Abstract
Age is irrelevant to the understanding of compassion and its real-life application. Based on this, it is safe to assume that the new generation of healthcare professionals will be able to understand and actively implement compassion starting as early as possible in their training. If healthcare professional training focuses solely on the biomedical sciences, this can lead to neglecting a patient-centered and compassionate care approach. However, can compassion be taught? Strong evidence suggests that it can. Development of compassion happens in two fundamental ways—the experiential learning of values such as empathy, trust, and honesty and the practical and didactic learning of skills such as communication skills, shared decision making, self-compassion, and self-reflection. These values and skills are not sufficiently, if at all, addressed in a number of medical and healthcare education curricula. The delivery of a hybrid, modular, overarching theme in healthcare teaching across all years of study is suggested to be one of the strongest ways of teaching compassion. Combined with the 3C approach (Cultivate, Check, Conserve) and quantitative compassionate care metrics, studies show that teaching compassion can be very fruitful for patients, healthcare professionals, and hospitals. This chapter discusses the need and practical application of compassionate care training in prospective healthcare professionals, with a translatable focus on medical education.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
FormalPara Learning Objectives-
1.
Understand the importance of developing compassion in the new generation of healthcare professionals
-
2.
Determine if compassion can be taught
-
3.
Outline methods that can be used to teach compassion
-
4.
Give examples of what skills and values need to be cultivated
-
5.
List ways to measure the effectiveness of Compassionate Care education
We suggest using this chapter as evidence-based guidelines when deciding on educational reforms in healthcare. Real-life patient experiences from healthcare professionals are also included in boxes throughout the chapter. These can be combined with the teaching methods described to cultivate compassion in the new generation.
Introduction
Spanning more than 2000 years ago, compassion has been defined in many ways. An example worth looking at is the one of a child: “When someone gets hurt, we go and look after them and then we make funny faces.” This response practically demonstrates that compassion includes an awareness of the suffering of another, coupled with the wish to relive it. In contrast, empathy encompasses only the understanding of the pain of another and sympathy, the reaction of pity towards them.
This definition also alludes to the irrelevance of age in the understanding and real-life application of compassion. If a 5-year-old can do it, it is safe to assume that medical students can.
A more practical definition of Compassionate Care (CC) is also required before we proceed. In the words of patients and clinicians across many studies, compassion is described as therapeutic actions or inactions: “helped control your pain,” “understood your medical problems,” “small acts of kindness,” “going over and above,” “attending to the little things,” “giving others the gift of quiet, time, and space,” visible, persistent, and dedicated presence of the clinician [1, 2]. Compassion is, therefore, a combination of virtues and skills such as empathy, altruism, self-reflection, advanced communication skills, intercultural communication competence, active listening, supportive body language, conflict transformation, trust, honesty, and teamwork.
The following patient experience, kindly narrated by Dr Nicholas Herodotou, a Palliative Medicine consultant, illustrates a heartfelt example of therapeutic inaction that prioritizes quality of life over prolonging life.
“ Please Dr, let me die” ; When Overtreating a Palliative Patient Causes Greater Harm than Good.
Therapeutic inactions
I was requested to assess a 68-year-old married man who had multiple progressive co-morbidities over a period of 19 years, significantly affecting his quality of life. He was confined mostly to bed, had limited social interaction and suffered a loss of marital intimacy due to a huge enterocutaneous fistula which discharged over 2L/day into his stoma bag. His other medical conditions included cardiac disease, recurrent pulmonary emboli, ischemic limbs, intra-abdominal bleed post-surgery and recurrent sepsis. He was receiving artificial nutrition and had deteriorating renal function. Over four years, he had a total of 144 days of hospital admissions. The consultant in charge was struggling to maintain homeostasis regarding his nutritional input and worsening renal disease. The patient repeatedly expressed the wish to be allowed to die over several months as he felt he could not continue with his futile medical interventions. The medical teams did not listen to the patient’s wishes.
