Abstract
Since December 2019, a novel coronavirus called severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has begun to infect people. The virus first occurred in Wuhan, China, but the whole world is now struggling with the pandemic. Over 13 million confirmed cases and 571,000 deaths have been reported so far, and this number is growing. Older people, who constitute a notable proportion of the world population, are at an increased risk of infection because of altered immunity and chronic comorbidities. Thus, appropriate health care is necessary to control fatalities and spread of the disease in this specific population. The chapter provides an overview of diagnostic methods, laboratory and imaging findings, clinical features, and management of COVID-19 in aged people. Possible mechanisms behind the behavior of SARS-CoV-2 in the elderly include immunosenescence and related impaired antiviral immunity, mature immunity and related hyper-inflammatory responses, comorbidities and their effects on the functioning of critical organs/systems, and the altered expression of angiotensin-converting enzyme 2 (ACE2) that acts as an entry receptor for SARS-CoV-2. This evidence defines the herding behavior of COVID-19 in relation to ACE2 under the influence of immune dysregulation. Then, identifying the immunogenetic factors that affect the disease susceptibility and severity and as well as key inflammatory pathways that have the potential to serve as therapeutic targets needs to remain an active area of research.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
13.1 Introduction
While humanity was ever proud of his superheroic facilities, a little virus, distinguished first in Wuhan, China, could have fatal effects on the global economy, diplomacy, and especially social life. In December 2019, Chinese health authorities reported pneumonia of unknown origin associated with an exposure to a seafood market in some cases (Rabi et al. 2020). The causative pathogen was unknown, so researchers started to investigate its origin, reservoir, and suspected intermediate hosts. Investigations revealed that the viral genome sequences share about 80% similarity to that of severe acute respiratory syndrome coronavirus (SARS-CoV). The virus was then called SARS-CoV-2, and the disease caused by this virus was named coronavirus disease 2019 (COVID-19) (Zhou et al. 2020; Gorbalenya et al. 2020; Rabi et al. 2020). Over the last 6 months, this novel coronavirus has continued to infect people with a great contagion over the boundaries, with more than 13 million confirmed cases as of July 13, 2020.
SARS-CoV and SARS-CoV-2 belong to the Coronaviridae family (Coronavirinae subfamily), possessing spikes on the superficial part and positive-stranded RNA in the central part (Coronaviridae—Positive Sense RNA Viruses—Positive Sense RNA Viruses. 2011). Coronavirinae subfamily contains four main genera: Alphacoronavirus, Betacoronavirus, Gammacoronavirus, and Deltacoronavirus. Gammacoronaviruses and deltacoronaviruses occur in pigs and birds, while alphacoronaviruses and betacoronaviruses are detected in mammals (Coronaviridae—Positive Sense RNA Viruses—Positive Sense RNA Viruses. 2011; Velavan and Meyer 2020). The history of coronaviruses dates back to 54 years ago when the virus was isolated from nasal washing specimens of patients with the common cold (Tyrrell and Bynoe 1966). Until this day, seven types of coronaviruses have been discovered with the ability to infect humans, among which the natural reservoir of five types are probably bats (Cui et al. 2019). From these seven types, four types, including human coronavirus (HCoV)-NL63, HCoV-229E, HCoV-OC43, and HCoV-HKU1, mainly cause the common cold, and three others, including the Middle East respiratory syndrome coronavirus (MERS-CoV), SARS-CoV, and SARS-CoV-2, can represent with fatal pneumonia (Yang et al. 2020; Su et al. 2016; Zhu et al. 2020). SARS-CoV-2 siblings, e.g., MERS-CoV and SARS-CoV, mainly involve the respiratory system and could cause horrifying outbreaks with massive mortality during the past two decades (Hanaei and Rezaei 2020; Jabbari et al. 2020).
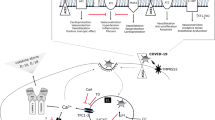
Detection of the origin, hosts, and transmission routes of the virus can help to stop the virus from spreading and infecting more people. Further investigations found that the SARS-CoV-2 genome shares a 96% similarity with bat-CoV (Zhou et al. 2020) and put forward pangolins as the intermediate host of SARS-CoV-2 because of more than 90% concordance of pangolin-CoV genome with both bat-CoV and SARS-CoV-2 (Zhang et al. 2020). SARS-CoV-2 transmission mainly occurs through human-to-human contact by inhaling droplets and aerosols (Lotfi et al. 2020). Current evidence suggests the angiotensin-converting enzyme 2 (ACE2) as a cell surface receptor for the virus (Wilder-Smith and Freedman 2020; Wilson and Chen 2020; Sharifkashani et al. 2020; Rezaei 2020b) and the immune responses as the source of variability in the vulnerability of people to infection (Saghazadeh and Rezaei 2020a; Yazdanpanah et al. 2020a; Bahrami et al. 2020; Lotfi and Rezaei 2020; Nasab et al. 2020). Older adults are a high-risk group to this infection as they have an immune system with a decreased ability to fight with infectious diseases (Huang et al. 2020). It is important to notice the clinical features of the disease in aged patients to reduce total mortality.
13.2 Elderlies: Too Frail for COVID-19
Geriatrics is a medical subspecialty aimed at providing health care for old patients. The elderly can be defined in different ways, though it mainly applies to people aged 65 years or over (Orimo et al. 2006; Singh and Bajorek 2014; (WHO) 2002), and that some divide old ages into early elderly (65–74 years old) and late elderly (75 years and older). The World Health Organization (WHO) claims that the world’s population is going to be old very soon and that the percentage of the people with the age of 60 or more would surpass the 22% of the whole population by 2050 ((WHO) Updated May 2017).
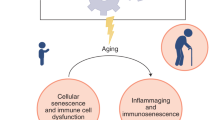
Children are different from adults in the risk of developing and dying from COVID-19. Studies show that only 2% of cases with confirmed COVID19 are in the age group 0–19 years (Wu and McGoogan 2020). About 15% of patients over age 80 die. Also, patients with severe COVID-19 are older than patients with non-severe COVID-19 (Wang et al. 2020a). Therefore, children and the elderly have high contrast in the behavior of COVID19 (Figs. 13.1 and 13.2). Below are about possible mechanisms behind this behavior of COVID-19.
13.2.1 The Aged Immune System
The human body is a multiphysiological system, and all of its systems would be affected by the aging process, including the immune system, which has an essential role in fighting with infection. The impact of aging on the immune system, which is referred to as immunosenescence, involves both innate and adaptive immunity (Nikolich-Zugich 2018; Fuentes et al. 2017; Wong and Goldstein 2013) and extends over the skin and mucosal immune system (Lichterfeld-Kottner et al. 2020).
Aging-associated changes in in the immune system include, but are not limited to, the acquisition of old cells in the immune system and other organs/systems, reduction in naïve T cells releasing from the thymus, mRNA processing changes, and dysregulation of immune receptors (Pietilä et al. 2015; Walford 1964; Fuentes et al. 2017). Natural killer cells (NK Cells) are an essential member of the innate immune system that play a significant role not only in eliminating malignant cells but also removing cells infected with viruses. They are affected by aging, as indicated by decreased expression of activating receptors and CD56 marker on their surface (Baume et al. 1992; Carson et al. 1997; Saito et al. 1993). Similarly, as we get older, T cells undergo reductions in their number, function, and surface receptors. Inevitably, the ability of these cells to recognize infectious or tumoral cells would also be impaired (Larbi et al. 2006, 2014; Vallejo 2005).
