Abstract
A comparative assessment of socioeconomic determinants of stunting between India and Bihar is displayed in this study. The data from the National Family Health Survey-4 is used in this study to examine the comparative scenario of stunting between Bihar and India. Primary evidence of childhood stunting from Bhagalpur District has used to represent the eastern Bihar in our study. The bivariate and binary logistic regression models are used to accomplish the study objectives. A comparison in child growth between WHO standard and the sample from Bhagalpur District of Bihar has been also done. There is an over 10% difference in stunting prevalence between India and Bihar. We find that older children, children of higher birth order, children practicing unsafe disposal of stool, children born to lower educated mothers, and belong to poor households have significantly higher odds of stunting in Bihar as well as India. Child height for age only aligned with WHO standards in early childhood (0–12 months) for Bhagalpur District, but the likelihood of child stunting rises as age increases. Thus, we recommend effective program interventions keeping the socioeconomic and demographic vulnerabilities of children into consideration, reducing children stunting to attain the Sustainable Development Goals by 2030 in Bihar as well as India.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Nutritional status plays a significant role in children’s physical and mental development informative stage of life (Kumar et al. 2010). Stunting is one of the key indicators of chronic malnutrition and is closely associated with failure of ideal linear growth potential (Fenske et al. 2013). Postnatal child death is significantly associated with child height and the presence of diseases; a stunted child is more likely at risk of death (Bozzoli et al. 2009). The United Nations' estimates that about 45% of death of children under 5 years are due to malnutrition in India (UNICEF 2014). Stunting is linked with poor cognitive development and physical growth in the early stage of life and lower school achievement than non-stunted children in late adolescence (Grantham-McGregor et al. 1991). Furthermore, the meager psychological functioning of stunted children is probable to affect their quality of life as well as social and personal spheres throughout their whole life (Walker et al. 2007). Given the physical, mental, and economic significance of healthy child growth, reduction of the proportion of under-5 malnourished children through lessening hunger and poverty by 2015 was the important key indicator of MDG Goal 1. SDG 2 targeted to end all forms of malnutrition and hunger by 2030.
Recent estimates of the WHO suggested that globally the prevalence of stunting has been reducing from 32.4% to 21.3% during 2000–2019. Nevertheless, about 144 million children under 5 years of age were found to be stunted in 2019 (WHO 2020). Regionally, South Asia alone shares about 38.9% of the world’s stunted children (WHO 2020). Furthermore, about 38% of children under age 5 years are stunted in 2015–2016 (IIPS and ICF 2017). Among the neighboring countries of India, Bangladesh and Nepal are advanced in reducing the prevalence of stunting than India and Pakistan; more progress is found among highly educated and wealthy household (Frongillo Jr et al. 1997; Krishna et al. 2018). In India, severe stunting of children noticeably declined, and remarkable progress of declining stunting are found in the central, eastern, and northern regions, especially among the poorest household (Nie et al. 2019). A persisting gap in the prevalence of stunting exist among the states ranging from 48% in Bihar to 20% in Kerala in 2015–2016 (IIPS and ICF 2017). A noticeable high stunting prevalence is found in empowered action group (EAG) states. Bihar is one of the members of this high policy focus of India. Malnutrition was extremely concentrated among the poorest in the areas with the ICDS program and other government-sponsored nutritional programs during 1992–2006 in India (Pathak and Singh 2011).
There are socioeconomic, regional, and demographic differentials in child malnutrition in India. The rural-urban gap in stunting is highly observed in Assam, Maharashtra, Gujarat, and Punjab (IIPS and ICF 2017; Banerjee et al. 2017). The district-level prevalence of stunting and wealth disparity is more closely correlated than other nutritional status such as underweight and overweight (Khan & Mohanty 2018). The wealth disparity in stunting has noticeably been observed among districts in Bihar and other disadvantageous states in India (Liou et al. 2020). Young et al. (2016) suggested that child malnutrition is one of the major public health challenges in Bihar; poor breastfeeding practices, household hunger, low-income status, poor dietary practices, and illiteracy are major causes of malnutrition in Bihar. Meenakshi (2016) suggested that the triple burden of malnutrition increased in India. As per food, the quality of food is highly correlated with child nutrition. A study by Sharma (2019) finds a limited improvement in the child’s nutritional status during recent decades; malnutrition continued to be high among poor households. Khan and Mohanty (2018) show the prevalence of stunting child heterogeneously spread in India and highly clustered in districts belonging to Uttar Pradesh, Bihar, Jharkhand, and Madhya Pradesh. The districts with high poverty, low education, and low mother’s BMI have a higher risk of stunting. A detailed literature review on the correlates of stunting in India is discussed in the following.
