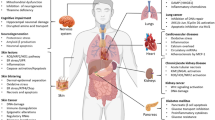
Abstract
Contamination of drinking groundwater with arsenic is a looming problem in several countries and has affected millions of people, distributed over some 20 countries, globally including people in West Bengal (India) and Bangladesh. Continued exposure to Arsenic (‘As’) leads to various disorders and malfunctioning of renal, reproductive, cardiovascular and respiratory system along with the lethal effects manifested on skin and epidermal cells. In the review, an effort was made to incorporate the findings of other investigators and to evaluate the relation among arsenic metabolism and the consequences of numerous chronic disease. Early indications/manifestations of arsenicosis is difficult because of the occurrence of non-specific symptoms in various water-borne ailments. It has emerged that orthodox drugs used for treating arsenicosis was highly unsatisfactory as they have their own toxic side effects. In such a scenario, insights to the biological and epidemiological meanings of arsenic metabolism can help in mitigating the risk of arsenic toxicity and provide a prospective means for disease prophecy, prevention and control.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Arsenic is a naturally occurring metalloid that is extensively dispersed on the Earth's crust with the chemical symbol (As), atomic number (Z-33) and which is placed between phosphorus and antimony in group 15 of the periodic table. Arsenic exist in minerals, usually in amalgamation with sulphur iron and other metals, and also exist in its elemental form. This metalloid is found in groundwater as it percolates through rock and soils, air, food-grains and vegetables. It is also released into the environment by volcanic eruptions and indiscriminate mining. Arsenic in groundwater is a widespread and alarming problem that tends to be higher in drinking water drawn from ground sources, such as dug-well and tube-wells, than from surface water sources such as ponds, lakes or natural reservoirs. The maximum permissible content of inorganic arsenic in ground water as set by the U.S. Environmental Protection Agency (EPA) is 10 ppb in the USA. But the levels of arsenic in certain countries like India and Bangladesh have been measured at over 500 ppb (Naujokas et al. 2013).
Arsenic exist in environment in the form of trivalent arsenite (As3+) or pentavalent arsenate (As5+). As3+ form in particular is high in drinking water where the condition is anaerobic while the pentavalent form is predominant in aerobic conditions. The surge in cancer risk detected in several epidemiological investigations is mainly due to the occurrence of trivalent arsenic (arsenite) as its pentavalent form in water is quickly reduced when it enters a cell. The main reason for arsenite to enter a cell is because it is uncharged at pH 7 which is the normal physiological pH of the body while arsenate is negatively charged and impermeable to the cell membrane. Arsenite and arsenate, both the forms are genuine and established human carcinogens, but not a true animal carcinogen. In standard assays it was reported that only arsenite has the ability to cross transplacental barrier and thereby acts as a carcinogen and also as a co-carcinogen (National Research Council 2000; IARC 2004). It has been reported that arsenate is transported by the phosphate transporter while arsenite is transported by aqua-glycoporin 7 and 9 (Huang and Lee 1996; Liu et al 2002). Efforts till date by both Governmental and non-Governmental establishments in innumerable countries to provide As-free drinking water to highly contaminated zones remain exceptionally insufficient. Arsenic enters the human bodies of innocent populations not only through drinking water they consume but also through food and vegetables grown in contaminated soil. The current review attempt to describe the latest information on the toxicological aspects of arsenic based on the informations obtained from PubMed, Science Direct and Google Scholar databases. A search was made through permutation and combination of keywords such as arsenic, human and animal toxicity, biological activity, endocrine disruption, carcinogenicity, genotoxicity, immunological toxicity, neurogenic effects of arsenic, thyro-toxicity, cardiovascular, musculoskeletal, dermal toxicities, and antinuclear antibody. There were no language limitations as the articles were carefully studied for information on the various aspects of toxicity.
2 Routes of Exposure for Arsenic
The primary routes of entry of arsenic in the body are ingestion and inhalation. Though dermal exposure can happen in humans, it is not considered a primary route. In Europe and American alone 80% of arsenic ingestion is through consumption of meat, fish, and poultry. Various marine organism like fish, bivalve and algae contains arsenic as arseno-betaine and arseno-choline, which is also called as fish arsenic and both these forms have low toxicity levels in humans and are rapidly excreted through urine (ATSDR 2007). Recent studies revealed that a certain form of seaweed contains a high level of inorganic arsenic (Rose et al. 2007). Bedrock containing arsenic is primarily responsible to contaminate groundwater and this is a natural phenomenon which has been reported as leading cause of arsenic toxicity all over the world including Indo-Gangetic plain. Arsenic in drinking-water has caught attention since its discovery in the 1990s due to its wide occurrence in well-water in Bangladesh and parts of India (WHO 2001).
3 Metal Toxicities in Human and Experimental Animal
The detrimental effects of arsenic vary from individual to individual and by the body metabolism process. Soon after absorption, inorganic arsenic both arsenite and arsenate are methylated into MMA and DMA in the liver and are excreted through urine after passing through the kidneys along with unmethylated arsenic (Vahter 2002; De Loma et al 2018; Skröder et al. 2018). A relative proportion of metabolites in urine varies significantly within and among population groups. It has been reported by others that about 10–30% iAs (inorganic arsenic), 10 to 20% MMA and 60–80% DMA is excreted through urine (Hernandez and Marcos 2008; Huang et al. 2008; Gonzalez-Martinez et al. 2018). It was estimated that 50–70% of absorbed pentavalent arsenic (AsV) is rapidly reduced to trivalent arsenic (AsIII), a biotransformation reaction common in most species. In all experimental animals specifically rodents, DMA is the main metabolite excreted in urine. The proportion of methylation varies substantially between species, for example it has been reported that apes such as the marmoset monkey (Zaris) and chimpanzee do not methylate inorganic arsenic, on the other hand, the marmoset monkey accumulates arsenic in the liver (Zakharyan et al. 1996). The rat, has an effective methylation pattern of arsenic but the formed DMA gets collected in the red blood cells (Lu et al. 2007). Hence, rats have been shown to excrete lower levels of arsenic through urine. When human and rodents were exposed to DMA, it was found that about 5% of the dose is excreted through urine in the form of trimethylarsine oxide (TMAO) (Hughes et al. 2008). Similar studies conducted by other investigators found that when human subjects were exposed to quantified doses of inorganic arsenic their rate of excretion surges with the methylation effectiveness, moreover inter-individual variations were also noticed in the methylation of arsenic (Bailey et al. 2013). Recent studies on human subjects exposed to arsenic in northern Argentina have shown that they excrete low amounts of MMA, on the other hand, children showed a lesser grade of methylation of arsenic than adults (Concha et al. 1998; Vahter 2007).
4 Some Specific Aspects of Arsenic Toxicities
4.1 Genotoxicities
It has been stated by Dulout et al. (1996) that there was an surge in chromosomal aberrations in lymphocytes of people residing in north-western Argentina who consumed arsenic contaminated drinking water. Ghosh et al. (2006) conducted studies on 422 individuals from Haringhata and 24 Parganas (N) district of West Bengal, concluding that person showing skin-symptoms were more vulnerable to arsenic-induced toxicity and genotoxicity than those persons who do not show any symptoms of arsenic poisoning. Further, it has been stated that sodium arsenite treatment of rat ovarian cells results in DNA fragmentation (Akram et al. 2009). It was also revealed by other workers that children exposed to arsenic from early childhood had increased telomere length compared to children unexposed to arsenic (Chatterjee et al. 2018).