On the other hand, COVID-19 itself would influence the immune system. It has been shown to decrease T cell numbers and that this might be related to disease severity and adverse outcomes of disease (Qin et al. 2020; Fathi and Rezaei 2020b). NK cells are also reduced in the count and cytotoxic function during this infection (Yaqinuddin and Kashir 2020). Given that hyper-inflammation in COVID-19 is a strong predictor of poor outcomes, inflamm-aging, known as a baseline subclinical mild chronic inflammation produced by aging, can also worsen the outcome of COVID-19 (Bonafè et al. 2020). Altogether, it is not surprising that COVID-19 can cause worst-case scenarios in the context of an aged immune system.
13.2.2 The Increased Risk of Chronic Diseases
The frailty of old patients is not only due to the old immune system. Aging is a significant risk factor for chronic diseases, including hypertension, cardiac diseases, cerebrovascular diseases, neurodegeneration, and cancer (Pawelec et al. 2014). Recent investigations have shown that SARS-CoV-2 could cause higher mortality or poorer prognosis in patients with comorbidities, in particular, hypertension, diabetes, and cardiovascular diseases, compared with patients without comorbidities (Guan et al. 2020; Chen et al. 2020a, 2020b; Singhal 2020; Grasselli et al. 2020; Du et al. 2020). Of note, hypertension is associated with about 2.5-fold increased risk of mortality related to COVID-19 (Lippi et al. 2020). Moreover, many elderlies deal with loneliness, which can lead to poor hygiene and neglect of disease symptoms at early stages and, therefore, presenting to hospitals with progressed manifestations. Also, living in care facilities would significantly affect person-to-person transmission.
13.2.3 The Mature Immunity
Generally speaking, T helper (Th) 2 cell and T regulatory (Treg) cell responses and Th17 cytokines decrease with age, whereas Th1 cell immune responses and pattern recognition receptor (PRR)-mediated signaling increase with age. In this manner, a sophisticated immune system, through the production of pro-inflammatory cytokines (IFNγ, TNFα, IL-2, IL-1β), leads to the recruitment of hyper-inflammatory immune responses under pathologic conditions. By contrast, an immature immune system induces hypo-inflammatory responses that are maintained by anti-inflammatory and immune-regulatory cytokines (IL-4, IL-5, IL-10, IL-13, IL-35, and TGFβ) and diminished PRR-mediated signaling. Due to decreased communication between the innate and adaptive immune system in the immature immune system, all responses generated from the adaptive immune system are declined, including T cell proliferation, cytotoxic T cell responses, memory T cells, and CD8+ T and CD4+ T cell activation (Maddux and Douglas 2015). Soluble factors known to maintain immune responses skewed to Th2 cell type come from both the maternal origin, e.g., TGFB, progesterone, and prostaglandin, and the child’s own origin, such as adenosine.
Dendritic cells (DCs) are professional myeloid cells that can detect pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs) released by invading pathogens or damaged cells and mediate their death through apoptosis, necrosis, or pyroptosis. Notably, DCs perform apoptosis of their own kind as being programmed. A decreased function of DCs in the clearance of apoptotic/necrotic DCs results in the accumulation of cells that should be dead but are alive, and this would cause critical conditions such as autoimmunity and tumorigenesis. Like mature DCs, immature DCs display the ability of up taking apoptotic/necrotic cells (Kushwah et al. 2010). The ability of immature DCs is, however, unique – whereas apoptotic cells are required inflammatory responses for being detectable by mature DCs, no evident inflammatory response is necessary for their recognition by immature DCs. Uptake of apoptotic DCs would be appropriate for immature DCs to be educated of a tolerogenic character, as indicated by increased expression of TGFβ that is a critical driver of Treg cell induction by naïve CD4+ T cells. More interestingly, cord DCs can, upon exposure to PAMPs, elicit immune responses compatible with those of adult DCs (Langrish et al. 2002). While due to the below-required expression of cytokines, IL12P70 and IFNY, inducing differentiation of naïve CD4+ T cells into Th2 cell dichotomy (Langrish et al. 2002), cord DCs are in an immaturity-enforcement capacity against the pro-inflammatory Th1 cell polarization.
A systematic review of cytokine expression in children has confirmed that the expression of pro-inflammatory cytokines, including IFNY, IL6, IL10, and TNFA, increases with age (Decker et al. 2017). A closer look at individual studies included in the review reveals to us an age-associated increase most being pronounced for the percentage of CD4+ T and CD8+ T cells that express IFNY and TNFA.
13.2.4 The Aberrant Expression of ACE2
13.2.4.1 ACE2: A Receptor for SARS-CoV2 (2019-nCoV) Cell Entry That Is Present on Lungs, Heart, Kidney, and Testis
An insufficient response to classical angiotensin-converting enzyme (ACE) inhibitors among patients with hypertension and cardiovascular diseases posed the possibility that the target may be wrong, i.e., ACE. Efforts led to the recognition of ACE2 (angiotensin-converting enzyme 2) that acts as a human carboxypeptidase that utilizes zinc. The lack of or deficiency of ACE2 correlates with diabetic nephropathy, heart dysfunction, and reduced cardiac contractility and accumulation of angiotensin II and hypoxia-induced genes (Guy et al. 2003).
ACE2 is primarily present on specific tissue like renal, cardiac, and testicular tissue. Besides, its expression exists in other tissue like the liver, lung, pancreas, ovary, colon, small intestine, placenta, and retina (Bindom and Lazartigues 2009). Thereby, ACE2 can ubiquitously exert anti-fibrotic and anti-inflammatory effects through the degradation of its primary substrate, angiotensin II, and also by inhibition of TGFB and MIF (Bindom and Lazartigues 2009). However, ACE2 can mediate the degradation of different substrates, as shown in Fig. 13.3.
Antiserum that contains antibodies against human ACE2 could hinder the entry of pseudotyped SARS-2-S. It supports the notion that SARS-2-S utilizes ACE2 as an entry receptor (Hoffmann et al. 2020).
13.2.4.2 Dual-Function ACE2: Zinc Metalloproteinase and Microbial Collagenase
ACE2 and ACE share 42% sequence identity and 61% sequence conservation around the active site (Guy et al. 2003). Sequence alignment has confirmed that ACE2 possesses an active site with high similarity to that of testicular ACE (tACE), and therefore like other ACE family members, ACE2 can function as a zinc metalloproteinase (Guy et al. 2003). However, it dissociated tACE and ACE2 on a zinc ligand; for tACE, there is a third zinc ligand that occurs within the Glu-(Xaa)3-Asp motif, and for ACE2, the motif lacks the aspartate residue and has obtained a glutamate residue (Guy et al. 2003). This motif, Glu-(Xaa)3-Glu, allows ACE2 to function as a microbial collagenase (Guy et al. 2003).
Having a basic structure like ACE and on the other side having a zinc-binding motif (HEXXH) resembling the M32 family of peptidases have ranked ACE2 as the first mammalian carboxypeptidase structurally related to ACE, neurolysin, and PfuCP (Guy et al. 2003).
13.2.4.3 ACE2 Is Not Sensitive to ACEI
ACE2 functions as a carboxypeptidase that removes one single amino acid from the C terminus of its substrates, e.g., angiotensin I, angiotensin II, and des-Arg9-bradykinin. ACE is a peptidyl dipeptidase that removes a dipeptide from the C terminus of its substrates, angiotensin I and bradykinin, to reduce respective vasodilatory effects. Also, ACE2 and ACE differ in their ligand-binding pockets that mainly occur at the S2’ site (Guy et al. 2003).
