Abstract
Volume overload induced by arteriovenous shunt for 4 and 16 weeks has been shown to produce sex-specific alterations in cardiac hypertrophy and heart failure, respectively. These changes were accompanied by sex-dependent alterations in the pro- and anti-apoptotic protein content and cardiomyocyte apoptosis in the heart. Cardiac hypertrophy in both male and female hearts produced a small depression in the extent of apoptosis without any change in mRNA levels for caspases 3 and 9. On the other hand, heart failure in males, unlike females, showed a marked increase in apoptosis and elevated mRNA levels for both caspase isoforms. Content for unphosphorylated and phosphorylated Bad proteins as well as Bax protein content in failing male hearts were higher than those in female hearts. Phosphorylated Bcl-2 protein content in male failing hearts were lower and that for females were higher in comparison to the respective sham control values. Increased apoptosis as well as the protein content for caspase 3, caspase 9, phosphorylated Bad and Bax in 16 weeks AV-shunt ovariectomized animals were attenuated by treatment with estrogen. AV-shunt induced alterations in Bcl-2 and phosphorylated Bcl-2 protein content in ovariectomized hearts were also prevented by estrogen treatment. These alterations in cardiomyocyte apoptosis as well as, pro-and anti-apoptotic factors in the heart may provide a possible mechanism to explain the sex-specific differences in the cardiac remodelling and cardiac function induced by volume overload.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Volume-overload
- Heart failure
- Cardiac hypertrophy
- Cardiomyocyte apoptosis
- Anti-apoptotic factors
- Pro-apoptotic factors
Introduction
Apoptosis is a tightly regulated and energy-requiring mechanism in which cell death follows a programmed sequence of structural changes including cell shrinkage, plasma membrane blebbing, nuclear condensation, DNA fragmentation, formation of apoptotic bodies in the nucleus and inflammation [1,2,3,4,5]. Various cellular stress signals including intracellular Ca2+-overload, alterations in cytokines, loss of growth factors, oxidative stress, functional hypoxia and nitric oxide are considered to participate in the occurrence of apoptosis [6,7,8,9,10,11,12,13,14,15,16]. Apoptosis, in the cell is initiated by two major pathways: (i) extrinsic/death receptor pathway via ligand binding to external death receptors and (ii) intrinsic/mitochondrial pathway near the surface of the mitochondria. These are regulated by pro- and anti-apoptotic protein content including caspases 3 and 9, Bcl-2, Bad as well as BAX, which play a critical role in the development of apoptotic cell death in the myocardium [16,17,18,19,20,21,22].
Since apoptosis causes structural deformities in the myocardium, which has a limited ability for self-renewal, an increase in the rate of cardiomyocyte apoptosis has been shown to profoundly affect cardiac contractility and induce cardiac dysfunction [23,24,25,26,27]. Contribution of this mechanism is now well known in the development of contractile heart failure due to different etiologies such as myocardial infarction [28,29,30,31,32,33,34], ischemia-reperfusion injury [35,36,37,38], pressure overload [21, 39,40,41,42,43,44], volume overload [45,46,47,48,49,50,51,52,53,54], cardiomyopathies (dilated, ischemic, toxic and hypertrophic) [24,25,26, 55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70], hypertension [34, 71, 72], as well as atherosclerosis and restenosis [73,74,75,76,77]. Although cardiac hypertrophy is considered to be an adaptive mechanism for maintaining heart function, the ongoing loss of cardiomyocytes by apoptosis may result in the transition of cardiac hypertrophy to heart failure. In view of the well known differences in the responses of male and female hearts to various stressful situations, it appears that the development of cardiac hypertrophy and heart failure are gender-dependent events. Accordingly, the present article is intended to focus discussion on whether the occurrence of cardiomyocyte apoptosis and alterations of the associated pro-and anti-apoptotic proteins in different types of heart diseases are gender-dependent. In particular, it is planned to discuss the role and mechanisms of cardiomyocyte apoptosis in male and female hearts during the development of cardiac hypertrophy and heart failure upon the induction of volume overload.
Gender Differences of Cardiomyocyte Apoptosis in Heart Disease
It is now well known that the status of cardiac function and the extent of cardiomyocyte apoptosis in healthy males are essentially not different from those in the normal female hearts. However, cardiomyocyte apoptosis and cardiac dysfunction in diverse heart diseases have been found more prevalent in men compared to women [21, 25, 31,32,33,34, 44,45,46, 78,79,80,81,82,83,84,85,86,87,88]. This could be due to the difference in the presence of apoptosis-related genes on the Y chromosomes or the role of estrogen and estrogen receptors in female population [25, 89,90,91,92,93,94]. Also, with aging the prevalence of cardiomyocyte apoptosis activity in human hearts has been found more pronounced in males than females [95,96,97,98]. In this regard, it is noteworthy that, unlike the females, a 4-fold increase in cardiomyocyte apoptosis has been described in the senescent male monkey hearts; this observation has signified the role of aging in gender differences [98].
Cardiomyocyte loss, which is invariably associated with heart failure, has been reported to exhibit gender difference [31, 99]. The extent of cardiomyocyte apoptosis was lower in female failing hearts in various heart diseases such as myocardial infarction [100], volume overload [25], pulmonary hypertension [101], and different cardiomyopathies [25, 88, 102, 103]. Improved cardiac function, and a greater reversibility of heart failure were observed in women with dilated cardiomyopathy [104,105,106]. However, the occurrence of heart failure as well as morbidity and mortality in patients with ≥20 years of age, were found to be equal in both genders [107]. Furthermore, the treatment approaches for heart failure in both males and females are similar except for using angiotensin-converting enzyme inhibitors and angiotensin receptor antagonists in females during pregnancy due to the risk of birth defects [108,109,110,111]. Nonetheless, there are dramatic sex differences with respect to heart dysfunction during the development of heart failure [112]. In comparison to males, females with heart failure have shown improved survival and were found to maintain normal left ventricular size and preserve ejection fraction when challenged with myocardial infarction [55, 93, 113,114,115,116,117,118]; atherosclerotic burden [93, 119]; and ischemia/reperfusion injury [114, 120,121,122,123,124,125,126]. In addition to, common causes including aging, pregnancy, environmental factors and lifestyle changes, there are other pathological influences such as hypertension which have shown sex differences with respect to hormonal imbalances, as well as cardiac remodeling processes, and signal transduction mechanisms for apoptosis [88, 89, 108, 127,128,129,130,131,132].
