Abstract
Disasters like the recent COVID-19 pandemic can benefit from the use of digital tools and Knowledge Management Systems (KMSs) to manage the emergency and improve the resilience of the system. Such KMSs must prove the quality of the system, service, situation, and knowledge which is gathered, transferred, and shared. However, KMSs must cope with the presence of knowledge barriers, which limit to manage data and information successfully. Our chapter wants to deepen such a topic through the analysis of the case study of a web application developed by the IHU Strasbourg, one research and clinical centre, to collect and share knowledge between the end-users (citizens) and healthcare institutions, decision-makers, and public entities during the COVID-19 pandemic. Our findings highlight the need to ensure that not only the KMS possesses the recommended quality standards, but that specific features are put in place to cope with the presence of knowledge barriers, and the need for speed in the information flows to enhance resilience.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
The COVID-19, caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) (WHO, 2020a), was defined as a pandemic by the WHO Director-General on March 11th, 2020, given its cross-country and cross-continent spread (WHO, 2020b) and probably represents one of the recent biggest disasters followed by a health emergency. According to Dorasamy et al. (2013, p. 1834), a disaster is “a social crisis situation, a deadly event, usually unexpected and unanticipated and cause human suffering”. The definition of disasters includes “significant outbreak of infectious disease, bioterrorist attack, and other significant or catastrophic events” (He & Liu, 2015, p. 178) and often are followed by public health emergencies. Zibulewsky recalls the definition given by the American College of Emergency Physicians, who outlines a disaster “when the destructive effects of natural or man-made forces overwhelm the ability of a given area or community to meet the demand for health care” (Zibulewsky, 2001, p. 144). Recent examples of public health emergencies encompass the outbreak of H1N1 influenza, the Ebola virus disease in Central Africa, the SARS (Severe Acute Respiratory Syndrome), the Marburg haemorrhagic fever, in addition to widespread dysentery, cholera, measles, encephalitis B, and other conditions after relevant disasters.
When a disaster happens, disaster resilience can be defined as the ability of individuals, communities, organisations, and states to adapt to and recover from hazards, shocks, or stresses without compromising long-term prospects of development (Hernantes et al., 2017). Knowledge management systems (KMSs) have proved to help effective disaster management (Dorasamy et al., 2013, 2017), increasing the ability of the entire system to support resilience (Barbisch & Koenig, 2006; Cobianchi et al., 2020a; Therrien et al., 2017).
This chapter has the aim of investigating the characteristics of a KMS in disaster management through the use of digital tools to improve the resilience of the system, employing the case of a platform developed by the Institut Hospitalo-Universitaire (IHU), a primary research and clinical centre located in Strasbourg, France (Cobianchi et al., 2020c).
2 Disaster Management, Resilience, and Knowledge Management Systems
Disasters occur suddenly and demand quick reactions, creating, at the same time, uncertainty and stress (Dorasamy et al., 2013). Healthcare systems periodically need to confront and manage crises, like the recent COVID-19 pandemic, the Severe Acute Respiratory Syndrome, H1N1, and Ebola, plus natural disasters, accidents of enormous intensity, and terroristic attacks, during which they are required to deal with exceptional situations without interrupting essential services to the population.
The ability to effectively accomplish this dual mandate is at the heart of resilience strategies, which means, for healthcare organisations, the need to develop surge capacity to manage a sudden influx of patients and people in need (Therrien et al., 2017), offering a timely response (AminShokravi & Heravi, 2020). The aims of activating surge capacity and, at the same time, maintaining other essential services require resilience, which can also be defined as “the capacity of a social system (e.g. an organisation, city, or society) to proactively adapt to and recover from disturbances that are perceived within the system to fall outside the range of normal and expected disturbances” (Boin et al., 2010, p. 9).
In this regard, surge capacity can be defined as “the ability to respond to a sudden increase in patient care demands” (Hick et al., 2008, p. S51), providing “a potential means to capture and coordinate the commonalities of pandemic and disaster planning needs in order to generate a model for health systems’ readiness for and response to a wide range of scenarios” (Watson et al., 2013, p. 82), also involving the local communities, who are called to cooperate (Adini et al., 2017; Berawi, 2020). Barbisch and Koenig (2006) have defined the “four S’s” of surge capacity: trained personnel (staff), supplies and equipment (stuff), beds’ availability and specific areas in which to treat patients (structure), and policies and procedures (systems).