Arsenic is both genotoxic and carcinogenic to human and animals however it displayed tricky mutagenic potentials in bacterial systems. In bacterial system it induces DNA damage indirectly by inhibiting DNA repair mechanism. But the exact DNA repair inhibition mechanism could not be deciphered accurately (Samavarchi Tehrani et al. 2018). Rossman et al. (1977) had showed that arsenite supresses the post-replication repair pathway in E. coli. A similar study conducted by Lee-Chen et al. (1992) on UV irradiated Chinese hamster ovarian cells found that arsenite exerts its co-genotoxic consequence by preventing DNA repair mechanisms. By single cell gel (SCG) assay Hartmann and Speit (1996) noticed increased DNA damage in cells that were treated with sodium arsenite in various concentrations (from 200 to 1500 M) than the control culture. Similar experiments conducted by Schaumloffel and Gebel (1998), found that there was a significant induction of DNA damage when the cells were insulted with 0.01 M As (III). Further, when the frequency of micro-nucleated cells between people exposed to high concentration of arsenic in ground water (1312 g/L) was compared with low exposure to arsenic (16 g/L), it was found that there was a sudden elevation in the frequency of micronuclei in persons who drank high concentration of contaminated water when compared to lower groups Warner et al. (1994). Moreover, they were also assured that the incidence of micro nucleated bladder cells was certainly related with the urinary content and concentration of arsenic. It was also reported by the same group that frequencies of micronuclei containing acentric fragments and whole chromosomes also increased. Two cross sectional studies were conducted by Moore et al. (1997), in the states of Nevada and Chile to observe the association between arsenic ingestion and genetic damage in the urothelium and they concluded that amplified levels of arsenic in drinking water resulted in an increase in micro-nucleated cells in bladder.
4.2 Immunological Toxicities
It was earlier reported that low concentrations of iAs significantly repressed the action of macrophages and T lymphocytes (T cells), the two immune cell types involved in controlling infection and tumour development (Soto-Peña et al. 2006; Lemarie et al. 2006, 2008). As a carcinogenic environmental contaminant inorganic arsenic exerts immunosuppressive action on human T lymphocytes. A considerable reduction was found in interleukin-2 (IL2) secretion which is a cytokine and plays a pivotal role in immunology and also reduces T cell proliferation. It was revealed that in vivo, treatment of mice with iAs induced thymus atrophy caused by suppression of many genes which are involved in cell cycle advancement. Further, it also diminished in vitro proliferation of mitogen stimulated spleenocytes (Nohara et al. 2008; Soto-Peña and Vega 2008). Interleukin 2 (IL2) plays a big role in instigation of T-cells and progression through cell cycle. iAs-dependant inhibition of peripheral T cell proliferation was generally accompanied by repression of interleukin-2 (IL2) exudation (Lemarie et al. 2006, 2008), decreased adhesion of macrophages, reduced production of nitric oxide (NO) and dwindling chemotactic and phagocytotic indices (Sengupta and Bishayi 2002; Bishayi and Sengupta 2003, 2006). It was reported that people living in areas having groundwater arsenic contaminated by arsenic had increased antinuclear antibodies (ANA) compared to normal subjects (Belon et al. 2006). Several investigators have proved earlier that arsenic traverses the placental barrier, posing a threat to the normal development of the foetus (Rahman et al. 2009; Ferrario et al. 2009). A study in Bangladesh revealed that arsenic exposure during pregnancy was co-related with increased placental inflammatory reactions, diminished placental T cells, and altered cord blood cytokines. The findings of this study recommended unfavorable effects of arsenic on immunobiology that leads to weakened new-born function (Ferrario et al. 2009). Macrophages plays a vital role in immunological functions, it has been investigated that persons residing in ground water contaminated areas showed circularization of macrophages, diminished cellular adhesion, decreased phagocytic activity and expression of proteins such as CD54 compared to those living in arsenic free areas (Lemarie et al. 2006; Banerjee et al. 2009). Some also reported that the ratio of CD4/CD8 decreased when exposed to iAs, which could indicate immune suppression (Soto-Peña and Vega 2008). Arsenic also inhibit mitogen stimulated proliferation of SMC (Splenic mononuclear cells) and PBMC (Peripheral blood mononuclear cells) in broiler chickens. In some investigations with cat fish, it has been revealed that there was a general increase in the population of lymphocytes and a sudden decrease in IL4 when contaminated with arsenic (Ghosh et al. 2007a, b). This group also detected that arsenic inhibits humoral immunity by supressing primary and secondary antibody forming cells. Further, it was also stated that arsenic suppressed type IV hypersensitivity, (a delayed type of response to cutaneous sensitization) in mice, rats and chicken (Savabiesfahani et al. 1998, Patterson et al. 2004; Aggarwal et al. 2008).
4.3 Carcinogenicity
Investigators stated that dimethylarsinic acid (DMA V) administration to rats promoted for tumor development in various organs (Yamamoto 1995). Further, it was also observed that when mice were treated with arsenic at a concentration of 10 and 25 ppm in drinking water it resulted in formation of papilloma and carcinoma respectively and this was due to augmented proliferation of cells. Arsenic induces DNA damage, produces (ROS)/free radicals which modifies the expression of protein p21 and p53, which are regarded as tumour suppressors. Further, DMMTA (V) caused diminished protein expression of tumor suppressor along with enhanced damage of DNA and production of ROS (reactive oxygen species). Investigators reported a plausible association between incidence of prostate cancer and exposure to high concentrations of arsenic (Lin et al. 2013). But the link between exposure to low concentrations of arsenic and the onset of prostate cancer is unclear, and needs more epidemiological research. Investigation of pregnant mothers exposed to arsenic resulted in leukaemia which was reported by Heck et al. (2014). Recently, results of a 20-year retrospective cohort study on hepatocarcinogenesis involving 802 males and 301 females members belonging to 138 communities in Taiwan revealed significant increase in hepatocarcinogenesis in both genders after exposure to arsenic concentration above 0.64 mg/L. However, the same group also reported no significant changes which were lower than 0.64 mg/L (Baastrup et al. 2008). There are a few contradictory reports where investigators found no connection between occurence of bladder cancer even after exposure to low concentrations of arsenic and smoking (Meliker et al. 2010). Further confirmation in this area is needed as the group has incapacity to accurately measure smoking and correctly measure arsenic exposure levels. On the other hand, few groups also reported that ground water intake elevates bladder cancer incidence in a population-based study in New England (Zolot 2016). The reason for high rates of urinary bladder cancer might be attributed to hindrance/impediment of the detoxification process, thereby inhibiting repair mechanism of DNA and reduced essential nutrients levels.