A growing number of studies have supported the view regarding gender differences for cardiomyocyte apoptosis in heart failure. Compared to men, a markedly lower extent of cardiomyocytes apoptosis was seen in the women’s failing hearts [133, 134]. In hearts of patients undergoing cardiac transplantation, a significantly lesser degree of apoptosis in female heart was observed in comparison to males, and it has been pointed out that higher cardiomyocyte death in men was associated with earlier onset of heart failure [55]. It was also reported that due to increased extent of cardiomyocyte apoptosis after myocardial infarction [100], men were at much higher risk of worsened myocardial function and cardiac rupture while women showed greater myocardial retrieve [135]. Furthermore, females were found relatively more protected than males in response to prolonged acute coronary ischemia [55, 93, 110]. It may also be noted that there is a rapid progress in the transition from cardiac hypertrophy to heart failure in males compared to females, and cardiomyocyte apoptosis may play a role at the late stage of this transition [58, 63, 136,137,138,139,140,141,142]. The development of heart failure in pathological conditions such as pressure overload [143,144,145,146,147,148,149] and volume overload [25, 150,151,152] have been observed to be slower in females compared to males. These observations indicate sex-specific differences concerning apoptosis in a wide variety of cardiovascular diseases and provide evidence that cardiomyocyte apoptosis may play an important role in determining the gender-dependent differences in the development of heart failure.
Gender Differences of Cardiomyocyte Apoptosis in Heart Failure Due to Volume Overload
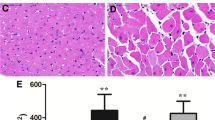
Since cardiomyocytes apoptosis plays a significant role in transition from cardiac hypertrophy to heart failure, this section is concerned with discussion on differences in cardiomyocyte apoptosis during the development of cardiac hypertrophy and heart failure induced by volume overload as a consequence of arteriovenous (AV) shunt in male and female rats [25]. Upon induction of volume overload, the degree of cardiac hypertrophy was increased and the cardiac output was unaltered, but the extent of apoptosis was depressed in both male and female hearts at early stage (4 weeks) (Fig. 7.1a). These events were not accompanied by any changes in mRNA levels for both caspase 3 or caspase 9 (Fig. 7.1b, c). On the other hand, at late stage of heart failure (16 weeks), the parameters of cardiac performance were considerably reduced in males hearts, while, these were maintained in female hearts [25]. Compared to the females, the levels of mRNA for caspase 3 and caspase 9 were higher (Fig. 7.1d, e) and extent of apoptosis was significantly greater in the male hearts (Fig. 7.1a). Furthermore, the data for different signaling transduction pathways involved in the regulation of apoptosis at 16 weeks volume overload are shown in Fig. 7.2a–e. The pro-apoptotic Bad protein content was higher in both phosphorylated and non- phosphorylated forms in male failing hearts whereas no change was seen in female volume overload hearts (Fig. 7.2a, b). The anti-apoptotic Bcl-2 protein content was remained unaltered in the non-phosphorylated form in both sexes (Fig. 7.2c) but the level of phosphorylated form was higher in female hearts and lower in male hearts upon the induction of volume overload for 16 weeks (Fig. 7.2d). Furthermore, protein content of pro-apoptotic factor BAX was higher in male failing hearts but was unaltered in the female volume overload heart (Fig. 7.2e). These results have demonstrated that the potential for the occurrence of apoptosis in the female heart is less than the male heart at the hypertrophic as well as the failing stages after the induction of volume overload. It appears that the observed decrease in the extent of apoptosis in both males and females may be due to an adaptive response to volume overload at the early stage of cardiac hypertrophy. However, the male failing heart showed a marked increase in the extent of apoptosis whereas female volume overload heart exhibited a lesser extent of apoptosis 16 weeks post AV shunt. These observations are consistent with the view that there are sex-specific differences in volume overload induced heart failure.
Sex-specific changes in apoptosis as well as mRNA levels for caspases 3 and 9 in sham and AV shunt failing (4 weeks and 16 weeks) hearts due to volume overload in male and female rats. Data are taken from our paper—Dent MR, Tappia PS, Dhalla NS. Apoptosis 15: 499–510, 2010. Erratum in: Apoptosis. 16, 757–758, 2011. *_ P < 0.05 versus sham; #_ P < 0.05 versus corresponding value for male
Sex-specific changes in Bad, phosphorylated Bad (p-Bad), Bcl-2, phosphorylated Bcl-2 (p- Bcl-2) and BAX protein content in sham and 16 weeks AV shunt hearts due to volume overload in male and female rats. Data are taken from our paper—Dent MR, Tappia PS, Dhalla NS. Apoptosis 15: 499–510, 2010. Erratum in: Apoptosis. 16, 757–758, 2011. *_ P < 0.05 versus sham; #_ P < 0.05 versus corresponding value for male
Role of Estrogen in Cardiomyocyte Apoptosis Due to Volume Overload
Several studies have been reported that cardiomyocyte apoptosis is affected by sex hormones such as estrogen, testosterone and progesterone, which exert different actions during the development of heart failure in males and females [25, 92,93,94, 120, 153,154,155,156,157,158,159,160,161,162,163]. The effects of estrogens in the females include the delay in heart failure and improved survival during the pre-menopausal period in addition to slowing down the development of left ventricular hypertrophy [112, 144, 164,165,166,167]. Moreover, in comparison to male heart, the loss of viable cardiomyocytes was found to be markedly low in the healthy aging female heart [141, 145, 167, 168]. These effects in female hearts are believed to be due to estrogens and estrogen receptors signaling, particularly mediated by the estrogen receptor-β [90, 152,153,154, 169,170,171,172]. Since sex-specific differences in cardiovascular systems have been attributed to the consequence of higher levels of estrogen, as well as the presence or absence of other hormones, which modify apoptosis and reduce the risk of heart failure in women [144], estrogen has been suggested to prevent cardiomyocyte apoptosis due to volume overload in females [25].