13.2.4.4 ACE2 Exists in Membrane-Bound and Soluble Forms
ACE2 is a type I transmembrane protein having a long extracellular N-terminal domain and a short intracellular C-terminal tail. Its soluble form can interfere with ACE2 binding to the SARS-CoV spike protein. ADAM metallopeptidase domain 17, ADAM17, is a TNFA convertase that mediates ACE2 shedding in the soluble form (Lambert et al. 2005). However, ADAM17-mediated ACE2 cleavage does not influence SARS-CoV cell entry as TMPRSS2-mediated ACE2 cleavage did it significantly (Heurich et al. 2014).
13.2.4.5 ACE2 Expression Decreases with Age
The study of rats has confirmed the expression of ACE2 in the lungs, kidneys, heart, and the gastrointestinal system. For the lungs, the ACE2 expression occurs in both the bronchus and pulmonary parenchyma, alveolar type I epithelium, alveolar type II epithelium, bronchiolar epithelium, endothelium, and smooth muscle cells of the pulmonary vascular structure. The expression of ACE2 in the rat lungs significantly decreases with age, and that this decrease is relatively higher in males than females (Xudong et al. 2006). Both the elderly and the male population are at higher risk of dying from COVID-19 (Saghazadeh and Rezaei 2020a).
13.2.4.6 The Herding Behavior of COVID19 in Relation to ACE2 Under the Cytokine Storm
When a large number of people gather in the same event, a real concern arises regarding the risk of injury and death. For example, the event “2015 Mina stampede” occurred in Mina when people were performing the rites of Hajj. What that caused people to stampede is not apparent. Whatever the primary cause was, the movement of a large number of people led to a disaster associated with 769 deaths. Such behavior of people arising from a sudden fear is referred to as panic behavior. Statistical physicists developed several models for the prediction of human behavior in real crowds and led to the conclusion that individual-centered behavior, like collective behavior, would influence the optimization of the escape from the crowds (Helbing et al. 2000). Suppose a two-exit room filled with fire. A traditional fluid-flow model believes that people will be able to use both doors correctly and succeeded in exit safely. The individual-centered model predicts that a large number of people may leave the room using only one exit, resulting in the blocking of that exit, which is known as the herding behavior (Low 2000).
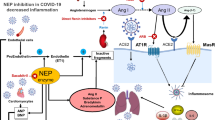
The SARS-CoV-2 enters the body. Upon its recognition, the immune system would elicit the cytokine storm in the peripheral blood. In a cytokine-filled body, the only optimal strategy is cell surface receptors through which the virus can enter the cell and escape the immune responses. Thus, the virus will find organs, e.g., exit doors, that express the highest density of ACE2 expression. The virus reaches the vital organs, lungs, heart, and kidney, and bind to transmembrane ACE2 as rapidly as possible as much as possible—reduction of functional ACE2, in turn, causes cardiac dysfunction, inflammation, and fibrosis.
The herding behavior of SARS-CoV-2 can explain the most prominent epidemic characteristics of COVID-19. Higher death rates among adults and older adults and patients with underlying conditions, e.g., cancer, diabetes, cardiovascular diseases, and hypertension, linked to limited or aberrant ACE2 expression, can be predicted by occupying ACE2 and blocking its function to the life-threatening extent. Children and young adults who have none of those, as mentioned earlier, conditions have a good repertoire of ACE2. Therefore, when the virus is occupying ACE2, there is a subset of ACE2 that remained functional. It would allow the immune responses to clear the viral infection effectively.
In this manner, the herding behavior of COVID-19 depends on the individual-centered factors, e.g., age and underlying condition, and collective behavior, e.g., the cytokine storm. Three main points of intervention are as follows: 1. hindering the virus binding to ACE2 throughout the disease course, 2. downregulation of cytokine release within the mild stage of the disease and before a severe stage of disease appears, and 3. upregulation of ACE2 expression during a severe stage of the disease to extend the deadline for immunity to act effectively.
13.3 COVID-19 in Aged Patients
History taking and physical examination are the keys in diagnosis, followed by laboratory testing and further paraclinical diagnostics. Understanding disease features is mandatory to diagnose disease in its earliest stages, thereby providing optimal health care and disease management. COVID-19 can manifest in a variety of forms, from a common cold to a severe form of disease like respiratory distress syndrome. Old ages (mostly aged 65 and over) and the presence of comorbidities crucially predict poor prognosis and an increased risk of mortality. The role of immunogenetic background is still under investigation in this regard (Babaha and Rezaei 2020; Darbeheshti and Rezaei 2020; Yousefzadegan and Rezaei 2020).
13.3.1 Clinical Features
The incubation period means the interval time from exposure to a virus source or infected people until the initiation of disease symptoms. It varies from about 1 day to 2 weeks, and the median incubation time is about 4 or 5 days (Xu et al. 2020a; Lauer et al. 2020; Nie et al. 2020). Overall, the most common symptoms of the disease are fever and cough (mostly dry cough). Fatigue, myalgia, shortness of breath, and dyspnea are also common among patients with COVID-19. Other symptoms can include conjunctival and nasal congestion, sore throat, chills, skin rashes, rhinorrhea, nausea or vomiting, sputum production, headache, diarrhea and hemoptysis, loss of smell sensation, loss of taste sensation, and altered mental status. Moreover, it must be noticed that asymptomatic patients have also been reported (Wang et al. 2020d; Lai et al. 2020; Breslin et al. 2020). Asking a history of exposure to symptomatic or suspicious patients or exposure to the Huanan seafood market would be useful.
In elderly patients, the disease does not include very different clinical manifestations from what is seen commonly. However, probably because of aging and its related comorbidities, these manifestations are more severe compared with younger adults. Besides, old patients may develop more atypical manifestations (Olde Rikkert et al. 2020); for example, in some cases, changes in mental status and orientation have been represented as initial symptoms of COVID-19 in aged patients (Wang et al. 2020c; Ward et al. 2020). Dyspnea, tachypnea, tachycardia, and chest discomfort may occur in elderlies (Nanda et al. 2020).
13.3.2 Laboratory Findings
Laboratory findings can be useful for predicting the prognosis and outcome of the disease. Although a significant number of patients can represent disease with normal laboratory data such as normal complete blood count, the following changes in laboratory data of patients might have been seen: abnormal white cell count, lymphocytopenia, low platelet count, hyponatremia, and increases in c-reactive protein (CRP), aminotransferases, erythrocyte sedimentation rate (ESR), lactate dehydrogenase (LDH), D-dimer, procalcitonin, creatine kinase, and IL-6. In addition to dyspnea and lymphocytopenia, high levels of CRP, ESR, LDH, and IL-6 might be predictive of developing severe or critical conditions.
13.3.3 Imaging Findings
Chest CT scan findings of patients may include ground-glass opacities (GGO), patchy infiltrations, consolidation, pleural effusion, pleural thickening, crazy-paving pattern, and interlobular septal thickening. It seems extensive pulmonary involvement occurs in elderlies more than younger patients.
13.3.4 Diagnosis
We can consider a person suspected to have COVID-19 when that person has had recent travel to Wuhan, China, or at least one of the people whom he is in close contact with, recently recognized as a confirmed case of COVID-19, begins to develop fever or common respiratory symptoms of COVID-19 or chest radiogram of pneumonia (Kim et al. 2020).