4.4 Endocrine Effects
It was also reported that presence of arsenic in air was responsible for greater incidence in breast cancer (Khanjani et al 2017). Further, the same group has reported that emissions of arsenic, lead, and mercury were linked to the prevalence of estrogen receptor (ER)-positive breast cancer (Vu et al. 2019). The gonadal endocrine system plays a vital in regulating human reproductive behaviour. Investigation by earlier researchers showed that arsenic accumulates in the gonadal tissues and induces profound inhibitory effect on the development of the gonads (Zarooogian and Hoffman 1982; Shukla and Pandey 1985). Few other investigators reported that arsenic interacts with few sex hormones and causes inhibition of ovarian steroidogenesis, spermatogenesis and also impairs testicular function (Chattopadhyay et al. 1999, 2003; Zadorozhnaja et al. 2000; da Silva et al. 2017). Arsenic have also reported to have negative effects on semen quality and quantity in males (Kim and Kim 2015) in addition to inducing menarcheal age and abortions in females (Milton et al. 2005; Sen and Chaudhuri 2008). Chow et al. (2004) reported that after a 48 h exposure to 150 µg/L of AsIII transcription of ERα was repressed while AsIII did not compete with estradiol. Subsequent studies also revealed that AsIII caused immense toxicity in estrogen production by interfering with signalling pathways (Watson and Yager 2007). It was also known that AsIII had a high affinity to the sulfhydryl groups of proteins with the formation of stable cyclic thio-arsenite complexes thereby leading to glucocorticoid dysfunction and blocking of steroids from binding to glucocorticoids. Further studies on the thyroid hormone of fish revealed that 78 hours exposure to arsenic amplified thyroxine hormone levels in fish larvae. Sun et al. (2017) found that thyroxine levels in mice, rats increased by 18% on exposure to 50 mg/L AsIII for 10 days. Allen and Rana (2007) reported that treatment of rats with 40 mg per kg of AsIII enhanced the thyroxine content from 20.1 to 52.0 nmol/L. They concluded that rodents toughened their metabolism process by elevating thyroxine levels, resulting in more removal of arsenic from their bodies. This hypothesis was substantiated by another search which reported elevated levels of thyroxine stimulated arsenic excretion through urine in rats (Rana and Allen 2006). Other workers also observed that raised levels of thyroxine modulated rat immune systems, thereby lessening the unfavorable effects of contaminants by increasing the levels of thyroxine which in turn helps to decrease the body load of arsenic (Lam et al. 2005).
4.5 Neurogenic Effects
Arsenicals are known to harshly affect the nervous system. Long-lasting exposure to arsenicals is linked to developmental neurotoxicity, neurological complications and gradual weakening of cognitive progress, learning and reminiscence (Vahidnia et al. 2007; Tolins et al 2014). Astrocytes are macroglial cells in central nervous system (CNS) derived from progenitor cells in the neuroepithelium that help form the brain’s physical structures. Astrocyes are involved in the exudation or absorption of neural transmitters and maintain the blood–brain barrier, populate the grey and white matter of the brain and spine in addition to maintaining the homeostasis of CNS (Abbot et al. 2006). Arsenicals saturate the blood–brain barrier and astrocytes are the first to counter them in the brain. Because of their strategical significant localization and high detoxification potential, astrocytes are the first line of defence against toxins which enters the brain (Dringen et al. 2016). Arsenic prevents alteration of pyruvate to acetyl coenzyme A thereby blocking the Krebs cycle and inducing neuropathy (Bjørklund et al 2020). The Agency for Toxic Substances and Disease Registry (2007) reported that Japanese kids who consumed arsenic-contaminated milk showed increased perceptive deficits, epilepsy and severe hearing loss.
4.6 Gastrointestinal Effects
Lee and Kissel (1995) stated that intake of 80 mg/kg of organic arsenicals lead to queasiness, abdominal ache, hyperactive bowel and diarrhoea and concluded that the gastrointestinal tract was the target for noxiousness following oral administration of MMA. Further investigations showed that feeding of MMA at a concentration of 72.4 mg/kg/day created pathophysiological situations in the large intestine and an upsurge in squamous metaplasia of the epithelial columnar absorptive cells in colon and rectum. Squamous metaplasia was described to exist in the colon of mice when chronically exposed to 67 mg MMA/kg per day (Gur et al. 1991; Arnold et al. 2003).Clinical manifestation of gastrointestinal irritation, like nausea, diarrhoea and occasional abdominal pain, were noticed/reported in all cases of chronic ground water arsenic contamination (Vantroyen et al. 2004; Belon et al. 2007). Chiocchetti et al. (2019a, b) described that exposure to arsenic III and V lead to production of ROS (reactive oxygen species) which thereby augmented the release of IL-8. ROS generated interfere with the proteins in tight junctions such as claudin, occluding and resulting in barrier function loss of the intestinal epithelium. Clinical investigation also established liver damage (Liu et al. 2002) and blood tests revealed elevated levels of hepatic enzymes after arsenic contamination (Belon et al. 2007; Khuda-Bukhsh et al. 2011). Histological observation of the livers of human exposed to ground water arsenic contamination revealed hepatic portal fibrosis (Mazumder 2005). Also chronic exposure to arsenic caused cirrhosis, a secondary effect of damage to the hepatic blood vessels.
4.7 Musculoskeletal Effects
Arsenic trioxide is often used to treat patients with cancer like promyelocytic leukaemia but clinical use of As2O3 has been restricted due to increased ill effects such as cardiotoxicity (Vinetha and Raghu 2019). Investigations on the muscle of tail of King prawn (Penaeus latisulcatus) revealed presence of arseno-betaine which is a water-soluble arsenic constituent. (Maher 1985; Francesconi and Edmonds 1987). It was also reported that As2O3 inhibits myogenic differentiation by inhibiting Akt-regulated signalling (Yen et al. 2010), inducing long-term muscle mitochondrial dysfunction and impaired metabolism (Ambrosio et al. 2014).
4.8 Cardiovascular Effects
High arsenic concentration in drinking water is associated with an increased prevalence of stroke. However, there are contradictory reports on the association between low concentration of arsenic in water and stroke. Ersbøll et al. (2018) conducted a study by taking into consideration 57,053 individuals from two major cities in Denmark. He found that 2195 individuals had incidence of stroke. The results proposed that the presence of arsenic even in small concentration in drinking water instigated high rate of stroke. Similar results were also revealed by another study conducted by the same group which concluded that there could be some association between the risk of myocardial infarction and low concentration of arsenic in drinking water (Milton et al. 2017; Monrad et al. 2017). Other investigators reported that chronic exposure to low-level iAs (inorganic arsenic) in drinking water was linked with amplified risk of coronary disease (James et al. 2015; Wade et al. 2015; Moon et al 2017). It is thus established that people with the highest concentration of arsenic in urine are more prone to cardiovascular disease compared to a population with low concentration of arsenic in urine.
4.9 Dermal Effects
There are several reports on the carcinogenicity of arsenic carried out in numerous countries such as Argentina, India, Taiwan, Bangladesh and Chile,where drinking water holds more than 150 ppb of arsenic (IARC 2012).
An investigation conducted by Haque et al. (2003) stated that ground water contaminated with high levels of arsenic induces skin cancer but this study was limited to few districts of West Bengal. Few external changes of chronic exposure observed through naked eyes includes pigment changes on the skin, hyperkeratosis, hyperpigmentation and patchy hyperpigmentation which may lead to malignancy. Mee’s lines which crisscrosses the nails are effects of severe or long term exposure to arsenic (Sharma et al. 2016). Patchy hyperpigmentation is commonly visible in axillae, groin, nipples, temples and neck (Dastgiri et al. 2010). “Rain Drop syndrome” which is the appearance of dark brown patches present over the chest, back, and abdomen has often been visible in inhabitants who regularly consumed 400 µg/L or more arsenic in drinking water (ATSDR 2007).