The extent of cardiomyocyte apoptosis was increased markedly in ovariectomized female rats upon induction of volume overload at 16 weeks (Fig. 7.3a), but was depressed upon treatment of these animals with estrogen (Fig. 7.3a). It was seen that the level of protein content for caspase 3 was increased, whereas, that for caspase 9 remained unchanged due to volume overload in ovariectomized animals. Treatment of ovariectomized volume overload rats with estrogen, protein content for both caspase 3 and caspase 9 was observed to be depressed (Fig. 7.3b, c). Alterations in different signaling transduction pathways involved in the regulation of apoptosis after inducing AV shunt in the ovariectomized rats are depicted in Fig. 7.4a–e. Induction of volume overload in ovariectomized rats were found to reduce protein content for Bcl-2 and phosphorylated Bcl-2 but increased phosphorylated Bad and BAX protein content without any changes in bad protein content (Fig. 7.4). It can also be seen from Fig. 7.4d that protein content for phosphorylated Bcl-2 was increased in sham control ovariectomized rats. Treatment of ovariectomized volume overload rats with estrogen was found to attenuate the ovariectomy-induced changes in these parameters fully or partially (Fig. 7.4). Thus, estrogen may modify both pro-apoptotic and anti-apoptotic regulatory mechanisms and prevent the occurrence of cardiomyocyte apoptosis in females. Accordingly, these observations are consistent with the view that estrogen may play an important role in determining the reduced susceptibility of females to different cardiovascular risk factor.
Changes in apoptosis as well as protein content for caspases 3 and 9 in sham and 16 weeks post AV-shunt female rats with or without ovariectomy (OVX) as well as OVX animals treated with estrogen. Data are taken from our paper – Dent MR, Tappia PS, Dhalla NS. Apoptosis 15: 499–510, 2010. Erratum in: Apoptosis. 16, 757–758, 2011. *_ P < 0.05 vs sham; †_ P < 0.05 versus corresponding value for control female; ∂_ P < 0.05 versus corresponding value for OVX animals without 17-β estradiol treatment
Changes in Bad, phosphorylated Bad (p-Bad), Bcl-2, phosphorylated Bcl-2 (p- Bcl-2), and BAX protein content in sham and 16 weeks post AV-shunt female rats with or without ovariectomy (OVX) as well as OVX animals treated with estrogen (16 weeks post AV-shunt). Data are taken from our paper – Dent MR, Tappia PS, Dhalla NS. Apoptosis 15: 499–510, 2010. Erratum in: Apoptosis. 16, 757–758, 2011. *_ P < 0.05 vs sham; †_P < 0.05 versus corresponding value for control female; ∂_P < 0.05 versus corresponding value for OVX animals without 17-β estradiol treatment
Conclusions
This study has provided evidence that cardiac hypertrophy due to induction of volume overload at early stages in both male and female rats was associated with an equal extent of depressions in cardiomyocyte apoptosis without any changes in the mRNA levels of caspase 3 and 9. However, a marked degree of apoptosis in male hearts, unlike female hearts, was evident in heart failure at late stage of volume overload. These sex-dependent differences in the cardiomyocyte apoptosis in the failing heart were associated elevated levels of mRNA for both caspase 3 and 9. Sex-specific differences in some pro-apoptotic and anti apoptotic parameters such as Bad, BAX and Bcl-2 protein content were also seen in the failing hearts due to volume overload. Volume overload in ovariectomized animals was found to increase the extent of apoptosis in association with increased levels of caspase 3 as well as BAX protein content and decreased protein of phosphorylated Bcl-2. These alterations in ovariectomized volume overload animals were partially or fully prevented by treatment with estrogen. These observations support the view that cardiomyocyte apoptosis and associated heart failure is sex-specific. Furthermore, this study provides evidence for the role of estrogen in reducing the susceptibility of female population to different cardiovascular risk factor.
References
Kerr JFR, Wyllie AH, Currie AR (1972) Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer 26:239–257
Wyllie AH, Kerr JF, Currie AR (1980) Cell death: the significance of apoptosis. Int Rev Cytol 68:251–306
Searle J, Kerr JFR, Bishop CJ (1982) Necrosis and apoptosis: distinct modes of cell death with fundamentally different significance. Pathol Annu 17:229–259
Ucker DS (1991) Death by suicide: one way to go in mammalian cellular development? New Biol 3:103–109
Arends MJ, Wyllie AH (1991) Apoptosis: mechanisms and roles in pathology. Int Rev Exp Pathol 32:223–254
Brown KA, Page MT, Nguyen C et al (1996) Tumor necrosis factor alpha-induced apoptosis in cardiac myocytes. Involvement of the sphingolipid signaling cascade in cardiac cell death. J Clin Invest 98:2854–2865
Xu YJ, Saini HK, Zhang M et al (2006) MAPK activation and apoptotic alterations in hearts subjected to calcium paradox are attenuated by taurine. Cardiovasc Res 72:163–174
Nakamura T, Ueda Y, Juan Y et al (2000) Fas-mediated apoptosis in adriamycin-induced cardiomyopathy in rats: in vivo study. Circulation 102:572–578
Azhar G, Liu L, Zhang X, Wei JY (1999) Influence of age on hypoxia/reoxygenation-induced DNA fragmentation and bcl-2, bcl-xl, bax and fas in the rat heart and brain. Mech Ageing Dev 112:5–25
Chao W, Shen Y, Li L et al (2002) Importance of FADD signaling in serum-deprivation- and hypoxia-induced cardiomyocyte apoptosis. J Biol Chem 277:31639–31645
