Abstract
Dermatophytosis may affect the scalp and mostly present as tinea capitis in children. Here we present a 7-year-old girl patient with a 2-month history of itching followed by a round scaly patch of the scalp. She also presented with alopecia with visible short and dull hairs accompanied by whitish fine scales in the middle and around the ill-defined lesion. The lesion gave blue-green fluorescence in Wood lamp examination. KOH prep of the scalp and infected hair revealed hyphae and spores, ectothrix spores invasion on hair shaft. Fungal growth by culture found the growth of Microsporum canis. The patient is diagnosed as gray patch tinea capitis and treated with oral micronized griseofulvin 375 mg daily and topical ketoconazole 2% shampoo three times a week for 8 weeks resulted in complete clearance both clinically and microscopically.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
A seven-year-old Japanese girl was referred to the Department of Dermatology and Venerology with severe pruritus and scaly patch on the scalp since two months. The patient had a cat. She denied pulling her hair. No family members had similar skin lesions.
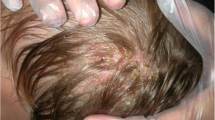
On physical examination, we found an ill-defined area of hair loss approximately six cm in diameter. Short and dull hairs with coexisted whitish, fine scales in the center and around the lesion were observed. A Wood’s lamp examination revealed blue-green fluorescence (Fig. 50.1). Her body weight was 17 kg.
Based on the case description and the photographs, what is your diagnosis?
-
1.
Gray patch tinea capitis.
-
2.
Seborrheic dermatitis.
-
3.
Alopecia areata.
-
4.
Trichotillomania.
Tinea capitis.
Discussion
The diagnosis of tinea capitis is mainly established based on patient’s history and clinical features supported by Wood’s lamp examination, direct mycological examination with potassium hydroxide and fungal culture. Fungal culture still remains as a gold standard diagnostic method [1, 2].
Treatment of choice for tinea capitis in children is microsized griseofulvin 20–25 mg/kg/day [1, 3]. Ketokonazol 2% shampoo two–four times weekly for two–four weeks is recommended as adjuvant therapy [1]. The differential diagnoses for the presented patient included seborrhoeic dermatitis , alopecia areata and tinea capitis. In seborrheic dermatitis, no broken hairs are presented [4]. Alopecia areata is characterized by the presence of well-defined areas of hair loss within the skin remains normal [5]. The patient did not have habit of hair pulling, thus trichotillomania was excluded [6].
In the presented patient, a direct mycological examination showed an ectothrix invasion on the hair shaft (Fig. 50.2). In fungal culture, Microsporum canis was isolated (Fig. 50.3
). The patient was treated with oral micronized griseofulvin 375 mg daily and topical ketoconazole 2% shampoo three times a week for eight weeks. Complete resolution of the skin lesions was observed. A follow-up mycological examination was negative.
Key Points
-
Tinea capitis is a superficial fungal infection commonly seen in children and caused by Microsporum and Trichophyton.
-
Tinea capitis typically requires oral treatment.
References
Craddock LN, Schieke SM. Superficial fungal infection. In: Kang S, Amagai M, Bruckner AL, Enk AH, Margolis DJ, McMichael AJ, et al., editors. Fitzpatrick’s dermatology. 9th ed. New York: McGraw Hill; 2019. p. 2923–51.
Shemer A, Grunwald MH, Gupta AK, Lyakhovetsky A, Daniel CR, Amichai B. Griseofulvin and fluconazole reduce transmission of tinea capitis in schoolchildren. Pediatr Dermatol. 2015;32(5):696–700.
Chen X, Jiang X, Yang M. Systemic antifungal therapy for tinea capitis in children (Review). Cochrane Library. 2016:3–39.
Suh DH. Seborrheic dermatitis. In: Kang S, Amagai M, Bruckner AL, editors. Fitzpatrick’s Dermatology, vol. 1. 9th ed. New York: McGraw-Hill Education; 2019. p. 428–37.
Islam N, Leung PSC, Huntley AC, Eric Gershwin M. The autoimmune basis of alopecia areata: a comprehensive review. Autoimmun Rev. 2015;14(2):81–9.
Grant JE, Redden SA, Leppink EW, Chamberlain SR. Trichotillomania and co-occurring anxiety. Compr Psychiatry. 2017;72:1–5.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Sari, P., Monica, Sugianto, Y.F.R., Ametati, H., Kusumaningrum, N., Afriliana, L. (2022). An Infectious Scalp Disorder. In: Waśkiel-Burnat, A., Sadoughifar, R., Lotti, T.M., Rudnicka, L. (eds) Clinical Cases in Scalp Disorders. Clinical Cases in Dermatology. Springer, Cham. https://doi.org/10.1007/978-3-030-93426-2_50
Download citation
DOI: https://doi.org/10.1007/978-3-030-93426-2_50
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-93425-5
Online ISBN: 978-3-030-93426-2
eBook Packages: MedicineMedicine (R0)