4.10 Metabolic Effects
Sattar et al. (2016) investigated arsenic’s influence on the disintegration of carbohydrates and the enzymes that participates in carbohydrate breakdown and glucose homeostasis. Once arsenic enters a mammalian body it is gathered in the liver, kidney and pancreas and shows detrimental effects on glucogenesis, gluconeogenesis by alterating and weakening the key enzymes involved in metabolism. Variation of hepatic glucose homeostasis has a major role in the pathobiology of diabetes. It is known fact that organisms have developed a complex system for the interaction of enzymes such as, Superoxide dismutase (SOD), Glutathione-s-tranferase (GST), catalase and myeloperoxidase. These enzymes are involved in the counteraction of both endogenous and exogenous oxidative stress. This array of Phase I and Phase II enzymes work stepwise to maintain a low ROS levels in the body (Wang et al. 1997; Banerjee et al. 2010). These investigators studied the effects of arsenic exposure on the human population from Murshidabad district and the concomitant levels of both enzymes. They reported that the activity of both enzymes was appreciably high in subjects exposed to arsenic compared to normal populations. They concluded that chronic arsenic exposure augmented the activity of serum catalase and myeloperoxidase due to which ROS activity increased thereby resulting in a huge amounts of DNA damage. Other investigators evaluated the association between arsenic exposure and antioxidant enzyme defence and oxidative stress in aquatic vertebrates i.e. Salmo trutta, and their investigation concluded that arsenic bioaccumulation induced lipid peroxidation and interfered with the antioxidant defence system (Greani et al. 2017).
4.11 Hematologic Effects of Arsenic
Severe or chronic arsenic intoxication leads to bone marrow depression which is manifested as pancytopenia initially. People suffering from arsenicosis often suffer from anaemia, eosinophila, leukopenia and thrombocytopenia. The above finding indicates that most studies were conducted on rural populations in India and Bangladesh who have low socioeconomic status. The anaemia varies from a normocytic or macrocytic condition with basophilic stippling being located on peripheral blood smears (Kyle and Pearse 1965; Selzer and Ancel 1983; Heck et al. 2008). It was reported by different agencies that chronic arsenic exposure or acute exposure to gaseous form of arsenic i.e. arsine gas causes intravascular haemolysis. (NRC 2000, 2001; IARC 2004).
5 Effects on Plants
Arsenic contamination hinder critical biochemical and metabolic progressions that results in plant death. A significant reduction in plant height was noticed with increasing arsenic loads in irrigation water (Majumder et al. 2019). Arsenic exposed seedlings of Cicer arietinum and Oryza sativa revealed remarkable stunted growth of roots and shoots (Malik et al. 2011; Vromman et al. 2013). Arsenic also suppresses the quantity of leaves, leaf surface area, and the fresh and dry mass of plants. Arsenic also induces chromatid and chromosomal aberrations in plants (Wu et al. 2010; Ghiani et al. 2014; Aksakal and Esin 2015) in addition to an increase in the occurrence of micro-nuclei in peripheral root tip cells of both Zea mays and Vicia faba (Duquesnoy et al. 2010).
6 Arsenic Mitigation and Management
Though arsenic calamity was reported in the early eighties true mitigation progressed slowly (Johnston et al. 2014) and hence the burden on public health remains very high. Flanagan et al. (2012) estimated that arsenic contamination alone could affect 19–20 thousand people annually in Bangladesh at >50 μg/L concentration levels. In a situation of very inadequate mitigation success, the challenge is to improve, enhance, develop and boost a sustainable and economic option that the public can adopt, install and maintain themselves. There are two main methods to eliminate arsenic from the water; one, to find an alternative source of arsenic free water and two,removal of arsenic from water through use of chemicals. It is known that water from deep wells with depths of more than 200 m is arsenic-free but what limits this process is the expense involved drawing it which most communities cannot afford. A few months after installation high amounts of metals like Mn and Fe often can cause intolerable taste and stains leading to discontinuation. Another option is the introduction of surface water bodies such as ponds and rivers after antimicrobial treatment which is also expensive and not feasible under certain climatic conditions (during rainy season). Rainwater harvesting can be implemented in areas known for arsenic contaminated ground water. A critical limitations to implementing rain water harvesting is the high installation cost and inequal rainfall over the year (Ahmed and Rahman 2003; Islam et al. 2011). Removal of arsenic by adsorption is considered a suitable option due to its simple operational procedure, less costs, sludge free operation, and regeneration and reusability of the adsorbents. Orthodox medicines such as di-mercapto succinic acid (DMSA), diethylene triamine pentaacetic acid (DTPA) and British Anti Lewisite (BAL) have been ineffective so far to treat patients suffering from arsenicosis, further they have a fluctuating efficacy and harmful side effects, hence there is a necessity for alternative agents which are cheap and can easily be procured by common masses (Chou et al. 2002; Belon et al. 2007; Biswas et al. 2019). People living in the ground water contaminated areas should be made aware to take nutritional diets with high amounts of folate, antioxidant and proteins. This natural silent calamity in the Indo-Gangetic plain especially in the region of Bengal and Bangladesh requires a sustainable solution.
7 Conclusion
Of all the heavy metal poisonings arsenic poisoning has received prominent attention especially in the Indo-Gangetic plain. Toxicity reports of arsenic are well documented and numerous molecular and cellular mechanisms have been proposed to explain arsenic’s toxicological profile. To avoid risk it is recommended that people living in arsenic contaminated ground water areas undergo regular check-ups for arsenic levels in their blood and urine. Parents should educate their children to make them aware of arsenic-related toxicity and treatment strategies (which at times may not be effective due to the genetic makeup of individual, environmental factors and diet). The review summarizes the various aspects of arsenic toxicity is intended to serve as a reference to researchers involved in elucidating mechanism of toxicity and is intended to serve as a refrence for researchers involved in studying the mechanism of arsenic toxicity, provide results for the betterment of human-kind and conservation of biodiversity.
Abbreviations
- As:
-
Arsenic
- AsIII:
-
Arsenite
- AsV:
-
Arsenate
- DMAV:
-
Dimethylarsinic
- DMAIII:
-
Dimethyl arsinous
- MMAV:
-
Monomethyl arsonic
- MMAIII:
-
Monomethyl arsonous
- ROS:
-
Reactive oxygen species
References
Abbott, N., Rönnbäck, L., & Hansson, E. (2006). Astrocyte–endothelial interactions at the blood–brain barrier. Nature Reviews Neuroscience, 7, 41–53.
Aggarwal, M., Naraharisetti, S. B., Dandapat, S., Degen, G. H., & Malik, J. K. (2008). Perturbations in immune responses induced by concurrent sub-chronic exposure to arsenic and endosulfan. Toxicology, 251(1–3), 51–60.
Ahmed, F., & Rahman, M. (2003). Low-cost water supply technologies. In: F. Ahmed & M. Rahman (Eds.), Water supply and sanitation. Rural and low-income urban Communities. ITN-Bangladesh, Dhaka, pp. 407–441.
Akram, Z., Jalali, S., Shami, S. A., Ahmad, L., Batool, S., & Kalsoom, O. (2009). Genotoxicity of sodium arsenite and DNA fragmentation in ovarian cells of rat. Toxicology Letters, 190(1), 81–85.
Aksakal, O., & Esim, N. (2015). Evaluation of arsenic trioxide genotoxicity in wheat seedlings using oxidative system and RAPD assays. Environmental Science Pollution Research International, 22(9), 7120–7128.
Allen, T., & Rana, S. V. (2007). Effect of n-propylthiouracil or thyroxine on arsenic trioxide toxicity in the liver of rat. Journal of Trace Elements in Medicine and Biology, 21(3), 194–203.
Ambrosio, F., Brown, E., Stolz, D., Ferrari, R., Goodpaster, B., Deasy, B., et al. (2014). Arsenic induces sustained impairment of skeletal muscle and muscle progenitor cell ultrastructure and bioenergetics. Free Radical Biology and Medicine, 74, 64–73.
