai Rising-Star Program (21QA1409700), Program of Shanghai Academic Research Leader (19XD1404200), the Youth Innovation Promotion Association of the Chinese Academy of Sciences (2020266), the Young Elite Scientist Sponsorship Program by CAST (2019QNRC001), National Ten Thousand Talents Program, the China Postdoctoral Innovative Talent Support Program (BX20190345), and China Postdoctoral Science Foundation (2020M671262). The authors gratefully acknowledge the support of SA-SIBS scholarship program.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Ethics declarations
The authors declare no competing interests.
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Lin, C., Wang, S., Chen, J. (2023). α4 Integrins in Immune Homeostasis and Disease. In: Gullberg, D., Eble, J.A. (eds) Integrins in Health and Disease. Biology of Extracellular Matrix, vol 13. Springer, Cham. https://doi.org/10.1007/978-3-031-23781-2_9
Download citation
DOI: https://doi.org/10.1007/978-3-031-23781-2_9
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-23780-5
Online ISBN: 978-3-031-23781-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)