1.1 Review of Literature: Socioeconomic and Demographic Correlates
Many previous studies examined socioeconomic correlates of malnutrition especially stunting in India and elsewhere (Rengma et al. 2015; Kanjilal et al. 2010; Jena et al. 2019; Singh et al. 2018; Singh et al. 2019; Khadse and Chaurasia 2020; Sultana et al. 2019). Interstate inequality exists in India; the disproportionate burden of stunting existed among children from poor socioeconomic status. Despite the high prevalence of stunting in rural areas, the urban poor are more vulnerable in terms of child stunting. The state domestic product (NSDP) is negatively associated with the risk of stunting in India (Kanjilal et al. 2010). Lower-middle developed countries have been moving toward the dual burden of malnutrition due to changing socioeconomic conditions, demographic transition, food habits, and noncommunicable diseases during recent two decades (Rengma et al. 2015). Jena et al. (2019) found that severe acute malnutrition is more prevalent among male child, 6–12 months of age group, and rural and socioeconomically backward groups. Inadequate breastfeeding practice and poor child care are significant factors of severe acute malnutrition in Odisha. Singh et al. (2019) presented that district-level variation and socioeconomic inequalities in malnutrition present in India are mainly concentrated among districts of western, central, and eastern regions with high birth order and underdeveloped. Children belong to a low socio-economic background with illiterate women mother, less likely to maintain water, sanitation, and hygiene (WASH) practice in households, making children more vulnerable to malnutrition . Khadse and Chaurasia (2020) showed that stunting is heavily concentrated among socially backward groups, especially in scheduled caste and rural communities. The mother’s body mass index (BMI), breastfeeding practice, and mobility of children are the strong predictors of stunting. The probability of stunting increased with increasing child’s age, illiteracy, poor wealth status, and first birth at an early age. Mothers with normal BMI are less likely to have stunting children (Sultana et al. 2019).
Studies by Fenske et al. (2013) covered all possible factors of child stunting such as socioeconomic, maternal, and regional characteristics as well as nutritional, healthcare facility, and infection-related factors in India. This study confirms that child’s age and sex are non-modifiable factors and highlights that maternal education, household wealth, ideal BMI of the mother, and proper utilization of healthcare facilities are significant protective factors of child stunting. Nie et al. (2019) observed that severe stunting of children has been noticeably declined and remarkable progress of declining stunting has been found in the central, eastern, and northern regions, especially among the poorest household. The prominent factors of declining child stunting are mother’s BMI and education, and autonomy level has a relatively significant contribution to the decline in the level of stunting. Bozzoli et al. (2009) presented that postnatal child death is significantly associated with child height and the presence of diseases. Energy availability, female literacy, health expenditure, and gross national product (GNP) are closely associated with child stunting (Frongillo Jr et al. 1997).
Besides these socioeconomic , demographic, and regional factors, maternal health-related characteristics play crucial roles in the likelihood of childhood stunting. As stunting is the result of chronic malnutrition, stunting during the neonatal stage of life is closely associated with a maternal causes such as malnutrition of the mother and nonexclusive breastfeeding, but after the appearance of stunting during the postnatal period is mainly caused by poor nutritional dietary practice (Singh et al. 2018). Lack of early breastfeeding, insufficient food supply, and security, micronutrient deficiency, poor wealth and healthcare status, low standard of living, illiteracy, and poor quality of child care are leading factors of malnutrition in South Asia (Akhtar 2016). Similarly, the ideal BMI of mothers and proper utilization of healthcare facilities are significant protective factors of child stunting (Fenske et al. 2013). In addition, disease prevalence of children during childhood period, maternal factors such as nutritional status of mother and breastfeeding practice, and environmental factors are significant predictors of child stunting. The preceding birth interval and birth order of the children have significant effects on childhood stunting in South Asian countries, especially in India (Rana et al. 2019; Rana and Goli 2018).
In India, most of the studies examined socioeconomic correlates of stunting, socioeconomic inequalities in malnutrition, intersocial and intrasocial group differentials, prevalence and correlates of malnutrition, and also at district and regional level patterns of malnutrition. Among the EAG states, Bihar is one of the populous states of India which has a very high level of childhood stunting. Bhagalpur District, being a socioeconomically prominent district of western Bihar, remains to have high prevalence of childhood stunting. This is the first ever study in India that has focused on a comparative analysis of socioeconomic determinants of stunting between India and Bihar, using both primary and secondary data. Therefore, in this paper, we examine a comparative assessment of the socioeconomic determinants of stunting between India and Bihar. Further, we present primary evidence of childhood stunting from Bhagalpur District representing the eastern Bihar .
2 Data and Methods
2.1 Data Sources and Sample Selection
Data from the National Family Health Survey-4 (NFHS-4) is used in this study for a comparative analysis of India and Bihar. The NFHS is a large-scale multi-round survey, conducted throughout the country in 2015–2016. The Ministry of Health and Family Welfare (MOHFW) , Government of India, designated the International Institute for Population Sciences (IIPS) , Mumbai, as the nodal agency responsible for providing coordination and technical guidance for the survey. This nationally representative survey is an Indian version of the Demographic and Health Surveys (DHS) , providing consistent and reliable estimates of fertility, mortality, family planning, child’s nutritional status, morbidity, utilization of maternal and child healthcare services, anemia, utilization and quality of health and family planning, and other related indicators at the national, state, and regional levels. The data from the NFHS is extensively used in various policy and program formulations; as of now, four rounds have been conducted during the years 1992–1993, 1998–1999, and 2014–2016. The NFHS-4 covered a nationally representative sample of 601,509 households, comprising 699,686 women of reproductive age (aged 15–49 years), 103,525 men (aged 15–54 years), and 259,627 children (0–5 years). In our study, the unit of analysis is births which took place 5 years preceding the survey. The selected sample for this study included children with valid height measurements. The study used a total sample of 225,002 and 22,275 births for India and Bihar, respectively (IIPS and ICF 2015–2016).