Arnold, L. L., Eldan, M., van Gemert, M., Capen, C. C., & Cohen, S. M. (2003). Chronic studies evaluating the carcinogenicity of monomethylarsonic acid in rats and mice. Toxicology, 190(3),197–219.
ATSDR. (2007). Agency for toxic substances and disease registry. Toxicological profile for arsenic. Draft for Public Comment. Atlanta GA. www.atsdr.cdc.gov/toxprofiles.
Baastrup, R., Sørensen, M., Balstrøm, T., Frederiksen, K., Larsen, C. L., Tjønneland, A., et al. (2008). Arsenic in drinking-water and risk for cancer in Denmark. Environmental Health Perspectives, 116(2), 231–237.
Bailey, K. A., Wu, M. C., Ward, W. O., Smeester, L., Rager, J. E., García-Vargas, G., et al. (2013). Arsenic and the epigenome: Interindividual differences in arsenic metabolism related to distinct patterns of DNA methylation. Journal of Biochemical and Molecular Toxicology, 27(2), 106–115.
Banerjee, M., Banerjee, N., Ghosh, P., Das, J. K., Basu, S., Sarkar, A. K., et al. (2010). Evaluation of the serum catalase and myeloperoxidase activities in chronic arsenic-exposed individuals and concomitant cytogenetic damage. Toxicology Applied Pharmacology, 249(1), 47–54.
Banerjee, N., Banerjee, S., Sen, R., Bandyopadhyay, A., Sarma, N., Majumder, P., et al. (2009). Chronic arsenic exposure impairs macrophage functions in the exposed individuals. Journal of Clinical Immunology, 29(5), 582–594.
Belon, P., Banerjee, A., Karmakar, S. R., Biswas, S. J., Choudhury, S. C., Banerjee, P., et al. (2007). Homeopathic remedy for arsenic toxicity? Evidence-based findings from a randomized placebo-controlled double blind human trial. Science of Total Environment, 384(1–3), 141–150.
Belon, P., Banerjee, P., Choudhury, S. C., Banerjee, A., Biswas, S. J., Karmakar, S. R., et al. (2006). Can administration of potentized homeopathic remedy, Arsenicum album, alter antinuclear antibody (ANA) titer in people living in high-risk arseniccontaminated areas? I. A correlation with certain hematological parameters. Evidence-Based Complementary and Alternative Medicine, 3(1), 99–107.
Bishayi, B., & Sengupta, M. (2003). Intracellular survival of Staphylococcus aureus due to alteration of cellular activity in arsenic and lead intoxicated mature Swiss albino mice. Toxicology, 184(1), 31–39.
Bishayi, B., & Sengupta, M. (2006). Synergism in immunotoxicological effects due to repeated combined administration of arsenic and lead in mice. International Immunopharmacology., 3, 454–464.
Biswas, S. J., Ghosh, G., & Dubey, V. P. (2019). Modulation of sodium arsenite-induced toxicity in mice by ethanolic seed extract of Trigonella foenum graecum. Pharmacognosy Magazine, 15, S386-395.
Bjørklund, G., Tippairote, T., Rahaman, M. S., & Aaseth, J. (2020). Developmental toxicity of arsenic: A drift from the classical dose–response relationship. Archives of Toxicology, 94, 67–75.
Chatterjee, D., Adak, S., Banerjee, N., Bhattacharjee, P., Bandyopadhyay, A. K., & Giri, A. K. (2018). Evaluatıon of health effects, genetıc damage and telomere length ın children exposed to arsenic in West Bengal, İndia. Mutation Research Genetic Toxicology Environmental Mutagenesis, 836(Pt A), 82–88.
Chattopadhyay, S., Ghosh, S., Chaki, S., Debnath, J., & Ghosh, D. (1999). Effect of sodium arsenite on plasma levels of gonadotrophins and ovarian steroidogenesis in mature albino rats: Duration-dependent response. The Journal of Toxicological Sciences, 24(5), 425–431.
Chattopadhyay, S., Pal (Ghosh), S., Ghosh, D., & Debnath, J. (2003). Effect of dietary co-administration of sodium selenite on sodium arsenite-induced ovarian and uterine disorders in mature albino rats. Toxicological Sciences, 75(2), 412–422.
Chiocchetti, G. M., Vélez, D., & Devesa, V. (2019). Effect of chronic exposure to inorganic arsenic on intestinal cells. Journal of Applied Toxicology, 39(6), 899–907.
Chiocchetti, G. M., Vélez, D., & Devesa V. (2019b). Inorganic arsenic causes intestinal barrier disruption. Metallomics, 11(8), 1411–1418.
Chou, C. J., Tsai, M. S., Tsai, J. L., Lee, H. H., & Lin, T. J. (2002). The chelating treatment is notuseful in human’s intoxication with acute herbicidal organic arsenic. Human and Experimental Toxicology, 21(12), 631–634.
Chow, S. K., Chan, J. Y., & Fung, K. P. (2004). Suppression of cell proliferation and regulation of estrogen receptor alpha signaling pathway by arsenic trioxide on human breast cancer MCF-7 cells. Journal of Endocrinology, 182(2), 325–337.
Concha, G., Nermell, B., & Vahter, M. V. (1998). Metabolism of inorganic arsenic in children with chronic high arsenic exposure in northern Argentina. Environmental Health Perspective, 106(6), 355–359.
da Silva, R. F., Borges, C. D. S., de Almeida Lamas, C., Cagnon, V. H. A., & de Grava Kempinas, W. (2017). Arsenic trioxide exposure impairs testicular morphology in adult male mice and consequent fetus viability. Journal of Toxicology and Environment Health A, 80(19–21), 1166–1179.
Dastgiri, S., Mosaferi, M., Fizi, M. A., Olfati, N., Zolali, S., Pouladi, N., & Azarfam, P. (2010). Arsenic exposure, dermatological lesions, hypertension, and chromosomal abnormalities among people in a rural community of northwest Iran. Journal of Health Population and Nutrition, 28(1), 14–22.
De Loma, J., Skröder, H., Raqib, R., Vahter, M., & Broberg, K. (2018). Arsenite methyltransferase(AS3MT) polymorphisms and arsenic methylation in children in rural Bangladesh. Toxicology and Applied Pharmacology, 357, 80–87.
Dringen, R., Spiller, S., Neumann, S., & Koehler, Y. (2016). Uptake, metabolic effects and toxicity of arsenate and arsenite in astrocytes. Neurochemistry Research, 41(3), 465–475.
Dulout, F. N., Grillo, C. A., Seoane, A. I., Maderna, C. R., Nilsson, R., Vahter, M., et al. (1996). Chromosomal aberrations in peripheral blood lymphocytes from native Andean women and children from northwestern Argentina exposed to arsenic indrinking water. Mutation Research, 370(3–4), 151–158.
Duquesnoy, I., Champeau, G. M., Evray, G., Ledoigt, G., & Piquet-Pissaloux, A. (2010). Enzymatic adaptations to arsenic-induced oxidative stress in Zea mays and genotoxic effect of arsenic in root tips of Vicia faba and Zea mays. Comptes Rendus Biologies, 333, 814–824.
Ersbøll, A. K., Monrad, M., Sørensen, M., Baastrup, R., Hansen, B., Bach, F. W., et al. (2018). Low-level exposure to arsenic in drinking water and incidence rate of stroke: A cohort study in Denmark. Environment International, 120, 72–80.