Confirmation of COVID-19 in a patient occurs when the pharyngeal swab specimen turns positive for real-time reverse transcription-polymerase chain reaction (RT-PCR) for the SARS-CoV-2 genome (Kim et al. 2020). However, because of probable false negatives for RT-PCR, it is better to repeat the test (Long et al. 2020). Moreover, a chest CT scan is a sensitive diagnostic method for early diagnosis (Wang et al. 2020b; Xu et al. 2020b). Elderlies with mild or uncommon symptoms of the disease can undergo diagnostic assessments for the virus (Nikolich-Zugich et al. 2020). Although immunoglobulins are not used for diagnosis of the disease, positive IgG antibody levels for SARS-CoV-2 can be highly suggestive for recent infection (Gosch et al. 2020). An active area of research is devoted to finding diagnostic methods for more rapid, reliable detection of SARS-CoV-2. Microfluidic devices offer promising platforms in this context (Basiri et al. 2020a).
13.3.5 Management
Overall, there is not a specific treatment or drug for COVID-19, and most of the treatments and care are supportive (Nikolich-Zugich et al. 2020). Considering complications related to altered mental status, such as falling, and underlying diseases is an essential factor to help manage the disease in elderlies. Conventional therapies are high-flow nasal oxygen, non-invasive positive-pressure ventilation, taking care of underlying illness and comorbidities, and treatment of co-infections. Routine use of corticosteroids is controversial (Saghazadeh and Rezaei 2020b); however, in severe cases, it may lead to a better outcome (Veronese et al. 2020). In patients with hypertension, the use of angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin-2 receptor blockers (ARBs) can lead to a better outcome (Meng et al. 2020). Patients with coagulopathy who undergo low molecular weight heparin may have better outcomes (Tang et al. 2020). The use of other drugs, such as antiretrovirals, is uncertain and may need further investigations (Ford et al. 2020). Considering respiratory rehabilitation may also be useful in the post-acute phase (Liu et al. 2020).
13.3.6 The Immune System, Inflammation, and Therapeutic Opportunities
Research shows that while the immune system is expected to elicit antiviral immune responses, the SARS-CoV-2 causes the immune system to induce pro-inflammatory signaling to the extent that the functioning of vital organs/systems, especially the central nervous system and the cardiovascular system, is impaired in the shocking production of these inflammatory cytokines (Bahrami et al. 2020; Jahanshahlu and Rezaei 2020a; Saleki et al. 2020; Yazdanpanah et al. 2020b). Moreover, immune cells having the responsibility of viral clearance show markers of exhaustion during the disease course. Therefore, there has been an increasing interest in identifying critical inflammatory targets and evaluating the adoptive transfer of immune cells as potential therapeutic opportunities (Fathi and Rezaei 2020a; Basiri et al. 2020b; Jahanshahlu and Rezaei 2020b; Mansourabadi et al. 2020; Pashaei and Rezaei 2020). However, the heavy burden of the pandemic (Rezaei 2020a) and the concern that it tends to stay (Jabbari and Rezaei 2020) have attracted much attention from other disciplines around the possible ways and means for prevention and management of the disease, too (Sahu et al. 2020; Moazzami et al. 2020; Rabiee et al. 2020; Mohamed et al. 2020; Momtazmanesh et al. 2020; Moradian et al. 2020).
13.4 Conclusion
Aging affects the immune system function, therefore increasing the risk of infection and adverse outcomes. Moreover, aging is a significant risk factor for chronic comorbidities that can put an aged person in a fragile state. Old patients with COVID-19 tend to develop severe illness and have a higher risk of death. They also are more likely to have abnormal laboratory findings and extensive pulmonary lesions. Old age and pre-existing chronic diseases such as hypertension, cardiovascular diseases, COPD, and diabetes can increase the risk of mortality. It is important to consider mild or atypical symptoms in the setup of an early diagnostic assessment of COVID-19 in an old patient. Monitoring and controlling underlying illness might help to have a better outcome in old patients with COVID-19.
References
(WHO) WHO (2002) Proposed working definition of an older person in Africa for the MDS Project. https://www.who.int/healthinfo/survey/ageingdefnolder/en/. Accessed May 2 2020
(WHO) WHO (Updated May 2017) 10 facts on ageing and health. https://www.who.int/features/factfiles/ageing/en/. Accessed May 2 2020.
Babaha F, Rezaei N (2020) Primary immunodeficiency diseases in COVID-19 pandemic: a predisposing or protective factor? Am J Med Sci. https://doi.org/10.1016/j.amjms.2020.07.027
Bahrami A, Vafapour M, Moazzami B, Rezaei N (2020) Hyperinflammatory shock related to COVID-19 in a patient presenting with multisystem inflammatory syndrome in children: first case from Iran. J Paediatr Child Health. https://doi.org/10.1111/jpc.15048
Basiri A, Heidari A, Nadi MF, Fallahy MTP, Nezamabadi SS, Sedighi M, Saghazadeh A, Rezaei N (2020a) Microfluidic devices for detection of RNA viruses. Rev Med Virol n/a (n/a):e2154. https://doi.org/10.1002/rmv.2154
Basiri A, Pazhouhnia Z, Beheshtizadeh N, Hoseinpour M, Saghazadeh A, Rezaei N (2020b) Regenerative medicine in COVID-19 treatment: real opportunities and range of promises. Stem Cell Rev Rep:1–13. https://doi.org/10.1007/s12015-020-09994-5
Baume DM, Robertson MJ, Levine H, Manley TJ, Schow PW, Ritz J (1992) Differential responses to interleukin 2 define functionally distinct subsets of human natural killer cells. Eur J Immunol 22(1):1–6. https://doi.org/10.1002/eji.1830220102
Bindom SM, Lazartigues E (2009) The sweeter side of ACE2: physiological evidence for a role in diabetes. Mol Cell Endocrinol 302(2):193–202
Bonafè M, Prattichizzo F, Giuliani A, Storci G, Sabbatinelli J, Olivieri F (2020) Inflamm-aging: why older men are the most susceptible to SARS-CoV-2 complicated outcomes. Cytokine Growth Factor Rev. https://doi.org/10.1016/j.cytogfr.2020.04.005