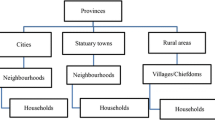
The evidence from the Bhagalpur District has been presented based on the sample collected during March–April 2019. A sample of 512 under-5 children has been collected from 512 households of four sample blocks of Bhagalpur District. Out of 16 blocks of Bhagalpur District, four blocks and nine sample villages were selected for the survey. A multilevel sampling method for selecting blocks, place of residence, villages, and households has been applied. Nine villages have been selected purposively such as Fatehpur, Mansarpur, Bhiti, and Rajpur of Sabour C.D. block, Asandpur of Jagdishpur C.D. block, Agarpur of Goradih C.D. block, and Karela, Nurpur, and Mahandpur of Nathanagar C.D. block. These blocks are situated in the southern part of the District of Bhagalpur. Within these blocks, households with at least one child born within the last 5 years were selected randomly for the primary survey.
2.2 Variable Description
2.2.1 Outcome Variable
The outcome variable for this study is stunting, which refers to height for age. It expressed a low height relative to age and resulted from a slowing in skeletal growth. Stunting can be caused by poor dietary intake over time as well as poor health condition and reflects a failure to reach growth potential. Children whose height-for-age Z-score are below minus two standard deviations (−2 SD) from the median of the reference population are considered short for their age (stunted) or chronically undernourished (WHO 2007).
2.2.2 Predictor Variables
We included explanatory variables at the child, mother, and household levels. We selected the confounders after an extensive review of existing literature. Child’s age at months 0–5, 6–11, 12–23, 24–35, 36–47, 48–59, sex of the child (male and female), child’s birth order (1, 2, 2–3, and 4+), child’s breastfeeding timing (immediately, within 1 h, after 1 h, missing), diarrhea status (no, yes, and missing), and child’s stool disposal (unsafe, safe, and missing) are considered the child level. At the mother level, the confounders selected were consumption of vitamin A (no, yes, and missing), mother’s age at child’s birth (years) (<19, 20–24, 25–30, and 30+), mother’s education (no education, primary, secondary, and higher), mother’s nutritional status (normal, underweight, overweight, obese, and other), antenatal care during pregnancy (0, 1–3, 4+, and missing), social groups (scheduled tribe, scheduled caste, other backward class, and other castes), and religion (Hindu, Islam, and other). Wealth index (poorest, poorer, middle, richer, and richest) and area of residence (urban and rural) were selected at the household level. The wealth index is used to measure the household’s socioeconomic status in NFHS and similar surveys; the details of the wealth index can be found in the NFHS report (IIPS and ICF 2015–2016).
2.3 Statistical Analyses
The univariate , bivariate, and multivariate statistical analyses were carried out for this study. The univariate descriptive statistics have been computed to understand the sample characteristics. The percentage of stunted children has been estimated for showing the prevalence of stunting across different socioeconomic, demographic, and regional factors. The binary logistic regression model has been applied to examine the determinants of stunting prevalence in India and Bihar. For the estimation of prevalence and correlates of stunting in Bihar, we used state-level wealth quintiles and state weights to account the state-level heterogeneity and poverty level. A comparison in childhood growth for age has been made between WHO standard and the evidence from Bhagalpur District of Bihar. The WHO growth standard for height for age is a standard for the linear growth of children constructed based on height for 0–24 months’ children and 25–60 months’ children. Further, LMS-based methods used to merge both age groups to model for the whole age range (0–60 months of children) and power transformation of age applied to stretch the age scale (WHO 2006). For the data analyses, the STATA 15.1 software was used .
3 Results
3.1 Sample Characteristics
Table 13.1 presents the sample characteristics of the children under the age of 5 by background characteristics in India and Bihar (2015–2016). Our study included a total of 225,002 births in India and 22,275 births in Bihar which took place in the last 5 years before 2015–2016. Overall, the percentage distribution of children under the age of 5 had a similar distribution in India and Bihar across sociodemographic characteristics. Almost half (48%) of which were female, and 42% of the sample at the national level reported to breastfeed immediately. More than one-third (38%) of these births were first in order, and 14% were four or more in order. Approximately half (46%) of the mothers were between 20 and 24 years of age, with normal nutritional status (52%), and three-fourths (76%) residing in rural areas. The highest education attended by most (46%) of the mothers was secondary education. Almost four in five mothers (78%) belong to the Hindu religion, and 44% belong to the other backward caste, while 24% belong to other or general caste. The majority (39%) of mothers received four or more antenatal care during pregnancy. Among the sample births, 66% of the children’s stool is disposed in an unsafe way, while 55% of the children’s mothers consume vitamin A during pregnancy. Almost half of the children lived in households with poor socioeconomic status.