In particular, systems refer to organisational procedures and specific crisis management plans able to develop surge capacity development tools (Therrien et al., 2017). The literature has highlighted how there has been little research on how these relate to system surge capacity (Therrien et al., 2017; Watson et al., 2013) from a resilience perspective. Disaster management requires activities like “mitigation, risk reduction, prevention, preparedness, response and recovery” (Dorasamy et al., 2013, p. 1834).
Knowledge management can help when a disaster occurs, and a well-designed KMS can help in handling it. Lacks in KMSs may cause major issues in managing the emergency (Dorasamy et al., 2013) as well as delays in the transition and recovery phases (Blackman et al., 2017; Dorasamy et al., 2017). On the contrary, a well-designed system can contribute to increasing resilience by empowering the fourth “S” factor (Barbisch & Koenig, 2006).
According to the literature, a well-designed KMS for disaster management should gather a group of experts together (Abouei et al., 2019; Dorasamy et al., 2017), allowing an effective platform for sharing prior experience in disaster management, helping with a timely response (Berawi, 2020; Dorasamy et al., 2013). Experts’ viewpoints can help to address disaster management issues (Dorasamy et al., 2013) as well as pre-allocate resources (Arora et al., 2010). Modern systems need to facilitate more “a robust and flexible creation, storage, sharing and ultimately dissemination of a disaster-related knowledge base” (Dorasamy et al., 2013, p. 1850). In this perspective, the literature suggests how such systems can profit from the avail of social networking ideas driven by web 2.0 architectures to provide a more vibrant and live use of KMSs in a disaster emergency (Berawi, 2020; Howe et al., 2011; Huang et al., 2010; Massaro et al., 2020). This includes the use of wikis, blogs (Linstone & Turoff, 2010), mobile apps, and big data analytics (Reuter & Spielhofer, 2017; Wang et al., 2020). The ideal KMS should facilitate both informational and knowledge requirements of different roles run by multiple institutions and decision-makers (Turoff et al., 2004), coordinating efforts and allowing the effective sharing of data of various kinds (Shaw et al., 2017).
A successful KMS model (Jennex & Olfman, 2006), which can be applied for emergencies in a resilience perspective according to Barbisch and Koenig’s “four S’s” of surge capacity framework (2006), has four critical success factors (Dorasamy et al., 2017). The first one is System Quality (SQ), and it can be defined as “how well the KMS performs the functions of knowledge creation, storage/retrieval, transfer, and application; how much of the knowledge is represented in the computerised portion of the OM (organisational memory); and the KM infrastructure” (Jennex & Olfman, 2006, p. 40). When applied to emergency management, the system must enhance its usability, availability, reliability, adaptability, and response time (Dorasamy et al., 2017). The second success factor is Knowledge Quality (KQ), which is about understanding which knowledge the KMS must capture and process. The third success factor is Service Quality, which allows the KMS to use and benefit from knowledge in the best possible way, ensuring accuracy, sufficiency, timeliness, relevance, usability, and comprehension of the possessed knowledge (Dorasamy et al., 2017). Last but not least, the KMS must ensure enough Situational Quality (SQ), which deals with the unique features of a certain situation that require various responses and attitude (Dorasamy et al., 2017).
In general terms, designing and implementing effective KMSs may be difficult because of the presence of knowledge barriers (Riege, 2005), which limit the effective sharing and capture of knowledge. The literature identifies potential individual barriers (e.g. the fear to share, the presence of various skills and competencies), organisational barriers (e.g. differences in aims, goals, and culture, shortage of appropriate infrastructure, …), and technology barriers (e.g. lack of integration of IT systems, reluctance to use IT tools, …) (Massaro et al., 2012; Riege, 2005). Given the importance of KMSs to support the management and recovery phase of emergencies, it is thus essential to understand how to develop a proper KMS, ensuring the presence of key features, and trying to overcome barriers.