Breslin N, Baptiste C, Gyamfi-Bannerman C, Miller R, Martinez R, Bernstein K, Ring L, Landau R, Purisch S, Friedman AM, Fuchs K, Sutton D, Andrikopoulou M, Rupley D, Sheen J-J, Aubey J, Zork N, Moroz L, Mourad M, Wapner R, Simpson LL, D’Alton ME, Goffman D (2020) Coronavirus disease 2019 infection among asymptomatic and symptomatic pregnant women: two weeks of confirmed presentations to an affiliated pair of new York City hospitals. Am J Obstet Gynecol MFM 2(Suppl):100118. https://doi.org/10.1016/j.ajogmf.2020.100118
Carson WE, Fehniger TA, Caligiuri MA (1997) CD56bright natural killer cell subsets: characterization of distinct functional responses to interleukin-2 and the c-kit ligand. Eur J Immunol 27(2):354–360. https://doi.org/10.1002/eji.1830270203
Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, Qiu Y, Wang J, Liu Y, Wei Y, Xia J, Yu T, Zhang X, Zhang L (2020a) Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet 395(10223):507–513. https://doi.org/10.1016/s0140-6736(20)30211-7
Chen Y, Li T, Ye Y, Chen Y, Pan J (2020b) Impact of fundamental diseases on patients with COVID-19. Disaster Med Public Health Prep:1–6. https://doi.org/10.1017/dmp.2020.139
Coronaviridae—Positive Sense RNA Viruses—Positive Sense RNA Viruses. (2011). https://talk.ictvonline.org/ictv-reports/ictv_9th_report/positive-sense-rna-viruses-2011/w/posrna_viruses/222/coronaviridae. Accessed 26 Apr 2020
Cui J, Li F, Shi ZL (2019) Origin and evolution of pathogenic coronaviruses. Nat Rev Microbiol 17(3):181–192. https://doi.org/10.1038/s41579-018-0118-9
Darbeheshti F, Rezaei N (2020) Genetic predisposition models to COVID-19 infection. Med Hypotheses 142:109818. https://doi.org/10.1016/j.mehy.2020.109818
Decker M-L, Grobusch MP, Ritz N (2017) Influence of age and other factors on cytokine expression profiles in healthy children—a systematic review. Front Pediatr 5:255
Du Y, Tu L, Zhu P, Mu M, Wang R, Yang P, Wang X, Hu C, Ping R, Hu P, Li T, Cao F, Chang C, Hu Q, Jin Y, Xu G (2020) Clinical features of 85 fatal cases of COVID-19 from Wuhan: a retrospective observational study. Am J Respir Crit Care Med. https://doi.org/10.1164/rccm.202003-0543OC
Fathi N, Rezaei N (2020a) Lymphopenia in COVID-19: therapeutic opportunities. Cell Biol Int 44(9):1792–1797. https://doi.org/10.1002/cbin.11403
Fathi N, Rezaei N (2020b) Lymphopenia in COVID-19: therapeutic opportunities. Cell Biol Int
Ford N, Vitoria M, Rangaraj A, Norris SL, Calmy A, Doherty M (2020) Systematic review of the efficacy and safety of antiretroviral drugs against SARS, MERS or COVID-19: initial assessment. J Int AIDS Soc 23(4):e25489. https://doi.org/10.1002/jia2.25489
Fuentes E, Fuentes M, Alarcon M, Palomo I (2017) Immune system dysfunction in the elderly. An Acad Bras Cienc 89(1):285–299. https://doi.org/10.1590/0001-3765201720160487
Gorbalenya AE, Baker SC, Baric RS, de Groot RJ, Drosten C, Gulyaeva AA, Haagmans BL, Lauber C, Leontovich AM, Neuman BW, Penzar D, Perlman S, Poon LLM, Samborskiy D, Sidorov IA, Sola I, Ziebuhr J (2020) Severe acute respiratory syndrome-related coronavirus: The species and its viruses – a statement of the Coronavirus Study Group. bioRxiv:2020.2002.2007.937862. doi:https://doi.org/10.1101/2020.02.07.937862
Gosch M, Singler K, Kwetkat A, Heppner HJ (2020) Geriatrics in times of corona. Z Gerontol Geriatr 53(3):228–232. https://doi.org/10.1007/s00391-020-01725-2
Grasselli G, Zangrillo A, Zanella A, Antonelli M, Cabrini L, Castelli A, Cereda D, Coluccello A, Foti G, Fumagalli R, Iotti G, Latronico N, Lorini L, Merler S, Natalini G, Piatti A, Ranieri MV, Scandroglio AM, Storti E, Cecconi M, Pesenti A, Nailescu A, Corona A, Zangrillo A, Protti A, Albertin A, Forastieri Molinari A, Lombardo A, Pezzi A, Benini A, Scandroglio AM, Malara A, Castelli A, Coluccello A, Micucci A, Pesenti A, Sala A, Alborghetti A, Antonini B, Capra C, Troiano C, Roscitano C, Radrizzani D, Chiumello D, Coppini D, Guzzon D, Costantini E, Malpetti E, Zoia E, Catena E, Agosteo E, Barbara E, Beretta E, Boselli E, Storti E, Harizay F, Della Mura F, Lorini FL, Donato Sigurtà F, Marino F, Mojoli F, Rasulo F, Grasselli G, Casella G, De Filippi G, Castelli G, Aldegheri G, Gallioli G, Lotti G, Albano G, Landoni G, Marino G, Vitale G, Battista Perego G, Evasi G, Citerio G, Foti G, Natalini G, Merli G, Sforzini I, Bianciardi L, Carnevale L, Grazioli L, Cabrini L, Guatteri L, Salvi L, Dei Poli M, Galletti M, Gemma M, Ranucci M, Riccio M, Borelli M, Zambon M, Subert M, Cecconi M, Mazzoni MG, Raimondi M, Panigada M, Belliato M, Bronzini N, Latronico N, Petrucci N, Belgiorno N, Tagliabue P, Cortellazzi P, Gnesin P, Grosso P, Gritti P, Perazzo P, Severgnini P, Ruggeri P, Sebastiano P, Covello RD, Fernandez-Olmos R, Fumagalli R, Keim R, Rona R, Valsecchi R, Cattaneo S, Colombo S, Cirri S, Bonazzi S, Greco S, Muttini S, Langer T, Alaimo V, Viola U (2020) Baseline characteristics and outcomes of 1591 patients infected with SARS-CoV-2 admitted to ICUs of the Lombardy region, Italy. JAMA 323 (16):1574–1581. doi:https://doi.org/10.1001/jama.2020.5394
Guan WJ, Liang WH, Zhao Y, Liang HR, Chen ZS, Li YM, Liu XQ, Chen RC, Tang CL, Wang T, Ou CQ, Li L, Chen PY, Sang L, Wang W, Li JF, Li CC, Ou LM, Cheng B, Xiong S, Ni ZY, Xiang J, Hu Y, Liu L, Shan H, Lei CL, Peng YX, Wei L, Liu Y, Hu YH, Peng P, Wang JM, Liu JY, Chen Z, Li G, Zheng ZJ, Qiu SQ, Luo J, Ye CJ, Zhu SY, Cheng LL, Ye F, Li SY, Zheng JP, Zhang NF, Zhong NS, He JX (2020) Comorbidity and its impact on 1590 patients with COVID-19 in China: a nationwide analysis. Eur Respir J 55(5). https://doi.org/10.1183/13993003.00547-2020
Guy JL, Jackson RM, Acharya KR, Sturrock ED, Hooper NM, Turner AJ (2003) Angiotensin-converting enzyme-2 (ACE2): comparative modeling of the active site, specificity requirements, and chloride dependence. Biochemistry 42(45):13185–13192
Hanaei S, Rezaei N (2020) COVID-19: developing from an outbreak to a pandemic. Arch Med Res. https://doi.org/10.1016/j.arcmed.2020.04.021