3.2 Prevalence of Stunting
The prevalence of stunting in children under the age of 5 by selected socioeconomic and background characteristics is presented in Table 13.2 for both India and Bihar (2015–2016). The prevalence of stunting was compared between India and Bihar by different background characteristics. Overall, at the national level, almost two in five children are stunted (38%), whereas in Bihar almost half of the children were stunted (48%). The prevalence of stunting in children varies significantly with socioeconomic characteristics in both India and Bihar. In both India and Bihar, the prevalence of stunting was significantly higher in children who were aged 36–47 months, four and above birth order, breastfed within 1 hour of birth, and practicing unsafe stool disposal and whose mother is underweight, had no antenatal care during pregnancy, aged less than 18 years, had no education, belong to the poorest wealth quintiles , and lived in rural areas.
The result suggests that there is over 10% difference in stunting prevalence between India and Bihar, among mothers who consume vitamin A tablet, mothers’ practices of safe disposal of children’s stool, mothers’ delivery of the baby in age 25–30 years, and mothers who belong to the scheduled caste and poorer, middle and richer wealth quintiles. There is also a significant difference over 20–30% observed by the age of the child, mother’s educational level, and wealth quintiles and over 10% by the area of residence and social groups in both India and Bihar. The results show that the prevalence of stunting is 10% higher in Bihar than the national level. The bivariate analysis shows a significant difference, almost on an average of 5–10%, in the prevalence of stunting across the background characteristics in both India and Bihar level. Among the children under the age of 6 months, there is a difference of 1% in stunting prevalence between India and Bihar; it increased with an increase in the age of children and reached the highest difference of 13% at age 36–59 months. Among the mothers who breastfeed their child immediately among them, there is a difference of 11% in stunting prevalence, and it reduces to 9% among those who breastfeed after an hour. Concerning the birth order of the children, the result shows that prevalence of stunting increase with an increase in birth order in India and Bihar as well. The difference in stunting prevalence among the first and four and above birth order is 17% in India and 9% in Bihar.
3.3 Determinants of Childhood Stunting
Table 13.3 displays the determinants of stunting using binary logistic regression for both India and Bihar, respectively. The prevalence of stunting was compared between India and Bihar with different background characteristics. Furthermore, the prevalence of stunting among the different background characteristics was compared separately for India and Bihar. At the India level, the child is strongly linked to the probability of being stunted by increasing age. Children aged 36–47 months are three times more likely (OR: 3.08, 95% CI: 2.95–3.22) to be stunted than children aged 0–5 months. Children whose mothers were less educated were more likely to be stunted than their counterparts (OR: 1.68, 95% CI: 1.68–1.76); similarly, if the child’s mother was underweight, they were more likely to be stunted (OR: 1.25, 95% CI: 1.22–1.28). The result also indicats that mother’s social group and socioeconomic status linked strongly with odds of child stunting, and children from scheduled caste more likely to be stunted with an odd of 1.33 (95% CI: 1.29–1.37) as well as children who belonged to the poorest households (OR: 1.95, 95% CI: 1.87–2.04).
The odds of childhood stunting is significantly varied across the background characteristics in both India and Bihar. The odds of stunting were significantly higher among older children, children of higher birth order, and children practicing unsafe disposal of stool. Similarly, both in India and Bihar, significantly higher odds of stunting were found among children whose mothers were less than 19 years of age during the childbirth, had no education, were underweight, had no antenatal care visits during pregnancy, belong to the scheduled caste and tribe groups, follow Islam religion, and belong to the poor economic status than their counterparts. The significant difference in the probability of stunting is found by the age of the child, mother’s educational level, social group, and wealth status. The sex of the child, diarrhea status, consumption of vitamin A, antenatal care during pregnancy, and place of residence are not significantly associated with stunting prevalence in Bihar.
3.4 Child Growth in Bhagalpur District
Figure 13.1 shows the comparison in child growth between the WHO growth standard and Bhagalpur District of Bihar separately for boys and girls. During the infancy phase (0–12 months), the child growth of the Bhagalpur District almost followed the WHO growth standards both for boys and girls. However, there was a decline in the height for age after 12 months onwards of the child’s age in Bhagalpur District in comparison to WHO growth standard showing prevailing stunting among boys and girls till late childhood. For the boys between the ages of 20 and 35 months, the height was shorter than girls compared to WHO growth standards.