Ing DJ, Zang J, Dzau VJ et al (1999) Modulation of cytokine-induced cardiac myocyte apoptosis by nitric oxide. Bak and Bcl-x. Circ Res 84:21–33
Bialik S, Cryns VL, Drincic A et al (1999) The mitochondrial apoptotic pathway is activated by serum and glucose deprivation in cardiac myocytes. Circ Res 85:403–414
de Moissac D, Gurevich RM, Zheng H et al (2000) Caspase activation and mitochondrial cytochrome c release during hypoxia-mediated apoptosis of adult ventricular myocytes. J Mol Cell Cardiol 32:53–63
Adams JW, Pagel AL, Means CK et al (2000) Cardiomyocyte apoptosis induced by Gαq signaling is mediated by permeability transition pore formation and activation of the mitochondrial death pathway. Circ Res 87:1180–1187
Itoh G, Tamura J, Suzuki M et al (1995) DNA fragmentation of human infarcted myocardial cells demonstrated by the nick end labeling method and DNA agarose gel electrophoresis. Am J Pathol 146:1325–1331
Bishopric NH, Andreka P, Slepak T, Webster KA (2001) Molecular mechanisms of apoptosis in the cardiac myocyte. Curr Opin Pharmacol 1:141–150
Kitsis RN, Narula J (2008) Introduction – cell death in heart failure. Heart Fail Rev 13:107–109
Hengartner MO (2000) The biochemistry of apoptosis. Nature 407:770–776
Antonsson B, Martinou JC (2000) The Bcl-2 protein family. Exp Cell Res 256:50–57
Adams JM, Cory S (1998) The Bcl-2 protein family: arbiters of cell survival. Science 281:1322–1326
Condorelli G, Morisco C, Stassi G et al (1999) Increased cardiomyocyte apoptosis and changes in proapoptotic and antiapoptotic genes bax and bcl-2 during left ventricular adaptations to chronic pressure overload in the rat. Circulation 99:3071–3078
Regula KM, Kirshenbaum LA (2005) Apoptosis of ventricular myocytes: a means to an end. J Mol Cell Cardiol 38:3–13
Tamarappoo BK, John BT, Reinier K et al (2012) Vulnerable myocardial interstitium in patients with isolated left ventricular hypertrophy and sudden cardiac death: a post-mortem histological evaluation. J Am Heart Assoc 1:1–9
Dent MR, Das S, Dhalla NS (2007) Alterations in both death and survival signals for apoptosis in heart failure due to volume overload. J Mol Cell Cardiol 43:726–732
Dent MR, Tappia PS, Dhalla NS. Gender differences in apoptotic signaling in heart failure due to volume overload. Apoptosis 15: 499–510, 2010a. Erratum in: Apoptosis 16, 757–758, 2011
Das S, Babick AP, Xu YJ et al (2010) TNF-alpha-mediated signal transduction pathway is a major determinant of apoptosis in dilated cardiomyopathy. J Cell Mol Med 14:1988–1997
Hassan AF, Kamal MM (2013) Effect of exercise training and anabolic androgenic steroids on hemodynamics, glycogen content, angiogenesis and apoptosis of cardiac muscle in adult male rats. Int J Health Sci. 7:47–60
Kajstura J, Cheng W, Reiss K et al (1996) Apoptotic and necrotic myocyte cell deaths are independent contributing variables to infarct size in rats. Lab Invest 74:86–107
Baldi A, Abbate A, Bussani R et al (2002) Apoptosis and post-infarction left ventricular remodelling. J Mol Cell Cardiol 34:165–174
Kurrelmeyer K, Michael L, Baumgarten G et al (2000) Endogenous myocardial tumor necrosis factor protects the adult cardiac myocyte against ischemic-induced apoptosis in a murine model of acute myocardial infarction. Proc Natl Acad Sci USA 290:5456–5461
Cheng W, Kajstura J, Nitahara JA et al (1996) Programmed cell death affects the viable myocardium after infarction in rats. Exp Cell Res 226:316–327
Narula J, Haider N, Virmani R et al (1996) Apoptosis in myocytes in end-stage heart failure. N Engl J Med 335:1182–1189
Olivetti G, Abbi R, Quaini F et al (1997) Apoptosis in the failing human. N Engl J Med 336:1131–1141
Mihailidou AS, Loan Le TY, Mardini M, Funder JW (2009) Glucocorticoids activate cardiac mineralocorticoid receptors during experimental myocardial infarction. Hypertension 54:1306–1312
Gottlieb R (2005) ICE-ing the heart. Circ Res 96:1036–1038
Yaoita H, Ogawa K, Maehara K et al (1998) Attenuation of ischemia/reperfusion injury in rats by a caspase inhibitor. Circulation 97:276–281
Meldrum DR, Wang M, Tsai BM et al (2005) Intracelllular signaling mechanisms of sex hormones in acute myocardial inflammation and injury. Front Biosci 10:1835–1867
Booij HG, Yu H, De Boer RA et al (2016) Overexpression of A kinase interacting protein 1 attenuates myocardial ischaemia/reperfusion injury but does not influence heart failure development. Cardiovasc Res 111:217–226
Bing OH (1994) Hypothesis: apoptosis may be a mechanism for the transition to heart failure with chronic pressure overload. J Mol Cell Cardiol 26:943–948
Fu HY, Okada K, Liao Y et al (2010) Ablation of C/EBP homologous protein attenuates endoplasmic reticulum-mediated apoptosis and cardiac dysfunction induced by pressure overload. Circulation 122:361–369
O’Connell TD, Swigart PM, Rodrigo MC et al (2006) Alpha1-adrenergic receptors prevent a maladaptive cardiac response to pressure overload. J Clin Invest 116:1005–1015
Zankov DP, Sato A, Shimizu A, Ogita H (2017) Differential effects of myocardial afadin on pressure overload-induced compensated cardiac hypertrophy. Circ J 81:1862–1870
Chen C, Zou LX, Lin QY et al (2019) Resveratrol as a new inhibitor of immunoproteasome prevents PTEN degradation and attenuates cardiac hypertrophy after pressure overload. Redox Biol 20:390–401
Gogiraju R, Hubert A, Fahrer J et al (2019) Endothelial leptin receptor deletion promotes cardiac autophagy and angiogenesis following pressure overload by suppressing Akt/mTOR signaling. Circ Heart Fail 12:1–16