Ferrario, D., Collotta, A., Carfi, M., Bowe, G., Vahter, M., Hartung, T., & Gribaldo, L. (2009). Arsenic induces telomerase expression and maintains telomere length in human cordblood cells. Toxicology, 260(1–3), 132–141.
Flanagan, S. V., Johnston, R. B., & Zheng, Y. (2012). Arsenic in tube well water in Bangladesh: Health and economic impacts and implications for arsenic mitigation. Bulletin of World Health Organization, 90(11), 839–846.
Francesconi, K. A., & Edmonds, J. S. (1987). The identification of arsenobetaine as the sole water-soluble arsenic constituent of the tail muscle of the western king prawn Penaeus latisulcatus. Comparative Biochemistry and Physiology C, 87(2), 345–347.
Ghiani, A., Fumagalli, P., Nguyen Van, T., Gentili, R., & Citterio, S. (2014). The combined toxic and genotoxic effects of Cd and As to plant bioindicator Trifolium repens L. PLoS One, 109(6), e99239. https://doi.org/10.1371/journal.pone.0099239.
Ghosh, D., Datta, S., Bhattacharya, S., & Mazumder, S. (2007). Long-term exposure to arsenic affects head kidney and impairs humoral immune responses of Clarias batrachus. Aquatic Toxicology, 81 (1), 79–89.
Ghosh, P., Banerjee, M., De Chaudhuri, S., Chowdhury, R., Das, J. K., Mukherjee, A., et al. (2007). Comparison of health effects between individuals with and without skin lesions in the population exposed to arsenic through drinking water in West Bengal, India. Journal of Exposure Science and Environmental Epidemiology, 17(3), 215–223.
Ghosh, P., Basu, A., Mahata, J., Basu, S., Sengupta, M., Das, J. K., et al. (2006). Cytogenetic damage and genetic variants in the individuals susceptible to arsenic-induced cancer through drinking water. International Journal of Cancer, 118(10), 2470–2478.
González-Martínez, F., Sánchez-Rodas, D., Cáceres, D. D., Martínez, M. F., Quiñones, L. A., Johnson-Restrepo, B. (2018). Arsenic exposure, profiles of urinary arsenic species, and polymorphism effects of glutathione-s-transferase and metallothioneins.Chemosphere, 212, 927–936.
Greani, S., Lourkisti, R., Berti, L., Marchand, B., Giannettini, J., Santini, J., & Quilichini, Y. (2017). Effect of chronic arsenic exposure under environmental conditionson bioaccumulation, oxidative stress, and antioxidant enzymatic defenses in wild trout Salmo trutta (Pisces, Teleostei). Ecotoxicology, 26(7), 930–941.
Gur, E., Pirak, M., & Waner, T. (1991). Methane arsonic acid oncogenicity study in the mouse. Luxembourg Industries (Pamol) Ltd. Submitted to the U.S. Environmental Protection Agency. MRID42173201.
Haque, R., Mazumder, D. N., Samanta, S., Ghosh, N., Kalman, D., Smith, M. M., et al. (2003). Arsenic in drinking water and skin lesions: Dose-response data from West Bengal, India. Epidemiology, 14(2), 174–182.
Hartmann, A., & Speit, G. (1996). Effect of arsenic and cadmium on the persistence of mutagen-induced DNA lesions in human cells. Environment and Molecular Mutagenesis, 27(2), 98–104.
Heck, J. E., Chen, Y., Grann, V. R., Slavkovich, V., Parvez, F., & Ahsan, H. (2008). Arsenic exposure and anemia in Bangladesh: A population-based study. Journal of Occupational Environmental Medicine, 50(1), 80–87.
Heck, J. E., Park, A. S., Qiu, J., Cockburn, M., & Ritz, B. (2014). Risk of leukemia in relation to exposure to ambient air toxics in pregnancy and early childhood. International Journal of Hygiene and Environ Health, 217(6), 662–668.
Hernández, A., & Marcos, R. (2008). Genetic variations associated with interindividual sensitivity in the response to arsenic exposure. Pharmacogenomics, 9(8), 1113–1132.
Huang, R. N., & Lee, T. C. (1996). Cellular uptake of trivalent arsenite and pentavalent arsenate in KB cells cultured in phosphate-free medium. Toxicology and Applied Pharmacology, 136(2), 243–249.
Huang, Y., Zhang, J., McHenry, K. T., Kim, M. M., Zeng, W., Lopez-Pajares, V., et al. (2008). Induction of cytoplasmic accumulation of p53: A mechanism for low levels of arsenic exposure to predispose cells for malignant transformation. Cancer Research, 68(22), 9131–9136.
Hughes, M. F., Devesa, V., Adair, B. M., Conklin, S. D., Creed, J. T., Styblo, M., et al. (2008). Tissue dosimetry, metabolism and excretion of pentavalent and trivalent dimethylated arsenic in mice after oral administration. Toxicology and Applied Pharmacology, 227(1), 26–35.
IARC. (2012). Monographs on the Evaluation of Carcinogenic Risks to Humans, No. 100C. IARC Working Group on the Evaluation of Carcinogenic Risk to Humans. Lyon: International Agency for Research on Cancer.
IARC. (2004). Monographs on the evaluation of carcinogenic risks to humans. Some Drinking-water Disinfectants and Contaminants, including Arsenic, 84. Lyon: IARC Scientific Publications 1-229.
Islam, M. A., Sakakibara, H., Karim, M. R., Sekine, M., & Mahmud, Z. H. (2011). Bacteriological assessment of drinking water supply options in coastal areas of Bangladesh. Journal of Water and Health, 9(2), 415–428.
James, K. A., Byers, T., Hokanson, J. E., Meliker, J. R., Zerbe, G. O., & Marshall, J. A. (2015). Association between lifetime exposure to inorganic arsenic in drinking water and coronary heart disease in Colorado residents. Environmental Health Perspectives, 123(2), 128–134.
Johnston, R., Hug, S. J., Inauen, J., Khan, N. I., Mosler, H. J., & Yang, H. (2014). Enhancing arsenic mitigation in Bangladesh: Findings from institutional, psychological, and technical investigations. Science of Total Environment, 488–489, 477–483.
Khanjani, N., Jafarnejad, A. B., & Tavakkoli, L. (2017). Arsenic and breast cancer: A systematic review of epidemiologic studies. Reviews on Environmental Health, 32(3), 267–277.
Khuda-Bukhsh, A. R., Roy-Karmakar, S., Banerjee, A., Banerjee, P., Pathak, S., Biswas, S. J., et al. (2011). A follow-up study on the efficacy of the homeopathic remedy arsenicum album in volunteers living in high risk arsenic contaminated areas. Evidence-Based Complementary and Alternative Medicine, 2011, 129214.
Kim, Y. J., & Kim, J. M. (2015). Arsenic toxicity in male reproduction and development. Development and Reproduction, 19(4), 167–180.
Kyle, R. A., & Pease, G. L. (1965). Hematologic aspects of arsenic intoxication. New England Journal of Medicine, 273, 18–23.
Lam, S. H., Sin, Y. M., Gong, Z., & Lam, T. J. (2005). Effects of thyroid hormone on the developmentof immune system in zebrafish. General and Comparative Endocrinology, 142(3), 325–335.
Lee, R. C., & Kissel, J. C. (1995). Probabilistic prediction of exposures to arsenic contaminated residential soil. Environmental Geochemistry and Health, 17(4), 159–168.