A comparison in child growth between WHO standard and the sample from Bhagalpur District of Bihar (2019). Note: World Health Organization’s child growth standard (WHO 2006)
4 Discussion
Childhood growth is an acute problem in India. The latest estimate from NFHS-4 suggests that almost two in five children are stunted (38%) at the national level in 2015–2016, whereas every second child in Bihar is stunted (48%) (IIPS and ICF 2017). The findings from this study indicate that the demographic factors such as child’s age, mothers’ age at childbirth, and birth order; social factors like mothers’ education, place of residence, and religion; economic factors, i.e., wealth quintiles; and other mother-related factors such as mothers’ height and weight and access to the maternity care affect the likelihood of childhood stunting in India and Bihar. The risk of child stunting is higher in Bihar than the national average for the majority of the socioeconomic and demographic factors, which implies the disadvantageous position of Bihar. The evidence from Bhagalpur, an eastern district of Bihar, shows that as the age of the children increases, the likelihood of child stunting increases.
Our finding indicates the significant differences in the prevalence of stunting across the demographic factors such as child’s age and birth order in both Bihar and national levels. Children’s age is a cabalistic predictor of childhood stunting. This finding is consistent with many previous studies. As child’s age increases, the risk of being stunted increased (Kamal 2011; Rakotomanana et al. 2017; Ntenda and Chuang 2018; Gebru et al. 2019). In our study, we found that children who were aged 36–47 months have a significantly higher prevalence of stunting in both India and Bihar. However, the effects of child’s age on stunting in Bihar are higher than the national average. The study also confirmed that multiple birth order and childhood stunting were found statistically significant for both India and Bihar. Multiple birth order involves child defects like shrunk, low weight, premature birth, and cerebral paralysis which can suppress child growth (WHO 2006; Magadi 2011; Adekanmbi et al. 2013). The significant difference has been found in the first birth order in stunting prevalence between India and Bihar. On the other hand, the difference of multiple birth order in stunting prevalence is very insignificant between India and Bihar. This study finds that mothers whose age was less than 19 years at the time of delivery have a high risk of stunting among their children than mothers whose age was above 20 years at the time of delivery for both Bihar and India levels. Similar findings were found in the previous studies (Kismul et al. 2018; Fall et al. 2015). A higher risk of childhood stunting in Bihar for these demographic factors indicates that Bihar suffers the disadvantageous situation in terms of early age at marriage, early age at childbearing, and high birth order which call for family planning program interventions.
Social determinants such as mothers’ education, religion, and place of residence have significant effects on child stunting in India and Bihar. The inverse relationship between mothers’ level of education and childhood stunting is found in both India and Bihar. A similar finding was also reported by Gebru et al. (2019). Women from highly educated households and high wealth quintile households have less stunted children (Kimani et al. 2015; Frost et al. 2005). Our results indicate that children who reside in urban areas are less prevalent of stunting than rural areas for both India and Bihar. A similar pattern was also found in low-income and middle-income countries (Paciorek et al. 2013). This study also demonstrated that the prevalence of childhood stunting is higher among those who follow Islam compared to other religions in both India and Bihar. A similar result was found in Bangladesh (Levay et al. 2013; Mkandawire and Hendriks 2018). This might be due to poor socioeconomic status of Muslim households (Chowdhury et al. 2016). By all the social factors, the likelihood of child stunting is higher in Bihar than the national average, possibly because of social backwardness and economic disadvantage, especially in education and ruralization of the population in Bihar.
The economic factors play a crucial role in childhood stunting. The findings from this study demonstrated that there is a strong positive association between wealth quintiles and child stunting for both India and Bihar. Children from the poorest wealth quintiles had higher odd of stunting than the wealthiest quintiles. The degree of difference is higher in Bihar than the national average. This finding is consistent with previous studies (Semba et al. 2008; Hong and Hong 2007).
Other mother-level factors such as mothers’ height and weight and access to maternity care for the child are also important predictors for the childhood stunting in both India and Bihar. The findings reflect on the mother’s height for childhood stunting (Singh et al. 2017). The effect of the mother’s height on childhood stunting is due to genetic transfers and endowments (Bosch et al. 2008; Subramanian et al. 2009; Özaltin et al. 2010). Our study showed that children whose mothers are underweight had higher odds of childhood stunting than the normal mother for both India and Bihar (Teshome et al. 2009). Moreover, findings indicate that mothers who had no antenatal care during pregnancy have a higher prevalence for both India and Bihar. Another key result is the age of the mother for childhood stunting for the State of Bihar and the national level.