A psychologist was supporting the patient. I advised the patient that legally, he has the right to refuse any medical treatment, providing he is deemed to have capacity and is not so severely depressed as to affect his decision making. His face lit up for the first time and he expressed his gratitude that I was the only doctor to listen to his wishes.
A psychiatrist reviewed the patient and deemed him to have capacity and that he was not so severely depressed as to affect his decision making. Plans were made for the artificial nutrition and other medical treatments to be stopped and to transfer him to a hospice for terminal care. I did emphasize that this was not euthanasia or physician assisted suicide but allowing him to die naturally from his illness.
Before leaving the hospital, he hugged his wife and said to her: “I'm sorry my love, but I can’t cope anymore.” They both wept in my presence, but there was both a serenity and acceptance; the struggle had finally ended. He died peacefully in the hospice five days later with his wife and young son present.
The patient’s consultant’s comment to me after stopping all this treatment was that: “This patient’s clinical management has been fundamentally altered for the good by what you did.”
We must give patient’s their dignity by maximizing their quality of life in their last days and avoiding futile overtreatments that merely prolong life.
Dr Nicholas Herodotou BSc, MB, BS, DGM, DRCOG, DPM, MRCGP, FRCP, FHEA
Palliative Medicine Consultant
Honorary Clinical Lecturer, UCLMS
Bedfordshire Hospitals NHS Foundation Trust
Why Is This Important for Students?
Educating the mind without educating the heart is no education at all
Aristotle [3]
Compassion is the cornerstone of the healthcare profession. Patients have systematically ranked it as the most or one of the most important factors in their treatment [4,5,6]. A compassionate approach works in two ways. Firstly, it allows the patient to easily disclose information as they know the person listening deeply cares. This approach ensures that what is essential to the patient has been said. Thus, healthcare professionals will treat the patient, not just the symptoms. Critical details are not missed and patients are less likely to lie, and more likely to comply [7, 8]. Secondly, it works on a biochemical level by accelerating recovery, increasing pain tolerance, gaining better control of the chronic illness, and improving psychological symptoms such as anxiety and depression [9,10,11]. Simply put, imagine you are sick, and you feel that no one cares about you versus the situation where many people care, want you to become better and are actively doing something about it. The second situation is more likely to lead to a healthier and happier patient.
It is also proven to be better for Healthcare Professionals (HP): “Happier patients equal happier clinicians.” Studies show that CC increases job satisfaction and sustainability and decreases the risk of burnout [2, 7, 12, 13]. Therefore, compassion increases patients’ quality of life and the HPs. It is thus to no one’s surprise that the UK General Medical Council recommends CC teaching in medical education [14]. Since we aim is to provide quality of life, we should aim to cultivate and sustain CC in the new generation of healthcare and management students.
How Compassion Is Developed or Eroded
If you talk to a man in a language he understands, that goes to his head. If you talk to him in his language, that goes to his heart.
Nelson Mandela
The question of whether virtues such as compassion can be taught can be dated back to ancient Greece. Socrates believed virtues are a “gift of the Gods,” whereas Protagoras argued that everybody teaches them. In 1983 Pence published an essay, “Can compassion be taught?,” where he concluded that Protagoras was correct, and a healthcare system can develop moral ideas [15]. Pence argues that medical education should reward compassion alongside clinical skills and factual knowledge. Many others, such as Saunders, Chochinov, Egan, Rogers, and Haslam, report the same conclusion: Compassion can be developed and eroded [5, 16,17,18,19]. Successful modular CC teachings at hospitals around the world also fortify this conclusion [20,21,22].
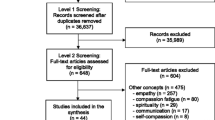
Following a distillation of the current literature surrounding compassion, barriers and factors that erode compassion are ranked.
-
1.