Chen YW, Pat B, Gladden JD et al (2011) Dynamic molecular and histopathological changes in the extracellular matrix and inflammation in the transition to heart failure in isolated volume overload. Am J Physiol Heart Circ Physiol 300:H2251–H2260
Moorjani N, Westaby S, Narula J et al (2009) Effects of left ventricular volume overload on mitochondrial and death-receptor-mediated apoptotic pathways in the transition to heart failure. Am J Cardiol 103:1261–1268
Treskatsch S, Shakibaei M, Feldheiser A et al (2015) Ultrastructural changes associated with myocardial apoptosis, in failing rat hearts induced by volume overload. Int J Cardiol 197:327–332
Kolpakov MA, Seqqat R, Rafiq K et al (2009) Pleiotropic effects of neutrophils on myocyte apoptosis and left ventricular remodeling during early volume overload. J Mol Cell Cardiol 47:634–645
Mohamed BA, Schnelle M, Khadjeh S et al (2016) Molecular and structural transition mechanisms in long-term volume overload. Eur J Heart Fail 18:362–371
Reddy S, Zhao M, Hu DQ et al (2013) Physiologic and molecular characterization of a murine model of right ventricular volume overload. Am J Physiol Heart Circ Physiol 304:H1314–H1327
Shaqura M, Mohamed DM, Aboryag NB et al (2017) Pathological alterations in liver injury following congestive heart failure induced by volume overload in rats. PLoS ONE 12:1–19
Aboryag NB, Mohamed DM, Dehe L et al (2017) histopathological changes in the kidney following congestive heart failure by volume overload in rats. Oxid Med Cell Longev 1–10:2017
Wang X, Ren B, Liu SY et al (2003) Characterization of cardiac hypertrophy and heart failure due to volume overload in the rat. J Appl Physiol 94:752–763
Dent MR, Dhalla NS, Tappia PS (2004) Phospholipase C gene expression, protein content, and activities in cardiac hypertrophy and heart failure due to volume overload. Am J Physiol Heart Circ Physiol 287:H719–H727
Guerra S, Leri A, Wang X et al (1999) Myocyte death in the failing human heart is gender dependent. Circ Res 85:856–866
Chen SN, Lombardi R, Karmouch J et al (2019) dna damage response/tp53 pathway is activated and contributes to the pathogenesis of dilated cardiomyopathy associated with LMNA (Lamin A/C) mutations. Circ Res 124:856–873
Takagi C, Urasawa K, Yoshida I et al (1999) Enhanced GRK5 expression in the hearts of cardiomyopathic hamsters, J2N-k. Biochem Biophys Res Commun 262:206–210
Cesselli D, Jakoniuk I, Barlucchi L et al (2001) Oxidative stress-mediated cardiac cell death is a major determinant of ventricular dysfunction and failure in dog dilated cardiomyopathy. Circ Res 89:279–286
Takeda N (2003) Cardiomyopathy: molecular and immunological aspects. Int J Mol Med 11:13–26
Bennett, Martin R (2002) Apoptosis in the cardiovascular system. Heart 87:480–487
Rodrigues PG, Miranda-Silva D, Costa SM et al (2019) Early myocardial changes induced by doxorubicin in the nonfailing dilated ventricle. Am J Physiol Heart Circ Physiol 316:H459–H475
Xia Y, Chen Z, Chen A et al (2017) LCZ696 improves cardiac function via alleviating Drp1-mediated mitochondrial dysfunction in mice with doxorubicin-induced dilated cardiomyopathy. J Mol Cell Cardiol 108:138–148
Xie D, Liao Y, Wu B et al (2018) Cardiac nestin + cells derived from early stage of dilated cardiomyopathy enhanced the survival of the doxorubicin-injured cardiac muscle hl-1 cells. Int Heart J 59:180–189
Major JL, Salih M, Tuana BS (2017) E2F6 protein levels modulate drug induced apoptosis in cardiomyocytes. Cell Signal 40:230–238
Wu J, Guo W, Lin SZ et al (2016) Gp130-mediated STAT3 activation by S-propargyl-cysteine, an endogenous hydrogen sulfide initiator, prevents doxorubicin-induced cardiotoxicity. Cell Death Dis 7:1–13
Wu L, Chen Y, Chen Y et al (2019) Effect of HIF-1α/miR-10b-5p/PTEN on hypoxia-induced cardiomyocyte apoptosis. J Am Heart Assoc 8:1–15
De Angelis A, Piegari E, Cappetta D et al (2010) Anthracycline cardiomyopathy is mediated by depletion of the cardiac stem cell pool and is rescued by restoration of progenitor cell function. Circulation 121:276–292
Li Z, Bing OH, Long X et al (1997) Increased cardiomyocyte apoptosis during the transition to heart failure in the spontaneously hypertensive rat. Am J Physiol 272:H2313–H2319
Mitsuhashi S, Saito N, Watano K et al (2003) Defect of delta-sarcoglycan gene is responsible for development of dilated cardiomyopathy of a novel hamster strain, J2N-k: calcineurin/PP2B activity in the heart of J2N-k hamster. J Biochem 134:269–276
Sakamoto A, Ono K, Abe M et al (1997) Both hypertrophic and dilated cardiomyopathies are caused by mutation of the same gene, delta-sarcoglycan, in hamster: an animal model of disrupted dystrophin-associated glycoprotein complex. Proc Natl Acad Sci USA 94:13873–13878
Ren J (2007) Influence of gender on oxidative stress, lipid peroxidation, protein damage and apoptosis in hearts and brains from spontaneously hypertensive rats. Clin Exp Pharmacol Physiol 34:432–438
Liu JJ, Peng L, Bradley CJ et al (2000) Increased apoptosis in the heart of genetic hypertension, associated with increased fibroblasts. Cardiovasc Res 45:729–735
Bennett MR, Evan GI, Schwartz SM (1995) Apoptosis of human vascular smooth muscle cells derived from normal vessels and coronary atherosclerotic plaques. J Clin Invest 95:2266–2274
Moe GW, Marin-Garcia J (2016) Role of cell death in the progression of heart failure. Heart Fail Rev 21:157–167