3 Case Study
The case study (Yin, 2014) was employed in collaboration with the Institut Hospitalo-Universitaire (IHU) of Strasbourg, France, a primary research and clinical centre active in medical education as well as technological transfer, dedicated to Image-Guided Surgery (Cobianchi et al., 2020c; Garcia Vazquez et al., 2020). Data were gathered during the months of March, April, and May 2020, through various sources, like the project plan, the Slack project channel, and online interviews with several staff members, to ensure validity and data triangulation (Massaro et al., 2019). All results were verified with the project team and scientific chief, and principal investigator.
The COVID-19 pandemic has severely affected the healthcare sector (Cobianchi et al. 2020a, 2020b), and the decision-makers are struggling to find effective epidemiological tools and aggregate data to rely on (Xu & Kraemer, 2020). The IHU team decided to answer the call to reduce such a gap, through the creation of a web software tool. The crisis has forced healthcare professionals worldwide to shift from individual patient-centred care to more public health ethics (Angelos, 2020; Ferguson Bryan et al., 2020), to reach more population and give more comprehensive solutions. The aim is to maximise the outcomes for the general population (Dal Mas et al., 2019) through the use of an easy human-machine tool.
In the absence of pharmaceutical treatments such as vaccines or effective drugs, non-pharmaceutical intervention (NPI) like social distancing, home isolation of suspect cases, home quarantine of those living in the same household as suspect cases, and social distancing of the elderly and others at most risk of severe disease, enforced by Governments may be the only way to limit the spreading of the virus, which, without containment, accelerates quickly, like it has happened in China, Iran, Italy, the UK, Spain, and France (Massaro et al., 2021). The fast spreading (Ji et al., 2020) shows like health authorities are often informed in a delayed manner of the development of the epidemic and, in particular, only detect the spread of the virus at a late stage, especially the minor or moderate forms of the disease (Pisano et al., 2020). In all the affected countries, web-based applications are developing in an anarchic way with similar objectives, which can be summarised as follows: (1) to help patients to make a first own diagnosis (self-assessment); (2) to advise them on what to do, depending on the epidemiological context of the country and its healthcare system; (3) to help health professionals to make medical decisions quickly; (4) to help health professionals to collect data about their patients easily. Collecting even only parts of the information gathered by all available applications on the web and from smartphones would probably make it possible to anticipate and monitor the territorial development of the virus, providing valuable epidemiological data for the future.
The IHU team, made by physicians, engineers, researchers, and information technology (IT) experts, decided to design and develop a web-based solution to federate the collection of data generated by all the web software initiatives that give patients and medical doctors access to patient counselling, patient orientation, or medical decision support.
The first aim of the project was to develop a free, open-source, non-commercial web-based platform (Dal Mas et al., 2020b; Presch et al., 2020) that allows any team around the world that is developing or wishes to develop applications to help manage the COVID-19 crisis to find the resources they need to both collect data and build their apps, by relying on a comprehensive and rigorous protocol and dataset, which is updated and validated with the latest scientific and epidemiological results. The platform allows collecting on a centralised platform all the information gathered to record it in an open-source format (OpenEHR).Footnote 1
The second aim was to enable real-time operational reporting for healthcare organisations, regions, and nations. Such a purpose is consistent with all the International and WHO guidelines, which recommend publishing all pertinent information in real-time using unique and consistent dashboards, allowing to download the collected knowledge and data free of charge for scientific or public health purposes (Xu & Kraemer, 2020).
Moreover, the platform aimed to provide a pre-formatted toolkit, built in a rigorous and scientific-verified way, through collaboration with the international clinical community active in the research of the disease so that local initiatives can quickly publish new web-based applications for COVID while ensuring easy centralised collection. The derived web applications can be designed using layouts, languages, and measures, which can translate knowledge (Dal Mas et al., 2020a; Graham et al., 2006; Lemire et al., 2013; Savory, 2006) in an easier way for the end-users, but at the same time maintaining the common architecture for homogeneous data collection and analysis. The way the platform is built makes it suitable for any other transmissible flu-based infectious disease.
Also, the web application had to allow supporting frontline physicians and healthcare professionals in providing healthcare assessment, letting thus coproduction of the healthcare service together with the patient (Batalden et al., 2016; Biancuzzi et al., 2019; Elwyn et al., 2020), and involving the communities as recommended by the literature on healthcare resilience (Adini et al., 2017; Berawi, 2020; Blackman et al., 2017).