Medical schools, nursing schools, and healthcare professional training can be a barrier to compassion and even “teach it out” of students. If, during training, the basic and clinical sciences are not coupled alongside the application of virtues it can cause the neglect and even decrease of a holistic, patient-centered, CC approach. Research reports that medical students may lose the ability to empathize with their patients during clinical training—also referred to as “hardening of the heart” [16, 23]. This is a well-documented phenomenon observed in many countries that dates to 1961 [24] and one that should alarm us. If left unattended, situations arise and assist in producing tragedies such as the Francis report. A report into the serious healthcare failings of a UK hospital Trust [25]. The Francis report identified the absence of compassion as a contributory factor and advised the use of compassion aptitude tests.
-
2.
The result orientated, “box-ticking” environment. Although in many cases students may be taught the application of virtues during pre-clinical years, once they enter the battlefield these become a luxury not a priority. This phenomenon is evident from several studies looking at components of quality care, where clinicians prioritized technical skills over intrinsic qualities, opposite to patients’ views [26,27,28,29]. Both technical skills and intrinsic qualities should be of equal importance.
-
3.
Compassion fatigue/Burnout is an epidemic among healthcare professionals worldwide. It affects approximately 500,000 physicians in the USA alone and is estimated to cost 12 billion dollars annually in terms of burnout cost, which causes increased physician turnover [30]. It is estimated that 80% of burnout is related to organizational factors. To address these organizational factors, the American Medical Association promotes the Stanford Wellness Framework, which includes three domains. One of them is a “Culture of Wellness” promoting “compassion for colleagues, patients, and self” [31].
-
4.
Absence of personal life experiences. Experiential learning is regarded amongst academics as the best way of teaching. As a result, variability in experiences, goals, and motivations causes variability in the inherent virtues present in students at baseline.
-
5.
Shortage of compassionate role models during clinical training, and therefore the absence of corrective behaviour towards students neglecting the application of virtues [8]. If the next generation is to be more compassionate than the current, the culture in healthcare needs to change, starting with each of us individually. Problems start at the top of pyramids.
-
6.
Unmet need for validated quantitative CC metrics. Literature is flourishing in this area albeit, it is in its infancy. An updated critical review in 2022 highlighted the need for validated psychometric instruments identified the Sinclair Compassion Questionnaire (SCQ) as the best available tool [32].
Other barriers that are more difficult to address but deserve mentioning include high work stress, case complexity, long hours, difficult patients, time pressure, lack of teamwork and communication, and bad organizational structure.
Remedying the above barriers will create many opportunities to develop compassion in the younger generations. These opportunities will act as CC enablers. Other important CC enablers are also noted below:
-
1.
Culture change. Shaping the ethos of a group of people has troubled leaders over the years. Many criticised it as an impossible task to achieve in short periods. However, if the focus is shifted to changing the environment and not the people then some noteworthy outcomes can be seen. Manifestations of Nature in the clinical environment such as windows, images, and indoor plants significantly decrease patient pain, anxiety, depression, and ultimately length of stay [33]. Other environmental factors such as the architectural layout and organization of hospital units affect the visibility of patients and thus patient outcomes. Although physician outcomes were not recorded in the above studies, it is imprudent to think these changes will not positively affect HPs. The HPs may act as mediators of patient outcomes. Higher quality research is needed to determine if this is a true phenomenon. Nonetheless, our behaviour is undoubtedly shaped more than we believe by our environment.
-
2.
Personal experience. These enabling experiences can occur prior to medical school through personal events or can take place through training. Role models that exhibit compassionate behaviour must be highlighted and prompted to teach or preferably have students spend time shadowing them [34]. Nursing students have also identified fewer mentoring opportunities as a barrier to developing compassion through healthcare training [35].
-
3.
Positive Reinforcement should come from senior clinicians, when compassionate behaviour is noticed at all levels of HP.
-
4.
Starting as early as possible. One can argue that values are habits repeated many times, Will Durant, in his work “the story of philosophy”, remarks, “We are what we repeatedly do. Excellence, then, is not an act, but a habit.” We believe the same applies here, since compassion is a set of applicable virtues, it’s a matter of creating and reinforcing positive habits over a long period of time. The longer that period, the stronger the habit. James Clear’s work on habit building can be of use [36].