Perlman H, Maillard L, Krasinski K et al (1997) Evidence for the rapid onset of apoptosis in medial smooth muscle cells after balloon injury. Circulation 95:981–987
Pollman MJ, Hall JL, Mann MJ et al (1998) Inhibition of neointimal cell Bcl-x expression induces apoptosis and regression of vascular disease. Nature Med 4:222–227
Shekhar A, Heeger P, Reutelingsperger C et al (2018) Targeted imaging for cell death in cardiovascular disorders. JACC Cardiovasc Imaging 11:476–493
Brill A, Torchinsky A, Carp H, Toder V (1999) The role of apoptosis in normal and abnormal embryonic development. J Assist Reprod Genet 16:512–519
Reed, Douglas R (2011) Apoptosis: physiology and pathology. John C. Green (ed) Cambridge University Press, London. 978-0-521-88656-7
Singh R, Letai A, Sarosiek K (2019) Regulation of apoptosis in health and disease: the balancing act of BCL-2 family proteins. Nat Rev Mol Cell Biol 20:175–193
Cotter TG (2009) Apoptosis and cancer: the genesis of a research field. Nat Rev Cancer 9:501–507
Mattson MP (2000) Apoptosis in neurodegenerative disorders. Nat Rev Mol Cell Bio 1:120–129
Mughal W, Dhingra R, Kirshenbaum LA (2012) Striking a balance: autophagy, apoptosis, and necrosis in a normal and failing heart. Curr Hypertens Rep 14:540–547
Teringova E, Tousek P (2017) Apoptosis in ischemic heart disease. J Transl Med 87
Favaloro B, Allocati N, Graziano V et al (2012) Role of apoptosis in disease. Aging 4:330–349
Whelan RS, Kaplinskiy V, Kitsis RN (2010) Cell death in the pathogenesis of heart disease: mechanisms and significance. Annu Rev Physiol 72:19–44
Kessler EL, Rivaud MR, Vos MA, van Veen TAB (2019) Sex-specific influence on cardiac structural remodeling and therapy in cardiovascular disease. Biol Sex Differ 10:1–11
Meyer S, van der Meer P, van Tintelen JP, van den Berg MP (2014) Sex differences in cardiomyopathies. Eur J Heart Fail 16:238–247
Winham SJ, de Andrade M, Miller VM (2014) Genetics of cardiovascular disease: importance of sex and ethnicity. Atherosclerosis 241:219–228
Pedram A, Razandi M, Lubahn D et al (2008) Estrogen inhibits cardiac hypertrophy: role of estrogen receptor-β to inhibit calcineurin. Endocrinology 149:3361–3369
Voloshenyuk TG, Gardner JD (2010) Estrogen improves TIMP-MMP balance and collagen distribution in volume-overloaded hearts of ovariectomized females. Am J Physiol Integr Comp Physiol 299:683–693
Kararigas G, Fliegner D, Gustafsson J-A, Regitz-Zagrosek V (2011) Role of the estrogen/estrogen-receptor-beta axis in the genomic response to pressure overload-induced hypertrophy. Physiol Genomics 43:438–446
Dunlay SM, Roger VL (2012) Gender differences in the pathophysiology, clinical presentation, and outcomes of ischemic heart failure. Curr Heart Fail Rep 9:267–276
Chen C, Hu LX, Dong T et al (2013) Apoptosis and autophagy contribute to gender difference in cardiac ischemia-reperfusion induced injury in rats. Life Sci 93:265–270
Tower J (2015) Programmed cell death in aging. Ageing Res Rev 23:90–100
Mallat Z, Fornes P, Costagliola R et al (2001) Age and gender effects on cardiomyocyte apoptosis in the normal human heart. J Gerontol A Biol Sci Med Sci 56:M719–M723
Olivetti G, Giordano G, Corradi D et al (1995) Gender differences and aging: effects on the human heart. J Am Coll Cardiol 26:1068–1079
Zhang XP, Vatner SF, Shen YT et al (2007) Increased apoptosis and myocyte enlargement with decreased cardiac mass; distinctive features of the aging male, but not female, monkey heart. J Mol Cell Cardiol 43:487–491
Kang PM, Izumo S (2000) Apoptosis and heart failure. A critical review of the literature. Circ Res 86:1107–1113
Biondi-Zaccai GGL, Abbate A, Bussani R et al (2005) Reduced post-infarction myocardial apoptosis in women: a clue to their different clinical course? Heart 91:99–101
Shehata ML, Lossnitzer D, Skrok J et al (2011) Myocardial delayed enhancement in pulmonary hypertension: pulmonary hemodynamics, right ventricular function, and remodeling. Am J Roentgenol 196:87–94
Fairweather DL, Cooper LT, Blauwet LA (2013) Sex and gender differences in myocarditis and dilated cardiomyopathy. Curr Probl Cardiol 38:7–46
Akdis D, Saguner AM, Shah K et al (2017) Sex hormones affect outcome in arrhythmogenic right ventricular cardiomyopathy/dysplasia: from a stem cell derived cardiomyocyte-based model to clinical biomarkers of disease outcome. Eur Heart J 38:1498–1508
Arimura T, Onoue K, Takahashi-Tanaka Y et al (2013) Nuclear accumulation of androgen receptor in gender difference of dilated cardiomyopathy due to Lamin A/C mutations. Cardiovasc Res 99:382–394
Calkins H (2015) Arrhythmogenic right ventricular dysplasia/cardiomyopathy – three decades of Progress. Circ J 79:901–913
Bauce B, Frigo G, Marcus FI et al (2008) Comparison of clinical features of arrhythmogenic right ventricular cardiomyopathy in men versus women. Am J Cardiol 102:1252–1257
Benjamin EJ, Blaha MJ, Chiuve SE et al (2017) Heart disease and stroke statistics-2017 update: a report from the american heart association. Circulation 135:1–775
Bozkurt B, Shaden K (2017) Heart failure in women. Methodist Debakey Cardiovasc J 13:216–223
Cohn JN, Tognoni G (2001) A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N Engl J Med 345:1667–1675
Pfeffer MA, Swedberg K, Granger CB et al (2003) Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet 362:759–766
Pitt B, Poole-Wilson PA, Segal R et al (2000) Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial – the losartan heart failure survival study ELITE II. Lancet 355:1582–1587