Helbing D, Farkas I, Vicsek T (2000) Simulating dynamical features of escape panic. Nature 407(6803):487–490
Heurich A, Hofmann-Winkler H, Gierer S, Liepold T, Jahn O, Pöhlmann S (2014) TMPRSS2 and ADAM17 cleave ACE2 differentially and only proteolysis by TMPRSS2 augments entry driven by the severe acute respiratory syndrome coronavirus spike protein. J Virol 88(2):1293. https://doi.org/10.1128/JVI.02202-13
Hoffmann M, Kleine-Weber H, Schroeder S, Krüger N, Herrler T, Erichsen S, Schiergens TS, Herrler G, Wu N-H, Nitsche A (2020) SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell
Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, Zhang L, Fan G, Xu J, Gu X, Cheng Z, Yu T, Xia J, Wei Y, Wu W, Xie X, Yin W, Li H, Liu M, Xiao Y, Gao H, Guo L, Xie J, Wang G, Jiang R, Gao Z, Jin Q, Wang J, Cao B (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395(10223):497–506. https://doi.org/10.1016/s0140-6736(20)30183-5
Jabbari P, Rezaei N (2020) With risk of reinfection, is COVID-19 Here to stay? Disaster Med Public Health Prep:1. https://doi.org/10.1017/dmp.2020.274
Jabbari P, Jabbari F, Ebrahimi S, Rezaei N (2020) COVID-19: a chimera of two pandemics. Disaster Med Public Health Prep:1–2. https://doi.org/10.1017/dmp.2020.223
Jahanshahlu L, Rezaei N (2020a) Central Nervous System Involvement in COVID-19. Arch Med Res. https://doi.org/10.1016/j.arcmed.2020.05.016
Jahanshahlu L, Rezaei N (2020b) Monoclonal antibody as a potential anti-COVID-19. Biomed Pharmacother 129:110337. https://doi.org/10.1016/j.biopha.2020.110337
Kim ES, Chin BS, Kang CK, Kim NJ, Kang YM, Choi JP, Oh DH, Kim JH, Koh B, Kim SE, Yun NR, Lee JH, Kim JY, Kim Y, Bang JH, Song KH, Kim HB, Chung KH, Oh MD (2020) Clinical course and outcomes of patients with severe acute respiratory syndrome coronavirus 2 infection: a preliminary report of the first 28 patients from the Korean cohort study on COVID-19. J Korean Med Sci 35(13):e142. https://doi.org/10.3346/jkms.2020.35.e142
Kushwah R, Wu J, Oliver JR, Jiang G, Zhang J, Siminovitch KA, Hu J (2010) Uptake of apoptotic DC converts immature DC into tolerogenic DC that induce differentiation of Foxp3+ Treg. Eur J Immunol 40(4):1022–1035
Lai CC, Liu YH, Wang CY, Wang YH, Hsueh SC, Yen MY, Ko WC, Hsueh PR (2020) Asymptomatic carrier state, acute respiratory disease, and pneumonia due to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2): facts and myths. J Microbiol Immunol Infect. https://doi.org/10.1016/j.jmii.2020.02.012
Lambert DW, Yarski M, Warner FJ, Thornhill P, Parkin ET, Smith AI, Hooper NM, Turner AJ (2005) Tumor necrosis factor-α convertase (ADAM17) mediates regulated ectodomain shedding of the severe-acute respiratory syndrome-coronavirus (SARS-CoV) receptor, angiotensin-converting enzyme-2 (ACE2). J Biol Chem 280(34):30113–30119
Langrish CL, Buddle JC, Thrasher AJ, Goldblatt D (2002) Neonatal dendritic cells are intrinsically biased against Th-1 immune responses. Clin Exp Immunol 128(1):118–123
Larbi A, Dupuis G, Khalil A, Douziech N, Fortin C, Fulop T Jr (2006) Differential role of lipid rafts in the functions of CD4+ and CD8+ human T lymphocytes with aging. Cell Signal 18(7):1017–1030. https://doi.org/10.1016/j.cellsig.2005.08.016
Larbi A, Fortin C, Dupuis G, Berrougui H, Khalil A, Fulop T (2014) Immunomodulatory role of high-density lipoproteins: impact on immunosenescence. Age (Dordr) 36(5):9712. https://doi.org/10.1007/s11357-014-9712-6
Lauer SA, Grantz KH, Bi Q, Jones FK, Zheng Q, Meredith HR, Azman AS, Reich NG, Lessler J (2020) The incubation period of coronavirus disease 2019 (COVID-19) from publicly reported confirmed cases: estimation and application. Ann Intern Med 172(9):577–582. https://doi.org/10.7326/m20-0504
Lichterfeld-Kottner A, El Genedy M, Lahmann N, Blume-Peytavi U, Buscher A, Kottner J (2020) Maintaining skin integrity in the aged: a systematic review. Int J Nurs Stud 103:103509. https://doi.org/10.1016/j.ijnurstu.2019.103509
Lippi G, Wong J, Henry BM (2020) Hypertension in patients with coronavirus disease 2019 (COVID-19): a pooled analysis. Pol Arch Intern Med 130(4):304–309. https://doi.org/10.20452/pamw.15272
Liu K, Zhang W, Yang Y, Zhang J, Li Y, Chen Y (2020) Respiratory rehabilitation in elderly patients with COVID-19: a randomized controlled study. Complement Ther Clin Pract 39:101166. https://doi.org/10.1016/j.ctcp.2020.101166
Long C, Xu H, Shen Q, Zhang X, Fan B, Wang C, Zeng B, Li Z, Li X, Li H (2020) Diagnosis of the coronavirus disease (COVID-19): rRT-PCR or CT? Eur J Radiol 126:108961. https://doi.org/10.1016/j.ejrad.2020.108961
Lotfi M, Rezaei N (2020) SARS-CoV-2: a comprehensive review from pathogenicity of the virus to clinical consequences. J Med Virol. https://doi.org/10.1002/jmv.26123
Lotfi M, Hamblin MR, Rezaei N (2020) COVID-19: transmission, prevention, and potential therapeutic opportunities. Clinica chimica acta; Int J Clin Chem 508:254–266. https://doi.org/10.1016/j.cca.2020.05.044
Low DJ (2000) Following the crowd. Nature 407(6803):465–466
Maddux AB, Douglas IS (2015) Is the developmentally immature immune response in paediatric sepsis a recapitulation of immune tolerance? Immunology 145(1):1–10
Mansourabadi AH, Sadeghalvad M, Mohammadi-Motlagh HR, Rezaei N (2020) The immune system as a target for therapy of SARS-CoV-2: a systematic review of the current immunotherapies for COVID-19. Life Sci 258:118185. https://doi.org/10.1016/j.lfs.2020.118185
Meng J, Xiao G, Zhang J, He X, Ou M, Bi J, Yang R, Di W, Wang Z, Li Z, Gao H, Liu L, Zhang G (2020) Renin-angiotensin system inhibitors improve the clinical outcomes of COVID-19 patients with hypertension. Emerg Microbes Infect 9(1):757–760. https://doi.org/10.1080/22221751.2020.1746200
Moazzami B, Razavi-Khorasani N, Dooghaie Moghadam A, Farokhi E, Rezaei N (2020) COVID-19 and telemedicine: immediate action required for maintaining healthcare providers Well-being. J Clin Virol: The Official Publication of the Pan American Society for Clinical Virology 126:104345. https://doi.org/10.1016/j.jcv.2020.104345