In this study, the evidence from Bhagalpur District on child growth showed that child’s height for age in early childhood aligned with the WHO standards. However, we found that from the end of the infancy to late childhood, the likelihood of stunting increases in the Bhagalpur District. Our study revealed the evidence of children’s age in the change of child growth. The possible explanation for such a situation from Bhagalpur District on child growth may be the impact of dietary pattern change with age, which might play a complex role in the nexus of dietary intake, food security, and economic status. Studies had found that during the infancy, children are more dependent on the breastfeeding along with other food intakes that positively influence the children’s growth conditions (Syeda et al. 2020; Muldiasman et al. 2018). It is important to consider the dietary practice and children age as increase in the age of the children, specifically during the mid-childhood, the introduction of semi-solid and solid food is essential for the overall growth of children. Perhaps the insufficient supplementary food during childhood elevates the risk of childhood stunting in Bhagalpur. Previous researches have also shown that if children do not have considerable protein and carbohydrate in their dietary practices, they are more likely to be stunted (Esfarjani et al. 2013; Krasevec et al. 2017). As per the NFHS-4 report (2015), about 46.6% of children aged under 5 years were stunted in Bhagalpur District, and almost 55% of mothers were illiterate. Mothers’ educational status was found to affect the children’s nutritional status. Educated mothers were more concerned and aware of the children’s dietary and health conditions than uneducated mothers (Mzumara et al. 2018; Nshimyiryo et al. 2019). On the other hand, household wealth status also has a significant effect on child’s nutritional status because poor households may distribute a low per capita food availability (Howe et al. 2009; Boyle et al. 2006). Similarly, earlier studies have also shown that children from the poorest wealth status household were having substantially higher stunting (Tiwari et al. 2014; Habimana and Biracyaza 2019).
The study was based on the DHS data, a cross-sectional survey that only provides a snapshot of children stunting in Bihar. Using cross-sectional data, the causal relationship between two variables is not possible. Child growth trajectory from Bhagalpur District needs a cohort data. Further study is recommended for conducting a cohort study for understanding child growth trajectories. However, we have tried to assess the factors determining childhood stunting in India and Bihar.
In conclusion, our study highlighted the differences among the determinants of childhood stunting between samples from the whole of India and Bihar. In addition, the evidence from the Bhagalpur District, an eastern district of Bihar, has shown the insightful findings. The major implications of the findings of this study are the following: First, demographic disadvantages, i.e., early marriage and early childbearing, lower use of contraceptive methods, and resultant higher fertility rate, are the major demographic drivers of childhood stunting. Family planning should be promoted, and the age of marriage needs to be raised in the State of Bihar. Second, Bihar is one of the resource-poor states of India that also has educational underdevelopment. These drawbacks of the state hold the progress in reducing the prevalence of childhood stunting. Hence, awareness on child-feeding practices and provision of supplementary foods need to be ensured in the state. Third, along with the samples from India and Bihar, the evidence from Bhagalpur also confirms that as the age of the children increases, the risk of childhood stunting also elevates. This finding indicates that strengthened child care and supplementary food are required for the middle-aged and relatively older children. Summarily, the findings from the present study will help in the development of potential interventions and actions associated with mothers’ role in children’s malnutrition at the state level in Bihar and Bhagalpur District. Thus, with effective policy and program interventions and keeping the findings into consideration, childhood stunting may be reduced to achieve the Sustainable Development Goals by 2030 in Bihar as well as India.
References
Adekanmbi VT, Kayode GA, Uthman OA (2013) Individual and contextual factors associated with childhood stunting in Nigeria: a multilevel analysis. Maternal & child nutrition 9(2):244-259
Banerjee K, Dwivedi LK, Ranjan M (2017) Spatio-temporal trends in malnourishment clustering among under-five siblings from 1992 to 2016: the Indian paradox. In 2017 International Population Conference, IUSSP
Bosch AM, Baqui AH, van Ginneken JK (2008) Early-life determinants of stunted adolescent girls and boys in Matlab, Bangladesh. Journal of health, population, and nutrition 26(2):189
Boyle MH, Racine Y, Georgiades K et al (2006) The influence of economic development level, household wealth and maternal education on child health in the developing world. Social science & medicine 63(8): 2242-2254
Bozzoli C, Deaton A, Quintana-Domeque C (2009) Adult height and childhood disease. Demography 46(4):647-669.
Chowdhury MRK, Rahman MS, Khan MMH et al (2016) Risk factors for child malnutrition in Bangladesh: a multilevel analysis of a nationwide population-based survey. The Journal of paediatrics 172:194-201
Esfarjani F, Roustaee R, Mohammadi-Nasrabadi F et al (2013) Major dietary patterns in relation to stunting among children in Tehran, Iran. Journal of health, population, and nutrition 31(2):202
Fall CH, Sachdev HS, Osmond C et al (2015) Association between maternal age at childbirth and child and adult outcomes in the offspring: a prospective study in five low-income and middle-income countries (COHORTS collaboration). The Lancet Global Health 3(7):e366-e377.
Fenske N, Burns J, Hothorn T et al (2013) Understanding Child Stunting in India: A Comprehensive Analysis of Socioeconomic, Nutritional and Environmental Determinants Using Additive Quantile Regression. PLoS One8(11): e78692
Frongillo Jr EA, de Onis M, Hanson KM (1997) Socioeconomic and demographic factors are associated with worldwide patterns of stunting and wasting of children. The Journal of nutrition 127(12):2302-2309
Frost MB, Forste R, Haas DW (2005) Maternal education and child nutritional status in Bolivia: finding the links. Social science & medicine 60(2):395-407
Gebru KF, Haileselassie WM, Temesgen AH et al (2019) Determinants of stunting among under-five children in Ethiopia: a multilevel mixed-effects analysis of 2016 Ethiopian demographic and health survey data. BMC paediatrics 19(1):176
Grantham-McGregor, S. M., Powell, C. A., Walker, S. P., & Himes, J. H. (1991). Nutritional supplementation, psychosocial stimulation, and mental development of stunted children: the Jamaican Study. The Lancet, 338(8758), 1-5.