Blenck CL, Harvey PA, Reckelhoff JF, Leinwand LA (2016) the importance of biological sex and estrogen in rodent models of cardiovascular health and disease. Circ Res 118:1294–1312
Wang F, He Q, Sun Y et al (2010) Female adult mouse cardiomyocytes are protected against oxidative stress. Hypertension 55:1172–1178
Cavasin MA, Tao Z, Menon S et al (2004) Gender differences in cardiac function during early remodeling after acute myocardial infarction in mice. Life Sci 75:2181–2192
Shaw LJ, Bairey Merz CN, Pepine CJ et al (2006) Insights from the NHLBI-sponsored women’s ischemia syndrome evaluation (WISE) study: Part I: gender differences in traditional and novel risk factors, symptom evaluation, and gender-optimized diagnostic strategies. J Am Coll Cardiol 47:S4–S20
Kanaya AM, Grady D, Barrett-Connor E (2002) Explaining the sex difference in coronary heart disease mortality among patients with type 2 diabetes mellitus: a meta-analysis. Arch Intern Med 62:1737–1745
Gregg EW, Gu Q, Cheng YJ et al (2007) Mortality trends in men and women with diabetes, 1971 to 2000. Ann Intern Med 147:149–155
Taylor AL (2015) Heart failure in women. Curr Heart Failure Rep 12:187–195
Schulman-Marcus J, Hartaigh BO, Gransar H et al (2016) Sexspecific associations between coronary artery plaque extent and risk of major adverse cardiovascular events the CONFIRM long-term registry. JACC Cardiovasc Imaging 9:364–372
Wang M, Baker L, Tsai BM et al (2005) Sex differences in the myocardial inflammatory response to ischemia-reperfusion injury. Am J Physiol Endocrinol Metab 288:E321–E326
Wang M, Crisostomo PR, Markel TA et al (2008) Mechanisms of sex differences in TNFR2-mediated cardioprotection. Circulation 118:S38–S45
Wang M, Tsai BM, Kher A et al (2005) Role of endogenous testosterone in myocardial proinflammatory and proapoptotic signaling after acute ischemia-reperfusion. Am J Physiol Heart Circ Physiol 288:H221–H226
Alves MG, Machado NG, Sardao VA et al (2011) Anti-apoptotic protection afforded by cardioplegic celsior and histidine buffer solutions to hearts subjected to ischemia and ischemia/reperfusion. J Cell Biochem 112:3872–3881
Eefting F, Rensing B, Wigman J et al (2004) Role of apoptosis in reperfusion injury. Cardiovasc Res 61:414–426
Gill C, Mestril R, Samali A (2002) Losing heart: the role of apoptosis in heart disease-a novel therapeutic target? FASEB J 16:135–146
Liu H, Pedram A, Kim JK (2011) Oestrogen prevents cardiomyocyte apoptosis by suppressing p38 alpha-mediated activation of p53 and by down-regulating p53 inhibition on p38 beta. Cardiovasc Res 89:119–128
Regitz-Zagrosek V, Kararigas G (2017) Mechanistic pathways of sex differences in cardiovascular disease. Physiol Rev 97:1–37
Hartman RJG, Huisman SE, den Ruijter HM (2018) Sex differences in cardiovascular epigenetics-a systematic review. Biol Sex Differ 9:1–8
Chella Krishnan K, Mehrabian M, Lusis AJ (2018) Sex differences in metabolism and cardiometabolic disorders. Curr Opin Lipidol 29:404–410
Appelman Y, van Rijn BB, ten Haaf ME et al (2014) Sex differences in cardiovascular risk factors and disease prevention. Atherosclerosis 241:211–218
Salton CJ, Chuang ML, O’Donnell CJ, et al (2002) Gender differences and normal left ventricular anatomy in an adult population free of hypertension. A cardiovascular magnetic resonance study of the Framingham heart study offspring cohort. J Am Coll Cardiol 39:1055–1060
Sandstede J, Lipke C, Beer M et al (2000) Age- and gender-specific differences in left and right ventricular cardiac function and mass determined by cine magnetic resonance imaging. Eur Radiol 10:438–442
Narula J, Kharbanda S, Khaw BA (1997) Apoptosis and the heart. Chest 112:1358–1362
Narula J, Hajjar RJ, Dec GW (1998) Apoptosis in the failing heart. Cardiol Clin 16:691–710
Mehilli J, Ndrepepa G, Kastrati A et al (2005) Gender and myocardial salvage after reperfusion treatment in acute myocardial infarction. J Am Coll Cardiol 45:828–831
Cleland JG, Swedberg K, Follath F, et al (2003) The EuroHeart failure survey programme–a survey on the quality of care among patients with heart failure in Europe. Part 1: patient characteristics and diagnosis. Eur Heart J 24:442–463
Carroll JD, Carroll EP, Feldman T et al (1992) Sex-associated differences in left ventricular function in aortic stenosis of the elderly. Circulation 86:1099–1107
Rohini A, Agrawal N, Koyani CN, Singh R (2010) Molecular targets and regulators of cardiac hypertrophy. Pharmacol Res 61:269–280
Petrov G, Regitz-Zagrosek V, Lehmkuhl E et al (2010) Regression of myocardial hypertrophy after aortic valve replacement: faster in women? Circulation 122:S23–S28
Dent MR, Tappia PS, Dhalla NS (2011) Gender differences in beta-adrenoceptor system in cardiac hypertrophy due to arteriovenous fistula. J Cell Physiol 226:181–186
Crabbe DL, Dipla K, Ambati S et al (2003) Gender differences in post-infarction hypertrophy in end-stage failing hearts. J Am Coll Cardiol 41:300–306
Regitz-Zagrosek V, Seeland U (2011) Sex and gender differences in myocardial hypertrophy and heart failure. Wien Med Wochenschr 161:109–116
Schipke J, Grimm C, Arnstein G et al (2016) Cardiomyocyte loss is not required for the progression of left ventricular hypertrophy induced by pressure overload in female mice. J Anat 229:75–81
Fliegner D, Schubert C, Penkalla A et al (2010) Female sex and estrogen receptor-beta attenuate cardiac remodeling and apoptosis in pressure overload. Am J Physiol Regul Integr Comp Physiol 298:R1597–R1606