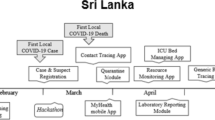
Figure 14.1 shows some screenshots gathered from the web application.
The platform should be built around some relevant pillars: the quality of medical data collection, with particular attention towards all the possible questions, and how these should be posed; the security and regulatory constraints to comply with GDPR (General Data Protection Regulation), HIPAA (Health Insurance Portability and Accountability Act), and all the active regulations worldwide; the implementation, to ensure full data sharing; and the self-assessment tool generator, to allow healthcare institutions or government to quickly customise the form, for a better response of patients.
More details about the application are summarised in Table 14.1, which maps such characteristics according to the features of a KM system in crisis management and the potential KM barriers.
Although modern technology can offer pioneering solutions and opportunities to collect and share knowledge, technological barriers like lack in compatibility can limit the effectiveness of the KMS. Analysing such aspect, the IHU team decided, for instance, to use a web-based platform, avoiding the need to download it, and to create ex-ante protocols and dashboards to process data without any further test, which may be complicated because of a lack in compatibility.
Organisational barriers make it difficult to incorporate the KMS into the culture of the institution. Pandemic disaster management requires overcoming any cultural bias or limit, to ensure that the standard is rigorous and scientific robust. An unknown disease requires a big effort by the international community, which must share epidemiological data, clinical recommendations, organisational best practice, and lessons learned. Ensuring the presence of multidisciplinary experts worldwide (Dorasamy et al., 2013) can help to update the scientific and clinical dataset and outcome (for instance, about symptoms and experimental drugs).
Last but not least, individual barriers can also represent a severe obstacle in the effective use of KMSs. In the IHU Strasbourg case, data is collected from people, who can also benefit from the app as a coproduced first aid healthcare service. Ensuring that such knowledge is well-managed, meaning collected and shared, is essential, especially taken into consideration the different competencies, skills, culture, and emotional states of the end-users. Translating knowledge (Dal Mas et al., 2020a; Graham et al., 2006; Savory, 2006) is thus important to reach the outcome. For this reason, the IHU team made sure that full customisation of the front-end was possible, in order to select the language, the look of the template, the way to formulate the questions, the measures according to the local standards (for example, Celsius versus Fahrenheit). At the same time, the dataset and internal architecture should elaborate and aggregate information in a standardised and rigorous way.
4 Discussions and Conclusions
The IHU Strasbourg experience allows highlighting in practice the features of a KMS which can help disaster management, more specifically during the COVID-19 pandemic, enhancing resilience. The literature has stressed the relevance of KMSs in crisis management, to share good knowledge in a fast way, through a high-quality and well-designed system (Dorasamy et al., 2013, 2017). In ensuring the collection, transfer, and sharing of useful knowledge, some recommendations have been identified, such as gathering experts and stakeholders (Abouei et al., 2019; Dorasamy et al., 2013), and using modern technologies like web apps and data analytics to develop a KMS (Reuter & Spielhofer, 2017; Wang et al., 2020). However, the development of a KMS for disaster management, which can foster the fourth “S” factor of the Barbisch and Koenig’s “four S’s” of surge capacity framework, has specific requirements that must be considered.
First, KMS must be integrated within all the institutions that are managing the recovery strategy from the disaster. The web platform under development by IHU Strasbourg allowed us to highlight the importance not only to ensure the quality of the system, service, situation, and knowledge but also to put in place effective tools and practical actions to overcome the potential knowledge barriers (Riege, 2005). Such knowledge barriers may involve both the end-user, but also the institution or decision-maker that needs to access knowledge to plan the actions to manage the crisis. When barriers are in place, the knowledge flow is less smooth, and even the kind of knowledge can be compromised.
Second, speed is a crucial element in disaster management. Being fast, however, requires the development of a knowledge flow that proceeds fluently. Knowledge barriers can limit the exchange of essential information and the knowledge application to solve specific issues (Riege, 2005). While existing literature focuses on the characteristics of a KMS, less attention has been paid to the elements that can limit the knowledge flow and turn into an action paste reduction. In the case of the COVID-19, considering its deadly rate and its spread capacity, those problems might end up with severe consequences if not appropriately addressed.
