Abstract
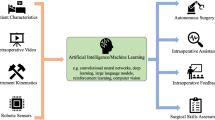
Artificial intelligence (AI) is the study of algorithms that give machines the ability to reason and perform cognitive functions. Applications of AI in medicine broadly and surgery, more specifically, have grown over the last few years as technology has advanced and clinical data has become more digitally accessible. It is becoming more important for surgeons to develop a fundamental understanding of the common techniques, applications, limitations, and ethical considerations of AI in surgery. This chapter provides an overview of AI for surgeons and describes ways in which surgeons can play a role in future development of AI applications.
Similar content being viewed by others
References
Bellman R. An introduction to artificial intelligence: can computers think? Thomson Course Technology; 1978.
Administration USF & D, U.S. Food & Drug Administration. FDA permits marketing of artificial intelligence-based device to detect certain diabetes-related eye problems. Case Med Res. 2018. https://doi.org/10.31525/fda2-ucm604357.htm.
Hashimoto DA, Rosman G, Rus D, Meireles OR. Artificial intelligence in surgery: promises and perils. Ann Surg. 2018;268(1):70–6.
Hashimoto DA, Witkowski E, Gao L, Meireles O, Rosman G. Artificial intelligence in anesthesiology. Anesthesiology. 2019;132:379. https://doi.org/10.1097/aln.0000000000002960.
Avanzolini G, Barbini P, Gnudi G. Unsupervised learning and discriminant analysis applied to identification of high risk postoperative cardiac patients. Int J Biomed Comput. 1990;25(2–3):207–21. https://doi.org/10.1016/0020-7101(90)90010-r.
DiPietro R, Hager GD. Unsupervised learning for surgical motion by learning to predict the future, vol. 2018. Medical Image Computing and Computer Assisted Intervention – MICCAI; 2018. p. 281–8. https://doi.org/10.1007/978-3-030-00937-3_33.
Skinner BF. The behavior of organisms: an experimental analysis. B. F. Skinner Foundation; 1990.
Silver D, Schrittwieser J, Simonyan K, et al. Mastering the game of go without human knowledge. Nature. 2017;550(7676):354–9.
Hebb DO. The organization of behavior. Taylor and Francis; 2005. https://doi.org/10.4324/9781410612403.
Natarajan P, Frenzel JC, Smaltz DH. Demystifying big data and machine learning for healthcare. Taylor and Francis; 2017. https://doi.org/10.1201/9781315389325.
Esteva A, Robicquet A, Ramsundar B, et al. A guide to deep learning in healthcare. Nat Med. 2019;25(1):24–9.
Grzybowski A, Brona P, Lim G, et al. Artificial intelligence for diabetic retinopathy screening: a review. Eye. 2019. https://doi.org/10.1038/s41433-019-0566-0.
Esteva A, Kuprel B, Novoa RA, et al. Dermatologist-level classification of skin cancer with deep neural networks. Nature. 2017;542(7639):115–8.
Rodas NL, Padoy N. Augmented reality for reducing intraoperative radiation exposure to patients and clinicians during x-ray guided procedures. In: Mixed and augmented reality in medicine. CRC Press; 2018. p. 217–29. https://doi.org/10.1201/9781315157702-15.
Nadkarni PM, Ohno-Machado L, Chapman WW. Natural language processing: an introduction. J Am Med Inform Assoc. 2011;18(5):544–51.
Hughes KS, Zhou J, Bao Y, Singh P, Wang J, Yin K. Natural language processing to facilitate breast cancer research and management. Breast J. 2020;26(1):92–9.
Zunic A, Corcoran P, Spasic I. Sentiment analysis in health and well-being: systematic review. JMIR Med Inform. 2020;8(1):e16023.
Shen F, Larson DW, Naessens JM, Habermann EB, Liu H, Sohn S. Detection of surgical site infection utilizing automated feature generation in clinical notes. Int J Healthc Inf Syst Inform. 2019;3(3):267–82.
Healey MA, Shackford SR, Osler TM, Rogers FB, Burns E. Complications in surgical patients. Arch Surg. 2002;137(5):611–7; discussion 617–618.
Lee TH, Marcantonio ER, Mangione CM, et al. Derivation and prospective validation of a simple index for prediction of cardiac risk of major noncardiac surgery. Circulation. 1999;100(10):1043–9.
Gupta PK, Gupta H, Sundaram A, et al. Development and validation of a risk calculator for prediction of cardiac risk after surgery. Circulation. 2011;124(4):381–7.