Habimana S, Biracyaza E (2019) Risk Factors Of Stunting Among Children Under 5 Years Of Age In The Eastern And Western Provinces Of Rwanda: Analysis Of Rwanda Demographic And Health Survey 2014/2015. Pediatric Health, Medicine and Therapeutics 10:115
Hong R, Hong R (2007) Economic inequality and undernutrition in women: multilevel analysis of individual, household, and community levels in Cambodia. Food and Nutrition Bulletin 28(1):59-66
Howe LD, Hargreaves JR, Gabrysch S et al (2009) Is the wealth index a proxy for consumption expenditure? A systematic review. Journal of Epidemiology & Community Health 63(11):871-877
International Institute for Population Sciences [IIPS] and ICF (2017) National Family Health Survey (NFHS-4), 2015-16.Mumbai, India
Jena P, Rath S, Nayak MK et al (2019) Study of social and demographic determinants of severe acute malnutrition in children aged 6-59 months in a tertiary care centre of Odisha, India. International Journal of Contemporary Pediatrics 6(1):46-51
Kamal SM (2011) Socioeconomic determinants of severe and moderate stunting among under-five children of rural Bangladesh. Malaysian journal of nutrition 17(1)
Kanjilal B, Mazumdar PG, Mukherjee M et al (2010) Nutritional status of children in India: household socioeconomic condition as the contextual determinant. International Journal for equity in health 9(1):19
Khadse RP, Chaurasia H (2020) Nutrition status and inequality among children in different geographical regions of Maharashtra, India. Clinical Epidemiology and Global Health8(1):128-137
Khan J, Mohanty SK (2018) Spatial heterogeneity and correlates of child malnutrition in districts of India. BMC public health 18(1):1027
Kimani-Murage EW, Muthuri SK, Oti SO et al (2015) Evidence of a double burden of malnutrition in urban poor settings in Nairobi, Kenya. PloS one 10(6):e0129943
Kismul H, Acharya P, Mapatano MA et al (2018) Determinants of childhood stunting in the Democratic Republic of Congo: further analysis of Demographic and Health Survey 2013–13. BMC public health 18(1):74
Krasevec J, An X, Kumapley R et al (2017) Diet quality and risk of stunting among infants and young children in low-and middle-income countries. Maternal & child nutrition 13:e12430
Krishna A, Mejía-Guevara I, McGovern M et al (2018) Trends in inequalities in child stunting in South Asia. Maternal & child nutrition14:e12517
Kumar A, Kamath VG, Kamath A et al (2010) Nutritional status assessment of under-five beneficiaries of Integrated Child Development Services program in rural Karnataka. AMJ 3(8):495–8
Levay AV, Mumtaz Z, Rashid SF et al (2013) Influence of gender roles and rising food prices on poor, pregnant women's eating and food provisioning practices in Dhaka, Bangladesh. Reproductive Health 10(1):1-11
Liou L, Kim R, Subramanian SV (2020) Identifying geospatial patterns in wealth disparity in child malnutrition across 640 districts in India. SSM-population health 10:100524
Magadi MA (2011) Household and community HIV/AIDS status and child malnutrition in sub-Saharan Africa: evidence from the demographic and health surveys. Social science & medicine 73(3):436-446
Meenakshi JV (2016) Trends and patterns in the triple burden of malnutrition in India. Agricultural Economics 47(S1):115-134
Mkandawire E, Hendriks SL (2018) A qualitative analysis of men's involvement in maternal and child health as a policy intervention in rural Central Malawi. BMC pregnancy and childbirth 18(1):1-12
Muldiasman M, Kusharisupeni K, Laksminingsih E et al (2018) Can early initiation to breastfeeding prevent stunting in 6–59 months old children? Journal of Health Research
Mzumara B, Bwembya P, Halwiindi H et al (2018) Factors associated with stunting among children below five years of age in Zambia: evidence from the 2014 Zambia demographic and health survey. BMC nutrition 4(1):51
Nie P, Rammohan A, Gwozdz W et al (2019) Changes in child nutrition in India: A decomposition approach. International journal of environmental research and public health 16(10):1815
Nshimyiryo A, Hedt-Gauthier B, Mutaganzwa C et al (2019) Risk factors for stunting among children under five years: a cross-sectional population-based study in Rwanda using the 2015 Demographic and Health Survey. BMC public health 19(1):1-10
Ntenda PAM, Chuang YC (2018) Analysis of individual-level and community-level effects on childhood undernutrition in Malawi. Pediatrics & Neonatology 59(4):380-389
Özaltin E, Hill K, Subramanian SV (2010) Association of maternal stature with offspring mortality, underweight, and stunting in low-to middle-income countries. Jama 303(15): 1507-1516.