-
5.
Humanities and Art. Haslam and Chochinov suggest that humanities and arts such as literature, poetry, music, film, and theatre can be fruitful channels in developing compassion since they help us visualize and better comprehend the lives of others [5, 16].
Most of the above barriers and enablers of compassion will be further discussed and practically addressed in the following section.
What to Teach and How to Teach It?
Education without values, as useful as it is, seems rather to make a man a more clever devil.
C. S. Lewis
Following a thorough screening of the current evidence for teaching compassion, we introduce the 3C approach: Cultivate, Check, Conserve [1, 37, 38]. Each step in the 3C process is defined individually for each stage of medical education: Prospective Medical Students, Medical Students, Junior Doctors, and Senior Doctors. The practical advice for these four stages is also applicable and advisable to all other healthcare professionals, such as nurses, psychologists, and even healthcare managerial staff.
Cultivate, Check, Conserve
The word cultivate is used instead of teaching because it refers to the intrinsic ability of the individual to acquire virtues or skills through experiential learning contrary to the attainment of information and facts through teaching.
Table 4.1 outlines the “material” to be communicated when aiming to culture compassion. Table 4.2 is a non-exhaustive list of the different teaching methods that can be used in each of the four medical journey stages. Teaching methods are also divided into didactic (theoretical tuition in seminar form), practical (hands-on tuition such as role play), and experiential (exposure to planned patient interactions imitating actual clinical situations).
The reasoning behind the division of Table 4.1 into skills and virtues is that they are encouraged differently; thus, approaches to teaching will vary. Skills can be taught in didactic and practical ways similar to the way we teach other practical skills such as taking blood and inserting catheters. Virtues are primarily taught by experiential learning since they are much harder to communicate and stem from a uniquely personal and multifactorial background.
It is vital for the development of compassion that skills are accompanied by Virtues. Virtues make the skills a genuine reaction that can be deeply felt by the individuals and not a robotic movement or even a facade. It is surprising how easily patients can tell that someone is putting on an act or is genuinely empathetic. Addressing these is more challenging but achievable if we allow experiences to teach and not ourselves.
Prospective Medical Students
Cultivate: It is crucial that we start as early as possible in medical training by introducing these virtues and skills. We would go to the extent in saying even before medical school. CC at this stage can be cultivated through work experience, especially if it becomes examinable in medical school interviews. Moreover, to facilitate this development Medical Schools can provide short online and in-person CC courses (view teaching methods Table 4.2) in secondary schools with current medical students, perhaps as part of Student Selected Components (SSC). Experts argue that this will not only foster compassion in prospective medical students but also prevent verbal, physical, and emotional aggressive behavior in all class members [51]. Starting early is key.
Check: Applications for medical or healthcare education require a checklist of items to be completed (volunteering, shadowing, personal statement and educational achievements) which is then examined through panel interviews or multiple mini interviews (MMIs). A recent change towards MMIs has been observed in the UK due to their effectiveness at testing a greater variety of skills, with tasks such as role play and professional judgment stations. MMIs can, therefore, facilitate the examination of compassion through the virtues and skills outlined in the introduction. It will then be made an area to work on before applying to medical school through shadowing and volunteering experiences. Prospective students will learn to value its importance and practice its application in real situations even before attending interviews.
Conserve: Preservation of CC will occur subsequently throughout medical school.
Medical Students
Cultivate: In behaviour modification strategies and other successful teaching methodologies, the idea of spaced repetition is prevalent. The same is true for teaching compassion. Following the examples of modules delivered in Cyprus, Greece, and the UK that generated successful qualitative and quantitative evidence, delivering a hybrid modular overarching theme in healthcare teaching across all years of study is suggested to be one of the strongest ways of teaching compassion [20,21,22]. Modules should include the cultivation of skills and virtues as seen in Table 4.1 with methods of teaching seen in Table 4.2. The design of modules should be a product of focus group meetings with medical schools’ administrative staff, professors, human resources staff, clinicians, and medical students regarding their Needs, Ideas, Concerns and Expectations (NICE). An analogous process should take place with the respective managerial staff of hospitals when designing modules for Junior and Senior Doctors.