Lee-Chen, S. F., Yu, C. T., & Jan, K. Y. (1992). Effect of arsenite on the DNA repair ofUV-irradiated Chinese hamster ovary cells. Mutagenesis, 7(1), 51–55.
Lemarie, A., Bourdonnay, E., Morzadec, C., Fardel, O., & Vernhet, L. (2008). Inorganic arsenicactivates reduced NADPH oxidase in human primary macrophages through a Rhokinase/p38 kinase pathway. Journal of Immunology, 180(9), 6010–6017.
Lemarie, A., Morzadec, C., Bourdonnay, E., Fardel, O., & Vernhet, L. (2006). Human macrophagesconstitute targets for immunotoxic inorganic arsenic. Journal of Immunology, 177(5), 3019–3027.
Lin, H. J., Sung, T. I., Chen, C. Y., & Guo, H. R. (2013). Arsenic levels in drinking water and mortality of liver cancer in Taiwan. Journal of Hazardous Materials, 262, 1132–1138.
Liu, F. P., Chen, X. H., Fu, M., & Chen, Y. (2002). Determination of arsenic in animal liver by atomic fluorescence spectrometry. Guang Pu Xue Yu Guang Pu Fen Xi, 22(3), 491–492.
Lu, M., Wang, H., Li, X. F., Arnold, L. L., Cohen, S. M., & Le, X. C. (2007). Binding of dimethylarsinousacid to cys-13 alpha of rat hemoglobin is responsible for the retention of arsenic in rat blood. Chemical Research in Toxicology, 20(1), 27–37.
Maher, W. A. (1985). The presence of arsenobetaine in marine animals. Comparative Biochemistry Physiology C, 80(1), 199–201.
Majumder, B., Das, S., Mukhopadhyay, S., & Biswas, A. K. (2019). Identification ofarsenic-tolerant and arsenic-sensitive rice (Oryza sativa L.) cultivars on thebasis of arsenic accumulation assisted stress perception, morpho-biochemicalresponses, and alteration in genomic template stability. Protoplasma, 256(1), 193–211.
Malik, J. A., Goel, S., Sandhir, R., & Nayyar, H. (2011). Uptake and distribution of arsenic in chickpea: Effects on seed yield and seed composition. Communication in Soil Science and Plant Analysis, 42, 1728–1738.
Mazumder, D. N. (2005). Effect of chronic intake of arsenic-contaminated water on liver. Toxicology and Applied Pharmacology, 206(2), 169–175.
Meliker, J. R., Slotnick, M. J., AvRuskin, G. A., Schottenfeld, D., Jacquez, G. M., Wilson, M. L., et al. (2010). Lifetime exposure to arsenic in drinkingwater and bladder cancer: a population-based case-control study in Michigan, USA.Cancer Causes and Control, 21(5), 745–757.
Milton, A. H., Smith, W., Rahman, B., Hasan, Z., Kulsum, U., Dear, K., et al. (2005). Chronic arsenic exposure and adverse pregnancy outcomes in Bangladesh. Epidemiology, 16(1), 82–86.
Milton, A. H., Smith, W., Rahman, B., Hasan, Z., Kulsum, U., Dear, K., et al. (2017). Low-level arsenic in drinking water and risk of incident myocardial infarction: A cohort study. Environmental Research, 154, 318–324.
Monrad, M., Ersbøll, A. K., Sørensen, M., Baastrup, R., Hansen, B., Gammelmark, A., et al. (2017). Low-level arsenic in drinking water and risk of incident myocardial infarction: A cohort study. Environmental Research, 154, 318–324.
Moon, K. A., Oberoi, S., Barchowsky, A., Chen, Y., Guallar, E., Nachman, K. E., et al. (2017). A dose-response meta-analysis of chronic arsenic exposure and incident cardiovascular disease. International Journal of Epidemiology, 46(6), 1924–1939.
Moore, L. E., Smith, A. H., Hopenhayn-Rich, C., Biggs, M. L., Kalman, D. A., & Smith, M. T. (1997). Decrease in bladder cell micronucleus prevalence after intervention to lower the concentration of arsenic in drinking water. Cancer Epidemiology and Biomarker Prevention, 6(12), 1051–1056.
Naujokas, M. F., Anderson, B., Ahsan, H., Aposhian, H. V., Graziano, J. H., Thompson, C., et al. (2013). The broad scope of health effects from chronic arsenic exposure: Update on a worldwide public health problem. Environmental Health Perspectives, 121(3), 295–302. https://doi.org/10.1289/ehp.1205875.
Nohara, K., Ao, K., Miyamoto, Y., Suzuki, T., Imaizumi, S., Tateishi, Y., et al. (2008). Arsenite-induced thymus atrophy is mediated by cell cycle arrest: A characteristic downregulation of E2F-related genes revealed by a microarray approach. Toxicological Sciences, 101(2), 226–238.
NRC (National Research Council). (2000). Arsenic in drinking water. Washington, DC: National Academy Press.
NRC (National Research Council). (2001). Arsenic in drinking water. Washington, DC: National Academy Press.
Patterson, R., Vega, L., Trouba, K., Bortner, C., & Germolec, D. (2004). Arsenic-induced alterations in the contact hypersensitivity response in Balb/c mice. Toxicology and Applied Pharmacology, 198(3), 434–443.
Rahman, A., Vahter, M., Smith, A. H., Nermell, B., Yunus, M., El Arifeen, S., et al. (2009). Arsenic exposure during pregnancy and size at birth: A prospective cohort study in Bangladesh. American Journal of Epidemiology, 169(3), 304–312.
Rana, S. V., & Allen, T. (2006). Influence of thyroxine and n-propylthiouracil on nephro-toxicity of inorganic arsenic in rat. Toxicology and Industrial Health, 22(3), 137–145.
Rose, M., Lewis, J., Langford, N., Baxter, M., Origgi, S., Barber, M., et al. (2007). Arsenic in seaweed–forms, concentration and dietary exposure. Food Chemical Toxicology, 45(7), 1263–1267.
Rossman, T. G., Meyn, M. S., & Troll, W. (1977). Effects of arsenite on DNA repair in Escherichia coli. Environmental Health Perspectives, 19, 229–233.
Samavarchi Tehrani, S., Mahmoodzadeh Hosseini, H., Yousefi, T., Abolghasemi, M., Qujeq, D., Maniati, M., et al. (2018). The crosstalk between trace elements with DNA damage response, repair, and oxidative stress in cancer. Journal of Cellular Biochemistry, 1–26. https://doi.org/10.1002/jcb.27617.
Sattar, A., Xie, S., Hafeez, M. A., Wang, X., Hussain, H. I., Iqbal, Z., et al. (2016). Metabolism and toxicity of arsenicals in mammals. Environmental Toxicology and Pharmacology, 48, 214–224.
Savabieasfahani, M., Lochmiller, R. L., Rafferty, D. P., & Sinclair, J. A. (1998). Sensitivity of wild cotton rats (Sigmodon hispidus) to the immunotoxic effects of low-level arsenic exposure. Archives of Environmental Contamination and Toxicology, 34(3), 289–296.
Schaumlöffel, N., & Gebel, T. (1998). Heterogeneity of the DNA damage provoked by antimony and arsenic. Mutagenesis, 13(3), 281–286.
Selzer, P. M., & Ancel, M. A. (1983). Chronic arsenic poisoning masquerading as pernicious anemia. The Western Journal of Medicine, 139(2), 219–220.