In all, in a situation like the current COVID-19 pandemic, not only the quality of knowledge matters but also the speed in transferring and sharing knowledge, information, data among meaningful stakeholders, including the communities, who appear as central actors in the resilience perspective. Quick actions can prevent dangerous results. Ensuring that enough tools are put in place to avoid knowledge barriers can thus help the KMS to allow fast knowledge sharing and rapid responses to the crisis.
Our chapter contributes to the knowledge management theory by addressing the features of a KMS for disaster management to foster resilience, including the need to overcome the knowledge barriers to ensure effective implementation in a galaxy of institutions involved in the recovery and the speed in the information flows. Thus, the implications of our study may be useful for practitioners, which may consider our results while designing their KMSs to increase their surge capacity.
Notes
- 1.
See https://www.openehr.org/, accessed May fifth, 2020.
References
Abouei, M., Dal Mas, F., Ghazvini, A., Attaran, M., Ansari, K., Nozari, K., Massaro, M., et al. (2019). Knowledge management in a public entity in the area of urban regeneration: The importance of stakeholder participation. In D. Remeniy (Ed.), 5th knowledge management and intellectual capital excellence awards (pp. 1–14). Academic Conferences and Publishing International Limited, Reading.
Adini, B., Cohen, O., Eide, A. W., Nilsson, S., Aharonson-Daniel, L., & Herrera, I. A. (2017). Striving to be resilient: What concepts, approaches and practices should be incorporated in resilience management guidelines? Technological Forecasting and Social Change, 121, 39–49.
AminShokravi, A., & Heravi, G. (2020). Developing the framework for evaluation of the inherent static resilience of the access to care network. Journal of Cleaner Production, 267, 122123.
Angelos, P. (2020). Surgeons, ethics, and COVID-19 : Early lessons learned. Journal of the American College of Surgeons, 230(6), 1119–1120.
Arora, H., Raghu, T. S., & Vinze, A. (2010). Resource allocation for demand surge mitigation during disaster response. Decision Support Systems, 50(1), 304–315.
Barbisch, D. F., & Koenig, K. L. (2006). Understanding surge capacity: Essential elements. Academic Emergency Medicine, 13(11), 98–1102.
Batalden, M., Batalden, P., Margolis, P., Seid, M., Armstrong, G., Opipari-arrigan, L., & Hartung, H. (2016). Coproduction of healthcare service. BMJ Quality & Safety, 25(7), 509–517.
Berawi, M. A. (2020). Empowering healthcare, economic, and social resilience during global pandemic Covid-19. International Journal of Technology, 11(3), 436–439.
Biancuzzi, H., Miceli, L., Bednarova, R., & Garlatti, A. (2019). Post-breast cancer coaching: The synergy between health and fitness through coproduction. Igiene e Sanità Pubblica, 75(3), 181–187.
Blackman, D., Nakanishi, H., & Benson, A. M. (2017). Disaster resilience as a complex problem: Why linearity is not applicable for long-term recovery. Technological Forecasting and Social Change, 121(March), 89–98.
Boin, A., Comfort, L. K., & Demchak, C. C. (2010). The rise of resilience. In L. K. Comfort, A. Boin, & C. C. Demchak (Eds.), Designing resilience: Preparing for extreme events (pp. 1–12). University of Pittsburgh Press.
Cobianchi, L., Dal Mas, F., Peloso, A., Pugliese, L., Massaro, M., Bagnoli, C., & Angelos, P. (2020a). Planning the full recovery phase: An Antifragile perspective on surgery after COVID-19. Annals of Surgery, 272(6), e296–e299.
Cobianchi, L., Dal Mas, F., Piccolo, D., Peloso, A., Secundo, G., Massaro, M., Takeda, A., et al. (2020b). Digital transformation in healthcare. The challenges of translating knowledge in a primary research, educational and clinical Centre. In K. S. Soliman (Ed.), International business information management conference (35th IBIMA) (pp. 6877–6888). IBIMA.
Cobianchi, L., Pugliese, L., Peloso, A., Dal Mas, F., & Angelos, P. (2020c). To a new normal: Surgery and COVID-19 during the transition phase. Annals of Surgery, 272(2), e49–e51.