An example of a successful module structure delivered to healthcare professionals (nurses, clinicians) and managerial staff in a hospital in Cyprus can be seen in Table 4.3. Modules were cumulative (built on each other) and were taught through presentations, theory-based discussion, real-life examples, stories, videos, and role-playing. Randomization of participants into working groups and qualitative/quantitative feedback were also core elements of the course.
An example of using a real-life story to teach active listening (AL) and shared decision making (SDM) has been kindly provided by Dr George Samoutis. In this case scenario the patient, Maria* is presented (until**).
“Dr, please listen to me,” Treating the Whole Person
Therapeutic actions
Maria* a 40-year-old female academic professor came to see me due to chronic episodic migraine headaches over the last couple of years which recently had become unbearable. She had no other past medical history, had tried trigger avoidance, several medications (triptans, magnesium, NSAIDs). She was married with 2 children, was a non-smoker, took no illicit drugs, and took limited exercise. She visited several doctors but couldn’t find a solution and she was desperate to be relieved from the pain. She ran several tests (e.g., blood testing, MRI brain) without any pathological findings. **
We sat and talked for 15 min. I realized that I needed to listen to her more, so I asked my secretary to reschedule my next appointment. It was a critical time to actively listen to her. I used active listening, shared decision making and the 3S CC model (Chapter 10: Compassionate Spirituality) and at some point, she started crying and said “Can I tell you something I haven’t told anyone before ?”
I nodded and Maria began, “I am an introverted person and do not share my emotions easily. I have been bullied at my university by my colleagues in a promotion process and have been exhausted emotionally having thoughts of hurting myself. Not even my husband knows about my problems at work and my thoughts.” I replied, “Now that we know the root cause we can move on together to treat your headaches.” We used therapeutic relationships, CBT and adversity activated development models, exercise as well as homeopathic remedies (aurum, natrium muriaticum) based on patients wishes and beliefs. The results were remarkable: After 5 years she is still pain-free and fully functioning with very rare episodes of migraine that resolved without the use of painkillers.
Prof George Samoutis MD,PhD, CCT, PGCertHBE(UK)
*pseudopatient names used, facilitating compassion
Participants are asked thereafter to describe how they would communicate with Maria, what questions they would ask and why. Following discussion, the case scenario reading is completed. A reflective discussion is facilitated, and the take-home message is highlighted.
Take-Home Message
AL, SDM in Clinical Practice
Define the problem, from the patient and doctor’s point of view
Active listening, empathy, therapeutic relationship, patient-centered and 3S approach (Chapter 10: Compassionate Spirituality)
Explain/educate without overloading
Assess patient’s level of health literacy
Check for understanding
Identify and repeat most salient points
Listen and reflect patient’s preference
Discuss plan forward: What happens next? Safety netting
We also strongly propose training medical students to include a patient-centered pneumonic in history taking. Namely IS NICE. Impact of the condition on patients’ quality of life/daily living, Safety netting to manage clinical emergencies and promptly report “red flags,” Needs (Physical, Emotional, and Spiritual needs), Ideas, Concerns and Expectations.
Check: CC in medical schools can be tested in a few ways. By using measures such as the Sinclaire Compassion Questionnaire (SCQ) (https://www.compassionmeasure.com/) and the 12-item Schwartz Center CC Scale [32, 52] we can test CC in Objective Structured Clinical Examinations (OSCE) stations and at placements. CC can also be tested at the end of medical school situational judgment tests with unambiguously targeted questions.
Conserve: Preservation of CC will occur subsequently throughout junior doctor placements.