POISE Study Group, Devereaux PJ, Yang H, et al. Effects of extended-release metoprolol succinate in patients undergoing non-cardiac surgery (POISE trial): a randomised controlled trial. Lancet. 2008;371(9627):1839–47.
Wijeysundera DN, Pearse RM, Shulman MA, et al. Assessment of functional capacity before major non-cardiac surgery: an international, prospective cohort study. Lancet. 2018;391(10140):2631–40.
Wolters U, Wolf T, Stützer H, Schröder T. ASA classification and perioperative variables as predictors of postoperative outcome. Br J Anaesth. 1996;77(2):217–22.
Owens WD, Felts JA, Spitznagel EL Jr. ASA physical status classifications: a study of consistency of ratings. Anesthesiology. 1978;49(4):239–43.
Bilimoria KY, Liu Y, Paruch JL, et al. Development and evaluation of the universal ACS NSQIP surgical risk calculator: a decision aid and informed consent tool for patients and surgeons. J Am Coll Surg. 2013;217(5):833–42.e1–e3.
Corey KM, Kashyap S, Lorenzi E, et al. Development and validation of machine learning models to identify high-risk surgical patients using automatically curated electronic health record data (Pythia): a retrospective, single-site study. PLoS Med. 2018;15(11):e1002701.
Bihorac A, Ozrazgat-Baslanti T, Ebadi A, et al. MySurgeryRisk: development and validation of a machine-learning risk algorithm for major complications and death after surgery. Ann Surg. 2019;269(4):652–62.
Bertsimas D, Dunn J, Velmahos GC, Kaafarani HMA. Surgical risk is not linear. Ann Surg. 2018;268(4):574–83. https://doi.org/10.1097/sla.0000000000002956.
Birkmeyer JD, Stukel TA, Siewers AE, Goodney PP, Wennberg DE, Lucas FL. Surgeon volume and operative mortality in the United States. ACC Curr J Rev. 2004;13(2):59. https://doi.org/10.1016/j.accreview.2003.12.065.
Birkmeyer JD, Finks JF, O’Reilly A, et al. Surgical skill and complication rates after bariatric surgery. N Engl J Med. 2013;369(15):1434–42.
Bonrath EM, Gordon LE, Grantcharov TP. Characterising “near miss” events in complex laparoscopic surgery through video analysis. BMJ Qual Saf. 2015;24(8):516–21. https://doi.org/10.1136/bmjqs-2014-003816.
Krizhevsky A, Sutskever I, Hinton GE. ImageNet classification with deep convolutional neural networks. Commun ACM. 2017;60(6):84–90. https://doi.org/10.1145/3065386.
Hashimoto DA, Rosman G, Witkowski ER, et al. Computer vision analysis of intraoperative video: automated recognition of operative steps in laparoscopic sleeve gastrectomy. Ann Surg. 2019;270(3):414–21.
Kannan S, Yengera G, Mutter D, Marescaux J, Padoy N. Future-state predicting LSTM for early surgery type recognition. IEEE Trans Med Imaging. 2019. https://doi.org/10.1109/TMI.2019.2931158.
Kitaguchi D, Takeshita N, Matsuzaki H, et al. Real-time automatic surgical phase recognition in laparoscopic sigmoidectomy using the convolutional neural network-based deep learning approach. Surg Endosc. 2019. https://doi.org/10.1007/s00464-019-07281-0.
Twinanda AP, Yengera G, Mutter D, Marescaux J, Padoy N. RSDNet: learning to predict remaining surgery duration from laparoscopic videos without manual annotations. IEEE Trans Med Imaging. 2019;38(4):1069–78.
Mascagni P, Fiorillo C, Urade T, et al. Formalizing video documentation of the Critical View of Safety in laparoscopic cholecystectomy: a step towards artificial intelligence assistance to improve surgical safety. Surg Endosc. 2019. https://doi.org/10.1007/s00464-019-07149-3.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this entry
Cite this entry
Filicori, F., Meireles, O.R. (2021). Artificial Intelligence in Surgery. In: Lidströmer, N., Ashrafian, H. (eds) Artificial Intelligence in Medicine. Springer, Cham. https://doi.org/10.1007/978-3-030-58080-3_171-1
Download citation
DOI: https://doi.org/10.1007/978-3-030-58080-3_171-1
Received:
Accepted:
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-58080-3
Online ISBN: 978-3-030-58080-3
eBook Packages: Springer Reference MedicineReference Module Medicine