Dal Mas, F., Massaro, M., Lombardi, R., & Garlatti, A. (2019). From output to outcome measures in the public sector. A structured literature review. International Journal of Organizational Analysis, 27(5), 1631–1656.
Dal Mas, F., Biancuzzi, H., Massaro, M., & Miceli, L. (2020a). Adopting a knowledge translation approach in healthcare coproduction. A case study. Management Decision, 58(9), 1841–1862.
Dal Mas, F., Piccolo, D., & Ruzza, D. (2020b). Overcoming cognitive bias through intellectual capital management. The case of pediatric medicine. In P. Ordonez de Pablos & L. Edvinsson (Eds.), Intellectual capital in the digital economy (pp. 123–133). Routledge.
Dorasamy, M., Raman, M., & Kaliannan, M. (2013). Knowledge management systems in support of disasters management: A two decade review. Technological Forecasting and Social Change, 80(9), 1834–1853.
Dorasamy, M., Raman, M., & Kaliannan, M. (2017). Integrated community emergency management and awareness system: A knowledge management system for disaster support. Technological Forecasting and Social Change, 121, 139–167.
Elwyn, G., Nelson, E., Hager, A., & Price, A. (2020). Coproduction: When users define quality. BMJ Quality and Safety, 29(9), 711–716.
Ferguson Bryan, A., Milner, R., Roggin, K. K., Angelos, P., & Matthews, J. B. (2020). Unknown unknowns: Surgical consent during the COVID-19 pandemic. Annals of Surgery, 272(2), e161–e162.
Garcia Vazquez, A., Verde, J. M., Dal Mas, F., Palermo, M., Cobianchi, L., Marescaux, J., Gallix, B., et al. (2020). Image-guided surgical e-learning in the post-COVID-19 pandemic era: What is next? Journal of Laparoendoscopic & Advanced Surgical Techniques, 30(9), 993–997.
Graham, I. D., Logan, J., Harrison, M. B., Straus, S. E., Tetroe, J., Caswell, W., & Robinson, N. (2006). Lost in knowledge translation: Time for a map? Journal of Continuing Education in the Health Professions, 26(1), 13–24.
He, Y., & Liu, N. (2015). Methodology of emergency medical logistics for public health emergencies. Transportation Research Part E: Logistics and Transportation Review, 79, 178–200.
Hernantes, J., Labaka, L., Turoff, M., Hiltz, S. R., & Bañuls, V. A. (2017). Moving forward to disaster resilience: Perspectives on increasing resilience for future disasters. Technological Forecasting and Social Change, 121(May), 1–6.
Hick, J. L., Koenig, K. L., Barbisch, D., & Bey, T. A. (2008). Surge capacity concepts for health care facilities: The CO-S-TR model for initial incident assessment. Disaster Medicine and Public Health Preparedness, 2(S1), S51–S57.
Howe, A. W., Jennex, M. E., Bressler, G. H., & Frost, E. G. (2011). Exercise 24: Using social media for crisis response. International Journal of Information Systems for Crisis Response and Management, 3(4), 36–54.
Huang, C. M., Chan, E., & Hyder, A. (2010). Web 2.0 and internet social networking: A new tool for disaster management? Lessons from Taiwan. BMC Medical Informatics and Decision Making, 10(57), 1–5.
Jennex, M. E., & Olfman, L. (2006). A model of knowledge management success. International Journal of Knowledge Management, 2(3), 51–68.
Ji, Y., Ma, Z., Peppelenbosch, M. P., & Pan, Q. (2020). Potential association between COVID-19 mortality and healthcare resource availability. The Lancet Global Health, 8(4), e480.
Lemire, N., Souffez, K., & Laurendeau, M. C. (2013). Facilitating a knowledge translation process. Knowledge review and facilitation tool. Institut Publique de Santé du Quebec.
Linstone, H. A., & Turoff, M. (2010). Delphi: A brief look backward and forward. Technological Forecasting and Social Change, 78(9), 1712–1719.
Massaro, M., Dal Mas, F., Bardy, R., & Mazzola, D. (2012). Knowledge management in alliances between mncs and smes: Evidence from the pharmaceutical field. In Proceedings of the European conference on knowledge management, ECKM, (708–716). Academic Conferences and Publishing International Limited, Reading.