Junior Doctors
Cultivate: Professional Development Courses on CC development and prevention of Compassion fatigue can be run as overarching modules throughout placements as per the teaching methods and material presented (Tables 4.1 and 4.2). Short (1–2 week) shadowing schemes of role-model physicians can also be effective.
Check: Quantitative and qualitative compassion scales [32, 52] are used to evaluate junior doctors at placements and major examinations such as the MRCP (UK).
Conserve: Preservation of CC will occur subsequently throughout senior doctor practice.
Senior Doctors
Cultivate: Professional Development Courses on CC development and prevention of Compassion fatigue can also be run to include Senior and Junior Doctors. Shadowing fellow role model clinicians (1–2 consultations) would facilitate interprofessional learning of CC and form an ongoing part of professional development for trained practitioners.
Check: Quantitative and qualitative compassion scales [32, 52] are used to evaluate senior doctors at revalidation.
Conserve: Preservation of CC will continue throughout a HP career.
Conclusion
Compassion’s absence or presence can be felt at all levels of human relationships, between patients and HP, between HP and even within ourselves. It is in our very nature to benefit from compassion mentally and physiologically. Consequently, it is of utmost importance to develop this quality in the individuals people seek in their darkest hours. We hope this chapter can be of use in healthcare educational reforms.
Into Practice
Prospective Medical Students
-
1.
Short courses online and/or face to face in secondary school
-
2.
Experiential learning through work experience at nursing homes and hospitals
Medical Students
-
1.
Integration of CC teaching in the curriculum
-
2.
Experiential learning of CC skills and behaviors during clinical placements
-
3.
OSCE stations testing CC
-
4.
Testing of CC at end of medical school exam
Junior Doctors
-
1.
Professional Development Courses on CC and prevention of Compassion fatigue
-
2.
Shadowing Role-Model physicians (1–2 weeks)
-
3.
Development of CC and fatigue quantitative scales
Senior Doctors
-
1.
CC should be part of revalidation
-
2.
Professional Development Courses on CC and prevention of Compassion fatigue
-
3.
Shadowing Fellow Role Model Clinicians (1–2 consultations)
-
4.
Development of CC and fatigue quantitative scales
References
Sinclair S, Norris JM, McConnell SJ, Chochinov HM, Hack TF, Hagen NA, et al. Compassion: a scoping review of the healthcare literature. BMC Palliat Care. 2016;15:6.
Way D, Tracy S. Conceptualizing compassion as recognizing, relating and (re)acting: a qualitative study of compassionate communication at hospice. Communication Monographs. 2012;79
Aristotle. Nicomachean ethics. Book II, Chapter 9, Paragraph 1340 BCE.
Heyland DK, Dodek P, Rocker G, Groll D, Gafni A, Pichora D, et al. What matters most in end-of-life care: perceptions of seriously ill patients and their family members. CMAJ. 2006;174(5):627–33.
Chochinov HM. Dignity and the essence of medicine: the A, B, C, and D of dignity conserving care. BMJ. 2007;335(7612):184–7.
Riggs JS, Woodby LL, Burgio KL, Bailey FA, Williams BR. “Don’t get weak in your compassion”: bereaved next of kin’s suggestions for improving end-of-life care in veterans affairs medical centers. J Am Geriatr Soc. 2014;62(4):642–8.
Van der Cingel M. Compassion in care: a qualitative study of older people with a chronic disease and nurses. Nurs Ethics. 2011;18(5):672–85.
Burack JH, Irby DM, Carline JD, Root RK, Larson EB. Teaching compassion and respect. Attending physicians’ responses to problematic behaviors. J Gen Intern Med. 1999;14(1):49–55.
Youngson R. Time to care: how to love your patients and your job. Raglan: Rebelheart Publishers; 2012.
Fogarty LA, Curbow BA, Wingard JR, McDonnell K, Somerfield MR. Can 40 seconds of compassion reduce patient anxiety? J Clin Oncol. 1999;17(1):371–9.