Sen, J., & Chaudhuri, A. (2008). Arsenic exposure through drinking water and its effect on pregnancy outcome in Bengali women. Archives of Industrial Hygiene and Toxicology, 59(4), 271–275.
Sengupta, M., & Bishayi, B. (2002). Effect of lead and arsenic on murine macrophage response. Drug Chemical Toxicology, 25(4), 459–472.
Sharma, S., Gupta, A., Deshmukh, A., & Puri, V. (2016). Arsenic poisoning and Mees’ lines. QJM an International Journal of Medicine, 109(8), 565–566.
Shukla, N. P., & Pandey, G. N. (1985). Effect of heavy metals on fish–a review. Reviews on Environmental Health, 5(1), 87–99.
Skröder, H., Engström, K., Kuehnelt, D., Kippler, M., Francesconi, K., Nermell, B., et al. (2018). Associations between methylated metabolites of arsenic and selenium in urine of pregnant Bangladeshi women and interactions between the main genes involved. Environmental Health Perspectives, 126(2), 027001.
Soto-Peña, G. A., Luna, A. L., Acosta-Saavedra, L., Conde, P., López-Carrillo, L., Cebrián, M. E., et al. (2006). Assessment of lymphocyte subpopulations and cytokine secretion in children exposed to arsenic. Federation of American Societies for Experimental BiologyJournal, 20(6), 779–781.
Soto-Peña, G. A., & Vega, L. (2008). Arsenic interferes with the signalling transduction pathway of T cell receptor activation by increasing basal and induced phosphorylation of Lck and Fyn in spleen cells. Toxicology and Applied Pharmacology, 230(2), 216-226.
Sun, H. J., Li, S. W., Li, C., Wang, W. Q., Li, H. B., & Ma, L. Q. (2017). Thyrotoxicity of arsenate and arsenite on juvenile mice at organism, sub-cellular, and gene levels under low exposure. Chemosphere, 186, 580–587.
Tolins, M., Ruchirawat, M., & Landrigan, P. (2014). The developmental neurotoxicity of arsenic: Cognitive and behavioural consequences of early life exposure. Annals of Global Health, 80(4), 303–314.
Vahidnia, A., van der Voet, G. B., & de Wolff, F. A. (2007). Arsenic neurotoxicity–a review. Human and Experimental Toxicology, 26(10), 823–832.
Vahter, M. (2002). Mechanisms of arsenic biotransformation. Toxicology, 181–182, 211–217.
Vahter, M. E. (2007). Interactions between arsenic-induced toxicity and nutrition in early life. Journal of Nutrition, 137(12), 2798–2804.
Vantroyen, B., Heilier, J. F., Meulemans, A., Michels, A., Buchet, J. P., Vanderschueren, S., et al. (2004). Survival after a lethal dose of arsenic trioxide. Journal of Toxicology: Clinical Toxicology, 42(6), 889–895.
Vineetha, V. P., & Raghu, K. G. (2019). An overview on arsenic trioxide induced cardiotoxicity. Cardiovascular Toxicology, 19(2), 105–119.
Vromman, D., Lutts, S., Lefèvre, I., Somer, L., De Vreese, O., Šlejkovec, Z., & Quinet, M. (2013). Effects of simultaneous arsenic and iron toxicities on rice (Oryza sativa L.) development, yield-related parameters and As and Fe accumulation in relation to As speciation in the grains. Plant and Soil, 371, 199–217.
Vu, V., Navalkar, N., & Wei, Y. (2019). Endocrine disrupting metals in ambient air and female breast cancer incidence in US. Gynecological Endocrinology, 35(12), 1099–1102.
Wade, T. J., Xia, Y., Mumford, J., Wu, K., Le, X. C., Sams, E., et al. (2015). Cardiovascular disease and arsenic exposure in Inner Mongolia, China: A case control study. Environmental Health, 14, 35.
Wang, T. S., Shu, Y. F., Liu, Y. C., Jan, K. Y., & Huang, H. (1997). Glutathione peroxidase and catalase modulate the genotoxicity of arsenite. Toxicology, 121(3), 229–237.
Warner, M. L., Moore, L. E., Smith, M. T., Kalman, D. A., Fanning, E., & Smith, A. H. (1994). Increased micronuclei in exfoliated bladder cells of individuals who chronically ingest arsenic-contaminated water in Nevada. Cancer Epidemiology Biomarkers Prevention, 3(7), 583–590.
Watson, W. H., & Yager, J. D. (2007). Arsenic: Extension of its endocrine disruption potential to interference with estrogen receptor-mediated signalling. Toxicological Sciences, 98(1), 1–4.
World Health Organization (WHO). (2001) Arsenic and arsenic compounds, 2nd Edn. Environmental Health Criteria 224. Geneva CH [updated 2001; accessed August 25, 2019]. Available from: https://www.inchem.org/documents/ehc/ehc/ehc224.htm.
Wu, L., Yi, H., & Yi, M. (2010). Assessment of arsenic toxicity using Allium/Vicia root tip micro nucleus assays. Journal of Hazardous Materials, 176(1–3), 952–956.
Yamamoto, S., Konishi, Y., Matsuda, T., Murai, T., Shibata, M. A., Matsui-Yuasa, I., et al. (1995). Cancer induction by an organic arsenic compound, dimethylarsinic acid (cacodylic acid), in F344/DuCrj rats afterpre-treatment with five carcinogens. Cancer Research, 55(6), 1271–1276.
Yen, Y. P., Tsai, K. S., Chen, Y. W., Huang, C. F., Yang, R. S., & Liu, S. H. (2010). Arsenic inhibits myogenic differentiation and muscle regeneration. Environmental Health Perspectives, 118(7), 949–956.
Zadorozhnaja, T. D., Little, R. E., Miller, R. K., Mendel, N. A., Taylor, R. J., Presley, B. J., et al. (2000). Concentrations of arsenic, cadmium, copper, lead, mercury, and zinc in human placentas from two cities in Ukraine. Journal of Toxicology and Environmental Health A, 61(4), 255–263.
Zakharyan, R. A., Wildfang, E., & Aposhian, H. V. (1996). Enzymatic methylation of arseniccompounds. III. The marmoset and tamarin, but not the rhesus, monkeys are deficient in methyl transferases that methylate inorganic arsenic. Toxicology and Applied Pharmacology, 140(1), 77–84.
Zaroogian, G. E., & Hoffman, G. L. (1982). Arsenic uptake and loss in the American oyster, Crassostrea virginica. Environmental Monitoring and Assessment, 1(4), 345–358.
Zolot, J. (2016). Arsenic levels in drinking water linked to bladder cancer in News England. American Journal of Nursing, 116(8), 16.
Acknowledgements
The authors sincerely acknowledge Department of Science and Technology, Govt. of India, DST-FIST (SR/FST/LS-I/2018/173) and DBT-BOOST No.118/14/BT(Estt)/1P-4/2013 for providing infrastructural support.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Biswas, S.J. et al. (2021). Primary Concept of Arsenic Toxicity: An Overview. In: Adhikary, P.P., Shit, P.K., Santra, P., Bhunia, G.S., Tiwari, A.K., Chaudhary, B.S. (eds) Geostatistics and Geospatial Technologies for Groundwater Resources in India. Springer Hydrogeology. Springer, Cham. https://doi.org/10.1007/978-3-030-62397-5_16
Download citation
DOI: https://doi.org/10.1007/978-3-030-62397-5_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-62396-8
Online ISBN: 978-3-030-62397-5
eBook Packages: Earth and Environmental ScienceEarth and Environmental Science (R0)