Massaro, M., Dumay, J., & Bagnoli, C. (2019). Transparency and the rhetorical use of citations to Robert Yin in case study research. Meditari Accountancy Research, 27(1), 44–71.
Massaro, M., Dal Mas, F., Chiappetta Jabbour, C. J., & Bagnoli, C. (2020). Crypto-economy and new sustainable business models: Reflections and projections using a case study analysis. Corporate Social Responsibility and Environmental Management, 27(5), 2150–2160.
Massaro, M., Tamburro, P., La Torre, M., Dal Mas, F., Thomas, R., Cobianchi, L., & Barach, P. (2021). Non-pharmaceutical interventions and the Infodemic on twitter: Lessons learned from Italy during the Covid-19 pandemic. Journal of Medical Systems, 45(50), 1–12.
Pisano, G., Sadun, R. M., & Zanini, M. (2020). Lessons from Italy’s response to coronavirus. Harvard Business Review. Available at: https://hbr.org/2020/03/lessons-from-italys-response-to-coronavirus.
Presch, G., Dal Mas, F., Piccolo, D., Sinik, M., & Cobianchi, L. (2020). The World Health Innovation Summit (WHIS) platform for sustainable development. From the digital economy to knowledge in the healthcare sector. In P. Ordonez de Pablos & L. Edvinsson (Eds.), Intellectual capital in the digital economy (pp. 19–28). Routledge.
Reuter, C., & Spielhofer, T. (2017). Towards social resilience: A quantitative and qualitative survey on citizens’ perception of social media in emergencies in Europe. Technological Forecasting and Social Change, 121, 168–180.
Riege, A. (2005). Three-dozen knowledge-sharing barriers managers must consider. Journal of Knowledge Management, 9(3), 18–35.
Savory, C. (2006). Translating knowledge to build technological competence. Management Decision, 44(8), 1052–1075.
Shaw, D. R., Grainger, A., & Achuthan, K. (2017). Multi-level port resilience planning in the UK: How can information sharing be made easier? Technological Forecasting and Social Change, 121, 126–138.
Therrien, M. C., Normandin, J. M., & Denis, J. L. (2017). Bridging complexity theory and resilience to develop surge capacity in health systems. Journal of Health Organisation and Management, 31(1), 96–109.
Turoff, M., Chumer, M., Walle, B. V. D., & Yao, X. (2004). The design of a dynamic emergency response management information system (DERMIS). Journal of Information Technology Theory and Application, 5(4), 1–35.
Wang, C. J., Ng, C. Y., & Brook, R. H. (2020). Response to COVID-19 in Taiwan: Big data analytics, new technology, and proactive testing. JAMA, 323(14), 1341–1342.
Watson, S. K., Rudge, J. W., & Coker, R. (2013). Health systems’ ‘surge capacity’: State of the art and priorities for future research. Milbank Quarterly, 91(1), 78–122.
WHO. (2020a). Novel Coronavirus(2019-nCoV) Situation report – 13. Available at: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200202-sitrep-13-ncov-v3.pdf.
WHO. (2020b). WHO Director-General’s opening remarks at the media briefing on COVID-19 – 11 March 2020, WHO. Accessed April 1, 2020, from https://www.who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19%2D%2D-11-march-2020.
Xu, B., & Kraemer, M. U. G. (2020). “Open access epidemiological data from the COVID-19 outbreak ”, the lancet. Infectious Diseases, 20(5), p534.
Yin, R. K. (2014). Case study research: Design and methods. Sage Publications.
Zibulewsky, J. (2001). Defining disaster: The emergency department perspective. Baylor University Medical Center Proceedings, 14(2), 144–149.
Acknowledgements
This research was partially support by Investissement d’avenir ANR-10-IAHU-02.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Dal Mas, F. et al. (2022). Resilience, Digital Tools, and Knowledge Management Systems in the Pandemic Era: The IHU Strasbourg Experience. In: Matos, F., Selig, P.M., Henriqson, E. (eds) Resilience in a Digital Age. Contributions to Management Science. Springer, Cham. https://doi.org/10.1007/978-3-030-85954-1_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-85954-1_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-85953-4
Online ISBN: 978-3-030-85954-1
eBook Packages: Business and ManagementBusiness and Management (R0)