Shaltout HA, Tooze JA, Rosenberger E, Kemper KJ. Time, touch, and compassion: effects on autonomic nervous system and well-being. Explore (NY). 2012;8(3):177–84.
Perry B. Conveying compassion through attention to the essential ordinary. Nurs Older People. 2009;21(6):14–21. Quiz 2
Graber DR, Mitcham MD. Compassionate clinicians: take patient care beyond the ordinary. Holist Nurs Pract. 2004;18(2):87–94.
GMC (GMC). Guidance for doctors. 9 May 2011. https://www.gmc-uk.org/ethical-guidance/ethical-guidance-for-doctors/making-and-using-visual-and-audio-recordings-of-patients
Pence GE. Can compassion be taught? J Med Ethics. 1983;9(4):189–91.
Haslam D. More than kindness. J Compassionate Health Care. 2015;2(1):6.
Saunders J. Compassion. Clin Med (Lond). 2015;15(2):121–4.
Rogers CR. A way of being. Boston: Houghton Mifflin; 1980.
Egan G. The skilled helper: a problem-management and opportunity-development approach to helping/edition 10.2013.
Shea S, Samoutis G, Wynyard R, Samoutis A, Lionis C, Anastasiou A, et al. Encouraging compassion through teaching and learning: a case study in Cyprus. J Compassionate Health Care. 2016;3(1):10.
Lionis C, Shea S, Markaki A. Introducing and implementing a compassionate care elective for medical students in Crete. J Holist Healthc. 2011;8:38–41.
Adamson E, Smith S. Can compassionate care be taught? Experiences from the leadership in compassionate care programme. In: Shea S, Wynyard R, Lionis C, editors. Providing compassionate health care: challenges in policy and practice. London: Routledge; 2014. p. 235–51.
Newton BW, Barber L, Clardy J, Cleveland E, O’Sullivan P. Is there hardening of the heart during medical school? Acad Med. 2008;83(3):244–9.
Becker H, Geer B, Hughes EC, Strauss AL. Boys in white: student culture in medical school. New Brunswick, NJ; London: Transaction Publishers; 1961.
Francis R. QC. Report of the mid Staffordshire NHS foundation trust public inquiry. 2013.
Flocke SA, Miller WL, Crabtree BF. Relationships between physician practice style, patient satisfaction, and attributes of primary care. J Fam Pract. 2002;51(10):835–40.
McDonagh JR, Elliott TB, Engelberg RA, Treece PD, Shannon SE, Rubenfeld GD, et al. Family satisfaction with family conferences about end-of-life care in the intensive care unit: increased proportion of family speech is associated with increased satisfaction. Crit Care Med. 2004;32(7):1484–8.
Attree M. Patients’ and relatives’ experiences and perspectives of ‘good’ and ‘not so good’ quality care. J Adv Nurs. 2001;33(4):456–66.
Thorne SE, Kuo M, Armstrong EA, McPherson G, Harris SR, Hislop TG. ‘Being known’: patients’ perspectives of the dynamics of human connection in cancer care. Psychooncology. 2005;14(10):887–98; discussion 99-900.
Arnhart K, Privitera MR, Fish E, Young A, Hengerer AS, Chaudhry HJ, et al. Physician burnout and barriers to care on professional applications. J Leg Med. 2019;39(3):235–46.
Sinsky C, Shanafelt T, Murphy ML, et al. Creating the organizational foundation for joy in medicine™. American Medical Association (AMA); 2017. https://edhub.ama-assn.org/steps-forward/module/2702510
Sinclair S, Kondejewski J, Hack TF, Boss HCD, Macinnis CC. What is the most valid and reliable compassion measure in healthcare? An updated comprehensive and critical review. Patient. 2022;15:399.
Jamshidi S, Parker JS, Hashemi S. The effects of environmental factors on the patient outcomes in hospital environments: a review of literature. Front Archit Res. 2020;9(2):249–63.