Paciorek CJ, Stevens GA, Finucane MM et al (2013) Children’s height and weight in rural and urban populations in low-income and middle-income countries: a systematic analysis of population-representative data. The Lancet Global Health1(5):e300-e309
Pathak PK, Singh A (2011) Trends in malnutrition among children in India: growing inequalities across different economic groups. Social science & medicine 73(4):576-585
Rakotomanana H, Gates GE, Hildebrand D et al (2017) Determinants of stunting in children under 5 years in Madagascar. Maternal & child nutrition 13(4):e12409
Rana MJ, Goli S (2018) Does planning of births affect childhood undernutrition? Evidence from demographic and health surveys of selected South Asian countries. Nutrition 47: 90-96.
Rana MJ, Gautam A, Goli S et al (2019) Planning of births and maternal, child health, and nutritional outcomes: recent evidence from India. public health 169:14-25
Rengma MS, Sen J, Mondal N(2015) Socio-Economic, Demographic and Lifestyle Determinants of Overweight and Obesity among Adults of Northeast India. Ethiop J Health Sci 25:199–208
Akhtar S (2016) Malnutrition in South Asia-A Critical Reappraisal. Critical Reviews in Food Science and Nutrition 56(14) 2320-2330, doi: https://doi.org/10.1080/10408398.2013.832143
Semba RD, de Pee S, Sun K et al (2008) Effect of parental formal education on risk of child stunting in Indonesia and Bangladesh: a cross-sectional study. The lancet 371(9609): 322-328
Sharma A (2019) Trends & Patterns of Child Malnutrition in India: A Disaggregated Analysis. Indian Journal of Industrial Relations 55(1)
Singh A, Upadhyay AK, Kumar K (2017) Birth size, stunting and recovery from stunting in Andhra Pradesh, India: evidence from the Young Lives Study. Maternal and child health journal 21(3):492-508
Singh R, Rao S, Charlette L et al (2018) Socio-demographic correlates of stunting among children in Port Blair, India. International Journal of Community Medicine and Public Health 5(10):4231
Singh S, Srivastava S, Upadhyay AK (2019) Socioeconomic inequality in malnutrition among children in India: an analysis of 640 districts from National Family Health Survey (2015–16). International Journal for Equity in Health 18(1):203
Subramanian SV, Ackerson LK, Smith GD et al (2009) Association of maternal height with child mortality, anthropometric failure, and anemia in India. Jama 301(16):1691-1701
Sultana P, Rahman MM, Akter J (2019) Correlates of stunting among under-five children in Bangladesh: a multilevel approach. BMC nutrition 5(1):41
Syeda B, Agho K, Wilson L et al (2020) Relationship between breastfeeding duration and undernutrition conditions among children aged 0–3 Years in Pakistan. International Journal of Pediatrics and Adolescent Medicine
Teshome B, Kogi-Makau W, Getahun Z et al (2009) Magnitude and determinants of stunting in children under five years of age in food surplus region of Ethiopia: the case of West Gojjam zone. Ethiopian Journal of Health Development 23(2)
Tiwari R, Ausman LM, Agho KE (2014) Determinants of stunting and severe stunting among under-fives: evidence from the 2011 Nepal Demographic and Health Survey. BMC paediatrics 14(1):239
UNICEF (2014) Levels and trends in child mortality: report 2013. United Nations Children's Fund, New York URL: https://www.unicef.org/media/files/Levels_and_Trends_in_Child_Mortality_2013.pdf
Walker, S. P., Chang, S. M., Powell, C. A., Simonoff, E., & Grantham-McGregor, S. M. (2007). Early childhood stunting is associated with poor psychological functioning in late adolescence and effects are reduced by psychosocial stimulation. The Journal of nutrition, 137(11), 2464-2469.
World Health Organization (2006) WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age: methods and development. World Health Organization
World Health Organization (2020) UNICEF/WHO/The World Bank Group joint child malnutrition estimates: levels and trends in child malnutrition: key findings of the 2020 edition.
World Health Organization (2007) WHO multicentre growth reference study group: WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age: methods and development. WHO, Geneva
Young MF, Mehta R, Larson L et al (2016) Poor Child Feeding Practices and Malnutrition in Bihar, India. The FASEB Journal 30:1149-20
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Ajmer, S., Islam, S., Rana, M.J., Rahaman, M., Hossain, M., Hossain, B. (2021). Determinants of Childhood Stunting in India: Comparative Evidence from Bihar. In: Rukhsana, Alam, A. (eds) Agriculture, Food and Nutrition Security. Springer, Cham. https://doi.org/10.1007/978-3-030-69333-6_13
Download citation
DOI: https://doi.org/10.1007/978-3-030-69333-6_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-69332-9
Online ISBN: 978-3-030-69333-6
eBook Packages: Earth and Environmental ScienceEarth and Environmental Science (R0)