Aurigenvna GP, Gaasch WH (1995) Gender differences in older patients with pressure-overload hypertrophy of the left ventricle. Cardiol 86:310–317
Villari B, Campbell SE, Schneider J et al (1995) Sex-dependent differences in left ventricular function and structure in chronic pressure overload. Eur Heart J 16:1410–1419
Weinberg EO, Thienelt CD, Katz SE et al (1999) Gender differences in molecular remodeling in pressure overload hypertrophy. J Am Coll Cardiol 34:264–273
Previlon M, Pezet M, Vinet L et al (2014) Gender-specific potential inhibitory role of Ca2+/calmodulin dependent protein kinase phosphatase (CaMKP) in pressure-overloaded mouse heart. PLoS ONE 9:1–12
Douglas PS, Katz SE, Weinberg EO et al (1998) Hypertrophic remodeling: gender differences in the early response to left ventricular pressure overload. J Am Coll of Cardiol 32:1118–1125
Gardner JD, Brower GL, Janicki JS (2002) Gender differences in cardiac remodeling secondary to chronic volume overload. J Card Fail 8:101–107
Beaumont C, Walsh-Wilkinson E, Drolet MC et al (2017) Female rats with severe left ventricle volume overload exhibit more cardiac hypertrophy but fewer myocardial transcriptional changes than males. Sci Rep 7:729
Dent MR, Tappia PS, Dhalla NS (2010) Gender differences in cardiac dysfunction and remodeling due to volume overload. J Card Fail 16:439–449
Van Eickels M, Grohe C, Cleutjens JP et al (2001) 17 β-estradiol attenuates the development of pressure-overload hypertrophy. Circulation 104:1419–1423
Skavdahl M, Steenbergen C, Clark J et al (2005) Estrogen receptor-β mediates male-female differences in the development of pressure overload hypertrophy. Am J Physiol Circ Physiol 288:H469–H476
Patten RD, Pourati I, Aronovitz MJ et al (2008) 17-Estradiol differentially affects left ventricular and cardiomyocyte hypertrophy following myocardial infarction and pressure overload. J Card Fail 14:245–253
Gardner JD, Murray DB, Voloshenyuk TG et al (2010) Estrogen attenuates chronic volume overload induced structural and functional remodeling in male rat hearts. Am J Physiol Heart Circ Physiol 298:H497–H504
Bouma W, Noma M, Kanemoto S et al (2010) Sex-related resistance to myocardial ischemia-reperfusion injury is associated with high constitutive ARC expression. Am J Physiol 298:H1510–H1517
Huang C, Gu H, Zhang W et al (2010) Testosterone-down-regulated Akt pathway during cardiac ischemia/reperfusion: a mechanism involving BAD, Bcl-2 and FOXO3a. J Surg Res 64:1–11
Appiah D, Schreiner PJ, Demerath EW et al (2016) Association of age at menopause with incident heart failure: a prospective cohort study and meta-analysis. J Am Heart Assoc 5:1–10
Schonfelder G (2005) The biological impact of estrogens on gender differences in congestive heart failure. Cardiovasc Res 67:573–574
Rossouw JE (2002) Hormones, genetic factors, and gender differences in cardiovascular disease. Cardiovasc Res 53:550–557
Wang M, Wang Y, Weil B et al (2009) Estrogen receptor beta mediates increased activation of PI3K/Akt signaling and improved myocardial function in female hearts following acute ischemia. Am J Physiol Regul Integr Comp Physiol 296:R972–R978
Richards RG, Di Augustine RP, Petrusz P et al (1996) Estradiol stimulates tyrosine phosphorylation of the insulin-like growth factor-1 receptor and insulin receptor substrate-1 in uterus. Proc Natl Acad Sci USA 93:12002–12007
Mendelsohn ME, Karas RH (1999) The protective effects of estrogen on the cardiovascular system. N Engl J Med 340:1801–1811
Mahmoodzadeh S, Fliegner D, Dworatzek E (2012) Sex differences in animal models for cardiovascular diseases and the role of estrogen. Handb Exp Pharmacol 214:23–48
Regitz-Zagrosek V, Oertelt-Prigione S, Seeland U, Hetzer R (2010) Sex and gender differences in myocardial hypertrophy and heart failure. Circ J 74:1265–1273
Ponikowski P, Voors AA, Anker SD et al (2016) 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 37:2129–2200
Olivetti G, Melissari M, Capasso JM, Anversa P (1991) Cardiomyopathy of the aging human heart. Myocyte loss and reactive cellular hypertrophy. Circ Res 68:1560–1568
Mahmoodzadeh S, Eder S, Nordmeyer J et al (2006) Estrogen receptor alpha up-regulation and redistribution in human heart failure. FASEB J 20:926–934
Mendelsohn ME (2002) Genomic and nongenomic effects of estrogen in the vasculature. Am J Cardiol 90:3F–6F
Ventetuolo CE, Ouyang P, Bluemke DA et al (2011) Sex hormones are associated with right ventricular structure and function: the MESA-right ventricle study. Am J Respir Crit Care Med 183:659–667
Kuroski De Bold ML (1999) Estrogen, natriuretic peptides and the reninangiotensin system. Cardiovasc Res 41:524–531
Acknowledgments
The infrastructure support for this project was provided by the St. Boniface Hospital Research Foundation, Winnipeg, Canada.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Bhullar, S.K., Shah, A.K., Dhalla, N.S. (2020). Sex-Specific Differences of Apoptosis in Heart Failure Due to Volume-Overload. In: Ostadal, B., Dhalla, N.S. (eds) Sex Differences in Heart Disease. Advances in Biochemistry in Health and Disease, vol 21. Springer, Cham. https://doi.org/10.1007/978-3-030-58677-5_7
Download citation
DOI: https://doi.org/10.1007/978-3-030-58677-5_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-58676-8
Online ISBN: 978-3-030-58677-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)