Mohamed K, Rodríguez-Román E, Rahmani F, Zhang H, Ivanovska M, Makka SA, Joya M, Makuku R, Islam MS, Radwan N, Rahmah L, Goda R, Abarikwu SO, Shaw M, Zoghi S, Irtsyan S, Ling I, Cseprekal O, Faten AB, Hazar Sayar E, Soloukey C, Grancini G, Rezaei N (2020) Borderless collaboration is needed for COVID-19-a disease that knows no borders. Infect Control Hosp Epidemiol:1–2. https://doi.org/10.1017/ice.2020.162
Momtazmanesh S, Ochs HD, Uddin LQ, Perc M, Routes JM, Vieira DN, Al-Herz W, Baris S, Prando C, Rosivall L, Abdul Latiff AH, Ulrichs T, Roudenok V, Aldave Becerra JC, Salunke DB, Goudouris E, Condino-Neto A, Stashchak A, Kryvenko O, Stashchak M, Bondarenko A, Rezaei N (2020) All together to fight COVID-19. Am J Trop Med Hyg 102(6):1181–1183. https://doi.org/10.4269/ajtmh.20-0281
Moradian N, Ochs HD, Sedikies C, Hamblin MR, Camargo CA Jr, Martinez JA, Biamonte JD, Abdollahi M, Torres PJ, Nieto JJ, Ogino S, Seymour JF, Abraham A, Cauda V, Gupta S, Ramakrishna S, Sellke FW, Sorooshian A, Wallace Hayes A, Martinez-Urbistondo M, Gupta M, Azadbakht L, Esmaillzadeh A, Kelishadi R, Esteghamati A, Emam-Djomeh Z, Majdzadeh R, Palit P, Badali H, Rao I, Saboury AA, Jagan Mohan Rao L, Ahmadieh H, Montazeri A, Fadini GP, Pauly D, Thomas S, Moosavi-Movahed AA, Aghamohammadi A, Behmanesh M, Rahimi-Movaghar V, Ghavami S, Mehran R, Uddin LQ, Von Herrath M, Mobasher B, Rezaei N (2020) The urgent need for integrated science to fight COVID-19 pandemic and beyond. J Transl Med 18(1):205. https://doi.org/10.1186/s12967-020-02364-2
Nanda A, Vura N, Gravenstein S (2020) COVID-19 in older adults. Aging Clin Exp Res:1–4. https://doi.org/10.1007/s40520-020-01581-5
Nasab MG, Saghazadeh A, Rezaei N (2020) SARS-CoV-2-a tough opponent for the immune system. Arch Med Res. https://doi.org/10.1016/j.arcmed.2020.05.020
Nie X, Fan L, Mu G, Tan Q, Wang M, Xie Y, Cao L, Zhou M, Zhang Z, Chen W (2020) Epidemiological characteristics and incubation period of 7,015 confirmed cases with coronavirus disease 2019 outside Hubei Province in China. J Infect Dis. https://doi.org/10.1093/infdis/jiaa211
Nikolich-Zugich J (2018) The twilight of immunity: emerging concepts in aging of the immune system. Nat Immunol 19(1):10–19. https://doi.org/10.1038/s41590-017-0006-x
Nikolich-Zugich J, Knox KS, Rios CT, Natt B, Bhattacharya D, Fain MJ (2020) SARS-CoV-2 and COVID-19 in older adults: what we may expect regarding pathogenesis, immune responses, and outcomes. Geroscience 42(2):505–514. https://doi.org/10.1007/s11357-020-00186-0
Olde Rikkert MGM, Vingerhoets RW, van Geldorp N, de Jong E, Maas H (2020) Atypical clinical picture of COVID-19 in older patients. Ned Tijdschr Geneeskd 164
Orimo H, Ito H, Suzuki T, Araki A, Hosoi T, Sawabe M (2006) Reviewing the definition of “elderly”. Geriatr Gerontol Int 6. https://doi.org/10.1111/j.1447-0594.2006.00341.x
Pashaei M, Rezaei N (2020) Immunotherapy for SARS-CoV-2: potential opportunities. Expert Opin Biol Ther:1–5. https://doi.org/10.1080/14712598.2020.1807933
Pawelec G, Goldeck D, Derhovanessian E (2014) Inflammation, ageing and chronic disease. Curr Opin Immunol 29:23–28. https://doi.org/10.1016/j.coi.2014.03.007
Pietilä M, Neuvonen M, Borodulin K, Korpela K, Sievänen T, Tyrväinen L (2015) Relationships between exposure to urban green spaces, physical activity and self-rated health. J Outdoor Recreat Tour 10:44–54. https://doi.org/10.1016/j.jort.2015.06.006
Qin C, Zhou L, Hu Z, Zhang S, Yang S, Tao Y, Xie C, Ma K, Shang K, Wang W, Tian DS (2020) Dysregulation of immune response in patients with COVID-19 in Wuhan. China Clin Infect Dis. https://doi.org/10.1093/cid/ciaa248
Rabi FA, Al Zoubi MS, Kasasbeh GA, Salameh DM, Al-Nasser AD (2020) SARS-CoV-2 and coronavirus disease 2019: what we know so far. Pathogens 9(3). https://doi.org/10.3390/pathogens9030231
Rabiee N, Rabiee M, Bagherzadeh M, Rezaei N (2020) COVID-19 and picotechnology: potential opportunities. Med Hypotheses 144:109917. https://doi.org/10.1016/j.mehy.2020.109917
Rezaei N (2020a) COVID-19 affects healthy pediatricians more than pediatric patients. Infect Control Hosp Epidemiol 1. https://doi.org/10.1017/ice.2020.139
Rezaei N (2020b) COVID-19 and medical biotechnology. Avicenna J Med Biotechnol 12(3):139
Saghazadeh A, Rezaei N (2020a) Immune-epidemiological parameters of the novel coronavirus–a perspective. Expert Rev Clin Immunol:1–6
Saghazadeh A, Rezaei N (2020b) Towards treatment planning of COVID-19: rationale and hypothesis for the use of multiple immunosuppressive agents: anti-antibodies, immunoglobulins, and corticosteroids. Int Immunopharmacol:106560
Sahu KK, Siddiqui AD, Rezaei N, Cerny J (2020) Challenges for management of immune thrombocytopenia during COVID-19 pandemic. J Med Virol. https://doi.org/10.1002/jmv.26251
Saito S, Morii T, Enomoto M, Sakakura S, Nishikawa K, Narita N, Ichijo M (1993) The effect of interleukin 2 and transforming growth factor-beta 2 (TGF-beta 2) on the proliferation and natural killer activity of decidual CD16- CD56bright natural killer cells. Cell Immunol 152(2):605–613. https://doi.org/10.1006/cimm.1993.1316
Saleki K, Banazadeh M, Saghazadeh A, Rezaei N (2020) The involvement of the central nervous system in patients with COVID-19. Rev Neurosci 31(4):453–456. https://doi.org/10.1515/revneuro-2020-0026
Sharifkashani S, Bafrani MA, Khaboushan AS, Pirzadeh M, Kheirandish A, Yavarpour Bali H, Hessami A, Saghazadeh A, Rezaei N (2020) Angiotensin-converting enzyme 2 (ACE2) receptor and SARS-CoV-2: potential therapeutic targeting. Eur J Pharmacol 884:173455. https://doi.org/10.1016/j.ejphar.2020.173455
Singh S, Bajorek B (2014) Defining ‘elderly’ in clinical practice guidelines for pharmacotherapy. Pharm Pract (Granada) 12(4):489. https://doi.org/10.4321/s1886-36552014000400007
Singhal T (2020) A review of coronavirus Disease-2019 (COVID-19). Indian J Pediatr 87(4):281–286. https://doi.org/10.1007/s12098-020-03263-6
Su S, Wong G, Shi W, Liu J, Lai ACK, Zhou J, Liu W, Bi Y, Gao GF (2016) Epidemiology, genetic recombination, and pathogenesis of coronaviruses. Trends Microbiol 24(6):490–502. https://doi.org/10.1016/j.tim.2016.03.003