Wear D, Zarconi J. Can compassion be taught? let’s ask our students. J Gen Intern Med. 2008;23(7):948–53.
Curtis K. 21st century challenges faced by nursing faculty in educating for compassionate practice: embodied interpretation of phenomenological data. Nurse Educ Today. 2013;33(7):746–50.
Clear J. Atomic habits: an easy & proven way to build good habits & break bad ones; Tiny changes, remarkable results. New York: Avery; Penguin Random House; 2018.
Patel S, Pelletier-Bui A, Smith S, Roberts MB, Kilgannon H, Trzeciak S, et al. Curricula for empathy and compassion training in medical education: a systematic review. PLoS One. 2019;14(8):E0221412.
Sinclair S, Hack TF, McClement S, Raffin-Bouchal S, Chochinov HM, Hagen NA. Healthcare providers perspectives on compassion training: a grounded theory study. BMC Med Educ. 2020;20(1):249.
Rueb M, Siebeck M, Rehfuess EA, Pfadenhauer LM. Cinemeducation in medicine: a mixed methods study on students’ motivations and benefits. BMC Med Educ. 2022;22(1):172.
Care IIOC. IICC video gallery. http://symponesi.org/iicc-video-gallery/
Jamkar AV, Burdick W, Morahan P, Yemul VY, Sarmukadum SG. Proposed model of case based learning for training undergraduate medical student in surgery. Indian J Surg. 2007;69(5):176–83.
Smits PB, De Buisonjé CD, Verbeek JH, Van Dijk FJ, Metz JC, Ten Cate OJ. Problem-based learning versus lecture-based learning in postgraduate medical education. Scand J Work Environ Health. 2003;4:280–7.
Zhao W, He L, Deng W, Zhu J, Su A, Zhang Y. The effectiveness of the combined problem-based learning (PBL) and case-based learning (CBL) teaching method in the clinical practical teaching of thyroid disease. BMC Med Educ. 2020;20(1):381.
Joyner B, Young L. Teaching medical students using role play: twelve tips for successful role plays. Med Teach. 2006;28(3):225–9.
HSE. Health Service Executive 2019. https://www.hse.ie/eng/about/who/nqpsd/qps-connect/schwartz-rounds/schwartz-rounds.html
Koh AWL, Lee SC, Lim SWH. The learning benefits of teaching: a retrieval practice hypothesis. Appl Cogn Psychol. 2018;32(3):401–10.
Sivarajah RT, Curci NE, Johnson EM, Lam DL, Lee JT, Richardson ML. A review of innovative teaching methods. Acad Radiol. 2019;26(1):101–13.
Milota MM, Van Thiel GJMW, Van Delden JJM. Narrative medicine as a medical education tool: a systematic review. Med Teach. 2019;41(7):802–10.
Mileder LP, Schmidt A, Dimai HP. Clinicians should be aware of their responsibilities as role models: a case report on the impact of poor role modeling. Med Educ Online. 2014;19(1):23479.
White T. Telling patient stories to teach new medical students. Scope by Stanford Medicine. January 30, 2017.
Whitson S. 2014. [cited 2022]. http://www.huffingtonpost.com/signe-whitson/8-ways-to-teach-compassio_b_5568451.html
Rodriguez AM, Lown BA. Measuring compassionate healthcare with the 12-item Schwartz center compassionate care scale. PLoS One. 2019;14(9):E0220911.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Samoutis, A., Samouti, S., Samouti, G., McCrorie, P. (2023). Cultivating Compassion in the New Generation. In: Samoutis, A., Samoutis, G., Stylianou, N., Anastasiou, A., Lionis, C. (eds) The Art and Science of Compassionate Care: A Practical Guide. New Paradigms in Healthcare. Springer, Cham. https://doi.org/10.1007/978-3-031-21524-7_4
Download citation
DOI: https://doi.org/10.1007/978-3-031-21524-7_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-21523-0
Online ISBN: 978-3-031-21524-7
eBook Packages: MedicineMedicine (R0)