Tang N, Bai H, Chen X, Gong J, Li D, Sun Z (2020) Anticoagulant treatment is associated with decreased mortality in severe coronavirus disease 2019 patients with coagulopathy. J Thromb Haemost 18(5):1094–1099. https://doi.org/10.1111/jth.14817
Tyrrell DAJ, Bynoe ML (1966) Cultivation of viruses from a high proportion of patients with colds. Lancet 287(7428):76–77. https://doi.org/10.1016/S0140-6736(66)92364-6
Vallejo AN (2005) CD28 extinction in human T cells: altered functions and the program of T-cell senescence. Immunol Rev 205:158–169. https://doi.org/10.1111/j.0105-2896.2005.00256.x
Velavan TP, Meyer CG (2020) The COVID-19 epidemic. Tropical Med Int Health 25(3):278–280. https://doi.org/10.1111/tmi.13383
Veronese N, Demurtas J, Yang L, Tonelli R, Barbagallo M, Lopalco P, Lagolio E, Celotto S, Pizzol D, Zou L, Tully MA, Ilie PC, Trott M, López-Sánchez GF, Smith L (2020) Use of corticosteroids in coronavirus disease 2019 pneumonia: a systematic review of the literature. Front Med (Lausanne) 7:170. https://doi.org/10.3389/fmed.2020.00170
Walford RL (1964) The immunologic theory of aging. The Gerontologist 4(4):195–197. https://doi.org/10.1093/geront/4.4.195
Wang H, Luo S, Shen Y, Li M, Zhang Z, Dong Y, Zhou H, Lin L, Guo W, Kang Z (2020a) Multiple enzyme release, inflammation storm and hypercoagulability are prominent indicators for disease progression in COVID-19: a multi-centered, Correlation Study with CT Imaging Score
Wang K, Kang S, Tian R, Zhang X, Zhang X, Wang Y (2020b) Imaging manifestations and diagnostic value of chest CT of coronavirus disease 2019 (COVID-19) in the Xiaogan area. Clin Radiol 75(5):341–347. https://doi.org/10.1016/j.crad.2020.03.004
Wang L, He W, Yu X, Hu D, Bao M, Liu H, Zhou J, Jiang H (2020c) Coronavirus disease 2019 in elderly patients: characteristics and prognostic factors based on 4-week follow-up. J Infect 80(6):639–645. https://doi.org/10.1016/j.jinf.2020.03.019
Wang Y, Liu Y, Liu L, Wang X, Luo N, Li L (2020d) Clinical outcomes in 55 patients with severe acute respiratory syndrome coronavirus 2 who were asymptomatic at hospital admission in Shenzhen, China. J Infect Dis 221(11):1770–1774. https://doi.org/10.1093/infdis/jiaa119
Ward CF, Figiel GS, McDonald WM (2020) Altered mental status as a novel initial clinical presentation for COVID-19 infection in the elderly. Am J Geriatr Psychiatry. https://doi.org/10.1016/j.jagp.2020.05.013
Wilder-Smith A, Freedman DO (2020) Isolation, quarantine, social distancing and community containment: pivotal role for old-style public health measures in the novel coronavirus (2019-nCoV) outbreak. J Travel Med 27(2). https://doi.org/10.1093/jtm/taaa020
Wilson ME, Chen LH (2020) Travellers give wings to novel coronavirus (2019-nCoV). J Travel Med 27(2). https://doi.org/10.1093/jtm/taaa015
Wong C, Goldstein DR (2013) Impact of aging on antigen presentation cell function of dendritic cells. Curr Opin Immunol 25(4):535–541. https://doi.org/10.1016/j.coi.2013.05.016
Wu Z, McGoogan JM (2020) Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention. Jama
Xu XW, Wu XX, Jiang XG, Xu KJ, Ying LJ, Ma CL, Li SB, Wang HY, Zhang S, Gao HN, Sheng JF, Cai HL, Qiu YQ, Li LJ (2020a) Clinical findings in a group of patients infected with the 2019 novel coronavirus (SARS-Cov-2) outside of Wuhan, China: retrospective case series. BMJ 368:m606. https://doi.org/10.1136/bmj.m606
Xu YH, Dong JH, An WM, Lv XY, Yin XP, Zhang JZ, Dong L, Ma X, Zhang HJ, Gao BL (2020b) Clinical and computed tomographic imaging features of novel coronavirus pneumonia caused by SARS-CoV-2. J Infect 80(4):394–400. https://doi.org/10.1016/j.jinf.2020.02.017
Xudong X, Junzhu C, Xingxiang W, Furong Z, Yanrong L (2006) Age-and gender-related difference of ACE2 expression in rat lung. Life Sci 78(19):2166–2171
Yang Y, Peng F, Wang R, Guan K, Jiang T, Xu G, Sun J, Chang C (2020) The deadly coronaviruses: the 2003 SARS pandemic and the 2020 novel coronavirus epidemic in China. J Autoimmun 109:102434. https://doi.org/10.1016/j.jaut.2020.102434
Yaqinuddin A, Kashir J (2020) Innate immunity in COVID-19 patients mediated by NKG2A receptors, and potential treatment using Monalizumab, Cholroquine, and antiviral agents. Med Hypotheses 140:109777. https://doi.org/10.1016/j.mehy.2020.109777
Yazdanpanah F, Hamblin MR, Rezaei N (2020a) The immune system and COVID-19: friend or foe? Life Sci:117900
Yazdanpanah N, Saghazadeh A, Rezaei N (2020b) Anosmia: a missing link in the neuroimmunology of coronavirus disease 2019 (COVID-19). Rev Neurosci. https://doi.org/10.1515/revneuro-2020-0039
Yousefzadegan S, Rezaei N (2020) Case report: death due to COVID-19 in three brothers. Am J Trop Med Hyg 102(6):1203–1204. https://doi.org/10.4269/ajtmh.20-0240
Zhang T, Wu Q, Zhang Z (2020) Probable pangolin origin of SARS-CoV-2 associated with the COVID-19 outbreak. Curr Biol 30(7):1346–1351.e1342. https://doi.org/10.1016/j.cub.2020.03.022
Zhou P, Yang X-L, Wang X-G, Hu B, Zhang L, Zhang W, Si H-R, Zhu Y, Li B, Huang C-L, Chen H-D, Chen J, Luo Y, Guo H, Jiang R-D, Liu M-Q, Chen Y, Shen X-R, Wang X, Zheng X-S, Zhao K, Chen Q-J, Deng F, Liu L-L, Yan B, Zhan F-X, Wang Y-Y, Xiao G-F, Shi Z-L (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579(7798):270–273. https://doi.org/10.1038/s41586-020-2012-7
Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, Zhao X, Huang B, Shi W, Lu R, Niu P, Zhan F, Ma X, Wang D, Xu W, Wu G, Gao GF, Tan W (2020) A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med 382(8):727–733. https://doi.org/10.1056/NEJMoa2001017
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Mirbeyk, M., Saghazadeh, A., Rezaei, N. (2021). Geriatrics and COVID-19. In: Rezaei, N. (eds) Coronavirus Disease - COVID-19. Advances in Experimental Medicine and Biology, vol 1318. Springer, Cham. https://doi.org/10.1007/978-3-030-63761-3_13
Download citation
DOI: https://doi.org/10.1007/978-3-030-63761-3_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-63760-6
Online ISBN: 978-3-030-63761-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)